Abstract
Psychiatric illness in adolescence is associated with long-term impairments, making it critical to identify predictors of adolescent psychiatric distress. Individual differences in stress sensitivity could be associated with longitudinal trajectories of internalizing symptoms. Historically, researchers have operationalized stress sensitivity by assessing either objective or subjective responses to stress. However, we posit that the relative discordance between subjective and objective responses to stress is a critical metric of stress sensitivity. We examined whether two discordance-based indices of stress sensitivity were related to one another and to trajectories of internalizing psychopathology among a sample of 101 adolescent youths (Mage = 12.80 at baseline; 55% males) across two successive stressors: the high school transition and the COVID-19 pandemic. Using latent growth curve modeling, we found that greater discordance between subjective (i.e., affective) and objective (i.e., cortisol) responses to a social-evaluative stressor was associated with higher internalizing symptoms at baseline and an accelerated symptom growth trajectory across the first year of the pandemic. In contrast, early life stress sensitivity was not associated with internalizing symptoms. Findings suggest that the discordance between objective and subjective experiences of social-evaluative stress predicts a pernicious growth trajectory of internalizing symptoms during adolescence. This work advances current methodologies, contributes to theoretical models of internalizing psychopathology, and with replication could have implications for policy and practice by identifying a key vulnerability factor that increases adolescents’ psychiatric distress over time.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Symptoms of internalizing disorders increase sharply during adolescence (Kessler et al., 2012; Merikangas et al., 2010; Solmi et al., 2022) and are associated with long-term impairments in health and wellbeing (Belfer, 2008; Merikangas et al., 2009). As such, it is important to elucidate factors present during early adolescence (i.e., before rates of psychiatric illnesses increase) that contribute to pernicious trajectories of internalizing symptoms from early to mid-adolescence. The early adolescent period includes ages 10 through 14 years and is a pivotal developmental stage characterized by biological, cognitive, psychosocial, and emotional changes that contribute to mental health across the lifespan (Blum et al., 2014; Sawyer et al., 2012). Indeed, given the significant neural plasticity and development occurring in early adolescence, the adolescent brain is remarkably sensitive to the neurotoxic effects of stress (Romeo & McEwen, 2006), which have been linked to the onset and maintenance of internalizing symptoms (e.g., anxiety and depression; Eiland and Romeo, 2013). Thus, exposure to stress during this period has the potential to exert a powerful influence on wellbeing across the lifespan – including on the development of internalizing symptoms during adolescence.
Although stress exposure is a ubiquitous experience, not all youth who experience stressors go on to develop elevated levels of internalizing symptoms. Instead, individual differences in the stress response (i.e., in the affective, biological, and/or cognitive responses to a stressor) have been posited as a central mechanism influencing trajectories of internalizing symptoms following stress exposure (LeMoult, 2020). Historically, researchers have typically operationalized individual differences in the stress response by assessing objective or subjective responses to stress. Discrepancies (i.e., the discordance) between objective and subjective responses has often been conceptualized as methodological ‘noise’ or the result of unmeasured confounding variables (Hollenstein & Lanteigne, 2014). However, seminal models of stress posit that the discordance between objective and subjective responses to stress is meaningful as it indexes stress sensitivity, an individual’s tendency to respond more or less strongly following stress exposure (Hammen, 2015; Harkness et al., 2015). There is recent support for this proposition. For instance, greater stress sensitivity (modeled as the residual variance in subjective stress severity after accounting for objective stress severity) has been cross-sectionally associated with higher levels of anxiety and depressive symptoms, and with constructs related to internalizing symptoms, such as poorer autonomic and affective regulation (Conway et al., 2012; Ho et al., 2017, 2020). Further, discordance between subjective and objective aspects of the stress response (indexed via discordance between self-reported affect and biological responsivity) has been cross-sectionally associated with greater difficulties in emotion regulation and greater internalizing symptoms (Lanteigne et al., 2014; Sommerfeldt et al., 2019). Thus, discordance-based markers of stress have received recent support as indices of stress sensitivity and have promise to further our current understanding of the associations between stress exposure and psychopathology.
To date, however, studies have included only one discordance-based index of stress sensitivity (e.g., Conway et al., 2012; Ho et al., 2017, 2020; Lanteigne et al., 2014; Sommerfeldt et al., 2019). By including two distinct discordance-based indices of stress sensitivity, the present study is able to examine associations of discrete indices with trajectories of internalizing symptoms. Consistent with Ho (2017, 2020), we indexed early life stress sensitivity as the discordance between subjective and objective reports of early life stress. This index models the discrepancy between an individual’s subjective appraisals of the severity of early life stress experiences and the objective severity of those experiences. Next, consistent with Lanteigne (2014) and Sommerfeldt (2019), we indexed social-evaluative stress sensitivity as the discordance between subjective (i.e., affective) and objective (i.e., biological) responses to a social-evaluative stressor. The stressor used in the current study was the Trier Social Stress Test for Children (TSST-C), a well-validated laboratory social-evaluative stressor that reliably indices both affective and biological responses (Buske-Kirschbaum et al., 1997).
The present study extends previous work by examining whether two discordance-based indices of stress sensitivity were associated with trajectories of internalizing symptoms during the early to mid-adolescent transition. It is important to examine trajectories of internalizing symptoms across this transition given that it is a developmental period wherein rates of both anxiety and depressive disorders sharply increase (Costello et al., 2011; Kessler et al., 2007). Understanding trajectories of symptoms is critical to identifying youth most at risk for persistent difficulties (McLaughlin & King, 2015). In addition, for the present cohort, superimposed upon this developmental period were two significant stressors: the transition to high school and the onset of the COVID-19 pandemic, both of which have documented impacts on internalizing symptoms in youth (Benner, 2011; Racine et al., 2021). Yet, not all youth experience increases in internalizing symptoms in response to these stressors (Golberstein et al., 2020; Racine et al., 2021). As such, both the high school transition and the COVID-19 pandemic are valuable contexts in which to examine mechanisms associated with individual differences in the trajectories of youth’s internalizing symptoms. We used a latent growth curve modeling (LCGM) approach to examine whether both the social-evaluative and early life stress sensitivity indices were associated with one another and with trajectories of internalizing symptoms.
We hypothesized that increased stress sensitivity (i.e., greater subjective stress in relation to objective stress) within either stress-sensitivity index would be associated with greater internalizing symptoms at baseline and increasing levels of internalizing symptoms across the first year of the COVID-19 pandemic. Further, we predicted that social-evaluative stress sensitivity would be associated with early life stress sensitivity, such that elevations in one index of stress sensitivity would be associated with elevations in the second index. Through the use of distinct methods to operationalize stress sensitivity and by incorporating multiple methods of measurement (e.g., affective, biological, cognitive), the present study responds to calls for work examining whether multiple indices of stress sensitivity converge, both with one another and with relevant outcomes over time (Hammen, 2015).
