Abstract
Ischemia-reperfusion injury (I/R injury) is a common feature of ischemic stroke which occurs when blood supply is restored after a period of ischemia. Although stroke is an important cause of death in the world, effective therapeutic strategies aiming at improving neurological outcomes in this disease are lacking. Various studies have suggested the involvement of different mechanisms in the pathogenesis of I/R injury in the nervous system. These mechanisms include oxidative stress, platelet adhesion and aggregation, leukocyte infiltration, complement activation, blood-brain barrier (BBB) disruption, and mitochondria-mediated mechanisms. Curcumin, an active ingredient of turmeric, can affect all these pathways and exert neuroprotective activity culminating in the amelioration of I/R injury in the nervous system. In this review, we discuss the protective effects of curcumin against I/R injury in the nervous system and highlight the studies that have linked biological functions of curcumin and I/R injury improvement.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Stroke is a major cause of death and disability in the world. Epidemiological studies have indicate that 80% of stroke cases are cerebral stroke [1]. The goal of treatment in ischemic stroke is to repair damaged tissues by restoring blood flow (reperfusion). Although reperfusion is a signal for the termination of hypoxia, it may subsequently increase cell death and damage [2]. Indeed, stroke can lead to cognitive and memory impairment, motor dysfunctions and, ultimately, dementia and neuronal death. Several signaling mechanisms are involved in the pathophysiology of ischemia-reperfusion injury (I/R injury) including inflammation, oxidative stress, disruption of the blood-brain barrier (BBB), mitochondria-mediated mechanisms, and leukocyte infiltration [3,4,5,6]. Innate and adaptive immune systems as well as the platelets, complement system and coagulation factors are also involved in I/R injury. After activation of these systems, necrosis and apoptosis occur via a number of mechanisms that ultimately lead to cell death. These processes stimulate the inflammatory system and lead to further release of nucleotides which make phagocytosis progress and ultimately worsen reperfusion injury [7, 8].
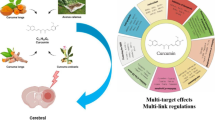
Several lines of experimental evidence have shown that phytocompounds such as crocin [9], carvacrol [10], thymoquinone [11], and curcumin [12] as well as different plants such as Artemisia absinthium, Ocimum basilicum, Ocimum sanctum, Ginkgo biloba, Gastrodia elata, Camellia sinensis, Olea europaea, Oleaceae europaea, and Lavandula officinalis have the potential to be efficacious in the treatment of stroke because of their antioxidant, free radical-scavenging, anti-thrombotic, anti-apoptotic, and neuroprotective properties [13].
Previous investigations have indicated that one of the compounds that can be effective in the treatment of stroke is curcumin. Curcumin is a yellow polyphenolic compound derived from turmeric. Previous reports have proposed that curcumin can be used as a potential drug for the treatment of many diseases such as cancer [14,15,16,17,18,19], diabetes [20, 21], cardiovascular [22,23,24,25,26,27], arthritic [28,29,30], psychological [31, 32], hepatic [33,34,35,36], pulmonary [37,38,39], and neurodegenerative disorders [40]. Most of these therapeutic effects have been attributed to the anti-inflammatory [29, 41, 42], antioxidant [43], and immunomodulatory [44,45,46,47] properties of curcumin. One of the beneficial features of curcumin is that despite its daily and long-term use in Asian countries, toxicity has not been reported [48, 49]. Several studies on the protective effects of curcumin have been presented in I/R experimental models [50,51,52]. For example, it has been shown that administration of curcumin prevents the negative effects of stroke on biochemical parameters, neurological scores, apoptosis, and subsequently infarct volume, edema, and hemorrhage in rats [53,54,55]. The aim of the present review was to explore these protective effects of curcumin against I/R injury in the nervous system.
I/R Injury in the Nervous System
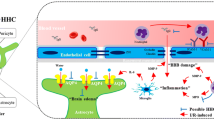
Brain ischemia is caused when brain arteries are blocked acutely and cannot be recovered in a short time [56]. It has been shown that brain tissue and spinal cord are more sensitive to ischemia compared with other tissue such as the heart and kidney. In this regard, the blockage of blood flow to the brain for only 5 min can lead to the death of neurons, while cell death in cardiac or kidney tissues occurs after 20–40 min of ischemia [57, 58]. Ischemia-reperfusion (I/R) is the restoration of blood supply to an organ with seriously decreased or entirely stopped blood flow. Reperfusion is the main treatment for acute stroke and, at the same time, it can also worsen tissue damage and limit the recovery of function [8, 59]. Reperfusion may occur spontaneously after a stroke or it can also be achieved by thrombolytic therapy or endovascular therapy [60]. It has been shown in previous studies [61,62,63] that while reperfusion may improve complications in some cases, it may worsen brain injury in others. It has been indicated that the mechanisms underlying I/R injury include leukocyte infiltration, platelet activation, oxidative stress, complement activation, mitochondria-mediated mechanisms, disruption of the BBB, and ultimately post-ischemic hyperperfusion leading to edema or hemorrhagic transformation (HT) in the brain and spinal cord (Fig. 1) [6, 58, 64]. Leucocyte infiltration plays the main role in initiating the inflammatory process of cerebral ischemia-reperfusion injury. During reperfusion, chemical signals trigger binding of leukocytes to endothelial cells, followed by the production of neutrophil-derived oxidants and matrix metallo-proteinases that impair BBB [65]. It has been shown that after reperfusion platelets are activated and produce oxygen radicals and release pro-inflammatory factors such as platelet-derived growth factor, thromboxane A2, arachidonic acid metabolites, platelet factor 4, and serotonin [66].
Schematic diagram showing the various mechanisms of ischemia-reperfusion injury. The mechanisms of ischemia-reperfusion injury involves leukocyte infiltration, platelet activation, oxidative stress, complement activation, mitochondrial-mediated mechanisms, disruption of the BBB, and eventually post-ischemic hyperperfusion leading to edema or hemorrhagic transformation
Oxidative stress also plays an important role in the pathogenesis of cerebral I/R injury. Oxidative stress occurs when the reactive oxygen species (ROS) surpass the antioxidant capacity of a cell or tissue. Prior studies have shown that production of ROS is increased after cerebral I/R injury, and these species can damage nearly all cellular components such as membrane lipids, proteins, and nucleic acids [67,68,69]. In I/R, due to increased amounts of free radicals, and deterioration and inactivation of antioxidant enzymes, defensive mechanisms are not enough to protect the tissue. Ischemia causes cell death through deprivation of oxygen supply, cell energy evacuation, and accumulation of toxic metabolites in the tissue. In contrast, reperfusion causes more tissue damage than that caused by ischemia [70, 71]. Cell energy evacuation causes inhibition of the Na+, K+-ATPase pump in the cell membrane. Consequently, intracellular Ca2+ ion concentration increases and activates several Ca2+-dependent enzymes like phospholipases, proteases, and endonucleases which may be involved in the production of ROS [72, 73]. Xanthine oxidase, NADPH oxidase (Nox), mitochondria, and uncoupled nitric oxide synthase are the main sources of ROS involved in reperfusion-induced oxidative stress.
Nitric oxide (NO) and superoxide anion (O2−) are generated in the brain during I/R via Nox and neuronal nitric oxide synthase (nNOS) activity, respectively. Peroxynitrite (ONOO−) produced by the interaction between NO and O2−. ONOO− is a potent oxidative radical that causes protein nitration and impairment. .OH, another oxidant, which is produced from H2O2, causes lipid peroxidation and protein, DNA and RNA oxidation, and subsequently cell death. Small amounts of these oxidants as signaling molecules are needed for the body but their increase in I/R injury leads to dysfunction [74,75,76].
The complement system is another main cause of I/R injury. It is a part of the innate immune system and consists of numerous cascades which are involved in the onset of inflammation induced by pathogens and therefore neuronal cell death. The complement system is implicated in I/R injury via different pathways including the antibody-dependent classical pathway, the lectin pathway or the alternative pathway, which are started by C1q, MBL/ficolins/collectin-11, and C3b, respectively. All of these pathways may cause the activation and cleavage of C3 into C3a and C3b. Finally, a complex called membrane attack complex (MAC) is formed through the activity of inflammatory mediators (anaphylatoxin C5a, distal complement component C5b-9), which cause various impairments including increased cell membrane permeability by formation of transmembrane channels, recruitment of leukocytes to the reperfused tissue, and induction of endothelial expression of monocyte chemo-attractant protein-1 (MCP-1), which has a main role in inflammation in the central nervous system (CNS) [77, 78].
