Abstract
Alzheimer's disease is the most common neurodegenerative disorder that usually occurs after the age of 65 for which there is currently no cure. The predominant feature of this disease is the appearance of beta amyloid plaques next to the neurons in the brain. Numerous studies have investigated the possible causes of the disease and in particular the role of metals. In the present study, while briefly reviewing the effect of various lifestyle factors on the incidence and prevalence of the disease, by presenting the latest clinical reports and cohort studies regarding the role of metals in the disease, we try to provide a comprehensive overview of this issue to the reader. Some studies have shown changes in the concentration of metals in the brain or body fluids of AD patients, while others have not indicated any change. Therefore, it can be concluded that metals are not causative factor, but they are risk factor in certain conditions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It is estimated that 1.5 billion people on Earth will be over 65 years of age by 2050. Aging is associated with changes in different cellular processes caused by different factors that lead to reduce function of various organs and tissues, including the brain. Old age is also a major risk factor for neurodegenerative diseases, including Alzheimer's disease (AD) [1]. AD is a deadly disease that is characterized by beta-amyloid (Aβ) plaques and neurofibrillary tangles outside and inside brain neurons, respectively [2] (Fig. 1). Unfortunately, this disease can be detected in the advanced stages and after the onset of symptoms, which is too late for any effective treatment, and on the other hand, the drugs approved for its treatment do not have a significant effect on the well-being of patients [3]. For these reasons, there is an urgent need to identify and treat this devastating disorder.
AD is a complex and multifactorial disease, and various factors such as amyloid protein, tau protein, metals, and other issues have been studied as its possible causes [4]. Naturally, there are small amounts of metals such as zinc, copper, and iron in our body that are essential for the proper functioning of the brain and body and involved in various processes such as energy production, oxygen transport, and the production and regulation of many important molecules in the body [5]. Apart from essential metals, there are other metals that people are exposed to or contaminated with in various ways [6]. The body is resistant to small amounts of these elements (e.g., aluminum and lead) [7,8,9,10]; however, if these elements are not excreted due to the intake of large amounts of them or kidney failure, they can be deposited in the body and can cause adverse effects in the brain and cause neurological complications [7]. Relatively much research has been done on the relationship between different metals and AD, but there is no consensus. In this review article, while briefly reviewing the preventable factors, the role of metals in the development of this disease has been specifically addressed.
In the past, diagnostic efforts have focused on patients who are in the dementia stage, but more recently, the importance of the long pre-dementia period (a period in which clinical symptoms have not yet developed) has been noted. The initial stage, which is silent and asymptomatic, is called the pre-clinical stage and is characterized by symptoms that begin approximately 20 years before the onset of the disease [11].
Unfortunately, the reason of AD has not yet been diagnosed and therefore there is no cure for it. However, epidemiological studies have provided information on its risk factors that, in addition to helping to identify the cause, can provide appropriate measures to prevent it [12]. According to these documents, in addition to factors such as aging, gender and the presence of genetic mutations that cannot be avoided, preventable risk factors including "environmental factors" and "lifestyle" are also involved in causing this deadly disease [13].
Preventable influencing factors in Alzheimer's disease
So far, no drug has been shown to be effective in treating AD; therefore, studies in this area have focused on healthy people who may be at risk for AD to prevent AD with this strategy. Since genetics is not often the cause, other factors have come to the fore, and the impact of "environmental factors" and "lifestyle" on the progression of AD is becoming increasingly apparent [14]. Diabetes mellitus, smoking, depression, mental inactivity, physical inactivity, and poor diet were initially identified as risk factors [15], which later added blood pressure, obesity, and low education to this list [16]. It is worth noting that diet is a highly modifiable lifestyle factor that can reduce the risk of AD [17].
Risk factors for cardiovascular diseases such as unhealthy diets, physical inactivity, and stress (anxiety) are now also known as risk factors for AD [12, 18]. Interestingly, a significant association has recently been reported between the risk factors for cardiovascular disease in the "mid-life" and amyloid deposition in the "later years" [19].
Smoking in a large fraction of sufferers' population has made it a serious risk factor. Tobacco smoke contains hundreds of chemicals that are toxic to neurons and can damage neurons by causing oxidative stress and inflammation [16, 20]. Among the compounds in cigarette smoke, it has been shown that Pb(IV) can interact with the N-terminal of Aβ and cause it to precipitate [21].
Although some cohort studies have shown that the risk of developing AD has been halved in people who have had high physical activity [22, 23], no randomized controlled trial (RCT) study has confirmed this [24]. However, in a recent study [25], the researchers did not find any neuroprotective effects of physical activity and suggested that reduced physical activity may be due to dementia.
Cohort and interventional studies have shown that taking vitamin supplements cannot prevent AD, but high fat, diabetes, and lifestyle factors (alcohol, smoking, obesity, etc.) increase the risk of AD on average, and fish, the Mediterranean diet, unsaturated fats, and social activities play a protective role [26]. In addition, epidemiological studies and animal model researches have shown a positive effect of caffeine consumption on the brain function and prevention of AD [27,28,29]. Some reports have suggested that these effects are due to improve antioxidant status, reduce lipid peroxidation, and inhibit acetylcholinesterase, adenosine deaminase, and arginase activities in the brain and cortex [30, 31]. Acetylcholinesterase [32], adenosine deaminase [29, 33, 34], and arginase [35] are enzymes that inhibition of them can be considered as a possible solution in the field of disease control or treatment.
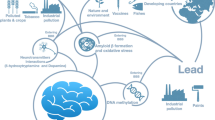
Environmental factors include exposure to toxic metals, pesticides, industrial chemicals, and air pollutants. Exposure to these environmental pollutants and their biological accumulation during a person's lifetime can cause inflammation and neurological disease leading to the development of AD [36]. Since the 1980s, much attention has been paid to the role of metals in AD because various cell processes, such as energy production, repair, and proliferation, depend on metals. On the other hand, a significant part of the population is usually exposed to metals such as aluminum, lead, iron, and copper, which are obtained from various sources and are all considered risk factors [37] (Fig. 2).
The role of metals in the development of Alzheimer's disease
One of the main cellular processes that is impaired with age is the homeostasis of metals and the function of proteins related to them, which directly and indirectly affect the disorders of aging [1]. Metals are natural compounds that easily lose electrons and are converted to cations. Metals are found throughout the earth, including the atmosphere, the earth's crust, and water, and therefore can accumulate in plant and animal organisms. Among the 35 natural metals, 23 have a density of more than 5 g/cm3 and an atomic weight of over 40, which are called heavy metals [38]. This group of metals is not only famous for their high density, but also because of their detrimental effects on ecosystem and living organisms [39].
Metals are generally classified to essential and non-essential groups [40]. An essential metal must have several properties: first, it must be present in human tissues, second, its absence in the body can cause severe and irreversible damage to biological functions, and third, the reduction in physiological function returns to normal with appropriate supplements [5]. Some metals, such as copper, cobalt, iron, nickel, magnesium, molybdenum, chromium, selenium, manganese, and zinc, have functional roles and are essential for a variety of biochemical and physiological activities in the body [41]. Although large amounts of some of these metals can be harmful to the body, very small amounts of non-essential metals such as cadmium, mercury, lead, chromium, silver, and arsenic have delusional effects and can cause acute or chronic intoxication [39].
Metals associated with Alzheimer's disease
Aluminum
The only metal previously was considered as a risk factor for AD was aluminum that is controversial today [37]. Aluminum is the third most common element in the nature after oxygen and silicon; however, no role has been identified for it in living systems. Aluminum is broadly used in medicine, pharmacy, food industry, and cosmetics, also, in the manufacture of kitchen utensils and food preparation, and through these ways, it enters the human body [42]. Aluminum is a light metal, and its alloys with other metals are strong and durable; therefore, it is used in the manufacture of kitchen utensils. Numerous studies have shown that aluminum leaks into food from aluminum containers and foils, but leaking depends on many factors such as degree of acidity, temperature, cooking method, food content, cooking time (contact with aluminum), and the presence of fluoride, sugar, salt, and organic acids [43].
On the other hand, the absorption of aluminum is affected by elements such as iron, calcium, zinc, and citrate [44]. Aluminum foil is widely used for food packaging, cosmetics, and chemicals. Aluminum foil is easy to use, disposable, having twice the heat transfer of other metals; therefore, it is widely used for cooking. Aluminum leakage has been observed in some foods due to cooking in aluminum foil. Although the amount of food aluminum in this method has been reported to increase up to 40 times, this amount of aluminum is not a concern for healthy people [44]. Antacids are other notable cases in the field of aluminum intake. Antacids are aluminum-rich drugs that are widely used. Regular use of antacids has not been linked to AD in either case–control or cohort studies [45].
In 1965, researchers injected very high doses of aluminum (accidentally) into rabbits, increasing tau protein deposition and increasing plaque in the brain led to speculation that aluminum in cans, cookware and processed foods, and even drinking water can cause dementia [46]. However, subsequent studies have shown that food contact with aluminum containers cannot increase the concentration of aluminum in the blood so much that it reaches the millimolar levels, the levels needed to reduce glucose metabolism in the brain. In fact, the pathophysiological mechanisms of "non-diet" lead to the accumulation of aluminum, while most dietary aluminum is excreted by the kidneys [47]. On average, about 10 mg of aluminum enters the human body daily, of which about 9.6 mg is obtained from food and the rest is due to the use of aluminum containers. It is noteworthy that in healthy people, about 0.01–1% of the received aluminum is absorbed into the blood and the rest is excreted from the body [42, 43]. In addition, the Food and Agriculture Organization and the World Health Organization have reported in 2011 that receiving 2 mg/kg body weight per week is safe [43].
Tea is one of the few plants that has a high accumulation of aluminum in its leaves [48], but the prevalence of dementia in areas with high consumption of tea has not been reported. On the other hand, epidemiological and systematic studies have shown that the green tea has positive effects in preventing dementia and AD, and drinking tea is considered as a natural remedy [49,50,51]. In fact, the amounts of various metals, including aluminum, that enter the body through tea drinking are not high enough to raise concerns about AD [52]. In addition, some studies have shown that the tea extract in C. elegans worm model of AD delays some of the complications of the disease and increases the life of the worm [53].
