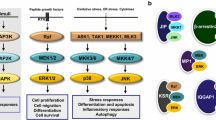
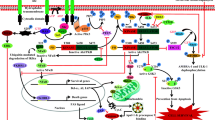
Abstract
Pyruvate kinase M2 (PKM2) is a key rate-limiting enzyme in glycolysis. It is well known that PKM2 plays a vital role in the proliferation of tumor cells. However, PKM2 can also exert its biological functions by mediating multiple signaling pathways in neurological diseases, such as Alzheimer’s disease (AD), cognitive dysfunction, ischemic stroke, post-stroke depression, cerebral small-vessel disease, hypoxic-ischemic encephalopathy, traumatic brain injury, spinal cord injury, Parkinson’s disease (PD), epilepsy, neuropathic pain, and autoimmune diseases. In these diseases, PKM2 can exert various biological functions, including regulation of glycolysis, inflammatory responses, apoptosis, proliferation of cells, oxidative stress, mitochondrial dysfunction, or pathological autoimmune responses. Moreover, the complexity of PKM2’s biological characteristics determines the diversity of its biological functions. However, the role of PKM2 is not entirely the same in different diseases or cells, which is related to its oligomerization, subcellular localization, and post-translational modifications. This article will focus on the biological characteristics of PKM2, the regulation of PKM2 expression, and the biological role of PKM2 in neurological diseases. With this review, we hope to have a better understanding of the molecular mechanisms of PKM2, which may help researchers develop therapeutic strategies in clinic.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pyruvate kinase (PK), as the key enzymes in regulating the final rate-limiting step of glycolysis, catalyzes the transfer of phosphate groups from phosphoenolpyruvate (PEP) to adenosine diphosphate (ADP) to produce pyruvate and adenosine triphosphate (ATP) [1, 2]. PK is composed of four isoenzymes encoded by two different genes (PKLR and PKM) in mammals [3], namely PKM1, PKM2, PKL, and PKR [4]. Among them, PKM2 is a key rate-limiting enzyme of glycolysis and a key regulator of tumor metabolism [1]. It has been shown to be overexpressed in various cancers and promote the proliferation and metastasis of tumor cells [1]. However, the capabilities of PKM2 are not limited to this. There is growing evidence that PKM2 also plays important roles in neurological diseases [5, 6]. Furthermore, PKM2 has multiple biological roles in addition to its abilities to regulate glycolysis and cell proliferation. And the enzymatic activity of PKM2 is complexly regulated by multiple signaling pathways, allowing cells to adapt to different physiological states [7].
In this review, we will introduce the biological characteristics of PKM2 and the regulation of PKM2 expression in non-neoplastic diseases, as well as its biological roles by mediating multiple signaling pathways, and focuses on the role of PKM2 in multiple signaling pathways related to neurological diseases. A better understanding of these contents has important implications for the treatment of neurological diseases in which PKM2 is involved.
The Biological Characteristics of PKM2
Studies have shown that the PKM gene produces a pre-mRNA product that is alternatively spliced to produce two different subtypes, PKM1 mRNA and PKM2 mRNA [8, 9]. The difference between the mRNA encoding PKM1 and PKM2 lies only in exon 9 containing PKM1 information or exon 10 containing PKM2 information [10, 11]. PKM1 is expressed in most adult tissues with high catabolic needs, such as muscles and brain [12]. However, PKM2 is present in all tissues of the embryonic stage and is gradually replaced by other isoenzyme forms in specific tissues during development [13]. Studies have shown that PKM2 is also expressed in other cells or tissues in addition to embryonic tissue, such as cancerous tissue, myocardium, liver, brain, stem cells, endothelial cells, monocytes, macrophages, T cells, and platelets [12, 14,15,16,17,18,19]. Notably, PKM1 is the most abundantly expressed subtype in nerve cells under normal conditions, while PKM2 is less expressed, mainly in proliferating cells, especially embryonic cells and neural progenitor cells of the hippocampus, cerebellum, and subventricular region [9, 20]. Studies have also shown that PKM1 is specifically expressed in neurons, while PKM2 is expressed in astrocytes and other glial cells in the nervous system [5, 6].
Functions of PKM2 are heavily regulated by multiple mechanisms, such as endogenous allosteric effectors and intracellular signaling pathways [21], and are largely dependent on its oligomerization, subcellular localization, and post-translational modifications [2, 22,23,24]. Post-translational modifications include phosphorylation, methylation, acetylation, oxidation, hydroxylation, lactylation, succinylation, and glycination [24, 25]. Oligomers of PKM2 mainly exist in high activity tetramer and low activity dimer/monomer forms [26, 27]. The increase in lactylation of PKM2 at K62 inhibits its tetramer-to-dimer transition, which promotes its pyruvate kinase activity and reduces nuclear distribution [24]. However, the phosphorylation, acetylation, sulfinylation, succinylation, and oxidation of PKM2 promote its conformational transformation from tetramers to dimers [28,29,30,31]. The oligomers of PKM2 are present in the cytoplasm in the tetramer forms and exhibit pyruvate kinase activity (metabolic enzyme activity) [32, 33]. PKM2 is localized in the nucleus and induced by various mechanisms to exert protein kinase activity [34]. PKM2 can also translocate to the nucleus through its dimer forms, regulating the transcription and expression of downstream genes [1, 27]. Furthermore, PKM2 nuclear translocation is thought to depend on various complex protein–protein interactions [22]. PKM2 dimers dominate in cancer cells and play an integral role in cancer metabolism [22]. Therefore, the diversity of PKM2’s biological roles is determined by the complexity of its biological characteristics.
Common Signaling Pathways that Regulate PKM2 Expression
The gene for the PKM2 protein is PKM [8, 9]. The synergistic effect of PKM transcription and the alternative splicing of the pre-mRNA lead to PKM2 protein expression [35]. The transcription of PKM and the alternative splicing of its pre-mRNA are regulated by multiple signaling pathways.
Hypoxia-inducible factor 1α (HIF-1α) is a common transcription factor that regulates PKM gene transcription. One study has shown that HIF-1α expression is upregulated in microglia after cerebral ischemia [32]. Moreover, under hypoxic conditions, prolyl hydroxylation of HIF-1α being inhibited, which leads to proteasome degradation of HIF-1α being inhibited, thereby stabilizing and activating HIF-1α protein [36]. HIF-1α dimerizes with HIF-1β and recruits the hypoxia response element (HRE) site of the PKM gene in the nucleus, thereby activating the transcription of the PKM gene [32, 34]. And the resulting HIF-1α-PKM2 complex can enhance PKM2 nuclear translocation in the dimer form [32]. In turn, PKM2 can interact directly with the HIF-1α subunit and promote transactivation of HIF-1 target genes [34]. The interaction between HIF-1α and PKM2 forms a positive feedback loop [34]. In addition, activation of the phosphoinositide 3-kinase (PI3K)/mammalian target of rapamycin (mTOR) signaling pathway upregulates HIF-1α-mediated PKM gene transcription [37, 38]. The AMP-activated protein kinase (AMPK)/mTOR signaling pathway can also promote HIF-1α protein expression, thereby upregulating PKM2 protein levels [39]. This signaling pathway links the regulation of PKM2 to hypoxia-ischemic conditions [40]. However, increased expression of phosphatase and tensin homolog (PTEN) can inhibit mTOR activation, thereby reducing the expression of PKM2 [41] (Fig. 1).
PKM2 expression and common signaling pathways for regulation of PKM2 expression. The pre-mRNA transcribed by the PKM gene is spliced by alternative splicing factors, such as PTBP1, hnRNPA1/A2, or SRSF3, to produce PKM2 mRNA. Due to the presence of post-translational modifications, oligomers of PKM2 mainly exist in tetramer and dimer/monomer forms. Signaling pathways, such as PI3K/AKT/mTOR/HIF-1α, AMPK/mTOR/HIF-1α, PTEN/mTOR/HIF-1α, EGFR/NF-κB/HIF-1α, EGFR/NF-κB, Sin1/mTORC2/AKT/PPAR-γ, Apelin-13/APJ, or Oct4, can regulate expression of the PKM gene. MiR-146a-5p interferes with translation of HIF-1α mRNA. CircSRRM4 can bind SRSF3 and inhibit its ubiquitination. The Mbd2/c-Myc and estradiol-17β/c-Myc pathways regulate the expression of hnRNPA1/A2. MiR-290/371 blocks the inhibition of c-Myc transcription by Mbd2. MiR-369 facilitates the translation of hnRNP mRNA. However, PHB2 directly inhibits the splicing effect of hnRNPA1/A2. MiR-124 interferes with translation of PTBP1 mRNA. RBM4 inhibits the splicing effect of PTBP1. MiR-143 and miR-338-3p interfere with translation of PKM2 mRNA. CircMAT2B and LINC00689 block the interference effect of miR-338-3p. However, miR-155-5p and miR-19a-3p can facilitate the translation of PKM2 mRNA. HIF-1α, hypoxia-inducible factor 1α; HRE, hypoxia response element; PI3K, phosphoinositide 3-kinase; mTOR, mammalian target of rapamycin; AMPK, AMP-activated protein kinase; PTEN, phosphatase and tensin homolog; EGFR, epidermal growth factor receptor; NF-κB, nuclear factor kappa enhancer binding protein; PPAR-γ, peroxisome proliferator-activated receptor γ; mTORC2, mammalian target of rapamycin complex 2; AKT, protein kinase B; APJ, angiotensin II receptor-like 1; SRSF3, arginine rich splicing factor 3; PTBP1, polypyrimidine tract binding protein 1; hnRNPA1/A2, heterogeneous nuclear ribonucleoprotein A1/A2; circSRRM4, circRNA serine/arginine repetitive matrix 4; miR-124, microRNA-124; RBM4, RNA-binding motif 4; PHB2, prohibitin 2; LINC00689, lncRNA long intergenic non-protein coding RNA 689; circMAT2B, circular RNA MAT2B; Mbd2, methyl-CpG binding domain protein 2
Furthermore, activation of the epidermal growth factor receptor (EGFR) mediates upregulation of protein kinase C (PKC) and nuclear factor kappa enhancer binding protein (NF-κB)-dependent PKM2 expression [35]. Among them, the activation of NF-κB can bind to GCGACTTTCC in the PKM gene promoter and activate its transcription [35]. NF-κB activation can also increase the expression of PKM2 by inducing HIF-1α expression [42]. In addition, the nucleus pluripotent factor Oct4 binds to the region of the PKM gene and directly controls the expression of PKM2 in embryonic stem cells [43]. Peroxisome proliferator-activated receptor γ (PPAR-γ) is a nuclear hormone receptor that specifically transcribes and regulates the expression of PKM2 [40, 44, 45]. Research has shown that the Sin1 (the basic component of mTORC2)/mammalian target of rapamycin complex 2 (mTORC2)/protein kinase B (AKT)-dependent PPAR-γ nuclear translocation can mediate the expression of PKM2 in thymic cells [46]. In addition, apelin is an endogenous ligand of angiotensin II receptor-like 1 (APJ), a G protein-coupled receptor, and both apelin and APJ receptors are distributed in vascular smooth muscle cells [47]. Apelin-13 promotes PKM2 expression in human aortic vascular smooth muscle cells in a dose- and time-dependent manner [47] (Fig. 1).
After the PKM gene transcription into the pre-mRNA, the alternative splicing of the pre-mRNA is regulated by several alternative splicing factors. Studies have shown that overexpression of alternative splicing factors, such as serine and arginine rich splicing factor 3 (SRSF3), polypyrimidine tract binding protein 1 (PTBP1), and heterogeneous nuclear ribonucleoprotein A1/A2 (hnRNPA1/A2), can reduce the ratio of PKM1 to PKM2, which contributes to glycolysis-dominated metabolism [8, 48,49,50,51,52]. Among them, SRSF3 collaborates with PTBP1 or hnRNPA1 to participate in the splicing of PKM mRNA [48] (Fig. 1).
One study found that the circular RNA (circRNA) serine/arginine repetitive matrix 4 (circSRRM4) can bind SRSF3 and inhibit its ubiquitination in epilepsy models, improving SRSF3-mediated the alternative splicing of PKM, thereby stimulating glycolysis in cells [51]. In addition, microRNAs (miRNAs) are small non-coding RNAs that regulate genes expression by targeting mRNAs [53]. MicroRNA-124 (miR-124) controls alternative splicing of PKM1 and PKM2 by regulating the expression of PTBP1 in pulmonary hypertension [52]. Moreover, the downregulation of miR-124 is responsible for the increase in PTBP1 expression, resulting in an increase in the ratio of PKM2 to PKM1, which can promote glycolysis and cell proliferation even under aerobic environment [52, 54]. In addition, EGFR activation can also stimulate the expression of PTBP1 [35]. However, the splicing regulator RNA-binding motif 4 (RBM4) antagonizes the function of PTB and induces the expression of PTB isoforms with reduced splicing activity in mesenchymal stem cells [55]. Furthermore, the overexpression of miR-369 can stimulate PKM2 splicing by stabilizing the translation of hnRNPA2B1 and enhance the induction of cell reprogramming by inducing pluripotent stem cell factors in embryonic stem cells [56]. Research has also shown that the estradiol-17β can enhance PKM splicing into the PKM2 subtype by activating the c-Myc/hnRNP axis in human embryonic stem cells [57]. Prohibitin 2 (PHB2) can also inhibit the alternative splicing function of hnRNPA1 by its C-terminus interacting directly with hnRNPA1 [50] (Fig. 1).
In addition, the long non-coding RNA(lncRNA) long intergenic non-protein coding RNA 689 (LINC00689) promotes the expression of PKM2 by interacting directly with miR-338-3p, thereby playing the role of competing endogenous RNA (ceRNA) [58]. Circular RNA MAT2B (circMAT2B) upregulates the expression levels of miR-338-3p target gene PKM2 by “sponging” miR-338-3p [59]. Studies have shown that the gene for the PKM2 protein is one of the target genes of miR-122 in the liver [53, 60]. Moreover, in polycystic ovary syndrome, the expression of exosome miR-143-3p in follicular fluid was upregulated, which inhibited PKM2 expression and glycolysis in cells, while the overexpression of miR-155-5p can significantly promote PKM2 expression and glycolysis in cells [61]. Similarly, miR-143 is significantly induced by ischemic injury in primary neurons, thereby inhibiting PKM2 expression [62]. Moreover, miR-19a-3p is also significantly induced by ischemic injury, which aggravates ischemic stroke by mediating glycometabolism [63]. Furthermore, the miR-290/371-methyl-CpG binding domain protein 2 (Mbd2)-Myc circuit facilitates glycolysis and reprogramming in human fibroblasts, and PKM2 is essential for miR-290-mediated reprogramming [64]. Among them, the miR-371 cluster is a human congener of the miR-290 cluster [64]. The miR-290 cluster reverses inhibition of the transcriptional activator Myc transcription by Mbd2 through targeting the transcriptional inhibitor Mbd2, a reader of methylated CpGs, and inhibiting its function, thereby regulating glycolysis and metabolic reprogramming [64]. In addition, miR-146a-5p in microglia is reduced in acute spinal cord injury, resulting in increased expression of HIF-1α [65] (Fig. 1).
To sum up, multiple signaling factors or signaling pathways can directly or indirectly affect PKM2 protein expression. Moreover, different diseases and types of stimulation/injury, as well as different cells, result in the signaling molecules that affect PKM2 expression are not completely the same.
PKM2 Exerts Its Biological Roles by Various Signaling Pathways and Modalities
PKM2 and Glycometabolism
PKM2 and Glycolysis
Glycometabolism is precisely regulated by several glycolytic enzymes, including PK, hexokinase, and pyruvate dehydrogenase [66]. Among the isoenzymes of PK, PKM1 is a tetrameric protein with enzymatic activity that efficiently converts PEP to pyruvate, contributing to pyruvate flow to support mitochondrial oxidative phosphorylation [16, 24]; however, PKM2 directs its pyruvate kinase activity through its own complex allosteric regulation, and the oligomers of PKM2 exist mainly in monomer or dimer forms, resulting in its enzymatic activity being lower than PKM1 [25]. The low catalytic activity of PKM2 dimers prevents pyruvate production at normal rates, leading to the accumulation of upstream glycolysis intermediates [34]. These intermediates are then transferred to other pathways, such as the pentose phosphate pathway (PPP), which supports biosynthesis in cells [34, 67]. PPP is an alternative metabolic pathway parallel to glycolysis in the nervous system, not only providing key intermediates for biosynthesis, but also controlling the fate of nerve stem/progenitor cells [68]. Thus, PKM2 is highly dimerized in cells or tissues with high nucleic acid synthesis [34]. When most PKM2 molecules are in highly active tetrameric conformations, they have a high affinity for PEP and bind to other glycolytic enzymes in the glycolytic enzyme complex, such as hexokinase, glyceraldehyde 3-phosphate dehydrogenase, phosphoglycerol transferase, and enolase, resulting in the degradation of glucose mainly to pyruvate and lactic acid and regenerating energy [2, 69, 70]. Notably, PKM2 has a low affinity for PEP even as a tetramer in the absence of fructose-1,6-bisphosphate (FBP) [21]. FBP binds to PKM2 at a site different from the active PEP binding site, which will promote and stabilize the tetramerization of PKM2 and increase the binding affinity between PEP and PKM2, so that the kinetic parameters of PKM2 are almost the same as those of PKM1 [21, 71, 72]. In addition, a study showed that PKM2 contains an inducible nuclear transposition signal that allows cells to regulate their glycolysis flow based on local energy states [5]. However, PKM1 is not regulated by allosteric and locks neurons into a steady state of glycolysis [5] (Fig. 2).
