Abstract
Objective
Our aim was to explore trends in price evolution and prescription volumes of anticonvulsants (AEDs, antiepileptic drugs) in Germany between 2000 and 2017.
Method
This study used data from annual reports on mean prescription frequency and prices of defined daily doses (DDD) of AEDs in Germany to analyze nationwide trends. Interrupted time series (ITS) analysis was employed to test for significant effects of several statutory healthcare reforms in Germany on AED price evolution. These data were compared to cohort-based prescription patterns of four German cohort studies from 2003, 2008, 2013, and 2016 that included a total of 1368 patients with focal and generalized epilepsies.
Results
Analysis of national prescription data between 2000 and 2017 showed that mean prices per DDD of third-generation AEDs decreased by 65% and mean prices of second-generation AEDs decreased by 36%, whereas mean prices of first-generation AEDs increased by 133%. Simultaneously, mean prescription frequency of third- generation AEDs increased by 2494%, while there was a substantial decrease in the use of first- (− 55%) and second- (− 16%) generation AEDs. ITS analysis revealed that in particular the introduction of mandatory rebates on drugs in 2003 affected prices of frequently used newer AEDs. These findings are consistent with data from cohort studies of epilepsy patients showing a general decrease of prices for frequently used AEDs in monotherapy by 62% and in combination therapies by 68%. The analysis suggests that overall expenses for AEDs remained stable despite an increase in the prescription of “newer” and “non-enzyme-inducing” AEDs for epilepsy patients.
Conclusion
Between 2000 and 2017, a distinct decline in AED prices can be observed that seems predominately caused by a governmentally obtained price decline of third- and second-generation drugs. These observations seem to be the result of a German statutory cost containment policy applied across all health-care sectors. The increasing use of third-generation AEDs to the disadvantage of “old” and “enzyme-inducing” AEDs reflects the preferences of physicians and patients with epilepsy and follows national treatment guidelines.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Prices of the most common antiepileptic drugs decreased markedly between 2000 and 2017. |
Prescription patterns show an expenditure-neutral trend towards the use of “newer” and “less interacting” AEDs. |
In particular, prices of newer and frequently prescribed AEDs probably decreased because of efforts of German statutory healthcare reforms. |
1 Introduction
Epilepsy disorders represent a substantial burden for medical, social, and economic structures, and affect more than 39 million people worldwide [1, 2]. Annual disease-related healthcare expenses in Germany are around 1.6 billion Euro for the treatment and care of up to 800 thousand people with epilepsy (www.destatis.de, GENESIS database). Epilepsy is characterized by a sustained risk of recurrent seizures [3]. As the main direct cost driving factors behind the expenses of treatment anticonvulsants (antiepileptic drugs [AEDs]) and inpatient treatment have been previously identified [4,5,6,7,8,9]. However, AEDs remain the mainstay of therapy, and expenses for AEDs increase with a refractory course of disease. Patients in seizure remission are less likely to receive AED polytherapy and have a lower risk for hospitalization or diagnostic procedures [10].
To stop growing drug expenditures in general, several statutory healthcare reforms have been introduced to the German pharmaceutical market, starting from the 1970s, with different cost-containment approaches over time [11]. The social health insurance modernization act (GKV-Modernisierungsgesetz) was introduced in 2003 (coming into effect on 1 January 2004), permitting individual rebate contracts between healthcare providers and pharmaceutical companies [12]. The “rebates approach” was further extended by the Pharmaceutical Care Efficiency Act in 2006 (Arzneimittelversorgungs-Wirtschaftlichkeitsgesetz [AVWG], coming into effect on 1 May 2006, with first implementation in 2007) and another act to increase pro-competitive effects in the healthcare system was introduced in 2007 (GKV-Wettbewerbsstärkungsgesetz, coming into effect on 1 January 2009). Both acts adopted fixed rebates for generic medications of up to 7.0% of their sales price, as well as other, additional rebate possibilities [13].
A mandatory early benefit assessment (EBA) by the Federal Joint Committee (Gemeinsamer Bundesausschuss, G-BA) was established to analyze the value-for-money of newly approved drugs. It implements reimbursement negotiations based on the pharmaceuticals’ individual additional benefit. None of the newly approved AEDs for add-on treatment of focal epilepsies on the German pharmaceutical market, such as retigabine, perampanel, or brivaracetam, received this status of added benefit, which resulted in a disagreement on market price and reimbursement, and led to temporary market withdrawals accompanied by widespread criticism and controversial discussions among scientific societies and patient advocacy groups [14, 15]. In line with these efforts regarding the German healthcare system, many other countries in Europe introduced similar statutory reforms [16, 17].
The objective of this study was to analyze the effects of German cost-containment efforts as well as general trends in price evolution and prescription patterns for AEDs in Germany between 2000 and 2017. Since national data on prescriptions do not specify the indication for each drug used, we used both national data and cohort-based data from epilepsy patients.
2 Methods
2.1 Study Cohorts, Settings, and Design
A total of 1368 adult patients with focal and generalized epilepsies from four cross-sectional studies conducted at the Epilepsy Center Hessen (University Hospital Marburg) and/or the Epilepsy Center Frankfurt Rhine-Main (University Hospital Frankfurt) in 2003, 2008, 2013, and 2016 were analyzed in this study [6, 18,19,20]. Both regions comprise large rural and metropolitan areas with both comprehensive and specialized healthcare systems, and the area around Marburg has previously been used for population-based studies on epilepsy and status epilepticus [19, 21]. The definition of epilepsy and seizures was based on the recommendations of the International League Against Epilepsy (ILAE) [3, 22, 23]. All studies were approved by the local ethics committees and STROBE and RECORD guidelines were followed [24, 25].