Methods
Participants
Youth were eligible for inclusion if they were between 11 and 13 years of age at baseline and were fluent in English. Participants were excluded if parent or youth reported that the adolescent had a medical condition known to affect the neuroendocrine system, or were currently using corticosteroids, depot neuroleptics, or oral or inhaled steroids given that each can alter cortisol levels (Granger et al., 2009). Youth were recruited from diverse communities throughout the Vancouver metropolitan area using various methodologies, including via partnerships with community organizations such as school boards and both online and paper advertisements. Compensation was offered for transportation to the university, so that transportation costs were not a barrier to participation. The final sample included 101 adolescents, which is in line with current sample size guidelines for the use of LGCM (Curran et al., 2010). Youth were between 11.86 and 13.86 at baseline (M = 12.82), and 55% of participants were assigned male at birth. Regarding racial identity, 63% of participants identified as White; 14% identified as Chinese; 3% identified as Canadian Indigenous; 3% identified as Japanese; 3% identified as Latinx/e; 3% identified as South Asian; and 11% identified with additional endorsed racial identities. Participant characteristics are presented in Table 1 and are generally representative of the Vancouver metropolitan area (Statistics Canada, 2022). Additional details are presented in the online supplement.
Measures
Social-Evaluative Stressor
To assess responses to social-evaluative stress, participants completed the Trier Social Stress Test for Children (TSST-C), a standardized stress paradigm that reliably generates both an affective and a biological stress response (Buske-Kirschbaum et al., 1997). The TSST-C consists of four phases: baseline, preparation, stressor, and recovery. After watching a 15-minute calming nature video (Baseline), youth were told that they would complete a speech task and were given 5 min to prepare (Preparation). Following this preparation period, participants completed a 10-minute stressor during which they were asked to perform both a standard speech task and an unexpected math task in front of a panel of judges (Stressor). Following the stressor, participants watched a 20-minute nature video and completed a 10-minute debriefing session, thus concluding the 30-minute recovery period (Recovery). Participants provided affect ratings and saliva samples at six points throughout the TSST-C: at the end of the Baseline period (S1), at the end of the Preparation period (S2), and at 0, 10, 20, and 30 min after the end of the Stressor period (S3-S6). The TSST-C was conducted in accordance with best-practice guidelines (Allen et al., 2017; Linares et al., 2020).
Subjective Stress Response- Affect. Subjective response to the social-evaluative stressor was assessed based on self-reported state-level negative affect, which was measured using a brief questionnaire adapted from the Positive and Negative Affect Scale for Children (PANAS-C; Hughes and Kendall, 2009). Reliability for negative affect across the stressor was excellent, α = 0.90. Responses were summed across each of the six administrations to create a total negative affect score. Using trapezoidal integration, area under the curve with respect to ground (AUCg) was calculated for negative affect across the TSST-C (Pruessner et al., 2003). We chose to calculate AUCg given that it emphasizes cumulative output rather than change over time (as in the case with area under the curve with respect to increase; AUCi). As such, AUCg closely mirrors the method in which both subjective and objective early life stress severity is modeled in previous work and in the calculation of social-evaluative stress sensitivity in the current study (see below; Ho et al., 2017, 2020).
Objective Stress Response - Cortisol. Objective response to the social-evaluative stressor was assessed based on cortisol responses across the TSST-C. Saliva samples were collected using Sarstedt Salivettes across the TSST-C. All participants completed the TSST-C in the afternoon to control for diurnal variations in cortisol (Pruessner et al., 1997). After collection, saliva samples were frozen and stored at -20 °C until analysis. During analysis, salivettes were centrifuged at 3,000 rpm for 5 min, resulting in a clear supernatant of low viscosity. Salivary concentrations were then measured using a commercially available chemiluminescence immunoassay with high sensitivity (IBL International, Hamburg, Germany). The intra and interassay coefficients for cortisol were both below 8%. Before calculating AUCg, we tested whether days since last period, menstruation status, sleep the night prior to the laboratory session, sex, and medication use were associated with cortisol across the TSST-C given the potential for these variables to effect HPA axis functioning (Granger et al., 2009; Leproult et al., 1997; Wolfram et al., 2011). None of the variables were associated significantly with cortisol levels at any sampling point, ps ≥ 115. Using trapezoidal integration, the area under the curve with respect to ground (AUCg) was calculated for cortisol across the TSST-C (Pruessner et al., 2003). This method captures both intensity (i.e., overall distance of each measure to ground) and sensitivity (i.e., the difference between individual measurements). Additional details are presented in the online supplement.
Early Life Stress
Using the gold standard approach to assessing early life stress and consistent with recent work (Ho et al., 2020; King et al., 2017), youth completed a contextual interview for the assessment of early life stress. Standardized interview-based assessments have the benefit of being able to characterize experiences of early life stress more precisely compared to self-report measures, and are also characterized by less mood-related reporting biases (Grant et al., 2004; Vanaelst et al., 2012). In the present study, youth completed a modified version of the Traumatic Events Screening Inventory for Children (TESI-C; King et al., 2017; Ribbe, 1996), a contextual interview which assesses youths’ lifetime exposure to 30 types of stressful events (e.g., parental divorce, serious illness, bullying). For each event that was endorsed, interviewers gathered extensive contextual details to characterize the event.
Subjective Stress Severity. For each endorsed event, youth provided subjective severity ratings on a 4-point scale from 0 (not scared, confused, or helpless) to 3 (extremely scared, confused, or helpless). Subjective early life stress exposure was calculated by summing youths’ maximum subjective severity ratings for each type of stressor that was endorsed. This method ensures that frequent but less severe events within each type of stressor are not excessively weighted (King et al., 2017).
Objective Stress Severity. Consistent with best-practice recommendations for assessing objective stress severity and in line with previous work (Grant et al., 2004; Ho et al., 2017, 2020), descriptions and contextual details of each stressor were presented to a panel of three raters. To reduce bias, raters were blind to details such as youths’ emotional responses during the interview and youths’ subjective severity ratings. Specifically, trained research assistants transcribed and delivered a description of each stressor to the panel, excluding any details that could reveal the youth’s subjective perception of the event’s severity. Raters, who underwent rigorous training, then coded each endorsed stressor for objective stress severity using a modified version of the UCLA Life Stress Interview coding system (King et al., 2017; Rudolph & Hammen, 1999). Objective stress ratings were scored on a 0 (no impact) to 4 (extremely severe impact) scale with half-point increments. Interrater reliability was excellent (ICC = 0.97). Objective early life stress exposure was then calculated by summing the panel-rated maximum objective severity score for each type of stressor endorsed. Additional details are presented in the online supplement.
Internalizing Symptoms
To assess internalizing symptoms, participants completed the Children’s Depression Inventory (CDI; Kovacs, 2015), the Center for Epidemiological Studies Depression Scale for Children (CES-DC; Faulstich et al., 1986), the Multidimensional Anxiety Scale for Children (MASC-10; March et al., 1997), and the Anxiety Problems subscale of the Youth Self-Report (YSR-AP; Achenbach, 1991). Higher scores indicate greater symptoms of depression (i.e., CDI, CES-DC) or anxiety (i.e., MASC-10, YSR-AP). All measures have been used widely in studies of both clinical and non-clinical children and adolescents, and have strong psychometric properties (Baldwin & Dadds, 2007; Ebesutani et al., 2011; Fendrich et al., 1990; Saylor et al., 1984). For further detail, including descriptive statistics, reliability estimates, and correlations between internalizing symptom measures, see the online supplement. We examined linear as well as quadratic trajectories of internalizing symptoms given evidence of a non-linear change in rates of anxiety and depression across adolescence (Copeland et al., 2014; Hankin et al., 1998).
