Abstract
Introduction
Compromised bone quality and the need for early mobilization still lead to high rates of implant failure in geriatric patients with distal femoral fractures. With the newest generation of polyaxial locking plates and the proven retrograde femoral nails today two minimally invasive surgical procedures have been established. Indications for both procedures overlap. This study attempts to define the strength and failure mode of both surgical procedures.
Materials and methods
A standardized fracture model was established to simulate an unstable AO/OTA 33-A3 fracture. Eight pairs of human cadaver femora (mean age 79 years, range 63–100 years) with compromised bone quality were used. Osteosyntheses with eight retrograde femoral nails and eight locking plates were randomly performed. A materials testing machine (Instron 5566) was used to perform cyclic stress tests according to a standardized loading protocol, up to a maximum load of 5,000 N.
Results
All specimens survived loading of at least 2,500 N. Three nail and one plate construct survived a maximum load of 5,000 N. The mean compressive force leading to failure was 4,400 N (CI 4,122–4,678 N) for nail osteosynthesis and 4,429 N (CI 3,653–5,204 N) for plate osteosynthesis (p = 0.943). Proximal cutting out of the osteosynthesis was the most common reason for interruption in the nail and plate osteosyntheses. Significant differences between the retrograde femoral nail and plate osteosyntheses were seen under testing conditions for plastic deformation and stiffness of the constructs (p = 0.002 and p = 0.001, respectively).
Conclusion
Based on our results, no statements regarding the superiority of either of the devices can be made. Even though the load to failure values for both osteosyntheses were much higher than the loads experienced during normal walking; however, because only axial loading was applied, it remains unclear whether both osteosyntheses meet the estimated requirements for postoperative full weight-bearing for an average heavy patient with a distal femoral fracture.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Distal femoral fractures are often considered to be the result of high-energy trauma typically occurring in young men. However, previous epidemiologic studies have shown that the incidence of these fractures increases dramatically in old age [33, 37, 39, 40]. Moreover, these fractures mostly occur in women, and are linked to only moderate trauma and osteoporosis [27]. Due to an ongoing demographic change, a further increase in geriatric distal femoral fractures is expected. Due to preexisting comorbidities in such an elderly group of patients with additionally poor bone stock quality, unstable distal femoral fractures can be difficult to treat.
In this context, achieving total relief (or at least partial weight-bearing) postoperatively presents an additional challenge.
For early mobilization, recovery of the axis, length and rotation in the dia- and metaphyseal area and proper fixation of the condylar region are of major importance. Until the 1990s, open reduction internal fixation (ORIF) osteosynthesis, in which anatomical reconstruction is achieved through extensive surgical approaches, was performed. This often affected microvascular circulation, leading to delayed fracture healing, non-union and infections following plate osteosyntheses in up to 80 % of treated patients [24, 29]. Because of these complications, a shift towards “biological” osteosynthesis using minimally invasive approaches, such as those already performed in nailing, occurred in plate osteosynthesis.
During the last decade, a series of new implants have been developed, in particular, locking plates and nailing systems [16]. Retrograde intramedullary nails allow minimally invasive fracture fixation due to their anatomic design and the surgical approach. Nevertheless, opening of the knee joint can be problematic. The primary drawbacks of this approach include persistent knee pain in up to 25–55 % of cases [21, 30] and difficulties in anatomical repositioning, resulting in high rates of malrotation (11–22 %) [17, 30] and non-union (6–15 %) [5, 19, 25, 30].
With the newest generation of polyaxial plates with angular stability, promising extramedullary fixation devices are now available for the treatment of supracondylar femoral fractures. In addition to improved stability, angle-stable plate systems also offer the possibility of soft tissue protection and indirect fracture repositioning by plate insertion through a minimally invasive approach [32].
Currently, retrograde femoral nails and the minimally invasive implantation of plates are the two main osteosynthesis strategies for the surgical treatment of extra-articular distal femoral fractures. Nevertheless, the optimal choice of surgical treatment device for these fractures remains unclear [42]. Therefore, the purpose of the present study was to compare the characteristics of a polyaxial angle-stable plate with those of a retrograde intramedullary femoral nailing device for the surgical stabilization of unstable distal femoral fractures in a biomechanical testing setup.
