Abstract
Oral cancer accounts for around 30 percent of all cancers in India. These cancers are usually managed either by surgery, radiotherapy, chemotherapy or a combination of these modalities. Dental oncologists play an integral part in the multidisciplinary team, including surgeons, radiation and medical oncologists, nurses, physician assistants, nutritionists, psychologists and social workers to efficiently manage cancer patients. Oral complications associated with cancer therapy can range from minor mucositis or infections to severely debilitating conditions such as osteonecrosis of jaws, which can disrupt the ongoing cancer therapy and jeopardize the overall quality of life of the patient. This highlights the primary role of a dentist in the efficient identification and management of potential oral foci of infection and subsequent prevention of the onset of these complications. This necessitates accurate, evidence-based knowledge and extensive training of dental oncologists to provide state-of-the-art management strategies. This article aims to review oral management before, during and after therapy in patients undergoing treatment for cancers affecting the head and neck region.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oral cancer is ranked among the top three of all cancers in India, accounting for over thirty percent of all cancers [1]. Based on the site, stage and pathological variant of the disease, the major modes of therapy include surgery, radiotherapy, chemotherapy or a combination of these. Careful planning and execution of the treatment components including surgery, chemoradiation and rehabilitation is crucial in the management of oral cancer. The paper does not attempt to give the details of such management and that may be out of the scope of this review. However, these modalities are associated with several complications to the stomatognathic system. Hence, emphasis must be given to oral management before, during and after therapy to prevent these complications, as the severity of these may disrupt the ongoing treatment [2].
Surgery
Surgery is one of the most frequently employed techniques for head and neck cancers, which generally results in surgical defects, ranging from distortion of the soft tissue to extensive defects where significant amounts of the region may be lost. It can also compromise the aesthetic and functional aspect of the individual, thus compromising the grinding ability due to loss of the stable and reproducible stomatognathic system.
Oral Management Before Surgical Therapy
It is highly recommended to conduct an initial screening of the oral cavity prior to surgery to assess the overall prognosis of teeth and associated oral environment. Since the surgical procedure is carried out under general anesthesia, it would be wise to undergo extractions of prognostically compromised teeth during surgery to ensure a favorable postoperative healing period. This has an added advantage to ensure that the healing of the extraction socket would occur simultaneously with the surgical site. If the patient is planned for radiotherapy, this would rule out the unwanted time lag between surgery and radiotherapy. Additionally, the impressions of the maxillary arch can be recorded preoperatively for the patients requiring maxillofacial prosthesis or obturators during the postoperative period. Restorative treatment planning with patient understanding is important prior to the treatment. Planning and consultation with the patient presenting the treatment plan is vital to avoid misunderstanding and unmet expectations. Treatment planning has greatly advanced with the widening use of intraoral scanners and CADCAM software.
Oral Management After Surgical Therapy
The severely disfigured site associated with surgery is repaired and reconstructed in two ways: surgical reconstruction and prosthetic rehabilitation. Reconstruction involves surgical management. Rehabilitation is more of a multidisciplinary effort. The oral rehabilitation of patients with head and neck cancer presents a challenge to the treating physician since many activities, including speech, deglutition, control of oral secretions and mastication, might be impacted. The primary objective of oral rehabilitation is to recover the patient's oral functioning after surgery because the patient will alter forever as a result of the procedure. Head and neck cancer patients who receive various treatments may experience a wide range of side effects, such as xerostomia, mucositis, dysgeusia, dental hypersensitivity, fungal infections, ulceration, gingival bleeding, trismus, pain, decreased salivary flow and the inability to wear removable prosthetics. All of these side effects must be taken into consideration during the oral rehabilitation process because they will all have an impact on the patient's recovery. According on the type of cancer, its extent, whether it was invasive or noninvasive, the lymph nodes and metastases involved, the type of surgery and the radiation modalities employed, the approach and techniques for the rehabilitation of head and neck cancer patients will vary.
Surgical Reconstruction
Surgical reconstruction is done by alloplastic or autologous grafts, free tissue flaps or local flaps.
Prosthetic Rehabilitation/ Obturators
The prosthetic rehabilitation of patients undergoing surgical management depends on multiple factors such as the amount of remaining supportive tissue, number and prognosis of the remaining supporting teeth, age and comorbidities, preferences and physical dexterity of the patient [3].
The maxillofacial prosthesis could be of two types, conventional adhesive retained prosthesis or implant-retained. Conventional adhesive retained prosthesis employs several retentive methods such as adhesives or undercuts. However, the rehabilitation with removable appliances may be challenging due to deteriorated anatomy of the surgical site, decreased salivary flow or the patient’s emotional resilience after the surgery.
