Abstract
Swallowing discomfort is a common postoperative complaint in patients undergoing thyroidectomy. Contraction of the strap muscles might cause resistance to elevation of the laryngotracheal unit, and downward movement of the laryngotracheal unit may lead to swallowing discomfort. However, few studies have evaluated the mechanism related to limited laryngotracheal elevation after thyroidectomy. We aimed to objectively verify the presence of postoperative impaired laryngotracheal elevation through ultrasound evaluation in patients undergoing thyroidectomy and evaluate its relationship with limitation of laryngotracheal elevation. This is a prospective clinical study. Among patients undergoing hemithyroidectomy and total thyroidectomy, the patients who were followed up for ≥ 6 months were selected (N = 40). Ultrasound evaluation was done preoperatively and at 1, 3, and 6 months postoperatively. Laryngotracheal movement was recorded and the length of elevation was measured. Symptom after thyroidectomy was evaluated through swallowing-related items of thyroidectomy-related voice questionnaire. Ultrasound evaluation verified the presence of limited laryngotracheal elevation postoperatively in patients undergoing thyroidectomy. After thyroidectomy, the swallowing-related score was significantly increased, and was recovered time-dependently at 1 month. Laryngotracheal elevation showed significant decrease after thyroidectomy. The symptom score of swallowing was significantly correlated with the length of laryngotracheal elevation. Post-thyroidectomy ultrasound evaluation verified that laryngotracheal elevation was significantly impaired. Presence of adhesion between the laryngotracheal unit and the superficial soft tissue was the probable cause of the limitation at 6 months after thyroidectomy. The length of laryngotracheal elevation was related to the symptom score of swallowing after thyroid surgery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Subjective swallowing discomfort is a common postoperative adverse effect in patients undergoing thyroidectomy. More than half of these patients complain of non-specific dysphagia [1] and 15% experience symptoms for more than 2–5 years [2]. However, importance of the complication is often overlooked by surgeons. The most reported symptoms related to swallowing include sensation of the presence of lump, foreign body, too-tightly-buttoned shirt collar, of being strangled, and/or obstacle during swallowing [3]. Symptoms are usually transient and occur in the first week after thyroid surgery, although they are reported to occasionally occur long after the operation [1].
Under conventional open thyroidectomy, it is necessary to elevate a sub-platysma muscle flap, and the strap muscles are retracted laterally to create working space. Occurrence of adhesion between the flap and the strap muscle and excessive retraction of the strap muscles could cause fibrosis of the muscles [4], which results in the limitation of laryngotracheal elevation and swallowing difficulty.
Among three phases, oral, pharyngeal, and esophageal phases, of swallowing, pharyngeal phase is the shortest phase and the most complex phase. During pharyngeal phase, laryngotracheal elevation is a vital component of the airway protection, and plays an important role in relaxation and opening of the upper esophageal sphincter. The opening of the upper esophageal sphincter, together with the cessation of the tonic activity are brought about by traction of the suprahyoid muscles, which produce the anterosuperior displacement of the larynx. It is the reason that limitation of laryngotracheal elevation could cause swallowing difficulty and dysphagia [5].
Ultrasound (US) is a valuable diagnostic tool for disorders of the neck, especially the thyroid gland. Its application has expanded to setting of the airway for identifying the cricothyroid membrane in difficult airway intubation, confirming endotracheal tube placement, and evaluating the vocal folds and tracheal lesions [6, 7]. However, it has not been applied to evaluate the movement of the laryngotracheal unit in patients undergoing thyroidectomy.
In this study, we aimed to objectively verify the presence of postoperative limitation of laryngotracheal elevation in patients undergoing thyroid surgery through US evaluation and evaluate the relationship between swallowing difficulty and limitation of laryngotracheal movement.
Materials and Methods
The prospective study was approved by our Institutional Review Board. From June 1, 2017, to May 31, 2018, 83 patients who underwent thyroid surgery were enrolled. After exclusion of patients who underwent thyroidectomy with neck dissection and those with < 6 months’ follow-up duration, 40 patients were dichotomized by extent of surgery into two groups: hemithyroidectomy (HT) group (n = 22) and total thyroidectomy (TT) group (n = 18). Thyroidectomy was performed in a similar fashion by two surgeons (J.C. and J. W. with experience in thyroid surgery). Initially, the thyroid gland was exposed after detaching the skin and dividing the strap muscles by midline incision. The strap muscles were retracted laterally without cutting, for exposure of the thyroid gland. The recurrent laryngeal nerve and parathyroid glands were first identified and the lateral part of the thyroid lobe was excised.
