Abstract
We conducted a systematic review of the literature on the electronic databases Medline, Embase, Ovid and Cochrane to identify studies from 1990 to 2011 regarding the surgical management of non-parasitic liver cysts treated with laparoscopy (LT) and/or laparotomy (OT) to identify short-term and long-term outcomes of the relative treatments. Two reviewers independently extracted data regarding the following parameters: first author, year of publication, type of journal, study design, number of patients operated on, male/female ratio, mean age, mean size of the cysts treated, laparoscopic conversion rate, morbidity, mortality and recurrence in both groups (LT and OT). A qualitative analysis was carried out using the Pearson Chi square test and the Fischer’s exact test where necessary. The data analysis was conducted by dividing the sample into three periods in relation to the development of laparoscopic surgery: period 1 (P1), 1990–1995 “pioneering” period of laparoscopy; period 2 (P2), 1996–2000 period of the “development of laparoscopy”; period 3 (P3), 2001–2011 period of “diffusion of laparoscopy.” Thirty studies involving 948 patients comparing LT with OT were included in the final pooled analysis. Twenty-two studies were retrospective (73.3 %) and only 8 (26.7 %) were prospective. The number of publications increased during the three periods analysed. The correlation between the type of journal and the year of publication showed an increase (p = 0.048) in journals dedicated to LT during the three periods. In P1, the preferred approach was open surgery (66.3 %) with only 11 cases treated with LT. The conversion rate was 18.1 %. The overall complication rate was 33.3 % with a substantial equivalence between the two approaches (27.2 % for laparoscopic surgery and 36.6 % for laparotomic). The overall recurrence rate was 18.1 % with 36.3 % in the laparoscopic group and 9.2 % in the laparotomic group. In P2, the preferred approach was laparoscopic (56.7 %). The conversion rate was 2.3 %. The overall complication rate was 5.8 % but with some differences between the two approaches (10.3 % for the laparoscopic approach and 0 % for open surgery). The overall recurrence rate was 14.4 % with 17.4 % in the laparoscopic group and 10.4 % in the laparotomic group. In P3, the preferred approach was laparoscopic (69.9 %). The overall recurrence rate was 11.1 %; it was 6.1 % for the laparoscopic approach while it was 11.5 % for laparotomic. In all three periods analysed, the laparoscopic approach showed a statistically significant reduction in operative time (p = 0.009) and hospital stay (p = 0.001) and a significant (p < 0.05) reduction rate in symptomatic recurrences in patients with polycystic liver disease (25 %) as compared with simple liver cysts (7.5 %). The current data in the literature show that the laparoscopic approach may be the treatment of choice in patients with symptomatic non-parasitic cysts of the liver, providing the short-term advantages of minimally invasive surgery. Recurrence rates were acceptable and comparable to those of conventional surgery. Long-term outcomes should be verified by additional randomised controlled trials and long-term follow-ups.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Non-parasitic cysts constitute the most common pathology found in the liver having a prevalence ranging from 2.5 to 5 % in the general population [1]. In the past 20 years, the widespread use of first and second level imaging studies, such as ultrasound (US) and computed tomography (CT) abdomen, has led to an increase up to 18 % in the prevalence of these lesions [2]. On the basis of embryological origin and relationship with the biliary system, non-parasitic hepatic cysts are classified as simple liver cysts (SLCs) which represent the most common form, polycystic liver disease (PLD), congenital liver cystic ectasia, ciliated hepatic foregut cysts, biliary cyst tumours (cystadenoma, biliary benign cystoadenoma (BCA), and biliary cystadenocarcinoma (BCAC)) and inflammatory and traumatic cysts [3]. Non-parasitic hepatic cysts can be treated surgically when symptomatic, when there is the suspicion of a neoplastic origin or when complicated. Various treatment procedures have been proposed, such as a simple US or CT-guided aspiration, injection of sclerosing agents, fenestration, enucleation, hepatic resection and transplantation [4, 5]. The recent development of laparoscopic surgery and the short-term benefits associated with it (reduced hospitalisation, better cosmetic results and quicker return to normal activities) has produced an increase in resection or fenestration in recent years. However, some authors have described a higher rate of recurrence after using the laparoscopic approach, up to 44 % [6, 7]. The purpose of this study was to compare the short- and long-term results in the surgical treatment of hepatic cysts using laparoscopy (LT) and laparotomy (OT) by means of a systematic review of the literature.
