Abstract
Skin fibrosis is a common pathological process characterized by fibroblast proliferation and excessive deposition of extracellular matrix. However, the pathogenesis of the disease is still not clear. Previous studies have shown that microRNA-21 may play pivotal roles in the regulation of a variety of skin fibrosis, including keloid, scleroderma, and hypertrophic scar. In this review, we outline the structure, expression, and regulation of microRNA-21 and its role in fibrotic skin diseases. In future, it may be useful as a prognostic or diagnostic marker. However, there is a significant amount of work required to increase our current understanding of the role of microRNA-21 in skin fibrosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
MicroRNA-21/Smad7 and microRNA-21/PTEN/AKT signaling pathways may play crucial roles in the proliferation and transdifferentiation of keloid fibroblasts. |
MicroRNA-21/PTEN/AKT signaling pathway may participate in the regulation of epithelial-mesenchymal transition of keloid keratinocytes. |
MicroRNA-21 can regulate cell proliferation and apoptosis of fibroblasts in systemic sclerosis by targeting Bcl2 and Smad7. |
MicroRNA-21 regulates the cell growth of hypertrophic scar fibroblast via PTEN/PI3K/AKT, transforming growth factor-β/microRNA-21/Smad7, and microRNA-21/transforming growth factor-β2 signaling pathways. |
1 Introduction
Fibrosis is characterized by fibroblast proliferation, excessive synthesis, and deposition of extracellular matrix (ECM) [1]. Skin fibrosis is a common fibrotic disease, which includes scleroderma, hypertrophic scar, keloid, and graft- vs. -host disease [2]. It often affects the patients’ appearance; thus, they may experience social and occupational discrimination. These diseases will finally develop into organ dysfunction, greatly affecting the quality of patients’ lives [3,4,5] and bringing an enormous healthcare burden to the families of patients and society (Table 1). However, the specific mechanism of skin fibrosis is still not completely clear.
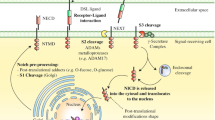
Fibroblast activation is a key link in skin fibrosis (Fig. 1) [18]. Chronic inflammation, infection, autoimmune and allergic reactions, and skin damage owing to radiation or chemical injury may induce uncontrolled proliferation of fibroblasts [19, 20]. Persistent activation of skin fibroblasts promotes the synthesis of ECM, which is mainly composed of collagen, elastin, non-collagen glycoprotein, and proteoglycan. Excessive ECM deposition in the dermis results in skin fibrosis [21, 22]. A variety of cytokines and growth factors such as transforming growth factor (TGF)-β, connective tissue growth factor, and platelet-derived growth factor can stimulate the activation of fibroblasts, of which TGF-β1 is the most important profibrotic cytokine [23]. Transforming growth factor-β can promote the proliferation of fibroblasts, regulate the synthesis of ECM, inhibit the degradation of ECM, and stimulate the transformation of fibroblasts into muscle fibroblasts by chemoattracting inflammatory cells [18]. Transforming growth factor-β/Smad signaling pathway has been shown to play a key role in a variety of fibrotic diseases [24].
MicroRNAs (miRNAs) are endogenous non-coding RNAs consisting of 18–22 nucleotides that inhibit messenger RNA (mRNA) translation or promote mRNA degradation by partial complementarity recognizing and binding to the 3′ untranslated region of target mRNAs [25]. Therefore, miRNAs regulate protein-coding gene expression, participating in different biological processes such as differentiation, propagation, apoptosis, and metastasis [26]. Previous studies have shown that miRNAs have a crucial role in pathological wound healing and may be closely related to the development and progression of skin fibrosis [27, 28]. In recent years, studies have focused on the effects of miRNA-21 (miR-21) on skin fibrosis [29]. Studies have shown that the overexpression of miR-21 plays a vital role in the biological progress of multiple fibrotic diseases; therefore, miR-21 is expected to become a biomarker for the diagnosis and treatment of fibrotic diseases [30,31,32].
2 Literature Research
We performed a comprehensive search for studies related to regulation mechanisms of miR-21 in various skin fibrotic diseases using databases including PubMed, EMBASE, and China National Knowledge Infrastructure. The keywords used were microRNA-21, miRNA-21, miR-21 and scleroderma, systemic sclerosis, graft-versus-host disease, GVHD, hypertrophic scar, and keloid. For this review, original articles were further identified by manual searching. Articles published up to March 2017 were included with the focus on key animal and human studies related to skin fibrosis.
3 Results
We retrieved 102 articles and a total of 72 articles were screened after duplicates were removed. Checking of title and abstract was conducted and 42 papers were irrelevant to skin fibrosis. Finally, we included 30 articles that met inclusion criteria in this review.
4 Biogenesis of MicroRNA-21
4.1 Characteristics of MicroRNA-21
The gene encoding for the human pri-miR-21 is located at 17q23.2, within an intron of the transmembrane protein 49 (TMEM49) gene. Although pri-miR-21 is located in the overlapping region of the TMEM49 gene intron, pri-miR-21 has its own promoter and poly-A tail. The promoter region of miR-21 is located 900 bp upstream of the transcription start site. There are possible binding sites of activated protein 1 (AP-1), CCAAT enhancer binding protein α, nuclear factor-I, serum response factor, p53, signal transducer and activator of transcription factor 3, and other transcription factors in this region. It is reported that AP-1 and signal transducer and activator of transcription factor 3 promote the transcription of miR-21, and nuclear factor-I and CCAAT enhancer binding protein α inhibit the transcription of miR-21 [33,34,35].
4.2 Regulation of MicroRNA-21 Expression
Lin et al. [37] found that the expression of miR-21 was upregulated in vascular smooth muscle cells after reactive oxygen species treatment [36]. In addition, miR-21 can reduce hydrogen peroxide-induced apoptosis. Programmed cell death protein 4 (PDCD4) is a direct target of miR-21, and inhibits its expression. AP-1 is the downstream signaling molecule of PDCD4, and is a transcription factor of miR-21 that can also promote the expression of miR-21. It is therefore possible to regulate the expression of miR-21 at the transcriptional level by PDCD4 and AP-1, forming a self-feedback regulatory pathway [38,39,40].