2.2 Assessment of Prices and Prescription Patterns
Calculations of AED prices and prescription frequencies on the national level were performed according to current recommendations for health economic analyses using standardized price units and daily defined AED doses (DDD) [26]. This methodological approach is consistent with general German recommendations for health-economic analysis [27, 28]. Data were derived for each year from 2000 to 2017 from the annually published German report on usage and prices on medication by Schwabe et al. which is based on dispensing frequency of AEDs [29]. The data from 2000 were given in Deutsche Marks (DM), which were converted to Euros (€) at the official exchange rate (1€:1.995 DM) and all other prices were given in €. Due to the frequent use of several AEDs to treat other diseases, for example, valproate and lamotrigine as mood stabilizers and pregabalin and gabapentin for chronic pain syndromes, findings on the national level were validated using real-world prescription patterns. Therefore, four cross-sectional cohorts in 2003, 2008, 2013, and 2016 of patients with active epilepsy (2003) as well as patients with active epilepsy and epilepsy in remission (2008, 2013, and 2016) were employed [4, 6, 7, 18]. Prescription patterns of commonly used AED monotherapies and therapies with two AEDs were determined from standardized questionnaires. Drug expenditures were calculated based on the prices at the national level using DDD to avoid bias from different original and generic formulations [27, 28]. After taking into account the data on different prescription patterns daily, annual expenditures were calculated for a fictive cohort of 100 patients. All prices are displayed in € and refer to DDDs of individual AEDs or to a weighted means for AED generations considering the annual prescription volume of each AED in relation to the total number of prescriptions per generation. Therefore, total annual expenditures were calculated for each AED by multiplication of its prices per DDD and the number of DDDs prescribed. Next, annual expenditures of AED generations were summed up and divided by the total number of DDDs per generation. All given prices for AEDs and different AED generations are shown constantly without adjustment for inflation.
2.3 Classification of Anti-Epileptic Drugs (AEDs) into First, Second, and Third Generation
AEDs were classified as first-, second-, and third-generation drugs according to the recommendations of Löscher and Schmidt [30]. This classification considers the year of approval as well as the structural derivation of each single drug. AEDs that were approved between 1857 and 1958, such as potassium bromide and phenobarbital (PB), or derivates of the barbiturate structure, for example phenytoin (PHT), primidone (PRM), trimethadione, and ethosuximide (ESM), were classified as first-generation AEDs. Between 1960 and 1975, chlordiazepoxide, sulthiame (STM), diazepam (DZP), carbamazepine (CBZ), valproate (VPA), clonazepam (CLP), and clobazam (CLB) were approved and are categorized as second-generation AEDs. Progabide, vigabatrin (VGB), zonisamide (ZNS), lamotrigine (LTG), oxcarbazepine (OXC), felbamate (FLB), gabapentin (GBP), topiramate (TPM), tiagabine (TGB), levetiracetam (LEV), pregabalin (PGB), stiripentol (STP), rufinamide (RUF), lacosamide (LCM), and eslicarbazepine (ESL) entered the market after 1975 and were classified as third-generation AEDs. In line with this classification, newer AEDs like retigabine (RTG), perampanel (PER), and brivaracetam (BRV) were also categorized as third-generation AEDs. Moreover, AEDs were classified into enzyme-inducing (EIAEDs) and non-enzyme-inducing AEDs (non-EIAEDs), as well as into old and new AEDs, after Strzelczyk et al. [7]. This classification categorizes VPA, CBZ, PB, PRM, and PHT historically as “old” AEDs (frequently used first- and second-generation AEDs approved before 1975) as well as CBZ, PB, PRM, and PHT as EIAEDs based on their individual pharmacokinetic profiles. For further details on AEDs and their classification please refer to Table 1.
2.4 Data Entry and Statistical Analysis
Statistical analyses were performed using SPSS Statistics 22 (IBM Corporation, Armonk, NY, USA) and BiAS for Windows Version 10.01 (epsilon-Verlag, Frankfurt/Main, Germany). Price data are presented as mean values. Statistical comparisons between groups were performed using Chi square tests and a p < 0.05 was considered as significant. Figures were made using GraphPad PRISM (GraphPad Software Inc., La Jolla, CA, USA) and Pixelmator (Pixelmator Team, Vilnius, Lithuania). Interrupted Time Series Analysis (ITS) was employed to assess the individual effect of the implementation of two German healthcare acts introducing mandatory rebates for AEDs in 2004, i.e., the social health insurance modernization act (GKV-Modernisierungsgesetz), and 2006, i.e., the Arzneimittelversorgungs-Wirtschaftlichkeitsgesetz (AVWG). All analyses were performed using the autoregressive integrated moving average function (ARIMA) of SPSS Statistics 22. Following established paradigms, slopes of segmented linear regression of a pre- and post-intervention interval were tested for significant differences [31, 32].
3 Results
3.1 AED Prices and Prescription Patterns Between 2000 and 2017 on a National Level
For most AEDs, a decline in prices between 2000 and 2017 was observed, except for ESM (+ 20%), PB (+ 150%), PHT (+50%), and STM (+ 40%). The most eminent decline was seen for LEV (− 86%) and LTG (− 87%) followed by TPM (− 71%), GBP (− 70%), and CBZ (− 50%). Mean price per DDD from first-generation AEDs more than doubled between 2000 and 2017 from 0.3€ to 0.7€ per DDD, whereas mean prices for third-generation AEDs decreased by 65% from 6.0€ to 2.1€ per DDD, and after exclusion of GBP and PGB by 73% from 6.3€ to 1.7€ per DDD. Prices of second-generation AEDs decreased by 36% from 1.1€ to 0.7€ per DDD. For detailed information on AED prices between 2000 and 2017 please refer to Table 2.
