Abstract
This study was conducted to compare the changes in different clinical scores and imaging indexes of patients who underwent robot-assisted total knee arthroplasty (RA-TKA) and manual total knee arthroplasty (M-TKA). PubMed, Web of Science, Cochrane Library and Embase were searched according to PRISMA guidelines in June 2024. Search terms included “robot-assisted”, “manual” and “total knee arthroplasty”. Outcome indicators included American Knee Society Score (KSS), Western Ontario McMaster Universities Osteoarthritis Index (WOMAC), Oxford Knee Score (OKS), range of motion (ROM), Hospital for Special Surgery (HSS) score, Forgotten Joint Score (FJS), 36-Item Short Form Health Survey (SF-36), operation duration (min), intraoperative blood loss (ml), pain score, patient’s satisfaction scores, hip–knee–ankle (HKA) angle, frontal femoral component angle, frontal tibia component angle, lateral femoral component angle and lateral tibia component angle. A total of 1,033 articles were obtained after removing duplicates, and 12 studies involving 2,863 patients (1,449 RA-TKAs and 1,414 M-TKAs) were finally meta-analyzed (22–32). The baseline data of both groups were similar in all results. Meta-analysis suggested a better performance of the RA-TKA group than the M-TKA group regarding the HKA angle. The manual TKA reduced the operation time and significantly improved the range of motion. The results of > 6 months follow-up showed that M-TKA was better than RA-TKA in terms of KSS score and WOMAC. Compared with M-TKA, RA-TKA can produce more accurate prosthetic alignment, but it does not lead to better clinical results. Orthopedic surgeons should choose between two surgical procedures according to their own experience and patients’ characteristics.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Total knee arthroplasty (TKA) is highly effective for treating advanced knee osteoarthritis [1]. Despite its great success and rapid development over the past two decades, 20% of patients experience unsatisfactory clinical outcomes after surgery [2, 3]. The precise positioning of components and alignment of the limb are critical factors influencing patient satisfaction and functional results following TKA [4]. In practice, achieving these standards manually can be very challenging for surgeons. The development of orthopedic robots has facilitated the widespread adoption of robot-assisted total knee replacement systems in clinical settings [5,6,7,8]. Many reports have indicated that robotic-assisted total knee arthroplasty (RA-TKA) enables more accurate bone cutting and implant placement and achieves balanced extension and flexion gaps tailored to the patient's skeletal anatomy and natural ligament balance, reducing the probability of detrimental stress and wear [9, 10]. The approach can theoretically promise more significant improvements in clinical outcomes. However, controversy persists regarding whether RA-TKA yields superior functional and clinical outcomes compared to manual TKA (M-TKA). Multiple studies report no statistically significant difference in clinical outcomes, despite favorable radiological outcomes during follow-up visits [11,12,13]. Based on that, many scholars have disputed its clinical significance. Therefore, we collected relevant articles and performed a meta-analysis. The study aims to compare the clinical outcomes and radiological results of RA-TKA and M-TKA through the analysis of relevant studies, thus providing a basis for physicians’ decision-making processes. The hypothesis of this study is that RA-TKA yields significantly superior outcomes than M-TKA, both clinically and radiologically.
Materials and methods
Literature retrieval
This study complied with the standards for Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA 2020) [14] and registered in PROSPERO prospectively (CRD420234731153). Articles published in English were systematically retrieved from PubMed, Web of Science, Cochrane Library and Embase up to June 1, 2024 to comprehensively compare the efficacy and/or safety of RA-TKA and M-TKA in treating knee osteoarthritis. The following terms were searched in the database: "robot-assisted", "robotic-assisted", "robot", "robotic", “Arthroplasty”, "Knee Replacement Arthroplasties", "Robotic Assisted Surgery" and "Total Knee Arthroplasty” (Table S1). Two authors independently and impartially examined the articles that met the inclusion criteria according to the search strategy, performed data extraction and manually examined the reference list of all included studies.
