Abstract
Introduction
Surgical education consists often times of a discrepancy between necessary amount of provided operative teaching and amount of organizational and ward duties. Operative education is often cut to a minimum. As public awareness toward surgical competence raises, so must the educational system. Courses that provide pre-fractured cadaveric specimens can facilitate surgical teaching realistically, prior to operating on living patients. The aim of this study is to introduce a realistic distal radius fracture simulation setup.
Materials and methods
12 cadaveric specimens (3 male, 9 female) were fixed onto a custom drop-test-bench in the hyperextension of the wrist. The forearm was cut midway between elbow and carpus. The distal part of the forearm was potted, and the specimen was exposed to a high energetic impulse. CT imaging was performed after fracture simulation to detect the exact fracture patterns. We used the AO/ASIF recommendations and four-corner concept to classify the achieved fractures by two independent trauma surgeons.
Results
All cadaveric specimens could be successfully fractured. 11 fractures were classified as type 23C3.2 and one was classified as type 23C3.3, as additional fracture of diaphysis occurred. Subclassification according to the four-corner concept showed all fractures to be type C. A concomitant ulnar styloid fracture was observed in 4 cases. Furthermore, all cases showed at least one fragment involving the sigmoid notch. There was no statistically significant correlation found regarding Hounsfield Units (HU) and age (p value 0.402), as well as HU and required kinetic energy (p value 0.063).
Conclusion
A high energetic impulse induced by a custom-made drop-test bench can successfully simulate realistic distal radius fractures in cadaveric specimens with intact soft tissue. Furthermore, these pre-fractured specimens can be utilized in surgical education to provide a teaching experience as realistic as possible without harming living patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The steadily advancing specialization in the surgical fields, combined with a constantly increasing public awareness toward surgical competence, raises the bar for professional education. As in any surgical field, this is also true in orthopaedic trauma surgery. Educating trauma surgeons is complex, time consuming and requires financial resources, as besides lectures and theoretical items, also many manual and practical tasks need to be taught to the future surgeons [1]. Yet, not only future surgeons need education, but also surgeons who already finished their training should be introduced into newly developing techniques and implants [2,3,4]. However, as many modern medical systems find themselves under distinct economic pressure, surgical teaching during daily clinical work may be difficult to be performed on a level, necessary to fulfil the aforementioned complex tasks. To enhance surgical training, practical courses have been conducted for years. In musculoskeletal training courses, the surgeons are being educated at hands of either artificial bone samples that are closely matched to the human anatomy, or teaching is being conducted at hands of formalin fixed or fresh frozen human cadaveric specimens. With such items and specimens, the surgeons can appreciate the anatomy and perform, learn at first hand or refine surgical techniques and procedures. Yet, these methods do not allow realistic training conditions, especially in the case of orthopaedic trauma courses, fracture treatment shall be taught. Specimens with life-like fracture patterns would allow realistic training conditions, comparable with a flight simulator in aviation. Hence, the aim of the present study was to investigate a method to induce realistic fractures into human cadaveric specimens of the distal radius, aiming to make realistic fracture patterns available for such surgical training courses. The advantage would be clearly a more realistic course environment, and as published recently by our group, a possibly enhanced learning experience [5]. As it is the most commonly fractured bone, ORIF of the distal radius is one of the most typical surgical procedures in trauma surgery [6, 7]. Standard treatment of dorsally displaced fractures is volar locking plate fixation [8, 9]. The fracture itself represents a prearthrotic factor, making exact anatomical reduction and fixation an absolute necessity [10,11,12]. When facing multi-fragmentary intraarticular fractures, adaption of the numerous well-described techniques can be essential to guarantee the best possible outcome [13]. Hence, in the present paper, we aimed to reproduce realistic complex articular fracture patterns of the distal radius, by inducing a high energy axial impulse onto specifically fixed fresh frozen human cadaveric forearm specimens. As the specimens are to be used for cadaveric surgical training courses, it is mandatory that the outer soft tissue envelope remains intact, or offers typical accompanying lesions and hence, was a fundamental prerequisite for the study.
Materials and methods
Specimens
For the present study, 12 fresh-frozen human cadaveric upper extremities were available. The specimens were obtained from body donors; written consent was guaranteed. Institutional ethics committee approval was given prior to this study (VT 19-442).