Implant retained reconstruction is where implants are placed into the maxillofacial region to retain the prosthesis. It has the added advantage of reducing the reliance on patient’s oral coordination or dexterity [4]. Trismus is a major factor that has to be considered while planning the prosthesis.
Guided Prosthetic Appliances/ Guiding Flange Prosthesis
When surgery involves a segmental mandibulectomy, one of the most common problems faced is the loss of occlusion and deviation of the mandible toward one side. This happens because of the muscular imbalance caused by unilateral muscle removal, modified maxillo-mandibular relationship and diminished tooth-to-tooth contact [5]. Such an issue is managed using guided prosthetic appliances, which hold the deviated mandible to the midline to correct the occlusion.
Radiotherapy
Radiotherapy is another mode of treating head and neck cancer, which may be given either as a sole treatment or as a combination treatment along with surgery and/or chemotherapy. However, irrespective of whether being administered as a single or combined treatment, radiotherapy is associated with various short-term and long-term side effects in the oral cavity.
Oral Management Before Radiotherapy
The primary role of dental oncologist prior to radiotherapy lies in the prevention or reduction of the unwanted side effects related to radiotherapy and thereby promoting the preservation of good oral health after the treatment [6]. After the initial workup involving the history and clinical examination, the patient is assessed for the requirement of any dental procedures such as oral prophylaxis, restorations and extractions.
Teeth with less extensive caries or abrasion with a good prognosis are ideally considered for restorative procedures. However, it is advisable to undergo extraction of non-restorable teeth with active or extensive periapical infections, periodontal disease, lack of antagonistic teeth, compromised oral hygiene, partially erupted or impacted teeth [7]. During the extraction, good care must be taken to perform the extraction as atraumatic as possible, perform adequate alveoloplasty to eliminate sharp bony projections, possibly achieve primary closure, advise antibiotics for a week post extraction. There have been many schools of thought concerning the timing for pre-radiotherapy dental extractions. Marx et al. suggested that extractions must be undertaken at least 21 days before the initiation of radiotherapy to ensure adequate postoperative healing [8]. However, Starcke et al. showed that pre-RT extractions carried out in < 10 days were not associated with Osteoradionecrosis [9]. Proper patient counseling regarding the importance of oral health maintenance must be instituted. If a patient is less motivated to maintain oral hygiene, then extraction must be promptly considered.
Tongue Stabilizers
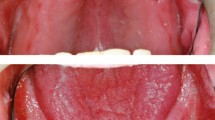
Tongue stabilizers are prosthetic appliances/stents fabricated to protect normal peripheral tissue from the field of radiation. (Fig. 1) These appliances are fabricated on maxillary and mandibular casts using acrylic or any other biocompatible materials [10].
Oral Management During Radiotherapy
Mucositis
It is a painful, debilitating condition caused by the inflammation of mucosa subsequent to chemotherapy or radiotherapy. Patients often present with severe pain, difficulty in phonation and ingesting food [11]. Although various agents have been studied for efficacy in managing oral mucositis, none has been confirmed to be a complete remedy for this condition. Hence, the treatment of mucositis is greatly confined to the symptomatic management.
Pain Control
Mouth rinses using baking soda and benzydamine hydrochloride are primarily used for short-term pain control while undergoing therapy [12, 13]. Ice chips and topical mouth rinses containing an anesthetic such as 2% viscous lidocaine are also given for adequate pain control. In cases of severe pain, systemic analgesics such as opioids are commonly prescribed based on the World health organization (WHO) step analgesic ladder.
Nutritional Support
The patients usually lack nutrition due to the pain and taste changes. Hence, it is advisable to monitor the nutritional intake and weight of the individuals. Patients are advised to take soft and liquid supplements during radiotherapy. In patients with dysphagia or dysgeusia, gastrostomy tubes are placed prophylactically, and parenteral nutrition is provided via catheters [14].
Xerostomia
It is the sensation of dryness in the mouth. It starts as early as the second week of radiotherapy and persists as subacute and late side effects. Patients may also complain of thickening of saliva due to a decrease in the serous component of saliva [15]. The degree of xerostomia is determined by the number of the major glands included in the radiation field. If only one side is irradiated, then compensatory hypertrophy of the remaining glands occurs. The following measures can manage xerostomia.
Protectants
Patients are counseled to sip water as needed to alleviate mouth dryness. Additionally, they are made to rinse with a solution of half a teaspoon of baking soda in one cup of warm water several times a day to clean and lubricate the oral tissues and to buffer the oral environment.
Salivary-Sparing Radiation Techniques
The use of IMRT has been tremendously successful in confining the dosage to the required treatment volume, thereby sparing the normal tissues, including the salivary glands, from the radiation field [16].
