Abstract
Purpose
To estimate the total number of articles on traumatic brain injury (TBI)-related hypopituitarism and patients (including children and adolescents) with such disorder that were published until now, particularly after the author’s review published on April 2000.
Methods
Review of the literature retrievable on PubMed.
Results
TBI-related hypopituitarism accounts for 7.2% of the whole literature on hypopituitarism published during the 18 years and half between May 2000 and October 2018. As a result, the total number of patients with TBI-related hypopituitarism now approximates 2200. A number of patients, both adults and children, continue to be published as case reports. Articles, including reviews and guidelines, have been published in national languages in order to maximize locally the information on TBI-related hypopituitarism. TBI-related hypopituitarism has been also studied in animals (rodents, cats and dogs).
Conclusions
The interest for the damage suffered by anterior pituitary as a result of TBI continues to remain high both in the adulthood and childhood.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
This paper can be considered an update of the article [1] that appeared on December 2005 in a special issue of this journal (Brain injury-induced hypopituitarism, by G. Aimaretti and E. Ghigo). That article made the point after four fundamental reviews on post-head trauma anterior hypopituitarism, also termed traumatic brain injury (TBI)-related anterior hypopituitarism [2,3,4,5].
Impact of reference no. 5
With 20 articles, three of which being the first ones from an ad hoc study group of a National Society of Endocrinology [6,7,8], 12 reviews, and the first consensus guideline [9] that were published after May 2000 and prior to the said 2005 special issue of Pituitary, the review of Benvenga et al. published on April 2000 [5] clearly generated much interest on the endocrine consequences of head trauma as a result of the damaged secretion of one or more adenohypophyseal hormones. Illustrative examples of the value attributed to that review [5] by other authors [10,11,12,13,14,15,16,17,18] are given in Table 1. In contrast, over the threefold longer period of time between the April 2000 review [5] and the September 1986 review [4], only 11 articles and one short review in Japanese [19] were published. As summarized in the subsequent paragraph, the review of April 2000 [5] was followed by decreased attention on the damaged secretion of the antidiuretic hormone (ADH) secretion in favor of increased attention on the damaged secretion of the anterior pituitary hormones.
After the review of April 2000 [5] and through October 16, 2018, 326 items (81/326 [24.8%] being reviews) were retrieved in PubMed upon entering the string “head trauma AND hypopituitarism”, while 4495 items were retrieved upon searching for “hypopituitarism”. Thus, TBI-related hypopituitarism accounts for 7.2% of the whole literature on hypopituitarism published during the 18 years and half between May 2000 and October 2018. By comparison, the corresponding proportion for the 100 years between January 1900 and April 2000 was 1.5% (90/6117).
In contrast, only 159 items (38/159 [23.9%] being reviews) were retrieved upon entering the string “head trauma AND diabetes indipidus”. The situation was the opposite prior to April 2000, with 88 items (5/88 [5.7%] being reviews) related to the search on “head trauma AND hypopituitarism”, as compared to 188 items (9/188 [4.8%] being reviews) related to the search on “head trauma AND diabetes indipidus”. Of the mentioned 81 reviews that were published between April 2000 and October 2018, 19 (23.5%) appeared in the year 2005. Twelve reviews were published in national languages (viz. French, Spanish, Czech, Hungarian, Polish, Danish, Swedish and Japanese) [20,21,22,23,24,25,26,27,28,29,30,31], indicating the intention to maximize locally the information on TBI-related hypopituitarism.
Further to the papers by the study group of the Italian Society of Endocrinology [6,7,8], only after the 2000 review [5] there were studies from other national societies or studies based on national databases [32,33,34,35,36,37,38,39,40,41,42,43,44]. The aforementioned first consensus guideline [9] was followed by other guidelines or recommendations at either national or international level [29, 33, 45,46,47].
After the 367 patients in the literature reported up to the April 2000 review [5], another approximately 1800 patients with post-TBI hypopituitarism could be retrieved in the liteature retrievable on PubMed search as of October 16, 2018 [string entered “head trauma AND hypopituitarism”]. Thus, the total number of such patients becomes almost 2200. Of these, 32 patients (1.5%) were described as case reports, with 5/32 being children or adolescents.