Mitochondrial mechanisms play an important role in mediating cerebral I/R injury in several ways such as ROS generation, apoptosis, and necrosis [67, 79]. Studies have shown that disruption of BBB occurs in cerebral reperfusion injury and this leads to edema and hemorrhagic transformation following hyperperfusion [80, 81]. Within the CNS, astrocytes are fundamental for processes such as the development and maintenance of the BBB, promotion of neurovascular coupling, recruitment of cells through the release of chemokines, release of gliotransmitters, regulation of calcium levels, release and transport of glutamate by calcium signaling through the GLAST and EAAT transporters, maintenance of brain general metabolism, control of cerebral pH, uptake of GABA (γ-aminobutyric acid) by specific transporters, and the production of antioxidant enzymes [3, 5, 82,83,84,85]. During I/R, astrocyte undergoes morphological changes and turn into a reactive-like hyperplasic state. This may result in the formation of a glial scar [86] and secretion of various inflammatory and damaging molecules that may worsen the still intact nervous tissue and expands the penumbra towards the healthy brain tissue. It is important to note that neurons are more susceptible to I/R injury than astrocytes, since these cells have a lower antioxidant capacity and require a great deal of metabolic coupling with astrocytes to combat oxidative stress [85], especially during an I/R event. Previous studies have shown mitochondrial dysfunction in astrocytes upon glucose deprivation in an in vitro model of ischemia. The reported mitochondrial dysfunction was reflected by reduced mitochondrial mass, increased oxidative stress, and reduced mitochondrial membrane potential [87, 88]. On the contrary, other studies pointed that improving mitochondrial function in astrocytes by targeting neuroglobin, a protein of globin family, aimed at protecting neurons is an important experimental strategy to counteract inflammatory stimuli [89,90,91].
Potential Therapeutic Strategies in Stroke: Curcumin
Curcuma longa L., generally known as turmeric, is a native plant of South Asia, India, and Indonesia and is mainly grown in South India [92]. It belongs to the ginger family. The main bioactive constituents of turmeric are curcuminoids that include demethoxycurcumin (DMC), bisdemethoxycurcumin (BDMC), and curcumin. Curcumin is the predominant curcuminoid which can constitute as high as 80% of total curcuminoids in turmeric [93, 94]. Commercial extracts of curcumin are a mixture of all three mentioned curcuminoids [95]. Curcumin is used as a spice, food preservative, and coloring agent while having a long history of use in the Ayurvedic medicine for the treatment of various diseases [96]. Vogel and Pelletier for the first time isolated impure form of curcumin in 1815, and its chemical structure was discovered by Milobedzka and Lampe in 1910 as diferuloylmethane or 1,6-heptadiene-3,5-dione-1,7-bis (4-hydroxy-3-methoxyphenyl)-(1E, 6E) (Fig. 2) [97]. Curcumin has a light yellow color and is used as a natural coloring agent in the food industry (the code for this usage is E100) [98]. Because of low oral absorption of curcumin and its rapid metabolism in the liver, consumption of curcumin with piperine has been suggested as an efficient strategy to increase the bioavailability of curcumin [99, 100]. Also, micellar surfactants and phospholipid complexed have been shown to increase the absorption of curcumin by significant orders [101, 102].
Curcumin is a pleiotropic molecule and has numerous molecular and cellular targets by which it can exert its biological effects. These targets include growth factor receptors, transcription factors, protein kinases, adhesion molecules, apoptosis-related proteins, inflammatory cytokines, enzymes like ATPase, cyclooxygenase-2 (COX-2), and matrix metallo-proteinases [103]. Spectroscopic results showed that curcumin binds to human serum albumin with a strong affinity [104]. Furthermore, curcumin has been reported to possess wide range of biological activities including antioxidant [105], antivenom [106], antimicrobial [107], anti-HIV [108], anti-tumor [109], anti-inflammatory [110], antiprotozoal [111], nephroprotective [112], and antirheumatic [113] activities plus therapeutic effects against myocardial infarction [114], skin diseases [115], and cystic fibrosis [116].
Neuroprotective Effects of Curcumin
It has been shown that curcumin has protective effects against neuronal damage risk factors like inflammation [117], free radicals [118], ischemia [119], amyloid [120], and apoptosis [121]. Previous research has also shown that curcumin regulates adhesion molecules, cytokines, protein kinases, and enzymes that are related to inflammation [122, 123]. Studies have revealed that curcumin can improve many neurological disorders such as anxiety, depression, neuronal injury, Alzheimer’s disease, Parkinson’s disease, multiple sclerosis, Huntington’s pathology, head trauma, and stroke [124]. Moreover, curcumin has been proposed as a potential candidate to increase the cholinergic activity of neurons in streptozotocin-induced dementia in rats [125].
Docosahexaenoic acid (DHA) is an omega-3 fatty acid that is essential for development and protection of the brain. DHA deficiency is related to some neurological disorder like anxiety [126, 127]. Wu et al. showed that curcumin raises the levels of enzymes such as FADS2 and elongase 2 which are involved in the synthesis of DHA in both liver and brain tissues, and increases the production of DHA [128]. Numerous studies reported that curcumin protects cerebellar granule cells, hippocampal cells, and retinal cells against glutamate excitotoxicity [129, 130]. One prior study determined that curcumin can improve cognitive impairment by acting through the brain-derived neurotrophic factor (BDNF) system in a rat traumatic brain injury (TBI) model. In this regard, curcumin may increase BDNF protein levels, which then activate TrkB phosphorylation and hence promote neuronal survival [131]. Furthermore, it has been suggested that curcumin promotes neuronal damage induced by chronic stress via upregulation of serotonin receptor 1A (5-HT1A receptor) mRNA and BDNF [132]. Curcumin has beneficial actions on seizures via its function as a free radical scavenger and an antioxidant [133]. For example, Ono et al. reported that curcumin treatment significantly increased glutathione (GSH) levels in the brain tissue of epileptic mice. GSH is one of the free radical scavengers which protect cells against oxidative damage [134].
Curcumin also regulates monoamine neurotransmission and oxidation in the brain, neuroinflammation, and hypothalamus–pituitary–adrenal (HPA) axis and, through these effects, it can act as an antidepressant [135]. Recently, a randomized double-blind study on 123 subjects with depression showed that curcumin supplementation for 12 weeks could reduce the symptoms of depression in comparison with the control group [136]. It is also hypothesized that neuroprotection of curcumin might be mediated via BDNF/tyrosine kinase B (TrkB)MAPK/PI-3K-cyclic AMP response element binding protein (CREB) signaling pathway. In this sense, Wang et al. confirmed the effect of curcumin on the activation of this signaling cascade and showed that this compound induced the viability of cultured rodent cortical neurons [137].
It is proven that curcumin has anti-inflammatory, antioxidant, and anti-amyloid activity; therefore, it can be useful in the treatment and/or prevention of Alzheimer’s disease (AD) as shown previously [138]. Previous works have indicated that curcumin inhibits lipoxygenase and COX-2, two enzymes that are responsible for the synthesis of the pro-inflammatory leukotrienes, prostaglandins, and thromboxanes [139]. Another factor that is involved in the pathophysiology of AD is cholesterol, which is involved in β-amyloid (Aβ) deposition. It has been shown that the use of curcuminoids (500 mg/day) for 7 days decreased the levels of serum cholesterol and lipid peroxides in healthy volunteers [140]. Furthermore, Yang et al. reported that in AD mice model, administration of curcumin decreased the level of Aβ by 40% in comparison with control mice [141]. Several studies support the clinical application of curcumin in Parkinson’s disease (PD) [142, 143]. Aggregation of oxidized DNA is involved in the pathophysiology of PD [144] and transition metal ions such as Fe (II/III) and Cu (II) inhibit DNA repair enzymes [145]. As such, curcumin can reverse such inhibition of DNA repair enzymes both in vitro and in vivo [143]. Furthermore, the antioxidant activity of curcumin protects substantia nigra neurons, improves striatal dopamine levels and chelates Fe2+ in the 6-OHDA rat model of PD [142].
Protective Effects of Curcumin Against Neurological I/R Injury
Curcumin has many protective effects against neurological IRI in brain and spinal cord. In this section, we will address some signaling mechanisms that are sought to be protective upon treatment with curcumin.
Effect of Curcumin Against I/R Injury in Brain
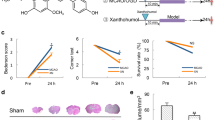
Administration of curcumin (300 mg/kg ip) prior to reperfusion in rat middle cerebral artery occlusion (MCAO) model reduced infarct size and brain edema at 24 h, improved microvascular hemodynamics, and restored blood velocity and shear rate. Treatment with curcumin also improved neurological function and subsequently neurological scores at 24 h. The main protective effect of curcumin was recognized in the striatum, where the highest reduction in infarct size and brain edema was observed [146]. In another study, significant impairment of the motor performance was seen in the embolic occlusion of the MCAO model of rats [147]. Increased neurological defects and reduced dwell-time on the rotarod occurred in animals which may be due to neural damage in the cerebellum that regulates motor coordination [148, 149]. Results from another study showed that occlusion-induced ischemia caused severe neurobehavioral deficits in animals and the defects were significantly smaller in curcumin-treated animals at 3, 7, and 12 day after stroke. It has been shown that curcumin did not improve neurobehavioral recovery at 1 day after stroke, possibly because of the dose and administration route used. Furthermore, curcumin treatment increases BrdU (marker of migrating cells) labeled cells 12 days after MCAO, suggesting rapid migration of new cells into the ischemic region and indicating DNA replication [150]. Investigators suggest that 12 day-period is suitable for observing a major part of neurogenesis and migration that occurs after stroke in rats [151]. In a recent study conducted by Altinay et al., cellular damage indices such as shrunken cytoplasm, atrophic neurons, and damaged nuclei were present in hematoxylin and eosin-stained forebrain sections of stroke animals and these parameters were found to be reduced upon administration of curcumin [53]. It has also been demonstrated that astrogliosis plays a main role in the pathology of cerebral ischemia [5, 152, 153]. In this regard, Kalani et al. showed that curcumin-loaded embryonic stem cell exosomes (MESC-exocur) normalized astrogliosis and improved neuronal survival following I/R injury in mice. Moreover, tight junction protein loss induced by IRI was alleviated in mice treated with MESC-exocur [54]. Major findings from another study indicated that a single-dose administration of FeTPPs, curcumin, or minocycline improved 24-h post-stroke bleeding at the reperfusion site in diabetic animals and this was associated with reduced matrix metallo-proteinases-9 activity [55]. Dietary supplementation with curcumin (2.0 g/kg) for 2 months reduced neuronal death in the hippocampal CA1 region in an experimental I/R-induced brain ischemia model [154]. Furthermore, reduction in locomotor count and decrease in grip strength were improved in middle cerebral artery (MCA)-occluded rats following intranasal delivery of curcumin, DMC, and BDMC [155]. A summary of protective effects of curcumin in I/R injury is displayed in Table 1.
