Abstract
Radioimmunoassay (RIA) for C-reactive protein (CRP) is a clinical tool to quantify CRP, a cardiovascular diseases (CVDs) marker, in human serum. Development of the Radioimmunoassay includes radioiodination of CRP with 125I radioisotope, where radioiodination is conducted following the Chloramine-T method. The present study standardizes the radiolabeling procedure and key reagent concentrations like chloramine-T (oxidizing reagent), sodium metabisulfite, and potassium iodide. The outcome of the standardized radioiodination includes a reaction time of 60 s, iodination analytical parameters like % Radiochemical purity was ~ 97% with specific activity ~ 17 µCi/µg, and the tracer was stable for the 60 days. The optimized radioiodination method is simple, reproducible, and has high tracer stability with high immunoreactivity to develop an RIA procedure to quantify CRP in human serum.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
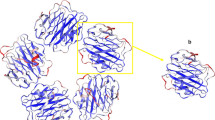
C-reactive protein (CRP), discovered in 1930 by Tillett and Francis while working with Streptococcus pneumoniae [1], is an annular (ring-shaped) pentraxin family protein always present in trace amounts (> 0.8 mg/L) in the blood [2, 3]. CRP is synthesized in the liver and dumped into the blood [4]. Usually, the concentration of CRP varies in serum from 1 to 500 mg/L; however, the concentration increases in abnormal physiological conditions [5, 6]. Normal CRP level in serum is always maintained at less than 1 mg/L. In acute inflammation, CRP concentration elevates up to 100 mg/L [7]. Various reports note that CRP is a potent cardiovascular disease (CVD) marker [8]. Scientific publications report the association between CRP level and relative CVDs risk; 1 mg/L indicates low CVDs risk, 2–3 mg/L indicates moderate risk, and more than 3 mg/L indicates high risk for the future [9,10,11]. In-vitro CRP analysis has clinical importance for early risk management of CVDs. Clinical CRP analysis is carried out by insensitive assays, which cannot achieve sensitive detection [10]. Therefore, antibody-based immunoassay methods are preferred because of their high sensitivity to overcome the challenges of insensitive assays [12, 13].
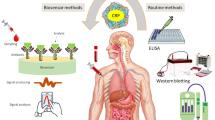
Radioimmunoassay is one of the sensitive antibody-based immunoassay methods that can be used for CRP clinical analysis. The Radioimmunoassay (RIA) method is used to measure trace concentrations of protein from complex biological samples [14]. In radioimmunoassay, iodine radioisotope (125I), which has a half-life of nearly 60 days, is labelled to the analyte’s tyrosine/histidine amino acid residues [15]. The process of 125I labelling of analyte/antibody is known as radioiodination. The labelled molecules are used as a radiolabeled tracer [16].
Various methods have been described for the radioiodination of the protein, but the Chloramine-T method has been widely accepted in various published iodination procedures [15, 17, 18]. Simplicity and reproducibility make this method more popular than others. Standardization of the iodination procedure includes the radiolabeling, purification, and validation of the purified radiolabeled protein [19]. In the present study, the radiolabeling procedure for CRP was standardized using chloramine-T as an oxidizing agent to develop an RIA procedure to quantify CRP in human serum.
Experimental
Materials
Human C-reactive protein (CAS 9007-41-4, purity ≥ 99% Sigma, purified from human serum), anti-human C-reactive protein polyclonal antibodies (CAS-C3527, Sigma, raised in rabbit) Bovine serum albumin (BSA), Chloramine-T (Sodium chloro(4-methylbenzene-1-sulfonyl)azanide) and Sodium metabisulfite (MBS) (procured from Sigma, USA), magnetizable cellulose particles for the separation system (prepared in Board of Radiation and Isotope Technology (BRIT), Indian Patent No. 193445), Na125I for labelling (obtained from Bhabha Atomic Research Centre (BARC), Mumbai, India), Sephadex G-25 (purchased from Pharmacia Fine Chemicals Company, Sweden), Di-hydrogen phosphate and hydrogen Di-phosphate of AR grade and Bovine serum for standard preparation (procured from HiMedia, India), Whatman 3 mm chromatography paper (obtained from Whatman Limited, England).
