Abstract
Purpose
Late postoperative complications in choledochal cyst (CC) patients are severe problems that affect the quality of life (QOL). We evaluated the postoperative complications and health-related QOL (HRQOL) of CC patients ≥ 18 years of age.
Methods
From April 1984 to January 2018, 114 CC patients underwent definitive surgery at our institution. Seventy-nine patients reached ≥ 18 years of age. The HRQOL was assessed using the Japanese version of the SF-36v2. Eight health domain (physical functioning, role-physical, body pain, general health, role-emotional, vitality, mental health, and social functioning) scores and three component summary [physical component summary, mental component summary (MCS), and role-social component summary] scores were compared between the patients with and without complications (C [+] vs. C [−]).
Results
Thirty-five patients answered the questionnaires. Twelve patients had postoperative complications. Among the eight domains, the score of general health was significantly lower in C [+] patients than in C [−] patients (p = 0.0488). Among the three component scores, the MCS score in C [+] patients was lower than in C [−] patients without significance (p = 0.0953).
Conclusions
The HRQOL of CC patients ≥ 18 years of age was mostly acceptable. However, postoperative complications can impair the sense of well-being and affect the mental health.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Choledochal cyst (CC) is a rare congenital anomaly involving cystic dilation of the biliary tree; the incidence is relatively high in Asia [1]. The current surgical strategy for CC is cyst excision and hepaticoenterostomy. Owing to this surgical procedure, CC is thought to be completely curable without complications in many cases. However, the rate of postoperative complications, such as intrahepatic bile duct stone or biliary carcinoma, is relatively constant. Intrahepatic bile duct stones are detected in approximately 10% of patients with late postoperative complications [2,3,4,5]. The malignant potential after surgical treatment is higher than the baseline population level [6]. Long-term surveillance for late complications, including malignancy, is therefore absolutely necessary [7, 8].
Another important concern in the long-term postoperative assessment of CC patients is the health-related quality of life (HRQOL). The HRQOL is a multi-dimensional concept that includes domains related to physical, mental, emotional, and social functioning. The HRQOL has become a major evaluation parameter and is useful in the planning of treatment for patients with chronic illness or morbidity. Many pediatric surgeries are functionalization procedures. Patients who undergo functionalization procedures might have varying degrees of chronic morbidity, even after a definitive operation. The current surgical strategy for CC has produced appreciable results. However, the postoperative outcome is not necessarily correlated with the HRQOL. The state of the HRQOL of postoperative CC patients remains uncertain. There are no reports discussing the HRQOL of CC patients. Pediatric surgeons must take care regarding not only the postoperative course but also the postoperative HRQOL.
Our recent clinical study showed that the long-term (> 20 years) follow-up rate of CC patients who underwent a definitive operation was very low (14.5%) [9]. However, data on the long-term outcomes and current status of postoperative CC patients are insufficient.
The aims of the present study were to evaluate the long-term postoperative course and current HRQOL status of CC patients ≥ 18 years of age and to clarify the relationship between postoperative complications and the HRQOL.
Methods
Study participants
The CC patients who underwent a definitive operation at our institution from April 1984 to January 2018 were enrolled in this study. Postoperative complications and the QOL were evaluated during clinical follow-up via a questionnaire survey. All patients provided their informed consent to participate in the present study.
The evaluation of the HRQOL
The HRQOL was assessed using the Japanese version of the SF-36v2 [10, 11]. The same questionnaire was sent by mail to patients ≥ 18 years of age. The SF-36v2 includes 36 questions that measure functional health and well-being from the patient’s point of view. It provides scores for each of eight health domains (physical functioning, role-physical, body pain, general health, role-emotional, vitality, mental health, and social functioning). Using the scores of these eight domains, the physical component summary (PCS), mental component summary (MCS), and role-social component summary (RCS) scores are calculated by a formula [10, 11]. A normalized base score of 50 represents the average QOL score of the Japanese general population. A score of 10 corresponds to the standard deviation. To evaluate the natural change in the HRQOL, the correlation between the HRQOL scores and patient age was also calculated.