Prescription frequency significantly decreased for first-generation AEDs by 55% (p < 0.001) and by 16% (p ≤ 0.001) for second-generation AEDs, while the use of third-generation AEDs dramatically increased (2494% [p < 0.001], and 1884% [p < 0.001] after exclusion of GBP and PGB). At the same time there was an increase of both third-generation AEDs recommended since 2008 as first-line treatment for focal epilepsies (LTG [519%], LEV [2681%]). These changes were accompanied by a significantly reduced prescription frequency of “older AEDs” by 49% (p < 0.001) and “enzyme-inducing” AEDs by 67% (p < 0.001). For further details please refer to Table 3.
Of note, between 2000 and 2017, nine new AEDs appeared for the first time in the national prescription reports after their introduction to the market, i.e., ESM (2004), OXC (2001), LEV (2002), PGB (2004), ZNS (2006), LCM (2009), PER (2013), BRV (2016), and ESL (2016). The evolution of prices and prescription volumes of AEDs are displayed for AED generations in Fig. 1 and for frequently used individual AEDs in Fig. 2.

Based on Schwabe et al. [29]
Anti-epileptic drug (AED) prices and prescriptions between 2000 and 2017. a Mean prices per defined daily dose (DDD) for each AED generation were calculated considering their individual prescription volumes showing a steady decrease of mean expenses per DDD of second- and third-generation drugs. b Prescription frequency of third-generation AEDs increased over time to the disadvantage of second- and third-generation AEDs. Due to the approval of gabapentin (GBP) and pregabalin (PGB) for neuropathic pain and other diseases, third-generation AED prices are displayed with and without (w/o) both drugs. The reported findings persist after exclusion of GBP and PGB from the analysis. c Total expenses for prescriptions of AEDs increased but remained stable since 2010/11.

Based on Schwabe et al. [29]
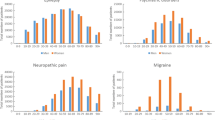
Evolution of prices and prescription frequencies of frequently used anti-epileptic drugs (AEDs) between 2000 and 2017. a Over time, a relevant decline in prices for all frequently used AEDs can be observed, with most drugs showing daily therapy expenditures of less than €3. b A trend towards the use of third-generation AEDs, especially for levetiracetam (LEV) and lamotrigine (LTG), can be observed since their approval. c Since 2010, overall AED expenditures decreased; however, the price share of the different AEDs remained more or less stable with trends towards an increased use of lacosamide (LCM). CBZ carbamazepine, OXC oxcarbazepine, TPM topiramate, VPA valproate, ZNS zonisamide.
3.2 Interrupted Time Series Analysis (ITS) on the Effect of Statutory Cost-Containment Measures on AED Prices
ITS analysis of prices per DDD based on national drug prescription data using the GKV-Modernisierungsgesetz as intercept revealed a significant reduction of prices for second-generation AEDs in general (p = 0.014), especially of CBZ (p = 0.007) and VPA (p = 0.023), as well as for third-generation AEDs (p = 0.045), i.e.. GBP (p = 0.001) and LTG (p = 0.005). The difference between pre- and post-intervention slopes of third-generation AEDs without GBP and PGB did not reach a level of significance. A similar ITS analysis was performed using the Arzneimittelversorgungs-Wirtschaftlichkeitsgesetz as intercept, and revealed a significant stabilization of DDD price for GBP, a drug that is approved for several indications and only sparingly used in modern epileptology, on a low level (p = 0.003) after a relevant initial decrease after the introduction of GKV-Modernisierungsgesetz (p = 0.001). All results of the ITS analysis are shown in Table 4. Exemplary graphs of ITS for PHT, CBZ, VPA, OXC, LTG, and GBP are given in Fig. 3.
Interrupted time series (ITS) analysis of phenytoin (PHT, a), carbamazepine (CBZ, b), valproate (VPA, c), oxcarbazepine (OXC, d), lamotrigine (LTG, e), and gabapentin (GBP, f), showing the effect of several statutory cost-containment measures in Germany between 2000 and 2017, i.e., the GKV-Modernisierungsgesetz (GKV MG, coming into effect on 1 January 2004) and the Arzneimittelversorgungs-Wirtschaftlichkeitsgesetz (AMV WG, coming into effect on 1 May 2006, with actual implementation 2007). In contrast to PHT, a first-generation AED, both, especially the GKV MG, had a significant effect on price reduction of newer anti-epileptic drugs (AEDs) of second- (CBZ, VPA) and third-generation AEDs (OXC, LTG, GBP). Implementation of measures of the AMV WG did not lead to an additional significant reduction in AED prices
3.3 Cohort-Based AED Prices and Prescription Frequency in 2003, 2008, 2013, and 2016
3.3.1 Characteristics of Study Populations
The 2003 cohort comprised 101 patients with a mean age of 40.7 years (range 18–78), a mean disease duration of 18.1 years, and 53.5% female patients. A focal epilepsy was reported in 76.2% and the mean number of AEDs per regime was 1.7 (range 0–4) [6]. In 2008, there were 494 patients with a mean age of 46.4 years (range 18–89), a mean disease duration of 25.0 years (range 0.1–81), and predominantly focal epilepsies (68.5%) were enrolled. The gender distribution was balanced (53.0% female) and a mean intake of 1.3 AEDs (range 0–4) was reported [19]. The 2013 cohort included 292 patients with a mean age of 40.8 years (range 18–86), a mean disease duration of 14.2 years (range 0.1–63), and a proportion of 54.8% female patients. A focal epilepsy was reported in 75.0% and the mean AED regime was 1.6 (range 0–4) [20]. In 2016, there were 481 patients with a mean age of 43.4 years (range 18–94), a mean disease duration of 17.4 years (range 0.4–63), and predominantly focal epilepsies were enrolled (75.9%). The gender distribution was balanced (53.6% female) and a mean AED intake of 1.7 (range 0–5) was reported [18]. For a detailed comparison of sociodemographic characteristics of the cohorts please refer to Table 5.