PKM2 is involved in the glycolytic process. The tetramer PKM2 catalyzes the production of pyruvate from PEP and is more stable in the presence of FBP. Multiple stimuli promote the tetramer-to-dimer transition of PKM2 by protein modifications. The dimer PKM2 leads to the transfer of glycolysis intermediates to the pentose phosphate pathway. The dimer PKM2 nuclear translocation interacts with HIF-1α and PHD3 to promote the transcription of glycolytic genes, ultimately leading to the Warburg effect. PEP, phosphoenolpyruvate; HIF-1α, hypoxia-inducible factor 1α; FBP, fructose-1,6-bisphosphate; PHD3, prolyl hydroxylase 3; GLUT1, glucose transporter 1; LDHA, lactate dehydrogenase A; PDK1, pyruvate dehydrogenase kinase 1; HRE, hypoxia response element
Warburg pointed out in 1920 that tumor cells, unlike their normally differentiated counterparts, have an increased rate of glucose uptake and lactate production in the presence of oxygen [73, 74]. This phenomenon is known as aerobic glycolysis or the Warburg effect [73, 74]. Aerobic glycolysis is capable of transferring glucose metabolites from ATP production to the synthesis of cellular building blocks (nucleotides, amino acids, and lipids) to meet proliferation needs [33]. Studies have shown that activated immune cells, such as macrophages, dendritic cells, and T cells, also have the ability to switch from oxidative phosphorylation to aerobic glycolysis in a manner similar to tumor cells [75,76,77,78]. FBP and serine have a synergistic allosteric effect on PKM2 [79]. And bound PKM2 has higher information transfer efficiency than the FBP/PKM2 or the serine/PKM2 [79]. Moreover, FBP-K433-T459-R461-A109-V71-R73-MG2-OXL and Ser-I47-C49-R73-MG2-OXL are two possible collaborative allosteric pathways [79]. Other amino acids, such as Asn, Asp, Val, and Cys, have also been shown to bind to the amino acid-binding pockets of PKM2 and modulate its oligomerization, substrate binding affinity, and activity [80]. However, when cells are stimulated by certain growth factors, the binding of phosphotyrosine peptides with PKM2 leads to the release of the allosteric activator FBP, thereby inhibiting the enzymatic activity of PKM2 and transferring glucose metabolites from energy production to anabolic processes [81]. In addition, as mentioned earlier, several post-translational modifications, such as phosphorylation, acetylation, sulfinylation, succinylation, and oxidation, facilitate the conversion of PKM2 to its dimer. The dimer PKM2 is a key regulator of aerobic glycolysis, promoting metabolic reprogramming and lactic acid production [12]. With a decrease in PKM2 activity, the monomer/dimer PKM2 can transfer to the nucleus and form a complex with HIF-1α and prolyl hydroxylase 3 (PHD3) on the promoter of HIF-1α, which then regulates the expression of many glycolysis-related genes, such as glucose transporter 1 (GLUT1), lactate dehydrogenase A (LDHA), and pyruvate dehydrogenase kinase 1 (PDK1) [76, 78, 82]. Nuclear PKM2 dimers can also induce c-Myc expression by their histone kinase action, promoting the expression of glycolytic proenzymes that induce the Warburg effect [73]. An imbalance in favor of PKM2 leads to the accumulation of glycolytic metabolites and an increase in lactic acid production [16, 78]. And the PKM2-driven change is a major component of the Warburg effect [16, 78]. In addition to playing a significant role in many cancers [22, 83], this effect is also evident in induced neurons (iNs) and postmortem prefrontal cortex tissue in patients with AD [16]. One study showed that PKM2 promotes Warburg effect-like glycolytic reprogramming in older neurons, and the expression of several genes induced by the PKM2/HIF1α signaling pathway is involved in the production of precursor metabolites and energy and the metabolism of carbohydrates [16]. In addition, boosting pyruvate kinase activity of PKM2 can lead to a decrease in lactic acid production, which is known as the PKM2 paradox in the Warburg effect [24] (Fig. 2).
Potential Effects of Glycolytic Metabolites on the Nervous System
Neuronal activity is a high-energy-demanding process that recruits all nerve cells adapted to their metabolism to maintain neuronal energy and normal physiological functions [84]. PKM2-mediated aerobic glycolysis plays a critical role in energy metabolism and proliferation of tumor cells, but it may not be suitable for normal metabolism of neurons. One study showed that chemical inhibition of PKM2 nuclear translocation can reduce PKM2 load in the nucleus and restore metabolic patterns in mature neurons [16]. Moreover, the inhibition of PKM2 can slow down the rate of glycolysis to prevent the toxic effect of glycolytic products on neurons [16, 83, 85]. This phenomenon may be related to the fact that neurons compensate for their energy shortages mainly rely on oxidative phosphorylation and cannot use aerobic glycolysis or mitochondrial biogenesis [85]. Similar conclusions have been reached in studies of other diseases. For example, one study found that the activation (tetramerization) of PKM2 can increase glucose metabolic flux by activating the glycolytic pathway, which inhibits the accumulation of highly glucose-induced toxic glucose-derived end products in podocytes [29].
However, lactic acid produced by the glycolysis pathway appears to be essential for regulating neuronal functions. Lactic acid in the brain is mainly formed from glucose or glycogen in astrocytes under normal physiological conditions [51, 86]. Glucose is transferred from cerebral vessels to astrocyte via glucose transporters and then converted to pyruvate and lactic acid by catalysis by PKM2 and lactate dehydrogenase isoform 5 (LDH5) [87, 88]. Lactic acid is transferred from astrocytes to nearby neurons via monocarboxylate transporters (MCTs) to meet the energy needs of neurons and provide signals that regulate neuronal functions, including plasticity, excitability, and memory consolidation [6, 86, 87, 89]. The LDH1 converts lactic acid back to pyruvate in neurons, which is then transferred to mitochondria via the tricarboxylic acid cycle for aerobic energy production [88]. The study showed that L-lactate in neurons can stimulate the expression of synaptic plasticity-related genes, such as Arc, c-Fos, and Zif268, by the N-methyl-D-aspartate (NMDA) receptor (NMDAR)/extracellular signal-regulated protein kinases 1 and 2 (ERK1/2) signaling pathway [90]. Failure to utilize lactic acid can lead to increased neuronal death due to glutamate [91]. In addition, PKM2 deletion mediates impaired lactate homeostasis and mitochondrial ATP production in myelinating Schwann cells of the sciatic nerve, resulting in slowed mitochondrial transport of the axon, the axon terminal retraction of the muscle, and cellular stress of motor neurons [89]. This suggests that aerobic glycolysis is necessary to maintain transport of peripheral nerve axons and neuromuscular junctions [89].
Therefore, the role of PKM2-mediated aerobic glycolysis on the nervous system cannot be generalized. The biological activity of neurons mainly depends on the energy provided by oxidative phosphorylation, and the right amount of lactic acid is also essential for maintaining neuronal energy requirements and physiological functions. However, excessive accumulation of glycolytic metabolites has a toxic effect on neurons.
PKM2 and Apoptosis
Apoptosis is a tightly regulated cell death program involving the caspase cascade and the B-cell lymphoma 2 (Bcl-2) family, such as the anti-apoptosis members Bcl-2 and Bcl-xl, as well as pro-apoptosis members Bcl2-associated X (Bax) and Bak [92, 93]. PKM2 can regulate apoptosis by various signaling pathways.
The Change in Enzymatic Activity (the Dimer-to-Tetramer Transition) of PKM2 Can Antagonize Apoptosis
Vallée et al. [94] suggest that inactivation of PKM2 may lead to the death of neurons in AD. A study also showed that nuclear PKM2 combines with the signal transducers and activators of transcription 3 (STAT3) and HIF1α to induce relevant genes expression, promoting damage signaling, cytokine activity, and apoptosis of elderly neurons in AD iNs [16]. Conversely, inhibition of non-metabolic nuclear effect of PKM2 in neurons not only leads to a decrease in toxic glycolytic metabolites but also reverses the loss of fate, thereby restoring neuronal braking to prevent apoptosis [16]. This seems to suggest the difference between human elderly neurons and tumor cells that promote their proliferation by the PKM2/STAT3 signaling pathway [95]. In addition, PKM2 is also able to regulate apoptosis in other non-neoplastic diseases. Zhou et al. [96] found that pharmacological activation (tetramerization) of PKM2 alleviated the death process of photoreceptor in the rd10 mouse model. Zhao et al. [97] found that PKM2 accumulates in mitochondria and is highly acetylated during lung ischemia/reperfusion injury. In contrast, the K433 deacetylation of PKM2 leads to a change in its enzymatic activity, which reverses Bcl-2 degradation and significantly reduces apoptosis [97] (Fig. 3).
PKM2 is involved in the regulation of apoptosis. The deacetylation of mitochondrial PKM2 gives it the effect of inhibiting Bcl2 degradation, which then inhibits oxidative stress-induced apoptosis. PKM2 inhibits ER stress but promotes the inactivation of p-AKT in nerve cells, which then regulates apoptosis. Nuclear PKM2 can activate HIF-1α, STAT3, or block P53, which then regulates the transcription of glycolytic genes, inflammatory genes, or apoptotic genes. Excess glycolytic metabolites are neurotoxic. However, lactic acid regulates neuronal excitability and synaptic plasticity and provides a source of energy. Bcl-2, B-cell lymphoma 2; STAT3, signal transducers and activators of transcription 3; HIF-1α, hypoxia-inducible factor 1α; AKT, protein kinase B; ROS, reactive oxygen species; ER, endoplasmic reticulum
Decreased Expression of PKM2 Can Regulate Apoptosis
Zhao et al. [98] found that silencing PKM2 promoted Bcl-2 expression and reduced the level of Bax and the ratio of Bax to Bcl-2 in the nerve growth factor-PC12 cells treated with hyperglycemia and 6-hydroxydopamine (6-OHDA). Several studies have also shown that PKM2 mediates the inactivation of phosphorylated PI3K/AKT to participate in neuronal apoptosis in hypoxic-ischemic encephalopathy and traumatic brain injury, as well as anesthesia-induced apoptosis of hippocampal neurons [99,100,101]. Conversely, silencing PKM2 can improve neuronal apoptosis in these diseases [99,100,101]. This appears to be different from PKM2 promoting tumor cells proliferation by mediating phosphorylation of the PI3K/AKT signaling pathway [102] (Fig. 3).
In summary, the change in enzymatic activity (the dimer-to-tetramer transition) or silencing of PKM2 can antagonize apoptosis. Moreover, the way PKM2 regulates apoptosis in different cells is not entirely the same. For example, PKM2 leads to apoptosis by mediating dephosphorylation of PI3K/AKT and phosphorylation of STAT3 in the nervous system [16, 99,100,101]. However, PKM2 promotes the proliferation of various tumors by mediating phosphorylation of PI3K/AKT or STAT3 [95, 102]. Therefore, further research and exploration of the similarities and differences in metabolic switches between neurons or other non-tumor cells and different types of cancer are needed (Fig. 3).
Interestingly, the above research results still have some controversy, and there are even completely opposite research results. Gu et al. [103] found that MiR-326 reduced PKM2 expression in SH-SY5Y cells treated with Aβ25-35, leading to persistent endoplasmic reticulum stress and subsequent apoptosis. Kang et al. [87] found that the loss of PKM2 increased the degree of hippocampal neuronal damage and lactic acid metabolism disorders after global cerebral ischemia (GCI). Conversely, the neuronal death was significantly reduced, and the neuronal survival was saved after lactate supplementation, which may be related to the ability of lactic acid to maintain energy metabolism in neurons [87]. Inoue et al. [104] found that overexpression of PKM2 improved neuronal apoptosis and defects in zebrafish induced by the 5′ tRNA fragments derived from tyrosine pre-tRNA (5′ Tyr-tRF). 5′Tyr-tRF binds directly to PKM2, and it may enhance the phosphorylation of p53 at serine 15 by inhibiting the interference of nuclear PKM2 on the phosphorylation of classical apoptosis-associated protein p53 [104]. These findings suggest that overexpression of PKM2 appears to be beneficial for the anti-apoptotic effects of cells. However, which oligomerized form of PKM2 exerts an anti-apoptotic effect has not been clearly identified in these studies (Fig. 3).
Thus, PKM2 regulates apoptosis by several not complete same signaling pathways in different diseases or cells. Moreover, there is some controversy among some studies. This phenomenon may be related to the oligomerization, subcellular localization, and post-translational modification of PKM2 in different diseases or cells.
PKM2 Is Associated with Cell Proliferation, Differentiation, or Migration
Cell proliferation is an important life characteristic of an organism and the basis for its growth, development, reproduction and heredity. It is precisely controlled by genetically programmed regulatory pathways. In normally developing tissues, these pathways are able to specify when and where cells can increase or subtract. Both cancer and normal cells utilize the same “universal molecular toolbox” to coordinate cell proliferation. However, compared to normal cells, cancer cells have the abilities to proliferate independently of exogenous growth-promoting or growth-inhibitory signals, to invade surrounding tissues and metastasize to distant sites, to elicit angiogenesis responses, and to evade mechanisms that limit cell proliferation, such as apoptosis and replicative senescence [105]. This allows cancer cells to survive and multiply while normal cells cannot survive and proliferate. The cell cycle, as a complex process, is a core event that regulates cell proliferation [106, 107]. It consists of DNA synthesis (S) and mitosis (M), which are separated by two intervals (G1 and G2); these phases are carried out in the order of G1-S-G2-M [107, 108]. Cell cycle switching is primarily driven by cyclin-dependent kinases (CDKs) and cyclins [108]. It is well known that metabolic regulation plays a key role in cell proliferation, differentiation, or migration [109].
One study showed that the deletion of PKM2 led to PKM1 expression and proliferation arrest in primary cells [109]. PKM1 expression impairs nucleotide production and the ability to synthesize DNA, as well as progression of the cell cycle; however, the expression of PKM2 supports influx into metabolic pathways to support DNA synthesis [109]. Qiao et al. [110] found that a-synuclein regulates glucose metabolism by the PKM2-dependent signaling pathways in microglia, thereby promoting the cell migration. In traumatic spinal cord injury (SCI), PKM2 nuclear translocation further interacts with β-catenin and p27, and they are recruited into the cyclin D1 gene (CCND1) promoter, regulating the expression of the gene CCND1, thereby promoting astrocytes proliferation [111]. Lu et al. [112] found that the inhibition of PKM2 can lead to significant downregulation of protein levels of β-catenin, c-Myc, and CCND1, as well as a decrease in the number of hippocampal microglia. Similarly, Wu et al. [30] demonstrated that PKM2 located in the nucleus rescues cell survival by mediating the β-catenin/T-cell factor 4 (TCF4) signaling cascade under the conditions of ischemic injury. β-catenin and its induced TCF4 are combined with upregulating gene induction of Myc, CCND1, and Sgk1, thereby regulating cell proliferation and anti-apoptotic effects [30, 113,114,115] (Fig. 4).
