Abstract
Purpose
The hypothalamic hormone oxytocin plays a major role in regulation of behavior and body composition. Quality of survival is frequently impaired in childhood craniopharyngioma patients due to sequelae such as behavioral deficits and severe obesity caused by tumor or treatment-related hypothalamic lesions.
Methods
In our pilot cross-sectional study, we analyzed emotion recognition abilities and oxytocin concentrations in saliva and urine before and after single nasal administration of 24 IU oxytocin in 10 craniopharyngioma patients. Four craniopharyngioma presented with grade I lesions (limited to anterior hypothalamic areas) and 6 craniopharyngioma with grade II lesions (involving mammillary bodies and posterior hypothalamic areas). Emotional tasks were assessed before and after administration of oxytocin using the Geneva multimodal emotion portrayals corpus and the Multidimensional Mood Questionnaire.
Results
All patients presented with detectable levels of oxytocin before administration. Nasal administration of oxytocin was well-tolerated and resulted in increased oxytocin concentrations in saliva and urine. After oxytocin administration, craniopharyngioma patients with postsurgical lesions limited to the anterior hypothalamus area showed improvements in emotional identifications compared to craniopharyngioma patients with lesions of anterior and posterior hypothalamic areas. Focusing on correct assignments to positive and negative emotion categories, craniopharyngioma patients improved assignment to negative emotions.
Conclusions
Oxytocin might have positive effects on emotion perception in craniopharyngioma patients with specific lesions of the anterior hypothalamic area. Further studies on larger cohorts are warranted.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oxytocin is a pituitary neuropeptide hormone synthesized by paraventricular and supraoptic hypothalamic nuclei. Through the neurohypophysis, oxytocin is secreted into the systemic circulation to act as a hormone, thereby influencing several body functions. Oxytocin plays a pivotal role in parturition and maternal behavior and has been demonstrated to be important in the formation of pair bonding between mother and infants as well as in mating pairs. Furthermore, oxytocin has been proven to play a key role in the regulation of body weight [1, 2] as well as several behaviors associated with neuropsychiatric disorders, including social interactions, social memory, response to social stimuli, decision-making in the context of social interactions, feeding behavior, and emotional reactivity [3]. An increasing body of evidence suggests that deregulations of the oxytocinergic system might be involved in the pathophysiology of certain neuropsychiatric disorders such as autism, eating disorders, schizophrenia, and anxiety disorders. The potential use of oxytocin in these mental health disorders is attracting growing interest since numerous beneficial properties are ascribed to this neuropeptide [4–10].
Childhood-onset craniopharyngiomas (CP) are rare embryonal malformations of the sellar region [11]. CPs show low-grade histological malignancy and frequently affect hypothalamic and pituitary regions. Hypothalamic involvement of CP is resulting in neuroendocrine deficits, neuropsychological disorders, pathological patterns of eating behavior, and obesity with major negative impact on prognosis and quality of life in surviving patients [12–16]. The most consistent findings in the neuropsychological domain are deficits in learning and episodic memory, largely sparing other memory components [17, 18], and social-emotional deficits such as emotional lability, rage attacks, and social withdrawal [19–21]. Social and emotional dysfunctions have only recently gained more attention and may indicate reduced integrity in fronto-limbic circuitries. In a first systematic review on neurobehavioral dysfunction in CP patients, Zada et al. [21] speculated that impaired social interaction may relate to oxytocin deficiency. In the healthy brain, there is a high density of oxytocin receptor binding sites in limbic areas and it is assumed that the effects of oxytocin on social-emotional processes are mediated by the limbic system [22]. In CP patients, an fMRI study using a face recognition memory task indicated alterations in the patients’ fronto-limbic areas. Compared to healthy controls, the patients’ amygdala revealed a higher reactivity for emotional relative to neutral faces and a differential recruitment of fronto-limbic brain areas during correct trials in the recognition phase was observed [23]. Deficits in emotional and social emotional domains have been linked in several neuropsychiatric disorders with oxytocin, and nasal delivery of oxytocin has in many cases shown clear improvements in tasks requiring these skills. A recent case study about a parent having observed neurobehavioral and pro-social improvement with oxytocin therapy following surgical resection of their child’s CP [24], is supporting earlier reports on oxytocin effects on social cognition and affiliative behavior [5–7].
In the present study, we evaluated oxytocin concentrations in saliva and urine after administration of a single dose of oxytocin in 10 CP patients. We hypothesized that oxytocin will influence emotion recognition, which is a significant component of social cognition. To assess emotion recognition abilities, we used an experimental task, probing the perception and identification of emotions in vocal expressions before and after oxytocin administration. Similar to facial expressions, which are much more frequently studied, the identification of the emotional significance of vocal expressions or autonomic responses to human affective sounds were also shown to be enhanced with oxytocin administration [25, 26].
