Abstract
This study aimed to investigate whether Cr(VI) can induce ferroptosis in chicken hepatocytes and determine the role of PERK-mediated endoplasmic reticulum stress (ERS). First, a model of Cr(VI) poisoning was established by exposing chicken hepatocytes to Cr(VI). The levels of ferroptosis-related proteins, meanwhile, GSH, SOD, MDA, and lipid ROS, were measured. Furthermore, the expression of GRP78 and PERK proteins was examined. Changes in ERS and ferroptosis were evaluated by silencing the PERK gene. Results showed that Cr(VI) led to the accumulation of lipid ROS, decreased expression of GPX4 and HSP27, increased expression of COX2, and induced ferroptosis in chicken hepatocytes. Exposure to Cr(VI) increased the protein expression of GRP78 and PERK, and silencing of PERK worsened Cr(VI)-induced ferroptosis. In conclusion, Cr(VI) can induce ferroptosis in chicken hepatocytes, and PERK plays an important role as a negative regulator.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
With the ongoing promotion of urban industrialization, chromium (Cr) is increasingly used in processes such as textiles and electroplating, leading to increased Cr pollution [1]. Despite continuous efforts to study bioremediation methods, incidents of Cr contamination and poisoning remain unresolved [2, 3]. In contrast to the organic Cr that is essential for organisms, Cr(VI) is an environmental pollutant that can accumulate in water and soil and continuously enrich through the biological chain. It not only seriously damages the ecological environment but also causes unavoidable harm to organisms [4,5,6,7].
The mechanism by which Cr(VI) exerts toxic effects after entering cells can be broadly classified as follows: Cr(VI) is reduced by antioxidants, especially GSH, to produce large amounts of free radicals. These free radicals induce oxidative stress, leading to damage to lipids, proteins, and even DNA [8]. The reduction of Cr(VI) produces Cr(III), which can create complexes with DNA, leading to DNA double-strand breaks and carcinogenic effects [9,10,11]. Cr(VI) affects the expression of DNA repair genes [12]. Several pathways leading to cell death, including apoptosis and autophagy, have been linked to Cr(VI)-induced liver diseases. Cr(VI) induces apoptosis in HepG2 cells by disrupting redox homeostasis [13]. It also triggers mitochondrial autophagy and liver toxicity by enhancing Drp1 mitochondrial translocation and increasing Drp1 expression [14]. However, it is unknown whether ferroptosis contributes to the liver injury triggered by Cr(VI).
Ferroptosis is a newly recognized form of programmed cell death that occurs due to the extensive buildup of lipid peroxides [15]. Membrane phospholipids undergo Fenton reactions with the participation of iron, generating a large number of lipid ROS and eliciting lipid peroxidation. This phenomenon ultimately leads to cellular ferroptosis as it exceeds the cells’ own regulatory threshold [16]. The presence of polyunsaturated fatty acids in membrane lipids, the production of ROS radicals, and the occurrence of lipid peroxidation are three essential factors for the onset of ferroptosis. A balanced and stable intracellular antioxidant system is particularly important for preventing the occurrence of ferroptosis. Cellular oxidative stress induced by Cr(VI) may lead to ferroptosis because Cr(VI) is highly oxidizing and can significantly increase intracellular oxidative stress.
The abundance of membrane structures in the endoplasmic reticulum (ER) indicates its extremely important biological functions. This organelle is vulnerable to various environmental changes, which can affect its normal function. If only mild ERS is present, the homeostatic unfolded protein response (UPR) will restore ER homeostasis and maintain cell survival by reducing protein synthesis or increasing the degradation of unfolded and misfolded proteins. However, if the cell fails to fully restore homeostasis, the aggregated misfolded and unfolded proteins in the ER lumen will initiate pathways that induce cellular suicide [17]. Increasing evidence indicates that the rise in ERS during ferroptosis is triggered by various factors [18, 19]. Previous studies have shown that Cr(VI) upregulates ERS-related genes in the human hepatocyte line (L-02) and stimulates the release of large amounts of Ca2+ from the ER, inducing ERS in L-02 [20]. Therefore, we assume that ERS may be involved in Cr(VI)-induced ferroptosis in chicken hepatocytes.
PERK is one of the three transmembrane sensors of ER. Under normal physiological conditions, PERK remains inactive and binds to GRP78. When stimulation induces sustained or high levels of ERS, PERK is activated upon dissociation from GRP78, thereby initiating the cell death program. There is increasing evidence that PERK is involved in the process of ferroptosis in the development of various diseases, including liver and lung injury, and colorectal cancer [21,22,23]. However, we found that most of these studies focused on mammals and humans, while the impact of PERK on avian cellular ferroptosis has not been reported. Moreover, the impact of PERK on ferroptosis varies under different conditions. This study aims to determine whether Cr(VI) induces ferroptosis in chicken hepatocytes and to examine the role of PERK in this process.
