Abstract
Purpose Human breath analysis is proposed with increasing frequency as a useful tool in clinical application. We performed this study to find the characteristic volatile organic compounds (VOCs) in the exhaled breath of patients with idiopathic pulmonary fibrosis (IPF) for discrimination from healthy subjects. Methods VOCs in the exhaled breath of 40 IPF patients and 55 healthy controls were measured using a multi-capillary column and ion mobility spectrometer. The patients were examined by pulmonary function tests, blood gas analysis, and serum biomarkers of interstitial pneumonia. Results We detected 85 VOC peaks in the exhaled breath of IPF patients and controls. IPF patients showed 5 significant VOC peaks; p-cymene, acetoin, isoprene, ethylbenzene, and an unknown compound. The VOC peak of p-cymene was significantly lower (p < 0.001), while the VOC peaks of acetoin, isoprene, ethylbenzene, and the unknown compound were significantly higher (p < 0.001 for all) compared with the peaks of controls. Comparing VOC peaks with clinical parameters, negative correlations with VC (r =−0.393, p = 0.013), %VC (r =−0.569, p < 0.001), FVC (r = −0.440, p = 0.004), %FVC (r =−0.539, p < 0.001), DLco (r =−0.394, p = 0.018), and %DLco (r =−0.413, p = 0.008) and a positive correlation with KL-6 (r = 0.432, p = 0.005) were found for p-cymene. Conclusion We found characteristic 5 VOCs in the exhaled breath of IPF patients. Among them, the VOC peaks of p-cymene were related to the clinical parameters of IPF. These VOCs may be useful biomarkers of IPF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Idiopathic pulmonary fibrosis (IPF) is a chronic, progressive, and heterogeneous lung disease of unknown cause [1–4]. The main pathologic features of IPF is paraseptal fibrosis and honeycombing in the subpleural area, and mild inflammation with patchy lymphoplasmacytic interstitial infiltrate [1]. Recent studies about the pathogenesis of IPF have indicated that the fibrotic response is driven by abnormally activated alveolar epithelial cells [1, 2]. During chronic inflammation in the interstitium, epithelial cells, fibroblasts, lymphocytes, or macrophages interact with each other and release metabolic products that diffuse into the alveoli from the interstitium. These cells also produce many mediators that induce the formation of fibroblast foci, attraction of circulating fibrocytes, and stimulation of the epithelial to mesenchymal transition. Therefore, pathological process in IPF consists of complex interactions between epithelial and mesenchymal cells at the interstitium in the lung.
More than a thousand different volatile organic compounds (VOCs) have been detected at low concentrations in the normal human breath, with wide inter-individual variations [5]. Exhaled breath contains some endogenous molecules produced during metabolic processes in epithelial cells, mesenchymal cells, or blood-borne substances [5]. VOCs in exhaled breath have been reported as biomarkers for discriminating several respiratory diseases form healthy subjects [6–20]. However, few studies have examined the VOCs in IPF patients. As far as we known, there was one report that exhaled ethane was elevated in patients with interstitial lung disease and was correlated with clinical outcome [21].
Recently, the multi-capillary column (MCC), which is a variation of a capillary gas chromatography, has been used in combination with ion mobility spectrometer (IMS) [6, 10, 11, 19, 22–25]. MCC/IMS provides quick separation and highly selective analyses of VOCs from exhaled breath samples. The general operation of ion mobility spectrometry was reviewed recently by Cumeras et al. [26, 27].
The aim of this study was to find the characteristic VOCs in the exhaled breath of IPF patients for discrimination from healthy subjects using MCC/IMS, and to examine the relationship between the VOCs and the clinical parameters, including pulmonary function tests (PFT), blood gas analysis (BGA) and serum biomarkers of IPF.
Methods
Study Design and Study Subjects
The study had a cross-sectional case-control design. We recruited patients with interstitial pneumonia from Sapporo Medical University Hospital between December 2012 and May 2013, and radiologic findings including high-resolution computed tomography (HRCT) and clinical information from medical record were evaluated retrospectively. In total, 81 patients were identified: 25 had non-specific interstitial pneumonia (NSIP), 3 had desquamative interstitial pneumonia and 11 had collagen vascular disease-associated interstitial pneumonia (CVD-IP), two had other interstitial pneumonia; thus, 40 IPF patients were recruited into our study.