Patients and methods
Patients
For this study, 466 patients with childhood-onset CP, recruited in the German Craniopharygioma Registry and evaluated in the multicenter trials HIT Endo, KRANIOPHARYNGEOM 2000 (Clinical Trial No.: NCT00258453) and KRANIOPHARYNGEOM 2007 (Clinical Trial No.: NCT01272622) were identified to fulfill the inclusion criteria for this trial. Patients were supposed to be at minimum age of 18 years at time of evaluation and suffering from proven hypothalamic lesions. Patients suffering from cardiac failures or arrhythmia were excluded from the trial to avoid potential cardiac side effects of oxytocin treatment. In addition, patients with severe visual limitation were excluded because of need of visual capacity in visual based neuropsychological tests. Ten patients finally agreed to participate. Participants were analyzed for actual weight and height at time of study. The degree of obesity was evaluated by calculating the BMI SDS according to the references of Rolland–Cachera et al. [27]. The histological diagnosis of adamantinomatous CP was confirmed by reference assessment in all cases. Hypothalamic involvement of CP was assessed by magnetic resonance imaging (MRI). Preoperative hypothalamic involvement was defined as involvement of hypothalamic structures either by tumor growth into the hypothalamus or displacement of hypothalamic structures by the tumor. Surgical hypothalamic lesions were assessed on postoperative MRI based on a previously published grading system [28, 29] by a neuroradiologist blinded for the clinical data. Actual medication was evaluated and because of potential cardiac side effects of oxytocin, each participant was checked for cardiac arrhythmia by electrocardiogram before entering the trial.
Procedure
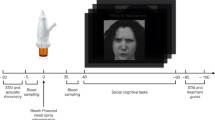
The trial started with the collection of a first urine and saliva sample. While chewing a white cylindrical swab for 15 min for saliva sampling, patients completed a mood questionnaire. Subsequently, patients performed in the experimental paradigm, which lasted for 20–30 min. Then, oxytocin was administrated intranasally. After an interval of 45 min, patients again were prompted to chew a cylindrical swab for 15 min for the second saliva sample and to complete the mood questionnaire again. Subsequently, patients performed in the second part of the experimental paradigm, which lasted again for 20–30 min. Finally, the second urine sample was collected about 90 min after oxytocin administration.
Oxytocin analysis in saliva and urine
To measure oxytocin saliva concentrations, saliva was collected before and 45 min after oxytocin administration using a standardized method for saliva sampling. A white cylindrical swab was chewed gently for 15 min and then returned with the absorbed saliva. All salivettes were placed immediately and kept on ice until centrifugation. After centrifugation, saliva samples were stored frozen until analysis. For urine measurement of oxytocin, urine samples were collected before and 90 min after nasal oxytocin administration and stored frozen until analysis.
Oxytocin concentrations in saliva and urine were quantified by radioimmunoassay (RIA) (RIAgnosis, Sinzing, Germany). In brief, for each sample 300 µl of saliva was evaporated (SpeedVac, Thermoscientific Inc, Waltham, MA, USA), and 50 µl of assay buffer was added followed by 50 µl antibody (raised in rabbits against oxytocin). After a 60-min preincubation interval, 10 µl 125I-labeled tracer (PerkinElmer, Waltham, MA, USA) was added and samples were allowed to incubate for 3 days at 4 °C. Unbound radioactivity was precipitated by activated charcoal (Sigma-Aldrich, St Louis, MO, USA). Under these conditions, an average of 50% of total counts are bound with <5% non-specific binding. The detection limit is in the 0.5 pg/sample range, depending on the age of the tracer, with typical displacements of 20–25% at 2 pg, 60–70% at 8 pg, and 90% at 32 pg of standard neuropeptide. The intra-assay and inter-assay variabilities were <10%. Serial dilutions of saliva samples containing high levels of endogenous oxytocin run strictly parallel to the standard curve indicating immune-identity [30, 31].
Administration of Oxytocin
Each patient received a single intranasal administration of 24 UI oxytocin (Syntocinon® Spray, Novartis, Basel, Switzerland) divided into three puffs per nostril.
Experimental paradigm and questionnaire
Perception and identification of emotional expressions in voices was tested with verbal stimuli by the Geneva multimodal emotion portrayals (GEMEP) corpus [32]. We used an auditory emotion identification task rather than a visual task to exclude that visual deficits, often present in CP patients confound our results. The subset selected comprised 10 core emotional expressions (joy, pleasure, amusement, relief, hot anger (rage), cold anger (irritation), panic fear, despair, anxiety, sadness). Expressions of ‘pride’ and ‘interest’ were excluded due to the difficulty to recognize them in the auditory modality. All emotional expressions were embedded in two pseudo sentences, which sound similar to a real but unknown language. The sentences consisting of meaningless words were spoken by 10 professional theater actors. The experiment was run on 15.4-inch laptops (resolution 1440 × 990) and the paradigm was programed using Cogent 2000 (www.vislab.ucl.ac.uk/Cogent). Each trial started with the presentation of a simplified version of the Geneva emotion wheel, which was adapted for the subset of stimuli chosen for our experiment (Supplemental Fig. 1). During the presentation of the emotion wheel, sentences were presented via headphones and participants were instructed to assign by a mouse-click the emotional expression perceived to the corresponding expression depicted on the emotion wheel. Participants had no time pressure and could replay the sentences as often as needed. A total of 100 trials were presented during the experiment, 10 trials for each of the emotions used. The whole experiment lasted for 20–30 min, depending on the individual speed of operation. For descriptive and inferential statistics, we assessed (i) percent correct responses to single emotions and (ii) percent responses assigned to one of the emotions of corresponding emotion category. For the latter analysis, we used the emotion categories suggested by Banziger et al. [20].
Multidimensional mood questionnaire (MDMQ; Mehrdimensionaler Befindlichkeitsfragebogen [33]); The MDMQ is an assessment instrument that measures the current mental state with three bipolar subscales (good/bad mood, alertness/fatigue, calmness/restlessness) with a total of 24 items. Each subscale comprises eight adjectives, of which four belong to the negative (e.g., “bad,” “uncomfortable”) and four to the positive (e.g., “well,” “satisfied”) pole. These items are rated on a five-point likert scale ranging from one (“not at all”) to five (“very”). The MDMQ can be used to evaluate changes in mental states associated with therapies and interventions. The completion of the questionnaire requires approximately 8 min and the possible scores of each of the subscores range from 8 (bad mental state) to 40 (good mental condition). The questionnaire was used to assess possible influences oxytocin delivery may have on mood, wakefulness, and arousal.
