Abstract
Pseudoaneurysm is a rare complication after intertrochanteric fracture fixation. Herein, we present a rare case of late development of a pseudoaneurysm with silent clinical symptoms. The case was a 91-year-old woman treated with proximal femoral nailing and cerclage wiring. Postoperatively, the patient was able to ambulate with a walker without abnormal symptoms. During the follow-ups, the radiographic images showed progressive cortical scalloping on the medial femoral shaft. Ultrasonography revealed a yin-yang sign, and a CT scan confirmed a pseudoaneurysm at the profunda femoris artery (PFA). In this case, many possible causes of pseudoaneurysm were hypothesized. We showed that the excessive displaced, long spiral pattern of an intertrochanteric fracture, which was irreducible by a closed technique, is the risk of a PFA injury. An atherosclerotic vessel was seen in preoperative radiography, indicating poor vessel elasticity which may be a risk of vessel tear during fracture reduction using multiple reduction instruments in excessive displaced fracture. Moreover, over-penetration when drilling should not be overlooked. We also discuss the predisposing factors, surgical techniques which may lead to this type of PFA injury and summarize the literature of pseudoaneurysms related to intertrochanteric fracture fixation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Intertrochanteric fractures are common, for which the standard treatment is internal fixation. Vascular injury related to internal fixation of an intertrochanteric fracture is rare but serious and requires specific treatment. The incidence of vascular injury after internal fixation of a proximal femoral fracture was reported at 0.49% in one review, of which pseudoaneurysm is the most common type accounting for 67.03% of cases [6]. Untreated pseudoaneurysms can lead to morbidity or serious complications such as infected hematoma, delayed fracture healing, thigh compartment syndrome, or deep vein thrombosis [70]. Rupture of a pseudoaneurysm leads to massive haemorrhage.
Herein we present a case of late development of a pseudoaneurysm after intramedullary nail fixation with cerclage wiring augmentation. Postoperatively, the patient had no abnormal symptoms. Cortical scalloping seen in routine fracture follow-up plain radiography was the only clue for further investigation. The ultrasonography and computed tomography angiography (CTA) were carried out to confirm the diagnosis of pseudoaneurysm of PFA. Pseudoaneurysm was eventually treated by coil embolization. In this case, many possible causes of pseudoaneurysm were hypothesized. An atherosclerotic vessel was seen in preoperative radiography, indicating poor vessel elasticity which may be a risk of vessel tear during fracture reduction using multiple reduction instruments in excessive displaced fracture. Moreover, over-penetration when drilling should not be overlooked.
The patient consented to the publication of this case report. The paper was approved by the Ethics Committee of Faculty of Medicine, Prince of Songkla University.
Case presentation
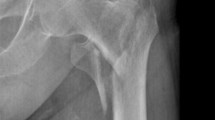
A 91-year-old woman presented with an intertrochanteric fracture of the right femur (AO classification; 31-A1). Initial radiographic images showed a long spiral trochanteric fracture extending to the subtrochanteric area (Fig. 1). No preoperative signs or symptoms of vascular injury, such as swelling or a pulsatile mass, were seen. The preoperative haematocrit level was 26.7% (normal range 37–47%), and haemoglobin was 8.3 g/dL (normal range 11–15 g/dL). Enoxaparin 20 mg was injected subcutaneously for deep vein thrombosis prophylaxis and stopped 24 h prior to the surgery.
