Abstract
Sickle cell disease (SCD) is characterized by a hypercoagulable state as a result of multiple factors, including chronic hemolysis and the presence of circulating cell-derived microparticles (MPs). The aim of this work was to study the impact of erythrocyte-derived circulating microparticles (glycophorin A; CD235 positive) on coagulation activation and their probable role in contribution to painful crisis in SCD patients. Peripheral blood samples of 25 SCD patients during painful crisis and in steady state were studied for the presence of erythrocyte-derived MPs using flow cytometry. Estimation of D-dimer level, as a marker of coagulation activation, was done using semiquantitative assay. Thirty-six healthy individuals, age- and sex-matched, were included as a control group. Erythrocyte-derived MPs level was significantly higher in SCD patients during painful crisis compared to control group (p = 0.02), but no statistically significant difference was found between erythrocyte-derived MPs level in SCD patients in steady state compared to controls or to SCD patients during painful crisis (p = 0.3 and 0.49, respectively). D-dimer level was higher in SCD patients both during crisis and in steady state compared to controls (p < 0.001). SCD during painful crisis is associated with increased levels of erythrocyte-derived MPs and D-dimer which may contribute to the hypercoagulable state observed in such group of patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sickle cell disease (SCD) is a progressive hemoglobinopathy caused by substitution of glutamic acid by valine in the sixth amino acid of β-globin chain (Dover and Platt 1998). This amino acid substitution results in polymerization of abnormal sickle hemoglobin (HbS) upon de-oxygenation and causes erythrocytes to take on its characteristic sickle shape (Bunn and Forget 1986; Edelstein et al. 1973).
Formation of deoxy-HbS polymer fibers triggers a whole series of changes of red blood cell membrane; ion channels are affected and their dysfunction is responsible for cellular dehydration which favors deoxy-HbS polymerization, creating a vicious circle leading to more deoxy-HbS formation, release of hemichromes leads to formation of protein band 3 aggregates on which anti-band 3 IgGs accumulate, and release of heme and Fe3+ favors an oxidizing microenvironment. Furthermore, loss of normal cell membrane phospholipid asymmetry leads to exposure of anionic phosphatidylserines (PS) at the external side of membrane creating a procoagulant surface. Finally, microparticles are released (Stuart and Nagel 2004).
Microparticles (MPs) represent a heterogeneous population of vesicles with a diameter of 0.15–1 μm that are released by budding of the plasma membrane from nearly every type of cell during activation, injury, or apoptotic processes (Ardoin et al. 2007). MPs express high levels of PS on their outer leaflet together with surface markers from their cell of origin (Hugel et al. 2005). The function of MPs is dependent on cell type from which they originate (Mezentsev et al. 2005).
MPs play important role in the painful vaso-occlusive crisis process through activating properties conferred to them by their reorganized membrane (Piccin et al. 2007). Erythrocyte-derived MPs are known to expose a high amount of PS at their outer surface, thus providing an anionic phospholipid surface suitable to the assembly of the tenase and prothrombinase complexes (Nébor et al. 2013). MPs derived from monocytes and endothelial cells express tissue factor (Shet et al. 2003); once coagulation cascade is initiated by tissue factor, thrombin generation is greatly accelerated in the presence of PS (Zwaal and Schroit 1997; Mann 1999; Setty et al. 2001). Moreover, hydrolysis of PS by secretory phospholipase A2 leads to generation of vasoactive prostaglandins, leukotrienes, and thromboxanes (Neidlinger et al. 2005, 2006).
The aim of our work was to study the impact of erythrocyte-derived circulating microparticles (glycophorin A; CD235 positive) on coagulation activation and their probable role in contribution to painful crisis in SCD patients.
