Abstract
Purpose
The purpose of the study was to investigate the usefulness of quantitative salivary single-photon emission computed tomography/computed tomography (SPECT/CT) using Tc-99m pertechnetate in Sjögren’s syndrome (SS).
Methods
We retrospectively reviewed quantitative salivary SPECT/CT data from 95 xerostomic patients who were classified as either SS (n = 47, male:female = 0:47, age = 54.60 ± 13.16 y [mean ± SD]) or non-SS (n = 48, male:female = 5:43, age = 54.94 ± 14.04 y) by combination of anti-SSA/Ro antibody, labial salivary gland biopsy, unstimulated whole saliva flow rate, and Schirmer’s test. Thyroid cancer patients (n = 43, male:female = 19:24, age = 46.37 ± 12.13 y) before radioactive iodine therapy served as negative controls. Quantitative SPECT/CT was performed pre-stimulatory 20 min and post-stimulatory 40 min after injection of Tc-99m pertechnetate (15 mCi). The %injected dose at 20 min and the %excretion between 20 and 40 min were calculated for parotid and submandibular glands, generating four quantitative parameters: %parotid uptake (%PU), %submandibular uptake (%SU), %parotid excretion (%PE), and %submandibular excretion (%SE). The most useful parameter for SS diagnosis was investigated.
Results
The uptake parameters (%PU and %SU) were significantly different among the SS, non-SS, and negative controls (p = 0.005 for %PU and p < 0.001 for %SU, respectively), but the excretion parameters (%PE and %SE) were not (p > 0.05 for both). The %PU and %SU were significantly lower in SS than in the negative controls and non-SS (p < 0.05 for all pair-wise comparisons). Additionally, the %SU was significantly lower in non-SS than in the negative controls (p < 0.05). Receiver-operating characteristic analysis revealed that the %SU had the greatest area-under-the curve of 0.720 (95% confidence interval = 0.618–0.807). Using the optimal cut-off value of %SU ≤ 0.07%, SS was identified with a sensitivity of 70.21% and a specificity of 70.83%.
Conclusion
Reduced submandibular uptake of Tc-99m pertechnetate at 20 min (%SU) was proved useful for the diagnosis of SS. Quantitative salivary gland SPECT/CT holds promise as an objective imaging modality for assessment of salivary dysfunction and may facilitate accurate classification of SS.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Sjögren’s syndrome (SS) is an autoimmune disease that affects the exocrine glands, such as salivary and lacrimal glands, and can manifest as a primary exocrine gland disease (primary SS) or as concomitant exocrine involvement of other rheumatologic diseases (secondary SS) [1,2,3]. The diagnosis of SS depends on the combination of clinical, laboratory, functional, and histologic assessment of exocrine glands, and salivary gland scintigraphy (SGS) has been used as one of the main diagnostic items for objective salivary involvement of SS [1, 2, 4, 5]. However, the role of SGS for diagnosis of SS has been minimized [3, 6, 7], mainly because of lack of a standardized protocol for SGS [8].
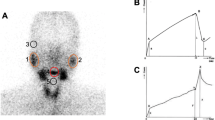
The SGS has been performed in a 2-dimensional planar mode using Tc-99m pertechnetate in patients with xerostomia since the early 1970s [9]. Using multiple static images [10,11,12] or dynamic time–activity curves (TACs) [13,14,15,16,17], the degree of uptake/excretion of Tc-99m pertechnetate has been employed for functional evaluation of the salivary glands. However, the wide variability and poor reliability of all 2-dimensional approaches did not meet the standards required for clinical trial application or disease classification. In addition, no practice guideline has been recommended for the SGS by the major nuclear medicine societies (the Society of Nuclear Medicine and the European Society of Nuclear Medicine) [18, 19], requiring a dire need for a gamma camera imaging method of salivary gland evaluation using Tc-99m pertechnetate.