Covariates
To assess youths’ demographic characteristics, caregivers completed a brief questionnaire assessing variables including youth’s age, sex assigned at birth (hereafter referred to as sex), and household income. Youth concurrently completed a questionnaire assessing variables relevant to the assessment of cortisol, including menstruation status and days since last menstrual period (if relevant), amount of sleep the night before the laboratory session, and medication use.
Pubertal staging was measured using the self-report Tanner staging questionnaire (Marshall & Tanner, 1968), which correlates highly with physicians’ physical examinations of pubertal development (Shirtcliff et al., 2009). Youth viewed a series of drawings depicting developmental stages of pubic hair and breast/testes development, with stages ranging from 1 (pre-pubertal) to 5 (post-pubertal) and were asked to indicate which drawings best approximated their own development. In line with previous work, we averaged Tanner scores for each participant to create an index of average pubertal development at each timepoint (Dorn et al., 2006).
Procedure
The study was approved by the University of British Columbia Institutional Review Board. At baseline (immediately prior to the high school transition; Time 1), participants and their caregivers attended an initial laboratory session at the University of British Columbia during which informed consent was obtained from caregivers, and informed assent was obtained from youth.
Youth then completed the TSST-C, the TESI, measures of internalizing symptoms, and a measure of pubertal staging. The laboratory session took place in the afternoon to control for diurnal variations in cortisol, which was collected during the TSST-C (Pruessner et al., 1997). Caregivers and youth completed brief questionnaires assessing demographic and health variables. Approximately 13 months later (Mdays = 414.35; SD = 86.62), during May–July of 2020 when the first pandemic-related lockdown in the region was in place (during the COVID-19 pandemic; Time 2), participants once again completed measures of internalizing symptoms as well as pubertal status. Approximately one year later (Mdays = 363.48; SD = 12.49), in May–July of 2021 (approximately 15 months following the onset of the COVID-19 pandemic; Time 3), participants re-completed measures of internalizing symptoms and pubertal status. Time 2 and Time 3 assessments were completed virtually using Qualtrics.
Planned Analyses
Discordance Indices of Stress Sensitivity
Social-Evaluative Stress Sensitivity. AUCg values were standardized using a z-transformation for both negative affect and cortisol. Using the standardized AUCg values, a social-evaluative stress sensitivity index was computed by calculating the residual variance in subjective (i.e., affective) responsivity to the stressor after accounting for objective (i.e., biological) responsivity to the stressor. This method of calculating standardized residuals is a well-established approach for comparing subjective and objective scores (De Los Reyes & Prinstein, 2004; Krackow & Rudolph, 2008). Higher values represent greater stress sensitivity, indicated by an exaggerated subjective response to the stressor in relation to the objective response, while lower values represent greater concordance between objective and subjective components of the stress response.
Early Life Stress Sensitivity. Subjective and objective early life stress exposure values were standardized using a z-transformation. As in previous work (Ho et al., 2017, 2020), an early life stress sensitivity index was computed by calculating the residual variance in subjective stress severity after accounting for objective stress severity using a linear regression model. As such, an individual with high early life stress sensitivity would not necessarily have high early life stress exposure. Higher values represent greater stress sensitivity, indicated by a tendency to exhibit exaggerated subjective responses to early life stress in relation to objective stress severity.
Main Analyses
Data analyses were conducted in R version 4.1.1 (R core team, 2021). A series of variables were first tested as potential covariates in relation to youths’ internalizing symptoms across time including age, pubertal stage, sex, household income, and number of days between timepoints (Dahl & Gunnar, 2009; Nolen-Hoeksema & Girgus, 1994). Time-varying covariates (e.g., pubertal stage) were specified to predict the outcome measures at corresponding time points, while time-invariant covariates (e.g., sex assigned at birth) were specified to predict the latent intercept and slope growth factors (Wang & Wang, 2019). Taking a data-driven approach and based on best-practice recommendations, only significant covariates were retained in the final model to maximize power and prioritize model parsimony (Murtaugh, 1998).
Missing values for cortisol and affect ratings collected during the TSST-C were addressed using Bayesian Stochastic regression imputation, for the purpose of AUCg calculation. Less than 1.5% of data was missing for both cortisol and affect ratings across the TSST-C. Given that Little’s MCAR test indicated that both cortisol and affect data were missing at random (MAR; ps ≥ 0.919), the multivariate imputation by chained equations (MICE) approach implemented in the ‘mice’ package for R (Buuren & Groothuis-Oudshoorn, 2011) was used. We then extracted scores on latent internalizing symptom factors that were developed for symptoms at Time 1, Time 2, and Time 3 using the lavPredict() function in lavaan (Wang & Wang, 2020). Specifically, latent factors representing internalizing symptoms at Times 1–3 were based on scores from the CDI, CES-DC, MASC-10, and YSR-AP at Time 1, Time 2, and Time 3, respectively. Fit statistics associated with latent internalizing symptom factor models are presented in the online supplement. Extracted factor scores were then included as observed endogenous variables in subsequent analyses. The number of indicators used in the present study (n = 4 at each timepoint) was selected for statistical and methodological reasons. Statistically, four indicators is considered to be ideal as it increases the stability of the latent factor and decreases the possibility of empirical under-identification (Kline, 2016; Mueller & Hancock, 2018). Methodologically, having three or more indicators improves the quality of the construct’s measurement, including both the replicability of the construct across samples and its theoretical breadth through greater symptom coverage (Mueller & Hancock, 2018). Indeed, recent empirical work suggests that different assessment tools assess different symptoms and, thus, the use of multiple questionnaires is recommended to both capture the full range of symptom presentations and to increase robustness of measurement (Fried, 2017; Fried et al., 2022).
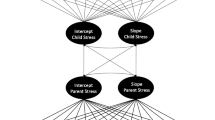
To test associations between discordance indices of stress sensitivity and internalizing symptoms over time, a latent growth curve modeling (LGCM) approach was employed using the ‘lavaan’ package for R (Rosseel, 2012). We first fit unconditional candidate growth models describing both linear and quadratic trajectories of internalizing symptoms over time, given that three or more time points provide the opportunity to test for nonlinear trajectories (see best-practice guidelines in the estimation of structural equation models described by Duncan and Duncan, 2009 and Kline, 2016). After identifying the best-fitting model using Akaike Information Criteria (AIC), Bayesian Information Criteria (BIC), and a chi-square difference test (Δχ2), a conditional model was developed by regressing growth factors on both social-evaluative stress sensitivity and early life stress sensitivity, which were allowed to covary (see Fig. 1). Model parameters were estimated using the maximum likelihood (ML) estimator, employing full information maximum likelihood (FIML) for missing data estimation (Wang & Wang, 2020). The variances of the intercept and growth factors were fixed for model identification (Duncan et al., 2006; Rosseel, 2015). To evaluate model fit, we used the chi-square (χ2) test, with a non-significant chi-square test indicating good model fit. However, as the chi-square statistic is sensitive to sample size, we also used incremental fit indices, including the root mean square error of approximation (RMSEA), the standardized root mean square residual (SRMR), and the comparative fit index (CFI), which is consistent with recommendations put forth by Kline (2016). RMSEA and SRMR values of less than 0.05 and CFI values over 0.90 indicate good model fit (Hu & Bentler, 1999; Schermelleh-Engel et al., 2003).
