Abstract
Introduction
Pancreatoduodenectomy is the standard procedure for duodenal carcinoma of the third or fourth portion. As an alternative option, we developed a novel segmental resection (SR) with partial mesopancreatic and mesojejunal excision (pMME) that enhances radicality. In this report, the surgical technique with video and outcomes are described.
Method
We performed SR with pMME on seven consecutive patients with third or fourth duodenal carcinoma between 2009 and 2021. We divided the procedure into four sections, including (1) wide Kocher’s maneuver, (2) supracolic anterior artery-first approach, (3) dissection of the mesopancreas and mesojejunum, and (4) devascularization of the uncinate process and dissection of duodenum.
Result
Median operative time was 348 min (range, 222–391 min), and median blood loss was 100 mL (range, 30–580 mL). Major complications of Clavien-Dindo classification grade 3a or more occurred in one patient. All patients achieved R0 resections with 10 mm or more proximal margin. Six cases (85%) were alive without recurrence.
Conclusion
We developed a radical and safe procedure of SR with pMME as an alternative and less invasive approach for duodenal carcinoma of the third or fourth portion.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Duodenal carcinoma is a rare malignancy that accounts for 0.8% of gastrointestinal carcinoma cases [1]. Pancreatoduodenectomy (PD) is the standard procedure for duodenal carcinoma [2]; however, the high morbidity and mortality following PD make surgeons think twice before performing this invasive procedure.
Segmental resection (SR) is an alternative option in patients with duodenal carcinoma that results in reduced postoperative morbidity [3, 4]. Another advantage of SR compared with PD is the potential to preserve the pancreas. However, given that 57% of duodenal carcinoma with T1b or grater involved lymoh node metastasis [2], and lymph node metastasis is predictive of worse outcomes [2, 5,6,7], SR without lymph node dissection is not sufficient as a radical procedure. Furthermore, in patients with duodenal carcinoma of the third or fourth portion, systematic lymph node dissection is technically demanding due to the complex structure of the mesopancreas [8].
We developed a novel SR with partial mesopancreatic and mesojejunal excision (pMME) that balances radicality and safety for duodenal carcinoma of the third or fourth portion. In this report, the surgical technique and outcomes are described for seven patients who underwent SR with pMME.
Methods
Patients
We performed SR with pMME on seven consecutive patients with distal third or fourth duodenal carcinoma (five patients from the Cancer Institute Hospital and two patients from the Juntendo University Hospital) between 2009 and 2021. Our institutional review board approved this retrospective study with waived informed consent. Demographic data, clinical history, operation record, morbidity, mortality, and pathological data were reviewed.
Indications for SR with pMME
Duodenal carcinoma of the third or fourth portion away from the pancreas was an indication for SR with pMME. Tumor extension was confirmed using computed tomography and endoscopic ultrasonography preoperatively. Patients with the tumor deeper than T1b (submucosal invasion) were candidates for this procedure. Tumors with suspicious lymph node metastases around the pancreas head (hepatic, pyloric, or pancreaticoduodenal station) were excluded. Intraoperatively, lymph node metastases around the pancreas head were routinely explored, and PD was performed when lymph node metastases were confirmed by frozen section.
Surgical procedure
We divided the procedure into four sections, including (1) wide Kocher’s maneuver, (2) supracolic anterior artery-first approach, (3) dissection of the mesopancreas and mesojejunum, and (4) devascularization of the uncinate process and dissection of duodenum.
Wide Kocher maneuver (Fig. 1 and video Section 1)
After laparotomy with upper abdominal midline incision, abdominal exploration and a wide Kocher maneuver were conducted. A routine frozen section biopsy of para-aortic nodes was performed. And if lymph node metastasis around the pancreas head was suspected, a frozen section biopsy was done. The cholecystectomy and insertion of cystic duct tube was done to identify the location of the major papilla.
Supracolic anterior artery-first approach (Fig. 2 and video Section 2)
The superior mesenteric vein (SMV) was exposed and taped. The mesopancreatic dissection preserving the entire pl-SMA (level 2) was conducted by supracolic anterior artery-first approach, which we previously described as a surgical practice for pancreatoduodenectomy [9]. With a pinpoint rotation of the superior mesenteric artery (SMA) via retracting the pl-SMA, the common trunk of the inferior pancreatoduodenal artery (IPDA) and the first jejunal artery (JA) was exposed and ligated. With full mobilization, the SMA was exposed and taped. After isolation of the SMA, Treitz’s ligament was divided to the level of the left renal vein.