For the operation, the patient was placed in the supine left hemi-lithotomy position on the fracture table. A closed fracture reduction was attempted but failed to achieve anatomical alignment (Fig. 2A), so the reduction was converted to an open reduction. An incision was made on the lateral aspect of the thigh at the lesser trochanteric level and the fracture was reduced and maintained by a colinear clamp (Fig. 2B). Kirschner wires were then inserted for temporary fixation. Cerclage wiring was done at the subtrochanteric level using a wire passer to maintain the anatomical reduction (Fig. 2C). Radiographic fluoroscopy was performed to check the alignment. A proximal femoral nail antirotation (PFNA, Synthes, 200 mm in length) was inserted. No intraoperative complications were noted. Postoperatively, routine deep vein thrombosis prophylactic protocol was applied including pneumatic calf compression and early ambulation within a few days. No sign and symptom of deep vein thrombosis was found. The patient could ambulate with a walker after a few days neither thigh pain nor swelling. Her haematocrit was normal. Postoperative radiography demonstrated a good position of the implant. No soft tissue hypodensity was seen on the medial aspect at the subtrochanteric level.
Intraoperative findings: the fracture was irreducible by a closed technique on the fracture table (a, b). The fracture was reduced properly by a collinear clamp and cerclage wiring using a wire passer (c). Proximal femoral nail antirotation was inserted without immediate complications (d). Application of various instruments may stretch the atherosclerotic profunda femoris artery (e)
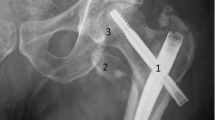
At the 3-month follow-up, the patient was able to walk with a walker without thigh pain. There was no palpable mass, and the distal pulse can be palpated. However, a plain radiograph showed obvious bony scalloping on the medial cortex of the right femur. Calcification was seen at the surrounding soft tissue density mass (Fig. 3). Ultrasonography demonstrated a well-defined heterogenous hypo- and hyperechoic lesion with a yin-yang sign on the colour flow (Fig. 4A). CT angiography revealed a partially thrombosed pseudoaneurysm on the perforating branch of the right profunda femoris artery (Fig. 4B, C). The thrombosed mass compressed medial cortex of proximal femoral shaft causing bone scalloping. The distal locking screw did not appear to be excessively long (Fig. 5). Her haematocrit (32.2%) and haemoglobin (9.9 g/dL) were normal. Coil embolization was performed without complications. At 1-year follow-up, the fracture was healed.
Profunda femoris artery (PFA) injury in a long spiral fracture of the intertrochanter with excessive posterior displacement of the femoral shaft. PFA could displace and be close to the fracture site. Fracture manipulation during cerclage wiring in this type of subtrochanteric fracture may involve a risk of PFA injury. The yellow highlighted area indicates the danger zone in which there is a risk of potential injury to the 1st and 2nd branches of the perforator artery (PA)
Discussion
Vascular injury related to internal fixation can be detected in the early or late follow-ups. A patient with a vascular rupture or tear may present with hard signs such as haemorrhage. Thigh pain and swelling accompanying decreased haematocrit are commonly found. A pulsatile mass can be found if the mass is in the superficial layer. A pseudoaneurysm can develop soon or longer following the surgery and can be asymptomatic. An enlarged pseudoaneurysm can cause thrombosis presenting with swelling and pain.
The profunda femoris artery (PFA) is the most common structure at risk of arterial injury in a proximal femoral fracture [6]. The PFA branches at the posterolateral aspect of the femoral artery. At the trochanteric level, the PFA is separated from the femoral bone by the rectus femoris, iliopsoas and pectineus muscles. At the proximal one-third of the femoral shaft, the PFA courses between the adductor longus and adductor brevis muscles and provides three perforating arteries to supply posterior thigh muscles. At this level, the PFA is close to the medial to posteromedial aspect of the femur. Therefore, the PFA is vulnerable to injury during any orthopaedic procedure at the subtrochanteric to the proximal one-third of the shaft [59, 69]. During a fracture reduction using a fracture table, traction and internal rotation are applied to the affected leg, and the perineal pole may press against the femoral shaft, pushing the PFA closer to the shaft [66]. A large perineal pole may increase the risk of PFA injury.
