Abstract
Background
Surgical intervention is the most accurate method for the treatment of hepatic hemangioma. The advantages of laparoscopic surgery on quality of life should be clarified by prospective studies.
Methods
The sample sizes of the laparoscopic and open surgery groups were calculated based on previous retrospective literature. Intraoperative and postoperative parameters were prospectively collected and analyzed. Quality of life in both groups was predicted by a mixed linear model.
Results
Sixty patients were enrolled in the laparoscopic surgery group and open surgery group. The laparoscopic group had a longer operation time (P = 0.040) and more hospitalization expenses (P = 0.001); however, the Clavien–Dindo classification and comprehensive complication index suggested a lower incidence of surgical complications in the laparoscopic group, with P values of 0.049 and 0.002, respectively. After mixed linear model prediction, between-group analysis indicated that the laparoscopic group had little impact on role-physical functioning and role-emotional functioning; in addition, within-group analysis showed a rapid recovery time on role-physical functioning and role-emotional functioning in the laparoscopic group. Quality of life in both groups recovered to the preoperative level within 1 year after the operation.
Conclusion
The advantages of laparoscopic hepatectomy for hepatic hemangioma were fewer postoperative complications, lower impact on quality of life and faster recovery from affected quality of life.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Hepatic hemangiomas are the most common benign liver tumors in adults, with an incidence rate of 0.4–20% [1]. Despite the high incidence rate, a conservative approach is recommended unless symptoms or severe complications such as Kasabach–Merrit syndrome and even tumor rupture develop [2,3,4]. In addition, a few studies believe that rapidly enlarging hemangiomas are also reference factors for surgical intervention [5].
Radiofrequency ablation, hepatic artery embolization and surgical resection are commonly recommended treatment methods for these lesions [6, 7]. Among them, surgical resection is the most important treatment method at present because of its curative effect [8]. With a benign course, surgical trauma and postoperative recovery should be taken into serious consideration. However, compared with the open approach, the potential advantages and inferiorities of the laparoscopic approach have not been demonstrated by prospective research.
This study prospectively designed and collected hepatic hemangioma patients who underwent traditional open and laparoscopic surgery and comprehensively analyzed the intraoperative technical parameters, postoperative recovery and quality of life to provide a high-quality reference for the surgical treatment of hepatic hemangioma resection.
Materials and methods
Experimental design
This study was designed as a prospective, nonrandomized controlled trial. The primary endpoints were the length of postoperative hospital stay and the cost of hospitalization, and the secondary endpoint was quality of life after surgery, which was evaluated by the SF-36 Quality of Life Questionnaire [9].
This study has been reviewed by the Ethics Review Committee of the Chinese Clinical Trial Registry (CHIECRCT-20180243) and has completed the clinical trial registration in the Chinese Clinical Trial Registry (ChiCTR1800018145).
Patient selection
Inclusion criteria for surgical patients: (1) Combined with preoperative imaging and postoperative pathology, patients diagnosed with hepatic hemangioma; (2) Single or multiple tumors, clear clinical symptoms or rapid increase in tumor diameter in asymptomatic patients (average annual increase of ≥ 2 cm); (3) Aged 18 to 65 years; (4) Preoperative Child–Pugh score ≤ 7 points; (5) Eligible to be treated by both laparoscopic resection and open resection; (6) Normal cardio-pulmonary function.
The exclusion criteria for surgical patients were as follows: (1) previous history of upper abdomen surgeries; (2) preoperative treatment for hepatic hemangioma; (3) absence of an informed consent file; and (4) infectious disease.
Sample size
The number of patients needing to be prospectively included was based on the primary endpoint of previous retrospective literature data, and the sample size for this study was calculated based on a two-sided α of 0.05 and 80% power [10]. In addition, a dropout rate of 20% was estimated. Patients converted from laparoscopic to open surgery were analyzed in the laparoscopic group.
Quality of life
The SF-36 Quality of Life Questionnaire was used to assess patientsʼ quality of life before surgery and at 1, 3 and 12 months postoperatively. The checklist contains eight dimensions: Physical Functioning, Role-physical Functioning (RP), Bodily Pain (BP), and General Health. Vitality (VT), Social Functioning (SF), Role-Emotional Functioning (RE) and Mental Health (MH). Scores per dimension range from 0 to 100, and a higher score indicates a better health status. Data were collected preoperatively by filling in a scale and postoperatively by telephone return visit.