Results
Preliminary Analyses
Participant demographic and clinical characteristics are presented in Table 1. Covariate analyses indicated that only sex was significantly associated with internalizing symptoms, β = 0.39, p = .036, such that females had higher levels of internalizing symptoms. Thus, sex was included as a time-invariant covariate in the final structural model. Correlations between study variables are presented in Table 2.
Growth Models
A quadratic growth model was retained as the best-fitting growth curve model. The AIC and BIC values for the quadratic growth model were smaller (AIC = 850.33, BIC = 845.27) than values associated with the linear growth model (AIC = 863.75, BIC = 860.37). A significant chi-square difference test provided additional support for the superior fit of the quadratic growth model, Δχ2(3) = 19.42, p < .001. As the quadratic growth model was just-identified (i.e., df = 0), fit indices are not reported for the baseline model. On average, trajectories were characterized by a negative intercept (β = -0.02), a negative linear slope (β = -0.08), and a positive quadratic slope (β = 0.11).
Stress Sensitivity and Trajectories of Internalizing Symptoms
We then fit a conditional model in which growth factors were regressed on both social-evaluative stress sensitivity and early life stress sensitivity (see Fig. 1). Results indicated that this hypothesized structural model was a good fit to the data: χ2(2) = 1.54, p = .464, RMSEA = 0.000, SRMR = 0.032, and CFI = 1.00. Statistics for the structural model are presented in Fig. 1.
In line with hypotheses, social-evaluative stress sensitivity was associated with internalizing symptoms at baseline, β = 0.47, p = .011, such that greater discordance between subjective (i.e., affective) and objective (i.e., biological) responses to the stressor was associated with higher pre-pandemic internalizing symptoms. Further, social-evaluative stress sensitivity was associated with the linear slope, β = -0.59, p = .022, and quadratic slope of internalizing symptoms over time, β = 0.56, p = .038, such that greater discordance was associated with a nonlinear symptom trajectory with an initial downward trend, but greater quadratic growth in symptoms over time (i.e., an overall acceleration in the internalizing symptom growth trajectory). For the purposes of illustration, we plotted trajectories of internalizing symptoms among individuals with high (+ 1 SD), average, and low (-1 SD) levels of social-evaluative stress sensitivity (Fig. 2).
In contrast, early life stress sensitivity was not associated with internalizing symptoms at baseline, β = -0.08, p = .624, or with either the linear, β = 0.12, p = .574, or quadratic slope of change, β = -0.15, p = .471 (see Table 3). In addition, although theoretically similar, social-evaluative stress sensitivity was not associated with early life stress sensitivity, cov = − 0.08, p = .475.Footnote 1
Discussion
Stress exposure is a powerful predictor of the onset, maintenance, and recurrence of internalizing symptoms in adolescence; however, not all youth exposed to stressors develop elevated levels of internalizing symptoms. Stress sensitivity has therefore been posited as a key mechanism through which stress exposure influences internalizing psychopathology (Hammen, 2015). In the present study we found that sensitivity to social-evaluative stress (but not early life stress) was associated with higher pre-pandemic levels of internalizing symptoms and with an accelerated trajectory of increasing symptoms. We examined trajectories of symptom change across the transition from early to mid-adolescence, a developmental period involving well-documented increases in rates of both anxiety and depression upon which two significant contextual stressors were superimposed: the transition to high school and the COVID-19 pandemic.
The present work represents a methodological step forward for the field by conceptualizing stress sensitivity through two distinct discordance indices, each of which is consistent with theoretical formulations of stress sensitivity (i.e., elevated subjective appraisal of the severity of a stressor in relation to the objective severity; Conway et al., 2012; Hammen, 2015). Discordance indices allow for a multi-method approach through the incorporation of variables across methods of measurement (e.g., affective, biological, cognitive), thus generating a more nuanced understanding of stress sensitivity. Findings indicated that greater social-evaluative stress sensitivity was associated with higher levels of internalizing symptoms pre-pandemic, and with a symptom trajectory characterized by an initial downward trend but greater quadratic growth in symptoms for adolescents during the pandemic. These results support the proposition that greater subjective appraisals of stress severity in relation to objective markers of stress severity predict trajectories of internalizing symptoms. Intriguingly, findings are also in line with previous work showing that greater subjective than objective stress severity is linked with poorer coping strategies (e.g., Sommerfeldt et al., 2019). Converging evidence suggests that it is the subjective experience of stress, rather than objective exposure to stress, that is most strongly related to psychopathology across the lifespan (Danese & Widom, 2020, 2021; Walker et al., 2004). There is reason to believe this association could be related to coping in the context of stress exposure. For example, previous work has shown that greater stress sensitivity (conceptualized as greater discordance between subjective and objective responses to stress) is associated with greater difficulty regulating emotions and the use of maladaptive regulation strategies (Lanteigne et al., 2014). Thus, individuals with higher stress sensitivity may respond to stressors with maladaptive emotion regulation strategies that, over time, increase risk for the onset, maintenance, and recurrence of internalizing psychopathology (LeMoult, 2020).
When both indices of stress sensitivity were included in the model, we found that social-evaluative stress sensitivity, but not early life stress sensitivity, was associated with trajectories of internalizing symptoms. This suggests that each index may tap into a distinct vulnerability, which is supported by our finding of limited concordance between the two discordance indices. By modeling the discordance between two aspects of the stress response, the social-evaluative stress sensitivity index is closely related to the concept of emotional discordance. It may therefore be a particularly relevant index of stress sensitivity during adolescence given the remarkable neural changes occurring during this period. The transition from childhood to adolescence involves a profound shift in the neural circuitry underlying emotional behavior. Whereas childhood is dominated by an information flow from the amygdala to the dorsal anterior cingulate cortex (dACC) and ventromedial prefrontal cortex (vmPFC), adolescence is marked by an opposite flow, indicative of a change from bottom-up excitatory processing to top-down regulatory functioning (Gee et al., 2022). Given the dramatic neural restructuring occurring in early adolescence, a diminished ability to recruit regulatory regions of the brain to downregulate limbic activity could result in greater stress sensitivity to social-evaluative stress, which we found in turn to predict exacerbations in internalizing symptoms in the context of stress exposure. In addition, social-evaluative stress sensitivity could be a particularly relevant index of stress sensitivity during early adolescence given that the adolescent transition (and corresponding transition to high school) is characterized by shifts in social roles and responsibilities and is a time when youth become more sensitive to both peer acceptance and rejection (Kilford et al., 2016). As such, it is possible that stress sensitivity operationalized based on responses to a psychosocial stressor in which youth are overtly evaluated on their performance, could be distinctly relevant during the adolescent period. One final possibility is that task characteristics could account for the observed pattern of findings. The social-evaluative index of stress sensitivity was assessed contemporaneously with baseline internalizing symptoms, whereas the early life index of stress sensitivity (assessed via the TESI-C; Ribbe, 1996) reflected events occurring earlier in time and, thus, more distal to the measures of current internalizing symptoms. Nevertheless, there is an abundance of evidence demonstrating that early life stress is strongly associated with internalizing psychopathology across the lifespan (Infurna et al., 2016; LeMoult et al., 2020; Li et al., 2016).
