Abstract
Background
The late-stage diagnosis and distant metastasis of oral squamous cell carcinoma (OSCC) remain a huge challenge to clinical treatment for OSCC. During the past decades, targeting glycolysis-inducing factors becomes an attractive new strategy in OSCC therapies.
Methods
OSCC cells were stimulated with hypoxia or transfected with agomir-199a-5p, antagomir-199a-5p, and siRNA for HIF1A, cell proliferation was detected by CCK-8 assay; HIF1α, GLUT1, HK2 and LDHA expression levels were examined with western blot; miR-199 expression was determined with RT-PCR; cell migratory and invasive abilities were examined using wound healing and transwell assays; the lactate and glucose in culture medium were also determined. Luciferase assay or CHIP assay was applied for confirm the binding between miR-199a-5p and HIF1A 3′UTR, or between HIF1α and miR-199a promoter.
Results
HIF1α showed to be abnormally up-regulated, and miR-199a-5p showed to be abnormally down-regulated within OSCC under hypoxia. Hypoxia considerably enhanced OSCC cell proliferation, glycolysis, migratory ability, and invasive ability. MiR-199a-5p bound to HIF1A 3′‐UTR and suppressed HIF1A expression; HIF1α targeted miR-199a-5p promoter region and downregulated miR-199a-5p expression. Under hypoxia, miR-199a-5p overexpression significantly repressed HIF1α up-regulation inresponse to hypoxia, OSCC cell proliferation, glycolysis, migratory ability, and invasive ability.
Conclusion
miR-199a-5p and HIF1α form a dual-regulatory axis in OSCC cells; the miR-199a-5p/HIF1α dual-regulatory axis contributes to hypoxia-induced aggressive OSCC phenotypes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oral squamous cell carcinoma, which arises from the mucosal surfaces lining the oral cavity, pharynx, and larynx, is one of the most commonly seen malignancies globally [1]. Over the long term, the overall 5-year relative survival rate of oral cancer patients did not change remarkably [2]. The high mortality rate in oral cancer patients could be mainly attributed to late stage diagnosis and distant metastasis [3]. Developing the understanding of the genetic changes and molecular mechanisms of OSCC progression may provide new strategies for early diagnosis and targeted therapy.
Hypoxia is one of the main characteristics of solid tumors, and has been shown to correlate with aggressive behaviors of tumors and impaired prognosis of cancer patients. Induced by hypoxia, HIF1α (the hypoxia‐inducible transcription factor 1α) acts as a critical molecule involved in the modulation of hypoxia and glucose metabolism of tumor cells. Together with the GLUT-1 (glucose transporter 1) and HK2 (Hexokinase 2), these three factors exert critical effects on tumor cell glycolysis [4] and, subsequently, are tightly associated with OSCC nodal metastasis [5, 6]. Considering that HIF1α is commonly upregulated in OSCC [7, 8], searching for agent that efficiently block HIF1α might provide promising strategies for OSCC treatment.
MicroRNAs (miRNAs) are a large group of, small, noncoding, endogenous RNA molecules, which act as regulators in gene expression [9, 10]. A variety of studies have demonstrated that miRNAs could perform their functions as tumor screening, diagnostic and prognostic biomarkers [11, 12]. MiR-199a-5p attracted our attention because of its aberrant downregulation and tumor-suppressive role in several cancers [13,14,15]. Given these findings, it is worthwhile to examine the specific effects of miR-199a-5p on OSCC glycolysis. More importantly, by using Targetscan, we identified the possible miR-199a-5p binding site in HIF1A; JASPER and TransmiR v2.0 predicted the HIF1α binding site in miR-199a-5p promoter region. Considering these findings, miR-199a-5p was selected for further study.
Herein, we examined both HIF1α and miR-199a-5p expression within OSCC cells exposed to normoxia or hypoxia. Then, hypoxia-induced changes in OSCC cell phenotypes, including glycolysis, migration, and invasion were monitored. The predicted bindings between miR-199a-5p and HIF1A 3′-UTR, and HIF1α and miR-199a-5p promoter region were verified. Finally, the dynamic effects of miR-199a-5p and hypoxia-induced HIF1α on the phenotypes of OSCC cells were investigated.
