Abstract
Introduction
In operative treatment of distal radius fractures satisfying outcome mainly relies on anatomical fracture reduction and correct implant placement. Examination with two-dimensional fluoroscopy may not provide reliable information about this. The aim of this study was to determine the effectiveness of additional intraoperative three-dimensional imaging in the operative treatment of comminuted distal radius fractures.
Materials and methods
From August 2001 to June 2015, patients with a distal radius fracture who were treated operatively and received intraoperative three-dimensional scan were included. The findings of the three-dimensional scan were documented by the operative surgeon and analyzed retrospectively with regard to incidence and the need for intraoperative revisions. Clinical evaluation included the patient’s medical history, the injury pattern of the affected wrist (according to the OTA/AO fracture classification) and concomitant injuries. Intraoperative and postoperative complications and revision surgeries were evaluated as well.
Results
Of 4515 operatively treated distal radius fractures, 307 (6.8%) received additional intraoperative three-dimensional imaging during surgery. 263 of 307 patients (85.7%) had a distal radius fracture type C. Intraoperative three-dimensional imaging revealed findings in 125 patients (40.7%) that were not detected on conventional two-dimensional fluoroscopy. In 54 patients (17.6%) these findings led to an immediate revision. Most commonly, revision was done in the case of remaining steps in the articular surface ≥ 1 mm (n = 25, 8.1%) followed by intra-articular screw placement (n = 23, 7.5%).
Conclusions
Intraoperative three-dimensional imaging can provide additional information compared to conventional two-dimensional fluoroscopy in the operative treatment of distal radius fractures with the possibility of immediate intraoperative revision.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Distal radius fractures are the most common upper extremity fractures with 162 fractures per 100,000 persons per year and the prevalence of intra-articular distal radius fractures accounts for approximately 60% of all radius fractures [9, 16, 19]. Volar plating is most commonly treatment of care for comminuted and displaced distal radius fractures [21, 22, 31, 34]. Complications of palmar plating are reported in 0–44% of cases depending on the type of injury [1, 5, 27, 35]. Surgical revision is necessary in 0–36% patients, in most cases due to implant-related complications such as hardware failure, malunion or tendon ruptures [5].
Correct fracture reduction and implant placement is conventionally verified by intraoperative two-dimensional fluoroscopy. Suboptimal positioning of implants, insufficient reconstructions and joint incongruities are frequently not revealed with standard two-dimensional fluoroscopy [11, 30]. The angulation of the subchondral screws, overlapping of anatomic structures, and the concavity of the joint surface are prone to misinterpretation by the operative surgeon [8, 11, 12, 30]. Subsequently, implant malposition and remaining steps in the articular surface are often recognized at first on postoperative computed tomography (CT) scans [8, 11, 25, 32].
It has been shown that specific intraoperative images such as the dorsal tangential view and the radial grove view can help improve the screw placement [6, 14, 18]. Alternatively, intraoperative three-dimensional imaging might be a useful imaging modality to decrease the surgical revision rate due to implant malpositioning or remaining steps in the articular surface. Preliminary reports with a small numbers of cases have shown that intraoperative three-dimensional imaging in the treatment of distal radius fractures can provide additional information compared to conventional two-dimensional fluoroscopy [3, 7, 17, 23]. These studies, however, lack detailed analysis of the intraoperative findings and postoperative course.
The objective of this study was to determine the effectiveness of intraoperative three-dimensional imaging in the operative treatment of distal radius fractures. We hypothesized that intraoperative three-dimensional imaging with a mobile C-arm could detect inadequate implant placement or fracture malreduction that had not been verified on conventional two-dimensional fluoroscopy leading to immediate intraoperative revision. Approval from the appropriate Ethics Committee was obtained for analysis of the data.
Materials and methods
This retrospective study was conducted at a level 1 trauma centre. From August 2001 to June 2015, all patients with operatively treated distal radius fractures, who had been evaluated with additional intraoperative three-dimensional imaging, were prospectively recorded. Evaluation of data was done in a retrospective chart review. Patients were included in this study regardless of age, comorbidities, or other injuries. All of the study data were collected on the basis of a normal standardized clinical investigation.
Imaging technique
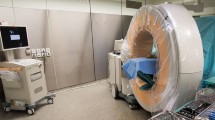
Preoperative CT was routinely performed in patients with type C fractures according to the OTA/AO fracture classification [20]. The intraoperative three-dimensional scans were performed with mobile C-arms. We used a SIREMOBIL Iso-C3D (Siemens, Erlangen, Germany) early in the series. From March 15, 2005 onwards the ARCADIS Orbic 3D (Siemens) was used and from 2011 onwards second-generation ARCADIS Orbic 3D was used.