Methods
The research was conducted on the electronic databases Medline, Embase, Ovid and Cochrane to identify all studies regarding the surgical treatment of non-parasitic hepatic cysts using LT and/or OT.
The following Mesh search headings were used:“laparoscopy”, “open fenestration”, “non-parasitic hepatic cysts” and “surgery” and their combinations; similar headings were also searched such as “laparoscopic fenestration”, “laparoscopic resection” and “minimally invasive surgery”. Abstracts, letters to the editor, case reports and articles in languages other than English were excluded. The research was completed June 1, 2011.
Subsequently, two reviewers (RC and BS) independently extracted data regarding the following parameters: first author, year of publication, type of journal, study design, number of patients operated on, male/female ratio, average age, average size of the treated cysts, laparoscopic conversion rate, complications, deaths in the postoperative follow-up period and number of recurrences. At the end of the data extraction, a 100 % agreement between the two reviewers was present.
Only the studies reporting more than five procedures in patients with cystic lesions of the liver, such as SLCs, PLD, BCAs and BCACs; those which clearly reported at least one of the results of the above parameters in patients treated surgically for hepatic cysts, those which clearly reported the indications for surgery and those which documented the technique used (OT and/or LT) were considered. When two studies had been published by the same author and/or by the same institution, the most recent study or that of the highest quality was included.
Studies were excluded from the analysis if the data were related exclusively to parasitic lesions, inflammatory or traumatic liver or congenital/cystic biliary ectasia, or if at least one of the outcomes of interest was not clearly reported, although it was impossible to extract or calculate the data of interest (mixed case studies where there were non-parasitic cystic lesions together with others) in data published before 1990.
A qualitative analysis was carried out using the Pearson Chi square test and the Fischer’s exact test where necessary. The data analysis was carried out by dividing the sample into three periods in relation to the development of laparoscopic surgery (P1: “pioneering” period of laparoscopy; P2: period of the “development of laparoscopy” and P3: period of the “diffusion of laparoscopy.” Data relating to discrete variables were reported as percentages and data relating to continuous variables as a weighted average.
Results
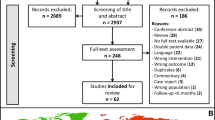
The preliminary qualitative analysis was conducted on 30 [4, 6–32] selected studies, all published between 1990 and 2011 and data of 948 patients were analysed. Twenty-two studies were retrospective (73.3 %) and only 8 (26.7 %) were prospective. None of the prospective studies provided any kind of randomisation. Only five studies (16.6 %) were comparative (two retrospective and three prospective) and only two of these had a proper “matching” of the groups compared. When comparing the number of publications regarding hepatic cysts an increase in the number of publications was evident in the periods 1990–1995 (P1), 1996–2000 (P2) and 2001–2011 (P3). The 30 publications were distributed as follows: P1, 3/30 (10 %); P2, 8/30 (26.7 %), 19/30 (63.3 %).
The correlation between the type of journal and the year of publication showed a statistically significant increase (p = 0.048) in the number of publications in journals devoted to LT during the three periods (P1: 0–12.5 %, P2–P3: 26.3 %) as compared to journals dedicated to liver surgery (P1: 66.7 %, P2: 12.5 %, P3:16.5 %). It also noted an increase in the percentage of prospective studies in the three periods considered (P1: 0 %, P2: 12.5 %, P3: 36.8 %) with a trend toward statistical significance (p = 0.098). Finally, the number of comparative studies also increased in relation to the period considered (0 % in P1 and P2, 26 % in P3) with a trend to statistical significance (p = 0.093).
