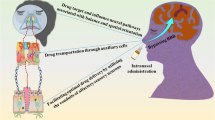
Abstract
While the intranasal administration of drugs to the brain has been gaining both research attention and regulatory success over the past several years, key fundamental and translational challenges remain to fully leveraging the promise of this drug delivery pathway for improving the treatment of various neurological and psychiatric illnesses. In response, this review highlights the current state of understanding of the nose-to-brain drug delivery pathway and how both biological and clinical barriers to drug transport using the pathway can been addressed, as illustrated by demonstrations of how currently approved intranasal sprays leverage these pathways to enable the design of successful therapies. Moving forward, aiming to better exploit the understanding of this fundamental pathway, we also outline the development of nanoparticle systems that show improvement in delivering approved drugs to the brain and how engineered nanoparticle formulations could aid in breakthroughs in terms of delivering emerging drugs and therapeutics while avoiding systemic adverse effects.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
The intranasal (IN) route can circumvent many issues with the delivery of drugs to the brain, but itself presents new challenges around clinical implementation and overcoming biological barriers. |
Existing approved IN formulations for CNS delivery primarily consist of a potent active ingredient combined with a minimal number of functional excipients, with delivery enabled by the inherent properties of the drug itself. |
Emerging intranasal formulations are focused on enabling efficient delivery of drugs that are not inherently IN permeable into the brain. |
1 Introduction
Central nervous system (CNS) disorders are the leading cause of disease globally and are currently experiencing increasing prevalence due to population growth, prolonged lifespans and more recently the COVID-19 pandemic [1, 2]. These disorders, which include neoplastic, neurodegenerative (e.g. Parkinson’s and Alzheimer’s), and major psychiatric disorders (e.g. depression, schizophrenia, and bipolar disorder), are inherently challenging to treat pharmacologically due to the blood-brain barrier (BBB)—the distinctive microvasculature in the brain that functions to tightly regulate the movement of ions, molecules, and cells between circulating blood plasma and the brain [3]. While the BBB serves to protect the brain from toxins and pathogens, it also creates a significant obstacle for the delivery of therapeutics, with 98% of small molecules and almost 100% of large molecules unable to cross into the brain [4, 5]. Thus, there remains a need to develop innovative strategies that can successfully target therapeutics to the brain for the treatment of CNS disorders.
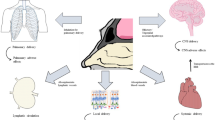
Intranasal (IN) delivery is increasingly being investigated as an alternative approach for delivering therapeutics to the CNS for the treatment of associated disorders (Fig. 1). The nose-to-brain (N2B) route offers several advantages for drug delivery as compared to traditional oral administration: (1) the N2B route circumvents major pharmacokinetic obstacles typically associated with oral CNS drug delivery including gastrointestinal pH and enzymes, delayed/variable absorption, first-pass hepatic drug metabolism, serum-associated degradation, kidney filtration, and the BBB [6, 7]; (2) the nasal epithelium provides an optimal absorption surface for drug delivery due to its high permeability, leaky intercellular junctional complexes, and extensive vascularization [8]; (3) the olfactory and trigeminal nerve pathways that innervate the nasal epithelium provide a direct route to the brain resulting in enhanced CNS therapeutic bioavailability, decreased peripheral side effects, and reduced dosage [9, 10]; and (4) from a patient care perspective, the IN route is non-invasive, easy to self-administer, and may be more acceptable for patients with movement disorders, nausea, impaired gastrointestinal function, and/or salivary gland dysfunction (dry mouth) [11].
Many reviews have recently been written on the mechanisms and benefits of the IN delivery of CNS therapeutics. Kashyap et al. [12] describe general nanoparticle-based approaches for nose-to-brain delivery, Xu et al. [13] and Rabiee et al. [14] both describe recent advances in nanoparticle-mediated IN drug delivery for IN antidepressants and Alzheimer’s disease (AD) therapeutics, respectively [12,13,14], while Keller et al. and Tan et al. [15, 16] both described what types of excipients are useful for IN delivery, the former with a more specific emphasis on toxicological challenges. These reviews all present a similar perspective of the physiology, mechanisms, and utility of IN delivery, although some ideas such as the nature of the N2B mediators are still being debated [17]. Since our own previous collaborative review (from 2017) focusing on IN nanotechnologies for antipsychotic drug delivery [18], several clinically approved CNS drugs have been formulated into approved IN delivery vehicles (see Table 1); however, to our knowledge, no review to date has focused on clinically approved IN drugs for the treatment of a broad spectrum of neurological and psychiatric disorders and their emerging nanoparticle designs.
In this review, we focus on the rational design of translational IN delivery approaches for drugs already approved for clinical use or currently under investigation. While the list of approved drugs included is comprehensive for the USA, the therapeutics are also often approved in other jurisdictions with similar dosages. We first provide a brief overview of IN drug delivery focused on the anatomy of the nasal cavity, pharmacokinetics, and translational shortcomings of direct N2B delivery; thereafter, we provide an engineering-oriented outlook of current clinically approved IN drugs, their intrinsic pharmacokinetic profiles, and appropriate excipient selection for effective IN delivery of such drugs, including nanoscale delivery vehicles recently reported to improve IN administration and brain penetration for similar drugs. Finally, we envision the outstanding needs in the field to further improve the efficacy of IN-based CNS therapeutics both within their current scope as well as in expanded fields.
2 Anatomy and Physiology of the Nasal Cavity
The nose is partitioned into two nasal cavities divided along the midsagittal plane by structures of bone and cartilage known as the nasal septum. Each cavity is lined by a continuous thin layer of nasal epithelial cells (one to two cells thick), beneath which lies the lamina propria that contains various types and amounts of blood and lymphatic vessels, nerves, glands, and mesenchymal cells, depending on the location of the nasal epithelium [19]. The nasal epithelium can be divided into three regions based on the type of cells present: the vestibule, respiratory epithelium, and olfactory epithelium (Fig. 2).
-
1.
The nasal vestibule is the most anterior part of the nasal cavity and is lined by squamous epithelial cells and coarse nasal hairs that function to filter out large particulates while allowing small particles such as odorants to pass. Therapeutics intended for localized nasal treatments are typically applied here since drug absorption is negligible due to this region’s small surface area (~ 0.6 cm2) and low vascularization [20].
-
2.
The respiratory epithelium is posterior to the vestibule and functions to filter, warm, and humidify inhaled air destined for the lungs. This region consists of four cell types: ciliated and non-ciliated columnar cells, goblet cells, and basal cells. Goblet cells secrete mucus, which consists of mucins, immunoglobulins, lysozymes, and water, while basal cells are progenitors for the other cell types [21, 22]. Together, these cells protect the respiratory system from inhaled pathogens by performing nasal mucociliary clearance (MCC), a defense mechanism intended to transport foreign pathogens and particles entrapped in mucus lining the nasal epithelium towards the nasopharynx to be swallowed into the gastrointestinal tract and thus avoid reaching lower respiratory tracts (i.e. the lungs) [23]. The typical MCC transit time in humans is ~ 15 min, making MCC an essential consideration for IN drug delivery as the contact time of therapeutics exposed to the nasal epithelium is limited by this clearance time unless the carrier itself manipulates these kinetics (i.e. by adhering to the mucous) [24]. The respiratory region is considered the main site for systemic drug entry due to its large surface area (~ 130 cm2/90% of nasal region) and extensive vascularization. The ophthalmic (V1) and maxillary branches (V2) of the trigeminal nerve (CNV)—which originate from the brainstem—innervate this region, and can provide a direct pathway to deliver therapeutics directly to the CNS.
-
3.
The olfactory epithelium is located in the superior posterior portion of the nasal cavity, which covers ~ 10% (~ 5–10 cm2) of the total nasal epithelial surface area [21, 25]. This region consists of several cell types including basal cells, sustentacular cells, Bowman’s (olfactory) glands, and (most notably) the olfactory sensory neurons (OSNs) [26]. OSNs are responsible for sensing and transducing odorant information to the brain through the olfactory nerve pathway, which consists of the OSNs, lamina propria, and the olfactory bulbs that project to various brain regions. This pathway has been shown to serve as a direct route for drug delivery to the brain. Axons of OSNs project directly to the olfactory bulb through perforations in the cribriform plate of the ethmoid bone and are enclosed by olfactory ensheathing cells (OECs) and olfactory nerve fibroblast (ONFs), which form a continuous perineural channel enveloping axons until they synapse with second-order neurons in the glomeruli of the olfactory bulbs [27, 28]. The lamina propria of the olfactory epithelium also houses the maxillary branch of the trigeminal nerve and can further serve as a pathway for direct CNS drug delivery.
Structure and composition of the human nasal cavity. The olfactory epithelium (OE) is the region highlighted in red. Olfactory sensory neuron (OSN) axons project from the OE through perforations in the cribriform plate to the olfactory bulb. These axons are bundled together by olfactory ensheathing cells (OECs) in the lamina propria. Sustencular cells, Bowman’s glands, and basal cells are also part of the OE. The respiratory epithelium, which lines most of the nasal cavity, is the region highlighted in green. The region is made up of ciliated and non-ciliated columnar cells, mucus secreting goblet cells, and basal cells. Branches of the trigeminal nerve originating from the brainstem innervate this region. Image constructed from information presented in [29]. Created with BioRender.com
3 Mechanisms of Nose-Brain (N2B) Drug Delivery
The transportation of therapeutics from the nasal epithelium directly to the CNS occurs primarily through the olfactory and trigeminal nerve pathways using intracellular- and/or extracellular-dependent processes. However, based on specific therapeutic and excipient properties, it is likely that one pathway and mechanism dominates transport. The surrounding blood and lymphatic vessels may absorb therapeutics and distribute them systemically, with a small portion of the drug also eventually reaching the brain via an indirect route.
3.1 The Olfactory Nerve Pathway
Therapeutics that reach the posterior-superior portion of the nasal cavity convene at the olfactory epithelium, which consists of OSNs. Axons of OSNs are bundled together in the lamina propria by the OECs and project directly to the olfactory bulbs. These axons form the olfactory nerve (CNI) and provide a direct connection between the olfactory epithelium and the brain. OECs enclose OSNs and form a continuous channel between the lamina propria and the subarachnoid space between the olfactory bulbs [26].
Intracellular transport within the olfactory nerve axons has been shown typically within hours after IN administration [30]. Non-specific fluid-phase pinocytosis and receptor-mediated endocytosis are the main intracellular mechanisms involved in internalizing substances into the apical dendrites of OSNs, depending on the nature of the therapeutic being transported. For example, horseradish peroxidase (HRP, 40 kDa) lacks binding sites to the plasma membrane of OSNs such that non-specific fluid phase pinocytosis is thought to be the principal mode of entry, resulting in packaging of HRP into lysosomes for degradation; in contrast, wheat-germ agglutinin HRP (WGA-HRP, 62 kDa) can bind to OSN surface glycoproteins, thus undergoing receptor-mediated endocytosis into neuronal Golgi-endoplasmic reticulum lysosomes and enabling its participation in cellular secretion and recycling [30,31,32]. Once substances are endocytosed by the OSNs in the olfactory epithelium, vesicles travel along the OSN axons towards the olfactory bulb to be exocytosed to second-order mitral-tufted cells in glomeruli that then project their axons (olfactory tracts) to various regions of the brain.
Extracellular transport of therapeutics from the olfactory epithelium to the brain occurs through diffusion into the paracellular space around support cells and OSNs or through the uptake and transcellular transportation by supporting cells into the lamina propria. Although the olfactory epithelium contains tight junction proteins, because of the contestant turnover of OSN (6–8 weeks), intercellular clefts exist that can serve as transport channels [33]. Furthermore, small lipophilic molecules (and many small nanoparticles) can diffuse through the epithelium tight junction proteins into the lamina propria, with the use of excipients that can increase tight junction permeability increasing transport via this mechanism to more hydrophilic/larger small molecules or nanoparticles [34]. Once substances cross into the lamina, propria may be further distributed in one of three ways: (1) travel through perineural and perivascular projections to the CNS, providing a direct route for N2B delivery; (2) be absorbed by blood vessels into systemic circulation; (3) be absorbed into lymphatic vessels that drain to the cervical lymph nodes and eventually into the bloodstream for systemic circulation [35, 36].
Systemic circulation and intracellular transport could require several hours to days for drugs to appear in olfactory bulbs. However, most IN delivery studies show substance detection in the olfactory bulbs within an hour of administration [37], suggesting extracellular pathways along the olfactory nerves are likely the primary transportation mechanism to the CNS. Extracellular diffusion along the perineural space from the lamina propria to the olfactory bulbs is estimated to take 0.73–2.3 h based on published studies [38]. However, studies using [125I]-labelled IGF-1demonstrate rapid delivery to the CNS (~ 30 min), such that perineural diffusion cannot fully explain this observed rapid delivery [39]. Since there are arteries that supply the olfactory nerve with nutrients, bulk flow in the perivascular space may be one mechanism that can mediate rapid N2B transport. Bulk flow occurs due to the systolic vascular waves, which create high-pressure waves within the perivascular space and have a predicted transport time of 0.33 h, consistent with the rate of [125I]-labelled IGF-1 delivery [38].
3.2 The Trigeminal Nerve Pathway
The primary function of the trigeminal nerve is to provide sensory and motor innervation to the facial area or facial tissues. Sensory information such as pain and temperature from the nasal epithelium is relayed through the main trigeminal nucleus to the brainstem. The ophthalmic (V1) and maxillary branches (V2) of the trigeminal nerve (CN5) innervate the nasal cavity and can serve as a direct route for brain drug delivery from the nasal cavity. The trigeminal nerve contains a third branch called the mandibular nerve (V3); however, it does not innervate the nasal cavity and therefore does not contribute to N2B delivery.
Various studies have demonstrated intraneuronal, perineuronal, perivascular, and perilymphatic transport of substances within the trigeminal nerve following IN administration using similar intracellular and extracellular transport mechanisms to the olfactory nerve pathway. Based on published studies, it is estimated that intracellular transport within trigeminal ganglion cells to the brainstem can occur in 3.7–13 h, extracellular diffusion along the trigeminal nerve can occur in 17–56 h, and extracellular bulk flow within the perivascular space of the trigeminal nerve can occur within 1.5–2 h; as such, rapid transport of [125I]-IGF-1 along the trigeminal nerve is likely primarily attributable to bulk flow transport [38, 39].
