Abstract
Purpose
Our and other’s studies showed that administration of neuropeptide galanin may mitigate insulin resistance via promoting glucose transporter 4 (GLUT4) expression and translocation in rats. The objective of this study is to investigate whether galanin receptor 2 (GAL2-R) in brain mediates the ameliorative effect of galanin on insulin resistance in adipose tissues of type 2 diabetic rats.
Methods
In this study galanin, GAL2-R agonist M1145 and GAL2-R antagonist M871 were respectively or cooperatively injected into intracerebroventricles of type 2 diabetic rats once a day for successive fifteen days. Then the plasma and fat tissues of rats were used to estimate the alterations of insulin resistance indexes.
Results
The central administration of galanin enhanced 2-deoxy-[3H]-d-glucose, peroxisome proliferator-activated receptor γ and adiponectin levels, food intake and body weight, GLUT4 mRNA expression and GLUT4 concentration in plasma membranes, as well as homeostasis model assessment-insulin resistance index. Those effects of galanin may be blocked by M817, and imitated by M1145 except for food intake and body weight.
Conclusion
Those results suggest that central GAL2-R mediates the beneficial effects of galanin on insulin sensitivity in type 2 diabetic rats. GAL2-R agonist may be taken as a potential antidiabetic agent to treat insulin resistance and type 2 diabetes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There is an upward trend in the incidence of insulin resistance and type 2 diabetes mellitus (T2DM) worldwide [1]. The characteristic of insulin resistance is an obstacle to glucose uptake, resulting in hyperglycemia. Despite considerable researches into the etiology, the precise mechanism for insulin resistance and T2DM remains elusive. Both endocrine and life-style factors are the vital etiology of the disorders.
Galanin is a 29/30 amino-acid neuropeptide, widely expressed in the endocrine, digestive and nervous systems. This peptide and its three G-protein coupled receptor subtypes, GAL1-3R play multiple regulative roles in food intake, body weight, pain threshold, antidepression, and hormone release [2,3,4]. The results of recent studies show that galanin plays important roles in amelioration of insulin resistance under the diabetic conditions. First, plasma galanin levels in healthy volunteers, type 2 diabetic patients and pregnant women with gestational diabetes mellitus are positively correlated with the blood glucose level, which is a direct reflection of insulin sensitivity [5]. Second, animals with abnormal plasma galanin levels take more risks to suffer T2DM [6]. Third, mice with knockout galanin gene manifested impaired glucose disposal, resulting from a decrease in insulin response and insulin-independent glucose elimination during a glucose tolerance test [7]. While the homozygous C57BL/6J mice with transgenic galanin gene exhibited an increase in lipid and carbohydrate metabolic rates, as well as insulin sensitivity [8]. Fourth, our previous studies showed that administration of M35, a galanin antagonist, reduced 2-deoxy-[3H]-d-glucose (2-DG) content in adipocytes and myocytes, and glucose infusion rates in a hyperinsulinemic-euglycemic clamp test, which was a direct assessment of insulin sensitivity in subjects [9,10,11]. Finally, an intracerebroventricular (i.c.v.) injection of galanin or GAL1-R agonist, M617 into diabetic rats, reliably and robustly stimulated caloric intake, body weight, blood non-esterified fatty acids content, glucose transporter 4 (GLUT4) mRNA and protein expression in adipocytes, but reduced blood glucose levels [12], suggesting that administration of galanin increased body weight and ameliorated insulin resistance of animals via activation of central GAL1-R.
Among three known galanin subtype receptors, GAL2-R is particularly attractive to be taken as a possible anti-diabetic candidate since GAL2-R, not GAL1-R, does not mediate the stimulative effects of galanin on appetite and body weight of subjects [2]. In the brain, the high levels of GAL2-R are found in the hypothalamus, the amygdala, the piriform cortex, the dentate gyrus, and the mammillary nuclei. To date, it is unclear whether central GAL2-R mediates the alleviative effect of galanin on insulin resistance in adipose tissue. Therefore, in this study we armed to investigate the central effects of GAL2-R antagonist M871 (WTLNSAGYLLGPEHPPPALALA-amide) and agonist M1145 (RGRGNWTLNSAGYLLGPVLPPPALALA-amide) on insulin resistance in the diabetic rats.
