Abstract
The venom of the Brazilian armed spider Phoneutria nigriventer is a rich source of biologically active peptides that have potential as analgesic drugs. In this study, we investigated the analgesic and adverse effects of peptide 3-5 (Tx3-5), purified from P. nigriventer venom, in several mouse models of pain. Tx3-5 was administered by intrathecal injection to mice selected as models of postoperative (plantar incision), neuropathic (partial sciatic nerve ligation) and cancer-related pain (inoculation with melanoma cells) in animals that were either sensitive or tolerant to morphine. Intrathecal administration of Tx3-5 (3–300 fmol/site) in mice could either prevent or reverse postoperative nociception, with a 50 % inhibitory dose (ID50) of 16.6 (3.2–87.2) fmol/site and a maximum inhibition of 87 ± 10 % at a dose of 30 fmol/site. Its effect was prevented by the selective activator of L-type calcium channel Bay-K8644 (10 μg/site). Tx3-5 (30 fmol/site) also produced a partial antinociceptive effect in a neuropathic pain model (inhibition of 67 ± 10 %). Additionally, treatment with Tx3-5 (30 fmol/site) nearly abolished cancer-related nociception with similar efficacy in both morphine-sensitive and morphine-tolerant mice (96 ± 7 and 100 % inhibition, respectively). Notably, Tx3-5 did not produce visible adverse effects at doses that produced antinociception and presented a TD50 of 1125 (893–1418) fmol/site. Finally, Tx3-5 did not alter the normal mechanical or thermal sensitivity of the animals or cause immunogenicity. Our results suggest that Tx3-5 is a strong drug candidate for the treatment of painful conditions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pain is the most common complaint in the medical field and the main reason people seek medical care. However, the arsenal of analgesics is small, only partially effective and can be accompanied by potentially serious adverse effects [1, 2]. It is estimated that around 600 million people worldwide will experience negative health impacts due to untreated pain in the next few years [1, 2]. Thus, there are several different types of pain which produce severe distress in many patients and dominate and disrupt their quality of life. Approximately half of all patients who have undergone surgery report severe to intolerable postoperative pain [29, 44, 49]. Nonsteroidal anti-inflammatory drugs and opioids are useful to prevent and treat postoperative pain, but these drugs can cause adverse effects that limit their use [10]. Neuropathic pain is a common clinical condition in which the current treatments are often inadequate and ineffective or produce potentially severe adverse effects [6–9, 15]. Moreover, it has been estimated that there is likely to be an increase of 70 % in cancer cases until 2030, with many cancer patients experiencing pain that negatively impacts on their quality of life [17]. This pain is severe and often requires chronic opioid treatment, which can lead to the development of tolerance to opioids after prolonged treatment [35, 38]. Thus, novel, effective and safe alternatives to the current analgesic drugs are needed.
An alternative for the treatment of patients that have postoperative, neuropathic or cancer-related pain and are refractory to opioid therapy has been the intrathecal administration of ziconotide [2, 42, 57, 61, 63, 73, 82]. Ziconotide is the synthetic form of the conopeptide ω-MVIIA (isolated from the venom of the Pacific fish-hunting snail, Conus magus), which acts as a blocker of N-type voltage-sensitive calcium channels (VSCC) [42]. Clinical and pre-clinical trials with ziconotide demonstrated efficacy in the treatment of pathological pain [13, 80]. However, it has a narrow therapeutic window and produces some serious adverse effects in analgesic doses that limit its use [47, 67, 68]. Thus, although VSCC seem to be interesting targets for the development of analgesic and opioid adjuvant drugs, adequately safe VSCC blockers remain elusive.
The venom of the Brazilian armed spider Phoneutria nigriventer contains a variety of peptides that display a diverse range of actions, including modulation of VSCC [21]. Of the six peptide isoforms purified from the fraction PhTx3 of the venom, we have previously demonstrated the analgesic potential of Tx3-6 (Phα1β), Tx3-3 and Tx3-4 in rodent models of inflammatory, neuropathic and oncological pain, with a good therapeutic window [11, 54–56, 65, 72, 74]. However, the analgesic potential of peptide 3-5 (Tx3-5) is currently unknown. Tx3-5 is known to be both a selective and potent blocker of L-type VSCC [31, 32], which has little structural similarity to other P. nigriventer venom isolates [9, 53]. Thus, in the present study, we aimed to investigate the antinociceptive potential and possible toxic effects of Tx3-5 in different pain models in mice.
Methods
Animals
The experiments were conducted using male Swiss mice (30–35 g, 8 weeks old) or C57BL/6 mice (20–30 g, 8 weeks old at the time of inoculation with melanoma cells). The animals had free access to food and water and were maintained in a temperature-controlled room (22 ± 2 °C) under a 12-h light–dark cycle. The animals were acclimatized to the laboratory for at least 1.5 h before the experiments and were used only once. The experiments were performed with the approval of the Ethics Committee of the Federal University of Santa Maria (process number 11/2010), and were carried out in accordance with the current guidelines for the care of laboratory animals [83]. The number of animals and the intensities of noxious stimuli used were the minimum necessary to consistently demonstrate the effects of the drug treatments.
A total of 221 mice were used in this study distributed as follows:
-
Effects of Tx3-5 on the acute thermal nociception or the mechanical threshold of mice: n = 4–6/group (total 27).
-
Effects of Tx3-5 on the postoperative pain model: n = 5–8/group (total 55).
-
Reversion of Tx3-5-induced antihyperalgesic effect by Bay-K8644 in the postoperative pain model: n = 6–7/group (total 25).
-
Effects of Tx3-5 on the neuropathic pain model: n = 6–8/group (total 14).
-
Effects of Tx3-5 on the cancer-related pain model and morphine tolerance in mice: n = 6–7/group (total 32; C57BL/6 mice).
-
Adverse effects induced by Tx3-5: total 68.
-
Behavioural evaluation was performed blindly with respect to drug administration.
Drugs
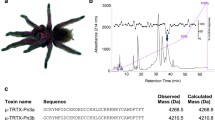
The peptide Tx3-5 was purified from the venom of P. nigriventer by a combination of chromatographic steps according to the method described by Corbett et al. [9]. Tx3-5 has a molecular weight of 5063 kDa, and the amino acid sequence is GCIGRNESCKFDRHGCCWPWSCSCWNKEGQPESDVWCECSLKIGK [53]. ω-Conotoxin MVIIA was purchased from Latoxan (Valence, France), and morphine was obtained from Cristália (São Paulo, Brazil). Bay-K8644, an activator of L-type calcium channels, was obtained from Sigma (St. Louis, MO, USA) and murine interleukin-1β (IL-1β) kits were purchased from PeproTech (Rocky Hill, USA).
Drug administration
Tx3-5, ω-conotoxin MVIIA and Bay-K8644 were administered by the intrathecal route (i.t.) according to the technique described by Hylden and Wilcox [26]. Except for Bay-K8644, which was dissolved in phosphate-buffered saline (PBS) containing 4 % dimethyl sulphoxide, all other drugs were dissolved only in PBS, which was used as a vehicle, and delivered in a volume of 5 μl/site for each mouse. Behavioural testing was performed blindly with respect to the drug treatments.
Assessment of Tx3-5 or morphine on the thermal sensitivity or the mechanical threshold of mice
Naïve animals received Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.). The mechanical threshold and thermal sensitivity of the animals were measured at 0.5, 1, 2 and 4 h after drug administration, as described below. Morphine (10 mg/kg, s.c.) was used as a positive control [75].