Analysis of samples per period
Period 1990–1995 (P1)
Three publications [4, 8, 9] suitable for the study were identified with a total of 33 patients (Tables 1, 2). All the studies were retrospective without comparison between laparoscopic and open surgery; their median impact factor was 1.6 (range 0.6–7.5) with a median citation rate of 21 citations (range 0–93). The average age of the patients was 54.4 years, with a male/female ratio of 0.2. The indication for surgery was the presence of symptomatic cysts in all cases. The pathology most commonly treated was SLCs (54.4 %). No cases of BCAs and BCACs were identified. The average size of the hepatic cysts was 12.1 cm. The preferred approach was open surgery (66.3 %). Only one study [4] reported 11 cases treated with LT (in all cases a fenestration of the cyst was performed). The conversion rate was 18.1 %. All patients with PLD were converted. The overall complication rate was 33.3 % with a substantial equivalence between the two approaches (27.2 % for LT and 36.6 % for open surgery; p = 0.60). The overall recurrence rate was 18.1 %. It was 36.6 % in the laparoscopic surgical group and 9.2 % for traditional surgery (p = 0.07).
Period 1995–2000 (P2)
Eight publications [10–17] suitable for the study were identified with a total of 222 patients (Tables 3, 4). Seven studies were retrospective and one was prospective; the median impact factro was 3.4 (range 0–7.5) with a median citation rate of 43 citations (range 10–164). The average age of the patients was 56.2 years with a male/female ratio of 0.25. The indication for surgery was the presence of symptomatic cysts in 95.3 % of cases. In 4.8 % of cases, however, the procedure was performed as the result of an incidental finding in the course of other surgical procedures. The diseases treated were: 58.6 % SLCs, 40.5 % PLD and 0.9 % BCAs. The average size of the hepatic cysts treated was 11.4 cm. The preferred approach was laparoscopic (56.7 %). The conversion rate was 2.3 %, and two out of three (66.6 %) patients with PLD were converted to open surgery. In the laparoscopic group two types of intervention were performed: deroofing in 55 % of cases and fenestration in 45 %. The laparotomic group of interventions included 61.4 % fenestrations, 17.1 % resections and deroofing and 3.1 % cystojejunostomies. The overall complication rate was 5.8 % but with some differences between the two approaches (10.3 % for the laparoscopic approach and 0 % for laparotomic surgery; p = 0.03). The overall recurrence rate was 14.4 %; in the case of a laparoscopic approach, it was 17.4 % while it was 10.4 % for conventional surgery (p = 0.14). Of all of the BCAs treated, 17 experienced a recurrence and in 50 % of cases, at the time of recurrence, a BCAC was observed. Instead, in the laparotomic group no recurrence was observed in the cases of resection, but it was frequently associated with PLD (70 %).
Period 2001–2011 (P3)
Nineteen publications [6, 18–35] suitable for the study were identified with a total of 693 patients (Tables 5, 6). Twelve studies were retrospective (63.1 %) and seven were prospective (36.9 %); five studies (26.3 %) were comparative but only two had proper patient matching. The median impact factor of the studies was 2.1 (range 0–4.5), with a median citation rate of 17 citations (range 1–79). The average age of the patients was 56.5 years, with a male/female ratio of 0.2. The indication for surgery was the presence of symptomatic cysts in 98.2 % of cases. In 1.8 % of cases, however, the procedure was performed as the result of an incidental finding of SLCs in the course of other surgical procedures. The diseases treated were 81.3 % SLCs, 15.6 % PLD and 3.1 % BCAs/BCACs. The average size of the hepatic cysts treated was 11.5 cm. The preferred approach was laparoscopic (69.9 %). The conversion rate was 5.6 %, most commonly related to the location of the cyst in the posterior-lateral hepatic segment (S7) and less frequently for massive bleeding. In the laparoscopic group, three types of procedures were performed: deroofing (79.6 %), fenestration (20.1 %) and only one case of liver resection (0.3 %). The laparotomic group included 16.2 % fenestrations, 45.3 % deroofing and 24.1 % resections and finally 2.3 % cystojejunostomies. The overall complication rate was 11.1 % with a substantial equivalence between the two approaches (9.7 % for the laparoscopic approach and 12.8 % for open surgery; p = 0.20). The overall recurrence rate was 11.1 %; it was 6.1 % in cases of laparoscopic surgery while it was 11.5 % for conventional surgery (p = 0.01). In the laparoscopic group the recurrence rate was 11.3 and 3.6 % after fenestration and deroofing, respectively. Instead, in the OT group, the recurrence rate was 1.1 % after resection, 18.4 % after deroofing and 35.7 % after fenestration. Recurrence in 75 % of the patients was associated with PLD.