Materials and Methods
Reagents and Antibodies
Potassium dichromate (K2Cr2O7) was supplied by Kaitong Chemical (Tianjin, China). High-glucose Dulbecco’s Modified Eagle’s Medium (DMEM), William’s E Medium (12,551,032), and Opti-MEM (31,985062) were obtained from Gibco Company (CA, USA). Percoll (P8370) and collagenase IV (C8160) were provided by Solarbio (Beijing, China). Erastin (HY-15763), ferrostatin-1 (HY-100579), and Cell Counting Kit-8 (HY-K0301) were supplied by MedChemExpress (MCE, NJ, USA). Total Glutathione Assay Kit (S0052), the Total Superoxide Dismutase Assay Kit with WST-8 (S0101), and Lipid Peroxidation MDA Assay Kit (S0131) were acquired from Beyotime (Jiangsu, China). C11 BODIPY 581/591 (GC40165) was obtained from GlpBio (CA, USA).
GPX4 antibody (A13309) and COX2 antibody (A1253) were purchased from ABclonal (MA, USA). The HSP27 antibody (DF6043) and PERK antibody (AF5304) were provided by Affinity (TX, USA). The GRP78 antibody was obtained from Proteintech (Wuhan, China).
Cell Culture
Fifteen percent of fetal bovine serum (FBS) was added as an addition to William’E medium. Insulin from bovine and dexamethasone were added to enhance cell adhesion. Liver tissues were collected from 1-day-old Hyland Brown chicks, ground, and digested with collagenase IV to remove adherent tissues. Percoll was utilized to remove red blood cells. The chicken primary cells were resuspended in an appropriate culture dish and incubated in a 5% CO2 at 37 °C. The chicken hepatocellular carcinoma cell line (LMH) was cultured in 5% CO2 at 37 °C until the cell density reached 70–80% confluence, and then it was passaged into six-well plates or 24-well plates.
Cell Treatment
Seven groups were set up as follows: (1) control group; (2) Cr(VI)-treated group; (3) erastin-treated group; (4) Fer-1-treated group; (5) Cr(VI) + Fer-1 group; (6) negative control (NC) group; and (7) Cr(VI) + siRNA group.
Different treatment times and concentrations of Cr(VI) were determined based on cell types: 40 μM Cr(VI) was given to primary cells for 6 h, while 20 μM Cr(VI) was given to LMH cells for 20 h. The concentrations of the ferroptosis-specific inducer erastin and the inhibitor Fer-1 were 2.5 and 10 μM, respectively. For siRNA silencing, the cells were incubated in Opti-MEM containing either NC or siRNA for 6 h. The medium was then switched to normal medium for an additional 24 h.
Cell Viability Assay
Chicken primary hepatocytes were inoculated into 96-well plates and incubated in an incubator for 24 h to assess the cell viability of chicken primary hepatocytes under various Cr(VI) treatment conditions. The cells were exposed to10, 20, 40, and 80 μM of Cr(VI) for 2, 4, and 6 h, respectively. The medium containing Cr(VI) was discarded and replaced with CCK-8 solution. The cells were incubated with CCK-8 solution in a 5% CO2 at 37 °C for 1 h. Absorbance was measured at 450 nm.
Western Blot
Total proteins were extracted from the treated cells for Western blot analysis. The cells were lysed using a commercial lysis solution. Electrophoresis was conducted using a 10% SDS-PAGE gel at 150 V for 40 min. The polyvinylidene fluoride (PVDF) membranes were treated with methanol. The gel was run at 220 mA for 1 h to ensure complete transfer of the protein sample to the PVDF membrane. Before being treated overnight at 4 °C with primary antibodies, the membranes were first sealed with 5% skim milk powder. After washing, the membranes were incubated with the appropriate secondary antibody at room temperature for 1.5 h. The target protein was then detected using ECL western detection reagents and analyzed with ImageJ. The primary antibodies used in the experiment and their dilution concentrations were as follows: GPX4 (1:1000), HSP27 (1:1000), COX2 (1:1000), GRP78 (1:1000), PERK (1:1000), and GAPDH (1:8000).
GSH, SOD, and MDA Assays
GSH, MDA, and SOD were quantified by colorimetric methods. After centrifuging the treated cells, they were lysed and then mixed with the appropriate reagents as instructed. Absorbance at 412, 450, and 532 nm was recorded to determine the levels of GSH, MDA, and SOD, respectively.
Lipid ROS Assay
LMH cells were treated with C11 BODIPY 581/591 and then incubated for 40 min in the dark, following the provide instructions. Next, the probes that did not enter the cells were washed with PBS and finally resuspended in DMEM without FBS. The samples were tested by flow cytometry. When observing lipid ROS by laser confocal microscopy, the instrument was washed three times with the same PBS solution. The sample was observed using an Eclipse Ti confocal microscope.
Immunofluorescence
After five steps of permeabilization with anhydrous ethanol, 5% BSA was used to fix cells, followed by incubation with primary and secondary antibodies. Nucleus staining was performed on treated LMH cells. The fluorescence intensity of the proteins was observed using confocal microscopy.