Submandibular Gland Transfer
If only one side of the neck is being irradiated, the submandibular gland can be surgically transferred to a shielded area in the submental space to protect it from the radiation, provided that it is a neck node-negative case of cancer [17].
Saliva Substitutes
Artificial saliva containing mucin, glycerine or carboxymethylcellulose, hydroxypropyl cellulose, hydroxyethylcellulose are available in the form of gels or solutions for application in the mouth. These agents mimic the physical characteristics of saliva, but neither can induce saliva production nor have any of the antimicrobial properties of the saliva [18].
Soft Tissue Infections
Oropharyngeal candidiasis (OPC) caused by Candida albicans is the main infection seen during the course of radiation. Patients often complain of burning sensations and taste alterations. Salivary gland hypofunction or mucositis increases the vulnerability of the mucosa to fungal infection. Topical antifungal agents are usually used to manage OPC due to its lower side effects and drug interactions. However, the administration of topical agents several times a day accounts for its compromised compliance to therapy [19].
Sometimes, it is not uncommon to find Herpes simplex viral infection in patients undergoing radiotherapy or chemotherapy. These patients are managed by administering antiviral drugs such as Acyclovir [20].
Halitosis (Oral Malodor)
The causes for oral malodor are multifactorial. Apart from any contributing systemic illness, radiation patients are prone to develop halitosis due to compromised oral hygiene, oral mucositis, microbial colonization, xerostomia and tissue necrosis [21]. Patients are advised to strictly adhere to basic oral hygiene procedures such as using a soft toothbrush for cleaning the teeth after every meal, flossing, mechanical tongue hygiene using gauze pads. It is recommended to use antiseptic mouthwashes without alcohol, as alcohol can cause tissue irritation. Water flossers may be used as a home care adjunct.
Oral Management After Radiotherapy
Radiation/Rampant Caries
Caries is one of the most common problems encountered after radiotherapy. It is caused by alterations in the chemical composition of saliva and abundant cariogenic oral bacteria, which leads to rapid decalcification of dental enamel. It tends to spread aggressively and extensively to all dental surfaces, ultimately causing increased friability and breakdown of teeth. However, it is not caused directly by irradiation but results from the sequelae of xerostomia and a cariogenic shift in microflora [22]. It is also common to encounter patients complaining of hypersensitivity of teeth. This may occur secondary to carious lesions, physiologic wearing away of teeth, gingival recession or other factors.
Management
Diet
Patients are advised to eliminate or reduce sugar intake or replace sticky foods. Frequent small meals with high joule foods are advocated. Advise rinsing with water after every meal to facilitate the rapid clearance of food sticking on the teeth and the microorganisms. Rinsing with sodium bicarbonate solution can elevate salivary pH and buffering capacity.
Fluorides
Fluorides are known for their ability to inhibit the demineralization of enamel and increase the rate of remineralization [23]. The efficacy of fluorides depends on the concentration of fluoride used, frequency of fluoride application and the specific fluoride compound employed. Sodium diamine fluoride usage is appropriate in many of these carious lesions. The common method of application is a brush-on technique or using customized trays. The customized tray is a vacuum-formed mouth guard material fabricated on study models, which are then trimmed to ensure no tissue irritation occurs. After careful brushing and flossing, spread several drops of the fluoride gel in the tray. The tray is then seated in the mouth and left in place for 5–10 min. The excess material is then spat out. The patient is advised not to eat, drink or rinse afterward for one hour. The fluoride application after radiation is a life-long necessity. Daily home fluoride treatment along with 3–6 month dental follow-up can prevent the development of radiation caries. However, lack of compliance is considered one of the major disadvantages of fluoride therapy.
Restorative Considerations
Restorations are considered as early as possible with the detection of an active carious lesion with a soft, leathery base and the potential for remineralization is poor. Earlier, dental amalgam over glass-ionomer lining was used for posterior teeth considering their ability to withstand high occlusal loading. However, they are not used in the current practice. The preferred restorative materials are glass-ionomer cements and composite resins.
Conventional glass-ionomer cement has the potential for tooth adhesion, extended fluoride release and fluoride uptake from toothpaste, gels and mouth rinses (fluoride reservoir effect). However, it requires a dry oral environment to prevent desiccation & acid erosion of the material within weeks of placement. Opacity and poor aesthetics mark the disadvantages associated with these materials. Modified glass-ionomer or light-activated glass-ionomer is known for its improved aesthetics and greater resistance to acid attack and desiccation. Composite restorations are known for their higher aesthetics, especially for anterior teeth. Notwithstanding, they risk marginal gap formation and are prone to recurrent caries underneath the restoration. In certain patients with hypersensitivity of teeth, dentin desensitizing toothpaste may also be helpful [24].
