Abstract
Purpose
Adolescent idiopathic scoliosis (AIS) is a common type of idiopathic scoliosis. Previous studies reported that the incidence of intraspinal abnormalities among the presumed idiopathic scoliosis was 13–43%. Intraspinal abnormalities were also considered increasing the risks of progressing of scoliosis and neurological complications following scoliosis corrective surgery. The surgical strategy of presumed adolescent idiopathic scoliosis (PAIS) associated with intraspinal abnormalities remains controversial. The purpose of this study was to investigate whether one-stage posterior surgery safe and effective for the PAIS patients associated with intraspinal abnormalities.
Materials and methods
One hundred and thirteen consecutive patients who underwent one-stage posterior correction surgery were included. Thirty PAIS patients with intraspinal abnormalities without preoperative neurological symptoms were matched with eighty-three AIS patients for sex, age, blood loss, operating time, number of levels and location of instrumentation and curve magnitude. Radiographic and clinical parameters of the patients were evaluated before surgery, within 1 week after surgery, and more than 3 years at the last follow-up for complications and changes in main curve correction, global coronal balance, thoracic kyphosis, sagittal vertical axis, and ODI scores.
Results
On average, the duration of follow-up was 51.5 months in the PAIS group compared to 52.5 months in the AIS group. The preoperative mean major coronal curve was 79.6° (ranged 56.2°–106.7°) and improved to 22.4° (ranged 6.4°–58.1°) at the last follow-up for a 71.9% of correction in the AIS group. The preoperative mean major coronal curve was 80.4° (ranged 63.4°–108.1°) and improved to 23.2° (ranged 4.8°–66.2°) at the last follow-up for a 71.1% of correction in PAIS group. The preoperative ODI score was 32.4 (10–42) in the PAIS group and improved to 11.4 (4–22) at last follow-up, 33.4 (12–42) in the AIS group and improved to 11.5 (5–22) at last follow-up. The global coronal balance, TK and SVA were all significantly improved after surgery and maintained to the last follow-up in the two groups. The neurological complications were observed in 3.3% of PAIS patients and 3.6% of AIS patients. No statistical difference in the parameters between the two groups was observed at the last follow-up.
Conclusion
One-stage posterior corrective surgery is safe and effective in PAIS patients associated with intraspinal abnormalities without preoperative neurological symptoms. Surgical guidelines of AIS are appropriate for the treatment of PAIS patients associated with intraspinal abnormalities.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Scoliosis is a common three-dimensional spinal deformity that has been classified as congenital, idiopathic, neuromuscular, and syndromic. Adolescent idiopathic scoliosis (AIS) is a common type of idiopathic scoliosis from 10 years to maturity. The treatment guidelines of AIS have been well established [1, 2]. With the development of magnetic resonance imaging (MRI), intraspinal abnormalities such as syringomyelia, Chiari malformations, tethered cord, split cord malformation, and intrinsic spinal cord tumor have been found increasingly in patients with presumed adolescent idiopathic scoliosis (PAIS). Previous studies reported that the incidence of intraspinal abnormalities among the presumed idiopathic scoliosis was 13–43% [3,4,5,6,7,8,9]. Intraspinal abnormalities were also considered increasing the risks of progressing of scoliosis and neurological complications following scoliosis corrective surgery. The surgical strategy of PAIS patients associated with intraspinal abnormalities remains controversial. Some spine surgeons considered that the intraspinal malformations should be proceeded before the correction of scoliosis because of its increase in the risk of neurological deterioration. But some studies suggested that proceeded neurosurgery may not need for asymptomatic patients [10,11,12,13,14,15,16,17,18, 28,29,30]. There has been no study investigated whether surgical guidelines of AIS appropriate for the PAIS patients associated with intraspinal abnormalities. In this study, we retrospectively analyzed 113 consecutive patients (30 PAIS patients associated with intraspinal abnormalities compared to 83 AIS patients) who underwent one-stage posterior correction surgery. The purpose of this study was to investigate whether one-stage posterior surgery safe and effective for the PAIS patients associated with intraspinal abnormalities.