Materials and methods
Cell lineage and cell culture
Human tongue squamous cell carcinoma cell line CAL-27 (CRL-2095) was collected from ATCC (Manassas, USA) and cultured in Dulbecco’s Modified Eagle’s Medium (DMEM, Gibco, Waltham, USA) supplemented with 10% FBS (Invitrogen, Waltham, USA). Human tongue squamous cell carcinoma cell line SCC-9 (CRL-1629) was procured from ATCC and cultivated within a 1:1 mixture of DMEM media and Ham’s F12 media (Gibco) added with 10% FBS (Invitrogen). All cells were cultured at 37 °C in a humidified atmosphere containing 5% CO2. For hypoxia treatment, cells were grown in airtight chambers with an atmosphere mixed of 5% CO2, 94% N2 and 1% O2.
Cell transfection
miR-199a-5p overexpression or miR-199a-5p inhibition was achieved by the trasfection of agomiR-199a-5p/antagomir199a-5p (GenePharma, Shanghai, China). The small interfering RNA targeting HIF1A (si-HIF1A)/HIF1A-overexpressing vector (HIF1A) was transfected to achieve HIF1A knockdown/overexpression [16]. Then, these plasmids in target cells were transfected using Lipofectamine 3000 Reagent (Thermo fisher scientific, Waltham, USA). The sequences of si-HIF1A, HIF1A-overexpressing vector, agomiR-199a-5p/antagomir199a-5p are listed in Table S1.
Immunoblotting
The total protein was isolated from target cells by centrifugation and the protein sample content was evaluated according to the BCA method. Then, following electrophoresis by SDS-PAGE, the separated proteins were electroblotted from the gel on PVDF membranes. 5% milk blocking solution was employed to block the membranes for 1 h, followed by an overnight incubation at 4℃ with the following primary antibodies: anti-HIF1α (20960-1-AP, Proteintech, Wuhan, China), anti-GLUT1 (21829-1-AP, Proteintech), anti-lactate dehydrogenase A (LDHA; 19987-1-AP, Proteintech), anti-HK2 (MBS475044, MyBioSource, San Diego, USA), anti-VEGFA (19003-1-AP, Proteintech), anti-EPO (17908-1-AP, Proteintech), and anti-β-actin (60008-1-Ig, Proteintech), followed by an 1-h incubation at room temperature (RT) with secondary antibodies (HRP-labeled goat anti-rabbit IgG and goat anti-mouse IgG). The signal was detected using ECL chemiluminescence method.
RT-qPCR
mRNA, lncRNA, and miRNA expression levels were examined by RT-qPCR. TRIzol reagent was utilized to collect total RNA. Then, RNA reversely transcribed into cDNA. Using a SYBR-Green Real-time PCR Master Mix, the RT-qPCR assay was conducted on a real-time PCR amplification equipment. β-actin (for mRNA) or U6 (for miRNA) was utilized as an internal reference. The primer sequence is represented in Table S1.
Wound healing assay for cell migration
Target cells (5 × 105 cells) were added to each well of 24-well plates and allowed to grow for 24 h. Next, one scratch was made with a pipette tip; the pipette tip was kept as perpendicular to the horizontal line as possible. Rinse the cells thrice with PBS, add complete media, incubate the cells at 37℃ in 5% CO2 for another 24 h, and then measure the migrating width and take pictures. Representative images were shown.
Transwell assay for cell invasion
Matrigel was diluted 1:5 with serum-free DMEM. After the addition of 80 μl mixture into the Transwell plate, the transwells were inserted into 24-well plates, followed by a 5-h incubation at 37℃ to solidify. After being digested with 0.25% trypsin, target cells were suspended in serum-free medium. Then, 200 μl cell suspension at a density of 5 × 105 cells/ml was planted to the top chamber, while 600 µl DMEM media containing 10% FBS was introduced into the bottom chamber. Following a 24-h incubation, a cotton swab was employed to remove the non-migrated cells upon the upper side of the membrane, and anhydrous methanol was applied to fix the remaining cells for 30 min, followed by a 2-h staining with 0.4% crystal violet. An optical microscope was employed to assess cell invasion across basement membrane [17].
Dual-luciferase reporter assay
The wild-type reporter vector (wt-HIF1A) was generated by fusing HIF1A 3′-UTR sequence with the binding sites of miR-199a-5p into luciferase reporter constructs (psicheck2 vector, Promega, Madison, USA); meanwhile, the mutant-type reporter vector (mut-HIF1A) was generated by using site-directed mutagenesis to mutate HIF1A 3′-UTR sequence containing the miR-199a-5p binding sites into luciferase reporter construct. Subsequently, using Lipofectamine 3000, 293T cells were co-transfected with agomiR-199a-5p/antagomiR-199a-5p with the reporter vectors and the luciferase activity was determined using Dual-Luciferase Reporter System (Promega) [18].