4 Challenges of Intranasal Delivery
Given the direct connection between the brain and the nasal cavity described above, IN delivery offers a unique way to circumvent many of the primary challenges around treating CNS disorders (i.e., the BBB and peripheral toxicity). However, delivery via the IN route also creates new challenges that need to be considered in the design and development of novel drug formulations for CNS disorders.
4.1 Chemical Limitations
Physiochemical properties of the drugs such as size, molecular weight, and lipophilic-hydrophilic balance significantly limit which drugs can be delivered intranasally and the efficacy of nasal drug absorption. Mucus comprises 90–95% water and thus represents a partitioning-based physiological barrier to the transport of many hydrophobic and highly lipophilic drugs (including many antipsychotics) as well as a diffusive barrier to the transport of larger molecular weight drugs to the nasal epithelium [40]. In addition, while small lipophilic drugs such as progesterone and dimethyl fumarate (DiF) are quickly absorbed through the nasal epithelia, the permeability of large molecules such as peptides and proteins (> 1 kDa) is limited [41, 42]. In general, drugs with a molecular weight < 300 Da can sufficiently permeate the epithelium for direct CNS delivery while substances > 1 kDa tend to get stuck in the mucus [43]. Particle size also affects the amount of drug absorbed, as larger droplets are rapidly cleared given that they are more likely to cause irritation and reflexive sneezing [44].
4.2 Biological Limitations
The nasal mucosa represents a significant barrier against the transport of substances from the external environment to the brain. IN administration of liquid-based formulations can undergo rapid elimination by MCC in as little as ~ 12–15 min, while an additional (often significant) amount is lost due to drainage down the nasopharynx, which limits the contact time for drug absorption [24, 45]. The nasal mucosa also contains defensive metabolic enzymes that act to protect the nasal cavity from harmful xenobiotic substances [46]. However, these enzymes can also metabolize drug products and other small molecules administered intranasally [47], changing their solubility profile and/or their chemical structure to alter drug activity and/or permeation properties [48]. Furthermore, analogous to the P-glycoprotein pumps in the BBB, p-glycoprotein pumps have been discovered in the nasal and olfactory epithelium, septum, sinonasal mucosa, inferior turbinate, and the olfactory bulb, in some cases reducing the absorption of low molecular-weight drugs [49,50,51]. Therefore, to maximize CNS absorption and minimize degradation, both slowing clearance and protecting the drug from enzymatic metabolism must be considered when developing and testing new drug-delivery vehicles.
4.3 Local Tissue Damage
Although, significantly less invasive than intracerebral injection for direct CNS administration [52,53,54], toxicity is a significant concern, especially for chronic conditions (like many CNS disorders) that require repeat treatment administration. Potential adverse effects include nasal irritation, itching, epistaxis, alterations in smell and taste, rhinosinusitis, and damage to the nasal and olfactory epithelium [54]. Maintaining the pH of IN-administered formulations around human nasal pH (5.5–6.5) is also critical for minimizing the risk of nasal irritation and tissue damage [55]; however, many antipsychotics including aripiprazole [56], clozapine [57], olanzapine [58], risperidone [59], and quetiapine [60] are moderately basic in solution, such that prolonged IN use could cause irritation and irreversible damage.
Toxicological considerations are relevant not only for the drug but also for the excipients within the formulations, including preservatives, surfactants and/or other absorption enhancers that may affect cellular contact [15]. In particular, drug formulations containing mucoadhesive agents that function to increase contact time with the nasal epithelium and/or penetration agents that disrupt cellular junctions within the nasal mucosa can pose increased risks of toxic effects. For example, tight junction modulators Clostridium perfringens enterotoxin (CPE) and Zonula occludens toxin (Zot) reversibly open tight junctions to facilitate paracellular drug absorption through nasal epithelia [61, 62], while the C-terminal fragment of CPE (C-CPE) disrupts tight junctions through modulation of claudins and has been used to increase absorption of human parathyroid hormone in rats [63]. However, toxicity is a major concern with such modulators, with repeated administration shown to increase C-CPE-specific serum IgG levels [64]. Hence, derivatives of these absorption enhancers have been synthesized to decrease toxicity and are currently being evaluated for IN administration in vivo [65, 66]. Some drugs can also affect the ciliary beat frequency (e.g. atropine) [67, 68] or inhibit ciliary movement (e.g. local anesthetics such as ketamine/xylazine and fentanyl) [69], increasing the potential for adverse effects.
Changes to or a loss of the sense of smell as a result of IN delivery can also be problematic since olfactory function contributes significantly to the flavour of food and is essential for detecting external hazards such as gas or fire [70, 71]. Indeed, a zinc-containing nasal decongestant spray known as Zicam was withdrawn from the US market in 2009 after it was shown to cause anosmia in some users [72]. Olfaction dysfunction can also diminish the quality of life by decreasing appetite and general enjoyment of aromas [73, 74], reducing long-term patient compliance.
4.4 Patient Heterogeneity
Nasal tolerability depends on many individual factors such as pre-existing illness, allergies, or infections, and patient differences in pH and metabolizing enzymes, influencing how drug formulations interact with the nasal mucosa and their subsequent absorbance [15]. Infections can change the pH and enzymatic makeup of the nasal cavity, and thus affect drug absorption and toxicity; for example, chronic bronchitis can increase nasal pH to 7.6–7.8 [75]. Race and gender differences could also contribute to differences in drug delivery due to related differences in olfaction or respiratory function [76, 77]. Given that many controlled-release vehicles are pH-sensitive, such individual differences in nasal pH may affect how drugs are absorbed, introducing variability in dosing not seen with other routes of administration [55].
4.5 Volume Limitations
A major disadvantage of the IN route is the small nasal cavity size and small surface area for absorption compared with the gastrointestinal tract or the circulatory system. This limits the volume of drug formulation that can be administered to ~ 200 μL, significantly restricting the utility of IN delivery to only the most potent drugs. This is particularly true when factoring in the significant drug losses to systemic circulation, swallowing, inhalation, or other clearance mechanisms [18, 37]; for example, esketamine, the S-enantiomer of ketamine approved as a nasal spray under the trade name Spravato, shows a bioavailability of ~ 48%, significantly higher than that of oral esketamine (~ 8%), but still suggesting that the majority of the drug is cleared through other mechanisms [78]. Currently approved IN drugs for CNS diseases are available in milligram doses (e.g. esketamine, sumatriptan, diazepam, midazolam, and naloxone) (see Table 1), although only small doses in the nanogram range are actually needed for the therapeutic effect in the brain [16].
4.6 Consistency of Administration
Since the olfactory region has a small surface area (~ 5–10 cm2) and is located in the upper part of the nasal cavity, targeting this region can be challenging and result in improper dosing [79]. Drugs intended for the olfactory nerve pathway, if improperly administered, may be absorbed in the highly vascularized respiratory region, limiting the amount of drug reaching the brain and increasing peripheral side effects. Administration devices such as bi-directional nasal insufflators and nasal atomizers are designed to facilitate distribution to specific regions of the nasal cavity while limiting lung deposition. However, the accuracy of these devices is complicated by patient-device interactions, which can result in significant variability in dosing. For example, while IN administration of insulin had been used in small-scale pilot studies to preserve cognitive performance in patients with AD and mild cognitive impairment (MCI) with great success [80], a larger phase 2/3 study revealed feasibility issues associated with the self-administration device. Of the 289 patients administered 40 IU insulin daily in the randomized, double-blind clinical trial, 49 used one administration device that was soon discontinued due to inconsistent dosing reliability; the remaining 240 patients used a new device that, while avoiding any apparent operational issues, resulted in no differences in cognitive (ADAS-cog-12), functional, or cerebrospinal fluid (CSF) markers between the insulin- and placebo-treated groups. This result was attributed to limitations in the consistency of administration between patients [81], and highlights the need for proper IN administration devices that are easy to use. Another recent study examining the quality of daily administration of IN corticosteroid sprays also found that most participants improperly administer the nasal spray according to the recommended steps, and concluded that administration techniques are inadequate in most patients [82]. As such, translational success of N2B delivery vehicles requires addressing this key point.
4.7 Airway Flow
For humans and most animals, the preferred airway is through the nose; as such, treatment of CNS disorders through the nasal cavity may interfere with natural breathing patterns. As almost half of an adult’s total airway resistance is nasal, minor increases in nasal resistance can have significant effects on breathing [83]. Repeat use of nasal sprays or mucoadhesive agents can cause drug-induced rhinitis, inflammation, and congestion of the airways, either due to the drug itself or the additional excipients. In addition, the nasal cycle aims to keep the airway surface hydrated and enables each passageway to take turns in either predominantly undertaking the air-conditioning or mucus clearance functions; this can pose a dosing consistency challenge for drug doses that are not administered to both nostrils evenly [84].
4.8 Animal Model Limitations
Rodents are often used as test subjects in preclinical studies; however, differences in anatomy, limited volume, and administration techniques can limit the translatability of rodent results to humans. While the general structure of the rodent nose is similar to that of humans, the surface area of the olfactory epithelium (the primary contact point for nose-to-brain delivery) accounts for 50% of the surface area of the nasal cavity in laboratory rats but only 10% in humans [85]. The significant difference in relative target area in these models may overestimate the efficacy of many formulations, leading to poor translational results. The small surface area of the rodent nasal cavity also greatly limits the amount of drug formulation that can be administered. In mice, the maximum volume of a drug solution that can be administered is 20–30 μL (for formulations that do not persist in the nasal mucosa) in 1- to 2-μL increments with a 3- to 4-min rest period between each inhalation, requiring between 30 and 45 min per animal [86]. The typical need for anesthesia for IN delivery in animals (again unlike with humans) further extends this required experiment time and may alter transport kinetics [87]. Devices engineered to allow for the IN administration of multiple mice simultaneously can increase feasibility; for example, a mouse-positioning device capable of holding four to eight anesthetized mice in head-down-and-forward position at a time was found to enable more efficient IN administration [86]. The typical use of pipetting for IN rodent delivery may also be a poor representation of practical IN administration techniques in humans that are almost uniformly based on aerosolization. Spray devices have been developed but pose challenges regarding variability in pressure uniformity and dose dispensed and effectiveness. The single-dose electronically pressurized spray device reported by Piazza et al. for IN delivery of nanoparticles to rats in part addressed this concern, with only 50–100 μL of a haloperidol-loaded NP suspension inducing a cataleptic response in rats and transport to the olfactory bulb and striatum at a higher concentration than with a pipette [88]; however, such devices are not trivial to use and are designed for clinic-only use rather than at-home use. As such, not only the formulation but also the delivery mechanism of the formulation (in both animal models and human clinical use) is critical for successful IN delivery.
5 Intranasal Formulation Design Considerations
In 2002 the US Food and Drug Administration (FDA) released documentation on the best practices for the chemistry and manufacturing controls of nasal spray solutions and suspensions. In the following section, we summarize those considerations with respect to each component of a typical IN formulation [89].
5.1 Active Ingredients
Active ingredients refer to the drug compound(s) used for the treatment of the targeted condition. Both the pharmacological function and the physical characteristics of the active ingredient (e.g. particle size distribution, morphology, orientation, impurities, microbial quality, etc.) must be specified within limits set by regulatory standards; for example, drug impurities must be < 0.1%. Active ingredients that can directly be delivered IN (at least without chemical alteration or specific formulation) are typically lipophilic to enable membrane partitioning, have a low molecular weight (< 1 kDa) to facilitate mucosal transport and paracellular transport, are either neutrally charged (to promote transcellular transport) or charged but small (to promote paracellular transport), are stable to oxidation or enzymatic degradation, and are sufficiently water soluble (salt forms) to enable clinically relevant dosing in the small volume suitable for IN delivery [90]. The physiochemical properties of the clinically approved and under investigation IN active ingredients (see Table 2) reflect these key properties, with most molecules being low molecular weight (< 600 Da), lipophilic but slightly water soluble, and potent at low dosages.
As summarized in Table 1, many currently approved IN CNS-targeted formulations contain < 20 mg drug doses per spray due to the high potency of the active ingredients used. Formulations such as nicotine are purposefully formulated at lower concentrations for lower abuse liability due to their quick absorption [91], while IN drugs delivered locally (e.g. allergies, local anesthetics) or low-level systemic drugs (e.g. pain management, diabetes) are often formulated at even lower doses (< 1 mg/spray) due to their improved IN bioavailability.
Of note, compounds with physical properties outside of the traditional range (e.g. insulin, oxytocin, and other larger peptides) are now under investigation in clinical trials for CNS treatment. As such, the highest-impact IN formulations moving forward are likely to enable the delivery of active ingredients that do not meet the conventional criteria for IN delivery but also have key limitations in terms of other delivery mechanisms. Specifically, IN delivery would be particularly useful for active ingredients with one (or more) of three key properties: (1) have low bioavailability via other routes (e.g. proteins and peptides, both of which suffer from high levels of degradation particularly via the oral route but also to some extent the intravenous (IV) route if CNS delivery is desired) [90, 92]; (2) have adverse effects or toxicity via other routes (e.g. zolmitriptan, which slows digestion and thus reduces its own absorption if administered orally) [90]; (3) require very fast action in emergency situations and/or the ability to be administered when the patient is unconscious (e.g. drugs used to treat opioid overdose (naloxone, ~ 3 min) or seizures (midazolam, ~ 12 min) [93], exploiting the fast transport kinetics of IN delivery).
5.2 Excipients
Excipients refer to the additional materials within a nasal spray that are added to improve the formulation and/or better meet the key criteria for IN delivery outlined above. Most excipients can be categorized into one of five major categories, all of which address some of the challenges of IN delivery outlined in section 4; the maximum potency and classification of such excipients (and examples in each class) that have been used in commercial N2B formulations are summarized in Table 3.
-
1.
Buffers can maintain pH and thus reduce nasal irritation and/or maintain the active ingredient in a specific ionization state to regulate its absorption rate.
-
2.
Co-solvents can improve the drug solubility and/or increase drug loading, although water alone is used in most of the already clinically approved formulations.
-
3.
Antioxidants can protect active ingredients from enzymatic or redox-induced degradation (particularly against enzymes in the nasal cavity).
-
4.
Chelating agents or absorption/penetration enhancers can disrupt paracellular tight junctions and/or membrane structures to accelerate active ingredient transport [90, 94].
-
5.
Viscosity enhancers or mucoadhesives can improve nasal cavity retention time and prevent dripping down the throat, thus improving bioavailability.