Pseudoaneurysms are difficult to detect, especially when the patient has no suggestive signs or and symptoms. Postoperative findings such as unexplained/disproportionate haematocrit reduction may help the surgeon to detect this subtle problem. In the early phases, plain radiographs may not show abnormal findings. Late radiographic signs during follow-up plain radiographs, such as bony scalloping of the femoral cortex indicating cortical resorption from external mass compression, are uncommon [44, 71]. In this report, we had early detection of bone scalloping of the femoral shaft at three months follow-up before the pseudoaneurysm may become symptomatic such as thigh swelling due to more enlargement of pseudoaneurysm.
In pseudoaneurysm cases, colour Doppler ultrasonography usually shows the yin-yang sign which demonstrates swirling of blood flow in the pseudoaneurysm. An MRI also reveals a cystic mass with multistage blood components representing blood leakage into the pseudoaneurysm.
Fixation-related vascular injuries can be caused by various factors. An atherosclerotic vessel, seen in a preoperative radiographic image, is an important predisposing factor for vascular injury in elderly patients. Calcification in a vessel drastically decreases vascular elasticity. Manipulation of brittle atherosclerotic vessels during fracture reduction may result in vascular injury [57]. Therefore, deeply inserting retractors to elevate a vessel from the bone should be avoided, or done with caution [23]. In our case, an atherosclerotic PFA was found on the preoperative image. The PFA was also running closely to the spike of a proximal fragment. Therefore, the first hypothesis for the PFA injury in this case was that it may have been related to soft tissue manipulation such as traction or multiple tool application through the limited soft tissue window (Fig. 2).
Some fracture configurations of an intertrochanteric fracture, such as a displaced lesser trochanteric (LT) fragment, can directly damage adjacent vessels [5, 41, 57, 62]. A displaced LT fragment is the most common cause of PFA injury. The LT-related pseudoaneurysm may have acute onset symptoms [31]. Delayed presentation may be associated with further LT displacement during rehabilitation [21]. The treatment sometimes requires LT excision [52].
Long spiral or posteromedial extension of a femoral fragment can directly damage surrounding vessels. To reduce this fracture type, cerclage wiring is a useful technique to improve stability and assist reduction without interruption of fracture healing [4, 24, 26, 35]. Cerclage wiring may pose a risk of vascular injury by strangulation. However, no reports of PFA injury or injury to its branches have been revealed regarding cerclage wiring [34].
Excessive displacement of the femoral shaft, such as posterior translation, may be a predisposing factor for vascular injury (Fig. 2B). A perforator of the PFA may proximally migrate into the fracture zone which increases the risk of injury during fracture manipulation (Fig. 5). Moreover, various reduction tools may be applied to assist fracture reduction making the surrounding vessels more vulnerable.
Another cause of PFA injury is over-penetration when drilling for a dynamic hip screw side plate and proximal femoral nails. Recently, Jaipurwala et al. [28] analysed CTAs of lower extremities showing the distance of the PFA to the femoral shaft. The mean distances of the first perforator to the shaft were 112.6 and 123.4 mm in women and men, respectively. The mean distances of the second perforator were 159.7 and 178.9 mm, respectively. Over-penetration drilling may be prevented by conscious concentration to the change of the drilling sound. An over-length screw may cause late development of a PFA injury by irritation of an over-length screw tip on the vessels [20, 78]. In this case, a CT scan showed no protrusion of any screw tip.
To understand the clinical presentation of a pseudoaneurysm after intertrochanteric fracture fixation, case reports of pseudoaneurysm related to intertrochanteric fixation were searched in PubMed and the Scopus database during 2000–2022, and 74 cases were found. The fracture characteristics, onset, causes and symptoms were recorded (Table 1). The most common fracture type classified by AO classification type was 31A2 (59.46%). The LT was commonly involved. Interestingly, in 68.18% of all intertrochanteric fracture with LT fractures, an LT fragment was the cause of the PFA injury. Atherosclerotic vessels were seen in radiographic images in approximately 9.46% of the cases. Most patients presented with swelling (85.14%) and/or pain (70.27%). Palpable masses were not common (24.32%). Only 1.35% of the cases were asymptomatic. Thus, our case was very rare as only a radiographic sign was noted without clinical signs or symptoms. Patients with a pseudoaneurysm may have an acute (< 1 week; 29.73%), subacute (1–4 weeks; 31.08%) or late (> 4 weeks; 36.49%) presentation. Direct injury from an LT fragment spike was the most common cause of PFA injury (40.54%). Over-penetration with a drill and screw over-length were also common (18.92%). The data from the literature review are shown in Table 2, and the predisposing factors, signs and symptoms, and causes of pseudoaneurysms are shown in Table 3.