Inclusion and exclusion criteria
Studies that contained the following features were included: 1. studies with a randomized control, cohort or case–control design; 2. patients with end-stage knee osteoarthritis; 3. studies that compared RA-TKA and M-TKA; 4. evaluations including no less than one of the following indicators: American Knee Society Score (KSS), Western Ontario McMaster Universities Osteoarthritis Index (WOMAC), Oxford Knee Score (OKS), joint range of motion (ROM), 36-Item Short Form Health Survey (SF-36) score, Hospital for Special Surgery (HSS) score, Forgotten Joint Score (FJS), pain score, patient satisfaction score, operation length (min), intraoperative blood loss (ml), hip–knee–ankle (HKA) angle, frontal femoral component angle, frontal tibia component angle, lateral femoral component angle and lateral tibia component angle; 5. articles containing enough data for calculating odds ratio (OR) or weighted mean difference (WMD).
Studies were excluded if they were reviews, letters, comments, case reports, abstracts for conference presentation, articles on pediatrics and unpublished articles. We included studies on patients who underwent unilateral RA-TKA or M-TKA, and also excluded studies involving single-compartment knee arthroplasty.
Data extraction
Data was extracted systematically and independently by two investigators (Fu Xinyu and She Yiming). Disagreements were finally resolved by the third researcher (Jin Ri). We extracted the data on first author and publication year of the article, research duration, research country, research design, sample size, patient’s age and body mass index (BMI), follow-up time and interventions. Continuous variables in the included studies presented as the median and interquartile range (IQR) or range were calculated to obtain the mean ± standard deviation using verified mathematical methods [15, 16]. For studies with missing or unreported data, the corresponding author was contacted to request for complete (if any) data.
Quality assessment
Randomized controlled trials (RCTs) as well as cohort studies were evaluated, respectively, using the Cochrane Quality Assessment Scale and Newcastle–Ottawa Scale (NOS) [17]. The scale mainly includes three dimensions: subject selection, comparability between groups and measurement of results. Studies were given a score from 0 to 9, with a score of 7–9 representing high quality [18]. Research quality and level of evidence were separately reviewed by two researchers, and differences were handled via discussion.
Statistical analysis
Evidence synthesis was conducted using Review Manager 5.4 (Cochrane Collaboration, Oxford, UK). Weighted mean difference (WMD) and risk ratio (OR) were adopted to assess continuous and binary variables, respectively. Indicators were all presented using 95% confidence interval (CI). Then heterogeneity (Cochran's Q) and inconsistency index (I2) of all studies were assessed by the Chi-square (X2) test [19]. A p value for the χ 2 test beneath 0.05 or I2 over 50% was considered as remarkable heterogeneity. If there was remarkable heterogeneity, a random effects model was employed to approximate the pooled WMD or OR. If not, the fixed effects model was utilized. To assess the influence of the eligible studies on the pooled results containing remarkable heterogeneity, one-way sensitivity analysis was also performed. The funnel plot was produced using Review Manager 5.4 (Cochrane Collaboration, Oxford, UK). The results involving ≥ three studies were tested by the Egger’s regression test in Stata 15.0 (Stata Corp, College Station, TX, USA) [20], and the publication bias was visually assessed. A p value of lower than 0.05 was deemed to have statistical significance.
Results
Literature retrieval and study characteristics
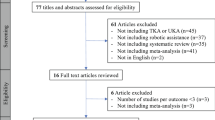
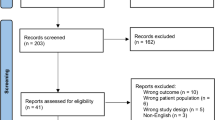
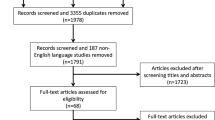
The process of literature retrieval and screening is displayed in detail in Fig. 1. Through systematic literature retrieval, 1,711 related articles were finally obtained from PubMed (n = 342), Embase (n = 644), Cochrane (n = 150) and Web of Science (n = 575). Then 1,033 titles and abstracts of studies were screened after deleting duplicates. Finally, 12 full-text articles were included, concerning 2,863 patients (1,449 RA-TKAs and 1,414 M-TKAs) for pooled analysis [11,12,13, 21,22,23,24,25,26,27,28,29]. Among them, five were RCTs [11, 12, 21,22,23] and seven were cohort studies [13, 24,25,26,27,28,29]. The specific features of all included studies are presented in Table 1. Quality evaluation of eligible cohort studies and RCTs is shown in Table S2 and Fig. 2, respectively.
