Abstract
The aim of the present study was to evaluate the effects of photobiomodulation (PBM) with the simultaneous use of red and infrared LEDs on pain and mandibular range of motion in individuals with temporomandibular disorder (TMD). Eighteen participants were randomly allocated to an LED group or control group. The device had 18 red LEDs (660 nm) and 18 infrared LEDs (850 nm), with a total power irradiated of 126 mW and 75.6 J per point. The device was placed in the regions of the temporomandibular joint (TMJ) and masticatory muscles once per day three times per week for 2 weeks. Pain intensity was measured using the visual analog scale (VAS). Mandibular range of motion was determined using digital calipers and considering different conditions (unassisted opening without pain, maximum opening with and without assistance, right and left lateral movements, and protrusion). Evaluations were performed before treatment, immediately after the first LED irradiation session and at the end of six sessions. A significant reduction in pain intensity was found in the LED group at the end of treatment compared to the control group (p < 0.001) as well as in the comparison between the pretreatment and end of treatment evaluations (p < 0.001). Regarding mandibular movements, no statistically significant differences between the LED group and control group were found at the end of treatment for any of the conditions analyzed or in the comparison between the beginning and end of treatment with LED. Photobiomodulation using a cluster with red and infrared LEDs induced a reduction in pain in individuals with temporomandibular disorder but did not alter mandibular range of motion in these individuals. Trial registration number: NCT03696706; retrospectively registered (ClinicalTrials.gov).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Temporomandibular disorder (TMD) is a generic term for clinical signs and symptoms that affect the temporomandibular joint (TMJ), masticatory muscles, and associated structures [1,2,3]. Due to the complexity of this condition, Freire et al. (2014) [4] suggest multidisciplinary treatment. Different non-surgical approaches have been used for the treatment of TMD, such as pharmacological resources [5, 6], the use of a rigid occlusal splint for myorelaxation [7], physiotherapeutic treatments, such as electrotherapy [8], massage therapy, and joint mobilizations [9, 10], and the use of therapeutic light (photobiomodulation) [11,12,13,14,15].
Photobiomodulation (PBM) is non-ionizing radiation that promotes the interaction of light and biological tissues, enabling photophysical effects with photochemical and photobiological responses [11]. PBM in the form of low-level laser therapy (LLLT) stimulates blood flow, promotes an anti-inflammatory response [16], and influences the synthesis, release, and metabolism of numerous signaling molecules involved in analgesia [17,18,19]. Other advantages of treatment with PBM included its ease of administration, noninvasive nature with minimal contraindications, and the possibility of shorter, low-cost treatments, making it a treatment option for individuals with TMD [1, 3, 20,21,22,23].
Light-emitting diodes (LEDs) constitute an attractive form of therapeutic PBM, with an increasing number of clinical trials demonstrating positive effects in cases of TMD [14, 15, 24]. PBM with LED achieves similar results as those found with the use of LLLT and offers the advantages of a more affordable device [25] and possibility of customization with clusters of multiple LEDs, enabling the irradiation of a larger area [24].
Studies suggest that red or infrared LED therapy increases muscle activity after the induction of masseter muscle fatigue [26], promotes pain relief of the masseter muscle [15, 27], and reduces the inflammatory process of the TMJ [28] in individuals with TMD. Furthermore, comparative studies in the literature report similar effects of red and infrared LED administered to the TMJ and masticatory muscles regarding pain relief and improvements in mandibular range of motion [29].
Herpich et al. (2017) [14] showed that the combination of different wavelengths is beneficial for individuals with TMD. The energy absorption rate and penetration into biological tissues differ between red and infrared spectra, enabling distinct cellular responses to this form of stimulus [14, 30]. However, no previous studies have investigated the simultaneous use of multiple red and infrared LEDs in the same device for the treatment of TMD.
Therefore, the aim of the present study was to analyze the effects of photobiomodulation with simultaneous use of red LEDs (660 nm) and infrared LEDs (850 nm) in the same device on pain intensity and mandibular range of motion in individuals with TMD.
Materials and methods
Design
A randomized, controlled, double-blind, clinical trial was conducted at the dental clinic of Universidade Nove de Julho (UNINOVE) in the city of São Paulo, Brazil. The methods were previously specified in a published protocol study [31]. This study received approval from the local human research ethics committee (process number: 2.962.857). All potential participants received clarifications regarding the objectives and procedures and those who agreed to participate voluntarily signed a statement of informed consent, as stipulated in Resolutions 466/2012 and 510/2016 of the Brazilian National Board of Health. This study was registered with Clinicaltrials.gov (NCT 03,696,706).