Before moving to the next section, which deals with particular forms of TBI-related hypothyroidism [34, 48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71], including animals [72,73,74,75,76,77,78,79], it is appropriate to remind the importance of some original papers [80,81,82,83,84] whose messages were echoed in some reviews [85,86,87,88,89]. These articles are worthy of note because have focussed on the decreased quality of life of patients with TBI-related hypopituitarism, including impairment of cognitive, behavioral, neuropsychological and even cardiorespiratory fitness. These consequences were essentially the results of a more or less severe GH deficiency, and could be managed by appropriate GH replacement therapy. Another article [89] has historical value for the setting of the screening for TBI-related hypopituitarism (that is, subjects recruited from a community-based postacute residential rehabilitation facility for patients with a history of acquired brain injury), and having detected an unexpectedly high frequency of central hypothyroidism (approximately one in ten patients) or, as shown by serum concentration of both TSH and free T4 levels below the corresponding midnormal levels, high frequency of subtle disturbance of the hypothalamus-pituitary thyroid axis (approximately nine in ten patients).
Particular forms of TBI-related hypopituitarism
Children and adolescents
Of the 81 reviews published between April 2000 [5] and through October 16, 2018, 11 (13.6%) concerned children and adolescents [48,49,50,51,52,53,54,55,56,57,58].
The review by Acerini et al. in 2006 [49] collected a total of 20 patients in whom TBI had occurred in the pediatric age (0.1–16 years), 1–42 years before the diagnosis of post-head trauma hypopituitarism. With three exceptions (interval between TBI and diagnosis = 22–42 years), in the remaining 17 patients the diagnosis occurred in the pediatric age. These 20 patients were published in 10 papers. Four papers, which described six children/adolescents, were published prior to the Edwards and Blake review [4], precisely between 1976 and 1980; five papers, which reported another six chidren/adolescents, were published between that review [4] and the review by Benvenga et al. [5]. The remaining paper, which also described 4 patients with TBI in childhood/adolescence, was published in 2004 [59]. It should be noted that the Acerini et al. review [49] missed two children/adolescents with isolated or multiple pituitary hormone deficiencies following TBI [60, 61].
After the 2000 review [5], there were another 74 cases of post-TBI hypopituitarism with this diagnosis made, and trauma occurred in the pediatric age; these cases were reported in 15 papers. Based on the Acerini et al. review [49], the frequencies of hormone deficiencies were: 55% for ACTH, 80% for FSH/LH, 85% for GH, and 75% for TSH. Based on the review by Soliman et al. [57], rates were 2–43% for ACTH, 6–16% for FSH/LH, 6–48% for GH, and 2–33% for TSH. In the same review, the corresponding frequencies reported for adults were 1–60%, 2.2–41%, 2–37.5%, and 2.2–22% [57].
Sports
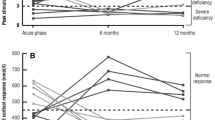
Only after the 2000 review [5], with its Table 1 summarizing 2 of the 15 patients from the personal experience having had TBI-related hypopituitarism after diving, sports were investigated in more detail, though the interest was for the contact/combative types. The first paper was published in 2004 [62]. The study concerned 11 actively competing or retired male boxers with a mean age of 38.0 ± 3.6 years and seven age-, sex- and BMI-matched healthy non-boxing controls. Peak GH levels in 5 (45%) boxers were found to be lower than 10 µg/L and considered as severe GH deficient. Mean IGF-1 levels (367 ± 18.8 ng/ml) were significantly lower than in controls (237 ± 23.3 vs. 367 ± 18.8 ng/ml). All the other pituitary hormones were normal, including ADH. Other original articles or reviews from the same Turkish group appeared subsequently [63,64,65,66], including the most recent review on hypopitutarism subsequent to sports-related TBI [66]. It was in the setting of sports-related hypopituitarism that an autoimmune pathogenesis was elaborated [67]. In a total of 61 male boxers (competing, n = 44; retired, n = 17; mean age = 26 years, range 17–53) and 60 controls, serum anti-hypothalamus antibodies (AHAs) and anti-pituitary antibodies (APAs) were measured. AHAs were detected in 13 of 61 boxers (21.3%), and APAs were detected in 14 of 61 boxers (22.9%), but in none of the normal controls. Pituitary dysfunction was significantly higher in AHA-positive boxers than in AHA-negative boxers (46.2% vs. 10.4%) [67].
