Abstract
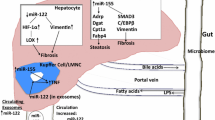
In this review, we summarize the current understanding of microRNA (miRNA)-mediated modulation of the gene expression in the fatty liver as well as related signaling pathways. Because of the breadth and diversity of miRNAs, miRNAs may have a very wide variety of biological functions, and much evidence has confirmed that miRNAs are involved in the pathogenesis of fatty liver. In the pathophysiological mechanism of fatty liver, miRNAs may be regulated by upstream regulators, and have their own regulatory targets. miRNAs display important roles in the pathological mechanisms of alcoholic liver disease and non-alcoholic fatty liver disease. At present, most of the miRNA studies are focused on cell and tissue levels, and in vivo studies will help us elucidate the regulation of miRNAs and help us evaluate the potential of miRNAs as diagnostic markers and therapeutic targets. Furthermore, there is evidence that miRNAs are involved in the mechanism of natural medicine treatment in fatty liver. Given the important roles of miRNAs in the pathogenesis of fatty liver, we predict that studies of miRNAs in the pathogenesis of fatty liver will contribute to the elucidation of fatty liver pathology and the treatment of fatty liver patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
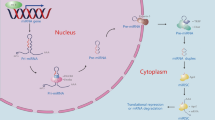
microRNAs (miRNAs) are a class of non-coding single-stranded RNA molecules about 22 nucleotides in length encoded by endogenous genes that are involved in post-transcriptional gene regulation in animals and plants. Each miRNA can have multiple target genes, and several miRNAs can also regulate the same gene. Most miRNA genes are present in the genome in the form of a single copy, multiple copies, or cluster. It is speculated that miRNA regulates one-third of the human gene (Rupaimoole and Slack 2017; Kumar et al. 2017; Daugaard and Hansen 2017). Mature miRNAs are produced by the cleavage of longer primary transcripts by a series of nucleases and are subsequently assembled into the RNA-induced silencing complex (RISC). The RISC recognizes the target mRNA by way of base-pairing and guides the silencing complex to degrade the target mRNA or repress the translation of the target mRNA according to the degree of complementarity. Recent studies have shown that miRNAs are involved in a variety of regulatory pathways, including development, viral defense, hematopoiesis, organogenesis, cell proliferation and apoptosis, fat metabolism, and more (Barciszewska 2016). In addition, a study showed that a decrease in the level of two miRNAs was significantly associated with chronic lymphocytic leukemia, suggesting a potential relationship between miRNAs and cancer (An et al. 2017; Arora et al. 2016).
Fatty liver is a chronic reversible liver disease characterized by liver injury caused by excessive accumulation of fat in liver cells. The liver is the important digestive organ of the human body, which is responsible for maintaining the balance of human metabolism, and plays an important role in the digestion, absorption, oxidation, decomposition, synthesis, and transportation of fat (Akhlaghi 2016; Handzlik-Orlik et al. 2016). Evidence suggests that miRNA plays an important regulatory role in the pathogenesis of fatty liver. For example, microarray analysis shows that, compared with the control, 170 miRNAs are maladjusted in the CD4+T lymphocytes from the liver of non-alcoholic fatty liver disease (NAFLD) mice, and 80 mRNAs are corresponding to the miRNA target genes, including the miR-128 and miR-130b, which are confirmed to participate in mitogen-activated protein kinase (MAPK) pathway (Zhang et al. 2017). In this review, we summarize the current understanding of miRNA-mediated modulation of the gene expression in the fatty liver as well as related signaling pathways in the last 3 years, with special emphasis on the role of miRNAs in the pathogenesis of NAFLD, and insight into the role of in vivo injection of miRNAs and their antagonists in the fatty liver model animals. Furthermore, the potential therapeutic value of miRNAs for fatty liver treatment, the role of miRNAs in alcoholic liver disease (ALD), and natural medicine treatment will also be discussed.
Circulating miRNAs Display as Biomarkers in Fatty Liver
Finding markers of disease diagnosis is an important field of medical foundation and clinical research. The disease markers in serum are of great value in early diagnosis, individualized treatment, and prognosis. Many studies have shown that the expression of miRNA in tissues and blood is stable, and is disease specific, including fatty liver (Miya Shaik et al. 2018).
Sun et al. (2015) found that the expression of miR-21 in the serum of NAFLD patients was significantly lower than that in healthy controls, and the expression of 3-hydroxy-3-methylglutaryl-co-enzyme A reductase (HMGCR) was significantly up-regulated as the direct action target of miR-21 in serum of NAFLD patients. Overexpression of miR-21 can significantly reduce the formation of triglyceride, free cholesterol, and total cholesterol, and this regulatory mechanism can be blocked by the overexpression of HMGCR, indicating the regulatory relationship between miR-21 and HMGCR is further demonstrated.
Abnormal expression of miR-23a is closely related to endoplasmic reticulum (ER) pressure abnormality, and the expression of miR-23a stimulated with tunicamycin is rescued by melatonin treatment, leading to reduced ER stress in primary hepatocytes treated with tunicamycin (Suzuki 2017; Kim et al. 2015). Salvoza et al. (2016) found that compared with the control, the levels of miR-34a and miR-122 in the serum of NAFLD patients were significantly higher, and the two miRNA expressions were positively correlated with the levels of the triglyceride and very low-density lipoprotein cholesterol (VLDL-C), suggesting that miR-34a and miR-122 were involved in the pathogenesis of fatty liver and may be diagnostic markers and therapeutic targets for fatty liver (Elhanati et al. 2016).
Evidence shows that the abnormality of miR-122 expression may be related to pathological transformation from NAFLD to HCC. The level of miR-122 expression in the serum of NAFLD was directly associated with the levels of AST and ALT, and the level of miR-122 in the serum of patients without HCC was significantly higher than that of the third phase of patients with HCC. Moreover, the expression level of miR-122 in serum was down-regulated before the stage of liver fibrosis, suggesting that miR-122 was involved in the pathological development of NAFLD (Akuta et al. 2016a; Baffy 2015).
In a model of fatty liver disease induced by high-fat diet (HFD), the overexpressed miR-155 alleviates the severity of NAFLD, which may be done by carboxylesterase 3/triacylglycerol hydrolase. The carboxylesterase 3/triacylglycerol hydrolase is identified as a potential target for miR-155 (Csak et al. 2015; Lin et al. 2015). Wang et al. (2016b) showed that the expression of miR-155 in peripheral blood and liver of NAFLD patients was significantly down-regulated compared with healthy controls. Overexpression of miR-155 inhibited the liver lipid accumulation by inhibiting the X receptor alpha-dependent fat-producing signal transduction pathway.
Many studies have shown that miRNA has the characteristics of disease diagnosis markers. The advantage of miRNA detection in serum is that the method is simple and accurate, which can improve the accuracy of disease diagnosis and prognosis evaluation. In view of the maturity of the detection technique of miRNA expression in the blood, and the accuracy and sensitivity have reached clinical requirements, miRNA is expected to be a new molecular marker for the diagnosis and prognosis of fatty liver.
miRNAs are Involved in the Pathogenesis of NAFLD
NAFLD is a clinical pathological syndrome characterized by excessive deposition of lipids in the liver cells, except for alcohol and other specific liver damage factors, which is metabolic stress liver injury closely related to insulin resistance and genetic predisposition, including simple fatty liver (SFL), non-alcoholic steatohepatitis (NASH), and its associated cirrhosis (Boutari et al. 2018). With the trend of globalization of obesity and its related metabolic syndrome, NAFLD has now become an important cause of chronic liver disease in developed countries and rich area, and evidence suggests that miRNAs are involved in the pathogenesis of NAFLD (Silva Figueiredo et al. 2018). For example, when young Finns suffer from fatty liver, the levels of miR-122-5p and miR-885-5p are up-regulated, and these abnormal expressions of miRNAs may be involved in the formation of fatty liver by regulating lipid metabolism. The level of miR-122-5p is related to the components of small IDL, VLDL, and large LDL lipoprotein subclasses, and the miR-885-5p is negatively correlated with the levels of XL HDL cholesterol and oxysterol-binding protein 2 (OSBPL2) (Raitoharju et al. 2016).
miRNAs and the Obesity Mechanism
Obesity is a chronic metabolic disease caused by a variety of factors, resulting from an imbalance between energy intake and energy output, which often leads to a range of health problem and chronic disease, such as fatty liver. The excess intake of dietary saturated fatty acids (SFA) is the leading cause of obesity and hepatic steatosis, inevitably leading to an increased intracellular lipid accumulation in the liver (Walsh and Vilaca 2017).