Sample size calculation
The sample size was calculated considering α = 0.05, 1 − β = 0.9, and data described in the study by Herpich et al. (2017) [14]. The sample was determined to be 11 participants in each group (experimental and control). Suresh and Chandrashekara (2012) [32] suggest a minimum sample of eight participants per group to enable adequate statistical analyses in clinical studies with difficulty recruiting volunteers.
Participants
The clinical diagnosis of mixed TMD using the Research Diagnostic Criteria for Temporomandibular Disorders (RDC/TMD) [33] was used to diagnose the participants. This evaluation tool, which has been validated in its Portuguese language version [34], has two axes for a detailed physical evaluation of the mouth opening pattern, vertical extension of mandibular movement, lateral excursions, and protrusion as well as an evaluation of TMJ noises upon palpation. The questionnaire is composed of items addressing general health, oral health, a history of facial pain, limited mouth opening, joint noises, habits, bite, tinnitus, general diseases, joint problems, headache, current behavior, and socioeconomic profile. The participants should have a complete dentition (except third molars) and present mandibular deviation and/or deflection.
The exclusion criteria were occlusal alterations, any type of dental prosthesis, currently undergoing orthodontic or physiotherapeutic treatment, and starting the use of medication during any of the phases of the study.
Eligible volunteers were instructed to remain without any physiotherapeutic and/or dental interventions and not to use any medications for 2 weeks. This period was considered the control phase. Randomization was performed via www.randomization.com, using 1:1 block randomization with permutation and changing block sizes. The participants were then sent to the interventions according to allocation to the different groups: LED group (active PBM in six non-consecutive sessions) and the control group (sham PBM with the device “off” mode in six non-consecutive sessions). Evaluations were performed before and after the first session as well as at the end of the treatment.
The procedures were performed by three different researchers (dentists having undergone training exercises for data collection and evaluations). Each researcher was exclusively in charge of one part of the study. The first researcher was responsible for screening the participants and administering the questionnaires. The second was responsible for the randomization process, allocation concealment (other researchers were blinded to the treatment of each volunteer), and the administration of PBM (active or placebo). The third researcher was responsible for data analysis and processing.
Photobiomodulation—red and infrared LED treatment
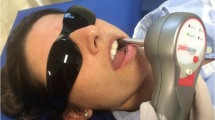
Photobiomodulation was performed following the protocol described by Sousa et al. (2019) [31]. Treatment was administered using the Sportllux device (Cosmedical®, Mauá, SP, Brazil), which is a plate containing a total of 36 LEDs (Fig. 1a) that was attached with an elastic strap to the hemiface of the participant covering the regions of the temporomandibular joints, masseter muscles, and anterior bundle of the temporal muscles (Fig. 1b). The treatment was performed three times per week on non-consecutive days for 2 weeks, totaling six treatment sessions. For placebo treatment (control group), all the procedures described for the LED group were adopted, but with the equipment switched off. Only the volunteer to be treated and the operator were present during treatment, both of whom wore protective eyewear. The LED device was composed of a flexible rectangular plate (120 cm2) that adapts to the shape of the area to be treated, containing 18 red LEDs (660 nm) and 18 infrared LEDs (850 nm). The dosimetric parameters for LED irradiation are shown in Table 1.
A total of 78 participants were screened for the present study. Sixty were excluded for the reasons listed in the flowchart (Fig. 2), which was designed following the Consolidated Standards for Reporting Trials (CONSORT statement) [35]. A total of 18 patients were divided into two groups (nine patients for each group) and were assessed before the first intervention, immediately after the first therapeutic intervention, and at the end of treatment.
Measures
Pain intensity
The visual analog scale (VAS) was used to measure pain intensity. This scale consists of a 10-cm line with 0 (no pain) printed at one end and 10 (worst pain ever experienced) printed at the other end. The participants were instructed to mark a perpendicular line between the two ends to represent their current pain intensity. This mark was subsequently measured, recording the distance from zero to obtain a numerical representation of pain intensity [36].
Range of motion
The extent of vertical mandibular movement (mouth opening), right and left excursions, and protrusion were measured (in millimeters) with the aid of digital calipers (Starrett®, Athol, MA), considering the distance between the maxillary and mandibular central incisors [13, 14]. For the extent of vertical movement, three situations were considered: (1) opening without assistance and without pain, (2) maximum opening without assistance, and (3) maximum opening with assistance. For right and left excursions, the participant was instructed to move the mandible to the right and left sides and the distances between the midlines of the upper and lower dental arches were measured. Lastly, the participant was instructed to perform a protrusive movement.