Currently approved IN formulations use minimal and conventional excipients given that the inherent pharmacokinetics of most of the drugs used are already suitable to traverse the N2B route [90]. For example, the esketamine formulation Spravato (from the FDA label) contains citric acid (buffer and antioxidant), disodium ethylenediaminetetraacetate (EDTA, chelator), sodium hydroxide (pH modification), and water (solvent), while the naloxone formulation Narcan contains benzalkonium chloride (preservative), EDTA (chelator), sodium chloride (to maintain osmotic balance), and hydrochloric acid (pH modification). The selection of absorption enhancers (if required) is particularly challenging, with existing approaches outlined by Davis and Illum in their highly cited 2012 review [95]. Absorption enhancers must balance between transiently disrupting membrane/tight junctions while avoiding toxicity, with the use of chelating agents or surfactants in particular requiring very specific dosing to avoid side effects [96, 97]. Biological polymers such as cellulose variants (including salt forms), chitosan (also including salt forms), cyclodextrins, and biosurfactants (e.g. bile salts, phospholipids, and fatty acids) can avoid some of these toxicity issues but may need to be formulated at higher doses [98]. Although not yet implemented in commercial IN formulations, chitosan (via ionic interactions with membranes) and cyclodextrins (which extract cholesterol from cell membranes via host-guest interactions) are particularly widely studied as nasal permeation enhancers, resulting in up to tenfold increases in drug permeation at concentrations relevant for IN sprays [99].
Materials with mucoadhesive properties are increasingly being explored as soluble excipients and/or for the formation of nanoscale vehicles for IN delivery, aiming to reduce the rate of mucociliary clearance. However, to date, very few commercial CNS-targeting formulations contain a mucoadhesive. Natestro, a testosterone nasal spray for hypogonadism, relies on systemic delivery rather than N2B delivery, but includes colloidal silicon dioxide as a viscosity-enhancing excipient formulation [100], while the Lazanda fentanyl formulation contains pectin, described to turn into a gel in situ with the mucosa [101]. Chitosan is of particular interest moving forward given that it can play a dual role as a permeation enhancer and a mucoadhesive, the latter based on ionic interactions between positively charged primary amines and anionic sialic acid residues in mucin [102]. Illum’s review outlines the utility of chitosan in this context for IN dosages for over two dozen different medications for both N2B CNS treatment and systemic therapy, including formulations for sumatriptan (migraines) and insulin (although focused on systemic delivery for reducing blood glucose levels rather than CNS therapy) [103]. Alternatively, or in combination with using viscosity/mucoadhesion enhancers, the use of in situ-forming hydrogels that can form spontaneously in the nasal cavity following the nebulization of a low viscosity precursor solution can be considered to increase material lifetime within the nasal cavity while also enabling tunable long-term-controlled release of active ingredients that do not need the fast onset of some IN delivered drugs (see sections 7.1 and 7.2). The work of the Berkop-Schnurch group [104,105,106,107] on thiolated polymers is particularly notable with regard to developing mucoadhesive, permeation enhancing, and in situ gelling formulations, with cationic thiolated carbohydrates particularly of interest given their potential to enable mucosal penetration but retain very high mucosal cohesion based on the reversible disulfide formation (Fig. 3); as another example, thiolated xanthan increased mucoadhesion by a factor of 2.5 while reducing muciliary beat frequency by ~50% compared to unmodified xanthan [108]. However, the stabilization of thiolated polymers to long-term storage must be addressed prior to commercial translation of this approach.
Schematic illustrating inter-polymer crosslinking after mucopenetration to establish intimate mucoadhesion, with a chain link cartoon representing the interpenetration and in situ crosslinking of polymers and mucus. Adapted with permission from [105]. Created with BioRender.com
As an alternative to in situ formation, shear stress can also be used to dynamically reduce viscosity to enable the spraying of viscous formulations. Corticosteroid formulations such as Rhinocort and Nasanex as well as the CNS-delivered Imitrex (sumatriptan) use microcrystalline cellulose (MCC) and carboxymethyl cellulose (CMC) as viscosity enhancers that can keep active ingredients/other excipients in suspension upon storage but shear thin upon spraying, with their thixotropy enabling a rapid return to their viscous state within a few seconds once in the nose [16, 109].
6 Nano-Delivery Design Considerations
Nanoscale excipients are an emerging subset of delivery vehicles that aim to address multiple barriers associated with IN delivery in a single vehicle. While simple mixing of drugs and traditional excipients works when dealing with the most potent drugs, nanoparticles can improve active transport via the nasal epithelium, sustain drug-release kinetics, avoid pH limitations (particularly relevant for many antipsychotic drugs), or eliminate the use of solvents and surfactants to reduce nasal epithelial irritation. While the use of nanoparticles to directly transport drug to the brain is the typical paradigm for a nanomedicine-based IN delivery strategy, growing evidence suggests that the use of nanoparticles to pass the initial key barriers to IN delivery (i.e. the mucous and nasal epithelium) may be sufficient to significantly improve IN delivery capacity, leaving the released bioactive itself to navigate the final part of the N2B pathway; indeed, many research groups have found low levels of nanoparticles present in the brain but high efficacy in terms of behavioural results [110], suggesting effective drug transport but not nanoparticle transport. However, there is a trade-off in terms of the role of nanoparticles in increasing the complexity of the formulation and thus perhaps the regulatory pathway to approval; as such, for drugs with high intrinsic pharmacological activity (e.g. esketamine), nanoformulation is typically not pursued [18, 110, 111]. While multiple properties of nanoparticles may influence their success or failure in different delivery contexts (e.g. mucoadhesion/mucopenetration, ability for cell uptake, mechanism of cell uptake, and deformability), size, surface chemistry, charge, and degradability are most commonly used as design variables to tune nanoparticle properties and thus therapeutic efficacy; for additional information on these design variables beyond that provided herein, the reader is referred to many excellent reviews on the topic [105, 112,113,114,115].
6.1 Size, Surface Chemistry, and Charge
Administration though the N2B pathways is limited by size. Nanoparticle sizes of < 200 nm are typically understood to be able to travel through the paracellular tight junctions of the nasal epithelial cells, with nanoparticles of sizes 20–100 nm ideal for both epithelial and axonal transport [116, 117]. For nanoparticles of similar size, the surface chemistry of the nanoparticle primarily dictates its primary transport pathway; introducing hydrophobic surface chemistry (e.g. using lipid nanoparticles) can help increase transcellular transport while the introduction of hydrophilic groups and penetration enhancers can improve paracellular travel [119]. Cationic surface charge in particular can govern two key biological responses to nanoparticles: (1) disrupt tight junctions to allow for increased binding to, and subsequent penetration through, the nasal epithelium; and (2) complex with the highly anionic nasal mucus to promote transmucosal transport [16]. Manipulating charge can also help load therapeutics and/or other excipients that themselves have charges to spontaneously form bioactive nanostructures (e.g. chitosan and lecithin) [118,119,120,121]. Surface chemistry is also key to the stability of nanoparticles in the complex physiological environment, with most nanoparticles stabilized either by high net charge (enabling electrostatic stabilization) or dense PEG-based layers (enabling steric stabilization).
A 2001 study using radiolabelled polystyrene (PS) nanoparticles best illustrates these effects of nanoparticle physical properties on IN penetration [117]. Nanoparticles 20 nm in size had twice the penetration rate of 100 nm nanoparticles, which themselves were twice as effective in penetration than 500–1,000 nm particles (3.25%:2%:1.25% of particles, respectively, reach systemic circulation). Coating the PS nanoparticles with poloxamine 908 (a PEG-like polymer) reduced cellular interactions and thus decreased penetration, while coating with mucoadhesive chitosan doubled particle delivery into systemic circulation (0.3–0.6%) [122]; similar results were shown comparing polysorbate 80 and chitosan-coated lecithin nanoparticles [119].
6.2 Degradation
For chronic use, as required with many CNS-related drugs, the nanoparticle carrier systems need to be degradable as a whole or degradable into their original cytocompatible precursors/monomers. Many inorganic nanoparticles such as metals (silver and gold), quantum dots, and carbon nanotubes have been investigated for CNS delivery and therapy, but most were found to be neurotoxic due to poor clearance and lack of a safe degradation pathway [123]. Polymers that break down into metabolic by-products (e.g. poly(lactic acid), PLA or poly(lactic-co-glycolic acid, PLGA) or carbohydrates that can degrade by hydrolysis or enzymatic action are thus preferable, particularly those that (e.g. PLA/PLGA) degrade into innate metabolic by-products that are regularly processed by the body [109, 122]. However, toxicity of any degradation product must consider not only cell death but also downstream stresses to the cell junctions, membranes, and the BBB and/or nasal epithelium, both of which pose long-term health risks [111]. Nanoparticles with a high drug-loading capacity are thus preferred to deliver the required drug dose at as low as possible an excipient content [109, 123].
7 Nano-Delivery Design for N2B Delivery
The use of nanoparticulate systems for CNS delivery for various therapeutic classes (e.g. antipsychotics [15, 17], peptides/proteins [124,125,126,127], anti-depressants [13], or vaccines [128, 129]) and/or conditions (e.g. AD [14, 130, 131], epilepsy/anxiety [132], and neurodegenerative diseases [126, 133, 134]) has been extensively reviewed by other papers. In this section, we focus specifically on nano-systems designed for already clinically approved IN drugs and/or that use already clinically approved IN excipients to streamline clinical translation. Although the promise of nanoparticles is evident in these examples, we note that it is often hard to quantify those benefits given the lack of direct comparisons between nanoformulations and other already successful formulations in the literature [17, 111, 116]. As such, in the following discussion, we highlight only representative papers that apply different types of nanocarriers to deliver approved drugs, have in vivo proof-of-concept experiments presented, and explicitly show some direct benefit of the nanoparticle formulation for improving IN delivery efficacy versus a solution or conventional formulation.
7.1 Polymeric Nanoparticles
Polymeric nanoparticles consisting of a solid and typically degradable polymer offer highly customizable properties, chemistries, and sizes, with PLGA-based nanoparticles most broadly used for nanoparticle-based formulations given that PLGA is FDA approved. For example, diazepam-loaded PLGA nanoparticles achieved 87% drug entrapment coupled with significantly higher brain accumulation, with brain:blood ratios of 1.4 achieved with the PLGA nanoparticle formulation; in comparison, ratios of 0.17 for IV administration and 0.38 for IN administration (both using a diazepam suspension containing stannous chloride dihydrate, ethanol, acetone, and saline) were achieved [135]. Block copolymers consisting of PLGA linked to a hydrophilic polymer (typically poly(ethylene glycol), PEG) can also be used as the building block for the polymeric nanoparticle, with the PEG block serving to enhance nanoparticle stability and modify the mucoadhesion between the nanoparticle and the nasal mucosa. For example, we previously reported the use of PEG-PLGA nanoparticle bearing Solanum tuberosum lectin (STL-NPs) to deliver haloperidol (HP), a hydrophobic schizophrenia drug. Minimal HP was observed in the striatal tissue and none in the olfactory bulb tissue 1 h after intraperitoneal (IP) injection of an HP drug solution or HP-loaded nanoparticles; in contrast, IN administration of the nanoparticle + drug resulted in significant levels of drug in the brain (Fig. 4a, b) [136]. However, the relatively long degradation time and the acidic degradation by-products of PLGA may cause challenges over long-term repeated IN dosing.
Haloperidol detection in the a brain striatal tissue or b olfactory bulb tissue 1 h after intraperitoneal (IP) or intranasal (IN) administration of haloperidol delivered alone in solution or loaded in PEG-PLGA nanoparticles (NPs) with or without Solanum tuberosum lectin (STL) targeting of the nasal mucosa. Adapted with permission from [136]
7.2 Hydrogels
Hydrogels are water-swollen crosslinked polymer networks that offer the benefits of high hydration, physical deformability, and high loading capacity and stabilization potential particularly for biopolymer-based drugs (e.g. proteins, peptides, polynucleotides) [128]. The polymer matrix can also be designed to be responsive to physiological stimuli either in terms of forming the crosslinks (in situ gelling) or triggering the release of drugs (responsive); in particular, rapidly in situ forming hydrogels can be advantageous to deliver minimally viscous precursor solutions under the shear stress of nebulization (facilitating well-distributed spray uniformity and droplet size for optimal deposition) while ensuring high retention in the nasal cavity [114, 136, 137]. Creating nanoparticles of hydrogels, or incorporating other types of nanoparticles inside a hydrogel, can combine the useful benefits of a hydrogel with the penetration benefits of nanoparticles to create effective IN delivery vehicles [127, 137, 138].
7.2.1 Hydrogel Nanocomposites and Nanoparticle Networks
Hydrogel nanocomposites and nanoparticle networks work on a similar philosophy of utilizing the hydrogel matrix to be a mucoadhesive “depot” within the nose while the entrapped (nanocomposite) or crosslinked nanoparticles (nanoparticle network) actively transport drug across the nasal epithelium upon the mucociliary degradation of the hydrogel (Fig. 5). Such an approach ensures nanoparticle suspension (promoting active transport), enables facilely tunable degradation mechanisms, and (depending on the choice of nanoparticle) can enable the delivery of more hydrophobic therapeutics that are otherwise difficult to deliver using a hydrogel formulation [18].
We recently published the use of an in situ-forming Schiff base-crosslinked hydrogel between oxidized (aldehyde-functionalized) starch nanoparticles (SNPs) and carboxymethyl chitosan to deliver a short peptide (PAOPA, 254 Da molecular weight). The Schiff base crosslinks form rapidly upon spraying the liquid precursors inside the nose to form a thin film of mucoadhesive hydrogel droplets that degrade to release the ultra-small (20–50 nm diameter) SNPs that can subsequently penetrate the nasal epithelium and transport to the brain, enabling full functional recovery of MK-801-induced schizophrenic symptoms over at least 3 days following a single spray due to the dual role of the hydrogel in controlled release and promoting IN transport (Fig. 6) [139]. Efficacy is linked to both direct SNP transport to the brain as well as apparent uptake of the SNPs by nasal epithelial cells to act as a drug depot for olfactory nerve transport. A similar system could be used for other peptides such as oxytocin, a 1007 Da peptide with potential for autism treatment but with significant short-term and long-term adverse side effects if administered non-specifically [140].