Change of Knee Society Score
In the analysis of KSS improvement from preoperative to postoperative stages, the RA-TKA and M-TKA groups exhibited similar changes in KSS scores (WMD: −1.18; 95%CI: −3.41, 1.05: p = 0.30), with significant heterogeneity observed (I2 = 98%, p < 0.00001) (Fig. 3a). The subgroup analysis of > 6-month follow-up duration revealed a significantly lower KSS score in the RA-TKA group compared to the M-TKA group (WMD: −0.61; 95%CI: −0.89, −0.33: p < 0.00001) (Table 2).
Change of Western Ontario McMaster Universities Osteoarthritis Index
Five studies reported WOMAC. The pooled analysis indicated that RA-TKA and M-TKA groups demonstrated similar changes in WOMAC scores (MD: 2.32; 95%CI: -4.27, 8.91; p = 0.49), with salient heterogeneity observed (I2 = 98%, p < 0.00001) (Fig. 3b). The subgroup analysis of > 6-month follow-up duration unveiled a significantly lower WOMAC score in the RA-TKA group in contrast to the M-TKA group (WMD: −3.40; 95%CI: −3.72, −3.08; p < 0.00001) (Table 2).
Change of Oxford Knee Score
OKS was reported in four studies, which unraveled that the RA-TKA and M-TKA groups presented with similar OKS scores (WMD: 5.70; 95% CI: -0.97, 12.37; p = 0.09), with salient heterogeneity found (I2 = 100%, p < 0.00001) (Fig. 3). Sensitivity analysis showed that after excluding the research published by Lincon et al. in 2016 [23], the result changed from insignificant to significant, indicating instability of the index (Fig. 4c). The subgroup analysis of cohort studies, > 6-month follow-up duration, and European population revealed a significantly higher ROM score in the RA-TKA group compared to the M-TKA group (Table 2).
Change of joint range of motion
Seven studies reported ROM. The comprehensive analysis suggested a significantly lower ROM score improvement in the RA-TKA group in contrast to the M-TKA group (WMD: −2.84; 95% CI: −3.72, −1.95; p = 0.00001), with significant heterogeneity observed (I2 = 98%, p < 0.00001) (Fig. 3d). Sensitivity analysis uncovered that after excluding the research published by Kim et al. in 2020 [12] or Jin et al. in 2018, the result changed from significant to insignificant, indicating instability of the index (Fig. 4d).
Change of the 36-Item Short Form Health Survey score
The primary analysis demonstrated no statistically significant difference in postoperative SF-36 values between the RA-TKA group and the M-TKA group (WMD: −1.47; 95% CI: −4.02, 1.08; p = 0.26) (Fig. 3e), with significant heterogeneity (I2 = 6%, p < 0.30). Subgroup analysis similarly found no statistical difference.
Change of hospital for special surgery
In the analysis of KSS improvement from preoperative to postoperative stages, the RA-TKA group and the M-TKA group indicated no statistical difference (WMD: −1.06; 95% CI: −3.75, 1.64; p = 0.44) (Fig. 3F) and notable heterogeneity was discovered (I2 = 98%, p < 0.00001).
Forgotten Joint Score (FJS)
Six studies reported FJS. The pooled analysis unveiled a significantly higher FJS score in the RA-TKA group in contrast to the M-TKA group (WMD: 5.59; 95% CI: 3.53, 7.66; p < 0.0001) (Fig. 3g), with no significant heterogeneity (I2 = 21%, p = 0.27).
Change of pain score
Four studies reported pain scores. The comprehensive analysis found no significant difference in pain scores between the RA-TKA and M-TKA groups (WMD: 1.51; 95% CI: -0.34, 3.36; p = 0.11). Sensitivity analysis showed that after excluding the research published by Linkon et al. in 2016, the result changed from insignificant to significant, indicating instability of the index (Fig. 4d).
Patient satisfaction score
Three studies reported patient satisfaction scores. The pooled analysis showed that the RA-TKA and M-TKA groups exhibited similar patient satisfaction scores (WMD: -0.08; 95% CI: −1.40, 1.24; p = 0.91), with no salient heterogeneity (I2 = 0%, p = 0.82) (Fig. 5b).