PKM2 is involved in the proliferation, differentiation, and migration of cells. Nuclear PKM2 participates in the proliferation, differentiation, and migration of cells via activating signaling pathways, such as β-catenin/TCF4, β-catenin/P27, STAT3, STAT3/FAK, HIF-1α, or NF-κB/HIF-1α. HIF-1α-mediated glycolysis provides an energy source for the proliferation, differentiation, and migration of cells. HIF-1α-mediated VEGF can participate in the expression of cell proliferative genes via the MAPK/ERK pathway. CCND1, cyclin D1; MAPK, mitogen-activated protein kinase; TCF4, T-cell factor 4; FAK, focal adhesion kinase; VEGF, vascular epithelial growth factor; HIF-1α, hypoxia-inducible factor 1α; HRE, hypoxia response element; NF-κB, nuclear factor kappa enhancer binding protein; STAT3, signal transducers and activators of transcription 3
In addition, STAT3 is a transcription factor that regulates proliferation, growth, and apoptosis [116]. Chen et al. [40] found that PKM2 accelerates cell migration by regulating key adhesion/migration factors, such as the focal adhesion kinase (FAK), and nuclear PKM2 dimers can directly phosphorylate STAT3, resulting in STAT3 activation and downstream associated gene transcription. Activation of FAK and STAT3 can increase angiogenesis, neurogenesis, and functional recovery in adult mice with ischemic stroke [40]. PKM2 can also mediate the activity of the MAPK/ERK pathway by activating the vascular epithelial growth factor (VEGF), thereby upregulating oligodendrocytes proliferation [117]. VEGF can promote the proliferation and differentiation of neural precursor cells, neural stem cells, and even glial cells, playing a vital role in brain injury repair and neuronutrition [117, 118]. ERK1/2, as a member of the mitogen-activated protein kinase (MAPK) signaling pathway, has been shown to regulate cell proliferation, differentiation, and motility, as well as cytoskeletal construction [117, 119]. In addition, one study showed that extracellular PKM2 can enhance the proliferation of skeletal muscle cells and the axon growth of cultured neurons [120]. Extracellular PKM2/the valosin-containing protein (VCP) signaling molecules in neurons drive ATPase activity in chronic SCI, mediating axon increase and motor function recovery [121] (Fig. 4).
In summary, PKM2 regulates gene expression of cell proliferation by multiple signaling pathways, especially gene expression of proteins related to driving cell cycle transition, thereby promoting cell proliferation.
PKM2 and Inflammatory Response
Inflammation is a well-controlled process triggered by signals from damaged tissues or infections, aimed at re-establishing tissue homeostasis [21]. The inflammatory reaction involves metabolic reprogramming, directing nutrients to the efficient production of ATP, and the synthesis of macromolecules in order to adapt to a highly active metabolic state [6, 21]. These macromolecules are required for the production of pro-inflammatory mediators, cytoskeletal rearrangements, and proliferation of immune cells [21]. Compared with the oxidative phosphorylation of mitochondria, the glycolytic pathway, although less efficient in the utilization of glucose, can produce more energy per unit time during immune cell hypermetabolism to accommodate the rapidly increasing ATP requirement [6, 122]. Therefore, the metabolic conversion from oxidative phosphorylation to glycolysis is the way to adapt to this high metabolic demand. PKM2 regulates aerobic glycolysis and is an important regulator of metabolism and function of inflammatory cells, implying its potential role in inflammation [19]. At the same time, the dimer PKM2 can also be used as a transcription factor for the expression of target genes in inflammation to promote inflammatory responses [9, 123]. Moreover, HIF-1α, which interacts with PKM2, can also play an important role in the metabolic reprogramming of inflammatory cells by promoting the expression of target genes in inflammation [124].
PKM2 Is Involved in the Activation of Macrophages and Their Mediated Local or Systemic Inflammatory Responses
Toll-like receptors (TLRs) play a key role in regulating inflammation and abnormal activation of immune cells [125, 126]. Activation of TLR2 can induce PKM2 nuclear transposition [127]. Zhang et al. [125] found that PKM2 can enhance the activation of TLR4, TLR7, and TLR9 by activating proline-rich tyrosine kinase 2 (Pyk2). And they speculate that PKM2 may promote Pyk2 activation by promoting glycolysis and ATP production [125]. Histone deacetylases (HDACs) can drive inflammation mediated by innate immune cells [128, 129]. One study showed that class IIa HDACs (HDAC4, 5, 7, and 9), specifically HDAC7, are key molecules that link TLR-induced aerobic glycolysis and inflammatory responses in macrophages [128]. Moreover, the HDAC7-PKM2 complex, acting as an immune metabolic signaling center, mediates the deacetylation of PKM2 at lysine 433 and enhances its pro-inflammatory function [128]. In addition, Wang et al. [24] demonstrated that the lactation of PKM2 inhibits its tetramer-to-dimer transition, promotes its pyruvate kinase activity, and reduces its nuclear distribution, thereby promoting the transition of pro-inflammatory macrophages to repair phenotypes and limiting the inflammatory response. Li et al. [130] also found that the downregulation of the intracellular ratio of dimer/monomer-to-tetramer of PKM2 led to the inhibition of nuclear translocation of functional PKM2 in macrophages, which then increased the percentage of infiltrated M2 macrophages in the brain after stroke. In addition, Palsson-McDermott et al. [82] found that PKM2 upregulates and phosphorylates in lipopolysaccharides (LPS)-treated macrophages and forms a complex with HIf-1α, which can bind directly to the promoter of interleukin (IL)-1β. They believe that PKM2 is a key determinant of LPS activating macrophages and promoting the inflammatory response. Wang et al. [31] came to a similar conclusion, and they believe that succinylation of PKM2 promotes the conversion of PKM2 from tetramer to dimer. Moreover, the PKM2/HIF-1α/peroxisome proliferator-activated receptor-γ co-activator 1-α (PGC-1α) signaling pathway can also regulate polarization of macrophages and inflammatory responses [131] (Fig. 5).
PKM2 is involved in inflammatory responses. Multiple stimuli promote PKM2 nuclear translocation via TLR4-mediated signaling pathways. Nuclear PKM2 mediates the expression of inflammatory genes via signaling pathways, such as ATF2, STAT3, STAT3/NF-κB, HIF-1α/NF-κB, or HIF-1α, ultimately leading to inflammation. Lactic acid produced by the glycolytic pathway is involved in the transcription of inflammatory genes and can regulate the expression of inflammatory genes by activating EIF2AK2. In addition, lactic acid can interact with HDAC to block the deacetylation of HMGB1. Acetylated HMGB1 chelates it within the cytoplasmic vesicle and subsequently releases it into the extracellular environment. The HMGB1-mediated TLR4/MyD88/TRAF6 signaling pathway promotes neuroinflammatory responses and damage of cells. HDAC7, histone deacetylase 7; TLR4, toll-like receptor 4; PGC-1α, peroxisome proliferator-activated receptor-γ co-activator 1-α; HMGB1, high-mobility group box 1; NLRP3, NLR family, pyrin domain containing 3; AIM2, absent in melanoma 2; EIF2AK2 or PKR, eukaryotic translation initiation factor 2 alpha kinase 2; MyD88, myeloid differentiation factor 88; TRAF6, TNF receptor-associated factor 6; ATF2, activation transcription factor 2; TNF, tumor necrosis factor; IL, interleukin; JNK, c-Jun N-terminal kinase; NF-κB, nuclear factor kappa enhancer binding protein; STAT3, signal transducers and activators of transcription 3; PEP, phosphoenolpyruvate
In addition, Rao et al. [132] and Yang et al. [78] confirmed that PKM2-mediated aerobic glycolysis contributes to the activation of macrophages and the resulting inflammatory response. Moreover, the PKM2/HIF1α glycolytic pathway plays a key role in regulating the release of high-mobility group box 1 (HMGB1) by activated macrophages [78, 133]. In this signaling pathway, lactic acid produced by glycolysis can increase hyperacetylation of HMGB1 by inhibiting HDAC activity [78, 134]. Activated macrophages/monocytes acetylating HMGB1 in their nuclear localization sequences, leading to chelation of HMGB1 within cytoplasmic vesicles and subsequent release into the extracellular environment [78]. HMGB1 is a late mediator of fatal systemic inflammation [133]. One study showed that PKM2-mediated glycolysis promotes the activation of NLRP3, also known as NLR family, pyrin domain containing 3, and absent in melanoma 2 (AIM2) inflammasomes by regulating phosphorylation of eukaryotic translation initiation factor 2 alpha kinase 2 (EIF2AK2, also known as PKR) in macrophages, thereby promoting the release of IL-1β, IL-18, and HMGB1 by macrophages [135]. In this signaling pathway, lactic acid-mediated phosphorylation of EIF2AK2 is the main event that controls the activation of inflammasomes in macrophages [135]. In addition, nuclear PKM2-mediated signaling pathways related to inflammatory responses also include JAK1-STAT1/3, NF-κB, MAPK, p65, inducible nitric oxide synthase (iNOS), and cyclooxygenase-2 (COX-2) in macrophages, which are activated by PKM2 to further promote the release of pro-inflammatory cytokines [136] (Fig. 5).
PKM2 Is Involved in the Activation of Glial Cells and Their Mediated Neuroinflammatory Responses
There is evidence that PKM2 plays a key role in neuroinflammation and central nervous system disorders [23, 137]. Zhang et al. [137] found that PKM2 aggravates oxygen–glucose deprivation and reoxygenation induced neuroinflammatory responses and damage of cells by activating the HMGB1-mediated TLR4/myeloid differentiation factor 88 (MyD88)/tumor necrosis factor (TNF) receptor-associated factor 6 (TRAF6) signaling pathway. TLR4 belongs to the type 1 transmembrane proteins family with an extracellular leucine-rich repeat domain and an intracellular domain homologous to Toll and the IL-1 receptor in mammals [138]. MyD88 is a transfer factor of TLR4 and mainly promotes signal transduction of TLR4 [138]. Furthermore, PKM2 can mediate activation of glycolysis and NLRP3 inflammasomes in mouse models of LPS-induced neuroinflammation [139] (Fig. 5).
Activation of glial cells and production of inflammatory mediators are the main events of neuroinflammation [140]. Microglia, as tissue-resident macrophages of the central nervous system, are key nervous system-specific immune cells [141, 142]. PKM2 plays a potential role in microglia-mediated neuroinflammation [23]. One study showed an increase in PKM2 expression in LPS-treated microglia cultures [9]. PKM2 can be recruited as a transcription factor and localized in the nucleus under inflammatory conditions [9]. Moreover, microglia polarize into M1-type cells with pro-inflammatory activity in inflammatory diseases, which are activated along with the TLR4 signaling [143]. Inhibition of PKM2 can inhibit polarization of BV2 cells and activation of the TLR4 signaling [143]. Similarly, Zhai et al. [144] found that NADPH oxidase 4 (NOX4) promotes PKM2 expression in microglia treated with LPS and interferon-γ (IFN-γ) by increasing the expression of reactive oxygen species (ROS), thereby accelerating polarization of M1-type cells and production of inflammatory factors. Furthermore, Li et al. [23] found that the dimer PKM2 directly interacts with the pro-inflammatory transcription factor activation transcription factor 2 (ATF2) and regulates ATF2 phosphorylation and nuclear accumulation to bridge glycolysis and pyroptosis in microglia, which may be a key crosstalk between metabolic reprogramming and neuroinflammation in central nervous system. In addition, lactic acid can also further promote the release of pro-inflammatory cytokines by glial cells under pathological conditions [145] (Fig. 5).
In addition, p300 acetyltransferase can catalyze PKM2 acetylation to enter the nucleus and bind to histone 3 (H3) and STAT3 [146]. Moreover, Gao et al. [32] found that stroke-mediated translocation of PKM2 into the nucleus in a dimer forms in microglia, followed by phosphorylation and activation of the transcription factor STAT3, thereby promoting transcription of pro-inflammatory genes and subsequent production of pro-inflammatory factors TNF-a and IL-1β. Dhanesha et al. [17] also found that nuclear PKM2 regulates excessive activation of neutrophils after cerebral ischemia by promoting STAT3 phosphorylation, driving the thrombo-mediated inflammatory response, thereby aggravating the severity of stroke, and it is likely that the PKM2/STAT3/NF-κB axis plays a role in it. The PKM2/STAT3 signaling pathway also plays an important role in the activation of astrocytes. Wei et al. [6] found that activated astrocytes after LPS treatment take up more glucose to increase aerobic glycolysis and promote sustained activation of active astrocytes and HMGB1 secretion by the PKM2/STAT3 signaling pathway. In addition, knocking out PKM2 in epilepsy inhibits microglial activation and secretion of inflammatory factors, such as complement component 1q (C1q), TNF-α, and IL-1α, by inhibiting the activation of NF-κB, resulting in decreased expression of complement component 3 (C3) in astrocytes and subsequent neuronal damage caused by the interaction of C3 with neuronal C3a receptors (C3aR) [147] (Fig. 5).
Thus, the non-enzymatic nucleogenesis of PKM2, as well as PKM2-mediated metabolic reprogramming and glycolytic products, play important roles in various inflammatory diseases by regulating multiple signaling pathways.
PKM2 and Pathological Autoimmune Responses
Autoimmunity is the phenomenon in which the body’s immune system responds to autoantigens and produces autoantibodies and/or self-sensitized lymphocytes [148]. Autoimmune diseases are diseases in which the body reacts to autoantigens and causes damage to its own tissues [148]. The emerging field of immunometabolism focuses on the functional link between metabolic reprogramming and the immune system, which provides an additional dimension to understanding immunity in health and disease [149].
Elevated PKM2 levels have been reported in several autoimmune diseases, such as autoimmune encephalomyelitis, rheumatoid arthritis (RA), inflammatory bowel disease, idiopathic inflammatory myopathy, and dermatomyositis/polymyosis [150,151,152,153]. A study showed that CD4 + T cells are a population of immune cells that play a key role in the immune response [34]. They induce B cells to produce antibodies; induce microbicidal activity of macrophages; recruit neutrophils, eosinophils, and basophils to the site of infection; and produce cytokines and chemokines to induce the immune response [154]. Among them, helper T cells 17 (Th17) and Th1 cells play important roles in the pathogenesis of autoimmune diseases, and their energy source relies on glycolysis [155, 156]. A study has shown that PKM2 is necessary for the development and differentiation of Th1 and Th17 cells [155]. Angiari et al. [153] found that inducing PKM2 tetramerization and inhibiting its nuclear translocation can limit the development of Th17 and Th1 cells and improve the immune response in experimental autoimmune encephalomyelitis. Similarly, PKM2 was expressed in T cells infiltrating the central nervous system in a mouse model of multiple sclerosis, and the regulation of PKM2 may provide a new avenue for the treatment of multiple sclerosis [157]. In addition, dendritic cells (DCs) play a central role in innate and adaptive immunity [158, 159]. One study showed that the c-Jun N-terminal kinase (JNK) signaling pathway stimulates the binding of p300 and PKM2 when DCs are activated by LPS, resulting in PKM2 acetylation and nuclear translocation [158]. Subsequently, nuclear PKM2 binds to c-Rel to enhance IL12p35 expression, which then regulates differentiation of Th1 cells [158]. Moreover, PKM2 with low enzyme activity promotes glycolysis and fatty acid synthesis, helping DCs meet the demand for biological macromolecules [158].
These findings suggest that PKM2-mediated metabolic and non-metabolic pathways can modulate pathological autoimmune responses by promoting differentiation and activation of several immune cells. Therefore, it plays a crucial role in autoimmune diseases.
Antioxidant Damaging Effects of PKM2
The body produces excess ROS and reactive nitrogen species (RNS) in response to various harmful stimuli [160]. They accumulate in tissues or cells and cause an imbalance between high ROS/RNS and low antioxidant defenses, which will lead to a state of oxidative stress and cause cytotoxic reactions and tissue damage [160,161,162]. Therefore, the body’s antioxidant capacity is essential for maintaining the function of cells or tissues. PKM2 is an important signaling molecule in the body to regulate antioxidant capacity and plays a crucial role in oxidative damage.
Zhu et al. [163] found that light-induced oxidative stress levels of retinal cone cells in mouse were significantly reduced after treatment with PKM2 inhibitors, which might be related to upregulation of PPP. The S-nitrosation (decreased enzyme activity) or inhibition of PKM2 can increase substrate flow through PPP to produce reducing equivalents, such as nicotinamide adenine dinucleotide phosphate hydride (NADPH) and reduced glutathione (GSH), and protect cells from oxidative stress [163,164,165,166]. This is because PKM2 is slower than PKM1 in enzymatic activity, and the decrease in its pyruvate kinase activity promotes an anabolic pathway that replaces the glycolytic pathway, i.e., PPP, resulting in generation of reducing equivalents to prevent oxidative stress [2, 67, 167] (Fig. 6).