Quantitative single-photon emission computed tomography/computed tomography (SPECT/CT) is a promising gamma camera imaging modality [20, 21]. Due to the development of robust algorithms for attenuation correction, scatter correction, and resolution recovery, the quantitative SPECT/CT is emerging as a breakthrough method for true quantitative gamma imaging, especially for Tc-99m pertechnetate- or Tc-99m-labeled radiopharmaceuticals [22,23,24,25,26,27]. We previously tested the feasibility of Tc-99m pertechnetate SPECT/CT and proved the usefulness of the quantitative parameters in a variety of thyroid diseases [23, 24, 27]. In those studies, we concluded that just a 1 min-long SPECT was reliable for accurate assessment of quantitative parameters such as %uptake or standardized uptake value (SUV) [23, 24, 26, 27]. Thus, we applied this novel quantitative SPECT/CT technology to SGS because Tc-99m pertechnetate is the radiopharmaceutical of choice for salivary gland evaluation [23, 28].
In this study, we attempted to develop novel salivary gland SPECT/CT using Tc-99m pertechnetate. Useful quantitative parameters of the salivary gland SPECT/CT were investigated to differentiate between SS patients and controls.
Materials and Methods
Patients
Ninety-five xerostomic patients (age = 54.77 ± 13.53 [mean ± standard deviation (SD)] years (y); male:female = 5:90) who had been referred for the salivary gland SPECT/CT from the rheumatology clinic of (anonymous) Hospital from Oct 2015 to Feb 2017 were retrospectively included in the study. In addition to the salivary gland SPECT/CT, patients underwent biochemical auto-antibody test (anti-SSA/Ro) in 98.95% (94/95), labial salivary gland biopsy in 63.16% (60/95), unstimulated whole saliva flow rate in 27.37% (26/95), or Schirmer’s test in 69.47% (66/95), according to the late scoring system for SS (2016 America College of Rheumatology/European League against Rheumatism (ACR/ELAR) classification system) [3]. Patients with a summed score of ≥ 4 (n = 47) were allocated to SS while those with < 4 to non-SS (n = 48).
Forty-three thyroid cancer patients post-total thyroidectomy (age = 46.37 ± 12.13 y; male:female = 19:24) served as negative controls. They were high or intermediate risk thyroid cancer patients according to the ATA (American Thyroid Association) risk stratification system [29]. The salivary gland SPECT/CT was requested from the department of nuclear medicine of (anonymous) Hospital for the evaluation of baseline salivary function before radioactive iodine therapy from Aug 2015 to Nov 2016 [28]. No control patients were taking medications that affect salivary gland function, such as acetaminophen, hydrocodone, lisinopril, simvastin, amlodipine, alprazolam, hydrochlorothiazide, omeprazole, lipitor, furosemide, metoprolol, sertraline, zolpidem, oxycodone, or citalopram [30], and no control patients complained of any xerostomic symptom or sign at the time of salivary gland SPECT/CT.
This study design was approved by the institutional review board (IRB), and the acquisition of consent was waived by the IRB.
Salivary Gland SPECT/CT
A schematic of the salivary gland SPECT/CT protocol is shown in Fig. 1. The patients had been fasting for more than 6 h at the time of SPECT/CT. Tc-99m pertechnetate was eluted from a Mo-99m/Tc-99m generator (Samyoung, Korea), and the injected dose was 15 mCi. Quantitative SPECT/CT was performed twice at 20 and 40 min post-injection of Tc-99m pertechnetate. At 30 min, we administered lemon-flavored powder (Lemona™, 2 g, Kyung Nam Pharm. Co., Korea) as sialogogue and allowed patients to keep it in their mouths for 5 min, and then swallow.
A SPECT/CT scanner (NM/CT670; GE Healthcare, Pittsburgh, PA) equipped with low-energy high-resolution collimator was used. The scanner was cross-calibrated with a dose calibrator (CRC-15R; Capintec, Ramsey, NJ) that was used for the measurement of Tc-99m pertechnetate dose. The cross-calibration factor (or the system sensitivity of the SPECT/CT scanner) was determined to be 152.5 cpm per μCi for the software combination (Preparation for Q.Metrix™ for image reconstruction and Q.Metrix™ for quantitative analysis) [23, 24, 27].
For calculation of quantitative parameters, the following variables were recorded: body weight (kg), pre-injection radioactivity (mCi) and the measurement time, the injection time, post-injection radioactivity (mCi), and the measurement time, and the image acquisition start time. The SPECT parameters were the following: one-minute continuous mode acquisition, no body contour option, peak energy at 140 KeV with 20% energy window (126–154 KeV), and scatter energy at 120 KeV with 10% energy window (115–125 KeV). The acquired SPECT images were reconstructed under the following conditions: ordered subset expectation maximization (OSEM) algorithm (2 iterations and 10 subsets), triple corrections (CT-based attenuation correction, dual-energy window-based scatter correction, and resolution recovery), post-reconstruction low-pass filter (Butterworth filter with frequency of 0.48 and order of 10), zoom factor of 1.5, matrix of 128 × 128, and slice thickness of 2.95 mm.