Statistical analyses
The PCS, MCS, and RCS scores were presented as median values and range. Differences were assessed using the Mann–Whitney U test. The relationship between the HRQOL score and patient age was examined using Pearson’s product-moment correlation coefficient. p values of < 0.5 were considered to indicate statistical significance. All of the statistical analyses were performed using the EZR software program [12].
Ethical approval
This study was performed according to the Ethical Guidelines for Medical and Health Research Involving Human Subjects by the Ministry of Health, Labour and Welfare of Japan in 2014, complied with the 1964 Declaration of Helsinki (revised in 2013), and was approved by the local ethics committee of our institution (28-313).
Results
Background characteristics and postoperative complications of the patients
One hundred and fourteen CC patients underwent a definitive operation at our institution from April 1984 to January 2018. The median age at operation was 4 years and 3 months (range 12 days–17 years). Eleven (9.6%) patients underwent surgery at < 1 year of age, while 14 (12.3%) underwent surgery at > 18 years of age. All cases underwent cyst excision and hepaticoenterostomy. The last 4 surgeries were performed through a laparoscope and the remaining 110 were performed by opening the abdomen. Regarding the operative procedure, hepaticoduodenostomy was performed in 1 case (0.9%), and hepaticojejunostomy was performed in the remaining 113 (99.1%) cases. The median postoperative period was 24.5 years (range 5–32 years).
Seventy-nine (69.3%) patients reached ≥ 18 years of age. The median age was 29 years (range 18 to 44 years). The patient background characteristics and postoperative complications are shown in Table 1. Among the 79 patients ≥ 18 years of age, 35 (44.3%) answered the questionnaires. The study population included 12 male patients and 23 female patients. The median age was 29 years (range 18–42 years), and the median postoperative period was 24 years (range 5–31 years). Nineteen (54.3%) patients regularly attended follow-up appointments at our institution or other hospitals. The remaining 16 patients dropped out of follow-up.
Twelve (34.2%) patients had postoperative complications. The incidence of complications is shown in Table 1. The complications included adhesive ileus, n = 6 (17.1%); liver dysfunction, n = 3 (8.6%); cholangitis, n = 3 (8.6%); intrahepatic stone, n = 3 (8.6%) pancreatitis, n = 2 (5.7%); fatty liver, n = 2 (5.7%); and pancreatic stone, n = 1 (2.9%). No patients had liver cirrhosis or biliary carcinoma. Of the 12 patients who had postoperative complications, 6 underwent regular checkups.
The HRQOL outcomes
The distribution of the HRQOL component summary scores
Using the eight HRQOL domains, the PCS, MCS, and RCS scores were calculated. The score distribution is shown in Fig. 1. Two patients scored less than 30 (− 2 SD) in the physical (Fig. 1a) and role-social component summary (Fig. 1c); one patient scored less than 30 (− 2 SD) in the mental component summary (Fig. 1b). The HRQOL component summary scores were within the normal range in the majority of the patients.
A comparison of the eight health domain scores between patients with and without complications (C [+] and C [−] patients)
The eight health domain scores of C [+]/C [−] patients were compared to determine the effects of postoperative complications on the HRQOL as shown in Table 2. Among the eight domains, the score of general health was significantly lower in C [+] patients than in C [−] patients (p = 0.0488). Furthermore, the scores of role-physical, body pain, and vitality were lower in C [+] patients than in C [−] patients (p = 0.0602, p = 0.0699, and p = 0.0711, respectively).
A comparison of the HRQOL component summary scores between C [+]/C [−] patients
The HRQOL summary scores of C [+]/C [−] patients were compared as shown in Table 3. The median scores of C [+]/C [−] patients for the physical, mental, and role-social components were 53.9/56.2, 44.6/49.6, and 55.5/53.7, respectively. No significant differences were observed between the two groups (physical, mental, and role-social components: p = 0.348, p = 0.0953, p = 0.862, respectively).