The donors had an average age of 70 years (range 41–91 years) at the time of death, 3 were male and 9 were female. 5 right and 7 left specimens were available. Before testing, X-ray imaging of the specimens was used to check for marked degenerative changes or sequelae from previous fractures or the presence of implants or other foreign bodies that might influence fracture simulation.
Test-bench and fracture simulation
After thawing at room temperature, the specimens were dissected free from soft tissues over a span of 5 cm, beginning 12 cm proximal to the carpus. Then the forearm was osteotomized just proximal to the dissected area using an oscillating saw. Proceeding like this allowed to keep enough bone stock distal to the elbow joint, to be able to bring the rest of the specimens to reasonable use, which the study group sees as a prerequisite for scientific work with human cadaveric specimens. Moreover, reducing the length proximal to the carpus helps with concentrating the induced forces to the area of the desired fracture.
After the specimens were prepared in that manner, the dissected span of the radius and the ulna were potted into custom-made steel cylinders using polymethyl methacrylate (PMMA). The cylinders were equipped with a 4 mm thick baseplate, to be able to fix the construct into the fracture unit later. During the potting process, it was made sure to align the forearm bones rectangular with the baseplate of the potting cylinder, to allow precise axial force induction.
To generate the necessary forces, a custom drop-test-bench had been constructed (Fig. 1). A similar system has been used in a previous work of the study group [14]. The test-bench mainly consists of a steel frame, mounted on a 15 mm thick steel baseplate, measuring 1.5 × 1.5 m. This allows stable positioning of the test-bench and uniform distribution of the forces into the ground. The frame of the test-bench encloses a height-adjustable crossbeam and an impact beam. Within the crossbeam, two slide holes allow passing of the two stems to an impact stamp, that features two contact plates, one above and one below the crossbeam. The baseplate of the potting cylinder can be mounted to the distal contact plate of the impact stamp. In that manner, the distal end of the specimen with the hand and wrist comes to rest on the baseplate of the test-bench (Fig. 1). By levelling the adjustable crossbeam, the amount of overhang of the impacting stamp above the crossbeam can be set. When the impacting beam is dropped onto the upper contact plate of the impacting-stamp, the stamp is pushed downwards and compresses the specimen according to the amount of overhang of the stamp above the crossbeam. The compression of the specimen shall then lead to the required fracture (Fig. 2). With a calculated impact speed of 4 m/s, we are able to hit the specimen with up to 210 Joule (J) of kinetic energy \(\left( {E = \frac{1}{2}mv^{2};\,E = {\text{energy}},\; m = {\text{mass}}, \;v = {\text{velocity}}} \right)\) [14]. Damping mechanisms whatsoever, exceeding the damping effects of the specimens itself, are not needed or implemented.
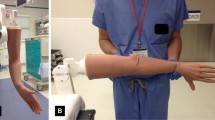
To achieve fractures of the distal radius, the specimens were fixed in extension within the drop-test-bench. Therefore, the potted forearm is fixed against the inferior baseplate of the stamp, and the wrist, which is left free is positioned in extension against the baseplate of the frame. As the crossbeam is height-adjustable, different lengths of specimens can be brought into the desired position. We placed the wrist in 80° of dorsal extension. Following the fracture process, X-ray and CT imaging was conducted to analyse the injury.
Our Institutions Picture Archiving and Communication System (IMPAX) was further used to calculate Hounsfield Units (HU) as a reference to bone mineral density in our specimens [15,16,17]. According to Wagner et al. measurements were performed on three sequential coronal computed tomography scan slices at the level of the distal radial–ulnar joint [18]. The region of interest was measured via a circle to best fit the ulna head without involving the cortical surface. Mean of three measurements was then calculated for each specimen [19].
All fractures were classified independently by two trauma surgeons (KW, AH) according to the AO/ASIF recommendations [20]. Further subclassification was performed according to the recently introduced four-corner concept by Rikli et al. as a useful characterization to enable a tailored approach to the treatment [21].
Statistical analysis
Correlation analysis to age and HU, as well as kinetic energy was conducted, and two-sided t tests were performed to detect any statistically significant differences. We used descriptive statistics to summarize the means and standard deviations. The level of significance was defined as a p value of < 0.05.