Helical CT images for attenuation correction and image co-registration were acquired using the following parameters: tube voltage of 120 KVp, tube current of 30 mA, beam collimation of 20 mm (= 16 × 1.25), table speed of 37 mm/s, table feed per rotation of 18.75 mm/rotation, tube rotation time of 0.5 s, pitch of 0.938:1, matrix size of 512 × 512, and slice thickness of 2.5 mm. All processes were performed using a vendor-provided workstation (Xeleris 3.1; GE Healthcare).
Quantitative Parameters from SPECT/CT
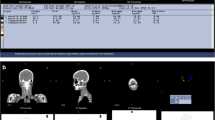
The vendor-provided software (Q.MetrixTM; GE Healthcare) was used for the quantitative analyses. Multiple regions-of-interest (ROIs) were manually drawn over each salivary gland on the transaxial CT images. ROIs were drawn in every slice, and at least 18 or 12 ROIs were required for parotid or submandibular glands, respectively. Multiple ROI slices were integrated to make a volume-of-interest (VOI) that generated the %injected dose (%ID) for individual salivary glands (Fig. 2). The %ID was calculated according to the following equation:
The process of individual salivary gland segmentation. Upon the transaxial CT images of SPECT/CT, multiple 2-dimensional regions-of-interest (ROIs) were manually drawn. Then, the integration of the ROIs resulted in volume-of-interest (VOI) for each salivary gland. The %injected dose for the glands was automatically generated on the vendor-provided software
The %ID of individual parotid or submandibular glands was measured at 20 min (pre-stimulation) and 40 min (post-stimulation) of SPECT/CT images. The %IDs from the bilateral glands were averaged, and the excretion of parotid and submandibular glands was calculated using the following equation:
Therefore, there were four quantitative SPECT/CT parameters employed in the current study.
-
1)
% parotid uptake (%PU) = %ID of parotid glands at 20 min of pre-stimulation
-
2)
% submandibular uptake (%SU) = %ID of submandibular glands at 20 min of pre-stimulation
-
3)
% parotid excretion (%PE) = %excretion of parotid glands from 20 to 40 min
-
4)
% submandibular excretion (%SE) = %excretion of submandibular glands from 20 to 40 min
Classification of SS
The most recent classification system (2016 ACR/ELAR criteria) was employed to identify the SS and non-SS patients. Anti-SSA/Ro antibody was positive in 55.32% (52/94) of patients, labial salivary gland biopsy was positive with lymphocytic focus score of ≥ 1 foci/4 mm2 in 60.0% (36/60), unstimulated whole saliva flow rate was positive with ≤ 0.1 ml/min in 73.08% (19/26), and Schirmer’s test was positive with ≤ 5 mm/5 min in at least one eye in 62.12% (41/66). For each item, a score of 3 was allocated for anti-SSA/Ro antibody and labial salivary gland biopsy or 1 for unstimulated whole saliva flow rate and Schirmer’s test. When the summed total score was ≥ 4, the patients were classified as SS (n = 47), while those with a score < 4 were designated as non-SS (n = 48) [3].
Statistical Analysis
All data were expressed as mean ± SD. Statistical software (Medcalc® Software 12.4.0.0, Mariakerke, Belgium) was used for the statistical analyses. Group comparisons were performed using ANOVA (analysis of variance) with subsequent post-hoc analysis using Student-Newman-Keuls test when the assumption of variances equality was not rejected. If the equality of variances was not accepted, Kruskal-Wallis test was performed. In addition, chi-square test and ROC (receiver-operating characteristic) analyses were conducted. p values less than 0.05 were considered statistically significant.