The trend towards the different periods for recurrence and complication rates was then analysed. The overall recurrence rate was similar among the three periods, with no statistical differences between P1 and P2, P2 and P3 or P1 and P3 (p = 0.57, p = 0.19 and p = 0.22, respectively) as were recurrences in the open approach group for the various periods of time (p = 0.85, p = 0.76 and p = 0.74, respectively). On the other hand, when only the recurrence rate of the laparoscopic approach group was considered, it was noted that the rate of recurrence was significantly lower in P3, with 6.1 versus 36.3 % for P1 and 17.4 % for P2 (p = 0.002 and p < 0.001, respectively). No statistical difference was recorded between P1 and P2 (36.3 and 17.4 %, p = 0.088).
Concerning the overall complication rate, a statistical difference was found between P1 and P2 (33.3 and 5.8 %; p < 0.001) as well as for complications in the open approach group (36.6 and 0 %; p < 0.001) while no difference was recorded in the laparoscopic group (27.2 vs. 10.3 %; p = 0.11). In analysing periods P2 and P3, the same scenario was found, with a statistical difference for overall and open approach complications (5.8 and 11.1 %; p = 0.020 and 0 and 12.8 %; p = 0.020, respectively. As before, the complication rate in the laparoscopic group did not differ between P2 and P3 (10.3 and 9.7 %; p = 0.85). Finally, analysing P1 and P3, there was a statistical difference for overall complications (33.3 vs. 11.1 %; p = 0.004) and open approach complications (36.6 vs. 12.8 %; p = 0.004) while no differences were seen in laparoscopic approach complications (27.2 vs. 9.7 %; p = 0.07).
Discussion
A review of the literature on the surgical treatment of hepatic cysts showed the presence of low-quality studies with no randomised studies, few prospective studies (27 %) and only five comparative studies (17 %). Only two comparative studies (7 %) had an adequate “matching” of patients, but they were not homogeneous enough to allow a meta-analysis of the data reported. Overall, however, the studies analysed showed growing interest in the surgical treatment of non-parasitic hepatic cysts. In fact, we observed an increase in the number of patients treated in the three periods considered (P1: n = 33, P2: n = 222, P3: n = 693). This is probably due to the wide diffusion of diagnostic imaging such as US and CT which have allowed the identification of an increasing number of hepatic cysts with an estimated prevalence of 4.5–7 % in the general population. In all three periods considered, the main surgical indication was the presence of symptomatic cysts (P1: 100 %, P2: 95 %, P3: 99 %). The demographic data reported a higher prevalence of cystic disease in females with a ratio of 0.2, and the average age of onset of symptoms was the fifth decade of life. Overall, the presence of single SLCs remained the main indication for surgery with an increase in percentage over the three periods analysed (P1: 54.4 %, P2: 58.6 %, P3: 81.3 %). This is probably due both to the wide diffusion of diagnostic imaging and to the increased development of the minimally invasive approach which could have resulted in an increase in the number of patients undergoing surgery.
The data also confirmed the rarity of BCAs/BCACs with 21 cases out of 948 (2.2 %) patients with an extremely low percentage of malignancy (0.2 %).