Some studies in 2013 found that the long-term effects of aluminum dust inhalation by miners, which were common between 1950 and 1960 (even up to the time of the study), did not make a significant difference in the development of AD [54]. In addition, a meta-analysis study in 2015 found that occupational exposure to aluminum was not significantly associated with AD [55]. In general, several studies on the relationship between aluminum in drinking water and AD have reported different results [56]. Some believe that aluminum in drinking water is involved in causing disease [57] and some consider it ineffective [58,59,60] and even protective [61]. A meta-analysis study in 2016 with a total of 10,567 participants [62] has shown that people who were chronically exposed to aluminum were 71% more likely to develop AD. Moreover, a recent study has shown that aluminum concentration is very high in the brains of familial AD patients [63]. The presence of aluminum in the core of amyloid plaques has already been reported [64]. In addition, it has been shown that aluminum accumulates selectively in the arterial walls from the aorta to the PCA (posterior cerebral artery; the main artery in the hippocampus) so that it precipitates 9 times as much as the aortic wall in the PCA wall [65].
Copper
The copper needed by the body is provided by the water and food consumption. The average copper concentration in the US tap water is about 0.02–0.075 mg/L, and drinking water makes up about 6–13% of the copper intake [66]. On the other hand, the National Research Council (USA) has declared that the intake of 1.3 mg/L copper in drinking water or in the milk of infants receiving copper-enriched milk is safe. In addition, the European Chemicals Agency has reported environmental copper concentrations without concern [67]. Foods containing copper include the organs meats (brain, tongue, liver, offal, etc.), nuts, seafood, seeds, legumes, and whole grains [68]. The average daily intake of copper in the USA is 1–1.6 mg/day for adults [67].
Copper can be as monovalent or divalent cation in food, but only is in divalent form in water. The initial uptake of copper occurs actively in the form of monovalent in the gastrointestinal tract [69]. Divalent copper is rapidly reduced on the surface of intestinal cells by metalloreductase activity [70]. Exposure to too much copper internalizes the copper transporter in the intestine, and as a result, copper absorption decreases and its excretion increases [71]. In fact, daily copper intake in the range of 0.57–6.9 mg has been shown to have no effect on plasma copper concentrations [72]. Some evidence indicated that AD patients who received copper for 1 year did not show any unpleasant changes compared with those who received placebo. Therefore, the causative effect of "excess copper" to develop the disease is ruled out [73]. Excessive copper intake seems to be problematic when accompanied with saturated fats. A prospective epidemiologic study on 3,718 participants showed that the rate of cognitive decline was tripled in those who had high saturated fat diets with high copper intake over a 6-year period, that is, their global cognitive score (the mean of the 4 tests) decreased as much as 19 years over 6 years [74].
Some studies have suggested that copper in food is healthy, but inorganic copper, which is in vitamin supplements and tap water, can pass through the liver and enter the bloodstream and brain directly. It is especially dangerous when accompanied by saturated and trans fats [75, 76]. Copper binds to the histidine or proteins such as albumin and macroglobulin in the bloodstream [71, 77]. Some reports have found no clear correlation between copper uptake and factors such as zinc, ascorbic acid, and fiber, but some have reported an inverse relationship between copper, zinc, and iron uptake [68].
Involvement of copper transporter genes in Menkes and Wilson’s diseases where copper deficiency and accumulation occur, respectively, also neurological disorders and cognitive decline that occur in both of them, can indicate the effect of impaired copper homeostasis on serious damages to nerve cells [78]. Aβ homeostasis in the brain of AD mouse models was impaired by reducing copper intake [79]. Another study showed that reducing copper intake in healthy men led to a significant reduction in the plasma opioid peptides that returned to normal levels with copper intake [80, 81]. Opioid peptides have analgesic and wound-healing properties. A longitudinal cohort study has revealed that anxiety and pain are major problems for dementia patients [82]. On the other hand, various studies have shown an association between opioid system dysfunction and AD (reviewed in [83]).
Iron
Iron accumulation in the brain occurs naturally with age. Data from a research project on healthy people revealed that in addition to aging, smoking and body mass index also have a significant effect on iron accumulation in the brain and its distribution similar to AD [84]. Too much iron can be toxic [85]. On the other hand, iron deficiency causes anemia, which increases the risk of dementia [86]. Some data have shown that the women with the highest cognitive scores had the lowest levels of copper and iron in their blood [87]. Also, another research has indicated that people with high hemoglobin (an indicator of iron content) are more likely to develop AD [88], while the latest meta-analysis shows that serum iron is lower in AD patients compared to controls [89]. In addition, recent findings suggest that iron concentrations in deep gray matter and neocortical areas are higher in AD patients, and changes in iron levels in the temporal lobe over time are associated with cognitive decline in AD patients [90]. A similar study shows that increased cortical iron in AD patients is closely related to the rate of cognitive decline, presumably by stimulating oxidative stress, inflammation, or ferroptosis cell death [91]. The results of new researches indicate that low-oxidation-state iron, which is dangerous in AD and increases the oxidative stress, can be caused by the interaction of Aβ with ferritin (inert iron) [92].
Zinc
Zinc plays essential roles in various functions related to AD such as Aβ production and tau phosphorylation; thus, zinc dyshomeostasis can disrupt these functions of zinc and interfere with the development or progression of AD [93]. Some studies have shown that zinc deficiency, a metal that involves in DNA synthesis and short-term learning and memory, may lead to cognitive problems [94, 95], and several small studies have shown that taking zinc supplements can help to improve brain function [96,97,98]. The latest meta-analysis shows that AD patients have less serum zinc than their healthy counterparts do [89]. New findings show that mRNA or protein levels of major zinc transporters have changed at different stages of AD in brains of patients [99]. Although both copper and zinc accumulate in amyloid plaques, the evidence generally suggests a protective role for zinc. It has been shown that zinc can decrease the toxicity of amyloid peptides by changing their conformation in plaques [100].
Lead
Lead is a heavy metal with which acute poisoning is common and severe poisoning with this element leads to known neurological symptoms [101]. However, mild lead poisoning is associated with symptoms of AD [102, 103]. There is also evidence that lead poisoning in early life can lead to increased DNA methylation, amyloid production, and APP expression in old age [104,105,106]. Lead is a chronic and potent toxin in the brain that has detrimental effects through a variety of mechanisms, including mitochondrial dysfunction, dysfunction of neurotransmitters, and inappropriate nerve responses (by substituting calcium and zinc) [107]. Recently, data from an animal study have revealed that lead in sub-toxic and toxic levels straightly attacks cerebral vascular system and damages the blood–brain barrier (BBB) [108]. Furthermore, another study shows that in subchronic exposure to lead, lead accumulates in choroid plexus and decreases the clearance of Aβ from the cerebrospinal fluid (CSF), which in turn results in an increase in Aβ in the CSF [109]. Although special attention is paid to the toxicity of lead during development, due to the ability of lead to cross the BBB, its toxicity in adults is also very important. About 95% of lead accumulation occurs in bone [110], where it can replace calcium and be stored in hydroxyapatite (the main bone and tooth material). While the half-life of lead in the blood is about 30 days, its half-life in bone is about 20–30 years, and various factors cause it to be released from the bone marrow into the bloodstream [107]. It is noteworthy that the latest meta-analysis has shown that the blood lead concentration in AD patients has decreased [111].
Mercury
Mercury is another heavy metal with which acute poisoning is common and leads to well-known neurological symptoms [101] and the mild poisoning caused by it causes AD symptoms [102, 103]. Mercury has a half-life of about 20 years in the brain, and its effects in AD are exacerbated due to the brain being specifically targeted by mercury [112]. Recent studies show that mercury binds specifically to Aβ and prevents it from fibrillization [113, 114]. The results of a meta-analysis show that AD patients have more blood mercury than healthy people [111]. Moreover, a recent cross-sectional study has reported a significant relationship between increased exposure to ethylmercury and cognitive decline [115].
Mercury is a highly toxic pollutant for living systems. In general, dental amalgams are the first source of mercury accumulated in the human brain [116]. The results of some studies show that a high prevalence of memory impairment among dentists and dental staff (who are more exposed to mercury than others) has been reported [117, 118]. Moreover, personnel are more likely than others to complain of problems such as neurobehavioral problems, decreased psychomotor speed, decreased cognitive flexibility, attention deficit, and also memory loss, fatigue, and sleep problems [117, 119]. An investigation in 2019 that was conducted on more than 16,666 dementia patients and 33,332 healthy controls showed no relationship between amalgam use and the spread of dementia but indicated that those who had dementia showed more accelerated progression of the disease depending on the amount of amalgam used [120]. However, public health agencies, including the FDA, the US Public Health Service, and the World Health Organization, have approved the use of amalgam as a safe, durable, and cost-effective material for dental restorations [120].
Air pollution with this metal (mercury leakage from mines) and its accumulation in seafood has increased its toxicity potential for humans. On the other hand, preservatives containing mercury in vaccines are still controversial. Mercury in vapor and in organic compounds can enter hydrophobic tissues. Many studies have shown a causal link between exposure to mercury and the incidence and progression of AD, and this is not surprising because mercury is a powerful inhibitor of many biochemical pathways, each of which can damage the central nervous system and reduce cognitive function. The association of this metal with AD needs further study [116, 121].
Manganese
Manganese is an essential metal; therefore, its toxicity to neurons occurs in large quantities, and long-term environmental exposure to low levels of it has been shown to cause serious damage to the brain cells [122]. Particular attention is paid to this metal in Parkinson-like syndrome, which is very common in occupational exposure [123]. The proposed mechanism of neurotoxicity for this metal is not specific to Parkinson's disease and may play a role in other neurological diseases such as AD [110, 124]. A cohort study on more than 1,000 people in Australia showed that manganese was lower in the serum of AD patients than in healthy people [110]. A more recent meta-analysis, including 836 cases and 1,254 healthy controls, also found that serum manganese levels in AD patients were significantly decreased compared with controls [125]. These results contradict some studies on smaller groups that have shown an increase in plasma manganese concentration in AD patients [126, 127]. It is noteworthy that manganese is distributed differently in different parts of the blood, with about 66% in red blood cells, 30% in buffy coat, and 4% in plasma [128].
Some data indicate that plasma Aβ increases with increasing manganese and there is a significant relationship between manganese and Mini-Mental State Exam (MMSE) and Clinical Dementia Rating Scale scores of the elderly subjects with different cognitive statuses [129]. Further investigation in this study, both in vitro and in vivo, suggest that manganese may cause neurotoxicity by disrupting Aβ degradation. Recent studies have confirmed this issue because they have shown that treatment of SH-SY5Y cells with manganese reduces APP expression [130, 131]. Numerous other studies have shown that manganese can play a role in the neurotoxicity of AD by causing oxidative stress, mitochondrial dysfunction, and malfunction of neurotransmitter systems (reviewed in [132]).
