Abstract
This study was designed to investigate the protective effects of extracellular superoxide dismutase (SOD3) against amyloid beta (Aβ25–35)-induced damage in human neuroblastoma SH-SY5Y cells and to elucidate the mechanisms responsible for this beneficial effect. SH-SY5Y cells overexpressing SOD3 were generated by adenoviral vector-mediated infection and Aβ25–35 was then added to the cell culture system to establish an in vitro model of oxidative stress. Cell viability, the generation of intracellular reactive oxygen species (ROS), the expression and activity of antioxidant enzymes, the levels of lipid peroxidation malondialdehyde (MDA), the expression of mitochondrial apoptosis-related genes and calcium images were examined. Following Aβ25–35 exposure, SOD3 overexpression promoted the survival of SH-SY5Y cells, decreased the production of ROS, decreased MDA and calcium levels, and decreased cytochrome c, caspase-3, caspase-9 and Bax gene expression. Furthermore, SOD3 overexpression increased the expression and activity of antioxidant enzyme genes and Bcl-2 expression. Together, our data demonstrate that SOD3 ameliorates Aβ25–35-induced oxidative damage in neuroblastoma SH-SY5Y cells by inhibiting the mitochondrial pathway. These data provide new insights into the functional actions of SOD3 on oxidative stress-induced cell damage.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is the most common type of dementia in the elderly. AD is a progressive neurodegenerative disorder clinically characterized by cognitive decline that includes impairment in learning, episodic memory, decision making and orientation (Blennow et al. 2006). One of the major histopathological features of AD is the appearance of extracellular amyloid plaques that are composed principally of fibrillar β-amyloid (Aβ) peptide (Wilquet and De Strooper 2004). Aβ neurotoxic effects have been reported to be a hallmark of AD in vitro and in vivo.
Aβ invokes a cascade of oxidative damage to neurons and eventually leads to neuronal death in AD (Zhang et al. 2010). A previous study has demonstrated that Aβ generates free radicals in the synaptosomal membranes in the neocortex after fragmenting (Hensley et al. 1995). Another study has demonstrated that Aβ leads to free radical-induced oxidative stress, resulting in peroxidation and cell death (Markesbery and Carney 1999). Zhang et al. (2010) indicated that intracellular ROS levels markedly increased in a cellular model of AD induced by Aβ25–35. The generation of reactive oxygen species (ROS), such as hydrogen peroxide and hydroxyl radicals, induced by Aβ is a key molecular mechanism underlying the pathogenesis of AD (Tabner et al. 2010).
ROS, including the superoxide anion radical (O2 −), the hydroxyl radical (OH) and hydrogen peroxide (H2O2), are products of normal metabolic reactions in cells and are usually formed at low levels. Oxidative stress occurs as a result of an imbalance between ROS formation and the capacity of antioxidant defences and is widely implicated in neuronal cell death (Lobo et al. 2010). To offset the detrimental effects of ROS, the human body has innate defence mechanisms in the form of antioxidant enzymes such as superoxide dismutase (SOD), glutathione peroxidase (GPx) and catalase (CAT), among others. Hence, a series of antioxidants are known to delay or prevent the oxidation of cellular oxidizable substrates, including protecting against Aβ-induced neurotoxicity (Li et al. 2008).
SOD is the first and most important antioxidant defence system against ROS, particularly superoxide anion radicals (Fukai et al. 2002). SOD is responsible for catalyzing the conversion of superoxide anions into hydrogen peroxide (Zelko et al. 2002), which is in turn further metabolized into water and oxygen by CAT. Three forms of SOD, cytoplasmic SOD (SOD1), mitochondrial SOD (SOD2) and extracellular SOD (SOD3) are present in mammals (Miao 2009). SOD activity has been found to be significantly lower in the cortex and hippocampus of Tg2576 mice compared with normal mice (Chelikani et al. 2004). In a previous report, chronic treatment with a low concentration of H2O2 (5 µM) was found to decrease SOD2 activity in HeLa cells and the authors concluded that SOD2 activity is affected by ROS (Miguel et al. 2009). SOD2, but not the cytosolic SOD1, had a protective effect against oxidative stress-mediated neuronal cell death (Fukui and Zhu 2010). It has been shown that, although SOD3 is expressed at lower levels in the brain compared with other SODs, it is essential for the protection against oxidative damage (Van Rheen et al. 2011). However, little is known about the roles of SOD3 in oxidative stress-induced neuronal cell death.
It is well known that ROS play a critical role in the activation of the apoptotic process via mitochondria-dependent and mitochondria-independent pathways (Sinha et al. 2013). There is ample literature supporting a crucial role for mitochondrial dysfunction in AD, with altered energy metabolism and ROS production being the major correlates (Lin and Beal 2006). It is widely believed that Aβ is responsible for these mitochondrial alterations, although the mechanism has not yet been fully elucidated (Moreira et al. 2010). Mitochondria are essential for the intrinsic apoptosis pathway, and it has been shown that mitochondrial dysfunction leads to apoptotic cell death (Green and Kroemer 2004). Endogenous antioxidants such as mitochondrial SOD2, which localizes to the mitochondrial matrix and catalyses the dismutation of superoxide radicals, normally regulates the ROS generated in the mitochondria (Kasahara et al. 2005).
In the present study, we hypothesized that SOD3 overexpression provides beneficial effects to SH-SY5Y cells exposed to Aβ25–35 and that the beneficial effect of SOD3 against Aβ25–35-induced SH-SY5Y cell death occurs via the mitochondria-dependent pathway.
Materials and Methods
Cell Culture
The SH-SY5Y cell line was a gift from Prof. He Gui-Qiong at the Chongqing Medical University and was cultured in DMEM (HyClone, Logan, UT, USA) supplemented with 10 % FBS (Tian Jin Hao Yang Biological Manufacture CO., LTD, Tianjin, China), 1 % penicillin–streptomycin (Beyotime Biotechnology, Nantong, China) in an incubator (Thermo Fisher, USA) at 37 °C in the presence of 5 % CO2.