However, the number of BCAs removed increased over the three periods (P1: 0 %, P2: 0.9 %, P3: 2.8 %). This finding confirmed an increase in surgical indications in patients with liver cysts rather than a real increase in its incidence. With regard to the approach (laparoscopic vs. open surgery) and the results over the short- and long-term periods, the preliminary qualitative analysis clearly showed a trend toward LT. This was clearly stated comparing the number of studies published in the three periods in different types of journals. In fact, the correlation between the type of journal and the year of publication showed a statistically significant increase (p = 0.048) in the number of publications in journals devoted to laparoscopic surgery during the three periods analysed (P1: 0 %, P2: 12.5 %, P3: 26.3 %). On the contrary, the rate of publications on liver cysts in journals dedicated to liver surgery showed a progressive reduction during the three periods (P1: 66.7 %, P2: 12.5 %, P3: 16.5 %). During the first period (P1: 1990–1995), only 18 % of patients [4] were treated with a minimally invasive approach. These were exclusively simple fenestrations in selected patients; the conversion rate reported was higher (18.8 %) but the overall morbidity was lower than the laparotomic group [8] (27.2 vs. 36 %, respectively).
However, these results should be interpreted with caution; indeed, the two groups of patients considered (laparoscopic/laparotomic) are strongly dishomogeneous due to the different treatments received; the patients in the laparoscopic group were treated only with simple fenestration procedures while one-third of the patients in the laparotomic group underwent liver resection. The percentage of overall recurrence appeared low (18 %) with a higher rate of recurrence in the laparoscopic group as compared to the laparotomic group (37 vs. 9 %, respectively). However, even these data appeared to be influenced more by the type of treatment (simple fenestration) than by the type of approach used (laparoscopic vs. laparotomic) and also by the operative difficulties related to the use of a completely new technique.
During the second period (P2:1996–2000) [10–17], widespread use of the laparoscopic approach (58.6 %) was recorded. Five studies out of a total of eight reported the use of LT (62.5 %). The effect produced by the technological innovation of the instrumentation and the completion of the learning curves in LT was also evident. In fact, the conversion rate was reduced as compared to the previous year (2.3 vs. 18.8 %); the overall morbidity for the laparoscopic approach dropped to 10.3 %, even with an increase in surgical procedure complexity. Deroofing was performed in 55 % of cases and simple fenestration in 45 %. Once again, the comparison between the laparoscopic and the open surgery groups appeared to be affected by heterogeneity mainly due to the poor quality of the studies analysed. The recurrence rate was even higher in the laparoscopic group when compared to the open surgery group (17.4 vs. 10.4 %, respectively). Even in this case, it could be attributed to the higher number of simple fenestrations performed in the laparoscopic group than in the open group.
In fact, in the laparotomic group, no recurrence was observed in cases of resection but it was observed in 70 % of the patients treated for PLD. All cases of BCAs treated laparoscopically experienced a recurrence and, in 50 % of cases, a BCAC was observed at the time of recurrence. However, neither a cytologic examination of the cystic fluid, nor intraoperative biopsies or histopathological examination of the cystic wall was carried out in any of these procedures; this would have allowed proper diagnosis and treatment with complete resection of the cyst. These data are probably related to the widespread diffusion of LT among surgeons who are not experienced in liver surgery. Intraoperative examination of the cystic fluid and the cystic wall is of vital importance due to the well-known malignant evolution of BCAs.
During the third period (P3: 2001–2011) [6, 18–35], almost 70 % of the patients were treated using a laparoscopic approach (Fig. 1). Only one study did not include cases laparoscopically treated while 8/18 studies reported the use of only LT. The conversion rate was 5.6 % and the most common causes were the location of the cyst in the right postero-lateral liver segments and less frequently for bleeding. Compared to the previous period, there was an increased number of laparoscopic deroofings (79.6 vs. 55.5 %, respectively) and resections (0.3 %). The overall complication rate was 33.3 % with substantial equivalence between the two approaches (27.2 % for the laparoscopic approach and 36.6 % for open surgery). The apparent increase in the rate of complications as compared to the previous period can be attributed to improvement in the quality of studies leading to a better extraction of data and to the increased complexity of the laparoscopic procedures performed. The overall recurrence rate was 11.7 %; it was 11.8 % for the laparoscopic approach while it was 14.4 % for conventional surgery. The reduction in the recurrence rate after laparoscopic resection as compared to the previous period could be attributed to the more complex procedures performed (in fact, the number of fenestrations decreases from 45.5 to 20.1 %).