Functional capacity assessment
The German daily life ability scale Fertigkeitenskala Münster-Heidelberg (FMH) was used for self-assessment of functional capacity [34]. The FMH measures the capability for routine actions. It was normalized with 971 persons (45.5% female), ages between 0 and 102 years, resulting in age-dependent percentiles. The average time for answering the FMH questionnaire was 4.5 min in first-time users.
Statistical analyses
Data were analyzed using the statistical package SPSS, version 24 (SPSS, INC., Chicago, IL). The Mann–Whitney U-test was used for comparison of two independent groups for a continuous variable. The chi-square test was used for comparison of different groups for categorical variables. Correlation between two variables was analyzed using the Spearman correlation coefficient. Due to small sample size, the interpretation of statistical findings is limited.
Results
The group of CP patients with hypothalamic lesions who received a single nasal administration of oxytocin comprised 5 men and 5 women diagnosed with CP at an age between 7.4 and 19.6 yr. Median age at study was 27 yr, ranging from 20.4 to 41.8 yr. The characteristics of this trial cohort in terms of BMI and functional capacity were comparable with the total cohort of 250 CP patients with hypothalamic lesions recruited in the German Craniopharyngioma Registry (Table 1). Postsurgical hypothalamic damage was determined by neuroradiological analysis to be grade I (anterior hypothalamic lesion) in 4 cases and to be grade II (anterior and posterior hypothalamic lesion) in 6 cases. Time since diagnosis ranges from 10.2 to 31.9 yr in patients with grade I lesions and from 4.1 to 25.6 yr in patients with grade II lesions (Table 2) with no difference in terms of follow-up interval between grade I and II patients. All patients presented with detectable concentrations of oxytocin in saliva and urine at baseline before administration of oxytocin (median baseline oxytocin concentration in saliva: 0.32 pg/ml, range: 0.25–3.60 pg/ml; median baseline oxytocin concentration in urine: 0.90 pg/ml, range: 0.42–1.59 pg/ml). The measurement of oxytocin saliva concentration before and 45 min after application of oxytocin as well as the measurement of oxytocin in urine before and 90 min after administration showed, that oxytocin was absorbed efficiently by nasal epithelium. In one case (patient no. 3), the oxytocin concentration in saliva only increased from 0.30 to 5.2 pg/ml, which might be explained by ineffective spraying or reduced resorption due to nasal obstruction. By detection of increased oxytocin urine concentrations after nasal administration it was proven that the hormone was indeed systemically absorbed and not only detectable in saliva due to high concentrations in the nasopharynx after nasal administration (Table 3).
Results from the experimental task on emotion identification showed slight improvements for four patients after the application of oxytocin. In these patients, we observed an increased percentage of correct assignments of emotional vocal expressions to emotion categories. All these patients presented with a postsurgical lesion of the anterior hypothalamus (grade I). Task performance in the six remaining patients with both, anterior and posterior lesions remained stable or slightly worsened (Fig. 1a). An additional analysis, separately focusing on correct assignments to positive and negative emotion categories revealed that improvements in performance in three of the patients with anterior hypothalamic lesions (patient no. 1, 2, and 3) were largely due to an improved assignment of negative emotions to the respective emotion category (Fig. 1c). In addition, two of the three patients (no. 1 and 2) showing improvements in this condition had the lowest baseline performance of the whole group. Similar results for all these analyses were obtained for correct assignments to single emotions. Here, three of the participants who showed improved performance after oxytocin administration were those with the lowest baseline performance (Fig. 2c; patients no. 1 and 2 with anterior hypothalamic lesions and no. 8 with anterior and posterior hypothalamic lesion). Possible effects of body weight on changes in task performance from pre-oxytocin to post-oxytocin administration were assessed using scatter plots (Fig. 3).
Percent of responses correctly assigned to one of the emotions of the corresponding emotion category. a. All emotion categories, b. positive emotion categories, and c. negative emotion categories. Solid lines depict patients with postsurgical lesions classified as grade I (anterior hypothalamic lesions), dashed lines depict patients with postsurgical lesions classified as grade II (anterior and posterior hypothalamic lesions) according to the grading system published by Müller et al. [28, 29]. Numbering of patients with grade I lesions is shown on the right side of the figures
Percent of responses correctly assigned to single emotions. a. All emotions, b. positive emotions, and c. negative emotions. Solid lines depict patients with postsurgical lesions classified as grade I (anterior hypothalamic lesions), dashed lines depict patients with postsurgical lesions classified as grade II (anterior and posterior hypothalamic lesions) according to the grading system published by Müller et al. [28, 29]. Numbering of patients with grade I involvement is shown to the right of the figures
The evaluation of oxytocin effects on the mental state of patients’ with the Multidimensional Mood State Questionnaire (MDBF) revealed stable or improved mood after oxytocin administration for most of the participants (Fig. 4). Only few patients reported decreased mood (patient no. 3), increased tiredness (patient no. 3, 8), or increased restlessness (patient no. 4). There were no positive associations between changes in mood and changes in task performance. Changes in oxytocin urine and serum concentrations did not significantly correlate with changes in neuropsychological findings (GEMEP, MDMQ) before and after oxytocin administration. Patients with grade I hypothalamic lesions presented with a trend towards lower oxytocin urine concentrations (p = 0.06) at baseline before oxytocin administration when compared with patients with grade II hypothalamic lesion. The correlations between baseline oxytocin urine concentration and oxytocin urine concentration after administration did not reach statistical significance (P = 0.06). There was no correlation between oxytocin concentrations in saliva and urine (p = 0.09).