MicroRNA-21 can be induced by bone morphogenetic protein-4 and TGF-β [41, 42]. R-Smad knockout prevents the inhibitory action of bone morphogenetic protein-4 and TGF-β on the expression of mature miR-21 and pre-miR-21, but did not affect the transcription of pri-miR-21. Further studies showed that bone morphogenetic protein-4 and TGF-β increased the expression of pre-miR-21 and mature miR-21 at the post-transcriptional level by promoting the processing of the Drosha enzyme [43].
5 Functions of MicroRNA-21 in Skin Fibrosis
5.1 Keloid
Keloid is a benign skin tumor characterized by abnormal proliferation of fibroblasts and excessive ECM deposition [44, 45]. This disease often occurs subsequent to a burn, surgery, or trauma and the keloid often extends beyond the original incision and can progressively enlarge in size. The pathogenesis of keloid is complicated, and still remains unclear [46]. Compared with a hypertrophic scar, a keloid has a more obvious family genetic predisposition [47]. Growing evidence shows miRNA plays an important role in regulating the proliferation of fibroblasts and the excessive deposition of collagen, proteoglycan, and glycoprotein [48, 49].
5.1.1 MicroRNA Expression Profiles in Keloid
The miRNA differential expression profiles of keloids have been explored in keloid tissue, fibroblasts, and serum [49,50,51,52,53,54,55]. Wu et al. [51] found 17 differentially expressed miRNAs in four keloid tissue samples compared with three normal skin samples using miRNA microarrays. In another study of 12 pairs of keloid tissues and corresponding normal skin tissues, a total of 32 differentially expressed miRNAs were screened [50]. Using a miRNA polymerase chain reaction array consisting of 88 miRNAs, miRNA expression patterns were evaluated in three keloid samples compared with three normal skin samples [52]. Interestingly, the abnormal expression of hsa-miR-21 was detected in all three studies. Accordingly, we speculate that miR-21 may play a key role in the development of keloid scarring.
5.1.2 Role of MicroRNA-21 in Keloid
The miR-21/SMAD7 pathway mediates collagen I synthesis in keloid-derived fibroblasts. Li et al. [56] found that miR-21 was downregulated and SMAD7 was upregulated by irradiation (Fig. 2). Therefore, miR-21 was negatively correlated with SMAD7 in keloid. A further study showed SMAD7 was a direct target of miR-21. Moreover, SMAD7 controls synthesis of type I collagen by mediating p38 phosphorylation [56]. Zhou et al. [31] also reported that miR-21 promoted collagen production in keloid by negatively regulating the expression of SMAD7. They also found miR-21 mimics enhanced the expression of Col1A1, Col3A1 by downregulating SMAD7.
Interaction between microRNA-21 and relevant signaling pathways in the regulation of keloid, systemic sclerosis, and hypertropic scar. AKT AKT serine/threonine kinase, Bax BCL2-associated X, Bcl2 B-cell leukemia/lymphoma 2, EMT epithelial-mesenchymal transition, FasL Fas ligand, hTERT human telomerase reverse transcriptase, MAPK mitogen-activated protein kinase, PDCD4 programmed cell death 4, PI3K phosphoinositide-3 kinase, PTEN phosphatase and tensin homolog, SIRT6 sirtuin 6, Smad drosophila mothers against decapentaplegic protein, TGF transforming growth factor, ↑ increased, ↓ decreased
Transforming growth factor-β1 can promote cell proliferation, transdifferentiation and inhibit cell apoptosis via upregulation of miR-21. Wang et al. [57] found the interaction between miR-21 and TGF-β1 might be associated with the regulation of the FasL protein, which is involved in keloid formation. Liu et al. [58] demonstrated upregulation of miR-21 increased fibroblast proliferation by regulating the expression of PTEN and phosphorylated AKT in human keloid. This result was confirmed by another study [59]. They found overexpression of miR-21 could downregulate the expression of PTEN and had similar effects to TGF-β1 on proliferation and transdifferentiation [58, 59]. Therefore, the miR-21/PTEN/AKT signaling pathway may play a crucial role in TGF-β1-induced proliferation and transdifferentiation of keloid fibroblasts.
MicroRNA-21 also contributes to the processes of epithelial-mesenchymal transition (EMT) and cell stemness involved in keloid scarring. Using miRNA microarray analysis, Yan et al. [60] found miR-21 was significantly upregulated in the keloid epidermis. Upregulation of miR-21 significantly increased the migration, invasion, and sphere-forming abilities of keloid-derived keratinocytes, and the phenotypes of EMT and cell stemness were also enhanced. Furthermore, PTEN and p-AKT were shown to participate in the regulation of miR-21 on EMT phenotypes and stemness signatures of keloid keratinocytes, which might account for the invasion and recurrence of keloid [58, 60].
5.2 Scleroderma
Scleroderma (systemic sclerosis, SSc) is a chronic autoimmune disease characterized by vasculopathy and progressive fibrosis of skin or/and internal organs, and prolonged activation of dermal fibroblasts is considered to be the main trigger factor for SSc [61,62,63]. An increasing number of studies have confirmed that systemic multiple organ fibrosis and dysfunction is responsible for the high mortality rate of SSc [64, 65]. Despite this, the cellular and molecular mechanisms of SSc are still uncertain; some research has highlighted that TGF-β plays a main role in this progress [66]. Transforming growth factor-β is a multifunctional cytokine that can regulate fibroblast proliferation, differentiation, and apoptosis, induce cytokine secretion, and upregulate the synthesis of collagen and ECM. Studies demonstrated that miRNAs could play important roles in the fibrosis of SSc by regulating the TGF-β signaling pathway [67,68,69].