Endodontic Treatment
Endodontic treatment is advocated when caries have extended toward the pulp, hyperemic pulp or the presence of periapical pathology. Root canal treatment can be technically challenging due to limited rubber dam use and reduced access for instrumentation & restoration in most cases due to restricted mouth opening. It can also be considered an alternative option in patients where extractions can pose an increased risk of osteoradionecrosis (ORN). It is advised to carry out root canal treatment (RCTs) with utmost care and maximum regard, taking into account the fragility of the periapical tissues [25].
Trismus
Trismus is defined as restricted mouth opening. Most commonly, the mouth opening would be 35 mm or less to be considered trismus. It occurs due to inflammation of the pterygomasseteric sling that occurs secondary to insult to the pterygoid muscles, mandible or masseter muscle. The proximity of large tumors close to the masticatory muscles or temporomandibular joint requiring extensive cancer treatment increases the likelihood of trismus [26].
Management
The prime goal of management is to restore the range of motion and alleviate pain and dysfunction. Early intervention is the key to the management of trismus. Physical therapies such as active and passive range of motion exercises manual therapy, including joint and muscle mobilization, are performed to minimize edema, remove fibrosis and increase the range of motion [27]. The patients are advised to massage the muscles associated with the joint area at least 2–3 times a day, in a circular direction for 30 s. Certain devices used for stretching the muscles of mastication are stacked tongue depressors, Therabite jaw motion rehabilitation system and Dynasplint Trismus System. The patients are usually advised to open the mouth to stretch the muscles 5–7 times during one session, hold their mouth open for 30 s and then close it. This has to be repeated 5–7 times per day. Although the literature review reports no significant differences between all these methods in improving trismus, it is recommended that the patients be self-motivated to employ jaw opening exercises using any of these methods under the supervision of the dental oncologist as early as possible [28, 29]. A Myofunctional therapist will be an important addition to the treating team. Patients with any type of jaw surgery will benefit from such an intervention. Such dedicated therapists may not be available in most instances when the dysphagia therapists can take care of this important component of the treatment. If conservative methods seem to be ineffective, coronoidectomy is considered as the next line of treatment.
Osteoradionecrosis
ORN is one of the chronic complications defined as the exposed irradiated bone that fails to heal over three months without a residual or recurrent tumor. Local factors such as tumor stage, site, radiation dose, radiation field, dental extraction, poor oral hygiene and smoking/tobacco use and systemic factors such as infection, immune-deficient states, comorbidities and malnutrition are certain risk factors that are associated with ORN. Clinically, the patient presents with pain, swelling, exposed bone, drainage, fistulization to mucosa/skin and trismus. The mandible is the most common site for ORN, especially the buccal cortices of the premolar & retromolar trigone, due to its higher density of compact bone with higher mineral content and lesser blood supply [30].
Management
The primary goal of a dentist must always be the prevention of ORN. If that is not possible, elimination of pain and associated infections and prevention of deformity (fistulas, bone exposures, bone defects, pathological fractures) must be considered. Conservative management strategy includes medication, local wound care and oral hygiene maintenance. Penicillin and Metronidazole are given as empiric therapy to treat the condition.
Tocopherols or Vitamin E are known for their capacity to scavenge the reactive oxygen species (ROS) generated during oxidative stress and protect cell membranes against lipid peroxidation. It also reduces fibrosis. Hence, it is advisable to perform extraction under Vitamin E and antibiotic coverage in post-radiation patients to facilitate rapid healing of the extraction socket. The Vitamin E shall be continued until complete healing of the extraction socket is established [30].
In those cases where delayed healing of the extraction socket is encountered, hyperbaric oxygen therapy (HBOT) is considered as the next line of therapy. It acts by increasing tissue oxygenation through angiogenesis, controlling infection, stimulating fibroblast replication and development of a collagen matrix (healing). HBOT is administered within a small monoplace chamber/multiplace chamber. A typical HBO session contains 20 sessions of HBO at 2–2.4 atmospheres, delivered in 90–120 min daily for 5–6 days per week prior to surgery, followed by ten such sessions after surgery [31]. The target tissue in HBOT is not the necrotic bone but the compromised living tissue under great metabolic demands to simply remain viable [32].
In advanced, symptomatic cases that have failed conservative measures, surgery is advocated. The indications for surgery are the presence of large intraoral ulcerations with/without fistula, pathological fracture or evident osteolysis of the inferior mandibular border. The preoperative workup using CT or MRI scans is done to rule out malignancy and estimate resection bony margins. Nevertheless, the definite margins are decided only intraoperatively until a healthy, bleeding bone is seen. The defect may be restored by reconstructive surgery using microvascular free flaps to restore the appearance and function of the jaw bone [33].