Materials and methods
Patients
We performed a retrospective review of all patients with scoliosis who underwent posterior spinal fusion at our hospital from January 2012 to December 2015. The inclusion criteria were (1) presumed AIS in the anterior–posterior (AP) and lateral whole spine X-ray (2) preoperative MRI was acquired (3) a minimum of 3 years follow-up (4) no neurologic symptoms before surgery (5) no congenital spinal deformity and history of spine surgery (6) no neurological intervention (7) All right thoracic curves. Solo chiari malformation patients were excluded. One hundred and thirteen consecutive patients who underwent one-stage posterior correction surgery were included. 83 AIS patients (59 female and 24 male) and 30 PAIS patients associated with intraspinal abnormalities (22 female and 8 male) were included in this study. Syringomyelia was found in 15 patients, Syringomyelia with Chiari deformity was found in 7 patients (All grade I Chiari deformity), syringomyelia with a tethered cord was found in four patients, Splitcord was found in three patients, myelocyst was found in one patient. The characteristics of patients with intraspinal abnormalities were summarized in Table 1.
Surgical procedures
All the patients received Occipital-jaw belt traction for 2 weeks starting with 1/6 bodyweight and finally reached 1/3 bodyweight. Posterior spinal correction and fusion with pedicle screw (titanium; Wego) instrumentation was performed by the same senior surgeon (Y.H.) for all patients. Somatosensory evoked potentials (SSEP) and motor evoked potentials (MEP) and the wake-up test was applied for all patients during surgery.
Data collection
Radiographic parameters including major coronal curve, global coronal balance (C7PL-CSVL), thoracic kyphosis (TK, cobb angle from T5-T12) and the sagittal vertical axis (SVA) were measured preoperatively, early postoperatively (within 1 week), and at a minimum of 3 years postoperatively. The global coronal balance was the horizontal distance from a vertical line extended from the center of the C7 vertebrae to the CSVL. SVA was defined as the distance between the C7 plumb line and the posterior superior corner of S1, it was considered positive when the vertical plumb line lies anterior to the posterior superior corner of S1. Oswestry Disability Index (ODI) were also compared between the PAIS and AIS groups.
Statistical analysis
SPSS version 19.0 (IBM) was used. The data were compared between the groups using Fisher’s exact or Student’s t test according to the data type. P-value < 0.05 was considered to be significant.
Results
Preoperative characteristics
The baseline data of patients in the two groups were similar and summarized in Table 2. On the initial physical examinations, no neurological deficits or just mild low back pain were found in all the patients.
Preoperative radiographic and clinical data of the two groups are summarized in Table 3. For patients in the AIS group, the mean major coronal curve was 79.6°, the mean global coronal balance was 19.8 mm, the mean TK was 53.7° and the mean SVA was -18.8 mm, the mean ODI score was 34.1. For patients in the PAIS group associated with intraspinal abnormalities, the mean major coronal curve was 80.4°, the mean global coronal balance was 21.3 mm, the mean TK was 54.6° and the mean SVA was − 21.2 mm, the mean ODI score was 33.4. All the preoperative parameters were comparable without statistical difference between the two groups (Table 2).
Postoperative characteristics
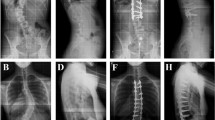
On average, the duration of follow-up was 51.5 months in the PAIS group compared to 52.5 months in the AIS group. Radiographic measurement was made by the same independent blinded reviewer (Fig. 1). The results of the postoperative radiographic data of the two groups are summarized in Table 4. The preoperative mean major coronal curve was 79.6° (ranged 56.2°–106.7°) and improved to 22.4° (ranged 6.4°–58.1°) at the last follow-up for a 71.9% of correction in the AIS group. The preoperative mean major coronal curve was 80.4° (ranged 63.4°–108.1°) and improved to 23.2° (ranged 4.8°–66.2°) at the last follow-up for a 71.1% of correction in PAIS group. The global coronal balance, TK and SVA were all significantly improved after surgery and maintained to the last follow-up in the two groups. No statistical difference in the parameters between the two groups was observed at the last follow-up. Furthermore, the preoperative ODI score was 33.4 (12–42) in the PAIS group and improved to 11.7 (5–22) at last follow-up, 34.1 (12–43) in the AIS group and improved to 11.1 (4–21) at last follow-up. It was also comparable without statistical difference between the two groups (Table 4).
