Abstract
Background
There is very scant literature on the impact of inguinal hernia mesh repair on testicular functions and sexual functions following open and laparoscopic repair. The present randomized study compares TAPP and TEP repairs in terms of testicular functions, sexual functions, quality of life and chronic groin pain.
Methods
This study was conducted from April 2012 to October 2014. A total of 160 patients with uncomplicated groin hernia were randomized to either trans-abdominal pre-peritoneal (TAPP) repair or totally extra-peritoneal (TEP) repair. Testicular functions were assessed by measuring testicular volume, testicular hormone levels preoperatively and at 3 months postoperatively. Sexual functions were assessed using BMSFI, and quality of life was assessed using WHO-QOL BREF scale preoperatively and at 3 and 6 months postoperatively. Chronic groin pain was evaluated using the VAS scale at 3 months, 6 months and at 1 year.
Results
The median duration of follow-up was 13 months (range 6–18 months). The mean preoperative pain scores (p value 0.35) as well as the chronic groin pain were similar between TEP and TAPP repairs at 3 months (p value 0.06) and 6 months (p value 0.86). The testicular resistive index and testicular volume did not show any significant change at follow-up of 3 months (p value 0.9) in the study population. No significant difference was observed in testicular resistive index and testicular volume when comparing TEP and TAPP groups at at follow-up of 3 months (p value >0.05). There was a statistically significant improvement in the sexual drive score, erectile function and overall satisfaction over the follow-up period following laparoscopic inguinal hernia repair. However, sexual function improvement was similar in patients undergoing both TEP and TAPP repairs. All the domains of quality of life in the study population showed a significant improvement at a follow-up of 3 and 6 months. Subgroup analysis of all the domains of quality of life in both TAPP and TEP groups showed a similar increment as in the study population (p value <0.001); however, the mean scores of all the domains were comparable between the two subgroups (p value >0.05), preoperatively and 3 and 6 months follow-up.
Conclusions
Laparoscopic groin hernia repair improves the testicular functions, sexual functions and quality of life, but TEP and TAPP repairs are comparable in terms of these long-term outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Inguinal hernia repair is the most common general surgical operation performed worldwide. Laparoscopic repair has become standard of care for patients with inguinal hernia [1]. Recurrence rate was a major outcome measure in majority of the studies in the past, but with standardization of surgical technique the recurrence rate has come down significantly [2]. The focus of research now has shifted to other adverse outcomes like chronic groin pain, sexual dysfunction, alteration in testicular functions and quality of life. Although animal studies have suggested a strong correlation between mesh repairs for inguinal hernia and structural damage to elements of the spermatic cord and testicle [3, 4], but this has not been studied extensively clinically and very few studies have reported infertility or testicular atrophy after inguinal hernia repair [5, 6]. Few studies have shown that testicular perfusion is impaired preoperatively on affected (hernia) side by elevated resistive index on Doppler [7]. But there is limited literature comparing testicular functions in open and laparoscopic repair and TEP and TAPP repairs [8–10]. The testicular volume with resistive index and analysis of the serum levels of follicle-stimulating hormone (FSH), luteinizing hormones (LH) and testosterone indicate testicular function and help in assessing testicular functions in patients undergoing groin hernia repair [7, 9, 11, 12] and have been used as markers to assess the testicular functions postoperatively after inguinal hernia repair.
Patients with inguinal hernia are known to have some impairment of sexual functions. Post-herniorrhaphy inguinal or genital pain during ejaculation occurs in a small percentage of men [13, 14]. The incidence is probably underestimated because of the reluctance of patients to discuss their sexual problems. Erectile dysfunction is another complication which men occasionally report after inguinal hernia repair, but the exact incidence is unknown. Few studies have also reported improvement in the sexual function following inguinal hernia repair [14]. The testicular functions and sexual functions following inguinal hernia repair have not been studied well. There is no literature comparing TEP and TAPP repairs in terms of sexual functions and testicular functions. This prospective randomized study compares chronic groin pain, testicular functions, sexual functions and quality of life in patients undergoing TAPP repair or TEP repair.