PKM2 is involved in the regulation of oxidative stress. The dimer PKM2 leads to the transfer of glycolysis intermediates to the pentose phosphate pathway, which then produces reducing equivalents, such as GSH and NADPH. Nuclear PKM2 interacts with Nrf2 to promote the expression of antioxidant genes, resulting in the production of antioxidant molecules. The lactic acid produced by the glycolysis process produces L-pyruvate and NADH under the action of L-LDH. These antioxidant molecules can antagonize oxidative stress. NADPH, nicotinamide adenine dinucleotide phosphate hydride; GSH, reduced glutathione; Nrf2, nuclear factor-erythroid-2-related factor 2; GPX4, glutathione peroxidase 4; Gclc, the catalyzing subunit of glutamate-cysteine ligase; Gclm, the modifying subunit of glutamate-cysteine ligase; NQO1, NADPH quinone oxidoreductase 1; TrxR1, thioredoxin reductase 1; Trx, thioredoxin; NADH, reduced nicotinamide adenine dinucleotide; L-LDH, L-lactate dehydrogenase; PEP, phosphoenolpyruvate; FBP, fructose-1,6-bisphosphate; ARE, antioxidant response element
In addition, nuclear factor-erythroid-2-related factor 2 (Nrf2) is the main regulator of cytoprotective responses in response to oxidative stress [168]. Ren et al. [169] found that nuclear PKM2 can bind to Nrf2 and form a complex that activates and facilitates cytoplasmic Nrf2 entry into the nucleus in hippocampal HT-22 neurons. The PKM2-Nrf2 complex further regulates the transcription of mitochondrial glutathione peroxidase 4 (GPX4) [169]. One study showed that levels of PKM2 expression in the blood were inversely correlated with the PD comprehensive score scale [170]. Nrf2, trans-activated by the PKM2 dimer in astrocytes, can upregulate expression of the catalyzing subunit (Gclc) and modifying subunit (Gclm) of glutamate-cysteine ligase (GSH-synthesized rate-limiting enzyme) by binding to promoters of their genes, thereby improving oxidative stress of PD [171]. Moreover, dimerized PKM2 binds to Nrf2 and activates the Nrf2/antioxidant response element (ARE) pathway in PC12 cells, triggering upregulation of Nrf2-driven antioxidant molecules, such as NADPH quinone oxidoreductase 1 (NQO1), thioredoxin reductase 1 (TrxR1), thioredoxin (Trx), and GSH, thereby improving antioxidant capacity and exerting neuroprotective effects [14].
In addition, lactic acid, as a crucial bioenergetic metabolite, is formed under anaerobic or aerobic glycolytic conditions and can also be used by cells as an oxidation substrate [86, 90, 172]. One study showed that L-lactate is transported into cells through MCTs, and L-lactate dehydrogenase converts it to L-pyruvate with the help of the cofactor nicotinamide adenine dinucleotide (NAD +), resulting in elevated levels of intracellular reduced nicotinamide adenine dinucleotide (NADH), thereby regulating the redox state of neurons [90]. L-lactic acid can also upregulate cellular defense mechanisms by promoting outbreaks of mild ROS, including the unfolded protein response (UPR) and Nrf2 activation [172] (Fig. 6).
These studies suggest that the PKM2-mediated Nrf2 signaling pathway and PPP, as well as lactic acid produced by glycolysis, play a crucial role in improving oxidative damage.
PKM2 and Mitochondrial Dysfunction
Mitochondria are organelles coated by two layers of membranes and are crucial structures in cells for producing energy [173]. In addition to oxidative phosphorylation to produce ATP, mitochondria are capable of fission and fusion, mitophagy, and mitochondrial biogenesis [174]. Mitochondrial dysfunction is associated with apoptosis, aging, cancer, and many neurodegenerative and muscle diseases [175, 176]. PKM2 plays an important role in regulating mitochondrial functions.
Mitochondria are constantly dividing and fusing to repair damaged components of mitochondria, with the division process separating damaged mitochondria and the fusion process enabling material exchange between healthy mitochondria [177]. Lack of fission or fusion reduces mitochondrial transport, leading to abnormal mitochondrial distribution and functional defects in cells [178]. A study has shown that elevated PKM2 can lead to abnormal mitochondrial division/fusion events and mitochondrial dysfunction by weakening the stability of P53 targeting dynamin-related protein 1 (Drp1) [178]. Furthermore, Zhao et al. [98] found that diabetes-mediated PKM2 overexpression leads to increased vulnerability of dopaminergic neurons to 6-OHDA by promoting high glycolysis and abnormal mitochondrial fusion (upregulation of mitochondrial fusion protein 2 (Mfn2) expression) in neurons. Conversely, silencing PKM2 can increase the number of mitochondria and improve the metabolic homeostasis of mitochondria [98]. However, a study showed that weakened interaction between Mfn2 and PKM2 and mitochondrial defects were found in rat hippocampal tissues after exposure to 2% sevoflurane [179]. Conversely, promoting Mfn2-PKM2 interaction can prevent brain damage and maintain mitochondrial fusion [179]. In addition, Qi et al. [29] found that hyperglycemia or diabetes reduced the tetramerization and activity of PKM2 by its sulfenylation and oxidation. Conversely, PKM2 activation could improve or even reverse diabetes or hyperglycemia-induced mitochondrial dysfunction by increasing levels of PGC-1α protein, mitochondrial membrane potential (MMP), and mitochondrial quality [29]. This phenomenon may be related to PKM2-mediated enhancement of the optic atrophy 1 (OPA1) protein [29, 180]. The activation or tetramerization of PKM2 can also promote PGC-1α-mediated mitochondrial biogenesis by inhibiting the phosphorylated PI3K/Akt signaling pathway [181]. Furthermore, the PKM2/AMPK signaling pathway mediates the activation of mitophagy [182]. In addition, Li et al. [19] found that PKM2 can upregulate the PINK1/Parkin signaling pathway-mediated mitophagy. Shen et al. [183] suggested that the interaction of PKM2 with protein phosphatase 1 (PP1) mediates the binding of PP1 to FUN14 domain-containing 1 (FUNDC1), resulting in FUNDC1 dephosphorylation and occurrence of FUNDC1-dependent mitophagy.
These findings suggest that PKM2 can modulate mitochondrial fission and fusion, mitophagy, or mitochondrial biogenesis by mediating multiple signaling pathways. However, some of these studies do not point to how different forms of PKM2 oligomerization regulate mitochondrial functions. Therefore, how PKM2 regulates mitochondrial functions in different diseases or cells needs further research and exploration.
In summary, PKM2 has diverse biological functions. In addition to the classical regulation of glycolysis and metabolic reprogramming, it also has the effects of regulating apoptosis and proliferation of cells, inflammatory responses, pathological autoimmune responses, oxidative stress, and mitochondrial dysfunction. However, the pathophysiological mechanisms of PKM2 in different tissues/cells or diseases need to be further studied.
Potential Link of PKM2 to Neurological Diseases
PKM2 and Cognitive Dysfunction
PKM2 and Amyloid β-Peptide (Aβ) Production
It is known that β-amyloid plaques are the main pathological feature of AD, the main component of which is fibrillar aggregates formed by Aβ aggregation [184]. PKM2 expression was increased in brain samples of patients with AD and in the cerebral cortex of mice with AD [185]. Moreover, upregulation of PKM2 was concentrated in microglia near Aβ plaques in mice with AD [186]. One study found that hypoxia induced upregulation of PKM2 expression in the nucleus of neurons with AD, the PKM2 dimer modulated the aph-1 homolog (APH1)-nicastrin (NCT) subcomplex to regulate gamma-secretase by transcriptional control of Aph-1a, and activation of gamma-secretase could promote Aβ production [185]. In addition, elevated PKM2 promotes abnormal activation of aerobic glycolysis in microglia with AD, leading to excessive production of lactic acid [186]. Lactic acid-mediated histone lactification, especially when elevated H4K12la markers are detected, can modify genes of multiple transcription factors that activate genes of glycolytic enzymes, such as HIF-1α, PKM, and LDHA [186]. Lactic acid can also directly promote the release of microglial pro-inflammatory factors, such as TNF-α, IL-6, and IL-1β, to mediate neuroinflammation [145]. Subsequently, inflammatory cytokines induce interferon-induced transmembrane protein 3 (IFITM3) expression in neurons and astrocytes, which then binds to and activates γ-secretase, increasing Aβ production [187]. Therefore, the positive feedback loop of glycolysis/H4K12la/PKM2 aggravates the glucose metabolism disorder and microglial dysfunction of the cortex and hippocampus in patients with AD, thereby promoting the formation of Aβ plaques [186] (Fig. 7).
PKM2 is involved in the production of Aβ. PKM2 modulated APH1-NCT subcomplex to regulate γ-secretase by transcriptional control of Aph-1a. In addition, PKM2 promotes aerobic glycolysis-mediated the overproduction of lactic acid. Lactic acid promotes the release of pro-inflammatory factors to mediate neuroinflammation. Subsequently, inflammatory cytokines induce IFITM3 expression to bind to and activate γ-secretase. Activation of γ secretase promotes the production of Aβ. Aβ, amyloid β-peptide; APH1, aph-1 homolog; NCT, nicastrin; IFITM3, interferon-induced transmembrane protein 3
Thus, both non-enzymatic nuclear action of PKM2 and glycolytic metabolites mediated by PKM2 can regulate Aβ production by relevant signaling pathways.
PKM2 Is Involved in the Regulation of Cognitive Dysfunction Associated with Various Diseases
Cognitive function belongs to the advanced functions of the brain, including memory, language expression, visuospatial ability, executive ability, calculation ability, and ability to understand and judge [188]. Impaired one or more of the above can manifest cognitive dysfunction [188]. Several diseases, including AD, cerebral small vessel disease, neuropsychiatric systemic lupus erythematosus (NPSLE), and AIDS, can cause cognitive dysfunction, and PKM2 has been shown to be involved in the regulation of cognitive dysfunction via related signaling pathways in these diseases [112, 123, 186, 189].
The Downregulation of PKM2 Can Improve Cognitive Dysfunction
As mentioned earlier, nuclear PKM2 regulates the relevant gene expression and assists Aβ production by some signaling pathways. Conversely, PKM2-specific deletion in microglia can improve spatial learning and memory in mice with AD by reducing the burden of Aβ [186]. Lu et al. [112] found that the PKM2-mediated β-catenin signaling pathway promoted microglial activation and phagocytosis of over-activated microglia, aggravated the loss of neuronal synapses, and then promoted cognitive dysfunction in mice with NPSLE. Conversely, inhibiting the expression of PKM2 in microglia could alleviate the above symptoms [112]. In addition, Bian et al. [123] found that serum PKM2 levels in patients with cerebral small vessel disease were positively correlated with the white matter hyperintensity and increased perivascular space and negatively correlated with cognitive function. Moreover, higher levels of serum PKM2 may lead to chronic inflammation, decreased cerebral blood flow, and cognitive dysfunction [123]. Conversely, inhibiting PKM2 expression may help suppress inflammation, restore cerebral blood flow, and reduce cerebral infarction area, as well as reduce cognitive impairment after stroke [190] (Fig. 8).
Potential link of PKM2 to neurological diseases. PKM2 can exert various biological functions, including regulation of Aβ production, glycolysis, inflammatory responses, apoptosis, proliferation of cells, oxidative stress, mitochondrial dysfunction, or pathological autoimmune responses. In addition, PKM2 is involved in the occurrence and development of neurological diseases, such as cognitive dysfunction, ischemic stroke, PSD, cerebral small vessel disease, hypoxic-ischemic encephalopathy, traumatic brain injury, traumatic SCI, PD, epilepsy, neuropathic pain, GCI, and autoimmune encephalitis by different biological roles. Aβ, amyloid β-peptide; PSD, post-stroke depression; PD, Parkinson’s disease; SCI, spinal cord injury; GCI, global cerebral ischemia
Inactivation of PKM2 Can Worsen Cognitive Dysfunction
Impaired activity of PKM2 is exhibited in methamphetamine-induced deficits in neurocognitive function [191]. One study found that protein oxidation played an important role in the progression of mild cognitive impairment (MCI) to AD [192]. PKM2, functionally involved in the regulation of energy metabolism and synaptic plasticity, was also found to be significantly oxidized in the hippocampus of subjects with MCI [192]. In HIV-related neurocognitive dysfunction, the HIV-1 protein gp120 alters the expression of PKM1 and PKM2 by promoting the expression of PTBP1, leading to the accumulation of advanced glycation end products and preventing the cleavage of the pro-brain-derived neurotrophic factor (pro-BDNF) protein into mature brain-derived neurotrophic factor (BDNF), which ultimately alters normal synaptic plasticity [189]. Instead, these events can be reversed by stabilizing the tetrameric form of PKM2 [189] (Fig. 8).
PKM2-Mediated Aerobic Glycolysis or Antioxidant Damaging Effects Can Improve Cognitive Dysfunction
PKM2 is thought to also improve cognitive dysfunction. Some studies have shown that electroacupuncture can improve cognitive function of AD by boosting glucose metabolism in the brain [193,194,195]. Li et al. [195] believe that aerobic glycolysis decreases significantly in AD. In contrast, electroacupuncture can promote the expression of aerobic glycolysis-related proteins in the hippocampus, including PKM2, thereby improving the learning and memory ability of APP/PS1 mice [195]. Similarly, Kang et al. [87] found that lactic acid supplementation after GCI restored exacerbation of neuronal damage and cognitive dysfunction due to PKM2 gene deletion. In addition, Ren et al. [169] suggested that nuclear PKM2 in hippocampal HT-22 neurons can inhibit iron death by mediating the PKM2/NRF2/GPX4 signaling pathway, thereby mitigating radiation-induced damage of hippocampal neurons and improving cognitive and memory consolidation decline (Fig. 8).
In summary, regulatory effects of PKM2 on cognitive dysfunction cannot be generalized. The oligomerized form of PKM2 and the biological role it plays differently in different cognitive-related diseases will lead to different ways in which it regulates cognitive dysfunction. Therefore, disease-specific analysis should be carried out. However, the link between PKM2 and cognitive dysfunction needs to be verified by a large number of experimental studies.
PKM2 and Neuropathic Pain
Neuropathic pain is usually a chronic disease caused by lesions or pathological changes within the nervous system [66, 140]. Peripheral and central sensitization can lead to highly sensitive pain behaviors and are considered crucial mechanisms of neuropathic pain [196]. Inflammatory processes and metabolic disorders are two aspects of central sensitization [66, 197, 198]. Neurons and glial cells, such as microglia and astrocytes, as well as bloodborne macrophages, play a key role in inducing and maintaining neuropathic pain by releasing powerful neuromodulators, such as pro-inflammatory cytokines and chemokines, to enhance neuronal excitability [66, 140, 199]. Studies have shown that glial cells can synthesize and secrete many inflammatory factors and cytokines by PKM2-mediated aerobic glycolysis, which can bind to the corresponding receptors of neurons to enhance the excitability of neurons, thus playing a key role in chronic pain [6, 200]. Activated astrocytes exacerbate inflammatory pain via PKM2-mediated aerobic glycolysis and the STAT3 signaling pathway [6]. In contrast, Wang et al. [66] found that inhibition of PKM2 effectively attenuated the neuropathic pain and inflammatory responses in rats induced by chronic compressive injury, which might be achieved by modulating the ERK and STAT3 signaling pathways. In addition, the accumulation of lactic acid can cause a decrease in intracellular pH and acidification of tissues under pathological conditions, which can also lead to painful behavior [6] (Fig. 8).
Thus, both PKM2-mediated aerobic glycolysis and inflammatory responses can worsen neuropathic pain.
PKM2 and Post-stroke Depression (PSD)
PSD is a common psychiatric disorder after cerebrovascular injury [201]. Depression is characterized by low mood, lack of energy, sadness, insomnia, and an inability to enjoy life [202]. Pathological mechanisms of PSD may involve an increase in inflammatory factors, dysregulation of the hypothalamic–pituitary–adrenal axis, decreased levels of monoamines, glutamate-mediated neuronal excitotoxicity, and abnormal neurotrophic responses [203, 204]. However, disruption of hippocampal synaptic plasticity may be a significant pathological mechanism in depression [205]. Yang et al. [206] found that hydrogen sulfide can inhibit β2-microglobulin-induced depression-like behavior, which may be associated with improving hippocampal synaptic plasticity by enhancing the hippocampal Warburg effect. Feng et al. [117] found that PKM2 improves PSD by activating the VEGF-mediated MAPK/ERK signaling pathway, which may be associated with improving of inflammatory responses and oxidative stress and proliferation of oligodendrocytes. In addition, some studies on PKM2 in stroke may indirectly suggest a potential link between PKM2 and PSD. For example, PKM2 plays a vital role in the inflammatory response after stroke [32]; PKM2-mediated lactate production plays an important role in maintaining neuronal excitability and synaptic plasticity [90]. As mentioned earlier, inflammatory responses, neuronal excitatory toxicity, and impaired synaptic plasticity may be pathological mechanisms of PSD [203,204,205] (Fig. 8).
Therefore, there is a certain connection between PKM2 and PSD. However, the mechanism of the link between the two needs to be further studied.
PKM2 and Other Neurological Diseases
In addition to the above neurological diseases, PKM2 is also involved in pathological changes in other neurological diseases. For example, PKM2 is involved in neuronal apoptosis in GCI, hypoxic-ischemic encephalopathy, and traumatic brain injury, as well as anesthetic-induced apoptosis of hippocampal neurons [87, 99,100,101], proliferation of astrocytes in traumatic SCI [111], angiogenesis, neurogenesis, and functional recovery after ischemic stroke [40], as well as activation of neutrophils and infiltrating macrophages in the brain after stroke [17, 130], activation of glial cells in epilepsy [147], immune responses in autoimmune encephalitis [153], regulating oxidative stress of dopaminergic neurons in PD [171], and regulating mitochondrial dysfunction in anesthesia-induced brain injury [179]. Therefore, PKM2 has a crucial role in neurological diseases (Fig. 8).