To evaluate voice- and swallowing-related conditions associated with thyroid surgery, all patients were assessed pre- and postoperatively through the thyroidectomy-related voice questionnaire (TVQ) [8]. The questionnaire is a self-assessment tool for the quality of voice and swallowing function that consists of 20 questions, each scored from 0 to 4: voice-related symptoms, ten items; throat- or swallowing-related symptoms, ten items [9]. All patients underwent questionnaires preoperatively and at 1, 3, and 6 months postoperatively. For symptom scores, we used ten questions related to swallowing from the TVQ.
US evaluation was done preoperatively and at 1, 3, and 6 months postoperatively with use of Philips Affiniti 50G US system with L12-4 transducer. After fixation of the end of the transducer on the sternal notch for preventing movement of the transducer, the transducer was placed sagittally on laryngotrachea. The video recording of US image of elevation of the laryngotracheal unit was conducted by an intrinsic function of US machine under swallowing condition three times in each patient. At resting, the length between sternal notch and first tracheal ring was measured (L1). During swallowing, the length between sternal notch and first tracheal ring was measured again in the highest position of laryngotracheal elevation (L2). The length of laryngotracheal elevation (L3) was calculated by L2−L1. (Figure 1).
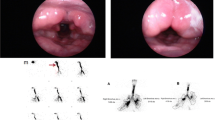
Ultrasound images captured from video recording under swallowing condition of patients after 6 months of thyroidectomy. a Pre-swallowing image. The white arrow marks the first ring of the trachea, and distance from the trachea immediately below the sternal notch was 2.36 cm. b Image during swallowing. Under condition of highest elevation of the first ring of the trachea, the distance measured per pre-swallowing protocol was 3.24 cm. The length of laryngotracheal elevation was 0.88 cm
Time-dependent changes (comparison between four groups) of the swallowing-related TVQ scores and the length of laryngotracheal movement in all patients who underwent thyroidectomy were analyzed by repeated measures analysis of variance, and the results were adjusted by Bonferroni correction method for multiple comparison. Paired t test was used to assess differences of paired samples (comparison between two groups, hemithyroidectomy and total thyroidectomy groups). Correlation was measured by linear regression analysis comparing swallowing-related TVQ scores, 1 month, 3 months, and 6 months with each length of laryngotracheal elevation. Probability values < .05 were considered statistically significant. Statistical analyses were performed using Statistical Package for the Social Sciences version 20 for Windows (SPSS, IBM Inc., Chicago, IL, USA).
Results
Swallowing-Related TVQ Scores in Patients Who Underwent Thyroidectomy
Temporal changes in swallowing-related TVQ scores were examined (Fig. 2a). The mean preoperative swallowing-related TVQ score was 4.03 ± 1.29. At 1 month postoperatively, it was significantly increased to 12.40 ± 2.28 (P < .001); at 3 months and 6 months postoperatively, each score was decreased to 9.78 ± 1.93, and 7.23 ± 1.90 compared to the score of 1 month; however, swallowing-related TVQ score was significantly different from the preoperative value (P = .024 at 3 months, P = .034 at 6 months).
Time-dependent changes in thyroidectomy-related voice questionnaire scores of the ten swallowing-related items in all patients who underwent thyroidectomy. Scores at 1, 3, and 6 months postoperatively were significantly increased compared to the preoperative scores. b In the total thyroidectomy group, scores at 1 and 3 months postoperatively were significantly increased compared to those in the hemithyroidectomy group
Temporal changes in swallowing-related TVQ scores in the TT or HT groups were significantly different (Fig. 2b). At 1 month postoperatively, the mean preoperative swallowing-related TVQ score in the TT group was significantly higher than that in the HT group; but it was decreased at 3 and 6 months postoperatively, without significant groupwise difference.
