Abstract
The base of the tongue has been recognized as a significant site of obstruction in patients with obstructive sleep apnea (OSA). Our aim was to determine the independent predictors of surgical success in tongue base resection combined with lateral pharyngoplasty for OSA. Thirty-one OSA patients who underwent endoscopie-guided coblator or transoral robotic tongue base resection in combination with lateral pharyngoplasty for the treatment of retroglossal obstruction between March 2012 and December 2015 were enrolled in this study. Retroglossal obstruction was identified by preoperative nasopharyngoscopy with drug-induced sleep endoscopy and/or Müller’s maneuver in supine position. Patients were divided into success and failure groups according to surgical outcome (postoperative apnea–hypopnea index (AHI) less than 20 and reduction more than 50% in baseline AHI). Physical profile, polysomnography, cephalometry parameters, and drug-induced sleep endoscopy and/or Müller’s maneuver findings were compared between the two groups. Tonsil grade (p = 0.002), lateral oropharyngeal wall collapse on Müller’s maneuver (p = 0.002), and AHI during rapid eye movement (REM AHI) (p = 0.038) were significantly higher in the success group than in the failure group. Tongue base collapse was more evident in the failure group than in the success group when patients open their mouth. (p = 0.037) Bigger tonsil size and higher REM AHI are favorable predictive factors, even in multilevel surgery such as tongue base resection, whereas tongue base collapse during mouth opening may be an unfavorable predictive factor.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Obstructive sleep apnea (OSA) is a chronic disease affecting at least 2–4% of the adult population [1] and leading to increased risk of cardiovascular or metabolic diseases [2]. Continuous positive airway pressure (CPAP) is the first-line treatment for OSA, but patients with poor compliance for CPAP or other types of conservative treatment should be considered for surgery [3]. The main target of sleep apnea surgery has been the oropharynx, including tonsils, uvula, and soft palate. However, the better understanding of the pathophysiology of OSA (e.g., that the base of the tongue is a major contributor to OSA) and the improvement of diagnostic methods has led to the development of multi-level surgery, which targets both oropharyngeal and retroglossal obstruction. Surgery options for retroglossal obstruction include midline partial glossectomy, genioglossus advancement, hyoid suspension, maxillomandibular advancement, tongue base radiofrequency channeling or resection, and transoral robotic surgery [4]. The aim of these surgical procedures is to enlarge the airway space and/or increase the muscular tension around the retroglossal region either by reducing soft tissue volume or by altering the facial skeleton framework. However, because of its deep-seated location, surgical intervention into the retroglossal region is still challenging, and the predictors of surgical success remain unknown. Surgical criteria for base-of-tongue surgery are ambiguous, which may explain the heterogeneity of patient populations across studies and the disparity in surgical success rates. Moreover, surgical outcome varies from surgeon to surgeon, even if the surgical procedure is the same. Therefore, the choice of the optimal surgical procedure remains controversial. Recently, techniques for downsizing the tongue volume, such as in tongue base resection, have become very popular as the surgical devices develop.
The aim of this study was to identify predictors of surgical outcomes in tongue base resection with lateral pharyngoplasty. This paper describes the physical, radiologic, and polysomnographic findings of OSA patients who underwent a combination of tongue base resection and lateral pharyngoplasty.
Materials and methods
Participants
This study included 31 consecutive OSA patients who underwent endoscope-guided coblator or transoral robotic tongue base resection in combination with lateral pharyngoplasty for the treatment of retroglossal obstruction at the Department of Otorhinolaryngology at Severance Hospital between March 2012 and December 2015. The mean age of all patients was 40.2 ± 2.1 years, and male:female ratio was 27:4. Retroglossal obstruction was determined by drug-induced sleep endoscopy (DISE) and/or preoperative fiberoptic nasopharyngoscopy with Müller’s maneuver in supine position. All patients were informed of other conservative treatment modalities, including CPAP and oral appliance, before surgery. Patients who had not yet undergone postoperative polysomnography were excluded from the analysis.
Anthropometric characteristics, physical findings of oral cavity (tonsillar hypertrophy, tongue size using modified Mallampati grading, and Friedman scoring [5]), and standardized lateral cephalometric radiographic data [6, 7] were collected. All data were retrospectively analyzed. This study was approved by the institutional review board (IRB) at Yonsei University College of Medicine (IRB No.4-2014-0863).