Preparation of Aged Aβ25–35
As previously described (Liu et al. 2010), 99.6 % pure Aβ25–35 (Sangon Biotech, Shanghai, China) was dissolved in sterilized double-distilled water at a concentration of 1 mM and incubated in a capped vial at 37 °C for 7 days to form an aggregated form. The aggregated form of Aβ25–35 was used for the subsequent experiments.
Construction of the Ad-SOD3-EGFP Adenoviral Expression Vector
Ad-SOD3-EGFP, an adenoviral vector containing the human SOD3 gene and a nuclear-targeted enhanced green fluorescence protein (EGFP) gene under the control of the cytomegalovirus (CMV) promoter, was constructed in our laboratory. Briefly, the Homo sapiens SOD3 gene was synthesized with insert sites (NotI and HindIII) (Sangon, Shanghai, China) according to the coding sequence in GenBank. Then, the restriction enzyme digestion product of the T vector containing SOD3 and the adenovirus shuttle vector pDC316-mCMV-EGFP was ligated into pDC316-SOD3-EGFP by T4 DNA ligase (TaKaRa, Otsu Japan). pDC316-SOD3-EGFP was linearized by PmeI, transformed into competent DH-5α cells, amplified, extracted and purified (TaKaRa, Otsu Japan). pDC316-SOD3-EGFP and pBHGloxΔE1, 3Cre were co-transfected into HEK293 cells by Lipofectamine™ 2000 (Invitrogen, Carlsbad, CA, USA) to obtain the adenoviral expression vector Ad-SOD3-EGFP. The retrieved virus DNA was amplified by PCR, and after repeated infections, amplifications and purifications, the virus titre of adenovirus Ad-SOD3-EGFP was determined as 1.6 × 1010 IU/ml by the TCID50 method.
Gene Transfer into SH-SY5Y Cells
SH-SY5Y cells were seeded on 6-well plates at 1.5 × 105 cells per well in 1.5 mL of complete growth culture medium, incubated for 2 h and infected with the adenoviral expression vector Ad-SOD3-EGFP. Forty-eight hours after infection, the expression of SOD3 was detected by semi-quantitative RT-PCR. The primers are listed in Table 1.
CCK8 Assay
Cell viability was measured by CCK8 assay (cell counting kit-8, Dojindo Molecular Technologies, Tokyo, Japan). The SH-SY5Y cells were seeded at 1 × 104 cells per well in 100 μl of complete growth culture media. The cells were then exposed to various concentrations of the aggregated form of Aβ25–35 (20, 40, 60, 80, 100 μM) for 6 h. Control cells were cultured without any treatment. Finally, CCK-8 solution (10 μl/well) was added to the wells. After 2 h incubation at 37 °C, the absorbance of each well was determined at 450 nm using a microplate reader.
Cell Proliferation
SH-SY5Y cells were infected with either an empty vector (Ad-EGFP) or with Ad-SOD3-EGFP for 48 h. Then, SH-SY5Y cells were treated with Aβ25–35 at a final LD50 concentration of 40 μM for 6 h as determined by the CCK8 assay. These results were measured at 450 nm by a microplate reader and were expressed as the percentages of control values.
Intracellular Reactive Oxygen Species (ROS) Level
SH-SY5Y cells were incubated with adenoviral expression vector Ad-SOD3-EGFP for 72 h, and 40 μM Aβ25–35 was added for the final 6 h. The cells were also treated with 40 μM Aβ25–35 for 6 h as a control. ROS were detected with the cell-permeable, peroxide-sensitive fluorophore (Life Technologies, USA), according to the manufacturer’s instructions. SH-SY5Y cells were incubated with 5 μmol/l CellROX Orange reagent for 30 min at 37 °C and then washed twice with pre-warmed PBS. A Beckman Gallios flow cytometer (Beckman Coulter, California, USA) was used to measure ROS by the fluorescence emission of the CellROX dye. The reported fluorescence intensity values representing the arithmetic means of the results were determined for 10,000 analysed cells. The cultured cells were illuminated at 488 nm and emitted at 525–530 nm.
Semi-quantitative Polymerase Chain Reaction
SH-SY5Y cells were treated as described above for the ROS level tests and subsequently harvested with 0.25 % trypsin containing 0.02 % ethylenediaminetetraacetic acid (EDTA) (Beyotime Biotechnology, Nantong, China). Total RNA was extracted from the SH-SY5Y cells with TRIzol reagent according to the manufacturer’s protocol (TaKaRa, Tokyo, Japan). The reaction system (20 μl) contained cDNA (5 μl), 10 × buffer (2 μl), 25 mmol/L MgCl2 (0.8 μl), 2.5 mmol/L dNTP (2 μl), DNA polymerase (0.2 μl; TaKaRa, Tokyo, Japan) and upstream and downstream primers (1 μl each). PCR amplification conditions were performed as follows: initial denaturation at 95 °C for 5 min, 35 cycles of denaturation at 56 °C for 30 s, annealing at 60 °C for 60 s, elongation at 72 °C for 60 s and final elongation at 72 °C for 7 min. The samples were analysed by gel electrophoresis on 2.0 % agarose gels (1 × TAE buffer) containing 0.5 μg/ml bromoethane, visualized by imaging with an ultraviolet projection reflectometer (ChemiDoc MP, Bio-Rad, Hercules, CA, USA), and quantified by densitometry using ImageJ software (Bio-Rad, Hercules, USA). All primers were synthesized by Sangon Biotech (Shanghai, China). The primer sets are listed in Table 1.