The diagnosis of IPF patients was made based on the ATS/ERS/JRS/ALAT statement [4]. In all patients, a medical history was obtained and physical examination, HRCT, PFT, BGA and serum biomarker measurements were performed. The diagnosis was performed by a multidisciplinary clinical-radiological-pathological review of the patient data. Patients with inflammatory diseases or malignancies were excluded. The control subjects were healthy volunteers recruited from our medical staff.
All patients and controls underwent VOC measurement in the exhaled breath. Informed written consent was obtained from all patients and the controls. This study was approved by the Institutional Review Board of Sapporo Medical University.
MCC/IMS
We used an ion mobility analyser for breath analysis. This device was composed of a breath-sampling unit (SpiroScout, Ganshorn Medizin Electronic, Niederlauer, Germany) and MCC/IMS (BioScout, B&S Analytik, Dortmund, Germany).
The exhaled breath from the subjects was collected through a mouthpiece connected to the SpiroScout, feeding the exhaled breath to the BioScout. At the end of the collection of exhaled breath, 10 mL of gas in the sample loop was given to the MCC (type Ov-5, Multichrom Ltd, Novosibirsk, Russia). In the MCC, the exhaled breath gas was sent through 1000 parallel capillaries, each with an inner diameter of 40 μm and a film thickness of 200 nm. After a 95 MBq 63Ni β-radiation source was applied to ionize the carrier gas, sample gas was fed into the IMS by the carrier gas (compressed air with grade 1, Taiyo Nippon Sanso Co, Japan).
The carrier gas was ionized by the 63Ni β-radiation source and ion–molecule reactions formed ionized molecules of the analytes through different types of collisions, including charge transfer reactions (chemical ionization, e.g. proton or electron transfer). The drift gas flowed from the Faraday-plate to the ionization region to prevent neutral substances from entering the drift region. Ionized analytes were detected on the Faraday plate at the end of the drift region of the IMS by directly measuring the charge. The drift times of the ions formed from the analytes were recorded.
Using an MCC as a pre-separation unit, IMS chromatograms were represented as a three-dimensional matrix as described in previous studies [19]. The intensity is related to the concentration of the analyte as well as other parameters, including drift time and retention time. Therefore, the detected metabolites are represented as a list of peaks described by the drift time (ms) and the retention time (s) according to their local maxima in the data matrix. Retention time and drift time were plotted on the x- and y-axes, respectively. The intensity of charge (V) measured at the Faraday plate was plotted on the z-axis as a measure of the analyte concentration within the breath sample. Each analyte was calibrated.
Measurement of VOCs
We measured VOCs in the exhaled breath of IPF patients and controls using MCC/IMS. The IPF patients and controls had fasted for at least 6 h before examination and stopped consuming alcohol on the previous day. Current smokers had not smoked for at least 24 h before examination, while IPF patients continued oral medication. Just before examination, all subjects promptly washed their mouths by gargling with pure water.
IPF patients and controls breathed through a disposable mouthpiece (Ganshorn Medizin Electronic) connected to a tube on the MCC/IMS. Collection of exhaled breath gas took for 30 s during respiration at rest. Tidal breathing of IPF patients and controls were approximately 10–15 times per minute. The MCC/IMS system was used to analyse all VOCs in the exhaled breath within 12 min.
After the breath samples were analysed by MCC/IMS, VOC peaks in the IPF patients and controls were determined using the software Visual Now 3.4 (B&S Analytik). The VOCs were identified by peak comparisons with reference data using the software Visual Now Version 110,801 (B&S Analytik).
PFT
A Chestac 9800 (Chest Co, Tokyo, Japan) was used for the PFT. We examined the following parameters: vital capacity (VC), predicted percentage of vital capacity (%VC), forced vital capacity (FVC), predicted percentage of FVC (%FVC), forced expiratory volume in one second to FVC ratio (FEV1/FVC), residual volume divided by total lung capacity (RV/TLC), and predicted percentage of RV to TLC (%RV/TLC). We measured diffusion capacity (DLco), predicted percentage of diffusion capacity (%DLco), DL divided by the alveolar volume (DLco/VA) and predicted percentage of DLco/VA (%DLco/VA) according to single-breath carbon monoxide uptake.
BGA and Serum Biomarkers
We measured arterial oxygen tension (PaO2), arterial carbon dioxide tension (PaCO2), alveolar-arterial difference of oxygen (AaDO2) by BGA, surfactant protein A (SP-A), surfactant protein D (SP-D), and Krebs von den Lungen-6 (KL-6) by sera in IPF patients.