Wild- and mutant-type miR-199a-5p promoter reporter vectors were constructed, namely psicheck2-promiR-199a-5p and psicheck2-promiR-199a-5p-mut, for the binding between HIF1α and miR-199a-5p promoter. psicheck2-promiR-199a-5p/psicheck2-promiR-199a-5p-mut and HIF1α/vector were employed to co-transfect 293T cells. The luciferase activity was determined using Dual-Luciferase Reporter System (Promega).
Chromatin immunoprecipitation (ChIP)
The Pierce Agarose ChIP Kit (Pierce, Rockford, USA) was utilized as directed by the manufacturer’s protocol to conduct the ChIP assay. 293T cells were transfected with HIF1α/vector. Cross-linking was carried out in 1% formaldehyde, followed by cell lysis and nuclei preparation. Micronuclease digestion was employed to shear chromatin. Subsequently, anti-HIF1α antibody was applied to incubate sheared DNA. Normal immunoglobulin G (IgG) was utilized as a negative control. DNA was purified and analyzed using real-time PCR. Each primer is presented in Table S1.
Culture medium lactate and glucose levels
Lactate Assay Kit II (Eton Bioscience Inc., San Diego, USA) was employed to perform colorimetric assays as per the manufacturer’s protocol, subsequently analyzing the levels of lactate secreted into the medium. A Glucose Assay Kit (S0201S; Beyotime, Shanghai, China) was utilized as per the instructions to examine glucose levels in the culture media.
Cell counting kit-8 (CCK8) assay
CAL-27 and SCC-9 cells were planted onto 96-well plates (5 × 103 cells/well), followed by incubation at 37 °C. Following transfection and exposure to either normoxic or hypoxic conditions, each well was supplemented with 10 μl CCK-8 reagent (Beyotime), followed by 2-h incubation. The optical density (OD) of each well, indicative of cell viability, was determined with a microplate reader (BioTek, Winooski, USA) at 450 nm [19].
Statistical analysis
Statistical analyses were performed using SPSS 21.0 (IBM, Armonk, NY, USA). Data were presented in terms of means ± standard deviation (SD) of experimental results from at least three repetitions. Kolmogorov–Smirnov test showed whether the data were in normal distribution. A Student’s t test was carried out for comparisons between groups. One-way analysis of variance (ANOVA) followed by LSD test or Dunnett T3 test for comparisons among multi-groups. Not normally distributed data were analyzed by Kruskal–Wallis test. A P value of less than 0.05 was regarded as significant.
Results
Hypoxia increases HIF1α and decreases miR-199a-5p
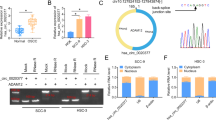
Firstly, we determined HIF1α and miR-199a-5p expression within CAL-27 and SCC-9 cells upon hypoxia to validate hypoxia-induced deregulation of these two factors. Under 1% O2 exposure, the protein levels of HIF1α were increased (Fig. 1A), whereas miR-199a-5p expression showed to be reduced within CAL-27 and SCC-9 cell lines (Fig. 1B). Thus, hypoxia induces HIF1α and miR-199a-5p deregulation within oral cancer cells.
Hypoxia increases HIF1α and decreases miR-199a-5p. CAL-27 and SCC-9 cells were exposed to 1% O2 and examined for the protein levels of HIF1α by Immunoblotting (A) and miR-199a-5p expression by qRT-PCR (B). Data are analyzed using unpaired Student’s t test. n = 3 in each group, ** P < 0.01, as compared to normoxia group
Hypoxia enhances the glycolysis, migration, and invasion of oral cancer cell
Secondly, we examined the effects of hypoxia upon CAL-27 and SCC-9 cell glycolysis, migration, and invasion. Under hypoxia condition (1% O2), GLUT1, HK2, and LDHA protein contents were all dramatically increased, as compared to those under normal oxygen (Fig. 2A). Meanwhile, hypoxia condition increased lactate levels and decreased glucose levels in culture medium, compared with those under normoxia condition (Fig. 2B, C). Moreover, hypoxia exposure significantly promoted cell migration and invasion of both cell lines, compared with that under normoxia condition (Fig. 2D, E).