Conclusion
A pseudoaneurysm is rare but it is the most common vascular injury associated with proximal femoral fracture fixation. Fracture configurations such as a long spiral fracture or lesser trochanteric involvement or excessive shaft displacement are common risk factors for vascular injury. Being aware of possible profunda femoris artery injury is crucial when performing surgeries in this area. Performing fixation with a proper technique of cerclage wiring, distal screw length selection and drilling, may help prevent this serious complication.
References
Abed YY, Nour K (2017) Neglected false aneurysm of the profunda femoris artery after proximal femoral fracture with failure of fixation and bone erosion: case report and review of the literature. Curr Orthop Pract 28(1):116–123
Alwhouhayb M, Howard A (2005) A false aneurysm mistaken for a DVT after hip surgery. Ulus Travma Acil Cerrahi Derg 11(2):178–179
Anderson OG, Brookes JA, Cobb J (2005) False aneurysm caused by failed fracture fixation. Hosp Med (London, England: 1998) 66(7):422–423
Apivatthakakul T, Phaliphot J, Leuvitoonvechkit S (2013) Percutaneous cerclage wiring, does it disrupt femoral blood supply? A cadaveric injection study. Injury 44(2):168–174
Arbeloa-Gutierrez L, Arenas-Miquelez A, Munoa L et al (2019) Lateral circumflex femoral artery false aneurysm as a complication of intertrochanteric hip fracture with displaced lesser trochanter. J Surg Case Rep 2016(6):rjz184
Barquet A, Gelink A, Giannoudis PV (2015) Proximal femoral fractures and vascular injuries in adults: incidence, aetiology and outcomes. Injury 46(12):2297–2313
Bernstein I, Geks J, Walthers EM, Schnabel M (2004) False aneurysm and bleeding caused by a secondary dislocated lesser trochanter fragment. Unfallchirurg 107(12):1192–1195
Bowden S, Jaberi A, Roche-Nagle G (2020) Large pseudoaneurysm arising from the deep femoral artery after hip fracture fixation. J Surg Case Rep 2020(10):rjaa408
Chan WS, Kong SW, Sun KW, Tsang PK, Chow HL (2010) Pseudoaneurysm and intramuscular haematoma after dynamic hip screw fixation for intertrochanteric femoral fracture: a case report. J Orthop Surg (Hong Kong) 18(2):244–247
Chandrasenan J, Garner JP, Meiring PD, Kumar K (2006) Coil embolisation of an iatrogenic profunda femoris pseudoaneurysm. Inj Extra 37:249–252
Chong KC, Yap EC, Lam KS, Low BY (2004) Profunda femoris artery pseudoaneurysm presenting with triad of thigh swelling, bleeding and anaemia. Ann Acad Med Singap 33(2):267–269
Cowley A, Williams D, Butler M, Edwards A, Parsons S (2007) Pseudo-aneurysm of the profunda femoris artery as a late complication of hip fracture in a patient with myelodysplasia. Ann R Coll Surg Engl 89(7):W4–W6
Craxford S, Gale M, Lammin K (2013) Arterial injury to the profunda femoris artery following internal fixation of a neck of femur fracture with a compression hip screw. Case Rep Orthop 2013:181293
de Raaff CA, van Nieuwenhuizen RC, van Dorp TA (2016) Pseudoaneurysm after pertrochanteric femur fracture: a case report. Skelet Radiol 45(4):575–578
Dillon J, O’Brien G, Laing A, Adelowokan T, Dolan M (2004) Pseudoaneurysm of the profunda femoris artery following an inter-trochanteric fracture of the femur. Inj Extra 35:30–32