Radioiodination of C-reactive protein
CRP was radiolabeled using the most adopted method proposed by Hunter and Greenwood in 1962 [20]. Radioiodination of a protein or biomolecule needs the presence of an aromatic moiety—tyrosine or histidine. The present study follows the chloramine-T radioiodination protocol with minor modifications. In a typical radioiodine labelling procedure (Scheme 1), 10 µL of C-reactive protein (40 µg in 0.05 M phosphate buffer pH, 7.4) was mixed with 860 µCi of 125I in the form of Na 125I. The oxidation reaction was initiated by adding 10 µL chloramine-T (Stock solution-1 mg was diluted in 1 mL of 0.05 M phosphate buffer, pH 7.4). The oxidation reaction was allowed to proceed for 60 s, then terminated by adding a reducing agent, sodium metabisulfite (MBS) 20 µL (Stock Solution—4 mg was diluted in 1 mL of 0.05 M phosphate buffer pH, 7.4). Potassium iodide 50 µL (Stock solution—2 mg diluted in 1 mL of 0.05 M phosphate buffer pH 7.4) was added after the termination of the oxidation reaction.
The labelled product was purified by gel filtration using a Sephadex G-25 column. The specific activity of the labelled protein was calculated after radiolabeling using % radioiodination yield. The mean specific activity of radiolabeled CRP was determined with repeated iodination results.
Purification of the 125I-C-reactive protein
Purification of the radiolabeled CRP and free iodide is a crucial step. To purify the radiolabeled CRP and free iodide, 8 g of Sephadex G-25 was soaked a day before iodination in 200 mL of 0.05 M phosphate buffer, pH 7.4. Soaked Sephadex G-25 was loaded onto a chromatography column of size 1 cm × 30 cm. The column was filled with the prior soaked Sephadex G-25, and the elution buffer (0.05 M phosphate buffer) was passed continuously. Then, a 2 mL saturated solution of BSA (⁓ 80 mg/mL in 0.05 M phosphate buffer, pH 7.4) was passed through the column to saturate all the adsorption sites on the Sephadex to avoid the ‘adsorption losses’ of the radioiodinated C-reactive protein. After saturation, 50 mL of 0.05 M phosphate buffer, pH 7.4, was passed through the column, and excess BSA was washed out. The flow rate of the column was maintained at nine drops per minute. Purified fractions were collected in a tube containing 1 mL of 1% BSA in 0.05 M phosphate buffer. Each tube was marked at 2 mL and numbered (1–40) to maintain the order for further analysis. Collected elute tubes were measured for 10 s (Single-well manual gamma counter, Electronics Corporation of India Limited, India), and the protein peak fraction was separated and diluted for the tracer preparation. Counts Per Minute (CPM) was set up to 55000–57000. The tracer was lyophilized and stored at 4 °C.
Analysis of 125I-C-reactive protein
After labelling, the compound was analyzed for % radioiodination yield by paper electrophoresis using the radioiodination reaction mixture, and purified aliquots were analyzed from the purified protein peak to determine radiochemical purity (RCP). Finally, tracer stability was analyzed using paper electrophoresis at regular intervals on storage. The effect of temperature and lyophilization over the tracer was analyzed by measuring % RCP using paper electrophoresis at successive time intervals (weekly). After radiolabeling, the reaction mixture was run for the paper electrophoresis using a Whatman paper strip (length 35 cm with 1 cm width). The reaction mixture with potassium iodide (10µL) was spotted at the anode site, and 0.025 M phosphate buffer, pH 7.4, was used as a running buffer. Paper electrophoresis was run for 45 min at 240 Volts. Then, the paper strip was removed and dried thoroughly, and treated with Palladous chloride solution and iodide was located visually. Finally, to count (CPM), a paper strip was cut into one cm pieces, and CPM was recorded in a multi-well gamma counter (Stratec, Germany).
Results and discussion
The Chloramine-T method is the most widely accepted radiolabeling method because of its oxidizing capacity with minimum damage to the protein and high radioiodination yield. Parameters such as reaction time, reagent concentration, and reaction conditions for radioiodination of C-reactive protein were based on the established results available in the literature and trials carried out in the laboratory. A typical chromatography elution pattern for 125I radiolabeled CRP was observed, similar to the published results [17, 18, 21].
Reagent concentration for labelling
In CRP radioiodination, 40 µg/ 10 µL of CRP was used for the labelling, and reagent concentration was optimized to achieve a high % radioiodination with a high binding capacity. Chloramine-T and metabisulfite (MBS) reagents were dissolved in concentrations of 0.25, 0.5, 0.75, 1, 1.5, 2, 3, 5 and 1, 2, 3, 4, 6, 8, 10, 20, respectively (Table 1). Figure 1 illustrates the I–VIII trials with different reagent concentrations. The IV combination showed the highest % radiolabeling. This reagent combination must be standardized for iodination. The reagent recipe depends on the molecular weight of the analyte/antibody [18, 19].