3.3.2 Common Monotherapies and Polytherapies with Two AEDs and Estimated Prices in the 2003, 2008, 2013, and 2016 Cohorts
In 2003, 41.8% reported a daily intake of one, 31.6% of two, and 22.8% of three or more AEDs. The most frequently prescribed AEDs as monotherapy were CBZ (17.3%), VPA (14.3%), and LTG (4.1%). The most frequent combinations of AEDs were CBZ/LTG (6.1%), LEV/VPA (4.1%), and LTG/VPA (3.1%). Mean prices for monotherapy were calculated at 2.1€ per day and for frequent combinations of two AEDs at 8.8€ per day. In 2008, 46.0% reported monotherapy, 31.8% therapy with two, and 7.7% therapy with three or more AEDs. The most common AEDs for monotherapy were CBZ (15.0%), LTG (10.1%), VPA (6.8%), and LEV (5.7%). The most frequent combinations of AEDs were LEV/LTG (4.5%), CBZ/LEV (3.2%), VPA/LTG (2.6%), LEV/VPA (2.0%), CBZ/LTG (1.6%), and CBZ/VPA (1.6%). Mean daily AED prices amounted to 2.0€ for mono- and 4.9€ for combinations of two AEDs. In 2013, 48.3% were on an anticonvulsive monotherapy, 34.6% on two AEDs, and 15.5% on therapy with three or more AEDs. The most frequently prescribed monotherapies were LEV (20.2%), LTG (13.0%), VPA (6.5%), and CBZ (4.8%). The most frequent AED combinations were LEV/LTG (8.9%), LEV/LCM (4.8%), LEV/VPA (3.1%), LEV/CBZ (2.4%), VPA/LTG (2.1%), and LTG/ZNS (1.7%). Mean daily AED prices were estimated at 1.6€ for the frequent monotherapies and 4.6€ per day for common therapy regimens with two AEDs. In 2016, 46.6% reported monotherapy, 32.6% therapy with two AEDs, and 18.5% with three or four AEDs. The most frequent AEDs for monotherapy were LEV (17.5%), LTG (15.0%), VPA (6.0%), and CBZ (4.8%). The most common dual therapies were LTG/LEV (5.8%), LTG/VPA (3.1%), CBZ/LEV (2.1%), LCM/LEV (2.1%), LEV/OXC (1.9%), and LEV/VPA (1.5%). Daily costs of 1.0€ for monotherapy and of 2.8€ for patients with two AEDs were calculated.
The prescription shares of “old” AEDs significantly decreased from 63.7% in 2003 to 38.0% in 2008, to 17.0% in 2013, and to 20.7% in 2016 (p < 0.001, 2003 vs. 2016). Consistent with this, intake of “enzyme-inducing” AEDs significantly declined from 26.8% in 2003, to 22.4% in 2008, to 7.7% in 2013, and to 7.6% in 2016 (p < 0.001, 2003 vs. 2016). Further details on AED prescription patterns and price calculations are presented in Tables 5 and 6.
4 Discussion
Modern healthcare systems have to face the conflicting factors of increased demand for medical innovations and limited structural and economic resources. As a consequence, resource allocation and cost containment are increasingly important. In patients with epilepsy, AED expenses have been identified as the most important driving factor for disease-specific direct costs and are expected to have a high potential for savings [10, 20, 33]. During the last two decades, cost-containment reforms and measures to foster cost containment and economic efficiency were introduced to the German healthcare system by several statutory reforms focusing on savings of both newly approved and generic drugs [12, 13, 15]. In 2017, overall savings due to statutory rebates on drugs were estimated to be €6.7 billion (Report on Preliminary Results of Statutory Health Insurance 2017, www.bundesgesundheitsministerium.de).
National data from the Arzneimittelreport by Schwabe et al. for each year between 2000 and 2017 were used to show trends in AED prices and prescriptions in Germany [29]. As these data do not contain indications of the prescriptions, we confirmed the results in 1368 epilepsy patients recruited in four cross-sectional cohorts in 2003, 2008, 2013, and 2016. Prescription frequency of third-generation AEDs increased markedly, while use of first- and second-generation AEDs decreased as the share of all AEDs and in absolute numbers. In particular, the market share of LEV, LTG, LCM, and OXC dramatically increased, which is consistent with the reported good adherence, tolerability, and safety of these “newer” AEDs [34, 35]. Moreover, clinical practice guidelines (CPG) of the German Society for Neurology (Deutsche Gesellschaft für Neurologie, DGN) have recommended the use of LEV and LTG instead of CBZ as first-line AEDs for patients with newly diagnosed focal epilepsy since 2008 [36]. One effect of the systematic implementation and adherence to CPGs in all healthcare sectors seems to be the increased prescription of LEV and LTG since 2008 [37, 38].