Results
Patient Characteristics
The patient characteristics of each group are summarized in Table 1. Age was different among the negative controls, non-SS, and SS patients (p < 0.003): the negative control patients were younger than the non-SS and SS patients (p < 0.05). Sex was also different among the three groups: the non-SS and SS patients were female-dominant, but the negative control patients were not (p < 0.001). The following tests were not applicable to the negative controls but only to the certain portions of non-SS and SS patients: anti-SSA/Ro antibody positivity was greater in SS (85.11%; 40/47) than in non-SS (25.53%; 12/47) (p < 0.001); labial salivary gland biopsy was more frequently positive for SS (76.3%; 29/38) than non-SS (31.8%; 7/22) (p = 0.002); unstimulated whole saliva flow rate was more often impaired in SS (94.12%, 16/17) than in non-SS (33.33%, 3/9) (p = 0.004); and Schirmer’s test positivity was greater in SS (84.21%, 32/38) than in non-SS (32.14%, 9/28) (p < 0.001).
Quantitative Parameters of Salivary Gland SPECT/CT
The uptake parameters (%PU and %SU) at 20 min were significantly different among the negative controls, non-SS, and SS patients (p = 0.005 for %PU and p < 0.001 for %SU, respectively), whereas the excretion parameters (%PE and %SE) were not (Table 2, Fig. 3). Specifically, the %PU was significantly lower in the SS than in the negative controls and the non-SS patients (p < 0.05). The %SU was significantly lower in the SS than in the negative controls and the non-SS patients (p < 0.05); the %SU was also lower in the non-SS compared with the negative controls with a statistical significance (p < 0.05). When the SS and non-SS patients were compared, %PU and %SU were significantly lower for SS than for non-SS patients (p < 0.05 for both).
Comparison of the SPECT/CT parameters. a The %PU (%parotid uptake) was significantly lower in SS than in negative control and non-SS (*p < 0.05). b The %SU (%submandibular uptake) was the lowest in SS (**p < 0.05), and the second lowest in non-SS (*p < 0.05), compared to the negative control. c The %PE (%parotid excretion) and d the %SE (%submandibular excretion) were not significantly different among the negative control, non-SS, and SS (p > 0.05)
These findings indicate that impaired uptake of Tc-99m pertechnetate of parotid (%PU) and submandibular glands (%SU) at 20 min post injection may play a role in the diagnosis of SS (Fig. 3a,b). In addition, mildly reduced %SU with preserved %PU may suggest a certain xerostomic syndrome unrelated with SS (Fig. 3b).
ROC Analysis for Identification of SS
In the current study, the non-SS and SS patients were differentiated from each other using the most recent criteria for primary SS (2016 ACR/ELAR criteria). It is of note that the 2016 ACR/ELAR criteria do not include salivary gland scintigraphy. Thus, in order to know the potential application of SPECT/CT parameters for the diagnosis of SS, ROC analysis was performed to differentiate SS from non-SS patients. The negative controls were not included in this analysis. As a result, the AUC (area-under-the curve) was the highest for the %SU (AUC, 0.720; 95% confidence interval (C.I.), 0.618 to 0.807), which was followed by the %PE (AUC, 0.685; 95% C.I., 0.582 to 0.777), the %PU (AUC, 0.660; 95% C.I., 0.556 to 0.754), and the %SE (AUC, 0.576; 95% C.I., 0.470 to 0.676). A statistical difference was only found between the %SU and the %SE (p = 0.007). Using the optimal cut-off value of %SU ≤ 0.07%, sensitivity of 70.21% and specificity of 70.83% were achieved for the diagnosis of SS (Fig. 4).
ROC (receiver-operating characteristic) analysis for diagnosis of SS using the SPECT/CT parameters. The %SU (%submandibular uptake) had the greatest AUC (area-under-the curve) of 0.720 with a 95% confidence interval of 0.618 to 0.807 compared to other parameters. %PU, %parotid uptake; %SU, %submandibular uptake; %PE, %parotid excretion; %SE, %submandibular excretion
Typical Case Demonstration
Typical cases for SS, non-SS, and negative control are demonstrated in Figs. 5, 6, and 7.