Measurement of the mechanical threshold
The measurement of the mechanical threshold was carried out using the up-and-down paradigm as described previously by Chaplan et al. [6]. Briefly, mice were acclimatized in individual, clear, Plexiglas boxes (9 × 7 × 11 cm) on an elevated, wire mesh platform to allow access to the plantar surface of the right hind paw. Filaments of von Frey of increasing stiffness (0.02–10 g) were applied to the hind paw plantar surface with a pressure causing the filament to bend. Absence of a paw-lifting response after 5 s led to the use of the next filament with increasing weight, and paw lifting indicated a positive response and led to the use of the next weaker filament. This paradigm continued until a total of six measurements were made or until four consecutive positive or four consecutive negative responses had occurred. All measurements were carried out in the right hind paw. The 50 % withdrawal threshold (expressed in grams) was then calculated from the resulting scores, as described previously by Dixon [13]. The 50 % threshold was evaluated before (basal) and several times after each drug treatment or surgical procedure. A decrease in the 50 % paw withdrawal threshold, when compared with the same paw before surgery or melanoma injection (basal value), was considered to be mechanical hyperalgesia. Conversely, the antihyperalgesic effect after each treatment was considered as an increase in the 50 % paw withdrawal threshold when compared with the control group.
Measurement of acute thermal nociception
The acute nociception evoked by thermal stimulation was measured as previously described by Hargreaves et al. [24]. A radiant thermal stimulus was projected onto the paw of the animals and the paw withdrawal latency was measured (s) and was evaluated before (basal) and several times after drug treatment. To avoid tissue damage, the maximum time of exposure to the heat source was 40 s. A positive antihyperalgesic effect was defined as an increase in the paw withdrawal latency with respect to the control group.
Postoperative pain model
The postoperative pain model was carried out according to the procedure described by Oliveira et al. [45]. Mice were anaesthetized with 2 % halothane via a nose cone. After aseptic preparation of the right hind paw with 10 % povidone–iodine solution, a 5-mm longitudinal incision was made with a number 11 blade through the skin and fascia of the plantar foot. The incision was started 2 mm from the proximal plantar edge of the calcaneus/of the tarsus. The underlying flexor tendons were elevated with curved forceps and then returned to their normal anatomical position. The skin was apposed with a single mattress suture of 6.0 nylon.
To evaluate the preventive effect of Tx3-5 in the postoperative pain model, the mice were pretreated with Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.) 0.5 h before the surgical procedure, and the mechanical threshold was measured at 0.5, 1, 2 and 4 h after surgery (pretreatment protocol). In contrast, to assess the curative effect of Tx3-5 in the postoperative pain model, the animals were submitted to the surgical procedure, and the mechanical threshold was determined at 0.5 h after surgery (posttreatment protocol). Firstly, one group of animals was treated with a single injection of Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.), and the responses to mechanical stimuli were measured at 0.5, 1, 2 and 4 h after treatment. In a different group of animals, Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.) was repeatedly administered at 0.5 h and 1, 2, 3, 4 and 5 days after the plantar incision; the mechanical threshold of mice was measured at 1 h after the last administration every day.
To determine the dose–response curve, mice were submitted to postoperative treatment with Tx3-5 (3, 30 or 300 fmol/site, i.t.) or PBS (5 μl/site, i.t.), and the responses to mechanical hyperalgesia were measured at 1 h after treatment.
In another set of experiments, we assessed the possible role of L-type calcium channels in the antinociceptive effect of Tx3-5 (30 fmol/site, i.t.). Following the surgical procedure, the mechanical threshold was determined at 0.5 h after surgery, and immediately after the mechanical threshold determination, the mice received an intrathecal injection of Tx3-5 (30 fmol/site, i.t.) alone, Bay-K8644 (10 μg/site, i.t.) alone or Tx3-5 (30 fmol/site, i.t.) plus Bay-K8644 (10 μg/site, i.t.). The mechanical threshold was measured from 0.5 up to 4 h after administration of the treatments.
Neuropathic pain model
For induction of chronic mononeuropathy, male mice were first anaesthetized by intraperitoneal injection of 90 mg/kg of ketamine plus 3 mg/kg of xylazine hydrochloride. Then, a partial sciatic nerve ligation (PSNL) was made by tying one third to one half of the dorsal portion of the right sciatic nerve [36, 46, 78]. In the sham-operated mice, the nerve was exposed without ligation. Seven days after the surgical procedure, the mechanical threshold was measured to confirm the development of hyperalgesia. The animals that suffered PSNL and presented mechanical hyperalgesia were selected for the experiment and either Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.) was administered. Mechanical thresholds were measured at 0.5, 1, 2 and 4 h after treatments.
Cancer-related-pain and morphine tolerance model
B16–BL6 cells, a highly invasive variant of B16 melanoma derived from the C57BL/6 mouse, were incubated as monolayer cultures in Eagle’s minimum essential medium containing 5 % foetal bovine serum and 1 % penicillin–streptomycin. The melanoma cells (1 × 105 cells) were suspended in PBS, and 20 μl of this suspension was injected subcutaneously into the plantar region of the unilateral hind paw of C57BL/6 mice; those that demonstrated mechanical hyperalgesia 2 weeks postinoculation were selected for the experiment. This protocol was performed as previously described [54, 60]. Either Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.) was administered, and the responses to mechanical stimuli were measured 0.5, 1, 2 and 4 h after treatment.
Another group of animals that received intraplantar inoculation of B16–BL6 cells and those that demonstrated mechanical hyperalgesia after 2 weeks of administration were treated with morphine (10 mg/kg, s.c.) or saline (10 ml/kg, s.c.), and the mechanical hyperalgesia was observed from 0.5 up to 2 h after the injection of saline or morphine. To induce tolerance, the animals received three injections of morphine per day for 3 days (first day 10, 10 and 15 mg/kg; second day 15, 15 and 20 mg/kg; and third day 20, 20 and 25 mg/kg), according to Marshall and Weinstock [39], with some modifications. Saline injection was used as the control. On the fourth day, we injected the animals with morphine (10 mg/kg) or saline (10 ml/kg) and evaluated the development of tolerance to the antinociceptive effect from 0.5 up to 2 h after injection. Then, the morphine- and saline-treated groups were treated with PBS or Tx3-5 (30 fmol/site, i.t.), and the mechanical hyperalgesia was observed at 0.5, 1, 2 and 4 h after treatment.
Evaluation of adverse effects
To verify and quantify the possible development of behavioural adverse effects induced by Tx3-5 or ω-conotoxin MVIIA, mice were placed in individual boxes (25 × 25 cm) for behavioural observations at 0.5, 2 and 24 h after its administration. We observed the ratio of the number of animals that demonstrated adverse effects in relation to the number of animals that did not demonstrate adverse effects, and then quantified the possible adverse effects caused by Tx3-5 or ω-conotoxin MVIIA. The adverse effects were rated as nil, mild, moderate or severe using the following scores: 0, no effect—no adverse effect; 1, mild effects—Straub’s tail, licking of the back and the tail, rapid and transient acceleration of respiratory movements; 2, moderate effects—tail serpentine-like movements; and 3, severe effects—whole-body tremors and ataxia; these scores are according to Scott et al. [64], with modifications (adapted to a numerical scale). We determined the dose of Tx3-5 or ω-conotoxin MVIIA that produces any toxicity in 50 % of animals (TD50) following intrathecal injection. To determine the TD50 value, the animals received Tx3-5 (30–10,000 fmol/site, i.t.) or ω-conotoxin MVIIA (10,000–100,000 fmol/site, i.t., used as a positive control), and the adverse effects were observed from 0.5 up to 24 h postinjection.
We also evaluated the spontaneous and forced locomotor activity of animals that received Tx3-5 using the open-field and the rota-rod tests, respectively, as previously described [11, 46]. The open-field apparatus consisted of a box measuring 25 × 25 cm with a floor that was divided into nine identical areas. To evaluate the spontaneous locomotor activity of animals, at 0.5, 2 and 24 h after Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.) injection, the animals were transferred to the apparatus and the number of areas crossed with all paws (crossings) in 4 min was recorded. For the rota-rod test, the animals were trained on the rota-rod (3.7 cm in diameter, 8 rpm) until they could remain on the apparatus for 60 s without falling. On the day of the experiment, the animals were injected with Tx3-5 (30 fmol/site, i.t.) or PBS and subjected to the rota-rod test at 0.5, 2 and 24 h later. The number of falls from the apparatus was recorded for 120 s. Morphine (10 mg/kg, s.c.) was used as a positive control for both tests.