Effect of Curcumin Against I/R Injury in Spinal Cord
Lin et al. showed that curcumin strongly reduced RANTES production in reactive astrocytes both in vitro and in vivo, and this may contribute to its neuroprotection during spinal cord ischemia. The authors also indicated that curcumin inhibited neuronal loss and astrocyte activation, and improved neurological deficits [160]. Similarly, administration of curcumin significantly decreased axonal damage, neuronal degeneration, and glial cell infiltration parameters in I/R-induced spinal cord ischemia in rabbits [158]. In a recent study conducted by Gokce et al., rats from the I/R injury group that received saline treatment exhibited histological changes related to ischemic injury including widespread edema, diffused hemorrhage and congestion and neuronal damage, as evidenced by pyknosis, intense axonal swelling, loss of cytoplasmic features, and cytoplasmic eosinophilia. On the contrary, curcumin (200 mg/kg for 7 days before induction of I/R injury) markedly reduced these pathological changes in rats (153, 154), suggesting that curcumin protects spinal cord tissue in these animals against injury. Moreover, the mean number of normal motor neurons in the anterior spinal cords decreased in rats sufferring from spinal cord IRI while curcumin-treated rats had significantly greater numbers of normal motor neurons than rats sufferring from spinal cord IRI (153, 154). Furthermore, the authors also showed that ultrastructural abnormalities in white and gray matter induced by I/R injury such as severe interruptions and separations in small, medium, and large myelinated axons, separations and interruptions in myelin configuration, swollen neuronal mitochondria, and perineural edema were less severe in curcumin-treated animals. The severity of hind-limb motor dysfunction after spinal cord I/R injury in rats was determined using the Basso, Beattie, and Bresnahan grading scale. Animals in the I/R injury group showed severe neurological deficits and decreased score, while treatment with curcumin increased the abovementioned score [58, 157, 159].
Molecular Mechanisms Underlying Protective Effects of Curcumin Against I/R Injury
There are several molecular mechanisemes underlying protective effects of curcumin against I/R injury as described in details below.
The Effect of Curcumin on Inflammation and Oxidative Stress
In the early stages of I/R injury, inflammation accelerates the process of injury and determines the severity of cerebral damage [161]. Oxidative stress and overproduction of reactive oxygen species (ROS) is a constant feature and an important mechanism of I/R injury [162]. Althogh ROS play several key roles in normal physiology, excessive production of these species may contribute to the pathophysiology of I/R injury as the brain tissue is very sensitive to oxidative damage. Previous studies have identified that administration of curcumin improved I/R injury due to its antioxidant effects [163,164,165]. Morover, significantly prevented cerebral I/R injury (CIRI) via ameliorating oxidative damage [155, 166]. Possible mechanisms of the protective effect of curcumin against oxidative stress include decreasing lipid peroxidation (a sensitive marker of oxidative damage), enhancement of protein synthesis, scavenging of free radicals, increasing glutathione (GSH) content, and preservation of cell membrane integrity [155, 166, 167]. Jia et al. reported that peroxiredoxin 6 (PRDX6) upregulation by curcumin treatment attenuated ischemic oxidative damage through transcription factor specific protein 1 (SP1) induction in rats after stroke [166]. Another study showed that curcumin induced the expression of thioredoxin (an antioxidant protein) and protected neurons from oxygen-glucose deprivation-induced death in an in vitro model of I/R [168]. Among potential mediators of ischemic brain pathology are inflammatory cytokines such as IL-1β, IL-6, TNF-α, prostaglandin E2 (PGE2), NO, COX-2 and inducible nitric oxide synthase (iNOS). In this sense, curcumin protects the brain from ischemia via suppression of inflammatory cytokines like TNF-α and IL-6 [169].
Anti-apoptotic Effect of Curcumin
Apoptosis is one of the major pathways that can lead to the process of cell death after I/R injury [153]. Curcumin contributes to neuronal protection possibly through anti-apoptotic mechanisms [170]. Oxidative stress affects the mitochondrial outer membrane and, as a consequence, Bax moves from the cytosol to mitochondria and cytochrome c is released into cytosol, and this translocation is regulated by B-cell lymphoma 2 (Bcl-2) protein. Release of cytochrome c into cytosol leads to the formation of apoptosome, a complex composed of apoptotic-protease activating factor-1, procaspase-9, and ATP. Formation of apoptosome leads to the activation of procaspase-9 and, consequently, activation of procaspase-3. Eventually, caspase-3 leads to DNA fragmentation [171,172,173]. Interestingly, curcumin increased the levels of anti-apoptotic Bcl-2 protein in mitochondria and reduced subsequent translocation of cytochrome c into cytosol, therefore attenuating the downstream caspase activation (Fig. 3) [170]. It has been suggested that the mitochondrial pathway is an important target of curcumin. Ischemia-induced mitochondrial dysfunction in neurons can be detected by measuring the release of cytochrome c from mitochondria. Qun Wang et al. demonstrated that administration of curcumin completely suppressed the ischemia-induced release of cytochrome c [154]. Another mechanism through which curcumin prevents cerebral I/R injury is increasing silent information regulator 1 (Sirt1) expression, a key neuroprotective molecule that is involved in protection against cerebral I/R. In this regard, activation of Sirt1 leads to the deacetylation of p53 and attenuation of apoptosis in the ischemic brain [169].
The propose mechanism of anti-apoptotic effect of curcumin. Oxidative stress affects the mitochondrial outer membrane, Bax moves from the cytosol to mitochondria, and cytochrome c is released into cytosol. This translocation is regulated by Bcl-2 proteins. Release of cytochrome c into cytosol leads to the formation of a complex composed of apoptotic-protease activating factor-1, procaspase-9, and ATP (apoptosome), and this leads to the activation of procaspase-9 and then procaspase-3. Curcumin increases the levels of anti-apoptotic Bcl-2 protein in mitochondria and reduces the translocation of cytochrome c into cytosol, thereby exerting its anti-apoptotic effects
The Effect of Curcumin on Mitochondrial Biogenesis
It has been documented that mitochondrial number/mass, mitochondrial biogenesis, and the mitochondrial uncoupling protein 2 (UCP2) (an inner mitochondrial membrane anion carrier protein implicated in protecting neurons against cerebral ischemia injury), were significantly downregulated in rats with I/R injury, and these changes were reversed by curcumin pretreatment. It has also been demonstrated that mitochondrial biogenesis was increased in the MCAO reperfusion model of rats upon treatment with curcumin [174].
The Effect of Curcumin on Endoplasmic Reticulum
It has been suggested that in response to CIRI, numerous predisposing factors of endoplasmic reticulum stress (ERS) are activated in neurons including depletion of ER Ca2+, aggregation of proteins, decreased protein degradation, and accumulation of lipid peroxidation products in ER and Golgi structures [175]. ERS may induce pro-apoptotic processes and lead to apoptosis [176, 177]. DNA damage-inducible 153 (GADD153) and caspase-12 are among the main drivers of ERS-mediated apoptosis [178]. GADD153 is a signaling molecule which is involved in the development of apoptosis through several pathways such as affecting intracellular Ca2+ metabolism and downregulating Bcl-2 [178,179,180]. Caspase-12 is another important factor in ERS-mediated apoptosis. Caspase-12 is released from the ER during ERS and subsequently activates the caspase cascade and apoptosis. The precise mechanism of curcumin’s effect on ERS inhibition is still unknown, and this may be related to decreasing the activity of nuclear factor (NF)-κB, increasing the expression of PRDX6 or activating the sirtuin type 1 pathway. It has been shown that curcumin can improve ERS via decreasing the expression of the GADD153 and caspase-12, thereby exhibiting protective effects against CIRI in rats [178].