The contemporaneous increase in prescription of GBP and PGB appears to be mainly influenced by the wide application spectrum of these drugs and their main use as analgesics and psychoactive drugs rather than anticonvulsants [5, 39, 40]. Remarkably, the prescription frequency of VPA has decreased since evidence of its teratogenic effects when used during pregnancy became widely known in 2014 [41, 42]. Probably due to the frequent use of VPA as a mood stabilizer in psychiatric patients, these consequences were more distinct in the analysis of clinical cohorts with confirmed epilepsy than on the national level. Nevertheless, VPA is a highly efficient AED, especially in refractory as well as in idiopathic generalized epilepsies or epileptic encephalopathies, and is still one of the most frequently prescribed AEDs in Germany [43,44,45].
In addition, the prescription frequency of “old” and “enzyme-inducing” AEDs significantly decreased both on a national and a cohort-based level, consistent with other publications on adult patients with epilepsy [19, 33]. Given that several studies reported contradictory findings, the trend towards an increased use of “newer” AEDs in children and adolescents with epilepsy in Germany is not that obvious, which could relate to different prescription patterns of physicians specialized in pediatric neurology and prescriptions written by general pediatricians or family physicians [10, 46].
The trend for increased use of newer AEDs was accompanied by an overall price decline of third-generation AEDs on a national level by 65% (73% when excluding GBP and PGB) and of frequent monotherapy and therapies with two AEDs within the analyzed cohorts of 55% (2.2€–1.0€) and 68% (8.8€–3.1€), respectively. Mean prices for second-generation AEDs decreased by 36%. Mean prices for first-generation AEDs increased by + 133%, which seems to be based on inclusion of ethosuximide (ESM, 2.4€ per DDD in 2017) into the analysis in 2004. In addition, a moderate price increase for PB, PHT, and STM was observed, which was probably based on higher production expenditures, a smaller market share, and a small number of manufacturers. The market authorization of several new and therefore rather expensive AEDs between 2000 and 2017 did not noticeably increase general AED expenditures. Hence, the introduction of new and expensive AEDs seems to be historically balanced by price reductions of established AEDs being increasingly available as generic formulations, at least since 2000. In addition, a twofold increase (respectively 1.8-fold increase when excluding GPB and PGB) in prescription frequencies for all AEDs between 2000 and 2010 was observed, which may explain, together with the shift to more expensive AEDs, the general increase in total expenditures of AEDs between 2000 and 2010 on a national basis.
Whereas the reported trends towards using “newer” and “less interacting” AEDs with fewer pharmacokinetic interactions seem to be based on evidence-based CPGs [36], the observed price reduction of AEDs is probably driven by changes in German healthcare law. Our findings underline how effective statutory healthcare reforms can influence and decrease medication prices, at least regarding AEDs. In this context, the introduction of fixed rebates on generic medications, the possibility for health insurance to conclude individual rebate contracts with pharmaceutical companies, and the obligation for pharmacies to deliver the cheapest available product of the prescribed substance and dosage are of particular note [47, 48]. In particular, both rebate options were granted with a high saving potential, and in 2016, statutory savings due to rebate contracts added up to €6.6 billion at the federal level [49], which equals 1.8% of the predicted overall expenditures of €359.1 billion for health expenditures in Germany in 2016 [50]. This assumption is supported by the results of the ITS analysis performed on national prescription data (Table 4, Fig. 3), suggesting that the introduction of mandatory rebates on AED prices with the GKV-Modernisierungsgesetz led to lower prices especially of newer and frequently used AEDs, such as LTG, VPA, and GBP. In contrast, the results of a second large statutory healthcare reform in 2007, i.e., the Arzneimittelverordnungs-Wirtschaftlichkeitsgesetz, did not reveal any additional effect on AED price evolution in Germany. This finding could be related to a methodical weakness of the used method, especially due to the few numbers of timepoints for the compared intervals.
The statutory constraint to switch patients from original to generic formulations was controversial. Several publications associated the switch to generic AEDs with a general increase in seizure frequency or relapses in previously seizure-free patients [51,52,53]. However, larger analysis did not confirm these initial findings in general, but did not exclude individual seizure worsening in some patients [54, 55]. In this context, the distinct decline in prices for lamotrigine, topiramate, and levetiracetam after becoming available as generic formulations in 2005, 2009, and 2011 emanate from national data (Fig. 2). Similar effects for newer AEDs can be expected for frequently used “newer” drugs, for example, lacosamide, brivaracetam, and eslicarbazepine, after becoming available as generic formulations, which may contribute to a further cost containment in this medical sector.
With the early-benefit analysis by the Federal Joint Committee (Gemeinsamer Bundesausschuss, GBA) a new regulatory authority was founded in 2011 to evaluate efficiency, safety, and reimbursement of new drugs within less than 1 year after their market access [15, 56, 57]. Due to the lack of a consensus between GBA and its manufacturer on reimbursement, RTG and PER were temporarily withdrawn from the German market, and the availability of BRV was also at stake. In 2016, German health expenditures were €356.5 billion, with a share of €53.3 billion (15.4%) for drugs in general (www.destatis.de). Total expenditures for AEDs aggregated to approximately €700 million, equaling 1.3% of drug and 0.2% of health expenditures [29]. Given a 0.5–1% prevalence in Germany, disease-specific expenditures for epilepsy seem appropriate from a health economic point of view, especially when compared to other diseases or recently approved biologicals or biosimilars.
Within the next 2 years, cannabidiol and fenfluramine will probably be approved for the treatment of specific and rare epilepsy syndromes such as Dravet Syndrome, Lennox–Gastaut-Syndrome, and Tuberous Sclerosis Complex (TSC). Assuming market prices comparable to or exceeding that of STP [58, 59], the overall budget impact should be modest. In addition to AEDs, disease-modifying agents such as everolimus for TSC, which was also recently approved for treatment-resistant focal-onset seizures associated with TSC, will play an increasing role in the treatment of epilepsies [60, 61]. However, the overall budget impact and potential economic effectiveness of a personalized treatment approach is not foreseeable at the moment, but should be part of health economic assessments in the future [62, 63].