The level of miR-96 is significantly up-regulated in the liver of HFD mice or liver cells treated with palmitic acid, and evidence shows that miR-96 inhibits the expression of insulin receptor (INSR) and IRS-1 with the 3′UTR of INSR and IRS-1 as the targets at post-transcriptional levels (Yang et al. 2016). In the HepG2 hepatoblastoma cells, both IL-6 and TNF-α can significantly increase the expression of miR-101. In the macrophages derived from human THP-1, IL-6 treatment leads to a significant increase in the expression of miR-101. Furthermore, by inhibiting the expression of ATP-binding cassette transporter A1 (ABCA1), the increase of miR-101 by the IL-6 and TNF-α promotes the intracellular cholesterol retention under the inflammatory condition, suggesting that the miR-101-ABCA1 axis may play a key role in the pathological mechanism of NAFLD (Zhang et al. 2015a).
In human mononuclear cells, if the toll-like receptor (TLR) 4 signal pathway is activated, the tumor necrosis factor receptor-associated factor 6 (TRAF6) in the downstream pathway will be up-regulated, resulting in the final induction of proinflammatory cytokine production. It is found that palmitic acid can reduce the expression of miR-194, and TRAF6 is a direct target of miR-194. Overexpression of miR-194 directly inhibits the expression of TRAF6, and weakens the release of proinflammatory cytokines TNF-α in activated monocytes THP-1 (Tian et al. 2015).
Compared with lean subjects, the expression of miR-26a is decreased in liver of overweight humans, and the miR-26a expression also is down-regulated in obese model mice compared with control. In mice fed with high-fat diet, overexpression of miR-26a improved the insulin sensitivity, and decreased the fatty acid synthesis and the hepatic glucose production (Fu et al. 2015).
In the obese model mice induced by high-fat diet and the model rats of Zucker diabetes (fa/fa), the expression of miR-29 in the liver is abnormal, which will lead to the metabolic dysfunction of the model animals. Pioglitazone, a thiazolidinedione antidiabetic drug, can improve insulin sensitivity and blood lipid characteristics (Sharma and Verma 2016). It is found that Pioglitazone can restore the miR-29 expression in model rats and achieve the purpose of regulating the expression of key lipid metabolism genes. Kurtz et al. (2015) found that miR-29 knockout has obvious lipid-lowering benefits by inhibiting the liver’s fat generation program in dyslipidemia of NAFLD, so miR-29 may be a candidate for metabolic disorders and a target for treatment.
In addition to the signal miRNA target, the role of multitarget complexity of miRNA suppression in disease pathogenesis has recently raised much interest, which is pivotal for pathological mechanism and treatment research for fatty liver. Hanin et al. (2017) studies found that transgenic mice expressing miR-132 showed severe fatty liver phenotypes and increased weight, liver triglycerides, serum low-density lipoprotein (LDL), and VLDL, accompanied by a reduced miR-132 target, an increase in fatty formation and a transcriptional related to lipid accumulation, suggesting that miR-132 played an important role in the pathogenesis of fatty liver.
In the visceral adipose tissue (VAT) of the morbidly obese subjects, the miR-192-3p is negatively correlated with the serum triglyceride concentration and is positively correlated with the high-density lipoprotein (HDL). Importantly, miR-192-3p is negatively correlated with body mass index in patients with less obese patients, suggesting that miR-192-3p is involved in the pathogenesis of obesity. The fat-producing enzyme stearyl coenzyme A desaturase-1 (SCD) and fatty aldehyde dehydrogenase 3 family member A2 are confirmed as the direct targets of miR-192, and the regulation of the levels of these two targets can neutralize the pathological effect of miR-192-3p (Mysore et al. 2016).
After feeding Landes geese for 19 days, the expression of miR-33 in the liver of Landes geese increases significantly. It is also proved that the carnitine O-octanoyltransferase, Acyl-CoA dehydrogenase/3-ketoacyl-CoA thiolase/enoyl-CoA hydratase, beta subunit, and Niemann Pick C 1 are targets of miR-33 in Landes goose liver, indicating that miR-33 may be involved in the pathological development of human fatty liver and these targets may also be the targets of fatty liver prevention and treatment (Zheng et al. 2015). Obesity is an important cause of fatty liver formation, and a large number of studies have shown that miRNAs play important roles in the pathogenesis of obesity. Through the regulation of miRNA expression in obesity mechanisms, we may find molecular targets for the diagnosis and treatment of obesity in fatty liver patients.
miRNAs and the Lipid Metabolism
High triglyceride is hyperlipidemia; the main harm of this disorder of lipid metabolism to human body is to induce atherosclerosis, blood clots, and thrombosis, which may lead to the occurrence of cardiovascular and cerebrovascular diseases (Mooradian and Haas 2015). The increase of hepatic triglyceride content is closely related to the pathogenesis of NAFLD and related metabolic diseases. Evidence shows that some miRNA is involved in this mechanism. For example, recent studies have shown that the expression of miR-124 is obviously up-regulated in the liver of the fatty liver model mice, and the increase of miR-124 leads to the accumulation of excessive triglycerides in the liver of the model mice. Importantly, miR-124 can target the tribbles homolog 3 (TRB3) and induce the expression of lipid production-related genes through activation of AKT signaling pathway (Liu et al. 2016a). Furthermore, it has been reported that miR-124a has the function of promoting microglia quiescence and early neurogenesis in the pathological mechanism of NAFLD. MiR-124a can regulate lipid metabolism by the regulation of adipose triglyceride lipase (ATGL) and its co-activator comparative gene identification 58 (CGI-58) expression (Jeon et al. 2014).
The expression of spatio-temporal-related genes is related to circadian rhythm and participates in the pathogenesis of metabolic diseases. There is evidence that miR-124 plays an important role in the regulation mechanism of lipid metabolism which is caused by the regulation of fasting and refeeding, which is similar to the regulation of hypertension in clock genes. After fasting, the triglyceride lipase mRNAs in liver increased significantly, and the expression of miR-124a decreased correspondingly. After feeding again, the expression of triglyceride lipase mRNA and 124a returned to the original level (Das et al. 2015).
Disordered miR-33a/miR-33b* and miR-122 might be possible contributors to hepatic lipid metabolism in obese women with NAFLD (Auguet et al. 2016). The up-regulated miR-34a regulates the triglyceride accumulation and inhibits the LDL secretion in human and rat hepatocytes in an HNF4α-dependent manner. The up-regulated miR-34a also promotes the fatty degeneration and lipid lowering in the liver in the pathological mechanism of the disease, indicating that the miR-34a-HNF4α pathway induced by metabolic stress is involved in the regulation of lipid and lipoprotein metabolism (Xu et al. 2015b). In addition, the up-regulated miR-34a may potentially promote lipid metabolism by targeting peroxisome proliferator-activated receptor α (PPARα) in the pathomechanism of NAFLD. This study also suggests that inhibition of miR-34a may be a therapeutic target for NAFLD patients (Ding et al. 2015).
In lactating mothers, HFD consumption leads to a significant decrease in miR-122 expression. The expression of miR-370 increased significantly in the liver of weaning mice. The changes in these two miRNA expressions are associated with the high expression of Gpam, Agpat, and Scd1, and the low expression of fatty acid oxidation-related genes, the carnitine palmitoyltransferase 1a (Cpt1a), and Acadvl, suggesting that miR-122 and miR-370 participate in lipid metabolic disorders (Benatti et al. 2014). Furthermore, there is evidence that abnormal fatty acids in maternal blood lead to changes in the expression of miR-122 and miR-370, and these changes significantly enhance the susceptibility to obesity and abnormal lipid accumulation in the body. Excessive nutrition during pregnancy and lactation may lead to metabolic changes, which may permanently change the balance of lipid metabolism in the body by means of epigenetic modification, such as miRNA (de Paula Simino et al. 2017).
Liver miR-291b-3p promotes the development of hepatic adipogenesis and lipid accumulation in NAFLD. Knockout of miR-291b-3p significantly blocks the deterioration of adipose tissue and steatosis in the liver of model mice, and overexpression of miR-291b-3p results in the opposite observation. MiR-291b-3p significantly improves the synthesis of triglycerides induced by oleic acid/palmitic acid mixture in the knockout hepatocytes, and the AMP-activated protein kinase (AMPK)-α1 is the direct target. This mechanism may be an effective way to diagnose and treat NAFLD (Meng et al. 2016).