Materials and methods
This prospective randomized study was conducted in a single surgical unit of a tertiary care hospital. All the adult patients in the age group between 18 and 60 years with primary, uncomplicated, unilateral/bilateral inguinal hernia were included in the study. Female patients, patients with history of previous surgery in the inguino-scrotal region, recurrent inguinal hernia, complicated hernia (irreducible, obstructed, strangulated), history of orchiectomy, patients with significant co-morbidities like coronary artery disease, uncontrolled hypertension and diabetes mellitus, chronic bronchitis, renal and hepatic failure, patients unfit for general anesthesia (ASA 3 or 4), and patients with uncontrolled coagulopathy and patients not giving consent were excluded from the study. The study was registered in Clinical Trial Registry of India (CTRI 2015/07/009469), and Institute Ethics Committee clearance was obtained. The study was conducted as per the CONSORT guidelines
The sample size calculation was based on equivalence trial to see overall effect on sexual functions following laparoscopic inguinal hernia repair by TEP and TAPP. With proportion of effect on sexual function following TEP of 9 and 15 % in TAPP [2, 4], with alpha as 5 %, power 80 % and equivalence margin 20 %, a sample size of 132 was calculated with 66 patients in each group.
Randomization was done using computer-generated random numbers with sealed opaque envelopes to ensure concealed allocation with block randomization. The patients were randomized into two groups: Group I—trans-abdominal pre-peritoneal repair (TAPP) and Group II—totally extra-peritoneal repair (TEP). An informed consent was obtained for both the procedures before randomization, and those not giving consent were excluded but not denied treatment.
Demographic profile, preoperative data including clinical profile, hernia characteristics were recorded in a pre-structured proforma. Patients underwent either TEP repair or TAPP repair as per the standard procedure that has been described in our previous publication [15]. Chronic groin pain was defined as per the International Association for the Study of Pain (IASP) [16] and was assessed at 3 and 6 months follow-up. All patients were given the quality of life assessment proforma (WHO-QOL BREF) in Hindi or English after admission to hospital and then at 3 and 6 months follow-up, and findings were compared. Sexual functions were assessed preoperatively at admission and at 3 and 6 months follow-up using the Brief Male Sexual Function Inventory (BMSFI) which included parameters such as sexual drive, erection, ejaculation and overall satisfaction in sexual life.
The testicular function and volume were assessed preoperatively in all patients and at 3 and 6 months to look for any change. Testicular function assessment was done by measurement of testicular volume and blood flow by Doppler ultrasound and testicular hormonal markers. The dimensions of the testis in length (L), width (W) and height (H) were measured by gray-scale examination. The volume (V) of the testis was calculated as a rotational ellipsoid: V = L × W × H × 0.526. Blood flow was assessed by Color Doppler ultrasonography (CDUS). CDUS of the testes was performed on all patients the day before operation and repeated 3 and 6 months after operation. The scrotum was examined with a linear (5-MHz) transducer. Color Doppler settings were optimized to detect slow flow; the highest color gain setting allowing an acceptable signal-to-noise ratio, the lowest wall filter and the lowest velocity scale. Ultrasound of the scrotum was performed in the supine position, and the patient was asked to hold the penis supra-publically. Blood flow parameters of the testicular artery were evaluated and noted and resistive index calculated (RI).
Testicular hormonal markers, follicle-stimulating hormone (FSH), luteinizing hormone (LH) and Testosterone were measured preoperatively and postoperatively at 3 and 6 months by using commercially available diagnostic kits. All data were prospectively entered into a pre-structured proforma. In case the patients were unable to attend the follow-up clinic, the proformas were completed by telephonic conversation
Statistical analysis
Data were analyzed by SPSS 2.0 and presented in frequency (percentage), mean (SD)/median (minimum–maximum) as applicable. Continuous variables between the groups were compared using independent t test (for data following normal distribution) and Wilcoxon rank-sum test(for data following non-normal distribution). Change within the continuous variable was seen by paired t test/repeated measures ANOVA (for data following normal distribution) and Friedman test (for data following non-normal distribution). In case of Friedman test, multiple comparison was done by using Wilcoxon signed-rank test with Bonferroni correction. Categorical variables were compared by using Chi-square/Fischer’s exact test. p value <0.05 is considered statistically significant.