Length of Laryngotracheal Elevation in Patients Who Underwent Thyroidectomy
Laryngotracheal elevation was decreased significantly at 1 month postoperatively (Fig. 3a). The mean preoperative length of laryngotracheal elevation during swallowing was 1.30 ± 0.18 cm and was decreased significantly to 0.62 ± 0.19 cm at 1 month postoperatively. Laryngotracheal elevation was recovered to 0.81 ± 0.21 and 0.96 ± 0.18 cm at 3 and 6 months postoperatively, respectively;however, the length of laryngotracheal elevation was significantly different from the preoperative value at 6 months postoperatively (P = .021).
a Time-dependent changes in the length of laryngeal elevation in all patients who underwent thyroidectomy. The lengths at 1, 3, and 6 months postoperatively were significantly decreased compared to the preoperative length. b In the total thyroidectomy group, the lengths at 1 and 3 months postoperatively were significantly decreased compared to those in the hemithyroidectomy group
Length of laryngotracheal elevation in the TT or HT groups was significantly different at 1 and 3 months postoperatively (Fig. 3b). In the TT group, the length of laryngotracheal elevation was decreased to 0.48 ± 0.14 cm at 1 month postoperatively and 0.66 ± 0.16 cm at 3 months postoperatively compared to 1.27 ± 0.17 cm preoperatively. In the HT group, the length of laryngotracheal elevation was decreased to 0.73 ± 0.15 cm at 1 month postoperatively and 0.93 ± 0.15 cm at 3 months postoperatively compared to 1.31 ± 0.18 cm preoperatively. There was a significant difference in the length of laryngotracheal elevation between the TT group and HT groups at 1 and 3 months postoperatively (P = .034 and P = .0.30, respectively).
Relationship Between Swallowing-Related TVQ Score and Length of Laryngotracheal Elevation in Patients Who Underwent Thyroidectomy
Swallowing-related TVQ score was inversely associated with the length of laryngotracheal elevation at 1, 3, and 6 months postoperatively in the TT and HT groups (Fig. 4a, b). In the TT group, swallowing-related TVQ score was negatively correlated with the length of laryngotracheal elevation (γ = − 0.612, P = .024). In the HT group, swallowing-related TVQ score was negatively correlated with the length of laryngotracheal elevation (γ = − 0.404, P = .042).
Relationship between the swallowing-related TVQ score and the length of laryngotracheal elevation in the total thyroidectomy group. Length of laryngotracheal elevation was negatively correlated with swallowing-related TVQ score (γ = − 0.612, P = .024). b Relationship between the swallowing-related TVQ score and the length of laryngotracheal elevation in the hemithyroidectomy group. Length of laryngotracheal elevation was negatively correlated with swallowing-related TVQ score (γ = − 0.404, P = .042)
Postoperative Changes of the Soft Tissue on Laryngotracheal Unit
Preoperative video recording through the US system of the laryngotracheal elevation during swallowing showed independent movement of the laryngotracheal unit and the strap muscles from the superficial soft tissue. At 1 and 3 months postoperatively, laryngotracheal elevation was significantly decreased; hence, no definite adhesion between the superficial soft tissue and the laryngotracheal unit was observed; at 6 months postoperatively, laryngotracheal elevation was considerably recovered, but adhesion between the superficial soft tissue and the laryngotracheal unit was observed (Supplementary videos 1, 2, 3).
Discussion
Importance of the laryngotracheal unit in patients who have undergone thyroidectomy has attracted attention because of studies reporting swallowing difficulty and hoarseness as common discomfort after thyroidectomy. Swallowing includes sequential muscle activity as function of time and localization. During the act of swallowing, the velopharyngeal isthmus closes to protect the nasal, laryngeal, and tracheal airways, and laryngeal elevation is the vital component of the protective mechanism [10, 11]. Swallowing difficulty was suggested to be associated with limitation of laryngotracheal elevation secondary to impaired vertical laryngeal movement or temporary malfunction of the strap muscles after surgery [12]. Laryngotracheal elevation plays an important role in formation of the pharyngeal phase of swallowing. To the best of our knowledge, there are no studies evaluating motion of the laryngotracheal unit under swallowing condition of patients after thyroidectomy through US.
US is increasingly used in evaluation of the neck for presence of inflammatory lesion, benign and malignant lesions, and airway management [13]. Recently developed US system has video recording function that allows detection of movement of the laryngotracheal unit during swallowing that was not possible with previous imaging systems; in addition, it allows the measurement of the length of laryngotracheal elevation because sagittal image of the laryngotracheal unit can be acquired.
On preoperative video recording (Supplementary video), the laryngotracheal unit was elevated during swallowing without movement of the superficial soft tissue, indicating that the unit was separated from the subcutaneous soft tissue. At 6 months after thyroid surgery, the superficial soft tissue above the laryngotracheal unit was also elevated during swallowing followed by elevation of the laryngotracheal unit. If we recorded video at the upright position of patients, the adhesion effect between the laryngotracheal unit and above the soft tissue would have been more clearly observed.