This finding was confirmed by analysis of the recurrence rates related to the procedure performed in P3: 11.3 versus 3.6 % after fenestration and deroofing, respectively. In this period, only three BCAs were treated with laparoscopic resection (0.7 %). The first [31] of the two comparative studies with appropriate patient matching showed the potential benefits of the laparoscopic approach with statistically significant reduction in operative time (p = 0.009) and hospital stay (p = 0.001). Furthermore, the study failed to demonstrate a correlation between the number of cysts, type of procedure (deroofing vs. fenestration) and approach (laparoscopic vs. laparotomic) in relation to the onset of recurrence. The study by Tan et al. [23] confirmed the potential benefits of the laparoscopic approach (lower morbidity and shorter hospital stay). Finally, the study of Lohe et al. [32] showed a significant (p < 0.05) rate of symptomatic recurrences in patients with PLD (25 %) as compared with those having SLCs (7.5 %).
In conclusion, despite the absence of high-quality studies, the data in the literature which were analysed suggested that the laparoscopic approach could be the treatment of choice in patients with non-parasitic liver cysts. Indeed, this approach would ensure the typical advantages of minimally invasive surgery, such as reduced hospital stay and less postoperative pain. The recurrence rates are acceptable and comparable to those of conventional surgery. Recurrence seemed to be associated with the presence of PLD rather than with the type of technique used. Intraoperative histological examination of the cystic wall should always be performed to exclude a BCA/BCAC which requires a resection with clear margins.
References
Caremani M, Vincenti A, Benci A et al (1993) Ecographic epidemiology of non-parasitic hepatic cysts. J Clin Ultrasound 21:115–118
Carrim ZI, Murchison JT (2003) The prevalence of simple renal and hepatic cysts detected by spiral computed tomography. Clin Radiol 58:626–629
Seo JK, Kim SH, Lee SH et al (2010) Appropriate diagnosis of biliary cystic tumors: comparison with atypical hepatic simple cysts. Eur J Gastroenterol Hepatol 22(8):989–996
Morino M, De Giuli M, Festa V et al (1994) Laparoscopic management of symptomatic non parasitic cysts of the liver. Indications and results. Ann Surg. 219:157–164
Starzl TE, Reyes J, Tzakis A et al (1990) Liver transplantation for polycystic liver disease. Arch Surg 125:575–577
Petri A, Höhn J, Makula E et al (2001) Experience with different methods of treatment of nonparasitic liver cysts. Langenbecks Arch Surg 387:229–233
Gigot JF, Legrand M, Hubens G et al (1996) Laparoscopic treatment of nonparasitic liver cysts: adequate selection of patients and surgical technique. World J Surg 20:556–561
Furuta T, Yoshida Y, Saku M et al (1990) Treatment of symptomatic non-parasitic liver cysts—surgical treatment versus alcohol injection therapy. HPB Surg 2:269–277
Henne-Bruns D, Klomp HJ, Kremer B (1993) Non-parasitic liver cysts and polycystic liver disease: results of surgical treatment. Hepatogastroenterology 40(1):1–5
Kabbej M, Sauvanet A, Chauveau D et al (1996) Laparoscopic fenestration in polycystic liver disease. Br J Surg 83(12):1697–1701
Emmermann A, Zornig C, Lloyd DM et al (1997) Laparoscopic treatment of nonparasitic cysts of the liver with omental transposition flap. Surg Endosc 11(7):734–736
Koperna T, Vogl S, Satzinger U et al (1997) Nonparasitic cysts of the liver: results and options of surgical treatment. World J Surg 21(8):850–854
Hansen P, Bhoyrul S, Legha P et al (1997) Laparoscopic treatment of liver cysts. J Gastrointest Surg 1(1):53–59