Results
12 specimens were available for detailed analysis. Mean HU was 177.89 ± 72.86. All fractures were classified as type C fractures according to the AO/ASIF. There was an independent 100% agreement between the two surgeons classifying the fractures. We divided them further into subgroups of similar fracture patterns and described them additionally by the four-corner concept [21]. Each fractured specimen was suitable for osteosynthetic teaching and was thus successfully utilized in our courses.
Mean weight in our test setup was 16.3 ± 1.8 kg, mean overhang of the stamp was 0.9 ± 0.18 cm and mean kinetic energy was 134.7 ± 14.4 J. All data is summarized for each specimen in Table 1.
Correlation
No statistically significant correlation could be detected between HU and required kinetic energy to achieve fracture (t value 2.088, p value 0.063), and also between HU to age (t value − 0.875, p value 0.402).
Type 23C3.2 fractures
11 out of 12 fractures (92%) were classified as type 23C3.2 fractures. Fracture patterns consisted of at least three intraarticular fracture lines, comminuted metaphysis and intact diaphysis. Carpal subluxation was witnessed in 3 cases, two dorsal subluxations and one volar subluxation. One fracture pattern consisted of a deep central impression of the articular surface, which is seldom if ever seen. A typical extension fracture pattern can be seen in Fig. 3.
Each of those 11 fractures could be further classified as type C according to Rikli, meaning complete intraarticular fracture patterns [21]. A key corner could be described in 6 cases, one dorsal key corner and 5 volar. In 6 cases no key corner could be distinguished. A concomitant ulnar styloid (US) fracture was observed in 4 cases. All cases showed at least one fragment involving the sigmoid notch.
The fractures were produced with a kinetic energy between 120 and 168 J.
Type 23C3.3 fracture
One fracture showed that in addition to multi-fragmentary articular and metaphyseal portion one bony streamer to the distal diaphysis was also present. This streamer is part of a bony shell that has its origin at the dorsal metaphysis and runs towards the volar diaphysis where it ends approximately at 45 mm from the radial joint surface. No severe dislocation of diaphysis is detected. In this fracture a volar key corner can be described, as the fracture line extends coronally from the distal dorsal corner of the radius, involving Lister’s tubercle, to the volar metaphyseal portion with mainly dorsal comminution and carpal subluxation to the volar side (type C). This fracture was produced with a kinetic energy of 152 J.
Discussion
The present study shows, that by inducing a high energy impulse onto human cadaveric specimens of the forearm fixed in the hyperextension of the wrist, realistic fracture patterns can be achieved. Although, the procedure is technically demanding and a high-priced test-bench must be constructed, a clear advantage is that such “pre-fractured” specimens can be used for educational courses in trauma surgery training.
If we look at a typical surgical residency, we will come to notice that the first surgical experience as an operating doctor is often the reduction and fixation of a distal radius fracture, as they are very common and eventually are not highly demanding to fix, depending on the fracture pattern [6, 22]. Therefore, training with this kind of fracture model can facilitate early surgical education. However, the fracture patterns of our study consist of more demanding fracture types (AO type C3), enabling even more experienced surgeons to improve their technical skills, underlining the value of the presented simulation mechanism.
Only one fracture model in our study was found to be rather unrealistic, as a severe central impaction of the articular surface was found. Hyperextension and compression are the major force components that cause fractures in the wrist. Both force components can be transmitted onto the radiocarpal joint during a fall on the hand [23, 24]. An important aspect of the acting forces is the amount of extension of the wrist, as it determines the ratio between tension and compression forces on the radiocarpal joint [24, 25]. Thus, a different fracture pattern occurs by varying the degree of wrist extension [24]. Our specimens were fixed at a standardized angle of 80° wrist extension and axial load induction occurred. The outcome was 12 comparable’ but individually different fracture patterns. Bone density, individual anatomical shape and amount of axial load have a high impact on the definitive fracture pattern, comparable to real patients suffering from a distal radius fracture. Regarding this fact, every pre-fractured specimen suitable for surgical training presents a challenging and unique surgical experience. All 12 pre-fractured specimens were successfully included in our course system. Fracture reduction was, as mentioned before, demanding in many cases. The involvement of the sigmoid notch in each of our cases, demanded a precise fixation of these fragments in order to anatomically reconstruct the distal radioulnar joint (DRUJ) and achieve stability.