Statistical analysis
The data were analyzed using GraphPad Prism 8.0.1. The Kolmogorov–Smirnov test was used to assess normality. Parametric data were expressed as mean ± standard deviation. Nonparametric data were expressed as median and interquartile range. Comparisons between groups were performed using the t-test with Welch’s correction for parametric data, whereas the Mann–Whitney test was used for nonparametric data. Intragroup comparisons were performed using two-way analysis of variance (ANOVA) for parametric data and the Friedman test with Dunn’s post hoc test for nonparametric data. The significance level was set at 5% (p < 0.05) for all statistical tests.
Results
Among the 78 individuals recruited, exclusions occurred due to refusals to participate, failure to meet the eligibility criteria, and not agreeing to perform a facial shave. The final sample was composed of 18 women between 18 and 45 years of age with mixed TMD (myogenic and joint). The mean age was 23.66 (± 3.90) in the LED group and 23.55 (± 3.67) years in the control group. Sample losses occurred during the interventions and subsequent evaluations due to the use of analgesic medication (one participant) and dropouts (eight participants), as shown in Fig. 2. Each group had nine participants. Recruitment and follow-up of participants were conducted between January 2019 and December 2019.
Regarding the clinical diagnosis of TMD using the RDC/TMD, eight participants in the LED group (88.8%) were diagnosed with myofascial pain and one (11.1%) had myofascial pain with limited mouth opening. In the control group, seven participants (77.7%) were diagnosed with myofascial pain and two (22.2%) had myofascial pain with limited opening. In the overall sample (n = 18), only three participants (16.6%) had limited mouth opening and all participants (100%) had anterior disk displacement with reduction on the right and/or left side as well as right and/or left arthralgia.
Pain intensity
Significant differences between groups and evaluation periods were found regarding pain intensity measured using the VAS (Fig. 3). Pain intensity was significantly lower in the LED group compared to the control group at the end of treatment (p < 0.001). In the intra-group analysis, a significant reduction was found in the LED group between the pre-intervention and post-intervention evaluation (p < 0.001) as well as between the evaluation immediately after the first session and the post-intervention evaluation (p < 0.001).
Median and interquartile range [25–75%] of pain intensity using visual analog scale in the LED group and control group at different evaluation times. The Mann–Whitney test for inter-group analysis and Friedman test with Dunn’s post hoc test for intragroup analysis. Pre, pre-intervention evaluation; Immediate, evaluation after first session; Post, post-intervention evaluation (after six sessions). #Post LED × Post Control; &Post LED × Pre LED; $Post LED × Immediate LED
Range of motion
The results of the mandibular range of motion analysis are displayed in Table 2. No statistically significant differences between the LED group and control group were found at the preintervention evaluation, evaluation immediately after the first session, or the post-intervention evaluation for any of the conditions analyzed (p > 0.05). Moreover, no significant intra-group differences were found among the different evaluation times (p > 0.05).
Discussion
Eighteen women with TMD participated in this study, the aim of which was to analyze the effects of PBM with simultaneous administration of red (660 nm) and infrared (850 nm) LEDs in the same device on pain and mandibular range of motion in individuals with TMD. For such, a cluster composed of 36 LEDs (18 infrared and 18 red) was used in six non-consecutive sessions. The hypothesis was that the therapeutic use of a red and infrared LED cluster would modulate pain in the masticatory muscles and TMJ region and improve mandibular range of motion in individuals with TMD. The results revealed reductions in pain intensity between the pre-intervention and post-intervention evaluations as well as between the evaluation immediately after the first session and the post-intervention evaluation (after six sessions) in the LED group. However, no improvement in mandibular range of motion was found for any of the conditions analyzed.
The RDC/TMD defines a diagnosis of myofascial pain with mouth opening limitation for individuals with more than three painful sites upon palpation of the masticatory muscles, a report of facial pain on the same side as the palpation, and mouth opening without pain < 40 mm (after correction for horizontal incisal overjet), and passive stretching (maximum opening with assistance compared to opening without assistance and without pain) ≥ 5 mm [33]. The fact that only three participants in the present study (16.6%) had a diagnosis of myofascial pain with opening limitation could explain lack of changes in mandibular range of motion, as most participants did not have limited movements.