Magnesium
Some studies have suggested that plasma magnesium is lower in AD patients than that in healthy people [133] and other studies have shown a link between serum magnesium concentrations and the degree of AD [134]. Moreover, other findings have revealed that magnesium is lower in some brain areas in AD patients compared to controls [135, 136]. The results of a systematic review have indicated that magnesium in CSF and hair of AD patients are less than those of controls, but there is no difference in their serum magnesium [137]. A randomized trial in 2015 has shown that cognitive function in older participants remarkably improved by magnesium supplementation [138]. However, a prospective population-based cohort study with a total of 9,569 participants has indicated that both low serum magnesium and high serum magnesium are correlated with an increased risk of dementia [139].
Furthermore, recent studies provide evidence that magnesium supplementation can reduce methylation of the APOE gene (an important risk factor for AD) in people over 65 years of age and significantly improve their cognitive function as well [140]. On the other hand, previous evidence has shown that increased APOE methylation is correlated with age-associated cognitive decline [141]. Moreover, it has been shown that magnesium-induced neurotoxicity is determined by protein phosphatase 2 A (PP2A) demethylation, which is correlated with tau hyperphosphorylation and shortage of spatial learning and memory in rat models, and possibly S-adenosylmethionine (SAM) deficiency in the hippocampus determines the loss of PP2A methylation [142]. PP2A is a main tau phosphatase, which its activity is performed by the methylation state of catalytic C subunit, and SAM—downstream metabolite of methionine-acts as a methyl donor in transmethylation pathways [142]. In addition, some studies show that magnesium deficiency can result in detrimental effects in endothelium integrity and disrupt endothelial barrier functions [143] and other experimental evidence shows that magnesium can decrease permeability of in vitro BBB model and increase clearance of Aβ through BBB [143].
Cobalt
Cobalt is an essential component of cobalamin (vitamin B12) and is necessary for the normal functioning of the nervous system, the production of DNA, and energy metabolism [112]. MMSE has revealed that serum cobalt content can be directly related to cognition [144]. Moreover, vitamin B12 deficiency has been shown to ultimately increase the risk of AD and leads to disease progression in patients [145, 146], and also, some studies have shown the decrease in cobalt in the serum of AD patients [147]. In addition, recent in vitro studies have shown that vitamin B12 binds directly to tau protein and prevents its fibrillization [148] and other data show that cobalt complexes prevent tau aggregation [149]. Cobalt complexes also affect beta deposition and stabilize non-toxic species of beta deposits [150]. Cobalt-Schiff base complexes have been suggested as potential therapeutic agents for various situations including as inhibiting protein aggregation [151].
Arsenic
Arsenic causes toxicity in human, and its two main sources are drinking water and food [152, 153]. It has been revealed that serum arsenic levels are inversely related to cognitive test scores [154], and its high levels can cause phosphorylation of tau protein (a protein that is highly phosphorylated and precipitated in AD) [155] and transcription of APP [156]. An in vitro study showed that arsenic in APP overexpressing cells increased APP expression but decreased Aβ production [157]. Although it has been hypothesized that arsenic may be the cause of AD [158], no significant difference has been observed between serum arsenic in AD patients and healthy cases [154]. However, a recent study has reported a positive correlation between soil arsenic concentration and AD mortality [159] and other studies have reported a negative correlation between groundwater arsenic levels and neuropsychological performance [160, 161]. In addition, other findings have shown that high fat diet (in mice) exacerbates arsenic-induced memory impairment three times [162]. The permeability of the BBB to this metal has made it a powerful neurotoxin. By inducing pro-inflammatory cytokines such as TNF-α, IL-6, it directly affects the cortex, cerebellum, and especially microglia [163]. Pro-apoptotic signaling and activation of caspase by arsenic cause large-scale tissue damage [163].
MMSE scores from a case–control study showed that high urinary inorganic arsenic or low dimethylarsinic acid has significant associations with AD risk [164]. The molecular mechanisms of arsenic neurodegeneration effects involved mitochondrial dysfunction, oxidative stress, epigenetics, changes in neurotransmitter homeostasis and synaptic transmission, inflammation, and cell death pathways (reviewed in [165]).
Cadmium
Cadmium is a food contaminant that can be tolerated up to 62 µg/kg of body weight daily [166]. Cigarette smoke is another source of cadmium contamination [167]. People on normal diets get about 40–60% of this amount from the diet, but eating oysters, crustaceans, and spinach can increase that amount. However, some studies believe that this tolerable range should be reduced [166]. A meta-analysis study revealed that cadmium in the blood of AD patients was significantly higher compared to controls [111]. Findings from a study on 2,068 participants aged ≥ 60 years old [168] have indicated that elevated blood cadmium is accompanied with poorer cognitive function. Moreover, another study on a total of 4,064 participants aged ≥ 60 years old in the USA showed a significant relationship between blood cadmium levels and AD mortality in the elderly [169]. Animal studies have shown that cadmium can bypass the BBB [170] and even can alter the tight junction integrity of the BBB [171]. Some data from an in vitro study show that cadmium intervenes in the regulation of genes related to calcium regulation and other genes associated with microtubules dynamics and neuroprotection [172].
Sodium
The association between high sodium intake and hypertension and cardiovascular disease has led to a general recommendation to reduce sodium intake to improve cardiovascular health [173]. A systematic review study shows that although different associations have been reported between sodium levels and cognition, the only clinical trial study has shown that lower sodium intake is associated with improved cognition. In addition, three of the four high-quality studies have shown that higher sodium intake is associated with cognitive impairment [174]. Another study showed a direct link between nail sodium levels and the clinical stages of AD [175]. Some evidence suggests that sodium-coupled oligopeptide transport system is involved in Aβ uptake from brain into capillary endothelial cells and this transfer occurs in the direction of the sodium concentration gradient [176]. Furthermore, it has been shown that a salt-rich diet in mice resulted in cognitive dysfunction associated with tau hyperphosphorylation [177].
Other metals
There is a report on an increase in molybdenum in the blood of AD patients [178]. Moreover, it has been reported that potassium and rubidium are significantly reduced in all intracellular components in the AD brain. However, no significant change in their concentrations in serum, erythrocytes, and CSF was observed in patients and in the disease stages, which shows that, contrary to the hypothesis of impaired BBB in AD patients, ion leakage from the blood is minimal [179].
Conclusion
Metals play important roles in the human body including maintaining cell structure, regulating gene expression, neurotransmission, and antioxidant responses. However, the accumulation of high levels of them in the nervous system can be toxic, cause oxidative stress, impair mitochondrial function, and alter the activity of many enzymes. Metals accumulation can lead to permanent damages such as neurological diseases [40].
It is noteworthy that a significant fraction of population is exposed to high level of metals that are toxic to the nervous system. In addition, it has been observed that genetics and other trace metals can have a synergistic effect with them and increase their toxicity, in which case it is necessary to reconsider their use, whether in food (fish) or medicine (used in vaccines and other drugs) [180].
In general, various studies have shown the dyshomeostasis of some essential metals and the presence of some non-essential metals in AD patients, but a systematic study in 2017 shows that there is no evidence that metals are causative in AD [181].
Overall, the diversity of information about the relationship between metals and AD (Table 1) clarifies two points. First, because the change in metals concentrations with AD is not significant in some studies, metals cannot be considered as the cause of the disease. Second, due to the significant change in metal concentrations with AD in another part of the studies, it can be concluded that in favorable conditions for the disease, changes in metal homeostasis or the presence of toxic metals can contribute to the occurrence and progression of the disease.
References
P.A. Adlard, A.I. Bush, Metals and Alzheimer’s disease: how far have we come in the clinic? J. Alzheimer’s Dis. 62, 1369–1379 (2018). https://doi.org/10.3233/JAD-170662
C.J. Sarell, The Copper-Amyloid-Beta-Peptide Complex of Alzheimer’ s Disease : Affinity, Structure, Fibril Formation and Toxicity (University of London, London, 2010).