Operative duration
The operation time was reported in three studies. The comprehensive analysis found that the RA-TKA group exhibited a significantly longer operation time than the M-TKA group (WMD: 25.97; 95% CI: 12.59, 39.34; p = 0.0001), with significant heterogeneity (I2 = 85%, p = 0.001) (Fig. 5c). Sensitivity analysis uncovered that after excluding the research published by Kim et al. in 2020 or Xu et al. in 2022, the result changed from significant to insignificant, indicating instability of the index (Fig. 4f).
Intraoperative blood loss
The comprehensive analysis revealed no statistically significant difference in intraoperative blood loss between the RA-TKA group and the M-TKA group (WMD: −5.53; 95%CI: −1.90, 12.95; p = 0.14), with no salient heterogeneity (I2 = 0%, p = 0.65) (Fig. 5d).
Change of hip-knee-ankle angle
HKA was reported in six studies. The comprehensive analysis suggested a significantly superior HKA score improvement in the RA-TKA group than that in the M-TKA group (WMD: 1.10; 95%CI: 0.40, 1.80: p = 0.002), with significant heterogeneity (I2 = 99%, p < 0.00001) (Fig. 6a).
Frontal femoral component angle
Frontal femoral component (FFC) angle was reported in three studies. The comprehensive analysis found no clinical difference in the FFC angle between the RA-TKA group and the M-TKA group (WMD: 0.61; 95%CI: −0.19, 1.42; p = 0.14), with no salient heterogeneity (I2 = 90%, p < 0.0001) (Fig. 6b). Sensitivity analysis indicated that after excluding the research published by Jin et al. in 2018 [26], the result changed from insignificant to significant, indicating instability of the index (Fig. 4h). The subgroup analysis of RCT in a study revealed a significantly higher FFC score in the RA-TKA group compared to the M-TKA group (WMD: 1.01; 95%CI: 0.81, 0.21; p < 0.0001) (Table 2).
Frontal tibia component angle
Three studies reported frontal tibia component (FTC) angle. Pooled analysis revealed no meaningful difference in FTC angle between the RA-TKA group FFC and the M-TKA group (WMD: 0.13; 95%CI: -0.99, 1.25; p = 0.82), and there was remarkable heterogeneity (I2 = 93%, p < 0.00001) (Fig. 6c).
Lateral femoral component angle
Three studies reported lateral femoral component (LFC) angle. Pooled analysis revealed no significant difference in the LFC angle between the RA-TKA group FFC and the M-TKA group (WMD: −0.80; 95%CI: −3.73, 2.13; p = 0.59), and there was remarkable heterogeneity (I2 = 99%, p < 0.00001) (Fig. 6d). The cohort study subgroup analysis discovered a significantly lower LFC score in the RA-TKA group than in the M-TKA group (WMD: −2.90; 95%CI: −3.42, −2.38; p < 0.00001) (Table 2).
Lateral tibia component angle
Three studies reported lateral tibia component (LTC) angle. Pooled analysis found no meaningful difference in LTC score between the RA-TKA group and the M-TKA group (WMD: 0.65; 95%CI: -0.52, 1.81; p = 0.28), and remarkable heterogeneity was noted (I2 = 93%, p < 0.00001) (Fig. 6f). Sensitivity analysis discovered that when the research published by Jin et al. in 2018 [26] was excluded, the result changed from insignificant to significant, indicating that the index was unstable (Fig. 4k). RCT subgroup analysis revealed a significantly higher FFC score in the RA-TKA group than in the M-TKA group (WMD: 1.06; 95%CI: 0.80, 1.31; p < 0.0001) (Table 2).
Publication bias
A visual assessment of funnel plots for all outcome measures (Fig. 7) was performed. Outcome measures showing potential publication bias were subjected to Egger’s test. No statistically significant publication bias was observed.
Discussion
The most important findings of this meta-analysis are as follows: 1. The RA-TKA group demonstrated significantly better improvements in HKA angle and postoperative FJS score compared to the M-TKA group. 2. In contrast to the RA-TKA group, the operation time was shorter in the M-TKA group. Subgroup analysis of > 6-month follow-up results showed that the M-TKA group exhibited more significant improvements in KSS score and WOMAC score.