Results for the three bipolar subscales of the MDMQ (a. good/bad mood, b. attentiveness/tiredness, c. calm/restlessness). Subscale scores are ranging from a minimum of 8 (bad mental state) to a maximum of 40 (good mental condition). Solid lines depict patients with postsurgical lesions classified as grade I (anterior hypothalamic lesion), dashed lines depict patients with postsurgical lesions classified as grade II (anterior and posterior hypothalamic lesions) according to the grading system published by Müller et al. [28, 29] Numbering of patients with grade I lesions is shown on the right side of the figures
Discussion
Oxytocin seems to be implicated in several and complex social behaviors in a range of mammals [35, 36]. One of the most studied aspects is the regulation of maternal behavior [36]. In particular, oxytocin promotes maternal care in lactating rats and plays a key role in bond formation between mother and offspring [5].
Oxytocin is also involved in the mechanisms regulating the development of adult-adult pair in animal studies [37]. The identification of conspecifics is a crucial requirement for the formation of pair bonds [38]; oxytocin takes part in the processes that regulate social memory, in terms of social learning and social recognition [39–41] and the pretreatment with an oxytocin-receptor antagonist prevents this ability in animal studies [39, 40, 42, 43]. The effects of oxytocin on social behavior are complex and may be dependent on the context in which they occur. In fact, oxytocin seems to promote sociality when social cues in the environment are interpreted as “safe” and oxytocin may induce defensive behavior when the social cues are interpreted as “unsafe” [4, 44].
It is well known that “mind reading” is an essential basis of human social interaction and the role that oxytocin plays in the formation of social bonds is also related to its role of promoting the understanding of the mental state of individuals from the interpretation of their facial cues [45].
Prader–Willi syndrome (PWS) is known for hyperphagia with impaired satiety and a specific behavioral phenotype with stubbornness, temper tantrums, manipulative, and controlling behavior and obsessive-compulsive features. PWS is associated with hypothalamic and oxytocinergic dysfunction. In humans without PWS, intranasal oxytocin administration had positive effects on social and eating behavior, and weight balance [46]. A randomized double-blind placebo-controlled study in 25 PWS patients suggested that intranasal oxytocin administration (dose range 24–48 IU/day for 4 weeks) has beneficial effects on social behavior and food-related behavior in PWS patients younger than 11 years of age, but not in those older than 11 years [47].
On the other hand, Einfeld et al. [48] analyzed 30 PWS patients aged 12–30 years in an 18-week randomized double-blind placebo-controlled crossover trial. The only difference found between the baseline oxytocin and placebo measures was an increase in temper outbursts with higher oxytocin doses. The authors speculated that the lack of oxytocin effects might reflect the importance of endogenous release of oxytocin in response to exogenous oxytocin. Johnson et al. [49] examined overnight fasting plasma oxytocin levels in 23 PWS children having genetic confirmation and 18 age-matched healthy unrelated siblings without PWS and a similar gender ratio. Oxytocin plasma levels were significantly elevated in children with PWS compared with unrelated and unaffected siblings without the diagnosis of PWS and the diagnosis of PWS predicted oxytocin level in controlled regression analysis. The authors speculated that the symptoms of hyperphagia, anxiety and repetitive behaviors classically seen in PWS might be related to the disruption of oxytocin responsivity or feedback in the hypothalamic paraventricular nucleus possibly influencing vasopressin signaling.
It might have been suspected that oxytocin synthesis and release are decreased in CP patients since oxytocin synthesis takes place in the hypothalamus and is released mainly via the pituitary gland. However, Daubenbuchel et al. [50] recently published data on oxytocin saliva concentrations in CP patients, suggesting that this is not a general finding in CP patients with hypothalamic lesions. In that pilot cross-sectional study, a small group of CP patients were analyzed for oxytocin concentrations in saliva in comparison to normal controls. The main findings were, that CP patients are still able to produce and secrete oxytocin, even when pituitary and hypothalamic structures were damaged. However, CP patients with grade I hypothalamic lesions presented with lower oxytocin concentrations before breakfast when compared with CP patients with grade II hypothalamic involvement or normal controls. In addition, changes in oxytocin concentrations before and after breakfast correlated with BMI in CP patients demonstrating that patients with hypothalamic obesity showed less variation in oxytocin secretion due to nutrition. Therefore, the authors concluded that substitution of oxytocin might be a therapeutic tool in CP patients with hypothalamic obesity due to specific lesions of anterior hypothalamic areas [50]. This therapeutic potential is further reinforced by a recent case report on a parent having observed neurobehavioral and pro-social improvement with oxytocin therapy following surgical resection of their child’s CP [24], supporting earlier reports on beneficial oxytocin effects on social cognition and affiliative behavior [5–7].
The current pilot study is the first to evaluate oxytocin concentrations in two compartments (saliva and urine) and neuropsychological effects before and after a single dose of intranasal oxytocin in a small representative cohort of patients with childhood-onset CP and postsurgical hypothalamic lesions of different degree. Supporting a previous report [50], it was shown that all patients presented with detectable levels of oxytocin before administration of oxytocin.