Subjects and methods
Subjects
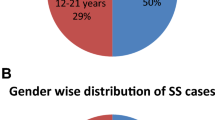
This is a prospective case-control study that included 25 SCD patients, 14 males (56 %) and 11 females (44 %). Their ages ranged between 3 and 27 years (median 11 and mean 12.56 ± 6.07 years). Diagnosis of SCD was established using hemoglobin electrophoresis and/or high-performance liquid chromatography at Pediatric Hematology Clinic, New Children Hospital, Cairo University; 15/25 cases (60 %) had Hb S-beta thalassemia, 9/25 cases (36 %) had Hb SS, while 1 case (4 %) had Hb SC disease. Thirty-six age- and sex-matched healthy subjects were enrolled as a control group. All participants and/or their guardians gave informed consent before recruitment. The study was approved by the Ethics Committee, Cairo University and in accordance with the principles of Helsinki Declaration.
Methods
Patients’ medical records were thoroughly reviewed for disease course, transfusion history, splenectomy, and hydroxyurea therapy. Detailed history of painful crisis, its frequency and duration of hospitalization, was obtained. Peripheral blood samples were collected for 25 SCD patients during painful crisis and for 17/25 SCD patients in steady state during a subsequent follow-up visit. Painful crisis was defined as seeking medical treatment for not otherwise explained pain in extremities, back, abdomen, chest, or head, while steady state was defined as a period without pain or painful crisis for at least 4 weeks (Ballas and Lusardi 2005). Laboratory work-up included complete blood count, markers of hemolysis (reticulocyte count, serum bilirubin, and lactate dehydrogenase), coagulation profile (prothrombin time, activated partial thromboplastin time, and D-dimer assay), and erythrocyte-derived MPs using anti CD235 (glycophorin A) monoclonal antibodies.
For each patient, 2 ml venous blood samples were collected from the antecubital vein without a tourniquet to avoid stressing the cells. Blood was collected into sodium citrate vacutainer, and within 15 min, cells were removed by centrifugation (20 min at 1550×g at 20 °C) to prevent platelet destruction and concurrent formation of platelet-derived MPs. Thus, prepared platelet-poor plasma was free of leukocytes and erythrocytes, and contains about 1 % of the original number of platelets (van Beers et al. 2009). Plasma aliquots of 250 μL were immediately stored at−80 °C until used.
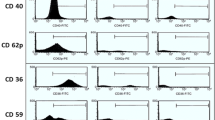
Detection of erythrocyte-derived microparticles by flow cytometry
Frozen plasma samples (250 μL) were thawed on melting ice for 1 h and centrifuged for 30 min at 18,890×g at 20 °C to pellet the MPs. Two hundred twenty-five microliters of the supernatant were removed and the pellet resuspended in 225 μL phosphate-buffered saline (PBS) containing citrate (154 mmol/L NaCl, 1.4 mmol/L phosphate, 10.9 mmol/L trisodium citrate, pH 7.4). Again, the MPs suspension was centrifuged for 30 min at 18,890×g at 20 °C and 225 μL of supernatant were removed. The MPs pellet was resuspended in 75 μL PBS-citrate.
Five microliters of MPs suspension were added to 35 μL CaCl2-containing PBS (154 mmol/l NaCl, 1.4 mmol/l phosphate, 2.5 mmol/l CaCl2), then 5 μL FITC-labeled annexin V (PN IM2375- Beckman coulter) and 10 μL of PE-labeled CD 235 (anti-glycophorin A) monoclonal antibody (AO7792, Beckman Coulter) or isotype-matched control antibodies were added to tubes. After sample incubation for 15 min at room temperature in the dark, 900 μL of PBS-CaCl2 were added to all tubes (except for the control tube, 900 μL of PBS-citrate were added) to make a total volume of 955 μL. Samples were analyzed for 1 min in flow cytometer (FC500, Beckman Coulter). Both forward scatter and side scatter were set at logarithmic gain. MPs were identified on the basis of their size and on their ability to bind cell-type specific CD 235 (anti-glycophorin A) antibodies and annexin V. Number of microparticles (NMP) per milliliter of plasma was estimated using number of events (N) of cell-specific antibody binding as follows:
NMP/mL = N × [955 μL / μL flow rate in 1 min] × [100 μL / 5 μL] × [1,000 μL / 250 μL] (Berckmans et al. 2005; van Beers et al. 2009).