S. Bagheri, R. Squitti, T. Haertlé, M. Siotto, A.A. Saboury, Role of copper in the onset of Alzheimer’s disease compared to other metals. Front. Aging Neurosci. 9, 446 (2018). https://doi.org/10.3389/fnagi.2017.00446
X. Du, X. Wang, M. Geng, Alzheimer’s disease hypothesis and related therapies. Transl. Neurodegener. (2018). https://doi.org/10.1186/s40035-018-0107-y
M.A. Zoroddu, J. Aaseth, G. Crisponi, S. Medici, M. Peana, V.M. Nurchi, The essential metals for humans: a brief overview. J. Inorg. Biochem. 195, 120–129 (2019). https://doi.org/10.1016/J.JINORGBIO.2019.03.013
A.A.A. Saad, A. El-Sikaily, H. Kassem, Essential, non-essential metals and human health. Pollut. Status Environ. Prot. Renew. Energy Prod. Mar. Syst. 3, 47 (2016)
M. Jaishankar, T. Tseten, N. Anbalagan, B.B. Mathew, K.N. Beeregowda, Toxicity, mechanism and health effects of some heavy metals. Interdiscip. Toxicol. 7, 60–72 (2014). https://doi.org/10.2478/intox-2014-0009
S.G. Schäfer, W. Forth, Excretion of metals into the rat intestine. Biol. Trace Elem. Res. 5, 205–217 (1983). https://doi.org/10.1007/BF02916624
A.T. Jan, M. Azam, K. Siddiqui, A. Ali, I. Choi, Q.M.R. Haq, Heavy metals and human health: mechanistic insight into toxicity and counter defense system of antioxidants. Int. J. Mol. Sci. 16, 29592–29630 (2015). https://doi.org/10.3390/ijms161226183
S.J. Genuis, M. Sears, G. Schwalfenberg, J. Hope, R. Bernhoft, Incorporating environmental health in clinical medicine. J. Environ. Public Health. (2012). https://doi.org/10.1155/2012/103041
B. Dubois, H.H. Feldman, C. Jacova, H. Hampel, J.L. Molinuevo, K. Blennow, S.T. Dekosky, S. Gauthier, D. Selkoe, R. Bateman, S. Cappa, S. Crutch, S. Engelborghs, G.B. Frisoni, N.C. Fox, D. Galasko, M.O. Habert, G.A. Jicha, A. Nordberg, F. Pasquier, G. Rabinovici, P. Robert, C. Rowe, S. Salloway, M. Sarazin, S. Epelbaum, L.C. de Souza, B. Vellas, P.J. Visser, L. Schneider, Y. Stern, P. Scheltens, J.L. Cummings, Advancing research diagnostic criteria for Alzheimer’s disease: The IWG-2 criteria. Lancet Neurol. (2014). https://doi.org/10.1016/S1474-4422(14)70090-0
A.M. Fernandez, A. Santi, I. Torres Aleman, Insulin peptides as mediators of the impact of life style in Alzheimer’s disease. Brain Plast. 4, 3–15 (2018). https://doi.org/10.3233/bpl-180071
M. Baumgart, H.M. Snyder, M.C. Carrillo, S. Fazio, H. Kim, H. Johns, Summary of the evidence on modifiable risk factors for cognitive decline and dementia: a population-based perspective. Alzheimer’s Dement. 11, 718–726 (2015). https://doi.org/10.1016/j.jalz.2015.05.016
M. Crous-Bou, C. Minguillón, N. Gramunt, J.L. Molinuevo, Alzheimer’s disease prevention: from risk factors to early intervention. Alzheimer’s Res. Ther. 9, 71 (2017). https://doi.org/10.1186/s13195-017-0297-z
M.L. Daviglus, C.C. Bell, W. Berrettini, P.E. Bowen, E.S. Connolly, N.J. Cox, J.M. Dunbar-Jacob, E.C. Granieri, G. Hunt, K. McGarry, D. Patel, A.L. Potosky, E. Sanders-Bush, D. Silberberg, M. Trevisan, National Institutes of Health state-of-the-science conference statement: preventing Alzheimer disease and cognitive decline. Ann. Intern. Med. 153, 176–181 (2010). https://doi.org/10.7326/0003-4819-153-3-201008030-00260
D.E. Barnes, K. Yaffe, The projected impact of risk factor reduction on Alzheimer’s disease prevalence. Lancet Neurol. 10, 819–828 (2011). https://doi.org/10.1016/S1474-4422(11)70072-2
B.R. Cardoso, C. Cominetti, S.M.F. Cozzolino, Importance and management of micronutrient deficiencies in patients with Alzheimer’s disease. Clin. Interv. Aging. 8, 531–542 (2013). https://doi.org/10.2147/CIA.S27983
A.G. Pacholko, C.A. Wotton, L.K. Bekar, Poor diet, stress, and inactivity converge to form a “Perfect Storm” that drives Alzheimer’s disease pathogenesis. Neurodegener. Dis. 19, 60–77 (2019). https://doi.org/10.1159/000503451
R.F. Gottesman, A.L.C. Schneider, Y. Zhou, J. Coresh, E. Green, N. Gupta, D.S. Knopman, A. Mintz, A. Rahmim, A.R. Sharrett, L.E. Wagenknecht, D.F. Wong, T.H. Mosley, Association between midlife vascular risk factors and estimated brain amyloid deposition. JAMA J. Am. Med. Assoc. (2017). https://doi.org/10.1001/jama.2017.3090
J.K. Cataldo, J.J. Prochaska, S.A. Glantz, Cigarette smoking is a risk factor for Alzheimer’s disease: an analysis controlling for tobacco industry affiliation. J. Alzheimer’s Dis. 19, 465–480 (2010). https://doi.org/10.3233/JAD-2010-1240
C. Wallin, S.B. Sholts, N. Österlund, J. Luo, J. Jarvet, P.M. Roos, L. Ilag, A. Gräslund, S.K.T.S. Wärmländer, Alzheimer’s disease and cigarette smoke components: effects of nicotine, PAHs, and Cd(II), Cr(III), Pb(II), Pb(IV) ions on amyloid-β peptide aggregation. Sci. Rep. 7, 14423 (2017). https://doi.org/10.1038/s41598-017-13759-5
D. Laurin, R. Verreault, J. Lindsay, K. MacPherson, K. Rockwood, Physical activity and risk of cognitive impairment and dementia in elderly persons. Arch. Neurol. 58, 498–504 (2001). https://doi.org/10.1001/archneur.58.3.498
L.J. Podewils, E. Guallar, L.H. Kuller, L.P. Fried, O.L. Lopez, M. Carlson, C.G. Lyketsos, Physical activity, APOE genotype, and dementia risk: findings from the cardiovascular health cognition study. Am. J. Epidemiol. 161, 639–651 (2005). https://doi.org/10.1093/aje/kwi092
Y. Rolland, G. Abellan van Kan, B. Vellas, Physical activity and Alzheimer’s disease: from prevention to therapeutic perspectives. J. Am. Med. Dir. Assoc. 9, 390–405 (2008). https://doi.org/10.1016/j.jamda.2008.02.007
S. Sabia, A. Dugravot, J.F. Dartigues, J. Abell, A. Elbaz, M. Kivimäki, A. Singh-Manoux, Physical activity, cognitive decline, and risk of dementia: 28 year follow-up of Whitehall II cohort study. BMJ 357, j2709 (2017). https://doi.org/10.1136/bmj.j2709
M. Weih, J. Wiltfang, J. Kornhuber, Non-pharmacologic prevention of Alzheimer’s disease: nutritional and life-style risk factors. J. Neural Transm. 114, 1187–1197 (2007). https://doi.org/10.1007/s00702-007-0704-x
A. Mendonça, R.A. Cunha, Therapeutic opportunities for caffeine in Alzheimer’s disease and other neurodegenerative disorders. J. Alzheimer’s Dis. (2010). https://doi.org/10.3233/JAD-2010-01420
V. Flaten, C. Laurent, J.E. Coelho, U. Sandau, V.L. Batalha, S. Burnouf, M. Hamdane, S. Humez, D. Boison, L.V. Lopes, L. Buée, D. Blum, From epidemiology to pathophysiology: what about caffeine in Alzheimer’s disease? Biochem. Soc. Trans. 42, 587–592 (2014). https://doi.org/10.1042/BST20130229
Y. Chern, N. Rei, J.A. Ribeiro, A.M. Sebastião, Adenosine and its receptors as potential drug targets in amyotrophic lateral sclerosis. J. Caffeine Adenosine Res. 9, 157–166 (2019). https://doi.org/10.1089/caff.2019.0016
S.F. Akomolafe, The effects of caffeine, caffeic acid, and their combination on acetylcholinesterase, adenosine deaminase and arginase activities linked with brain function. J. Food Biochem. 41, e12401 (2017). https://doi.org/10.1111/jfbc.12401
S.F. Akomolafe, A.J. Akinyemi, O.B. Ogunsuyi, S.I. Oyeleye, G. Oboh, O.O. Adeoyo, Y.R. Allismith, Effect of caffeine, caffeic acid and their various combinations on enzymes of cholinergic, monoaminergic and purinergic systems critical to neurodegeneration in rat brain—in vitro. Neurotoxicology. 62, 6–13 (2017). https://doi.org/10.1016/j.neuro.2017.04.008
K. Sharma, Cholinesterase inhibitors as Alzheimer’s therapeutics (Review). Mol. Med. Rep. 20, 1479–1487 (2019). https://doi.org/10.3892/mmr.2019.10374
S. Bagheri, A.A. Saboury, T. Haertlé, Adenosine deaminase inhibition. Int. J. Biol. Macromol. 141, 1246–1257 (2019). https://doi.org/10.1016/j.ijbiomac.2019.09.078
G. Ataie, S. Bagheri, A. Divsalar, A.A. Saboury, S. Safarian, S. Namaki, A.A. Moosavi-Movahedi, A kinetic comparison on the inhibition of adenosine deaminase by purine drugs. Iran. J. Pharm. Res. 6, 43–50 (2007)
S.V. Ovsepian, V.B. O’Leary, Can arginase inhibitors be the answer to therapeutic challenges in Alzheimer’s disease? Neurotherapeutics. 15, 1032–1035 (2018). https://doi.org/10.1007/s13311-018-0668-6
Y. Manivannan, B. Manivannan, T. Beach, R. Halden, Role of environmental contaminants in the etiology of Alzheimers disease: a review. Curr. Alzheimer Res. 12, 116–146 (2015). https://doi.org/10.2174/1567205012666150204121719
A.R. Armstrong, Risk factors for Alzheimer’s disease. Folia Neuropathol. 57, 87–105 (2019). https://doi.org/10.5114/fn.2019.85929
F. Li, Z. Qiu, J. Zhang, W. Liu, C. Liu, G. Zeng, Investigation, pollution mapping and simulative leakage health risk assessment for heavy metals and metalloids in groundwater from a typical brownfield, middle China. Int. J. Environ. Res. Public Health. 14, 768 (2017). https://doi.org/10.3390/ijerph14070768
G. Azeh Engwa, P. Udoka Ferdinand, F. Nweke Nwalo, M. N. Unachukwu, Mechanism and Health Effects of Heavy Metal Toxicity in Humans, in Poisoning Mod World New Tricks an Old Dog? (2019). https://doi.org/10.5772/intechopen.82511.
P. Chen, M.R. Miah, M. Aschner, Metals and Neurodegeneration. F1000Research. (2016). https://doi.org/10.12688/f1000research.7431.1
WHO, Trace elements in human nutrition and health World Health Organization, World Heal. Organ. (1996).