Further evaluation of the simulation technique of our test setup can lead to knowledge on how to simulate distal radius fractures of different severity. So far, our test setup is able to simulate reproducible type C fractures, according to the AO/ASIF. By recruitment of further specimens with manipulation of axial load, overhang of the stamp and drop height, we will be able to produce a variety of fracture patterns that can be utilized in surgical courses of different educational levels.
Moreover, our fracture setting mechanism has been validated in other parts of the body, for instance proximal and distal humerus, proximal forearm, pelvis, cephalus, metacarpal and ankle joint. Expanding on this knowledge has enabled us to install a course system of excellent surgical teaching on many different and realistic bony injuries of the human body. These simulated injuries come along with typical accompanying soft tissue lesions, as we found by dissecting the specimens in the courses. This fact even rises the educational effect of this modification of conventional cadaver courses [5].
As new implants and techniques are being introduced to the market frequently, also experienced surgeons can profit from this course system to improve their technical skills in managing new implants and learn techniques at a low-risk, but realistic surrounding.
Correlation analysis of our specimens regarding HU, age and kinetic energy showed no significant results. CT imaging was only performed after simulation to detect the exact fracture pattern. It seems unreasonable and cost-intensive to scan specimens before fracture in order to calculate HU and scan for pathologies. Conventional fluoroscopic scans prior to fracture setting showed to be sufficient in each of our cases. This step is however crucial to detect for any pathologies, that might jeopardize fracture simulation. Additionally, our specimen cohort was rather small to detect any significant correlations. Investigation of a larger cohort might show significant correlation between HU, as a parameter of bone mineral density, and required kinetic energy to produce a certain fracture [17]. So far, our fracture simulation is based on profound experience from past projects. Future investigation into the simulation of distal radius fractures will lead to increasing knowledge on exact kinetic energies. Nevertheless, this study demonstrates the first study to generate course specimens with high impact energy induction.
One of our main goals was to produce fractures with intact skin envelope in order to teach and learn surgical approaches, operational reduction and fixation technique from skin incision to suture, providing the most realistic surgical experience as possible [26, 27]. Cadaveric models remain to be the benchmark in surgical training before operating on living patients [28, 29]. As technical improvements are being introduced frequently to the market, as mentioned before, and sub-specialisation becomes more and more necessary to guarantee an up to date therapy, every surgeon needs to stay on top of his educational level. Surgical courses on cadaveric specimens, therefore represent the ideal course system to provide a significant amount of realistic teaching [30, 31].
Major drawbacks of the use of cadaveric specimens in courses, pre-fractured or not, are the costs, limits on repeated use, difficulties in procurement of specimens and high demands regarding hygienic surroundings [26, 32]. Evaluation of our courses with pre-fractured specimens emphasizes, however, that these disadvantages dissolve against a profound learning experience in realistic trauma models [5]. These findings have also been reported in a different course that provided pre-fractured cadaveric specimens [33]. Nevertheless, further investigation into the value of course systems providing cadaveric specimens is necessary [34].
In Conclusion, realistic fracture patterns of the distal radius can be produced by high energy impulse onto the forearm of cadaveric specimens, fixed in hyperextension of the wrist. All 12 specimens included in this study could be successfully implemented in surgical courses. These pre-fractured specimens can, therefore, facilitate surgical education by providing realistic fracture models with intact soft tissues. Learning to reduce and to fix a fracture on cadaveric pre-fractured specimens is able to set the benchmark in surgical trauma education, before operating on living patients. Disadvantages, such as high costs and the challenging technical procedure to simulate a fracture, dissolve against the value of providing a realistic surgical learning experience.