D-dimer assay was performed using D-Dimer semiquantitative agglutination kit (D205-000, TECO, Germany) according to manufacturer’s instructions, and the results were interpreted as grades ranging from grade 1 to grade 7, where grade 1, <250 ng/ml (negative); grade 2, 250–500 ng/ml; grade 3, 500–1000 ng/ml; grade 4, 1000–2000 ng/ml; grade 5, 2000–4000 ng/ml; grade 6, 4000–8000 ng/ml; and grade 7, 8000–16,000 ng/ml.
Statistics
Data were statistically described in terms of mean ± standard deviation (SD), median and range, or frequencies (number of cases) and percentages when appropriate. Comparison of numerical variables between study groups was done using Mann Whitney U test for independent samples. For comparing categorical data, chi-square (χ 2) test was performed. Exact test was used instead when the expected frequency was less than 5. Correlation between various variables was done using Spearman rank correlation equation. p value less than 0.05 was considered statistically significant. All statistical calculations were done using computer programs SPSS (Statistical Package for the Social Science; SPSS Inc., Chicago, IL, USA) version 15 for Microsoft Windows.
Results
In the studied SCD patients, 15/25 (60 %) were on chronic transfusion, 11/25 (44 %) had been splenectomized, and 14/25 (56 %) were on hydroxyurea therapy.
During painful crisis, duration of hospital stay ranged from 1–13 days (median 2.5 days and mean of 2.95 ± 5.02 days). History of previous painful crisis showed that four patients (16 %) had low frequency (<1 time/year), 11 patients (44 %) had moderate frequency (1–5 times/year), while 10 patients (40 %) showed high frequency (>5 times/year) of painful attacks. Markers of hemolysis and coagulation in SCD during painful crisis are shown in Table 1.
The erythrocyte-derived MPs level in control group and SCD patients (during painful crisis and steady state) are shown in Table 2 and Fig. 1. SCD patients during painful crisis had significantly higher median number of erythrocyte-derived MPs than control group (p = 0.02). However, no statistically significant difference was detected between median numbers of erythrocyte-derived MPs of SCD patients in steady state when compared to control group or to patients during painful crisis (p = 0.3 and 0.49, respectively).
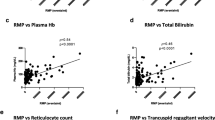
Our study showed that splenectomy, blood transfusion, frequency of painful crisis, and hydroxyurea therapy did not affect erythrocyte-derived MPs levels [data not shown]. However, the number of received blood transfusion/year is significantly correlated to the number of erythrocyte-derived MPs (p = 0.03, r = 0.44) (Fig. 2). Correlation of erythrocyte-derived MPs with markers of hemolysis and coagulation showed no correlation in SCD patients during painful crisis (Table 3).
D-dimer levels ranged between grades 1 and 7 with median grade 3 in SCD patients during painful crisis, while it ranged between grades 2 and 4 with median grade 3 during steady state. All control subjects showed negative D-dimer. There were statistically significant differences between D-dimer levels in SCD patients during crisis and steady state in comparison to normal control (p value < 0.001 for both), while no statistically significant difference was evident between D-dimer levels in patients during crisis and in steady state (p = 0.31).
No correlation was found between erythrocyte-derived MPs and D-dimer either in crisis (p = 0.19, r = −0.27) or in steady state (p = 0. 34, r = −0.25); however, borderline inverse correlation between activated partial thromboplastin time and erythrocyte-derived MPs during painful crisis was evident (Table 3).
Discussion
Erythrocyte-derived MPs were found to be increased in SCD patients. This increase is detected by flow cytometric measurement of cell specific anti- CD 235 (anti-glycophorin A) monoclonal antibody and annexin V. Annexin V provides a highly sensitive assay for exposure of phospholipids in erythrocytes (Tait and Gibson 1994) and correlates linearly with the ability of red blood cells to support prothrombinase activity (Kuypets et al. 1996).