Dorrucci V, Spinamano L, Petralia G, Griselli F, Cibi N, Adornetto R (2008) Endovascular repair of a large deep femoral artery branch pseudoaneurysm following a femur fracture: a case report. EJVES Extra 15(3):21–23
Entwisle JJ, De Nunzio M, Hinwood D (2001) Case report: transcatheter embolization of pseudoaneurysm of the profunda femoris artery complicating fracture of the femoral neck. Clin Radiol 56(5):424–427
Fohlen A, Le Pennec V, Florescu L, Vielpeau C (2007) CV-WS-37 complications vasculaires femorales de la chirurgie de hanche. J Radiol 88(10):1527
Giannakopoulos GF, Bruekers SE, Wüst AF, Steller EP (2009) Aneurysma spurium van arteria femoralis profunda bij pertrochantaire femurfractuur en intramedullaire fixatie. Ned Tijdschr Traum 17(4):113
Gong J, Liu P, Cai M (2017) Imaging evaluation of the safe region for distal locking screw of proximal femoral nail anti-rotation in patients with proximal femoral fracture. Med Sci Monit 23:719–724
Hamdulay KA, Beresford TP (2021) Profunda femoris pseudoaneurysm rupture post dynamic hip screw fixation after physiotherapy. Ann R Coll Surg Engl 103(3):e81–e84
Hamoui M, Larbi A, Bommart S, Fauré P, Largey A, Canovas F (2010) False aneurysm of perforating branch of the profunda femoris artery following intertrochanteric fracture, a rare vascular complication: Clinical, radiological features and management: Case report and review of the literature. Eur J Orthop Surg Traumatol 20(1):59–65
Hanna GB, Holdsworth RJ, McCollum PT (1994) Profunda femoris artery pseudoaneurysm following orthopaedic procedures. Injury 25(7):477–479
Hantouly AT, Salameh M, Toubasi AA et al (2022) The role of cerclage wiring in the management of subtrochanteric and reverse oblique intertrochanteric fractures: a meta-analysis of comparative studies. Eur J Orthop Surg Traumatol. https://doi.org/10.1007/s00590-022-03240-z
Helleman JN, Vos DI, Van Der Laan L (2011) Pseudoaneurysm of the deep femoral artery after pertrochanteric hip fracture: a case report. Vasc Dis Manag 8(6):E119–E120
Hoskins W, Bingham R, Joseph S et al (2015) Subtrochanteric fracture: the effect of cerclage wire on fracture reduction and outcome. Injury 46(10):1992–1995
Jain T, Katariya J, Archik S (2019) Pseudoaneurysm of profunda femoris artery: a rare complication after intramedullary fixation for an intertrochanteric femur fracture. Int J Res Orthop 5:969
Jaipurwala R, Galea M, Hardidge A (2019) Risk of arterial injury during hip internal fixation. JBJS 101(21):1961–1964
Jha R, Kant R, Banday MI, Sahu T (2022) Pseudo-aneurysm after fixation of intertrochanteric femur fracture: literature review and report of two cases. Eur J Mol Clin Med 9(2):180–189
Jiya TU, Bruijninckx MMM, Slis HW, De Rooij TPW, De Ridder VA (2000) False aneurysm of the profunda artery complicating dynamic hip screw osteosynthesis. Eur J Trauma 26(5):261–263
Karasugi T, Oe K, Nagamoto Y (2005) Complications of treatment of intertrochanteric fractures with gamma nail. Orthop Traumatol 54(4):660–663
Kickuth R, Anderson S, Kocovic L, Ludwig K, Siebenrock K, Triller J (2006) Endovascular treatment of arterial injury as an uncommon complication after orthopedic surgery. J Vasc Interv Radiol 17(5):791–799
Kikuzato N, Uehara T, Uehara T, Uezu K (2006) Pseudoaneurysm following internal fixation of femoral neck fracture. Orthop Traumatol 55(2):143–146