Materials and methods
Drugs and reagents
Galanin, 2-deoxy-[3H]-d-glucose (2DG) and streptozotocin were acquired from Sigma-Aldrich Inc, USA. Trizol reagent from Gibco Invitrogen, USA. M871 and M1145 were obtained from Tocris Cookson Inc, USA. Adiponectin and insulin ELISA kits from Uscn Life Science Inc, Wuhan, China. HRP-conjugated secondary antibody from Boster Inc, Wuhan, China. Antibodies against GLUT4 and peroxisome proliferator-activated receptor-γ (PPARγ) were obtained from Santa Cruz Biotechnology Inc, USA. Antibodies against β-actin from Jinqiao Inc, Beijing, China.
Diabetic animals
All studies were performed on freely moving male Wistar rats weighing 150 ± 10 g and coming from Yangzhou University Animal Center. The rats were housed in group on a 12:12-h light–dark cycle ad libitum with high-fat food (59% fat, 21% protein and 20% carbohydrate) and water in a controlled condition of 22 ± 2 °C and 50–60% humidity. Eight weeks later, 30 mg/kg streptozocin in 0.1 mM citrate buffer (pH 4.5) was intraperitoneally injected into the rats under a fasting state [9]. After another four weeks animals with fast blood glucose level over 11.1 mmol/l were used in this experiment as diabetic models. The body weight and food intake of the animals were recorded once a week. All experimental procedures for animal were conducted according to the guidelines of principles for care and use of experimental animals, and the study was approved by Ethics Committee of Yangzhou University.
Forty diabetic rats were employed in this experiment, randomly distributed into five groups of eight each: diabetic control, diabetic group with galanin, diabetic group with M1145, diabetic group with M871, diabetic group with galanin + M871. In addition, eight rats fed with high-fat food with normal glucose levels were set up as healthy controls.
Intracerebroventricular injection
The animals were anesthetized with 50 mg/kg amobarbital sodium (i.p.) and mounted on a stereotaxic instrument, and one stainless steel guide cannula was positioned to the lateral ventricle [12]: anterior–posterior (AP), −0.8 mm; V, 3.3 mm; and L, 1.4 mm, and was fixed to the skull with four jeweler’s screws and sealed with an obturator. The rats were allowed to recover from surgery for 7 days. Then galanin (1 nmol), M871 (1 nmol) and M1145 (1 nmol) in 0.5 µL artificial cerebrospinal fluid (in mM: 133.3 NaCl, 3.4 KCl, 1.2 MgCl2, 1.3 CaCl2, 32.0 NaHCO3, 0.6 NaH2 PO4 and 3.4 glucose, pH 7.4 by 0.5 M hydrochloric acid) were administered alone or in combination into lateral ventricles of rats in four drug groups. The reagent dosages used were replicated according to previously published researches [13, 14]. The administration of reagents were carried out once a day at 9:00–10:00 am for successive 15 days. An equivalent volume of vehicle was injected into rats in two control groups. Fasted for 24 h after the last injection, all rats were intraperitoneally treated with 250 mg kg−1 2DG. At 30 min thereafter, all rats were euthanized, and their artery blood and epididymal fat pad were rapidly collected and stored at –80 °C for further analysis.
HOMA index
The blood glucose and insulin levels were respectively monitored using a glucometer (HMD Biomedical, Taiwan) and competitive insulin ELISA kits as the manufacturer’s description. The homeostasis model assessment-insulin resistance index (HOMA) were calculated by blood glucose levels (mmol/l) × insulin levels (mU/ml)/22.5. The mean of double measurements was considered.
Quantitative real-time PCR
Total RNA was set up with Trizol reagent from adipose tissue following the manufacturer’s instructions [11, 15]. After determination of RNA contents by spectrophotometric assays of 260/280 nm, cDNA was synthesized from 1 μg RNA using MMLV reverse transcriptase. Quantitative PCR was performed for GLUT4 mRNA levels using a real-time PCR instrument (Exicycler™ 96, LG company, Korea). Specific primers were made up as follows: GLUT4 5′-ACAGGGCAAGGATGGTAGA-3′ and 5′-TGGAGGGGAACAAGAAAGT-3′, β-actin 5′-GGCTGTGTTGTCCCTGTATG-3′ and 5′-AATGTCACGCACGATTTCC-3′. The real-time PCR assays included an initial 95 °C × 10 min, followed by 40 × (95 °C × 30 s, 60 °C × 30 s, 72 °C × 60 s). The results were expressed in arbitrary units normalized to the expression levels of the internal control, β-actin.