Enzyme Activity Assays
SH-SY5Y cells were treated as described above for the ROS level tests, after which we assayed the enzyme activity of the cells. The activities of three enzymes, superoxide dismutase (SOD; EC1.15.1.1), glutathione peroxidase (GPx; EC 1.11.1.9) and catalase (CAT; EC1.11.1.6), were determined using commercial kits according to the manufacturer’s protocols (Nanjing Jiancheng Bioengineering Institute, Nanjing, China). The enzyme activity assays were carried out using a UV–visible spectrophotometer (UV-7504, Shanghai, China).
Analysis of Lipid Peroxidation
SH-SY5Y cells were treated as described above, after which we analysed lipid peroxidation of the cells, which was determined as the amount of malondialdehyde (MDA) based on the spectrophotometer measurement of a red-complex produced during the reaction of thiobarbituric acid (TBA) with MDA. A microplate reader (UV-7504, Shanghai, China) was used to measure the absorbance of cellular MDA at 532 nm, and the MDA content was calculated according to the detailed instructions of the MDA assay kit (Nanjing Jiancheng Bioengineering Institute, Nanjing, China).
Calcium Imaging
SH-SY5Y cells were treated as described above, and we then used calcium imaging to determine the [Ca2+]i levels using Fluo-3 AM (Sigma-Aldrich, St. Louis, USA), using an adaptation of a previously described method (Huang et al. 2012). Briefly, the prepared cells were loaded with the fluorescent calcium probe Fluo-3 AM (10 µM) in the dark for 30 min at 37 °C, washed twice with PBS and centrifuged at 300×g for 5 min to remove free Fluo-3 AM. Fluo-3 AM loaded cells were re-suspended, incubated for 20 min at 37 °C and then illuminated at 488 nm, and the emission light at 543 nm was detected.
Statistical Analysis
All of the experiments were conducted at least three times, and the representative data are expressed as the mean ± SD. The SOD3 expression in the SH-SY5Y cells was evaluated using a t-test, and other comparisons were evaluated using a one-way ANOVA followed by Tukey’s test. All of the statistical analyses were performed using SPSS statistics software, and p < 0.05 was considered statistically significant.
Results
SOD3 is Highly Expressed in Infected SH-SY5Y Cells Under Optimal Conditions
Based on our preliminary data, an MOI value of 100 was selected as the optimal condition for infection. When the MOI exceeded 100, infection efficiency no longer increased, and MOI values of 200 or more led to negative effects on cell growth. Therefore, adenoviral infection was performed at an MOI value of 100, and SOD3 transcription was analysed by semi-quantitative RT-PCR. In infected SH-SY5Y cells, SOD3 expression was 4.5-fold higher than in control cells (t 0.05/2,6 = 5.1, p < 0.001, Fig. 1a, b).
SOD3 was highly expressed in infected SH-SY5Y cells, and SOD3 overexpression prevented Aβ25–35-induced cell death. a SOD3 was highly expressed in neuroblastoma SH-SY5Y cells following infection with the Ad-SOD3-EGFP adenoviral vector. b SOD3 expression level in SH-SY5Y cells was normalized to the β-actin expression level, as determined by densitometric analysis (t 0.05,6 = 5.112, p < 0.001). c SH-SY5Y cells were exposed to increasing concentrations of Aβ25–35 (20, 40, 60, 80, 100 μM) for 6 h, and cell death was detected by CCK8. d SH-SY5Y cells were exposed to Aβ25–35 (40 μM) for 6 h in the presence or absence of SOD3 overexpression. Data are expressed as the mean ± SD (n = 6). **p < 0.001
SOD3 Overexpression Prevents Aβ25–35-Induced Cell Death in SH-SY5Y Cells
First, we examined the effect of increasing doses of Aβ25–35 (20, 40, 60, 80 and 100 μM) on SH-SY5Y cell death after 6 h of exposure. As shown by the CCK8 cell viability assay, exposure of SH-SY5Y cells to Aβ25–35 (40 μM) for 6 h resulted in approximately 50 % cell death (20 μM Aβ25–35 0.7 ± 0.1, 40 μM Aβ25–35 0.5 ± 0.1, 60 μM Aβ25–35 0.4 ± 0.2, 80 μM Aβ25–35 0.3 ± 0.0, 100 μM Aβ25–35 0.1 ± 0.3, F 0.05/6,6 = 27.5; p < 0.001, Fig. 1c). Thus, a concentration of 40 μM Aβ25–35 was chosen for subsequent experiments.
To determine whether SOD3 could prevent Aβ25–35-induced cell death, SH-SY5Y cells were incubated for 72 h with SOD3 adenovirus, followed by incubation with Aβ25–35 for 3 h, and the resulting level of cell death was observed to significantly decrease (CTRL 1.0 ± 0.0, Ad 1.0 ± 0.0, SOD3-Ad 1.3 ± 0.5, Aβ25–35 0.7 ± 0.2, Aβ25–35 + Ad 0.6 ± 0.1, Aβ25–35 + SOD3-Ad, 1.2 ± 0.1, F 0.05/6,6 = 12.9, p < 0.001) (Fig. 1d). We excluded further analysis of adenovirus Ad-EGFP because no beneficial effect was observed from the infection of SH-SY5Y cells with Ad-EGFP (Fig. 1d).