To assess the immunogenicity of Tx3-5, we also verified the levels of IL-1β in spinal cord samples by ELISA (TP-Reader, Thermoplate) using commercial kits according to the manufacturer’s instructions. Animals received either a single or repeated (once a day for 6 days) administration of Tx3-5 (30 fmol/site, i.t.). Twenty-four hours after the last injection, animals were euthanized and the lumbar (L1 to L6) spinal cord was collected by mechanical extrusion and homogenized in appropriate buffer (PBS containing 1 mM EDTA, 0.1 mM PMSF and BSA 0.5 %, pH 7.4) for IL-1β measurements. As a positive control, we injected lipopolysaccharide (LPS, 10 μg/site, i.t.) into a separate group of animals [5]. The results were expressed as picograms of IL-1β/mg protein. The detection limit of the used kit is 63 pg/ml of IL-1β.
Statistical analyses
The results were expressed as the mean ± standard error of the mean (S.E.M.), with the exception of the inhibitory dose 50 % (ID50) or the TD50 values (i.e. the Tx3-5 dose that reduces nociceptive responses to 50 % of that of the control value, or that produced toxicity in 50 % of animals), which were expressed as geometric means accompanied by their respective 95 % confidence limits. ID50 and TD50 values were determined using non-linear regression and probit analysis, respectively. Statistical analyses were carried out using GraphPad Prism 5.0 software. The significance of the differences between groups was evaluated with a one-way analysis of variance (ANOVA) followed by a Student–Newman–Keuls’ post hoc test or a two-way ANOVA (time and treatment as factors, and F values indicate the interaction between these factors) followed by Bonferroni’s post hoc test when appropriate. The data of spontaneous and forced locomotor activity of animals were analysed by chi-square test. Results were considered significant when p < 0.05. To calculate the TD50 value and their 95 % confidence limits the data were subjected to probit analysis using SPSS 8.0 software. No statistical methods were used to predetermine sample sizes, but our sample sizes are similar to those reported in previous publications in the field.
Results
Effects of Tx3-5 on the acute thermal nociception or the mechanical threshold
The administration of Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.) did not alter the acute thermal nociception or mechanical threshold of naïve animals (Fig. 1a, b). However, morphine (10 mg/kg, s.c., used as positive control) increased the paw withdrawal latency [F(8,64) = 6.5; p < 0.0001; Fig. 1c], but did not change the mechanical threshold (Fig. 1d) of animals, when compared with animals that received PBS.
Effects of intrathecal administration of Tx3-5 or morphine on acute thermal nociception or on the mechanical threshold in mice. a, b Time–response curves of the treatment with Tx3-5 (30 fmol/site, i.t.) on acute thermal nociception (a) or on the mechanical threshold (b) in mice. c, d Time–response curve of the treatment with morphine (10 mg/kg, s.c.) on acute thermal nociception (a) or on the mechanical threshold (d) in mice. B denotes basal threshold before treatment with Tx3-5 or PBS. Data are expressed as the means + S.E.M. of four to six animals per group (n = 6 to a and b; n = 5–6 to c; n = 4 to d). Two asterisks p < 0.001, three asterisks p < 0.001 when compared with the PBS group; two-way ANOVA followed by Bonferroni’s post hoc test
Effects of Tx3-5 on the postoperative pain model
The surgical procedure caused a significant decrease in the mechanical threshold at all time points measured (0.5 h to 5 days) in PBS-treated mice when compared with the baseline threshold, which suggests the development of mechanical hyperalgesia. The treatment with Tx3-5 (30 fmol/site, i.t.) after the incision promoted an antinociceptive effect [F(5,60) = 12.5; p < 0.0001; Fig. 2a] from 0.5 up to 2 h after treatment. Furthermore, the repeated posttreatment with Tx3-5 (30 fmol/site, i.t.) could reduce the observed hyperalgesia of the animals [F(6,72) = 8.3; p < 0.001; Fig. 2b] for 1 up to 4 days postsurgery. In the dose–response curve, Tx3-5 (30 or 300 fmol/site, but not 3 fmol/site, i.t.) was able to reverse the mechanical hyperalgesia induced by the incision [F(3,20) = 6.8; p < 0.001; Fig. 2c], with an ID50 value of 16.6 (3.2–87.2) fmol/site, i.t., and a maximum inhibition of 87 ± 10 % at the dose of 30 fmol/site, i.t.
Antinociceptive effects produced by the intrathecal injection of Tx3-5 in the postoperative pain model in mice. a, b, d Time–course curves of posttreatment (a, b) or pretreatment (d) with Tx3-5 (30 fmol/site, i.t.) or PBS. c The dose–response curve in mice posttreated with Tx3-5 (3, 30, or 300 fmol/site, i.t.) or PBS. B denotes baseline threshold before surgery, while B1 indicates basal mechanical threshold after surgery and before treatment with Tx3-5 or PBS. Data are expressed as the means + S.E.M. of five to seven animals per group (n = 7–8 to a; n = 6–8 to b and d; n = 5–7 to c). Number sign p < 0.01 when compared with the basal mechanical threshold (b); one asterisk p < 0.05, two asterisks p < 0.01 and three asterisks p < 0.001 when compared with the PBS group (one-way ANOVA followed by Student–Newman–Keuls’ test to c and two-way ANOVA followed by Bonferroni’s post hoc test to a, b and d
To assess the preventive effect of Tx3-5, a group of animals was pretreated with Tx3-5 (30 fmol/site) or vehicle (PBS; 5 μl/site, i.t.) before the surgical procedure and after evaluation of the mechanical paw withdrawal threshold of the animals (baseline; B). The animals treated with vehicle (prior to surgery) demonstrated mechanical hyperalgesia from 0.5 up to 4 h after surgery Conversely, the pretreatment with Tx3-5 prevented the development of mechanical hyperalgesia [F(4,52) = 4.6; p < 0.01; Fig. 2d] from 0.5 up to 2 h after surgery (inhibition of 70 ± 15 % at 2 h), but not at 4 h after surgery.
Reversion of Tx3-5-induced antihyperalgesic effect by Bay-K8644 in the postoperative pain model
We verified previously that Tx3-5 was able to prevent and reverse the mechanical hyperalgesia induced by the surgical procedure. Following from this, we evaluated the effect of Bay-K8644, an opener of L-type VSCC, on the antihyperalgesic effect induced by Tx3-5. Firstly, we found that Bay-K8644 (10 μg/site, i.t.) alone did not significantly alter the mechanical threshold of those animals who underwent surgery. However, the co-administration of Bay-K8644 (10 μg/site, i.t.) reversed the antihyperalgesic effect induced by Tx3-5 (30 fmol/site, i.t.) from 0.5 up to 2 h after its administration [F(15,105) = 3.2; p < 0.001; Fig. 3], with a maximum reversion of 92 ± 19 % at 1 h posttreatment.
Effects of the activator of L-type calcium channels Bay-K8644 (10 μg/site, i.t.), or vehicle, on antihyperalgesic effect induced by Tx3-5 (30 fmol/site) in the postoperative pain model. B denotes baseline threshold before surgery, and B1 indicates basal mechanical threshold after surgery and before the treatments. Vertical bars represent the means + S.E.M. of six to seven animals per group. Number sign p < 0.01 when compared with the basal mechanical threshold (B); three asterisks p < 0.001, when compared with the respective vehicle group; two-way ANOVA followed by Bonferroni’s post hoc test
Effects of Tx3-5 on the neuropathic pain model
Partial ligation of the sciatic nerve produced mechanical hyperalgesia 7 days after surgery, when compared with the baseline threshold (Fig. 4). The treatment with Tx3-5 (30 fmol/site, i.t.) had a limited effect (inhibition of 67 ± 10 %), being able only to partially reduce the mechanical hyperalgesia produced by nerve injury only at 1 h after treatment [F(5,60) = 3.4; p < 0.01].