The score distribution is shown in Fig. 2 (C [+] and C [−], separately). The scores of the C (−) patients showed an almost normal distribution. The role-social component of the C [+] group was similar to that of the C [−] group (Fig. 2c); however, the mental component of the C [+] group was lower than that of the C [−] group (Fig. 2b).
The correlation between the HRQOL scores and patient age in C [−] patients
The correlation between HRQOL scores and patient age in the C [−] patients was assessed to clarify the association between the HRQOL and advancing age. The purpose of this analysis was to determine the adequacy of following C [−] patients for a long time from the aspect of the HRQOL.
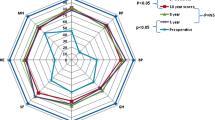
Among the eight domain scores, body pain, general health, and social functioning showed significant negative correlations with age (Pearson’s product-moment correlation coefficient: r = − 0.423, p = 0.0446; r = − 0.481, p = 0.0202; and r = − 0.595, p = 0.00277, respectively) (Fig. 3). With respect to component summary scores, the PCS score showed a significant negative correlation with age (Pearson’s product-moment correlation coefficient, r = − 0.421, p = 0.0452) (Fig. 4a). The MCS and RCS scores did not show a significant correlation with patient age (r = − 0.193, p = 0.378 and r = 0. 0565, p = 0.798) (Fig. 4b, c).
The correlation between the eight HRQOL domain scores and the age of C [−] patients. Among the eight domain scores, body pain, general health, and social functioning showed significant negative correlations with age (Pearson’s product-moment correlation coefficient, r = − 0.423, p = 0.0446, r = − 0.481, p = 0.0202; and r = − 0.595, p = 0.00277, respectively)
The correlation between the HRQOL summary scores and the age of C [−] patients. The PCS score showed a significant negative correlation with age (Pearson’s product-moment correlation coefficient, r = − 0.421, p = 0.0452) (a). The MCS and RCS scores did not show a significant correlation with patient age (r = − 0.193, p = 0.378 and r = 0.0565, p = 0.798, respectively) (b, c)
Discussion
In the present study, we clarified the long-term postoperative course and current status of the HRQOL in CC patients ≥ 18 years of age. The major findings of this study were as follows: (1) among the 35 CC patients ≥ 18 years of age who responded to this survey, 12 (34.2%) patients had postoperative complications of adhesive ileus, n = 6 (17.1%); liver dysfunction, cholangitis, n = 3 (8.6%); intrahepatic stone, n = 3 (8.6%); pancreatitis, n = 2 (5.7%); fatty liver, n = 2 (5.7%); and pancreatic stone, n = 1 (2.9%). (2) No patients developed postoperative liver cirrhosis or biliary carcinoma. (3) The score of general health was significantly lower in C [+] patients than in C [−] patients (p = 0.0488) (4) The MCS of the C [+] group was lower than that of the C [−] group (p = 0.0953). (5) Among domain scores, body pain, general health, and social functioning showed significant negative correlations with age in patients without complications (r = − 0.423, p = 0.0446; r = − 0.481, p = 0.0202; and r = − 0.595, p = 0.00277, respectively). (6) The PCS score showed a significant negative correlation with age (r = − 0.421, p = 0.0452) in patients without complications.
The most important finding of this study was that CC patients ≥ 18 years of age showed an acceptable HRQOL. The HRQOL component summary scores were within the normal range in the majority of patients, and the scores of the C [−] patients showed an almost normal distribution. The mental component of the HRQOL may be impaired after CC patients develop complications. Therefore, a mental/emotional assessment and mental healthcare should be performed for CC patients with complications.