Chemotherapy
Chemotherapy is usually administered in an extensive stage of cancer and in cases with skeletal metastasis. The various forms of oral complications associated with chemotherapy are mucositis, xerostomia, infection & hemorrhage. Some of the anticancer drugs with high direct stomatotoxic potential include vincristine, vinblastine, cisplatin, 5-fluorouracil and doxorubicin [34].
Oral Management Before Chemotherapy
As mentioned in Table 1, the dentist must undergo a strict pre-treatment oral evaluation of patients planned for chemotherapy. Consultation with the physician is also paramount as it provides an insight into the type of treatment, the drug involved and the stage of the disease. All routine dental procedures such as scaling and polishing, restoration of decayed teeth must be considered. Avoid trauma to the tissues from dentures. Endodontic treatment can be considered for pulpally and periapically involved teeth if an adequate time frame is available before the therapy. Teeth with a poor prognosis must be extracted atraumatically, at least 7–10 days before, considering the possibility of delayed healing [35].
Oral Management During Chemotherapy
Mucositis and Xerostomia
Chemotherapy-induced mucositis is limited to non-keratinized surfaces (i.e., lateral and ventral tongue, buccal mucosa and soft palate). These ulcers typically arise within two weeks after initiation of chemotherapy. Chemotherapy also decreases salivary flow. Patients often complain of difficulty tolerating dental prostheses and are more prone to dental caries. They also report burning and tingling sensations on the tongue. Fissuring of the lips and ulcerations in the mouth may increase the risk for secondary fungal infections. The management strategy for mucositis and xerostomia associated with chemotherapy and radiotherapy is essentially the same. Patients often feel more comfortable sucking ice chips in the mouth. This is usually begun 5 min before administration of chemotherapy and replenished as needed for up to 30 min. This decreases the delivery of the chemotherapeutic agent to the oral mucosa by local vasoconstriction and reduced blood flow [36].
Infection
Infection must be properly diagnosed and treated quickly since systemic involvement becomes fatal. The mouth serves as the most frequent source of sepsis in granulocytopenic cancer patient. The typical signs of infection are obscured in these patients as there is a failure to mount an inflammatory response. The most consistent signs and symptoms of oral infection in myelosuppressed patients are pain, fever and oral lesions such as necrotizing ulcerative gingivitis (NUG). In cases of odontogenic infection, the individuals are treated with antibiotics, and the source of infection has to be eliminated depending on the extent of leukopenia and thrombocytopenia. Soft tissue infections are commonly seen in the gingiva in areas of localized necrotic area similar to NUG. These areas extend laterally & apically to involve larger areas. Oral hygiene measures are done by wrapping 2*2 inch sponges around the finger and povidone-iodine rinses to clean the necrotic areas, and antibiotic coverage is established [37].
Oral Bleeding Caused by Thrombocytopenia
In the bone marrow, declined myeloproliferation leads to thrombocytopenia and neutropenia, causing hemorrhagic tendency. Hence, it is advisable to avoid trauma from the prosthesis, restorations or sharp teeth. Those individuals requiring extractions must undergo qualitative & quantitative assessment of platelets, including platelet count and bleeding time prior to the procedure. Consultation with the treating physician is of utmost importance to establish the fitness of the patient in undertaking the invasive procedure.
Usually, atraumatic extractions can be done on an out-patient basis if the platelet count is above 50,000 cells /mm3. However, it is advisable to place a hemostatic agent to control anticipated bleeding, and primary closure must be established with sutures. In patients with platelet count less than 50000cells/mm3, hospitalization is preferred for surgical procedures since platelet transfusions may be required. Antibiotic coverage must be provided pre- and postoperatively when the leukocyte count is less than 2000 cells/mm3 [37].
Oral Management After Chemotherapy
Medication-Related Osteonecrosis of Jaws (MRONJ)
This is a relatively rare condition that occurs on exposure to treatment agents such as bisphosphonates (zoledronic acid), tyrosine kinase inhibitors (denosumab), inhibitors of mammalian target of rapamycin, immunotherapeutic agents or angiogenesis inhibitors when administered for skeletal metastases in cancer patients. It usually manifests as exposed bone in the orofacial region [38]. MRONJ is also associated with the advent of targeted therapy and immunotherapy in oncology. Duration of drug use, concomitant treatments, old age and other pathologies are important predisposing systemic factors for MRONJ. Tooth extraction, local anatomic factors and concomitant oral diseases are also important triggering factors. There are reports of association of Tyrosine kinase inhibitors like Sorafenib and Imatinib, antiangiogenic agents like Bevacizumab with MRONJ [39].