Time–course curve of the effect of Tx3-5 (30 fmol/site, i.t.) or PBS treatment on mechanical hyperalgesia after partial sciatic nerve ligation (PSNL) in mice. B denotes baseline threshold before surgery, and B1 indicates basal mechanical threshold after surgery, but before treatment with Tx3-5 or PBS. Data are expressed as the means + S.E.M. of six to eight animals per group. Number sign p < 0.01 when compared with the basal mechanical threshold (B); two asterisks p < 0.01 when compared with the respective PBS-treated group; two-way ANOVA followed by Bonferroni’s post hoc test
Effects of Tx3-5 on the cancer-related pain model and morphine tolerance in mice
Fifteen days after the intraplantar inoculation of melanoma cells in C57BL/6 mice, we observed the development of mechanical hyperalgesia. The treatment with Tx3-5 (30 fmol/site, i.t.) substantially reduced the mechanical hyperalgesia induced by melanoma from 0.5 up to 2 h following i.t. administration [F(5,60) = 30; p < 0.0001; Fig. 5a], with a maximum inhibition of 96 ± 7 % at 1 h. Moreover, morphine (10 mg/kg, s.c.) also abolished the mechanical hyperalgesia induced by melanoma from 0.5 up to 1 h following i.t. injection [F(4,50) = 28; p < 0.0001; Fig. 5b], with a maximum inhibition of 100 % at 0.5 h, whereas the vehicle control group had no effect.
Antinociceptive effect of Tx3-5 (30 fmol/site, i.t.) or morphine (10 mg/kg, s.c.) at different time points in a cancer pain model (a, b) and in a cancer pain model in mice that have developed tolerance to morphine (c, d). Vertical bars represent the means + S.E.M. of six to seven animals per group (n = 6 to a and b; n = 6–7 to c and n = 7 to d). Number sign p < 0.01 when compared with the basal mechanical threshold (B, basal before injection of melanoma); tau symbol p < 0.01 when compared with the mechanical threshold before repeated morphine treatment (B1) or when compared with the respective saline-pretreated group; three asterisks p < 0.001 when compared with the respective saline or PBS group; two-way ANOVA followed by Bonferroni’s post hoc test. B2 (c, d) indicates basal mechanical threshold after tolerance induction
The treatment with morphine or vehicle was continued three times daily for 3 days with increasing doses to induce tolerance. On the fourth day (and approximately 12 h after the last injection of morphine), we measured the mechanical threshold of the animals again. The morphine-pretreated animals presented a higher degree of mechanical hyperalgesia when compared to the saline-pretreated group, or with the same animals before repeated morphine treatment (Fig. 5d; B2, basal mechanical threshold after tolerance induction). Thereafter, the mice received a challenge dose of morphine (10 mg/kg, s.c.) to confirm that morphine tolerance had been established. This dose of morphine, which previously abolished the mechanical hyperalgesia induced by melanoma at 0.5 and 1 h, was not capable of altering hyperalgesia in the animals that were pretreated with morphine, indicating the development of tolerance (Fig. 5d). Two hours after the morphine challenge, we administered Tx3-5 (30 fmol/site, i.t.) or PBS (5 μl/site, i.t.) to assess the effect of the peptide in morphine-tolerant animals. We observed that Tx3-5 (30 fmol/site, i.t.) was able to completely reverse the mechanical hyperalgesia induced by melanoma in morphine-tolerant animals [F(6,84) = 133; p < 0.0001; Fig. 5c] from 0.5 up to 2 h after Tx3-5 administration (inhibition of 100 % at 0.5 h).
Adverse effects induced by Tx3-5
We first verified the possible action of Tx3-5 (30 and 300 fmol/site, i.t.) on the locomotor activity of animals. At the dose where it produced antihyperalgesic effect (30 and 300 fmol/site, i.t.), Tx3-5 exhibited no effect on either the spontaneous or the forced locomotor activity of the animals, as assessed in the open-field and the rota-rod tests, respectively (Table 1). In contrast, morphine at an analgesic dose (10 mg/kg, s.c., used as positive control) increased the crossing number in the open-field test, but did not alter the number of falls in the rota-rod test, when compared with the PBS group (Table 1).
Next, we tested the possible toxicity of Tx3-5 at doses higher than used to cause antihyperalgesia. The i.t. administration of Tx3-5 at doses of 3000 or 10,000 fmol/site produced detectable adverse effects at 0.5, 2 and 24 h after injection, which included Straub’s tail, licking of the back and the tail and rapid and transient acceleration of respiratory movements as observed in Table 2. None of the animals demonstrated adverse effects at doses below 3000 fmol/site. The calculated 50 % toxic dose (TD50) for Tx3-5 was 1568 (1492–1650) fmol/site, i.t. To compare the toxic effect of Tx3-5 with a toxin that is clinically used to treat pain, we assessed the adverse effects produced by ω-conotoxin MVIIA. Intrathecal administration of high doses of ω-conotoxin MVIIA (30,000 and 100,000 fmol/site) produced licking of the back and the tail, acceleration of respiratory movements and spins around the body alternating with immobility in all tested animals at 0.5, 2 and 24 h after injection (Table 2). The dose of 10,000 fmol/site of ω-conotoxin MVIIA did not cause a visible behavioural change in the animals. The calculated TD50 value for ω-conotoxin MVIIA was 17,286 (16,976–17,603) fmol/site.
We also measured the IL-1β levels in the spinal cord of animals that received Tx3-5. The animals that received Tx3-5 (30 fmol/site, i.t.) only once, or during six consecutive days, contained cytokine levels below those detectable by the kit. Conversely, the animals that received a single administration of LPS (used as a positive control) contained elevated levels of IL-1β (750 ± 160 pg/mg).
Discussion
The venom of the Brazilian armed spider, P. nigriventer, is a rich source of biologically active peptides. In the present study, we verified that the intrathecal administration of the peptide Tx3-5 via the i.t. route produced antinociception in postoperative, neuropathic and cancer-related pain models. Tx3-5 also demonstrated an antihyperalgesic action in a cancer-related pain model using morphine-tolerant mice. Furthermore, the antinociceptive effects induced by Tx3-5 were observed at a far lower dose than the dose that induces adverse effects.
While physiological pain has an important protective function, some forms of pain occur in pathological conditions and can be a consequence of debilitating diseases [4, 30, 33]. Thus, an ideal analgesic drug should only inhibit pathological pain, without affecting physiological pain. We observed that intrathecal injection of Tx3-5 changed neither the noxious heat sensitivity nor the mechanical threshold, suggesting that this peptide does not affect physiological pain. However, morphine decreased heat nociception but did not alter the mechanical threshold of animals. Our findings agree with those of Scherrer et al. [62], who demonstrated that μ opioid receptors contribute to analgesia for thermal pain, but not mechanical pain.
Pain can manifest as hyperalgesia (increased sensitivity to painful stimuli) [33]. Thus, we investigated the effects of Tx3-5 in models of pathological and clinically relevant pain by measuring the degree of hyperalgesia. Initially, we evaluated the antinociceptive effect of intrathecal Tx3-5 in a postoperative pain model, demonstrating that it was able to prevent the development of mechanical hyperalgesia induced by a plantar incision, and reverse the established hyperalgesia produced by surgery up to 4 days postoperatively, by repeated treatment, without inducing tolerance to the antihyperalgesic effect or immunogenicity. Our results are in agreement with other studies that have demonstrated that L-type VSCC blockers exhibit antinociceptive action to varying degrees in inflammatory pain models (the later phase of the formalin test and the acetic acid test) [7, 43]. Our results also concur with those described by Wang et al. [79] and Souza et al. [70], whereby intrathecal ω-conotoxin MVIIA was able to prevent and reverse the postoperative mechanical hyperalgesia in rats and mice, with a similar level of efficacy. However, Tx3-5 is approximately 180 times more potent than ω-conotoxin MVIIA in inducing antinociception in the postoperative pain model, since the ID50 for i.t. ω-conotoxin MVIIA was approximately 3000 fmol/site [54]. Moreover, although intrathecal infusion of ω-conotoxin MVIIA is effective in reducing postoperative pain in patients, it can cause adverse effects at analgesic doses [2]. Thus, intrathecal injection of Tx3-5 might be a potentially interesting delivery modality in the development of new drugs for the management of postoperative pain, because Tx3-5 is effective in preventing and reversing postoperative nociception at doses that do not cause adverse effects.