It was expected that nail osteosynthesis would provide increased stiffness and allow less plastic deformation of the construct as compared with plate osteosynthesis. Similar failure loads for both osteosynthesis devices were expected.
Materials and methods
Eight pairs of matched adult human cadaver femora were available for this study. These paired femora were obtained from human cadavers that had been embalmed with a solution consisting of 96 % ethanol and <2 % formaldehyde. During perfusion, approximately 15 L of the solution was passed through the femoral artery. The human cadavers were stored for at least 1 year before use [38]. The femora were donated from the Institutes of Anatomy and Cell Biology of Philipps University, Marburg, Germany. All donors provided written consent by their own free will for the use of their body for research purposes. The specimens originated from three male and five female adults with an average age of 79 years (range 63–100 years).
To exclude damage related to preexisting fractures or osteolyses, all specimens were examined for integrity via a clinical examination and a X-ray examination using a c-arm unit. The surrounding soft tissue was stripped from the specimens. Bones were then wrapped in moist towels using the aforementioned embalming solution and stored in a cooling chamber at 4 °C to avoid drying artifacts. Peripheral quantitative computed tomography (pQCT) measurements were used to record bone mineral density (BMD). For the pQCT measurements, a Stratec XCT Research SA+ instrument was used (Stratec Medizintechnik GmbH, Pforzheim, Germany). Measurements of cortical and cancellous BMD were performed at the condylar region. The baseline intact stiffness of each specimen was calculated (loading curves/slopes of displacement). For this purpose, intact femora were tested with 20 compressive cyclic loads at 0.25 Hz, and the loads were ramped between 200 and 1,000 N. A regression line was then calculated using the crude data points. The bones were truncated to a length of 30 cm from the distal femoral end, thereafter.
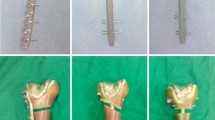
The implants compared in this study were the non-contact bridging plate for the distal femur (NCB-DF) (CE marketing 0086) and a M/DN retrograde femoral nail (CE marketing 0086) (both from Zimmer Inc., Winterthur, Switzerland). All locking plates (NCB-DF nine-hole plates) used were angle-stable. Five screws were positioned in the cancellous bone in the condylar region. The plates used, additionally provided ten holes for diaphyseal bone fixation. In the experimental setup eight of these holes were located proximal to the fracture gap. The screws in the four most proximal holes were bicortically positioned (Fig. 1). The retrograde femoral nails were fixed using two screws in the diaphyseal bone and using three locking screws in the condylar region. Osteosyntheses, using the original targeting devices for plate and retrograde femoral nail fixation, were performed on the specimens according to a randomized design. A single study surgeon (BC) implanted eight retrograde reamed femoral nails (Group A) and the same number of NCB-DF plates with polyaxial fixed angle screws (Group B). After performing the osteosynthesis, a standardized osteotomy was created using a surgical oscillating saw. As fracture model an unstable supracondylar femoral fracture was simulated (33-A3 in the AO/OTA classification). The fracture gap was established similarly to the fracture model published by Zlowodzki et al. [45]. A 2-cm gap osteotomy was created perpendicular to the anatomic axis of the femur. The distal cut was made at the level of three-quarters of the width of the distal femur above the intercondylar notch (Fig. 1). The femora were then embedded in Technovit 3040 (Heraeus, Wehrheim, Germany), a thermosetting resin that is suitable for biomechanical testing. The femora were potted into special containers in such a way that the femora were aligned in an anatomical, slightly valgus position of 5–7° relative to the ground. The samples were thawed at room temperature before testing. The proximal part of the bone construct was loaded through a hollow plastic cylinder which was approximately 4 cm tall and 3 cm wide. The cylinder was movable in two directions (anterior–posterior and medial–lateral), allowing movements of the proximal femur during loading. The femoral condyles were statically fixed in a metal cylinder.
Subsequently, each femur was subjected to cyclic loading on an Instron 5566 universal testing machine (Instron Corp., Darmstadt, Germany) (Fig. 2). According to a standardized protocol, each femur was subject to a preload of 100 N to compress the specimen and to avoid deformation artifacts in the bone construct, which might occur under minimal loading. Cyclic loading tests were then conducted at a constant speed of 125 mm/min. At this speed, loading was applied until the desired maximum force was reached. In this way, a maximum cycling frequency of 1 Hz was reached. As the compression force increased, the frequency declined. At the end of the test, the loading machine stopped automatically.