Complications
One patient got mild lower limb sensory dysfunction in the PAIS group postoperatively. Two patients had mild neurologic complications in the AIS group postoperatively, one of them got mild lower limb motor dysfunction, one of them got mild lower limb sensory dysfunction. All of them were detected changes of MEP or SSEP during surgery after which we performed milder correction and used 500 mg methylprednisolone for them. They all recovered after conservative treatment in 3 months. Besides, one patient had a superficial infection in the AIS group after surgery. No neurologic deteriorations in two groups were observed at the last follow-up.
Discussion
Scoliosis associated with intraspinal abnormalities has been reported increasingly in patients with PAIS with the common use of MRI. The incidence of intraspinal abnormalities among the presumed idiopathic scoliosis was 13–43% in the published literature. And most of them were unidentified by preoperative physical examinations. Routine MRI was suggested for the presumed idiopathic scoliosis patients [3,4,5,6,7,8,9]. The scoliosis patients received routine Pre-Op MRI in our hospital due to the high incidence of intraspinal abnormalities.
Previous studies have shown that scoliosis correction was associated with a higher risk of postoperative progression and neurological complications in PAIS patients associated with intraspinal abnormalities compared to AIS patients [19,20,21,22,23]. Bradley et al. [21] reported four syringomyelia-associated scoliosis (SMS) patients of progression in eleven surgically treated series. Charry et al. [13] also reported one case of SMS patient who developed motor dysfunction of lower extremities at 5 years follow-up. Increased traction on the abnormal spinal tissue and changes of cerebrospinal fluid pressure may be responsible for the increased risks of progression and neurological complications. Tomlinson et al. [24] and Qin et al. [25] investigated syringomyelia-associated scoliosis patients who underwent correction surgeries and indicated that scoliosis patients with intraspinal deformities were supposed to receive neurological intervention before spinal corrective surgery. The scoliosis correction in the PAIS group in this study was reported higher than the previous studies of syringomyelia cases [22, 23]. It could be that the previous studies have included more patients with syringomyelia within the instrumented field of surgery whereas in this study more patients had the abnormality above or below the correction. And the patients in this study had relatively soft and mild curves.
In contrast to previous studies, our patients’ series were all received single-stage corrective surgery. Over an average of 52 months follow-up, the radiographic and clinical outcomes are comparable between the PAIS group and the AIS group. The progression of over 10 degrees was found in 6% of intraspinal abnormalities patients and 7% of AIS patients. The neurological complications were observed in 3.3% of PAIS patients and 3.6% of AIS patients. Most of the patients got mild complications and all recovered within 6 months. We did not have postop MRI for these patients, because they have only mild symptoms. We chose conservative treatment for these patients after which they all recovered and had noneurologic deteriorations at the last follow-up. The correction rate, ODI scores in the PAIS group was comparable to the AIS group. The complications were also comparable and mild. Single-stage corrective surgery is safe and effective in PAIS patients associated with intraspinal abnormalities without preoperative neurological symptoms. Our study has similar results in some well-designed studies. Sha et al. [11] compared the radiographic and clinical outcomes of single-stage posterior spinal fusion between patients with right thoracic AIS and SMS and found no significant difference. Zhang et al. [10] also evaluated one-stage posterior scoliosis correction surgery in patients with syringomyelia with no or mild neurological symptom. They suggested that neurologic intervention was not necessary for intraspinal abnormalities in patients without preoperative neurological symptoms.