Effect of incubation time and temperature on radiolabeling
Standardization of the incubation time was performed at 20, 40, 60, 80, 100, and 120 s in the presence of chloramine-T. The suitable time for CRP radiolabeling was 60 s with 86.7 ± 3.13% radiolabeling % (Table 2). Before 60 s, the iodination rate was low (Fig. 2). The yields decreased above 80 s. The extent of iodination reaction time increased gradually with the reaction period to 60 s, which showed gain. Since CRP iodinated for 60 s had a radioiodination yield higher than that reacted for shorter periods and showed a decline in radioiodination yield, a reaction incubation time of 60 s was selected.
CRP Radiolabeling was performed at two temperatures (2 °C and 25 °C) to optimize the reaction temperature. CRP Radiolabeling yield was 90.95 ± 0.12% at 25 °C and 87.9 ± 2.09% at 2 °C. There was no significant difference in yield between the two temperatures. Hence, CRP radiolabeling can be carried out at both temperatures. However, 25 °C was selected as the incubation temperature for convenience (Fig. 3). Thus, 25 °C and 60 s for iodination were fixed for the % radiolabeling of CRP.
Radiolabeling incubation time varies with molecules, and standardization is challenging. The incubation time for bisphenol was 20 s [22], whereas, in motilin [23] and thromboxane B2 [24], the reaction was terminated at 30 s. Radiolabeling reaction time to theophylline was extended to 120 s [25]. Labelling to human C-peptide and human insulin was done at 60 s, as standardized in our published articles [26, 27].
Radiolabeled elution pattern
Purified collected fractions were subjected to 10 s counts in a single-well gamma counter. Figure 4 shows the CRP radiolabeled elution pattern. Fractions 8–12 had a high peak, labelled CRP, and fractions 21–24 (small peak) represent free iodide. Sephadex G-25 was chosen for purification based on previous literature [26].
Electrophoresis analysis of the tracer
From the reaction mixture, % radioiodination yield and RCP for labelled CRP were analyzed using the paper electrophoresis method. After the reaction, purification was carried out, and elute was collected at 1 mL per tube; a fraction containing labelled CRP was measured and separated to prepare the tracer. Selected pooled fractions, were mixed and diluted using assay buffer (0.5% BSA dissolved in 0.05 M phosphate buffer, pH-7.4). The pooled fraction containing the labelled component was analyzed for the % radiochemical purity (RCP). Specific activity was calculated after % radioiodination analysis using paper electrophoresis. Figure 5 shows the typical electrophoresis pattern of radiolabeled protein. Table 2 shows that the average radioiodination yield was ~ 86.6%, and RCP was > 97% for labelled CRP using the Chloramine-T method (Figs. 5, 6).
The mean specific activity of radioiodination was 17.9 μCi/μg. CRP radiolabeling using the iodogen method by Shine (1981) had shown similar results [25]. Hence, the Chloramine-T method can be adopted for the radiolabeling. Published RIA procedures reveal that different proteins have been radioiodinated following the Chloramine-T method [26,27,28,29]. Labelling by the unmodified chloramine-T procedure [29] or modified in some published articles [27,28,29,30] is most commonly used because of the simplicity, reproducibility, and efficiency of the procedures. Radioiodinated tracers were analyzed for tracer stability and binding capacity to ensure that the labelled protein (analyte) remains functionally unchanged by either the radiolabeling conditions or the presence of radioiodinated residues.
Radiolabeled CRP tracer stability
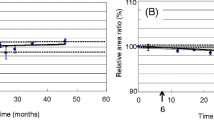
Prepared radiolabeled tracers were stored at different temperatures (− 20, 4, and 25 °C) in 0.5% BSA phosphate buffer (0.05 M, pH 7.4). The stability of the prepared tracer was checked using paper electrophoresis for RCP. The tracer stability was also checked using % binding (%B/T) of CRP tracer with CRP-antibody coupled with magnetizable cellulose particle. Tracer stored at − 20 °C and 4 °C showed no significant difference in % binding. However, the tracer stored at 25 °C was unstable compared to 4 °C and − 20 °C. Results presented in Table 3 suggest that % B/T at 4 °C and − 20 °C can be opted to store CRP tracer. Hence, labelled CRP was stored at 4 °C, and the CRP tracer was stable for two months.
Application of radiolabeled tracer
The prepared tracer was tested against the anti-CRP antibody coupled with the magnetizable cellulose particle. Analysis of the % binding showed the accomplishment of the 125I-CRP as a tracer. Magnetizable cellulose particle (BRIT, BARC, India) coupled antibody was diluted (1:600 factor) to standardize the CRP RIA procedure, and coupling procedure of antibody to magnetic cellulose particles was carried out using the 1,1-carbonyl diimidazole (CDI) activation method. Standards were prepared in bovine-free serum matrix, and controls were obtained from human serum samples. In the absence of unlabeled CRP (B0/T), total radiotracer bound to the coupled antibody, was about 25–30%. A typical standard curve for RIA was established using purified CRP protein with different concentrations (0, 6.25, 12.5, 25, 50, 100, 200 ng/mL). Results presented in Table 4 show that prepared assay reagents are suitable for sensitive assay development.