We evaluated the change in swallowing symptoms among patients who underwent thyroidectomy, from preoperative period to 6-month postoperative period, using the TVQ questionnaire. In the present study, swallowing-related TVQ scores were significantly changed at 1 month postoperatively, especially in the TT group and over time showed tendency of gradual improvement. However, after 6 months, swallowing-related TVQ scores did not recover to near preoperative values. In our previous study, at 1 year postoperatively, swallowing-related TVQ score was not improved to preoperative value and was worse in the TT group [14]. These results suggest that swallowing-related discomfort after thyroid surgery may have more serious effect on the quality of life of patients who undergo total thyroidectomy.
The length of laryngotracheal elevation was significantly decreased at 1 month postoperatively, especially in the TT group. It is likely that at 1 month postoperatively, altered retraction function of the strap muscle during surgery was not recovered to normal status. Likewise, Hong et al. reported that contraction of the sternohyoid and sternothyroid muscles caused the laryngotracheal downward movement [12]. Sternohyoid and sternothyroid muscles may be damaged by lateral retraction or incision during thyroid surgery or by wound contracture of the surrounding structures after surgery. Generally, in thyroidectomy, the strap muscles are retracted laterally unless the thyroid tissue is not enlarged. However, if the enlarged thyroid tissue prevents adequate visual field, incision of the strap muscles may be needed. Incision of the strap muscles increases risk of fibrosis. In our study, laryngotracheal elevation was improved, but did not attain normal value at 6 months post-thyroidectomy. In this time, the most important factor to affect limitation of laryngotracheal elevation might be adhesion of the laryngotracheal unit to the superficial soft tissue. Alkan et al. reported absence of electrophysiological differences of the strap muscles under swallowing condition of patients 3 months after TT [15]. Thus, the strap muscles have normal function after surgery, and causes of impaired laryngeal elevation are multiple and not related to function of the strap muscles alone.
The length of laryngotracheal elevation and swallowing-related TVQ score showed time-dependent improvement up to 6 months after thyroidectomy. Swallowing-related TVQ score was negatively correlated with the length of laryngotracheal elevation in the HT and TT groups. Therefore, swallowing difficulty may be related to discomfort of swallowing due to the importance of laryngotracheal elevation during swallowing.
Clinicians generally consider swallowing problems as related to oro-pharyngeal intubation and neglect the symptoms reported through subjective evaluation. However, in this study, we verified the limitation of laryngotracheal elevation after thyroidectomy, and determined its relationship with swallowing-related symptoms.
Laryngotracheal elevation and TVQ score were worse in TT group than those in HT group. The difference of extent of dissection during surgery bwtween two groups could make the difference of symptoms during swallowing. In total thyroidectomy, bilateral traction of strap muscles was done, and it would make the dysfunction or fibrosis of those muscles in early period. And bilateral dissection might make more fibrosis of soft tissue around trachea than unilateral dissection. It could be a cause of differences between two groups.
Our study has some limitations as follows: (1) The follow-up period (6 months) was relatively short and may have been insufficient to observe complete resolution of swallowing-related symptoms after thyroidectomy. But, in general, postoperative wound was stabilized in 6 month, and there was no differences of TVQ scores between postoperative 6 months and 12 months in previous study [14]. Therefore, the results of 6 months after surgery might be significant; (2) we video-recorded laryngotracheal elevation at supine position of patients; (3) we did not evaluate the effect of anti-adhesive agent to prevent adhesion between the laryngotracheal unit and the superficial soft tissue; and (4) our institution is a tertiary medical center that provides treatment to both referred and community patients; hence, selection bias is inevitable; therefore, results of the study should be interpreted with caution. A long-term follow-up, randomized controlled, and comparative study with anti-adhesive agent is required, using US at upright position of patients, to confirm the current results.
This study showed through US evaluation of patients undergoing thyroidectomy that laryngotracheal elevation was significantly impaired postoperatively. In the early period after thyroidectomy, impaired function of the strap muscle is possibly a cause of laryngotracheal elevation; adhesion between the laryngotracheal unit and the superficial soft tissue is possibly a cause of the limitation at 6 months after thyroidectomy. The length of laryngotracheal elevation was related to the symptom score of swallowing after thyroid surgery. Small and gentle elevation of the subplatysmal flap might be helpful to prevent swallowing impairment.