5.2.1 MicroRNA Expression Profiles in Systemic Sclerosis
Several studies investigated the miRNA profiles of patients with SSc and healthy control individuals. miRNA microarray chip analysis identified dozens of miRNAs that were differentially expressed in patients with SSc [67, 70,71,72,73,74,75]. These miRNAs may be correlated with the pathogenesis of SSc [67]. Zhu et al. [76] identified and confirmed that miR-21 was increased both in the skin tissues and fibroblasts. Makino et al. [52, 77] demonstrated miR-21 expression was upregulated in SSc skin both in vivo and in vitro, compared with normal skin tissues. Zhou et al. identified that 21 miRNAs were differentially expressed in SSc. Among these, 17 miRNAs were involved in Toll-like receptor, TGF-β, and Wnt signaling pathways. Validation experiments revealed that miR-21 and four other miRNA expression levels were higher in SSc skin tissues and fibroblasts, normal fibroblasts, and endothelial cells stimulated with SSc serum. They found miR-21 was specifically expressed at higher levels in SSc serum, in which serum miR-135b was also measured [78, 79]. Systemic sclerosis miRNA microarray data showed lung fibroblasts mildly expressed miR-155/miR-21 after several stimuli [75].
Analysis of serum exosomal miRNAs from patients with SSc showed that six profibrotic miRNAs were increased and ten anti-fibrotic miRNAs were decreased. The expression level of miR-21 was significantly different in exosomes between limited SSc and diffuse SSc, suggesting a plausible mechanism for the extension of the fibrotic SSc process to non-affected tissues [80].
5.2.2 Role of MicroRNA-21 in the Regulation of Systemic Sclerosis
Long-term activation of dermal fibroblasts is the main cause of progressive fibrosis in SSc (Fig. 2). Jafarinejad-Farsangi et al. [30] found miR-21 was a pro-fibrotic factor with high expression in lesional areas of SSc skin and fibroblasts. The rate of apoptosis in SSc fibroblasts increased following miR-21 inhibition, which may be associated with a decrease in Bcl-2 expression and a shift in the Bax:Bcl-2 ratio. Bcl-2 is considered to be an inhibitor of apoptosis and the Bax:Bcl-2 ratio may represent a cell fate determinant. Therefore, inhibition of miR-21 in dermal fibroblasts may harness progressive fibrosis in SSc [30, 81].
Meanwhile, TGF-β activation plays a fundamental role in the process of uncontrolled fibrosis in SSc. After stimulation with TGF-β, the expression of miR-21 was increased and that of SMAD7 mRNA was decreased [76]. Thus, TGF-β can regulate the expression of miR-21 and SMAD7 [81].
5.3 Hypertrophic Scar
Hypertrophic scar is abnormal wound healing after trauma. Although the hypertrophic scar is raised above the skin surface, it does not extend beyond the original wound [82, 83]. In the process of scar formation, fibroblasts synthesize and secrete redundant collagen, so that ECM components are deposited in the tissue. Because fibroblasts are participating in the whole process of scar formation, inhibiting the proliferation and transformation of fibroblasts is important for the treatment of scars [84, 85]. As a key regulatory factor, miR-21 plays a pivotal role in the regulation of scar formation, therefore, it may be a new target for treating hypertrophic scar.
5.3.1 MicroRNA Expression Profiles in Hypertrophic Scar
The differences of miRNA expression between human hypertrophic scars and normal skin have also been obtained. Using a preliminary screen, Ning et al. [86] found 92 miRNA genes were upregulated and 13 downregulated from five human hypertrophic scar tissues compared with normal skin tissues. They then further demonstrated that the trend of hsa-miR-21 through reverse transcription-polymerase chain reaction was consistent with the microarray results. Another microarray analysis was performed and 152 miRNAs were observed to be differentially expressed in hypertrophic scar tissues compared with normal skin tissues. Among the identified miRNAs, miR-21 was significantly increased in hypertrophic scar tissues and fibroblasts [87].
Previous studies have indicated that mesenchymal stem cells (MSCs) can promote skin regeneration and contribute to scar formation [88, 89]. In a skin-defect mouse model, Fang et al. found that umbilical cord-derived MSCs reduced scar formation and myofibroblast accumulation, which may be associated with umbilical cord-derived MSC-derived exosomes and especially exosomal miRNAs [90]. Using high-throughput RNA sequencing, they found a group of umbilical cord-derived MSC-derived exosomes enriched in specific miRNAs, including miR-21, miR-23a, miR-125b, and miR-145. Bioinformatic analysis demonstrated miR-21 played a critical role in suppressing myofibroblast formation by inhibiting the TGF-β2/SMAD2 pathway [90]. Therefore, in addition to keloid, miR-21 may also be a marker for the phenotype of hypertrophic scar fibroblasts.
5.3.2 Role of miR-21 in the Regulation of Hypertrophic Scar
MicroRNA-21 regulates the cell growth of hypertrophic scar fibroblasts (Fig. 2). The underlying mechanism may be that miR-21 regulates hTERT expression via the PTEN/PI3K/AKT signaling pathway by directly targeting PTEN [91]. PDCD4 is another key target gene of miR-21. Downregulation of miR-21 level can promote the expression of PDCD4, reduce the expression of cell-cycle-associated protein C-MYC, CCND1, and inhibit the PI3K/AKT signaling pathway [92].
Another experiment noted that the TGF-β/miR-21/Smad7 pathway might participate in the pathogenesis of the hypertrophic scar [32]. Upregulation of miR-21 promoted the expression of fibrosis markers such as Col1A1, Col3A1, Fn, and α-SMA in fibroblasts. It has also been found that miR-21 enhanced TGF-β1-induced fibroproliferative expression by repressing SMAD7 expression in vitro.
Transforming growth factor-β2 was predicted to be a target of miR-21. Fan et al. [93] demonstrated that overexpressed SIRT6 suppressed the TGF-β2 level by promoting the expression of miR-21. SIRT6 suppressed the proliferation of the fibroblasts, expression of TGF-β2 and interleukin-1α, and the production of collagen type I via the miR-21/TGF-β2 pathway [93, 94]. These results indicated that miR-21 was a critical regulator for hypertrophic scar formation and miR-21 may be a potential novel molecular target for the treatment of hypertrophic scarring.