This study has several limitations, which are mainly based on the chosen study design. The usage of national data on drug expenses and prescriptions, and cohort-based prescription patterns for the calculation of mean AED prices only allows drawing conclusions for Germany. However, most of the discussed cost-containment efforts have been introduced in a more or less comparable way in other European and non-European countries. Moreover, the diverse composition of the four cohorts in view of subjects with active epilepsy and epilepsy in remission could have influenced the results of our analyses. Based on the comparable usage of frequently used AEDs in each of the cohorts compared to the year-specific national prescription frequencies, the possible resulting bias seems negligible. Another source of error could derive from the different coverage area of the used cohort studies, which were performed in Frankfurt and/or Marburg, Germany. However, due to national epilepsy guidelines that are well adopted in Germany [38, 64], different AED prescription preferences in both areas seem unlikely. Due to the analysis of general trends, a clear allocation between price reduction in general and a specific cost-containment effort was not possible, therefore only general conclusions are drawn. In addition, a common problem in longitudinal analysis is the comparability of different cohorts at different time points. As a trend-study, the given analysis is only able to identify general tendencies and allow no conclusions on individual level.
5 Conclusion
Prices for the most common AEDs decreased markedly between 2000 and 2017. Furthermore, these findings were accompanied by an expenditure-neutral trend towards the use of “newer” and “less interacting” third-generation AEDs. German statutory healthcare reforms and the introduction of generic formulations appear to have influenced prices of newer and frequently used AEDs; however, total annual expenditures for AEDs remained stable.
Data availability statement
National prescription frequency and prices: The data that support the findings of this part of the study have been fully published in the annual ‘Arzneiverordnungs-Reports’ by Ulrich Schwabe, Dieter Pfaffrath, Wolf-Dieter Ludwig, and Jürgen Klauber, and are accessible as digital or printed version of the annual ‘Arzneiverordnungs-Report’, published by Springer Verlag Deutschland GmbH. Data for the cohort studies: The data that support the findings of this part of the study are available from the corresponding author [AS], and anonymized data will be shared by request from any qualified investigator. The data are not publicly available due to restrictions by the local ethics commissions prohibiting the publication of unprocessed data that could compromise research participant privacy.
References
GBD 2015 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet. 2016;388:1545–602.
Strzelczyk A, Reese JP, Dodel R, et al. Cost of epilepsy: a systematic review. PharmacoEconomics. 2008;26:463–76.
Fisher RS, Acevedo C, Arzimanoglou A, et al. ILAE Official Report: a practical clinical definition of epilepsy. Epilepsia. 2014;55:475–82.
Willems L, Richter S, Watermann N, et al. Trends in resource utilization and prescription of anticonvulsants for patients with active epilepsy in Germany from 2003 to 2013—a ten-year overview. Epilepsy Behav. 2018;83:28–35.
Hamer HM, Dodel R, Strzelczyk A, et al. Prevalence, utilization, and costs of antiepileptic drugs for epilepsy in Germany—a nationwide population-based study in children and adults. J Neurol. 2012;259:2376–84.
Hamer HM, Spottke A, Aletsee C, et al. Direct and indirect costs of refractory epilepsy in a tertiary epilepsy center in Germany. Epilepsia. 2006;47:2165–72.
Strzelczyk A, Haag A, Reese JP, et al. Trends in resource utilization and prescription of anticonvulsants for patients with active epilepsy in Germany. Epilepsy Behav. 2013;27:433–8.
Strzelczyk A, Ansorge S, Hapfelmeier J, et al. Costs, length of stay, and mortality of super-refractory status epilepticus: A population-based study from Germany. Epilepsia. 2017;58:1533–41.
Schubert-Bast S, Zöllner JP, Ansorge S, et al. Burden and epidemiology of status epilepticus in infants, children, and adolescents: A population-based study on German health insurance data. Epilepsia. 2019;60:911–20.
Riechmann J, Strzelczyk A, Reese JP, et al. Costs of epilepsy and cost-driving factors in children, adolescents, and their caregivers in Germany. Epilepsia. 2015;56:1388–97.
von der Schulenburg G, Uber A. Current issues in German healthcare. Pharmacoeconomics. 1997;12:517–23.
Steinbronn R. 18 months law for the modernisation of the SHI—review and prospects. Z Kardiol. 2005;94:15–8.
Herr A. Wettbewerb und Rationalisierung im deutschen Arzneimittelmarkt: ein Überblick. List Forum für Wirtschafts- und Finanzpolitik. 2013;39:163–81.
Strzelczyk A. Hamer HM [Impact of early benefit assessment on patients with epilepsy in Germany: current healthcare provision and therapeutic needs]. Nervenarzt. 2016;87:386–93.
Ruof J, Schwartz FW, Schulenburg JM, et al. Early benefit assessment (EBA) in Germany: analysing decisions 18 months after introducing the new AMNOG legislation. Eur J Health Econ. 2014;15:577–89.
Duerden MG. Generic substitution. Reimbursement requires reform. BMJ (Clin Res Ed). 2010;341:c3566.
Duerden MG, Hughes DA. Generic and therapeutic substitutions in the UK: are they a good thing? Br J Clin Pharmacol. 2010;70:335–41.
Kadel J, Bauer S, Hermsen AM, et al. Use of Emergency Medication in Adult Patients with Epilepsy: a Multicentre Cohort Study from Germany. CNS Drugs. 2018;32:771–81.