The Effect of Curcumin on Blood-Brain Barrier Integrity
After stroke, there is an increase in the permeability of the vessels and this causes BBB disruption and vasogenic edema. Previous studies have indicated that NO contributes to ischemia-induced disruption of BBB. NO is a free radical which is involved in the pathogenesis of cerebral ischemia due to its neurotoxic effects. NO reacts with O2− quickly and produces ONOO− [181,182,183]. ONOO− is a toxic anion that produces hydroxyl radicals. These radicals impair key enzymes of the tricarboxylic acid cycle, mitochondrial respiratory chain, mitochondrial Ca2+ metabolism and induce DNA damage, leading to endothelial injury. Jiang et al. showed that curcumin prevented ONOO−−mediated BBB disruption and improved cerebral I/R injury (179). The authors hypothesized that curcumin acts via reducing ONOO− production by inhibiting iNOS expression in astrocytes or by a direct route preventing cerebral capillaries’ endothelial cell injury induced by ONOO− [183, 184]. In general, curcumin has been shown to prevent I\R-induced disruption of BBB via numerous mechanisms such as inhibiting the cytotoxicity of SIN-1 on BCECs, reducing water content of the brain in ipsilateral hemisphere, preventing the absorbance of Evans blue dye after focal cerebral ischemia, inhibiting iNOS expression in cultured astrocytes, and blocking NF-κB activation [183,184,185].
Conclusions
In the present review, we discussed the neuroprotective effects of curcumin against I/R injury. Accumulating evidence has shown that curcumin ameliorate I/R injury through different mechanisms such as mitigation of inflammation, apoptosis and ERS, and enhancement of mitochondrial biogenesis. Nevertheless, prospective studies are needed to further elucidate how curcumin could exert its protective effects against cerebral I/R injury and possible therapeutic applications thereof. In particular, supportive evidence from randomized controlled trials would be crucial.
References
Della-Morte D, Guadagni F, Palmirotta R, Testa G, Caso V, Paciaroni M, Abete P, Rengo F et al (2012) Genetics of ischemic stroke, stroke-related risk factors, stroke precursors and treatments. Pharmacogenomics 13(5):595–613
Nour M, Scalzo F, Liebeskind DS (2012) Ischemia-reperfusion injury in stroke. Interv Neurol 1(3–4):185–199
Posada-Duque RA, Barreto GE, Cardona-Gomez GP (2014) Protection after stroke: cellular effectors of neurovascular unit integrity. Front Cell Neurosci 8:231
Sun X, Budas GR, Xu L, Barreto GE, Mochly-Rosen D, Giffard RG (2013) Selective activation of protein kinase C∊ in mitochondria is neuroprotective in vitro and reduces focal ischemic brain injury in mice. J Neurosci Res 91(6):799–807
Barreto G, E White R, Ouyang Y, Xu L, G Giffard R (2011) Astrocytes: targets for neuroprotection in stroke. Cent Nerv Syst Agents Med Chem 11(2):164–173
Lin L, Wang W, Yu Z (2016) Ischemia-reperfusion injury in the brain: mechanisms and potential therapeutic strategies. Biochem Pharmacol (Los Angel) 5(213):2167–0501.1000213
Elliott MR, Chekeni FB, Trampont PC, Lazarowski ER, Kadl A, Walk SF, Park D, Woodson RI et al (2009) Nucleotides released by apoptotic cells act as a find-me signal to promote phagocytic clearance. Nature 461(7261):282
Chen GY, Nuñez G (2010) Sterile inflammation: sensing and reacting to damage. Nat Rev Immunol 10(12):826
Sarshoori JR, Asadi MH, Mohammadi MT (2014) Neuroprotective effects of crocin on the histopathological alterations following brain ischemia-reperfusion injury in rat. Iran J Basic Med Sci 17(11):895
Yu H, Zhang Z-L, Chen J, Pei A, Hua F, Qian X, He J, Liu C-F et al (2012) Carvacrol, a food-additive, provides neuroprotection on focal cerebral ischemia/reperfusion injury in mice. PLoS One 7(3):e33584
Silachev DN, Plotnikov EY, Zorova LD, Pevzner IB, Sumbatyan NV, Korshunova GA, Gulyaev MV, Pirogov YA et al (2015) Neuroprotective effects of mitochondria-targeted plastoquinone and thymoquinone in a rat model of brain ischemia/reperfusion injury. Molecules 20(8):14487–14503
Silva RF, Pogačnik L (2017) Food, polyphenols and neuroprotection. Neural Regen Res 12(4):582
Jivad N, Rabiei Z (2015) Review on herbal medicine on brain ischemia and reperfusion. Asian Pac J Trop Biomed 5(10):789–795
Momtazi AA, Sahebkar A (2016) Difluorinated curcumin: a promising curcumin analogue with improved anti-tumor activity and pharmacokinetic profile. Curr Pharm Des 22(28):4386–4397
Momtazi AA, Shahabipour F, Khatibi S, Johnston TP, Pirro M, Sahebkar A (2016) Curcumin as a microRNA regulator in cancer: a review. Rev Physiol Biochem Pharmacol 171:1–38. https://doi.org/10.1007/112_2016_3
Rezaee R, Momtazi AA, Monemi A, Sahebkar A (2017) Curcumin: a potentially powerful tool to reverse cisplatin-induced toxicity. Pharmacol Res 117:218–227. https://doi.org/10.1016/j.phrs.2016.12.037
Teymouri M, Pirro M, Johnston TP, Sahebkar A (2017) Curcumin as a multifaceted compound against human papilloma virus infection and cervical cancers: a review of chemistry, cellular, molecular, and preclinical features. Biofactors 43(3):331–346. https://doi.org/10.1002/biof.1344
Mirzaei H, Naseri G, Rezaee R, Mohammadi M, Banikazemi Z, Mirzaei HR, Salehi H, Peyvandi M et al (2016) Curcumin: A new candidate for melanoma therapy? Int J Cancer 139(8):1683-1695. https://doi.org/10.1002/ijc.30224
Iranshahi M, Sahebkar A, Hosseini ST, Takasaki M, Konoshima T, Tokuda H (2010) Cancer chemopreventive activity of diversin from Ferula diversivittata in vitro and in vivo. Phytomedicine 17(3–4):269–273. https://doi.org/10.1016/j.phymed.2009.05.020
Panahi Y, Khalili N, Sahebi E, Namazi S, Simental-Mendia LE, Majeed M, Sahebkar A (2018) Effects of curcuminoids plus piperine on glycemic, hepatic and inflammatory biomarkers in patients with type 2 diabetes mellitus: A randomized double-blind placebo-controlled trial. Drug Res (Stuttg). https://doi.org/10.1055/s-0044-101752
Panahi Y, Khalili N, Sahebi E, Namazi S, Karimian MS, Majeed M, Sahebkar A (2017) Antioxidant effects of curcuminoids in patients with type 2 diabetes mellitus: a randomized controlled trial. Inflammopharmacology 25(1):25–31. https://doi.org/10.1007/s10787-016-0301-4
Sahebkar A (2013) Why it is necessary to translate curcumin into clinical practice for the prevention and treatment of metabolic syndrome? Biofactors 39(2):197–208. https://doi.org/10.1002/biof.1062
Panahi Y, Khalili N, Hosseini MS, Abbasinazari M, Sahebkar A (2014) Lipid-modifying effects of adjunctive therapy with curcuminoids-piperine combination in patients with metabolic syndrome: results of a randomized controlled trial. Complement Ther Med 22(5):851–857. https://doi.org/10.1016/j.ctim.2014.07.006
Simental-Mendia LE, Pirro M, Gotto AM Jr, Banach M, Atkin SL, Majeed M, Sahebkar A (2017) Lipid-modifying activity of curcuminoids: a systematic review and meta-analysis of randomized controlled trials. Crit Rev Food Sci Nutr:1–10. https://doi.org/10.1080/10408398.2017.1396201
Sahebkar A (2014) Curcuminoids for the management of hypertriglyceridaemia. Nat Rev Cardiol 11(2):123. https://doi.org/10.1038/nrcardio.2013.140-c1
Ganjali S, Blesso CN, Banach M, Pirro M, Majeed M, Sahebkar A (2017) Effects of curcumin on HDL functionality. Pharmacol Res 119:208–218. https://doi.org/10.1016/j.phrs.2017.02.008
Momtazi AA, Banach M, Pirro M, Katsiki N, Sahebkar A (2017) Regulation of PCSK9 by nutraceuticals. Pharmacol Res 120:157–169. https://doi.org/10.1016/j.phrs.2017.03.023
Panahi Y, Alishiri GH, Parvin S, Sahebkar A (2016) Mitigation of systemic oxidative stress by curcuminoids in osteoarthritis: results of a randomized controlled trial. J Diet Suppl 13(2):209–220. https://doi.org/10.3109/19390211.2015.1008611