SS patient. A 58-year-old female patient with severe dry mouth and dry eyes was suspected for SS. All tests for SS (anti-SSA/Ro antibody, unstimulated whole salivary flow rate, Schirmer’s test, and labial salivary gland biopsy) were positive for this patient. Her %PU, %SU, %PE, and %SE were 0.14%, 0.02%, 29.63%, and 0.00%, respectively
Non-SS patient. A 48-year-old male patient complained of xerostomia. His anti-SSA/Ro antibody was positive, but other tests (labial salivary gland biopsy, unstimulated whole salivary flow rate, and Schirmer’s test) were all negative. His %PU, %SU, %PE, and %SE were 0.42%, 0.11%, 78.57%, and 54.55%, respectively
Discussion
The proper role of SGS regarding SS diagnosis has been highly debated until the development of recent consensus criteria. Initially, reduced uptake/excretion of Tc-99m pertechnetate of the salivary glands was considered to represent xerostomia (here, the presence of xerostomia itself is needed to be defined by the abnormal SGS), but the abnormal uptake/excretion was not concretely described, and it was not clear whether the abnormal salivary glands indicated parotid glands or submandibular glands [1, 31]. The classification criteria by the American-European consensus group adopted the SGS as one piece of objective evidence of salivary gland involvement of SS, but the definition of abnormal SGS was still obscure. For example, “how much delayed uptake/excretion is critical?” and “how much reduced concentration is serious?” were not properly addressed in the criteria [2]. A Japanese group introduced their own classification criteria for SS, but they did not even contemplate to include the SGS as one of the items for the criteria [6]. Furthermore, mainly due to low specificity concerns, SGS has not been included in recent large-scale international criteria [3, 7]. In this regard, the result of the current study may introduce revival of SGS as one of the objective items of salivary gland involvement of SS.
In the present study, we did not use the conventional SGS approach that has been performed as either multiple planar imaging [10,11,12] or dynamic acquisition with TAC analysis [13,14,15,16,17]. Instead, quantitative SPECT/CT was applied to the functional evaluation of salivary gland disease. In fact, 3-dimensional SPECT approach without CT has rarely been applied to the salivary gland imaging [32, 33]. SPECT with integrated CT (hybrid SPECT/CT) has been anecdotally performed for the functional evaluation of salivary glands without true quantitative assessment [23, 34]. In the current study using quantitative SPECT/CT technology, the uptake/excretion of Tc-99m pertechnetate was absolutely quantitated under base of %ID that had been corrected for attenuation, scatter, and variation of distance between detector and patient (resolution recovery). This advanced technology of state-of-the-art SPECT/CT may have an advantage over conventional planar SGS in terms of accurate functional evaluation of the salivary glands.
The main finding of the current study was that %SU was the key parameter of SS, which has already been suggested in the literature. Using planar SGS and TAC analysis, studies report that reduced Tc-99m pertechnetate uptake on the submandibular glands was one of the SS-specific imaging biomarkers [13,14,15,16]. Serial planar anterior imaging also demonstrated that dysfunction of the submandibular glands was closely associated with SS-induced xerostomia [28]. It is well-known that the submandibular glands contribute to the major portion of the saliva amount (~ 70%) at non-stimulated state [35] and that patients usually feel xerostomia at resting state [28]. Therefore, the reduced %SU, which was measured at 20 min post-injection prior to stimulation, may play a key role for SS diagnosis.
Regarding the meaning of reduced %PU in the SS but not non-SS, it may represent a relatively later stage of SS progression. SS has been reported to involve submandibular glands first and then parotid glands [13,14,15,16]. The reason why the parotid glands are affected later in SS than the submandibular glands is not clearly explained by other studies. The possible mechanism may lie in the cellular composition feature of the salivary glands. The parotid glands consist of only serous cells, whereas the submandibular glands are constituted of a mixture of serous and mucous cells. The serous cells have been reported to be radiation-sensitive, and thus, the high vulnerability of parotid glands to radio-active iodine therapy has been ascribed to the cellular characteristics of the parotid glands [36, 37]. Conversely, the absence of mucous component in the parotid glands may endow the parotid glands with resistance to immunologic aggression of SS, and the parotid glands, as a result, may be involved at later time points during SS progression. The timing of progression needs to be clarified in further studies.
Regarding the excretory parameters, we could not prove the utility of %PE and %SE for differential diagnosis of SS. In the literature, some studies have advocated the usefulness of excretion parameters for SS diagnosis [38], whereas others could not find any difference of excretion parameters between SS and controls [17]. These findings seem to reflect the difficulty of achieving a standard stimulation procedure and the diversity of normal excretion fraction during static SGS. It is also noteworthy that the salivary gland spontaneously discharges its content even without any stimulation [35]. This unwanted natural excretion, as well as a variety of gustatory stimulation methods (i.e., variable concentration/amount of lemon juice per oral [12, 15,16,17, 37, 39,40,41,42], lemon candy suction [35, 43], subcutaneous injection of carbachol as a cholinergic agonist [33], or vitamin C powder per oral [28, 34]), may have led to the inconsistent results for the excretory parameters that have been tested in many SGS protocols using Tc-99m pertechnetate. The issue of proper stimulation method needs to be addressed in the future SPECT/CT studies.