Dissection of the mesopancreas and mesojejunum (Fig. 3 and video Section 3)
In infracolic section, the mesosjejunum was dissected. The proximal jejunum supplied by the first or up to the second jejunal artery was resected following a central vascular ligation method [10, 11]. In supracolic section, the first jejunal vein was divided. The third and fourth duodenum with dissected mesopancreas was passed to the right side below the superior mesenteric vessels.
Devascularization of uncinate process and dissection of duodenum (Fig. 4 and video Section 4)
Tiny distal branches of the IPDA and IPDV to the pancreas head were carefully divided. The distal second portion of the duodenum was divided with enough surgical margin to preserve the major papilla. Reconstruction was performed by end-to-end or end-to-side duodenojejunal anastomosis with retrocolic or original retroperitoneal route.
Results
Table 1 summarizes the outcomes of seven patients. Median operative time was 348 min (range, 222–391 min), and median blood loss was 100 mL (range, 30–580 mL). Major complications of Clavien-Dindo classification grade 3a or more occurred in one patient (anastomotic bleeding), who was treated by arterial embolization. Pancreatic fistula of grade B as defined by the International Study Group on Pancreatic Fistula was found in one patient. Six patients with postoperative diarrhea treated by antidiarrheal drugs (4 patients with non-opioid antidiarrheal drugs, 2 patients with opioid antidiarrheal drugs), and all of them were controllable. The median number of lymph nodes resected was 21 (range, 10–46). All patients achieved R0 resections with 10 mm or more proximal margin. The median follow-up duration was 46 months (range, 2–75 months). Six cases (85%) were alive without recurrence. Case number 2, the most advanced stage, had recurrence with peritoneal and ovarian metastasis 11 months after surgery.
Discussion
In this report, we are the first to demonstrate the technique of SR with pMME in patients with duodenal carcinoma of the third or fourth portion. In seven patients, SR with pMME was safely performed, and the number of lymph nodes resected (LNR) ensured the radicality of this procedure.
Mesopancreatic excision is a part of the surgical procedures performed during PD for pancreatic carcinoma [12,13,14]. The concept of pMME is high ligation of the supplying arteries and en bloc resection of the mesenteries [10, 11]. In pMME, part of the mesopancreas, so-called PLPh1, is preserved, which may correspond to the concept of partial mesorectal excision [15]. Although the term “mesopancreas” remains controversial [16], it is helpful to understand the complex anatomy around the SMA. Embryonic rotation leads the mesopancreas to form spirally (Fig. 3). However, a de-rotated mesopancreas is a simple fan-shaped structure similar to the mesorectum shown in Fig. 4 [8]. The fact that fourth duodenal carcinomas spread to the superior mesenteric lymph nodes [2] suggests the mesopancreas is the mesentery of the fourth duodenum. Hence, pMME is a regional lymph node dissection of fourth duodenal carcinoma. A large population-based cohort study including 1611 patients with duodenal carcinoma demonstrated that SR had the smaller number of LNR (6.8 vs. 11 [P < 0.0001)) than conventional PD [17]. In our seven cases, the median number of LNR was 21. The number of LNR and the long-term outcomes warrant the oncological radicality of SR with pMME.