Blast
Only after the 2000 review [5], which reminded of bullets and explosions as the causes of TBI-related hypopituitarism in approximately 5% of the 147 cases of TBI-related hypopituitarism of the literature in whom a cause could be identified, the first paper dealing with hypopituitarism occurring after blast exposure did appear in the literature [68]. This paper from USA was soon followed by a paper from England [34], both evaluating individuals who had suffered TBI at least 1 year earlier. Worthy-of-note, in the year 2010, endocrinologists at the Walter Reed Army Medical Center in Washington, DC, USA, alerted that there were no data on TBI-related hypopituitarism in the military population, and that combat veterans could be at risk [69]. Two years earlier (April, 2008), not so far from Washington, DC, the National Institutes of Health convened a workshop [70]. A multidisciplinary group of neuroscientists, engineers, and clinicians were invited to share insights on blast-induced traumatic brain injury (bTBI), specifically pertaining to: physics of blast explosions, acute clinical observations and treatments, preclinical and computational models, and lessons from the international community on civilian exposures. Of interest, endocrine consequences of bTBI were totally ignored, with not a single citation among the 70 papers appearing in the bibliography.
The American paper evaluated 26 male veterans of combat in Iraq or Afghanistan who had reported experiencing at least one blast exposure in the war zone [68]. The control group consisted of seven veterans of deployment to Iraq and/or Afghanistan who did not experience blast trauma. The authors found that 42% of the 26 blast-exposed veterans, but none of the control veterans, had anterior pituitary hypofunction involving one or more hormones. In another paper by the same research team on a larger number of veterans [71], 12 of 39 veterans (31%) in the study group and 3 of 20 (15%) in the control group had pituitary dysfunction.
The English paper included 19 male soldiers who had suffered moderate to severe brain injury caused directly by a single exposure to a blast between December 2009 and March 2012, and who were considered representative of the 183 UK soldiers who had survived a moderate to severe blast TBI in Afghanistan during this 27-month period [34]. The control group consisted of 39 patients after nonblastTBI. This represented all the patients seen in our multidisciplinary Traumatic Brain Injury clinic at Charing Cross Hospital, London, United Kingdom between August 2009 and March 2012. In this study [34], the rate of anterior pituitary dysfunction was 32% in the study group, significantly more than the 2.6% rate in the control group. No hypothalamic–pituitary abnormalities were seen on MRI brain scans in any soldiers in the blast TBI group [34], a neuroradiological evaluation that was not performed in the American study [68].
Animals
Studies were conducted in mice [72], rats [73,74,75], cats [76, 77], and dogs [78, 79]. The studies in male rodents showed impaired GH secretion and, when investigated [75], gonadotropin secretion. At a mechanistic level, repeated brain trauma caused vascular permeability of the pituitary gland [74], chronic inflammation of the pituitary and hypothalamus [73]. Furthermore, the distributions of claudin-1 and zonula occludens-1 between tanycytes in the median eminence were disorganized, suggesting tight junction disruptions [72].
The case reports in cats showed diabetes insipidus and central hypothyroidism, with the additional presence of hypocortisolism and low levels of IGF-1 in one of the two felines [76], while the canine case report described isolated hypocortisolism [78]. The retrospective study on 17 dogs referred to four centers for non-fatal TBI showed this order of frequency for deficiencies of these anterior pituitary axes: 41% (GH/IGF-1), 23% (TSH/T4), 12% (ACTH/cortisol) [79].
Conclusions
The interest for the damage suffered by the anterior pituitary gland as a result of TBI continues to remain high both in the adulthood and childhood, clearly outnumbering the interest for the damage suffered by the posterior pituitary.