The test sequence started with 500 cycles at 1,000 N. The load was continuously raised in steps of 500 N every 500 cycles until the maximum force of 500 cycles with 5,000 N was reached. Criteria that lead to premature discontinuation of testing were the failure of osteosynthesis. As secure indicators of osteosynthesis failure sudden loss of measured force (>20 %) and major deformation of the bone construct (>30 mm) were defined.
Stiffness was calculated for all osteosyntheses using a method analogous to that described above for determining the baseline stiffness of the specimens.
The data were collected at 100 ms intervals using the instrument-specific Bluehill Software. In all tests plastic deformation, as a measure of irreversible deformation under the influence of forces, was recorded automatically by the Bluehill software using the maximum value in the last cycle. Therefore, plastic deformation indicated deformation that persisted after removal of the deformation-inducing load.
Loading (N), compression set (mm) and the number of cycles were recorded. In addition 95 % confidence intervals (CIs) were determined. The data were statistically analyzed using either Student’s t test or, where appropriate, a paired Student’s t test. Statistical significance was set at p < 0.05.
Results
BMD measurements and baseline axial stiffness testing before osteosynthesis
BMD analysis, using the pQCT measurements, revealed compromised bone quality for the cancellous bone in all examined specimens (mean 146.13 mg/cm3) in comparison to a reference specimen (198.53 mg/cm3) obtained from a 31-year-old patient (Fig. 3). BMD was comparable in all examined matched pairs of cadaver femora (p = 0.671).
All constructs survived loading with 20 compressive load cycles at 0.25 Hz, when the force was ramped between 200 and 1,000 N. No significant differences in axial bone stiffness were observed between the matched contralateral sides of the specimens (p = 0.135). Figure 4 shows the calculated bone stiffness of the eight paired femora and compares the right and left sides. The highest axial stiffness was exhibited by a right side sample at 0.94 kN/mm, and the lowest axial stiffness was exhibited by a left side sample at 0.36 kN/mm. The average difference between contralateral sides was 0.16 kN/mm (CI 0.05–0.26 kN/mm).
Cyclic testing of nail and plate osteosynthesis
All examined specimens survived at least 2,500 N. Five plate osteosyntheses and five nail osteosyntheses failed at a compressive force between 4,000 and 5,000 N. Four of the 16 specimens survived a maximum load of 5,000 N (three specimens with nail osteosyntheses and one specimen with plate osteosynthesis) (Fig. 5). The mean compressive force at failure was 4,400 N (CI 4,122–4,678 N) for the five nail osteosynthesis that failed and 4,429 N (CI 3,653–5,204 N) for the seven plate osteosynthesis that failed (p = 0.943) (Fig. 5). No significant differences in mean BMD (153.25 vs. 143.87 mg/cm3; p = 0.467) or in baseline axial bone stiffness (0.80 vs. 0.65 kN/mm; p = 0.116) were observed for the four surviving specimens compared to the 12 failing specimens.
In Group A, five nail osteosyntheses failed. All collapsed specimens failed due to diaphyseal transverse fracture through the proximal screws. Testing was not discontinued due to deformation of the construct for the nail osteosyntheses. In Group B, seven specimens with plate osteosynthesis failed. In four specimens diaphysis developed a fracture line that included all four proximal and distal screw holes. In one specimen, the cancellous bone screws in the condylar region in the distal part of the osteosynthesis broke out. Major deformation of the bone construct occurred for two specimens and their testing was discontinued (Fig. 6a–d).
Plastic deformation and stiffness of the osteosynthesis
Figure 7 shows a graph of plastic deformation in the plate and nail osteosyntheses up to a maximum load of 5,000 N. Failing osteosyntheses are not included in the graph; thus, not all specimens are included beyond a load of more than 2,500 N. The plastic deformation measured in the plated group was significantly larger (p = 0.002) than that measured in the nail group (Fig. 7). In addition, construct stiffness significantly differed between the two osteosynthesis groups (p < 0.001). With a mean stiffness of 1.52 kN/mm (CI 1.38–1.66 kN/mm) nail osteosynthesis was stiffer than plate osteosynthesis, which had a mean stiffness value of 0.97 kN/mm (CI 0.82–1.12 kN/mm).