Transfection with siRNA
Opti-MEM was used to complex Lipofectamine 3000 with siRNA of negative control or PERK to prepare Lipofectamine 3000-siRNA conjugates. The medium was added with LMH cells, which were then cultured for 6 h and replaced with normal medium for 24 h to complete the transfection process. PERK was silenced by the following siRNA: sense, 5ʹ-GAUGAAAGAUACAGUGAUATT-3ʹ, and antisense, 5ʹ-UAUCACUGUAUCUUUCAUCTT-3ʹ.
Statistical Analysis
All results were expressed as the mean ± standard (SD) of at least three independent experiments. Statistical analyses were performed using SPSS 25.0 (SPSS Inc., Chicago, IL, USA). Comparisons were analyzed using either one-way ANOVA or t-test. The levels of significance are as follows: * P < 0.05, ** P < 0.01 vs. control group. # P < 0.05, ## P < 0.01 vs. Cr(VI)-treated group. ns means not significant.
Results
Establishment of a Cr(VI) Poisoning Model in Chicken Hepatocytes
First, chicken primary hepatocytes were extracted according to the method previously developed [24]. Based on CCK-8 detection, the cell viability at different times and Cr(VI) concentrations is displayed in Fig. 1a. When cells were exposed to Cr(VI) for 6 h at a concentration of 40 μM, the cell inhibition was reduced to 50%. Thus, 6 h and 40 μM were used to establish a poisoning model. Referring to previous studies [25], we established various time gradients (6, 15, and 20 h) and concentration gradients (5, 10, and 20 μM) to observe alterations in the GPX4 protein in LMH cells. As portrayed in Fig. 1b and c, the GPX4 protein level did not decrease at 6 and 15 h for all three concentrations of Cr(VI) until 20 h and 20 μM (Fig. 1d). Thus, 20 h and 20 μM were used as the standard for Cr(VI) in the following experiments related to LMH cells.
Determination of Cr(VI) treatment concentration and time. a Cell viability of chicken primary hepatocytes was tested by CCK8 assay after being exposed to indicate concentration of Cr(VI) (10, 20, 40, 80 µM) at 2, 4, and 6 h. b–d GPX4 protein levels and the relative intensities. LMH cells were supplied with different concentration (5, 10, 20 μM) Cr(VI) for 6, 15, and 20 h. Results shown expressed as means ± SEM (n = 3). ** means P < 0.01. ns, not significant
Cr(VI)-Induced Ferroptosis in Chicken Primary Hepatocytes
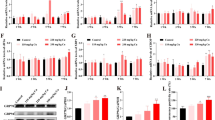
The protein expression levels of ferroptosis-related proteins COX2, GPX4, and HSP27 were detected to determine whether Cr(VI) could induce ferroptosis in chicken primary hepatocytes (Fig. 2a). In this part of the experiment, erastin was utilized to induce ferroptosis. In comparison with the control group, the levels of COX2 protein increased, while the GPX4 and HSP27 levels were significantly lower in the Cr(VI)-treated group (Fig. 2b–d). As shown in Fig. 2e–g, the intracellular levels of GSH and SOD decreased, while the levels of MDA increased significantly after Cr(VI) treatment in comparison with the control. The addition of Fer-1 alleviated cellular damage to the antioxidant system due to Cr(VI) exposure, accompanied with an increase in GSH and SOD content and a drop in MDA levels. This data suggests that Cr(VI) could induce ferroptosis in chicken primary hepatocytes.
Cr(VI)-induced ferroptosis in chicken primary hepatocytes. The chicken primary hepatocytes were supplied with Cr(VI) (40 μM) and erastin (2.5 μM). a COX2, HSP27, and GPX4 protein levels. b–d The relative intensities of COX2 (b), HSP27 (c), and GPX4 (d) were assessed. e–g The relative GSH (e), SOD (f), and MDA (g) content were identified in cells by corresponding kits. Results are shown as means ± SEM (n = 3). *, # means P < 0.05, ** means P < 0.01
Ferrostatin-1 (Fer-1) Can Attenuate Cr(VI)-Induced Cell Death in LMH Cells
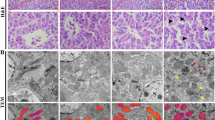
Based on the above results, we aim to understand whether Cr(VI) could trigger ferroptosis in LMH cells (Fig. 3a). The levels of GPX4 as well as HSP27 substantially decreased (Fig. 3c–d), and the level of COX2 significantly increased (Fig. 3b) in the Cr(VI)-treated group compared to the control group. However, Fer-1 reversed this change. The same assay of the intracellular redox profile revealed a dramatic drop in GSH (Fig. 3e) and SOD (Fig. 3f), as well as a significant rise in MDA (Fig. 3g). With respect to lipid ROS generated during ferroptosis (Fig. 3h), there was a noticeable shift to the right of the peak during ferroptosis in the Cr(VI)-treated group in comparison with that in the control. The use of Fer-1 led to a diminished rightward shift of the peak and a decrease in lipid peroxidation. The green fluorescence intensity was notably highest in the Cr(VI)-treated group and significantly weaker in the Cr(VI) + Fer-1 group (Fig. 3i). All of the above findings show that Cr(VI) can induce ferroptosis in LMH cells.