References
Benvenga S (2005) Brain injury and hypopituitarism: the historical background. Pituitary 8:193–195
Escamilla RF, Lisser H (1942) Simmonds disease. J Clin Endocrinol 2:65–96
Altman R, Pruzanski W (1961) Post-traumatic hypopituitarism. Ann Intern Med 55:149–154
Edwards OM, Clark JDA (1986) Post-traumatic hypopituitarism. Six cases and review of the literature. Medicine (Baltimore) 65:281–290
Benvenga S, Campennì A, Ruggeri RM, Trimarchi F (2000) Hypopituitarism secondary to head trauma. J Clin Endocrinol Metab 85:1353–1361
Aimaretti G, Ambrosio MR, Di Somma C, Fusco A, Cannavò S, Gasperi M, Scaroni C, De Marinis L, Benvenga S, degli Uberti EC, Lombardi G, Mantero F, Martino E, Giordano G, Ghigo E (2004) Traumatic brain injury and subarachnoid haemorrhage are conditions at high risk for hypopituitarism: screening study at 3 months after the brain injury. Clin Endocrinol (Oxf) 61:320–326
Aimaretti G, Ambrosio MR, Benvenga S, Borretta G, De Marinis L, De Menis E, Di Somma C, Faustini-Fustini M, Grottoli S, Gasco V, Gasperi M, Logoluso F, Scaroni C, Giordano G, Ghigo E, Italian Society of Endocrinology (2004) Hypopituitarism and growth hormone deficiency (GHD) after traumatic brain injury (TBI). Growth Horm IGF Res 14(Suppl A): S114–S117
Aimaretti G, Ambrosio MR, Di Somma C, Gasperi M, Cannavò S, Scaroni C, Fusco A, Del Monte P, De Menis E, Faustini-Fustini M, Grimaldi F, Logoluso F, Razzore P, Rovere S, Benvenga S, Degli Uberti EC, De Marinis L, Lombardi G, Mantero F, Martino E, Giordano G, Ghigo E (2005) Residual pituitary function after brain injury-induced hypopituitarism: a prospective 12-month study. J Clin Endocrinol Metab 90:6085–6092
Ghigo E, Masel B, Aimaretti G, Léon-Carrión J, Casanueva FF, Dominguez-Morales MR, Elovic E, Perrone K, Stalla G, Thompson C, Urban R (2005) Consensus guidelines on screening for hypopituitarism following traumatic brain injury. Brain Inj 19:711–724
Aimaretti G, Ghigo E (2005) Traumatic brain injury and hypopituitarism. Sci World J 5:777–781
Medic-Stojanoska M, Pekic S, Curic N, Djilas-Ivanovic D, Popovic V (2005) Evolving hypopituitarism as a consequence of traumatic brain injury (TBI) in childhood—call for attention. Endocrine 31:268–271
Maiya B, Newcombe V, Nortje J, Bradley P, Bernard F, Chatfield D, Outtrim J, Hutchinson P, Matta B, Antoun N, Menon D (2008) Magnetic resonance imaging changes in the pituitary gland following acute traumatic brain injury. Intensive Care Med 34:468–475
Hohl A, Mazzuco TL, Coral MH, Schwarzbold M, Walz R (2009) Hypogonadism after traumatic brain injury. Arq Bras Endocrinol Metab 53:908–914
Heather N, Cutfield W (2011) Traumatic brain injury: is the pituitary out of harm’s way? J Pediatr 159:686–690
Javed Z, Qamar U, Sathyapalan T (2015) Pituitary and/or hypothalamic dysfunction following moderate to severe traumatic brain injury: current perspectives. Indian J Endocrinol Metab 19:753–763
Scranton RA, Baskin DS (2015) Impaired pituitary axes following traumatic brain injury. J Clin Med 4:1463–1479
Tanrivedi F, Kelestimur F (2015) Neuroendocrine disturbances after brain damage: an important and often undiagnosed disorder. J Clin Med 4:847–857
Reifschneider K, Auble BA, Rose SR (2015) Update of endocrine dysfunction following pediatric traumatic brain injury. J Clin Med 4:1536–1560
Itabashi A, Ishii J (1993) Post-traumatic hypopituitarism. Ryoikibetsu Shokogun Shirizu 1:58–61
Lecoq AL, Chanson P (2015) Hypopituitarism following traumatic brain injury: diagnostic and therapeutic issues. Ann Endocrinol (Paris) 76(6 Suppl 1):S10–S18