The mean plastic deformation in plate and nail groups plotted against the applied load. For each mean value, half bars illustrating the standard deviation are shown. For the mean values of plate osteosynthesis, the half bars only go upwards. For the mean values of nail osteosynthesis, the half bars only go downwards. At loading steps from 1,000 to 2,500 N eight nails and eight plates were tested. Due to implant failure, only eight nails and seven plates were tested at a load of 3,000 N. At a load of 3,500 N eight nails and six plates remained for testing. At a load of 4,000 N seven nails and six plates were tested. At a load of 4,500 N three nails and four plates were tested. At a maximum load of 5,000 N three nails and one plate were tested
Based on a load of 2,500 N, an additional analysis of plastic deformation was performed in both osteosynthesis groups. The mean plastic deformation, which is a measure of irreversible deformation, was 0.29 mm (CI 0.07–0.50 mm) for nail osteosynthesis and 0.76 mm (CI 0.27–1.25 mm) for plate osteosynthesis. Differences in plastic deformation between the retrograde femoral nail and plate osteosynthesis at 2,500 N were statistically significant (p = 0.006). A separate stiffness calculation was also performed at a load of 2,500 N. As previously shown for stiffness over all loading steps, at a load of 2,500 N, the nail osteosynthesis (mean 1.55 kN/mm; CI 1.25–1.85 kN/mm) was significantly stiffer than the plate osteosynthesis (mean 0.91 kN/mm; CI 0.58–1.25 kN/mm) (p < 0.001) (Fig. 8).
Discussion
Compromised bone stock quality and the need for early mobilization in a mostly elderly patient group have always been considered difficult to arrange. For the surgical treatment of extra-articular distal femoral fractures, the retrograde femoral nail, as an intramedullary device, and locking plates for extramedullary fixation are commonly used [12, 22, 43]. The indications for both procedures overlap. Implant failure in supracondylar femoral fractures remain a common problem with retrograde nail osteosynthesis failure reported in up to 38 % of cases [36]. Similar results using the less invasive stabilization system (LISS plate) with implant failure rates of up to 20 %, have been published [8]. Due to these high rates of osteosynthesis-related failures, further experimental investigations concerning the strength and failure modes of these implants used are necessary. Therefore, in this study, the properties of the newest generation of a polyaxial locking plate were analyzed and compared with a retrograde femoral nail for the stabilization of unstable extra-articular distal femoral fractures. As assumed, the present study could prove that nail osteosynthesis provided increased stiffness and less plastic deformation as compared to plate osteosynthesis. Failure loads for both osteosynthesis devices were comparable.
In plate osteosyntheses, two failures due to major deformation and one failure due to cutting out of the cancellous bone screws in the condylar region occurred. In all other failing specimens diaphysis developed a fracture line that included all four proximal and distal screw holes which was the reason for collapse. No fracture of screws or screw loosening occurred. These biomechanical findings agree with the results of several clinical studies reporting on the failure of locking plate osteosynthesis, which is mostly located within the zone proximal to the fracture and is attributed to screw pull out or screw loosening [20, 31, 34]. The present experimental setup used bicortical screw fixation; however, in clinical trails reporting on the failure of plate osteosynthesis, monocortical screw fixation has mostly been performed, which might be a cause for failure. In all of the failing specimens fixed with nail osteosynthesis, the results of the present study revealed that diaphyseal transverse fracture through the proximal screw was the reason for failure. These results contradict to our own clinical experience and the results of a multitude of clinical studies that have primarily reported failure of the distal screws [1, 26, 36], even enabling the opportunity for nail migration into the knee [13, 30]. This elevated rate of diaphyseal transverse fracture through the proximal screw in nail osteosynthesis might be explained by the fact that only an axial load was applied. Under in vivo conditions, the femur is subjected not only to axial loading but also to bending, shearing and torsional loads during many daily activities. For some activities, such as rising from a chair or climbing stairs with the hip and knee in moderate to high flexion, both torsion and bending can contribute substantially to local stresses in the femoral mid-shaft. Closer to the knee joint, it is likely that the amount of bending decreases. Nevertheless, the complexity of the in vivo loading on the femur is unlikely to be fully captured under the axial-only loading condition used here.