Subcellular fractionation of adipose tissue
Sucrose-gradient centrifugation was used to separate membrane fractions from fat homogenates [11]. In brief, the epididymal fat pads were washed, minced and homogenized at 4 °C in buffer. Then the homogenate was centrifuged at 13,000g for 20 min at 4 °C. The 2DG uptake was measured with part of the supernatant. The remains were centrifuged (31,000g, 60 min, 4 °C) to yield intracellular membranes. The pellet was layered on a 25% and 50% sucrose gradient and re-centrifuged (75,000g, 60 min, 4 °C). The pellet was re-spun (39,000g, 20 min, 4 °C) to yield plasma membranes.
Measurement of plasma adiponectin levels
According to the manufacturer’s specification, the adiponectin contents were quantified by using adiponectin ELISA kits. All measurements were performed in duplicate and the mean of the two measurements was considered.
Western blot analysis
Western blot analyses were used to analyze the PPARγ and GLUT4 levels in the fat tissues [16]. Briefly, 50 mg samples from subcellular fractions were separated with 12% SDS-PAGE and transferred to a nitrocellulose membrane. The membranes were probed with primary antibodies against PPARγ or GLUT4, and subsequently with a HRP-conjugated secondary antibody. The immunoreactive bands were visualized by chemiluminescence and quantified by densitometry using a HPIAS-2000 image analysis system (Champion images, China).
Statistical analysis
All parametric data were presented as mean ± SEM. The significant differences between the means of six groups were evaluated via one-way ANOVA, followed by a post-hoc Tukey multiple comparisons test. The discrepancies in food intake and body weight between before and after the experiments were compared by paired Student’s t test. Significance was accepted at the P < 0.05 level.
Results
Food intake and body weight
As showed in Table 1, food intake and weight gain after the experiment increased by 12.6% (P < 0.01) and 20.3% (P < 0.01) in the galanin group compared with the diabetic controls, but reduced by 12.2% (P < 0.05) and 15.2% (P < 0.01) in the galanin + M871 group compared with the galanin group, respectively. The difference of both indexes in the M1145 or M871 group compared with diabetic controls was non-significant. Before and after the experiment the food intake was higher, but the weight gain was lower in the diabetic control group than the healthy control group. The both indexes in the galanin and M1145 groups were higher after the experiment than that before.
HOMA index
Compared with the diabetic controls, the blood glucose and insulin levels, and HOMA index significantly attenuated by 43.8% (P < 0.01), 32.1% (P < 0.01) and 61.4% (P < 0.01) in the galanin group, and by 37.1% (P < 0.01), 30.9% (P < 0.01) and 56.1% (P < 0.01) in the M1145 group respectively as shown in Table 2. In addition, the glucose and insulin levels, and HOMA index in the galanin + M871 group increased by 78.3% (P < 0.01), 22.3% (P < 0.01) and 155.9% (P < 0.01) compared with the galanin group. The three indexes were higher in the diabetic control group than the healthy controls.
2DG uptake
The central administration of galanin significantly stimulated glucose uptake in adipocytes. Compared with diabetic controls, the 2DG uptake enhanced by 41.32% (P < 0.01) and 28.5% P < 0.01) in the galanin- and M1145-treated groups, but reduced by 15.2% (P < 0.05) in the M817-treated group (Fig. 1). The beneficial effects of galanin were blunted by the administration of M817. In the galanin + M817 group the 2DG uptake significantly decreased by 36.8% (P < 0.01) compared with the galanin group, but insignificantly increased 18.6% (P > 0.05) compared with the M817 group. The 2DG uptake was lower in the diabetic control group than the healthy controls (P < 0.01) in adipose cells.