Hypoxia promotes the glycolysis, migration, and invasion of oral cancer cell. CAL-27 and SCC-9 cells were exposed to 1% O2 and examined for the protein levels of GLUT1, HK2, and LDHA by Immunoblotting (A); lactate levels in culture medium (B); glucose levels in culture medium (C); cell migration by Wound healing assay (D); cell invasion by Transwell assay (E). Data are analyzed using unpaired Student’s t test. n = 3 in each group, * P < 0.05, ** P < 0.01, as compared to normoxia group
The dual-regulatory axis consists of miR-199a-5p and HIF1α
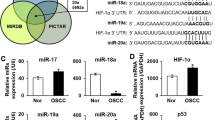
Since hypoxia induces the alterations in oral cancer cell phenotypes and miR-199a-5p and HIF1α levels, next, the regulation between miR-199a-5p and HIF1α was examined. AgomiR-199a-5p or antagomiR-199a-5p was transfected into cells to achieve miR-199a-5p overexpression or inhibition in CAL-27 and SCC-9 cell lines, as confirmed by qRT-PCR (Fig. 3A). In CAL-27 and SCC-9 cells, miR-199a-5p overexpression decreased, whereas miR-199a-5p inhibition elevated HIF1α proteins (Fig. 3B). To validate the negative regulatory effect of miR-199a-5p on HIF1α, dual-luciferase reporter assay was conducted. We constructed wild- and mutant-type HIF1A luciferase reporter vectors, and co-transfected them into 293T cells with agomiR-199a-5p/antagomiR-199a-5p; the predicted miR-199a-5p binding site in HIF1A was mutated. When co-transfected with wt-HIF1A, miR-199a-5p overexpression inhibited, while miR-199a-5p inhibition enhanced the luciferase activity of wt-HIF1A; when co-transfected with mut-HIF1A, miR-199a-5p caused no significant changes in luciferase activity (Fig. 3C).
The dual-regulatory axis consists of miR-199a-5p and HIF1α. A miR-199a-5p overexpression and inhibition was achieved in CAL-27 and SCC-9 cells by transfecting agomiR-199a-5p or antagomiR-199a-5p. The overexpression and inhibition of miR-199a-5p were confirmed by qRT-PCR. B CAL-27 and SCC-9 cells were transfected by agomiR-199a-5p or antagomiR-199a-5p and examined for the protein levels of HIF1α by Immunoblotting. C The binding sites of miR-199a-5p and HIF1α were predicted by TargetScanHuman 8.0 online database (https://www.targetscan.org/vert_80/). Then, Wild- and mutant-type HIF1A luciferase reporter vectors were constructed and co-transfected to 293T cells with agomiR-199a-5p or antagomiR-199a-5p. Luciferase activity was determined. Data are analyzed using one-way ANOVA followed LSD test. n = 3 in each group; * P < 0.05, ** P < 0.01, as compared to agomir-NC group; # P < 0.05, ## P < 0.01, as compared to antagomir-NC group. D HIF1α overexpression and knockdown were achieved in CAL-27 and SCC-9 cells by transfecting the HIF1α-overexpressing vector (HIF1α) or small interfering RNA targeting HIF1α (si-HIF1α). The overexpression and inhibition of HIF1α was confirmed by Immunoblotting. E CAL-27 and SCC-9 cells were transfected by HIF1α or si-HIF1α and examined for miR-199a-5p expression by qRT-PCR. Data are analyzed using one-way ANOVA followed LSD test. n = 3 in each group; ** P < 0.01, as compared to vector group; ## P < 0.01, as compared to si-NC group. F ChIP assay was performed in 293T cells transfected with vector or HIF1α using anti-IgG or anti-HIF1α. The levels of miR-199a-5p promoter in immunoprecipitate were determined by real-time PCR. Data are analyzed using unpaired Student’s t test. n = 3 in each group; ** P < 0.01, as compared to IgG group; ## P < 0.01, as compared to anti-HIF1α group. G Wild- and mutant-type miR-199a-5p luciferase reporter vectors, psicheck2-promiR-199a-5p or psicheck2-promiR-199a-5p-mut, were constructed and co-transfected to 293T cells with vector or HIF1α. The luciferase activity was determined. Data are analyzed using unpaired Student’s t test. n = 3 in each group, ** P < 0.01, ## P < 0.01 as compared to corresponding group