6 MicroRNA-21 as a Diagnostic and Therapeutic Target for Skin Fibrosis
6.1 MicroRNA-21 as a Biomarker for Diagnosis of Skin Fibrosis
Increasingly, studies have shown that miRNAs can serve as biomarkers for the diagnosis of skin fibrosis and assessment of disease state and severity [62, 95]. There was a strong correlation between the miR-21 level and the severity of skin fibrosis in the skin, serum, and hair of each patient, suggesting that miR-21 can be an independent biomarker [69, 96, 97]. Koba et al. also found the combination of serum levels of miR-206 and miR-21 was more useful in distinguishing patients with SSc from normal subjects than either miR-206 or miR-21 alone [72].
Although skin and serum miRNA levels are known as useful biomarkers for various diseases, hair may be more accessible than sera when looking at human samples. Inoue et al. [96] and Wang et al. [97] found miRNA levels in hair roots or hair shafts may become effective and independent biomarkers in SSc.
6.2 MicroRNA-21 as a Therapeutic Target for Skin Fibrosis
The expression of miR-21 in skin fibrosis provides a potential target to treat this series of diseases. Guo et al. [87] indicated that the miR-21 antagomir has a therapeutic effect on the hypertrophic scar. MicroRNA-21 may also function in an amplifying circuit to enhance TGF-β signaling events in SSc fibrosis, and it is suggested that miR-21 may act as a potential therapeutic target [81]. This molecular mechanism of miR-21 on keloid keratinocytes linked EMT with cell stemness and suggests novel therapeutic targets for keloids [58]. These studies offer a novel strategy for the development of new anti-fibrotic drugs.
The basic anti-fibrotic strategy is to design a small-molecule miRNA inhibitor according to the Watson–Crick base pairing rule, which can be used to suppress or downregulate the expression level of the relevant miRNAs [98, 99]. Currently, the common inhibitors for miR-21 include: anti-miRNA oligonucleotides, locked nucleic acid (LNA), and miRNA small-molecule inhibitors [100,101,102]. Locked nucleic acid is a unique class of nucleic-acid modification possessing very high binding affinity, thermal stability, and excellent specificity toward complementary RNA or DNA oligonucleotides [103]. Obad et al. injected intravenously radiolabeled LNA into mice [104, 105]. Autoradiography showed that LNA was absorbed in all organs except the brain in the mice; then, the luciferase assay showed that LNA could inhibit the activity of miR-21 in the long term, which suggested that LNA has potential pharmacological value for anti-fibrosis [104].
Vascular abnormalities in SSc may induce a reduction in the transfer of exosomes from the skin tissue to the blood stream, resulting in a decrease of serum exosome levels, causing a delay in wound healing. Therefore, exosomal miRNA research will lead to a detailed understanding of SSc pathogenesis and new therapeutic approaches [106].
Although miRNA has proven to be a great prospect in the treatment of skin fibrosis, there are still a number of problems to be solved before it could be an effective clinical treatment. The targets will need to be refined, as targeting just one miRNA may have a limited effect given that often multiple miRNAs target one mRNA and will all affect protein production. Furthermore, miRNA can also bind to the sequences of multiple target genes as a result of incomplete pairing and can regulate their expressions, which may produce off-target effects [107, 108].
7 Conclusion
Improving our knowledge on the function of miR-21 may provide a new direction for the study of the pathogenesis of skin fibrosis. The regulation of the relevant signaling pathways involved in miR-21 will produce new diagnostic and therapeutic options. However, the application of miR-21 in the future is still a great challenge. Prospective cohort studies are necessary to identify and establish miR-21 as a biomarker of skin fibrosis for clinical applications in the near future.
References
Habiel DM, Hogaboam C. Heterogeneity in fibroblast proliferation and survival in idiopathic pulmonary fibrosis. Front Pharmacol. 2014;5:2.
Andrews JP, Marttala J, Macarak E, Rosenbloom J, Uitto J. Keloids: the paradigm of skin fibrosis. Pathomechanisms and treatment. Matrix Biol. 2016;51:37–46.
Bijlard E, Kouwenberg CA, Timman R, Hovius SE, Busschbach JJ, Mureau MA. Burden of keloid disease: a cross-sectional health-related quality of life assessment. Acta Derm Venereol. 2017;97(2):225–9.
Walliczek U, Engel S, Weiss C, Aderhold C, Lippert C, Wenzel A, et al. Clinical outcome and quality of life after a multimodal therapy approach to ear keloids. JAMA Facial Plast Surg. 2015;17(5):333–9.
Bock O, Schmid-Ott G, Malewski P, Mrowietz U. Quality of life of patients with keloid and hypertrophic scarring. Arch Dermatol Res. 2006;297(10):433–8.
Zhai XM. The epidermiology investigation of scars and the keloid susceptible gene’s mRNA expression in human skin, hypertrophic scar and keloid. Graduate thesis of Peking University. 2003. pp 18–19.
Kundan P. Keloid removal cost. 2013. http://www.buzzle.com/articles/keloid-removal-cost.html. Accessed 21 June 2013.
Sun LM, Wang KH, Lee YC. Keloid incidence in Asian people and its comorbidity with other fibrosis-related diseases: a nationwide population-based study. Arch Dermatol Res. 2014;306(9):803–8.
Ketchum LD, Cohen IK, Masters FW. Hypertrophic scars and keloids: a collective review. Plast Reconstruct Surg. 1974;53(2):140–54.
Halim AS, Emami A, Salahshourifar I, Kannan TP. Keloid scarring: understanding the genetic basis, advances, and prospects. Arch Plast Surg. 2012;39(3):184–9.
Arias-Nunez MC, Llorca J, Vazquez-Rodriguez TR, Gomez-Acebo I, Miranda-Filloy JA, Martin J, et al. Systemic sclerosis in northwestern Spain: a 19-year epidemiologic study. Medicine. 2008;87(5):272–80.
Lopez-Bastida J, Linertova R, Oliva-Moreno J, Serrano-Aguilar P, Posada-de-la-Paz M, Kanavos P, et al. Social/economic costs and health-related quality of life in patients with scleroderma in Europe. Eur J Health Econom. 2016;17(Suppl. 1):109–17.