Regarding the postoperative complications, a high incidence (34.2%) of complications requiring treatment was recognized. There were some cases in which biliary complications developed contrary to expectations. Fortunately, there were no cases of postoperative biliary carcinoma in this study. However, the incidence of biliary carcinoma after cyst excision is reported to be 0.7–5.4% [18, 19]. Postoperative biliary carcinoma is often related to pre-existing cholangitis or intrahepatic stone. Among the 79 CC patients ≥ 18 years of age to whom we mailed the questionnaire, 44 (55.7%) patients did not respond. Twenty-six of the surveys’ questionnaires that were sent to the 44 non-responders were returned, because they were no longer living at their original address. Thus, it is possible that there were more biliary complications, such as cholangitis and intrahepatic stone, among the patients who were lost to follow-up. To detect and treat complications before they become severe, the transition of follow-up from pediatric care to adult care—for example, regular visits to a gastroenterology clinic—is desirable [9].
In addition to late physical complications, the mental and emotional condition of CC patients are important for their postoperative QOL. We previously clarified the bowel function and QOL of Hirschsprung’s disease patients [13]. That study revealed the importance of assessing the emotional component of the postoperative QOL. We therefore used the SF-36v2 to assess the HRQOL in the present study. The SF-36v2 is composed of physical, mental, and role-social components.
Although the eight health domains of SF-36v2 are subscales, their analysis and evaluation are important. In our study, the general health score was significantly lower in C [+] patients than in C [−] patients. According to the definition, a high score of general health indicates excellent personal health and vice versa. It is reflected not only by specific health problems but also one’s personal feelings concerning their health. The CC patients with complications may always feel that they are vaguely unhealthy, which can affect the sense of well-being negatively. Self-rated health has recently received substantial attention as a notion of the QOL. Heistaro et al. revealed that a poor self-rated health was a strong predictor of mortality in random samples of working-age people [14]. Several other studies supported the same relationship between self-rated health and mortality [15, 16]. Pediatric surgeons should therefore make an effort to reduce the postoperative complications to decrease the mortality in CC patients by maintaining their subjective health.
The distribution of the HRQOL component summary scores appeared to be similar to that in the Japanese general population. However, two patients scored less than 30 (-2 standard deviations [SD]) in the PCS and RCS, and one patient scored less than 30 (-2 SD) in the MCS. All patients who scored less than 30 (-2 SD) experienced postoperative complications. The MCS was relatively low in C [+] patients; however, the difference was not statistically significant. Among C [+] patients, consultation with a mental health professional should be considered even when they do not show emotional or mental problems. Mental or emotional support involves more than consulting with a professional. Versteegh et al. [17] suggested that active psychological support for parents and other family members during the child’s treatment may represent a major point of intervention for improving the patient’s long-term QOL. Maternal anxiety is a risk factor for behavioral and emotional problems after surgery [18]. We should make efforts to help not only patients but also their parents and families come to terms with their illness and educate them on how to adjust and coexist with their symptoms. The transition from pediatric care to adult services is another causative factor of mental health issues. The transition should never occur before patients have achieved some understanding of their disease and have begun to manage their condition independently of their parental figures [19].
There is no consensus regarding the ideal follow-up strategy for C [−] CC patients. To reach a consensus from the aspect of the HRQOL, the correlation between the HRQOL scores and patient age in C [−] patients was assessed in this study. Among domain scores, body pain, general health, and social functioning showed significant negative correlations with age. With respect to component summary scores, the PCS score showed a significant negative correlation with age, while no such relationship was noted for the MCS or RCS. Regarding reductions in these scores, it is not clear whether this was an effect of physiological aging or whether it occurred due to the influence of CC. If scores are found to decrease as a postoperative consequence of CC, we should follow-up C [−] CC patients for a long time. We should continue our surveillance to accumulate more data from patients without complications.
The assessment of the HRQOL is important not only for CC but also for patients with other pediatric surgical diseases, such as anorectal malformation, including cloacal anomaly, Hirschsprung’s disease, and gastroesophageal reflux disease. Large-scale surveillance of pediatric surgical disease inevitably takes the form of a multicenter study. By performing a multicenter study, the HRQOL measurement could thus become the standard evaluation tool of the postoperative QOL for pediatric patients who have undergone this operation in childhood.