Panhoca et al. (2015) [29] conducted a study involving PBM as a therapeutic resource for TMD, comparing LED and LLLT. The authors irradiated five points (three on the TMJ, one on the masseter muscle, and one on the temporalis muscle) in eight sessions held twice a week, with evaluations immediately after the first session as well as 7 and 30 days after treatment. Groups treated with red LED (630 ± 10 nm) and infrared LED (850 ± 10 nm) were evaluated, both with radiant exposure of 18 J/cm2, an output power of 150 mW, 60 s/point, and 9 J of energy per point (45 J per session). Another group was treated with LLLT (780 nm), radiant exposure of 105 J/cm2, power output of 70 mW, and 4.2 J per spot. Despite using different parameters for the different types of devices, which the authors considered a limitation of the study, the three therapies achieved similar results in terms of muscle pain and mandibular range of motion. However, the study showed that therapeutic PBM with LEDs led to improvements in terms of pain relief and maximum mouth opening immediately after the first session as well as 7 and 30 days after treatment, demonstrating that PBM with LED is an attractive treatment option for individuals with TMD.
In the present study, 18 red LEDs and 18 infrared LEDs were used simultaneously, covering the anterior temporalis and masseter muscle region at the same time, with a power of 126 mW, 1200 s, and total energy of 151.2 J per application. The results revealed a significant reduction in pain intensity at the end of treatment (six sessions over 2 weeks). Panhoca et al. (2015) [29] reported similar results in individuals with TMD after 7 days of treatment. In the present investigation, no differences in mandibular range of motion were found, as only three patients had mouth opening limitation prior to treatment. In contrast, all participants in this study had limited mouth opening.
No clinical trial was found in the literature using a device similar to that employed in the present study, which enables covering both the TMJ and masticatory muscle regions and the simultaneous irradiation of 18 points with red LEDs and 18 with infrared LEDs in an easy way. Langella et al. (2019) [24] proposed a clinical study protocol using a plate with 36 LEDs only in the infrared spectrum (780 nm), a total power of 180 mW, 0.8 J/cm2, and 600 s in eight sessions. Thus, there were differences between the study cited and the present investigation with regard to the number of sessions, dosimetric parameters, and type of light sources used. Costa et al. (2021) [37] evaluated the effects of punctually infrared LED (880 nm), divided into 16 points on the face, with a power of 30 mW, 3 J/cm2, and 70 s, and compared the one or two irradiation frequencies and the association of this therapy with an occlusal splint. The authors found a reduction in the groups irradiated once and two times in the post-therapy and 30 days post-therapy in comparison to initial evaluation in the pain intensity outcome. Moreover, the results of the association of LED therapy and occlusal splint showed superior results.
Herpich et al. (2017) [14] only evaluated the immediate effect of PBM using different light sources (LED and LLLT) in women in the same age group as those in the present investigation. For such, four red LEDs (640 nm), four infrared LEDs (875 nm), and super-pulsed low-level laser (905 nm) were used, with a power of 33.4 mW on each side of the face in a single session (lower than the power of 126 mW/session used in the present study), comparing different exposure times (20, 40, and 60 s). Ten points were irradiated (five on each side of the face) on the masseter (two points) and temporalis (three points) muscles. The authors performed evaluations immediately after application as well as after 24 and 48 h, reporting a reduction in pain intensity in the post-treatment evaluations in comparison to the pre-treatment evaluation, after 24 h in the group irradiated for 60 s, and especially after 48 h in the groups exposed to irradiation for 20 and 40 s. In the present study, no significant reduction in pain intensity was found immediately after the first session, but a significant reduction was found after six sessions. Herpich et al. (2017) [14] also found no effect on mandibular range of motion, which is in agreement with the present findings.
In another study involving individuals with TMD, Al-Quisi et al. (2019) [15] used only red LED (660 nm), with 1.6 J/cm2, 1600 mW, and an energy of 1.6 J per second for 180 s irradiated on points of the TMJ and lateral pterygoid muscle as well as points on the masseter and temporalis muscles if the patient reported sensitivity in sessions held once per week for 4 weeks (total of four sessions). The authors found a reduction in pain evaluated using the VAS after treatment, but no change in mandibular range of motion, as occurred in the present study. The authors also found that joint sounds were resolved in all patients (100%) treated with red LED.