SOD3 Overexpression in SH-SY5Y Cells Prevents the Aβ25–35-Induced Activation of the Mitochondria-Mediated Apoptosis Pathway
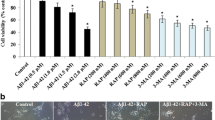
Mitochondria-mediated apoptosis has been suggested to be involved in Aβ25–35-induced cell toxicity. We therefore investigated whether the beneficial role of SOD3 in preventing Aβ25–35-induced SH-SY5Y cell death involved the inhibition of the mitochondria-mediated apoptosis pathway. Mitochondria-mediated apoptosis requires the interplay of a number of pro- and anti-apoptotic B-cell lymphoma-2 (Bcl-2) family proteins and the caspase cascade (Soriano and Scorrano 2011). To assess the status of the mitochondria-mediated apoptosis pathway, we measured the levels of the pro-apoptotic molecules, including cytochrome c, caspase 3, caspase 9, and Bax, as well as the anti-apoptotic molecule Bcl-2 in SH-SY5Y cells by RT-PCR. Exposure of the cells to Aβ25–35 resulted in significantly higher levels of cytochrome c (29.3 ± 0.9, F 0.05/3,3 = 76.7, p < 0.001), caspase-3 (34.1 ± 1.0, F 0.05/3,3 = 631.0, p < 0.001), caspase-9 (31.8 ± 0.2, F 0.05/3,3 = 17.3, p < 0.001), Bax (33.3 ± 0.4, F 0.05/3,3 = 52.2, p < 0.001) and lower levels of Bcl-2 (20.9 ± 0.8, F 0.05/3,3 = 11.6, p < 0.001) in SH-SY5Y cells compared with controls (cytochrome c 24.1 ± 0.1, F 0.05/3,3 = 76.7, p < 0.001; caspase-3 19.4 ± 0.2, F 0.05/3,3 = 631.0, p < 0.001; caspase-9 22.6 ± 0.4, F 0.05/3,3 = 17.3, p < 0.001; Bax 24.1 ± 0.2, F 0.05/3,3 = 52.2, p < 0.001; Bcl-2 25.7 ± 0.4, F 0.05/3,3 = 11.6, p < 0.001) (Fig. 2). The levels of cytochrome c (24.1 ± 0.1), caspase-3 (19.4 ± 0.2), caspase-9 (22.6 ± 0.4) and Bax (24.1 ± 0.2) in SOD3-infected SH-SY5Y cells were significantly lower than those in the cells treated with Aβ25–35 alone (Fig. 2). The level of Bcl-2 (25.7 ± 0.4) in SOD3-infected SH-SY5Y cells was significantly higher than in cells treated with Aβ25–35 alone (Fig. 2f).
SOD3 overexpression prevents the Aβ25–35-induced activation of the mitochondria-mediated apoptosis pathway in SH-SY5Y cells. a The expression of mitochondrial apoptotic-related genes was examined by RT-PCR and cytochrome c (b), caspase-3 (c), caspase-9 (d), Bax (e) and Bcl-2 (f) were normalized to the expression level of β-actin (F 0.05,6 = 3.223, p = 0.027). Data are expressed as the mean ± SD (n = 6). *p < 0.05, **p < 0.001
SOD3 Overexpression Modulates the Redox State in SH-SY5Y Cells
Because oxidative stress has been shown to trigger and sustain the pathogenesis of Aβ25–35-induced cell toxicity, we examined whether SOD3 treatment decreased oxidative stress by determining the MDA content, and whether treatment restored antioxidant status by determining the gene expression and enzymatic activities of SOD, CAT and GPx. In SOD3-infected SH-SY5Y cells, the MDA level (2.6 ± 0.7, F 0.05/3,6 = 14.0, p < 0.001) was significantly lower than that in cells treated with Aβ25–35 alone (4.6 ± 1.0) (Fig. 3a). In SOD3-infected SH-SY5Y cells, the expression levels of SOD1 (25.7 ± 0.7, F 0.05/3,6 = 14.2, p = 0.002), SOD2 (27.8 ± 1.1, F 0.05/3,6 = 127.3, p < 0.001), SOD3 (48.6 ± 6.4, F 0.05/3,6 = 85.2, p < 0.001), CAT (25.3 ± 2.4, F 0.05/3,6 = 12.9, p = 0.002) and GPx (26.2 ± 0.2, F 0.05/3,6 = 37.5, p < 0.001), and the enzymatic activities of total SOD (34.2 ± 1.2, F 0.05/3,3 = 187.5, p < 0.001), CAT (34.0 ± 3.3, F 0.05/3,3 = 7.2, p = 0.005) and GPx (50.2 ± 1.6, F 0.05/3,3 = 15.4, p < 0.001) were significantly higher than those levels in cells treated with Aβ25–35 alone (SOD1 expression level 21.5 ± 2.2, F 0.05/3,3 = 14.2, p = 0.002; SOD2 expression level 19.6 ± 0.6, F 0.05/3,3 = 127.3, p < 0.001; SOD3 expression level 11.1 ± 2.7, F 0.05/3,3 = 85.2, p < 0.001; CAT expression level 19.9 ± 2.1, F 0.05/3,3 = 12.9, p = 0.002; GPx expression level 21.7 ± 0.3, F 0.05/3,3 = 37.5, p < 0.001; total SOD enzymatic activity 25.5 ± 0.3, F 0.05/3,3 = 187.5, p < 0.001; CAT enzymatic activity 27.3 ± 5.0, F 0.05/3,3 = 7.2, p = 0.005; GPx enzymatic activity 22.5 ± 3.7, F 0.05/3,3 = 15.4, p < 0.001) (Fig. 3b–h).