The present study is associated with several limitations. The low collection rate (44.3%) undermines the efficacy of the study. The inhomogeneous characteristics of the C [+] group are also a problem. The complications were varied, and their severity differed, which affects the results of the comparison of HRQOL scores between the C [+] and C [−] groups. Regarding the instrument used to measure the HRQOL, we adopted the SF-36v2. Although this instrument is widely used in the assessment of surgical patients [20], it was not developed with surgical patients in mind. An instrument that can assess the HRQOL of surgical patients should be used simultaneously. Our HRQOL data were not comparison data, as the HRQOL was only measured once in each case. Regarding the correlation between the HRQOL scores and patient age in C [−] patients, we were unable to compare our findings with those of the normal healthy population.
We were also unable to evaluate the extent to which the postoperative condition affected the HRQOL scores. Of note, one patient without complications of CC was being treated for depression.
Conclusion
We evaluated the postoperative complications and QOL of CC patients ≥ 18 years of age. No patients developed liver cirrhosis or biliary carcinoma. The HRQOL of CC patients ≥ 18 years was mostly acceptable. Patients without complications have an almost normal HRQOL. Because postoperative complication might impair the sense of well-being and affect the mental health, we should practice care with C [+] patients, including assessing the HRQOL and providing mental care.
References
Lipsett PA, Pitt HA (2003) Surgical treatment of choledochal cysts. J Hepatobiliary Pancreat Surg 10:352–359. https://doi.org/10.1007/s00534-002-0797-4
Todani T, Watanabe Y, Urushihara N, Noda T, Morotomi Y (1995) Biliary complications after excisional procedure for choledochal cyst. J Pediatr Surg 30:478–481
Chijiiwa K, Tanaka M (1994) Late complications after excisional operation in patients with choledochal cyst. J Am Coll Surg 179:139–144
Saing H, Han H, Chan KL, Lam W, Chan FL, Cheng W, Tam PK (1997) Early and late results of excision of choledochal cysts. J Pediatr Surg 32:1563–1566
Tsuchida Y, Takahashi A, Suzuki N, Kuroiwa M, Murai H, Toki F, Kawarasaki H, Hashizume K, Honna T (2002) Development of intrahepatic biliary stones after excision of choledochal cysts. J Pediatr Surg 37:165–167
Ohashi T, Wakai T, Kubota M, Matsuda Y, Arai Y, Ohyama T, Nakaya K, Okuyama N, Sakata J, Shirai Y, Ajioka Y (2013) Risk of subsequent biliary malignancy in patients undergoing cyst excision for congenital choledochal cysts. J Gastroenterol Hepatol 28:243–247. https://doi.org/10.1111/j.1440-1746.2012.07260.x
Ono S, Fumino S, Shimadera S, Iwai N (2010) Long-term outcomes after hepaticojejunostomy for choledochal cyst: a 10- to 27-year follow-up. J Pediatr Surg 45:376–378. https://doi.org/10.1016/j.jpedsurg.2009.10.078
Soares KC, Kim Y, Spolverato G, Maithel S, Bauer TW, Marques H, Sobral M, Knoblich M, Tran T, Aldrighetti L, Jabbour N, Poultsides GA, Gamblin TC, Pawlik TM (2015) Presentation and clinical outcomes of choledochal cysts in children and adults: a multi-institutional analysis. JAMA Surg 150:577–584. https://doi.org/10.1001/jamasurg.2015.0226
Mukai M, Kaji T, Masuya R, Yamada K, Sugita K, Moriguchi T, Onishi S, Yamada W, Kawano T, Machigashira S, Nakame K, Takamatsu H, Ieiri S (2018) The long-term postoperative outcomes of choledochal cysts, focusing on the follow-up rate and late complications at a single institution. Surg Today 48:835–840