There are several limitations in the study. The number of enrolled patients was not large enough for a verification of the utility of the SPECT/CT parameters for SS. Second, the salivary gland segmentation procedure was performed by only an operator. Although she was an experienced nuclear medicine physician, repeatability of the segmentation process was not evaluated. Third, spontaneous salivary secretion may have caused underestimation of salivary uptake (%PU and %SU). The excretion parameters (%PE and %SE) based on the underestimated %PU/%SU would also have been seriously biased. This is another critical limitation of this kind of static study. SPECT is not a dynamic study but another static study. Rapid dynamic acquisition of SPECT may address this problem, which needs further investigation. Finally, it is not clear whether the thyroid cancer patients can be proper negative controls. Of course, completely normal subjects should have been employed as true negative controls, but it was not possible to include those subjects in the current retrospective study. However, we made an utmost effort to screen the medication history of the thyroid cancer patients, and no control patients were under pharmacologic influence that could affect the salivary gland function. Furthermore, the control patients did not complain of any xerostomia at the time of SPECT/CT. Therefore, the main finding of the current study with the reference of thyroid cancer patients may be justified.
Conclusion
The degree of submandibular gland uptake at 20 min post-injection of Tc-99m pertechnetate, as represented by %SU of the quantitative SPECT/CT, may be useful for the diagnosis of SS. Therefore, quantitative SPECT/CT may play a crucial role for objective and unbiased assessment of salivary gland dysfunction, whereby SS may be more effectively identified.
References
Manthorpe R, Frost-Larsen K, Isager H, Prause JU. Sjogren's syndrome. A review with emphasis on immunological features. Allergy. 1981;36:139–53.
Vitali C, Bombardieri S, Jonsson R, Moutsopoulos HM, Alexander EL, Carsons SE, et al. Classification criteria for Sjogren's syndrome: a revised version of the European criteria proposed by the American-European Consensus Group. Ann Rheum Dis. 2002;61:554–8.
Shiboski CH, Shiboski SC, Seror R, Criswell LA, Labetoulle M, Lietman TM, et al. 2016 American College of Rheumatology/European League Against Rheumatism classification criteria for primary Sjogren's syndrome: a consensus and data-driven methodology involving three international patient cohorts. Ann Rheum Dis. 2017;76:9–16.
Vitali C, Bombardieri S, Moutsopoulos HM, Balestrieri G, Bencivelli W, Bernstein RM, et al. Preliminary criteria for the classification of Sjogren's syndrome. Results of a prospective concerted action supported by the European Community. Arthritis Rheum. 1993;36:340–7.
Fujibayashi T, Sugai S, Miyasaka N, Hayashi Y, Tsubota K. Revised Japanese criteria for Sjogren's syndrome (1999): availability and validity. Mod Rheumatol. 2004;14:425–34.
Fox RI, Robinson CA, Curd JG, Kozin F, Howell FV. Sjogren's syndrome. Proposed criteria for classification. Arthritis Rheum. 1986;29:577–85.
Shiboski SC, Shiboski CH, Criswell L, Baer A, Challacombe S, Lanfranchi H, et al. American College of Rheumatology classification criteria for Sjogren's syndrome: a data-driven, expert consensus approach in the Sjogren's International Collaborative Clinical Alliance cohort. Arthritis Care Res. 2012;64:475–87.
Vivino FB, Hermann GA. Role of nuclear scintigraphy in the characterization and management of the salivary component of Sjogren's syndrome. Rheum Dis Clin N Am. 2008;34:973–86 ix.
Schall GL, Anderson LG, Wolf RO, Herdt JR, Tarpley TM Jr, Cummings NA, et al. Xerostomia in Sjogren's syndrome. Evaluation by sequential salivary scintigraphy. JAMA. 1971;216:2109–16.