Based on findings of deficits in the social-emotional domain in CP patients [21] and on many studies showing enhancement of emotion identification after intranasal application of oxytocin [51], we used an emotion identification task. Our results provide evidence for improved emotion identification after oxytocin administration in some patients. Perceiving and identifying emotions in facial expressions or by vocal prosody is an important dimension of social cognition and performance improvements after intranasal oxytocin administration has been shown in many studies [51]. In case of emotion identification across all emotion categories, improvements in our study were exclusively observed in patients with grade I hypothalamic lesion, i.e. anterior hypothalamic lesions that did not involve the mammillary bodies. The overall improvement of emotion identification was driven by enhanced performance with respect to identification of negative emotions. CP patients with grade II hypothalamic lesions, i.e. hypothalamic lesions involving anterior and/or posterior hypothalamus, did not present with such an improvement after oxytocin application. In addition, CP patients with grade I hypothalamic lesions show already at baseline slightly lower performance in identification of negative emotional expressions than those with grade II hypothalamic lesions. Note however that the sample size is rather small, so these results can only be regarded as preliminary observations.. Noteworthy, performance improvements were not due to improvements in mental state as there were no positive associations between changes in mood and changes in task performance. This is consistent with previous literature, showing that oxytocin administration has no noticable effects on mood state [52].
In our previous study, we speculated already that in some patients, oxytocin production and release is diminished after hypothalamic damage due to surgical treatment. Based on our current findings, we speculate that in case of anterior hypothalamic lesion—not involving mammillary bodies and the hypothalamic areas beyond mammillary bodies—an external administration of oxytocin might have beneficial neuropsychological effects.
However, results on improvements in task performance might be confounded by the observation that CP patients with grade I hypothalamic lesions presented with lower body weight at the time of study compared to those with a grade II hypothalamic lesions. The negative association between body weight and changes in task performance might indicate that the dose of 24 UI oxytocin—which is most frequently reported dose in the literature—may be inappropriate for many patients with hypothalamic involvement of their CP. These patients frequently suffer from hypothalamic obesity, which is even more prominent with grade II involvement [28, 29]. Dose-response curves for oxytocin administration are merely researched in humans. In experiments with rats, intracerebroventricularly injected oxytocin revealed improvements in social behavior up to a certain dose per kg body weight, but not beyond [39]. A similar facilitation of social recognition was reported in another study with rats, showing U-shaped dose response curve with low doses per kg facilitating and high doses per kg attenuating social recognition [53]. Noteworthy, dose-response relationships may also explain the week intranasal oxytocin effects in studies on PWS, which did not account for body weight but used to administer standard doses [46]. A randomized, double-blind, placebo-controlled study in 25 PWS patients suggested that intranasal oxytocin administration (dose range 24–48 IU/day for 4 weeks) has beneficial effects on social behavior and food-related behavior in children with PWS younger than 11 years of age, but not in those older than 11 years of age [47]. The dose of oxytocin in this study was calculated based on the body surface of the patients.
Another explanation for the lack of beneficial effect in patients with grade II hypothalamic lesions might be a dysfunction of important regulatory hypothalamic regions in oxytocin recruits. These regions are more likely preserved in patients with grade I hypothalamic lesions due to the growth pattern of the tumor which typically takes place from an anterior inferior region of the hypothalamus (tuberal region) to an upwards posterior direction [54]. Thus, in presence of a smaller tumor size or certain directions of growth, the paraventricular and supraoptic nuclei may be spared, resulting in preserved oxytocin synthesis in this group. To elucidate this, further research on the compartmentalization of the hypothalamus is needed.
A third explanation for beneficial effects of intranasal oxytocin administration in patients with grade 1 hypothalamic lesions is related to the lower baseline functional capability observed in this group. An influential theoretical model of intranasal oxytocin effects on social cognition postulates that the hormone’s effects on social cognition are dependent on baseline social cognition skills, with performance improvements to be expected with a low baseline performance [55].
Limitations of the study include the low patient number. Studies on larger cohorts should provide statistical evidence whether changes in oxytocin concentrations after administration were accompanied by significant changes in neuropsychological findings and whether these changes showed specific patterns in relation to different grades of hypothalamic damage. Besides statistical limitations, the reliability of oxytocin measurement is still under debate and issues have been raised regarding the importance of preanalytical procedures. Because of this debate, we did not use the ELISA method but chose RIA measurements. For this method, a higher specificity for active oxytocin metabolites is supposed, compared to ELISA methods [56, 57]. In addition, the missing correlation between saliva and urine concentrations of oxytocin might indicate that individual variations in dynamics of resorption, metabolism and excretion have impact on the response to exogenous oxytocin. Furthermore, a therapeutic trial with a regular medication over a specific period would be more meaningful compared to a single administration. This will be part of a planned future multicenter trial in the context of the German craniopharyngioma registry.