Strzelczyk A, Nickolay T, Bauer S, et al. Evaluation of health-care utilization among adult patients with epilepsy in Germany. Epilepsy Behav. 2012;23:451–7.
Willems LM, Richter S, Watermann N, et al. Trends in resource utilization and prescription of anticonvulsants for patients with active epilepsy in Germany from 2003 to 2013—a ten-year overview. Epilepsy Behav. 2018;83:28–35.
Knake S, Rosenow F, Vescovi M, et al. Incidence of status epilepticus in adults in Germany: a prospective, population-based study. Epilepsia. 2001;42:714–8.
Fisher RS, Cross JH, French JA, et al. Operational classification of seizure types by the International League Against Epilepsy: position Paper of the ILAE Commission for Classification and Terminology. Epilepsia. 2017;58:522–30.
Scheffer IE, Berkovic S, Capovilla G, et al. ILAE classification of the epilepsies: position paper of the ILAE Commission for Classification and Terminology. Epilepsia. 2017;58:512–21.
von Elm E, Altman DG, Egger M, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Epidemiology. 2007;18:800–4.
Benchimol EI, Smeeth L, Guttmann A, et al. The REporting of studies Conducted using Observational Routinely-collected health Data (RECORD) statement. PLoS Med. 2015;12:e1001885.
Pfannkuche M, Glaeske G, Neye H, et al. Kostenvergleiche für Arzneimittel auf der Basis von DDD im Rahmen der Vertragsärztlichen Versorgung. Gesundh ökon Qual manag. 2009;2009:17–23.
Bock JO, Brettschneider C, Seidl H, et al. Calculation of standardised unit costs from a societal perspective for health economic evaluation. Gesundheitswesen. 2015;77:53–61.
Krauth C, Hessel F, Hansmeier T, et al. Empirical standard costs for health economic evaluation in Germany—a proposal by the working group methods in health economic evaluation. Gesundheitswesen. 2005;67:736–46.
Schwabe U. Antiepileptika. In: Schwabe U, Pfaffrath D, Ludwig W-D, et al., eds., Arzneiverordnungs-Report. Berlin, Germany: Springer-Verlag GmbH, 2001-2018
Löscher W, Schmidt D. Modern antiepileptic drug development has failed to deliver: ways out of the current dilemma. Epilepsia. 2011;52:657–78.
Jandoc R, Burden AM, Mamdani M, et al. Interrupted time series analysis in drug utilization research is increasing: systematic review and recommendations. J Clin Epidemiol. 2015;68:950–6.
Koskinen H, Mikkola H, Saastamoinen LK, et al. Time series analysis on the impact of generic substitution and reference pricing on antipsychotic costs in Finland. Value Health. 2015;18:1105–12.
Strzelczyk A, Griebel C, Lux W, et al. The Burden of Severely Drug-Refractory Epilepsy: A Comparative Longitudinal Evaluation of Mortality, Morbidity, Resource Use, and Cost Using German Health Insurance Data. Front Neurol. 2017;8:712.
Adelson PD, Black PM, Madsen JR, et al. Use of subdural grids and strip electrodes to identify a seizure focus in children. Pediatr Neurosurg. 1995;22:174–80.
Gollwitzer S, Kostev K, Hagge M, et al. Nonadherence to antiepileptic drugs in Germany: a retrospective, population-based study. Neurology. 2016;87:466–72.
Elger C, Berkenfeld R. S1-Leitlinie Erster epileptischer Anfall und Epilepsien im Erwachsenenalter., Deutsche Gesellschaft für Neurologie: Leitlinien für Diagnostik und Therapie in der Neurologie, 2017.
Ertl J, Hapfelmeier J, Peckmann T, et al. Guideline conform initial monotherapy increases in patients with focal epilepsy: a population-based study on German health insurance data. Seizure. 2016;41:9–15.
Strzelczyk A, Bergmann A, Biermann V, et al. Neurologist adherence to clinical practice guidelines and costs in patients with newly diagnosed and chronic epilepsy in Germany. Epilepsy Behav. 2016;64:75–82.
French J, Glue P, Friedman D, et al. Adjunctive pregabalin vs gabapentin for focal seizures: interpretation of comparative outcomes. Neurology. 2016;87:1242–9.
Goodman CW, Brett AS. Gabapentin and pregabalin for pain—is increased prescribing a cause for concern? N Engl J Med. 2017;377:411–4.
European Medicines Agency. PRAC recommends strengthening the restrictions on the use of valproate in women and girls. 2014. EMA/612389/2014
Virta LJ, Kalviainen R, Villikka K, et al. Declining trend in valproate use in Finland among females of childbearing age in 2012-2016—a nationwide registry-based outpatient study. Eur J Neurol. 2018;25:869–74.
Mole TB, Appleton R, Marson A. Withholding the choice of sodium valproate to young women with generalised epilepsy: are we causing more harm than good? Seizure. 2015;24:127–30.
Nariai H, Duberstein S, Shinnar S. Treatment of epileptic encephalopathies: current state of the art. J Child Neurol. 2018;33:41–54.
Kortland LM, Alfter A, Bähr O, et al. Costs and cost-driving factors for acute treatment of adults with status epilepticus: a multicenter cohort study from Germany. Epilepsia. 2016;57:2056–66.
Dorks M, Langner I, Timmer A, et al. Treatment of paediatric epilepsy in Germany: antiepileptic drug utilisation in children and adolescents with a focus on new antiepileptic drugs. Epilepsy Res. 2013;103:45–53.
Graf J. The effects of rebate contracts on the health care system. Eur J Health Econ. 2014;15:477–87.
Natz A. Rebate contracts: risks and chances in the German generic market. J Generic Med. 2008;5:99–103.