References
Lombardi CP, Raffaelli M, D’Alatri L, Marchese MR, Rigante M, Paludetti G, Bellantone R. Voice and swallowing changes after thyroidectomy in patients without inferior laryngeal nerve injuries. Surgery. 2006;140:1026–32. https://doi.org/10.1016/j.surg.2006.08.008discussion 1032–1024.
Pereira JA, Girvent M, Sancho JJ, Parada C, Sitges-Serra A. Prevalence of long-term upper aerodigestive symptoms after uncomplicated bilateral thyroidectomy. Surgery. 2003;133:318–22. https://doi.org/10.1067/msy.2003.58.
Lombardi CP, Raffaelli M, De Crea C, D’Alatri L, Maccora D, Marchese MR, Paludetti G, Bellantone R. Long-term outcome of functional post-thyroidectomy voice and swallowing symptoms. Surgery. 2009;146:1174–81. https://doi.org/10.1016/j.surg.2009.09.010.
Akyildiz S, Ogut F, Akyildiz M, Engin EZ. A multivariate analysis of objective voice changes after thyroidectomy without laryngeal nerve injury. Arch Otolaryngol Head Neck Surg. 2008;134:596–602. https://doi.org/10.1001/archotol.134.6.596.
Ertekin C, Aydogdu I. Neurophysiology of swallowing. Clin Neurophysiol. 2003;114:2226–44. https://doi.org/10.1016/S1388-2457(03)00237-2.
Lakhal K, Delplace X, Cottier JP, Tranquart F, Sauvagnac X, Mercier C, Fusciardi J, Laffon M. The feasibility of ultrasound to assess subglottic diameter. Anesth Analg. 2007;104:611–4. https://doi.org/10.1213/01.ane.0000260136.53694.fe.
Votruba J, Zemanova P, Lambert L, Vesela MM. The role of airway and endobronchial ultrasound in perioperative medicine. Biomed Res Int. 2015;2015:754626. https://doi.org/10.1155/2015/754626.
Nam IC, Bae JS, Shim MR, Hwang YS, Kim MS, Sun DI. The importance of preoperative laryngeal examination before thyroidectomy and the usefulness of a voice questionnaire in screening. World J Surg. 2012;36:303–9. https://doi.org/10.1007/s00268-011-1347-5.
Chun BJ, Bae JS, Chae BJ, Hwang YS, Shim MR, Sun DI. Early postoperative vocal function evaluation after thyroidectomy using thyroidectomy related voice questionnaire. World J Surg. 2012;36:2503–8. https://doi.org/10.1007/s00268-012-1667-0.
Ertekin C, Aydogdu I. Neurophysiology of swallowing. Clin Neurophysiol. 2003;114:2226–44.
Martin BJ, Logemann JA, Shaker R. Dodds WJ (1994) Coordination between respiration and swallowing: respiratory phase relationships and temporal integration. J Appl Physiol. 1985;76:714–23. https://doi.org/10.1152/jappl.1994.76.2.714.
Hong KH, Kim YK. Phonatory characteristics of patients undergoing thyroidectomy without laryngeal nerve injury. Otolaryngol Head Neck Surg. 1997;117:399–404. https://doi.org/10.1016/S0194-5998(97)70133-5.
Kristensen MS. Ultrasonography in the management of the airway. Acta Anaesthesiol Scand. 2011;55:1155–73. https://doi.org/10.1111/j.1399-6576.2011.02518.x.
Park YM, Oh KH, Cho JG, Baek SK, Kwon SY, Jung KY, Woo JS. Changes in voice- and swallowing-related symptoms after thyroidectomy: one-year follow-up study. Ann Otol Rhinol Laryngol. 2018;127:171–7. https://doi.org/10.1177/0003489417751472.
Alkan Z, Yigit O, Adatepe T, Uzun N, Kocak I, Sunter V, Server EA. Effect of anti-adhesive barrier use on laryngotracheal movement after total thyroidectomy: an electrophysiological study. Indian J Otolaryngol Head Neck Surg. 2014;66:71–7. https://doi.org/10.1007/s12070-011-0319-2.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary material 1 (MOV 75277 kb)
Supplementary material 2 (MOV 73248 kb)
Supplementary material 3 (MOV 72946 kb)
Appendix
Rights and permissions
About this article
Cite this article
Cho, JG., Byeon, H.K., Oh, K.H. et al. Objective Assessment of Postoperative Swallowing Difficulty Through Ultrasound in Patients Undergoing Thyroidectomy. Dysphagia 35, 253–260 (2020). https://doi.org/10.1007/s00455-019-10020-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-019-10020-1