Ferroptosis inhibitor Fer-1 can attenuate Cr(VI)-induced cell injury in LMH cells. LMH cells were supplied with Cr(VI) (20 μM) and Fer-1(10 μM). a COX2, HSP27, and GPX4 protein levels. b–d The relative intensities of COX2 (b), HSP27 (c), and GPX4 (d) were assessed. e–g The relative GSH (e), SOD (f), and MDA (g) content in LMH cells. h–i Cells were stained with C11 BODIPY 581/591, and Cr(VI)-induced accumulation of lipid ROS was observed by flow cytometry (h) and by confocal microscopy (i). Results are shown as means ± SEM (n = 3). *, # means P < 0.05, **, ## means P < 0.01
Cr(VI)-Induced ERS in Chicken Hepatocytes
As the largest intracellular organelle in terms of volume, the ER plays an extremely important role in maintaining normal cellular physiological functions, particularly in lipid metabolism and synthesis. Thus, the ERS was likely involved in Cr(VI)-induced ferroptosis in chicken hepatocytes. As predicted, the GPR78 level increased in chicken primary hepatocytes and LMH cells when ferroptosis was induced by Cr(VI) (Fig. 4a–b). In the Cr(VI)-treated group, the fluorescence intensity of GRP78 was considerably higher than in the control group (Fig. 4d). Furthermore, the expression of PERK exposed to Cr(VI) significantly increased, as demonstrated by a Western blot study (Fig. 4c), consistent with the immunofluorescence results (Fig. 4e). Hence, the ERS is involved in ferroptosis caused by Cr(VI) in chicken hepatocytes.
Cr(VI)-induced ERS in chicken hepatocytes. a GRP78 protein levels and the relative intensities. The chicken primary hepatocytes were supplied with Cr(VI) (40 μM). b–c GRP78 (b) and PERK (c) protein levels and the relative intensities. The LMH cells were supplied with Cr(VI) (20 μM). d GRP78 protein levels observed by a confocal microscope. e PERK protein levels observed by a confocal microscope. Results are shown as means ± SEM (n = 3). * means P < 0.05, ** means P < 0.01
PERK-siRNA Promotes Cr(VI)-Induced Ferroptosis in Chicken Hepatocytes
siRNA was designed to silence PERK, and silencing efficiency was tested to characterize the effects of PERK on ferroptosis caused by Cr(VI) in chicken hepatocytes (Fig. 5a–b). Compared with that in the Cr(VI)-treated group, PERK-siRNA caused a remarkable decline in GPX4 and an increase in COX2 (Fig. 5c–f). However, the HSP27 protein level did not change significantly between the Cr(VI) + siRNA and Cr(VI)-treated groups (Fig. 5e), suggesting that it may not be involved in the PERK-mediated ferroptosis process. The production of lipid ROS was detected by flow cytometry after live cell staining. The findings demonstrated that the mean fluorescence intensity of the siRNA + Cr(VI) group was higher than that of the Cr(VI)-treated group alone (Fig. 5g). Hence, the silencing of PERK exacerbated Cr(VI)-induced ferroptosis in chicken hepatocytes.
Effects of PERK in Cr(VI)-induced ferroptosis in LMH cells. a The protein levels of PERK after treatment with NC and siRNA. b The relative intensities of PERK were assessed. c Effects of Cr(VI) and siRNA on COX2, HSP27, and GPX4 in LMH cells. d–f The relative intensities of COX2 (d), HSP27 (e), and GPX4 (f) were assessed. g Flow cytometry analysis of the impacts of siRNA on the Cr(VI)-induced formation of lipid ROS by C11 BODIPY 581/591 staining. Results are shown as means ± SEM (n = 3). *, # means P < 0.05, **, ## means P < 0.01
Discussion
In their search for medications to target the mutant RAS (rat sarcoma) gene, Dixon et al. [26] developed the concept of “ferroptosis,” which is recognized as a new type of programmed cell death. Ferroptosis involves a complex biological process that arises from a dynamic imbalance of antioxidants, iron, and lipid [27]. The ER is responsible for lipid synthesis in cells, and there is an inseparable relationship between ERS and ferroptosis. The hepatotoxicity of Cr(VI) is quite common, and previous studies have reported that liver injury associated with Cr(VI) is linked to oxidative stress and lipid peroxidation [28, 29]. However, whether ferroptosis is involved in Cr(VI)-induced liver damage remains unclear. The present study found that Cr(VI) disrupts the intracellular redox system because of its potent oxidative properties, leading to lipid peroxidation and inducing ferroptosis in chicken hepatocytes.
The Chinese National Standard for Food Safety Limits for Contaminants in Food (GB 2762–2017) sets the limit value for Cr at 0.5 mg/kg. However, some studies have shown that the current Cr content in agricultural soil in certain areas of China is as high as 3883.77 mg/kg, exceeding the national standard threshold. Additionally, there is evidence that the chromium content in the edible portion of some agricultural products ranges from 2.38 to 139.76 mg/kg, also surpassing the national standard threshold. This indicates that Cr contamination is a serious issue in some areas [30]. In a study by Peng et al., 20 μM of Cr(VI) was used to treat LMH cells for 72 h to investigate its effect on lipid metabolism [31]. In this experiment, 20 μM and 40 μM Cr(VI) were used to treat cells for 20 h and 6 h, corresponding to 1–2 mg/L. Therefore, this dosage of dose seems to be understood both in real life and as an experimental model concentration.