Andreasson K, Saxne T, Bergknut C, Hesselstrand R, Englund M. Prevalence and incidence of systemic sclerosis in southern Sweden: population-based data with case ascertainment using the 1980 ARA criteria and the proposed ACR-EULAR classification criteria. Ann Rheum Dis. 2014;73(10):1788–92.
Scolnik M, Lancioni E, Saucedo C, Marin J, Sabelli M, Bedran Z, et al. Systemic sclerosis in Argentina: evaluation of a large cohort from a single centre and comparison with other international series. Clin Exp Rheumatol. 2014;32(6 Suppl. 86):S-94–7.
Kanecki K, Gorynski P, Tarka P, Wierzba W, Tyszko P. Incidence and prevalence of systemic sclerosis (SSc) in Poland: differences between rural and urban regions. Ann Agric Environ Med. 2017;24(2):240–4.
Kawalec PP, Malinowski KP. The indirect costs of systemic autoimmune diseases, systemic lupus erythematosus, systemic sclerosis and sarcoidosis: a summary of 2012 real-life data from the Social Insurance Institution in Poland. Exp Rev Pharmacoeconom Outcomes Res. 2015;15(4):667–73.
Mirastschijski U, Sander JT, Zier U, Rennekampff HO, Weyand B, Vogt PM. The cost of post-burn scarring. Ann Burns Fire Disasters. 2015;28(3):215–22.
Wang W, Qu M, Xu L, Wu X, Gao Z, Gu T, et al. Sorafenib exerts an anti-keloid activity by antagonizing TGF-beta/Smad and MAPK/ERK signaling pathways. J Mol Med. 2016;94(10):1181–94.
Hong MJ, Ko EB, Park SK, Chang MS. Inhibitory effect of Astragalus membranaceus root on matrix metalloproteinase-1 collagenase expression and procollagen destruction in ultraviolet B-irradiated human dermal fibroblasts by suppressing nuclear factor kappa-B activity. J Pharm Pharmacol. 2013;65(1):142–8.
Sahin H, Wasmuth HE. Chemokines in tissue fibrosis. Biochim Biophys Acta. 2013;1832(7):1041–8.
Jara P, Calyeca J, Romero Y, Placido L, Yu G, Kaminski N, et al. Matrix metalloproteinase (MMP)-19-deficient fibroblasts display a profibrotic phenotype. Am J Physiol Lung Cell Mol Physiol. 2015;308(6):L511–22.
Messadi DV, Doung HS, Zhang Q, Kelly AP, Tuan TL, Reichenberger E, et al. Activation of NFkappaB signal pathways in keloid fibroblasts. Arch Dermatol Res. 2004;296(3):125–33.
Mun JH, Kim YM, Kim BS, Kim JH, Kim MB, Ko HC. Simvastatin inhibits transforming growth factor-beta1-induced expression of type I collagen, CTGF, and alpha-SMA in keloid fibroblasts. Wound Repair Regen. 2014;22(1):125–33.
Unahabhokha T, Sucontphunt A, Nimmannit U, Chanvorachote P, Yongsanguanchai N, Pongrakhananon V. Molecular signalings in keloid disease and current therapeutic approaches from natural based compounds. Pharm Biol. 2015;53(3):457–63.
Li L, Xu J, Yang D, Tan X, Wang H. Computational approaches for microRNA studies: a review. Mamm Genome. 2010;21(1–2):1–12.
Sanchez CA, Andahur EI, Valenzuela R, Castellon EA, Fulla JA, Ramos CG, et al. Exosomes from bulk and stem cells from human prostate cancer have a differential microRNA content that contributes cooperatively over local and pre-metastatic niche. Oncotarget. 2016;7(4):3993–4008.
Deng Z, He Y, Yang X, Shi H, Shi A, Lu L, et al. MicroRNA-29: a crucial player in fibrotic disease. Mol Diagn Ther. 2017;21(3):285–94.
O’Reilly S. MicroRNAs in fibrosis: opportunities and challenges. Arthritis Res Ther. 2016;13(18):11.
Babalola O, Mamalis A, Lev-Tov H, Jagdeo J. The role of microRNAs in skin fibrosis. Arch Dermatol Res. 2013;305(9):763–76.
Jafarinejad-Farsangi S, Farazmand A, Gharibdoost F, Karimizadeh E, Noorbakhsh F, Faridani H, et al. Inhibition of microRNA-21 induces apoptosis in dermal fibroblasts of patients with systemic sclerosis. Int J Dermatol. 2016;55(11):1259–67.
Zhou R, Wang C, Wen C, Wang D. miR-21 promotes collagen production in keloid via Smad7. Burns. 2017;43(3):555–61.
Zhou R, Zhang Q, Zhang Y, Fu S, Wang C. Aberrant miR-21 and miR-200b expression and its pro-fibrotic potential in hypertrophic scars. Exp Cell Res. 2015;339(2):360–6.
Lorenzen JM, Schauerte C, Hubner A, Kolling M, Martino F, Scherf K, et al. Osteopontin is indispensible for AP1-mediated angiotensin II-related miR-21 transcription during cardiac fibrosis. Eur Heart J. 2015;36(32):2184–96.
Kumarswamy R, Volkmann I, Thum T. Regulation and function of miRNA-21 in health and disease. RNA Biol. 2011;8(5):706–13.
Kim YJ, Park SJ, Choi EY, Kim S, Kwak HJ, Yoo BC, et al. PTEN modulates miR-21 processing via RNA-regulatory protein RNH1. PLoS One. 2011;6(12):e28308.
Lin Y, Liu X, Cheng Y, Yang J, Huo Y, Zhang C. Involvement of microRNAs in hydrogen peroxide-mediated gene regulation and cellular injury response in vascular smooth muscle cells. J Biol Chem. 2009;284(12):7903–13.