SOD3 overexpression modulates the redox state of SH-SY5Y cells exposure to Aβ25–35. a Malondialdehyde (MDA) level in the cell supernatant was measured by a UV–visible spectrophotometer. b The enzymatic activities of total SOD (T-SOD), CAT and GPx in the cell supernatant were determined. c The expression of intracellular antioxidant enzyme genes was detected by RT-PCR, and the expression levels of SOD1 (d), SOD2 (e), SOD3 (f), GPx (g) and CAT (h) were normalized to the expression level of β-actin (F 0.05,6 = 12.877, p < 0.001). Data are expressed as the mean ± SD (n = 6). *p < 0.05; **p < 0.001
Exposure to Aβ25–35 resulted in significantly higher MDA levels (Fig. 3a), lower SOD1, SOD2, CAT and GPx expression levels (Fig. 3c–h), and lower SOD, CAT and GPx enzymatic activities in SH-SY5Y cells compared with controls (SOD1 expression level 25.9 ± 0.2, F 0.05/3,3 = 127.3, p < 0.001; SOD2 expression level 24.5 ± 0.3, F 0.05/3, 3 = 127.3, p < 0.001; SOD3 expression level 14.2 ± 3.6, F 0.05/3,3 = 85.2, p < 0.001; CAT expression level 26.0 ± 0.6, F 0.05/3,6 = 12.9, p = 0.002; GPx expression level 25.6 ± 0.3, F 0.05/3,3 = 37.5, p < 0.001; total SOD enzymatic activity 23.6 ± 0.9, F 0.05/3, 3 = 187.5, p < 0.001; CAT enzymatic activity 34.6 ± 3.5, F 0.05/3,3 = 7.2, p = 0.005; GPx enzymatic activity 46.6 ± 6.9, F 0.05/3,3 = 15.4, p < 0.001) (Fig. 3b–h).
SOD3 Overexpression in SH-SY5Y Cells Decreases Intracellular ROS Generation
The accumulation of ROS has been observed in Aβ25–35-induced cell toxicity, and mitochondria have been considered to be the targets sensitive to ROS. To determine whether SOD3 could decrease intracellular ROS levels, we used a ROS-sensitive dye, CellROX Orange. Exposure to Aβ25–35 resulted in significantly higher ROS levels (127.5 ± 8.0, F 0.05/3,3 = 13.7, p = 0.001) in SH-SY5Y cells compared with controls (106.0 ± 5.7, Fig. 4). The ROS levels (112.8 ± 5.9) were significantly lower in SOD3-infected SH-SY5Y cells than those in cells treated with Aβ25–35 alone (Fig. 4).
SOD3 overexpression decreases the generation of intracellular ROS in SH-SY5Y cells exposure to Aβ25–35. The generation of reactive oxygen species was analysed by flow cytometry in normal control cells (a), Aβ25–35 single-treated SH-SY5Y cells (b) and SOD3-infected SH-SY5Y cells. c The results were compared across the different treatments (d). Data are expressed as the mean ± SD (n = 3). *p < 0.05; **p < 0.001
SOD3 Overexpression Prevents Intracellular Ca2+ Overloading in SH-SY5Y Cells
Ca2+ overload is associated with mitochondrial dysfunction, which contribute to apoptosis. Exposure to Aβ25–35 resulted in a significantly higher [Ca2+]i (161.7 ± 2.9, F 0.05/3,3 = 13.1, p = 0.002) in SH-SY5Y cells compared with controls (127.0 ± 11.8, Fig. 5). The [Ca2+]i in SOD3-infected SH-SY5Y cells (136.7 ± 12.1) was significantly lower than that in cells treated with Aβ25–35 alone (Fig. 5).
SOD3 overexpression prevents intracellular Ca2+ overloading in SH-SY5Y cells exposure to Aβ25–35. [Ca2+]i was analysed using Ca2+ imaging in control cells (a), Aβ25–35 single-treated SH-SY5Y cells (b) and SOD3 infected SH-SY5Y cells (c). The results were compared between different treatments (d). Data are expressed as the mean ± SD (n = 3). *p < 0.05; **p < 0.001
Summary of Results
The outcome measures obtained with adenoviral SOD3-infected SH-SY5Y cells relative to those exposed to Aβ25–35 are listed in Table 2. The analysis of five mitochondrial apoptosis molecules, namely cytochrome c, caspase-3, caspase-9, Bax and Bcl-2, revealed that the expression of all genes except for Bcl-2 was 42 % higher in Aβ25–35-treated cells compared with controls (range +21 to +75 %, all differences significant). However, Bcl-2 gene expression was 22 % lower compared with controls. In SOD3-overexpressed cells, the expression of all mitochondrial apoptosis molecules except Bcl-2 was 41 % lower compared with cells treated with Aβ25–35 alone (range −21 to −71 %, all differences significant) but 4 % higher compared with controls (range −6 to +7 %, two of four of the differences were significant). Bcl-2 expression was similar between controls and SOD3-overexpressed cells (range: 0 to +3 %, no difference was significant). The extracellular enzymatic activities of T-SOD, CAT and GPx was 36 % higher in SOD3-treated SOD3-overexpressed cells compared with cells treated with Aβ25–35 alone (range +20 to +60 %, all differences significant) and 4 % higher compared with controls (range −1 to +8 %, two of three differences not significant). Lipid oxidation (MDA) was increased by 86 % after SOD3 treatment compared with that after treatment with Aβ25–35 alone and was similar to the control levels. The expression of enzymes SOD1, SOD2, GPx and CAT was 22 % higher in SOD3-overexpressed cells compared with those in cells treated with Aβ25–35 alone (range 16–33 %, all differences significant) and 5 % higher compared with those in controls (range −3 to +13 %, three of four differences not significant). After SOD treatment, the intracellular ROS levels were decreased 14 % compared with those in cells treated with Aβ25–35 alone and were not significantly different from controls. Calcium imaging in SOD3-overexpressed cells was better by 19 % compared with that in cells treated with Aβ25–35 alone and was not significantly different from controls. In summary, our data demonstrated that SOD3 treatment resulted in a 30 % improvement in all parameters tested compared with those in cells treated with Aβ25–35 alone (range −86 to +60 %, all differences significant) because SOD3 treatment restored these parameters to levels similar to control levels (range −6 to +13 %, eleven of fifteen differences not significant).