Wide Kocher maneuver. After mobilization of the duodenum and colon, the left renal vein and superior mesenteric artery were exposed. We routinely performed frozen section biopsy of para-aortic nodes (black asterisk) to confirm the contraindication of resection. Cholecystectomy and insertion of tube (black arrowhead) via the cystic duct were performed to identify the location of the major papilla. The site opposite the major papilla in the second duodenum was marked with suture thread (white arrowhead). SMA, superior mesenteric artery; RV, renal vein; IVC, inferior vena cava; Ao, aorta; Duo, duodenum
The supracolic anterior artery-first approach. The superior mesenteric vein was taped. Rotating the superior mesenteric artery with retraction of the plexus, the common trunk of the inferior pancreatoduodenal artery and the first jejunal artery as central vessel (white arrowhead) were exposed. SMV, superior mesenteric vein; pl-SMA, plexus of superior mesenteric artery
Dissection of the mesopancreas and mesojejunum. Treitz’s ligament and the top of the mesopancreas (white asterisk) were dissected (red dotted arrow). The white, black, and grey arrowheads and white arrow show the common trunk of the inferior pancreatoduodenal artery, the first jejunal artery, the second jejunal artery, the third jejunal artery, and the first jejunal vein trunk, respectively. The blue dotted arrow shows the en-bloc dissecting line of the mesojejunum (black asterisk) and mesopancreas (white asterisk) and preservation of the third jejunal artery (grey arrow). SMV, superior mesenteric vein; SMA, superior mesenteric artery
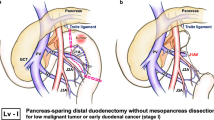
Devascularization of the uncinate process and dissection of the duodenum. The distal duodenum and proximal jejunum with dissected mesopancreas (white asterisk) and mesojejunum were passed to the right side below the superior mesenteric vessels and de-rotated (red arrow). Distal tiny branches of inferior pancreatoduodenal vessels (white arrowheads) lead to the uncinate process of the pancreas. After resection of these tiny branches, the partial mesopancreatic and mesojejunal excision were finished. Uncus, uncinate process of the pancreas
The devascularization of uncinate process (section four of the procedure) is a specific procedure of SR with pMME, which is different from that of PD. In this section, it is important to avoid injury of the major papilla by confirming the location with tube insertion, performed in Sect. 1. Additionally, an important point is to avoid tumor exposure that leads to worse outcomes [5,6,7, 18,19,20,21]. The horizontal and vertical margins are regulated by the location of the major papilla and the presence of pancreatic invasion, respectively. These margins need to be established with intraoperative frozen section analysis, and conversion to PD should be considered when tumor invasion is confirmed.
A recently published report of 16 patients with fourth duodenal tumor demonstrated the possibility of SR with lymph node dissection with a minimally invasive approach. In this report, four patients with fourth duodenal adenocarcinoma had laparoscopic SR with superior mesenteric lymph node dissection. Oncological outcomes of the four patients were feasible, achieving R0 resection and no recurrence during the follow-up period [22]. Nowadays, a robotic approach is being applied to complicated surgeries including PD. The next step may be to develop and promote robotic SR with pMME by investigating the safety and feasibility of the procedures.
In this report, SR with pMME was performed with no postoperative mortality. The major complication of Clavien-Dindo grade 3a or more was found in only one patient who had a severe comorbidity classed as ASA-PS 3. Available evidence revealed that surgery for duodenal carcinoma is associated with significant mortality. Cloyd et al. reported that the 90-day mortality rate of 1611 patients undergoing surgery for duodenal carcinoma was 12.5% [17]. Importantly, PD for the soft pancreatic parenchyma in patients with non-pancreatic tumors bears a risk of life-threatening pancreatic fistula [23]. In our series, pancreatic fistula of grade B occurred in one case, which may have been caused by minor injury to the pancreatic parenchyma during devascularization of the uncinate process. Although six patients had postoperative diarrhea, all of them were well controlled by antidiarrheal drugs. The key to SR with pMME for duodenal carcinoma is to preserve the pl-SMA not to compromise the health-related quality of life of patients because the dissection of pl-SMA significantly increases the risk of refractory diarrhea [24]. We recently reported that postoperative diarrhea is manageable with antidiarrheal drugs in patients undergoing radical PD for pancreatic adenocarcinoma. In that report, more than half of patients with diarrhea stopped using the antidiarrheal drugs, and the nutritional status recovered within 2 years.
Currently, there is no standardized chemotherapy for duodenal carcinoma, and surgical resection is the only effective treatment. Although a latest meta-analysis demonstrated the long-term outcomes following SR were not inferior to those after PD in patients with duodenal carcinoma, this study has certain drawbacks because tumor location and T categories were not taken into consideration for prognostic assessment [25]. We have to stress that the best practice for advanced duodenal carcinoma is still unknown. In this report, we provided with a new surgical choice for cancers of the third or fourth portion of the duodenum. Further investigation is needed to assess that, compared with radical PD, SR with pMMR does not impair the oncological radicality and yet improves the health-related quality of life by preserving the pancreas in patients with distal duodenal carcinoma.
Conclusion
We developed a radical and safe procedure of SR with pMME for duodenal carcinoma of the third or fourth portion.