Statistical methods
Continuous variables that conformed to a normal distribution were tested by t test, those that did not conform to a normal distribution were tested by the Mann–Whitney U test, and classified variables were tested by the Chi-square test. A mixed linear model was used to predict the scores of eight domains of the SF-36®. A fixed effect was arranged in each model, including treatment type (laparoscopic/open surgery), time (measured in months after surgery), type × time interaction and a random intercept. Based on linear mixed models, the mean score of each domain with 95% CI was estimated for each time point: baseline (time of operation) and 1, 3, and 12 months after surgery. The mean change in within-group and between-group differences in change at each time point were calculated. P < 0.05 was considered statistically significant. Statistical analysis was performed by SPSS 22.0 (IBM Corp).
Results
Characteristics of patients
All of the laparoscopic and open surgical procedures were performed by experienced surgeons without learning curve effects. According to the published retrospective research literature [11], the sample size was calculated based on two parameters: the hospitalization cost and the length of postoperative hospital stay. The results showed that 49 and 8 cases were needed, respectively. The larger sample size parameter 49 was selected, and after further expansion by 20% in the case of drop-out, 60 patients with hepatic hemangioma in each group were prospectively enrolled in this study and the final patient flow chart for the trial was shown in Fig. 1. As shown in Table 1, there were no statistically significant differences in baseline characteristics between the two groups. In Table 1, the proposal of difficulty of laparoscopic liver resection by Kawaguchi et al. was used to quantify the surgical difficulty grade of each patient [12], and the detailed classification criteria are described in Supplementary Table 1. Of the 120 patients, 101 patients finished the questionnaires and were available for final analysis of quality of life.
Intra- and postoperative conditions
A detailed comparison of the intraoperative parameters of the patients is shown in Supplementary Table 2. There were no differences among intraoperative bleeding and transfusion, while the laparoscopic group had a longer surgery time, occlusion time and occlusion frequency than the open group. Of the 60 cases of laparoscopic surgery, five patients were converted to open surgery, with a conversion rate of 8.3%.
The detailed postoperative results of the two groups are shown in Supplementary Table 3. In addition to some blood test indicators, a longer postoperative recovery time and postoperative hospital stay and a lower total cost were found in the open group.
As shown in Supplementary Tables 4 and 5, there were marked differences in the postoperative complications between these groups. There were significant differences between the two groups according to the Comprehensive Noticing Index, and correspondently, the classification of complications in the Clavien–Dindo surgery also showed significant differences between the two groups; the incidence of complications in the open group was higher than that in the laparoscopic group.
Quality of life
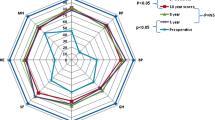
As shown in Fig. 2, the quality of life analysis results showed that there were significant differences in RP (P = 0.002), BP (P = 0.023) and RE (P = 0.001) scores between the open group and the laparoscopic group, and the scores of the laparoscopic groups were higher than those of the open groups. In addition, there were statistically significant changes in the scores of the eight domains at different time points (P < 0.001). Interaction effects of treatment × time were detected in RP (P = 0.001), VT (P = 0.009), RE (P = 0.003) and MH (P = 0.035).
Between-group analysis compared the effects of the two groups on quality of life at different time points, and within-group analysis compared the recovery rate on quality of life at different time points. Between-group analysis (Table 2) indicated that the RP and RE scores of the laparoscopic groups were higher than those of the open groups at 1 and 3 months after surgery, and the difference disappeared one year after surgery. Within-group comparison (Table 3) indicated that at 1 month after surgery, the MH score of the laparoscopic group increased, while the RP, VT, and RE scores of both groups decreased. 3 months after surgery, compared with the baseline, the MH score of the laparoscopic group increased, while the RP and RE scores of the open group were lower than those before surgery, and the difference was restored to baseline at 12 months after surgery.
Discussion
As a benign tumor, hepatic hemangioma generally is not recommended for surgical treatment. To ensure that the surgical indication was sufficient, we carefully screened and excluded a number of patients who might have had symptoms due to other diseases prior to this study. Common diseases include chronic gastritis, irritable bowel syndrome, and peptic ulcer.
Liver function injury
In this study, the laparoscopic group had a longer total operation and portal occlusion time, as well as more frequencies of hepatic portal occlusion. This might be related to the limited operation space and difficulty of laparoscopic operation. These results were consistent with the increase in ALT and AST in the laparoscopic group compared with the open group. The blood concentrations of these enzymes are sensitive markers of liver cell injury and inflammation [13]. Longer hepatic portal occlusion means a longer ischemia time, causing worse damage to liver cells, which is directly reflected by higher levels of ALT and AST [14]. At the same time, reperfusion of open blood flow after occlusion can also lead to ischemia reperfusion injury of liver cells, which can also be manifested as an increase in ALT and AST [15].