In all patients, the wrist was positioned on a radiolucent, carbon fiber, arm-table for the operative procedure. The C-arm position is perpendicular to the upper limb. After operative reduction and fracture fixation, conventional two-dimensional imaging with a mobile C-arm was performed. Intraoperative antero-posterior and lateral views were obtained with respect to the palmar and radial tilt to obtain full insight into the radiocarpal joint. In addition, dynamic fluoroscopy was performed to detect intra-articular screw placement in the radiocarpal as well as in the distal radioulnar joint. The dorsal tangential view was not performed in this study. The surgeon evaluated these two-dimensional images; if fracture reduction was considered to be anatomical (no intra-articular step, no dorsal tilt, radial tilt of 20°–30°, ulna aligned with the distal radius with neutral or slightly negative ulnar variance) and implant position were judged to be appropriate (no intra-articular screw placement, no screw penetration of the dorsal cortical bone), an intraoperative three-dimensional scan was performed (1) if the assessment of fracture reduction was difficult due to comminuted fracture pattern with defects and possible central impression of the articular surface according to the preoperative CT and/or (2) assessment of implant placement was difficult due to screw placement very close to the radiocarpal and/or distal radioulnar joint. In case of immediate intraoperative revision, the same sequence of intraoperative imaging was followed as before, i.e., two-dimensional fluoroscopy, dynamic fluoroscopy and then intraoperative three-dimensional scan.
Assessment of the data
The total number of intraoperative three-dimensional scans and the intraoperative findings and the consequences (revision or no revision) of each intraoperative three-dimensional scan were documented in the immediate postoperative period by the surgeon while still in the operating room (index procedure). Retrospectively, the intraoperative findings could be categorized according to the following criteria: (1) correct implant positioning and screw placement, (2) remaining step-off ≥ 1 mm in the articular surface, (3) intra-articular screw placement, and (4) prominent screw on the opposite cortex. Prominent screws were defined as those screws protruding equal to or greater than 1 millimeter from the opposite cortex of the radius.
For each patient, the medical history and previous surgeries of the affected wrist were assessed. The mechanism of injury, the injury pattern of the wrist, and concomitant injuries were recorded. All fractures were classified according to the OTA/AO fracture classification by the operative surgeon according to preoperative radiographs, preoperative CT and the intraoperative assessment [20].
Statistics
Mean and standard deviation (SD) were calculated for continuous variables.
Results
Of 4515 operatively treated distal radius fractures, 307 patients (6.8%) were evaluated by additional intraoperative three-dimensional imaging during the study period. The study group consisted of 180 men (58.6%) and 127 women (41.4%) with an average age of 50.0 (SD 16.1) years (range 14.9–87.5). The right side was injured in 158 patients (51.5%). 55 patients (17.9%) had at least one comorbidity; most frequent were hypertension (n = 32, 10.4%) and diabetes (n = 11, 3.6%). The mean body mass index was 27.0 (SD 5.2) kg/m2. 263 patients (85.7%) had a type C fracture according to the OTA/AO fracture classification (Fig. 1).
In 234 patients (76.2%), three-dimensional imaging was performed during primary surgical treatment of the distal radius fracture 7.2 (SD 7.7) days after injury. Another 73 patients (23.8%) had prior surgical treatment, 40 patients (13%) were treated with an external fixator during primary surgery and 33 patients (10.7%) had failed osteosynthesis requiring revision surgery. Twelve of these 33 patients (36.4%) were referred from another hospital for revision surgery. Mean time between application of the external fixator and definitive fracture stabilization (index procedure) was 8.9 (SD 5.6) days. After failed previous osteosynthesis, the index procedure was performed after an average of 26.4 (SD 26.4) days.
During the index procedure most patients were treated with locked plate osteosynthesis (n = 289, 94.1%, Table 1). Three patients (1.0%) had dorsal plating, 286 patients (93.2%) had volar plating of the distal radius. 90 patients (29.3%) received allogeneic or autologous bone substitution. Mean operative time was 65.9 ± 32.2 min.