References
Pellegrini CA (2006) Surgical education in the United States: navigating the white waters. Ann Surg 244(3):335–342. https://doi.org/10.1097/01.sla.0000234800.08200.6c
Darzi SA, Munz Y (2004) The impact of minimally invasive surgical techniques. Annu Rev Med 55:223–237. https://doi.org/10.1146/annurev.med.55.091902.105248
Depres-Tremblay G, Chevrier A, Snow M, Hurtig MB, Rodeo S, Buschmann MD (2016) Rotator cuff repair: a review of surgical techniques, animal models, and new technologies under development. J Shoulder Elbow Surg 25(12):2078–2085. https://doi.org/10.1016/j.jse.2016.06.009
Pennington DG (2006) The impact of new technology on cardiothoracic surgical practice. Ann Thorac Surg 81(1):10–18. https://doi.org/10.1016/j.athoracsur.2005.11.031
Wegmann K, Engel K, Burkhart KJ, Ebinger M, Holz R, Bruggemann GP, Muller LP (2014) Sequence of the Essex-Lopresti lesion—a high-speed video documentation and kinematic analysis. Acta Orthop 85(2):177–180. https://doi.org/10.3109/17453674.2014.887952
Nellans KW, Kowalski E, Chung KC (2012) The epidemiology of distal radius fractures. Hand Clinics 28(2):113. https://doi.org/10.1016/j.hcl.2012.02.001
Unglaub F, Langer MF, Hohendorff B, Muller LP, Unglaub JM, Hahn P, Krimmer H, Spies CK (2017) Distal radius fracture of the adult. Diagnostics and therapy. Orthopade 46(1):93–110. https://doi.org/10.1007/s00132-016-3347-5
Quadlbauer S, Pezzei C, Jurkowitsch J, Rosenauer R, Pichler A, Schattin S, Hausner T, Leixnering M (2018) Early complications and radiological outcome after distal radius fractures stabilized by volar angular stable locking plate. Arch Orthop Trauma Surg 138(12):1773–1782. https://doi.org/10.1007/s00402-018-3051-5
Pillukat T, Fuhrmann R, Windolf J, van Schoonhoven J (2016) The volar locking plate for extension fractures of the distal radius. Oper Orthop Traumato 28(1):47–63. https://doi.org/10.1007/s00064-015-0433-5
Erhart S, Toth S, Kaiser P, Kastenberger T, Deml C, Arora R (2018) Comparison of volarly and dorsally displaced distal radius fracture treated by volar locking plate fixation. Arch Orthop Trauma Surg 138(6):879–885. https://doi.org/10.1007/s00402-018-2925-x
Gologan RE, Koeck M, Suda AJ, Obertacke U (2019) > 10-year outcome of dislocated radial fractures with concomitant intracarpal lesions as proven by MRI and CT. Arch Orthop Trauma Surg 139(6):877–881. https://doi.org/10.1007/s00402-019-03186-8
Schnetzke M, Fuchs J, Vetter SY, Swartman B, Keil H, Grutzner PA, Franke J (2018) Intraoperative three-dimensional imaging in the treatment of distal radius fractures. Arch Orthop Trauma Surg 138(4):487–493. https://doi.org/10.1007/s00402-018-2867-3
Diwersi N, Babst R, Link BC (2016) Miniplates as augmentation implants in osteosynthesis of complex distal radial fractures. Oper Orthop Traumato 28(5):402–406. https://doi.org/10.1007/s00064-016-0469-1
Wegmann K, Rausch V, Burkhart KJ, Hackl M, Leschinger T, Muller L (2019) Advanced surgical trauma care course – evaluation of a fracture simulation course concept with intact soft tissue. Z Orthop Unfall. https://doi.org/10.1055/a-0983-8322
Lee S, Chung CK, Oh SH, Park SB (2013) Correlation between bone mineral density measured by dual-energy X-ray absorptiometry and Hounsfield units measured by diagnostic CT in lumbar spine. J Korean Neurosurg S 54(5):384–389. https://doi.org/10.3340/jkns.2013.54.5.384
Patel SP, Lee JJ, Hecht GG, Holcombe SA, Wang SC, Goulet JA (2016) Normative vertebral Hounsfield unit values and correlation with bone mineral density. J Clin Exp Orthopaed 2(114):1–7
Schreiber JJ, Anderson PA, Hsu WK (2014) Use of computed tomography for assessing bone mineral density. Neurosurg Focus. https://doi.org/10.3171/2014.5.Focus1483
Wagner SC, Dworak TC, Grimm PD, Balazs GC, Tintle SM (2017) Measurement of distal ulnar Hounsfield units accurately predicts bone mineral density of the forearm. J Bone Joint Surg. https://doi.org/10.2106/JBJS.15.01244
Dworak TC, Wagner SC, Nappo KE, Balazs GC, Grimm PD, Colantonio DF, Tintle SM (2018) The use of distal Ulnar Hounsfield units to predict future fragility fracture risk. J Hand Surg-Am 43(11):1010–1015. https://doi.org/10.1016/j.jhsa.2018.04.017