E. Inan-Eroglu, A. Ayaz, Is aluminum exposure a risk factor for neurological disorders? J. Res. Med. Sci. 2018, 23–51 (2018). https://doi.org/10.4103/jrms.JRMS_921_17
Y.K. Gupta, M. Meenu, S.S. Peshin, Aluminium utensils: Is it a concern? Natl. Med. J. India. 32, 38–40 (2019). https://doi.org/10.4103/0970-258X.272116
D. Dordevic, H. Buchtova, S. Jancikova, B. Macharackova, M. Jarosova, T. Vitez, I. Kushkevych, Aluminum contamination of food during culinary preparation: case study with aluminum foil and consumers’ preferences. Food Sci. Nutr. 7, 3349–3360 (2019). https://doi.org/10.1002/fsn3.1204
S.A. Virk, G.D. Eslick, Brief report: meta-analysis of antacid use and Alzheimer’s disease: implications for the aluminum hypothesis. Epidemiology. 26, 769–773 (2015). https://doi.org/10.1097/EDE.0000000000000326
T.I. Lidsky, Is the aluminum hypothesis dead? J. Occup. Environ. Med. 56, 73–79 (2014). https://doi.org/10.1097/JOM.0000000000000063
D.L. Marcus, D.L. Wong, M.L. Freedman, Dietary aluminum and alzheimer’s disease. J. Nutr. Elder. 12, 55–61 (1992). https://doi.org/10.1300/J052v12n02_04
H.P. Carr, E. Lombi, H. Küpper, S.P. McGrath, M.H. Wong, Accumulation and distribution of aluminium and other elements in tea (Camellia sinensis) leaves. Agronomie. 23, 705–710 (2003). https://doi.org/10.1051/agro:2003045
S. Kakutani, H. Watanabe, N. Murayama, Green tea intake and risks for dementia, Alzheimer’s disease, mild cognitive impairment, and cognitive impairment: a systematic review. Nutrients. 11, 1165 (2019). https://doi.org/10.3390/nu11051165
M. Noguchi-Shinohara, S. Yuki, C. Dohmoto, Y. Ikeda, M. Samuraki, K. Iwasa, M. Yokogawa, K. Asai, K. Komai, H. Nakamura, M. Yamada, Consumption of green tea, but not black tea or coffee, is associated with reduced risk of cognitive decline. PLoS ONE 9, e96013 (2014). https://doi.org/10.1371/journal.pone.0096013
C.A. Polito, Z.Y. Cai, Y.L. Shi, X.M. Li, R. Yang, M. Shi, Q.S. Li, S.C. Ma, L.P. Xiang, K.R. Wang, J.H. Ye, J.L. Lu, X.Q. Zheng, Y.R. Liang, Association of tea consumption with risk of alzheimer’s disease and anti-beta-amyloid effects of tea. Nutrients. 10, 655 (2018). https://doi.org/10.3390/nu10050655
S.C. Sofuoglu, P. Kavcar, An exposure and risk assessment for fluoride and trace metals in black tea. J. Hazard. Mater. 158, 392–400 (2008). https://doi.org/10.1016/j.jhazmat.2008.01.086
T. Fei, J. Fei, F. Huang, T. Xie, J. Xu, Y. Zhou, P. Yang, The anti-aging and anti-oxidation effects of tea water extract in Caenorhabditis elegans. Exp. Gerontol. 97, 89–96 (2017). https://doi.org/10.1016/j.exger.2017.07.015
S. Peters, A. Reid, L. Fritschi, N. De Klerk, A.W. Musk, Long-term effects of aluminium dust inhalation. Occup. Environ. Med. (2013). https://doi.org/10.1136/oemed-2013-101487
S.A. Virk, G.D. Eslick, Occupational exposure to aluminum and Alzheimer disease a meta-analysis. J. Occup. Environ. Med. 57, 893–896 (2015). https://doi.org/10.1097/JOM.0000000000000487
S. Meshitsuka, D.A. Aremu, T. Nose, A risk of Alzheimer’s disease and aluminum in drinking water. Psychogeriatrics. 2, 263–268 (2002). https://doi.org/10.1111/j.1479-8301.2002.tb00039.x
V. Rondeau, H. Jacqmin-Gadda, D. Commenges, C. Helmer, J.F. Dartigues, Aluminum and silica in drinking water and the risk of Alzheimer’s disease or cognitive decline: findings from 15-year follow-up of the PAQUID cohort. Am. J. Epidemiol. 169, 489–496 (2009). https://doi.org/10.1093/aje/kwn348
C.N. Martyn, D.N. Coggon, H. Inskip, R.F. Lacey, W.F. Young, Aluminum concentrations in drinking water and risk of Alzheimer’s disease. Epidemiology. 8, 281–286 (1997). https://doi.org/10.1097/00001648-199705000-00009
D.P. Forster, A.J. Newens, D.W.K. Kay, J.A. Edwardson, Risk factors in clinically diagnosed presenile dementia of the Alzheimer type: A case-control study in northern England. J. Epidemiol. Community Health. 49, 253–258 (1995). https://doi.org/10.1136/jech.49.3.253
G.A. Taylor, A.J. Newens, J.A. Edwardson, D.W.K. Kay, D.P. Forster, Alzheimer’s disease and the relationship between silicon and aluminium in water supplies in northern England. J. Epidemiol. Community Health. 49, 323–324 (1995). https://doi.org/10.1136/jech.49.3.323
X.L. Shen, J.H. Yu, D.F. Zhang, J.X. Xie, H. Jiang, Positive relationship between mortality from Alzheimer’s disease and soil metal concentration in mainland China. J. Alzheimer’s Dis. 42, 893–900 (2014). https://doi.org/10.3233/JAD-140153
Z. Wang, X. Wei, J. Yang, J. Suo, J. Chen, X. Liu, X. Zhao, Chronic exposure to aluminum and risk of Alzheimer’s disease: a meta-analysis. Neurosci. Lett. 610, 200–206 (2016). https://doi.org/10.1016/j.neulet.2015.11.014
A. Mirza, A. King, C. Troakes, C. Exley, Aluminium in brain tissue in familial Alzheimer’s disease. J. Trace Elem. Med. Biol. 40, 30–36 (2017). https://doi.org/10.1016/j.jtemb.2016.12.001
S. Yumoto, S. Kakimi, A. Ohsaki, A. Ishikawa, Demonstration of aluminum in amyloid fibers in the cores of senile plaques in the brains of patients with Alzheimer’s disease. J. Inorg. Biochem. 103, 1579–1584 (2009). https://doi.org/10.1016/j.jinorgbio.2009.07.023
S. Bhattacharjee, Y. Zhao, J.M. Hill, F. Culicchia, T.P.A. Kruck, M.E. Percy, A.I. Pogue, J.R. Walton, W.J. Lukiw, Selective accumulation of aluminum in cerebral arteries in alzheimer’s disease (ad). J. Inorg. Biochem. 126, 35–37 (2013). https://doi.org/10.1016/j.jinorgbio.2013.05.007
L.M. Gaetke, H.S. Chow-Johnson, C.K. Chow, Copper: toxicological relevance and mechanisms. Arch. Toxicol. 88, 1929–1938 (2014). https://doi.org/10.1007/s00204-014-1355-y
I. of Medicine, Dietary Reference Intakes for Vitamin A, Vitamin K, Arsenic, Boron, Chromium, Copper, Iodine, Iron, Manganese, Molybdenum, Nickel, Silicon, Vanadium, and Zinc (2001). https://doi.org/10.17226/10026.
A.A. Taylor, J.S. Tsuji, M.R. Garry, M.E. McArdle, W.L. Goodfellow, W.J. Adams, C.A. Menzie, Critical review of exposure and effects: implications for setting regulatory health criteria for ingested copper. Environ. Manage. 65, 131–159 (2020). https://doi.org/10.1007/s00267-019-01234-y
M.J. Ceko, J.B. Aitken, H.H. Harris, Speciation of copper in a range of food types by X-ray absorption spectroscopy. Food Chem. 164, 50–54 (2014). https://doi.org/10.1016/j.foodchem.2014.05.018
R.S. Ohgami, D.R. Campagna, A. McDonald, M.D. Fleming, The Steap proteins are metalloreductases. Blood 108, 1388–1394 (2006). https://doi.org/10.1182/blood-2006-02-003681
P.V.E. Van Den Berghe, L.W.J. Klomp, New developments in the regulation of intestinal copper absorption. Nutr. Rev. 67, 658–672 (2009). https://doi.org/10.1111/j.1753-4887.2009.00250.x
M. Bost, S. Houdart, M. Oberli, E. Kalonji, J.F. Huneau, I. Margaritis, Dietary copper and human health: Current evidence and unresolved issues. J. Trace Elem. Med. Biol. 35, 107–115 (2016). https://doi.org/10.1016/j.jtemb.2016.02.006
H. Kessler, F.-G. Pajonk, D. Bach, T. Schneider-Axmann, P. Falkai, W. Herrmann, G. Multhaup, J. Wiltfang, S. Schafer, O. Wirths, T.A. Bayer, Effect of copper intake on CSF parameters in patients with mild Alzheimer’s disease: a pilot phase 2 clinical trial. J. Neural Transm. 115, 1181–1187 (2008). https://doi.org/10.1007/s00702-008-0080-1
M.C. Morris, D.A. Evans, C.C. Tangney, J.L. Bienias, J.A. Schneider, R.S. Wilson, P.A. Scherr, Dietary copper and high saturated and trans fat intakes associated with cognitive decline. Arch. Neurol. 63, 1085–1088 (2006). https://doi.org/10.1001/archneur.63.8.1085
G.J. Brewer, Copper toxicity in Alzheimer’s disease: cognitive loss from ingestion of inorganic copper. J. Trace Elem. Med. Biol. 26, 89–92 (2012). https://doi.org/10.1016/j.jtemb.2012.04.019
G.J. Brewer, S.H. Kanzer, E.A. Zimmerman, D.F. Celmins, S.M. Heckman, R. Dick, Copper and ceruloplasmin abnormalities in Alzheimer’s disease. Am. J. Alzheimers. Dis. Other Demen. 25, 490–497 (2010). https://doi.org/10.1177/1533317510375083
G.R. Behbehani, L. Barzegar, M. Mohebbian, A.A. Saboury, A comparative interaction between copper ions with Alzheimer’s amyloid peptide and human serum albumin. Bioinorg. Chem. Appl. (2012). https://doi.org/10.1155/2012/208641
H.W. Hsu, S.C. Bondy, M. Kitazawa, Environmental and dietary exposure to copper and its cellular mechanisms linking to Alzheimer’s disease. Toxicol. Sci. 163, 338–345 (2018). https://doi.org/10.1093/toxsci/kfy025
I. Singh, A.P. Sagare, M. Coma, D. Perlmutter, R. Gelein, R.D. Bell, R.J. Deane, E. Zhong, M. Parisi, J. Ciszewski, R.T. Kasper, R. Deane, Low levels of copper disrupt brain amyloid-β homeostasis by altering its production and clearance. Proc. Natl. Acad. Sci. 110, 14771–14776 (2013). https://doi.org/10.1073/pnas.1302212110