Kilinc BE, Oc Y, Kara A, Erturer RE (2018) The effect of the cerclage wire in the treatment of subtrochanteric femur fracture with the long proximal femoral nail: a review of 52 cases. Int J Surg (London, England) 56:250–255
Kim CH, Yoon YC, Kang KT (2022) The effect of cerclage wiring with intramedullary nail surgery in proximal femoral fracture: a systematic review and meta-analysis. Eur J Trauma Emerg Surg. https://doi.org/10.1007/s00068-022-02003-z
Kim JW, Lee JI, Park KC (2017) Pseudoaneurysm of the deep femoral artery caused by a guide wire following femur intertrochanteric fracture with a hip nail: a case report. Acta Orthop Traumatol Turc 51(3):266–269
Kinoshita H, Hashimoto M, Hirayama J et al (2018) Huge pseudoaneurysm of the femoral artery after internal fixation of femoral trochanteric fracture. Case Rep Orthop 2018:3182643
Kinugawa K, Matsumura KA, Nakanishi KA (2011) A case of pseudoaneurysm following internal fixation of intertrochanteric fracture. Cent Jap J Orthop Surg Traumatol 54(2):315–316
Kizilates U, Nagesser SK, Krebbers YM, Sonneveld DJ (2009) False aneurysm of the deep femoral artery as a complication of intertrochanteric fracture of the hip: options of open and endovascular repairs. Perspect Vasc Surg Endovasc Ther 21(4):245–248
Kulshrestha V, Dhillan R, Sood M (2020) Unusual presentation of a profunda femoris pseudoaneurysm following osteosynthesis of proximal femur fracture. J Mar Med Soc 22(1):87–90
Labronici PJ, Santos Filho FCD, Diamantino YLO, Loureiro E, Ezequiel M, Alves SD (2019) Proximal femur fracture and vascular injury in adults-case report. Rev Bras Ortop 54(3):343–346
Laohapoonrungsee A, Sirirungruangsarn Y, Arpornchayanon O (2005) Pseudoaneurysm of profunda femoris artery following internal fixation of intertrochanteric fracture: two cases report. J Med Assoc Thail = Chotmaihet Thangphaet 88(11):1703–1706
Li X, Luckeroth P, Curry E, Eslami M, Leclair W (2011) Pseudoaneurysm of the profunda femoris artery following a long anterograde intramedullary nail for an unstable intertrochanteric hip fracture: a case report and review of the literature. Eur J Orthop Surg Traumatol 21:293–299
Lidder SS, Epstein DJ, Courtice V, George MD (2019) Proximal femoral erosion: a sequelae of psuedoaneursym formation following operative fixation of an intertrochanteric neck of femur fracture. Indian J Orthop 53(3):479–481
Lohmann H, Esenwein S, Geier B, Vogel T, Kleinert H (2009) False aneurysm of the deep femoral artery due to pertrochanteric fracture of the hip with displaced fragment of the lesser trochanter. Z Orthop Unfall 147(1):23–25
Lopes FA, Morato AE, Andrade MA (2001) Pseudo-aneurisma da artéria femoral: complicaçäo tardía na evoluçäo da fratura intertrochanteriana: relato de caso. Rev Bras Ortop 36(4):132–134
Maheshwari R, Pemmaraju K, Sloan R, Hamlet M (2004) Pseudoaneurysm of profunda femoris artery following intertrochanteric fracture of the hip. Eur J Orthop Surg Traumatol 14(3):192–194
Mayurasakorn C, Phiphobmongkol V, Sridermma W, Bavonratanavech S (2018) Profunda femoris artery injury caused by lesser trochanter fragment in intertrochanteric fracture: a case report. Trauma Case Rep 13:14–17
Molthof H, Van Der Linde JA, Leijdekkers V (2010) Vaatletsel als late complicatie van een pertrochantere femurfractuur. Ned Tijdschr Traum 18(5):143–146