In a case report, Costa et al. (2017) [17] found a reduction in pain intensity assessed using the VAS after the administration of infrared LED (880 ± 20 nm) with 7 J/cm2, a power of 0.03 W, and point application for 70 s/point. Despite the different dosimetric parameters used in comparison to the present investigation, both studies demonstrated a reduction in pain in individuals with TMD treated with LED. However, Costa et al. (2017) [17] warn that LED therapy on the TMJ has no effect on the etiology of temporomandibular disorder. Thus, the authors consider PBM with LED to be supportive therapy for the reduction of signs and symptoms, but the identification and elimination of etiological factors are essential to treatment.
LED as a therapeutic resource has been used for cases of muscle injury [38, 39], to increase muscle activity after the induction of fatigue [40], and in sports rehabilitation [41, 42], but its use for the treatment of TMD has been explored little. The sample size was a limitation of the present study. However, we found the cluster of LEDs as a therapeutic resource for TMD to be effective at reducing pain intensity in a short treatment period (six sessions in 2 weeks). In contrast, no statistically significant differences were found regarding mandibular range of motion. However, only three participants had considerable mouth opening limitation at the onset of the study.
Conclusion
The use of PBM with a cluster of red (660 nm) and infrared (850 nm) LEDs administered simultaneously over the TMJ and masticatory muscle regions led to an improvement in pain intensity in individuals with TMD. There is a need for further studies on PBM using LED to determine the most effective irradiation parameters for improvements in pain and mandibular range of motion in this population.
Data availability
The data that support the findings of this study are available from the corresponding author, Raquel Agnelli Mesquita-Ferrari, upon reasonable request.
References
Chen J, Huang Z, Ge M, Gao M (2015) Efficacy of low-level laser therapy in the treatment of TMDs: a meta-analysis of 14 randomised controlled trials. J Oral Rehabil 42:291–299
Aisaiti A, Zhou Y, Wen Y, Zhou W, Wang C, Zhao J, Yu L, Zhang J, Wang K, Svensson P (2021) Effect of photobiomodulation therapy on painful temporomandibular disorders. Sci Rep 11:9049. https://doi.org/10.1038/s41598-021-87265-0
Sobral APT, de Sobral SS, Campos TM, Horliana ACRT, Fernandes KPS, Bussadori SK, Motta LJ (2021) Photobiomodulation and myofascial temporomandibular disorder: systematic review and meta-analysis followed by cost-effectiveness analysis. J Clin Exp Dent 13:e724–e732. https://doi.org/10.4317/jced.58084
Freire AB, de Nardi AT, Boufleur J, Chiodelli L, Pasinato F, Corrêa ECR (2014) Multimodal physiotherapeutic approach: effects on the temporomandibular disorder diagnosis and severity. Fisioterapia em Movimento 27:219–227. https://doi.org/10.1590/0103-5150.027.002.ao07
Khalighi HR, Mortazavi H, Mojahedi SM, Azari-Marhabi S, Abbasabadi FM (2016) Low level laser therapy versus pharmacotherapy in improving myofascial pain disorder syndrome. J Lasers Med Sci 7:45–50. https://doi.org/10.15171/jlms.2016.10
de Carli BMG, Magro AKD, Souza-Silva BN, de Matos F, S, de Carli JP, Paranhos LR, Magro ED, (2016) The effect of laser and botulinum toxin in the treatment of myofascial pain and mouth opening: a randomized clinical trial. J Photochem Photobiol, B 159:120–123. https://doi.org/10.1016/j.jphotobiol.2016.03.038
Carvalho Bortoletto C, Cordeiro Da Silva F, Fernanda Da Costa Silva P, Haddad Leal De Godoy C, Agnelli Mesquita-Ferrari R, Porta K, Fernandes S, Romano R, Bussadori SK (2014) Evaluation of cranio-cervical posture in children with bruxism before and after bite plate therapy: a pilot project. J Phys Ther Sci 26:1125–1128. https://doi.org/10.1589/jpts.26.1125