Ciancia S (2012) Pituitary insufficiency after traumatic brain injury: consequences? screening? Ann. Fr Anesth Reanim 31:e117–e124
Valdes-Socin H, Vroonen L, Robe P, Martin D, Beckers A (2009) Traumatic brain injury and subarachnoid hemorrhage as a cause of hypopituitarism: a review. Rev Med Liege 64:457–463
Belmont A, Agar N, Hugeron C, Gallais B, Azouvi P (2006) Fatigue and traumatic brain injury. Ann Readapt Med Phys 49:283–288
Obiols Alfonso G (2012) Impact of head trauma on pituitary function. Endocrinol Nutr 59:505–515
Cáp J (2006) Hormonal diseases after traumatic brain injury. Vnitr Lek 52:941–946
Czirják S, Rácz K, Góth M (2012) Neuroendocrine dysfunctions and their consequences following traumatic brain injury. Orv Hetil 153:927–933
Krysiak R, Okopień B (2012) Pituitary disorders in patients after traumatic brain injury and radiotherapy. Wiad Lek 65:174–186
Klose MC, Juul A, Poulsgaard L, Kosteljanetz M, Brennum J, Feldt-Rasmussen UF (2007) Pituitary insufficiency following head trauma. Ugeskr Laeger 169:211–213
Rosén T, Burman P, Dahlqvist P, Dahm P, Edén-Engström B, Ekman B, Höybye C, Jakobsson KE, Koskinen LO, Tölli A, Valdemarsson S, Ulfarsson T (2012) Traumatic brain injury can cause pituitary deficiency. Suggestions for guidelines for assessment of pituitary function. Lakartidningen 109:629–632
Suzuki H, Kawakita F, Liu L, Nakano F (2015) Delayed brain injury after aneurysmal subarachnoid hemorrhage: update and perspective. No Shinkei Geka 43:869–877
Arita K, Hirano H, Tominaga A, Kurisu K (2008) Diagnosis and treatment of adult growth hormone deficiency (aGHD) resulting from brain injury—role of aGHD. Brain Nerve 60:1445–1454
Gardner CJ, Mattsson AF, Daousi C, Korbonits M, Koltowska-Haggstrom M, Cuthbertson DJ (2015) GH deficiency after traumatic brain injury: improvement in quality of life with GH therapy: analysis of the KIMS database. Eur J Endocrinol 172:371–381
Tan CL, Alavi SA, Baldeweg SE, Belli A, Carson A, Feeney C, Goldstone AP, Greenwood R, Menon DK, Simpson HL, Toogood AA, Gurnell M, Hutchinson PJ (2017) The screening and management of pituitary dysfunction following traumatic brain injury in adults: British Neurotrauma Group guidance. J Neurol Neurosurg Psychiatry 88:971–981
Baxter D, Sharp DJ, Feeney C, Papadopoulou D, Ham TE, Jilka S, Hellyer PJ, Patel MC, Bennett AN, Mistlin A, McGilloway E, Midwinter M, Goldstone AP (2013) Pituitary dysfunction after blast traumatic brain injury: the UK BIOSAP study. Ann Neurol 74:527–536
Krewer C, Schneider M, Schneider HJ, Kreitschmann-Andermahr I, Buchfelder M, Faust M, Berg C, Wallaschofski H, Renner C, Uhl E, Koenig E, Jordan M, Stalla GK, Kopczak A (2016) Neuroendocrine disturbances one to five or more years after traumatic brain injury and aneurysmal subarachnoid hemorrhage: data from the German database on hypopituitarism. J Neurotrauma 33:1544–1553
Renner C, Hummelsheim H, Kopczak A, Steube D, Schneider HJ, Schneider M, Kreitschmann-Andermahr I, Jordan M, Uhl E, Stalla GK (2012) The influence of gender on the injury severity, course and outcome of traumatic brain injury. Brain Inj 26:1360–1371
Schneider HJ, Schneider M, Kreitschmann-Andermahr I, Tuschy U, Wallaschofski H, Fleck S, Faust M, Renner CI, Kopczak A, Saller B, Buchfelder M, Jordan M, Stalla GK (2011) Structured assessment of hypopituitarism after traumatic brain injury and aneurysmal subarachnoid hemorrhage in 1242 patients: the German interdisciplinary database. J Neurotrauma 28:1693–1698
Kreitschmann-Andermahr I, Hartmann Y, Poll E, Schneider HJ, Buchfelder M, Stalla GK (2011) The German database on hypopituitarism after traumatic brain injury and aneurysmal subarachnoid hemorrhage—description, objectives and design. Exp Clin Endocrinol Diabetes 119:15–20