Contrary to hypotheses, the two indices of stress sensitivity were not significantly correlated with one another. This indicates that indices of stress sensitivity cannot be treated as indistinguishable and underscores the importance of examining whether different indicators of stress sensitivity converge with one another and with outcomes over time (Hammen, 2015). Our finding of limited concordance between indices of stress sensitivity has important methodological implications for the field: to advance theoretical understanding of the antecedents and consequences of stress sensitivity, future work in this area ought to include multiple indices of stress sensitivity across multiple levels of assessment.
Limitations
Results of this study should be interpreted in the context of several limitations. Although our sample is generally representative of the Vancouver metropolitan area, the majority of youth in the present sample identified as White and many participant households exceeded the median Canadian household income (Statistics Canada, 2021). Therefore, the present study should be replicated in more generalizable samples with greater racial and socioeconomic diversity. Next, although the current sample exceeds best-practice recommendations of sample sizes (Boomsma, 1985), larger samples offer multiple advantages including more closely replicating population demographics. Additionally, it is possible that early life stress sensitivity could emerge as a significant predictor of internalizing symptom trajectories in a larger, more diverse, and/or high-risk sample (Aron & Aron, 1999), highlighting the importance of replication. The sample size in the present study also limited the complexity of the model we were able to develop due to power-related considerations. For instance, though there is reason to expect that both anxiety and depression would be associated with discordance indices of stress sensitivity, differential associations could emerge with anxiety versus depression given evidence that discordance-based early life stress sensitivity is associated with symptoms of both generalized and social anxiety in youth (Ho et al., 2017, 2020). Thus, future work with larger sample sizes should investigate anxiety and depression separately to test whether there are distinct associations of stress-sensitivity indices with each outcome. Similarly, it is possible that gender differences exist in the observed associations. For instance, recent work found stronger support for a stress-reactivity versus stress-exposure model in the development of depression among adolescent girls but not among adolescent boys (Morken et al., 2023). Given the theoretical similarities between stress-sensitivity and stress-reactivity models, these findings highlight the importance of future well-powered work investigating gender differences in the associations between discordance-based stress sensitivity and internalizing symptoms. Future work could also consider an additional metric of objective early life stress sensitivity (e.g., court records) to further reduce bias: while we took several measures to reduce the potential for bias across the rating process, the involvement of humans in the rating process inherently introduces a degree of subjectivity. Next, although three or more timepoints allow for the possibility of testing quadratic growth over time, future studies should include a greater number of sampling occasions to determine whether the identified trend generalizes across time in a less restricted model (Duncan & Duncan, 2009; Kamata et al., 2013). Finally, while the variances of the intercept and growth factors were fixed for model identification in the present study, it would be interesting for future work to consider testing the intercept and growth factors as random effects.
Conclusions
Adolescence is a developmental period of marked “storm and stress” (Hall, 1904). We identified an association wherein sensitivity to social-evaluative stress (but not early life stress) was associated with higher pre-pandemic levels of internalizing symptoms and an accelerated trajectory of increasing symptoms for adolescents during the pandemic. These findings identify a key vulnerability factor (i.e., social-evaluative stress sensitivity) that may place youth on a pernicious trajectory during times of stress. If replicated, findings could have implications for policy and practice. For instance, policies establishing school curricula designed to ameliorate social-evaluative stress sensitivity have the potential to promote mental health wellbeing for youth (Greenberg et al., 2017; Greenberg & Abenavoli, 2016). In addition, this work responds to a recent call put forth by Hammen (2015), which states that the field is hampered by the absence of work examining concurrent and predictive associations between indices of stress sensitivity (and, in particular, indices involving multiple measures at different levels of conceptualization) and outcomes. The present study responds to this call and, in doing so, highlights the importance of approaches that utilize multiple stress sensitivity indicators. In addition, this work demonstrates that the discordance between objective and subjective responses to stress is not simply methodological noise; as such, it should continue to be explored as a meaningful metric of stress sensitivity.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Notes
The main analyses were repeated after replacing latent factor scores with summed standardized symptom scores. An identical pattern of findings emerged: social-evaluative stress sensitivity was associated with higher levels of internalizing symptoms at baseline, and with a nonlinear symptom trajectory with an initial downward trend and greater quadratic growth in symptoms over time (ps ≤ 0.05). Early life stress sensitivity was not associated significantly either with symptoms at baseline or with longitudinal symptom trajectories.
References
Achenbach, T. M. (1991). Manual for the child behavior checklist/4–18 and 1991 profile. Dept. of Psychiatry, University of Vermont.
Allen, A. P., Kennedy, P. J., Dockray, S., Cryan, J. F., Dinan, T. G., & Clarke, G. (2017). The trier social stress test: principles and practice. Neurobiology of Stress, 6, 113–126.
Aron, A. (1999). In E. N. Aron (Ed.), Statistics for psychology (2nd ed., pp. xxiii–643). Prentice-Hall, Inc.
Baldwin, J. S., & Dadds, M. R. (2007). Reliability and validity of parent and child versions of the multidimensional anxiety scale for children in Community samples. Journal of the American Academy of Child & Adolescent Psychiatry, 46(2), 252–260. https://doi.org/10.1097/01.chi.0000246065.93200.a1.
Belfer, M. L. (2008). Child and adolescent mental disorders: The magnitude of the problem across the globe. Journal of Child Psychology and Psychiatry, 49(3), 226–236. https://doi.org/10.1111/j.1469-7610.2007.01855.x.
Benner, A. D. (2011). The transition to High School: Current knowledge, future directions. Educational Psychology Review, 23(3), 299–328. https://doi.org/10.1007/s10648-011-9152-0.
Blum, R. W., Astone, N. M., Decker, M. R., & Mouli, V. C. (2014). A conceptual framework for early adolescence: A platform for research. International Journal of Adolescent Medicine and Health, 26(3), 321–331. https://doi.org/10.1515/ijamh-2013-0327.
Boomsma, A. (1985). Nonconvergence, improper solutions, and starting values in lisrel maximum likelihood estimation. Psychometrika, 50(2), 229–242. https://doi.org/10.1007/BF02294248.
Buske-Kirschbaum, A., Jobst, S., Wustmans, A., Kirschbaum, C., Rauh, W., & Hellhammer, D. (1997). Attenuated free cortisol response to psychosocial stress in children with atopic dermatitis. Psychosomatic Medicine, 59(4), 419–426. https://doi.org/10.1097/00006842-199707000-00012.
Conway, C. C., Hammen, C., Espejo, E. P., Wray, N. R., Najman, J. M., & Brennan, P. A. (2012). Appraisals of Stressful Life events as a genetically-linked mechanism in the stress–depression relationship. Cognitive Therapy and Research, 36(4), 338–347. https://doi.org/10.1007/s10608-011-9368-9.
Copeland, W. E., Angold, A., Shanahan, L., & Costello, E. J. (2014). Longitudinal patterns of anxiety from childhood to Adulthood: The Great Smoky Mountains Study. Journal of the American Academy of Child & Adolescent Psychiatry, 53(1), 21–33. https://doi.org/10.1016/j.jaac.2013.09.017.