Sahebkar A, Cicero AFG, Simental-Mendia LE, Aggarwal BB, Gupta SC (2016) Curcumin downregulates human tumor necrosis factor-alpha levels: a systematic review and meta-analysis of randomized controlled trials. Pharmacol Res 107:234–242. https://doi.org/10.1016/j.phrs.2016.03.026
Sahebkar A, Henrotin Y (2016) Analgesic efficacy and safety of curcuminoids in clinical practice: a systematic review and meta-analysis of randomized controlled trials. Pain Med 17(6):1192–1202. https://doi.org/10.1093/pm/pnv024
Esmaily H, Sahebkar A, Iranshahi M, Ganjali S, Mohammadi A, Ferns G, Ghayour-Mobarhan M (2015) An investigation of the effects of curcumin on anxiety and depression in obese individuals: a randomized controlled trial. Chin J Integr Med 21(5):332–338. https://doi.org/10.1007/s11655-015-2160-z
Panahi Y, Badeli R, Karami GR, Sahebkar A (2015) Investigation of the efficacy of adjunctive therapy with bioavailability-boosted curcuminoids in major depressive disorder. Phytother Res 29(1):17–21. https://doi.org/10.1002/ptr.5211
Zabihi NA, Pirro M, Johnston TP, Sahebkar A (2017) Is there a role for curcumin supplementation in the treatment of non-alcoholic fatty liver disease? The data suggest yes. Curr Pharm Des 23(7):969–982. https://doi.org/10.2174/1381612822666161010115235
Panahi Y, Kianpour P, Mohtashami R, Jafari R, Simental-Mendia LE, Sahebkar A (2017) Efficacy and safety of phytosomal curcumin in non-alcoholic fatty liver disease: a randomized controlled trial. Drug Res (Stuttg) 67(4):244–251. https://doi.org/10.1055/s-0043-100019
Panahi Y, Kianpour P, Mohtashami R, Jafari R, Simental-Mendia LE, Sahebkar A (2016) Curcumin lowers serum lipids and uric acid in subjects with nonalcoholic fatty liver disease: a randomized controlled trial. J Cardiovasc Pharmacol 68(3):223–229. https://doi.org/10.1097/FJC.0000000000000406
Rahmani S, Asgary S, Askari G, Keshvari M, Hatamipour M, Feizi A, Sahebkar A (2016) Treatment of non-alcoholic fatty liver disease with curcumin: a randomized placebo-controlled trial. Phytother Res 30(9):1540–1548. https://doi.org/10.1002/ptr.5659
Panahi Y, Ghanei M, Hajhashemi A, Sahebkar A (2016) Effects of curcuminoids-piperine combination on systemic oxidative stress, clinical symptoms and quality of life in subjects with chronic pulmonary complications due to sulfur mustard: a randomized controlled trial. J Diet Suppl 13(1):93–105. https://doi.org/10.3109/19390211.2014.952865
Lelli D, Sahebkar A, Johnston TP, Pedone C (2017) Curcumin use in pulmonary diseases: state of the art and future perspectives. Pharmacol Res 115:133–148. https://doi.org/10.1016/j.phrs.2016.11.017
Panahi Y, Ghanei M, Bashiri S, Hajihashemi A, Sahebkar A (2015) Short-term curcuminoid supplementation for chronic pulmonary complications due to sulfur mustard intoxication: positive results of a randomized double-blind placebo-controlled trial. Drug Res (Stuttg) 65(11):567–573. https://doi.org/10.1055/s-0034-1389986
Hu S, Maiti P, Ma Q, Zuo X, Jones MR, Cole GM, Frautschy SA (2015) Clinical development of curcumin in neurodegenerative disease. Expert Rev Neurother 15(6):629–637. https://doi.org/10.1586/14737175.2015.1044981
Ghandadi M, Sahebkar A (2017) Curcumin: an effective inhibitor of interleukin-6. Curr Pharm Des 23(6):921–931. https://doi.org/10.2174/1381612822666161006151605
Karimian MS, Pirro M, Majeed M, Sahebkar A (2017) Curcumin as a natural regulator of monocyte chemoattractant protein-1. Cytokine Growth Factor Rev 33:55–63. https://doi.org/10.1016/j.cytogfr.2016.10.001
Sahebkar A, Serban MC, Ursoniu S, Banach M (2015) Effect of curcuminoids on oxidative stress: a systematic review and meta-analysis of randomized controlled trials. J Funct Foods 18:898–909. https://doi.org/10.1016/j.jff.2015.01.005
Mollazadeh H, Cicero AFG, Blesso CN, Pirro M, Majeed M, Sahebkar A (2017) Immune modulation by curcumin: the role of interleukin-10. Crit Rev Food Sci Nutr:1–13. https://doi.org/10.1080/10408398.2017.1358139
Panahi Y, Hosseini MS, Khalili N, Naimi E, Majeed M, Sahebkar A (2015) Antioxidant and anti-inflammatory effects of curcuminoid-piperine combination in subjects with metabolic syndrome: a randomized controlled trial and an updated meta-analysis. Clin Nutr 34(6):1101–1108. https://doi.org/10.1016/j.clnu.2014.12.019
Abdollahi E, Momtazi AA, Johnston TP, Sahebkar A (2018) Therapeutic effects of curcumin in inflammatory and immune-mediated diseases: a nature-made jack-of-all-trades? J Cell Physiol 233(2):830–848. https://doi.org/10.1002/jcp.25778
Ganjali S, Sahebkar A, Mahdipour E, Jamialahmadi K, Torabi S, Akhlaghi S, Ferns G, Parizadeh SM et al (2014) Investigation of the effects of curcumin on serum cytokines in obese individuals: a randomized controlled trial. ScientificWorldJournal 2014:898361. https://doi.org/10.1155/2014/898361
Ammon HP, Wahl MA (1991) Pharmacology of Curcuma longa. Planta Med 57(01):1–7
Soleimani V, Sahebkar A, Hosseinzadeh H (2018) Turmeric (Curcuma longa) and its major constituent (curcumin) as nontoxic and safe substances: review. Phytother Res. https://doi.org/10.1002/ptr.6054
Jeong CW, Yoo KY, Lee SH, Jeong HJ, Lee CS, Kim SJ (2012) Curcumin protects against regional myocardial ischemia/reperfusion injury through activation of RISK/GSK-3beta and inhibition of p38 MAPK and JNK. J Cardiovasc Pharmacol Ther 17(4):387–394. https://doi.org/10.1177/1074248412438102
Kim YS, Kwon JS, Cho YK, Jeong MH, Cho JG, Park JC, Kang JC, Ahn Y (2012) Curcumin reduces the cardiac ischemia-reperfusion injury: involvement of the toll-like receptor 2 in cardiomyocytes. J Nutr Biochem 23(11):1514–1523. https://doi.org/10.1016/j.jnutbio.2011.10.004
Sahebkar A (2010) Molecular mechanisms for curcumin benefits against ischemic injury. Fertil Steril 94(5):e75–e76; author reply e77. https://doi.org/10.1016/j.fertnstert.2010.07.1071
Altinay S, Cabalar M, Isler C, Yildirim F, Celik DS, Zengi O, Tas A, Gulcubuk A (2017) Is chronic curcumin supplementation neuroprotective against ischemia for antioxidant activity, neurological deficit, or neuronal apoptosis in an experimental stroke model? Turk Neurosurg 27(4):537–545
Kalani A, Chaturvedi P, Kamat PK, Maldonado C, Bauer P, Joshua IG, Tyagi SC, Tyagi N (2016) Curcumin-loaded embryonic stem cell exosomes restored neurovascular unit following ischemia-reperfusion injury. Int J Biochem Cell Biol 79:360–369
Kelly-Cobbs AI, Prakash R, Li W, Pillai B, Hafez S, Coucha M, Johnson MH, Ogbi SN et al (2013) Targets of vascular protection in acute ischemic stroke differ in type 2 diabetes. Am J Phys Heart Circ Phys 304(6):H806–H815
Heiss W-D, Thiel A, Grond M, Graf R (1999) Which targets are relevant for therapy of acute ischemic stroke? Stroke 30(7):1486–1489
Lee J-M, Grabb MC, Zipfel GJ, Choi DW (2000) Brain tissue responses to ischemia. J Clin Invest 106(6):723
Akar İ, İnce İ, Arici A, Benli İ, Aslan C, Şenol S, Demir O, Altunkas F et al (2017) The protective effect of curcumin on a spinal cord ischemia-reperfusion injury model. Ann Vasc Surg 42:285–292
Baird A, Donnan GA, Austin M, Fitt GJ, Davis S, McKay W (1994) Reperfusion after thrombolytic therapy in ischemic stroke measured by single-photon emission computed tomography. Stroke 25(1):79–85
Del Zoppo GJ, Saver JL, Jauch EC, Adams HP (2009) Expansion of the time window for treatment of acute ischemic stroke with intravenous tissue plasminogen activator. Stroke 40(8):2945–2948
Yang G-Y, Betz AL (1994) Reperfusion-induced injury to the blood-brain barrier after middle cerebral artery occlusion in rats. Stroke 25(8):1658–1664
Kuroda S, Siesjö B (1997) Reperfusion damage following focal ischemia: pathophysiology and therapeutic windows. Clin Neurosci 4(4):199–212
Aronowski J, Strong R, Grotta JC (1997) Reperfusion injury: demonstration of brain damage produced by reperfusion after transient focal ischemia in rats. J Cereb Blood Flow Metab 17(10):1048–1056
Carden DL, Granger DN (2000) Pathophysiology of ischaemia–reperfusion injury. J Pathol 190(3):255–266