Schall GL, Larson SM, Anderson LG, Griffith JM. Quantification of parotid gland uptake of pertechnetate using a gamma scintillation camera and a “region-of-interest” system. Am J Roentgenol Radium Therapy, Nucl Med. 1972;115:689–97.
Solans R, Bosch JA, Galofre P, Porta F, Rosello J, Selva-O'Callagan A, et al. Salivary and lacrimal gland dysfunction (sicca syndrome) after radioiodine therapy. J Nucl Med. 2001;42:738–43.
Caglar M, Tuncel M, Alpar R. Scintigraphic evaluation of salivary gland dysfunction in patients with thyroid cancer after radioiodine treatment. Clin Nucl Med. 2002;27:767–71.
Sugihara T, Yoshimura Y. Scintigraphic evaluation of the salivary glands in patients with Sjogren's syndrome. Int J Oral Maxillofac Surg. 1988;17:71–5.
Hakansson U, Jacobsson L, Lilja B, Manthorpe R, Henriksson V. Salivary gland scintigraphy in subjects with and without symptoms of dry mouth and/or eyes, and in patients with primary Sjogren's syndrome. Scand J Rheumatol. 1994;23:326–33.
Umehara I, Yamada I, Murata Y, Takahashi Y, Okada N, Shibuya H. Quantitative evaluation of salivary gland scintigraphy in Sjorgen's syndrome. J Nucl Med. 1999;40:64–9.
Aung W, Yamada I, Umehara I, Ohbayashi N, Yoshino N, Shibuya H. Sjogren's syndrome: comparison of assessments with quantitative salivary gland scintigraphy and contrast sialography. J Nucl Med. 2000;41:257–62.
Nishiyama S, Miyawaki S, Yoshinaga Y. A study to standardize quantitative evaluation of parotid gland scintigraphy in patients with Sjogren's syndrome. J Rheumatol. 2006;33:2470–4.
SNM guideline. In http://www.snmmi.org/ClinicalPractice/content.aspx?ItemNumber=6414&navItemNumber=10790.
EANM guideline. In http://www.eanm.org/publications/guidelines/index.php?navId=37.
Ritt P, Vija H, Hornegger J, Kuwert T. Absolute quantification in SPECT. Eur J Nucl Med Mol Imaging. 2011;38(Suppl 1):S69–77.
Bailey DL, Willowson KP. An evidence-based review of quantitative SPECT imaging and potential clinical applications. J Nucl Med. 2013;54:83–9.
Suh MS, Lee WW, Kim YK, Yun PY, Kim SE. Maximum standardized uptake value of (99m)Tc hydroxymethylene diphosphonate SPECT/CT for the evaluation of temporomandibular joint disorder. Radiology. 2016;280:890–6.
Lee H, Kim JH, Kang YK, Moon JH, So Y, Lee WW. Quantitative single-photon emission computed tomography/computed tomography for technetium pertechnetate thyroid uptake measurement. Medicine (Baltimore). 2016;95:e4170.
Kim HJ, Bang JI, Kim JY, Moon JH, So Y, Lee WW. Novel application of quantitative single-photon emission computed tomography/computed tomography to predict early response to methimazole in Graves’ disease. Korean J Radiol. 2017;18:543–50.
Kim J, Lee HH, Kang Y, Kim TK, Lee SW, So Y, et al. Maximum standardised uptake value of quantitative bone SPECT/CT in patients with medial compartment osteoarthritis of the knee. Clin Radiol. 2017;72:580–9.
Kang YK, Park S, Suh MS, Byun SS, Chae DW, Lee WW. Quantitative single-photon emission computed tomography/computed tomography for glomerular filtration rate measurement. Nucl Med Mol Imaging. 2017;51:338–46.
Kim JY, Kim JH, Moon JH, Kim KM, Oh TJ, Lee DH, et al. Utility of quantitative parameters from single-photon emission computed tomography/computed tomography in patients with destructive thyroiditis. Korean J Radiol. 2018;19:470–80.
Kang JY, Jang SJ, Lee WW, Jang SJ, Lee YJ, Kim SE. Evaluation of salivary gland dysfunction using salivary gland scintigraphy in Sjogren's syndrome patients and in thyroid cancer patients after radioactive iodine therapy. Nucl Med Mol Imaging. 2011;45:161–8.
Haugen BR, Alexander EK, Bible KC, Doherty GM, Mandel SJ, Nikiforov YE, et al. 2015 American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid. 2016;26:1–133.