When Chang liver cells are treated with free fatty acids, the expression of miR-511 is significantly decreased, while the expression of OATP1B1 increases significantly. Evidence suggests that SLCO1B1 is a direct target gene of miR-511, and transfection of miR-511 will inhibit the expression of SLCO1B1 and OATP1B1 in these cells (Peng et al. 2015). By interacting with the 3′-untranslated regions (3′-UTR) of apoB mRNA to enhance post-transcriptional degradation, miR-548p significantly inhibits the expression of apoB in human hepatoma cells and primary hepatocytes. Interestingly, miR-548p has a significant inhibition of lipid synthesis in human hepatoma cells by inhibiting the ACSL4 (Acyl-CoA synthetase long-chain family member 4) and HMGCR involved in cholesterol and fatty acid synthesis, suggesting that miR-548p may be useful in the treatment of fatty liver by regulating apoB secretion (Zhou and Hussain 2017).
Recently, miR-21 has been reported as a link between NAFLD and the pathogenesis of HCC by regulating the HBP1-p53-sterol regulatory element-binding protein 1 (SREBP1) pathway. In the liver of HFD-treated mice and human HepG2 cells incubated with fatty acids, the knockdown of miR-21 damages the lipid synthesis of xenograft tumors. Evidence also shows that Hbp1 is a transcriptional activator of p53 and a new target for miR-21 (Bhat et al. 2015; Wu et al. 2016).
Many evidence shows that estrogen has a protective effect on the liver lipid accumulation, which is the cause of the prevalence of NAFLD in premenopausal women lower than those of the same age male and postmenopausal women, suggesting the importance of the balance of hormones in the liver to maintain the lipid metabolism. Interestingly, miRNA may be involved in the process of estrogen-regulating lipid metabolism. For example, miR-125b in the liver is activated by estrogen through estrogen receptor alpha (ERα), and the increased miR-125b strongly inhibits the liver lipid accumulation (Zhang et al. 2015b). This is a novel mechanism by which estrogen protects against NAFLD in female via up-regulating the miR-125b expression.
The genomic loci of miR-26a/b have been located in the introns of the C-terminal domain RNA polymerase II polypeptide A small phosphatase (CTDSP) gene. In goat mammary epithelial cells, blocking miR-26a/b or its host gene CTDSP reduces the accumulation of triglycerides and the synthesis of unsaturated fatty acids, and reduces the production of SCD1, GPAM, LXRA, FASN, and other genes related to fatty acid synthesis, including the LPIN1 and DGAT1. The insulin-induced gene (INSIG)1 is a protein that plays a key role in the process of regulating fat formation in rodent liver, and it has been proved to be the direct target of miR-26a/b (Wang et al. 2016a). In addition to rats, other animals are also used to replicate fatty liver diseases to study the relationship between miRNA and fatty liver pathology. Using animal models to study the pathological mechanism of fatty liver is helpful to elucidate the pathogenesis of human fatty liver and study the prevention and treatment of diseases.
miRNAs and the Glucose Metabolism
During the development of NAFLD, the expression of miR-9 increases significantly, and the increased expression is directly related to glucose metabolism. It is found that Onecut2 and SIRT1 are the direct targets of miR-9, and miR-9 affects the pathogenesis of NAFLD through targeting Onecut2 and SIRT1 (Ao et al. 2016). In hepatocytes, diet or palmitic acid salt-induced obesity significantly up-regulated the expression of miR-15b, and the increase of miR-15b can inhibit the protein expression of INSR by direct target to INSR 3′-UTR, resulting in impaired insulin signal transduction and glycogen synthesis in diet-induced obese mice liver cells. This discovery reveals a new mechanism that the obesity-induced miR-15b has a causal relationship with the development of insulin resistance by inhibiting INSR in the pathogenesis of the glucose metabolism in NAFLD (Yang et al. 2015).
HNF-4α is involved in controlling carbohydrate metabolism, glucose regulation, insulin synthesis, and many other important processes (Rastinejad et al. 2013). In addition, maturity-onset diabetes of the young (MODY) is a rare diabetes, and evidence shows that the occurrence of this diabetes is related to the mutation of HNF-4α gene. In type 2 diabetic model mice or HepG2 cells treated with palmitic acid, the expressions of miR-122 and HNF-4α are significantly up-regulated compared with the control, and the up-regulated HNF-4α increases the expression of miR-122, whereas the HNF-4 knockdown significantly inhibits the expression of miR-122, suggesting that the influence of HNF-4 on miR-122 production is helpful for the development of gluconeogenesis and lipid metabolism (Wei et al. 2016).
In the NAFLD model mice induced by insulin resistance and diabetes, the expression of miR-21 is obviously down-regulated, and this miRNA may be involved in the pathogenesis of NAFLD by regulating the expression of the PPAR subtype (Zhao and Shao 2016). There is evidence that miR-29a regulates the SCD expression by transcriptional regulation with 3′-UTR as target in a genetically modified tilapia disease model. After miR-29a antagomir transfection is used to inhibit the expression of miR-29a, the expression of SCD is significantly up-regulated and serum insulin is activated, suggesting that miR-29a is involved in the pathological mechanism of the disease by using SCD as a target in the genetically modified cultured tilapia livers (Qiang et al. 2017).
The obesity paradox (OP) model prepared by apoE−/−/miR-155−/− [double knockout (DKO)] mice has reduced atherosclerosis, increased obesity, and NAFLD. MiR-155 is significantly up-regulated in the aorta of apoE−/− mice with high-fat diet. However, in the DKO model, miR-155 deficiency inhibits the atherosclerosis, characterized by high-fat diet-induced NAFLD, obesity, and adipocyte hypertrophy. MiR-155 deficiency also showed a high-fat diet-induced plasma resistin, leptin, and fasting insulin, but it was lack of insulin resistance and glucose intolerance. These findings provide miR-155 as a new biomarker and new therapeutic target for OP-related metabolic diseases (Virtue et al. 2017).
MiR-206 is another miRNA associated with fatty liver pathology, which can be inhibited by lipid accumulation in human hepatocytes. Animal experiment shows that miR-206 delivery has a strong therapeutic effect on hyperglycemia and liver fat accumulation. Interestingly, miR-206 can interact with the 3′-UTR of protein tyrosine phosphatase non-receptor type 1 (PTPN1) and induce its degradation, thereby promoting insulin signaling by promoting the phosphorylation of INSR and the damage of liver fat formation (Wu et al. 2017). It may be concluded that miR-206 is a potent inhibitor of lipid and glucose production and a potentially treatment target for both hyperglycemia and hepatosteatosis.
miRNAs and the NASH
Although the study of miRNAs is still at an early stage, it is presumed that the regulation of miRNAs in gene expression in advanced eukaryotes may be as important as transcription factors. In experimental sinusoidal endothelial injury of NASH, leptin mediates the miR-21 overexpression and Grhl3 inhibition, and the up-regulated miR-21 leads to the time-dependent inhibition of the target Grhl3. In this process, the Grhl3-controlled nitric oxide synthase 3 (NOS) 3-p/NOS3 ratio decreases significantly (Pourhoseini et al. 2015). Increased miR-21 induced by leptin displays as a key regulator of transforming growth factor (TGF)-β signaling and fibrogenesis in NASH by targeting SMAD7 (Dattaroy et al. 2015).
NASH patients have significantly higher plasma-saturated free fatty acid level than normal controls, and these toxic fatty acids can promote the liver cell death and the biliary epithelium impair. In animal model of NASH, palmitate induction of miR-34a is abolished in cholangiocytes transduced with FoxO3 shRNA, demonstrating that the FoxO3 activation is upstream of miR-34a and the FoxO3 is a novel transcriptional regulator of miR-34a (Natarajan et al. 2017). This mechanism suggests that FoxO3 up-regulates the miR-34a expression to cause palmitate-induced cholangiocyte lipoapoptosis.
MiR-21 is overexpressed primarily in biliary and inflammatory cells in mouse models as well as in patients with NASH, but not in patients with bland steatosis. Studies have shown that PPAR alpha is reduced in the liver of NASH mice, and the up-regulation of miR-21 is directly involved in the pathogenesis of NASH with PPAR alpha as the target. By inducing the expression of PPAR alpha, the knockout of miR-21 is helpful to the recovery of disease in the experimental model (Rodrigues et al. 2017). Other evidence suggests that increased miR-21 is associated with fibrosis in a rat model of NASH and has the potential to serve as a plasma biomarker for hepatic fibrosis (Loyer et al. 2016).