Li Y, Yan L, Zhang W, Hu N, Chen W, Wang H, et al. MicroRNA-21 inhibits platelet-derived growth factor-induced human aortic vascular smooth muscle cell proliferation and migration through targeting activator protein-1. Am J Transl Res. 2014;6(5):507–16.
Chen B, Huang SG, Ju L, Li M, Nie FF, Zhang Y, et al. Effect of microRNA-21 on the proliferation of human degenerated nucleus pulposus by targeting programmed cell death 4. Braz J Med Biol Res. 2016. doi:10.1590/1414-431X20155020.
Zhang Z, Zha Y, Hu W, Huang Z, Gao Z, Zang Y, et al. The autoregulatory feedback loop of microRNA-21/programmed cell death protein 4/activation protein-1 (MiR-21/PDCD4/AP-1) as a driving force for hepatic fibrosis development. J Biol Chem. 2013;288(52):37082–93.
Zhu Q, Wang Z, Hu Y, Li J, Li X, Zhou L, et al. miR-21 promotes migration and invasion by the miR-21-PDCD4-AP-1 feedback loop in human hepatocellular carcinoma. Oncol Rep. 2012;27(5):1660–8.
Kang H, Davis-Dusenbery BN, Nguyen PH, Lal A, Lieberman J, Van Aelst L, et al. Bone morphogenetic protein 4 promotes vascular smooth muscle contractility by activating microRNA-21 (miR-21), which down-regulates expression of family of dedicator of cytokinesis (DOCK) proteins. J Biol Chem. 2012;287(6):3976–86.
Ahmed MI, Mardaryev AN, Lewis CJ, Sharov AA, Botchkareva NV. MicroRNA-21 is an important downstream component of BMP signalling in epidermal keratinocytes. J Cell Sci. 2011;124(Pt 20):3399–404.
Smith CM, Michael MZ, Watson DI, Tan G, Astill DS, Hummel R, et al. Impact of gastro-oesophageal reflux on microRNA expression, location and function. BMC Gastroenterol. 2013;8(13):4.
Mari W, Alsabri SG, Tabal N, Younes S, Sherif A, Simman R. Novel insights on understanding of keloid scar: article review. J Am Coll Clin Wound Spec. 2015;7(1–3):1–7.
Sidgwick GP, Bayat A. Extracellular matrix molecules implicated in hypertrophic and keloid scarring. J Eur Acad Dermatol Venereol. 2012;26(2):141–52.
van Leeuwen MC, Stokmans SC, Bulstra AE, Meijer OW, Heymans MW, Ket JC, et al. Surgical excision with adjuvant irradiation for treatment of keloid scars: a systematic review. Plast Reconstruct Surg Glob Open. 2015;3(7):e440.
Wang CM, Hiko H, Nakazawa N. Investigation of p53 polymorphism for genetic predisposition of keloid and hypertrophic scar. Zhonghua zheng xing wai ke za zhi. 2005;21(1):32–5.
He Y, Deng Z, Alghamdi M, Lu L, Fear MW, He L. From genetics to epigenetics: new insights into keloid scarring. Cell Prolif. 2017. doi:10.1111/cpr.12326 (Epub 2017 Jan 5).
Kashiyama K, Mitsutake N, Matsuse M, Ogi T, Saenko VA, Ujifuku K, et al. miR-196a downregulation increases the expression of type I and III collagens in keloid fibroblasts. J Invest Dermatol. 2012;132(6):1597–604.
Liu Y, Yang D, Xiao Z, Zhang M. miRNA expression profiles in keloid tissue and corresponding normal skin tissue. Aesthet Plast Surg. 2012;36(1):193–201.
Wu ZY, Lu L, Liang J, Guo XR, Zhang PH, Luo SJ. Keloid microRNA expression analysis and the influence of miR-199a-5p on the proliferation of keloid fibroblasts. Genet Mol Res. 2014;13(2):2727–38.
Makino K, Jinnin M, Hirano A, Yamane K, Eto M, Kusano T, et al. The downregulation of microRNA let-7a contributes to the excessive expression of type I collagen in systemic and localized scleroderma. J Immunol. 2013;190(8):3905–15.
Guo XR, Liang J, Huang RL, Lu L, Jin YD, Luo SJ, et al. Differential expression of microRNAs in human keloids. Zhongguo Zuzhi Gongcheng Yanjiu. 2012;16:9370–5.
Li C, Bai Y, Liu H, Zuo X, Yao H, Xu Y, et al. Comparative study of microRNA profiling in keloid fibroblast and annotation of differential expressed microRNAs. Acta Biochim Biophys Sin. 2013;45(8):692–9.
Luan Y, Liu Y, Liu C, Lin Q, He F, Dong X, et al. Serum miRNAs signature plays an important role in keloid disease. Curr Mol Med. 2016;16(5):504–14.
Li S, Liu W, Lei Y, Long J. Regulatory effects of electronic beam irradiation on mir-21/smad7-mediated collagen I synthesis in keloid-derived fibroblasts. Biol Open. 2016;5(11):1567–74.
Wang X, Liu Y, Chen X, Zhang M, Xiao Z. Impact of MiR-21 on the expression of FasL in the presence of TGF-beta1. Aesthet Surg J. 2013;33(8):1186–98.
Liu Y, Wang X, Yang D, Xiao Z, Chen X. MicroRNA-21 affects proliferation and apoptosis by regulating expression of PTEN in human keloid fibroblasts. Plastic Reconstruct Surg. 2014;134(4):561e–73e.
Liu Y, Li Y, Li N, Teng W, Wang M, Zhang Y, et al. TGF-beta1 promotes scar fibroblasts proliferation and transdifferentiation via up-regulating microRNA-21. Sci Rep. 2016;24(6):32231.
Yan L, Cao R, Liu Y, Wang L, Pan B, Lv X, et al. MiR-21-5p links epithelial-mesenchymal transition phenotype with stem-like cell signatures via AKT signaling in keloid keratinocytes. Sci Rep. 2016;6(6):28281.
Sperber K, Ash J, Gutwein F, Wasserrman A, Rao V, Tratenberg M. Localized scleroderma: a clinical review. Curr Rheumatol Rev. 2016 (Epub ahead of print).