The chloramine-T for CRP labelling method described here is easy and reproducible. Its advantages in terms of specific activity, radiolabeled tracer stability, and radiochemical purity are discovered to be useful in assay development. In conclusion, the iodination yield is high in the Chloramine-T method, with less damage to the labelled molecule. So, the method is widely accepted for radiolabeling. The current study is the first to use the Chloramine-T method for CRP RIA development. Current standardized labelling procedures have many advantages, including minimum radioiodination incubation time, optimum binding capacity, and easy preparation of the radiolabeling reagents such as chloramine-T, metabisulfite, and potassium iodide. Radiochemical purity was linear for up to two months. In this context, this sensitive assay for CRP quantification is a valuable tool for the medical fraternity for the early risk management of CVDs and providing a reliable predictor for the risks of cardiovascular events [31,32,33]. Cardiac diseases are a leading cause of morbidity and mortality worldwide. Cytokines have a potential role in atherosclerosis, and several investigations reveal the association between C-reactive protein and the severity of CADs [34].
Conclusions
In CRP radiolabeling, maximum iodination yield was obtained with 1 mg/mL chloramine-T (10µg/10µL) and 4 mg/mL metabisulfite (80µg/20µL) concentrations. Iodination reaction conditions were optimized as 60 s incubation time at 25 °C. Radiolabeling was performed using the ~ 860 µCi activity, which gave a maximum specific activity of 17 µCi/µg. % radioiodination was 86.6 ± 3% with a radiochemical purity of ~ 97%. Lyophilization enhanced the shelf-life of the prepared tracer. The % B/T of tracer to antibody coupled with magnetizable cellulose particle was linear. Hence, the prepared tracer was adopted to develop the RIA procedure to quantify CRP.
References
Tillett WS, Francis T (1930) Serological reactions in pneumonia with a non-protein somatic fraction of pneumococcus. J Exp Med 52(4):561–571
Volanakis JE (2001) Human C-reactive protein: expression, structure, and function. Mol Immunol 38(2–3):189–197
Pathak A, Agrawal A (2019) Evolution of C-reactive protein. Front Immunol 10(943):1–12
Mantovani A, Garlanda C, Doni A, Bottazzi B (2008) Pentraxins in innate immunity: from C-reactive protein to the long pentraxin PTX. J Clin Immunol 28(1):1–13
Ridker PM, Silvertown JD (2008) Inflammation, C-reactive protein, and atherothrombosis. J Periodontol 79(8):1544–1551
Hirschfield GM, Pepys MB (2003) C-reactive protein and cardiovascular disease: new insights from an old molecule. QJM Int J Med 96(11):793–807
Pepys MB, Hirschfield GM (2003) C-reactive protein: a critical update. J Clin Invest 111(12):1805–1812
Sproston NR, Ashworth JJ (2018) Role of C-reactive protein at sites of inflammation and infection. Front Immunol 9:754
Ridker PM, MacFadyen JG, Glynn RJ, Bradwin G, Hasan AA, Rifai N (2020) Comparison of interleukin-6, C-reactive protein, and low-density lipoprotein cholesterol as biomarkers of residual risk in contemporary practice: secondary analyses from the cardiovascular inflammation reduction trial. Eur Heart J 41(31):2952–61
Ridker PM (2016) From C-reactive protein to interleukin-6 to interleukin-1: moving upstream to identify novel targets for atheroprotection. Circ Res 118:145–156
Ridker PM (2018) Clinician’s guide to reducing inflammation to reduce atherothrombotic risk: JACC review topic of the week. J Am Coll Cardiol 72:3320–3331
Ellington AA, Kullo IJ, Bailey KR, Klee GG (2010) Antibody-based protein multiplex platforms: technical and operational challenges. Clin Chem 56(2):186–193
Borrebaeck CA (2000) Antibodies in diagnostics—from immunoassays to protein chips. Immunol 21:379–382
Yalow RS, Berson SA (1960) Immunoassay of endogenous plasma insulin in man. J Clin Investig 39(7):1157–1175
Youfeng H, Coenen HH, Petzold G, Stöcklin G (1982) A comparative study of radioiodination of simple aromatic compounds via N-halosuccinimides and chloramine-T in TFAA. J Label Compd Radiopharm 19(7):807–819