Through targeting TLR2-negative regulation mode, the decrease of miR-144 promotes the secretion of TNF-α and IFN-γ, resulting in the pathological development of NASH induced by HFD in E3 model rats (Li et al. 2015). Meanwhile, overexpression of miR-146b can improve the HFD-induced NASH pathology by directly inhibiting the IL-1 receptor-associated kinase 1 (IRAK1) and TRAF6 (Jiang et al. 2015). There is evidence that the expression of miR-421 in the liver tissue of NAFLD model mice is obviously up-regulated, and the inhibition of miR-421 expression in the liver can reduce the oxidative damage in the liver of NAFLD model mice, which is beneficial to the recovery of liver tissue lesions in the NAFLD model mice. SIRT3 is identified as a direct target of miR-421, and the increase of miR-421 expression can inhibit the expression of SIRT3, and lead to a significant decrease in the expression of MnSOD and CAT, which is downstream target molecules of the SIRT3/FOXO3 pathway (Cheng et al. 2016). The expression of miR-451 in palmitic acid-exposed HepG2 cells, HFD-induced NASH mice, and liver tissues of NASH patients is significantly decreased. It is found that the decrease of miR-451 expression in NASH can inhibit the production of fatty acid-induced proinflammatory cytokines and participate in the pathogenesis of disease through the AMPK/AKT pathway (Hur et al. 2015).
miRNAs and the Bile Metabolism
Deoxycholic acid (DCA) is a cytotoxic bile acid implicated in the pathogenesis of NAFLD, and the DCA has recently showed that its production is enhanced in the serum of NASH patients (Steinacher et al. 2017). There is evidence that miR-21 expression decreases after a short period of exposure to DCA, accompanied by PIDD processing and the activation of p53 and caspase-2 in the miR-21 downstream pathway, which leads to DCA-induced liver damage. At the same time, the miR-21 gene promoter contains NF-κB binding site, and the decrease of NF-κB, which is reduced by DCA, will lose the transcriptional regulation of miR-21 expression, suggesting the important role of NF-κB and miR-21 in the mechanism of hepatocyte apoptosis (Rodrigues et al. 2015).
It is proved that the knockout of Dicer1 in the liver of mice leads to a slight increase in the expression of free cholesterol and a significant increase in the expression of cholesteryl ester. The miRNA mechanism behind this phenomenon is still unclear, and further research will help us to elucidate the role of epigenetic modification represented by miRNA in the pathological mechanism of this disease (Stewart et al. 2016). Liver-specific Dicer1 knockout leads to the accumulation of free cholesterol in the liver, accompanied by a significant increase in HMGCR expression, a rate-limiting enzyme for cholesterol synthesis in the liver. During the course of pathogenesis, the expression of miR-29a was down-regulated, and the inhibited miR-29a leads to a loss of the HMGCR inhibition by targeting the HMGCR 3′-UTR (Liu et al. 2017; Mattis et al. 2015) (Table 1).
miRNAs and ALD
ALD is a liver disease caused by prolonged heavy drinking. The initial performance is usually fatty liver, which can develop into alcoholic hepatitis, liver fibrosis, and cirrhosis. The main clinical features are nausea, vomiting, jaundice, enlarged liver, and tenderness, and may be complicated by liver failure and upper gastrointestinal bleeding. Severe alcohol abuse can induce extensive liver cell necrosis and even liver failure. ALD is one of the common liver diseases, which seriously endangers people’s health (Woolbright and Jaeschke 2018).
miRNA plays an important role in the pathogenesis of alcohol-induced liver injury, and participates in the release of inflammatory cytokines, liver lipid metabolism disorder, and liver cirrhosis. For example, alcohol-induced miR-27a regulates the differentiation of normal human monocytes and the polarization of M2 macrophages in the pathogenesis of alcohol-induced liver injury. Through the activation of ERK signal transduction, the over expression of miR-27a can produce more IL-10, and the activation of ERK signal may be caused by inhibition of ERK inhibitor Sprouty2 expression in monocytes, suggesting that Sprouty2 is a direct target of miR-27a (Saha et al. 2015).
ALD is a long-term heavy drinking caused by liver disease. Early symptoms are fatty liver, which can develop into alcoholic hepatitis, liver fibrosis, and cirrhosis. The abnormal expression of miR-155 may be closely related to the pathogenesis of ALD. Animal experiments show that miR-155 knockout mice are free from alcohol-induced inflammation and fatty degeneration, and the decrease of alcohol-induced fat accumulation in miR-155 knockout mice is associated with the decrease of MCP1 production and the increase of PPAR alpha. MCP1 and PPAR alpha may be the direct target of miR-155, in ALD pathological mechanism (Bala et al. 2016).
ALD occurs only in a subset (~ 30%) of alcoholics, indicating that excessive ethanol consumption is necessary but not sufficient to induce liver injury (Stickel et al. 2017). Therefore, additional factors are required during the ALD development. There is evidence that gut-derived endotoxin appears to be this required co-factor, and that miRNAs are involved in the mechanism. For example, compared with healthy controls, miR-212 expression in colon biopsy samples from ALD patients increased significantly. The increased miR-212 expression in Caco-2 intestinal epithelial cells is accompanied by the decrease of Zonula Occludens-1 (ZO-1) protein and the enhanced permeability of Caco-2 monolayer cells. It is interesting that the damage of the intestinal barrier induced by inducible nitric oxide synthase (iNOS) can be mediated by miR-212 overexpression, which in turn leads to a significant reduction in the expression of the target gene ZO-1 (Tang et al. 2015). MiR-212 inhibition may represent a new mechanism for therapeutic intervention to prevent leaky gut and liver injury in alcoholics.
The evidence suggests that remote ischemic preconditioning (RIPC) can prevent ischemia reperfusion and other cardiovascular damage, but the role and mechanism of RIPC in NAFLD liver ischemia and reperfusion (IR) injury is still unclear. MiR-29a/b/c may be involved in the pathogenesis of hepatic IR injury in NAFLD. In RIPC rat model and RIPC + IR group, the expression of miR-29a/b/c decreases significantly, but there is no change in IR group compared with control group. Up-regulation of miR-29a/b/c expression is beneficial to repair of injury (Duan et al. 2017).
As far as we know, alcohol-induced liver injury can significantly stimulate the production of proinflammatory cytokines, leading to the exacerbation of liver inflammation. In the pathology of liver injury induced by alcohol, overexpression of miR-217 will promote the fatty degeneration and inflammation in the liver of alcoholic liver model mice, and the increase of miR-217 mediating the sirtuin 1 inhibition leads to the activation of the two important inflammatory modulators, the NF-κB and the nuclear factor T cells c4 (Yin et al. 2016). The expression of miR-223 is significantly down-regulated in the peripheral blood neutrophils of alcoholics, and the expressions of IL-6 and p47phox are up-regulated, compared with the control group. And miR-223 can directly inhibit the expression of IL-6 and subsequently inhibit the expression of p47phox in neutrophils that is involved in the pathological development of alcoholic liver (Li et al. 2017b). This shows that miR-223 is a crucial regulator to prevent the neutrophil infiltration and could be used as a novel therapeutic target for the treatment of patients with ALD (Table 1).
In Vivo Injection Therapy of miRNAs in Fatty Liver
Mir-26a has been reported that displayed a crucial role in the regulation of cell proliferation, cell apoptosis, cellular differentiation, and metastasis, as well as its role in insulin resistance, glucose metabolism, and lipid metabolism. After injection of lentivirus vector encoding miRNAs, such as the mir-26a, miR-30c, in mouse tail vein, lentivirus-mediated liver miR-30c overexpression can significantly inhibit the pathological development of hyperlipidemia and atherosclerosis in mice and do not cause hepatic steatosis. This in vivo animal experiment further verified the prospect of miRNA in vivo (He et al. 2017; Zarrinpar et al. 2016). Furthermore, the experiment shows that the delivery of miR-30c mimics into C57BL/6 J mice liver can significantly inhibit the diet-induced hypercholesterolemia, resulting in a continuous reduction in plasma cholesterol, without significant side effects. MiR-30c mimic delivery also can reduce lipoprotein production by down-regulating the expression of microsomal triglyceride transport protein, and has no effect on LDL clearance (Irani et al. 2016). This means that miRNAs and their expression vectors can be injected into animals to carry out experiments in vivo. Similar in vivo experiments have resulted in certain effects, such as changes in animal body weight, organ weight, fatty liver-related indicators, and the expression of miRNA targets.