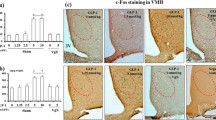
The i.c.v. administration of galanin and M1145 significantly elevated 2DG levels in adipocytes (n = 8). Compared with the diabetic controls (DC), the 2DG contents were increased in the galanin- and M1145-treated groups, but reduced in the M817-treated group. In the galanin + M817 group the 2DG uptake was significantly decreased compared with the galanin-injected group, but insignificantly increased compared with the M817 group. The 2DG uptake was lower in the diabetic control group than healthy controls in adipocytes. The data shown are the means ± SEM. ●●P < 0.01 vs. healthy controls (HC); ○P < 0.05, ○○P < 0.01 vs. DC; + +P < 0.01 vs. galanin group (Gal)
Plasma PPARγ levels
Compared with the diabetic controls, the PPARγ concentration increased by 28.5% (P < 0.01) and 18.6% (P < 0.05) in the galanin and M1145 groups, but reduced by 23.5% (P < 0.05) in the M817 group as shown in Fig. 2. In the galanin + M871 group the PPARγ level reduced by 18.1% (P < 0.01) compared with the galanin group, but insignificantly increased 20.9% (P > 0.05) compared with the M817 group. The concentration was lower in the diabetic control group than healthy controls (P < 0.01) in adipose cells.
The PPARγ levels were significantly elevated after central administration of galanin and M1145 in adipocytes of the type 2 diabetic rats (n = 8). Compared with the diabetic controls (DC), the PPARγ contents were increased in the galanin- and M1145-treated groups, but reduced in the M817-treated group. In the galanin + M817 group the levels were significantly decreased compared with the galanin-injected group, but insignificantly increased compared with the M817 group. The levels were lower in the diabetic control group than healthy controls in adipocytes. The data shown are the means ± SEM. ●●P < 0.01 vs. healthy controls (HC); ○P < 0.05, ○○P < 0.01vs. DC; ++P < 0.01 vs. galanin group (Gal)
Plasma adiponectin levels
The plasma adiponectin concentration increased by 34.4% (P < 0.01) and 22.8% (P < 0.01) in the galanin and M1145 groups, but reduced by 11.4% (P < 0.05) in the M817 group compared with diabetic controls (Fig. 3). In the galanin + M871 group the adiponectin concentration reduced by 27.1% (P < 0.01) compared with the galanin group, but insignificantly increased 10.1% (P > 0.05) compared with the M817 group. The index was lower in the diabetic control group than healthy controls (P < 0.01) in adipose cells.
The i.c.v. administration of galanin and M1145 significantly elevated adiponectin concentration in the rats (n = 8). The plasma adiponectin concentration was higher in the galanin- and M1145-treated groups, but lower in the M871-treated groups than diabetic controls (DC). The concentration was lower in the galanin + M817 group than the galanin group, and in the diabetic control group than healthy controls. The data shown are the means ± SEM. ●●P < 0.01 vs. healthy controls (HC); ○P < 0.05, ○○P < 0.01vs. DC; ++P < 0.01 vs. galanin group (Gal)
GLUT4 contents in cell membranes
In the present study, the i.c.v. treatment of galanin and M1145 significantly elevated GLUT4 protein levels in both total cell membranes and plasma membranes (Fig. 4a), as well as the ratios of the GLUT4 levels in plasma membranes to total cell membranes (Fig. 4b) of adipose cells. Compared with the diabetic controls, the GLUT4 immunoreactivities in the galanin and M1145 groups were respectively elevated by 13.1% (P < 0.05) and 12.8% (P < 0.05) in total cell membranes, and by 65.5% (P < 0.01) and 49.1% (P < 0.01) in plasma membranes, as well as by 46.3% (P < 0.01) and 32.1% (P < 0.01) in their ratios, but reduced by 12.9% (P < 0.05) in total cell membranes, by 33.2% (P < 0.01) in plasma membranes and 23.3% (P < 0.01) in their ratios in the M817-treated group, respectively. The galanin-induced increase in both total cell membranes and plasma membranes as well as their ratios were reversed by co-administration of M871. The GLUT4 levels in the galanin + M871 group were decreased by 12.2% (P < 0.05) in the total cell membranes and by 48.1% (P < 0.01) in the plasma membranes, as well as by 40.8% (P < 0.01) in their ratios compared with the galanin group. The GLUT4 contents in both membranes and their ratios in diabetic controls were significantly lower (P < 0.01) than healthy controls.