References
J.E. Blevins, J.M. Ho, Role of oxytocin signaling in the regulation of body weight. Rev. Endocr. Metab. Disord. 14(4), 311–329 (2013). doi:10.1007/s11154-013-9260-x
J.M. Ho, J.E. Blevins, Coming full circle: contributions of central and peripheral oxytocin actions to energy balance. Endocrinology 154(2), 589–596 (2013). doi:10.1210/en.2012-1751
I.D. Neumann, R. Landgraf, Balance of brain oxytocin and vasopressin: implications for anxiety, depression, and social behaviors. Trends. Neurosci. 35(11), 649–659 (2012). doi:10.1016/j.tins.2012.08.004
M. Olff, J.L. Frijling, L.D. Kubzansky, B. Bradley, M.A. Ellenbogen, C. Cardoso, J.A. Bartz, J.R. Yee, M. van Zuiden, The role of oxytocin in social bonding, stress regulation and mental health: an update on the moderating effects of context and interindividual differences. Psychoneuroendocrinology. 38(9), 1883–1894 (2013). doi:10.1016/j.psyneuen.2013.06.019
H.E. Ross, L.J. Young, Oxytocin and the neural mechanisms regulating social cognition and affiliative behavior. Front. Neuroendocrinol. 30(4), 534–547 (2009). doi:10.1016/j.yfrne.2009.05.004
T.R. Insel, The challenge of translation in social neuroscience: a review of oxytocin, vasopressin, and affiliative behavior. Neuron 65(6), 768–779 (2010). doi:10.1016/j.neuron.2010.03.005
P.S. Churchland, P. Winkielman, Modulating social behavior with oxytocin: how does it work? What does it mean? Horm. Behav. 61(3), 392–399 (2012). doi:10.1016/j.yhbeh.2011.12.003
A. Romano, B. Tempesta, M.V. Micioni Di Bonaventura, S. Gaetani, From autism to eating disorders and more: the role of oxytocin in neuropsychiatric disorders. Front. Neurosci. 9, 497 (2015). doi:10.3389/fnins.2015.00497
E.A. Lawson, D.A. Marengi, R.L. DeSanti, T.M. Holmes, D.A. Schoenfeld, C.J. Tolley, Oxytocin reduces caloric intake in men. Obesity. (Silver. Spring). 23(5), 950–956 (2015). doi:10.1002/oby.21069
D. Cai, S. Purkayastha, A new horizon: oxytocin as a novel therapeutic option for obesity and diabetes. Drug Discov. Today Dis. Mech. 10(1-2), e63–e68 (2013). doi:10.1016/j.ddmec.2013.05.006
H.L. Muller, Craniopharyngioma. Endocr. Rev. 35(3), 513–543 (2014). doi:10.1210/er.2013-1115
A.S. Sterkenburg, A. Hoffmann, U. Gebhardt, M. Warmuth-Metz, A.M. Daubenbuchel, H.L. Muller, Survival, hypothalamic obesity, and neuropsychological/psychosocial status after childhood-onset craniopharyngioma: newly reported long-term outcomes. Neuro. Oncol. 17(7), 1029–1038 (2015). doi:10.1093/neuonc/nov044
O.M. Dekkers, N.R. Biermasz, J.W. Smit, L.E. Groot, F. Roelfsema, J.A. Romijn, A.M. Pereira, Quality of life in treated adult craniopharyngioma patients. Eur. J. Endocrinol. 154(3), 483–489 (2006). doi:10.1530/eje.1.02114
P. Mortini, M. Losa, G. Pozzobon, R. Barzaghi, M. Riva, S. Acerno, D. Angius, G. Weber, G. Chiumello, M. Giovanelli, Neurosurgical treatment of craniopharyngioma in adults and children: early and long-term results in a large case series. J. Neurosurg. 114(5), 1350–1359 (2011). doi:10.3171/2010.11.JNS10670
H.L. Muller, Consequences of craniopharyngioma surgery in children. J. Clin. Endocrinol. Metab. 96(7), 1981–1991 (2011). doi:10.1210/jc.2011-0174
H.L. Muller, A. Emser, A. Faldum, G. Bruhnken, N. Etavard-Gorris, U. Gebhardt, R. Oeverink, R. Kolb, N. Sorensen, Longitudinal study on growth and body mass index before and after diagnosis of childhood craniopharyngioma. J. Clin. Endocrinol Metab. 89(7), 3298–3305 (2004). doi:10.1210/jc.2003-031751
S.D. Vann, J.P. Aggleton, The mammillary bodies: two memory systems in one? Nat. Rev. Neurosci. 5(1), 35–44 (2004). doi:10.1038/nrn1299
J. Ozyurt, H.L. Muller, C.M. Thiel, A systematic review of cognitive performance in patients with childhood craniopharyngioma. J. Neurooncol. 125(1), 9–21 (2015). doi:10.1007/s11060-015-1885-z
H.L. Muller, Childhood craniopharyngioma. Recent advances in diagnosis, treatment and follow-up. Horm. Res. 69(4), 193–202 (2008). doi:10.1159/000113019
A. Pierre-Kahn, C. Recassens, G. Pinto, C. Thalassinos, S. Chokron, J.C. Soubervielle, R. Brauner, M. Zerah, C. Sainte Rose, Social and psycho-intellectual outcome following radical removal of craniopharyngiomas in childhood. A prospective series. Child. Nerv. Syst. 21(8-9), 817–824 (2005). doi:10.1007/s00381-005-1205-6
G. Zada, N. Kintz, M. Pulido, L. Amezcua, Prevalence of neurobehavioral, social, and emotional dysfunction in patients treated for childhood craniopharyngioma: a systematic literature review. PLoS ONE 8(11), e76562 (2013). doi:10.1371/journal.pone.0076562
A. Meyer-Lindenberg, G. Domes, P. Kirsch, M. Heinrichs, Oxytocin and vasopressin in the human brain: social neuropeptides for translational medicine. Nat. Rev. Neurosci. 12(9), 524–538 (2011). doi:10.1038/nrn3044