By observing the expression of miRNA in NAFLD patients, the level of circulating miR-122 is obviously up-regulated, and the level of serum miR-122 can be used for early warning of early NAFLD and monitoring of the development of fatty liver disease (Yamada et al. 2015). Animal experiment has shown that miR-122 antagonists have a certain therapeutic effect in the treatment of fatty liver model mice, revealing the new molecular target for lipid metabolism in the liver. Furthermore, 12 months of atorvastatin treatment reduces the circulating miR-122 level, indicating that circulating miR-122 is strongly associated with the risk of metabolic syndrome and type 2 diabetes and is the potential marker of fatty liver (Willeit et al. 2017) (Table 1).
miRNAs and Natural Medicine Treatment in Fatty Liver
Carnosic acid has the effect of antioxidant, anti aging, weight loss lipid-lowering, treatment of cardiovascular disease, anti-cancer. Carnosic acid also is a novel antioxidant and a potential inhibitor of apoptosis in organ injury, including liver injury (Xu et al. 2017; Shan et al. 2015). The expression of miR-33 and miR-122 that directly regulate the liver ABCA1 and CPT1a and the indirect regulation of fatty acid synthase are significantly reduced in mice hepatocytes. MiR-33 and miR-122 may be the possible regulators of molecular mechanism of LPPs in inducing blood lipid reduction in the liver of mice (Su et al. 2017).
More and more attention has been paid to the effective components of plants, especially edible plants, in the prevention and treatment of diseases. Xylobiose, a β-1,4-linked d-xylose dimer, is the main component of xylo-oligosaccharides (XOS). The content of xylobiose in bamboo is relatively rich, which is the most favorite food for Chinese people. Studies have shown that the intake of xylobiose can significantly regulate the expression of miR-33a and miR-122a in liver, regulate the inflammation, lipid metabolism, and liver oxidative stress. Xylobiose plays an important role in preventing or reducing the pathological development of type 2 diabetes and plays a key role in improving the process of lipid metabolism (Lim et al. 2016).
MiR-103-3p, miR-107-3p, and miR-122-5p, these three kinds of miRNA account for 70% of the total miRNAs in the liver, and evidence suggests that their targets are involved in the prevention of resveratrol for hepatic steatosis. Resveratrol-treated fatty liver model rats reduces the expression of these three kinds of miRNAs and SREBP1, accompanied by the increase of CPT1a expression. In the model rats fed with obesity diet, the hepatic steatosis recovered by resveratrol may be mediated by the increase in expression and activity of CPT1a protein and inhibition of miRNA-107-3p expression (Xu et al. 2015a; Gracia et al. 2017). Interestingly, there is evidence that miRNAs are involved in the mechanism of NAFLD prevention mediated by physical exercise, such as miR-212.
MiR-212 level is strongly up-regulated in HFD-induced fatty liver, and miR-212 also promotes the lipid production in HepG2 cells treated with long-chain fatty acid (FFA). Interestingly, miR-212 expression can be reduced by physical exercise through a long-term observation, suggesting the molecular mechanism of physical exercise for pathological recovery of fatty liver patients. In HepG2 cells, miR-212 negatively regulates the expression of fibroblast growth factor (FGF)-21, which is a key regulator of lipid metabolism, and may be the target gene of miR-212. Therefore, increased miR-212 may be a target for diagnosis and treatment of fatty liver induced by HFD (Boursier and Diehl 2016; Xiao et al. 2016) (Table 1).
Future Challenges and Research Directions
In the pathogenesis of disease, there is often a mutual regulation between miRNA and target, which we call feedback loop. For example, in transgenic mice, overexpression of miR-17-5p promotes the fatty liver and produced more triglyceride and cholesterol but lower levels of PPAR-α compared with control. Interestingly, PPARα is a target of miR-17-5p, and PPARα also can bind to the promoter of miR-17 and promoted its expression, together constitute a feedback loop (Du et al. 2015).
miRNA can not only inhibit the different molecules in the same signal pathway, but also form a signal feedback loop with the members of the same signal pathway to accurately regulate the cell proliferation and apoptosis in the pathological mechanism of fatty liver, as well as the abnormal accumulation of fat and abnormal glucose metabolism. In addition, the same miRNA can also regulate different signaling pathways, affecting the physiological and pathological mechanisms of fatty liver at different stages (Huang and He 2011).
There is a view that miRNA, as one of the epigenetic modification methods, represents a new way to regulate gene expression at the new level. Previously, most of the pathological mechanism of miRNA and fatty liver is focused on cell level in order to explore the relationship between miRNAs and the regulatory factors or signaling pathways involved in the pathology of fatty liver. At present, miRNA research is turning to explore new therapies, such as the tail vein injection of miRNAs in fatty liver animal model. Injection of miR-34a inhibitor strongly inhibits the highly expressed miR-34a, resulting in increased expression of PPARα, which is a target gene of miR-34a (Castro et al. 2013). It is worth noting that the injection of miR-367 adenovirus expressing vector to C57BL/6 mice can promote the accumulation of triglyceride in the cells and lean mice, and lead to the inhibition of fatty acid oxidation and the liver fatty degeneration in the model mice (Li et al. 2017a). It is suggests that the tail vein injection may be a valuable treatment for miRNA application.
Similar to other new therapies, before using miRNAs for human trials, it is the first necessary to solve some problems that exist in the method itself. At present, the method of small molecules accurately injected into the target cells is still a technical problem. In addition, it is necessary to ensure that the target gene for miRNAs action does not appear to be detrimental to the body after its expression has been altered. Many miRNAs have multiple targets, and a single miRNA can regulate dozens or hundreds of genes. Increasing or decreasing the expression level of a certain miRNA can significantly affect the expression of downstream genes, changes in the expression of a gene in vivo are serious. However, many researchers believe that after a period of time, miRNAs will eventually bring new dawn to the field of disease treatment.
Conclusion
miRNAs are a class of endogenous regulatory non-coding RNAs found in eukaryotes that are about 20–25 nucleotides in size. Only a small part of the biological function of miRNAs has been elucidated, these miRNAs regulate cell growth, tissue differentiation, organ development, and pathological mechanisms of some diseases, such as the fatty liver. miRNA is highly conserved, and its expression is time dependent and tissue specific. A large number of studies have shown that miRNA in the circulation may be an important marker for the diagnosis and prognosis of fatty liver disease. In retrospect, several miRNAs, such as miR-21, miR-34a, and miR-122, are potential indicators for the diagnosis and prognosis of fatty liver. The serum miR-122 is associated with hepatic steatosis and inflammatory activity, the serum miR-122 ratio of second biopsies to the first biopsy is significantly associated with the histopathological score in NAFLD patients with no hepatocellular carcinoma (HCC) (Akuta et al. 2016b; Becker et al. 2015).
With the further in-depth study of miRNA mechanism, and the use of the latest high-throughput technologies, such as the miRNA microarray, to study the relationship between miRNA and human disease, it will enable the understanding of the regulation of higher eukaryotic gene expression to a new level. miRNA may become a new biomarker for disease diagnosis and a drug treatment target, or we can simulate this molecule for new drug development, suggesting that miRNA may provide a new means for the treatment of human diseases (Liu et al. 2016b).
In this review, we summarized the current understanding of miRNA-mediated modulation of the gene expression in the pathogenesis of fatty liver in recent years. According to the research reports, miRNAs were involved in the mechanism of obesity, the lipid metabolism, the glucose metabolism, the NASH pathogenesis, the bile metabolism, and the mechanism of remote ischemic preconditioning. We also reviewed the roles of miRNAs in the pathogenesis of ALD and their molecular mechanisms, and studies have shown that several miRNAs significantly participated in the pathogenesis of ALD. miRNAs play important roles in the pathological process of fatty liver and attract more and more researchers’ attention. With the further study on the mechanism of miRNA and fatty liver, it will make us to understand the pathogenesis of fatty liver to a new level.