The i.c.v. injection of galanin and M1145 boosted GLUT4 expression and trafficking in adipocytes (n = 8). The central treatment with galanin and M1145 elevated GLUT4 immunoreactivity in plasma membranes and in intracellular membranes of adipocytes as well as their ratios compared with the diabetic controls (DC), but treatment with M817 reduced the immunoreactivity in both membranes and their ratios. The immunoreactivity in both membranes and their ratios were lower in the galanin + M871 and DC groups than the galanin and healthy control (HC) groups, respectively. The sum of the GLUT4 concentration in plasma membranes and in intracellular membranes was calculated as the GLUT4 concentration of total cell membranes. The data shown are the means ± SEM. ●●P < 0.01 vs. non-diabetic control (NC); ○P < 0.05, ○○P < 0.01 vs. DC; +P < 0.05, ++P < 0.01 vs. galanin group (Gal)
GLUT4 mRNA expression
In the current study, we measured the GLUT4 mRNA expression in adipose cells using real-time PCR (Fig. 5). Compared with diabetic controls, central injection of galanin or M1145 significantly augmented GLUT4 mRNA expression by 19.6% (P < 0.05) and 18.2% (P < 0.05), but reduced by 19.8% (P < 0.05) in the M817 group, respectively. The GLUT4 mRNA expression decreased by 19.8% (P < 0.05) in the galanin + M871 group compared with the galanin group, but insignificantly increased 16.8% (P > 0.05) compared with the M817 group. Again, the index in the diabetic control group was significantly lower than the healthy controls (P < 0.01) in adipose cells.
The i.c.v. injection of galanin and M1145 significantly increased GLUT4 mRNA expression in adipocytes (n = 8). The GLUT4 mRNA levels were higher in the galanin- and M1145-treated groups, but lower in the M871-treated groups than diabetic controls (DC). The expression was lower in the galanin + M817 group than the galanin group, and in the diabetic control group than healthy controls. The data shown are the means ± SEM. ●●P < 0.01 vs. healthy control (HC); ○P < 0.05 vs. DC; ++P < 0.01 vs. galanin group (Gal)
Discussion
It is well known that adipose tissue is not only a fat depot as our past view, but also an important endocrine organ to regulate energy homeostasis and insulin sensitivity via discharge of adipokines [17, 18]. Adipose tissue undertakes only 10% of insulin-stimulated glucose uptake, but it is important to regulate whole-body insulin sensitivity and energy homeostasis, as the GLUT4 expression is especially down-regulated in adipose tissue, not in skeletal muscle during the progression of insulin resistance [12]. The disorder of lipid metabolism is closely relative to impaired insulin sensitivity as fatty acids can disturb insulin signaling [10, 19]. In the present study, we collected the adipose tissues of diabetic animals as the experimental samples to evaluate the effect of galanin system on insulin sensitivity from various aspects.
The first, HOMA index offers a indirect assessment of insulin sensitivity and β-cell function in laboratory and clinic via determination of fasting glucose and insulin levels, and presents the glucose-insulin homeostasis in the fasting state. The second, 2DG is an analog of glucose via removal of each oxygen atom from double positions of the hydroxyl group [19, 20]. This prevents it is metabolized through glycolysis as glucose does after its transportation into cells. Therefore, the quantity of trapped 2DG in cells reflects glucose uptake ability and insulin sensitivity. The third, PPARγ can promote glucose utilization via enhancing triglyceride decomposition, phosphatidylinositol 3-kinase and GLUT4 gene expression [19]. The PPARγ gene knockout mice showed decreased insulin sensitivity [21], and deletion of PPARγ from brain resulted in reduced food intake and increased energy expenditure. The fourth, adiponectin is secreted by adipose tissue to promote glucose metabolism and to inhibit the oxidative stress response [22, 23]. The plasma adiponectin content is negatively correlative to plasma insulin and triglyceride levels, as well as severity of obesity and insulin resistance [24]. The adiponectin-knockout mice [adipo(−/−)] exhibited moderate insulin resistance and impaired hepatic insulin signaling pathway [25]. The fifth, GLUT4 is responsible for the insulin-induced glucose intake. It is acknowledged that after transported onto the cell surface from intracellular storage organelles only, GLUT4 can move glucose into cells. So the GLUT4 levels in plasma membranes of cells mirrors glucose clearance ability and insulin sensitivity. The last, the GLUT4 mRNA level presents a change in GlLUT4 synthesis rather than its half-life [10]. The streptozotocin-dependent changes in the GLUT4 mRNA level occur much more rapidly in adipose tissue than in skeletal muscle [26].