Conclusion
This article focuses on the key role of PKM2 in neurological diseases, expanding the understanding of the typical and atypical biological role of PKM2. Moreover, PKM2 does not work exactly the same in different diseases or cells, which is related to its oligomerization, subcellular localization, and post-translational modifications. Multiple signaling pathways intricately regulate the biological activity of PKM2, allowing cells to adapt to different physiological states. Therefore, PKM2 may have potential links with neurological diseases and may be used as a research direction for the treatment of these diseases and become a potential new target for clinical treatment of these diseases.
Data Availability
Data sharing is not applicable to this article.
Abbreviations
- PKM2:
-
Pyruvate kinase M2
- AD :
-
Alzheimer’s disease
- PD:
-
Parkinson’s disease
- PK:
-
Pyruvate kinase
- PEP:
-
Phosphoenolpyruvate
- ADP:
-
Adenosine diphosphate
- ATP:
-
Adenosine triphosphate
- HIF-1α:
-
Hypoxia-inducible factor 1α
- HRE:
-
Hypoxia response element
- PI3K:
-
Phosphoinositide 3-kinase
- mTOR:
-
Mammalian target of rapamycin
- AMPK:
-
AMP-activated protein kinase
- PTEN:
-
Phosphatase and tensin homolog
- EGFR:
-
Epidermal growth factor receptor
- PKC:
-
Protein kinase C
- NF-κB:
-
Nuclear factor kappa enhancer binding protein
- PPAR-γ:
-
Peroxisome proliferator-activated receptor γ
- mTORC2:
-
Mammalian target of rapamycin complex 2
- AKT:
-
Protein kinase B
- APJ:
-
Angiotensin II receptor-like 1
- SRSF3:
-
Arginine rich splicing factor 3
- PTBP1:
-
Polypyrimidine tract binding protein 1
- hnRNPA1/A2:
-
Heterogeneous nuclear ribonucleoprotein A1/A2
- circRNA:
-
Circular RNAs
- circSRRM4:
-
CircRNA serine/arginine repetitive matrix 4
- miRNAs:
-
MicroRNAs
- miR-124:
-
MicroRNA-124
- RBM4:
-
RNA-binding motif 4
- PHB2:
-
Prohibitin 2
- lncRNAs:
-
Long non-coding RNAs
- LINC00689:
-
LncRNA long intergenic non-protein coding RNA 689
- ceRNA:
-
Competing endogenous RNA
- circMAT2B:
-
Circular RNA MAT2B
- Mbd2:
-
Methyl-CpG binding domain protein 2
- PPP:
-
Pentose phosphate pathway
- FBP:
-
Fructose-1,6-bisphosphate
- PHD3:
-
Prolyl hydroxylase 3
- GLUT1:
-
Glucose transporter 1
- LDHA:
-
Lactate dehydrogenase A
- PDK1:
-
Pyruvate dehydrogenase kinase 1
- iNs:
-
Induced neurons
- LDH5:
-
Lactate dehydrogenase isoform 5
- MCTs:
-
Monocarboxylate transporters
- NMDA:
-
N-methyl-D-aspartate
- NMDAR:
-
NMDA receptor
- ERK1/2:
-
Extracellular signal-regulated protein kinases 1 and 2
- Bcl-2:
-
B-cell lymphoma 2
- Bax:
-
Bcl2-associated X
- CDKs:
-
Cyclin-dependent kinases
- STAT3:
-
Signal transducers and activators of transcription 3
- 6-OHDA:
-
6-Hydroxydopamine
- LPS:
-
Lipopolysaccharide
- Wnt:
-
Wingless/integrated
- GCI:
-
Global cerebral ischemia
- 5′ Tyr-tRF:
-
5′ TRNA fragments derived from tyrosine pre-tRNA
- CCND1:
-
Cyclin D1
- HDACs:
-
Histone deacetylases
- MAPK:
-
Mitogen-activated protein kinase
- SCI:
-
Spinal cord injury
- TCF4:
-
T-cell factor 4
- FAK:
-
Focal adhesion kinase
- VEGF:
-
Vascular epithelial growth factor
- VCP:
-
Valosin-containing protein
- TLRs:
-
Toll-like receptors
- Pyk2:
-
Proline-rich tyrosine kinase 2
- PGC-1α:
-
Peroxisome proliferator-activated receptor-γ co-activator 1-α
- HMGB1:
-
High-mobility group box 1
- NLRP3:
-
NLR family, pyrin domain containing 3
- AIM2:
-
Absent in melanoma 2
- EIF2AK2 or PKR:
-
Eukaryotic translation initiation factor 2 alpha kinase 2
- iNOS:
-
Inducible nitric oxide synthase
- COX-2:
-
Cyclooxygenase-2
- MyD88:
-
Myeloid differentiation factor 88
- TRAF6:
-
TNF receptor-associated factor 6
- NOX4:
-
NADPH oxidase 4
- IFN-γ:
-
Interferon-γ
- ROS:
-
Reactive oxygen species
- ATF2:
-
Activation transcription factor 2
- H3:
-
Histone 3
- C1q:
-
Complement component 1q
- TNF:
-
Tumor necrosis factor
- IL:
-
Interleukin
- C3:
-
Complement component 3
- C3aR:
-
C3a receptors
- RA:
-
Rheumatoid arthritis
- Th17:
-
Helper T cells 17
- DCs:
-
Dendritic cells
- JNK:
-
C-Jun N-terminal kinase
- mDCs:
-
Myeloid dendritic cells
- RNS:
-
Reactive nitrogen species
- NADPH:
-
Nicotinamide adenine dinucleotide phosphate hydride
- GSH:
-
Reduced glutathione
- Nrf2:
-
Nuclear factor-erythroid-2-related factor 2
- GPX4:
-
Glutathione peroxidase 4
- Gclc:
-
The catalyzing subunit of glutamate-cysteine ligase
- Gclm:
-
The modifying subunit of glutamate-cysteine ligase
- NQO1:
-
NADPH quinone oxidoreductase 1
- TrxR1:
-
Thioredoxin reductase 1
- Trx:
-
Thioredoxin
- NAD + :
-
Nicotinamide adenine dinucleotide
- NADH:
-
Reduced nicotinamide adenine dinucleotide
- UPR:
-
Unfolded protein response
- ARE:
-
Antioxidant response element
- Drp1:
-
Dynamin-related protein 1
- Mfn2:
-
Mitochondrial fusion protein 2
- MMP:
-
Mitochondrial membrane potential
- OPA1:
-
Optic atrophy 1
- PP1:
-
Protein phosphatase 1
- FUNDC1:
-
FUN14 domain-containing 1
- Aβ:
-
Amyloid β-peptide
- APH1:
-
Aph-1 homolog
- NCT:
-
Nicastrin
- IFITM3:
-
Interferon-induced transmembrane protein 3
- NPSLE:
-
Neuropsychiatric systemic lupus erythematosus
- MCI:
-
Mild cognitive impairment
- BDNF:
-
Brain-derived neurotrophic factor
- PSD:
-
Post-stroke depression
References
Zhu S, Guo Y, Zhang X, Liu H, Yin M, Chen X, Peng C (2021) Pyruvate kinase M2 (PKM2) in cancer and cancer therapeutics. Cancer Lett 503:240–248. https://doi.org/10.1016/j.canlet.2020.11.018
Mazurek S (2011) Pyruvate kinase type M2: a key regulator of the metabolic budget system in tumor cells. Int J Biochem Cell Biol 43:969–980. https://doi.org/10.1016/j.biocel.2010.02.005
Liang J, Cao R, Wang X, Zhang Y, Wang P, Gao H, Li C, Yang F et al (2017) Mitochondrial PKM2 regulates oxidative stress-induced apoptosis by stabilizing Bcl2. Cell Res 27:329–351. https://doi.org/10.1038/cr.2016.159
Yang W, Lu Z (2015) Pyruvate kinase M2 at a glance. J Cell Sci 128:1655–1660. https://doi.org/10.1242/jcs.166629
Zhang Y, Chen K, Sloan SA, Bennett ML, Scholze AR, O’Keeffe S, Phatnani HP, Guarnieri P et al (2014) An RNA-sequencing transcriptome and splicing database of glia, neurons, and vascular cells of the cerebral cortex. J Neurosci 34:11929–11947. https://doi.org/10.1523/jneurosci.1860-14.2014
Wei X, Jin XH, Meng XW, Hua J, Ji FH, Wang LN, Yang JP (2020) Platelet-rich plasma improves chronic inflammatory pain by inhibiting PKM2-mediated aerobic glycolysis in astrocytes. Ann Transl Med 8:1456. https://doi.org/10.21037/atm-20-6502
Gui DY, Lewis CA, Vander Heiden MG (2013) Allosteric regulation of PKM2 allows cellular adaptation to different physiological states. Sci Signal 6:pe7. https://doi.org/10.1126/scisignal.2003925
Chen M, David CJ, Manley JL (2012) Concentration-dependent control of pyruvate kinase M mutually exclusive splicing by hnRNP proteins. Nat Struct Mol Biol 19:346–354. https://doi.org/10.1038/nsmb.2219
Romero-Ramírez L, García-Rama C, Wu S, Mey J (2022) Bile acids attenuate PKM2 pathway activation in proinflammatory microglia. Sci Rep 12:1459. https://doi.org/10.1038/s41598-022-05408-3
Davidson SM, Schmidt DR, Heyman JE, O’Brien JP, Liu AC, Israelsen WJ, Dayton TL, Sehgal R et al (2022) Pyruvate kinase M1 suppresses development and progression of prostate adenocarcinoma. Cancer Res 82:2403–2416. https://doi.org/10.1158/0008-5472.Can-21-2352
Takenaka M, Noguchi T, Sadahiro S, Hirai H, Yamada K, Matsuda T, Imai E, Tanaka T (1991) Isolation and characterization of the human pyruvate kinase M gene. Eur J Biochem 198:101–106. https://doi.org/10.1111/j.1432-1033.1991.tb15991.x
Nayak MK, Ghatge M, Flora GD, Dhanesha N, Jain M, Markan KR, Potthoff MJ, Lentz SR et al (2021) The metabolic enzyme pyruvate kinase M2 regulates platelet function and arterial thrombosis. Blood 137:1658–1668. https://doi.org/10.1182/blood.2020007140
Gupta V, Bamezai RN (2010) Human pyruvate kinase M2: a multifunctional protein. Protein Sci 19:2031–2044. https://doi.org/10.1002/pro.505
Ding Z, Da HH, Osama A, Xi J, Hou Y, Fang J (2022) Emodin ameliorates antioxidant capacity and exerts neuroprotective effect via PKM2-mediated Nrf2 transactivation. Food Chem Toxicol 160:112790. https://doi.org/10.1016/j.fct.2021.112790
Gao J, Zhao Y, Li T, Gan X, Yu H (2022) The role of PKM2 in the regulation of mitochondrial function: focus on mitochondrial metabolism, oxidative stress, dynamic, and apoptosis. PKM2 in Mitochondrial Function. Oxid Med Cell Longev 2022:7702681. https://doi.org/10.1155/2022/7702681
Traxler L, Herdy JR, Stefanoni D, Eichhorner S, Pelucchi S, Szücs A, Santagostino A, Kim Y et al (2022) Warburg-like metabolic transformation underlies neuronal degeneration in sporadic Alzheimer’s disease. Cell Metab 34:1248-1263.e6. https://doi.org/10.1016/j.cmet.2022.07.014
Dhanesha N, Patel RB, Doddapattar P, Ghatge M, Flora GD, Jain M, Thedens D, Olalde H et al (2022) PKM2 promotes neutrophil activation and cerebral thromboinflammation: therapeutic implications for ischemic stroke. Blood 139:1234–1245. https://doi.org/10.1182/blood.2021012322
Qin S, Yang D, Chen K, Li H, Zhang L, Li Y, Le R, Li X et al (2017) Pkm2 can enhance pluripotency in ESCs and promote somatic cell reprogramming to iPSCs. Oncotarget 8:84276–84284. https://doi.org/10.18632/oncotarget.20685
Li D, Shen C, Liu L, Hu J, Qin J, Dai L, Gao L, Cheng M et al (2022) PKM2 regulates cigarette smoke-induced airway inflammation and epithelial-to-mesenchymal transition via modulating PINK1/Parkin-mediated mitophagy. Toxicology 477:153251. https://doi.org/10.1016/j.tox.2022.153251
Tech K, Tikunov AP, Farooq H, Morrissy AS, Meidinger J, Fish T, Green SC, Liu H et al (2017) Pyruvate kinase inhibits proliferation during postnatal cerebellar neurogenesis and suppresses medulloblastoma formation. Cancer Res 77:3217–3230. https://doi.org/10.1158/0008-5472.Can-16-3304
Alves-Filho JC, Pålsson-McDermott EM (2016) Pyruvate kinase M2: a potential target for regulating inflammation. Front Immunol 7:145. https://doi.org/10.3389/fimmu.2016.00145
Puckett DL, Alquraishi M, Chowanadisai W, Bettaieb A (2021) The role of PKM2 in metabolic reprogramming: insights into the regulatory roles of non-Coding RNAs. Int J Mol Sci 22(3):1171. https://doi.org/10.3390/ijms22031171
Li M, Lu H, Wang X, Duan C, Zhu X, Zhang Y, Ge X, Ji F et al (2021) Pyruvate kinase M2 (PKM2) interacts with activating transcription factor 2 (ATF2) to bridge glycolysis and pyroptosis in microglia. Mol Immunol 140:250–266. https://doi.org/10.1016/j.molimm.2021.10.017
Wang J, Yang P, Yu T, Gao M, Liu D, Zhang J, Lu C, Chen X et al (2022) Lactylation of PKM2 suppresses inflammatory metabolic adaptation in pro-inflammatory macrophages. Int J Biol Sci 18:6210–6225. https://doi.org/10.7150/ijbs.75434
Zheng S, Liu Q, Liu T, Lu X (2021) Posttranslational modification of pyruvate kinase type M2 (PKM2): novel regulation of its biological roles to be further discovered. J Physiol Biochem 77:355–363. https://doi.org/10.1007/s13105-021-00813-0
Zahra K, Dey T, Ashish MSP, Pandey U (2020) Pyruvate kinase M2 and cancer: the role of PKM2 in promoting tumorigenesis. Front Oncol 10:159. https://doi.org/10.3389/fonc.2020.00159
Zhang Z, Deng X, Liu Y, Liu Y, Sun L, Chen F (2019) PKM2, function and expression and regulation. Cell Biosci 9:52. https://doi.org/10.1186/s13578-019-0317-8
Zhou Z, Li M, Zhang L, Zhao H, Şahin Ö, Chen J, Zhao JJ, Songyang Z et al (2018) Oncogenic kinase-induced PKM2 tyrosine 105 phosphorylation converts nononcogenic PKM2 to a tumor promoter and induces cancer stem-like cells. Cancer Res 78:2248–2261. https://doi.org/10.1158/0008-5472.Can-17-2726
Qi W, Keenan HA, Li Q, Ishikado A, Kannt A, Sadowski T, Yorek MA, Wu IH et al (2017) Pyruvate kinase M2 activation may protect against the progression of diabetic glomerular pathology and mitochondrial dysfunction. Nat Med 23:753–762. https://doi.org/10.1038/nm.4328
Wu X, Liu L, Zheng Q, Hao H, Ye H, Li P, Yang H (2021) Protocatechuic aldehyde protects cardiomycoytes against ischemic injury via regulation of nuclear pyruvate kinase M2. Acta Pharm Sin B 11:3553–3566. https://doi.org/10.1016/j.apsb.2021.03.021
Wang F, Wang K, Xu W, Zhao S, Ye D, Wang Y, Xu Y, Zhou L et al (2017) SIRT5 desuccinylates and activates pyruvate kinase M2 to block macrophage IL-1β production and to prevent DSS-induced colitis in mice. Cell Rep 19:2331–2344. https://doi.org/10.1016/j.celrep.2017.05.065
Gao J, Yao M, Zhang W, Yang B, Yuan G, Liu JX, Zhang Y (2022) Panax notoginseng saponins alleviates inflammation induced by microglial activation and protects against ischemic brain injury via inhibiting HIF-1α/PKM2/STAT3 signaling. Biomed Pharmacother 155:113479. https://doi.org/10.1016/j.biopha.2022.113479
Wong N, De Melo J, Tang D (2013) PKM2, a central point of regulation in cancer metabolism. Int J Cell Biol 2013:242513. https://doi.org/10.1155/2013/242513
Liu Z, Le Y, Chen H, Zhu J, Lu D (2021) Role of PKM2-mediated immunometabolic reprogramming on development of cytokine storm. Front Immunol 12:748573. https://doi.org/10.3389/fimmu.2021.748573
Yang W, Xia Y, Cao Y, Zheng Y, Bu W, Zhang L, You MJ, Koh MY et al (2012) EGFR-induced and PKCε monoubiquitylation-dependent NF-κB activation upregulates PKM2 expression and promotes tumorigenesis. Mol Cell 48:771–784. https://doi.org/10.1016/j.molcel.2012.09.028
Selak MA, Armour SM, MacKenzie ED, Boulahbel H, Watson DG, Mansfield KD, Pan Y, Simon MC et al (2005) Succinate links TCA cycle dysfunction to oncogenesis by inhibiting HIF-alpha prolyl hydroxylase. Cancer Cell 7:77–85. https://doi.org/10.1016/j.ccr.2004.11.022