Change history
03 August 2018
The original version of this article unfortunately contained an error in the Acknowledgement section. The corrected text has been given below:
Abbreviations
- miRNAs:
-
microRNAs
- NAFLD:
-
Non-alcoholic fatty liver disease
- MAPK:
-
Mitogen-activated protein kinase
- HCC:
-
Hepatocellular carcinoma
- ALD:
-
Alcoholic liver disease
- NOS:
-
Nitric oxide synthase
- TGF:
-
Transforming growth factor
- HMGCR:
-
3-Hydroxy-3-methylglutaryl-co-enzyme A reductase
- ER:
-
Endoplasmic reticulum
- 3′-UTR:
-
3′-untranslated regions
- NASH:
-
Non-alcoholic steatohepatitis
- SFA:
-
Saturated fatty acids
- HFD:
-
High-fat diet
- ABCA1:
-
ATP-binding cassette transporter A1
- MODY:
-
Maturity-onset diabetes of the young
- ERα:
-
Estrogen receptor alpha
- TLR:
-
Toll-like receptor
- TRAF6:
-
Tumor necrosis factor receptor-associated factor 6
- PTPN1:
-
Protein tyrosine phosphatase, non-receptor type 1
- INSR:
-
Insulin receptor
- PPARα:
-
Peroxisome proliferator-activated receptor α
- DCA:
-
Deoxycholic acid
- RIPC:
-
Remote ischemic preconditioning
- SREBP1:
-
Sterol regulatory element-binding protein 1
- CPT1a:
-
Carnitine palmitoyltransferase 1a
- CGI-58:
-
Comparative gene identification 58
- LDL:
-
Low-density lipoprotein
- VLDL:
-
Very low-density lipoprotein
- IRAK1:
-
IL-1 receptor-associated kinase 1
- DKO:
-
Double knockout
- VAT:
-
Visceral adipose tissue
- HDL:
-
High-density lipoprotein
- SCD:
-
Stearoyl coenzyme A desaturase-1
- AMPK:
-
AMP-activated protein kinase
- ZO-1:
-
Zonula Occludens-1
- iNOS:
-
Inducible nitric oxide synthase
- CTDSP:
-
C-terminal domain RNA polymerase II polypeptide A small phosphatase
- INSIG:
-
Insulin-induced gene
- XOS:
-
Xylo-oligosaccharides
References
Akhlaghi M (2016) Non-alcoholic fatty liver disease: beneficial effects of flavonoids. Phytother Res 30(10):1559–1571
Akuta N, Kawamura Y, Suzuki F, Saitoh S, Arase Y, Fujiyama S et al (2016a) Analysis of association between circulating miR-122 and histopathological features of nonalcoholicfatty liver disease in patients free of hepatocellular carcinoma. BMC Gastroenterol 16(1):141–148
Akuta N, Kawamura Y, Suzuki F, Saitoh S, Arase Y, Kunimoto H et al (2016b) Impact of circulating miR-122 for histological features and hepatocellular carcinoma of nonalcoholicfatty liver disease in Japan. Hepatol Int 10(4):647–656
An X, Sarmiento C, Tan T, Zhu H (2017) Regulation of multidrug resistance by microRNAs in anti-cancer therapy. Acta Pharm Sin B 7(1):38–51
Ao R, Wang Y, Tong J, Wang BF (2016) Altered microRNA-9 expression level is directly correlated with pathogenesis of nonalcoholic fatty liver disease by targeting Onecut2 and SIRT1. Med Sci Monit 22:3804–3819
Arora H, Qureshi R, Rizvi MA, Shrivastava S, Parihar MS (2016) Study of apoptosis-related interactions in colorectal cancer. Tumour Biol 37(11):14415–14425
Auguet T, Aragonès G, Berlanga A, Guiu-Jurado E, Martí A, Martínez S (2016) miR33a/miR33b* and miR122 as possible contributors to hepatic lipid metabolism in obese women with nonalcoholic fatty liver disease. Int J Mol Sci 17(10):E1620
Baffy G (2015) MicroRNAs in nonalcoholic fatty liver disease. J Clin Med 4(12):1977–1988
Bala S, Csak T, Saha B, Zatsiorsky J, Kodys K, Catalano D et al (2016) The pro-inflammatory effects of miR-155 promote liver fibrosis and alcohol-induced steatohepatitis. J Hepatol 64(6):1378–1387
Barciszewska AM (2016) MicroRNAs as efficient biomarkers in high-grade gliomas. Folia Neuropathol 54(4):369–374
Becker PP, Rau M, Schmitt J, Malsch C, Hammer C, Bantel H et al (2015) Performance of serum microRNAs -122, -192 and -21 as biomarkers in patients with non-alcoholic steatohepatitis. PLoS ONE 10(11):e0142661
Benatti RO, Melo AM, Borges FO (2014) Maternal high-fat diet consumption modulates hepatic lipid metabolism and microRNA-122 (miR-122) and microRNA-370 (miR-370) expression in offspring. Br J Nutr 111:2112–2122
Bhat A, Sebastiani G, Bhat M (2015) Systematic review: preventive and therapeutic applications of metformin in liver disease. World J Hepatol 7(12):1652–1659
Boursier J, Diehl AM (2016) Nonalcoholic fatty liver disease and the gut microbiome. Clin Liver Dis 20(2):263–275
Boutari C, Perakakis N, Mantzoros CS (2018) Association of adipokines with development and progression of nonalcoholic fatty liver disease. Endocrinol Metab 33(1):33–43
Castro RE, Ferreira DM, Afonso MB, Borralho PM, Machado MV, Cortez-Pinto H et al (2013) miR-34a/SIRT1/p53 is suppressed by ursodeoxycholic acid in the rat liver and activated by disease severity in human non-alcoholic fatty liver disease. J Hepatol 58(1):119–125
Cheng Y, Mai J, Hou T, Ping J (2016) MicroRNA-421 induces hepatic mitochondrial dysfunction in non-alcoholic fatty liver disease mice by inhibiting sirtuin 3. Biochem Biophys Res Commun 474(1):57–63
Csak T, Bala S, Lippai D, Kodys K, Catalano D, Iracheta-Vellve A et al (2015) MicroRNA-155 deficiency attenuates liver steatosis and fibrosis without reducing inflammation in a mouse model of steatohepatitis. PLoS ONE 10(6):e0129251
Das SK, Stadelmeyer E, Schauer S, Schwarz A, Strohmaier H, Claudel T et al (2015) Micro RNA-124a regulates lipolysis via adipose triglyceride lipase and comparative gene identification 58. Int J Mol Sci 16(4):8555–8568
Dattaroy D, Pourhoseini S, Das S, Alhasson F, Seth RK, Nagarkatti M et al (2015) Micro-RNA 21 inhibition of SMAD7 enhances fibrogenesis via leptin-mediated NADPH oxidase in experimental and human nonalcoholic steatohepatitis. Am J Physiol Gastrointest Liver Physiol 308(4):298–312
Daugaard I, Hansen TB (2017) Biogenesis and function of ago-associated RNAs. Trends Genet 33(3):208–219
de Paula Simino LA, de Fante T, Figueiredo Fontana M, Oliveira Borges F, Torsoni MA, Milanski M et al (2017) Lipid overload during gestation and lactation can independently alter lipid homeostasis in offspring and promote metabolic impairment after new challenge to high-fat diet. Nutr Metab 14(16):2017. https://doi.org/10.1186/s12986-017-0168-4
Ding J, Li M, Wan X, Jin X, Chen S, Yu C et al (2015) Effect of miR-34a in regulating steatosis by targeting PPARα expression in nonalcoholic fatty liverdisease. Sci Rep 5:13729
Du WW, Liu F, Shan SW, Ma XC, Gupta S, Jin T et al (2015) Inhibition of dexamethasone-induced fatty liver development by reducing miR-17-5p levels. Mol Ther 23(7):1222–1233
Duan YF, Sun DL, Chen J, Zhu F, An Y (2017) MicroRNA-29a/b/c targets iNOS and is involved in protective remote ischemic preconditioning in an ischemia-reperfusion rat model of non-alcoholic fatty liver disease. Oncol Lett 13(3):1775–1782
Elhanati S, Ben-Hamo R, Kanfi Y, Varvak A, Glazz R, Lerrer B et al (2016) Reciprocal regulation between SIRT6 and miR-122 controls liver metabolism and predicts hepatocarcinoma prognosis. Cell Rep 14(2):234–242
Fu X, Dong B, Tian Y, Lefebvre P, Meng Z, Wang X et al (2015) MicroRNA-26a regulates insulin sensitivity and metabolism of glucose and lipids. J Clin Invest 125(6):2497–2509
Gracia A, Fernández-Quintela A, Miranda J, Eseberri I, González M, Portillo MP (2017) Are miRNA-103, miRNA-107 and miRNA-122 involved in the prevention of liver steatosis induced by resveratrol? Nutrients 9(4):360. https://doi.org/10.3390/nu9040360