The results from the present experiment revealed that the central administration of galanin or M1145 significantly increased HOMA index, 2DG uptake, PPARγ and adiponectin levels, and GLUT4 mRNA expression as well as the GLUT4 contents in plasma membrane, suggesting that injection of galanin or M1145 not only enhances GLUT4 mRNA expression, but also accelerates GLUT4 translocation onto plasma membranes in adipose cells. Moreover, administration of M817 blocked the galanin-induced above events. These results implicate that the beneficial effects of galanin on insulin sensitivity may be mimicked by GAL2-R agonist and blocked by GAL2-R antagonist, i.e., the beneficial effects of galanin on insulin sensitivity may be mediated via activation of its type 2 receptor.
A great deal of studies demonstrate that galanin as an orexigenic peptide can stimulate food intake and body weight in satiated rats [27]. Besides, injection of GAL1-R agonist M617 markedly increased acute consumption of high-fat milk too [27]. While the central injection of GAL2-R agonist M1153 and M1145, or GAL2-R antagonist M871, did not impact food intake, body weight and c-Fos expression in rats and mice [27, 28]. The feeding behavior and body weight were indifferent between GAL2-R knockout mice and wild mice [29]. In line with these, the present results showed that central injection of M1145 and M871 did not affect food intake and body weight in rats, suggesting that galanin through activation of GAL1-R, not GAL2-R, motivated the high appetitive behavior. As not stimulating appetite and body weight, GAL2-R agonist is more suitable to treat insulin resistant and T2DM than galanin and GAL1-R agonist.
The difference for appetite behavior between GAL1-R and GAL2-R may involve their disparate signal pathways. Activation of GAL1-R inhibits adenyl cyclase and decrease the cAMP level through Gi/o receptors, whereas excitation of GAL2-R activates hydrolysis of inositol phosphate and atypical protein kinase C through the Gq/11 pathway to enhance intracellular Ca2+ concentration [30] or activation of the MAPK/ERK pathway via PKC in hippocampal neurons and microglial cells of rodents [30, 31]. It is essential for us to further explore which one (s) of the pathways refers to the ameliorative effect of GAL2-R on insulin resistance in the future.
In short, the current results showed that the central administration of galanin and M1145 enhanced HOMA index, 2DG uptake, PPARγ and adiponectin levels, GLUT4 protein and mRNA expression, as well as GLUT4 translocations to cellular surface in adipose cells. The mitigative effects of galanin on insulin resistance may be mimicked by M1145 and antagonized by M817, suggesting that activation of central GAL2-R can alleviate insulin resistance of the diabetic rats. The central injection of M1145 was unable to stimulate food intake and body weight of animals. This character of central GAL2-R are attractive for developing GAL2-R agonist as a promising agent to mitigate insulin resistance and T2DM.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- 2DG:
-
2-Deoxy-[3H]-d-glucose
- GAL1-R:
-
Galanin receptor 1
- GAL2-R:
-
Galanin receptor 2
- GLUT4:
-
Glucose transporter 4
- HOMA:
-
Homeostasis model assessment-insulin resistance
- M1145:
-
GalR2 agonist
- M817:
-
GalR2 antagonist
- PPARγ:
-
Peroxisome proliferator-activated receptor γ
- T2DM:
-
Type 2 diabetes
References
Malecki MT (2004) Type 2 diabetes mellitus and its complications: from the molecular biology to the clinical practice. Rev Diabet Stud 1:5–8. https://doi.org/10.1038/nm724
Webling KE, Runesson J, Bartfai T, Langel Ü (2012) Galanin receptors and ligands front endocrinol (Lausanne) 3:146–152. https://doi.org/10.3389/fendo.2012.00146
Sean P, Flynn H, White S (2015) Regulation of glucose and insulin release following acute and repeated treatment with the synthetic galanin analog nax-5055. Neuropeptides 50:35–42. https://doi.org/10.1016/j.npep.2015.01.001