Results
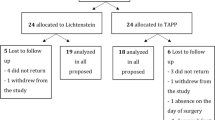
A total of 262 patients with inguinal hernia were operated between April 2012 and October 2014. A total of 102 patients were excluded as they either did not meet the inclusion criteria (96, 35.9 %) or did not give consent (6, 2.2 %) (Fig. 1, CONSORT diagram). A total of 160 patients were randomized into two groups (Group I—TAPP and Group II—TEP) with 80 patients in each group and analyzed.
Patients in both the groups were comparable in terms of demographic profile, clinical profile, hernia characteristics and intra operative variables (Table 1). Early postoperative pain scores were higher in TAPP group as compared to TEP group (Table 2). A total of 147 patients (91.9 %) completed 3 months follow-up, and 142 (88.7 %) patients completed 6 months follow-up.
Chronic groin pain was assessed at 3 and 6 months. The mean pain score at 3 months was still higher in TAPP group, but this difference was not statistically significant (1.7 ± 1 vs 1.4 ± 0.7, p value 0.06). However, at 6 months follow-up, the mean pain score was comparable between both the groups (0.87 ± 0.6 vs 0.86 ± 0.7, p value 0.86). Thus, both the groups were comparable in terms of chronic groin pain (Table 2).
No change in testicular volume and resistive index was observed at 3 and 6 months follow-up in the study population (p value 0.9 and 0.9, respectively) and between TEP and TAPP repairs (p value 0.79 and 0.72, respectively) (Table 3).
The mean preoperative serum FSH level was (3.5 ± 0.9). There was a slight increase in the serum FSH levels in the study population at 3 months (3.5 ± 1) and at 6 months (3.5 ± 0.8); however, this change was not statistically significant (p value 0.5). On subgroup analysis, there was no statistically significant change in the serum FSH levels both in TAPP and TEP groups when compared to preoperative mean levels (p value >0.05). Similar results were obtained in terms of serum LH and testosterone levels in both the groups, and both the groups were comparable at follow-up of 3 and 6 months (Table 4).
The study population showed a significant improvement in sexual function score from preoperative overall score of 24.8 ± 3 to a score of 27.2 ± 3.4 at the 3 months (p value <0.001) and 29.3 ± 3.4 at 6 months (p value <0.001) in the study population. All BMSFI domains also had statistically significant improvement after surgery. Although there was improvement in the ejaculation score at 3 months, this was not statistically significant (p value 0.10), but the score showed a significant improvement at 6 months (p value <0.001). Comparing sexual functions between TAPP and TEP groups, there was no statistically significant difference preoperatively and at 3 and 6 months follow-up (p value >0.05) (Table 5).
All quality of life domains in the study population showed a significant improvement at a follow-up of 3 and 6 months. Similar change was also seen in how the patients perceived their overall quality of life and overall health satisfaction. Analysis of each domain (viz., physical, psychological, social and environmental) showed a uniform improvement at 3 and 6 months follow-up. Subgroup analysis of all the domains of quality of life in both TAPP and TEP groups showed a similar increment as in the study population (p value <0.001); however, the mean scores of all the domains were comparable between the two subgroups (p value >0.05), preoperatively and 3 and 6 months follow-up (Fig. 2).
Discussion
The impact of inguinal hernia and mesh repair on testicular functions, sexual functions and quality of life has not been very well studied. There has been an ongoing debate of the impact of groin hernia and its repair on testicular functions and sexual functions.
Testicular dysfunction can be in the form of testicular atrophy or increase in the resistive index. Although testicular atrophy following hernioplasty has been reported occasionally with an incidence of 0.5 % for primary hernia repair [17].
The etiology of testicular atrophy has been studied in various animal studies. It has been shown that [18] direct tissue contact of ductus deferens with the mesh leads to formation of reactive induration, but the quality and quantity of the semen were not affected. A significant occlusion of vas with significant elevation of testicular temperature after Lichtenstein’s repair has also been observed. Peiper et al. [19] observed foreign body reaction on the ductus deferens with reduction in the testicular arterial perfusion and thrombosis of spermatic veins with subsequent reduction in the spermatogenesis when comparing the testicular parameters on the operated side with Lichtenstein and Shouldice repair in pigs and rabbits.