Discussion
AD is a neurodegenerative disease associated with ageing and is characterized by the deterioration of memory, learning and other cognitive functions due to the progressive loss of neuronal function (Tsunekawa et al. 2008). The cause of AD involves the accumulation of Aβ, oxidative stress, inflammation and dysfunction in several pathways including hormonal and mitochondrial pathways (Doraiswamy 2002). The increased proteolytic degradation of APP and aggregation and deposition of Aβ are considered to be two characteristic pathologies in the development and progression of AD (Tsunekawa et al. 2008). Aβ contributes to synaptic dysfunction and neuronal death and therefore contributes to cognitive impairment (Roher et al. 2009). Specifically, Aβ25–35 is the core toxic fragment of the full-length Aβ peptide (Kim et al. 2015).
Aβ25–35 can permeate through the cell membrane relatively more easily due to its smaller size. In addition, its toxicity is similar to that of Aβ1–40 and Aβ1–42 (Mattson et al. 1997). More importantly, Aβ25–35 is a particularly intractable peptide because it aggregates rapidly, unlike the full-length Aβ, which requires ageing for more than 1 week before it aggregates and becomes toxic (Hughes et al. 2000). As such, it is often used for in vitro studies of the neuroprotective effects of various drugs predicted to modulate Aβ toxicity (Yu et al. 2014). In our initial study, we used scrambled peptide in SH-SY5Y cells as negative control and no neurotoxicity in SH-SY5Y cells was observed (data not shown). Thus, we only used Aβ25–35 to induce neurotoxicity in SH-SY5Y cells.
The generation of ROS leading to oxidative damage and neuronal cell death plays an important role in the pathogenesis of neurodegenerative disorders (Paulsen et al. 2012), and antioxidants have been proposed to protect against Aβ25–35-induced toxicity in AD (Jung Choi et al. 2009). In the present study, ROS production increased after Aβ25–35 exposure and decreased after SOD3 treatment.
It is noteworthy that antioxidative systems, including antioxidant enzymes such as SOD and GPx and antioxidants such as GSH, have been shown to decrease the generation of free radicals. Increased expression of antioxidant enzymes attenuates AD phenotype (Dumont et al. 2009). SOD is the first and most important major line of antioxidant defence against ROS (Fukai et al. 2002). SODs are responsible for catalyzing the conversion of superoxide anions into hydrogen peroxide (Chiapinotto Spiazzi et al. 2015), which is then converted into water by catalase, glutathione peroxidase or peroxiredoxin. SOD activity was significantly diminished in the cortex and hippocampus of Tg2576 mice (Chelikani et al. 2004). Mammalian cells possess three distinct forms of SOD, namely copper–zinc SOD (CuZn-SOD or SOD1) located in the cytoplasm, manganese SOD (Mn-SOD or SOD2) found exclusively in the mitochondria, and extracellular SOD (EC-SOD or SOD3) present in the extracellular space (Zelko et al. 2002). In the study of Murakami (Murakami et al. 2011), the amounts of SOD1 protein were significantly decreased approximately 30 % in human AD cases as compared with non-AD cases, and no change in SOD2 or SOD3 levels was observed between AD and non-AD cases. As the frontal lobe was used for analysis in the Murakami’s study, the hippocampus in AD patients may show the differential expression profile of SOD as compared with the frontal lobe. Further study is needed to examine the SOD expression profile in different regions of AD cases.
Preventive antioxidants such as metal chelators, glutathione peroxidases and SOD enzymes including SOD1 (Marcus et al. 1998) and SOD2 (Nunomura et al. 2006) have been shown to be essential for neuronal survival and protection against oxidative damage (Gonzalez-Zulueta et al. 1998) and can be used to treat cognitive and behavioural symptoms of AD (Nunomura et al. 2006). The present study showed that the relevant reduction of SOD1, SOD2, SOD3, GPx and CAT gene expression was observed after 6 h of Aβ25–35 exposure, and SOD3 overexpression re-established the normal gene expression. SOD3 overexpression prevents the Aβ25–35-induced decreasing of SOD1 and SOD2 expression levels in SH-SY5Y cells. This observation may indicate a positive feedback loop in the antioxidant enzyme system in which SOD3 overexpression activated endogenous antioxidant defence system in SH-SY5Y cells against Aβ25–35.
SOD3 plays an important role in all stages of hippocampal neurogenesis and its associated cognitive functions (Van Rheen et al. 2011). Particularly intriguing is the role of SOD3; SOD3 is located mainly in the cytoplasm but can also be secreted into the extracellular space (Mondola et al. 2003). Therefore, it could detoxify the superoxide radical both within and outside of the cell. Our data confirmed the previous reports (Miguel et al. 2009; Sinha et al. 2013) that SOD3 overexpression promotes the survival of SH-SY5Y cells. However, it does not rule out the possibility of an important additional cytosolic role of SOD3. Further research is required to elucidate other roles of SOD3.
There is ample literature supporting a crucial role for mitochondrial dysfunction in AD, with altered energy metabolism and ROS production being the major correlates (Lin and Beal 2006; Moreira et al. 2010). It is widely believed that Aβ is responsible for these mitochondrial alterations, although the mechanism has not yet been fully elucidated (Moreira et al. 2010). It is generally accepted that Aβ could elevate oxidative stress and induce apoptotic cell death by initiating mitochondrial dysfunction, which is associated with changes in the proteins of Bcl-2 family, release of cytochrome c and activation of caspase-3 (Butterfield and Swomley 2013). In the present study, we used semi-quantitative RT-PCR to measure the gene expression levels of mitochondria-mediated apoptosis markers. We found that pretreatment of cells with SOD3 prior to Aβ25–35 exposure resulted in inhibition gene expression of cytochrome c, caspase-3, caspase-9 and Bax, and an increase in Bcl-2 expression induced by Aβ25–35 in SH-SY5Y cells. These data indicate that SOD3 overexpression could be used to ameliorate or treat neuroblastoma cell death through inhibition of mitochondrial apoptosis pathway.