Anselmi L, Salvatore L, Jr S, Lakhter A, Hirano A, Tonini M, Sternini C (2005) Galanin receptors in the rat gastrointestinal tract. Neuropeptides 39:349–352
Zhang Z, Gu C, Fang P, Shi M, Wang Y, Peng Y, Bo P, Zhu Y (2014) Endogenous galanin as a novel biomarker to predict gestational diabetes mellitus. Peptides 54:186–189. https://doi.org/10.1016/j.peptides.2014.01.024
Legalkis IN (2005) The role of galanin in metabolic disorders leading to type 2 diabetes mellitus. Drug News Perspect 18:173–177. https://doi.org/10.1358/dnp.2005.18.3.892762
Ahren B, Pacini G, Wynick D, Wierup N, Sundler F (2004) Loss-of-function mutation of the galanin gene is associated with perturbed islet function in mice. Endocrinology 145:3190–3196. https://doi.org/10.1210/en.2003-1700
Poritsanos NJ, Mizuno TM, Lautatzis ME, Vrontakis M (2009) Chronic increase of circulating galanin levels induces obesity and marked alterations in lipid metabolism similar to metabolic syndrome. Int J Obes (Lond) 33:1381–1389. https://doi.org/10.1038/ijo.2009.187
Guo LL, Shun XL, He B, Fang PH, Bo P, Zhu Y, Zhang ZW (2019) Cooperation between galanin and insulin in facilitating glucose transporter 4 translocation in adipose cells of diabetic rats. J Biol Regul Homeost Agents 33:1327–1335
Zhang Z, Fang P, Guo L, He B, Shi M, Zhu Y, Bo P (2017) Akt2-dependent beneficial effect of galanin on insulin-induced glucose uptake in adipocytes of diabetic rats. Cell Physiol Biochem 41:1777–1787. https://doi.org/10.1159/000471870
Zhang Z, Sheng S, Guo L, Li G, Zhang L, Zhang L, Shi M, Bo P, Zhu Y (2012) Intracerebroventricular administration of galanin antagonist sustains insulin resistance in adipocytes of type 2 diabetic trained rats. Mol Cell Endocrinol 361(1–2):213–218. https://doi.org/10.1016/j.mce.2012.04.012
Zhang Z, Fang P, He B, Guo L, Runesson J, Langel Ü, Shi M, Zhu Y, Bo P (2016) Central administration of galanin receptor 1 agonist boosted insulin sensitivity in adipose cells of diabetic rats. J Diabetes Res 2016:9095648–9095657. https://doi.org/10.1155/2016/9095648
Amorim D, David-Pereira A, Marques P, Puga S, Rebelo P, Costa P, Pertovaara A, Almeida A, Pinto-Ribeiro F (2014) A role of supraspinal galanin in behavioural hyperalgesia in the rat. PLoS ONE 9(11):e113077. https://doi.org/10.1371/journal.pone.0113077.eCollection2014
Fang P, He B, Yu M, Shi M, Zh ZZ, Ping B (2018) Central galanin receptor 2 mediates galanin action to promote systemic glucose metabolism of type 2 diabetic rats. Biochem Pharmacol 156:241–247. https://doi.org/10.1016/j.bcp.2018.08.036
Yue Q, Melissa F, Herbert H (2016) Y2 receptor signalling in NPY neurons controls bone formation and fasting induced feeding but not spontaneous feeding. Neuropeptides 55:91–97. https://doi.org/10.1016/j.npep.2015.09.009
Guillot TS, Richardson JR, Wang MZ, Li YJ, Taylor TN, Ciliax BJ, Zachrisson O, Mercer A, Miller GW (2008) PACAP38 increases vesicular monoamine transporter 2 (VMAT2) expression and attenuates methamphetamine toxicity. Neuropeptides 42:423–434. https://doi.org/10.1016/j.npep.2008.04.003
McGown C, Birerdinc A, Younossi ZM (2014) Adipose tissue as an endocrine organ. Clin Liver Dis 18:41–58. https://doi.org/10.1016/j.cld.2013.09.012
Harwood HJ Jr (2012) The adipocyte as an endocrine organ in the regulation of metabolic homeostasis. Neuropharmacology 63:57–75. https://doi.org/10.1016/j.neuropharm.2011.12.010
Lu M, Sarruf DA, Talukdar S, Sharma S, Li P, Bandyopadhyay G, Nalbandian S, Fan W, Gayen JR, Mahata SK, Webster NJ, Schwartz MW, Olefsky JM (2011) Brain PPAR-γ promotes obesity and is required for the insulin-sensitizing effect of thiazolidinediones. Nat Med 17:618–622. https://doi.org/10.1038/nm.2332
Bonen A, Dohm GL, van Loon LJ (2006) Lipid metabolism, exercise and insulin action. Essays Biochem 42:47–59. https://doi.org/10.1042/bse0420047