Abbreviations
- PD:
-
Pancreatoduodenectomy
- SR:
-
Segmental resection
- pMME:
-
Partial mesopancreatic and mesojejunal excision
- SMV:
-
Superior mesenteric vein
- SMA:
-
Superior mesenteric artery
- IPDA:
-
Inferior pancreatoduodenal artery
- JA:
-
Jejunal artery
References
Overman MJ, Hu CY, Kopetz S, Abbruzzese JL, Wolff RA, Chang GJ (2012) A population-based comparison of adenocarcinoma of the large and small intestine: insights into a rare disease. Ann Surg Oncol 19(5):1439–1445. https://doi.org/10.1245/s10434-011-2173-6
Sakamoto T, Saiura A, Ono Y, Mise Y, Inoue Y, Ishizawa T et al (2017) Optimal lymphadenectomy for duodenal adenocarcinoma: does the number alone matter? Ann Surg Oncol 24(11):3368–3375. https://doi.org/10.1245/s10434-017-6044-7
Cloyd JM, George E, Visser BC (2016) Duodenal adenocarcinoma: advances in diagnosis and surgical management. World J Gastrointestinal Surg 8(3):212–221. https://doi.org/10.4240/wjgs.v8.i3.212
Tocchi A, Mazzoni G, Puma F, Miccini M, Cassini D, Bettelli E et al (1960) 2003 Adenocarcinoma of the third and fourth portions of the duodenum: results of surgical treatment. Archives Surg (Chicago, Ill) 138(1):80–5. https://doi.org/10.1001/archsurg.138.1.80
Poultsides GA, Huang LC, Cameron JL, Tuli R, Lan L, Hruban RH et al (2012) Duodenal adenocarcinoma: clinicopathologic analysis and implications for treatment. Ann Surg Oncol 19(6):1928–1935. https://doi.org/10.1245/s10434-011-2168-3
Lee SY, Lee JH, Hwang DW, Kim SC, Park KM, Lee YJ (2014) Long-term outcomes in patients with duodenal adenocarcinoma. ANZ J Surg 84(12):970–975. https://doi.org/10.1111/ans.12112
Solaini L, Jamieson NB, Metcalfe M, Abu Hilal M, Soonawalla Z, Davidson BR et al (2015) Outcome after surgical resection for duodenal adenocarcinoma in the UK. Br J Surg 102(6):676–681. https://doi.org/10.1002/bjs.9791
Sugiyama M, Suzuki Y, Nakazato T, Yokoyama M, Kogure M, Matsuki R et al (2020) Vascular anatomy of mesopancreas in pancreatoduodenectomy using an intestinal derotation procedure. World J Surg 44(10):3441–3448. https://doi.org/10.1007/s00268-020-05605-z
Inoue Y, Saiura A, Yoshioka R, Ono Y, Takahashi M, Arita J et al (2015) Pancreatoduodenectomy with systematic mesopancreas dissection using a supracolic anterior artery-first approach. Ann Surg 262(6):1092–1101. https://doi.org/10.1097/sla.0000000000001065
Inoue Y, Saiura A, Tanaka M, Matsumura M, Takeda Y, Mise Y et al (2016) Technical details of an anterior approach to the superior mesenteric artery during pancreaticoduodenectomy. J Gastrointestinal Surg : Official J Soci Surg Alimentary Tract 20(10):1769–1777. https://doi.org/10.1007/s11605-016-3214-z
West NP, Hohenberger W, Weber K, Perrakis A, Finan PJ, Quirke P (2010) Complete mesocolic excision with central vascular ligation produces an oncologically superior specimen compared with standard surgery for carcinoma of the colon. J Clin Oncol : Official J American Soc Clin Oncol 28(2):272–278. https://doi.org/10.1200/jco.2009.24.1448
Popescu I, Dumitrascu T (2011) Total meso-pancreas excision: key point of resection in pancreatic head adenocarcinoma. Hepatogastroenterology 58(105):202–207
Gockel I, Domeyer M, Wolloscheck T, Konerding MA, Junginger T (2007) Resection of the mesopancreas (RMP): a new surgical classification of a known anatomical space. World J Surgical Oncol 5:44. https://doi.org/10.1186/1477-7819-5-44
Gaedcke J, Gunawan B, Grade M, Szöke R, Liersch T, Becker H et al (2010) The mesopancreas is the primary site for R1 resection in pancreatic head cancer: relevance for clinical trials. Langenbeck’s Arch Surg 395(4):451–458. https://doi.org/10.1007/s00423-009-0494-8