Tongue base resection procedure
Under general anesthesia via a nasotracheal tube, all patients underwent the tongue base resection procedure simultaneously combined with lateral pharyngoplasty for palatal surgery. Tracheostomy was not performed in all patients. Twenty patients underwent endoscope-assisted coblator tongue base resection using an endoscope-holding system as recently reported by us [8]. For the remaining 11 patients, transoral robotic tongue base resection was performed using the da Vinci surgical system (Intuitive Surgical Inv., Sunnyvale, CA) [9, 10]. All surgical procedures were performed by a single surgeon. Their representative intraoperative images are shown in Fig. 1.
Surgical criteria for tongue base resection
Preoperative nasopharyngoscopic examinations were performed using a Pentax FNL-10RP3 flexible nasopharyngoscope (Laryngograph Ltd, London, UK) and all patients were investigated with Müller’s maneuver in the awake state and supine position at the outpatient office as described previously [11–13]. After finishing Müller’s maneuver, patients were asked to close their mouth with full expiration through the nose to observe tongue base collapse in the relaxed condition. In addition, tongue base obstruction was also checked during mouth opening with mouth breathing. The patient selection criteria for tongue base resection were as follows. (i) Partial or complete retroglossal obstruction on DISE and/or Muller’s maneuver. (ii) Partial or complete retroglossal obstruction on full expiration and relaxation with closed mouth on nasopharyngoscopy. (iii) Partial or complete retroglossal obstruction by backward movement of tongue when opening mouth on nasopharyngoscopy. (iv) Moderate/severe OSA (AHI > 15).
Outcome measurement
All patients underwent pre- and postoperative (at least 3 months after surgery) overnight polysomnography [14]. To determine predictors of surgical success, patients were divided into two groups: success and failure. Success criteria were defined as postoperative apnea–hypopnea index (AHI) less than 20 and reduction more than 50% in baseline AHI [15]. Physical profile, polysomnography and cephalometry data, and DISE and/or Müller’s maneuver findings were compared between the two groups.
Statistics
All continuous data are displayed as means ± standard deviation. Paired t test, Mann–Whitney test, and Pearson’s correlation test were performed using IBM SPSS Statistics software (version 23). A p value < 0.05 was considered statistically significant.
Results
During the average follow-up period of 24.2 months, there were no significant complications, such as postoperative respiratory difficulties or serious postoperative bleeding from the tongue base, which would require emergent bleeder ligation surgery.
Postoperative polysomnography study showed improved sleep quality for the majority of patients. Their mean postoperative AHI was significantly reduced (44.8–17.7 events/h, p < 0.0001; Fig. 2a). The improvement rate (AHI reduction > 50%) was 71.0% (22/31). The success rate (AHI reduction > 50% and postoperative AHI < 20 events/h) was 61.3% (19/31). The lowest O2 saturation was also significantly increased from 78.1 to 84.7% (p = 0.0012) after surgery (Fig. 2b).
Comparison of physical profiles
The mean age of the success and failure groups was not significantly different (39.7 ± 2.6 vs. 41.1 ± 3.5 years, respectively; Table 1). The preoperative mean body mass index (BMI) of the failure group (26.0 ± 1.0 kg/m2) was higher than that of the success group (25.9 ± 0.9 kg/m2), but the difference was not statistically significant. The failure group also presented increased anthropometric measurements, including neck, waist and hip circumference measurements, but the differences were not statistically significant. Only tonsil grade was significantly larger in the success group (2.1 ± 0.2) than in the failure group (1.2 ± 0.2; p = 0.002). However, there were no significant differences in modified Mallampati grading and Friedman staging scores between the two groups.
Comparison of polysomnographic parameters
A comparison of preoperative polysomnography data between success and failure groups is shown in Table 1. The mean AHI, supine AHI, non-REM AHI, and lowest O2 saturation were higher in the success group than in the failure group, but the differences were not statistically significant. Interestingly, REM AHI was significantly higher in the success group (73.2 ± 6.6 events/h) than in the failure group (48.5 ± 9.9 events/h) (p = 0.038). To further understand the clinical significance of REM AHI, the correlation between preoperative REM AHI and postoperative total AHI change was investigated (Fig. 3). Preoperative REM AHI was correlated positively with the postoperative total AHI change (r = 0.438, p = 0.0137).