As for HIF1α regulation of miR-199a-5p, HIF1α-overexpressing vector (HIF1α) or small interfering RNA targeting HIF1α (si-HIF1α) was transfected to achieve HIF1α overexpression and knockdown in CAL-27 and SCC-9 cells, and Immunoblotting was carried out to verify the transfection efficiency (Fig. 3D). Within CAL-27 and SCC-9 cell lines, HIF1α overexpression downregulated, while HIF1α knockdown upregulated miR-199a-5p expression (Fig. 3E). As for predicted binding between HIF1α and the promoter region of miR-199a-5p, ChIP assay was performed within HIF1α/vector-transfected 293T cells using anti-IgG/anti-HIF1α. miR-199a-5p promoter levels within anti-HIF1α immunoprecipitate showed to be significantly higher as compared to anti-IgG immunoprecipitate, and miR-199a-5p promoter levels within HIF1α-transfected 293T cells showed to be significantly higher as compared to vector-transfected 293T cells (Fig. 3F). Furthermore, we conducted dual-luciferase reporter assay. We constructed wild- and mutant-type miR-199a-5p luciferase reporter vectors, namely psicheck2-promiR-199a-5p or psicheck2-promiR-199a-5p-mut, and co-transfected these reporter vectors into 293T cells with HIF1α/vector. When co-transfected with psicheck2-promiR-199a-5p, HIF1α overexpression significantly suppressed psicheck2-promiR-199a-5p luciferase activity; when co-transfected with psicheck2-promiR-199a-5p-mut containing mutated HIF1α binding site, HIF1α failed to change luciferase activity (Fig. 3G).
Dynamic effects of the miR-199a-5p/HIF1α dual-regulatory axis upon cancer cell phenotypes
Since the miR-199a-5p-HIF1α axis was reported to exert a dual-regulatory effect, next, we determined the dynamic effects of the axis upon the phenotypes of oral cancer cells. We transfected CAL-27 and SCC-9 cells with agomir-NC/agomiR-199a-5p, exposed to 1% or 20% O2, and examined for related indexes. When compared to normoxia condition, hypoxia significantly induced cancer cell proliferation; under normoxia or hypoxia conditions, miR-199a-5p overexpression notably inhibited cell proliferation; hypoxia treatment partially offseted the effect of miR-199a-5p overexpression on cell proliferation (Fig. 4A). As for glycolysis, hypoxia-induced miR-199a-5p inhibition increased HIF1α, GLUT1, HK2, and LDHA protein contents (Fig. 4B), increased culture medium lactate contents (Fig. 4C), and decreased culture medium glucose contents (Fig. 4D); conversely, miR-199a-5p overexpression reduced HIF1α, GLUT1, HK2, and LDHA protein contents (Fig. 4B), decreased culture medium lactate contents (Fig. 4C), and increased culture medium glucose contents (Fig. 4D). Moreover, under hypoxia, miR-199a-5p overexpression partially reversed hypoxia-induced changes in glycolysis (Fig. 4B–D). As for cell migration and invasion, hypoxia-induced miR-199a-5p inhibition enhanced, while miR-199a-5p overexpression inhibited oral cancer cell migration and invasion; similarly, under hypoxia, miR-199a-5p overexpression partially reversed hypoxia-induced changes in cell migration and invasion (Fig. 4E, F).
Dynamic effects of the miR-199a-5p/HIF1α dual-regulatory axis on cancer cell phenotypes. CAL-27 and SCC-9 cells were transfected with agomir-NC or agomiR-199a-5p, exposed to 1% or 20% O2, and examined for cell proliferation by CCK-8 assay (A); the protein levels of HIF1α, GLUT1, HK2, and LDHA by Immunoblotting (B); lactate levels in culture medium (C); glucose levels in culture medium (D); cell migration by Wound healing assay (E); cell invasion by Transwell assay (F). Data are analyzed using one-way ANOVA followed LSD test. n = 3 in each group; * P < 0.05, ** P < 0.01, compared with the Normoxia + agomir-NC group; ## P < 0.01, compared with the Hypoxia + agomiR-199a-5p group
Discussion
The present study found the aberrant increase of HIF1α and the abnormal reduction of miR-199a-5p in OSCC under hypoxia. Hypoxia dramatically enhanced the glycolysis, migratory ability, and invasive ability of OSCC cells. MiR-199a-5p bound to HIF1A 3′‐UTR and suppressed HIF1A expression; HIF1α targeted miR-199a-5p promoter region and down-regulated miR-199a-5p level. Under hypoxia, miR-199a-5p overexpression significantly repressed HIF1α up-regulation in response to hypoxia, the proliferation, glycolysis, migratory ability, and invasive ability of OSCC cells.