Costello, E. J., Copeland, W., & Angold, A. (2011). Trends in psychopathology across the adolescent years: What changes when children become adolescents, and when adolescents become adults? Journal of Child Psychology and Psychiatry, 52(10), 1015–1025. https://doi.org/10.1111/j.1469-7610.2011.02446.x.
Curran, P. J., Obeidat, K., & Losardo, D. (2010). Twelve frequently asked questions about growth curve modeling. Journal of Cognition and Development: Official Journal of the Cognitive Development Society, 11(2), 121–136. https://doi.org/10.1080/15248371003699969.
Dahl, R. E., & Gunnar, M. R. (2009). Heightened stress responsiveness and emotional reactivity during pubertal maturation: Implications for psychopathology. Development and Psychopathology, 21(1), 1–6. https://doi.org/10.1017/S0954579409000017.
Danese, A., & Widom, C. S. (2020). Objective and subjective experiences of child maltreatment and their relationships with psychopathology. Nature Human Behaviour, 4(8), https://doi.org/10.1038/s41562-020-0880-3. Article 8.
Danese, A., & Widom, C. S. (2021). The subjective experience of Childhood Maltreatment in Psychopathology. JAMA Psychiatry, 78(12), 1307–1308. https://doi.org/10.1001/jamapsychiatry.2021.2874.
De Los Reyes, A., & Prinstein, M. J. (2004). Applying depression-distortion hypotheses to the assessment of peer victimization in adolescents. Journal of Clinical Child and Adolescent Psychology: The Official Journal for the Society of Clinical Child and Adolescent Psychology American Psychological Association Division, 53(2), 325–335. https://doi.org/10.1207/s15374424jccp3302_14. 33.
Dorn, L. D., Dahl, R. E., Woodward, H. R., & Biro, F. (2006). Defining the boundaries of early adolescence: A user’s guide to assessing Pubertal Status and Pubertal timing in Research with Adolescents. Applied Developmental Science, 10(1), 30–56. https://doi.org/10.1207/s1532480xads1001_3.
Duncan, T. E., & Duncan, S. C. (2009). The ABC’s of LGM: An introductory guide to latent variable growth curve modeling. Social and Personality Psychology Compass, 3(6), 979–991. https://doi.org/10.1111/j.1751-9004.2009.00224.x.
Duncan, T. E., Duncan, S. C., & Strycker, L. A. (2006). An introduction to latent variable growth curve modeling: Concepts, issues, and applications, 2nd ed (pp. xii, 261). Lawrence Erlbaum Associates Publishers.
Ebesutani, C., Bernstein, A., Martinez, J. I., Chorpita, B. F., & Weisz, J. R. (2011). The Youth Self Report: Applicability and validity across younger and older Youths. Journal of Clinical Child & Adolescent Psychology, 40(2), 338–346. https://doi.org/10.1080/15374416.2011.546041.
Eiland, L., & Romeo, R. D. (2013). Stress and the developing adolescent brain. Neuroscience, 249, 162–171. https://doi.org/10.1016/j.neuroscience.2012.10.048.
Faulstich, M. E., Carey, M. P., Ruggiero, L., Enyart, P., & Gresham, F. (1986). Assessment of depression in childhood and adolescence: An evaluation of the Center for Epidemiological Studies Depression Scale for children (CES-DC). The American Journal of Psychiatry, 143(8), 1024–1027. https://doi.org/10.1176/ajp.143.8.1024.
Fendrich, M., Weissman, M., & Warner, V. (1990). Screening for depressive disorder in children and adolescents: Validating the Center for epidemiologic Studies Depression Scale for Children. American Journal of Epidemiology, 131, 538–551. https://doi.org/10.1093/oxfordjournals.aje.a115529.
Fried, E. I. (2017). The 52 symptoms of major depression: Lack of content overlap among seven common depression scales. Journal of Affective Disorders, 208, 191–197. https://doi.org/10.1016/j.jad.2016.10.019.
Fried, E. I., Flake, J. K., & Robinaugh, D. J. (2022). Revisiting the theoretical and methodological foundations of depression measurement. Nature Reviews Psychology, 1(6), 358–368. https://doi.org/10.1038/s44159-022-00050-2.
Gee, D. G., Hanson, C., Caglar, L. R., Fareri, D. S., Gabard-Durnam, L. J., Mills-Finnerty, C., Goff, B., Caldera, C. J., Lumian, D. S., Flannery, J., Hanson, S. J., & Tottenham, N. (2022). Experimental evidence for a child-to-adolescent switch in human amygdala-prefrontal cortex communication: A cross-sectional pilot study. Developmental Science, e13238. https://doi.org/10.1111/desc.13238.
Golberstein, E., Wen, H., & Miller, B. F. (2020). Coronavirus disease 2019 (COVID-19) and mental health for children and adolescents. JAMA Pediatrics, 174(9), 819–820.
Granger, D. A., Hibel, L. C., Fortunato, C. K., & Kapelewski, C. H. (2009). Medication effects on salivary cortisol: Tactics and strategy to minimize impact in behavioral and developmental science. Psychoneuroendocrinology, 34(10), 1437–1448. https://doi.org/10.1016/j.psyneuen.2009.06.017.
Grant, K. E., Compas, B. E., Thurm, A. E., McMahon, S. D., & Gipson, P. Y. (2004). Stressors and child and adolescent psychopathology: Measurement issues and prospective Effects. Journal of Clinical Child & Adolescent Psychology, 33(2), 412–425. https://doi.org/10.1207/s15374424jccp3302_23.
Greenberg, M., & Abenavoli, R. (2016). Universal Interventions: Fully exploring their impacts and potential to produce Population-Level Impacts. Journal of Research on Educational Effectiveness, 10, 00–00. https://doi.org/10.1080/19345747.2016.1246632.
Greenberg, M., Domitrovich, C. E., Weissberg, R. P., & Durlak, J. A. (2017). Social and Emotional Learning as a Public Health Approach to Education. The Future of Children, 27(1), 13–32.
Hall, G. S. (1904). Adolescence: Its psychology and its relation to physiology, anthropology, sociology, sex, crime, religion, and education. Prentice-Hall.
Hammen, C. (2015). Stress sensitivity in psychopathology: Mechanisms and consequences. Journal of Abnormal Psychology, 124(1), https://doi.org/10.1037/abn0000040.
Hankin, B. L., Abramson, L. Y., Moffitt, T. E., Silva, P. A., McGee, R., & Angell, K. E. (1998). Development of depression from preadolescence to young adulthood: Emerging gender differences in a 10-year longitudinal study. Journal of Abnormal Psychology, 107, 128–140. https://doi.org/10.1037/0021-843X.107.1.128.
Harkness, K. L., Hayden, E. P., & Lopez-Duran, N. L. (2015). Stress sensitivity and stress sensitization in psychopathology: An introduction to the special section. Journal of Abnormal Psychology, 124(1), 1–3. https://doi.org/10.1037/abn0000041.
Hollenstein, T., & Lanteigne, D. (2014). Models and methods of emotional concordance. Biological Psychology, 98, 1–5. https://doi.org/10.1016/j.biopsycho.2013.12.012.