Gomes NCMC, Berni-Schwarzenbeck KCS, Packer AC, Rdrigues-Bigaton D (2012) Efeito da estimulação elétrica de alta voltagem catódica sobre a dor em mulheres com DTM. Braz J Phys Ther 16:10–15. https://doi.org/10.1590/S1413-35552012000100003
el Hage Y, Politti F, Magalhães de Sousa DF, Marciela Herpich C, dos Santos Phillip, Gloria I, Fidelis André, de Paula Gomes C, Paula Amaral A, Cristina de Melo N, Correa da Silva T, Edmur Camargo Arruda E, Ferreira Amorim C, Caroline Gadotti I, Oliveira Gonzalez T, Berzin F, Kalil Bussadori S, Barbosa Santos Garcia M, Roberto Borges Barbosa B, Aparecida Biasotto-Gonzalez D (2013) Effect of mandibular mobilization on electromyographic signals in muscles of mastication and static balance in individuals with temporomandibular disorder: study protocol for a randomized controlled trial. Trials 14:316. https://doi.org/10.1186/1745-6215-14-316
Amaral AP, Politti F, Hage YE, Arruda EEC, Amorin CF, Biasotto-Gonzalez DA (2013) Immediate effect of nonspecific mandibular mobilization on postural control in subjects with temporomandibular disorder: a single-blind, randomized, controlled clinical trial. Braz J Phys Ther 17:121–127. https://doi.org/10.1590/S1413-35552012005000075
da Silva MM, Albertini R, de Tarso Camillo de Carvalho P, Leal-Junior ECP, Bussadori SK, Vieira SS, Bocalini DS, de Oliveira LVF, Grandinetti V, Silva JA, Serra AJ (2018) Randomized, blinded, controlled trial on effectiveness of photobiomodulation therapy and exercise training in the fibromyalgia treatment. Lasers Med Sci 33:343-351https://doi.org/10.1007/s10103-017-2388-2
Manfredini D, Cocilovo F, Favero L, Ferronato G, Tonello S, GUARDA-NARDINI L, (2011) Surface electromyography of jaw muscles and kinesiographic recordings: diagnostic accuracy for myofascial pain. J Oral Rehabil 38:791–799. https://doi.org/10.1111/j.1365-2842.2011.02218.x
Seifi M, Ebadifar A, Kabiri S, Badiee MR, Abdolazimi Z, Amdjadi P (2017) Comparative effectiveness of low level laser therapy and transcutaneous electric nerve stimulation on temporomandibular joint disorders. Journal of Lasers in Medical Sciences 8:S27–S31. https://doi.org/10.15171/jlms.2017.s6
Herpich CM, Leal-Junior ECP, Gomes CAF de P, Gloria IP dos S, Amaral AP, Amaral M de F de RS, Politti F, Biasotto-Gonzalez DA (2018) Immediate and short-term effects of phototherapy on pain, muscle activity, and joint mobility in women with temporomandibular disorder: a randomized, double-blind, placebo-controlled, clinical trial. Disabil Rehabil 40:2318-2324https://doi.org/10.1080/09638288.2017.1336648
Al-Quisi AF, Al-Anee AM, AL-jumaily HA, Bahr EF, Finjan DA, (2019) Efficacy of the LED red light therapy in the treatment of temporomandibular disorders: double blind randomized controlled trial. Pain Res Treat 2019:1–5. https://doi.org/10.1155/2019/8578703
Leal de Godoy CH, Motta LJ, Santos Fernandes KP, Mesquita-Ferrari RA, Deana AM, Bussadori SK (2015) Effect of low-level laser therapy on adolescents with temporomandibular disorder: a blind randomized controlled pilot study. J Oral Maxillofac Surg 73:622–629. https://doi.org/10.1016/j.joms.2014.09.018
Costa DR, Costa DR, Pessoa DR, Masulo LJ, Arisawa EÂLS, Nicolau RA (2017) Efeito da terapia LED na disfunção temporomandibular: estudo de caso. Scientia Medica 27:25872. https://doi.org/10.15448/1980-6108.2017.2.25872
Shobha R, Narayanan V, Jagadish Pai B, Jaishankar H, Jijin M (2017) Low-level laser therapy: a novel therapeutic approach to temporomandibular disorder – a randomized, double-blinded, placebo-controlled trial. Indian J Dent Res 28:380. https://doi.org/10.4103/ijdr.IJDR_345_15
Marini I, Gatto MR, Bonetti GA (2010) Effects of superpulsed low-level laser therapy on temporomandibular joint pain. Clin J Pain 26:611–616. https://doi.org/10.1097/AJP.0b013e3181e0190d
Borges RMM, Cardoso DS, Flores BC, da Luz RD, Machado CR, Cerveira GP, Daitx RB, Dohnert MB (2018) Effects of different photobiomodulation dosimetries on temporomandibular dysfunction: a randomized, double-blind, placebo-controlled clinical trial. Lasers Med Sci 33:1859–1866. https://doi.org/10.1007/s10103-018-2533-6