L. Pickart, J.M. Vasquez-Soltero, A. Margolina, The effect of the human peptide GHK on gene expression relevant to nervous system function and cognitive decline. Brain Sci. 7, 20 (2017). https://doi.org/10.3390/brainsci7020020
S.J. Bhathena, L. Recant, N.R. Voyles, K.I. Timmers, S. Reiser, J.C. Smith, A.S. Powell, Decreased plasma enkephalins in copper deficiency in man. Am. J. Clin. Nutr. 43, 42–46 (1986). https://doi.org/10.1093/ajcn/43.1.42
E.L. Sampson, N. White, K. Lord, B. Leurent, V. Vickerstaff, S. Scott, L. Jones, Pain, agitation, and behavioural problems in people with dementia admitted to general hospital wards: a longitudinal cohort study. Pain 156, 675–683 (2015). https://doi.org/10.1097/j.pain.0000000000000095
Z. Cai, A. Ratka, Opioid system and Alzheimer’s disease. Neuromol. Med. 14, 91–111 (2012). https://doi.org/10.1007/s12017-012-8180-3
L. Pirpamer, E. Hofer, B. Gesierich, F. De Guio, P. Freudenberger, S. Seiler, M. Duering, E. Jouvent, E. Duchesnay, M. Dichgans, S. Ropele, R. Schmidt, Determinants of iron accumulation in the normal aging brain. Neurobiol. Aging. 43, 149–155 (2016). https://doi.org/10.1016/j.neurobiolaging.2016.04.002
J. Stankiewicz, S.S. Panter, M. Neema, A. Arora, C.E. Batt, R. Bakshi, Iron in chronic brain disorders: imaging and neurotherapeutic implications. Neurotherapeutics. 4, 371–386 (2007). https://doi.org/10.1016/j.nurt.2007.05.006
B.B. Yavuz, M. Cankurtaran, I.C. Haznedaroglu, M. Halil, Z. Ulger, B. Altun, S. Ariogul, Iron deficiency can cause cognitive impairment in geriatric patients. J. Nutr. Heal. Aging. 16, 220–224 (2012). https://doi.org/10.1007/s12603-011-0351-7
P.K. Lam, D. Kritz-Silverstein, E. Barrett-Connor, D. Milne, F. Nielsen, A. Gamst, D. Morton, D. Wingard, Plasma trace elements and cognitive function in older men and women: the Rancho Bernardo study. J. Nutr. Heal. Aging. 12, 22–27 (2008). https://doi.org/10.1007/BF02982160
R.C. Shah, A.S. Buchman, R.S. Wilson, S.E. Leurgans, D.A. Bennett, Hemoglobin level in older persons and incident Alzheimer disease prospective cohort analysis. Neurology. 77, 219–226 (2011). https://doi.org/10.1212/WNL.0b013e318225aaa9
D.D. Li, W. Zhang, Z.Y. Wang, P. Zhao, Serum copper, zinc, and iron levels in patients with Alzheimer’s disease: a meta-analysis of case-control studies. Front. Aging Neurosci. 15, 300 (2017). https://doi.org/10.3389/fnagi.2017.00300
A. Damulina, L. Pirpamer, M. Soellradl, M. Sackl, C. Tinauer, E. Hofer, C. Enzinger, B. Gesierich, M. Duering, S. Ropele, R. Schmidt, C. Langkammer, Cross-sectional and longitudinal assessment of brain iron level in Alzheimer disease using 3-T MRI. Radiology 296, 619–626 (2020). https://doi.org/10.1148/radiol.2020192541
S. Ayton, Y. Wang, I. Diouf, J.A. Schneider, J. Brockman, M.C. Morris, A.I. Bush, Brain iron is associated with accelerated cognitive decline in people with Alzheimer pathology. Mol. Psychiatry. 25, 2932–2941 (2020). https://doi.org/10.1038/s41380-019-0375-7
J. Everett, J. Brooks, F. Lermyte, P.B. O’Connor, P.J. Sadler, J. Dobson, J.F. Collingwood, N.D. Telling, Iron stored in ferritin is chemically reduced in the presence of aggregating Aβ(1–42). Sci. Rep. 10, 10332 (2020). https://doi.org/10.1038/s41598-020-67117-z
Z. Xie, H. Wu, J. Zhao, Multifunctional roles of zinc in Alzheimer’s disease. Neurotoxicology. 80, 112–123 (2020). https://doi.org/10.1016/j.neuro.2020.07.003
S.D. Gower-Winter, C.W. Levenson, Zinc in the central nervous system: From molecules to behavior. BioFactors 38, 186–193 (2012). https://doi.org/10.1002/biof.1012
J. Chaudhary, R. Jora, P. Sharma, R. Gehlot, A study of iron and zinc deficiency on short term memory in children & effect of their supplementation. Asian J. Biomed. Pharm. Sci. 5, 12–15 (2015). https://doi.org/10.15272/ajbps.v5i42.664
J.E. De Moura, E.N.O. De Moura, C.X. Alves, S.H. De Lima Vale, M.M.G. Dantas, A. De Araújo Silva, M. Das Graças Almeida, L.D. Leite, J. Brandão-Neto, Oral zinc supplementation may improve cognitive function in schoolchildren. Biol. Trace Elem. Res. 155, 23–28 (2013). https://doi.org/10.1007/s12011-013-9766-9
E. Khodashenas, A. Mohammadzadeh, M. Sohrabi, A. Izanloo, The effect of zinc supplementation on cognitive performance in schoolchildren. Int. J. Pediatr. 3, 1033–1038 (2015). https://doi.org/10.22038/ijp.2015.5617
R.P. Tupe, S.A. Chiplonkar, Zinc supplementation improved cognitive performance and taste acuity in indian adolescent girls. J. Am. Coll. Nutr. 28, 388–396 (2009). https://doi.org/10.1080/07315724.2009.10718101
Y. Xu, G. Xiao, L. Liu, M. Lang, Zinc transporters in Alzheimer’s disease. Mol. Brain. 12, 1–12 (2019). https://doi.org/10.1186/s13041-019-0528-2
V. Tõugu, A. Karafin, K. Zovo, R.S. Chung, C. Howells, A.K. West, P. Palumaa, Zn(II)- and Cu(II)-induced non-fibrillar aggregates of amyloid-β (1–42) peptide are transformed to amyloid fibrils, both spontaneously and under the influence of metal chelators. J. Neurochem. 110, 1784–1795 (2009). https://doi.org/10.1111/j.1471-4159.2009.06269.x
J. Mutter, A. Curth, J. Naumann, R. Deth, H. Walach, Does inorganic mercury play a role in Alzheimer’s disease? A systematic review and an integrated molecular mechanism. J. Alzheimer’s Dis. 22, 357–374 (2010). https://doi.org/10.3233/JAD-2010-100705
T. Sanders, Y. Liu, V. Buchner, P.B. Tchounwou, Neurotoxic effects and biomarkers of lead exposure: a review. Rev. Environ. Health. 24, 15–45 (2009). https://doi.org/10.1515/REVEH.2009.24.1.15
T.W. Clarkson, L. Magos, G.J. Myers, The toxicology of mercury—current exposures and clinical manifestations. N. Engl. J. Med. 349, 1731–1737 (2003). https://doi.org/10.1056/NEJMra022471
M.R. Basha, W. Wei, S.A. Bakheet, N. Benitez, H.K. Siddiqi, Y.W. Ge, D.K. Lahiri, N.H. Zawia, The fetal basis of amyloidogenesis: exposure to lead and latent overexpression of amyloid precursor protein and β-amyloid in the aging brain. J. Neurosci. 25, 823–829 (2005). https://doi.org/10.1523/JNEUROSCI.4335-04.2005
J. Wu, M.R. Basha, B. Brock, D.P. Cox, F. Cardozo-Pelaez, C.A. McPherson, J. Harry, D.C. Rice, B. Maloney, D. Chen, D.K. Lahiri, N.H. Zawia, Alzheimer’s Disease (AD)-like pathology in aged monkeys after infantile exposure to environmental metal lead (Pb): evidence for a developmental origin and environmental link for AD. J. Neurosci. 28, 3–9 (2008). https://doi.org/10.1523/JNEUROSCI.4405-07.2008
S.W. Bihaqi, Early life exposure to lead (Pb) and changes in DNA methylation: relevance to Alzheimer’s disease. Rev. Environ. Health. (2019). https://doi.org/10.1515/reveh-2018-0076
L.H. Mason, J.P. Harp, D.Y. Han, Pb neurotoxicity: Neuropsychological effects of lead toxicity. Biomed. Res. Int. 2014, 840547 (2014). https://doi.org/10.1155/2014/840547
H. Gu, P.R. Territo, S.A. Persohn, A.A. Bedwell, K. Eldridge, R. Speedy, Z. Chen, W. Zheng, Y. Du, Evaluation of chronic lead effects in the blood brain barrier system by DCE-CT. J. Trace Elem. Med. Biol. 62, 126648 (2020). https://doi.org/10.1016/j.jtemb.2020.126648
X. Shen, L. Xia, L. Liu, H. Jiang, J. Shannahan, Y. Du, W. Zheng, Altered clearance of beta-amyloid from the cerebrospinal fluid following subchronic lead exposure in rats: Roles of RAGE and LRP1 in the choroid plexus. J. Trace Elem. Med. Biol. 61, 126520 (2020). https://doi.org/10.1016/j.jtemb.2020.126520
D.J. Hare, N.G. Faux, B.R. Roberts, I. Volitakis, R.N. Martins, A.I. Bush, Lead and manganese levels in serum and erythrocytes in Alzheimer’s disease and mild cognitive impairment: results from the Australian Imaging, biomarkers and lifestyle Flagship study of ageing. Metallomics (2016). https://doi.org/10.1039/c6mt00019c
L. Xu, W. Zhang, X. Liu, C. Zhang, P. Wang, X. Zhao, Circulatory levels of toxic metals (aluminum, cadmium, mercury, lead) in patients with Alzheimer’s disease: a quantitative meta-analysis and systematic review. J. Alzheimer’s Dis. 62, 361–372 (2018). https://doi.org/10.3233/JAD-170811
B.R. Roberts, T.M. Ryan, A.I. Bush, C.L. Masters, J.A. Duce, The role of metallobiology and amyloid-β peptides in Alzheimer’s disease. J. Neurochem. 120, 149–166 (2012). https://doi.org/10.1111/j.1471-4159.2011.07500.x
C. Wallin, M. Friedemann, S.B. Sholts, A. Noormägi, T. Svantesson, J. Jarvet, P.M. Roos, P. Palumaa, A. Gräslund, S.K.T.S. Wärmländer, Mercury and alzheimer’s disease: Hg(II) ions display specific binding to the amyloid-β peptide and hinder its fibrillization. Biomolecules. 10, 44 (2020). https://doi.org/10.3390/biom10010044
D. Meleleo, G. Notarachille, V. Mangini, F. Arnesano, Concentration-dependent effects of mercury and lead on Aβ42: possible implications for Alzheimer’s disease. Eur. Biophys. J. 48, 173–187 (2019). https://doi.org/10.1007/s00249-018-1344-9