Comparison of nasopharyngoscopic parameters
Müller’s maneuver findings in success and failure groups are presented in Table 2. According to the VOTE scoring system, the success group had a higher occurrence of collapse at the velum and oropharynx than the failure group. Lateral oropharyngeal wall collapse was significantly higher in the success group than in the failure group (1.5 ± 0.1 vs. 0.8 ± 0.2, respectively; p = 0.002), which may be related to bigger tonsil size in the former. During full expiration with the mouth closed, nasopharyngoscopy indicated that antero-posterior collapse at the tongue base was more frequent in the failure group, but the difference was not statistically significant. Interestingly, tongue base collapse during mouth opening was significantly more frequent in the failure group (1.6 ± 0.2) than in the success group (1.1 ± 0.2; p = 0.037). However, there was not important factor that statistically correlated with predictive values in DISE results (Table 3).
Comparison of cephalometric parameters
Although the mandibular plane-to-hyoid distance (MP-H) was longer in the failure group (16.3 ± 2.2 mm) than in the success group (14.5 ± 1.3 mm), no statistically significant difference was observed (p = 0.469). In comparison to the success group (69.4 ± 1.6 and 71.8 ± 2.4 mm, respectively), wider inferior airway space (IAS) and shorter vertical airway length (VAL), as well as features associated with retrognathic mandible, were seen in the failure group (70.6 ± 1.5 and 68.3 ± 1.8 mm, respectively); however, there was no statistically significant difference (p = 0.579 and 0.243, respectively). Subgroup analysis showed no correlation between other cephalometric parameters, including posterior airway space (PAS), tongue length (TGL), and possible predictive factors of success or failure.
Discussion
Multi-level obstruction of the upper airway in OSA is long known [16]. Up to 87% of OSA patients have multi-level obstruction, [17, 18] and it may involve all or any level of the upper airway. The base of the tongue has been particularly recognized as a significant site of obstruction in many patients with OSA. Numerous techniques to clear the obstruction at the base of tongue level have been suggested [4].
Tongue reconstruction and pharyngeal microarchitecture re-establishment may contribute to better surgical outcome of retroglossal obstruction. Favorable candidates for surgery may be selected after thorough preoperative evaluation, including Müller’s maneuver, DISE, cephalometry, polysomnography, and physical examination. A few studies about the surgical outcome of tongue base collapse have been published. Vicente et al. [19] reported that lower BMI was associated with better outcome in 55 patients who underwent tongue base suspension plus uvulopalatopharyngoplasty. Tongue volume is correlated with obesity, and OSA patients with higher BMI are likely to have greater tongue size [20]. In our study, there were no significant predictive factors among anthropometric measurements (Table 1). However, the failure group was more obese than the success group, which is in agreement with previous reports [21, 22].
The modified Mallampati grading and Friedman staging are simple methods to estimate the relationship between tongue and soft palate [21]. Moreover, nasopharyngoscopic examination, including Müller’s maneuver or DISE, can provide dynamic information about the base of the tongue and its surrounding structures. In this study, we showed that only tonsil size and lateral oropharyngeal wall collapse on Müller’s maneuver were reliable predictors even in patients who underwent tongue base resection. Bigger tonsil size and greater lateral oropharyngeal wall collapse were associated with better surgical outcome. Tonsil size could be the most predictive factor in patients who have tongue base obstruction. This indicates the importance of effective palatal surgery even in multilevel surgery.
Preoperative higher AHI in supine position was suggested as a favorable predictor for surgical success of tongue base coblation [23]. Lowest oxygen saturation has also been suggested as a predictive factor, which was much lower in the failure group who underwent coblation lingual tonsil removal in 47 Asian patients [24]. However, we could not find an association between those factors and surgical success in this study. Instead, we noticed that preoperative REM AHI was significantly higher in the success group than in the failure group. Correlation analysis also showed that higher preoperative REM AHI was significantly associated with greater reduction of AHI after TBR surgery. Tongue muscles, especially the genioglossus, exhibit lower motor activity during REM sleep [25] and higher REM AHI may be associated with tongue base collapse. This indicates that tongue base resection could be effective in OSA patients whose tongue muscle may be more hypotonic, thus resulting in tongue base collapse during the REM sleep stage.
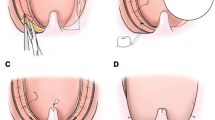
Interestingly, we also found that the success group showed less tongue base collapse in the antero-posterior dimension during mouth opening under nasopharyngoscopy (Fig. 4). Although the examination was performed with the patient awake, we think it could mirror tongue base obstruction if the patient tends to open the mouth during sleep. So far, the effect or mechanism of mouth opening on tongue base collapse is still controversial. This could be affected by either dynamic movement of the upper pharyngeal musculature or excessive hypotonia of tongue muscles during sleep.