Bhalla HL, Vavia PR, Samuel G, Sivaprasad N (1997) Development of radioimmunoassay: I. Preparation of radiolabeled tracers theophylline. J Radioanal Nucl Chem 220:73–76
Hunter R (1970) Standardization of the chloramine-T method of protein iodination. Proc Soc Exp Biol Med 133(3):989–992
Bailey GS (2002) The chloramine T method for radiolabeling protein. The Protein Protocols Handbook. Springer Protocols Handbooks, Humana Press, pp 963–965
McConahey PJ, Dixon FJ (1966) A method of trace iodination of proteins for immunologic studies. Int Arch Allergy Immunol 29(2):185–189
Hunter WM, Greenwood F (1962) Preparation of iodine-131 labelled human growth hormone of high specific activity. Nature 194:495–496
Pimpalkhute M, Majali M, Mani R (1986) Radioimmunoassay of human follicle stimulating hormone/HFSH. J Radioanal Nucl Chem 103(2):105–116
Kaddar N, Bendridi N, Harthé C, de Ravel MR, Bienvenu AL, Cuilleron CY, Mappus E, Pugeat M, Déchaud H (2009) Development of a radioimmunoassay for the measurement of Bisphenol A in biological samples. Anal Chim Acta 645(1–2):1–4
Tai HH, Chey WY (1978) Development of radioimmunoassay for motilin. Anal Biochem 87(2):350–358
Tai HH, Yuan B (1978) Development of radioimmunoassay for thromboxane B2. Anal Biochem 87(2):343–349
Shine B, De Beer FC, Pepys MB (1981) Solid phase radioimmunoassays for human C-reactive protein. Clin Chim Acta 117(1):13–23
Rasmi RR, Shenoy KB, Kadwad VB, Sarnaik J, Somashekarappa HM (2015) Application of novel magnetizable cellulose particles in the development of immunoradiometric assay for C-peptide. J Radioanal Nucl Chem 304:1115–1122
Rasmi RR, Kadwad VB, Sarnaik J, Shenoy KB, Somashekarappa HM (2021) Development of radioimmunoassay for estimation of C-peptide in human serum. J Radioanal Nucl Chem 327:923–928
Manupriya BR, Paradkar S, Ghodke TS, Kadwad V, Karunakara N, Shenoy KB (2023) Development of a magnetizable cellulose particle-based immunoradiometric assay for quantification of C-peptide in rat serum. J Radioanal Nucl Chem 332(3):517–525
Greenwood FC, Hunter WM, Glover JS (1963) Radioiodination of proteins with chloramine T. Biochem J 89:114–123
Gnanasekar R, Sarnaik JS, Joseph NC, Kadwad VB, Mathur A (2021) Development of two-step radioimmunoassay (RIA) for the measurement of free triiodothyronine in human serum based on antibody coated tubes. J Radioanal Nucl Chem 329(1):71–76
Borque L, Bellod L, Rus A, Seco ML, Galisteo-Gonzalez F (2000) Development and validation of an automated and ultrasensitive immunoturbidimetric assay for C-reactive protein. Clin Chem 46(11):1839–1842
Bouzidi N, Messaoud MB, Maatouk F, Gamra H, Ferchichi S (2020) Relationship between high sensitivity C-reactive protein and angiographic severity of coronary artery disease. J Geriatr Cardiol 17(5):256–263
Wang W, Ren D, Wang CS, Li T, Yao HC (2019) High sensitivity C-reactive protein to prealbumin ratio measurement as a marker of the prognosis in acute coronary syndrome. Sci Rep 9(1):11583
Kaptoge S, Di Angelantonio E, Pennells L, Wood AM, White IR, Gao P, Walker M (2012) C-reactive protein, fibrinogen, and cardiovascular disease prediction. N Engl J Med 367(14):1310–1320
Acknowledgements
The authors are grateful to BRNS, DAE, Government of India for the financial support of this work. The authors are grateful for the continuous support from Rani Gnanasekar and Shripriya Purohit. The authors acknowledge the support of the Centre for Application of Radioisotopes & Radiation Technology (CARRT), Mangalore University, Department of Applied Zoology, Mangalore University, and the Board for Radiation and Isotope Technology (BRIT), Vashi Complex, Vashi, Mumbai.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ghodke, T.S., Manupriya, B.R., Kadwad, V. et al. 125I labelling of C-reactive protein for the development of Radioimmunoassay (RIA). J Radioanal Nucl Chem 333, 3007–3013 (2024). https://doi.org/10.1007/s10967-024-09425-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10967-024-09425-6