There are few studies comparing the open and the laparoscopic repair in terms of testicular functions, but no studies have been reported comparing TAPP and TEP repairs. These studies are small pilot studies with vague protocols [9, 10, 14, 15]. The exact etiology of testicular dysfunction after hernia repair is unknown. It might be because of the handling of testicular vessels and cord structures during dissection in open mesh repair. Akbulut et al. [20] in their study found that patients undergoing TEP repair had significant decrease in testicular volume as compared to open mesh repair. However, the testicular volume was within normal limits, but they did not study the testicular blood flow. They also reported testicular atrophy as a rare complication, but the number of cases (13 in each group) was a major limitation of their study.
Ersin et al. [21] reported no statistically significant difference in Doppler flow parameters preoperatively, very early (Day 1) and early postoperatively (Day 7). But differences in Doppler flow parameters of testicular artery compared to open group were found statistically significant between preoperatively and very early postoperatively. The major drawback of this study was that the testicular blood flow was assessed in the immediate postoperative period which is not appropriate as hypervascularity and edema of testes and epididymis are known to cause decrease in blood flow at this time. In our previous study [22] comparing the open and laparoscopic repair, we have shown that there was a significant impairment of testicular functions following open mesh repair as compared to laparoscopic inguinal hernia repair in terms of significant decrease in testicular volume, lesser improvement in resistive index with significant decrease in testosterone and significant increase in both LH and FSH levels. However, there was no clinically apparent testicular atrophy in any patient in our study of 117 patients.
Štula et al. [23] comparing TAPP and open repair observed a significant increase in the anti-sperm antibody (ASA) and the mean intra-testicular vessels and capsular vessels RI at 3 months, but this change was statistically insignificant after 6 months of surgery. Moreover, the increase in RI was not observed in the testicular vessels thereby ruling out the role of mesh and its incorporation with the surrounding tissue with the vascular impedance. The increase in the ASA and RI was within the normal physiological range. However, this change in the testicular parameters was significantly higher in the open repair when compared with TAPP repair. They concluded that the transient increase in the RI and ASA in the early postoperative period was due to the tissue and vessel handling during surgery and subsequent inflammation and transient breach in the blood testes barrier. However, the reliability of these studies is doubtful. In a few studies, only testicular volume [20] or blood flow was assessed and in others only hormone markers or semen analysis [23] or anti-sperm antibody or only clinical examination was done. Moreover, timing of assessment of testicular blood flow was also variable and inappropriate [21].
In the present study, we found that there was an overall improvement in the testicular functions in terms of testicular volume and resistive index although not statistically significant and this change was comparable between TEP and TAPP groups. Moreover, there was no deterioration in the hormonal levels following laparoscopic inguinal hernia repair and the outcomes were similar in both TEP and TAPP repairs. This improvement can be attributed to the fact there is minimal handling of tissue in laparoscopic repair and lesser fibrotic response contrary to the conventional beliefs. Another important observation which has come out from this study is that inguinal hernia repair in general leads to decrease in the vascular impedance of testes and improvement in the testicular vascularity. This implies that the presence of inguinal hernia in itself is associated with some impairment in testicular blood flow which actually improves after laparoscopic repair.
Sexual function is an important concern for any patient undergoing inguinal hernia repair. Impairment of sexual activity is a known complaint in patients with inguinal hernia. Post-herniorrhaphy inguinal, genital or ejaculatory pain occurs in a small percentage of men. The incidence is probably underestimated because of the reluctance of patients to discuss their sexual functions. The etiology is not completely understood. Erectile dysfunction is another complication which is occasionally reported after inguinal hernia repair, but its relationship with hernia repair makes little anatomical sense. In a Danish study [24] comprising of men undergoing a laparoscopic inguinal hernia repair who were registered in the Danish hernia database, dysejaculation occurred in 0.1 %, some pain in the groin or genitals was reported during sexual activity in 10.9 and 2.4 % had impaired sexual activity which was moderate to severe in nature. Studies have also reported improvement in the sexual function following inguinal hernia repair [14]. But the majority of these studies were non-randomized with vague protocols and inconsistent results.