Statistical Analysis
Differences of VOC peaks between the IPF patients and controls were assessed using the Mann–Whitney U test and the results were confirmed by the permutation test (n = 100). The multiple testing was corrected using the Benjamini-Hchberg method for false discovery rate (FDR). Significance was set at FDR-adjusted p-value less than 0.05.
Cut-off value of each VOC was determined by area under the receiver operating characteristic (ROC) curve. Diagnostic accuracy of significant VOC was expressed in sensitivity, specificity, positive predictive value, negative predictive value, accuracy and odds ratio. The bootstrap method was used to obtain 95% confidence intervals (CI) of area under the ROC curve. Correlations between clinical parameters and signal intensities of the significant VOC peaks were compared using the Spearman’s signed rank test. The effect of smoking on the results was examined in a logistic regression model or a linear regression model. In the logistic regression model and linear regression model, we used standardized values of VOCs which were transformed using the formula of z = (x − μ)/σ because the raw data of VOCs were extremely small.
The differences were considered statistically significant when the p-value was less than 0.05. Analyses were completed using IBM SPSS statistics version 22 (SPSS Inc., Chicago, IL, USA). In addition, AUC with 95% CI by bootstrap method and p-value by permutation tests were calculated using R 3.0.2 with ‘pROC’ package.
Results
VOC Peaks in IPF Patients
Forty IPF patients and 55 control subjects underwent measurement of VOC in the exhaled breath (Table 1). A total of 85 VOC peaks were detected and numbered in both IPF patients and the controls (Supplementary Fig. 1). In a comparison of the signal intensities of VOC peaks in both groups, significant differences were found in 5 VOCs: peaks 2, 5, 10, 18, and 67. According to the database of known VOCs measured by MCC/IMS, peaks 2, 5, 10, and 18 were p-cymene (IUPAC name: 1-methyl-4-(1-methylethyl)benzene), acetoin (3-hydroxy-2-butanone), isoprene (2-methyl-1,3-butadiene), and ethylbenzene, respectively (Table 2). However, the peak 67 compound was not identified in the database.
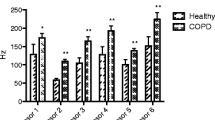
As shown in Fig. 1, the signal intensity of p-cymene was significantly lower in IPF patients than in controls (p < 0.001; Mann–Whitney U test). In contrast, the signal intensities of acetoin, isoprene, ethylbenzene, and the peak 67 compound were significantly higher in IPF patients than in controls (p < 0.001 for all compounds).
Comparison between patients with IPF and control subjects in significant 5 VOC peaks including p-cymene, acetoin, isoprene, ethylbenzene and an unknown VOC. Box plots show the signal intensity of VOC peaks in the ion mobility spectrometry (MCC/IMS). The box represents the 25th and 75th percentiles, the whiskers represent the extreme value, the lines in the box represent the median and the circle represents the outlier
To identify the optimal cut-off value of each significant VOCs for IPF patients, ROC analysis were performed using threshold value. As a result, each significant VOC cut-off value was provided (Supplementary Fig. 2). Using the value, we classified each significant VOC into four groups; true positive, true negative, false positive and false negative groups. P-cymene showed a specificity of 0.5 and a high specificity of 0.909 with an area under the curve of 0.803. Isoprene showed a high sensitivity of 0.825 and a specificity of 0.836 with an area under the curve of 0.810.
As our study subjects include current and former smokers, we evaluated influence of smoking factor using the multivariate analysis. A logistic regression model demonstrated that these results were not influenced by smoking factor and 5 VOCs had a statistically significant impact on discrimination of IPF from controls (Supplementary Table 1).
Correlation Between VOC Peaks and Clinical Parameters
We compared the signal intensities of 5 VOCs with clinical parameters in IPF patients. For p-cymene, acetoin, and ethylbenzene, we found significant correlations between the VOC peaks and several clinical parameters including PFT, BGA, and KL-6 (Table 3). In p-cymene, we found negative correlations with VC (r = −0.393, p = 0.013), %VC (r = −0.569, p < 0.001), FVC (r = −0.440, p = 0.004), %FVC (r = −0.539, p < 0.001), DLco (r = −0.394, p = 0.018), and %DLco (r = −0.413, p = 0.008) and a positive correlation with KL-6 (r = 0.432, p = 0.005) (Fig. 2). In acetoin, there was a negative correlation with PaO2 (r = −0.359, p = 0.027) and a positive correlation with AaDO2 (r = 0.369, p = 0.023). In ethylbenzene, there was a negative correlation with %DLCO/VA (r = −0.347, p = 0.038). However, there was no correlation between clinical parameters and both isoprene and the peak 67 compound.