We also evaluated the antinociceptive effect of the Tx3-5 in a cancer-related pain model. Pain is the most disruptive influence on the quality of life of cancer patients, and intrathecal infusion of ziconotide has been used as an analgesic in these patients [38, 73]. Moreover, literature data demonstrate that besides N-type VSCC blockers, L-type VSCC blockers are capable of inducing analgesia, and potentiate the analgesia of morphine, thus reducing the consumption of morphine in cancer patients [18, 59]. In the present study, we demonstrated that the intrathecal administration of Tx3-5 was able to reverse the mechanical hyperalgesia induced by intraplantar melanoma cells with an efficacy similar to that of systemically administered morphine. This result is relevant because morphine therapy is the most widely used therapy, and is the most effective, in controlling pain associated with cancer, according to the World Health Organization [48]. However, the chronic use of morphine and other opioids is limited by the development of analgesic tolerance [3, 8, 51]. Therefore, a search for new analgesic drugs and analgesic interventions to reduce the pain of cancer patients, including the patients who are refractory to conventional analgesics, is necessary. Unfortunately, there are no pre-clinical models to investigate the analgesic potential of new drugs which can be used for the treatment of cancer pain in patients who are refractory to opioids.
Additionally, we designed a protocol to evaluate the possible antinociception produced by Tx3-5 in animals that were tolerant to morphine that were submitted to a cancer-related pain model. As previously demonstrated [20, 60], the repeated injection of morphine produced tolerance to the analgesic effects in mice with melanoma 4 days after the treatment began. Moreover, we observed that the mechanical hyperalgesia 4 days after the repeated administration with morphine was more intense than after the repeated administration of the vehicle in mice with melanoma. The animals presented a more intense mechanical hyperalgesia than the hyperalgesia observed before the induction of morphine tolerance. This effect appears to be opioid-induced hyperalgesia and may complicate the clinical course of pain treatment in a patient receiving opioids [66]. However, intrathecal treatment with Tx3-5 was able to fully reverse the mechanical hyperalgesia induced by melanoma cell inoculation in morphine-tolerant mice. The ω-conotoxin MVIIA (ziconotide) is often used to treat patients with cancer pain who are refractory to opioid treatment [42]. Several studies have demonstrated that L-type VSCC blockers enhanced the analgesia and blocked the development of tolerance caused by opioids in experimental animals, both with and without cancer [1, 12, 28, 76], as well as in humans with cancer [58, 59]. Our results are accordant with those described by Rigo et al. [54], where intrathecal injection of the spider peptide Phα1β or ziconotide was able to reverse cancer-related hyperalgesia in mice with a similar efficacy. Thus, our model seems to be useful for assessing potential analgesic drugs that can treat cancer-related pain refractory to morphine.
Opioid tolerance and neuropathic pain have several common characteristics, such as changes in the expression of receptors and alterations of the properties of neuronal circuits [8, 80]. Therefore, we evaluated the antinociceptive effect of Tx3-5 on a neuropathic pain model. Chronic neuropathy, which is a debilitating condition that frequently results from partial injury to a peripheral nerve, resulting in the development of hyperalgesia, is often resistant to common therapeutic interventions [36, 80, 81]. In common with several other animal toxins, such as ω-conotoxin MVIIA or the P. nigriventer peptides Tx3-6 and Tx3-3, which demonstrate antihyperalgesic effects in neuropathic pain models [11, 54, 71, 72], we observed that Tx3-5 partially reversed the mechanical hyperalgesia induced by partial sciatic nerve ligation. Compared to the other very efficacious toxins, Tx3-5 had a limited efficacy to reverse the neuropathic hyperalgesia. In fact, several studies demonstrated that L-type VSCC is not as relevant to the maintenance of neuropathic pain as other types of VSCC, such as P/Q, N or R-type calcium channels [34, 40, 41]. Possibly, the mild antinociceptive effect presented by Tx3-5 in neuropathic pain is related to its selectivity for the subtypes of L-type channel, since L-type VSCC in the spinal dorsal horn plays an important role in pain processing, and that the maintenance of chronic neuropathic pain depends specifically on channels comprising L-type VSCC subtype CaV1.2 [14, 19]. Further, the effects of L-type VSCC blockers on nociception differ depending on the drug, dosage, route of administration and algesic test used [50]. However, the antihyperalgesic effect of Tx3-5 on partial sciatic nerve ligation is an important finding because the available analgesic drugs often have a limited therapeutic value in the management of neuropathic pain, due to their frequently observed adverse effects and low therapeutic index [81], whereas Tx3-5 has a lower efficacy but a much greater therapeutic index. Therefore, it is important to find new drugs that are more effective, and exhibit fewer adverse effects, than the current treatment modalities.
In addition to peptides that display antinociceptive properties, P. nigriventer venom has a diversity of potent toxins that cause neurotoxicity. Some of these toxins can be found in the fraction PhTx3 [9, 11, 21, 55, 72]. Similar to observations from previous experiments with Tx3-3 and Tx3-6 from P. nigriventer, and ω-conotoxins from the Conus genus [11, 37, 70, 72], intrathecal injection of Tx3-5 produced detectable adverse effects at high doses, but displayed a greater therapeutic index (80) than ω-conotoxin MVIIA, Tx3-3 or Tx3-6 (therapeutic indices of approximately 4, 10 or 16, respectively). From these results, it appears that Tx3-5 has a great advantage over the other toxins tested because Tx3-5 has antinociceptive effects at doses much lower than the doses that induce adverse effects. Moreover, Tx3-5 is about 300, 1000 and 7000 times more potent than ω-conotoxin MVIIA, Tx3-3 or Tx3-6, respectively, in relation to the analgesic effects observed in animal models. Additionally, Tx3-5 promoted its antinociceptive effects without producing detectable adverse effects, while morphine, used as a positive control, increased spontaneous locomotor activity. In contrast to the findings of Cordeiro et al. [9], who observed adverse effects such as paralysis in the posterior limbs, gradual decreases in movement and aggressive behaviour during 24 h of observation following Tx3-5 administration to mice by the intracerebroventricular (i.c.v.) route, our present study adverse effects displayed no similar neurological adverse effects at the therapeutic dose. It is probable that these discrepancies occurred because they used a dose of Tx3-5 33,000-fold higher (5 μg/mice) than that used in our study (30 fmol/site), and a different administration route (i.c.v.) to that used in our experiments (i.t.). Furthermore, we also verified that intrathecal administration of Tx3-5 did not cause immunogenicity, in contrast to the lipopolysaccharide positive control, which elevated the levels of interleukin-1β. This agrees with the results reported by Song et al. [69]. It is possible that the Tx3-5 did not trigger an immune response because the amount of this toxin used in the experiment was insufficient to do so. In order to assess the immunogenicity of the Tx3-5, a significant amount of this toxin would be required; this is very difficult to achieve because the Tx3-5 is the toxin with the lowest relative concentration in the venom of P. nigriventer [9].