Fukuhara S, Bito S, Green J, Hsiao A, Kurokawa K (1998) Translation, adaptation, and validation of the SF-36 Health Survey for use in Japan. J Clin Epidemiol 51:1037–1044
Fukuhara S, Ware JE Jr, Kosinski M, Wada S, Gandek B (1998) Psychometric and clinical tests of validity of the Japanese SF-36 Health Survey. J Clin Epidemiol 51:1045–1053
Kanda Y (2013) Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant 48:452–458. https://doi.org/10.1038/bmt.2012.244
Onishi S, Nakame K, Kaji T, Kawano M, Moriguchi T, Sugita K, Yano K, Nomura M, Yamada K, Yamada W, Masuya R, Kawano T, Machigashira S, Mukai M, Ieiri S (2017) The bowel function and quality of life of Hirschsprung disease patients who have reached 18 years of age or older—the long-term outcomes after undergoing the transabdominal soave procedure. J Pediatr Surg 52:2001–2005. https://doi.org/10.1016/j.jpedsurg.2017.08.036
Heistaro S, Jousilahti P, Lahelma E, Vartiainen E, Puska P (2001) Self rated health and mortality: a long term prospective study in eastern Finland. J Epidemiol Community Health 55:227–232
Kaplan GA, Camacho T (1983) Perceived health and mortality: a nine-year follow-up of the human population laboratory cohort. Am J Epidemiol 117:292–304
Okamoto K, Tanaka Y (2004) Subjective usefulness and 6-year mortality risks among elderly persons in Japan. J Gerontol B Psychol Sci Soc Sci 59:246–249
Versteegh HP, van Rooij IA, Levitt MA, Sloots CE, Wijnen RM, de Blaauw I (2013) Long-term follow-up of functional outcome in patients with a cloacal malformation: a systematic review. J Pediatr Surg 48:2343–2350. https://doi.org/10.1016/j.jpedsurg.2013.08.027
Guan G, Liu H, Wang Y, Han B, Jin Y (2014) Behavioural and emotional outcomes in school-aged children after surgery or transcatheter closure treatment for ventricular septal defect. Cardiol Young 24:910–917. https://doi.org/10.1017/s104795111300142x
Bell LE, Bartosh SM, Davis CL, Dobbels F, Al-Uzri A, Lotstein D, Reiss J, Dharnidharka VR (2008) Adolescent transition to adult care in solid organ transplantation: a consensus conference report. Am J Transplant 8:2230–2242. https://doi.org/10.1111/j.1600-6143.2008.02415.x
Clermonts S, van Loon YT, Wasowicz DK, Langenhoff BS, Zimmerman DDE (2018) Comparative quality of life in patients following transanal minimally invasive surgery and healthy control subjects. J Gastrointest Surg. https://doi.org/10.1007/s11605-018-3718-9
Acknowledgements
We thank Mr. Brian Quinn for his comments and help with the manuscript. This study was supported by a Grant-in-Aid for Scientific Research from the Japan Society for the Promotion of Science (JSPS, nos. 26670765, 16K10466, 16K10094, 16K10095, 16K10434, 16H07090, 17K10555, 17K11514, 17K10183, 17K11515), a Research Grant from the President’s Discretionary Expenses of our University, a Research Grant from The UBE Foundation, a Research Grant from Kawano Masanori Memorial Public Interest Incorporated Foundation for Promotion of Pediatrics, Research Grant from Tateishi Science and Technology Foundation, a Research Grant from Mitsui Life Social Welfare Foundation, and a Research Grant from The Kurata Grants of the Hitachi Global Foundation. Sponsor of Manuscript Submission: Atsuyuki Yamataka, M.D., Ph.D., F.A.A.P. (Hon), Department of Pediatric Surgery, Juntendo University, Tokyo, Japan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest in association with the present study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Baba, T., Mukai, M., Masuya, R. et al. The long-term health-related quality of life in patients operated for choledochal cyst. Pediatr Surg Int 35, 539–546 (2019). https://doi.org/10.1007/s00383-019-04456-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-019-04456-7