Postoperative complications
Laparoscopic surgery had certain advantages on complication incidence rate as well as severity of operative complications. Only three patients in the laparoscopic group suffered surgical complications, all of which were relatively mild Clavien–Dindo grade [16] I, II and IIIa, while a total of 15 patients had surgical complications in the open group.
There were cases of grade IIIb and grade IVa complications in the open group. The grade IIIb surgical complication was incisional hernia after surgery, which resulted in incisional hernia repair under general anesthesia. With a reported incidence of approximately 2–20%, incisional hernia is not rare for open surgery [17]. There are many risk factors for incisional hernia after hepatectomy, including age, nutritional status, and surgical procedure [18, 19]. Le Huu Nho compared the incidence of incisional hernia between open and laparoscopic surgery and found that the incidence of open surgery was significantly higher [20]. As we can imagine, open surgery is associated with a higher risk of incisional hernia due to its high level of trauma and damage to the abdominal wall.
The complication of IVa surgery was pulmonary embolism in the open group. In general, pulmonary embolism after liver surgery is not common because liver surgery has a negative impact on coagulation function, so it is not easy to form postoperative complications such as intravascular thrombosis [21]. However, studies have reported that in addition to common risk factors such as high BMI and major surgery, normal liver parenchyma surgery is also one of the risk factors for pulmonary embolism [22]. Recovery after open surgery is relatively long, while long-term immobilization may increase the risk of pulmonary embolism [23].
Quality of life
To date, most of the studies comparing the quality of life after laparoscopic and open surgery have focused on malignant diseases [24, 25]; however, quality of life might be affected by the differences in recurrence rates and mortality rates between the two prosedours. As a benign disease, hepatic hemangioma is regarded as a perfect background disease to study surgical modalities on quality of life.
In the between-group analysis, the laparoscopic group showed superiority in role-physical functioning, and role-emotional dimensions persisted to 3 months postoperatively at 1 month; however, at 12 months postoperatively, there was no statistically significant difference between the two groups, suggesting that the open group recovered to the same level as the laparoscopic group.
In the within-group comparison analysis, the laparoscopic group revealed advantages in recovery on quality of life. Three months after surgery, the role-physical functioning and role-emotional dimensions recovered to the preoperative level, while the open group did not. In addition, we found scores of the majority dimensions decreased significantly 1 month after surgery, indicating that both open and laparoscopic surgery had a great impact on the quality of life, suggesting that the surgical indication should be strictly evaluated. At 12 months postoperatively, similar to the between-group analysis, patients in both groups recovered to the same level as baseline, suggesting that the effects of the surgery on quality of life could be recovered one year after the surgery.
This study has the following limitations: (1) This study is a nonrandomized controlled trial, and the level of evidence is lower than that of a randomized controlled trial. (2) Although the sample size was calculated according to the formula, it was still small when analyzing postoperative complications, the conversion rate of laparoscopic surgery and other aspects. (3) Our research indicated that the quality of life for both groups could return to baseline 12 months after surgery; however, we missed this part of the data to determine whether they could recover in a shorter period of time, such as 6 months after surgery. (4) Our focus is not only on liver hemangioma disease itself, but also compare the impact of open and laparoscopic liver surgery on the quality of life, despite this conclusion has certain reference value for other diseases, but other disease types were not included in the study.
References
European Association for the Study of the Liver (2016) EASL Clinical Practice Guidelines on the management of benign liver tumours. J Hepatol 65:386–398
O’Rafferty C, O’Regan GM, Irvine AD, Smith OP (2015) Recent advances in the pathobiology and management of Kasabach-Merritt phenomenon. Br J Haematol 171:38–51
Bahirwani R, Reddy KR (2008) Review article: the evaluation of solitary liver masses. Aliment Pharmacol Ther 28:953–965
Schnelldorfer T, Ware AL, Smoot R, Schleck CD, Harmsen WS, Nagorney DM (2010) Management of giant hemangioma of the liver: resection versus observation. J Am Coll Surg 211:724–730