Correlations of the signal intensities of p-cymene with pulmonary function tests and KL-6 in IPF patients. There are negative correlations with VC, %VC, %FVC, DLco, DLco/VA and %DLco/VA, and a positive correlation with serum levels of KL-6. The unbroken line and the dotted line indicate the regression line and 95% confidence intervals, respectively
We examined the influence of smoking factor on the results by multivariate analysis. A linear regression model showed that the results of p-cymene were not influenced by smoking factor (Supplementary Table 2). However, both acetoin and ethylbenzene had a significant association with smoking factor as a confounder.
Discussion
In this study, we found 5 characteristic VOCs in IPF patients compared with controls by using MCC/IMS. Of the 5 VOCs, 4 were identified as p-cymene, acetoin, isoprene and ethylbenzene. However, peak 67 could not be identified. VOC peaks of p-cymene was significantly decreased, whereas VOC peaks of acetoin, isoprene, ethylbenzene and the peak 67 were significantly increased in IPF patients. Therefore, we thought that p-cymene was a negative biomarker and the others were positive biomarkers of IPF. These VOCs may be useful for discrimination of IPF patients from healthy subjects.
Although the source of the VOCs of IPF is unclear, these compounds are thought to be produced from interstitial inflammation and fibrosis during or after metabolism of epithelial and mesenchymal cells. Isoprene is an endogenous VOC that is a byproduct of cholesterol biosynthesis. Foster et al. [28] demonstrated isoprene in exhaled breath showed a significant increase following a temporally decrease after exposing to ozone which causes oxidative stress. They speculated that reactive oxygen species (ROS) as free radicals damaged cell membranes and epithelial membrane repair mechanisms would increase cholesterol biosynthesis in order to replenish the cholesterol fraction within cellular membrane. Therefore, epithelial membrane repair during persistent inflammation in IPF patients might lead to an increase of cholesterol biosynthesis focally in the lung and isoprene as intermediate would be increased in the breath. Acetoin is a flavoring chemical, which is widely used for food, cigarette, cosmetics, detergent, and so on. Jaiali et al. [29] reported acetoin was a significantly higher VOC in exhaled breath of workers exposed to silica and silicosis patients compared to the healthy subjects. Silicosis is considered to be an oxidative stress disease that can lead to the development of lung fibrosis and lung cancer. Increased oxidative DNA damage has been detected in IPF patients as well as workers with silicosis [30]. Acetoin in exhaled breath might be produced as a result of cellular damage due to ROS. In addition, ethylbenzene has carcinogenic activity and is considered to be a VOC breath biomarker of lung cancer. Experimental exposure to ethylbenzene resulted in an increase of lung tumor in mice [31, 32]. Similar to ethylbenzene, both isoprene [33] and acetoin [33, 34] are interestingly reported as a VOC breath biomarker of lung cancer [34]. These VOCs might be related with complication of lung cancer in IPF. On the other hand, p-cymene, a monoterpene and a major constituent of essential oils of various species of plants, has an antioxidant potential. In mouse model of lipopolysaccharide-induced acute lung injury, intraperitoneal preconditioning with p-cymene resulted in a significant reduction of proinflammatory cytokines, water gain, inflammatory cell infiltration, and lung tissue myeloperoxidase activity [35]. p-Cymene might play a protective effect against progression of IPF and a decrease of p-cymene might promote interstitial inflammation and fibrosis.
Of the 5 VOCs, p-cymene, acetoin, and ethylbenzene were correlated with several clinical parameters of interstitial pneumonia. The signal intensities of p-cymene revealed a negative correlation with both the decrease in spirometric testing including VC, %VC, FVC, and %FVC and decline in diffusion capacity including DLco, %DLco, DLco/VA, and %DLco/VA. These findings indicate the signal intensities of p-cymene might represent the deterioration of pulmonary function. Moreover, the signal intensities of p-cymene revealed a positive correlation with serum levels of KL-6, suggesting a relationship with the extent of alveolitis followed by fibrosis in the lung. P-cymene may be clinically useful for evaluating alveolitis in IPF patients. However, the signal intensities of p-cymene were paradoxically significantly higher in control subjects than in IPF patients. For the reason, we speculated that the production amount or metabolism of p-cymene in IPF patients differed from that in controls. On the other hand, acetoin showed a positive correlation with PaO2 and a negative correlation with AaDO2. Ethylbenzol showed a negative correlation with %DLco. Acetoin and ethylbenzene were thought to be related to oxygenation in the lung. In these results, we examined the influence of smoking factor on p-cymene, acetoin, and ethylbenzene using a linear regression model. The multivariate analysis showed a significant correlation between p-cymene and clinical parameters.