With the ultimate goal of building a stable, painless and long-lasting joint, M-TKA relies on surgical instruments to measure knee parameters, select a prosthesis and execute a surgical plan. Despite the proven efficacy and reproducibility of conventional knee arthroplasty, and ongoing innovations in prosthetics and surgical instruments, a notable number of patients remain dissatisfied with knee arthroplasty, attributed to various known and uncertain reasons [30, 31]. The primary reason often stems from the stringent standards of TKA for prosthesis placement, lower limb reconstruction and postoperative stability, while M-TKA struggles to consistently meet these criteria [32,33,34]. RA-TKA has been developed to eliminate potential inaccuracies in implant positioning and alignment, thus mitigating patient dissatisfaction. Numerous studies have unraveled that RA-TKA results in fewer outliers in component positioning, especially in the sagittal plane, irrespective of the knee alignment and balancing techniques employed. Surgeons may balance the knee more precisely with RA-TKA than with M-TKA [35]. However, it remains to be validated whether RA-TKA can improve postoperative function recovery and deliver superior clinical efficacy compared with M-TKA. On this basis, we conducted an up-to-date systematic review and meta-analysis.
The study has demonstrated that the RA-TKA group exhibited certain advantages in improving the HKA angle, thereby enhancing the alignment accuracy of the prosthesis and reducing the deviation of the lower limb force line from the neutral position. It has been reported that maintaining the (HKA) angle within a safe range of ± 3° can increase implant survival [36]. HKA angle is a crucial factor affecting the longevity of knee prosthesis. Abnormal HKA angle following TKA may result in prosthetic knee prosthesis dislocation, early postoperative prosthesis loosening, compromised functional recovery and heightened revision rate [37, 38]. Research by Mary K. Richardson et al. indicates that patients undergoing RA-TKA have a significantly closer-to-neutral postoperative HKA angle. In addition, compared to patients treated with conventional methods, fewer RA-TKA patients experience HKA angles outside the range of 0° ± 3° [39]. Byung Sun Choil et al. have demonstrated that the RA-TKA achieves superior accuracy and precision in femoral and tibial prosthesis placement compared to M-TKA, and all X-ray measurements were reproducible. These findings uncover that RA-TKA can enhance the accuracy and repeatability of component positioning and overall limb alignment [40,41,42,43]. It is worth noting that RA-TKA demonstrated the accuracy of prosthetic positioning and the enhancement of early patient-reported outcomes [35]. However, the correlation between accurate implant positioning and clinical outcomes remains contentious. A systematic review by Bensa et al. indicates that both procedures significantly improve patients’ symptoms, with no significant difference in clinical outcomes observed between RA-TKA and M-TKA, aligning with our own findings [44]. This raises questions about whether achieving a 180° alignment is universally “normal” and whether it should be the goal of TKA for all patients. Multiple studies have found that the HKA angle deviates from 0° in the general non-arthritic population. A study by Bellemans et al. has reported a varus angle of 1° in women and 2° in men based on a study of 250 healthy adults [45]. In addition, Almaavi et al. have reported a large variation in natural knee anatomy among 4884 CT scans of the knee, with only 5% of the general population exhibiting a natural neutral alignment (HKA angle: 0°) [46]. In most patients undergoing TKA, the knee may be compelled into an unnatural position, potentially contributing to the lack of corresponding clinical outcomes despite achieving better natural neutral alignment. Given the variability of coronal knee alignment in non-osteoarthritic knees and the wide variability of all coronal alignment parameters, the necessity is underscored for a more anatomically precise and individualized approach to knee arthroplasty [47].
The FJS is a joint-specific questionnaire designed to assess a patient’s ability to “forget" about a joint issue following joint treatment. It reflects not only the difference between “good” and “bad”, but also distinguishes between “good”, “very good” and “excellent” results [48]. In this study, the RA-TKA group was found to have a superior postoperative FJS in contrast to the M-TKA group. A study by Kafelov M et al. has unveiled that RA-TKA achieved a higher FJS at 1 year postoperatively compared with M-TKA [29]. Similarly, Kaanni et al. have reported that robot-assisted total knee arthroplasty is relevant to a statistically significant improvement in FJS compared to conventional total knee arthroplasty, although these differences fail to reach a minimal clinically important difference (MCID) at any follow-up interval [28]. Therefore, further comprehensive randomized controlled trials are needed for validation. The lower ceiling effect of the FJS allows monitoring of long-term outcomes, particularly in groups that show favorable outcomes following total joint arthroplasty. Measurable clinically significant differences between RA-TKA and M-TKA may be better demonstrated in future long-term studies [40].