Pan J, Konstas A-A, Bateman B, Ortolano GA, Pile-Spellman J (2007) Reperfusion injury following cerebral ischemia: pathophysiology, MR imaging, and potential therapies. Neuroradiology 49(2):93–102
Massberg S, Enders G, Leiderer R, Eisenmenger S, Vestweber D, Krombach F, Messmer K (1998) Platelet-endothelial cell interactions during ischemia/reperfusion: the role of P-selectin. Blood 92(2):507–515
Sanderson TH, Reynolds CA, Kumar R, Przyklenk K, Hüttemann M (2013) Molecular mechanisms of ischemia–reperfusion injury in brain: pivotal role of the mitochondrial membrane potential in reactive oxygen species generation. Mol Neurobiol 47(1):9–23
Yamato M, Egashira T, Utsumi H (2003) Application of in vivo ESR spectroscopy to measurement of cerebrovascular ROS generation in stroke. Free Radic Biol Med 35(12):1619–1631
Koc ER, Gökce EC, Sönmez MA, Namuslu M, Gökce A, Bodur AS (2015) Borax partially prevents neurologic disability and oxidative stress in experimental spinal cord ischemia/reperfusion injury. J Stroke Cerebrovasc Dis 24(1):83–90
Chan PH (1996) Role of oxidants in ischemic brain damage. Stroke 27(6):1124–1129
Zimmerman BJ, Granger DN (1992) Reperfusion injury. Surg Clin North Am 72(1):65–83
Green C, Gower J, Healing G, Cotterill L, Fuller B, Simpkin S (1989) The importance of iron, calcium and free radicals in reperfusion injury: an overview of studies in ischaemic rabbit kidneys. Free Radic Res Commun 7(3–6):255–264
Orrenius S, Burkitt MJ, Kass GE, Dypbukt JM, Nicotera P (1992) Calcium ions and oxidative cell injury. Ann Neurol 32(S1):S33–S42
Chen H, Yoshioka H, Kim GS, Jung JE, Okami N, Sakata H, Maier CM, Narasimhan P et al (2011) Oxidative stress in ischemic brain damage: mechanisms of cell death and potential molecular targets for neuroprotection. Antioxid Redox Signal 14(8):1505–1517
Chan PH (2001) Reactive oxygen radicals in signaling and damage in the ischemic brain. J Cereb Blood Flow Metab 21(1):2–14
Droge W (2002) Free radicals in the physiological control of cell function. Physiol Rev 82(1):47–95
Gorsuch WB, Chrysanthou E, Schwaeble WJ, Stahl GL (2012) The complement system in ischemia–reperfusion injuries. Immunobiology 217(11):1026–1033
Barnum SR (1999) Inhibition of complement as a therapeutic approach in inflammatory central nervous system (CNS) disease. Mol Med 5(9):569
Nieminen A-L (2003) Apoptosis and necrosis in health and disease: role of mitochondria. Int Rev Cytol 224:29–55
Khatri R, McKinney AM, Swenson B, Janardhan V (2012) Blood–brain barrier, reperfusion injury, and hemorrhagic transformation in acute ischemic stroke. Neurology 79(13 Supplement 1):S52–S57
Sage J, Van Uitert R, Duffy T (1984) Early changes in blood brain barrier permeability to small molecules after transient cerebral ischemia. Stroke 15(1):46–50
Barreto GE, Gonzalez J, Torres Y, Morales L (2011) Astrocytic-neuronal crosstalk: implications for neuroprotection from brain injury. Neurosci Res 71(2):107–113. https://doi.org/10.1016/j.neures.2011.06.004
Cabezas R, Avila M, Gonzalez J, El-Bacha RS, Baez E, Garcia-Segura LM, Jurado Coronel JC, Capani F et al (2014) Astrocytic modulation of blood brain barrier: perspectives on Parkinson’s disease. Front Cell Neurosci 8:211. https://doi.org/10.3389/fncel.2014.00211
Volterra A, Meldolesi J (2005) Astrocytes, from brain glue to communication elements: the revolution continues. Nat Rev Neurosci 6(8):626–640. https://doi.org/10.1038/nrn1722
Hamby ME, Sofroniew MV (2010) Reactive astrocytes as therapeutic targets for CNS disorders. Neurotherapeutics 7(4):494–506. https://doi.org/10.1016/j.nurt.2010.07.003
Barreto GE, White RE, Xu L, Palm CJ, Giffard RG (2012) Effects of heat shock protein 72 (Hsp72) on evolution of astrocyte activation following stroke in the mouse. Exp Neurol 238(2):284–296. https://doi.org/10.1016/j.expneurol.2012.08.015
Avila Rodriguez M, Garcia-Segura LM, Cabezas R, Torrente D, Capani F, Gonzalez J, Barreto GE (2014) Tibolone protects T98G cells from glucose deprivation. J Steroid Biochem Mol Biol 144(Pt B):294–303. https://doi.org/10.1016/j.jsbmb.2014.07.009
Avila-Rodriguez M, Garcia-Segura LM, Hidalgo-Lanussa O, Baez E, Gonzalez J, Barreto GE (2016) Tibolone protects astrocytic cells from glucose deprivation through a mechanism involving estrogen receptor beta and the upregulation of neuroglobin expression. Mol Cell Endocrinol 433:35–46. https://doi.org/10.1016/j.mce.2016.05.024
Baez E, Echeverria V, Cabezas R, Avila-Rodriguez M, Garcia-Segura LM, Barreto GE (2016) Protection by neuroglobin expression in brain pathologies. Front Neurol 7:146. https://doi.org/10.3389/fneur.2016.00146
Cabezas R, Vega-Vela NE, Gonzalez-Sanmiguel J, Gonzalez J, Esquinas P, Echeverria V, Barreto GE (2018) PDGF-BB preserves mitochondrial morphology, attenuates ROS production, and upregulates neuroglobin in an astrocytic model under rotenone insult. Mol Neurobiol 55(4):3085–3095. https://doi.org/10.1007/s12035-017-0567-6
Garzon D, Cabezas R, Vega N, Avila-Rodriguez M, Gonzalez J, Gomez RM, Echeverria V, Aliev G et al (2016) Novel approaches in astrocyte protection: from experimental methods to computational approaches. J Mol Neurosci 58(4):483–492. https://doi.org/10.1007/s12031-016-0719-6
Perrone D, Ardito F, Giannatempo G, Dioguardi M, Troiano G, Lo Russo L, De Lillo A, Laino L et al (2015) Biological and therapeutic activities, and anticancer properties of curcumin. Experimental and Therapeutic Medicine 10(5):1615–1623
Maheshwari RK, Singh AK, Gaddipati J, Srimal RC (2006) Multiple biological activities of curcumin: a short review. Life Sci 78(18):2081–2087
Jayaprakasha G, Rao LJM, Sakariah K (2005) Chemistry and biological activities of C. longa. Trends Food Sci Technol 16(12):533–548
Zhou H, Beevers CS, Huang S (2011) The targets of curcumin. Curr Drug Targets 12(3):332–347
Singh S (2007) From exotic spice to modern drug? Cell 130(5):765–768
Gupta SC, Patchva S, Koh W, Aggarwal BB (2012) Discovery of curcumin, a component of golden spice, and its miraculous biological activities. Clin Exp Pharmacol Physiol 39(3):283–299
Scotter MJ (2011) Methods for the determination of European Union-permitted added natural colours in foods: a review. Food Addit Contam 28(5):527–596
Shoba G, Joy D, Joseph T, Majeed M, Rajendran R, Srinivas P (1998) Influence of piperine on the pharmacokinetics of curcumin in animals and human volunteers. Planta Med 64(04):353–356
Sharma RA, McLelland HR, Hill KA, Ireson CR, Euden SA, Manson MM, Pirmohamed M, Marnett LJ et al (2001) Pharmacodynamic and pharmacokinetic study of oral Curcuma extract in patients with colorectal cancer. Clin Cancer Res 7(7):1894–1900
Liu A, Lou H, Zhao L, Fan P (2006) Validated LC/MS/MS assay for curcumin and tetrahydrocurcumin in rat plasma and application to pharmacokinetic study of phospholipid complex of curcumin. J Pharm Biomed Anal 40(3):720–727
Yu H, Huang Q (2012) Improving the oral bioavailability of curcumin using novel organogel-based nanoemulsions. J Agric Food Chem 60(21):5373–5379
Epstein J, Sanderson IR, MacDonald TT (2010) Curcumin as a therapeutic agent: the evidence from in vitro, animal and human studies. Br J Nutr 103(11):1545–1557
Mandeville J-S, Froehlich E, Tajmir-Riahi H (2009) Study of curcumin and genistein interactions with human serum albumin. J Pharm Biomed Anal 49(2):468–474
Menon VP, Sudheer AR (2007) Antioxidant and anti-inflammatory properties of curcumin. Adv Exp Med Biol 595:105–125
Ferreira LA, Henriques OB, Andreoni AA, Vital GR, Campos MM, Habermehl GG, de Moraes VL (1992) Antivenom and biological effects of ar-turmerone isolated from Curcuma longa (Zingiberaceae). Toxicon 30(10):1211–1218
Teow S-Y, Liew K, Ali SA, Khoo AS-B, Peh S-C (2016) Antibacterial action of curcumin against Staphylococcus aureus: a brief review. J Trop Med 2016:1–10