The analgesic and toxic effects of the previously studied fraction PhTx3 purified peptides, or of ω-conotoxin MVIIA, appear to be mediated by a blockade of VSCC, such as P/Q and R-type calcium channel in the case of Tx3-3, or N-type calcium channel in the case of Tx3-6 and ω-conotoxin MVIIA [11, 31, 72, 77]. In contrast to Tx3-3 and Tx3-6, which are non-selective VSCC blockers, Tx3-5 is a selective and potent blocker of L-type VSCC in vitro [31, 32]. Assessing this mechanism in vivo, we verified that the L-type calcium channel activator Bay-K8644 was able to prevent the antihyperalgesic effect induced by Tx3-5, indicating that Tx3-5 exerts its effects, at least in part, on L-type calcium channels. Accordingly, previously published data showed that some blockers of the L-type VSCC exhibit antinociceptive effects in models of inflammatory and neuropathic pain in rodents [19, 22]. Conversely, Bay-K8644 was not able to alter postoperative hyperalgesia when administered alone, which is in accordance with other studies that demonstrated that intrathecal administration of Bay-K8644 was not capable of altering the nociception caused by formalin or acetic acid in mice [23, 25, 52], but it was able to prevent the antinociceptive effect of L-type VSCC blockers [27]. Since Bay-K8644 can also interact with molecular targets other than L-type calcium channels (i.e. TRPA1 channels) [16], we cannot discard a role of non-L calcium channels in the antihyperalgesic action of Tx3-5, a possibility that warrants further study. Notably, L-type calcium channel blockers have been considered important future potential agents to treat cardiovascular, psychiatric and neurological disease [82].
In conclusion, the peptide Tx3-5 demonstrated antinociceptive effects in clinically relevant pain models, which was complimented by a wide therapeutic index. It also displayed efficacy in opioid-tolerant animals. Together, these results demonstrate that the peptide Tx3-5 has characteristics that make it a potential candidate for the development of new analgesics for the treatment of both acute and chronic pathological pain conditions.
Abbreviations
- ANOVA:
-
Analysis of variance
- BSA:
-
Bovine serum albumin
- EDTA:
-
Ethylenediamine tetraacetic acid
- ID50 :
-
Inhibitory dose 50 %
- IL-1β:
-
Interleukin-1 beta
- i.p.:
-
Intraperitoneal
- i.pl.:
-
Intraplantar
- i.t.:
-
Intrathecal
- LPS:
-
Lipopolysaccharide
- PBS:
-
Phosphate-buffered saline
- PMSF:
-
Phenylmethylsulphonyl fluoride
- PSNL:
-
Partial sciatic nerve ligation
- s.c.:
-
Subcutaneous
- TD50 :
-
Toxic dose 50 %
- Tx3-5:
-
Peptide 3-5
- VSCC:
-
Voltage-sensitive calcium channels
References
Antkiewicz-Michaluk L, Michaluk J, Romańska IVJ (1993) Reduction of morphine dependence and potentiation of analgesia by chronic co-administration of nifedipine. Psychopharmacol (Berl) 111:457–64
Atanassoff PG, Hartmannsgruber MW, Thrasher J, Wermeling D, Longton W, Gaeta R, Singh T, Mayo M, McGuire D, Luther RR (2000) Ziconotide, a new N-type calcium channel blocker, administered intrathecally for acute postoperative pain. Reg Anesth Pain Med 25:274–278. doi:10.1053/xr.2000.5662
Ballantyne JC, Shin NS (2008) Efficacy of opioids for chronic pain: a review of the evidence. Clin J Pain 24:469–478
Le Bars D, Gozariu M, Cadden SW (2001) Animal models of nociception. Pharmacol Rev 53:597–652
Brenneis C, Coste O, Altenrath K, Angioni C, Schmidt H, Schuh CD, Zhang DD, Henke M, Weigert A, Brüne B, Rubin B, Nusing R, Scholich K, Geisslinger G (2011) Anti-inflammatory role of microsomal prostaglandin E synthase-1 in a model of neuroinflammation. J Biol Chem 286:2331–2342
Chaplan SR, Bach FW, Pogrel JW, Chung JM, Yaksh TL (1994) Quantitative assessment of tactile allodynia in the rat paw. J Neurosci Methods 53:55–63
Coderre TJ, Melzack R (1992) The role of NMDA receptor-operated calcium channels in persistent nociception after formalin-induced tissue injury. J Neurosci 12:3671–5
Corbett AD, Henderson G, Mcknight AT, Paterson SJ (2006) 75 years of opioid research: the exciting but vain quest for the Holy Grail. Br J Pharmacol 1:153–162
Cordeiro Mdo N, de Figueiredo SG, Valentim Ado C, Diniz CR, von Eickstedt VR, Gilroy J, Richardson M (1993) Purification and amino acid sequences of six TX3 type neurotoxins from the venom of the Brazilian “armed” spider Phoneutria nigriventer. Toxicon 31:35–42
Dahl JB, Kehlet H (2006) Postoperative pain and its management. In: McMahon SB, Klotzenburg M (eds) Wall and Melzack’s Textbook of pain. Elsevier Churchill Livingstone, Philadelphia, p 635–651
Dalmolin GD, Silva CR, Rigo FK, Gomes GM, Cordeiro MDN, Richardson M, Silva MAR, Prado MAM, Gomez MV, Ferreira J (2011) Antinociceptive effect of Brazilian armed spider venom toxin Tx3-3 in animal models of neuropathic pain. Pain 152:2224–2232. doi:10.1016/j.pain.2011.04.015
Dierssen M, Flórez JHM (1990) Calcium channel modulation by dihydropyridines modifies sufentanil-induced antinociception in acute and tolerant conditions. Naunyn Schmiedebergs Arch Pharmacol 342:559–65
Dixon WJ (1980) Efficient analysis of experimental observations. Annu Rev Pharmacol Toxicol 20:441–462
Dobremez E, Bouali-Benazzouz R, Fossat P, Monteils L, Dulluc J, Nagy FLM (2005) Distribution and regulation of L-type calcium channels in deep dorsal horn neurons after sciatic nerve injury in rats. Eur J Neurosci 21:3321–33
Dworkin RH, O’Connor AB, Backonja M, Farrar JT, Finnerup NB, Jensen TS, Kalso EA, Loeser JD, Miaskowski C, Nurmikko TJ, Portenoy RK, Rice AS, Stacey BR, Treede RD, Turk DC, Wallace MS (2007) Pharmacologic management of neuropathic pain: evidence-based recommendations. Pain 132:237–251
Fajardo O, Meseguer V, Belmonte CVF (2008) TRPA1 channels: novel targets of 1,4-dihydropyridines. Channels (Austin) 2:429–38
Farmer P, Frenk J, Knaul FM, Shulman LN, Alleyne G, Armstrong L, Atun R, Blayney D, Chen L, Feachem R, Gospodarowicz M, Gralow J, Gupta S, Langer A, Lob-Levyt J, Neal C, Mbewu A, Mired D, Piot P, Reddy KS, Sachs JD, Sarhan M, Seffrin JR (2010) Expansion of cancer care and control in countries of low and middle income: a call to action. Lancet 376:1186–1193. doi:10.1016/S0140-6736(10)61152-X
Filos KS, Goudas LC, Patroni OTV (1993) Analgesia with epidural nimodipine. Lancet 342:1047
Fossat P, Dobremez E, Bouali-Benazzouz R, Favereaux A, Bertrand SS, Kilk K, Léger C, Cazalets JR, Langel U, Landry M, Nagy F (2010) Knockdown of L calcium channel subtypes: differential effects in neuropathic pain. J Neurosci 30:1073–1085
Gao YJ, Cheng JK, Zeng Q, Xu ZZ, Decosterd I, Xu X, Ji RR (2009) Selective inhibition of JNK with a peptide inhibitor attenuates pain hypersensitivity and tumor growth in a mouse skin cancer pain model. Exp Neurol 219:146–55
Gomez MV, Kalapothakis E, Guatimosim C, Prado MA (2002) Phoneutria nigriventer venom: a cocktail of toxins that affect ion channels. Cell Mol Neurobiol 22:579–588. doi:10.1023/A:1021836403433