Management
Knowledge and awareness of dentists about the risk factors play a pivotal role in the prevention management of MRONJ. Prior to commencing the medications, it is advisable to counsel and create awareness among the patients regarding the potential side effects of the drugs and the importance of maintaining oral hygiene. Advise the patients to reduce sugar intake and initiate fluoride therapy to protect the teeth from decay in the future. Routine dental checkups must be carried out to identify the initiation of any decay process. Eliminate oral foci of infection by extracting teeth with a potentially poor prognosis. Ensure proper healing of the extraction site prior to the initiation of the drugs. Remove irritation from the ill-fitting prosthesis. Oral prophylaxis and restoration of decayed teeth must be done. In patients with established MRONJ, the management strategy includes eliminating pain, control of the infection and decreasing the progression of bone necrosis. The teeth with foci of infection and the bone sequestra must be removed under antibiotic coverage and curetted for proper healing.
Limitations Associated with Proper Administration of Oral Care and Maintenance of Oral Hygiene
Physical Disability or Loss of Dexterity of the Patient
The cancer treatment is associated with loss of normal anatomic structures. This compromises the normal functioning and loss of dexterity in maintaining proper oral hygiene by the patient. Also, the inaccessibility to the posterior regions of the oral cavity due to trismus can make dental treatment difficult.
Emotional and Psychological Disabilities of the Patient
Cancer diagnosis can sometimes be associated with emotional and psychological trauma to the patient. This can lead to a lack of motivation in maintaining a hygienic oral cavity.
Financial Constraints
The treatment of cancer can be quite expensive to the patient. Thus, many of them consider the cost of dental treatment to be an added financial burden to them and hence reluctant in seeking dental treatment.
Negligence Toward Dental Treatment
Some people are unaware of maintaining a hygienic oral cavity and the potential oral complications associated with cancer therapy. This attitude poses difficulty in administering oral care to such patients.
Importance of Smoking, Tobacco and Alcohol cessation
Smoking, tobacco and alcohol habits are important factors that has to be addressed during oral cancer treatment. More than being the causative agents, the cessation of such habits is also important in healing and preventing recurrences. Oral care can be significantly affected due to their continuation. The team should be equipped with trained personal who can handle such cessation counseling and management.
The overall assessment and management of different oral conditions associated with respect to cancer therapy are summarized in Table 1 and Table 2.
Conclusion
Oral care forms an integral part of the treatment regime of cancer. The onset of oral complications may deteriorate the overall quality of life of the patient, thereby hampering the cancer treatment of the patient. Thus, thorough knowledge of the potential complications and management is required for the prevention and management of them. It is highly recommended to encourage the patients to conduct a routine follow-up visit with the dentist at least once every 6 month; thorough oral hygiene maintenance and mouth opening exercises must be instituted, strict compliance with the fluoride therapy must be advocated. Also, the dentist must identify the carious lesions and any potential oral foci of infection as early as possible to avoid the need for extractions or other invasive procedures in the future. In radiation or chemotherapy patients, every precaution must be taken to prevent the onset of osteonecrosis of the jaw, which can severely deteriorate the overall well-being of the individual.
References
Coelho KR (2012) Challenges of the oral cancer burden in India. J Cancer Epidemiol. https://doi.org/10.1155/2012/701932
Sroussi HY, Epstein JB, Bensadoun RJ et al (2017) Common oral complications of head and neck cancer radiation therapy: mucositis, infections, saliva change, fibrosis, sensory dysfunctions, dental caries, periodontal disease, and osteoradionecrosis. Cancer Med 6:2918–2931. https://doi.org/10.1002/cam4.1221