Schematic illustrating the use of nanoparticle (NP) network in situ-forming hydrogel for the controlled release of PAOPA (peptide), resulting in a significant behavioural improvement in a schizophrenia model over 3 days following a single spray. Reproduced with permission from [139]
7.2.2 Nanogels
Given their highly hydrated morphology, nanogels have been mainly used for the delivery of peptides, DNA, RNA, growth factors, and other biological hydrophilic therapeutics [124, 128]; while not generally not used for hydrophobic therapeutic delivery due to their water-swollen structure, recent advances in nanogel design are challenging this paradigm [141]. The key challenge for the use of nanogels is to access synthetic strategies that enable the fabrication of < 100 nm nanogels with sizes that enable effective IN transport, although the inherent deformability of nanogels may enable the transport of larger diameter nanogels IN relative to other types of (stiffer) nanoparticles. For example, the Di Carlo lab at the University of California at Los Angeles (UCLA) has reported several nanogel-based delivery strategies for insulin delivery, including recent work using e-beam irradiation to crosslink poly(N-vinyl pyrrolidone) (PVP) and acrylic acid to form a 70-nm nanogel that meets the size criteria for effective IN transport; insulin was conjugated via carbodiimide chemistry to ensure co-delivery of insulin and the nanogel to the targeted site, showing a promising biodistribution and toxicity profile in vivo (Fig. 7a) [142, 143]. Alternately, Masjedi et al. fabricated nanogels via ionic crosslinking of mucoadhesive chitosan with tripolyphosphate (TPP) in the presence of sumatriptan, resulting in nanoparticles with a mean particle diameter of ~ 105 nm and zeta potential of ~ + 27 mV (both ideal for IN drug capture and subsequent transport [113]), good loading efficiency (~ 59%) and controlled release of sumatriptan (~ 68% release over 72 h) (Fig. 7b) [144]. In vivo assessment comparing IV versus IN administrations showed a ~ 500% increase in the concentration of sumatriptan in the brain relative to IN or IV administration of a drug solution, with the nanogel acting as a permeation enhancer to deliver the drug via axonal transport while also slowing the drug release to enable prolonged therapeutic efficacy (albeit delaying the time to maximum concentration compared to the solution expected to travel solely along extracellular transport).
Nanogels for intranasal delivery to the brain: a Schematic illustrating the use of PVP/poly(acrylic acid) nanogels to deliver insulin to the brain along the trigeminal and olfactory nerves. Adapted with permission from [143]. b Drug concentration in the brain of animals comparing a sumatriptan solution in saline compared to chitosan/TPP nanogel encapsulated sumatriptan, with the nanogel resulting in a 1-h delay in maximum concentration time but a 5 times higher level of drug after 4 h. Adapted with permission from [144]
7.3 Lipid-Based Nanosystems
Lipid-based nanosystems have been gaining popularity for oral drug administration since they show high gastric mucoadhesion and penetration; given that the nasal mucosa is similar in composition but much less thick (5–20 μm [43]), similar benefits are anticipated for IN delivery [114]. The types of lipids used in these designs strongly govern their resulting morphology (e.g. solid lipid nanoparticles, nanoemulsions, micelles, liposomes, niosomes, and hybrid nanostructured lipid complexes; see Fig. 8), and thus their potential to deliver different drugs via different transport mechanisms.
7.3.1 Solid Lipid Nanoparticles
Solid lipid nanoparticles (SLNs) are the simplest type of lipid-based nanocarrier, consisting of a mixture of solid lipids and surfactants and typically fabricated by sonication or high-speed homogenization followed by solvent evaporation [144, 145]. Relative to other lipid-based nanoparticles, SLNs are easy to fabricate, have high uniformity, and can effectively load hydrophobic therapeutics, although the solid and often crystalline nature of the core can result in lower drug-carrying capacity than liquid structures. As an example of the use of SLNs for IN delivery, ~ 200 nm solid lipid nanoparticle naloxone nanocarriers fabricated using a combination of the lipid glyceryl monostearate (GMS, selected due to its ability to solubilize naloxone) and a combination of Pluronic F127 and Tween 80 surfactants were demonstrated to enable prolonged deposition in the nose and brain compared to an equivalent dose of labelled free NLX solution (Fig. 9) [146].
Pharmacoscintigraphy study showing intranasal nasal and brain retention of radiolabelled solid lipid nanoparticles (SLN) loaded with naloxone (NLX): (upper) NLX-loaded SLN-NLX; (lower) NLX free solution. Adapted with permission from [146]
7.3.2 Nanoemulsions
Nanoemulsions (NEs) have similar structures to SLNs but use liquid lipids (often natural lipids like coconut or sesame oil, selected to optimize the solubility of the drug to be encapsulated) instead of solid lipids [147]. Several reviews describe the use of nanoemulsions for delivering a diverse set of drugs IN including the antipsychotic drugs risperidone, ziprasidone hydrochloride, quetiapine, the antiepileptic drug amiloride and prospective Alzheimer’s disease therapeutics such as huperzine A, memantine, and donepezil [147, 148]. Nanoemulsions can also incorporate mucoadhesive components to further enhance their potential for IN delivery [149]. As one such example, the anti-migraine drug zolmitriptan (ZT) typically has low oral bioavailability (40%) and a short half-life (1–2 h) as well as high fat solubility and low permeation, suggesting the benefit of an IN delivery vehicle. A mixture of oils, surfactants, and co-surfactants consisting of Capryol PGMC (propylene glycol monocaprylate), Kolliphore RH40 (polyoxyl 40 hydrogenated castor oil), and Transcutol-P (diethylene glycol monoethyl ether) formulated into a nanoemulsion was observed to increase drug permeation from < 10% in solution (similar to its oral bioavailability) to ~ 70% (NE encapsulated) over 2 h, with further addition of mucoadhesive chitosan (MNE) enhancing uptake to > 85% over the same period (Fig. 10) [150].
Nanoemulsions (NEs) consisting of Capryol PGMC, Kolliphore RH40, and Transcutol-P significantly improve permeation relative to solution (Soln) formulations, with chitosan-containing formulations (MNE1—0.3 mg/mL chitosan or MNE2—0.5 mg/mL chitosan) further improving permeation in a murine model (measured in phosphate buffer, pH 6.8). Reproduced with permission from [150]
7.3.3 Micelles
Micelles are self-assembled lipid nanoparticles whose core is formulated solely from the tails of the surfactants and synthetic polymer co-surfactants also stabilizing the surface layer, unlike SLNs or NEs whose cores are primarily composed of another type of lipid material stabilized by surfactants. As such, micelles are typically much smaller but also potentially less cytocompatible for in vivo delivery applications depending on the surfactant(s) used. For example, zolmitriptan micelles fabricated by dissolving in the drug into diethylene glycol monoethyl ether (penetration enhancer) and benzyl alcohol (common excipient), followed by adding surfactants PF127 (50 mg), PEG-400 (100 mg), and TPGS (50 mg) showed a ~ 3.5- to 6-fold higher uptake into the brain following IN delivery compared to a radiolabelled solution over the 4-h measurement period [151]. The ease of fabrication (typically via water-induced self-assembly) coupled with the capacity for solubilizing hydrophobic drugs must be balanced with the potential toxicity of the surfactant(s) depending on the dose of drugs that must be delivered.
7.3.4 Liposomes and Niosomes
Liposome and niosomes are bilayer membrane-mimetic nanoparticles, typically made via either thin film hydration or membrane emulsification [151, 152]. Liposomes are more commonly used given that they consist of phospholipids that are natural penetration enhancers via membrane adsorption mechanisms; the non-ionic surfactants (e.g. polyoxyethylene and polyhydric alcohols) used to construct niosomes may have lower ciliotoxicity and congestion effects but also typically lower solubility [98, 115, 153]. In either case, the presence of both a hydrophilic inner cavity and the hydrophobic bilayer allows dual loading of both water-soluble and -insoluble drugs, although the stability and leakiness of liposomes in particular relative to other nanocarriers discussed can be a limitation in some applications. As an example of an IN liposome, 1,2-dimyristoyl-sn-glycero-3-phosphocholine (DMPC) and 1,2-dimyristoyl-sn-glycero-3-phosphoglycerol (DMPG) phospholipids were used to form liposomes via solvent evaporation/rehydration in a fentanyl solution could maintain analgesic effects for at least 45 min while the corresponding fentanyl citrate solution (in saline) lost efficacy at 30 min; in tandem, a ~ 20% reduced plasma concentration of fentanyl was observed over 2 h after IN delivery via the liposome, suggesting improved specificity of brain transport with the liposome [152]. As an example of a niosome, ZT was loaded at high efficiency (~ 93%) into niosomes via a thin film hydration of cholesterol, Span 80, and stearic acid, enabling significantly higher brain and reduced blood retention (2.36:1 brain:blood ratio after 24 h) of IN ZT compared to an IV injection of ZT (0.02:1 blood:brain ratio after 24 hours) in Swiss albino mice [153]. Tosymra, a sumatriptan nasal spray clinically approved in 2019, also uses an excipient called Intravail that consists of a blend containing alkyl glycosides and/or saccharide alkyl esters consistent with niosome formulations, although it is not entirely clear if the delivery vehicle is indeed a niosome once sprayed into the nose [94, 154, 155].
7.3.5 Nanostructured Lipid Complexes
Nanostructured lipid carriers (NLCs) are a second generation of lipid nanoparticles composed of physiological lipids such as mono-, di-, and triacyclglycerols that form imperfect, amorphous, or mixed/multiple phase structures [156]. The combination of liquid and solid lipids in the core typically allows for higher drug-loading capacity (typically in interstitial space between solid crystalline fatty acid domains), faster release rates, and higher storage stability, all beneficial for IN delivery [114]. Although no NLCs are used in current IN clinical trials, pre-clinical studies have suggested the promise of this approach [157]. For example, NLCs made of a combination of Brij 35, Brij 72, triolein, and cholesterol using a solvent diffusion/evaporation strategy resulted in the formation of ~ 100 nm nanoparticles that enabled 91% loading of sumatriptan and sustained release over 72 h. Compared to the earlier discussed example in which sumatriptan was loaded into chitosan-TPP nanogels, the NLC formulation enabled higher drug loading and improved pharmacokinetics (547 ng/mL per h area under the curve vs. 343 ng/mL per h for the nanogel formulation over the 4-h delivery time) but lower brain transport (258% increase relative to the drug solution compared to 493% for the nanogel formulation), the latter hypothesized to be due to the anionic rather than cationic charge of the NLCs. Using a similar approach, the seizure medication phenytoin sodium (fosphenytoin), typically used as a second-line IV treatment, was fabricated into an NLC formulation by melt emulsification of cholesterol, oleic acid, and poloxamer 188 using a probe sonicator (Fig. 11) [158]. NLC sizes from 32 to 125 nm could be achieved depending on the sonication time, with the highest encapsulation efficiency (~ 91%) achieved for < 50 nm nanoparticles that also showed the fastest degradation and release profile. A large IN pharmacokinetic study with Wistar rats comparing the small phenytoin-loaded NLC (IN solution and spray) to a marketed midazolam formulation (IN, the first-line benzodiazepine seizure medication) and marketed phenytoin (IV) at the same dosage indicated that the NLC formulation could deliver phenytoin with significantly higher brain:plasma ratios compared to the commercial midazolam spray, the latter of which showed a spike in plasma concentration within the first 5–20 min and little to no brain penetration overall after 10 min.
Fabricating phenytoin-loaded nanostructured lipid carriers enabling improved transport of antiseizure medication to the brain. Reproduced with permission from [158]
8 Future Perspectives
While a variety of IN small-molecule and peptide formulations have been investigated to address multiple CNS delivery challenges, the IN route is still overall underexplored for many therapeutics. Drugs or other therapeutics such as peptides, plasmids, or vaccines were initially assumed to be inefficient or impractical to use due to low bioavailability, low plasma stability, and/or safety concerns may be made practical using IN delivery and/or (even if they were previously ineffective via the IN route) using new IN excipients. Below, we highlight three key technological areas encompassing both novel excipient design and the delivery of diverse bioactives that will offer particular opportunities to leverage the benefits of IN delivery for real clinical impact.
8.1 Multi-Scale Drug Delivery Vehicles
As previously described, hydrogels are beneficial in IN delivery due to their viscosity (innate, stimulated, or in situ forming), which prevents mucocilliary clearance and enables sustained release of drugs; however, the benefits of nanoparticles in facilitating active transport to the brain are not leveraged with traditional hydrogels. In this context, nanogel clusters offer in our view particular promise given that the overall cluster properties (size, charge) can be designed to enable optimal mucoadhesion and deposition while the clustered nanoparticles can deliver any type of drug (depending on the type of nanocarrier chosen) across the nasal epithelium to leverage the N2B pathway the cluster breaks down. Successful application of this method depends on the fabrication of uniform ultra-small nanoparticles to use as the basis of cluster formation, which can be challenging for some nanocarrier types (particularly nanogels designed for protein/peptide delivery). The Akiyoshi group has done particularly innovative work on this point by leveraging their cholesteryl functionalized pullulan nanogels (cCHPs) for drug/therapeutic delivery [159, 160], including IN vaccine designs that have been validated in mice and macaques [161, 162]. cCHP nanogels are small (~ 40 nm), have a weak cationic surface charge promoting mucoadhesion and cell uptake (~ + 7 mV), are biodegradable (based on pullulan), and can load both hydrophilic drugs (nanogel bulk phase) and hydrophobic drugs (self-associated cholesterol nanodomains). Nanoclusters formed through the use of thiol-modified poly(ethylene glycol) to crosslink cCHPs into a ~ 120-nm nanocluster and/or the external decoration of exosomes with cCHPs to form a ~ 150-nm nanocluster both increase the overall nanoparticle size to the 100- to 200-nm size range optimal for sprayability and storage while controlling the degradation rate (via slow hydrolysis or electrostatic dissociation) to release the small cCHPs over time proximal to the nasal epithelium to enable effective parascapular transport (Fig. 12) [163]. Our starch nanoparticle-based sprayable nanoparticle network hydrogels (see Sect. 7.2.1) have a similar advantage, with the chitosan component providing mucoadhesion and the small SNP particle size (25–40 nm major fraction) enabling effective N2B transport [139]. Such nanocluster designs in our view balance the different biological and transport barriers while also providing high flexibility for delivering different types of therapeutic payloads.