Analysis of intraoperative three-dimensional scans
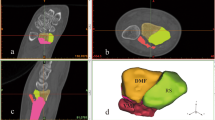
In 182 patients (59.3%), correct implant placement and anatomical reduction were documented (Table 2). Pathological findings were detected in 125 patients (40.7%). In 54 patients (17.6%), the findings of the intraoperative three-dimensional scan led to an immediate revision. In 25 patients (8.1%), a remaining step in the articular surface of ≥ 1 mm, and in 23 patients (7.5%), intra-articular screw placement was revised following the intraoperative three-dimensional scan. In all patients that received intraoperative revision, a second three-dimensional scan was performed to visualize the result of the immediate revision. In 42 of 54 patients (77.2%) completely successful revision was achieved and in 12 of 54 patients (22.2%) partial improvement (smaller step in the joint surface) was achieved with immediate revision. In these 12 patients, no further intraoperative revision was performed. In comminuted distal radius fracture type C2 and C3 according to the OTA/AO fracture classification, the highest intraoperative revision rates were found with 19.6 and 19.4%, respectively (Table 3). A patient example with central impression of the articular surface and improvement of the fracture reduction after intraoperative three-dimensional scan is shown in Fig. 2a-f.
a, b Distal radius fracture type 23C3 in a 53-year-old woman. c Conventional lateral view appeared to be adequately reduced with correct implant placement. d Intraoperative three-dimensional scan revealed a remaining step of 2 mm in the articular surface. e After immediate intraoperative revision of the fracture reduction the result was first checked with fluoroscopy. f Repeated three-dimensional scan shows almost anatomical reduction with correct screw placement (the remaining gap was accepted by the surgeon)
Discussion
The most important finding of the current study is that intraoperative three-dimensional imaging revealed pathological findings in 54 of 307 patients (17.6%), which were not seen on conventional fluoroscopy, leading to an immediate intraoperative revision. Most commonly, revision was done in the case of remaining steps in the articular surface ≥ 1 mm (n = 25, 8.1%) followed by intra-articular screw placement (n = 23, 7.5%). In this study, all scans were made after the surgeon had judged the reduction of the articular surface and the implant placement to be correct by means of a standard two-dimensional fluoroscopic examination. Therefore, all of the findings leading to correction in this series would not have been addressed without the three-dimensional scan.
Previous studies reported intraoperative revision rates after application of intraoperative three-dimensional imaging ranging from 10.5 to 34.7% [3, 4, 7, 17, 23, 24, 28]. In 2013, Mehling et al. published the largest series about the usefulness of intraoperative three-dimensional imaging in the treatment of distal radius fractures [23]. The authors compared the findings on conventional two-dimensional fluoroscopy with the findings of the intraoperative three-dimensional scan in 51 patients. Mehling et al. found that intra-articular screw placement in 31.3% of the operations was not revealed using standard two-dimensional fluoroscopy but was detected using intraoperative three-dimensional imaging [23].
Volar locked plating of distal radius fractures performed with fluoroscopic guidance continues to grow in popularity. However, the current study clearly demonstrates the difficulties of detecting intra-articular screw penetration or malreduction by fluoroscopic guidance alone. In 2010, Tweet et al. investigated a cadaveric study to detect intra-articular screw penetration during volar plating of the distal radius with fluoroscopy [33]. The authors concluded that no combination of imaging allowed detection of all intra-articular screws, and that a high level of suspicion for intra-articular screw penetration should be maintained during volar plating of distal radial fractures. Intraoperative three-dimensional imaging might be a possible solution to overcome these problems.
Alternatively, arthroscopically assisted fracture reduction has been described to visualize fracture reduction and screw placement in the operative treatment of distal radius fractures [11, 26, 30]. Ruch et al. found that patients who underwent arthroscopically assisted procedures had a greater degree of supination, flexion, and extension than patients undergoing fluoroscopic-assisted surgery [30]. Edwards et al. concluded that residual displacement noted by adjunctive arthroscopy may prompt another reduction effort and result in an improved articular alignment of intra-articular distal radius fractures [11]. These findings confirm the results of the current study that two-dimensional fluoroscopy is prone to misinterpretation in the operative treatment of distal radius fractures. Despite the good results described in the literature, arthroscopically assisted fracture reduction has not been implemented in daily clinical practice in the operative treatment of distal radius fractures. Alternatively, intraoperative three-dimensional imaging might be a less invasive alternative compared to wrist arthroscopy.