The setup and registration of the robotic system in RA-TKA are unique and may lead to increased total operative time [49]. This study observed that the RA-TKA group had longer operative times than the M-TKA group, possibly due to the complexity of robotic surgical steps, operator inexperience, and the longer learning curve associated with RA-TKA. The study by Xu et al. has unraveled that in RA-TKA, a significant portion of operative time is devoted to tasks such as setup, femoral and tibial fixation, and alignment [22]. Longer operative time may elevate the rate of TKA infection, causing devastating consequences of TKA [50]. This is one of the disadvantages of RA-TKA, which can be improved by reducing the time allocated to non-surgical activities. As surgeons gain proficiency and RA-TKA techniques are refined, operative times may further decrease. The change of postoperative ROM in the M-TKA group was superior than that in the RA-TKA group. However, given the variability of the results, this result should be interpreted cautiously. In the subgroup analysis of the > 6-month follow-up, it was suggested that the improvement of KSS and WOMAC scores in the M-TKA group was significantly higher than that in the RA-TKA group, indicating potential advantages of long-term outcomes for the former. Short-term follow-up results were similar between the two groups. A recent meta-analysis has revealed that short-term patient-reported outcomes (KSS and WOMAC) are improved in the RA-TKA group compared with the conventional TKA group. However, these differences do not exceed the threshold for MCID, suggesting that they may not be clinically significant [35].
Limitations of the study: firstly, not all of the included studies were RCTs (5 RCTs and 4 retrospective cohort studies); secondly, due to limited data availability, no subgroup analysis was performed for different brands of robotic assistance systems. Considering the underlying factors, the results should be interpreted cautiously and may not be applied to all systems. As robotic systems evolve, new high-quality studies are warranted to assess the latest advancements in robotic systems. Thirdly, the study was constrained by a limited number of included studies and relatively small sample sizes, potentially limiting its representativeness for the broader population. Future studies with long-term follow-up are needed to establish more definitive conclusions regarding outcomes and benefits. Despite these limitations, our study incorporated recent analyses from both prospective and retrospective cohort studies. Sensitivity analysis and subgroup analysis were used to test the stability and publication bias of the results, providing a theoretical basis for large-scale prospective clinical trials and evidence support for clinical workers’ treatment choices.
Conclusion
Our research results uncovered that the improvement of the HKA angle in the RA-TKA group was more significant than that in the M-TKA group. In terms of the operation time, improvement of ROM, KSS over 6 months and WOMAC score, M-TKA outperformed RA-TKA. The experimental follow-up time of this study was relatively short. Therefore, large-scale and well-designed clinical research with longer follow-up time is needed to comprehensively evaluate the advantages and disadvantages of the two surgical methods.
Data Availability
The data that support the findings of this study are Pubmed at 1.https://doi.org/10.7507/1002-1892.202212016;2.https://doi.org/10.1302/0301-620x.105b9.bjj-2023-0006.r3;3.https://doi.org/10.1007/s00264-018-4231-1;4.https://doi.org/10.1007/s00590-022-03274-3;5.https://doi.org/10.1055/s-0039-1684014;6.https://doi.org/10.1097/corr.0000000000000916;7.https://doi.org/10.1016/j.jot.2021.12.004;8.https://doi.org/10.1007/s00167-016-4076-3;9.https://doi.org/10.1111/os.13323;10.https://doi.org/10.1007/s00167-023-07578-7;11.https://doi.org/10.1007/s00167-023-07609-3;12.https://doi.org/10.1007/s00167-023-07426-8.