Ho, T. C., King, L. S., Leong, J. K., Colich, N. L., Humphreys, K. L., Ordaz, S. J., & Gotlib, I. H. (2017). Effects of sensitivity to life stress on uncinate fasciculus segments in early adolescence. Social Cognitive and Affective Neuroscience, 12(9), 1460–1469. https://doi.org/10.1093/scan/nsx065.
Ho, T. C., Pham, H. T., Miller, J. G., Kircanski, K., & Gotlib, I. H. (2020). Sympathetic nervous system dominance during stress recovery mediates associations between stress sensitivity and social anxiety symptoms in female adolescents. Development and Psychopathology, 32(5), 1914–1925. https://doi.org/10.1017/S0954579420001261.
Hughes, A. A., & Kendall, P. C. (2009). Psychometric Properties of the positive and negative affect scale for children (PANAS-C) in children with anxiety Disorders. Child Psychiatry and Human Development, 40(3), 343–352. https://doi.org/10.1007/s10578-009-0130-4.
Hu, L., & Bentler, P. M. (1999). Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling: A Multidisciplinary Journal, 6(1), 1–55. https://doi.org/10.1080/10705519909540118.
Infurna, M. R., Reichl, C., Parzer, P., Schimmenti, A., Bifulco, A., & Kaess, M. (2016). Associations between depression and specific childhood experiences of abuse and neglect: A meta-analysis. Journal of Affective Disorders, 190, 47–55.
Kamata, A., Nese, J. F. T., Patarapichayatham, C., & Lai, C. F. (2013). Modeling Nonlinear Growth With Three Data Points: Illustration With Benchmarking Data. Assessment for Effective Intervention, 38(2), 105–116. https://doi.org/10.1177/1534508412457872.
Kessler, R. C., Amminger, G. P., Aguilar-Gaxiola, S., Alonso, J., Lee, S., & Ustun, T. B. (2007). Age of onset of mental disorders: A review of recent literature. Current Opinion in Psychiatry, 20(4), 359–364. https://doi.org/10.1097/YCO.0b013e32816ebc8c.
Kessler, R. C., Avenevoli, S., Costello, E. J., Georgiades, K., Green, J. G., Gruber, M. J., He, J., Koretz, D., McLaughlin, K. A., Petukhova, M., Sampson, N. A., Zaslavsky, A. M., & Merikangas, K. R. (2012). Prevalence, persistence, and Sociodemographic Correlates of DSM-IV Disorders in the National Comorbidity Survey Replication adolescent supplement. Archives of General Psychiatry, 69(4), 372–380. https://doi.org/10.1001/archgenpsychiatry.2011.160.
Kilford, E. J., Garrett, E., & Blakemore, S. J. (2016). The development of social cognition in adolescence: An integrated perspective. Neuroscience & Biobehavioral Reviews, 70, 106–120.
King, L. S., Colich, N. L., LeMoult, J., Humphreys, K. L., Ordaz, S. J., Price, A. N., & Gotlib, I. H. (2017). The impact of the severity of early life stress on diurnal cortisol: The role of puberty. Psychoneuroendocrinology, 77, 68–74. https://doi.org/10.1016/j.psyneuen.2016.11.024.
Kline, R. B. (2016). Principles and practice of structural equation modeling (Fourth edition.). The Guilford Press.
Kovacs, M. (2015). Children’s Depression Inventory (CDI and CDI 2). The encyclopedia of clinical psychology (pp. 1–5). John Wiley & Sons, Ltd. https://doi.org/10.1002/9781118625392.wbecp419.
Krackow, E., & Rudolph, K. D. (2008). Life stress and the accuracy of cognitive appraisals in depressed youth. Journal of Clinical Child and Adolescent Psychology: The Official Journal for the Society of Clinical Child and Adolescent Psychology American Psychological Association Division, 53(2), 376–385. https://doi.org/10.1080/15374410801955797. 37.
Lanteigne, D. M., Flynn, J. J., Eastabrook, J. M., & Hollenstein, T. (2014). Discordant patterns among emotional experience, arousal, and expression in adolescence: Relations with emotion regulation and internalizing problems. Canadian Journal of Behavioural Science / Revue Canadienne Des Sciences Du Comportement, 46(1), 29–39. https://doi.org/10.1037/a0029968.
LeMoult, J. (2020). From stress to Depression: Bringing together cognitive and Biological Science. Current Directions in Psychological Science, 29(6), 592–598. https://doi.org/10.1177/0963721420964039.
Leproult, R., Copinschi, G., Buxton, O., & Van Cauter, E. (1997). Sleep loss results in an elevation of cortisol levels the next evening. Sleep, 20(10), 865–870.
Li, M., D’Arcy, C., & Meng, X. (2016). Maltreatment in childhood substantially increases the risk of adult depression and anxiety in prospective cohort studies: Systematic review, meta-analysis, and proportional attributable fractions. Psychological Medicine, 46(4), 717–730.
Linares, N. N., Charron, V., Ouimet, A. J., Labelle, P. R., & Plamondon, H. (2020). A systematic review of the trier social stress test methodology: Issues in promoting study comparison and replicable research. Neurobiology of Stress, 13, 100235.
March, J. S., Parker, J. D., Sullivan, K., Stallings, P., & Conners, C. K. (1997). The multidimensional anxiety scale for children (MASC): Factor structure, reliability, and validity. Journal of the American Academy of Child and Adolescent Psychiatry, 36(4), 554–565. https://doi.org/10.1097/00004583-199704000-00019.
Marshall, W. A., & Tanner, J. M. (1968). Growth and physiological development during adolescence. Annual Review of Medicine, 19(1), 283–300. https://doi.org/10.1146/annurev.me.19.020168.001435.
McLaughlin, K. A., & King, K. (2015). Developmental trajectories of anxiety and depression in early adolescence. Journal of Abnormal Child Psychology, 43, 311–323.
Merikangas, K. R., He, J., Burstein, M., Swanson, S. A., Avenevoli, S., Cui, L., Benjet, C., Georgiades, K., & Swendsen, J. (2010). Lifetime prevalence of Mental Disorders in U.S. adolescents: Results from the National Comorbidity Survey replication–adolescent supplement (NCS-A). Journal of the American Academy of Child & Adolescent Psychiatry, 49(10), 980–989. https://doi.org/10.1016/j.jaac.2010.05.017.
Merikangas, K. R., Nakamura, E. F., & Kessler, R. C. (2009). Epidemiology of mental disorders in children and adolescents. Dialogues in Clinical Neuroscience, 11(1), 7–20. https://doi.org/10.31887/DCNS.2009.11.1/krmerikangas.
Morken, I. S., Viddal, K. R., von Soest, T., & Wichstrøm, L. (2023). Explaining the female preponderance in adolescent Depression—A Four-Wave Cohort Study. Research on Child and Adolescent Psychopathology, 51(6), 859–869. https://doi.org/10.1007/s10802-023-01031-6.
Mueller, R. O., & Hancock, G. R. (2018). Structural equation modeling. The reviewer’s guide to quantitative methods in the Social Sciences. Second). Routledge.
Murtaugh, P. A. (1998). Methods of variable selection in regression modeling. Communications in Statistics - Simulation and Computation, 27(3), 711–734. https://doi.org/10.1080/03610919808813505.