In our study, we assessed the sexual functions using the Brief Male Sexual Function Inventory (BMSFI). We observed that there was an overall improvement in the sexual functions following laparoscopic inguinal hernia repair. There was a significant improvement in all the domains of sexual function which was more prominent in the sexual drive and the overall satisfaction in the sexual activity. This was attributed to the reduction in the pain and heaviness in the groin. However, TEP and TAPP repairs were comparable in the terms of their effect and outcome on sexual functions. We also studied the effect of unilateral and bilateral hernia on the sexual functions. The improvement in the sexual functions was comparable in patients with both the unilateral and bilateral inguinal hernia. However, the magnitude of improvement in patients with bilateral inguinal hernia was higher than patients with unilateral hernia. The findings from our study suggest that laparoscopic hernia repair actually improves the sexual functions in patients with inguinal hernia.
Quality of life (QOL) of patients has become the central evaluation parameter for the success of any treatment modality. Impairment of quality of life is a major reason for patients seeking surgical care. Often, inguinal hernia surgery is being performed on day care basis. Therefore, there are high expectations to resume normal activities and to return to work by both the patients and the society. Patients after inguinal hernia surgery want to join their duties at the earliest in an accepted state of health. There are very few studies in the literature reporting on quality of life after inguinal hernia repair. WHO-QOL BREF scale can be used cross-culturally and is a validated scale for Indian population which has been used in the literature to study quality of life outcomes in patients undergoing groin hernia repair. McCormack et al. [25] reviewed the literature in 2005 and reported that TAPP and TEP repairs provide better outcomes in terms of quality-adjusted life years than open repair. Recently, Myers et al. [4] also observed a significant improvement in all quality of life outcome measures following TEP repair except social functioning and mental health. Overall differences in physical and mental quality of life measures were significantly improved in the TEP group. In our previous randomized study with 314 patients randomized to TEP repair or TAPP repair [26], we have shown a significant improvement in the quality of life postoperatively using Short Form-36 version 2 questionnaire. In this study also we found significant improvement in all the aspects of the quality of life after laparoscopic inguinal hernia repair. This was more likely due to the disease-free state and the lower pain score perceived by the patients and subsequent return to normal daily activities. This change in the health status and quality of life of the patients was similar to the patients undergoing both TAPP and TEP repairs.
Laparoscopic repair of inguinal hernia offers the advantages of decreased postoperative pain, early ambulation and return to normal activities. Chronic groin pain has been considered a significant morbidity after inguinal hernia repair. It has been attributed to factors such as type of mesh, type of mesh fixation, preoperative pain, age, repair of recurrent hernia. The incidence of chronic groin pain after laparoscopic repair varies from 1 to 16 % [22]. In the present study, an internationally accepted standard definition of ‘pain persisting beyond the normal tissue healing time assumed to be 3 months’ was used [16]. The VAS has been studied and is often considered an ideal scale, because it is continuous, approximates a ratio scale, and is more independent from language than verbal scales.
In previous randomized studies [15, 22, 26], we have reported comparable outcomes between TAPP and TEP repairs in terms of chronic groin pain. In a meta-analysis, Bracale et al. [27] also reported similar incidence of chronic groin pain after both TAPP and TEP repairs. In the present study, the overall incidence of chronic groin pain was similar to that of the literature [13]. Although acute pain was higher in the TAPP group, but both the groups were comparable in terms of chronic groin pain which may be explained by the fact the peritoneal incision heals over a period of time and no longer adds to the pain score.
There are very few studies which have looked at the natural course of chronic groin pain after inguinal hernia repair. Poobalan et al. [28] described three chronic pain syndromes after herniorrhaphy; somatic, neuropathic and visceral pain. Cunningham et al. [29] reported the most common type of chronic post-herniorrhaphy syndrome is somatic. Our findings were also similar to that of the literature with most of the patients having somatic pain varying from dull aching to sharp pain.