Cholesterol-bearing pullulan-based nanoparticle intranasal delivery vehicles: a fabrication of nanogel clusters made of CHP nanogels and crosslinked with thiolated 4-arm PEG. Adapted with permission from [160]. b Chemical structure and schematic illustration of amino group-modified cholesterol-bearing pullulan and the nanogel. c Conceptual diagram of nanogel/exosome hybrid delivery. Adapted with permission from [163]
8.2 Gene Therapy
Given that IN delivery of proteins results in only a fraction of the intended dose reaching the brain target sites, gene therapy offers a potentially renewable source of any protein therapeutic. Monogenic disorders are typically thought to be ideal candidates for gene therapy because they are caused by a single gene mutation that simplifies the identification of the defective sequences. For instance, a single IV administration of an adeno-associated viral (AAV) vector coding for the mutated survival motor neuron 1 gene (which results in spinal muscular atrophy type 1) resulted in prolonged survival and better motor function than the control group [164]. Disorders such as Alzheimer’s disease, which may be caused by multigene mutations and environmental factors, are harder to treat using gene therapy; for example, while intracerebral gene delivery of AAV2 nerve growth factor (NGF) has been attempted, NGF expression did not reach the cholinergic neurons due to a limited spread and inaccurate stereotactic targeting [165, 166]. Thus, there remains a need for improved gene delivery to the CNS.
Several groups have demonstrated IN gene therapy delivery to the CNS, primarily using viral vectors such as AAV9 given that AAV therapy is safer than lentiviral therapy [167, 168]. However, even though AAV is non-pathogenic, currently approved AAV gene therapies are limited to a one-time administration due to the typically high immune response achieved on a second dose based on the immunogenicity of the viral protein [169]. As such, non-viral gene therapy is increasingly being investigated to circumvent these inherent risks, with cationic polymers, cationic lipids, nanoparticles, and naked DNA all having been shown to offer improved safety profiles while also being less expensive to produce compared to viruses [168, 170, 171]. For example, non-viral IN pGDNF has been previously delivered via polyelectrolyte complexation with 10-kDa polyethylene-glycol (PEG)-substituted lysine 30-mers (CK30PEG10K) in a rodent model of Parkinson’s disease, showing effective transfection while avoiding significant immunogenicity [172].
Many novel transfection designs, particularly those that use cationic liposomes, have been developed and could be translated to CNS-targeted IN administration. The potential for liposomes to carry the hydrophilic transfection agent in its aqueous core while also promoting transcellular uptake (via the lipophilic shell) and mucoadhesion (cationic charge, expected also to increase DNA loading) is highly attractive in this context. As an example, mRNA+ lipid nanoparticles composed of the cationic lipid dioleoylphosphatidylethanolamine (DOPE), cholesterol, and one of myristatic acid, retinoic acid (nuclear homing via vitamin A scaffold), or tocopherol succinate (most hydrophobic) resulted in a ~ 1:2:5-fold increase in transfection-induced luciferase activity [173]. Similarly shaped and functionalized 1,2-dioleoyl-3-trimethylammonium-propane (DOTAP) has also been used in IN vaccine delivery, with liposomes formed combining DOTAP with cholesterol and 1,2-distearoyl-sn-glycero-3-phosphoethanolamine-N-[methoxy(polyethyleneglycol)-2000 and mRNA demonstrating fluorescent protein gene expression in mice brains. However, the relatively lower transfection efficiency of most non-viral vehicles still remains a limitation of the wide-spread adoption of this approach, requiring improved solutions for effective DNA/RNA delivery in this context.
8.3 Improving Delivery Efficacy
The challenges and inconsistencies of nasal sprays suggest the need to develop more controllable and less user-dependent strategies to exploit the IN delivery route while ensuring appropriate doses of drugs are consistently delivered. As an alternative to sprays, fast dissolving films placed within the nose have been used to deliver insulin directly to the olfactory region [174, 175]. For example, Mohamad et al. encapsulated insulin in a thin film of hydroxypropyl methyl cellulose and polyvinyl alcohol that dissolves within < 1 min of being placed in the nasal cavity, leading to significantly improved olfactory performance in 49 post-COVID-19 patients suffering from anosmia [176]. While mucocilliary clearance typically limits drug absorbance, the lack of motile cilia in the olfactory region results in reduced drug clearance, suggesting the potential for fast-dissolving films to deliver therapeutics in this area. This technique does offer translational challenges given that film size/thickness would need to be nasal cavity-specific and patients may experience some short-term discomfort as the film dissolves; however, based on the defined size/shape of the film, both the location and the quantity of drug administered would be more consistent. Alternately, designing handheld IN spray devices that can be reliably and directly used by the full scope of patient populations targeted for IN CNS therapies offers tremendous potential benefits. For example, the recently published Precision Olfactory Delivery (POD) system is an upper nasal space-targeting delivery device that uses biphasic emission to first release the drug and second propel the formulation deeper into the upper turbinates. The device is currently in several clinical trials for its efficacy in the delivery of several CNS drugs such as dihydroergotamine mesylate (approved for migraines, see Tables 1 and 2), olanzapine (acute agitation), and carbidopa/levodopa (Parkinson’s disease) [11]. Other innovative methods to ensure consistent, even, and ideally automated sprays would also have a significant impact on the practicality of IN delivery for the broad potential target patient population.
9 Conclusions
IN treatment of CNS conditions enables the delivery of both new and old therapeutics to the brain through a more efficient, faster onset, safer, and more bioavailable route. The increasing sophistication of the design of IN delivery vehicles is now enabling the use of the IN drug delivery pathway for the therapeutics that do not have the required hydrophilic/hydrophobic balance, solubility, penetration, or stability to be directly administered IN. That being said, more complex formulations such as nanoparticles must only be pursued if the added benefits of higher surface area and penetration counterbalance the manufacturing and regulatory challenges of nanoscale carriers. More rigorous comparisons of IN formulations with free drug solutions also delivered IN are to date not always reported but represent a better measure of the true success of an IN formulation design. Similarly, while mucoadhesive/penetration, size, charge, and release are commonly reported for IN delivery vehicles, the nebulization capacity, NP in vivo tracking, and long-term formulation stability are not consistently described in the literature despite being key parameters in terms of enabling reliable administration and drug dosing essential for regulatory approval of new IN therapeutics.
Furthermore, despite the benefits of the IN route over oral and other routes, there are still significant challenges that limit the translatability of IN formulations for the treatment of neurological and psychiatric disorders. The successful transition of preclinical models to clinical practice is still a major obstacle given the anatomical differences in the nasal cavities of humans and laboratory test animals. Many nanotechnology-based delivery systems are still in the proof-of-concept stage, even for drugs that are already approved for human use via other routes (or vehicles based on materials already approved for other uses). Additionally, the balance between enhancing penetration through the nasal epithelium/mucosa, increasing transport to the brain, and minimizing the IN toxicity of IN formulations remains a challenge for many formulations. An improved understanding of how different types of excipients affect each step in the delivery pathway is essential to facilitate the rational design of new IN carriers.
References
Pfefferbaum B, North CS. Mental health and the Covid-19 pandemic. N Engl J Med. 2020;383(6):510–2.
Whiteford HA, Ferrari AJ, Degenhardt L, Feigin V, Vos T. The global burden of mental, neurological and substance use disorders: an analysis from the global burden of disease study 2010. PLoS ONE. 2015;10(2):1–14. https://doi.org/10.1371/journal.pone.0116820.
Daneman R, Prat A. The blood–brain barrier. Cold Spring Harb Perspect Biol. 2015. https://doi.org/10.1101/CSHPERSPECT.A020412.
Profaci CP, Munji RN, Pulido RS, Daneman R. The blood–brain barrier in health and disease: important unanswered questions. J Exp Med. 2020. https://doi.org/10.1084/JEM.20190062/151582.
Pardridge WM. The blood–brain barrier: bottleneck in brain drug development. NeuroRx. 2005;2(1):3–14. https://doi.org/10.1602/NEURORX.2.1.3.
Benedetti MS, et al. Drug metabolism and pharmacokinetics. Drug Metab Rev. 2009;41(3):344–90. https://doi.org/10.1080/10837450902891295.
Homayun B, Lin X, Choi HJ. Challenges and recent progress in oral drug delivery systems for biopharmaceuticals. Pharmaceutics. 2019. https://doi.org/10.3390/PHARMACEUTICS11030129.
Arora P, Sharma S, Garg S. Permeability issues in nasal drug delivery. Drug Discov Today. 2002;7(18):967–75. https://doi.org/10.1016/S1359-6446(02)02452-2.
Agarwal SK, Kriel RL, Brundage RC, Ivaturi VD, Cloyd JC. A pilot study assessing the bioavailability and pharmacokinetics of diazepam after intranasal and intravenous administration in healthy volunteers. Epilepsy Res. 2013;105(3):362–7. https://doi.org/10.1016/J.EPLEPSYRES.2013.02.018.
Dufes C, Olivier JC, Gaillard F, Gaillard A, Couet W, Muller JM. Brain delivery of vasoactive intestinal peptide (VIP) following nasal administration to rats. Int J Pharm. 2003;255(1–2):87–97. https://doi.org/10.1016/S0378-5173(03)00039-5.
Hoekman J, Ray S, Aurora SK, Shrewsbury SB. The upper nasal space—a novel delivery route ideal for central nervous system drugs. US Neurol. 2020;16(1):25. https://doi.org/10.17925/USN.2020.16.1.25.
Kashyap K, Shukla R. Drug delivery and targeting to the brain through nasal route: mechanisms, applications and challenges. Curr Drug Deliv. 2019;16(10):887–901. https://doi.org/10.2174/1567201816666191029122740.
Xu J, Tao J, Wang J. Design and application in delivery system of intranasal antidepressants. Front Bioeng Biotechnol. 2020;8: 626882. https://doi.org/10.3389/FBIOE.2020.626882.
Rabiee N, et al. Polymeric nanoparticles for nasal drug delivery to the brain: relevance to Alzheimer’s disease. Adv Ther. 2021;4(3):2000076. https://doi.org/10.1002/ADTP.202000076.
Keller LA, Merkel O, Popp A. Intranasal drug delivery: opportunities and toxicologic challenges during drug development. Drug Deliv Transl Res. 2021. https://doi.org/10.1007/S13346-020-00891-5.
Tan MSA, Parekh HS, Pandey P, Siskind DJ, Falconer JR. Nose-to-brain delivery of antipsychotics using nanotechnology: a review. Expert Opin Drug Deliv. 2020;17(6):839–53. https://doi.org/10.1080/17425247.2020.1762563.
Kumarasamy M, Sosnik A. The nose-to-brain transport of polymeric nanoparticles is mediated by immune sentinels and not by olfactory sensory neurons. Adv Biosyst. 2019. https://doi.org/10.1002/ADBI.201900123.
Katare YK, et al. Intranasal delivery of antipsychotic drugs. Schizophr Res. 2017;184:2–13. https://doi.org/10.1016/J.SCHRES.2016.11.027.
Sobiesk JL, Munakomi S. Anatomy, head and neck, nasal cavity. StatPearls. 2021. [Online]. https://www.ncbi.nlm.nih.gov/books/NBK544232/. Accessed 24 Jan 2022.
Illum L. Nasal drug delivery—possibilities, problems and solutions. J Control Release. 2003;87(1–3):187–98. https://doi.org/10.1016/S0168-3659(02)00363-2.
Patel RG. Nasal anatomy and function. Facial Plast Surg. 2017;33(1):3–8. https://doi.org/10.1055/S-0036-1597950.
Jafek BW. Ultrastructure of human nasal mucosa. Laryngoscope. 1983;93(12):1576–99. https://doi.org/10.1288/00005537-198312000-00011.
Bustamante-Marin XM, Ostrowski LE. Cilia and mucociliary clearance. Cold Spring Harb Perspect Biol. 2017. https://doi.org/10.1101/CSHPERSPECT.A028241.
Marttin E, Schipper NGM, Coos Verhoef J, Merkus FWHM. Nasal mucociliary clearance as a factor in nasal drug delivery. Adv Drug Deliv Rev. 1998;29(1–2):13–38. https://doi.org/10.1016/S0169-409X(97)00059-8.
Oneal RM, Beil J, Schlesinger J. Surgical anatomy of the nose. Otolaryngol Clin N Am. 1999;32(1):145–81. https://doi.org/10.1016/S0030-6665(05)70119-5.
Moran DT, Rowley JC, Jafek BW, Lovell MA. The fine structure of the olfactory mucosa in man. J Neurocytol. 1982;11(5):721–46. https://doi.org/10.1007/BF01153516.
Field PM, Li Y, Raisman G. Ensheathment of the olfactory nerves in the adult rat. J Neurocytol. 2003;32(3):317–24. https://doi.org/10.1023/B:NEUR.0000010089.37032.48.
Smith KE, Whitcroft K, Law S, Andrews P, Choi D, Jagger DJ. Olfactory ensheathing cells from the nasal mucosa and olfactory bulb have distinct membrane properties. bioRxiv. 2019. https://doi.org/10.1101/640839.
Harkema JR, Carey SA, Wagner JG. The nose revisited: a brief review of the comparative structure, function, and toxicologic pathology of the nasal epithelium. Toxicol Pathol. 2006;34(3):252–69. https://doi.org/10.1080/01926230600713475.
Thorne RG, Emory CR, Ala TA, Frey WH. Quantitative analysis of the olfactory pathway for drug delivery to the brain. Brain Res. 1995;692(1–2):278–82. https://doi.org/10.1016/0006-8993(95)00637-6.
Baker H, Spencer RF. Transneuronal transport of peroxidase-conjugated wheat germ agglutinin (WGA-HRP) from the olfactory epithelium to the brain of the adult rat. Exp Brain Res. 1986;63(3):461–73. https://doi.org/10.1007/BF00237470.
Balin BJ, Broadwell RD, Salcman M, El-Kalliny M. Avenues for entry of peripherally administered protein to the central nervous system in mouse, rat, and squirrel monkey. J Comp Neurol. 1986;251(2):260–80. https://doi.org/10.1002/CNE.902510209.
Purves D, et al. The olfactory epithelium and olfactory receptor neurons. 2001. [Online]. https://www.ncbi.nlm.nih.gov/books/NBK10896/. Accessed 24 Jan 2022.
Ahmad AB, Bennett PN, Rowland M. Influence of route of hepatic administration on drug availability. J Pharmacol Exp Ther. 1984;230(3):718–25.
Nedelcovych MT, et al. Pharmacokinetics of intranasal versus subcutaneous insulin in the mouse. ACS Chem Neurosci. 2018;9(4):809–16. https://doi.org/10.1021/ACSCHEMNEURO.7B00434.
Yoffey JM, Sullivan ER, Drinker CK. The lymphatic pathway from the nose and pharynx : the absorption of certain proteins. J Exp Med. 1938;68(6):941–7. https://doi.org/10.1084/JEM.68.6.941.
Erdő F, Bors LA, Farkas D, Bajza Á, Gizurarson S. Evaluation of intranasal delivery route of drug administration for brain targeting. Brain Res Bull. 2018;143:155–70. https://doi.org/10.1016/J.BRAINRESBULL.2018.10.009.