Iqbal MA, Siddiqui FA, Gupta V, Chattopadhyay S, Gopinath P, Kumar B, Manvati S, Chaman N et al (2013) Insulin enhances metabolic capacities of cancer cells by dual regulation of glycolytic enzyme pyruvate kinase M2. Mol Cancer 12:72. https://doi.org/10.1186/1476-4598-12-72
Sun Q, Chen X, Ma J, Peng H, Wang F, Zha X, Wang Y, Jing Y et al (2011) Mammalian target of rapamycin up-regulation of pyruvate kinase isoenzyme type M2 is critical for aerobic glycolysis and tumor growth. Proc Natl Acad Sci U S A 108:4129–4134. https://doi.org/10.1073/pnas.1014769108
Wang Y, Han X, Fu M, Wang J, Song Y, Liu Y, Zhang J, Zhou J et al (2018) Qiliqiangxin attenuates hypoxia-induced injury in primary rat cardiac microvascular endothelial cells via promoting HIF-1α-dependent glycolysis. J Cell Mol Med 22:2791–2803. https://doi.org/10.1111/jcmm.13572
Chen D, Wei L, Liu ZR, Yang JJ, Gu X, Wei ZZ, Liu LP, Yu SP (2018) Pyruvate kinase M2 increases angiogenesis, neurogenesis, and functional recovery mediated by upregulation of STAT3 and focal adhesion kinase activities after ischemic stroke in adult mice. Neurotherapeutics 15:770–784. https://doi.org/10.1007/s13311-018-0635-2
Liu M, Zhou P (2023) Effect and mechanism of atorvastatin on reversing drug resistance in leukemia by regulating glycolysis through PTEN/mTOR pathway. Zhongguo Shi Yan Xue Ye Xue Za Zhi 31:38–44. https://doi.org/10.19746/j.cnki.issn.1009-2137.2023.01.006
Jia C, Zhao Y, Huang H, Fan K, Xie T, Xie M (2022) Apigenin sensitizes radiotherapy of mouse subcutaneous glioma through attenuations of cell stemness and DNA damage repair by inhibiting NF-κB/HIF-1α-mediated glycolysis. J Nutr Biochem 107:109038. https://doi.org/10.1016/j.jnutbio.2022.109038
Kim H, Jang H, Kim TW, Kang BH, Lee SE, Jeon YK, Chung DH, Choi J et al (2015) Core pluripotency factors directly regulate metabolism in embryonic stem cell to maintain pluripotency. Stem Cells 33:2699–2711. https://doi.org/10.1002/stem.2073
Shimauchi T, Boucherat O, Yokokawa T, Grobs Y, Wu W, Orcholski M, Martineau S, Omura J et al (2022) PARP1-PKM2 axis mediates right ventricular failure associated with pulmonary arterial hypertension. JACC Basic Transl Sci 7:384–403. https://doi.org/10.1016/j.jacbts.2022.01.005
Panasyuk G, Espeillac C, Chauvin C, Pradelli LA, Horie Y, Suzuki A, Annicotte JS, Fajas L et al (2012) PPARγ contributes to PKM2 and HK2 expression in fatty liver. Nat Commun 3:672. https://doi.org/10.1038/ncomms1667
Ouyang X, Han Y, Qu G, Li M, Wu N, Liu H, Arojo O, Sun H et al (2019) Metabolic regulation of T cell development by Sin1-mTORC2 is mediated by pyruvate kinase M2. J Mol Cell Biol 11:93–106. https://doi.org/10.1093/jmcb/mjy065
Zhou Q, Xu J, Liu M, He L, Zhang K, Yang Y, Yang X, Zhou H et al (2019) Warburg effect is involved in apelin-13-induced human aortic vascular smooth muscle cells proliferation. J Cell Physiol 234:14413–14421. https://doi.org/10.1002/jcp.28218
Kuranaga Y, Sugito N, Shinohara H, Tsujino T, Taniguchi K, Komura K, Ito Y, Soga T, Akao Y (2018) SRSF3, a splicer of the PKM gene, regulates cell growth and maintenance of cancer-specific energy metabolism in colon cancer cells. Int J Mol Sci 19(10):3012. https://doi.org/10.3390/ijms19103012
Yang H, Zhu R, Zhao X, Liu L, Zhou Z, Zhao L, Liang B, Ma W et al (2019) Sirtuin-mediated deacetylation of hnRNP A1 suppresses glycolysis and growth in hepatocellular carcinoma. Oncogene 38:4915–4931. https://doi.org/10.1038/s41388-019-0764-z
Jia Y, Mao C, Ma Z, Huang J, Li W, Ma X, Zhang S, Li M et al (2022) PHB2 maintains the contractile phenotype of VSMCs by counteracting PKM2 splicing. Circ Res 131:807–824. https://doi.org/10.1161/circresaha.122.321005
Zhao W, Li M, Wang S, Li Z, Li H, Li S (2023) CircRNA SRRM4 affects glucose metabolism by regulating PKM alternative splicing via SRSF3 deubiquitination in epilepsy. Neuropathol Appl Neurobiol 49:e12850. https://doi.org/10.1111/nan.12850
Zhang H, Wang D, Li M, Plecitá-Hlavatá L, D’Alessandro A, Tauber J, Riddle S, Kumar S et al (2017) Metabolic and proliferative state of vascular adventitial fibroblasts in pulmonary hypertension is regulated through a MicroRNA-124/PTBP1 (polypyrimidine tract binding protein 1)/pyruvate kinase muscle axis. Circulation 136:2468–2485. https://doi.org/10.1161/circulationaha.117.028069
Wang X, Shao F, Yu J, Jiang H, Gong D, Gu Z (2015) MicroRNA-122 targets genes related to liver metabolism in chickens. Comp Biochem Physiol B Biochem Mol Biol 184:29–35. https://doi.org/10.1016/j.cbpb.2015.02.002
Caruso P, Dunmore BJ, Schlosser K, Schoors S, Dos Santos C, Perez-Iratxeta C, Lavoie JR, Zhang H et al (2017) Identification of MicroRNA-124 as a major regulator of enhanced endothelial cell glycolysis in pulmonary arterial hypertension via PTBP1 (polypyrimidine tract binding protein) and pyruvate kinase M2. Circulation 136:2451–2467. https://doi.org/10.1161/circulationaha.117.028034
Su CH, Hung KY, Hung SC, Tarn WY (2017) RBM4 Regulates neuronal differentiation of mesenchymal stem cells by modulating alternative splicing of Pyruvate Kinase M. Mol Cell Biol 37(3):e00466-16. https://doi.org/10.1128/MCB.00466-16
Konno M, Koseki J, Kawamoto K, Nishida N, Matsui H, Dewi DL, Ozaki M, Noguchi Y et al (2015) Embryonic MicroRNA-369 controls metabolic splicing factors and urges cellular reprograming. PLoS ONE 10:e0132789. https://doi.org/10.1371/journal.pone.0132789
Salama SA, Mohammad MA, Diaz-Arrastia CR, Kamel MW, Kilic GS, Ndofor BT, Abdel-Baki MS, Theiler SK (2014) Estradiol-17β upregulates pyruvate kinase M2 expression to coactivate estrogen receptor-α and to integrate metabolic reprogramming with the mitogenic response in endometrial cells. J Clin Endocrinol Metab 99:3790–3799. https://doi.org/10.1210/jc.2013-2639
Liu X, Zhu Q, Guo Y, Xiao Z, Hu L, Xu Q (2019) LncRNA LINC00689 promotes the growth, metastasis and glycolysis of glioma cells by targeting miR-338-3p/PKM2 axis. Biomed Pharmacother 117:109069. https://doi.org/10.1016/j.biopha.2019.109069
Li Q, Pan X, Zhu D, Deng Z, Jiang R, Wang X (2019) Circular RNA MAT2B promotes glycolysis and malignancy of hepatocellular carcinoma through the miR-338-3p/PKM2 axis under hypoxic stress. Hepatology 70:1298–1316. https://doi.org/10.1002/hep.30671
Nakao K, Miyaaki H, Ichikawa T (2014) Antitumor function of microRNA-122 against hepatocellular carcinoma. J Gastroenterol 49:589–593. https://doi.org/10.1007/s00535-014-0932-4
Cao J, Huo P, Cui K, Wei H, Cao J, Wang J, Liu Q, Lei X et al (2022) Follicular fluid-derived exosomal miR-143-3p/miR-155-5p regulate follicular dysplasia by modulating glycolysis in granulosa cells in polycystic ovary syndrome. Cell Commun Signal 20:61. https://doi.org/10.1186/s12964-022-00876-6
Zeng X, Liu N, Zhang J, Wang L, Zhang Z, Zhu J, Li Q, Wang Y (2017) Inhibition of miR-143 during ischemia cerebral injury protects neurones through recovery of the hexokinase 2-mediated glucose uptake. Biosci Rep 37 10.1042/bsr20170216
Ge XL, Wang JL, Liu X, Zhang J, Liu C, Guo L (2019) Inhibition of miR-19a protects neurons against ischemic stroke through modulating glucose metabolism and neuronal apoptosis. Cell Mol Biol Lett 24:37. https://doi.org/10.1186/s11658-019-0160-2
Cao Y, Guo WT, Tian S, He X, Wang XW, Liu X, Gu KL, Ma X et al (2015) miR-290/371-Mbd2-Myc circuit regulates glycolytic metabolism to promote pluripotency. Embo j 34:609–623. https://doi.org/10.15252/embj.201490441
Ni S, Yang B, Xia L, Zhang H (2021) EZH2 mediates miR-146a-5p/HIF-1α to alleviate inflammation and glycolysis after acute spinal cord injury. Mediators Inflamm 2021:5591582. https://doi.org/10.1155/2021/5591582
Wang B, Liu S, Fan B, Xu X, Chen Y, Lu R, Xu Z, Liu X (2018) PKM2 is involved in neuropathic pain by regulating ERK and STAT3 activation in rat spinal cord. J Headache Pain 19:7. https://doi.org/10.1186/s10194-018-0836-4
Vander Heiden MG, Cantley LC, Thompson CB (2009) Understanding the Warburg effect: the metabolic requirements of cell proliferation. Science 324:1029–1033. https://doi.org/10.1126/science.1160809
Tokuda K, Baron B, Yamashiro C, Kuramitsu Y, Kitagawa T, Kobayashi M, Sonoda KH, Kimura K (2020) Up-regulation of the pentose phosphate pathway and HIF-1α expression during neural progenitor cell induction following glutamate treatment in rat ex vivo retina. Cell Biol Int 44:137–144. https://doi.org/10.1002/cbin.11212
Mazurek S, Zwerschke W, Jansen-Dürr P, Eigenbrodt E (2001) Effects of the human papilloma virus HPV-16 E7 oncoprotein on glycolysis and glutaminolysis: role of pyruvate kinase type M2 and the glycolytic-enzyme complex. Biochem J 356:247–256. https://doi.org/10.1042/0264-6021:3560247
Liu C, Liu C, Fu R (2022) Research progress on the role of PKM2 in the immune response. Front Immunol 13:936967. https://doi.org/10.3389/fimmu.2022.936967
Jurica MS, Mesecar A, Heath PJ, Shi W, Nowak T, Stoddard BL (1998) The allosteric regulation of pyruvate kinase by fructose-1,6-bisphosphate. Structure 6:195–210. https://doi.org/10.1016/s0969-2126(98)00021-5
Srivastava D, Razzaghi M, Henzl MT, Dey M (2017) Structural investigation of a dimeric variant of pyruvate kinase muscle isoform 2. Biochemistry 56:6517–6520. https://doi.org/10.1021/acs.biochem.7b01013
Yang W, Xia Y, Hawke D, Li X, Liang J, Xing D, Aldape K, Hunter T et al (2012) PKM2 phosphorylates histone H3 and promotes gene transcription and tumorigenesis. Cell 150:685–696. https://doi.org/10.1016/j.cell.2012.07.018
Hsu PP, Sabatini DM (2008) Cancer cell metabolism: Warburg and beyond. Cell 134:703–707. https://doi.org/10.1016/j.cell.2008.08.021
O’Neill LA, Hardie DG (2013) Metabolism of inflammation limited by AMPK and pseudo-starvation. Nature 493:346–355. https://doi.org/10.1038/nature11862
Wen H, Ting JP, O’Neill LA (2012) A role for the NLRP3 inflammasome in metabolic diseases–did Warburg miss inflammation? Nat Immunol 13:352–357. https://doi.org/10.1038/ni.2228
Wang R, Green DR (2012) Metabolic checkpoints in activated T cells. Nat Immunol 13:907–915. https://doi.org/10.1038/ni.2386
Yang L, Xie M, Yang M, Yu Y, Zhu S, Hou W, Kang R, Lotze MT et al (2014) PKM2 regulates the Warburg effect and promotes HMGB1 release in sepsis. Nat Commun 5:4436. https://doi.org/10.1038/ncomms5436
Yang J, Liu H, Liu X, Gu C, Luo R, Chen HF (2016) Synergistic allosteric mechanism of fructose-1,6-bisphosphate and serine for pyruvate kinase M2 via dynamics fluctuation network analysis. J Chem Inf Model 56:1184–1192. https://doi.org/10.1021/acs.jcim.6b00115
Nandi S, Dey M (2023) Identification of residues involved in allosteric signal transmission from amino acid binding site of pyruvate kinase muscle isoform 2. PLoS ONE 18:e0282508. https://doi.org/10.1371/journal.pone.0282508
Christofk HR, Vander Heiden MG, Wu N, Asara JM, Cantley LC (2008) Pyruvate kinase M2 is a phosphotyrosine-binding protein. Nature 452:181–186. https://doi.org/10.1038/nature06667
Palsson-McDermott EM, Curtis AM, Goel G, Lauterbach MA, Sheedy FJ, Gleeson LE, van den Bosch MW, Quinn SR et al (2015) Pyruvate kinase M2 regulates Hif-1α activity and IL-1β induction and is a critical determinant of the warburg effect in LPS-activated macrophages. Cell Metab 21:65–80. https://doi.org/10.1016/j.cmet.2014.12.005
Zhao X, Zhu Y, Hu J, Jiang L, Li L, Jia S, Zen K (2018) Shikonin inhibits tumor growth in mice by suppressing pyruvate kinase M2-mediated aerobic glycolysis. Sci Rep 8:14517. https://doi.org/10.1038/s41598-018-31615-y
Bolaños JP (2016) Bioenergetics and redox adaptations of astrocytes to neuronal activity. J Neurochem 139(2):115–125. https://doi.org/10.1111/jnc.13486
Zheng X, Boyer L, Jin M, Mertens J, Kim Y, Ma L, Ma L, Hamm M, Gage FH, Hunter T (2016) Metabolic reprogramming during neuronal differentiation from aerobic glycolysis to neuronal oxidative phosphorylation. eLife 5:e13374. https://doi.org/10.7554/eLife.13374
Magistretti PJ, Allaman I (2018) Lactate in the brain: from metabolic end-product to signalling molecule. Nat Rev Neurosci 19:235–249. https://doi.org/10.1038/nrn.2018.19
Kang BS, Choi BY, Kho AR, Lee SH, Hong DK, Park MK, Lee SH, Lee CJ, Yang HW, Woo SY, Park SW, Kim DY, Park JB, Chung WS, Suh SW (2023) Effects of Pyruvate Kinase M2 (PKM2) gene deletion on astrocyte-specific glycolysis and global cerebral Ischemia-Induced neuronal death. Antioxidants (Basel, Switzerland) 12(2):491. https://doi.org/10.3390/antiox12020491
Deitmer JW, Theparambil SM, Ruminot I, Noor SI, Becker HM (2019) Energy dynamics in the brain: contributions of astrocytes to metabolism and pH homeostasis. Front Neurosci 13:1301. https://doi.org/10.3389/fnins.2019.01301
Deck M, Van Hameren G, Campbell G, Bernard-Marissal N, Devaux J, Berthelot J, Lattard A, Médard JJ et al (2022) Physiology of PNS axons relies on glycolytic metabolism in myelinating Schwann cells. PLoS ONE 17:e0272097. https://doi.org/10.1371/journal.pone.0272097
Yang J, Ruchti E, Petit JM, Jourdain P, Grenningloh G, Allaman I, Magistretti PJ (2014) Lactate promotes plasticity gene expression by potentiating NMDA signaling in neurons. Proc Natl Acad Sci U S A 111:12228–12233. https://doi.org/10.1073/pnas.1322912111
Zhou Q, Tang M, He L, Chen S (2020) PKM2: a crucial neuroprotective target against oxidative stress. Acta Biochim Biophys Sin (Shanghai) 52:1432–1434. https://doi.org/10.1093/abbs/gmaa121