MDA is an end product of lipid peroxidation and represents a reliable marker for lipid peroxidation in the AD model (Kim et al. 2015; Mattson et al. 1997). In the present study, SOD3 overexpression restored the lipid peroxidation level induced by Aβ25–35 in SH-SY5Y cells. These results suggest that oxidative overcharge could be restored by SOD3.
As mitochondria are subject to extensive oxidative damage, mitochondrial impairment causes disturbance of Ca2+ homeostasis and eventually results in apoptosis or necrosis (Witte et al. 2010). Our calcium imaging data demonstrated that SOD3 overexpression could restore Ca2+ homeostasis after oxidative stress.
In summary, we have demonstrated that SOD3 overexpression ameliorated Aβ25–35-induced oxidative damage in neuroblastoma SH-SY5Y cells through inhibition of the mitochondria-dependent pathway and provided new insights into the functional actions of SOD3 in oxidative stress-induced cell damage. To the best of our knowledge, this is the first study to evaluate and highlight the function of SOD3 against Aβ-induced cell insult.
References
Blennow K, de Leon MJ, Zetterberg H (2006) Alzheimer’s disease. Lancet 368:387–403
Butterfield DA, Swomley AM, Sultana R (2013) Amyloid beta-peptide (1-42)-induced oxidative stress in Alzheimer disease: importance in disease pathogenesis and progression. Antioxid Redox Signal 19:823–835
Chelikani P, Fita I, Loewen PC (2004) Diversity of structures and properties among catalases. Cell Mol Life Sci CMLS 61:192–208
Chiapinotto Spiazzi C, Bucco Soares M, Pinto Izaguirry A, Musacchio Vargas L, Zanchi MM, Frasson Pavin N, Ferreira Affeldt R, Seibert Lüdtke D, Prigol M, Santos FW (2015) Selenofuranoside ameliorates memory loss in Alzheimer-like sporadic dementia: AChE activity, oxidative stress, and inflammation involvement. Oxid Med Cell Longev 2015:976908
Doraiswamy PM (2002) Non-cholinergic strategies for treating and preventing Alzheimer’s disease. CNS Drugs 16:811–824
Dumont M et al (2009) Reduction of oxidative stress, amyloid deposition, and memory deficit by manganese superoxide dismutase overexpression in a transgenic mouse model of Alzheimer’s disease. FASEB J 23:2459–2466
Fukai T, Folz RJ, Landmesser U, Harrison DG (2002) Extracellular superoxide dismutase and cardiovascular disease. Cardiovasc Res 55:239–249
Fukui M, Zhu BT (2010) Mitochondrial superoxide dismutase SOD2, but not cytosolic SOD1, plays a critical role in protection against glutamate-induced oxidative stress and cell death in HT22 neuronal cells. Free Radic Biol Med 48:821–830
Gonzalez-Zulueta M, Ensz LM, Mukhina G, Lebovitz RM, Zwacka RM, Engelhardt JF, Oberley LW, Dawson VL, Dawson TM (1998) Manganese superoxide dismutase protects nNOS neurons from NMDA and nitric oxide-mediated neurotoxicity. J Neurosci 18:2040–2055
Green DR, Kroemer G (2004) The pathophysiology of mitochondrial cell death. Science 305:626–629
Hensley K, Hall N, Subramaniam R, Cole P, Harris M, Aksenov M, Aksenova M, Gabbita SP, Wu JF, Carney JM (1995) Brain regional correspondence between Alzheimer’s disease histopathology and biomarkers of protein oxidation. J Neurochem 65:2146–2156
Huang TT, Zou Y, Corniola R (2012) Oxidative stress and adult neurogenesis-effects of radiation and superoxide dismutase deficiency. Semin Cell Dev Biol 23:738–744
Hughes E, Burke RM, Doig AJ (2000) Inhibition of toxicity in the beta-amyloid peptide fragment beta-(25–35) using N-methylated derivatives: a general strategy to prevent amyloid formation. J Biol Chem 275(33):25109–25115
Jung Choi S, Kim MJ, Jin Heo H, Kim JK, Jin Jun W, Kim HK, Kim EK, Ok Kim M, Yon Cho H, Hwang HJ, Jun Kim Y, Shin DH (2009) Ameliorative effect of 1,2-benzenedicarboxylic acid dinonyl ester against amyloid beta peptide-induced neurotoxicity. Amyloid Int J Exp Clin Investig 16:15–24
Kasahara E, Lin LR, Ho YS, Reddy VN (2005) SOD2 protects against oxidation-induced apoptosis in mouse retinal pigment epithelium: implications for age-related macular degeneration. Invest Ophthalmol Vis Sci 46:3426–3434
Kim JH, Wang Q, Choi JM, Lee S, Cho EJ (2015) Protective role of caffeic acid in an Abeta25–35-induced Alzheimer’s disease model. Nutr Res Pract 9:480–488
Li RC, Pouranfar F, Lee SK, Morris MW, Wang Y, Gozal D (2008) Neuroglobin protects PC12 cells against beta-amyloid-induced cell injury. Neurobiol Aging 29:1815–1822
Lin MT, Beal MF (2006) Mitochondrial dysfunction and oxidative stress in neurodegenerative diseases. Nature 443:787–795
Liu X, Xu K, Yan M, Wang Y, Zheng X (2010) Protective effects of galantamine against Abeta-induced PC12 cell apoptosis by preventing mitochondrial dysfunction and endoplasmic reticulum stress. Neurochem Int 57:588–599
Lobo V, Patil A, Phatak A, Chandra N (2010) Free radicals, antioxidants and functional foods: impact on human health. Pharmacogn Rev 4:118–126
Marcus DL, Thomas C, Rodriguez C, Simberkoff K, Tsai JS, Strafaci JA, Freedman ML (1998) Increased peroxidation and reduced antioxidant enzyme activity in Alzheimer’s disease. Exp Neurol 150:40–44