Lochhead JJ, Thorne RG. Intranasal delivery of biologics to the central nervous system. Adv Drug Deliv Rev. 2012;64(7):614–28. https://doi.org/10.1016/j.addr.2011.11.002.
Thorne RG, Pronk GJ, Padmanabhan V, Frey WH. Delivery of insulin-like growth factor-I to the rat brain and spinal cord along olfactory and trigeminal pathways following intranasal administration. Neuroscience. 2004;127(2):481–96. https://doi.org/10.1016/J.NEUROSCIENCE.2004.05.029.
Ozsoy Y, Gngör S. Nasal route: an alternative approach for antiemetic drug delivery. Expert Opin Drug Deliv. 2011;8(11):1439–53. https://doi.org/10.1517/17425247.2011.607437.
Esposito E, et al. Nanoformulations for dimethyl fumarate: physicochemical characterization and in vitro/in vivo behavior. Eur J Pharm Biopharm. 2017;115:285–96. https://doi.org/10.1016/J.EJPB.2017.04.011.
Pires A, Fortuna A, Alves G, Falcão A. Intranasal drug delivery: how, why and what for? J Pharm Pharm Sci. 2009;12(3):288–311. https://doi.org/10.18433/J3NC79.
Donovan MD, Flynn GL, Amidon GL. Absorption of polyethylene glycols 600 through 2000: the molecular weight dependence of gastrointestinal and nasal absorption. Pharm Res. 1990;7(8):863–8. https://doi.org/10.1023/A:1015921101465.
Gänger S, Schindowski K. Tailoring formulations for intranasal nose-to-brain delivery: a review on architecture, physico-chemical characteristics and mucociliary clearance of the nasal olfactory mucosa. Pharmaceutics. 2018. https://doi.org/10.3390/PHARMACEUTICS10030116.
Shaikh R, Raj Singh T, Garland M, Woolfson A, Donnelly R. Mucoadhesive drug delivery systems. J Pharm Bioallied Sci. 2011;3(1):89. https://doi.org/10.4103/0975-7406.76478.
Dahl AR, Hadley WM. Nasal cavity enzymes involved in xenobiotic metabolism: effects on the toxicity of inhalants. Crit Rev Toxicol. 1991;21(5):345–72. https://doi.org/10.3109/10408449109019571.
Sarkar MA. Drug metabolism in the nasal mucosa. Pharm Res. 1992;9(1):1–9. https://doi.org/10.1023/A:1018911206646.
Oliveira P, Fortuna A, Alves G, Falcao A. Drug-metabolizing enzymes and efflux transporters in nasal epithelium: influence on the bioavailability of intranasally administered drugs. Curr Drug Metab. 2016;17(7):628–47. https://doi.org/10.2174/1389200217666160406120509.
Bleier BS, Nocera AL, Iqbal H, Hoang JD, Feldman RE, Han X. P-glycoprotein functions as an immunomodulator in healthy human primary nasal epithelial cells. Int Forum Allergy Rhinol. 2013;3(6):433–8. https://doi.org/10.1002/ALR.21166.
Graff CL, Pollack GM. Functional evidence for P-glycoprotein at the nose-brain barrier. Pharm Res. 2005;22(1):86–93. https://doi.org/10.1007/S11095-004-9013-3.
Henriksson G, Norlander T, Zheng X, Stierna P, Westrin KM. Expression of P-glycoprotein 170 in nasal mucosa may be increased with topical steroids. Am J Rhinol. 1997;11(4):317–21. https://doi.org/10.2500/105065897781446603.
Haumann R, Videira JC, Kaspers GJL, van Vuurden DG, Hulleman E. Overview of current drug delivery methods across the blood–brain barrier for the treatment of primary brain tumors. CNS Drugs. 2020;34(11):1121–31. https://doi.org/10.1007/S40263-020-00766-W/.
Musumeci T, Bonaccorso A, Puglisi G. Epilepsy disease and nose-to-brain delivery of polymeric nanoparticles: an overview. Pharmaceutics. 2019. https://doi.org/10.3390/PHARMACEUTICS11030118.
Emami A, et al. Toxicology evaluation of drugs administered via uncommon routes: intranasal, intraocular, intrathecal/intraspinal, and intra-articular. Int J Toxicol. 2018;37(1):4–27. https://doi.org/10.1177/1091581817741840.
England RJA, Homer JJ, Knight LC, Ell SR. Nasal pH measurement: a reliable and repeatable parameter. Clin Otolaryngol Allied Sci. 1999;24(1):67–8. https://doi.org/10.1046/J.1365-2273.1999.00223.X.
Łaszcz M, Witkowska A. Studies of phase transitions in the aripiprazole solid dosage form. J Pharm Biomed Anal. 2016;117:298–303. https://doi.org/10.1016/J.JPBA.2015.09.004.
Zeng F, Wang L, Zhang W, Shi K, Zong L. Formulation and in vivo evaluation of orally disintegrating tablets of clozapine/hydroxypropyl-β-cyclodextrin inclusion complexes. AAPS PharmSciTech. 2013;14(2):854–60. https://doi.org/10.1208/S12249-013-9973-X.
Jawahar N, et al. Enhanced oral bioavailability of an antipsychotic drug through nanostructured lipid carriers. Int J Biol Macromol. 2018;110:269–75. https://doi.org/10.1016/J.IJBIOMAC.2018.01.121.
Saibi Y, Sato H, Tachiki H. Developing in vitro-in vivo correlation of risperidone immediate release tablet. AAPS PharmSciTech. 2012;13(3):890–5. https://doi.org/10.1208/S12249-012-9814-3.
DeVane CL, Nemeroff CB. Clinical pharmacokinetics of quetiapine: an atypical antipsychotic. Clin Pharmacokinet. 2001;40(7):509–22. https://doi.org/10.2165/00003088-200140070-00003.
Kojima T, et al. Claudin-binder C-CPE mutants enhance permeability of insulin across human nasal epithelial cells. Drug Deliv. 2016;23(8):2703–10. https://doi.org/10.3109/10717544.2015.1050530.
Brunner J, Ragupathy S, Borchard G. Target specific tight junction modulators. Adv Drug Deliv Rev. 2021;171:266–88. https://doi.org/10.1016/J.ADDR.2021.02.008.
Uchida H, Kondoh M, Hanada T, Takahashi A, Hamakubo T, Yagi K. A claudin-4 modulator enhances the mucosal absorption of a biologically active peptide. Biochem Pharmacol. 2010;79(10):1437–44. https://doi.org/10.1016/J.BCP.2010.01.010.
Suzuki H, et al. A toxicological evaluation of a claudin modulator, the C-terminal fragment of Clostridium perfringens enterotoxin, in mice. Pharmazie. 2011;66(7):543–6. https://doi.org/10.1691/PH.2011.0365.
Song KH, Fasano A, Eddington ND. Enhanced nasal absorption of hydrophilic markers after dosing with AT1002, a tight junction modulator. Eur J Pharm Biopharm. 2008;69(1):231–7. https://doi.org/10.1016/J.EJPB.2007.10.011.
Song KH, et al. Paracellular permeation-enhancing effect of AT1002 C-terminal amidation in nasal delivery. Drug Des Dev Ther. 2015;9:1815–23. https://doi.org/10.2147/DDDT.S79383.
Ukai K, Sakakura Y, Saida S. Interaction between mucociliary transport and the ciliary beat of chicken nasal mucosa. Arch Otorhinolaryngol. 1985;242(3):225–31. https://doi.org/10.1007/BF00453544.
Van Donk HJMD, Merkus FWHM. Decreases in ciliary beat frequency due to intranasal administration of propranolol. J Pharm Sci. 1982;71(5):595–6. https://doi.org/10.1002/JPS.2600710530.
Feldman KS, Kim E, Czachowski MJ, Wu Y, Lo CW, Zahid M. Differential effect of anesthetics on mucociliary clearance in vivo in mice. Sci Rep. 2021;11(1):1–9. https://doi.org/10.1038/s41598-021-84605-y.
Doty RL, et al. Effect of esketamine nasal spray on olfactory function and nasal tolerability in patients with treatment-resistant depression: results from four multicenter, randomized, double-blind, placebo-controlled, phase III studies. CNS Drugs. 2021;35(7):781. https://doi.org/10.1007/S40263-021-00826-9.
Stockhorst U, Pietrowsky R. Olfactory perception, communication, and the nose-to-brain pathway. Physiol Behav. 2004;83(1):3–11. https://doi.org/10.1016/J.PHYSBEH.2004.07.018.
Kuehn BM. Zicam update. JAMA. 2010;303(16):1587–1587. https://doi.org/10.1001/JAMA.2010.457.
Boesveldt S, et al. Anosmia—a clinical review. Chem Sens. 2017;42(7):513–23. https://doi.org/10.1093/CHEMSE/BJX025.
Croy I, Nordin S, Hummel T. Olfactory disorders and quality of life–an updated review. Chem Sens. 2014;39(3):185–94. https://doi.org/10.1093/CHEMSE/BJT072.
Adler K, Wooten O, Philippoff W, Lerner E, Dulfano MJ. Physical properties of sputum. Am Rev Respir Dis. 1972;106(1):86–96. https://doi.org/10.1164/ARRD.1972.106.1.86.
Sorokowski P, et al. Sex differences in human olfaction: a meta-analysis. Front Psychol. 2019;10:242. https://doi.org/10.3389/FPSYG.2019.00242/.
Lomauro A, Aliverti A. Sex differences in respiratory function. Breathe. 2018;14(2):131. https://doi.org/10.1183/20734735.000318.
Fanta S, Kinnunen M, Backman JT, Kalso E. Population pharmacokinetics of S-ketamine and norketamine in healthy volunteers after intravenous and oral dosing. Eur J Clin Pharmacol. 2015;71(4):441–7. https://doi.org/10.1007/S00228-015-1826-Y.
Bourganis V, Kammona O, Alexopoulos A, Kiparissides C. Recent advances in carrier mediated nose-to-brain delivery of pharmaceutics. Eur J Pharm Biopharm. 2018;128:337–62. https://doi.org/10.1016/J.EJPB.2018.05.009.
Craft S, et al. Intranasal insulin therapy for Alzheimer disease and amnestic mild cognitive impairment: a pilot clinical trial. Arch Neurol. 2012;69(1):29–38. https://doi.org/10.1001/ARCHNEUROL.2011.233.
Craft S, et al. Safety, efficacy, and feasibility of intranasal insulin for the treatment of mild cognitive impairment and Alzheimer disease dementia: a randomized clinical trial. JAMA Neurol. 2020;77(9):1099–109. https://doi.org/10.1001/JAMANEUROL.2020.1840.
Rollema C, Van Roon EN, De Vries TW. Inadequate quality of administration of intranasal corticosteroid sprays. J Asthma Allergy. 2019;12:91–4. https://doi.org/10.2147/JAA.S189523.
Hutchison AA, Leclerc F, Nève V, Jane Pillow J, Robinson PD. The respiratory system. In: Pediatric and neonatal mechanical ventilation: from basics to clinical practice. 2015. p. 55–112. https://doi.org/10.1007/978-3-642-01219-8_4.
White DE, Bartley J, Nates RJ. Model demonstrates functional purpose of the nasal cycle. Biomed Eng Online. 2015. https://doi.org/10.1186/S12938-015-0034-4.
Crisler R, Johnston NA, Sivula C, Budelsky CL. Functional anatomy and physiology. Lab Rat. 2020. https://doi.org/10.1016/B978-0-12-814338-4.00004-0.
Ullah I, Chung K, Beloor J, Lee SK, Kumar P. A positioning device for the placement of mice during intranasal siRNA delivery to the central nervous system. JoVE (J Vis Exp). 2019;2019(150): e59201. https://doi.org/10.3791/59201.
Hanson LR, Fine JM, Svitak AL, Faltesek KA. Intranasal administration of CNS therapeutics to awake mice. J Vis Exp. 2013. https://doi.org/10.3791/4440.
Piazza JE, et al. A novel intranasal spray device for the administration of nanoparticles to rodents. J Med Devices Trans ASME. 2015. https://doi.org/10.1115/1.4029907/376773.
Ehrick JD, et al. Considerations for the development of nasal dosage forms. Sterile Prod Dev. 2013;6:99. https://doi.org/10.1007/978-1-4614-7978-9_5.
Costantino HR, Illum L, Brandt G, Johnson PH, Quay SC. Intranasal delivery: physicochemical and therapeutic aspects. Int J Pharm. 2007;337(1–2):1–24. https://doi.org/10.1016/J.IJPHARM.2007.03.025.
Benowitz NL, Hukkanen J, Jacob P. Nicotine chemistry, metabolism, kinetics and biomarkers. Handb Exp Pharmacol. 2009;192(192):29. https://doi.org/10.1007/978-3-540-69248-5_2.
Drucker DJ. Advances in oral peptide therapeutics. Nat Rev Drug Discov. 2019;19(4):277–89. https://doi.org/10.1038/s41573-019-0053-0.
Humphries LK, Eiland LS. Treatment of acute seizures: is intranasal midazolam a viable option? J Pediatr Pharmacol Ther JPPT. 2013;18(2):79. https://doi.org/10.5863/1551-6776-18.2.79.
Rabinowicz AL, Carrazana E, Maggio ET. Improvement of intranasal drug delivery with Intravail® alkylsaccharide excipient as a mucosal absorption enhancer aiding in the treatment of conditions of the central nervous system. Drugs R D. 2021;21(4):361. https://doi.org/10.1007/S40268-021-00360-5.
Davis SS, Illum L. Absorption enhancers for nasal drug delivery. Clin Pharmacokinet. 2012;42(13):1107–28. https://doi.org/10.2165/00003088-200342130-00003.
Ekelund K, Östh K, Påhlstorp C, Björk E, Ulvenlund S, Johansson F. Correlation between epithelial toxicity and surfactant structure as derived from the effects of polyethyleneoxide surfactants on caco-2 cell monolayers and pig nasal mucosa. J Pharm Sci. 2005;94(4):730–44. https://doi.org/10.1002/JPS.20283.
Turner JH, Wu J, Dorminy CA, Chandra RK. Safety and tolerability of surfactant nasal irrigation. Int Forum Allergy Rhinol. 2017;7(8):809–12. https://doi.org/10.1002/ALR.21959.
Ghadiri M, Young PM, Traini D. Strategies to enhance drug absorption via nasal and pulmonary routes. Pharmaceutics. 2019. https://doi.org/10.3390/PHARMACEUTICS11030113.