GPX4 functions as a primary inhibitor of ferroptosis by converting detrimental phospholipid hydroperoxides (PLOOH) into benign phospholipid alcohols (PLOH) [15]. Decreased levels of GPX4 are considered a marker of ferroptosis [32]. COX2 is encoded by PTGS2, and its expression increases most significantly in the death of ferroptotic cells in mice [33]. HSP27, a member of the heat shock protein family, can induce resistance to ferroptosis by inhibiting cytoskeleton-mediated iron uptake through phosphorylation. The two proteins can be used as markers for identifying ferroptosis [34]. As predicted, the treatment of cells with Cr(VI) resulted in decreased intracellular levels of GPX4 and HSP27 proteins and increased the COX2 level. These changes tentatively demonstrate the emergence of ferroptosis.
The decrease in cellular antioxidant capacity and the accumulation of lipid ROS can lead to oxidative cell death, known as ferroptosis. GSH is a substrate for the synthesis of GPX4 and is a crucial component in the inhibition of ferroptosis [35]. SOD can remove ROS from cells and prevent the accumulation of large amounts of ROS. Therefore, it is an essential antioxidant enzyme in the body [36]. MDA is the by-product of peroxidation processes that occur when free radicals interact with lipids. The extent of membrane lipid peroxidation is known by measuring MDA, which serves as an indirect indicator of the extent of damage to the membrane system [37]. In previous studies, ferroptosis triggered by various factors was always accompanied by changes in the intracellular levels of GSH, SOD, and MDA [19, 38, 39]. Fer-1 has been described to achieve anti-ferroptosis by lessening lipid peroxidation and is commonly used in experimental studies [38, 40]. Therefore, Fer-1 was applied in our study as a type of specific inhibitor of ferroptosis. We found that Fer-1 alleviated the decrease in GSH and SOD and the increase in MDA induced by Cr(VI) exposure. In summary, our data confirmed that Cr(VI) triggers the activation of ferroptosis by disrupting the intracellular antioxidant capacity.
LMH cells were utilized to conduct experiments concurrently with chicken primary hepatocytes to further confirm the significant impact of ferroptosis in Cr(VI)-induced liver injury. LMH cells are a chemically mutated oncogenic chicken hepatocyte cell line that retains many phenotypic features of chicken hepatocytes while exhibiting the characteristics of cancer cells that proliferate indefinitely [41]. The basal ferroptosis levels of LMH cells were examined and compared with those of chicken primary hepatocytes to determine whether LMH cells could be suitable as a model for the experiment. The findings demonstrated that the basal ferroptosis levels between the two cell types did not differ significantly (Fig. S1). This excludes the possibility of a cell line error for the experiment and confirms that LMH cells could serve as a model for the next step of the study. Further experimental results showed that in LMH cells, Cr(VI) triggered ferroptosis by reducing GPX4 and HSP27 protein expression. LMH cells treated with Cr(VI) also showed increased levels of COX2. The treatment with Cr(VI) reduced the GSH and SOD levels and on the other hand increased the MDA levels. These effects were reversed by Fer-1.
The C11 BODIPY 581/591 probe can detect the formation of lipid radicals and is frequently utilized to measure the extent of membrane lipid peroxidation [42]. Therefore, the green fluorescence intensity emitted by the probe upon activation typically indicates the level of lipid ROS. We discovered that the increased lipid ROS fluorescence intensity of Cr(VI) was quenched by Fer-1. These results verify those obtained in chicken primary hepatocytes.
The PERK protein is one of the three transmembrane sensors in the UPR. The activation of the PERK signaling pathway occurs at the early stage of ERS, which protects cells by inhibiting protein synthesis. Accumulating evidence suggests that researchers have differing views on the role of PERK in promoting cell survival or death. According to Wei et al., tagitinin C activates the nuclear translocation of nuclear factor erythroid 2-related factor 2 (Nrf2) by inducing ERS and oxidative stress, leading to ferroptosis in HCT116 cells through the activation of the PERK-Nrf2-HO-1 signaling pathway [21]. Chen et al. found that the activation of the PERK/ATF4/HSPA5 pathway led to an increase in GPX4 expression and lipid peroxidation, thereby preventing the ferroptosis of glioma cells [22]. The relationship between ERS and ferroptosis is not fully understood, although ferroptosis is likely to be initiated when the normal physiological function of the ER experiences an irreversible error. Therefore, we tested the occurrence of ERS by continuously exposing the cells to a Cr(VI) environment. We found that the expression of PERK significantly increased in response to Cr(VI) exposure. Therefore, PERK plays a crucial role in Cr(VI)-induced ferroptosis.