Magri LV, Carvalho VA, Rodrigues FCC, Bataglion C, Leite-Panissi CRA (2018) Non-specific effects and clusters of women with painful TMD responders and non-responders to LLLT: double-blind randomized clinical trial. Lasers Med Sci 33:385–392. https://doi.org/10.1007/s10103-017-2406-4
Basili M (2017) Low-level laser therapy in the treatment of muscle-skelet pain in patients affected by temporomandibular disorders. Oral & Implantology 10:406. https://doi.org/10.11138/orl/2017.10.4.406
Dostalová T, Hlinakova P, Kasparova M, Rehacek A, Vavrickova L, Navrátil L (2012) Effectiveness of physiotherapy and GaAlAs laser in the management of temporomandibular joint disorders. Photomed Laser Surg 30:275–280. https://doi.org/10.1089/pho.2011.3171
Langella LG, Silva PFC, Costa-Santos L, Gonçalves MLL, Motta LJ, Deana AM, Fernandes KPS, Mesquita-Ferrari RA, Bussadori SK (2018) Photobiomodulation versus light-emitting diode (LED) therapy in the treatment of temporomandibular disorder: study protocol for a randomized, controlled clinical trial. Trials 19:71. https://doi.org/10.1186/s13063-018-2444-7
Yeh NG, Wu C-H, Cheng TC (2010) Light-emitting diodes—their potential in biomedical applications. Renew Sustain Energy Rev 14:2161–2166. https://doi.org/10.1016/j.rser.2010.02.015
Kelencz CA, Muñoz ISS, Amorim CF, Nicolau RA (2010) Effect of low-power gallium–aluminum–arsenium noncoherent light (640 nm) on muscle activity: a clinical study. Photomed Laser Surg 28:647–652. https://doi.org/10.1089/pho.2008.2467
Muñoz-Cánoves P, Scheele C, Pedersen BK, Serrano AL (2013) Interleukin-6 myokine signaling in skeletal muscle: a double-edged sword? FEBS J 280:4131–4148. https://doi.org/10.1111/febs.12338
de Castro IC v., Rosa CB, Carvalho CM, Aragão JS, Cangussu MCT, dos Santos JN, Pinheiro ALB (2015)Assessment of different energy delivery settings in laser and LED phototherapies in the inflammatory process of rat’s TMJ induced by carrageenan. Lasers Med Sci 30:2105-2113https://doi.org/10.1007/s10103-015-1748-z
Panhoca VH, de Fatima Zanirato Lizarelli R, Nunez SC, Pizzo RC de A, Grecco C, Paolillo FR, Bagnato VS (2015)Comparative clinical study of light analgesic effect on temporomandibular disorder (TMD) using red and infrared led therapy. Lasers Med Sci 30:815-822https://doi.org/10.1007/s10103-013-1444-9
Bashkatov AN, Genina EA, Kochubey VI, Tuchin VV (2005) Optical properties of human skin, subcutaneous and mucous tissues in the wavelength range from 400 to 2000 nm. J Phys D Appl Phys 38:2543–2555. https://doi.org/10.1088/0022-3727/38/15/004
de Sousa DFM, Gonçalves MLL, Politti F, Lovisetto RDDP, Fernandes KPS, Bussadori SK, Mesquita-Ferrari RA (2019) Photobiomodulation with simultaneous use of red and infrared light emitting diodes in the treatment of temporomandibular disorder: study protocol for a randomized, controlled and double-blind clinical trial. Medicine (United States) 98:e14391. https://doi.org/10.1097/MD.0000000000014391
Suresh K, Chandrashekara S (2012) Sample size estimation and power analysis for clinical research studies. J Hum Reprod Sci 5:7. https://doi.org/10.4103/0974-1208.97779
Dworkin SF, LeResche L (1992) Research diagnostic criteria for temporomandibular disorders: review, criteria, examinations and specifications, critique. J Craniomandib Disord 6:301–355
de Lucena LBS, Kosminsky M, da Costa LJ, de Góes PSA (2006) Validation of the Portuguese version of the RDC/TMD Axis II questionnaire. Braz Oral Res 20:312–317. https://doi.org/10.1590/S1806-83242006000400006
Schiffman E, Ohrbach R, Truelove E, Look J, Anderson G, Goulet J-P, List T, Svensson P, Gonzalez Y, Lobbezoo F, Michelotti A, Brooks SL, Ceusters W, Drangsholt M, Ettlin D, Gaul C, Goldberg LJ, Haythornthwaite JA, Hollender L, Maixner W, van der Meulen M, Murray GM, Nixdorf DR, Palla S, Petersson A, Pionchon P, Smith B, Visscher CM, Zakrzewska J, Dworkin SF (2014) Diagnostic criteria for temporomandibular disorders (DC/TMD) for clinical and research applications: recommendations of the International RDC/TMD Consortium Network* and Orofacial Pain Special Interest Group†. J Oral Facial Pain Headache 28:6–27. https://doi.org/10.11607/jop.1151