Rassu G, Ferraro L, Pavan B, Giunchedi P, Gavini E, Dalpiaz A. The role of combined penetration enhancers in nasal microspheres on in vivo drug bioavailability. Pharmaceutics. 2018. https://doi.org/10.3390/PHARMACEUTICS10040206.
Ways TMM, Ng KW, Lau WM, Khutoryanskiy VV. Silica nanoparticles in transmucosal drug delivery. Pharm. 2020;12(8):751. https://doi.org/10.3390/PHARMACEUTICS12080751.
Lyseng-Williamson KA. Fentanyl pectin nasal spray: In breakthrough pain in opioid-tolerant adults with cancer. CNS Drugs. 2011;25(6):511–22. https://doi.org/10.2165/11207470-000000000-00000/.
Casettari L, Illum L. Chitosan in nasal delivery systems for therapeutic drugs. J Control Release. 2014;190:189–200. https://doi.org/10.1016/J.JCONREL.2014.05.003.
Gulati N, Nagaich U, Saraf SA. Intranasal delivery of chitosan nanoparticles for migraine therapy. Sci Pharm. 2013;81(3):843–54. https://doi.org/10.3797/SCIPHARM.1208-18.
Bernkop-Schnürch A, Schwarz V, Steininger S. Polymers with thiol groups: a new generation of mucoadhesive polymers? Pharm Res. 1999;16(6):876–81. https://doi.org/10.1023/A:1018830204170.
Bernkop-Schnürch A. Thiomers: a new generation of mucoadhesive polymers. Adv Drug Deliv Rev. 2005;57(11):1569–82. https://doi.org/10.1016/J.ADDR.2005.07.002.
Rohrer J, Lupo N, Bernkop-Schnürch A. Advanced formulations for intranasal delivery of biologics. Int J Pharm. 2018;553(1–2):8–20. https://doi.org/10.1016/J.IJPHARM.2018.10.029.
Zahir-Jouzdani F, Wolf JD, Atyabi F, Bernkop-Schnürch A. In situ gelling and mucoadhesive polymers: why do they need each other? Expert Opin Drug Deliv. 2018;15(10):1007–19. https://doi.org/10.1080/17425247.2018.1517741.
Menzel C, Jelkmann M, Laffleur F, Bernkop-Schnürch A. Nasal drug delivery: design of a novel mucoadhesive and in situ gelling polymer. Int J Pharm. 2017;517(1–2):196–202. https://doi.org/10.1016/J.IJPHARM.2016.11.055.
Sharpe SA, et al. Comparison of the flow properties of aqueous suspension corticosteroid nasal sprays under differing sampling conditions. Drug Dev Ind Pharm. 2003;29(9):1005–12. https://doi.org/10.1081/DDC-120025457.
Olivier JC. Drug transport to brain with targeted nanoparticles. NeuroRx. 2005;2(1):108. https://doi.org/10.1602/NEURORX.2.1.108.
Masserini M. Nanoparticles for brain drug delivery. ISRN Biochem. 2013;2013:1–18. https://doi.org/10.1155/2013/238428.
Illum L. Nanoparticulate systems for nasal delivery of drugs: a real improvement over simple systems? J Pharm Sci. 2007;96(3):473–83. https://doi.org/10.1002/JPS.20718.
Sonvico F, et al. Surface-modified nanocarriers for nose-to-brain delivery: from bioadhesion to targeting. Pharmaceutics. 2018;10(1):34. https://doi.org/10.3390/PHARMACEUTICS10010034.
Poonia N, Kharb R, Lather V, Pandita D. Nanostructured lipid carriers: versatile oral delivery vehicle. Future Sci OA. 2016. https://doi.org/10.4155/FSOA-2016-0030/ASSET/IMAGES/LARGE/FIGURE9.JPEG.
Smeets NMB, Hoare T. Designing responsive microgels for drug delivery applications. J Polym Sci Part A Polym Chem. 2013;51(14):3027–43. https://doi.org/10.1002/POLA.26707.
Li X, Montague EC, Pollinzi A, Lofts A, Hoare T. Design of smart size-, surface-, and shape-switching nanoparticles to improve therapeutic efficacy. Small. 2022;18(6):2104632. https://doi.org/10.1002/SMLL.202104632.
Brooking J, Davis SS, Illum L. Transport of nanoparticles across the rat nasal mucosa. J Drug Target. 2001;9(4):267–79. https://doi.org/10.3109/10611860108997935.
Hong SS, Oh KT, Choi HG, Lim SJ. Liposomal formulations for nose-to-brain delivery: recent advances and future perspectives. Pharmaceutics. 2019. https://doi.org/10.3390/PHARMACEUTICS11100540.
Clementino AR, et al. Structure and fate of nanoparticles designed for the nasal delivery of poorly soluble drugs. Mol Pharm. 2021;18(8):3132–46. https://doi.org/10.1021/ACS.MOLPHARMACEUT.1C00366/SUPPL_FILE/MP1C00366_SI_001.PDF.
Popescu R, Ghica MV, Dinu-Pîrvu CE, Anuța V, Lupuliasa D, Popa L. New opportunity to formulate intranasal vaccines and drug delivery systems based on chitosan. Int J Mol Sci. 2020;21(14):1–23. https://doi.org/10.3390/IJMS21145016.
Clementino A, et al. The nasal delivery of nanoencapsulated statins—an approach for brain delivery. Int J Nanomed. 2016;11:6575–90. https://doi.org/10.2147/IJN.S119033.
Mistry A, et al. Effect of physicochemical properties on intranasal nanoparticle transit into murine olfactory epithelium. J Drug Target. 2009;17(7):543–52. https://doi.org/10.1080/10611860903055470.
Teleanu DM, Chircov C, Grumezescu AM, Volceanov A, Teleanu RI. Impact of nanoparticles on brain health: an up to date overview. J Clin Med. 2018. https://doi.org/10.3390/JCM7120490.
Ul Islam S, Shehzad A, Bilal Ahmed M, Lee YS. Intranasal delivery of nanoformulations: a potential way of treatment for neurological disorders. Molecules. 2020. https://doi.org/10.3390/MOLECULES25081929.
Wong JC, et al. Nanoparticle encapsulated oxytocin increases resistance to induced seizures and restores social behavior in Scn1a-derived epilepsy. Neurobiol Dis. 2021;147: 105147. https://doi.org/10.1016/J.NBD.2020.105147.
Malerba F, Paoletti F, Capsoni S, Cattaneo A. Intranasal delivery of therapeutic proteins for neurological diseases. Expert Opin Drug Deliv. 2011;8(10):1277–96. https://doi.org/10.1517/17425247.2011.588204.
Meredith ME, Salameh TS, Banks WA. Intranasal delivery of proteins and peptides in the treatment of neurodegenerative diseases. AAPS J. 2015;17(4):780–7. https://doi.org/10.1208/S12248-015-9719-7/.
Salatin S, Barar J, Barzegar-Jalali M, Adibkia K, Milani MA, Jelvehgari M. Hydrogel nanoparticles and nanocomposites for nasal drug/vaccine delivery. Arch Pharm Res. 2016;39(9):1181–92. https://doi.org/10.1007/S12272-016-0782-0/.
Zaman M, Chandrudu S, Toth I. Strategies for intranasal delivery of vaccines. Drug Deliv Transl Res. 2013;3(1):100–9. https://doi.org/10.1007/S13346-012-0085-Z/.
Bahadur S, Sachan N, Harwansh RK, Deshmukh R. Nanoparticlized system: promising approach for the management of Alzheimer’s disease through intranasal delivery. Curr Pharm Des. 2020;26(12):1331–44. https://doi.org/10.2174/1381612826666200311131658.
Pandey M, et al. Nanoparticles based intranasal delivery of drug to treat Alzheimer’s disease: a recent update. CNS Neurol Disord Drug Targets. 2020;19(9):648–62. https://doi.org/10.2174/1871527319999200819095620.
Costa C, Moreira JN, Amaral MH, Sousa Lobo JM, Silva AC. Nose-to-brain delivery of lipid-based nanosystems for epileptic seizures and anxiety crisis. J Control Release. 2019;295:187–200. https://doi.org/10.1016/J.JCONREL.2018.12.049.
Gomez D, Martinez JA, Hanson LR, Frey WH, Toth CC. Intranasal treatment of neurodegenerative diseases and stroke. Front Biosci (Schol Ed). 2012;4(1):74–89. https://doi.org/10.2741/252.
Hanson LR, Frey WH. Intranasal delivery bypasses the blood–brain barrier to target therapeutic agents to the central nervous system and treat neurodegenerative disease. BMC Neurosci. 2008;9(Suppl 3):S5. https://doi.org/10.1186/1471-2202-9-S3-S5.
Sharma D, et al. Nose-to-brain delivery of PLGA-diazepam nanoparticles. AAPS PharmSciTech. 2015;16(5):1108–21. https://doi.org/10.1208/S12249-015-0294-0/FIGURES/9.
Piazza J, et al. Haloperidol-loaded intranasally administered lectin functionalized poly(ethylene glycol)–block-poly(d, l)-lactic-co-glycolic acid (PEG–PLGA) nanoparticles for the treatment of schizophrenia. Eur J Pharm Biopharm. 2014;87(1):30–9. https://doi.org/10.1016/J.EJPB.2014.02.007.
Campea MA, Majcher MJ, Lofts A, Hoare T. A review of design and fabrication methods for nanoparticle network hydrogels for biomedical, environmental, and industrial applications. Adv Funct Mater. 2021;31(33):2102355. https://doi.org/10.1002/ADFM.202102355.
Wang JTW, et al. Enhanced delivery of neuroactive drugs via nasal delivery with a self-healing supramolecular gel. Adv Sci. 2021;8(14):2101058. https://doi.org/10.1002/ADVS.202101058.
Majcher MJ, et al. In situ-gelling starch nanoparticle (SNP)/O-carboxymethyl chitosan (CMCh) nanoparticle network hydrogels for the intranasal delivery of an antipsychotic peptide. J Control Release. 2020;330:738–52. https://doi.org/10.1016/j.jconrel.2020.12.050.
Quintana DS, Smerud KT, Andreassen OA, Djupesland PG. Evidence for intranasal oxytocin delivery to the brain: recent advances and future perspectives. Ther Deliv. 2018;9(7):515–25. https://doi.org/10.4155/TDE-2018-0002/.
Dave R, Randhawa G, Kim D, Simpson M, Hoare T. Microgels and nanogels for the delivery of poorly water-soluble drugs. Mol Pharm. 2022. https://doi.org/10.1021/ACS.MOLPHARMACEUT.1C00967.
Picone P, et al. Ionizing radiation-engineered nanogels as insulin nanocarriers for the development of a new strategy for the treatment of Alzheimer’s disease. Biomaterials. 2016;80:179–94. https://doi.org/10.1016/J.BIOMATERIALS.2015.11.057.
Picone P, et al. Nose-to-brain delivery of insulin enhanced by a nanogel carrier. J Control Release. 2018;270:23–36. https://doi.org/10.1016/J.JCONREL.2017.11.040.
Masjedi M, Azadi A, Heidari R, Mohammadi-Samani S. Brain targeted delivery of sumatriptan succinate loaded chitosan nanoparticles: preparation, in vitro characterization, and (neuro-)pharmacokinetic evaluations. J Drug Deliv Sci Technol. 2021;61: 102179. https://doi.org/10.1016/J.JDDST.2020.102179.
Youssef NAHA, Kassem AA, Farid RM, Ismail FA, El-Massik MAE, Boraie NA. A novel nasal almotriptan loaded solid lipid nanoparticles in mucoadhesive in situ gel formulation for brain targeting: preparation, characterization and in vivo evaluation. Int J Pharm. 2018;548(1):609–24. https://doi.org/10.1016/J.IJPHARM.2018.07.014.
Hasan N, et al. Intranasal delivery of naloxone-loaded solid lipid nanoparticles as a promising simple and non-invasive approach for the management of opioid overdose. Int J Pharm. 2021;599: 120428. https://doi.org/10.1016/J.IJPHARM.2021.120428.
Bonferoni MC, et al. Nanoemulsions for ‘nose-to-brain’ drug delivery. Pharmaceutics. 2019. https://doi.org/10.3390/PHARMACEUTICS11020084.
Handa M, et al. Therapeutic potential of nanoemulsions as feasible wagons for targeting Alzheimer’s disease. Drug Discov Today. 2021;26(12):2881–8. https://doi.org/10.1016/J.DRUDIS.2021.07.020.
Bahadur S, Pardhi DM, Rautio J, Rosenholm JM, Pathak K. Intranasal nanoemulsions for direct nose-to-brain delivery of actives for CNS disorders. Pharm. 2020;12(12):1230. https://doi.org/10.3390/PHARMACEUTICS12121230.
Abdou EM, Kandil SM, Miniawy HMFE. Brain targeting efficiency of antimigrain drug loaded mucoadhesive intranasal nanoemulsion. Int J Pharm. 2017;529(1–2):667–77. https://doi.org/10.1016/J.IJPHARM.2017.07.030.
Jain R, Nabar S, Dandekar P, Vandana P. Micellar nanocarriers: potential nose-to-brain delivery of zolmitriptan as novel migraine therapy. Pharm Res. 2010;27(4):655–64. https://doi.org/10.1007/S11095-009-0041-X/.
Hoekman JD, Srivastava P, Ho RJY. Aerosol stable peptide-coated liposome nanoparticles: a proof-of-concept study with opioid fentanyl in enhancing analgesic effects and reducing plasma drug exposure. J Pharm Sci. 2014;103(8):2231. https://doi.org/10.1002/JPS.24022.
Abd-Elal RMA, Shamma RN, Rashed HM, Bendas ER. Trans-nasal zolmitriptan novasomes: in-vitro preparation, optimization and in-vivo evaluation of brain targeting efficiency. Drug Delivery. 2016;23(9):3374–86. https://doi.org/10.1080/10717544.2016.1183721.
Assistant Professor BK. Lipid nano particulate drug delivery: an overview of the emerging trend. Pharma Innov J. 2018;7(7):779–89. [Online]. www.thepharmajournal.com. Accessed 24 Jan 2022.
Maggio ET. IntravailTM: highly effective intranasal delivery of peptide and protein drugs. Expert Opin Drug Deliv. 2006;3(4):529–39. https://doi.org/10.1517/17425247.3.4.529.