In conclusion, patients undergoing laparoscopic inguinal hernia repair showed a considerable improvement in testicular functions, quality of life and sexual functions after surgery and there was no difference between TAPP and TEP repairs in terms of long-term outcomes such as quality of life, testicular functions and sexual functions.
References
Gass M, Banz V, Rosella L, Adamina M, Candinas D, Guller U (2012) TAPP or TEP? Population-based analysis of prospective data on 4,552 patients undergoing endoscopic inguinal hernia repair. World J Surg 36:2782–2786
Neumayer L, Hurdcr AG, Jonasson O, Fitzgibbons R, Dunlop D, Gibbs J, Reda D, Henderson W (2004) Open mesh vs laparoscopic mesh repair of inguinal hernia. N Engl J Med 350:1819–1827
Agnihotri K, Awasthi S, Chandra H, Singh U, Thakur S (2010) Validation of WHO QOL-BREF instrument in Indian adolescents. Indian J Pediatr 77:381–386
Myers E, Katherine M, Kavanagh D, Hurley M (2010) Laparoscopic (TEP) versus lichtenstein inguinal hernia repair: a comparison of quality-of-life outcomes. World J Surg 34:3059–3064
Tekatli H, Schouten N, van Dalen T, Burgmans I, Smakman N (2012) Mechanism, assessment, and incidence of male infertility after inguinal hernia surgery: a review of the preclinical and clinical literature. Am J Surg 204:503–509
Bittner R, Montgomery MA, Arregui E, Bansal V, Bingener J, Bisgaard T, Buhck H, Dudai M, Ferzli GS, Fitzgibbons RJ, Fortelny RH, Grimes KL, Klinge U, Koeckerling F, Kumar S, Kukleta J, Lomanto D, Misra MC, Morales-Conde S, Reinpold W, Rosenberg J, Singh K, Timoney M, Weyhe D, Chowbey P (2015) Update of guidelines on laparoscopic (TAPP) and endoscopic (TEP) treatment of inguinal hernia (International Endohernia Society). Surg Endosc 29:289–321
Melissa CS, Bun TA, Wing CK, Chung TY, Wai NE, Tat LH (2014) Randomized double-blinded prospective trial of fibrin sealant spray versus mechanical stapling in laparoscopic total extraperitoneal hernioplasty. Ann Surg 259:432–437
O’Reilly EA, Burke JP, Ronan O’Connell P (2012) A meta-analysis of surgical morbidity and recurrence after laparoscopic and open repair of primary unilateral inguinal hernia. Ann Surg 2012(255):846–853
Wang W-J, Chen J-Z, Fang Q, Li J-F, Jin P-F, Li Z-T (2013) Comparison of the effects of laparoscopic hernia repair and Lichtenstein tension-free hernia repair. J Laparoendosc Adv Surg Tech A 23:301–305
Elster EA, Hale DA, Mannon RB (2005) Surgical transplant physical examination: correlation of renal resistance index and biopsy-proven chronic allograft nephropathy. J Am Coll Surg 200:552–556
Bignell M, Partridge G, Mahon D, Rhodes M (2012) Prospective randomized trial of laparoscopic (trans-abdominal pre-peritoneal-TAPP) versus open (mesh) repair for bilateral and recurrent inguinal hernia: incidence of chronic groin pain and impact on quality of life: results of 10-year follow-up. Hernia 16:635–640
Abbas AE, Abd Ellatif ME, Noaman N, Negm A, El-Morsy G, Amin M, Moatamed A (2012) Patient-perspective quality of life after laparoscopic and open hernia repair: a controlled randomized trial. Surg Endosc 26:2465–2470
Bright E, Reddy VM, Wallace D, Garcea G, Dennison AR (2010) The incidence and success of treatment for severe chronic groin pain after open, transabdominal preperitoneal, and totally extraperitoneal hernia repair. World J Surg 34:692–696
Zheng B, Nan W, Qiao Q (2014) Meta-analysis of randomized controlled trials comparing Lichtenstein and totally extraperitoneal laparoscopic hernioplasty in treatment of inguinal hernias. J Surg Res 192:409–420