J. Ozyurt, A. Lorenzen, U. Gebhardt, M. Warmuth-Metz, H.L. Muller, C.M. Thiel, Remote effects of hypothalamic lesions in the prefrontal cortex of craniopharygioma patients. Neurobiol. Learn. Mem. 111, 71–80 (2014). doi:10.1016/j.nlm.2014.03.007
N. Cook, J. Miller, J. Hart, Parent observed neuro-behavioral and pro-social improvements with oxytocin following surgical resection of craniopharyngioma. J. Pediatr. Endocrinol. Metab. (2016). doi:10.1515/jpem-2015-0445
E. Hollander, J. Bartz, W. Chaplin, A. Phillips, J. Sumner, L. Soorya, E. Anagnostou, S. Wasserman, Oxytocin increases retention of social cognition in autism. Biol. Psychiatry 61(4), 498–503 (2007). doi:10.1016/j.biopsych.2006.05.030
I.F. Lin, M. Kashino, H. Ohta, T. Yamada, M. Tani, H. Watanabe, C. Kanai, T. Ohno, Y. Takayama, A. Iwanami, N. Kato, The effect of intranasal oxytocin versus placebo treatment on the autonomic responses to human sounds in autism: a single-blind, randomized, placebo-controlled, crossover design study. Mol. Autism. 5(1), 20 (2014). doi:10.1186/2040-2392-5-20
M.F. Rolland-Cachera, T.J. Cole, M. Sempe, J. Tichet, C. Rossignol, A. Charraud, Body Mass Index variations: centiles from birth to 87 years. Eur. J. Clin. Nutr. 45(1), 13–21 (1991)
H.L. Muller, U. Gebhardt, C. Teske, A. Faldum, I. Zwiener, M. Warmuth-Metz, T. Pietsch, F. Pohl, N. Sorensen, G. Calaminus, Post-operative hypothalamic lesions and obesity in childhood craniopharyngioma: results of the multinational prospective trial KRANIOPHARYNGEOM 2000 after 3-year follow-up. Eur. J. Endocrinol. 165(1), 17–24 (2011). doi:10.1530/EJE-11-0158
H.L. Muller, U. Gebhardt, A. Faldum, M. Warmuth-Metz, T. Pietsch, F. Pohl, G. Calaminus, N. Sorensen, Xanthogranuloma, Rathke’s cyst, and childhood craniopharyngioma: results of prospective multinational studies of children and adolescents with rare sellar malformations. J. Clin. Endocrinol. Metab. 97(11), 3935–3943 (2012). doi:10.1210/jc.2012-2069
R. Landgraf, Plasma oxytocin concentrations in man after different routes of administration of synthetic oxytocin. Exp. Clin. Endocrinol. 85(2), 245–248 (1985). doi:10.1055/s-0029-1210444
I. Neumann, M. Ludwig, M. Engelmann, Q.J. Pittman, R. Landgraf, Simultaneous microdialysis in blood and brain: oxytocin and vasopressin release in response to central and peripheral osmotic stimulation and suckling in the rat. Neuroendocrinology 58(6), 637–645 (1993)
T. Banziger, M. Mortillaro, K.R. Scherer, Introducing the Geneva Multimodal expression corpus for experimental research on emotion perception. Emotion 12(5), 1161–1179 (2012). doi:10.1037/a0025827
R. Steyer, O. Schwenkmezger, P. Notz, M. Eid. Der Mehrdimensionale Befindlicheitsfragebogen (MDBF). Hogrefe, Göttingen, (1997)
J.E. Wolff, E. Daumling, A. Dirksen, A. Dabrock, M. Hartmann, H. Jurgens, Munster Heidelberg Abilities Scale--a measuring instrument for global comparison of illness sequelae. Klin. Padiatr. 208(5), 294–298 (1996). doi:10.1055/s-2008-1046486
C.S. Carter, Oxytocin and sexual behavior. Neurosci. Biobehav. Rev. 16(2), 131–144 (1992)
O.J. Bosch, I.D. Neumann, Both oxytocin and vasopressin are mediators of maternal care and aggression in rodents: from central release to sites of action. Horm. Behav. 61(3), 293–303 (2012). doi:10.1016/j.yhbeh.2011.11.002
J.R. Williams, T.R. Insel, C.R. Harbaugh, C.S. Carter, Oxytocin administered centrally facilitates formation of a partner preference in female prairie voles (Microtus ochrogaster). J. Neuroendocrinol. 6(3), 247–250 (1994)
T.R. Insel, R.D. Fernald, How the brain processes social information: searching for the social brain. Ann. Rev. Neurosci. 27, 697–722 (2004). doi:10.1146/annurev.neuro.27.070203.144148
A. Benelli, A. Bertolini, R. Poggioli, B. Menozzi, R. Basaglia, R. Arletti, Polymodal dose-response curve for oxytocin in the social recognition test. Neuropeptides 28(4), 251–255 (1995)
M. Engelmann, K. Ebner, C.T. Wotjak, R. Landgraf, Endogenous oxytocin is involved in short-term olfactory memory in female rats. Behav. Brain Res. 90(1), 89–94 (1998)
K. Lancaster, C.S. Carter, H. Pournajafi-Nazarloo, T. Karaoli, T.S. Lillard, A. Jack, J.M. Davis, J.P. Morris, J.J. Connelly, Plasma oxytocin explains individual differences in neural substrates of social perception. Front. Hum. Neurosci. 9, 132 (2015). doi:10.3389/fnhum.2015.00132
M. Lukas, I. Toth, A.H. Veenema, I.D. Neumann, Oxytocin mediates rodent social memory within the lateral septum and the medial amygdala depending on the relevance of the social stimulus: male juvenile versus female adult conspecifics. Psychoneuroendocrinology 38(6), 916–926 (2013). doi:10.1016/j.psyneuen.2012.09.018