Nadal Bares L, Martinez Toribio M, de Miguel Artal M, Bonvehi Torres M (2018) Delayed pseudoaneurysm of deep femoral artery after surgical intervention of hip fracture. Presentation of a case. Rev Esp Geriatr Gerontol 53(3):165–167
Nakajima A, Hozawa K, Nakamura S (2019) Successful repair of a deep femoral artery injury caused by femoral trochanteric fracture surgery using a polytetrafluoroethylene-covered stent. JACC Cardiovasc Interv 12(8):796–797
Nossa JM, Márquez D, Rodriguez S et al (2019) Pseudoaneurysm of the deep femoral artery, an unusual complication in intertrochanteric hip fracture: a case study. Curr Orthop Pract 30(6):577–581
Pandey NN, Raju SN, Rajagopal R, Kumar S (2018) Iatrogenic profunda femoris artery pseudoaneurysm: late presentation with successful endovascular microcoil embolisation. BMJ Case Rep 11(1):e228314
Papageorgiou T, Gigis I, Goulios V, Beslikas T, Bisbinas I, Christoforidis J (2010) Pseudoaneurysm of medial branch of the profunda femoral artery following dynamic hip screw fixation of proximal femoral fracture. A case report. J Orthop 7(1):e10
Patelis N, Koutsoumpelis A, Papoutsis K et al (2014) Iatrogenic injury of profunda femoris artery branches after intertrochanteric hip screw fixation for intertrochanteric femoral fracture: a case report and literature review. Case Rep Vasc Med 2014:694235
Pengrung N, Sa-ngasoongsong P, Kulachote N, Sirisreetreerux N, Pootracool P, Jaovisidha S (2020) Delayed presentation of huge pseudoaneurysm of profunda femoris artery branch after dynamic hip screw fixation for intertrochanteric fracture: a case report and literature review. J Med Assoc Thail 103:409–414
Piolanti N, Giuntoli M, Nucci AM, Battistini P, Lisanti M, Andreani L (2017) Profunda femoris artery pseudoaneurysm after intramedullary fixation for a pertrochanteric hip fracture. J Orthop Case Rep 7(2):74–77
Popovic D, Stankovic S (2008) Deep femoral artery injury caused by non-fixed lesser trochanter 1 month after osteosynthesis. Inj Extra 39(10):337–340
Pretterklieber B, Pablik E, Dorfmeister K, Pretterklieber ML (2020) There are no safe areas for avoiding the perforating arteries along the proximal part of the femur: a word of caution. Clin Anat 33(4):507–515
Rajaesparan K, Amin A, Arora S, Walton NP (2008) Pseudoaneurysm of a branch of the profunda femoris artery following distal locking of an intramedullary hip nail: an unusual anatomical location. Hip Int 18(3):231–235
Rana N, Dhaked G, Sharma S, Tripathi S (2014) Unusual presentation of pseudoaneurysm with trochanteric fracture femur with associated long-term antiepileptic therapy. Case Rep Orthop 2014:896968
Regus S, Lang W (2015) Arterial injury and pseudoaneurysm formation after lesser trochanter fracture. Int J Surg Case Rep 14:4–6
Ritchie ED, Haverkamp D, Schiphorst TJ, Bosscha K (2007) False aneurysm of the profunda femoris artery, a rare complication of a proximal femoral fracture. Acta Orthop Belg 73(4):530–532
Roy KD, Aggarwal RA, Purohit S, Bandagi G, Marathe N (2016) Iatrogenic pseudo-aneurysm of profunda femoris artery following fixation of intertrochanteric femur fracture: a case report and review of literature. J Clin Diagn Res 10(3):RD01–RD03
Shah YR, Nagammanavar S, Syed TA, Zafar F, Wetherill MH (2008) Pseudoaneurysm of the profunda femoris artery: a rare complication of femoral intertrochanteric fracture fixation. Eur J Orthop Surg Traumatol 18(8):591–593