Müller ME (1991) The principle of the classification. In: Müller ME, Allgöwer M, Schneider R, Willenegger H (eds) Manual of internal fixation: techniques recommended by the AO-ASIF group, 3rd edn. Springer, New York, p 118
Brink PRG, Rikli DA (2016) Four-corner concept: CT-based assessment of fracture patterns in distal radius. J Wrist Surg 5(2):147–151. https://doi.org/10.1055/s-0035-1570462
Court-Brown CM, Caesar B (2006) Epidemiology of adult fractures: a review. Injury 37(8):691–697. https://doi.org/10.1016/j.injury.2006.04.130
Melone CP (1984) Articular fractures of the distal radius. Orthop Clin N A 15(2):217–236
Augat P, Iida H, Jiang Y, Diao E, Genant HK (1998) Distal radius fractures: mechanisms of injury and strength prediction by bone mineral assessment. J Orthop Res 16(5):629–635. https://doi.org/10.1002/jor.1100160517
Koebke J (1988) Anatomy of the wrist joint and carpus. Unfallchirurgie 14(2):74–79
Atesok K, Mabrey JD, Jazrawi LM, Egol KA (2012) Surgical simulation in orthopaedic skills training. J Am Acad Orthop Sur 20(7):410–422. https://doi.org/10.5435/Jaaos-20-06-410
Nutt J, Mehdian R, Parkin I, Dent J, Kellett C (2012) Cadaveric surgery: a novel approach to teaching clinical anatomy. Clin Teach 9(3):148–151. https://doi.org/10.1111/j.1743-498X.2012.00536.x
Holland JP, Waugh L, Horgan A, Paleri V, Deehan DJ (2011) Cadaveric hands-on training for surgical specialties: is this back to the future for surgical skills development? J Surg Educ 68(2):110–116. https://doi.org/10.1016/j.jsurg.2010.10.002
Sharma G, Aycart MA, Najjar PA, van Houten T, Smink DS, Askari R, Gates JD (2016) A cadaveric procedural anatomy course enhances operative competence. J Surg Res 201(1):22–28. https://doi.org/10.1016/j.jss.2015.09.037
Katz R, Hoznek A, Antiphon P, Van Velthoven R, Delmas V, Abbou CC (2003) Cadaveric versus porcine models in urological laparoscopic training. Urol Int 71(3):310–315. https://doi.org/10.1159/000072684
Kuhls DA, Risucci DA, Bowyer MW, Luchette FA (2013) Advanced surgical skills for exposure in trauma: a new surgical skills cadaver course for surgery residents and fellows. J Trauma Acute Care Surg 74(2):664–670. https://doi.org/10.1097/TA.0b013e31827d5e20
Garment A, Lederer S, Rogers N, Boult L (2007) Let the dead teach the living: the rise of body bequeathal in 20th-century America. Acad Med 82(10):1000–1005. https://doi.org/10.1097/ACM.0b013e318149e986
Christophel JJ, Park SS, Nogan SJ, Essig GF (2017) A facial trauma simulation course for evaluation and treatment of facial fractures. Jama Facial Plast Surg 19(6):464–467. https://doi.org/10.1001/jamafacial.2017.0313
Gilbody J, Prasthofer AW, Ho K, Costa ML (2011) The use and effectiveness of cadaveric workshops in higher surgical training: a systematic review. Ann R Coll Surg Engl 93(5):347–352. https://doi.org/10.1308/147870811X582954
Acknowledgements
We thank Ms. Jutta Knifka for valuable support in preparing the specimens for fracture simulation.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by KW and AH. The first draft of the manuscript was written by KW and AH and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors have received financial research support by Medartis and IBRA. Kilian Wegmann and Lars Peter Müller are paid consultants for Medartis and Arthrex. Michael Hackl has a travelling fellowship sponsored by Wright/Tornier. He is further a speaker and course instructor for Medartis and Arthrex.
Ethical approval
All procedures performed in our study involving human cadavers were in accordance with the ethical standards of the institutional research committee (Ethical Committee of the Medical Faculty of the University of Cologne—VT 19-442) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wegmann, K., Harbrecht, A., Hackl, M. et al. Inducing life-like distal radius fractures in human cadaveric specimens: a tool for enhanced surgical training. Arch Orthop Trauma Surg 140, 425–432 (2020). https://doi.org/10.1007/s00402-019-03313-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-019-03313-5