Volar locking plate fixation also bears the risks of extensor tendon rupture due to excessively long distal screws [2]. Ruptures of extensor tendons have been reported in as high as 8.6% of patients. Recently, Ganesh et al. compared intraoperative fluoroscopy and postoperative CT regarding the detection of prominent hardware in volar locked plating of distal radius fractures [13]. Postoperative CT showed that 5 of the 175 screws (3%) in 5 of the 30 (17%) fractures had prominent screws of 1 mm or greater not detected by the standard fluoroscopic views or dorsal tangential view. The authors concluded that intraoperative fluoroscopy including the dorsal tangential view is not sufficient to avoid dorsal screw prominence. In the current study, prominent screws were detected by intraoperative three-dimensional imaging in six patients and could be revised immediately. However, it should be noted that the dorsal tangential view was not performed.
One major criticisms of intraoperative three-dimensional imaging is the amount of time needed for performing the three-dimensional scan, editing, and interpreting the generated data. Richter et al. reported that the operation was interrupted for 7.2 min on average in their study for ISO-C-3D use and using the ARCADIS Orbic 3D for 5.2 min [23, 29]. A cost analysis of intraoperative three-dimensional imaging by Hüfner et al. has demonstrated that an economic benefit can be achieved if the revision rate is decreased by just 5% [15].
From our point of view, intraoperative three-dimensional imaging can be efficiently be integrated in the surgical workflow and the distal radius is easily assessable for intraoperative three-dimensional imaging. Especially in complex radius fractures with the need of very distal implant positioning and a considerable risk for intra-articular screw placement, the advantages of secure identification of malpositioned screws or remaining steps in the articular surface, as well as the possibility of an immediate correction, rule out the possible disadvantages [23].
This study has some limitations. Even if all cases were included in a prospectively recorded database, the evaluation was done in a retrospective chart review. The population selection was randomly chosen by the operative surgeon. However, a protocol to scan at predefined patients is difficult to apply on patients who have a great variety of pathologies, which qualify for the use of three-dimensional imaging. Furthermore, three different three-dimensional image intensifiers were used during the course of the study. Postoperative CT scan was not used in the current study to validate the data. It has been shown previously that intraoperative three-dimensional imaging is comparable to CT regarding the assessment of fracture reduction and implant placement [36]. It should be further noted that the dorsal horizon view was not performed in this study, which could have decreased the detection rate of pathological findings with an intraoperative three-dimensional imaging in this study. Finally, it should be mentioned that the clinical outcome of the patients was not assessed in the current study, and therefore, radiographic outcomes have not been correlated with clinical or functional outcomes. Previous studies found that variations of radiographic parameters did not affect the clinical outcome after operative treatment of distal radius fractures [10]. Further studies with assessment of the clinical outcome are necessary to prove the clinical benefit of intraoperative three-dimensional imaging in distal radius fractures.
Conclusion
In the present study, intraoperative three-dimensional imaging revealed findings in 17.6% of cases, which were not seen on conventional fluoroscopy, leading to immediate revision. The use of intraoperative three-dimensional imaging might be helpful to improve the fracture reduction and implant placement in the operative treatment of distal radius fractures, especially in comminuted fracture types.
References
Arora R, Lutz M, Deml C, Krappinger D, Haug L, Gabl M (2011) A prospective randomized trial comparing nonoperative treatment with volar locking plate fixation for displaced and unstable distal radial fractures in patients sixty-five years of age and older. J Bone Joint Surg Am 93(23):2146–2153. https://doi.org/10.2106/jbjs.j.01597