D.A. Geier, J.K. Kern, K.G. Homme, M.R. Geier, A cross-sectional study of blood ethylmercury levels and cognitive decline among older adults and the elderly in the United States. J. Alzheimer’s Dis. 72, 901–910 (2019). https://doi.org/10.3233/JAD-190894
G. Bjørklund, A.A. Tinkov, M. Dadar, M.M. Rahman, S. Chirumbolo, A.V. Skalny, M.G. Skalnaya, B.E. Haley, O.P. Ajsuvakova, J. Aaseth, Insights into the Potential Role of Mercury in Alzheimer’s Disease. J. Mol. Neurosci. 67, 511–533 (2019). https://doi.org/10.1007/s12031-019-01274-3
G. Bjørklund, B. Hilt, M. Dadar, U. Lindh, J. Aaseth, Neurotoxic effects of mercury exposure in dental personnel. Basic Clin. Pharmacol. Toxicol. 124, 568–574 (2019). https://doi.org/10.1111/bcpt.13199
N. Nagpal, S.S. Bettiol, A. Isham, H. Hoang, L.A. Crocombe, A review of mercury exposure and health of dental personnel. Saf. Health Work. 8, 1–10 (2017). https://doi.org/10.1016/j.shaw.2016.05.007
N. Attiya, R. Fattahi, A. El-Haidani, N. Lahrach, M.Y. Amarouch, Y. Filali-Zegzouti, Mercury exposure and dentists’ health status in two regions of centrall Morocco: Descriptive cross-sectional survey. Pan Afr. Med. J. 36, 1–13 (2020). https://doi.org/10.11604/pamj.2020.36.110.19623
N. Mikhailichenko, K. Yagami, J.Y. Chiou, J.Y. Huang, Y.H. Wang, J.C.C. Wei, T.J. Lai, Exposure to dental filling materials and the risk of dementia: a population-based nested case control study in Taiwan. Int. J. Environ. Res. Public Health. 16, 3283 (2019). https://doi.org/10.3390/ijerph16183283
R. Siblerud, J. Mutter, E. Moore, J. Naumann, H. Walach, A hypothesis and evidence that mercury may be an etiological factor in alzheimer’s disease. Int. J. Environ. Res. Public Health. 16, 5152 (2019). https://doi.org/10.3390/ijerph16245152
B.A. Racette, M. Aschner, T.R. Guilarte, U. Dydak, S.R. Criswell, W. Zheng, Pathophysiology of manganese-associated neurotoxicity. Neurotoxicology. 33, 881–886 (2012). https://doi.org/10.1016/j.neuro.2011.12.010
A.W. Dobson, K.M. Erikson, M. Aschner, Manganese neurotoxicity. Ann. N. Y. Acad. Sci. 1012, 115–128 (2004). https://doi.org/10.1196/annals.1306.009
M.A. Verity, Manganese neurotoxicity: a mechanistic hypothesis. Neurotoxicology. 20, 489–497 (1999)
K. Du, M. Liu, Y. Pan, X. Zhong, M. Wei, Association of serum manganese levels with Alzheimer’s disease and mild cognitive impairment: a systematic review and meta-analysis. Nutrients. 9, 231 (2017). https://doi.org/10.3390/nu9030231
L. Gerhardsson, T. Lundh, L. Minthon, E. Londos, Metal concentrations in plasma and cerebrospinal fluid in patients with Alzheimer’s disease. Dement. Geriatr. Cogn. Disord. 25, 508–515 (2008). https://doi.org/10.1159/000129365
I.M. Balmu, S.A. Strungaru, A. Ciobica, M.N. Nicoara, R. Dobrin, G. Plavan, C. Tefǎnescu, Preliminary data on the interaction between some biometals and oxidative stress status in mild cognitive impairment and Alzheimer’s disease patients. Oxid. Med. Cell. Longev. 2017, 7156928 (2017). https://doi.org/10.1155/2017/7156928
D.B. Milne, R.L. Sims, N.V.C. Ralston, Manganese content of the cellular components of blood. Clin. Chem. 36, 450–452 (1990). https://doi.org/10.1093/clinchem/36.3.450
Y. Tong, H. Yang, X. Tian, H. Wang, T. Zhou, S. Zhang, J. Yu, T. Zhang, D. Fan, X. Guo, T. Tabira, F. Kong, Z. Chen, W. Xiao, D. Chui, High manganese, a risk for Alzheimer’s disease: high manganese induces amyloid-β related cognitive impairment. J. Alzheimer’s Dis. 42, 865–878 (2014). https://doi.org/10.3233/JAD-140534
D. Gandhi, S. Sivanesan, K. Kannan, Manganese-induced neurotoxicity and alterations in gene expression in human neuroblastoma SH-SY5Y cells. Biol. Trace Elem. Res. 183, 245–253 (2018). https://doi.org/10.1007/s12011-017-1153-5
V. Venkataramani, T.R. Doeppner, D. Willkommen, C.M. Cahill, Y. Xin, G. Ye, Y. Liu, A. Southon, A. Aron, H.Y. Au-Yeung, X. Huang, D.K. Lahiri, F. Wang, A.I. Bush, G.G. Wulf, P. Ströbel, B. Michalke, J.T. Rogers, Manganese causes neurotoxic iron accumulation via translational repression of amyloid precursor protein and H-Ferritin. J. Neurochem. 147, 831–848 (2018). https://doi.org/10.1111/jnc.14580
A.C. Martins, P. Morcillo, O.M. Ijomone, V. Venkataramani, F.E. Harrison, E. Lee, A.B. Bowman, M. Aschner, New insights on the role of manganese in alzheimer’s disease and parkinson’s disease. Int. J. Environ. Res. Public Health. 16, 3546 (2019). https://doi.org/10.3390/ijerph16193546
H. Vural, H. Demirin, Y. Kara, I. Eren, N. Delibas, Alterations of plasma magnesium, copper, zinc, iron and selenium concentrations and some related erythrocyte antioxidant enzyme activities in patients with Alzheimer’s disease. J. Trace Elem. Med. Biol. 24, 169–173 (2010). https://doi.org/10.1016/j.jtemb.2010.02.002
A.E. Çilliler, Ş Öztürk, Ş Özbakır, Serum magnesium level and clinical deterioration in Alzheimer’s disease. Gerontology. 53, 419–422 (2007). https://doi.org/10.1159/000110873
E. Andrási, S. Igaz, Z. Molnár, S. Makó, Disturbances of magnesium concentrations in various brain areas in Alzheimer’s disease. Magnes. Res. 13, 189–196 (2000)
E. Andrási, N. Páli, Z. Molnár, S. Kösel, Brain aluminum, magnesium and phosphorus contents of control and Alzheimer-diseased patients. J. Alzheimer’s Dis. 7, 273–284 (2005). https://doi.org/10.3233/JAD-2005-7402
N. Veronese, A. Zurlo, M. Solmi, C. Luchini, C. Trevisan, G. Bano, E. Manzato, G. Sergi, R. Rylander, Magnesium status in Alzheimer’s disease: a systematic review. Am. J. Alzheimers. Dis. Other Demen. 31, 208–213 (2016). https://doi.org/10.1177/1533317515602674
G. Liu, J.G. Weinger, Z.L. Lu, F. Xue, S. Sadeghpour, Efficacy and safety of MMFS-01, a synapse density enhancer, for treating cognitive impairment in older adults: a randomized, double-blind, placebo-controlled trial. J. Alzheimer’s Dis. 49, 971–990 (2015). https://doi.org/10.3233/JAD-150538
B.C.T. Kieboom, S. Licher, F.J. Wolters, M.K. Ikram, E.J. Hoorn, R. Zietse, B.H. Stricker, M.A. Ikram, Serum magnesium is associated with the risk of dementia. Neurology. 89, 1716–1722 (2017). https://doi.org/10.1212/WNL.0000000000004517
X. Zhu, A.R. Borenstein, Y. Zheng, W. Zhang, D.L. Seidner, R. Ness, H.J. Murff, B. Li, M.J. Shrubsole, C. Yu, L. Hou, Q. Dai, Ca: Mg ratio, APOE cytosine modifications, and cognitive function: results from a randomized trial. J. Alzheimer’s Dis. 75, 85–98 (2020). https://doi.org/10.3233/jad-191223
J. Liu, W. Zhao, E.B. Ware, S.T. Turner, T.H. Mosley, J.A. Smith, DNA methylation in the APOE genomic region is associated with cognitive function in African Americans. BMC Med. Genom. 11, 43 (2018). https://doi.org/10.1186/s12920-018-0363-9
B. Wu, H. Cai, S. Tang, Y. Xu, Q. Shi, L. Wei, L. Meng, N. Zhang, X. Wang, D. Xiao, Y. Zou, X. Yang, X. Li, C. Lu, Methionine-mediated protein phosphatase 2A catalytic subunit (PP2Ac) methylation ameliorates the tauopathy induced by manganese in cell and animal models. Neurotherapeutics. (2020). https://doi.org/10.1007/s13311-020-00930-6
D. Zhu, J. You, N. Zhao, H. Xu, Magnesium regulates endothelial barrier functions through TRPM7, MagT1, and S1P1. Adv. Sci. 6, 1901166 (2019). https://doi.org/10.1002/advs.201901166
C. Smorgon, E. Mari, A.R. Atti, E. Dalla Nora, P.F. Zamboni, F. Calzoni, A. Passaro, R. Fellin, Trace elements and cognitive impairment: an elderly cohort study. Arch. Gerontol. Geriatr. 9, 393–402 (2004). https://doi.org/10.1016/j.archger.2004.04.050
J. Siuda, A. Gorzkowska, M. Patalong-Ogiewa, E. Krzystanek, E. Czech, B. Wiechuła, W. Garczorz, A. Danch, B. Jasińska-Myga, G. Opala, From mild cognitive impairment to Alzheimer’s disease—Influence of homocysteine, vitamin B 12 and folate on cognition over time: Results from one-year follow-up. Neurol. Neurochir. Pol. 43, 321–329 (2009)
C.I. Prodan, L.D. Cowan, J.A. Stoner, E.D. Ross, Cumulative incidence of vitamin B12 deficiency in patients with Alzheimer disease. J. Neurol. Sci. 284, 144–148 (2009). https://doi.org/10.1016/j.jns.2009.05.005
C. Guan, R. Dang, Y. Cui, L. Liu, X. Chen, X. Wang, J. Zhu, D. Li, J. Li, D. Wang, Characterization of plasma metal profiles in Alzheimer’s disease using multivariate statistical analysis. PLoS ONE 12, e0178271 (2017). https://doi.org/10.1371/journal.pone.0178271
S. Rafiee, K. Asadollahi, G. Riazi, S. Ahmadian, A.A. Saboury, Vitamin B12 inhibits tau fibrillization via binding to cysteine residues of tau. ACS Chem. Neurosci. 8, 2676–2682 (2017). https://doi.org/10.1021/acschemneuro.7b00230
N.V. Gorantla, E. Balaraman, S. Chinnathambi, Cobalt-based metal complexes prevent repeat tau aggregation and nontoxic to neuronal cells. Int. J. Biol. Macromol. 152, 171–179 (2020). https://doi.org/10.1016/j.ijbiomac.2020.02.278