Handzlik-Orlik G, Holecki M, Wilczyński K, Duława J (2016) Osteoporosis in liver disease: pathogenesis and management. Ther Adv Endocrinol Metab 7(3):128–135
Hanin G, Yayon N, Tzur Y, Haviv R, Bennett ER, Udi S et al (2017) miRNA-132 induces hepatic steatosis and hyperlipidaemia by synergistic multitarget suppression. Gut. https://doi.org/10.1136/gutjnl-2016-312869
He Q, Li F, Li J, Li R, Zhan G, Li G et al (2017) MicroRNA-26a-interleukin (IL)-6-IL-17 axis regulates the development of non-alcoholic fatty liverdisease in a murine model. Clin Exp Immunol 187(1):174–184
Huang S, He X (2011) The role of microRNAs in liver cancer progression. Br J Cancer 104(2):235–240
Hur W, Lee JH, Kim SW, Kim JH, Bae SH, Kim M et al (2015) Downregulation of microRNA-451 in non-alcoholic steatohepatitis inhibits fatty acid-induced proinflammatory cytokine production through the AMPK/AKT pathway. Int J Biochem Cell Biol 64:265–276
Irani S, Pan X, Peck BC, Iqbal J, Sethupathy P, Hussain MM (2016) MicroRNA-30c mimic mitigates hypercholesterolemia and atherosclerosis in mice. J Biol Chem 291(35):18397–18409
Jeon ES, Shin JH, Hwang SJ, Moon GJ, Bang OY, Kim HH (2014) Cobalt chloride induces neuronal differentiation of human mesenchymal stem cells through upregulation of microRNA-124a. Biochem Biophys Res Commun 444(4):581–587
Jiang W, Liu J, Dai Y, Zhou N, Ji C, Li X (2015) MiR-146b attenuates high-fat diet-induced non-alcoholic steatohepatitis in mice. J Gastroenterol Hepatol 30(5):933–943
Kim SJ, Kang HS, Lee JH, Park JH, Jung CH, Bae JH et al (2015) Melatonin ameliorates ER stress-mediated hepatic steatosis through miR-23a in the liver. Biochem Biophys Res Commun 458(3):462–469
Kumar S, Singh J, Rattan S, DiMarino AJ, Cohen S, Jimenez SA (2017) Review article: pathogenesis and clinical manifestations of gastrointestinal involvement in systemic sclerosis. Aliment Pharmacol Ther 45(7):883–898
Kurtz CL, Fannin EE, Toth CL, Pearson DS, Vickers KC, Sethupathy P (2015) Inhibition of miR-29 has a significant lipid-lowering benefit through suppression of lipogenic programs in liver. Sci Rep 5:12911
Li D, Wang X, Lan X, Li Y, Liu L, Yi J et al (2015) Down-regulation of miR-144 elicits proinflammatory cytokine production by targeting toll-like receptor 2 in nonalcoholic steatohepatitis of high-fat-diet-induced metabolic syndrome E3 rats. Mol Cell Endocrinol 402:1–12
Li DD, Liu Y, Xue L, Su DY, Pang WY (2017a) Up-regulation of microRNA-367 promotes liver steatosis through repressing TBL1 in obese mice. Eur Rev Med Pharmacol Sci 21(7):1598–1603
Li M, He Y, Zhou Z, Ramirez T, Gao Y, Gao Y et al (2017b) MicroRNA-223 ameliorates alcoholic liver injury by inhibiting the IL-6-p47 < sup > phox </sup > -oxidative stress pathway in neutrophils. Gut 66(4):705–715
Lim E, Lim JY, Kim E, Kim YS, Shin JH, Seok PR et al (2016) Xylobiose, an alternative sweetener, ameliorates diabetes-related metabolic changes by regulating hepatic lipogenesis and miR-122a/33a in db/db mice. Nutrients 8(12):E791
Lin X, Jia J, Du T, Li W, Wang X, Wei J et al (2015) Overexpression of miR-155 in the liver of transgenic mice alters the expression profiling of hepatic genes associated with lipid metabolism. PLoS ONE 10(3):e0118417
Liu X, Zhao J, Liu Q, Xiong X, Zhang Z, Jiao Y et al (2016a) MicroRNA-124 promotes hepatic triglyceride accumulation through targeting tribbles homolog 3. Sci Rep 6:37170
Liu XL, Pan Q, Zhang RN, Shen F, Yan SY, Sun C et al (2016b) Disease-specific miR-34a as diagnostic marker of non-alcoholic steatohepatitis in a Chinese population. World J Gastroenterol 22(44):9844–9852
Liu MX, Gao M, Li CZ, Yu CZ, Yan H, Peng C et al (2017) Dicer1/miR-29/HMGCR axis contributes to hepatic free cholesterol accumulation in mouse non-alcoholic steatohepatitis. Acta Pharmacol Sin 38(5):660–671
Loyer X, Paradis V, Hénique C, Vion AC, Colnot N, Guerin CL et al (2016) Liver microRNA-21 is overexpressed in non-alcoholic steatohepatitis and contributes to the disease in experimental models by inhibiting PPARα expression. Gut 65(11):1882–1894
Mattis AN, Song G, Hitchner K, Kim RY, Lee AY, Sharma AD et al (2015) A screen in mice uncovers repression of lipoprotein lipase by microRNA-29a as a mechanism for lipid distribution away from the liver. Hepatology 61(1):141–152
Meng X, Guo J, Fang W, Dou L, Li M, Huang X et al (2016) Liver MicroRNA-291b-3p promotes hepatic lipogenesis through negative regulation of adenosine 5′-monophosphate (AMP)-activated protein kinase α1. J Biol Chem 291(20):10625–10634
Miya Shaik M, Tamargo IA, Abubakar MB, Kamal MA, Greig NH, Gan SH (2018) The role of microRNAs in Alzheimer’s disease and their therapeutic potentials. Genes 9(4):E174
Mooradian AD, Haas MJ (2015) Targeting high-density lipoproteins: increasing de novo production versus decreasing clearance. Drugs 75(7):713–722
Mysore R, Zhou Y, Sädevirta S, Savolainen-Peltonen H, Nidhina Haridas PA, Soronen J et al (2016) MicroRNA-192* impairs adipocyte triglyceride storage. Biochim Biophys Acta 1861(4):342–351
Natarajan SK, Stringham BA, Mohr AM, Wehrkamp CJ, Lu S, Phillippi MA et al (2017) FoxO3 increases miR-34a to cause palmitate-induced cholangiocyte lipoapoptosis. J Lipid Res 58(5):866–875
Peng JF, Liu L, Guo CX, Liu SK, Chen XP, Huang LH et al (2015) Role of miR-511 in the regulation of OATP1B1 expression by free fatty acid. Biomol Ther 23(5):400–406
Pourhoseini S, Seth RK, Das S, Dattaroy D, Kadiiska MB, Xie G et al (2015) Upregulation of miR21 and repression of Grhl3 by leptin mediates sinusoidal endothelial injury in experimental nonalcoholic steatohepatitis. PLoS ONE 10(2):e0116780
Qiang J, Tao YF, He J, Sun YL, Xu P (2017) miR-29a modulates SCD expression and is regulated in response to a saturated fatty acid diet in juvenile genetically improved farmed tilapia (Oreochromis niloticus). J Exp Biol 220(Pt 8):1481–1489
Raitoharju E, Seppälä I, Lyytikäinen LP, Viikari J, Ala-Korpela M, Soininen P et al (2016) Blood hsa-miR-122-5p and hsa-miR-885-5p levels associate with fatty liver and related lipoprotein metabolism: The Young Finns Study. Sci Rep 6:38262
Rastinejad F, Huang P, Chandra V, Khorasanizadeh S (2013) Understanding nuclear receptor form and function using structural biology. J Mol Endocrinol 51(3):T1–T21
Rodrigues PM, Afonso MB, Simão AL, Borralho PM, Rodrigues CMP, Castro RE (2015) Inhibition of NF-κB by deoxycholic acid induces miR-21/PDCD4-dependent hepatocelular apoptosis. Sci Rep 5:17528
Rodrigues PM, Afonso MB, Simão AL, Carvalho CC, Trindade A, Duarte A et al (2017) miR-21 ablation and obeticholic acid ameliorate nonalcoholic steatohepatitis in mice. Cell Death Dis 8(4):e2748
Rupaimoole R, Slack FJ (2017) MicroRNA therapeutics: towards a new era for the management of cancer and other diseases. Nat Rev Drug Discov 16(3):203–222
Saha B, Bruneau JC, Kodys K, Szabo G (2015) Alcohol-induced miR-27a regulates differentiation and M2 macrophage polarization of normal human monocytes. J Immunol 194(7):3079–3087
Salvoza NC, Klinzing DC, Gopez-Cervantes J, Baclig MO (2016) Association of circulating serum miR-34a and miR-122 with dyslipidemia among patients with non-alcoholic fatty liver disease. PLoS ONE 11(4):e0153497
Shan W, Gao L, Zeng W, Hu Y, Wang G, Li M et al (2015) Activation of the SIRT1/p66shc antiapoptosis pathway via carnosic acid-induced inhibition of miR-34a protects rats against nonalcoholic fatty liver disease. Cell Death Dis 6:e1833