Gupta M, Singh J, Sood S, Arora B (2003) Mechanism of antinociceptive effect of nimodipine in experimental diabetic neuropathic pain. Exp Clin Pharmacol 25:49–52
Hagiwara K, Nakagawasai O, Murata A, Yamadera F, Miyoshi I, Tan-No K, Tadano T, Yanagisawa T, Iijima TMM (2003) Analgesic action of loperamide, an opioid agonist, and its blocking action on voltage-dependent Ca2+ channels. Neurosci Res 46:493–7
Hargreaves K, Dubner R, Brown F, Flores C, Joris J (1988) A new and sensitive method for measuring thermal nociception in cutaneous hyperalgesia. Pain 32:77–88
Horváth G, Brodacz BH-PU (2001) Role of calcium channels in the spinal transmission of nociceptive information from the mesentery. Pain 93:35–41
Hylden JL, Wilcox GL (1980) Intrathecal morphine in mice: a new technique. Eur J Pharmacol 67:313–316
Ishii K, Taira NYT (1985) Differential antagonism by Bay k 8644, a dihydropyridine calcium agonist, of the negative inotropic effects of nifedipine, verapamil, diltiazem and manganese ions in canine ventricular muscle. Br J Pharmacol 84:577–84
Michaluk J, Karolewicz B, Antkiewicz-Michaluk L, Vetulani J (1998) Effects of various Ca2q channel antagonists on morphine analgesia, tolerance and dependence, and on blood pressure in the rat. Eur J Pharmacol 352:189–197
King NB, Fraser V (2013) Untreated pain, narcotics regulation, and global health ideologies. PLoS Med 10:e1001411. doi:10.1371/journal.pmed.1001411
Kuner R (2010) Central mechanisms of pathological pain. Nat Med 16:1258–1266. doi:10.1038/nm.2231
Leão RM, Cruz JS, Diniz CR, Cordeiro MN, Beirão PS (2000) Inhibition of neuronal high-voltage activated calcium channels by the omega-phoneutria nigriventer Tx3-3 peptide toxin. Neuropharmacology 39:1756–67
Leão RM, Cruz JS, Diniz CR, Cordeiro MN, Beirão PLS (1997) Calcium channel blocking toxins in the venom of Phoneutria nigriventer. J Venom Anim Toxins 3:223
Loeser JD, Treede RD (2008) The Kyoto protocol of IASP basic pain terminology. Pain 137:473–477. doi:10.1016/j.pain.2008.04.025
Luvisetto S, Marinelli S, Panasiti MS, D’Amato FR, Fletcher CF, Pavone F, Pietrobon D (2006) Pain sensitivity in mice lacking the Cav2.1??1 subunit of P/Q-type Ca2+ channels. Neuroscience 142:823–832. doi:10.1016/j.neuroscience.2006.06.049
Makin MK (2001) Strong opioids for cancer pain. J R Soc Med 94:17–21
Malmberg AB, Basbaum AI (1998) Partial sciatic nerve injury in the mouse as a model of neuropathic pain: behavioral and neuroanatomical correlates. Pain 76:215–222
Malmberg AB, Yaksh TL (1994) Voltage-sensitive calcium channels in spinal nociceptive processing: blockade of N- and P-type channels inhibits formalin-induced nociception. J Neurosci 14:4882–4890
Mantyh PW, Clohisy DR, Koltzenburg M, Hunt SP (2002) Molecular mechanisms of cancer pain. Nat Rev Cancer 2:201–209
Marshall I, Weinstock M (1971) Quantitative method for assessing one symptom of the withdrawal syndrome in mice after chronic morphine administration. Nature 234:223–224
Matthews EA, Bee LA, Stephens GJ, Dickenson AH (2007) The Cav2.3 calcium channel antagonist SNX-482 reduces dorsal horn neuronal responses in a rat model of chronic neuropathic pain. Eur J Neurosci 25:3561–3569
Matthews EA, Dickenson AH (2001) Effects of spinally delivered N- and P-type voltage-dependent calcium channel antagonists on dorsal horn neuronal responses in a rat model of neuropathy. Pain 92:235–246
McGivern JG (2007) Ziconotide: a review of its pharmacology and use in the treatment of pain. Neuropsychiatr Dis Treat 3:69–85
Miranda HF, Bustamante D, Kramer V, Pelissier T, Saavedra HPC, Fernandez EPG (1992) Antinociceptive effects of Ca2+ channel blockers. Eur J Pharmacol 217:137–141
Nossaman VE, Ramadhyani U, Kadowitz PJ, Nossaman BD (2010) Advances in perioperative pain management: use of medications with dual analgesic mechanisms, tramadol and tapentadol. Anesth Clin 28:647–666
Oliveira SM, Drewes CC, Silva CR, Trevisan G, Boschen SL, Moreira CG, De Almeida CD, Da Cunha C, Ferreira J (2011) Involvement of mast cells in a mouse model of postoperative pain. Eur J Pharmacol 672:88–95. doi:10.1016/j.ejphar.2011.10.001
Oliveira SM, Silva CR, Wentz AP, Paim GR, Correa MS, Bonacorso HG, Prudente AS, Otuki MF, Ferreira J (2014) Antinociceptive effect of 3-(4-fluorophenyl)-5-trifluoromethyl-1H-1-tosylpyrazole. A Celecoxib structural analog in models of pathological pain. Pharmacol Biochem Behav 124:396–404. doi:10.1016/j.pbb.2014.07.005
Penn RD, Paice JA (2000) Adverse effects associated with the intrathecal administration of ziconotide. Pain 85:291–296. doi:10.1016/S0304-3959(99)00254-7
Pergolizzi J, Böger RH, Budd K, Dahan A, Erdine S, Hans G, Kress HG, Langford R, Likar R, Raffa RB, Sacerdote P (2008) Opioids and the management of chronic severe pain in the elderly: consensus statement of an International Expert Panel with focus on the six clinically most often used World Health Organization Step III opioids (buprenorphine, fentanyl, hydromorphone, met. Pain Pr 8:287–313
Pogatzki-Zahn EM, Zahn PK, Brennan TJ (2007) Postoperative pain—clinical implications of basic research. Best Pr Res Clin Anaesthesiol 21:3–13
Prado WA (2001) Involvement of calcium in pain and antinociception. Brazilian J Med Biol Res 34:449–461. doi:10.1590/S0100-879X2001000400003
Pud D, Cohen D, Lawental E, Eisenberg E (2006) Opioids and abnormal pain perception: new evidence from a study of chronic opioid addicts and healthy subjects. Drug Alcohol Depend 82:218–223
Quijada L, Germany A, Hernández CE (1992) Effects of calcium channel antagonists and Bay K 8644 on the analgesic response to pentazocine and U 50488H. Gen Pharmacol 23:837–4
Richardson M, Pimenta AM, Bemquerer MP, Santoro MM, Beirao PS, Lima ME, Figueiredo SG, Bloch C Jr, Vasconcelos EA, Campos FA, Gomes PC, Cordeiro MN (2006) Comparison of the partial proteomes of the venoms of Brazilian spiders of the genus Phoneutria. Comp Biochem Physiol - C Toxicol Pharmacol 142:173–187. doi:10.1016/j.cbpc.2005.09.010
Rigo FK, Dalmolin GD, Trevisan G, Tonello R, Silva MA, Rossato MF, Klafke JZ, Cordeiro MDN, Castro Junior CJ, Montijo D, Gomez MV, Ferreira J (2013) Effect of ω-conotoxin MVIIA and Phα1β on paclitaxel-induced acute and chronic pain. Pharmacol Biochem Behav 114-115:16–22. doi:10.1016/j.pbb.2013.10.014
Rigo FK, Trevisan G, Rosa F, Dalmolin GD, Otuki MF, Cueto AP, de Castro Junior CJ, Romano-Silva MA, Cordeiro MDN, Richardson M, Ferreira J, Gomez MV (2013) Spider peptide Phα1β induces analgesic effect in a model of cancer pain. Cancer Sci 104:1226–1230. doi:10.1111/cas.12209
Rosa F, Trevisan G, Rigo FK, Tonello R, Andrade EL, Cordeiro Mdo N, Calixto JB, Gomez MVFJ (2014) Phα1β, a peptide from the venom of the spider Phoneutria nigriventer shows antinociceptive effects after continuous infusion in a neuropathic pain model in rats. Anesth Analg 119:196–202
Sanford M (2013) Intrathecal ziconotide: a review of its use in patients with chronic pain refractory to other systemic or intrathecal analgesics. CNS Drugs 27:989–1002