Leask A. Possible strategies for anti-fibrotic drug intervention in scleroderma. J Cell Commun Signal. 2011;5(2):125–9.
Distler O, Cozzio A. Systemic sclerosis and localized scleroderma: current concepts and novel targets for therapy. Semin Immunopathol. 2016;38(1):87–95.
Hoa S, Stern EP, Denton CP, Hudson M, Scleroderma Clinical Trials Consortium Scleroderma Renal Crisis Working Group Investigators of the Scleroderma Clinical Trials Consortium Scleroderma Renal Crisis Working G. Towards developing criteria for scleroderma renal crisis: a scoping review. Autoimmun Rev. 2017;16(4):407–15.
Stern EP, Denton CP. The pathogenesis of systemic sclerosis. Rheum Dis Clin N Am. 2015;41(3):367–82.
Cong L, Xia ZK, Yang RY. Targeting the TGF-beta receptor with kinase inhibitors for scleroderma therapy. Archiv der Pharmazie. 2014;347(9):609–15.
Li H, Yang R, Fan X, Gu T, Zhao Z, Chang D, et al. MicroRNA array analysis of microRNAs related to systemic scleroderma. Rheumatol Int. 2012;32(2):307–13.
Lu J, Liu Q, Wang L, Tu W, Chu H, Ding W, et al. Increased expression of latent TGF-beta-binding protein 4 affects the fibrotic process in scleroderma by TGF-beta/SMAD signaling. Lab Invest. 2017;97(5):591–601.
Takemoto R, Jinnin M, Wang Z, Kudo H, Inoue K, Nakayama W, et al. Hair miR-29a levels are decreased in patients with scleroderma. Exp Dermatol. 2013;22(12):832–3.
Etoh M, Jinnin M, Makino K, Yamane K, Nakayama W, Aoi J, et al. microRNA-7 down-regulation mediates excessive collagen expression in localized scleroderma. Arch Dermatol Res. 2013;305(1):9–15.
Jimenez SA, Piera-Velazquez S. Potential role of human-specific genes, human-specific microRNAs and human-specific non-coding regulatory RNAs in the pathogenesis of systemic sclerosis and Sjogren’s syndrome. Autoimmun Rev. 2013;12(11):1046–51.
Koba S, Jinnin M, Inoue K, Nakayama W, Honda N, Makino K, et al. Expression analysis of multiple microRNAs in each patient with scleroderma. Exp Dermatol. 2013;22(7):489–91.
Steen SO, Iversen LV, Carlsen AL, Burton M, Nielsen CT, Jacobsen S, et al. The circulating cell-free microRNA profile in systemic sclerosis is distinct from both healthy controls and systemic lupus erythematosus. J Rheumatol. 2015;42(2):214–21.
Wuttge DM, Carlsen AL, Teku G, Steen SO, Wildt M, Vihinen M, et al. Specific autoantibody profiles and disease subgroups correlate with circulating micro-RNA in systemic sclerosis. Rheumatology. 2015;54(11):2100–7.
Christmann RB, Wooten A, Sampaio-Barros P, Borges CL, Carvalho CR, Kairalla RA, et al. miR-155 in the progression of lung fibrosis in systemic sclerosis. Arthritis Res Ther. 2016;18(1):155.
Zhu H, Li Y, Qu S, Luo H, Zhou Y, Wang Y, et al. MicroRNA expression abnormalities in limited cutaneous scleroderma and diffuse cutaneous scleroderma. J Clin Immunol. 2012;32(3):514–22.
Makino T, Jinnin M, Etoh M, Yamane K, Kajihara I, Makino K, et al. Down-regulation of microRNA-196a in the sera and involved skin of localized scleroderma patients. Eur J Dermatol. 2014;24(4):470–6.
Zhou B, Zuo XX, Li YS, Gao SM, Dai XD, Zhu HL, et al. Integration of microRNA and mRNA expression profiles in the skin of systemic sclerosis patients. Sci Rep. 2017;17(7):42899.
O’Reilly S, Ciechomska M, Fullard N, Przyborski S, van Laar JM. IL-13 mediates collagen deposition via STAT6 and microRNA-135b: a role for epigenetics. Sci Rep. 2016;26(6):25066.
Wermuth PJ, Piera-Velazquez S, Jimenez SA. Exosomes isolated from serum of systemic sclerosis patients display alterations in their content of profibrotic and antifibrotic microRNA and induce a profibrotic phenotype in cultured normal dermal fibroblasts. Clin Exp Rheumatol. 2017 (Epub ahead of print).
Zhu H, Luo H, Li Y, Zhou Y, Jiang Y, Chai J, et al. MicroRNA-21 in scleroderma fibrosis and its function in TGF-beta-regulated fibrosis-related genes expression. J Clin Immunol. 2013;33(6):1100–9.
Friedstat JS, Hultman CS. Hypertrophic burn scar management: what does the evidence show? A systematic review of randomized controlled trials. Ann Plast Surg. 2014;72(6):S198–201.
Gugatschka M, Ainodhofer H, Gruber HJ, Graupp M, Kieslinger P, Kiesler K, et al. Age effects on extracellular matrix production of vocal fold scar fibroblasts in rats. Eur Arch Otorhinolaryngol. 2014;271(5):1107–12.
Lian N, Li T. Growth factor pathways in hypertrophic scars: molecular pathogenesis and therapeutic implications. Biomed Pharmacother. 2016;84:42–50.
Xue M, Jackson CJ. Extracellular matrix reorganization during wound healing and its impact on abnormal scarring. Adv Wound Care. 2015;4(3):119–36.
Ning P, Liu DW, Mao YG, Peng Y, Lin ZW, Liu DM. Differential expression profile of microRNA between hyperplastic scar and normal skin. Zhonghua yi xue za zhi. 2012;92(10):692–4.
Guo L, Xu K, Yan H, Feng H, Wang T, Chai L, et al. MicroRNA expression signature and the therapeutic effect of the microRNA21 antagomir in hypertrophic scarring. Mol Med Rep. 2017;15(3):1211–21.