Arora R, Lutz M, Hennerbichler A, Krappinger D, Espen D, Gabl M (2007) Complications following internal fixation of unstable distal radius fracture with a palmar locking-plate. J Orthop Trauma 21(5):316–322. https://doi.org/10.1097/BOT.0b013e318059b993
Atesok K, Finkelstein J, Khoury A, Peyser A, Weil Y, Liebergall M, Mosheiff R (2007) The use of intraoperative three-dimensional imaging (ISO-C-3D) in fixation of intraarticular fractures. Injury 38(10):1163–1169. https://doi.org/10.1016/j.injury.2007.06.014
Beerekamp MS, Sulkers GS, Ubbink DT, Maas M, Schep NW, Goslings JC (2012) Accuracy and consequences of 3D-fluoroscopy in upper and lower extremity fracture treatment: a systematic review. Eur J Radiol 81(12):4019–4028. https://doi.org/10.1016/j.ejrad.2012.06.021
Bentohami A, de Burlet K, de Korte N, van den Bekerom MP, Goslings JC, Schep NW (2014) Complications following volar locking plate fixation for distal radial fractures: a systematic review. J Hand Surg Eur Vol 39(7):745–754. https://doi.org/10.1177/1753193413511936
Brunner A, Siebert C, Stieger C, Kastius A, Link BC, Babst R (2015) The dorsal tangential X-ray view to determine dorsal screw penetration during volar plating of distal radius fractures. J Hand Surg Am 40(1):27–33. https://doi.org/10.1016/j.jhsa.2014.10.021
Carelsen B, van Loon J, Streekstra GJ, Maas M, van Kemenade P, Strackee SD (2011) First experiences with the use of intraoperative 3D-RX for wrist surgery. Minim Invasive Therapy Allied Technol 20(3):160–166. https://doi.org/10.3109/13645706.2010.518807
Catalano LW 3rd, Barron OA, Glickel SZ (2004) Assessment of articular displacement of distal radius fractures. Clin Orthop Relat Res 423:79–84
Cooney WP 3rd, Linscheid RL, Dobyns JH (1979) External pin fixation for unstable Colles’ fractures. J Bone Joint Surg Am 61(6a):840–845
Dario P, Matteo G, Carolina C, Marco G, Cristina D, Daniele F, Andrea F (2014) Is it really necessary to restore radial anatomic parameters after distal radius fractures? Injury 45(Suppl 6):S21–S26. https://doi.org/10.1016/j.injury.2014.10.018
Edwards CC, 2nd, Haraszti CJ, McGillivary GR, Gutow AP (2001) Intra-articular distal radius fractures: arthroscopic assessment of radiographically assisted reduction. J Hand Surg Am 26(6):1036–1041. https://doi.org/10.1053/jhsu.2001.28760
Franke J, Wendl K, Suda AJ, Giese T, Grutzner PA, von Recum J (2014) Intraoperative three-dimensional imaging in the treatment of calcaneal fractures. J Bone Joint Surg Am 96(9):e72. https://doi.org/10.2106/jbjs.l.01220
Ganesh D, Service B, Zirgibel B, Koval K (2016) The detection of prominent hardware in volar locked plating of distal radius fractures: intraoperative fluoroscopy versus computed tomography. J Orthop Trauma 30(11):618–621. https://doi.org/10.1097/bot.0000000000000661
Hill BW, Shakir I, Cannada LK (2015) Dorsal screw penetration with the use of volar plating of distal radius fractures: how can you best detect? J Orthop Trauma 29(10):e408–e413. https://doi.org/10.1097/bot.0000000000000361
Hufner T, Stubig T, Gosling T, Kendoff D, Geerling J, Krettek C (2007) Cost-benefit analysis of intraoperative 3D imaging. Unfallchirurg 110(1):14–21. https://doi.org/10.1007/s00113-006-1202-6
Karl JW, Olson PR, Rosenwasser MP (2015) The epidemiology of upper extremity fractures in the united states, 2009. J Orthop Trauma 29(8):e242–e244. https://doi.org/10.1097/bot.0000000000000312
Kendoff D, Citak M, Gardner MJ, Stubig T, Krettek C, Hufner T (2009) Intraoperative 3D imaging: value and consequences in 248 cases. J Trauma 66(1):232–238. https://doi.org/10.1097/TA.0b013e31815ede5d
Lee SK, Bae KW, Choy WS (2013) Use of the radial groove view intra-operatively to prevent damage to the extensor pollicis longus tendon by protruding screws during volar plating of a distal radial fracture. Bone Joint J 95(b 10):1372–1376. https://doi.org/10.1302/0301-620x.95b10.31453
Leung KS, Shen WY, Tsang HK, Chiu KH, Leung PC, Hung LK (1990) An effective treatment of comminuted fractures of the distal radius. J Hand Surg Am 15(1):11–17
Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, DeCoster TA, Prokuski L, Sirkin MS, Ziran B, Henley B, Audige L (2007) Fracture and dislocation classification compendium-2007: orthopaedic trauma association classification, database and outcomes committee. J Orthop Trauma 21(10 suppl):S1–S133