Sharma SK, Verma SH (2016) A study of effects of pioglitazone and rosiglitazone on various parameters in patients of Type-2 diabetes mellitus with special reference to lipid profile. J Assoc Physicians India 64(9):24–28
Silva Figueiredo P, Inada AC, Ribeiro Fernandes M, Granja Arakaki D, Freitas KC, Avellaneda Guimarães RC (2018) An overview of novel dietary supplements and food ingredients in patients with metabolic syndrome and non-alcoholic fatty liver disease. Molecules 23(4):E877
Steinacher D, Claudel T, Trauner M (2017) Therapeutic mechanisms of bile acids and nor-ursodeoxycholic acid in non-alcoholic fatty liver disease. Dig Dis 35(3):282–287
Stewart CJ, Charles A, Foulkes WD (2016) Gynecologic manifestations of the DICER1 syndrome. Surg Pathol Clin 9(2):227–241
Stickel F, Datz C, Hampe J, Bataller R (2017) Pathophysiology and management of alcoholic liver disease: update 2016. Gut Liver 11(2):173–188
Su D, Zhang R, Hou F, Chi J, Huang F, Yan S et al (2017) Lychee pulp phenolics ameliorate hepatic lipid accumulation by reducing miR-33 and miR-122 expression in mice fed a high-fat diet. Food Funct 8(2):808–815
Sun C, Huang F, Liu X, Xiao X, Yang M, Hu G et al (2015) miR-21 regulates triglyceride and cholesterol metabolism in non-alcoholic fatty liver disease by targeting HMGCR. Int J Mol Med 35(3):847–853
Suzuki M (2017) Regulation of lipid metabolism via a connection between the endoplasmic reticulum and lipid droplets. Anat Sci Int 92(1):50–54
Tang Y, Zhang L, Forsyth CB, Shaikh M, Song S, Keshavarzian A (2015) The role of miR-212 and iNOS in alcohol-induced intestinal barrier dysfunction and steatohepatitis. Alcohol Clin Exp Res 39(9):1632–1641
Tian H, Liu C, Zou X, Wu W, Zhang C, Yuan D (2015) MiRNA-194 regulates palmitic acid-induced toll-like receptor 4 inflammatory responses in THP-1 cells. Nutrients 7(5):3483–3496
Virtue A, Johnson C, Lopez-Pastraña J, Shao Y, Fu H, Li X et al (2017) MicroRNA-155 deficiency leads to decreased atherosclerosis, increased white adipose tissue obesity, and non-alcoholic fatty liver disease: a novel mouse model of obesity paradox. J Biol Chem 292(4):1267–1287
Walsh JS, Vilaca T (2017) Obesity, Type 2 diabetes and bone in adults. Calcif Tissue Int 100(5):528–535
Wang H, Luo J, Zhang T, Tian H, Ma Y, Xu H et al (2016a) MicroRNA-26a/b and their host genes synergistically regulate triacylglycerol synthesis by targeting the INSIG1 gene. RNA Biol 13(5):500–510
Wang L, Zhang N, Wang Z, Ai DM, Cao ZY, Pan HP (2016b) Decreased MiR-155 level in the peripheral blood of non-alcoholic fatty liver disease patients may serve as a biomarker and may influence LXR activity. Cell Physiol Biochem 39(6):2239–2248
Wei S, Zhang M, Yu Y, Xue H, Lan X, Liu S et al (2016) HNF-4α regulated miR-122 contributes to development of gluconeogenesis and lipid metabolism disorders in Type 2 diabetic mice and in palmitate-treated HepG2 cells. Eur J Pharmacol 791:254–263
Willeit P, Skroblin P, Moschen AR, Yin X, Kaudewitz D, Zampetaki A et al (2017) Circulating MicroRNA-122 is associated with the risk of new-onset metabolic syndrome and Type 2 diabetes. Diabetes 66(2):347–357
Woolbright BL, Jaeschke H (2018) Alcoholic hepatitis: lost in translation. J Clin Transl Hepatol 6(1):89–96
Wu H, Ng R, Chen X, Steer CJ, Song G (2016) MicroRNA-21 is a potential link between non-alcoholic fatty liver disease and hepatocellular carcinoma via modulation of the HBP1-p53-Srebp1c pathway. Gut 65(11):1850–1860
Wu H, Zhang T, Pan F, Steer CJ, Li Z, Chen X et al (2017) MicroRNA-206 prevents hepatosteatosis and hyperglycemia by facilitating insulin signaling and impairing lipogenesis. J Hepatol 66(4):816–824
Xiao J, Bei Y, Liu J, Dimitrova-Shumkovska J, Kuang D, Zhou Q et al (2016) miR-212 downregulation contributes to the protective effect of exercise against non-alcoholic fatty liver via targeting FGF-21. J Cell Mol Med 20(2):204–216
Xu Q, Li Y, Shang YF, Wang HL, Yao MX (2015a) miRNA-103: molecular link between insulin resistance and nonalcoholic fatty liver disease. World J Gastroenterol 21(2):511–516
Xu Y, Zalzala M, Xu J, Li Y, Yin L, Zhang Y (2015b) A metabolic stress-inducible miR-34a-HNF4α pathway regulates lipid and lipoprotein metabolism. Nat Commun 6:7466
Xu T, Zhou J, Zhu J, Zhang S, Zhang N, Zhao Y et al (2017) Carnosic acid protects non-alcoholic fatty liver-induced dopaminergic neuron injury in rats. Metab Brain Dis 32(2):483–491
Yamada H, Ohashi K, Suzuki K, Munetsuna E, Ando Y, Yamazaki M et al (2015) Longitudinal study of circulating miR-122 in a rat model of non-alcoholic fatty liver disease. Clin Chim Acta 446:267–271
Yang WM, Jeong HJ, Park SW, Lee W (2015) Obesity-induced miR-15b is linked causally to the development of insulin resistance through the repression of the insulin receptor in hepatocytes. Mol Nutr Food Res 59(11):2303–2314
Yang WM, Min KH, Lee W (2016) Induction of miR-96 by dietary saturated fatty acids exacerbates hepatic insulin resistance through the suppression of INSR and IRS-1. PLoS ONE 11(12):e0169039
Yin H, Liang X, Jogasuria A, Davidson NO, You M (2016) miR-217 regulates ethanol-induced hepatic inflammation by disrupting sirtuin 1-lipin-1 signaling. Am J Pathol 185(5):1286–1296
Zarrinpar A, Gupta S, Maurya MR, Subramaniam S, Loomba R (2016) Serum microRNAs explain discordance of non-alcoholic fatty liver disease in monozygotic and dizygotic twins: a prospective study. Gut 65(9):1546–1554
Zhang N, Lei J, Lei H, Ruan X, Liu Q, Chen Y et al (2015a) MicroRNA-101 overexpression by IL-6 and TNF-α inhibits cholesterol efflux by suppressing ATP-binding cassette transporter A1 expression. Exp Cell Res 336(1):33–42
Zhang ZC, Liu Y, Xiao LL, Li SF, Jiang JH, Zhao Y et al (2015b) Upregulation of miR-125b by estrogen protects against non-alcoholic fatty liver in female mice. J Hepatol 63(6):1466–1475
Zhang YJ, Hu Y, Li J, Chi YJ, Jiang WW, Zhang F et al (2017) Roles of microRNAs in immunopathogenesis of non-alcoholic fatty liver disease revealed by integrated analysis of microRNA and mRNA expression profiles. Hepatobiliary Pancreat Dis Int 16(1):65–79
Zhao XY, Shao K (2016) Roles of microRNA-21 in the pathogenesis of insulin resistance and diabetic mellitus-induced non-alcoholic fatty liver disease. Acta Acad Med Sin 38(2):144–149
Zheng Y, Jiang S, Zhang Y, Zhang R, Gong D (2015) Detection of miR-33 expression and the verification of its target genes in the fatty liver of geese. Int J Mol Sci 16(6):12737–12752
Zhou L, Hussain MM (2017) Human MicroRNA-548p decreases hepatic apolipoprotein B secretion and lipid synthesis. Arterioscler Thromb Vasc Biol 37(5):786–793
Acknowledgements
This project was supported by the National Science Foundation of China (No. 81302783), the Stable Talent Personnel Project of Anhui Science and Technology University (No. ZRC2014473), and Excellent talent project of Anhui Science and Technology University (No. XJYXRC201801).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Miao, C., Xie, Z. & Chang, J. Critical Roles of microRNAs in the Pathogenesis of Fatty Liver: New Advances, Challenges, and Potential Directions. Biochem Genet 56, 423–449 (2018). https://doi.org/10.1007/s10528-018-9870-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10528-018-9870-9