Berg C, Oeffner A, Schumm-Draeger PM, Badorrek F, Brabant G, Gerbert B, Bornstein S, Zimmermann A, Weber M, Broecker-Preuss M, Mann K, Herrmann BL (2010) Prevalence of anterior pituitary dysfunction in patients following traumatic brain injury in a German multi-centre screening program. Exp Clin Endocrinol Diabetes 118:139–144
Kreitschmann-Andermahr I, Poll EM, Reineke A, Gilsbach JM, Brabant G, Buchfelder M, Fassbender W, Faust M, Kann PH, Wallaschofski H (2008) Growth hormone deficient patients after traumatic brain injury—baseline characteristics and benefits after growth hormone replacement—an analysis of the German KIMS database. Growth Horm IGF Res 18:472–478
Klose M, Stochholm K, Janukonyté J, Christensen LL, Cohen AS, Wagner A, Laurberg P, Christiansen JS, Andersen M, Feldt-Rasmussen U (2015) Patient reported outcome in posttraumatic pituitary deficiency: results from The Danish National Study on posttraumatic hypopituitarism. Eur J Endocrinol 172:753–762
Klose M, Stochholm K, Janukonyté J, Lehman Christensen L, Frystyk J, Andersen M, Laurberg P, Christiansen JS, Feldt-Rasmussen U (2014) Prevalence of posttraumatic growth hormone deficiency is highly dependent on the diagnostic set-up: results from The Danish National Study on Posttraumatic Hypopituitarism. J Clin Endocrinol Metab 99:101–110
Kokshoorn NE, Smit JW, Nieuwlaat WA, Tiemensma J, Bisschop PH, Groote Veldman R, Roelfsema F, Franken AA, Wassenaar MJ, Biermasz NR, Romijn JA, Pereira AM (2011) Low prevalence of hypopituitarism after traumatic brain injury: a multicenter study. Eur J Endocrinol 165:225–231
Leal-Cerro A, Dolores Rincón M, Puig Domingo M (2010) Grupo de Trabajo de Disfunción Neuroendocrina y Agresión Cerebral; Sociedad Española de Endocrinología y Nutrición (SEEN). Brain damage by trauma and hypopituitarism. Med Clin (Barc) 134:127–133
Leal-Cerro A, Rincón MD, Domingo MP (2009) Grupo de Trabajo de Disfunción Neuroendocrina y agresión Cerebral de la Sociedad Española de Endocrinología y Nutrición (SEEN). Neuroendocrine dysfunction and brain damage. A consensus statement. Endocrinol Nutr 56:293–302
Casanueva FF, Ghigo E, Popovic V, Athens TBI, Hypopituitarism Study Group (2004) Hypopituitarism following traumatic brain injury (TBI): a guideline decalogue. J Endocrinol Investig 27:793–795. (Erratum in: J. Endocrinol. Invest. 28, 299 (2005))
Tritos NA, Yuen KC, Kelly DF, AACE Neuroendocrine and Pituitary Scientific Committee (2015) American Association of Clinical Endocrinologists and American College of Endocrinology Disease State Clinical Review: A neuroendocrine approach to patients with traumatic brain injury. Endocr Pract 21:823–831
Baldelli R, Bellone S, Corneli G, Savastio S, Petri A, Bona G (2005) Traumatic brain injury-induced hypopituitarism in adolescence. Pituitary 8:255–257
Acerini CL, Tasker RC, Bellone S, Bona G, Thompson CJ, Savage MO (2006) Hypopituitarism in childhood and adolescence following traumatic brain injury: the case for prospective endocrine investigation. Eur J Endocrinol 155:663–669
Acerini CL, Tasker RC (2007) Endocrine sequelae of traumatic brain injury in childhood. Horm Res 68(Suppl 5):14–17
Acerini CL, Tasker RC (2007) Traumatic brain injury induced hypothalamic-pituitary dysfunction: a paediatric perspective. Pituitary 10:373–380
Einaudi S, Bondone C (2007) The effects of head trauma on hypothalamic-pituitary function in children and adolescents. Curr Opin Pediatr 19:465–470