Bundesministerium für Gesundheit. Gesetzliche Krankenversicherung, Vorläufige Rechnungsergebnisse, 1.-4. Quartal 2016. Berlin, 2017.
Brungs S. Gesundheitsausgaben im Jahr 2015 um 4,5 % gestiegen. [Health expenditure increase by 4.5% in 2015.] DeSTATIS: Pressemitteilung Nr. 061 vom 21. Februar 2017; Berlin, 2017. https://www.destatis.de/DE/Presse/Pressemitteilungen/2017/02/PD17_061_23611.html
Welty TE, Pickering PR, Hale BC, et al. Loss of seizure control associated with generic substitution of carbamazepine. Ann Pharmacother. 1992;26:775–7.
Wyllie E, Pippenger CE, Rothner AD. Increased seizure frequency with generic primidone. JAMA. 1987;258:1216–7.
Berg MJ, Gross RA, Tomaszewski KJ, et al. Generic substitution in the treatment of epilepsy: case evidence of breakthrough seizures. Neurology. 2008;71:525–30.
Kwan P, Palmini A. Association between switching antiepileptic drug products and healthcare utilization: a systematic review. Epilepsy Behav. 2017;73:166–72.
Kesselheim AS, Bykov K, Gagne JJ, et al. Switching generic antiepileptic drug manufacturer not linked to seizures: a case-crossover study. Neurology. 2016;87:1796–801.
Henschke C, Sundmacher L, Busse R. Structural changes in the German pharmaceutical market: price setting mechanisms based on the early benefit evaluation. Health Policy. 2013;109:263–9.
Kaier K, Fetzer S. The German Pharmaceutical Market Reorganization Act (AMNOG) from an economic point of view. Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz. 2015;58:291–7.
Strzelczyk A, Schubert-Bast S, Reese JP, et al. Evaluation of health-care utilization in patients with Dravet syndrome and on adjunctive treatment with stiripentol and clobazam. Epilepsy Behav. 2014;34:86–91.
Strzelczyk A, Kalski M, Bast T, et al. Burden-of-illness and cost-driving factors in Dravet syndrome patients and carers: a prospective, multicenter study from Germany. Eur J Paediatr Neurol EJPN. 2019. https://doi.org/10.1016/j.ejpn.2019.02.014.
Schubert-Bast S, Rosenow F, Klein KM, et al. The role of mTOR inhibitors in preventing epileptogenesis in patients with TSC: current evidence and future perspectives. Epilepsy Behav. 2019;91:94–8.
French JA, Lawson JA, Yapici Z, et al. Adjunctive everolimus therapy for treatment-resistant focal-onset seizures associated with tuberous sclerosis (EXIST-3): a phase 3, randomised, double-blind, placebo-controlled study. Lancet. 2016;388:2153–63.
Rosenow F, van Alphen N, Becker A, et al. Personalized translational epilepsy research—novel approaches and future perspectives: part I: clinical and network analysis approaches. Epilepsy Behav. 2017;76:13–8.
Bauer S, van Alphen N, Becker A, et al. Personalized translational epilepsy research—novel approaches and future perspectives: part II: experimental and translational approaches. Epilepsy Behav. 2017;76:7–12.
Noda AH, Reese JP, Berkenfeld R, et al. Leitlinienumsetzung und Kosten bei neudiagnostizierter Epilepsie. Zeitschrift für Epileptologie. 2015;28:304–10.
Author information
Authors and Affiliations
Contributions
LMW developed the idea for this study. LMW and AS conceived the paper, collected the data, and performed statistical analysis. LMW, JPR, and AS interpreted the statistical analysis and results. LMW and AS created the charts and figures. All authors wrote the paper, discussed the results, contributed to the final manuscript, and approved the final manuscript for publication.
Corresponding author
Ethics declarations
Study funding
This study was supported by the LOEWE Grant for the “Center for Personalized Translational Epilepsy Research (CePTER), Goethe-University Frankfurt, Frankfurt am Main, Germany.
Conflict of interest
LM. Willems and J.P. Reese report no conflicts of interest. H.M. Hamer has served on the scientific advisory board of Cerbomed, Desitin, Eisai, GW, Novartis, and UCB Pharma. He served on the speakers’ bureau of or received unrestricted grants from Amgen, Ad-Tech, Bial, Bracco, Cyberonics, Desitin, Eisai, Hexal, Nihon Kohden, Novartis, Pfizer, and UCB Pharma. S. Knake reports honoraria for speaking engagements from Desitin and UCB as well as educational grants from AD Tech, Desitin Arzneimittel, Eisai, GW, Medtronic, Novartis, Siemens and UCB. F. Rosenow reports personal fees from Eisai, grants and personal fees from UCB, grants and personal fees from Desitin Pharma, personal fees and others from Novartis, personal fees from Medronic, personal fees from Cerbomed, personal fees from ViroPharma and Shire, grants from the European Union, and grants from the Deutsche Forschungsgemeinschaft. A. Strzelczyk reports personal fees and grants from Desitin Arzneimittel, Eisai, GW Pharma, LivaNova, Medtronic, Sage Therapeutics, UCB Pharma, and Zogenix. All authors confirm that they have read the Journal’s position on issues involved in ethical publication and affirm that this report is consistent with those guidelines.
Rights and permissions
About this article
Cite this article
Willems, L.M., Hamer, H.M., Knake, S. et al. General Trends in Prices and Prescription Patterns of Anticonvulsants in Germany between 2000 and 2017: Analysis of National and Cohort-Based Data. Appl Health Econ Health Policy 17, 707–722 (2019). https://doi.org/10.1007/s40258-019-00487-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40258-019-00487-2