Several previous studies stated that high numbers of both erythrocyte-derived and platelet-derived MPs are present in patients with SCD (Allan et al. 1982; Wun et al. 1998; Shet et al. 2003; van Beers et al. 2009; Camus et al. 2012; Tantawy et al. 2012). In our study, the level of erythrocyte-derived MPs was higher in SCD patients than in controls; however, there was no statistically significant difference between the level of erythrocyte-derived MPs in SCD patients during their steady state and during painful crisis; it comes in agreement with van Beers et al. (2009) who found that the number of MPs did not differ significantly between baseline conditions and during a painful crisis in SCD.
The level of erythrocyte-derived MPs was higher in splenectomized SCD patients, although no statistically significant difference was found. The number of circulating abnormal RBC and MPs that express PS are increased after splenectomy and patients with hemolytic anemias are at risk of thromboembolic complications, particularly following splenectomy, and it has been stated that splenectomized patients with thalassemia intermedia have significantly higher levels of MPs and thrombin-antithrombin complexes when compared to non-splenectomized patients (Westerman et al. 2008).
The number of erythrocyte-derived MPs is significantly correlated to the number of received blood transfusion/year. MPs accumulate in blood products during storage (Rubin et al. 2008); therefore, repeated transfusion leads to the introduction of more MPs to multitransfused patients, accordingly leading to increased risk of adverse outcomes and patients are more prone to hypercoagulability (Kriebardis et al. 2012).
Semiquantitative assay of D-dimer level was used in our study as a marker of coagulation activation. There was statistically significant increase in the D-dimer level in SCD patients both in steady state and during crisis; SCD has been known to be a hypercoagulable state (Ataga and Key 2007; Adam et al. 2009). The mechanism of hypercoagulability is probably multifactorial and involves abnormalities in platelet function, thrombin generation, and fibrinolysis (Stuart and Setty 2001). Furthermore, it was demonstrated that even patients with sickle trait may be at increased risk for deep venous thrombosis (Austin et al. 2007; Adam et al. 2009); however, we did not find any significant correlation between erythrocyte-derived MPs and D-dimer in painful crisis or in steady state. This is in contrast to Shet et al. (2003) who stated that the total number of MPs, total tissue factor-positive MPs, monocyte-derived tissue factor-positive MPs, and erythrocyte-derived MPs are correlated with D-dimer, thrombin-antithrombin complexes, and F1 + 2 levels in SCD patients, suggesting that MPs may contribute to the hypercoagulable state observed in patients with SCD and other hemolytic anemias. van Beers and colleagues (2009) also reported that the majority of MPs in SCD patients originate from platelets and erythrocytes, and there is a strong association of erythrocyte-derived MPs and markers of fibrinolysis and coagulation activation (vWF-Ag, D-dimer, and F1 + 2) using enzyme-linked immunosorbent assay (ELISA). In addition, they found a relation between erythrocyte-derived MPs and the activation of factor XI and the ability of anti-factor XI to block thrombin generation by MPs isolated from plasma samples of SCD patients. This difference in our findings compared to others could be attributed to the use of semiquantitative latex agglutination test in our study to assess D-dimer levels versus the more sensitive, yet more costly, ELISA technique used in other studies.
Borderline inverse correlation between number of erythrocyte-derived MPs and activated partial thromboplastin time during painful crisis was found in our study. This comes in agreement with Horne et al. (2006) who were using ex vivo experiments with hemolysates and showed that erythrocyte-derived MPs enhance coagulation activation. Furthermore, in patients with idiopathic thrombocytopenic purpura, erythrocyte-derived MPs are correlated with shortening of activated partial thromboplastin time and increased factor XI activity (Fontana et al. 2008).