Subsequent experiments were conducted using LMH cells due to the challenges associated with transfecting primary cells, which is attributed to the high toxicity of the transfection reagent. PERK was silenced in LMH cells to investigate the role of PERK in Cr(VI)-induced ferroptosis. The alterations in GPX4 and COX2 were more obvious due to the silencing of PERK than when treated with Cr(VI) alone. Moreover, the production of lipid ROS was significantly increased in Cr(VI)-treated LMH cells transfected with PERK-siRNA. The above results indicate that silencing PERK exacerbates Cr(VI)-induced ferroptosis in chicken hepatocytes. Therefore, we suggest that PERK acts as a negative regulator of ferroptosis in chicken hepatocytes.
Ferroptosis quite frequently interacts with other types of programmed cell death, such as necrosis and apoptosis, and ERS plays a key role in this process [43]. Multiple factors can activate the PERK/eIF2α/ATF4/CHOP pathway, leading to apoptosis. There is also evidence suggesting that the PERK/eIF2α/ATF4/CHOP pathway may act as a potential mediator of ferroptosis. Therefore, further exploration is needed to determine whether the distinct role of PERK in ferroptosis is a result of interplay among different types programmed cell death or other unidentified factors.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Liu J, Xue J, Wei X, Su H, Xu R (2020) Optimization of Cr(6+) removal by Bacillus subtilis strain SZMC 6179J from chromium-containing soil. Indian J Microbiol 60(4):430–435. https://doi.org/10.1007/s12088-020-00886-3
M. K. Murthy, P. Khandayataray, S. Padhiary and D. Samal (2022) A review on chromium health hazards and molecular mechanism of chromium bioremediation. Reviews on environmental health 11;38(3):461–478. https://doi.org/10.1515/reveh-2021-0139
Li X, Zhang J, Ma J, Liu Q, Shi T, Gong Y, Yang S, Wu Y (2020) Status of chromium accumulation in agricultural soils across China (1989–2016). Chemosphere 256:127036. https://doi.org/10.1016/j.chemosphere.2020.127036
Ali A, Ma Y, Reynolds J, Wise JP, Inzucchi SE, Katz DL (2011) Chromium picolinate for the prevention of type 2 diabetes. Treatment strategies Diabetes 3(1):34–40. https://doi.org/10.1038/nature12828
Kooshki F, Moradi F, Karimi A, Niazkar HR, Khoshbaten M, Maleki V, Pourghassem Gargari B (2021) Chromium picolinate balances the metabolic and clinical markers in nonalcoholic fatty liver disease: a randomized, double-blind, placebo-controlled trial. Eur J Gastroenterol Hepatol 33(10):1298–1306. https://doi.org/10.1097/meg.0000000000001830
J. J. Coetzee, N. Bansal, E. J. E. Chirwa and health (2020) Chromium in environment, its toxic effect from chromite-mining and ferrochrome industries, and its possible bioremediation. 12 (1): 51–62. https://doi.org/10.1007/s12403-018-0284-z
Zill EH, Khan ZI, Noorka IR, Ahmad K, Wajid K, Nadeem M, Munir M, Malik IS, Kiran M, Hussain T, Qamar MF, Ahmad T, Rehman SU, Ullah MF (2021) Appraisal of chromium in chicken reared on maize irrigated with sewage water. Environ Sci Pollut Res Int 28(9):11509–11517. https://doi.org/10.1007/s11356-020-11393-9
Salnikow K, Zhitkovich A (2008) Genetic and epigenetic mechanisms in metal carcinogenesis and cocarcinogenesis: nickel, arsenic, and chromium. Chem Res Toxicol 21(1):28–44. https://doi.org/10.1021/tx700198a
Saran U, Tyagi A, Chandrasekaran B, Ankem MK, Damodaran C (2021) The role of autophagy in metal-induced urogenital carcinogenesis. Seminars in cancer biology 76:247–257. https://doi.org/10.1016/j.semcancer.2021.03.022
Li J, Zheng X, Ma X, Xu X, Du Y, Lv Q, Li X, Wu Y, Sun H, Yu L, Zhang Z (2019) Melatonin protects against chromium(VI)-induced cardiac injury via activating the AMPK/Nrf2 pathway. J Inorg Biochem 197:110698. https://doi.org/10.1016/j.jinorgbio.2019.110698
Lv Y, Jiang H, Li S, Han B, Liu Y, Yang D, Li J, Yang Q, Wu P, Zhang Z (2020) Sulforaphane prevents chromium-induced lung injury in rats via activation of the Akt/GSK-3β/Fyn pathway. Environmental pollution (Barking, Essex : 1987) 259:113812. https://doi.org/10.1016/j.envpol.2019.113812