Atkinson JC, Grisius M, Massey W. Salivary hypofunction and xerostomia: diagnosis and treatment. Dent Clin N Am. 2005;49:309–26.
Vitali C, Moutsopoulos HM, Bombardieri S. The European Community Study Group on diagnostic criteria for Sjogren's syndrome. Sensitivity and specificity of tests for ocular and oral involvement in Sjogren's syndrome. Ann Rheum Dis. 1994;53:637–47.
Nakamura T, Oshiumi Y, Yonetsu K, Muranaka T, Sakai K, Kanda S. Salivary SPECT and factor analysis in Sjogren's syndrome. Acta Radiol. 1991;32:406–10.
van Acker F, Flamen P, Lambin P, Maes A, Kutcher GJ, Weltens C, et al. The utility of SPECT in determining the relationship between radiation dose and salivary gland dysfunction after radiotherapy. Nucl Med Commun. 2001;22:225–31.
Chen J, Zhao X, Liu H, Zhou S, Yang Y, Li S, et al. A point-scoring system for the clinical diagnosis of Sjogren's syndrome based on quantified SPECT imaging of salivary gland. PLoS One. 2016;11:e0155666.
Hermann GA, Vivino FB, Shnier D, Krumm RP, Mayrin V, Shore JB. Variability of quantitative scintigraphic salivary indices in normal subjects. J Nucl Med. 1998;39:1260–3.
Stephens LC, Schultheiss TE, Price RE, Ang KK, Peters LJ. Radiation apoptosis of serous acinar cells of salivary and lacrimal glands. Cancer. 1991;67:1539–43.
Raza H, Khan AU, Hameed A, Khan A. Quantitative evaluation of salivary gland dysfunction after radioiodine therapy using salivary gland scintigraphy. Nucl Med Commun. 2006;27:495–9.
Hermann GA, Vivino FB, Goin JE. Scintigraphic features of chronic sialadenitis and Sjogren's syndrome: a comparison. Nucl Med Commun. 1999;20:1123–32.
Saito T, Fukuda H, Horikawa M, Ohmori K, Shindoh M, Amemiya A. Salivary gland scintigraphy with 99mTc-pertechnetate in Sjogren's syndrome: relationship to clinicopathologic features of salivary and lacrimal glands. J Oral Pathol Med. 1997;26:46–50.
Miyake H, Matsumoto A, Hori Y, Takeoka H, Kiyosue H, Hori Y, et al. Warthin's tumor of parotid gland on Tc-99m pertechnetate scintigraphy with lemon juice stimulation: Tc-99m uptake, size, and pathologic correlation. Eur Radiol. 2001;11:2472–8.
Adams BK, Al Attia HM, Parkar S. Salivary gland scintigraphy in Sjogren's syndrome: are quantitative indices the answer? Nucl Med Commun. 2003;24:1011–6.
Loutfi I, Nair MK, Ebrahim AK. Salivary gland scintigraphy: the use of semiquantitative analysis for uptake and clearance. J Nucl Med Technol. 2003;31:81–5.
Nakada K, Ishibashi T, Takei T, Hirata K, Shinohara K, Katoh S, et al. Does lemon candy decrease salivary gland damage after radioiodine therapy for thyroid cancer? J Nucl Med. 2005;46:261–6.
Funding Source
This work was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) and funded by the Ministry of Education (2015R1D1A1A01059146).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
Jihyun Kim, Hyunjong Lee, Hwanhee Lee, Ji-In Bang, Yeon-koo Kang, Sungwoo Bae, Yoo Sung Song, and Won Woo Lee declare that they have no conflicts of interest.
Ethical Approval
The study was approved by an institutional review board (IRB) and was performed in accordance with the ethical standards set in the 1964 Declaration of Helsinki and its later amendments.
Informed Consent
The need for patient’s informed consent was waived by the IRB.
Rights and permissions
About this article
Cite this article
Kim, J., Lee, H., Lee, H. et al. Quantitative Single-Photon Emission Computed Tomography/Computed Tomography for Evaluation of Salivary Gland Dysfunction in Sjögren’s Syndrome Patients. Nucl Med Mol Imaging 52, 368–376 (2018). https://doi.org/10.1007/s13139-018-0547-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13139-018-0547-4