In general, cephalometry is a standard radiologic examination that is widely used to determine anatomic parameters in OSA patients [26, 27]. Studies of the predictive value of cephalometrics for multi-level phase I surgery in OSA patients reported that the failure group had a more retrognathic mandible, and a hyperdivergent vertical pattern with a larger mandibular plane angle, longer, lower facial height, and steeper occlusal plane [7]. To our knowledge, there has been no report on predictors of tongue base resection according to cephalometric parameters. In our study, unfortunately, we could not identify any useful predictor from cephalometric measurements, which could have been a result of the relatively small sample size. Further larger scale studies and longer follow-up periods are needed to confirm the performance of the aforementioned variables in predicting tongue base resection.
Conclusion
This study was conducted in an attempt to determine useful predictors for tongue base resection by analysis of the relationship between preoperative parameters and postoperative success rate in OSA patients who underwent tongue base resection combined with lateral pharyngoplasty. A favorable surgical outcome was obtained when the patient had higher preoperative REM AHI. Tonsil size and lateral collapse of the oropharynx on Müller’s maneuver were significant predictive factors even in multi-level surgery including tongue base surgery. Observation of tongue base collapse using a nasopharyngoscope during mouth opening was useful to predict less surgical success. We suggest that these factors should be paid attention to achieve better surgical outcome when multi-level surgery including tongue base resection is considered.
References
Lee W, Nagubadi S, Kryger MH, Mokhlesi B (2008) Epidemiology of obstructive sleep apnea: a population-based perspective. Expert Rev Respir Med 2(3):349–364. doi:10.1586/17476348.2.3.349
Marin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365(9464):1046–1053. doi:10.1016/s0140-6736(05)71141-7
Haniffa M, Lasserson TJ, Smith I (2004) Interventions to improve compliance with continuous positive airway pressure for obstructive sleep apnoea. Cochrane Database Syst Rev 4:Cd003531. doi:10.1002/14651858.CD003531.pub2
Kao YH, Shnayder Y, Lee KC (2003) The efficacy of anatomically based multilevel surgery for obstructive sleep apnea. Otolaryngol Head Neck Surg 129(4):327–335
Friedman M, Tanyeri H, La Rosa M, Landsberg R, Vaidyanathan K, Pieri S, Caldarelli D (1999) Clinical predictors of obstructive sleep apnea. Laryngoscope 109(12):1901–1907. doi:10.1097/00005537-199912000-00002
Julia-Serda G, Perez-Penate G, Saavedra-Santana P, Ponce-Gonzalez M, Valencia-Gallardo JM, Rodriguez-Delgado R, Cabrera-Navarro P (2006) Usefulness of cephalometry in sparing polysomnography of patients with suspected obstructive sleep apnea. Sleep Breath 10(4):181–187. doi:10.1007/s11325-006-0073-y
Kim SJ, Kim YS, Park JH, Kim SW (2012) Cephalometric predictors of therapeutic response to multilevel surgery in patients with obstructive sleep apnea. J Oral Maxillofac Surg 70(6):1404–1412. doi:10.1016/j.joms.2011.03.016
Cho HJ, Park DY, Min HJ, Chung HJ, Lee JG, Kim CH (2016) Endoscope-guided coblator tongue base resection using an endoscope-holding system for obstructive sleep apnea. Head Neck 38(4):635–639. doi:10.1002/hed.24252
Vicini C, Dallan I, Canzi P, Frassineti S, La Pietra MG, Montevecchi F (2010) Transoral robotic tongue base resection in obstructive sleep apnoea-hypopnoea syndrome: a preliminary report. ORL J Otorhinolaryngol Relat Spec 72(1):22–27. doi:10.1159/000284352
Vicini C, Montevecchi F, Campanini A, Dallan I, Hoff PT, Spector ME, Thaler E, Ahn J, Baptista P, Remacle M, Lawson G, Benazzo M, Canzi P (2014) Clinical outcomes and complications associated with TORS for OSAHS: a benchmark for evaluating an emerging surgical technology in a targeted application for benign disease. ORL J Otorhinolaryngol Relat Spec 76(2):63–69. doi:10.1159/000360768
Sher AE, Thorpy MJ, Shprintzen RJ, Spielman AJ, Burack B, McGregor PA (1985) Predictive value of Muller maneuver in selection of patients for uvulopalatopharyngoplasty. Laryngoscope 95(12):1483–1487