Kakizaki K, Yamauchi H, Teshima S (1998) Symptomatic liver cyst: special reference to surgical management. J Hepatobiliary Pancreat Surg 5(2):192–195
Martin IJ, McKinley AJ, Currie EJ et al (1998) Tailoring the management of nonparasitic liver cysts. Ann Surg 228(2):167–172
Katkhouda N, Hurwitz M, Gugenheim J et al (1999) Laparoscopic management of benign solid and cystic lesions of the liver. Ann Surg 229(4):460–466
Zalaba Z, Tihanyi TF, Winternitz T et al (1999) The laparoscopic treatment of non-parasitic liver cysts. Five years experience. Acta Chir Hung 38(2):221–223
Hansman MF, Ryan JA Jr, Holmes JH et al (2001) Management and long-term follow-up of hepatic cysts. Am J Surg 181(5):404–410
Regev A, Reddy KR, Berho M et al (2001) Large cystic lesions of the liver in adults: a 15-year experience in a tertiary center. J Am Coll Surg 193(1):36–45
Tocchi A, Mazzoni G, Costa G et al (2002) Symptomatic nonparasitic hepatic cysts: options for and results of surgical management. Arch Surg 137(2):154–158
Pitale A, Bohra AK, Diamond T (2002) Management of symptomatic liver cysts. Ulster Med J 71(2):106–110
Fiamingo P, Tedeschi U, Veroux M et al (2003) Laparoscopic treatment of simple hepatic cysts and polycystic liver disease. Surg Endosc 17(4):623–626 (Epub 2003 Feb 10)
Tan YM, Chung A, Mack P et al (2005) Role of fenestration and resection for symptomatic solitary liver cysts. ANZ J Surg. 75(7):577–580
Kornprat P, Cerwenka H, Bacher H et al (2004) Minimally invasive management of dysontogenetic hepatic cysts. Langenbecks Arch Surg. 389(4):289–292
Szabó LS, Takács I, Arkosy P et al (2006) Laparoscopic treatment of nonparasitic hepatic cysts. Surg Endosc 20(4):595–597
Neri V, Ambrosi A, Fersini A et al (2006) Laparoscopic treatment of biliary hepatic cysts: short- and medium-term results. HPB (Oxford) 8(4):306–310
Palanivelu C, Jani K, Malladi V (2006) Laparoscopic management of benign nonparasitic hepatic cysts: a prospective nonrandomized study. South Med J 99(10):1063–1067
Caetano-Júnior EM, Linhares MM, Matos D et al (2006) Laparoscopic management of hepatic cysts. Surg Laparosc Endosc Percutan Tech. 16(2):68–72
Garcea G, Pattenden CJ, Stephenson J et al (2007) Nine-year single-center experience with nonparastic liver cysts: diagnosis and management. Dig Dis Sci 52(1):185–191
Bai XL, Liang TB, Yu J et al (2007) Long-term results of laparoscopic fenestration for patients with congenital liver cysts. Hepatobiliary Pancreat Dis Int 6(6):600–603
van Keimpema L, Ruurda JP, Ernst MF et al (2008) Laparoscopic fenestration of liver cysts in polycystic liver disease results in a median volume reduction of 12.5 %. J Gastrointest Surg 12(3):477–482
Loehe F, Globke B, Marnoto R et al (2010) Long-term results after surgical treatment of nonparasitic hepatic cysts. Am J Surg 200(1):23–31
Treckmann JW, Paul A, Sgourakis G et al (2010) Surgical treatment of nonparasitic cysts of the liver: open versus laparoscopic treatment. Am J Surg 199(6):776–781
Donati M, Stavrou GA, Wellmann A, Flemming P, Donati A, Oldhafer KJ (2010) Laparoscopic deroofing of hepatic cysts: the most effective treatment option. Clin Ter 161(4):345–348
Gigot JF, Metairie S, Etienne J, Horsmans Y, van Beers BE, Sempoux C, Deprez P, Materne R, Geubel A, Glineur D, Gianello P (2001) The surgical management of congenital liver cysts. Surg Endosc 15(4):357–363
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Antonacci, N., Ricci, C., Taffurelli, G. et al. Systematic review of laparoscopic versus open surgery in the treatment of non-parasitic liver cysts. Updates Surg 66, 231–238 (2014). https://doi.org/10.1007/s13304-014-0270-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-014-0270-3