Markesbery WR, Carney JM (1999) Oxidative alterations in Alzheimer’s disease. Brain Pathol 9:133–146
Mattson MP, Begley JG, Mark RJ, Furukawa K (1997) Abeta25–35 induces rapid lysis of red blood cells: contrast with Abeta1-42 and examination of underlying mechanisms. Brain Res 771:147–153
Miao L, St Clair DK (2009) Regulation of superoxide dismutase genes: implications in disease. Free Radic Biol Med 47:344–356
Miguel F, Augusto AC, Gurgueira SA (2009) Effect of acute vs chronic H2O2-induced oxidative stress on antioxidant enzyme activities. Free Radic Res 43:340–347
Mondola P, Ruggiero G, Serù R, Damiano S, Grimaldi S, Garbi C, Monda M, Greco D, Santillo M (2003) The Cu, Zn superoxide dismutase in neuroblastoma SK-N-BE cells is exported by a microvesicles dependent pathway. Brain Res Mol Brain Res 110:45–51
Moreira PI, Carvalho C, Zhu X, Smith MA, Perry G (2010) Mitochondrial dysfunction is a trigger of Alzheimer’s disease pathophysiology. Biochim Biophys Acta 1802:2–10
Murakami K, Murata N, Noda Y, Tahara S, Kaneko T, Kinoshita N, Hatsuta H, Murayama S, Barnham KJ, Irie K, Shirasawa T, Shimizu T (2011) SOD1 (copper/zinc superoxide dismutase) deficiency drives amyloid β protein oligomerization and memory loss in mouse model of Alzheimer disease. J Biol Chem 286:44557–44568
Nunomura A, Castellani RJ, Zhu X, Moreira PI, Perry G, Smith MA (2006) Involvement of oxidative stress in Alzheimer disease. J Neuropathol Exp Neurol 65:631–641
Paulsen BDS et al (2012) Altered oxygen metabolism associated to neurogenesis of induced pluripotent stem cells derived from a schizophrenic patient. Cell Transplant 21:1547–1559
Roher AE, Esh CL, Kokjohn TA, Castaño EM, Van Vickle GD, Kalback WM, Patton RL, Luehrs DC, Daugs ID, Kuo YM, Emmerling MR, Soares H, Quinn JF, Kaye J, Connor DJ, Silverberg NB, Adler CH, Seward JD, Beach TG, Sabbagh MN (2009) Amyloid beta peptides in human plasma and tissues and their significance for Alzheimer’s disease. Alzheimer’s Dement J Alzheimer’s Assoc 5:18–29
Sinha K, Das J, Pal PB, Sil PC (2013) Oxidative stress: the mitochondria-dependent and mitochondria-independent pathways of apoptosis. Arch Toxicol 87:1157–1180
Soriano ME, Scorrano L (2011) Traveling Bax and forth from mitochondria to control apoptosis. Cell 145:15–17
Tabner BJ, Mayes J, Allsop D (2010) Hypothesis: soluble abeta oligomers in association with redox-active metal ions are the optimal generators of reactive oxygen species in Alzheimer’s disease. Int J Alzheimer’s Dis 2011:546380
Tsunekawa H, Noda Y, Mouri A, Yoneda F, Nabeshima T (2008) Synergistic effects of selegiline and donepezil on cognitive impairment induced by amyloid beta(25–35). Behav Brain Res 190:224–232
Van Rheen Z, Fattman C, Domarski S, Majka S, Klemm D, Stenmark KR, Nozik-Grayck E (2011) Lung extracellular superoxide dismutase overexpression lessens bleomycin-induced pulmonary hypertension and vascular remodeling. Am J Respir Cell Mol Biol 44:500–508
Wilquet V, De Strooper B (2004) Amyloid-beta precursor protein processing in neurodegeneration. Curr Opin Neurobiol 14:582–588
Witte ME, Geurts JJ, de Vries HE, van der Valk P, van Horssen J (2010) Mitochondrial dysfunction: a potential link between neuroinflammation and neurodegeneration? Mitochondrion 10:411–418
Yu H, Yao L, Zhou H, Qu S, Zeng X, Zhou D, Zhou Y, Li X, Liu Z (2014) Neuroprotection against Abeta25–35-induced apoptosis by Salvia miltiorrhiza extract in SH-SY5Y cells. Neurochem Int 75:89–95
Zelko IN, Mariani TJ, Folz RJ (2002) Superoxide dismutase multigene family: a comparison of the CuZn-SOD (SOD1), Mn-SOD (SOD2), and EC-SOD (SOD3) gene structures, evolution, and expression. Free Radic Biol Med 33:337–349
Zhang L, Yu H, Zhao X, Lin X, Tan C, Cao G, Wang Z (2010) Neuroprotective effects of salidroside against beta-amyloid-induced oxidative stress in SH-SY5Y human neuroblastoma cells. Neurochem Int 57:547–555
Acknowledgments
This work was supported primarily by a grant through the cutting-edge research project of the Chongqing Science and Technology Committee (CSTC2014JCYJA10014) and a grant from the Scientific and Technological Research Programme of Chongqing Municipal Education Commission (KJ130320). It was also partially supported by grants from the National Natural Science Foundation of China (NSFC Grant Numbers 81001220 and 81370077), the Fundamental Research Funds for Nonprofit Public Scientific Research Institutions of Chongqing from Chongqing Science and Technology Commission (Grant Numbers 2015CSTC-JBKY-01702 and 2013CSCT-JBKY-01703).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Additional information
Rong Yang and Li Wei have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Yang, R., Wei, L., Fu, QQ. et al. SOD3 Ameliorates Aβ25–35-Induced Oxidative Damage in SH-SY5Y Cells by Inhibiting the Mitochondrial Pathway. Cell Mol Neurobiol 37, 513–525 (2017). https://doi.org/10.1007/s10571-016-0390-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-016-0390-z