There were several limitations in our study. First, although isoprene is endogenously produced during cholesterol synthesis, there is no exact knowledge about biochemical pathway for the production of endogenous acetoin, ethylbenzene and p-cymene in human at present. Second, serial measurement of VOCs was not performed. The VOC measurement was only conducted once. Variability in VOCs during the course of IPF remains unknown. VOC may vary with the progression of IPF. Third, pathologic confirmation was not performed in our study. IPF lesions are distributed unevenly in the lung, and the degree varies depending on the site [2–4]. The relationship between pathologic changes and VOCs may be important for speculating the sources of the VOCs. Fourth, age distribution of the controls is different from that of IPF group. We were not able to compare IPF group with age-matched controls. We need further investigation between IPF and age-matched control group in the future. Fifth, MCC/IMS did not identify all VOCs in the exhaled breath. We could not identify the peak 67 compound because there was no matching material in the database. A complete database is expected to be established in the future.
Since the measurement of VOCs using MCC/IMS is noninvasive and simple [22, 23, 25], patients with impaired pulmonary function can be easily measured. The advantages of MCC/IMS are its ability to detect very low concentrations of compounds without pre-concentration and the short time required for analysis. In contrast to other methods, MCC/IMS enables the detection of a large number of VOCs in exhaled breath. Analysis of VOCs in exhaled breath using MCC/IMS may be a clinically useful screening for IPF patients.
Conclusions
We found characteristic 5 VOCs in the exhaled breath of IPF patients. Among them, the VOC peak of p-cymene was related to the clinical parameters. These VOCs may be useful biomarkers of IPF.
References
King TE Jr, Pardo A, Selman M (2011) Idiopathic pulmonary fibrosis. The Lancet 378:1949–1961
Harari S, Caminati A (2010) IPF: new insight on pathogenesis and treatment. Allergy 65:537–553
Gross TJ, Hunninghake GW (2001) Idiopathic pulmonary fibrosis. N Engl J Med 345:517–525
Raghu G, Collard HR, Egan JJ et al (2011) An official ATS/ERS/JRS/ALAT statement: idiopathic pulmonary fibrosis: evidence-based guidelines for diagnosis and management. Am J Respir Crit Care Med 183:788–824
Rattray NJ, Hamrang Z, Trivedi DK et al (2014) Taking your breath away: metabolomics breathes life in to personalized medicine. Trends Biotechnol 32:538–548
Westhoff M, Litterst P, Maddula S et al (2010) Differentiation of chronic obstructive pulmonary disease (COPD) including lung cancer from healthy control group by breath analysis using ion mobility spectrometry. Int J Ion Mobility Spectrum 13:131–139
Van Berkel JJ, Dallinga JW, Möller GM et al (2010) A profile of volatile organic compounds in breath discriminates COPD patients from controls. Respir Med 104:557–567
Besa V, Teschler H, Kurth I et al (2015) Exhaled volatile organic compounds discriminate patients with chronic obstructive pulmonary disease from healthy subjects. Int J Chron Obstruct Pulmon Dis 10:399–406
Dragonieri S, Schot R, Mertens BJ et al (2007) An electronic nose in the discrimination of patients with asthma and controls. J Allergy Clin Immunol 120:856–862
Bunkowski A, Boedeker B, Bader S et al (2009) MCC/IMS signals in human breath related to sarcoidosis: results of a feasibility study using an automated peak finding procedure. J Breath Res 3:046001
Westhoff M, Litterst P, Freitag L et al (2007) Ion mobility spectrometry in the diagnosis of sarcoidosis: Results of a feasibility study. J Physiol Pharmacol 58:739–751
Phillips M, Cataneo RN, Condos R et al (2007) Volatile biomarkers of pulmonary tuberculosis in the breath. Tuberculosis 87:44–52
Phillips M, Basa-Dalay V, Blais J et al (2012) Point-of-care breath test for biomarkers of active pulmonary tuberculosis. Tuberculosis 92:314–320
Kamboures MA, Blake DR, Cooper DM et al (2005) Breath sulfides and pulmonary function in cystic fibrosis. Proc Natl Acad Sci USA 102:15762–15767