Ali A, Banerjea AC (2016) Curcumin inhibits HIV-1 by promoting Tat protein degradation. Sci Rep 6:27539
Notarbartolo M, Poma P, Perri D, Dusonchet L, Cervello M, D'Alessandro N (2005) Antitumor effects of curcumin, alone or in combination with cisplatin or doxorubicin, on human hepatic cancer cells. Analysis of their possible relationship to changes in NF-kB activation levels and in IAP gene expression. Cancer Lett 224(1):53–65
Jacob A, Wu R, Zhou M, Wang P (2007) Mechanism of the anti-inflammatory effect of curcumin: PPAR-γ activation. PPAR Res 2007:1–5
Llurba-Montesino N, Kaiser M, Brun R, Schmidt TJ (2015) Search for antiprotozoal activity in herbal medicinal preparations; new natural leads against neglected tropical diseases. Molecules 20(8):14118–14138
Ismail AFM, Salem AA (2016) Renoprotective effect of curcumin on acetaminophen-induced nephrotoxicity in rats. J Chem Pharm Res 8(2):773–779
Dcodhar S, Sethi R, Srimal R (2013) Preliminary study on antirheumatic activity of curcumin (diferuloyl methane). Indian J Med Res 138(1):632–634
Xiao J, Sheng X, Zhang X, Guo M, Ji X (2016) Curcumin protects against myocardial infarction-induced cardiac fibrosis via SIRT1 activation in vivo and in vitro. Drug Design, Development and Therapy 10:1267
Thangapazham RL, Sharma A, Maheshwari RK (2007) Beneficial role of curcumin in skin diseases. Adv Exp Med Biol 595:343–57
Accurso F (2004) Curcumin and cystic fibrosis. J Pediatr Gastroenterol Nutr 39(3):235
Buhrmann C, Mobasheri A, Busch F, Aldinger C, Stahlmann R, Montaseri A, Shakibaei M (2011) Curcumin modulates nuclear factor κB (NF-κB)-mediated inflammation in human tenocytes in vitro role of the phosphatidylinositol 3-kinase/akt pathway. J Biol Chem 286(32):28556–28566
Ak T, Gülçin İ (2008) Antioxidant and radical scavenging properties of curcumin. Chem Biol Interact 174(1):27–37
Shukla PK, Khanna VK, Ali MM, Khan MY, Srimal RC (2008) Anti-ischemic effect of curcumin in rat brain. Neurochem Res 33(6):1036–1043
Huang H-C, Xu K, Jiang Z-F (2012) Curcumin-mediated neuroprotection against amyloid-β-induced mitochondrial dysfunction involves the inhibition of GSK-3β. J Alzheimers Dis 32(4):981–996
Saha L, Chakrabarti A, Kumari S, Bhatia A, Banerjee D (2016) Antiapoptotic and neuroprotective role of Curcumin in Pentylenetetrazole (PTZ) induced kindling model in rat. Indian J Exp Biol 54(2):133–141
Acar A, Akil E, Alp H, Evliyaoglu O, Kibrisli E, Inal A, Unan F, Tasdemir N (2012) Oxidative damage is ameliorated by curcumin treatment in brain and sciatic nerve of diabetic rats. Int J Neurosci 122(7):367–372
Tizabi Y, Hurley LL, Qualls Z, Akinfiresoye L (2014) Relevance of the anti-inflammatory properties of curcumin in neurodegenerative diseases and depression. Molecules 19(12):20864–20879
Cole GM, Teter B, Frautschy SA (2007) Neuroprotective effects of curcumin. Adv Exp Med Biol 595:197–212
Awasthi H, Tota S, Hanif K, Nath C, Shukla R (2010) Protective effect of curcumin against intracerebral streptozotocin induced impairment in memory and cerebral blood flow. Life Sci 86(3–4):87–94
Chen H-F, Su H-M (2013) Exposure to a maternal n-3 fatty acid-deficient diet during brain development provokes excessive hypothalamic–pituitary–adrenal axis responses to stress and behavioral indices of depression and anxiety in male rat offspring later in life. J Nutr Biochem 24(1):70–80
Bhatia HS, Agrawal R, Sharma S, Huo Y-X, Ying Z, Gomez-Pinilla F (2011) Omega-3 fatty acid deficiency during brain maturation reduces neuronal and behavioral plasticity in adulthood. PLoS One 6(12):e28451
Wu A, Noble EE, Tyagi E, Ying Z, Zhuang Y, Gomez-Pinilla F (2015) Curcumin boosts DHA in the brain: implications for the prevention of anxiety disorders. Biochim Biophys Acta 1852(5):951–961
Matteucci A, Cammarota R, Paradisi S, Varano M, Balduzzi M, Leo L, Bellenchi GC, De Nuccio C et al (2011) Curcumin protects against NMDA-induced toxicity: a possible role for NR2A subunit. Invest Ophthalmol Vis Sci 52(2):1070–1077
Matteucci A, Frank C, Domenici M, Balduzzi M, Paradisi S, Carnovale-Scalzo G, Scorcia G, Malchiodi-Albedi F (2005) Curcumin treatment protects rat retinal neurons against excitotoxicity: effect on N-methyl-D-aspartate-induced intracellular Ca 2+ increase. Exp Brain Res 167(4):641–648
Wu A, Ying Z, Gomez-Pinilla F (2006) Dietary curcumin counteracts the outcome of traumatic brain injury on oxidative stress, synaptic plasticity, and cognition. Exp Neurol 197(2):309–317
Xu Y, Ku B, Cui L, Li X, Barish PA, Foster TC, Ogle WO (2007) Curcumin reverses impaired hippocampal neurogenesis and increases serotonin receptor 1A mRNA and brain-derived neurotrophic factor expression in chronically stressed rats. Brain Res 1162:9–18
Frautschy S, Hu W, Kim P, Miller S, Chu T, Harris-White M, Cole G (2001) Phenolic anti-inflammatory antioxidant reversal of Aβ-induced cognitive deficits and neuropathology. Neurobiol Aging 22(6):993–1005
Ono H, Sakamoto A, Sakura N (2000) Plasma total glutathione concentrations in epileptic patients taking anticonvulsants. Clin Chim Acta 298(1–2):135–143
Lopresti AL, Hood SD, Drummond PD (2012) Multiple antidepressant potential modes of action of curcumin: a review of its anti-inflammatory, monoaminergic, antioxidant, immune-modulating and neuroprotective effects. J Psychopharmacol 26(12):1512–1524
Lopresti AL, Drummond PD (2017) Efficacy of curcumin, and a saffron/curcumin combination for the treatment of major depression: a randomised, double-blind, placebo-controlled study. J Affect Disord 207:188–196
Wang R, Li Y-H, Xu Y, Li Y-B, Wu H-L, Guo H, Zhang J-Z, Zhang J-J et al (2010) Curcumin produces neuroprotective effects via activating brain-derived neurotrophic factor/TrkB-dependent MAPK and PI-3K cascades in rodent cortical neurons. Prog Neuro-Psychopharmacol Biol Psychiatry 34(1):147–153
Ringman JM, Frautschy SA, Cole GM, Masterman DL, Cummings JL (2005) A potential role of the curry spice curcumin in Alzheimer’s disease. Curr Alzheimer Res 2(2):131–136
Ammon H, Safayhi H, Mack T, Sabieraj J (1993) Mechanism of antiinflammatory actions of curcumine and boswellic acids. J Ethnopharmacol 38(2–3):105–112
Soni K, Kuttan R (1992) Effect of oral curcumin administration on serum peroxides and cholesterol levels in human volunteers. Indian J Physiol Pharmacol 36:273–273
Yang F, Lim GP, Begum AN, Ubeda OJ, Simmons MR, Ambegaokar SS, Chen PP, Kayed R et al (2005) Curcumin inhibits formation of amyloid β oligomers and fibrils, binds plaques, and reduces amyloid in vivo. J Biol Chem 280(7):5892–5901
Zbarsky V, Datla KP, Parkar S, Rai DK, Aruoma OI, Dexter DT (2005) Neuroprotective properties of the natural phenolic antioxidants curcumin and naringenin but not quercetin and fisetin in a 6-OHDA model of Parkinson’s disease. Free Radic Res 39(10):1119–1125
Hegde ML, Hegde PM, Holthauzen LM, Hazra TK, Rao JK, Mitra S (2010) Specific inhibition of neil-initiated repair of oxidized base damage in human genome by copper and iron and protection using curcumin: potential etiological linkage to neurodegenerative diseases. Alzheimers Dement 6(4):S383–S384
Rao KS (2007) DNA repair in aging rat neurons. Neuroscience 145(4):1330–1340
Grin I, Konorovsky P, Nevinsky G, Zharkov D (2009) Heavy metal ions affect the activity of DNA glycosylases of the fpg family. Biochem Mosc 74(11):1253
Funk JL, Frye JB, Davis-Gorman G, Spera AL, Bernas MJ, Witte MH, Weinand ME, Timmermann BN et al (2013) Curcuminoids limit neutrophil-mediated reperfusion injury in experimental stroke by targeting the endothelium. Microcirculation 20(6):544–554
Dohare P, Garg P, Jain V, Nath C, Ray M (2008) Dose dependence and therapeutic window for the neuroprotective effects of curcumin in thromboembolic model of rat. Behav Brain Res 193(2):289–297