Cejka C, Cejkova J, Trosan P, Zajicova A, Sykova E, Holan V. Transfer of mesenchymal stem cells and cyclosporine A on alkali-injured rabbit cornea using nanofiber scaffolds strongly reduces corneal neovascularization and scar formation. Histol Histopathol. 2016;31(9):969–80.
Liu S, Jiang L, Li H, Shi H, Luo H, Zhang Y, et al. Mesenchymal stem cells prevent hypertrophic scar formation via inflammatory regulation when undergoing apoptosis. J Invest Dermatol. 2014;134(10):2648–57.
Fang S, Xu C, Zhang Y, Xue C, Yang C, Bi H, et al. Umbilical cord-derived mesenchymal stem cell-derived exosomal microRNAs suppress myofibroblast differentiation by inhibiting the transforming growth factor-beta/SMAD2 pathway during wound healing. Stem Cell Transl Med. 2016;5(10):1425–39.
Zhu HY, Li C, Bai WD, Su LL, Liu JQ, Li Y, et al. MicroRNA-21 regulates hTERT via PTEN in hypertrophic scar fibroblasts. PLoS One. 2014;9(5):e97114.
Mu SZ, Sun YW, Wang GD. Down-regulation of miR-21 inhibits the HSF cells proliferation and the PI3K/Akt pathways via PDCD4. Chin J Aesthet Med. 2015;24(23):39–43.
Fan X, Chen J, Shi D, Jia J, He J, Li L, et al. The role and mechanisms of action of SIRT6 in the suppression of postoperative epidural scar formation. Int J Mol Med. 2016;37(5):1337–44.
Zhang C, Wen C, Lin J, Shen G. Protective effect of pyrroloquinoline quinine on ultraviolet A irradiation-induced human dermal fibroblast senescence in vitro proceeds via the anti-apoptotic sirtuin 1/nuclear factor-derived erythroid 2-related factor 2/heme oxygenase 1 pathway. Mol Med Rep. 2015;12(3):4382–8.
Glavac D, Ravnik-Glavac M. Essential role of microRNA in skin physiology and disease. Adv Exp Med Biol. 2015;888:307–30.
Inoue M, Jinnin M, Wang Z, Nakamura K, Inoue K, Ichihara A, et al. microRNA level is raised in the hair shafts of patients with dematomyositis in comparison with normal subjects and patients with scleroderma. Int J Dermatol. 2016;55(7):786–90.
Wang Z, Jinnin M, Kudo H, Inoue K, Nakayama W, Honda N, et al. Detection of hair-microRNAs as the novel potent biomarker: evaluation of the usefulness for the diagnosis of scleroderma. J Dermatol Sci. 2013;72(2):134–41.
Wu W. MicroRNA: potential targets for the development of novel drugs? Drugs R&D. 2010;10(1):1–8.
Hata A, Lieberman J. Dysregulation of microRNA biogenesis and gene silencing in cancer. Sci Signal. 2015;8(368):re3.
Lennox KA, Owczarzy R, Thomas DM, Walder JA, Behlke MA. Improved performance of anti-miRNA oligonucleotides using a novel non-nucleotide modifier. Mol Ther Nucleic Acids. 2013;27(2):e117.
Munoz-Alarcon A, Guterstam P, Romero C, Behlke MA, Lennox KA, Wengel J, et al. Modulating anti-microRNA-21 activity and specificity using oligonucleotide derivatives and length optimization. ISRN Pharm. 2012;2012:407154.
Lennox KA, Behlke MA. A direct comparison of anti-microRNA oligonucleotide potency. Pharm Res. 2010;27(9):1788–99.
Hanessian S, Wagger J, Merner BL, Giacometti RD, Ostergaard ME, Swayze EE, et al. A constrained tricyclic nucleic acid analogue of alpha-L-LNA: investigating the effects of dual conformational restriction on duplex thermal stability. J Organic Chem. 2013;78(18):9064–75.
Obad S, dos Santos CO, Petri A, Heidenblad M, Broom O, Ruse C, et al. Silencing of microRNA families by seed-targeting tiny LNAs. Nat Genet. 2011;43(4):371–8.
Garchow BG, Bartulos Encinas O, Leung YT, Tsao PY, Eisenberg RA, Caricchio R, et al. Silencing of microRNA-21 in vivo ameliorates autoimmune splenomegaly in lupus mice. EMBO Mol Med. 2011;3(10):605–15.
Nakamura K, Jinnin M, Harada M, Kudo H, Nakayama W, Inoue K, et al. Altered expression of CD63 and exosomes in scleroderma dermal fibroblasts. J Dermatol Sci. 2016;84(1):30–9.
Leoni G, Tramontano A. A structural view of microRNA-target recognition. Nucleic Acids Res. 2016;44(9):e82.
Saraiya AA, Li W, Wang CC. Transition of a microRNA from repressing to activating translation depending on the extent of base pairing with the target. PLoS One. 2013;8(2):e55672.
Acknowledgements
The authors thank Li He and Hui Jiang for assistance with the editing and grammar of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The authors are supported by grants from the National Natural Science Foundation of China (Grant No. 81560502), the Science and Technology Leading Talent Project of Yunnan Province (Grant No. 2017HA010), the National Natural Science Foundation of Yunnan Province (Grant No. 2016FB044, 2014FB008), the Health Science and Technology Project of Yunnan Province (Grant No. 2016NS005), the Education Department Fund of Yunnan Province (Grant No. 2014Y165, 2015Z082), and the 100 Talents Program of Kunming Medical University.
Conflict of interest
Yan Li, Juan Zhang, Yuying Lei, Lechun Lyu, Ruiling Zuo, and Ting Chen have no competing financial interests.
Rights and permissions
About this article
Cite this article
Li, Y., Zhang, J., Lei, Y. et al. MicroRNA-21 in Skin Fibrosis: Potential for Diagnosis and Treatment. Mol Diagn Ther 21, 633–642 (2017). https://doi.org/10.1007/s40291-017-0294-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40291-017-0294-8