Matschke S, Marent-Huber M, Audige L, Wentzensen A (2011) The surgical treatment of unstable distal radius fractures by angle stable implants: a multicenter prospective study. J Orthop Trauma 25(5):312–317. https://doi.org/10.1097/BOT.0b013e3181f2b09e
Matschke S, Wentzensen A, Ring D, Marent-Huber M, Audige L, Jupiter JB (2011) Comparison of angle stable plate fixation approaches for distal radius fractures. Injury 42(4):385–392. https://doi.org/10.1016/j.injury.2010.10.010
Mehling I, Rittstieg P, Mehling AP, Kuchle R, Muller LP, Rommens PM (2013) Intraoperative C-arm CT imaging in angular stable plate osteosynthesis of distal radius fractures. J Hand Surg Eur 38(7):751–757. https://doi.org/10.1177/1753193413476418
Meier R, Geerling J, Hufner T, Kfuri M, Krettek C (2011) The isocentric C-arm. Visualization of fracture reduction and screw position in the radius. Unfallchirurg 114(7):587–590. https://doi.org/10.1007/s00113-011-2008-8
Meier R, Kfuri M Jr, Geerling J, Hufner T, Krimmer H, Krettek C (2005) Intraoperative three-dimensional imaging with an isocentric mobile C-arm at the wrist. Handchir Mikrochir Plast Chir 37(4):256–259. https://doi.org/10.1055/s-2004-830563
Ono H, Furuta K, Fujitani R, Katayama T, Akahane M (2010) Distal radius fracture arthroscopic intraarticular displacement measurement after open reduction and internal fixation from a volar approach. J Orthop Sci 15(4):502–508. https://doi.org/10.1007/s00776-010-1484-y
Orbay JL, Fernandez DL (2004) Volar fixed-angle plate fixation for unstable distal radius fractures in the elderly patient. J Hand Surg Am 29(1):96–102
Rausch S, Marintschev I, Graul I, Wilharm A, Klos K, Hofmann GO, Florian Gras M (2015) Tangential view and intraoperative three-dimensional fluoroscopy for the detection of screw-misplacements in volar plating of distal radius fractures. Arch Trauma Res 4(2):e24622. https://doi.org/10.5812/atr.4(2)2015.24622
Richter M, Zech S (2009) Intraoperative 3-dimensional imaging in foot and ankle trauma-experience with a second-generation device (ARCADIS-3D). J Orthop Trauma 23(3):213–220. https://doi.org/10.1097/BOT.0b013e31819867f6
Ruch DS, Vallee J, Poehling GG, Smith BP, Kuzma GR (2004) Arthroscopic reduction versus fluoroscopic reduction in the management of intra-articular distal radius fractures. Arthroscopy 20(3):225–230. https://doi.org/10.1016/j.arthro.2004.01.010
Souer JS, Ring D, Jupiter JB, Matschke S, Audige L, Marent-Huber M (2009) Comparison of AO type-B and type-C volar shearing fractures of the distal part of the radius. J Bone Joint Surg Am 91(11):2605–2611. https://doi.org/10.2106/jbjs.h.01479
Takemoto RC, Gage M, Rybak L, Zimmerman I, Egol KA (2012) Accuracy of detecting screw penetration of the radiocarpal joint following volar plating using plain radiographs versus computed tomography. Am J Orthop (Belle Mead NJ) 41(8):358–361
Tweet ML, Calfee RP, Stern PJ (2010) Rotational fluoroscopy assists in detection of intra-articular screw penetration during volar plating of the distal radius. J Hand Surg Am 35(4):619–627. https://doi.org/10.1016/j.jhsa.2009.12.033
Vanhaecke J, Fernandez DL (2015) DVR plating of distal radius fractures. Injury. https://doi.org/10.1016/j.injury.2015.08.010
Ward CM, Kuhl TL, Adams BD (2011) Early complications of volar plating of distal radius fractures and their relationship to surgeon experience. Hand (N Y) 6(2):185–189. https://doi.org/10.1007/s11552-010-9313-5
Weil YA, Liebergall M, Mosheiff R, Singer SB, Joskowicz L, Khoury A (2011) Assessment of two 3-D fluoroscopic systems for articular fracture reduction: a cadaver study. Int J Comput Assist Radiol Surg 6(5):685–692. https://doi.org/10.1007/s11548-011-0548-6
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The MINTOS research group had grants/grants pending from Siemens (Erlangen, Germany); Jochen Franke, MD, is a paid lecturer for Siemens; Paul A Grützner, MD, is a paid lecturer for Siemens.
Rights and permissions
About this article
Cite this article
Schnetzke, M., Fuchs, J., Vetter, S.Y. et al. Intraoperative three-dimensional imaging in the treatment of distal radius fractures. Arch Orthop Trauma Surg 138, 487–493 (2018). https://doi.org/10.1007/s00402-018-2867-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-018-2867-3