Kezirian EJ, Hohenhorst W, de Vries N (2011) Drug-induced sleep endoscopy: the VOTE classification. Eur Arch Otorhinolaryngol 268(8):1233–1236. doi:10.1007/s00405-011-1633-8
Koutsourelakis I, Safiruddin F, Ravesloot M, Zakynthinos S, de Vries N (2012) Surgery for obstructive sleep apnea: sleep endoscopy determinants of outcome. Laryngoscope 122(11):2587–2591. doi:10.1002/lary.23462
Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. The report of an American Academy of Sleep Medicine Task Force (1999) Sleep 22(5):667–689
Sher AE, Schechtman KB, Piccirillo JF (1996) The efficacy of surgical modifications of the upper airway in adults with obstructive sleep apnea syndrome. Sleep 19(2):156–177
Fujita S (1984) UPPP for sleep apnea and snoring. Ear Nose Throat J 63(5):227–235
Lin HC, Friedman M, Chang HW, Gurpinar B (2008) The efficacy of multilevel surgery of the upper airway in adults with obstructive sleep apnea/hypopnea syndrome. Laryngoscope 118(5):902–908. doi:10.1097/MLG.0b013e31816422ea
Abdullah VJ, Hasselt CAv (2005) Video sleep nasendoscopy. In: Terris DJ, Goode RL (eds.) Surgical management of sleep apnea and snoring. CRC Press, New York, pp 143–154. doi:10.1201/b14408-8
Vicente E, Marin JM, Carrizo S, Naya MJ (2006) Tongue-base suspension in conjunction with uvulopalatopharyngoplasty for treatment of severe obstructive sleep apnea: long-term follow-up results. Laryngoscope 116(7):1223–1227. doi:10.1097/01.mlg.0000224498.09015.d9
Ahn SH, Kim J, Min HJ, Chung HJ, Hong JM, Lee JG, Kim CH, Cho HJ (2015) Tongue volume influences lowest oxygen saturation but not apnea-hypopnea index in obstructive sleep apnea. PLoS ONE 10(8):e0135796. doi:10.1371/journal.pone.0135796
Friedman M, Ibrahim H, Bass L (2002) Clinical staging for sleep-disordered breathing. Otolaryngol Head Neck Surg 127(1):13–21
Shie DY, Tsou YA, Tai CJ, Tsai MH (2013) Impact of obesity on uvulopalatopharyngoplasty success in patients with severe obstructive sleep apnea: a retrospective single-center study in Taiwan. Acta Otolaryngol 133(3):261–269. doi:10.3109/00016489.2012.741328
Babademez MA, Ciftci B, Acar B, Yurekli MF, Karabulut H, Yilmaz A, Karasen RM (2010) Low-temperature bipolar radiofrequency ablation (coblation) of the tongue base for supine-position-associated obstructive sleep apnea. ORL J Otorhinolaryngol Relat Spec 72(1):51–55. doi:10.1159/000298945
Wee JH, Tan K, Lee WH, Rhee CS, Kim JW (2015) Evaluation of coblation lingual tonsil removal technique for obstructive sleep apnea in Asians: preliminary results of surgical morbidity and prognosticators. Eur Arch Otorhinolaryngol 272(9):2327–2333. doi:10.1007/s00405-014-3330-x
McSharry DG, Saboisky JP, Deyoung P, Jordan AS, Trinder J, Smales E, Hess L, Chamberlin NL, Malhotra A (2014) Physiological mechanisms of upper airway hypotonia during REM sleep. Sleep 37(3):561–569. doi:10.5665/sleep.3498
Millman RP, Carlisle CC, Rosenberg C, Kahn D, McRae R, Kramer NR (2000) Simple predictors of uvulopalatopharyngoplasty outcome in the treatment of obstructive sleep apnea. Chest 118(4):1025–1030
Petri N, Suadicani P, Wildschiodtz G, Bjorn-Jorgensen J (1994) Predictive value of Muller maneuver, cephalometry and clinical features for the outcome of uvulopalatopharyngoplasty. Evaluation of predictive factors using discriminant analysis in 30 sleep apnea patients. Acta Otolaryngol 114(5):565–571
Acknowledgements
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Cho HJ was supported by a Yonsei University College of Medicine Faculty Research Grant (6-2016-0061) and Kim CH was supported by the 2014 Yonsei University Future-leading Research Initiative (2014-22-0131).
Conflict of interest
There are no financial or personal conflicts of interest to declare.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Hwang, C.S., Kim, J.W., Park, S.C. et al. Predictors of success in combination of tongue base resection and lateral pharyngoplasty for obstructive sleep apnea. Eur Arch Otorhinolaryngol 274, 2197–2203 (2017). https://doi.org/10.1007/s00405-017-4467-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-017-4467-1