Santillán R, Maestre JM, Hurle MAFJ (1994) Enhancement of opiate analgesia by nimodipine in cancer patients chronically treated with morphine: a preliminary report. Pain 58:129–132
Santillán R, Hurlé MA, Armijo JA, de los Mozos R, Flórez J (1998) Nimodipine‐enhanced opiate analgesia in cancer patients requiring morphine dose escalation: a double‐blind, placebo‐controlled study. Pain 76:17–26
Sasamura T, Nakamura S, Iida Y, Fujii H, Murata J, Saiki I, Nojima H, Kuraishi Y (2002) Morphine analgesia suppresses tumor growth and metastasis in a mouse model of cancer pain produced by orthotopic tumor inoculation. Eur J Pharmacol 441:185–191
Saulino M (2007) Successful reduction of neuropathic pain associated with spinal cord injury via of a combination of intrathecal hydromorphone and ziconotide: a case report. Spinal Cord 45:749–752
Scherrer G, Imamachi N, Cao Y-Q, Contet C, Mennicken F, O’Donnell D, Kieffer BL, Basbaum AI (2009) Dissociation of the opioid receptor mechanisms that control mechanical and heat pain. Cell 137:1148–1159. doi:10.1016/j.cell.2009.04.019
Schmidtko A, Lötsch J, Freynhagen R, Geisslinger G (2010) Ziconotide for treatment of severe chronic pain. Lancet 375:1569–1577. doi:10.1016/S0140-6736(10)60354-6
Scott DA, Wright CEAJ (2002) Actions of intrathecal x- conotoxins CVID, GVIA, MVIIA, and morphine in acute and neuropathic pain in the rat. Eur J Pharmacol 451:279–286
Da Silva JF, Castro-Junior CJ, Oliveira SM, Dalmolin GD, Silva CR, Vieira LB, Diniz DM, Cordeiro MDN, Ferreira J, Souza AH, Gomez MV (2015) Characterization of the antinociceptive effect of PhTx3-4, a toxin from Phoneutria nigriventer, in models of thermal, chemical and incisional pain in mice. Toxicon 108:53–61. doi:10.1016/j.toxicon.2015.09.043
Silverman SM (2009) Opioid induced hyperalgesia: clinical implications for the pain practitioner. Pain Physician 12:679–684
Skov MJ, Beck JC, De Kater AW, Shopp GM (2007) Nonclinical safety of ziconotide: an intrathecal analgesic of a new pharmaceutical class. Int J Toxicol 26:411–421. doi:10.1080/10915810701582970
Smith HS, Deer TR (2009) Safety and efficacy of intrathecal ziconotide in the management of severe chronic pain. Ther Clin Risk Manag 5:521–34
Song MJ, Wang YQ, Wu GC (2007) Lipopolysaccharide-induced protein kinase D activation mediated by interleukin-1beta and protein kinase C. Brain Res 11:19–27
de Souza AH, Lima MC, Drewes CC, da Silva JF, Torres KC, Pereira EM, de Castro Junior CJ, Vieira LB, Cordeiro MN, Richardson M, Gomez RS, Romano-Silva MA, Ferreira J, Gomez MV (2011) Antiallodynic effect and side effects of Phα1β, a neurotoxin from the spider Phoneutria nigriventer: comparison with ω-conotoxin MVIIA and morphine. Toxicon 58:626–633. doi:10.1016/j.toxicon.2011.09.008
De Souza AH, Castro CJ, Rigo FK, De Oliveira SM, Gomez RS, Diniz DM, Borges MH, Cordeiro MN, Silva MAR, Ferreira J, Gomez MV (2013) An evaluation of the antinociceptive effects of Phα1β, a neurotoxin from the spider phoneutria nigriventer, and ω-conotoxin MVIIA, a cone snail Conus magus toxin, in rat model of inflammatory and neuropathic pain. Cell Mol Neurobiol 33:59–67. doi:10.1007/s10571-012-9871-x
Souza AH, Ferreira J, Cordeiro MDN, Vieira LB, De Castro CJ, Trevisan G, Reis H, Souza IA, Richardson M, Prado MA, Prado VF, Gomez MV (2008) Analgesic effect in rodents of native and recombinant Ph alpha 1beta toxin, a high-voltage-activated calcium channel blocker isolated from armed spider venom. Pain 140:115–26. doi:10.1016/j.pain.2008.07.014
Staats PS, Yearwood T, Charapata SG, Presley RW, Wallace MS, Byas-Smith M, Fisher R, Bryce DA, Mangieri EA, Luther RR, Mayo M, McGuire D, Ellis D (2004) Intrathecal ziconotide in the treatment of refractory pain in patients with cancer or AIDS: a randomized controlled trial. Jama 291:63–70
Tonello R, Rigo F, Gewehr C, Trevisan G, Pereira EMR, Gomez MV, Ferreira J (2014) Action of Phα1β, a peptide from the venom of the spider Phoneutria nigriventer, on the analgesic and adverse effects caused by morphine in mice. J Pain 15:619–631. doi:10.1016/j.jpain.2014.02.007
Trevisan G, Rossato MF, Walker CIB, Klafke JZ, Rosa F, Oliveira SM, Tonello R, Guerra GP, Boligon AA, Zanon RB, Athayde ML, Ferreira J (2012) Identification of the plant steroid α-spinasterol as a novel transient receptor potential vanilloid 1 antagonist with antinociceptive properties. J Pharmacol Exp Ther 343:258–69. doi:10.1124/jpet.112.195909
Verma V, Mediratta PKSK (2001) Potentiation of analgesia and reversal of tolerance to morphine by calcium channel blockers. Indian J Exp Biol 39:636–42
Vieira LB, Kushmerick C, Hildebrand ME, Garcia E, Stea A, Cordeiro MN, Richardson M, Gomez MV, Snutch TP (2005) Inhibition of high voltage-activated calcium channels by spider toxin PnTx3-6. J Pharmacol Exp Ther 314:1370–1377
Villarinho JG, Oliveira SM, Silva CR, Cabreira TN, Ferreira J (2012) Involvement of monoamine oxidase B on models of postoperative and neuropathic pain in mice. Eur J Pharmacol 690:107–114. doi:10.1016/j.ejphar.2012.06.042
Wang Y-X, Pettus M, Gao D, Phillips C, Scott Bowersox S (2000) Effects of intrathecal administration of ziconotide, a selective neuronal N-type calcium channel blocker, on mechanical allodynia and heat hyperalgesia in a rat model of postoperative pain. Pain 84:151–158. doi:10.1016/S0304-3959(99)00197-9
Wang W, Gu J, Li YQ, Tao YX (2011) Are voltage-gated sodium channels on the dorsal root ganglion involved in the development of neuropathic pain? Mol Pain 7:16
Woolf CJ, Mannion RJ (1999) Neuropathic pain: aetiology, symptoms, mechanisms, and management. Lancet 353:1959–1964
Zamponi GW, Striessnig J, DA Koschak A (2015) The physiology, pathology, and pharmacology of voltage-gated calcium channels and their future therapeutic potential. Pharmacol Rev 67:821–70
Zimmermann M (1983) Ethical guidelines for investigations of experimental pain in conscious animals. Pain 16:109–110
Acknowledgments
This study was supported by the Instituto Nacional de Ciência e Tecnologia em Medicina Molecular MCT/CNPq, Coordenação de Aperfeiçoamento de Pessoal de Ensino Superior (CAPES), PRONEX and FAPEMIG. We also acknowledge the receipt of fellowships from CNPq, CAPES and FAPEMIG.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
The experiments were performed with the approval of the Ethics Committee of the Federal University of Santa Maria (process number 11/2010), and were carried out in accordance with the current guidelines for the care of laboratory animals.
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Oliveira, S.M., Silva, C.R., Trevisan, G. et al. Antinociceptive effect of a novel armed spider peptide Tx3-5 in pathological pain models in mice. Pflugers Arch - Eur J Physiol 468, 881–894 (2016). https://doi.org/10.1007/s00424-016-1801-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-016-1801-1