Our cyclic loading tests confirmed that retrograde femoral nail osteosynthesis creates a stiffer construct than locking plates (1.52 vs. 0.91 kN/mm at 2,500 N), possibly because the nail osteosynthesis is positioned intramedullary and therefore acts as a rod model. The decrease in plastic deformation for the nails past a load of 4,000 N is more likely related to the fact there are fewer specimen and those with higher plastic deformation had already failed than to the fact that stiffness would decrease at higher loading steps in general (Fig. 7). Plates exhibited greater plastic deformation than nails (0.29 vs. 0.76 mm at 2,500 N). These findings are in consistent with a multitude of other biomechanical studies investigating osteosynthesis stiffness and osteosynthesis movement in various fracture models [10, 23, 41, 44]. Using an osteoporotic saw-bone model Wähnert et al. [41] investigated four different implants (T2 intramedullary nail, supracondylar nail, distal femoral nail, AxSOS angular plate) under torsional and axial loading conditions. Concerning cyclic axial loading their results confirm findings of the present study, with intramedullary nails showing higher stiffness as compared to plate osteosynthesis.
In an experiment using matched pairs of fresh frozen human cadaveric bones, Zlowodzki et al. analyzed the properties of a retrograde intramedullary nail, an angled blade plate and a locked internal fixator (LISS plate) regarding fixation of distal femur fractures. The authors showed that intramedullary nails (696 N/mm) offered a higher degree of stiffness than angled blade plates (171 N/mm) and LISS plates (111 N/mm) [44]. In an experimental setup with synthetic femurs, Heiney et al. [14] showed that a retrograde intramedullary nail allowed significantly less micromotion across the osteotomy gap than a dynamic condylar screw and a locked condylar plate. Micromotion over the osteotomy gap was not analyzed; instead, motion of the osteosyntheses based on movements of the actuator were measured, which are typically an order of magnitude greater than measurements of fracture gap motion. Nevertheless, this biomechanical analysis provides further evidence that plate osteosynthesis is a more flexible construct than the retrograde intramedullary nail but has comparable loading capacities. In contrast to the use of conventional compression plates, which aim for primary bone healing, the bridge plating technique with locking plate osteosynthesis leads to secondary bone healing [3, 7]. In this context, it is known that secondary bone healing dispends on the existence of some strain at the fracture site [11]; thus, axial micro-movements in particular have been shown to be beneficial, as studied in clinical and simulated tibial fractures [18]. Due to its extramedullary design, especially locking plate osteosynthesis induces some interfragmentary motion at the cortex opposite to the plate, while motion is reduced at the cortex adjacent to the plate [6]. The opportunity for minimally invasive implantation of a plate, which would lead to lower rates of soft tissue complications, could additionally improve the healing process [32].
Nevertheless, when fracture strain exceeds the healing threshold, evidence exists from biomechanical and animal studies that bone healing can be disturbed, leading to nonunion, malunions or implant failure [4, 15]. Therefore, it should be noted that the optimal balance between fixation stiffness, elasticity and micromotion for fracture healing has not yet been entirely clarified.
In vivo biomechanical loading analyses of femur and hip contact forces during gait patterns were conducted by Bergmann et al. [2]. They could show that forces affecting the lower limb increase to as high as 240 % of body weight during normal walking so as up to 250 and 260 % of body weight when going upstairs and downstairs, respectively. Such a long-term stress test within the meaning of a gait simulator, using torsional so as bending forces, was not conducted in this experimental setting. Even though the load to failure values measured in this study were much higher than those experienced during normal walking, due to restrictions to the only axial loading mode with no muscle forces considered, it remains unclear whether both osteosyntheses exactly meet the estimated requirements for postoperative full weight-bearing for an average heavy patient (70 kg) [2]. Nevertheless, the loading values used represent the clinical situation of partial to full weight-bearing, which should be achieved after the surgical treatment of these fractures in geriatric patients. Considering the results of Bergmann et al. the results of this study suggest that both osteosyntheses enable satisfactory and comparable results.