Moreover, the patients in our study all received Occipital-jaw belt traction for 2 weeks. Preoperative traction is a safe and effective way to maximize correction and help to estimate the adaptation of the spinal tissue after corrective surgery. When doing the traction, physical examination was required every day, because complications were reported related to traction. Ginsburg et al. [26].reported a case of hypoglossal nerve injury with 40% of the patient’s body weight when doing traction.
Monitoring of SSEP and MEP and the wake-up test was conducted in all patients in this study during surgery. Previously published studies also indicated that spinal cord monitoring of SSEP and MEP and the wake-up test was necessary when doing spinal corrective procedure [10, 27].
Although the study was well-designed, we do have some limitations. We only investigated PAIS patients, and there are still some other patients who had either similar intraspinal anomalies with non-AIS like curves or with similar-looking curves who had staged procedures. The treatment for them also remained controversial and we will investigate these patients in our next study.
Conclusions
One-stage posterior corrective surgery is safe and effective in PAIS patients associated with intraspinal abnormalities without preoperative neurological symptoms. Surgical guidelines of AIS is appropriate for the treatment of PAIS patients associated with intraspinal abnormalities.
Availability of data and material
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
We have permissions for the use of software, questionnaires/(web) surveys and scales in their studies.
References
Lenke LG, Betz RR, Harms J, Bridwell KH, Clements DH, Lowe TG, Blanke K (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am 83(8):1169–1181
Rose PS, Lenke LG (2007) Classification of operative adolescent idiopathic scoliosis: treatment guidelines. Orthop Clin North Am 38(4):521–529
Singhal R (2013) The use of routine preoperative magnetic resonance imaging in identifying intraspinal anomalies in patients with idiopathic scoliosis: a 10-year review. Eur Spine J 22(2):355–359
Zhang Y (2019) Intraspinal neural axis abnormalities in severe spinal deformity: a 10-year MRI review. Eur Spine J 28(2):421–425
Swarup I, Silberman J, Blanco J, Widmann R (2019) Incidence of Intraspinal and Extraspinal MRI Abnormalities in Patients With Adolescent Idiopathic Scoliosis. Spine Deform 7(1):47–52
Zhang Y, Xie J, Wang Y, Bi N, Li T, Zhang J et al (2019) Intraspinal neural axis abnormalities in severe spinal deformity: a 10-year MRI review. Eur Spine J 28(2):421–425
Pahys JM, Samdani AF, Betz RR (2009) Intraspinal anomalies in infantile idiopathic scoliosis prevalence and role of magnetic resonance imaging. Spine (Phila Pa 1976) 34:434–438
Zhang W, Sha S, Xu L (2016) The prevalence of intraspinal anomalies in infantile and juvenile patients with “presumed idiopathic” scoliosis: a MRI-based analysis of 504 patients. BMC Musculoskelet Disord (Engl) 17:189
Nakahara D, Yonezawa I, Kobanawa K, Sakoda J, Nojiri H, Kamano S, Okuda T, Kurosawa H (2011) Magnetic resonance imaging evaluation of patients with idiopathic scoliosis: a prospective study of four hundred seventy-two outpatients. Spine (Phila Pa 1976) 36(7):E482–E485
Zhang ZX (2015) Surgical treatment of scoliosis associated with syringomyelia with no or minor neurologic symptom. Eur Spine J 24(7):1555–1559
Sha S (2016) Does surgical correction of right thoracic scoliosis in syringomyelia produce outcomes similar to those in adolescent idiopathic scoliosis? J Bone Joint Surg Am 98(4):295–302
Sengupta DK, Dorgan J, Findlay GF (2000) Can hindbrain decompression for syringomyelia lead to regression of scoliosis? Eur Spine J 9:198–201
Charry O, Koop S, Winter R, Lonstein J, Denis F, Bailey W (1994) Syringomyelia and scoliosis: a review of twenty-five pediatric patients. J Pediatr Orthop 14:309–317