McGrath LT, Patrick R, Mallon P et al (2000) Breath isoprene during acute respiratory exacerbation in cystic fibrosis. Eur Respir J 16:1065–1069
Cakir Y, Métraillier L, Baumbach JI et al (2014) Signals in asbestos related diseases in human breath—preliminary results. Int J Ion Mobil Spec 17:87–94
Philips M, Cataneo RN, Cummin ARC et al (2003) Detection of lung cancer with volatile markers in the breath. Chest 123:2115–2123
Machado RF, Raskowski D, Deffenderfer O et al (2005) Detection of lung cancer by sensor array analyses of exhaled breath. Am J Respir Crit Care Med 171:1286–1291
Westhoff M, Litterst P, Freitag L et al (2009) Ion mobility spectrometry for the detection of volatile organic compounds in exhaled breath of patients with lung cancer: results of a pilot study. Thorax 64:744–748
Darwiche K, Baumbach JI, Sommerwerck U et al (2011) Bronchoscopically obtained volatile biomarkers in lung cancer. Lung 189:445–452
Kanoh S, Kobayashi H, Motoyoshi K (2005) Exhaled ethane: an in vivo biomarker of lipid peroxidation in interstitial lung diseases. Chest 128:2387–2392
Buszewski B, Grzywinski D, Ligor T et al (2013) Detection of volatile organic compounds as biomarkers in breath analysis by different analytical techniques. Bioanalysis 5: 2287–2306
Baumbach JI (2009) Ion mobility spectrometry coupled with multi-capillary columns for metabolic profiling of human breath. J Breath Res 3:034001
Hauschild AC, Schneider T, Pauling J et al (2012) Computational methods for metabolomic data analysis of ion mobility spectrometry data-reviewing the state of art. Metabolites 2: 733–755
Fink T, Baumbach JI, Kreuer S (2014) Ion mobility spectrometry in breath research. J Breath Res 8:027104
Cumeras R, Figueras E, Davis CE et al (2015) Review on ion mobility spectrometry. Part 1: current instrumentation. Analyst 140:1376–1390
Cumeras R, Figueras E, Davis CE et al (2015) Review on ion mobility spectrometry. Part 2: hyphenated methods and effects of experimental parameters. Analyst 140:1391–1410
Foster WM, Jiang L, Stetkiewicz PT et al (1996) Breath isoprene: temporal changes in respiratory output after exposure to ozone. J Appl Physiol 80:706–710
Jalali M, Zare Sakhvidi MJ, Bahrami A et al (2016) Oxidative stress biomarkers in exhaled breath of workers exposed to crystalline silica dust by SPME-GC-MS. J Res Health Sci 16:153–161
Cheresh P, Kim SJ, Tulasiram S et al (2013) Oxidative stress and pulmonary fibrosis. Biochim Biophys Acta 1832: 1028–1040
Chan PC, Haseman JK, Mahleri J et al (1998) Tumor induction in F344/N rats and B6C3F1 mice following inhalation exposure to ethylbenzene. Toxicol Lett 99:23–32
Saghir SA, Zhang F, Rick DL et al (2010) In vitro metabolism and covalent binding of ethylbenzene to microsomal protein as a possible mechanism of ethylbenzene-induced mouse lung tumorigenesis. Regul Toxicol Pharmacol 57:129–135
Saalberg Y, Wolff M (2016) VOC breath biomarkers in lung cancer. Clin Chim Acta 459:5–9
Song G, Qin T, Liu H et al (2010) Quantitative breath analysis of volatile organic compounds of lung cancer patients. Lung Cancer 67:227–231
Xie G, Chen N, Soromou LW et al (2012) p-Cymene protects mice against lipopolysaccharide-induced acute lung injury by inhibiting inflammatory cell activation. Molecules 17:8159–8173
Acknowledgements
The authors thank Mr. Yusuke Yonemura (Harada Corp, Osaka, Japan) for his technical supports. A part of the work on this paper (JIBB) has been supported by Deutsche Forschungsgemeinschaft (DFG) within the Collaborative Research Center (Sonderforschungsbereich) SFB 876 “Providing Information by Resource-Constrained Analysis”, project TB1 “Resource-Constrained Analysis of Spectrometry Data”.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared no conflicts of interest in connection with this article.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in this study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yamada, Yi., Yamada, G., Otsuka, M. et al. Volatile Organic Compounds in Exhaled Breath of Idiopathic Pulmonary Fibrosis for Discrimination from Healthy Subjects. Lung 195, 247–254 (2017). https://doi.org/10.1007/s00408-017-9979-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-017-9979-3