References
Maradit Kremers H et al (2015) Prevalence of total hip and knee replacement in the United States. J Bone Joint Surg Am 97(17):1386–1397
Bourne RB et al (2010) Patient satisfaction after total knee arthroplasty: who is satisfied and who is not? Clin Orthop Relat Res 468(1):57–63
Neuprez A et al (2016) Patients’ expectations impact their satisfaction following total hip or knee arthroplasty. PLoS ONE 11(12):e0167911
Oussedik S et al (2020) Alignment in total knee arthroplasty. Bone Joint J 102-b(3):276–279
Chan J et al (2020) Active robotic total knee arthroplasty (TKA): initial experience with the TSolution One ® TKA System. Surg Technol Int 37:299–305
Batailler C et al (2021) Concepts and techniques of a new robotically assisted technique for total knee arthroplasty: the ROSA knee system. Arch Orthop Trauma Surg 141(12):2049–2058
Liow MH et al (2014) Robot-assisted total knee arthroplasty accurately restores the joint line and mechanical axis. A prospective randomised study. J Arthroplasty 29(12):2373–2377
Schafer P et al (2020) Assessing knee anatomy using Makoplasty software a case series of 99 knees. J Orthop 20:347–351
Batailler C et al (2020) New technologies in knee arthroplasty: current concepts. J Clin Med 10(1):47
Sires JD, Craik JD, Wilson CJ (2021) Accuracy of bone resection in MAKO total knee robotic-assisted surgery. J Knee Surg 34(7):745–748
Li Z et al (2022) HURWA robotic-assisted total knee arthroplasty improves component positioning and alignment - A prospective randomized and multicenter study. J Orthop Translat 33:31–40
Kim YH, Yoon SH, Park JW (2020) Does Robotic-assisted TKA result in better outcome scores or long-term survivorship than conventional TKA? A randomized controlled trial. Clin Orthop Relat Res 478(2):266–275
Turan K et al (2023) A comparison of robotic-assisted and manual techniques in restricted kinematically aligned total knee arthroplasty: coronal alignment improvement with no significant clinical differences. Knee Surg Sports Traumatol Arthrosc 31(11):4673–4679
Page MJ et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Syst Rev 10(1):89
Wan X et al (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135
Luo D et al (2018) Optimally estimating the sample mean from the sample size, median, mid-range, and/or mid-quartile range. Stat Methods Med Res 27(6):1785–1805
GA Wells, et al. (2011) The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomised Studies in Meta-Analyses.
Kim SR et al (2019) Effect of red, processed, and white meat consumption on the risk of gastric cancer: an overall and dose⁻response meta-analysis. Nutrients 11(4):826
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
Egger M et al (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Clement ND et al (2023) Robotic arm-assisted versus manual (ROAM) total knee arthroplasty: a randomized controlled trial. Bone Joint J 105(9):961–970
Xu J et al (2022) Early clinical and radiographic outcomes of robot-assisted versus conventional manual total knee arthroplasty: a randomized controlled study. Orthop Surg 14(9):1972–1980
Liow MHL et al (2017) Robotic-assisted total knee arthroplasty may lead to improvement in quality-of-life measures: a 2-year follow-up of a prospective randomized trial. Knee Surg Sports Traumatol Arthrosc 25(9):2942–2951
Kenanidis E et al (2023) Comparative outcomes between a new robotically assisted and a manual technique for total knee arthroplasty in patients with osteoarthritis: a prospective matched comparative cohort study. Eur J Orthop Surg Traumatol 33(4):1231–1236
Khlopas A et al (2020) Patient-reported functional and satisfaction outcomes after robotic-arm-assisted total knee arthroplasty: early results of a prospective multicenter investigation. J Knee Surg 33(7):685–690
Cho KJ et al (2019) Robotic versus conventional primary total knee arthroplasty: clinical and radiological long-term results with a minimum follow-up of ten years. Int Orthop 43(6):1345–1354
An H et al (2023) A comparative study of short-term effectiveness of “SkyWalker” robot-assisted versus traditional total knee arthroplasty. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 37(4):404–409
Kayani B et al (2023) Robotic-arm assisted total knee arthroplasty is associated with comparable functional outcomes but improved forgotten joint scores compared with conventional manual total knee arthroplasty at five-year follow-up. Knee Surg Sports Traumatol Arthrosc 31(12):5453–5462
Kafelov M et al (2023) Functional positioning principles for image-based robotic-assisted TKA achieved a higher Forgotten Joint Score at 1 year compared to conventional TKA with restricted kinematic alignment. Knee Surg Sports Traumatol Arthrosc 31(12):5591–5602