Ganesan P, Narayanasamy D. Lipid nanoparticles: different preparation techniques, characterization, hurdles, and strategies for the production of solid lipid nanoparticles and nanostructured lipid carriers for oral drug delivery. Sustain Chem Pharm. 2017;6:37–56. https://doi.org/10.1016/J.SCP.2017.07.002.
Costa CP, Moreira JN, Sousa Lobo JM, Silva AC. Intranasal delivery of nanostructured lipid carriers, solid lipid nanoparticles and nanoemulsions: a current overview of in vivo studies. Acta Pharm Sin B. 2021;11(4):925–40. https://doi.org/10.1016/J.APSB.2021.02.012.
Nair SC, Vinayan KP, Mangalathillam S. Nose to brain delivery of phenytoin sodium loaded nano lipid carriers: formulation, drug release, permeation and in vivo pharmacokinetic studies. Pharm. 2021;13(10):1640. https://doi.org/10.3390/PHARMACEUTICS13101640.
Shimoda A, et al. Dual crosslinked hydrogel nanoparticles by nanogel bottom-up method for sustained-release delivery. Colloids Surfaces B Biointerfaces. 2012;99:38–44. https://doi.org/10.1016/J.COLSURFB.2011.09.025.
Hasegawa U, et al. Raspberry-like assembly of cross-linked nanogels for protein delivery. J Control Release. 2009;140(3):312–7. https://doi.org/10.1016/J.JCONREL.2009.06.025.
Yuki Y, et al. Characterization and specification of a trivalent protein-based pneumococcal vaccine formulation using an adjuvant-free nanogel nasal delivery system. Mol Pharm. 2021;18(4):1582–92. https://doi.org/10.1021/ACS.MOLPHARMACEUT.0C01003/.
Nakahashi-Ouchida R, et al. A nanogel-based trivalent PspA nasal vaccine protects macaques from intratracheal challenge with pneumococci. Vaccine. 2021;39(25):3353–64. https://doi.org/10.1016/J.VACCINE.2021.04.069.
Sawada SI, et al. Nanogel hybrid assembly for exosome intracellular delivery: effects on endocytosis and fusion by exosome surface polymer engineering. Biomater Sci. 2020;8(2):619–30. https://doi.org/10.1039/C9BM01232J.
Mendell JR, et al. Single-Dose gene-replacement therapy for spinal muscular atrophy. N Engl J Med. 2017;377(18):1713–22. https://doi.org/10.1056/NEJMOA1706198/.
Castle MJ, Baltanás FC, Kovacs I, Nagahara AH, Barba D, Tuszynski MH. Postmortem analysis in a clinical trial of AAV2-NGF gene therapy for Alzheimer’s disease identifies a need for improved vector delivery. Hum Gene Ther. 2020;31(7–8):415. https://doi.org/10.1089/HUM.2019.367.
Rafii MS, et al. A phase 1 study of stereotactic gene delivery of AAV2-NGF for Alzheimer’s disease. Alzheimers Dement. 2014;10(5):571–81. https://doi.org/10.1016/J.JALZ.2013.09.004.
Belur LR, et al. Intranasal adeno-associated virus mediated gene delivery and expression of human iduronidase in the central nervous system: a noninvasive and effective approach for prevention of neurologic disease in mucopolysaccharidosis type I. Hum Gene Ther. 2017;28(7):576. https://doi.org/10.1089/HUM.2017.187.
Oviedo N, Manuel-Apolinar L, Orozco-Suárez S, Juárez-Cedillo T, Bekker Méndez VC, Tesoro-Cruz E. Intranasal administration of a naked plasmid reached brain cells and expressed green fluorescent protein, a candidate for future gene therapy studies. Arch Med Res. 2017;48(7):616–22. https://doi.org/10.1016/J.ARCMED.2018.03.003.
Mingozzi F, High KA. Immune responses to AAV vectors: overcoming barriers to successful gene therapy. Blood. 2013;122(1):23–36. https://doi.org/10.1182/BLOOD-2013-01-306647.
Hou X, Zaks T, Langer R, Dong Y. Lipid nanoparticles for mRNA delivery. Nat Rev Mater. 2021;6(12):1078–94. https://doi.org/10.1038/s41578-021-00358-0.
Pena SA, et al. Gene therapy for neurological disorders: challenges and recent advancements. J Drug Target. 2020;28(2):111–28. https://doi.org/10.1080/1061186X.2019.1630415.
Aly AEE, Harmon BT, Padegimas L, Sesenoglu-Laird O, Cooper MJ, Waszczak BL. Intranasal delivery of pGDNF DNA nanoparticles provides neuroprotection in the rat 6-hydroxydopamine model of Parkinson’s disease. Mol Neurobiol. 2019;56(1):688–701. https://doi.org/10.1007/S12035-018-1109-6/FIGURES/7.
Tanaka H, et al. In vivo introduction of mRNA encapsulated in lipid nanoparticles to brain neuronal cells and astrocytes via intracerebroventricular administration. Mol Pharm. 2018;15(5):2060–7. https://doi.org/10.1021/acs.molpharmaceut.7b01084.
Mohamad SA, Badawi AM, Mansour HF. Insulin fast-dissolving film for intranasal delivery via olfactory region, a promising approach for the treatment of anosmia in COVID-19 patients: design, in-vitro characterization and clinical evaluation. Int J Pharm. 2021;601: 120600. https://doi.org/10.1016/J.IJPHARM.2021.120600.
Lombardo R, Musumeci T, Carbone C, Pignatello R. Nanotechnologies for intranasal drug delivery: an update of literature. Pharm Dev Technol. 2021;26(8):824–45. https://doi.org/10.1080/10837450.2021.1950186.
Lechner M, et al. Anosmia as a presenting symptom of SARS-CoV-2 infection in healthcare workers—a systematic review of the literature, case series, and recommendations for clinical assessment and management. Rhinology. 2020;58(4):1–9. https://doi.org/10.4193/RHIN20.189.
Longmore J, et al. Differential distribution of 5HT(1D)- and 5HT(1B)-immunoreactivity within the human trigemino-cerebrovascular system: implications for the discovery of new antimigraine drugs. Cephalalgia. 1997;17(8):833–42. https://doi.org/10.1046/j.1468-2982.1997.1708833.x.
Dahlöf C, Maassen Van Den Brink A. Dihydroergotamine, ergotamine, methysergide and sumatriptan— basic science in relation to migraine treatment. Headache. 2012;52(4):707–14. https://doi.org/10.1111/J.1526-4610.2012.02124.X.
Sullivan HJ, Tursi A, Moore K, Campbell A, Floyd C, Wu C. Binding Interactions of ergotamine and dihydroergotamine to 5-hydroxytryptamine receptor 1B (5-HT 1b) using molecular dynamics simulations and dynamic network analysis. J Chem Inf Model. 2020;60(3):1749–65. https://doi.org/10.1021/ACS.JCIM.9B01082.
Lee A, Kuo B. Metoclopramide in the treatment of diabetic gastroparesis. Expert Rev Endocrinol Metab. 2010;5(5):653. https://doi.org/10.1586/eem.10.41.
Macario A, Lipman AG. Ketorolac in the era of cyclo-oxygenase-2 selective nonsteroidal anti-inflammatory drugs: a systematic review of efficacy, side effects, and regulatory issues. Pain Med. 2001;2(4):336–51. https://doi.org/10.1046/J.1526-4637.2001.01043.X.
Buckley MMT, Brogden RN. Ketorolac. Drugs. 2012;39(1):86–109. https://doi.org/10.2165/00003495-199039010-00008.
Lutz PE, Almeida D, Filliol D, Jollant F, Kieffer BL, Turecki G. Increased functional coupling of the mu opioid receptor in the anterior insula of depressed individuals. Neuropsychopharmacology. 2021;46(5):920–7. https://doi.org/10.1038/s41386-021-00974-y.
Nicholson MW, et al. Diazepam-induced loss of inhibitory synapses mediated by PLCδ/Ca2+/calcineurin signalling downstream of GABAA receptors. Mol Psychiatry. 2018;23(9):1851–67. https://doi.org/10.1038/s41380-018-0100-y.
Edwards Z, Preuss CV. GABA receptor positive allosteric modulators. StatPearls. 2021. [Online]. https://www.ncbi.nlm.nih.gov/books/NBK554443/. Accessed24 Jan 2022.
Lingamchetty TN, Hosseini SA, Saadabadi A. Midazolam. xPharm Compr Pharmacol Ref. 2021. https://doi.org/10.1016/B978-008055232-3.62185-3.
Spina SP, Ensom MHH. Clinical pharmacokinetic monitoring of midazolam in critically ill patients. Pharmacotherapy. 2007;27(3):389–98. https://doi.org/10.1592/PHCO.27.3.389.
Blondal T, Gudmundsson LJ, Olafsdottir I, Gustavsson G, Westin A, Stapleton J. Nicotine nasal spray with nicotine patch for smoking cessation: randomised trial with six year follow up. BMJ Br Med J. 1999;318(7179):285. https://doi.org/10.1136/BMJ.318.7179.285.
Perkins KA, Grobe JE, D’Amico D, Fonte C, Wilson AS, Stiller RL. Low-dose nicotine nasal spray use and effects during initial smoking cessation. Exp Clin Psychopharmacol. 1996;4(2):157–65. https://doi.org/10.1037/1064-1297.4.2.157.
Schneider NG, Lunell E, Olmstead RE, Fagerström KO. Clinical pharmacokinetics of nasal nicotine delivery. A review and comparison to other nicotine systems. Clin Pharmacokinet. 1996;31(1):65–80. https://doi.org/10.2165/00003088-199631010-00005.
Lee JH, Jahrling JB, Denner L, Dineley KT. Targeting Insulin for Alzheimer’s disease: mechanisms, status and potential directions. J Alzheimers Dis. 2018;64(s1):S427–53. https://doi.org/10.3233/JAD-179923.
Novak P, Maldonado DAP, Novak V. Safety and preliminary efficacy of intranasal insulin for cognitive impairment in Parkinson disease and multiple system atrophy: a double-blinded placebo-controlled pilot study. PLoS ONE. 2019. https://doi.org/10.1371/JOURNAL.PONE.0214364.
Bernaerts S, Boets B, Steyaert J, Wenderoth N, Alaerts K. Oxytocin treatment attenuates amygdala activity in autism: a treatment-mechanism study with long-term follow-up. Transl Psychiatry. 2020;10(1):1–12. https://doi.org/10.1038/s41398-020-01069-w.
Hollander E, et al. Intranasal oxytocin versus placebo for hyperphagia and repetitive behaviors in children with Prader–Willi syndrome: a randomized controlled pilot trial. J Psychiatr Res. 2021;137:643–51. https://doi.org/10.1016/J.JPSYCHIRES.2020.11.006.
Stauffer CS, Musinipally V, Suen A, Lynch KL, Shapiro B, Woolley JD. A two-week pilot study of intranasal oxytocin for cocaine-dependent individuals receiving methadone maintenance treatment for opioid use disorder. Addict Res Theory. 2016;24(6):490. https://doi.org/10.3109/16066359.2016.1173682.
Mischley LK, Lau RC, Shankland EG, Wilbur TK, Padowski JM. Phase IIb study of intranasal glutathione in Parkinson’s disease. J Parkinsons Dis. 2017;7(2):289. https://doi.org/10.3233/JPD-161040.
Perez-Ruixo C, et al. Population pharmacokinetics of esketamine nasal spray and its metabolite noresketamine in healthy subjects and patients with treatment-resistant depression. Clin Pharmacokinet. 2021;60(4):501–16. https://doi.org/10.1007/S40262-020-00953-4.
Bahr R, Lopez A, Rey JA. Intranasal esketamine (SpravatoTM) for use in treatment-resistant depression in conjunction with an oral antidepressant. Pharm Ther. 2019;44(6):340. Accessed 24 Jan 2022. [Online]. /pmc/articles/PMC6534172/.
Fuseau E, Petricoul O, Moore KH, Barrow A, Ibbotson T. Clinical pharmacokinetics of intranasal sumatriptan. Clin Pharmacokinet. 2002;41(11):801–11. https://doi.org/10.2165/00003088-200241110-00002.
Quadir M, Zia H, Needham TE. Development and evaluation of nasal formulations of ketorolac. Drug Deliv. 2000;7(4):223–9. https://doi.org/10.1080/107175400455155.
Tylleskar I, Skulberg AK, Nilsen T, Skarra S. Naloxone nasal spray—bioavailability and absorption pattern in a phase 1 study. Tidsskr Nor Laegeforen. 2019. https://doi.org/10.4045/TIDSSKR.19.0162.
Hogan RE, Gidal BE, Koplowitz B, Koplowitz LP, Lowenthal RE, Carrazana E. Bioavailability and safety of diazepam intranasal solution compared to oral and rectal diazepam in healthy volunteers. Epilepsia. 2020;61(3):455. https://doi.org/10.1111/EPI.16449.
Johansson CJ, Olsson P, Bende M, Carlsson T, Gunnarsson PO. Absolute bioavailability of nicotine applied to different nasal regions. Eur J Clin Pharmacol. 1991;41(6):585–8. https://doi.org/10.1007/BF00314989.
Nau J, Wyatt DJ, Rollema H, Crean CS. A phase I, open-label, randomized, 2-way crossover study to evaluate the relative bioavailability of intranasal and oral varenicline. Clin Ther. 2021;43(9):1595–607. https://doi.org/10.1016/J.CLINTHERA.2021.07.020.
Lougheed WD, Fischer U, Perlman K, Albisser AM. A physiological solvent for crystalline insulin. Diabetologia. 1981;20(1):51–3. https://doi.org/10.1007/BF00253817.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The Natural Sciences and Engineering Research Council of Canada (CHRPJ-508393-2017), Canadian Institutes of Health Research (CPG-151963), and the Milken Institute (2021-0825) are gratefully acknowledged for funding.
Conflicts of interest/competing interests
All authors declare no conflicts of interest.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Availability of data and material
Not applicable.
Code availability
Not applicable.
Authors contributions
AL: conceptualization, writing—original draft, FA: writing—original draft. NR: writing—original draft. RM: writing—review and editing, funding acquisition. TH: conceptualization, writing—review and editing, funding acquisition. All authors have read and approved the final submitted manuscript and agree to be accountable for the work.
Rights and permissions
About this article
Cite this article
Lofts, A., Abu-Hijleh, F., Rigg, N. et al. Using the Intranasal Route to Administer Drugs to Treat Neurological and Psychiatric Illnesses: Rationale, Successes, and Future Needs. CNS Drugs 36, 739–770 (2022). https://doi.org/10.1007/s40263-022-00930-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40263-022-00930-4