Hypoxia-induced HIF1α, which is essential for adaptive responses of the cells to hypoxia, inducing conformational changes under varying oxygen levels [20], serves as an oncogenic transcriptional factor in multiple cancers. Besides, hypoxia-regulated factor, VEGFA [21], GLUT1 [22], LDHA [23], and EPO [24], are also related to multiple tumor progression. The role of HIF1α in tumor progression is controversial, the increased protein level of HIF1α is frequently observed and correlated with poor prognosis in many cancer types, a long-lasting concept believes that HIF1α plays an oncogenic role in tumor growth [25, 26]. However, some studies challenged this concept. HIF1α deficiency apparently inhibited tumor growth and enhanced tumor invasion in microenvironment with sufficient oxygen supply [27]. HIF1α stabilization due to loss of VHL decreased tumor growth [28]. HIF1α can act as a tumor suppressor gene in murine acute myeloid leukemia [29]. In OSCC, several studies indicated the association of higher HIF1α levels with poorer prognosis [30, 31]. Consistently, here, we found the aberrant upregulation of HIF1α protein levels in OSCC cells under hypoxia, suggesting the oncogenic effect of HIF1α on OSCC cells. Notably, miR-199a-5p expression was dramatically reduced upon hypoxia within OSCC. The simultaneous alterations in miR-199a-5p and HIF1α expression suggest that these two factors might mediate OSCC cell phenotypes upon hypoxia.
HIF1α upregulation often accompanies highly aggressive tumor cell phenotypes. Herein, we observed hypoxia-induced increases in GLUT1, HK2, and LDHA levels. GLUT1 is a transmembrane protein facilitating the transport of glucose across a membrane [32]. HK2 is a major glycolytic enzyme that controls the first step of glycolysis and shows to be over-expressed within many malignancies [33]. LDHA, one of the glycolytic enzymes, helps in the rapid conversion of pyruvate to lactate and is correlated with cancer progression [34, 35]. Together with increased lactate levels and decreased glucose levels in the culture medium, these indexes demonstrated hypoxia-induced glycolysis by OSCC cells. In the meantime, hypoxia significantly promoted OSCC cell migration and invasion, further indicating hypoxia-induced aggressive phenotypes of OSCC cells.
miR-199a-5p has been revealed to serve as an antitumor miRNA within OSCC via binding to FDZ4 [13], SOX4 [14], or IKKβ [36]. Herein, miR-199a-5p targeted HIF1A and inhibited HIF1A expression. More importantly, as a transcriptional factor, HIF1α could activate or inhibit the transcription of downstream targets. For example, Li et al. [37] reported the direct binding of HIF1α to the HIF response element region of miR-21 under hypoxia. Herein, significantly higher miR-199a-5p promoter levels in anti-HIF1α immunoprecipitate compared with anti-IgG suggested the direct binding of HIF1α to the HIF response element region in miR-199a-5p. Within OSCC, HIF1α negatively modulated miR-199a-5p expression. Thus, miR-199a-5p and HIF1α form a dual-regulatory axis, negatively regulating each other. Since we already demonstrated hypoxia-induced aggressive OSCC cell phenotypes, secondly, the dynamic effects of the miR-199a-5p/HIF1α dual-regulatory axis on hypoxia-stimulated OSCC cells were examined. After overexpressing miR-199a-5p, hypoxia-induced OSCC cell proliferation, glycolysis, migration, and invasion were all partially reversed, indicating the involvement of miR-199a-5p/HIF1α dual-regulatory axis in hypoxia-induced aggressive phenotypes of OSCC cells.
However, the limitations of this study remain to be considered. Firstly, the HIF1A usually forms complexes with other genes, like HIF-beta [38], HDAC1 [39], p300 [40] and so on, to transcriptionally activates hundreds of genes promoting the adaptation to hypoxia that is implicated in tumor development. Hence, there could be other co-suppressors complex with HIF1A to regulate miR-199a-5p expression. Moreover, since all our experiments were carried out in cells, in future studies, we may employ experiments in animal models such as mice or rabbits.