Blum CL et al (2021) Patient expectations and satisfaction in robotic-assisted total knee arthroplasty: a prospective two-year outcome study. Arch Orthop Trauma Surg 141(12):2155–2164
Kahlenberg CA et al (2018) Patient satisfaction after total knee replacement: a systematic review. Hss J 14(2):192–201
Huang G et al (2016) Total knee arthroplasty using trochlear groove as guide for position of femoral component in severe knee osteoarthritis. BMC Surg 16(1):33
Sicat CS et al (2021) Component placement accuracy in two generations of handheld robotics-assisted knee arthroplasty. Arch Orthop Trauma Surg 141(12):2059–2067
Tan J et al (2021) Loss of knee flexion and femoral rollback of the medial-pivot and posterior-stabilized total knee arthroplasty during early-stance of walking in chinese patients. Front Bioeng Biotechnol 9:675093
Zhang J et al (2022) Robotic-arm assisted total knee arthroplasty is associated with improved accuracy and patient reported outcomes: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc 30(8):2677–2695
Vendittoli PA, Martinov S, Blakeney WG (2021) Restricted kinematic alignment, the fundamentals, and clinical applications. Front Surg 8:697020
Jeffery RS, Morris RW, Denham RA (1991) Coronal alignment after total knee replacement. J Bone Joint Surg Br 73(5):709–714
Ritter MA et al (1994) Postoperative alignment of total knee replacement. Its effect on survival. Clin Orthop Relat Res 299:153–156
Richardson MK et al (2024) Robotic-assisted total knee arthroplasty in obese patients. Arthroplast Today 26:101320
Hamilton DF et al (2017) Validation of the English language Forgotten Joint Score-12 as an outcome measure for total hip and knee arthroplasty in a British population. Bone Joint J 99-b(2):218–224
Nam CH et al (2022) Robot-assisted total knee arthroplasty improves mechanical alignment and accuracy of component positioning compared to the conventional technique. J Exp Orthop 9(1):108
Lee JH et al (2024) Functional alignment maximises advantages of robotic arm-assisted total knee arthroplasty with better patient-reported outcomes compared to mechanical alignment. Knee Surg Sports Traumatol Arthrosc 32(4):896–906
Choi BS et al (2023) Correction to: functional alignment with robotic-arm assisted total knee arthroplasty demonstrated better patient-reported outcomes than mechanical alignment with manual total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 31(3):1081
Bensa A et al (2023) Robotic-assisted mechanically aligned total knee arthroplasty does not lead to better clinical and radiological outcomes when compared to conventional TKA: a systematic review and meta-analysis of randomized controlled trials. Knee Surg Sports Traumatol Arthrosc 31(11):4680–4691
Bellemans J et al (2012) The Chitranjan Ranawat award: is neutral mechanical alignment normal for all patients? The concept of constitutional varus. Clin Orthop Relat Res 470(1):45–53
Almaawi AM et al (2017) The impact of mechanical and restricted kinematic alignment on knee anatomy in total knee arthroplasty. J Arthroplasty 32(7):2133–2140
Moser LB et al (2019) Native non-osteoarthritic knees have a highly variable coronal alignment: a systematic review. Knee Surg Sports Traumatol Arthrosc 27(5):1359–1367
Behrend H et al (2012) The “forgotten joint” as the ultimate goal in joint arthroplasty: validation of a new patient-reported outcome measure. J Arthroplasty 27(3):430-436.e1
Nogalo C et al (2023) Complications and downsides of the robotic total knee arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc 31(3):736–750
Naranje S et al (2015) Does operative time affect infection rate in primary total knee arthroplasty? Clin Orthop Relat Res 473(1):64–69
Funding
The study did not receive any specific funding from funding agencies in the public, commercial or non-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Writing—original draft preparation: XF; writing—review and editing: YS; conceptualization: GJ; methodology: ZL; formal analysis and investigation: WL; funding acquisition: RJ; resources: CL; supervision: RJ, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interests
The authors declared no competing interests.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11701_2024_2045_MOESM1_ESM.docx
Supplementary file1 (DOCX 15 KB)Table S1 Detailed search strategy in three databasesTable S2 Quality evaluation of the eligible studies with Newcastle–Ottawa scale.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Fu, X., She, Y., Jin, G. et al. Comparison of robotic-assisted total knee arthroplasty: an updated systematic review and meta-analysis. J Robotic Surg 18, 292 (2024). https://doi.org/10.1007/s11701-024-02045-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11701-024-02045-y