Lakhani SA, Masud A, Kuida K, Porter GA Jr, Booth CJ, Mehal WZ, Inayat I, Flavell RA (2006) Caspases 3 and 7: key mediators of mitochondrial events of apoptosis. Science 311:847–851. https://doi.org/10.1126/science.1115035
Youle RJ, Strasser A (2008) The BCL-2 protein family: opposing activities that mediate cell death. Nat Rev Mol Cell Biol 9:47–59. https://doi.org/10.1038/nrm2308
Vallée A, Lecarpentier Y, Guillevin R, Vallée JN (2018) Reprogramming energetic metabolism in Alzheimer’s disease. Life Sci 193:141–152. https://doi.org/10.1016/j.lfs.2017.10.033
Gao X, Wang H, Yang JJ, Chen J, Jie J, Li L, Zhang Y, Liu ZR (2013) Reciprocal regulation of protein kinase and pyruvate kinase activities of pyruvate kinase M2 by growth signals. J Biol Chem 288:15971–15979. https://doi.org/10.1074/jbc.M112.448753
Zhou J, Rasmussen M, Ekström P (2023) A potential neuroprotective role for pyruvate kinase 2 in retinal degeneration. Adv Exp Med Biol 1415:479–483. https://doi.org/10.1007/978-3-031-27681-1_70
Zhao J, Wang G, Han K, Wang Y, Wang L, Gao J, Zhao S, Wang G et al (2022) Mitochondrial PKM2 deacetylation by procyanidin B2-induced SIRT3 upregulation alleviates lung ischemia/reperfusion injury. Cell Death Dis 13:594. https://doi.org/10.1038/s41419-022-05051-w
Zhao Y, Wang Y, Wu Y, Tao C, Xu R, Chen Y, Qian L, Xu T et al (2023) PKM2-mediated neuronal hyperglycolysis enhances the risk of Parkinson’s disease in diabetic rats. J Pharm Anal 13:187–200. https://doi.org/10.1016/j.jpha.2022.11.006
Wu Q, Ge W, Chen Y, Kong X, Xian H (2019) PKM2 involved in neuronal apoptosis on hypoxic-ischemic encephalopathy in neonatal rats. Neurochem Res 44:1602–1612. https://doi.org/10.1007/s11064-019-02784-7
Fang Y, Zhao T, Ni H, Li Y, Zhu Y, Gao R, Zhang L, Jia Z et al (2023) USP11 exacerbates neuronal apoptosis after traumatic brain injury via PKM2-mediated PI3K/AKT signaling pathway. Brain Res 1807:148321. https://doi.org/10.1016/j.brainres.2023.148321
Bao F, Kang X, Xie Q, Wu J (2019) HIF-α/PKM2 and PI3K-AKT pathways involved in the protection by dexmedetomidine against isoflurane or bupivacaine-induced apoptosis in hippocampal neuronal HT22 cells. Exp Ther Med 17:63–70. https://doi.org/10.3892/etm.2018.6956
Wang C, Jiang J, Ji J, Cai Q, Chen X, Yu Y, Zhu Z, Zhang J (2017) PKM2 promotes cell migration and inhibits autophagy by mediating PI3K/AKT activation and contributes to the malignant development of gastric cancer. Sci Rep 7:2886. https://doi.org/10.1038/s41598-017-03031-1
Gu R, Liu R, Wang L, Tang M, Li SR, Hu X (2021) LncRNA RPPH1 attenuates Aβ(25–35)-induced endoplasmic reticulum stress and apoptosis in SH-SY5Y cells via miR-326/PKM2. Int J Neurosci 131:425–432. https://doi.org/10.1080/00207454.2020.1746307
Inoue M, Hada K, Shiraishi H, Yatsuka H, Fujinami H, Morisaki I, Nishida Y, Matsubara E et al (2020) Tyrosine pre-transfer RNA fragments are linked to p53-dependent neuronal cell death via PKM2. Biochem Biophys Res Commun 525:726–732. https://doi.org/10.1016/j.bbrc.2020.02.157
Martin GS (2003) Cell signaling and cancer. Cancer Cell 4:167–174. https://doi.org/10.1016/s1535-6108(03)00216-2
Hanahan D, Weinberg RA (2011) Hallmarks of cancer: the next generation. Cell 144:646–674. https://doi.org/10.1016/j.cell.2011.02.013
Li H, Zhong Y, Cao G, Shi H, Liu Y, Li L, Yin P, Chen J et al (2022) METTL3 promotes cell cycle progression via m(6)A/YTHDF1-dependent regulation of CDC25B translation. Int J Biol Sci 18:3223–3236. https://doi.org/10.7150/ijbs.70335
Israels ED, Israels LG (2001) The cell cycle. Stem Cells 19:88–91. https://doi.org/10.1634/stemcells.19-1-88
Lunt SY, Muralidhar V, Hosios AM, Israelsen WJ, Gui DY, Newhouse L, Ogrodzinski M, Hecht V et al (2015) Pyruvate kinase isoform expression alters nucleotide synthesis to impact cell proliferation. Mol Cell 57:95–107. https://doi.org/10.1016/j.molcel.2014.10.027
Qiao H, He X, Zhang Q, Yuan H, Wang D, Li L, Hui Y, Wu Z et al (2019) Alpha-synuclein induces microglial migration via PKM2-dependent glycolysis. Int J Biol Macromol 129:601–607. https://doi.org/10.1016/j.ijbiomac.2019.02.029
Zhang J, Feng G, Bao G, Xu G, Sun Y, Li W, Wang L, Chen J et al (2015) Nuclear translocation of PKM2 modulates astrocyte proliferation via p27 and -catenin pathway after spinal cord injury. Cell Cycle 14:2609–2618. https://doi.org/10.1080/15384101.2015.1064203
Lu L, Wang H, Liu X, Tan L, Qiao X, Ni J, Sun Y, Liang J et al (2021) Pyruvate kinase isoform M2 impairs cognition in systemic lupus erythematosus by promoting microglial synaptic pruning via the β-catenin signaling pathway. J Neuroinflammation 18:229. https://doi.org/10.1186/s12974-021-02279-9
Roué G, Pichereau V, Lincet H, Colomer D, Sola B (2008) Cyclin D1 mediates resistance to apoptosis through upregulation of molecular chaperones and consequent redistribution of cell death regulators. Oncogene 27:4909–4920. https://doi.org/10.1038/onc.2008.126
Schoenebeck B, Bader V, Zhu XR, Schmitz B, Lübbert H, Stichel CC (2005) Sgk1, a cell survival response in neurodegenerative diseases. Mol Cell Neurosci 30:249–264. https://doi.org/10.1016/j.mcn.2005.07.017
Thompson EB (1998) The many roles of c-Myc in apoptosis. Annu Rev Physiol 60:575–600. https://doi.org/10.1146/annurev.physiol.60.1.575
Zhang A, Yu F, Yu W, Ye P, Liu P, Gu Y, Chen S, Zhang H (2020) Pyruvate kinase M2 activation protects against the proliferation and migration of pulmonary artery smooth muscle cells. Cell Tissue Res 382:585–598. https://doi.org/10.1007/s00441-020-03245-2
Feng Y, Li X, Wang J, Huang X, Meng L, Huang J (2022) Pyruvate kinase M2 (PKM2) improve symptoms of post-ischemic stroke depression by activating VEGF to mediate the MAPK/ERK pathway. Brain Behav 12:e2450. https://doi.org/10.1002/brb3.2450
Theis V, Theiss C (2018) VEGF - a stimulus for neuronal development and regeneration in the CNS and PNS. Curr Protein Pept Sci 19:589–597. https://doi.org/10.2174/1389203719666180104113937
Zohrabian VM, Forzani B, Chau Z, Murali R, Jhanwar-Uniyal M (2009) Rho/ROCK and MAPK signaling pathways are involved in glioblastoma cell migration and proliferation. Anticancer Res 29:119–123
Kodani A, Kikuchi T, Tohda C (2019) Acteoside improves muscle atrophy and motor function by inducing new myokine secretion in chronic spinal cord injury. J Neurotrauma 36:1935–1948. https://doi.org/10.1089/neu.2018.6000
Kikuchi T, Tohda C, Suyama M (2020) Recovery of motor function of chronic spinal cord injury by extracellular pyruvate kinase isoform M2 and the underlying mechanism. Sci Rep 10:19475. https://doi.org/10.1038/s41598-020-76629-7
Krawczyk CM, Holowka T, Sun J, Blagih J, Amiel E, DeBerardinis RJ, Cross JR, Jung E et al (2010) Toll-like receptor-induced changes in glycolytic metabolism regulate dendritic cell activation. Blood 115:4742–4749. https://doi.org/10.1182/blood-2009-10-249540
Bian L, Zhou Y, Zhang D, Jiang T, Xing C, Wu X, Wang T, Zhu X (2023) Negative correlation between serum pyruvate kinase M2 and cognitive function in patients with cerebral small vessel disease. Clin Neurol Neurosurg 225:107586. https://doi.org/10.1016/j.clineuro.2023.107586
Corcoran SE, O’Neill LA (2016) HIF1α and metabolic reprogramming in inflammation. J Clin Invest 126:3699–3707. https://doi.org/10.1172/jci84431
Zhang X, Yang Y, Jing L, Zhai W, Zhang H, Ma Q, Li C, Yan F et al (2021) Pyruvate kinase M2 contributes to TLR-mediated inflammation and autoimmunity by promoting Pyk2 activation. Front Immunol 12:680068. https://doi.org/10.3389/fimmu.2021.680068
O’Neill LA, Golenbock D, Bowie AG (2013) The history of Toll-like receptors - redefining innate immunity. Nat Rev Immunol 13:453–460. https://doi.org/10.1038/nri3446
McGarry T, Biniecka M, Gao W, Cluxton D, Canavan M, Wade S, Wade S, Gallagher L et al (2017) Resolution of TLR2-induced inflammation through manipulation of metabolic pathways in rheumatoid arthritis. Sci Rep 7:43165. https://doi.org/10.1038/srep43165
Das Gupta K, Shakespear MR, Curson JEB, Murthy AMV, Iyer A, Hodson MP, Ramnath D, Tillu VA et al (2020) Class IIa histone deacetylases drive toll-like receptor-inducible glycolysis and macrophage inflammatory responses via pyruvate kinase M2. Cell Rep 30:2712-2728.e8. https://doi.org/10.1016/j.celrep.2020.02.007
Shakespear MR, Halili MA, Irvine KM, Fairlie DP, Sweet MJ (2011) Histone deacetylases as regulators of inflammation and immunity. Trends Immunol 32:335–343. https://doi.org/10.1016/j.it.2011.04.001
Li M, Lu W, Meng Y, Zhang W, Wang F, Sun L, Xu Y (2022) Tetrahydroxy stilbene glucoside alleviates ischemic stroke by regulating conformation-dependent intracellular distribution of PKM2 for M2 macrophage polarization. J Agric Food Chem 70:15449–15463. https://doi.org/10.1021/acs.jafc.2c03923
Chen Q, Shao X, He Y, Lu E, Zhu L, Tang W (2021) Norisoboldine attenuates sepsis-induced acute lung injury by modulating macrophage polarization via PKM2/HIF-1α/PGC-1α pathway. Biol Pharm Bull 44:1536–1547. https://doi.org/10.1248/bpb.b21-00457
Rao J, Wang H, Ni M, Wang Z, Wang Z, Wei S, Liu M, Wang P et al (2022) FSTL1 promotes liver fibrosis by reprogramming macrophage function through modulating the intracellular function of PKM2. Gut 71:2539–2550. https://doi.org/10.1136/gutjnl-2021-325150
Huang J, Liu K, Zhu S, Xie M, Kang R, Cao L, Tang D (2018) AMPK regulates immunometabolism in sepsis. Brain Behav Immun 72:89–100. https://doi.org/10.1016/j.bbi.2017.11.003
Latham T, Mackay L, Sproul D, Karim M, Culley J, Harrison DJ, Hayward L, Langridge-Smith P et al (2012) Lactate, a product of glycolytic metabolism, inhibits histone deacetylase activity and promotes changes in gene expression. Nucleic Acids Res 40:4794–4803. https://doi.org/10.1093/nar/gks066
Xie M, Yu Y, Kang R, Zhu S, Yang L, Zeng L, Sun X, Yang M et al (2016) PKM2-dependent glycolysis promotes NLRP3 and AIM2 inflammasome activation. Nat Commun 7:13280. https://doi.org/10.1038/ncomms13280
Ying ZH, Li HM, Yu WY, Yu CH (2021) Iridin prevented against lipopolysaccharide-induced inflammatory responses of macrophages via inactivation of PKM2-mediated glycolytic pathways. J Inflamm Res 14:341–354. https://doi.org/10.2147/jir.S292244
Zhang B, Shen J, Zhong Z, Zhang L (2021) PKM2 aggravates cerebral ischemia reperfusion-induced neuroinflammation via TLR4/MyD88/TRAF6 signaling pathway. NeuroImmunoModulation 28:29–37. https://doi.org/10.1159/000509710
Byrd-Leifer CA, Block EF, Takeda K, Akira S, Ding A (2001) The role of MyD88 and TLR4 in the LPS-mimetic activity of Taxol. Eur J Immunol 31:2448–2457. https://doi.org/10.1002/1521-4141(200108)31:8%3c2448::aid-immu2448%3e3.0.co;2-n
Gao CL, Hou GG, Liu J, Ru T, Xu YZ, Zhao SY, Ye H, Zhang LY et al (2020) Synthesis and target identification of benzoxepane derivatives as potential anti-neuroinflammatory agents for ischemic stroke. Angew Chem Int Ed Engl 59:2429–2439. https://doi.org/10.1002/anie.201912489
Penas C, Navarro X (2018) Epigenetic modifications associated to neuroinflammation and neuropathic pain after neural trauma. Front Cell Neurosci 12:158. https://doi.org/10.3389/fncel.2018.00158
Prinz M, Priller J (2014) Microglia and brain macrophages in the molecular age: from origin to neuropsychiatric disease. Nat Rev Neurosci 15:300–312. https://doi.org/10.1038/nrn3722
Orihuela R, McPherson CA, Harry GJ (2016) Microglial M1/M2 polarization and metabolic states. Br J Pharmacol 173:649–665. https://doi.org/10.1111/bph.13139
Shen H, Pei H, Zhai L, Guan Q, Wang G (2022) Salvianolic acid C improves cerebral ischemia reperfusion injury through suppressing microglial cell M1 polarization and promoting cerebral angiogenesis. Int Immunopharmacol 110:109021. https://doi.org/10.1016/j.intimp.2022.109021
Zhai L, Ruan S, Wang J, Guan Q, Zha L (2023) NADPH oxidase 4 regulate the glycolytic metabolic reprogramming of microglial cells to promote M1 polarization. J Biochem Mol Toxicol 37:e23318. https://doi.org/10.1002/jbt.23318
Andersson AK, Rönnbäck L, Hansson E (2005) Lactate induces tumour necrosis factor-alpha, interleukin-6 and interleukin-1beta release in microglial- and astroglial-enriched primary cultures. J Neurochem 93:1327–1333. https://doi.org/10.1111/j.1471-4159.2005.03132.x
Lv L, Xu YP, Zhao D, Li FL, Wang W, Sasaki N, Jiang Y, Zhou X et al (2013) Mitogenic and oncogenic stimulation of K433 acetylation promotes PKM2 protein kinase activity and nuclear localization. Mol Cell 52:340–352. https://doi.org/10.1016/j.molcel.2013.09.004
Li X, Zhou R, Peng H, Peng J, Li Q, Mei M (2023) Microglia PKM2 Mediates neuroinflammation and neuron loss in mice epilepsy through the astrocyte C3-Neuron C3R signaling pathway. Brain Sci 13(2):262. https://doi.org/10.3390/brainsci13020262
Wang L, Wang FS, Gershwin ME (2015) Human autoimmune diseases: a comprehensive update. J Intern Med 278:369–395. https://doi.org/10.1111/joim.12395
Mathis D, Shoelson SE (2011) Immunometabolism: an emerging frontier. Nat Rev Immunol 11:81. https://doi.org/10.1038/nri2922
Li XJ, Xu M, Zhao XQ, Zhao JN, Chen FF, Yu W, Gao DY, Luo B (2013) Proteomic analysis of synovial fibroblast-like synoviocytes from rheumatoid arthritis. Clin Exp Rheumatol 31:552–558
Chung-Faye G, Hayee B, Maestranzi S, Donaldson N, Forgacs I, Sherwood R (2007) Fecal M2-pyruvate kinase (M2-PK): a novel marker of intestinal inflammation. Inflamm Bowel Dis 13:1374–1378. https://doi.org/10.1002/ibd.20214