Nolen-Hoeksema, S., & Girgus, J. S. (1994). The emergence of gender differences in depression during adolescence. Psychological Bulletin, 115(3), 424–443. https://doi.org/10.1037/0033-2909.115.3.424.
Pruessner, J. C., Kirschbaum, C., Meinlschmid, G., & Hellhammer, D. H. (2003). Two formulas for computation of the area under the curve represent measures of total hormone concentration versus time-dependent change. Psychoneuroendocrinology, 28(7), 916–931. https://doi.org/10.1016/S0306-4530(02)00108-7.
Pruessner, J. C., Wolf, O. T., Hellhammer, D. H., Buske-Kirschbaum, A., von Auer, K., Jobst, S., Kaspers, F., & Kirschbaum, C. (1997). Free cortisol levels after awakening: A Reliable Biological marker for the Assessment of Adrenocortical Activity. Life Sciences, 61(26), 2539–2549. https://doi.org/10.1016/S0024-3205(97)01008-4.
Racine, N., McArthur, B. A., Cooke, J. E., Eirich, R., Zhu, J., & Madigan, S. (2021). Global prevalence of depressive and anxiety symptoms in children and adolescents during COVID-19: A Meta-analysis. JAMA Pediatrics, 175(11), 1142–1150. https://doi.org/10.1001/jamapediatrics.2021.2482.
Ribbe, D. (1996). Psychometric review of Traumatic Events Screening Inventory for Children (TESI-C). In Measurement of stress, trauma, and adaptation (pp. 386–387). Sidran.
Romeo, R. D., & McEwen, B. S. (2006). Stress and the adolescent brain. Annals of the New York Academy of Sciences, 1094(1), 202–214. https://doi.org/10.1196/annals.1376.022.
Rosseel, Y. (2012). lavaan: An R Package for Structural equation modeling. Journal of Statistical Software, 48, 1–36. https://doi.org/10.18637/jss.v048.i02.
Rosseel, Y. (2015). The Lavaan Tutorial. Ghent University.
Rudolph, K. D., & Hammen, C. (1999). Age and gender as determinants of stress exposure, Generation, and reactions in youngsters: A transactional perspective. Child Development, 70(3), 660–677. https://doi.org/10.1111/1467-8624.00048.
Sawyer, S. M., Afifi, R. A., Bearinger, L. H., Blakemore, S. J., Dick, B., Ezeh, A. C., & Patton, G. C. (2012). Adolescence: A foundation for future health. Lancet (London England), 379(9826), 1630–1640. https://doi.org/10.1016/S0140-6736(12)60072-5.
Saylor, C. F., Finch, A. J., Spirito, A., & Bennett, B. (1984). The children’s Depression Inventory: A systematic evaluation of psychometric properties. Journal of Consulting and Clinical Psychology, 52(6), 955–967. https://doi.org/10.1037/0022-006X.52.6.955.
Schermelleh-Engel, K., Moosbrugger, H., & Müller, H. (2003). Evaluating the fit of structural equation models: Tests of significance and descriptive goodness-of-fit measures. Methods of Psychological Research, 8(2), 23–74.
Shirtcliff, E. A., Dahl, R. E., & Pollak, S. D. (2009). Pubertal Development: Correspondence between Hormonal and Physical Development. Child Development, 80(2), 327–337. https://doi.org/10.1111/j.1467-8624.2009.01263.x.
Solmi, M., Radua, J., Olivola, M., Croce, E., Soardo, L., Salazar de Pablo, G., Il Shin, J., Kirkbride, J. B., Jones, P., Kim, J. H., Kim, J. Y., Carvalho, A. F., Seeman, M. V., Correll, C. U., & Fusar-Poli, P. (2022). Age at onset of mental disorders worldwide: Large-scale meta-analysis of 192 epidemiological studies. Molecular Psychiatry, 27(1), https://doi.org/10.1038/s41380-021-01161-7.
Sommerfeldt, S. L., Schaefer, S. M., Brauer, M., Ryff, C. D., & Davidson, R. J. (2019). Individual differences in the Association between subjective stress and heart rate are related to psychological and physical well-being. Psychological Science, 30(7), 1016–1029. https://doi.org/10.1177/0956797619849555.
Statistics Canada (2021). Distribution of total income by census family type and age of older partner, parent, or individual
Statistics Canada (2022). Census Profile (2021 Census).
Vanaelst, B., De Vriendt, T., Huybrechts, I., Rinaldi, S., & De Henauw, S. (2012). Epidemiological approaches to measure childhood stress. Paediatric and Perinatal Epidemiology, 26(3), 280–297. https://doi.org/10.1111/j.1365-3016.2012.01258.x.
van Buuren, S., & Groothuis-Oudshoorn, K. (2011). Mice: Multivariate imputation by chained equations in R. Journal of Statistical Software, 45, 1–67. https://doi.org/10.18637/jss.v045.i03.
Walker, E. F., Sabuwalla, Z., & Huot, R. (2004). Pubertal neuromaturation, stress sensitivity, and psychopathology. Development and Psychopathology, 16(4), 807–824. https://doi.org/10.1017/S0954579404040027.
Wang, J., & Wang, X. (2019). Structural equation modeling: Applications using Mplus. John Wiley & Sons.
Wang, J., & Wang, X. (2020). Structural equation modeling: Applications using Mplus (Second edition). Wiley.
Wolfram, M., Bellingrath, S., & Kudielka, B. M. (2011). The cortisol awakening response (CAR) across the female menstrual cycle. Psychoneuroendocrinology, 36(6), 905–912. https://doi.org/10.1016/j.psyneuen.2010.12.006.
Funding
This research was supported by a Vanier Canada Graduate Fellowship to EJ; a Michael Smith Foundation for Health Research Trainee Award, a Killam Postdoctoral Fellowship, a Social Sciences and Humanities Research Council (SSHRC) Postdoctoral Fellowship, and a Women’s Health Research Institute Postdoctoral Award to KR; a SSHRC Doctoral Fellowship to AT; and Canadian Institute of Health Research (CIHR) Grant F17-03749 and Michael Smith Foundation for Health Research Scholar Award 17713 to JL. Beyond this funding, my co-authors and I do not have any interests that influence the research.
Author information
Authors and Affiliations
Contributions
Ellen Jopling and Joelle LeMoult were involved in the study’ conception and design. All authors contributed to data collection and preparation. Formal analysis was performed by Ellen Jopling and Katerina Rnic. The first draft of the manuscript was written by Ellen Jopling and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. Joelle LeMoult supervised the work.
Corresponding author
Ethics declarations
Ethics Approval
This study was approved by The University of British Columbia’s (UBC) Behavioural Research Ethics Board (BREB: #H17-01901) and is in line with the principles of the Declaration of Helsinki.
Informed Consent
Informed consent was obtained from legal guardians, and informed assent was obtained from all youth.
Competing interests
The authors have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jopling, E., Rnic, K., Jameson, T. et al. Discordance Indices of Stress Sensitivity and Trajectories of Internalizing Symptoms in Adolescence. Res Child Adolesc Psychopathol 51, 1521–1533 (2023). https://doi.org/10.1007/s10802-023-01095-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10802-023-01095-4