Krishna A, Misra MC, Bansal VK, Kumar S, Rajeshwari S, Chabra A (2012) Laparoscopic inguinal hernia repair: transabdominal preperitoneal (TAPP) versus totally extraperitoneal (TEP) approach—a prospective randomized controlled trial. Surg Endosc 26:639–649
International Association for the Study of Pain (1986) Subcommittee on taxonomy. classification of chronic pain: description of chronic pain syndromes and definition of pain terms. Pain 3:S1–S226
Reid I, Devlin HE (1994) Testicular atrophy as a consequence of inguinal hernia repair. Br J Surg 81:91–93
Uzzo RG, Lemack GE, Morissey KP, Goldstein M (1999) The effect of mesh prosthesis on the spermatic cord structures: a preliminary report in a canine model. J Urol 161:1344–1349
Peiper C, Junge K, Klinge U, Strehlau E, Ottinger A, Schumpelick V (2006) Is there a risk of infertility after inguinal mesh repair? Experimental studies in the pig and the rabbit. Hernia 10:7–12
Akbulut G, Serteser M, Yücel A, Değirmenci B, Yilmaz S, Polat C, San O, Dilek ON (2013) Can laparoscopic hernia repair alter function and volume of testis? Randomized clinical trial. Surg Laparosc Endosc Percutan Tech 13:377–381
Ersin S, Aydin D, Makay O, Icoz G, Tamsel S, Sozbilen M, Killi R (2006) Is testicular perfusion influenced during laparoscopic inguinal hernia surgery? Surg Endosc 20:685–689
Singh AN, Bansal VK, Misra MC, Kumar S, Rajeshwari S, Kumar A, Sagar R, Kumar A (2012) Testicular functions, chronic groin pain, and quality of life after laparoscopic and open mesh repair of inguinal hernia: a prospective randomized controlled trial. Surg Endosc 2012(26):1304–1317
Štula I, Družijanić N, Sapunar A, Perko Z, Bošnjak N, Kraljević D (2014) Antisperm antibodies and testicular blood flow after inguinal hernia mesh repair. Surg Endosc 28:3413–3420
Bischoff JM, Linderoth G, Aasvang EK, Werner MU, Kehlet H (2012) Dysejaculation after laparoscopic inguinal herniorrhaphy: a nationwide questionnaire study. Surg Endosc 26:979–983
McCormack K, Wake BL (2005) Transabdominal pre-peritoneal (TAPP) versus totally extraperitoneal (TEP) laparoscopic techniques for inguinal hernia repair: a systematic review. Hernia 9:109–114
Bansal VK, Misra MC, Babu D, Victor J, Kumar S, Sagar R, Rajeshwari S, Krishna A, Rewari V (2013) A prospective, randomized comparison of long-term outcomes: chronic groin pain and quality of life following totally extraperitoneal (TEP) and transabdominal preperitoneal (TAPP) laparoscopic inguinal hernia repair. Surg Endosc 27:2373–2382
Bracale U, Melillo P, Pignata G, Di Salvo E, Rovani M, Merola G, Pecchia L (2012) Which is the best laparoscopic approach for inguinal hernia repair: TEP or TAPP? A systematic review of the literature with a network meta-analysis. Surg Endosc 26:3355–3366
Poobalan A, Bruce T, King PM, Chambers WA, Krukowski ZH, Smith WCS (2001) Chronic pain and quality of life following open inguinal hernia repair. BJS 88:1122–1126
Cunningham J, Temple WJ, Mitchell P (1996) Co-operative study: pain in the post repair patient. Ann Surg 224:598–602
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Virinder Kumar Bansal, Asuri Krishna, Pratik Manek, Subodh Kumar, Omprakash Prajapati, Rajeshwari Subramaniam, Anand Kumar, Atin Kumar, Rajesh Sagar, M. C. Misra have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Bansal, V.K., Krishna, A., Manek, P. et al. A prospective randomized comparison of testicular functions, sexual functions and quality of life following laparoscopic totally extra-peritoneal (TEP) and trans-abdominal pre-peritoneal (TAPP) inguinal hernia repairs. Surg Endosc 31, 1478–1486 (2017). https://doi.org/10.1007/s00464-016-5142-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5142-0