K.F. Roberts, C.R. Brue, A. Preston, D. Baxter, E. Herzog, E. Varelas, T.J. Meade, Cobalt(III) Schiff base complexes stabilize non-fibrillar amyloid-β aggregates with reduced toxicity. J. Inorg. Biochem. 213, 111265 (2020). https://doi.org/10.1016/j.jinorgbio.2020.111265
E.A. Bajema, K.F. Roberts, T.J. Meade, Cobalt-schiff base complexes: preclinical research and potential therapeutic uses. Met. Ions Life Sci. NLM (Medline) (2019). https://doi.org/10.1515/9783110527872-017
A.H. Smith, P.A. Lopipero, M.N. Bates, C.M. Steinmaus, Arsenic epidemiology and drinking water standards. Science 296, 2145–2146 (2002). https://doi.org/10.1126/science.1072896
S.S. Tao, P.M. Bolger, Dietary arsenic intakes in the United States: FDA total diet study, September 1991-December 1996. Food Addit. Contam. 16, 465–472 (1999). https://doi.org/10.1080/026520399283759
L. Baum, I.H.S. Chan, S.K.K. Cheung, W.B. Goggins, V. Mok, L. Lam, V. Leung, E. Hui, C. Ng, J. Woo, H.F.K. Chiu, B.C.Y. Zee, W. Cheng, M.H. Chan, S. Szeto, V. Lui, J. Tsoh, A.I. Bush, C.W.K. Lam, T. Kwok, Serum zinc is decreased in Alzheimer’s disease and serum arsenic correlates positively with cognitive ability. Biometals 23, 173–179 (2010). https://doi.org/10.1007/s10534-009-9277-5
B.I. Giasson, D.M. Sampathu, C.A. Wilson, V. Vogelsberg-Ragaglia, W.E. Mushynski, V.M.Y. Lee, The environmental toxin arsenite induces tau hyperphosphorylation. Biochemistry 41, 15376–15387 (2002). https://doi.org/10.1021/bi026813c
N.N. Dewji, C. Do, R.M. Bayney, Transcriptional activation of Alzheimer’s β-amyloid precursor protein gene by stress. Mol. Brain Res. 33, 245–253 (1995). https://doi.org/10.1016/0169-328X(95)00131-B
S. Zarazúa, S. Bürger, J.M. Delgado, M.E. Jiménez-Capdeville, R. Schliebs, Arsenic affects expression and processing of amyloid precursor protein (APP) in primary neuronal cells overexpressing the Swedish mutation of human APP. Int. J. Dev. Neurosci. 29, 389–396 (2011). https://doi.org/10.1016/j.ijdevneu.2011.03.004
S. Gharibzadeh, S.S. Hoseini, Arsenic exposure may be a risk factor for alzheimer’s disease. J. Neuropsychiatry Clin. Neurosci. 20, 501 (2008). https://doi.org/10.1176/jnp.2008.20.4.501
X.L. Li, R.Q. Zhan, W. Zheng, H. Jiang, D.F. Zhang, X.L. Shen, Positive association between soil arsenic concentration and mortality from alzheimer’s disease in mainland China. J. Trace Elem. Med. Biol. 59, 126452 (2020). https://doi.org/10.1016/j.jtemb.2020.126452
M. Edwards, L. Johnson, C. Mauer, R. Barber, J. Hall, S. Obryant, Regional specific groundwater arsenic levels and neuropsychological functioning: a cross-sectional study. Int. J. Environ. Health Res. 24, 546–557 (2014). https://doi.org/10.1080/09603123.2014.883591
S.E. O’Bryant, M. Edwards, C.V. Menon, G. Gong, R. Barber, Long-term low-level arsenic exposure is associated with poorer neuropsychological functioning: a project FRONTIER study. Int. J. Environ. Res. Public Health. 8, 861–874 (2011). https://doi.org/10.3390/ijerph8030861
S. Alboghobeish, M. Pashmforosh, L. Zeidooni, A. Samimi, M. Rezaei, High fat diet deteriorates the memory impairment induced by arsenic in mice: a sub chronic in vivo study. Metab. Brain Dis. 34, 1595–1606 (2019). https://doi.org/10.1007/s11011-019-00467-4
N. Medda, R. Patra, T.K. Ghosh, S. Maiti, Neurotoxic mechanism of arsenic: synergistic effect of mitochondrial instability, oxidative stress, and hormonal-neurotransmitter impairment. Biol. Trace Elem. Res. 198, 8–15 (2020). https://doi.org/10.1007/s12011-020-02044-8
Y.-W. Yang, S.-H. Liou, Y.-M. Hsueh, W.-S. Lyu, C.-S. Liu, H.-J. Liu, M.-C. Chung, P.-H. Hung, C.-J. Chung, Risk of Alzheimer’s disease with metal concentrations in whole blood and urine: a case–control study using propensity score matching. Toxicol. Appl. Pharmacol. 356, 8–14 (2018). https://doi.org/10.1016/j.taap.2018.07.015
C. Garza-Lombó, A. Pappa, M.I. Panayiotidis, M.E. Gonsebatt, R. Franco, Arsenic-induced neurotoxicity: a mechanistic appraisal. J. Biol. Inorg. Chem. 24, 1305–1316 (2019). https://doi.org/10.1007/s00775-019-01740-8
S. Satarug, D.A. Vesey, G.C. Gobe, Health risk assessment of dietary cadmium intake: do current guidelines indicate how much is safe? Environ. Health Perspect. 125, 284–288 (2017). https://doi.org/10.1289/EHP108
K.M. Bakulski, Y.A. Seo, R.C. Hickman, D. Brandt, H.S. Vadari, H. Hu, S.K. Park, Heavy metals exposure and Alzheimer’s disease and related dementias. J. Alzheimers. Dis. 76, 1215–1242 (2020). https://doi.org/10.3233/JAD-200282
H. Li, Z. Wang, Z. Fu, M. Yan, N. Wu, H. Wu, P. Yin, Associations between blood cadmium levels and cognitive function in a cross-sectional study of US adults aged 60 years or older. BMJ Open. 8, e020533 (2018). https://doi.org/10.1136/bmjopen-2017-020533
J.Y. Min, K.B. Min, Blood cadmium levels and Alzheimer’s disease mortality risk in older US adults. Environ. Heal. A Glob. Access Sci. Source. 15, 69 (2016). https://doi.org/10.1186/s12940-016-0155-7
J.R. Bondier, G. Michel, A. Propper, P.M. Badot, Harmful effects of cadmium on olfactory system in mice. Inhal. Toxicol. 20, 1169–1177 (2008). https://doi.org/10.1080/08958370802207292
J.J.V. Branca, M. Maresca, G. Morucci, T. Mello, M. Becatti, L. Pazzagli, I. Colzi, C. Gonnelli, D. Carrino, F. Paternostro, C. Nicoletti, C. Ghelardini, M. Gulisano, L.D.C. Mannelli, A. Pacini, Effects of cadmium on ZO-1 tight junction integrity of the blood brain barrier. Int. J. Mol. Sci. 20, 6010 (2019). https://doi.org/10.3390/ijms20236010
M. Forcella, P. Lau, M. Oldani, P. Melchioretto, A. Bogni, L. Gribaldo, P. Fusi, C. Urani, Neuronal specific and non-specific responses to cadmium possibly involved in neurodegeneration: a toxicogenomics study in a human neuronal cell model. Neurotoxicology. 76, 162–173 (2020). https://doi.org/10.1016/j.neuro.2019.11.002
T.M. Frisoli, R.E. Schmieder, T. Grodzicki, F.H. Messerli, Salt and hypertension: Is salt dietary reduction worth the effort? Am. J. Med. 125, 433–439 (2012). https://doi.org/10.1016/j.amjmed.2011.10.023
D. Mohan, K.H. Yap, D. Reidpath, Y.C. Soh, A. McGrattan, B.C.M. Stephan, L. Robinson, N. Chaiyakunapruk, M. Siervo, Link between dietary sodium intake, cognitive function, and dementia risk in middle-aged and older adults: a systematic review. J. Alzheimers. Dis. 76, 1347–1373 (2020). https://doi.org/10.3233/JAD-191339
E. Koseoglu, R. Koseoglu, M. Kendirci, R. Saraymen, B. Saraymen, Trace metal concentrations in hair and nails from Alzheimer’s disease patients: Relations with clinical severity. J. Trace Elem. Med. Biol. 39, 124–128 (2017). https://doi.org/10.1016/j.jtemb.2016.09.002
K. Higuchi, T. Sato, Y.D. Bhutia, V. Ganapathy, Involvement of a Na+-coupled oligopeptide transport system for β-amyloid peptide (Aβ1–42) in brain cells. Pharm. Res. 37, 98 (2020). https://doi.org/10.1007/s11095-020-02835-7
G. Faraco, K. Hochrainer, S.G. Segarra, S. Schaeffer, M.M. Santisteban, A. Menon, H. Jiang, D.M. Holtzman, J. Anrather, C. Iadecola, Dietary salt promotes cognitive impairment through tau phosphorylation. Nature 574, 686–690 (2019). https://doi.org/10.1038/s41586-019-1688-z
G. Paglia, O. Miedico, A. Cristofano, M. Vitale, A. Angiolillo, A.E. Chiaravalle, G. Corso, A. Di Costanzo, Distinctive pattern of serum elements during the progression of Alzheimer’s disease. Sci. Rep. 6, 22769 (2016). https://doi.org/10.1038/srep22769
B.R. Roberts, J.D. Doecke, A. Rembach, L.F. Yévenes, C.J. Fowler, C.A. McLean, M. Lind, I. Volitakis, C.L. Masters, A.I. Bush, D.J. Hare, Rubidium and potassium levels are altered in Alzheimer’s disease brain and blood but not in cerebrospinal fluid. Acta Neuropathol. Commun. 4, 119 (2016). https://doi.org/10.1186/s40478-016-0390-8
K. Schofield, The metal neurotoxins: an important role in current human neural epidemics? Int. J. Environ. Res. Public Health. 14, 1511 (2017). https://doi.org/10.3390/ijerph14121511
C.E. Cicero, G. Mostile, R. Vasta, V. Rapisarda, S.S. Signorelli, M. Ferrante, M. Zappia, A. Nicoletti, Metals and neurodegenerative diseases. A systematic review. Environ. Res. 159, 82–94 (2017). https://doi.org/10.1016/j.envres.2017.07.048
Acknowledgments
The authors would like to thank the Vice Chancellor for Research and Technology, Kermanshah University of Medical Sciences, for providing suitable conditions to conduct this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
It is declared that we do not have any conflicts of interest regarding the present study.
Rights and permissions
About this article
Cite this article
Bagheri, S., Saboury, A.A. What role do metals play in Alzheimer's disease?. J IRAN CHEM SOC 18, 2199–2213 (2021). https://doi.org/10.1007/s13738-021-02181-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13738-021-02181-4