Liu D, Xiao Y, Zhou B, Gao S, Li L, Zhao L, Chen W, Dai B et al (2021) PKM2-dependent glycolysis promotes skeletal muscle cell pyroptosis by activating the NLRP3 inflammasome in dermatomyositis/polymyositis. Rheumatology (Oxford) 60:2177–2189. https://doi.org/10.1093/rheumatology/keaa473
Angiari S, Runtsch MC, Sutton CE, Palsson-McDermott EM, Kelly B, Rana N, Kane H, Papadopoulou G et al (2020) Pharmacological activation of pyruvate kinase M2 inhibits CD4(+) T cell pathogenicity and suppresses autoimmunity. Cell Metab 31:391-405.e8. https://doi.org/10.1016/j.cmet.2019.10.015
Zhu J, Paul WE (2008) CD4 T cells: fates, functions, and faults. Blood 112:1557–1569. https://doi.org/10.1182/blood-2008-05-078154
Kono M, Maeda K, Stocton-Gavanescu I, Pan W, Umeda M, Katsuyama E, Burbano C, Orite SYK, Vukelic M, Tsokos MG, Yoshida N, Tsokos GC (2019) Pyruvate kinase M2 is requisite for Th1 and Th17 differentiation. JCI insight 4(12):e127395. https://doi.org/10.1172/jci.insight.127395
Liu Z, Xu J, Li H, Shu J, Su G, Zhou C, Yang P (2022) PD-1 targeted nanoparticles inhibit activated T cells and alleviate autoimmunity via suppression of cellular energy metabolism mediated by PKM2. Int J Nanomedicine 17:1711–1724. https://doi.org/10.2147/ijn.S349360
Mosure SA, Solt LA (2021) Uncovering new challenges in targeting glycolysis to treat Th17 cell-mediated autoimmunity. Immunometabolism 3(1):e210006. https://doi.org/10.20900/immunometab20210006
Jin X, Zhang W, Wang Y, Liu J, Hao F, Li Y, Tian M, Shu H et al (2020) Pyruvate kinase M2 promotes the activation of dendritic cells by enhancing IL-12p35 expression. Cell Rep 31:107690. https://doi.org/10.1016/j.celrep.2020.107690
Steinman RM (1991) The dendritic cell system and its role in immunogenicity. Annu Rev Immunol 9:271–296. https://doi.org/10.1146/annurev.iy.09.040191.001415
Duan X, Wen Z, Shen H, Shen M, Chen G (2016) Intracerebral hemorrhage, oxidative stress, and antioxidant therapy. Oxid Med Cell Longev 2016:1203285. https://doi.org/10.1155/2016/1203285
Peres BU, Allen AJH, Shah A, Fox N, Laher I, Almeida F, Jen R, Ayas N (2020) Obstructive sleep apnea and circulating biomarkers of oxidative stress: a cross-sectional study. Antioxidants 9:476. https://doi.org/10.3390/antiox9060476
Khan N, Lambert-Messerlian G, Monteiro JF, Hodosy J, Tothova L, Celec P, Eklund E, Curran P et al (2018) Oxidative and carbonyl stress in pregnant women with obstructive sleep apnea. Sleep and Breathing 22:233–240. https://doi.org/10.1007/s11325-017-1475-8
Zhu P, Yang Q, Li G, Chang Q (2021) PKM2 is a potential diagnostic and therapeutic target for retinitis pigmentosa. Dis Markers 2021:1602797. https://doi.org/10.1155/2021/1602797
Siragusa M, Thöle J, Bibli SI, Luck B, Loot AE, de Silva K, Wittig I, Heidler J et al (2019) Nitric oxide maintains endothelial redox homeostasis through PKM2 inhibition. Embo j 38:e100938. https://doi.org/10.15252/embj.2018100938
Wang C, Chao Y, Xu W, Liu Z, Wang H, Huang K (2020) Myeloid FBW7 deficiency disrupts redox homeostasis and aggravates dietary-induced insulin resistance. Redox Biol 37:101688. https://doi.org/10.1016/j.redox.2020.101688
Yang H, Zhu Y, Ye Y, Guan J, Min X, Xiong H (2022) Nitric oxide protects against cochlear hair cell damage and noise-induced hearing loss through glucose metabolic reprogramming. Free Radic Biol Med 179:229–241. https://doi.org/10.1016/j.freeradbiomed.2021.11.020
Magadum A, Singh N, Kurian AA, Munir I, Mehmood T, Brown K, Sharkar MTK, Chepurko E et al (2020) Pkm2 regulates cardiomyocyte cell cycle and promotes cardiac regeneration. Circulation 141:1249–1265. https://doi.org/10.1161/circulationaha.119.043067
Zhu J, Bi Z, Yang T, Wang W, Li Z, Huang W, Wang L, Zhang S et al (2014) Regulation of PKM2 and Nrf2-ARE pathway during benzoquinone induced oxidative stress in yolk sac hematopoietic stem cells. PLoS ONE 9:e113733. https://doi.org/10.1371/journal.pone.0113733
Ren C, Tan P, Gao L, Zeng Y, Hu S, Chen C, Tang N, Chen Y et al (2023) Melatonin reduces radiation-induced ferroptosis in hippocampal neurons by activating the PKM2/NRF2/GPX4 signaling pathway. Prog Neuropsychopharmacol Biol Psychiatry 126:110777. https://doi.org/10.1016/j.pnpbp.2023.110777
Santiago JA, Potashkin JA (2017) Evaluation of RNA blood biomarkers in individuals at risk of Parkinson’s disease. J Parkinsons Dis 7:653–660. https://doi.org/10.3233/jpd-171155
Wei Y, Lu M, Mei M, Wang H, Han Z, Chen M, Yao H, Song N et al (2020) Pyridoxine induces glutathione synthesis via PKM2-mediated Nrf2 transactivation and confers neuroprotection. Nat Commun 11:941. https://doi.org/10.1038/s41467-020-14788-x
Tauffenberger A, Fiumelli H, Almustafa S, Magistretti PJ (2019) Lactate and pyruvate promote oxidative stress resistance through hormetic ROS signaling. Cell Death Dis 10:653. https://doi.org/10.1038/s41419-019-1877-6
Chen Q, Ruan D, Shi J, Du D, Bian C (2023) The multifaceted roles of natural products in mitochondrial dysfunction. Front Pharmacol 14:1093038. https://doi.org/10.3389/fphar.2023.1093038
Pfanner N, Warscheid B, Wiedemann N (2019) Mitochondrial proteins: from biogenesis to functional networks. Nat Rev Mol Cell Biol 20:267–284. https://doi.org/10.1038/s41580-018-0092-0
Frank M, Duvezin-Caubet S, Koob S, Occhipinti A, Jagasia R, Petcherski A, Ruonala MO, Priault M et al (2012) Mitophagy is triggered by mild oxidative stress in a mitochondrial fission dependent manner. Biochim Biophys Acta 1823:2297–2310. https://doi.org/10.1016/j.bbamcr.2012.08.007
Zhu J, Wang KZ, Chu CT (2013) After the banquet: mitochondrial biogenesis, mitophagy, and cell survival. Autophagy 9:1663–1676. https://doi.org/10.4161/auto.24135
Al Ojaimi M, Salah A, El-Hattab AW (2022) Mitochondrial fission and fusion: molecular mechanisms, biological functions, and related disorders. Membranes 12(9):893. https://doi.org/10.3390/membranes12090893
Wu H, Yang P, Hu W, Wang Y, Lu Y, Zhang L, Fan Y, Xiao H et al (2016) Overexpression of PKM2 promotes mitochondrial fusion through attenuated p53 stability. Oncotarget 7:78069–78082. https://doi.org/10.18632/oncotarget.12942
Liu T, Wang B, Li G, Dong X, Yu G, Qian Q, Duan L, Li H et al (2020) Disruption of microRNA-214 during general anaesthesia prevents brain injury and maintains mitochondrial fusion by promoting Mfn2 interaction with Pkm2. J Cell Mol Med 24:13589–13599. https://doi.org/10.1111/jcmm.15222
Varanita T, Soriano ME, Romanello V, Zaglia T, Quintana-Cabrera R, Semenzato M, Menabò R, Costa V et al (2015) The OPA1-dependent mitochondrial cristae remodeling pathway controls atrophic, apoptotic, and ischemic tissue damage. Cell Metab 21:834–844. https://doi.org/10.1016/j.cmet.2015.05.007
Yi Z, Wu Y, Zhang W, Wang T, Gong J, Cheng Y, Miao C (2020) Activator-mediated pyruvate kinase M2 activation contributes to endotoxin tolerance by promoting mitochondrial biogenesis. Front Immunol 11:595316. https://doi.org/10.3389/fimmu.2020.595316
Yang Q, Zou Y, Wei X, Ye P, Wu Y, Ai H, Zhang Z, Tan J et al (2023) PTP1B knockdown alleviates BMSCs senescence via activating AMPK-mediated mitophagy and promotes osteogenesis in senile osteoporosis. Biochim Biophys Acta Mol Basis Dis 1869:166795. https://doi.org/10.1016/j.bbadis.2023.166795
Shen Y, Peng X, Ji H, Gong W, Zhu H, Wang J (2023) Dapagliflozin protects heart function against type-4 cardiorenal syndrome through activation of PKM2/PP1/FUNDC1-dependent mitophagy. Int J Biol Macromol 250:126116. https://doi.org/10.1016/j.ijbiomac.2023.126116
Thal DR, Walter J, Saido TC, Fändrich M (2015) Neuropathology and biochemistry of Aβ and its aggregates in Alzheimer’s disease. Acta Neuropathol 129:167–182. https://doi.org/10.1007/s00401-014-1375-y
Han J, Hyun J, Park J, Jung S, Oh Y, Kim Y, Ryu SH, Kim SH et al (2021) Aberrant role of pyruvate kinase M2 in the regulation of gamma-secretase and memory deficits in Alzheimer’s disease. Cell Rep 37:110102. https://doi.org/10.1016/j.celrep.2021.110102
Pan RY, He L, Zhang J, Liu X, Liao Y, Gao J, Liao Y, Yan Y et al (2022) Positive feedback regulation of microglial glucose metabolism by histone H4 lysine 12 lactylation in Alzheimer’s disease. Cell Metab 34:634-648.e6. https://doi.org/10.1016/j.cmet.2022.02.013
Hur JY, Frost GR, Wu X, Crump C, Pan SJ, Wong E, Barros M, Li T et al (2020) The innate immunity protein IFITM3 modulates γ-secretase in Alzheimer’s disease. Nature 586:735–740. https://doi.org/10.1038/s41586-020-2681-2
Liu T, Ouyang R (2021) Effect of continuous positive air pressure on cognitive impairment associated with obstructive sleep apnea. Zhong Nan Da Xue Xue Bao Yi Xue Ban 46:865–871. https://doi.org/10.11817/j.issn.1672-7347.2021.190600
Allen CNS, Arjona SP, Santerre M, De Lucia C, Koch WJ, Sawaya BE (2022) Metabolic reprogramming in HIV-associated neurocognitive disorders. Front Cell Neurosci 16:812887. https://doi.org/10.3389/fncel.2022.812887
Flick MJ (2022) Targeting neutrophil PKM2 for stroke treatment. Blood 139:1131–1132. https://doi.org/10.1182/blood.2021014199
Venkatesan A, Uzasci L, Chen Z, Rajbhandari L, Anderson C, Lee MH, Bianchet MA, Cotter R et al (2011) Impairment of adult hippocampal neural progenitor proliferation by methamphetamine: role for nitrotyrosination. Mol Brain 4:28. https://doi.org/10.1186/1756-6606-4-28
Butterfield DA, Poon HF, St Clair D, Keller JN, Pierce WM, Klein JB, Markesbery WR (2006) Redox proteomics identification of oxidatively modified hippocampal proteins in mild cognitive impairment: insights into the development of Alzheimer’s disease. Neurobiol Dis 22:223–232. https://doi.org/10.1016/j.nbd.2005.11.002
Liu W, Zhuo P, Li L, Jin H, Lin B, Zhang Y, Liang S, Wu J et al (2017) Activation of brain glucose metabolism ameliorating cognitive impairment in APP/PS1 transgenic mice by electroacupuncture. Free Radic Biol Med 112:174–190. https://doi.org/10.1016/j.freeradbiomed.2017.07.024
Xu A, Tang Y, Zeng Q, Wang X, Tian H, Zhou Y, Li Z (2020) Electroacupuncture enhances cognition by promoting brain glucose metabolism and inhibiting inflammation in the APP/PS1 mouse model of Alzheimer’s disease: a pilot study. J Alzheimers Dis 77:387–400. https://doi.org/10.3233/jad-200242
Li J, Zhang B, Jia W, Yang M, Zhang Y, Zhang J, Li L, Jin T et al (2021) Activation of adenosine monophosphate-activated protein kinase drives the aerobic glycolysis in hippocampus for delaying cognitive decline following electroacupuncture treatment in APP/PS1 mice. Front Cell Neurosci 15:774569. https://doi.org/10.3389/fncel.2021.774569
Gao YJ, Ji RR (2010) Chemokines, neuronal-glial interactions, and central processing of neuropathic pain. Pharmacol Ther 126:56–68. https://doi.org/10.1016/j.pharmthera.2010.01.002
Stemkowski PL, Smith PA (2012) Sensory neurons, ion channels, inflammation and the onset of neuropathic pain. Can J Neurol Sci 39:416–435. https://doi.org/10.1017/s0317167100013937
Rahman MH, Jha MK, Kim JH, Nam Y, Lee MG, Go Y, Harris RA, Park DH et al (2016) Pyruvate dehydrogenase kinase-mediated glycolytic metabolic shift in the dorsal root ganglion drives painful diabetic neuropathy. J Biol Chem 291:6011–6025. https://doi.org/10.1074/jbc.M115.699215
Zhang ZJ, Jiang BC, Gao YJ (2017) Chemokines in neuron-glial cell interaction and pathogenesis of neuropathic pain. Cell Mol Life Sci 74:3275–3291. https://doi.org/10.1007/s00018-017-2513-1
Hossain MZ, Unno S, Ando H, Masuda Y, Kitagawa J (2017) Neuron-Glia crosstalk and neuropathic pain: involvement in the modulation of motor activity in the Orofacial Region. Int J Mol Sci 18(10):2051. https://doi.org/10.3390/ijms18102051
Sebestova M, Lackner I, Inayat M, Ademaj A, Mikutta C (2021) Post stroke depression. Ther Umsch 78:299–304. https://doi.org/10.1024/0040-5930/a001274
Cui R (2015) Editorial: a systematic review of depression. Curr Neuropharmacol 13:480. https://doi.org/10.2174/1570159x1304150831123535
Guo J, Wang J, Sun W, Liu X (2022) The advances of post-stroke depression: 2021 update. J Neurol 269:1236–1249. https://doi.org/10.1007/s00415-021-10597-4
Li Z, Xu H, Xu Y, Lu G, Peng Q, Chen J, Bi R, Li J et al (2021) Morinda officinalis oligosaccharides alleviate depressive-like behaviors in post-stroke rats via suppressing NLRP3 inflammasome to inhibit hippocampal inflammation. CNS Neurosci Ther 27:1570–1586. https://doi.org/10.1111/cns.13732
Yu J, Xu W, Luo Y, Ou W, Li S, Chen X, Xu J (2019) Dynamic monitoring of depressive behavior induced by nonylphenol and its effect on synaptic plasticity in rats. Sci Total Environ 689:1012–1022. https://doi.org/10.1016/j.scitotenv.2019.06.250
Yang SQ, Tang YY, Zeng D, Tian Q, Wei HJ, Wang CY, Zhang P, Chen YJ et al (2022) Sodium hydrosulfide reverses β(2)-microglobulin-induced depressive-like behaviors of male Sprague-Dawley rats: involving improvement of synaptic plasticity and enhancement of Warburg effect in hippocampus. Behav Brain Res 417:113562. https://doi.org/10.1016/j.bbr.2021.113562
Funding
This work was supported by the National Natural Science Foundation of China (grant number 82060218).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. The first draft of the manuscript was written by Xiaoping Zhang, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, X., Lei, Y., Zhou, H. et al. The Role of PKM2 in Multiple Signaling Pathways Related to Neurological Diseases. Mol Neurobiol 61, 5002–5026 (2024). https://doi.org/10.1007/s12035-023-03901-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-023-03901-y