Barrowman RA, Wilson PR, Wiesenfeld D (2011) Oral rehabilitation with dental implants after cancer treatment. Aust Dent J 56:160–165. https://doi.org/10.1111/j.1834-7819.2011.01318.x
Ariani N, Visser A, van Oort RP et al (2013) Current state of craniofacial prosthetic rehabilitation. Int J Prosthodont 26:57–67. https://doi.org/10.11607/ijp.3220
Geramipanah F, Fallahi Sichani S, Mirmohammadrezaei S, Ghodsi S (2016) Practical guidelines for fabricating mandibular guide flange prostheses: a new technique for measuring the flange angulation. Prosthet Orthot Int 40:528–531. https://doi.org/10.1177/0309364615574160
Jansma J, Vissink A, Spijkervet FK, Roodenburg JL, Panders AK, Vermey A, Szabó BG, Gravenmade EJ (1992) Protocol for the prevention and treatment of oral sequelae resulting from head and neck radiation therapy. Cancer 70:2171–2180
Andrews N, Griffiths C (2001) Dental complications of head and neck radiotherapy: Part 2. Aust Dent J 46:174–182. https://doi.org/10.1111/j.1834-7819.2001.tb00278.x
Marx RE, Johnson RP (1987) Studies in the radiobiology of osteoradionecrosis and their clinical significance. Oral Surg Oral Med Oral Pathol 64:379–390. https://doi.org/10.1016/0030-4220(87)90136-8
Starcke EN, Shannon IL (1977) How critical is the interval between extractions and irradiation in patients with head and neck malignancy? Oral Surg Oral Med Oral Pathol 43:333–337. https://doi.org/10.1016/0030-4220(77)90317-6
Matsuzaki H, Tanaka-Matsuzaki K, Miyazaki F et al (2017) The role of dentistry other than oral care in patients undergoing radiotherapy for head and neck cancer. Jpn Dent Sci Rev 53:46–52. https://doi.org/10.1016/j.jdsr.2016.09.003
Lalla RV, Sonis ST, Peterson DE (2008) Management of oral mucositis in patients who have cancer. Dent Clin North Am 52(1):61–77. https://doi.org/10.1016/j.cden.2007.10.002
Rastogi M, Khurana R, Revannasiddaiah S et al (2017) Role of benzydamine hydrochloride in the prevention of oral mucositis in head and neck cancer patients treated with radiotherapy (>50 Gy) with or without chemotherapy. Support Care Cancer 25:1439–1443. https://doi.org/10.1007/s00520-016-3548-9
Chitapanarux I, Tungkasamit T, Petsuksiri J et al (2018) Randomized control trial of benzydamine HCl versus sodium bicarbonate for prophylaxis of concurrent chemoradiation-induced oral mucositis. Support Care Cancer 26:879–886. https://doi.org/10.1007/s00520-017-3904-4
Zheng Z, Zhao X, Zhao Q et al (2021) The effects of early nutritional intervention on oral mucositis and nutritional status of patients with head and neck cancer treated with radiotherapy. Front Oncol 10:595632. https://doi.org/10.3389/fonc.2020.595632
Al-Nuaimi DSA, Al-Rawaq KJ, Noori AGM, Fattah MAN (2019) Acute xerostomia in head and neck radiotherapy. Int J Otorhinolaryngol Head Neck Surg 5:262–268
Nutting CM, Morden JP, Harrington KJ et al (2011) PARSPORT trial management group. Parotid-sparing intensity modulated versus conventional radiotherapy in head and neck cancer (PARSPORT): a phase 3 multicentre randomised controlled trial. Lancet Oncol 12:127–136. https://doi.org/10.1016/S1470-2045(10)70290-4
Zhang Y, Guo CB, Zhang L et al (2012) Prevention of radiation-induced xerostomia by submandibular gland transfer. Head Neck 34:937–942. https://doi.org/10.1002/hed.21859
Epstein JB, Stevenson-Moore P (1992) A clinical comparative trial of saliva substitutes in radiation-induced salivary gland hypofunction. Spec Care Dentist 12:21–23. https://doi.org/10.1111/j.1754-4505.1992.tb00401.x
Redding SW, Zellars RC, Kirkpatrick WR et al (1999) Epidemiology of oropharyngeal candida colonization and infection in patients receiving radiation for head and neck cancer. J Clin Microbiol 37:3896–3900
Nicolatou-Galitis O, Athanassiadou P, Kouloulias V et al (2006) Herpes simplex virus-1 (HSV-1) infection in radiation-induced oral mucositis. Support Care Cancer 14(7):753–762. https://doi.org/10.1007/s00520-005-0006-5
Albuquerque DF, de Souza TE, Amado FM, Arakawa C, Chinellato LE (2010) Evaluation of halitosis and sialometry in patients submitted to head and neck radiotherapy. Med Oral Patol Oral Cir Bucal 15:e850–e854. https://doi.org/10.4317/medoral.15.e850
Chai WL, Ngeow WC, Ramli R, Rahman RA (2006) Managing complications of radiation therapy in head and neck cancer patients: Part II. Management of radiation-induced caries. Singapore Dent J. 28:4–6