Zaheer S, Pemberton JH, Farouk R, Dozois RR, Wolff BG, Ilstrup D (1998) Surgical treatment of adenocarcinoma of the rectum. Ann Surg 227(6):800–811. https://doi.org/10.1097/00000658-199806000-00003
Sharma D, Isaji S (2016) Mesopancreas is a misnomer: time to correct the nomenclature. J Hepatobiliary Pancreat Sci 23(12):745–749. https://doi.org/10.1002/jhbp.402
Cloyd JM, Norton JA, Visser BC, Poultsides GA (2015) Does the extent of resection impact survival for duodenal adenocarcinoma? Analysis of 1,611 cases. Ann Surg Oncol 22(2):573–580. https://doi.org/10.1245/s10434-014-4020-z
Nitta N, Ohgi K, Sugiura T, Okamura Y, Ito T, Yamamoto Y et al (2020) Prognostic impact of pancreatic invasion in duodenal carcinoma: a single-center experience. Ann Surg Oncol 27(11):4553–4560. https://doi.org/10.1245/s10434-020-08512-8
Mann K, Gilbert T, Cicconi S, Jackson R, Whelan P, Campbell F et al (2019) Tumour stage and resection margin status are independent survival factors following partial pancreatoduodenectomy for duodenal adenocarcinoma. Langenbecks Arch Surg 404(4):439–449. https://doi.org/10.1007/s00423-019-01779-w
Cecchini S, Correa-Gallego C, Desphande V, Ligorio M, Dursun A, Wargo J et al. 2012 Superior prognostic importance of perineural invasion vs. lymph node involvement after curative resection of duodenal adenocarcinoma. J Gastrointestinal Surger : Official J Soc Surg Alimentary Tract 16 1 113–20 discussion 20. https://doi.org/10.1007/s11605-011-1704-6
Sohn TA, Lillemoe KD, Cameron JL, Pitt HA, Kaufman HS, Hruban RH et al (1998) Adenocarcinoma of the duodenum: factors influencing long-term survival. J Gastrointestinal Surg : Official J Soc Surg Alimentary Tract 2(1):79–87. https://doi.org/10.1016/s1091-255x(98)80107-8
Bracale U, Pontecorvi E, Silvestri V, Cuccurullo D, D’Ambra M, Lionetti R et al (2021) Laparoscopic segmental resection for tumours of the Angle of Treitz: a challenging but feasible surgical option. Results Retrospective Case-Series Anal Updates Surg 73(1):179–86. https://doi.org/10.1007/s13304-020-00910-7
Fuks D, Piessen G, Huet E, Tavernier M, Zerbib P, Michot F et al (2009) Life-threatening postoperative pancreatic fistula (grade C) after pancreaticoduodenectomy: incidence, prognosis, and risk factors. Am J Surg 197(6):702–709. https://doi.org/10.1016/j.amjsurg.2008.03.004
Kuroki N, Ono Y, Sato T, Inoue Y, Oba A, Ito H et al (2022) Long-term outcome of patients with postoperative refractory diarrhea after tailored nerve plexus dissection around the major visceral arteries during pancreatoduodenectomy for pancreatic cancer. World J Surg. https://doi.org/10.1007/s00268-022-06457-5
Burasakarn P, Higuchi R, Nunobe S, Kanaji S, Eguchi H, Okada KI et al (2021) Limited resection vs. pancreaticoduodenectomy for primary duodenal adenocarcinoma: a systematic review and meta-analysis. Int J Clin Oncol 26(3):450–60. https://doi.org/10.1007/s10147-020-01840-510.1007/s10147-020-01840-5
Author information
Authors and Affiliations
Contributions
Study conception and design: R.I, M.Y, Y.T, Y.I, A.S. Acquisition of data: R.I. Analysis and interpretation of data: R.I, M.Y, A.S. Drafting of manuscript: R.I, M.Y. Critical revision of manuscript: Y.T, Y.I, A.S.
Corresponding author
Ethics declarations
Conflict of interest
Our institutional review board approved this retrospective study with waived informed consent. All authors have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 64459 KB)
Rights and permissions
About this article
Cite this article
Ito, R., Mise, Y., Takahashi, Y. et al. Segmental resection with partial mesopancreatic and mesojejunal excision (pMME) for duodenal carcinoma of the third or fourth portion. Langenbecks Arch Surg 407, 2143–2150 (2022). https://doi.org/10.1007/s00423-022-02569-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-022-02569-7