Sun H, Zhou X, Chen H, Li Q, Costa M (2009) Modulation of histone methylation and MLH1 gene silencing by hexavalent chromium. Toxicol Appl Pharmacol 237(3):258–266. https://doi.org/10.1016/j.taap.2009.04.008
Das J, Sarkar A, Sil PC (2015) Hexavalent chromium induces apoptosis in human liver (HepG2) cells via redox imbalance. Toxicol Rep 2:600–608. https://doi.org/10.1016/j.toxrep.2015.03.013
Zhang Y, Ma Y, Xiao Y, Lu C, Xiao F (2020) Drp1-dependent mitochondrial fission contributes to Cr(VI)-induced mitophagy and hepatotoxicity. Ecotoxicol Environ Saf 203:110928. https://doi.org/10.1016/j.ecoenv.2020.110928
Tang D, Kroemer G (2020) Ferroptosis. Current biology : CB 30(21):R1292-r1297. https://doi.org/10.1016/j.cub.2020.09.068
Hadian K, Stockwell BR (2020) SnapShot: ferroptosis. Cell 181(5):1188-1188.e1181. https://doi.org/10.1016/j.cell.2020.04.039
Oakes SA, Papa FR (2015) The role of endoplasmic reticulum stress in human pathology. Annu Rev Pathol 10:173–194. https://doi.org/10.1146/annurev-pathol-012513-104649
Huang J, Xie H, Yang Y, Chen L, Lin T, Wang B, Lin QC (2022) The role of ferroptosis and endoplasmic reticulum stress in intermittent hypoxia-induced myocardial injury. Sleep & breathing = Schlaf & Atmung 27(3):1005–1011. https://doi.org/10.1007/s11325-022-02692-1
Zhang X, Jiang L, Chen H, Wei S, Yao K, Sun X, Yang G, Jiang L, Zhang C, Wang N, Wang Y, Liu X (2022) Resveratrol protected acrolein-induced ferroptosis and insulin secretion dysfunction via ER-stress- related PERK pathway in MIN6 cells. Toxicology 465:153048. https://doi.org/10.1016/j.tox.2021.153048
Liang Q, Zhang Y, Huang M, Xiao Y, Xiao F (2019) Role of mitochondrial damage in Cr(VI)-induced endoplasmic reticulum stress in L-02 hepatocytes. Mol Med Rep 19(2):1256–1265. https://doi.org/10.3892/mmr.2018.9704
Wei R, Zhao Y, Wang J, Yang X, Li S, Wang Y, Yang X, Fei J, Hao X, Zhao Y, Gui L, Ding X (2021) Tagitinin C induces ferroptosis through PERK-Nrf2-HO-1 signaling pathway in colorectal cancer cells. Int J Biol Sci 17(11):2703–2717. https://doi.org/10.7150/ijbs.59404
Chen Y, Mi Y, Zhang X, Ma Q, Song Y, Zhang L, Wang D, Xing J, Hou B, Li H, Jin H, Du W, Zou Z (2019) Dihydroartemisinin-induced unfolded protein response feedback attenuates ferroptosis via PERK/ATF4/HSPA5 pathway in glioma cells. Journal of experimental & clinical cancer research : CR 38(1):402. https://doi.org/10.1186/s13046-019-1413-7
Wu Q, Liu C, Liu D, Wang Y, Qi H, Liu X, Zhang Y, Chen H, Zeng Y, Li J (2023) Polystyrene nanoplastics-induced lung apoptosis and ferroptosis via ROS-dependent endoplasmic reticulum stress. The Science of the total environment 912:169260. https://doi.org/10.1016/j.scitotenv.2023.169260
Wang L, Zheng P, Cui Y, Zhang Z, Song K, Liu Y, Liu J (2022) Regulation of Parkin in Cr (VI)-induced mitophagy in chicken hepatocytes. Ecotoxicol Environ Saf 248:114315. https://doi.org/10.1016/j.ecoenv.2022.114315
Liu K, Chen P, Lu J, Zhu Y, Xu Y, Liu Y, Liu J (2020) Protective effect of purple tomato anthocyanidin on chromium(VI)-induced autophagy in LMH cells by inhibiting endoplasmic reticulum stress. Biol Trace Elem Res 194(2):570–580. https://doi.org/10.1007/s12011-019-01795-3
Dixon SJ, Lemberg KM, Lamprecht MR, Skouta R, Zaitsev EM, Gleason CE, Patel DN, Bauer AJ, Cantley AM, Yang WS, Morrison B 3rd, Stockwell BR (2012) Ferroptosis: an iron-dependent form of nonapoptotic cell death. Cell 149(5):1060–1072. https://doi.org/10.1016/j.cell.2012.03.042
Hirschhorn T, Stockwell BR (2019) The development of the concept of ferroptosis. Free Radical Biol Med 133:130–143. https://doi.org/10.1016/j.freeradbiomed.2018.09.043
Bellouard M, Gasser M, Lenglet S, Gilardi F, Bararpour N, Augsburger M, Thomas A, Alvarez JC (2022) Toxicity and metabolomic impact of cobalt, chromium, and nickel exposure on HepaRG hepatocytes. Chem Res Toxicol 35(5):807–816. https://doi.org/10.1021/acs.chemrestox.1c00429
Y. Wang, Y. Liu, H. Wan, Y. Zhu, P. Chen, P. Hao, Z. Cheng and J. Liu (2017) Moderate selenium dosing inhibited chromium (VI) toxicity in chicken liver. Journal of biochemical and molecular toxicology 31:(8). https://doi.org/10.1002/jbt.21916