Shen WY (2005) Complications with the gamma nail and long gamma nail, and their prevention. Osteosynth Trauma Care 13(01):34–41
Singh S, Arora S, Thora A, Mohan R, Sural S, Dhal A (2013) Pseudoaneurysm of profunda femoris artery following dynamic hip screw fixation for intertrochanteric femoral fracture. Chin J Traumatol 16(4):233–236
Storm RK, Sing AK, De Graaf EJR, Tetteroo GWM (2000) Iatrogenic arterial trauma associated with hip fracture. J Trauma Inj Infect Crit Care 48(5):957–959
Sun Q, Fan G, Li X, Gong J, Ge W, Cai M (2017) Relationship between femur and femoral arteries for identifying risk factors for vascular injury. Med Sci Monit 23:1733–1740
Tai CC, Ramachandran M, Young SW, Nathan SS (2004) Unusual cause of deep vein thrombosis following dynamic hip screw fixation. Hip Int 14(4):262–264
Toyota T, Horiuchi H, Takizawa T et al (2017) A case of femoral pseudoaneurysm after surgery for intertrochanteric fracture. J Orthop Sci Off J Jpn Orthop Assoc 22(2):362–365
Tzeng YS, Huang GS, Shen HC, Liu HD (2005) Transcatheter embolization of a profunda femoris pseudoaneurysm complicating an intertrochanteric fracture. J Med Sci 25(6):305–307
Vaidyalingasharma R, Joshi YV, Sanger R (2008) Pseudoaneurysm of medial branch of the profunda femoris artery following dynamic hip screw fixation of proximal femoral fracture: a case report. Eur J Orthop Surg Traumatol 18(1):59–61
Vande Voorde K, Dauwe J, Van Oost J (2018) Late presentation of an iatrogenic pseudoaneurysm of the profunda femoris artery following intramedullary nailing. Case Rep Orthop 2018:8270256–8270256
Wells JM, Mahomed A (2008) Delayed presentation of profunda femoris pseudoaneurysm following an intertrochanteric neck of femur fracture. Inj Extra 39(3):83–85
Yoon HK, Oh HC, Park J, Oyunbat C, Kim T (2016) Rupture of the deep femoral artery during proximal femoral nailing following an intertrochanteric fracture: a case report. Hip Pelvis 28(1):54–59
Zhang B-F, Cong Y-X, Wang P-F, Huang H, Wang H, Zhuang Y (2018) Deep femoral artery branch pseudoaneurysm formation and injury after hip fracture surgery: a case series and a literature review. Medicine 97(6):e9872
Zheng XZ, Lin YC (2019) Huge Iatrogenic pseudoaneurysm of the profunda femoris artery. Eur J Vasc Endovasc Surg 57(5):675
Acknowledgements
The authors thank Mr. David Leslie Patterson of the International Affairs Office of the Faculty of Medicine, Prince of Songkla University, Thailand, for proof reading.
Funding
No funding was received to assist with the preparation of this manuscript. The authors did not receive any support from commercial company.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Ethical approval
This research is approved by the Ethics committee of Faculty of Medicine, Prince of Songkla University, Songkhla, Thailand. The approved project number is REC.65-283-11-1.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Orapiriyakul, W., Chewakidakarn, C., Dissaneewate, K. et al. Silent iatrogenic pseudoaneurysm after intertrochanteric fracture fixation with proximal femoral nailing and cerclage wiring: case report and review of literature. Eur J Orthop Surg Traumatol 33, 2667–2681 (2023). https://doi.org/10.1007/s00590-022-03471-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-022-03471-0