Conclusion
Altogether, miR-199a-5p and HIF1α form a dual-regulatory axis in OSCC cells; the miR-199a-5p/HIF1α dual-regulatory axis participates in hypoxia-induced aggressive phenotypes of OSCC cells (Fig. 5).
Data availability
All data and materials are available.
References
Warnakulasuriya S (2009) Global epidemiology of oral and oropharyngeal cancer. Oral Oncol 45(4–5):309–316
Pulte D, Brenner H (2010) Changes in survival in head and neck cancers in the late 20th and early 21st century: a period analysis. Oncologist 15(9):994–1001
Siegel RL, Miller KD, Jemal A (2019) Cancer statistics, 2019. CA Cancer J Clin 69(1):7–34
Lu H, Forbes RA, Verma A (2002) Hypoxia-inducible factor 1 activation by aerobic glycolysis implicates the Warburg effect in carcinogenesis. J Biol Chem 277(26):23111–23115
Chang CC et al (2011) HDAC2 promotes cell migration/invasion abilities through HIF-1alpha stabilization in human oral squamous cell carcinoma. J Oral Pathol Med 40(7):567–575
Eckert AW et al (2011) Coexpression of hypoxia-inducible factor-1alpha and glucose transporter-1 is associated with poor prognosis in oral squamous cell carcinoma patients. Histopathology 58(7):1136–1147
Mohamed KM et al (2004) Correlation between VEGF and HIF-1alpha expression in human oral squamous cell carcinoma. Exp Mol Pathol 76(2):143–152
Guo M et al (2018) Comparison of the expression of TGF-beta1, E-cadherin, N-cadherin, TP53, RB1CC1 and HIF-1alpha in oral squamous cell carcinoma and lymph node metastases of humans and mice. Oncol Lett 15(2):1639–1645
Bartels CL, Tsongalis GJ (2009) MicroRNAs: novel biomarkers for human cancer. Clin Chem 55(4):623–631
Cortes-Sempere M, Ibanez de Caceres I (2011) microRNAs as novel epigenetic biomarkers for human cancer. Clin Transl Oncol 13(6):357–362
Wu Y et al (2017) MiR-375/SLC7A11 axis regulates oral squamous cell carcinoma proliferation and invasion. Cancer Med 6(7):1686–1697
Shin KH et al (2011) miR-181a shows tumor suppressive effect against oral squamous cell carcinoma cells by downregulating K-ras. Biochem Biophys Res Commun 404(4):896–902
Jiang X et al (2020) CCL18-induced LINC00319 promotes proliferation and metastasis in oral squamous cell carcinoma via the miR-199a-5p/FZD4 axis. Cell Death Dis 11(9):777
Wei D et al (2019) MicroRNA199a5p suppresses migration and invasion in oral squamous cell carcinoma through inhibiting the EMTrelated transcription factor SOX4. Int J Mol Med 44(1):185–195
Lou Z et al (2018) Low expression of miR-199 in hepatocellular carcinoma contributes to tumor cell hyper-proliferation by negatively suppressing XBP1. Oncol Lett 16(5):6531–6539
Bu XN et al (2016) Inhibition of DACH1 activity by short hairpin RNA represses cell proliferation and tumor invasion in pancreatic cancer. Oncol Rep 36(2):745–754
Li M et al (2022) MiR-26a-5p regulates proliferation, apoptosis, migration and invasion via inhibiting hydroxysteroid dehydrogenase like-2 in cervical cancer cell. BMC Cancer 22(1):876
Chang QQ et al (2019) LncRNA PVT1 promotes proliferation and invasion through enhancing Smad3 expression by sponging miR-140-5p in cervical cancer. Radiol Oncol 53(4):443–452
Liu Y et al (2022) Lysyl oxidase promotes anaplastic thyroid carcinoma cell proliferation and metastasis mediated via BMP1. Gland Surg 11(1):245–257
Sasabe E et al (2010) Reactive oxygen species produced by the knockdown of manganese-superoxide dismutase up-regulate hypoxia-inducible factor-1alpha expression in oral squamous cell carcinoma cells. Free Radic Biol Med 48(10):1321–1329
Chen H et al (2022) BMP9-ID1 signaling activates HIF-1α and VEGFA expression to promote tumor angiogenesis in hepatocellular carcinoma. Int J Mol Sci 23(3):1475
Ma P et al (2021) GLUT1 targeting and hypoxia-activating polymer-drug conjugate-based micelle for tumor chemo-thermal therapy. Drug Delivery 28(1):2256–2267
Wang X-H et al (2021) Hypoxia-induced FOXO4/LDHA axis modulates gastric cancer cell glycolysis and progression. Clin Transl Med 11(1):e279