Lopes CCA, Soares CJ, Lara VC, Arana-Chavez VE, Soares PB, Novais VR (2018) Effect of fluoride application during radiotherapy on enamel demineralization. J Appl Oral Sci 27:e20180044. https://doi.org/10.1590/1678-7757-2018-0044
de Amorim DMG, Veríssimo AH, Ribeiro AKC et al (2021) Effects of ionizing radiation on surface properties of current restorative dental materials. J Mater Sci Mater Med 32:69. https://doi.org/10.1007/s10856-021-06543-5
de Araújo DA, da Mota MV, Carvalho BF (2021) Tratamento endodôntico em pacientes submetidos a radioterapia: revisão de literatura. Res Soc Dev. 10(7):e1010716127. https://doi.org/10.33448/rsd-v10i7.16127
Astradsson T, Laurell G, Ahlberg A, Nikolaidis P, Johansson H, Ehrsson YT (2018) Trismus in patients with head and neck cancer and 5-year overall survival. Acta Otolaryngol 138:1123–1127. https://doi.org/10.1080/00016489.2018.1511059
Shao CH, Chiang CC, Huang TW (2020) Exercise therapy for cancer treatment-induced trismus in patients with head and neck cancer: a systematic review and meta-analysis of randomized controlled trials. Radiother Oncol 151:249–255. https://doi.org/10.1016/j.radonc.2020.08.024
Lee R, Yeo ST, Rogers SN et al (2018) Randomised feasibility study to compare the use of Therabite® with wooden spatulas to relieve and prevent trismus in patients with cancer of the head and neck. Br J Oral Maxillofac Surg 56:283–291. https://doi.org/10.1016/j.bjoms.2018.02.012
van der Geer SJ, Reintsema H, Kamstra JI, Roodenburg JLN, Dijkstra PU (2020) The use of stretching devices for treatment of trismus in head and neck cancer patients: a randomized controlled trial. Support Care Cancer 28:9–11. https://doi.org/10.1007/s00520-019-05075-7
He Y, Ma C, Hou J, Li X et al (2020) Chinese expert group consensus on diagnosis and clinical management of osteoradionecrosis of the mandible. Int J Oral Maxillofac Surg 49:411–419. https://doi.org/10.1016/j.ijom.2019.06.015
Korambayil PM, Ambookan PV, Pillai S, Karangath RR, George D (2020) Role of hyperbaric medicine for osteoradionecrosis and post irradiation wounds: an institutional experience. Indian J Surg Oncol 11:469–474. https://doi.org/10.1007/s13193-020-01128-0
Dieleman FJ, Meijer GJ, Merkx MAW (2021) Does hyperbaric oxygen therapy play a role in the management of osteoradionecrosis? a survey of Dutch oral and maxillofacial surgeons. Int J Oral Maxillofac Surg 50:273–276. https://doi.org/10.1016/j.ijom.2020.06.014
Dai T, Tian Z, Wang Z, Qiu W, Zhang Z, He Y (2015) Surgical management of osteoradionecrosis of the jaws. J Craniofac Surg 26:e175–e179. https://doi.org/10.1097/SCS.0000000000001445
Sindhu SK, Bauman JE (2019) Current concepts in chemotherapy for Head and Neck Cancer. Oral Maxillofac Surg Clin North Am 31(1):145–154. https://doi.org/10.1016/j.coms.2018.09.003
Akashi M, Kishimoto M, Kusumoto J, Yakushijin K, Matsuoka H, Komori T (2018) Delayed socket healing after dental extraction in patients undergoing myelosuppressive chemotherapy for hematological malignancy: incidence and risk factors. J Oral Maxillofac Surg 76:2057–2065. https://doi.org/10.1016/j.joms.2018.05.023
Riley P, McCabe MG, Glenny AM (2016) Oral cryotherapy for preventing oral mucositis in patients receiving cancer treatment. JAMA Oncol 2:1365–1366. https://doi.org/10.1001/jamaoncol.2016.2680
McCaul LK (2012) Oral and dental management for head and neck cancer patients treated by chemotherapy and radiotherapy. Dent Update 39:135–138
Campisi G, Mauceri R, Bertoldo F et al (2020) Medication-related osteonecrosis of jaws (MRONJ) prevention and diagnosis: Italian consensus update 2020. Int J Environ Res Public Health 17:5998. https://doi.org/10.3390/ijerph17165998
Nifosì AF, Zuccarello M, Nifosì L, Hervas Saus V, Nifosì G (2019) Osteonecrosis of the jaw in the era of targeted therapy and immunotherapy in oncology. J Korean Assoc Oral Maxillofac Surg 45:3–8. https://doi.org/10.5125/jkaoms.2019.45.1.3
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Data availability
This is a review article and hence no data were collected.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Ethical approval.
Being a literature review, no formal ethical approval needed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nair, A.H., Patel, T., Nair, A.R. et al. Oral Management of Patients Undergoing Head and Neck Cancer Treatment. J. Maxillofac. Oral Surg. 23, 783–792 (2024). https://doi.org/10.1007/s12663-023-01911-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12663-023-01911-w