Schneider HJ, Corneli G, Kreitschman-Andermahr I, Rovere S, Bellone S, Bona G, Ghigo E, Aimaretti G (2007) Traumatic brain injury and hypopituitarism in children and adolescents: is the problem under-estimated? Pediatr. Endocrinol Rev 4:205–209
De Sanctis V, Sprocati M, Govoni MR, Raiola G (2008) Assessment of traumatic brain injury and anterior pituitary dysfunction in adolescents. Georgian Med News 156:18–23
Rose SR, Auble BA (2012) Endocrine changes after pediatric traumatic brain injury. Pituitary 15:267–275
Richmond E, Rogol AD (2014) Traumatic brain injury: endocrine consequences in children and adults. Endocrine 45:3–8
Soliman AT, Adel A, Soliman NA, Elalaily R, De Sanctis V (2015) Pituitary deficinecy following traumatic brain injury in early childhood: a review of the literature. Georgian Med News 244–245:62–71
Casano-Sancho P (2017) Pituitary dysfunction after traumatic brain injury: are there definitive data in children? Arch Dis Child 102:572–577
Benvenga S, Vigo R, Ruggeri RM, Lapa D, Almoto D, Lo Giudice F, Longo M, Blandino A, Campenni A, Cannavo S, Trimarchi F (2004) Severe head trauma in patients with unexplained central hypothyroidism. Am J Med 116:767–771
Lopez Guzman A, Salvador J, Albero R, Sastre J, Iglesias P, Diez JJ, Gomez-Pan A (1992) Selective growth hormone deficiency of hypothalamic origin following severe head injury. Acta Paediatr 81:698–699
Lim HS, Ang BK, Ngim RC (1990) Hypopituitarism following head injury—a case report. Ann Acad Med Singapore 19:851–855
Kelestimur F, Tanriverdi F, Atmaca H, Unluhizarci K, Selcuklu A, Casanueva FF (2004) Boxing as a sport activity associated with isolated GH deficiency. J Endocrinol Investig 27:RC28–R32
Keleştimur F (2005) Chronic trauma in sports as a cause of hypopituitarism. Pituitary 8:259–262
Tanriverdi F, Unluhizarci K, Coksevim B, Selcuklu A, Casanueva FF, Kelestimur F (2007) Kickboxing sport as a new cause of traumatic brain injury-mediated hypopituitarism. Clin Endocrinol (Oxf) 266:360–366
Tanriverdi F, Unluhizarci K, Karaca Z, Casanueva FF, Kelestimur F (2010) Hypopituitarism due to sports related head trauma and the effects of growth hormone replacement in retired amateur boxers. Pituitary 13:111–114
Sezgin Caglar A, Tanriverdi F, Karaca Z, Unluhizarci K, Kelestimur F (2018) Sports related repetitive head trauma: a novel cause of pituitary dysfunction. J Neurotrauma. https://doi.org/10.1089/neu.2018.5751
Tanriverdi F, De Bellis A, Battaglia M, Bellastella G, Bizzarro A, Sinisi AA, Bellastella A, Unluhizarci K, Selcuklu A, Casanueva FF, Kelestimur F (2010) Investigation of antihypothalamus and antipituitary antibodies in amateur boxers: is chronic repetitive head trauma-induced pituitary dysfunction associated with autoimmunity? Eur J Endocrinol 162:861–867
Wilkinson CW, Pagulayan KF, Petrie EC, Mayer CL, Colasurdo EA, Shofer JB, Hart KL, Hoff D, Tarabochia MA, Peskind ER (2012) High prevalence of chronic pituitary and target-organ hormone abnormalities after blast-related mild traumatic brain injury. Front Neurol 3:11
Guerrero AF, Alfonso A (2010) Traumatic brain injury-related hypopituitarism: a review and recommendations for screening combat veterans. Mil Med 175:574–580
Hicks RR, Fertig SJ, Desrocher RE, Koroshetz WJ, Pancrazio JJ (2010) Neurological effects of blast injury. J Trauma 68:1257–1263
Undurti A, Colasurdo EA, Sikkema CL, Schultz JS, Peskind ER, Pagulayan KF, Wilkinson CW (2018) Chronic hypopituitarism associated with increased postconcussive symptoms is prevalent after blast-induced mild traumatic brain injury. Front Neurol 9:72