Thiyagarajan M, Sharma SS (2004) Neuroprotective effect of curcumin in middle cerebral artery occlusion induced focal cerebral ischemia in rats. Life Sci 74(8):969–985
Tyagi N, Qipshidze N, Munjal C, Vacek JC, Metreveli N, Givvimani S, Tyagi SC (2012) Tetrahydrocurcumin ameliorates homocysteinylated cytochrome-c mediated autophagy in hyperhomocysteinemia mice after cerebral ischemia. J Mol Neurosci 47(1):128–138
Liu S, Cao Y, Qu M, Zhang Z, Feng L, Ye Z, Xiao M, Hou ST et al (2016) Curcumin protects against stroke and increases levels of Notch intracellular domain. Neurol Res 38(6):553–559
Zhang B, Wang R-z, Z-g L, Song Y, Yao Y (2009) Neurogenesis by activation of inherent neural stem cells in the rat hippocampus after cerebral infarction. Chin Med Sci J 24(1):41–45
Adelson JD, Barreto GE, Xu L, Kim T, Brott BK, Ouyang Y-B, Naserke T, Djurisic M et al (2012) Neuroprotection from stroke in the absence of MHCI or PirB. Neuron 73(6):1100–1107
Barreto GE, Sun X, Xu L, Giffard RG (2011) Astrocyte proliferation following stroke in the mouse depends on distance from the infarct. PLoS One 6(11):e27881
Wang Q, Sun AY, Simonyi A, Jensen MD, Shelat PB, Rottinghaus GE, MacDonald RS, Miller DK et al (2005) Neuroprotective mechanisms of curcumin against cerebral ischemia-induced neuronal apoptosis and behavioral deficits. J Neurosci Res 82(1):138–148
Ahmad N, Umar S, Ashafaq M, Akhtar M, Iqbal Z, Samim M, Ahmad FJ (2013) A comparative study of PNIPAM nanoparticles of curcumin, demethoxycurcumin, and bisdemethoxycurcumin and their effects on oxidative stress markers in experimental stroke. Protoplasma 250(6):1327–1338
Kakkar V, Muppu SK, Chopra K, Kaur IP (2013) Curcumin loaded solid lipid nanoparticles: an efficient formulation approach for cerebral ischemic reperfusion injury in rats. Eur J Pharm Biopharm 85(3):339–345
Liu Z-Q, Xing S-S, Zhang W (2013) Neuroprotective effect of curcumin on spinal cord in rabbit model with ischemia/reperfusion. The Journal of Spinal Cord Medicine 36(2):147–152
Kurt G, Yildirim Z, Cemil B, Celtikci E, Kaplanoglu GT (2014) Effects of curcumin on acute spinal cord ischemia-reperfusion injury in rabbits. J Neurosurg Spine 20(4):464–470
Gokce EC, Kahveci R, Gokce A, Sargon MF, Kisa U, Aksoy N, Cemil B, Erdogan B (2016) Curcumin attenuates inflammation, oxidative stress, and ultrastructural damage induced by spinal cord ischemia–reperfusion injury in rats. J Stroke Cerebrovasc Dis 25(5):1196–1207
Lin M-S, Sun Y-Y, Chiu W-T, Hung C-C, Chang C-Y, Shie F-S, Tsai S-H, Lin J-W et al (2011) Curcumin attenuates the expression and secretion of RANTES after spinal cord injury in vivo and lipopolysaccharide-induced astrocyte reactivation in vitro. J Neurotrauma 28(7):1259–1269
Berner MD, Sura ME, Alves BN, Hunter KW Jr (2005) IFN-γ primes macrophages for enhanced TNF-α expression in response to stimulatory and non-stimulatory amounts of microparticulate β-glucan. Immunol Lett 98(1):115–122
Raza SS, Khan MM, Ahmad A, Ashafaq M, Khuwaja G, Tabassum R, Javed H, Siddiqui MS et al (2011) Hesperidin ameliorates functional and histological outcome and reduces neuroinflammation in experimental stroke. Brain Res 1420:93–105
Sandur SK, Pandey MK, Sung B, Ahn KS, Murakami A, Sethi G, Limtrakul P, Badmaev V et al (2007) Curcumin, demethoxycurcumin, bisdemethoxycurcumin, tetrahydrocurcumin and turmerones differentially regulate anti-inflammatory and anti-proliferative responses through a ROS-independent mechanism. Carcinogenesis 28(8):1765–1773
Sun M, Zhao Y, Gu Y, Xu C (2009) Inhibition of nNOS reduces ischemic cell death through down-regulating calpain and caspase-3 after experimental stroke. Neurochem Int 54(5–6):339–346
Jayaprakasha G, Rao LJ, Sakariah K (2006) Antioxidant activities of curcumin, demethoxycurcumin and bisdemethoxycurcumin. Food Chem 98(4):720–724
Jia G, Tan B, Ma J, Zhang L, Jin X, Li C (2017) Prdx6 upregulation by curcumin attenuates ischemic oxidative damage via SP1 in rats after stroke. Biomed Res Int 2017:1–9
Avci G, Kadioglu H, Sehirli AO, Bozkurt S, Guclu O, Arslan E, Muratli SK (2012) Curcumin protects against ischemia/reperfusion injury in rat skeletal muscle. J Surg Res 172(1):e39–e46
Wu J-x, Zhang L-y, Chen Y-l, Yu S-s, Zhao Y, Zhao J (2015) Curcumin pretreatment and post-treatment both improve the antioxidative ability of neurons with oxygen-glucose deprivation. Neural Regen Res 10(3):481
Miao Y, Zhao S, Gao Y, Wang R, Wu Q, Wu H, Luo T (2016) Curcumin pretreatment attenuates inflammation and mitochondrial dysfunction in experimental stroke: the possible role of Sirt1 signaling. Brain Res Bull 121:9–15
Zhao J, Yu S, Zheng W, Feng G, Luo G, Wang L, Zhao Y (2010) Curcumin improves outcomes and attenuates focal cerebral ischemic injury via antiapoptotic mechanisms in rats. Neurochem Res 35(3):374–379
Kroemer G (2003) Mitochondrial control of apoptosis: an introduction. Biochem Biophys Res Commun 304(3):433–435
Kuwana T, Mackey MR, Perkins G, Ellisman MH, Latterich M, Schneiter R, Green DR, Newmeyer DD (2002) Bid, Bax, and lipids cooperate to form supramolecular openings in the outer mitochondrial membrane. Cell 111(3):331–342
Green DR, Reed JC (1998) Mitochondria and apoptosis. Science 281:1309–1312
Liu L, Zhang W, Wang L, Li Y, Tan B, Lu X, Deng Y, Zhang Y et al (2014) Curcumin prevents cerebral ischemia reperfusion injury via increase of mitochondrial biogenesis. Neurochem Res 39(7):1322–1331
DeGracia DJ, Montie HL (2004) Cerebral ischemia and the unfolded protein response. J Neurochem 91(1):1–8
Martin-Jiménez CA, García-Vega Á, Cabezas R, Aliev G, Echeverria V, González J, Barreto GE (2017) Astrocytes and endoplasmic reticulum stress: a bridge between obesity and neurodegenerative diseases. Prog Neurobiol 158:45–68
Avila MF, Cabezas R, Torrente D, Gonzalez J, Morales L, Alvarez L, Capani F, Barreto GE (2013) Novel interactions of GRP78: UPR and estrogen responses in the brain. Cell Biol Int 37(6):521–532
Zhu H, Fan Y, Sun H, Chen L, Man X (2017) Curcumin inhibits endoplasmic reticulum stress induced by cerebral ischemia-reperfusion injury in rats. Experimental and Therapeutic Medicine 14(5):4047–4052
Ferri KF, Kroemer G (2001) Organelle-specific initiation of cell death pathways. Nat Cell Biol 3(11):E255
Li G, Mongillo M, Chin K-T, Harding H, Ron D, Marks AR, Tabas I (2009) Role of ERO1-α–mediated stimulation of inositol 1, 4, 5-triphosphate receptor activity in endoplasmic reticulum stress–induced apoptosis. J Cell Biol 186(6):783–792
Veltkamp R, Siebing DA, Sun L, Heiland S, Bieber K, Marti HH, Nagel S, Schwab S et al (2005) Hyperbaric oxygen reduces blood–brain barrier damage and edema after transient focal cerebral ischemia. Stroke 36(8):1679–1683
Luo CX, Zhu XJ, Zhang AX, Wang W, Yang XM, Liu SH, Han X, Sun J et al (2005) Blockade of L-type voltage-gated Ca2+ channel inhibits ischemia-induced neurogenesis by down-regulating iNOS expression in adult mouse. J Neurochem 94(4):1077–1086
Jiang J, Wang W, Sun YJ, Hu M, Li F, Zhu DY (2007) Neuroprotective effect of curcumin on focal cerebral ischemic rats by preventing blood–brain barrier damage. Eur J Pharmacol 561(1–3):54–62
Zhu D-Y, Li R, Liu G-Q, Hua W-Y (2000) Tumor necrosis factor alpha enhances the cytotoxicity induced by nitric oxide in cultured cerebral endothelial cells. Life Sci 66(14):1325–1335
Pan M-H, Lin-Shiau S-Y, Lin J-K (2000) Comparative studies on the suppression of nitric oxide synthase by curcumin and its hydrogenated metabolites through down-regulation of IκB kinase and NFκB activation in macrophages. Biochem Pharmacol 60(11):1665–1676
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Bavarsad, K., Barreto, G.E., Hadjzadeh, MAR. et al. Protective Effects of Curcumin Against Ischemia-Reperfusion Injury in the Nervous System. Mol Neurobiol 56, 1391–1404 (2019). https://doi.org/10.1007/s12035-018-1169-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-1169-7