Farges O, Daradkeh S, Bismuth H (1995) Cavernous hemangiomas of the liver: are there any indications for resection? World J Surg 19:19–24
Zhang X, Yan L, Li B, Wen T, Wang W, Xu M, Wei Y, Yang J (2016) Comparison of laparoscopic radiofrequency ablation versus open resection in the treatment of symptomatic-enlarging hepatic hemangiomas: a prospective study. Surg Endosc 30:756–763
Shi Y, Song J, Ding M, Tang X, Wang Z, Chi J, Wang T, Ji J, Zhai B (2020) Microwave ablation versus transcatheter arterial embolization for large hepatic hemangiomas: clinical outcomes. Int J Hyperth 37:938–943
Xia F, Lau WY, Qian C, Wang S, Ma K, Bie P (2010) Surgical treatment of giant liver hemangiomas: enucleation with continuous occlusion of hepatic artery proper and intermittent Pringle maneuver. World J Surg 34:2162–2167
Ware JE (2000) SF-36 health survey update. Spine 25:3130–3139
Shein CC, Jun S, Hansheng W, Yuliya L (2018) Sample size calculations in clinical research, 3rd edn. Taylor & Francis Group, Boca Raton, p 48
Yu HB, Dong YD, Wang LC, Tian GJ, Mu SM, Cao Y, Peng YN, Lou CY, Liu P, Li DY (2015) Laparoscopic versus open resection for liver cavernous hemangioma: a single center of 2-year experience. Surg Laparosc Endosc Percutan Tech 25:e145-147
Kawaguchi Y, Fuks D, Kokudo N, Gayet B (2018) Difficulty of laparoscopic liver resection: proposal for a new classification. Ann Surg 267:13–17
Mpabanzi L, van Mierlo KM, Malago M, Dejong CH, Lytras D, Olde Damink SW (2013) Surrogate endpoints in liver surgery related trials: a systematic review of the literature. HPB (Oxford) 15:327–336
Li SQ, Liang LJ, Huang JF, Li Z (2004) Ischemic preconditioning protects liver from hepatectomy under hepatic inflow occlusion for hepatocellular carcinoma patients with cirrhosis. World J Gastroenterol 10:2580–2584
Heizmann O, Loehe F, Volk A, Schauer RJ (2008) Ischemic preconditioning improves postoperative outcome after liver resections: a randomized controlled study. Eur J Med Res 13:79–86
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibanes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien–Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Burger JW, Lange JF, Halm JA, Kleinrensink GJ, Jeekel H (2005) Incisional hernia: early complication of abdominal surgery. World J Surg 29:1608–1613
Hesselink VJ, Luijendijk RW, de Wilt JH, Heide R, Jeekel J (1993) An evaluation of risk factors in incisional hernia recurrence. Surg Gynecol Obstet 176:228–234
Dietz UA, Winkler MS, Hartel RW, Fleischhacker A, Wiegering A, Isbert C, Jurowich C, Heuschmann P, Germer CT (2014) Importance of recurrence rating, morphology, hernial gap size, and risk factors in ventral and incisional hernia classification. Hernia 18:19–30
Le Huu NR, Mege D, Ouaissi M, Sielezneff I, Sastre B (2012) Incidence and prevention of ventral incisional hernia. J Visc Surg 149:e3-14
De Pietri L, Montalti R, Begliomini B, Scaglioni G, Marconi G, Reggiani A, Di Benedetto F, Aiello S, Pasetto A, Rompianesi G, Gerunda GE (2010) Thromboelastographic changes in liver and pancreatic cancer surgery: hypercoagulability, hypocoagulability or normocoagulability? Eur J Anaesthesiol 27:608–616
Melloul E, Dondero F, Vilgrain V, Raptis DA, Paugam-Burtz C, Belghiti J (2012) Pulmonary embolism after elective liver resection: a prospective analysis of risk factors. J Hepatol 57:1268–1275
Anderson FA Jr, Spencer FA (2003) Risk factors for venous thromboembolism. Circulation 107:I9-16
Rees JR, Blazeby JM, Fayers P, Friend EA, Welsh FK, John TG, Rees M (2012) Patient-reported outcomes after hepatic resection of colorectal cancer metastases. J Clin Oncol 30:1364–1370
Fretland AA, Dagenborg VJ, Waaler Bjornelv GM, Aghayan DL, Kazaryan AM, Barkhatov L, Kristiansen R, Fagerland MW, Edwin B, Andersen MH (2019) Quality of life from a randomized trial of laparoscopic or open liver resection for colorectal liver metastases. Br J Surg 106:1372–1380
Funding
This work was supported by grants from the National Natural Science Foundation of China (Grant No. 71673193) and Key research and development project of science and technology department of Sichuan Province (Grant No. 2021YFS0106).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Dr. Lian Li, Liangliang Xu, Peng Wang, Fei Liu, Yonggang Wei, Mingqing Xu, Ming Zhang and Bo Li disclosed that this work was supported by noncommercial grants from the National Natural Science Foundation of China (Grant No. 71673193) and Key Research and Development Project of Science and Technology Department of Sichuan Province (Grant No. 2021YFS0106).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, L., Xu, L., Wang, P. et al. Advantages of laparoscopic hepatic hemangioma surgery in quality of life: a prospective study. Surg Endosc 36, 8967–8974 (2022). https://doi.org/10.1007/s00464-022-09348-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09348-x