S. Xu, C. Yu, Q. Wang, J. Liao, C. Liu, L. Huang, Q. Liu, Z. Wen and Y. Feng (2022) Chromium contamination and health risk assessment of soil and agricultural products in a rural area in Southern China. Toxics 11:(1). https://doi.org/10.3390/toxics11010027
Peng Y, Li H, Shen K, Pan W, Zhang J, Zhou D (2021) Nano-selenium alleviating the lipid metabolism disorder of LMH cells induced by potassium dichromate via down-regulating ACACA and FASN. Environ Sci Pollut Res Int 28(48):69426–69435. https://doi.org/10.1007/s11356-021-14775-9
Imai H, Matsuoka M, Kumagai T, Sakamoto T, Koumura T (2017) Lipid peroxidation-dependent cell death regulated by GPx4 and ferroptosis. Curr Top Microbiol Immunol 403:143–170. https://doi.org/10.1007/82_2016_508
Yang WS, SriRamaratnam R, Welsch ME, Shimada K, Skouta R, Viswanathan VS, Cheah JH, Clemons PA, Shamji AF, Clish CB, Brown LM, Girotti AW, Cornish VW, Schreiber SL, Stockwell BR (2014) Regulation of ferroptotic cancer cell death by GPX4. Cell 156(1–2):317–331. https://doi.org/10.1016/j.cell.2013.12.010
Yuan F, Sun Q, Zhang S, Ye L, Xu Y, Xu Z, Liu B, Zhang S, Chen Q (2022) HSP27 protects against ferroptosis of glioblastoma cells. Hum Cell 35(1):238–249. https://doi.org/10.1007/s13577-021-00645-6
Ursini F, Maiorino M (2020) Lipid peroxidation and ferroptosis: the role of GSH and GPx4. Free Radical Biol Med 152:175–185. https://doi.org/10.1016/j.freeradbiomed.2020.02.027
Wang Y, Branicky R, Noë A, Hekimi S (2018) Superoxide dismutases: dual roles in controlling ROS damage and regulating ROS signaling. J Cell Biol 217(6):1915–1928. https://doi.org/10.1083/jcb.201708007
Tsikas D (2017) Assessment of lipid peroxidation by measuring malondialdehyde (MDA) and relatives in biological samples: analytical and biological challenges. Anal Biochem 524:13–30. https://doi.org/10.1016/j.ab.2016.10.021
Liu P, Feng Y, Li H, Chen X, Wang G, Xu S, Li Y, Zhao L (2020) Ferrostatin-1 alleviates lipopolysaccharide-induced acute lung injury via inhibiting ferroptosis. Cell Mol Biol Lett 25:10. https://doi.org/10.1186/s11658-020-00205-0
Wang C, Yuan W, Hu A, Lin J, Xia Z, Yang CF, Li Y, Zhang Z (2020) Dexmedetomidine alleviated sepsis-induced myocardial ferroptosis and septic heart injury. Mol Med Rep 22(1):175–184. https://doi.org/10.3892/mmr.2020.11114
Degterev A, Linkermann A (2016) Generation of small molecules to interfere with regulated necrosis. Cellular and molecular life sciences : CMLS 73(11–12):2251–2267. https://doi.org/10.1007/s00018-016-2198-x
Kawaguchi T, Nomura K, Hirayama Y, Kitagawa T (1987) Establishment and characterization of a chicken hepatocellular carcinoma cell line. LMH Cancer research 47(16):4460–4464
Lee H, Zandkarimi F, Zhang Y, Meena JK, Kim J, Zhuang L, Tyagi S, Ma L, Westbrook TF, Steinberg GR, Nakada D, Stockwell BR, Gan B (2020) Energy-stress-mediated AMPK activation inhibits ferroptosis. Nat Cell Biol 22(2):225–234. https://doi.org/10.1038/s41556-020-0461-8
Lee YS, Lee DH, Choudry HA, Bartlett DL, Lee YJ (2018) Ferroptosis-induced endoplasmic reticulum stress: cross-talk between ferroptosis and apoptosis. Molecular cancer research : MCR 16(7):1073–1076. https://doi.org/10.1158/1541-7786.Mcr-18-0055
Funding
The project was supported by the National Natural Science Foundation of China (31872535) and Funds of Shandong “Double Tops” Program.
Author information
Authors and Affiliations
Contributions
Conceptualization, J.L.; data curation, Y.C.; formal analysis, P.Z.; funding acquisition, J.L.; investigation, Y.C.; methodology, K.S.; project administration, J.L.; resources, C.Q. and M.L.; software, P.Z.; supervision, J.L. and Y.L.; validation, Y.L.; visualization, K.S. and H.X.; writing, original draft, Y.C.; writing, review and editing, Y.L. and J.L.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cui, Y., Zhang, P., Song, K. et al. Role of PERK-Mediated Endoplasmic Reticulum Stress in Ferroptosis Caused by Hexavalent Chromium in Chicken Hepatocytes. Biol Trace Elem Res (2024). https://doi.org/10.1007/s12011-023-04046-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12011-023-04046-8