J.E. Ferguson 2nd, B.H. Head, F.H. Frank, M.L. Frank, J.S. Singer, T. Stefos, G. Mari, Misoprostol versus low-dose oxytocin for cervical ripening: a prospective, randomized, double-masked trial. Am. J. Obstet. Gynecol. 187(2), 273–279 (2002). discussion 279-280
J.A. Bartz, J. Zaki, N. Bolger, K.N. Ochsner, Social effects of oxytocin in humans: context and person matter. Trends Cogn. Sci. 15(7), 301–309 (2011). doi:10.1016/j.tics.2011.05.002
G. Domes, M. Heinrichs, A. Michel, C. Berger, S.C. Herpertz, Oxytocin improves “mind-reading” in humans. Biol. Psychiatry 61(6), 731–733 (2007). doi:10.1016/j.biopsych.2006.07.015
M. Tauber, C. Mantoulan, P. Copet, J. Jauregui, G. Demeer, G. Diene, B. Roge, V. Laurier, V. Ehlinger, C. Arnaud, C. Molinas, D. Thuilleaux, Oxytocin may be useful to increase trust in others and decrease disruptive behaviours in patients with Prader-Willi syndrome: a randomised placebo-controlled trial in 24 patients. Orphanet. J. Rare. Dis. 6, 47 (2011). doi:10.1186/1750-1172-6-47
R.J. Kuppens, S.H. Donze, A.C. Hokken-Koelega, Promising effects of oxytocin on social and food-related behavior in young children with Prader-Willi Syndrome: a randomized, double-blind, controlled crossover trial. Clin. Endocrinol. (2016). doi:10.1111/cen.13169
S.L. Einfeld, E. Smith, I.S. McGregor, K. Steinbeck, J. Taffe, L.J. Rice, S.K. Horstead, N. Rogers, M.A. Hodge, A.J. Guastella, A double-blind randomized controlled trial of oxytocin nasal spray in Prader Willi syndrome. Am. J. Med. Genet. A 164A(9), 2232–2239 (2014). doi:10.1002/ajmg.a.36653
L. Johnson, A.M. Manzardo, J.L. Miller, D.J. Driscoll, M.G. Butler, Elevated plasma oxytocin levels in children with Prader-Willi syndrome compared with healthy unrelated siblings. Am. J. Med. Genet. A 170(3), 594–601 (2016). doi:10.1002/ajmg.a.37488
A.M. Daubenbuchel, A. Hoffmann, M. Eveslage, J. Ozyurt, K. Lohle, J. Reichel, C.M. Thiel, H. Martens, V. Geenen, H.L. Muller, Oxytocin in survivors of childhood-onset craniopharyngioma. Endocrine 54(2), 524–531 (2016). doi:10.1007/s12020-016-1084-5
M. Mercedes Perez-Rodriguez, K. Mahon, M. Russo, A.K. Ungar, K.E. Burdick, Oxytocin and social cognition in affective and psychotic disorders. Eur. Neuropsychopharmacol. 25(2), 265–282 (2015). doi:10.1016/j.euroneuro.2014.07.012
P. Kirsch, C. Esslinger, Q. Chen, D. Mier, S. Lis, S. Siddhanti, H. Gruppe, V.S. Mattay, B. Gallhofer, A. Meyer-Lindenberg, Oxytocin modulates neural circuitry for social cognition and fear in humans. J. Neurosci. 25(49), 11489–11493 (2005). doi:10.1523/JNEUROSCI.3984-05.2005
P. Popik, J. Vetulani, J.M. van Ree, Low doses of oxytocin facilitate social recognition in rats. Psychopharmacology (Berl). 106(1), 71–74 (1992)
H.G. Bauer, Endocrine and other clinical manifestations of hypothalamic disease; a survey of 60 cases, with autopsies. J. Clin. Endocrinol. Metab. 14(1), 13–31 (1954). doi:10.1210/jcem-14-1-13
M. Fischer-Shofty, S.G. Shamay-Tsoory, Y. Levkovitz, Characterization of the effects of oxytocin on fear recognition in patients with schizophrenia and in healthy controls. Front. Neurosci. 7, 127 (2013). doi:10.3389/fnins.2013.00127
M.E. McCullough, P.S. Churchland, A.J. Mendez, Problems with measuring peripheral oxytocin: can the data on oxytocin and human behavior be trusted? Neurosci. Biobehav. Rev. 37(8), 1485–1492 (2013). doi:10.1016/j.neubiorev.2013.04.018
G. Lippi, G.C. Guidi, C. Mattiuzzi, M. Plebani, Preanalytical variability: the dark side of the moon in laboratory testing. Clin. Chem. Lab. Med. 44(4), 358–365 (2006). doi:10.1515/CCLM.2006.073
Acknowledgements
This study was funded by a grant (Forschungspool) of the European Medical School, Oldenburg, Germany, and a grant (DKS2014.13) of the German Childhood Cancer Foundation, Bonn, Germany. H. Müller is supported by the German Childhood Cancer Foundation, Bonn, Germany.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interest.
Ethical Approval
All procedures performed in our study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by the local standing committee on ethical practice as an individual medical treatment in ten cases and written patient consent was obtained in all cases.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Hoffmann, A., Özyurt, J., Lohle, K. et al. First experiences with neuropsychological effects of oxytocin administration in childhood-onset craniopharyngioma. Endocrine 56, 175–185 (2017). https://doi.org/10.1007/s12020-017-1257-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-017-1257-x