Baltaziak M et al (2013) The relationships between hypoxia-dependent markers: HIF-1alpha, EPO and EPOR in colorectal cancer. Folia Histochem Cytobiol 51(4):320–325
Malekan M, Ebrahimzadeh MA, Sheida F (2021) The role of hypoxia-inducible factor-1alpha and its signaling in melanoma. Biomed Pharmacother 141:111873
Young RM, Simon MC (2012) Untuning the tumor metabolic machine: HIF-α: pro- and antitumorigenic? Nat Med 18(7):1024–1025
Blouw B et al (2003) The hypoxic response of tumors is dependent on their microenvironment. Cancer Cell 4(2):133–146
Mack FA et al (2003) Loss of pVHL is sufficient to cause HIF dysregulation in primary cells but does not promote tumor growth. Cancer Cell 3(1):75–88
Velasco-Hernandez T et al (2014) HIF-1α can act as a tumor suppressor gene in murine acute myeloid leukemia. Blood 124(24):3597–3607
Eckert AW et al (2010) HIF-1alpha is a prognostic marker in oral squamous cell carcinomas. Int J Biol Markers 25(2):87–92
Tilakaratne WM, Nissanka-Jayasuriya EH (2011) Value of HIF-1alpha as an independent prognostic indicator in oral squamous cell carcinoma. Expert Rev Mol Diagn 11(2):145–147
Augustin R (2010) The protein family of glucose transport facilitators: it’s not only about glucose after all. IUBMB Life 62(5):315–333
Mathupala SP, Ko YH, Pedersen PL (2009) Hexokinase-2 bound to mitochondria: cancer’s stygian link to the “Warburg Effect” and a pivotal target for effective therapy. Semin Cancer Biol 19(1):17–24
Girgis H et al (2014) Lactate dehydrogenase A is a potential prognostic marker in clear cell renal cell carcinoma. Mol Cancer 13:101
Sun X et al (2014) Clinicopathological significance and prognostic value of lactate dehydrogenase A expression in gastric cancer patients. PLoS ONE 9(3):e91068
Wei D et al (2019) MicroRNA199a5p functions as a tumor suppressor in oral squamous cell carcinoma via targeting the IKKbeta/NFkappaB signaling pathway. Int J Mol Med 43(4):1585–1596
Li L et al (2016) Exosomes derived from hypoxic oral squamous cell carcinoma cells deliver miR-21 to normoxic cells to elicit a prometastatic phenotype. Cancer Res 76(7):1770–1780
Martínez-Sáez O et al (2017) Targeting HIF-2 α in clear cell renal cell carcinoma: a promising therapeutic strategy. Crit Rev Oncol Hematol 111:117–123
Zhu S et al (2016) MiR-548an, transcriptionally downregulated by HIF1α/HDAC1, suppresses tumorigenesis of pancreatic cancer by targeting vimentin expression. Mol Cancer Ther 15(9):2209–2219
Reece KM et al (2014) Epidithiodiketopiperazines (ETPs) exhibit in vitro antiangiogenic and in vivo antitumor activity by disrupting the HIF-1α/p300 complex in a preclinical model of prostate cancer. Mol Cancer 13:91
Funding
This study was supported by the key clinical Specialty Construction Project (Head&Neck Surgery) of Provincial Health Commission of Hunan Province and the Natural Science Foundation of Hunan Province (Youth grant, 2020JJ5333).
Author information
Authors and Affiliations
Contributions
Xing Chen conception and design the experiments. Xing Chen and Jianjun Yu drafted the article. Xu Cai revised the article critically for important intellectual content. Xing Chen, Jianjun Yu, Hao Tian contributed to experiments, analysis and manuscript preparation. All the authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None.
Consent for publication
All the authors read and approved the manuscript.
Ethical approval and consent to participate
The Research Ethics Committee of the Xiangya School of Medicine approved all experiments.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Chen, X., Yu, J., Tian, H. et al. The miR-199a-5p/HIF1α dual-regulatory axis participates in hypoxia-induced aggressive phenotypes of oral squamous cell carcinoma (OSCC) cells. Int J Clin Oncol 29, 1244–1254 (2024). https://doi.org/10.1007/s10147-024-02555-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-024-02555-7