Zhang J, Tang Q, Liang GY, Liu DR, Wang F, Wu Q, Yao G, Zhang DS (2013) Influence of siRNA-mediated PPARgamma gene knockdown on insulin resistance induced by myocardial ischemia-reperfusion in rats. Sichuan Da Xue Xue Bao Yi Xue Ban 44:891–896
Qi Y, Takahashi N, Hileman SM, Patel HR, Berg AH, Pajvani UB, Scherer PE, Ahima RS (2004) Adiponectin acts in the brain to decrease body weight. Nat Med 10:524–529. https://doi.org/10.1038/nm1029
Maeda N, Shimomura I, Kishida K, Nishizawa H, Matsuda M, Nagaretani H, Furuyama N, Kondo H, Takahashi M, Arita Y, Komuro R, Ouchi N, Kihara S, Tochino Y, Okutomi K, Horie M, Takeda S, Aoyama T, Funahashi T, Matsuzawa Y (2002) Diet-induced insulin resistance in mice lacking adiponectin/ACRP30. Nat Med 8:731–737. https://doi.org/10.1038/nm724
Li Y, Yatsuya H, Iso H, Toyoshima H, Tamakoshi K (2012) Inverse relationship of serum adiponectin concentration with type 2 diabetes mellitus incidence in middle-aged Japanese workers: six-year follow-up. Diabetes Metab Res Rev 28:349–356. https://doi.org/10.1002/dmrr.2277
Kubota N, Terauchi Y, Yamauchi T, Kubota T, Moroi M, Matsui J, Eto K, Yamashita T, Kamon J, Satoh H, Yano W, Froguel P, Nagai R, Kimura S, Kadowaki T, Noda T (2002) Disruption of adiponectin causes insulin resistance and neointimal formation. J Biol Chem 277:25863–25866. https://doi.org/10.1074/jbc.C200251200
Guo L, Fang P, Yu M, Shi M, Bo P, Zhang Z (2014) Central alarin ameliorated insulin resistance of adipocytes in type 2 diabetic rats. J Endocrinol 223:217–225. https://doi.org/10.1530/JOE-14-0102
Saar I, Runesson J, McNamara I, Jrv J, Robinson JK, Langel Ü (2011) Novel galanin receptor subtype specific ligands in feeding regulation. Neurochem Int 58:714–720. https://doi.org/10.1016/j.neuint.2011.02.012
Man PS, Lawrence CB (2008) The effects of galanin-like peptide on energy balance, body temperature and brain activity in the mouse and rat are independent of the GALR2/3 receptor. J Neuroendocrinol 20:128–137. https://doi.org/10.1111/j.1365-2826.2007.01625.x
Gottsch ML, Zeng H, Hohmann JG, Weinshenker D, Clifton DK, Steiner RA (2005) Phenotypic analysis of mice deficient in the type 2 galanin receptor (GAL1-R). Mol Cell Biol 25:4804–4811. https://doi.org/10.1128/MCB.25.11.4804-4811.2005
Lang R, Gundlach AL, Kofler B (2007) The galanin peptide family: receptor pharmacology, pleiotropic biological actions, and implications in health and disease. Pharmacol Ther 115:177–207. https://doi.org/10.1016/j.pharmthera.2007.05.009
Ifuku M, Okuno Y, Yamakawa Y, Izumi K, Seifert S, Kettenmann H, Noda M (2011) Functional importance of inositol-1,4,5-triphosphate-induced intracellular Ca2+ mobilization in galanin-induced microglial migration. J Neurochem 117:61–70. https://doi.org/10.1111/j.1471-4159.2011.07176.x
Acknowledgements
This work was supported by open projects of Zoonosis Key Laboratory of Jiangsu Province (R1504), Natural Scientific Fund of Jiangsu Traditional Chinese Medicine Office (YB2015138), Natural Scientific Fund of the Anhui Higher Education Institutions of China (KJ2017A427), Six top talent project of Jiangsu Province (WSN-113), Science and Technology Program of Chuzhou College (zrjz2019013) and 2018 visiting research project of key teachers of the Anhui Higher Education Institutions of China (gxgnfx2018048).
Author information
Authors and Affiliations
Contributions
ZZ contributed to the design and writing of the manuscript. BH, PF, LG and PB were involved in conduct/data collection and critical analysis.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This study was approved by Ethics Committee of Yangzhou University.
Informed consent
Informed consent was obtained from all participants included in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Guo, L., He, B., Fang, P. et al. Activation of central galanin receptor 2 mitigated insulin resistance in adipocytes of diabetic rats. J Endocrinol Invest 44, 515–522 (2021). https://doi.org/10.1007/s40618-020-01336-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-020-01336-z