On studying the relation between erythrocyte-derived MPs and markers of hemolysis, we did not find any correlations during painful crisis. This is in contrast to van Beers et al. (2009) whose study showed that erythrocyte-derived MPs strongly correlated with plasma levels of hemolytic markers, i.e., hemoglobin and lactate dehydrogenase. This difference may be attributed to the difference in disease severity where the median duration of hospital admission for treatment of painful attack in van Beers and colleagues study was 8 versus 3 days in our study, indicating more severe painful crisis in their cohort. Moreover, their patients were not treated with chronic blood transfusion in contrast to ours where 44 % received chronic blood transfusion and it was found that erythrocyte-derived MPs differ between in vivo and ex vivo condition regarding their properties and the stimulus for their generation (Tissot et al. 2010).
In conclusion, SCD is associated with increased levels of circulating erythrocyte-derived MPs and D- dimer which may contribute to the hypercoagulable state and precipitation of painful crisis in these patients. However, larger sample size and studying levels of MPs from other cellular origins are required for identification of exact mechanism of such hypercoagulable state. Approaches to control this hypercoagulable state in SCD patients are required and should be studied on large scale in the treatment regimen to reduce the frequency and severity of painful crisis.
References
Adam SS, Key NS, Greenberg CS (2009) D-dimer antigen: current concepts and future prospects. Blood 113(13):2878–2887
Allan D, Limbrick AR, Thomas P, Westerman MP (1982) Release of spectrin free spicules on reoxygenation of sickled erythrocytes. Nature 295:612–613
Ardoin SP, Shanahan JC, Pisetsky DS (2007) The role of microparticles in inflammation and thrombosis. Scand J Immunol 66:159–165
Ataga KI, Key NS (2007) Hypercoagulability in sickle cell disease: new approaches to an old problem. Hematol (Am Soc Hematol Educ Program) 91–96
Austin H, Key NS, Benson JM, Lally C, Dowling NF, Whitsett C et al (2007) Sickle cell trait and the risk of venous thromboembolism among blacks. Blood 110:908–912
Ballas SK, Lusardi M (2005) Hospital readmission for adult acute sickle cell painful episodes: frequency, etiology, and prognostic significance. Am J Hematol 79:17–25
Berckmans RJ, Nieuwland R, Kraan MC, Schaap M, Pots D, Smeets T et al (2005) Synovial microparticles from arthritic patients modulate chemokine and cytokine release by synoviocytes. Arthritis Res Ther 7:R536–R544
Bunn H, Forget BG (1986) Hemoglobin: molecular, genetic and clinical aspects. WB Saunders, Philadelphia, PA, USA
Camus SM, Gausserès B, Bonnin P, Loufrani L, Grimaud L, Charue D et al (2012) Erythrocyte microparticles can induce kidney vaso-occlusions in a murine model of sickle cell disease. Blood 120(25):5050–5058
Dover GJ, Platt OS (1998) Sickle Cell Disease. In: Nathan and Oski’s Hematology of infancy and childhood, DG Nathan and SH Orkin (eds), 5th Edition, WB Saunders Company Volume 1.