Ferreira-Valente MA, Pais-Ribeiro JL, Jensen MP (2011) Validity of four pain intensity rating scales. Pain 152:2399–2404. https://doi.org/10.1016/j.pain.2011.07.005
Costa DR, Pessoa DR, Seefeldt VB, Costa DR, Maia DTL, dos Santos MT, Mota BBM, Delpasso CA, Ribeiro CAD, Nicolau RA (2021) Orofacial evaluation of individuals with temporomandibular disorder after LED therapy associated or not of occlusal splint: a randomized double-blind controlled clinical study. Lasers Med Sci 36:1681–1689. https://doi.org/10.1007/s10103-021-03269-2
Souza NHC, Mesquita-Ferrari RA, Rodrigues MFSD, da Silva DFT, Ribeiro BG, Alves AN, Garcia MP, Nunes FD, da Silva Junior EM, França CM, Bussadori SK, Fernandes KPS (2018) Photobiomodulation and different macrophages phenotypes during muscle tissue repair. J Cell Mol Med 22:4922–4934. https://doi.org/10.1111/jcmm.13757
Lopez TCC, Malavazzi TC dos S, Rodrigues MFSD, Bach EE, Silva DT, Hi EMB, França CM, Bussadori SK, Mesquita-Ferrari RA, Fernandes KPS (2022) Histological and biochemical effects of preventive and therapeutic vascular photobiomodulation on rat muscle injury. J Biophotonics 15:e202100271. https://doi.org/10.1002/jbio.202100271
Leal Junior ECP, Lopes-Martins RÁB, de Almeida P, Ramos L, Iversen V, v., Bjordal JM, (2010) Effect of low-level laser therapy (GaAs 904 nm) in skeletal muscle fatigue and biochemical markers of muscle damage in rats. Eur J Appl Physiol 108:1083–1088. https://doi.org/10.1007/s00421-009-1321-1
de Marchi T, Leal-Junior ECP, Lando KC, Cimadon F, Vanin AA, da Rosa DP, Salvador M (2019) Photobiomodulation therapy before futsal matches improves the staying time of athletes in the court and accelerates post-exercise recovery. Lasers Med Sci 34:139–148. https://doi.org/10.1007/s10103-018-2643-1
Baroni BM, Leal Junior ECP, de Marchi T, Lopes AL, Salvador M, Vaz MA (2010) Low level laser therapy before eccentric exercise reduces muscle damage markers in humans. Eur J Appl Physiol 110:789–796. https://doi.org/10.1007/s00421-010-1562-z
Funding
This work was funded by São Paulo Research Foundation ‐ FAPESP (2020/13976–0), Coordenação de Aperfeiçoamento de Pessoal de Nível Superior—CAPES (88887.481244/2020–00), Conselho Nacional de Desenvolvimento Científico e Tecnológico—CNPq (310491/2021–5), and UNINOVE.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. The planning, execution of experiments, and collection were performed by Dowglas Fernando Magalhães de Sousa, Tainá Caroline dos Santos Malavazzi, Alessandro Melo Deana, and Anna Carolina Ratto Tempestini Horliana. Data analysis was performed by Tainá Caroline dos Santos Malavazzi. Original draft preparation was written by Dowglas Fernando Magalhães de Sousa, Tainá Caroline dos Santos Malavazzi, and Raquel Agnelli Mesquita-Ferrari. Review and editing were performed by Anna Carolina Ratto Tempestini Horliana, Kristianne Porta Santos Fernandes, and Sandra Kalil Bussadori. Supervision was made by Raquel Agnelli Mesquita-Ferrari, Kristianne Porta Santos Fernandes, and Sandra Kalil Bussadori.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed were in accordance with the ethical standards of Universidade Nove de Julho (UNINOVE; process number: 2.962.857).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
de Sousa, D.F.M., Malavazzi, T.C.d., Deana, A.M. et al. Simultaneous red and infrared light-emitting diodes reduced pain in individuals with temporomandibular disorder: a randomized, controlled, double-blind, clinical trial. Lasers Med Sci 37, 3423–3431 (2022). https://doi.org/10.1007/s10103-022-03600-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-022-03600-5