Emery E, Redondo A, Rey A (1997) Syringomyelia and Arnold Chiari in scoliosis initially classified as idiopathic: experience with 25 patients. Eur Spine J 6:158–162
Evans SC, Edgar MA, Hall-Graggs MA, Powell MP, Taylor BA, Noordeen HH (1996) MRI of ‘idiopathic’ juvenile scoliosis: a prospective study. J Bone Joint Surg Br 78:314–317
Strahle JM et al (2019) Radiological and clinical predictors of scoliosis in patients with Chiari malformation type I and spinal cord syrinx from the Park-Reeves Syringomyelia Research Consortium. J Neurosurg Pediatr 1–8
Wang K et al (2019) Opinion for different centers: surgical experience with Chiari malformation type I in children at Xuanwu Hospital, China. Childs Nerv Syst 35(10):1915–1919
McMaster MJ (1984) Occult intraspinal anomalies and congenital scoliosis. J Bone Joint Surg Am 66:588–601
Ono A, Ueyama K, Okada A (2002) Adult scoliosis in syringomyelia associated with Chiari I malformation. Spine (Phila Pa 1976) 27:E23–E28
Ono A, Suetsuna F, Ueyama K (2007) Surgical outcomes in adult patients with syringomyelia associated with Chiari malformation type I: the relationship between scoliosis and neurological findings. J Neurosurg Spine 6:216–221
Bradley LJ, Ratahi ED, Crawford HA, Barnes MJ (2007) The outcomes of scoliosis surgery in patients with syringomyelia. Spine (Phila Pa 1976) 32(21):2327–2333
Noordeen MH, Taylor BA, Edgar MA (1994) Syringomyelia. A potential risk factor in scoliosis surgery. Spine (Phila Pa 1976) 19:1406–1409
Xie JM, Zhang Y, Wang YS (2014) The risk factors of neurologic deficits of one-stage posterior vertebral column resection for patients with severe and rigid spinal deformities. Eur Spine J 23:149–156
Tomlinson RJ, Wolfe MW, Nadall JM et al (1994) Syringomyelia and developmental scoliosis. J Pediatr Orthop 14:580–585
Qin X (2016) Effectiveness of selective thoracic fusion in the surgical treatment of syringomyelia-associated scoliosis: a case-control study with long-term follow-up. Spine (Phila Pa 1976) 41(14):E887–E892
Ginsburg GM, Bassett GS (1998) Hypoglossal nerve injury caused by halo suspension traction. Spine (Phila Pa 1976) 23:1490–1493
Wang G (2015) One-stage correction surgery of scoliosis associated with syringomyelia: Is it safe to leave untreated a syrinx without neurological symptom? J Spinal Disord Tech 28(5):E260–E264
Lewonowski K, King JD, Nelson MD (1992) Routine use of magnetic resonance imaging in idiopathic scoliosis patients less than 11 years of age. Spine (Phila Pa 1976) 17:109–116
Park JK, Gleason PL, Madsen JR, Goumnerova LC, Scott RM (1997) Presentation and management of Chiari malformation in children. Pediatr Neurosurg 26:190–196
Bruzek AK et al (2019) Syringomyelia in children with closed spinal dysraphism: long-term outcomes after surgical intervention. J Neurosurg Pediatr 1–7
Funding
We do not have a funding.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Jingwei Liu, Shuo Zhang, Yong Hai, Nan Kang and Yiqi Zhang. The first draft of the manuscript was written by Jingwei Liu and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest/Competing interests
We do not have a financial or personal relationship with a third party. We have full control of all primary data and we agree to allow the journal to review their data if requested. On behalf of all authors, the corresponding author declares that there is no conflict of interest.
Ethics approval
The study was approved by the Department of Ethics, Beijing Chaoyang Hospital, Capital Medical University.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, J., Zhang, S., Hai, Y. et al. The safety and efficacy of one-stage posterior surgery in the treatment of presumed adolescent idiopathic scoliosis associated with intraspinal abnormalities a minimum 3-year follow-up comparative study. Eur Spine J 30, 692–697 (2021). https://doi.org/10.1007/s00586-020-06529-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06529-x