Edelstein SJ, Telford JN, Crépeau RH (1973) Structure of fibers of sickle cell hemoglobin. Proc Natl Acad Sci U S A 70:1104–1107
Fontana V, Jy W, Ahn ER, Dudkiewicz P, Horstman LL, Duncan R et al (2008) Increased procoagulant cell-derived microparticles (CMP) in splenectomized patients with ITP. Thromb Res 122:599–603
Horne MK, Cullinane AM, Merryman PK, Hoddeson EK (2006) The effect of red blood cells on thrombin generation. Br J Haematol 133:403–408
Hugel B, Martinez MC, Kunzelmann C, Freyssinet JM (2005) Membrane microparticles: two sides of the coin. Physiology (Bethesda) 20:22–27
Kriebardis A, Antonelou M, Stamoulis K, Papassideri I (2012) Cell-derived microparticles in stored blood products: innocent-bystanders or effective mediators of post-transfusion reactions. Blood Transfus 10(Suppl 2):s25–s38
Kuypets FA, Lewis RA, Hua M, Schott MA, Discher D, Ernst JD et al (1996) Detection of altered membrane phospholipid asymmetry in subpopulations of human red blood cells using fluorescently labeled annexin V. Blood 87:1179–1187
Mann KG (1999) Biochemistry and physiology of blood coagulation. Thromb Haemost 82:165–174
Mezentsev A, Merks RM, O’Riordan E, Chen J, Mendelev N, Goligorsky MS et al (2005) Endothelial microparticles affect angiogenesis in vitro: role of oxidative stress. Am J Physiol Heart Circ Physiol 289:H1106–H1114
Nébor D, Romana M, Santiago R, Vachiery N, Picot J, Broquere C et al (2013) Fetal hemoglobin and hydroxycarbamide modulate both plasma concentration and cellular origin of circulating microparticles in sickle cell anemia children. Haematologica 98(6):862–867
Neidlinger NA, Hirvela ER, Skinner RA (2005) Postinjury serum secretory phospholipase A2 correlates with hypoxemia and clinical status at 72 hours. J Am Coll Surg 200:173–178
Neidlinger NA, Larkin SK, Bhagat A (2006) Hydrolysis of phosphatidylserine exposing red blood cells by secretory phospholipase A2 generates lysophosphatidic acid and results in vascular dysfunction. J Biol Chem 281:775–781
Piccin A, Murphy WG, Smith OP (2007) Circulating microparticles: pathophysiology and clinical implications. Blood Rev 21:157–171
Rubin O, Crettaz D, Canellini G, Tissot JD, Lion N (2008) Microparticles in stored red blood cells: an approach using flow cytometry and proteomic tools. Vox Sang 95:288–297
Setty BN, Rao AK, Stuart MJ (2001) Thrombophilia in sickle cell disease: the red cell connection. Blood 98:3228–3233
Shet AS, Aras O, Gupta K, Hass MJ, Rausch DJ, Saba N et al (2003) Sickle blood contains tissue factor-positive microparticles derived from endothelial cells and monocytes. Blood 102:2678–2683
Stuart MJ, Nagel RL (2004) Sickle-cell disease. Lancet 364:1343–1360
Stuart MJ, Setty BN (2001) Hemostatic alterations in sickle cell disease: relationships to disease pathophysiology. Pediatr Pathol Mol Med 20:27–46
Tait JF, Gibson D (1994) Measurement of membrane phospholipid asymmetry in normal and sickle-cell erythrocytes by means of annexin V binding. J Lab Clin Med 123:741–748
Tantawy AA, Adly AA, Ismail EA, Habeeb NM, Farouk A (2012) Circulating platelet and erythrocyte microparticles in young children and adolescents with sickle cell disease: relation to cardiovascular complications. Platelets 18(1):167–178
Tissot JD, Rubin O, Canellini G (2010) Analysis and clinical relevance of microparticles from red blood cells. Curr Opin Hematol 17:571–577
van Beers E, Schaap M, Berckmans R, Nieuwland R, Sturk A, van Doormaal F et al (2009) Circulating erythrocyte-derived microparticles are associated with coagulation activation in sickle cell disease. Haematologica 94(11):1513–1519
Westerman M, Pizzey A, Hirschman J, Cerino M, Weil- Weiner Y, Ramotar P et al (2008) Microvesicles in haemoglobinopathies offer insights into mechanisms of hypercoagulability, haemolysis and the effects of therapy. Br J Haematol 142:126–135
Wun T, Paglieroni T, Rangaswami A, Franklin PH, Welborn J, Cheung A et al (1998) Platelet activation in patients with sickle cell disease. Br J Haematol 100:741–749
Zwaal RF, Schroit AJ (1997) Pathophysiologic implications of membrane phospholipid asymmetry in blood cells. Blood 89:1121–1132
Conflict of interest
The authors declare that they have no conflict of interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zayed, R.A., El-Ghamrawi, M., Alwakeel, H.A. et al. Impact of circulating erythrocyte-derived microparticles on coagulation activation in sickle cell disease. Comp Clin Pathol 24, 1123–1128 (2015). https://doi.org/10.1007/s00580-014-2045-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00580-014-2045-0