Osterstock G, El Yandouzi T, Romanò N, Carmignac D, Langlet F, Coutry N, Guillou A, Schaeffer M, Chauvet N, Vanacker C, Galibert E, Dehouck B, Robinson IC, Prévot V, Mollard P, Plesnila N, Méry PF (2014) Sustained alterations of hypothalamic tanycytes during posttraumatic hypopituitarism in male mice. Endocrinology 155:1887–1898
Kasturi BS, Stein DG (2009) Traumatic brain injury causes long-term reduction in serum growth hormone and persistent astrocytosis in the cortico-hypothalamo-pituitary axis of adult male rats. J Neurotrauma 26:1315–1324
Greco T, Hovda D, Prins M (2013) The effects of repeat traumatic brain injury on the pituitary in adolescent rats. J Neurotrauma 30:1983–1990
Greco T, Hovda DA, Prins ML (2015) Adolescent TBI-induced hypopituitarism causes sexual dysfunction in adult male rats. Dev Neurobiol 75:193–202
Smith JR, Elwood CMJ (2004) Traumatic partial hypopituitarism in a cat. Small Anim Pract 45:405–409
Mellanby RJ, Jeffery ND, Gopal MS, Herrtage ME (2005) Secondary hypothyroidism following head trauma in a cat. J Feline Med Surg 7:135–139
Platt SR, Chrisman CL, Graham J, Clemmons RM (1999) Secondary hypoadrenocorticism associated with craniocerebral trauma in a dog. J Am Anim Hosp Assoc 35:117–122
Murtagh K, Arrol L, Goncalves R, Granger N, German AJ, Smith PM (2015) Hypothalamic-anterior pituitary hormone deficiencies following traumatic brain injury in dogs. Vet Rec 176:20
Kelly DF, McArthur DL, Levin H, Swimmer S, Dusick JR, Cohan P, Wang C, Swerdloff R (2006) Neurobehavioral and quality of life changes associated with growth hormone insufficiency after complicated mild, moderate, or severe traumatic brain injury. J Neurotrauma 23:928–942
Bavisetty S, Bavisetty S, McArthur DL, Dusick JR, Wang C, Cohan P, Boscardin WJ, Swerdloff R, Levin H, Chang DJ, Muizelaar JP, Kelly DF (2008) Chronic hypopituitarism after traumatic brain injury: risk assessment and relationship to outcome. Neurosurgery 62:1080–1093 (discussion 1093–1094. Erratum in: Neurosurgery. 63, 683. Bavisetty, Supriya [added])
High WM Jr, Briones-Galang M, Clark JA, Gilkison C, Mossberg KA, Zgaljardic DJ, Masel BE, Urban RJ (2015) Effect of growth hormone replacement therapy on cognition after traumatic brain injury. J Neurotrauma 27:1565–1575
Englander J, Bushnik T, Oggins J, Katznelson L (2010) Fatigue after traumatic brain injury: association with neuroendocrine, sleep, depression and other factors. Brain Inj 24:1379–1388
Mossberg KA, Durham WJ, Zgaljardic DJ, Gilkison CR, Danesi CP, Sheffield-Moore M, Masel BE, Urban RJ (2017) Functional changes after recombinant human growth hormone replacement in patients with chronic traumatic brain injury and abnormal growth hormone secretion. J Neurotrauma 34:845–852
Agha A, Phillips J, Thompson CJ (2007) Hypopituitarism following traumatic brain injury (TBI). Br J Neurosurg 21:210–216
Zgaljardic DJ, Durham WJ, Mossberg KA, Foreman J, Joshipura K, Masel BE, Urban R, Sheffield-Moore M (2014) Neuropsychological and physiological correlates of fatigue following traumatic brain injury. Brain Inj 28:389–397
Masel BE, Urban R (2015) Chronic endocrinopathies in traumatic brain injury disease. J Neurotrauma 32:1902–1910
Masel BE, Zgaljardic DJ, Forman J (2017) Post-traumatic hypopituitarism and fatigue. Neuropsychol Rehabil 27:1071–1079
Lieberman SA, Oberoi AL, Gilkison CR, Masel BE, Urban RJ (2001) Prevalence of neuroendocrine dysfunction in patients recovering from traumatic brain injury. J Clin Endocrinol Metab 86:2752–2756
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Benvenga, S. The history of pituitary dysfunction after traumatic brain injury. Pituitary 22, 229–235 (2019). https://doi.org/10.1007/s11102-019-00949-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-019-00949-9