pQCT measurements were used to analyze the structural bone quality of the specimens examined. The mean bone mass of examined specimens in this study was 146.13 mg/cm3; thus, the measured bone mass was less than that of our reference specimen (198.53 mg/cm3) and less than the reference value of 158.01 mg/cm3 published by Niedhart et al. [28] who reported averaged pQCT measurements for the distal radius, lumbar spine and proximal femur in patients aged from 71 to 80 years. Among a group of 36 volunteers (mean age 39 years), Sievänen et al. [35] found a mean trabecular density of 231.3 mg/cm3 (±29.5 mg/cm3) based on pQCT measurements of the distal femur. The BMD of the specimens used in this experiment (mean value 146.13 mg/cm3) was far lower than that found by Sievänen et al. in a younger reference population. Considering the standard deviation for healthy young patients reported by Sievänen et al. the bone mass of our reference specimen (198.53 mg/cm3) appears within the normal range. Realistic test conditions for an elderly patient population were simulated using specimens with compromised structural bone quality. Unlike other biomechanical examinations of osteoporotic bones, in this experimental setup, failing specimens showed no significant difference in BMD as compared to surviving constructs (p = 0.467) [9]. A larger number of samples might have helped to reach statistical significance regarding this point. Although no statistical significance for BMD was observed in this experimental setup, it can be presumed that decreased bone quality is a limiting factor for fracture stabilization even if optimal reduction and implant positioning is achieved. The bone model itself appears to have not influenced the study results. A recently published biomechanical study showed that embalmed femura had characteristics similar to fresh frozen bones [38]. Therefore, it was suggested that embalmed human cadaveric bones are suitable for the mechanical testing of orthopedic and trauma devices.
Conclusion
Even though the load to failure values measured in this study were much higher than those experienced during normal walking, due to restrictions to the only axial loading mode it is not possible to decide which of the devices is superior. With respect to cyclic loading realistic conditions were simulated, suggesting that both osteosyntheses enable comparable results.
References
Aldrian S, Schuster R, Haas N, Erhart J, Strickner M, Blutsch B, Wernhart S, Leitgeb J, Platzer P (2013) Fixation of supracondylar femoral fractures following total knee arthroplasty: is there any difference comparing angular stable plate fixation versus rigid interlocking nail fixation? Arch Orthop Trauma Surg 133:921–927
Bergmann G, Deuretzbacher G, Heller M, Graichen F, Rohlmann A, Strauss J, Duda GN (2001) Hip contact forces and gait patterns from routine activities. J Biomech 34:859–871
Bottlang M, Doornink J, Fitzpatrick DC, Madey SM (2009) Far cortical locking can reduce stiffness of locked plating constructs while retaining construct strength. J Bone Joint Surg Am 91:1985–1994
Cristofolini L, Viceconti M, Cappello A, Toni A (1996) Mechanical validation of whole bone composite femur models. J Biomech 29:525–535
Duan X, Li T, Mohammed AQ, Xiang Z (2011) Reamed intramedullary nailing versus unreamed intramedullary nailing for shaft fracture of femur: a systematic literature review. Arch Orthop Trauma Surg 131:1445–1452
Döbele S, Horn C, Eichhorn S, Buchholtz A, Lenich A, Burgkart R, Nüssler AK, Lucke M, Andermatt D, Koch R, Stöckle U (2010) The dynamic locking screw (DLS) can increase interfragmentary motion on the near cortex of locked plating constructs by reducing the axial stiffness. Langenbecks Arch Surg 395:421–428
Egol KA, Kubiak EN, Fulkerson E, Kummer FJ, Koval KJ (2004) Biomechanics of locked plates and screws. J Orthop Trauma 18:488–493
Fankhauser F, Gruber G, Schippinger G, Boldin C, Hofer HP, Grechenig W, Szyszkowitz R (2004) Minimal-invasive treatment of distal femoral fractures with the LISS (Less Invasive Stabilization System): a prospective study of 30 fractures with a follow up of 20 months. Acta Orthop Scand 75:56–60
Fensky F, Nüchtern JV, Kolb JP, Huber S, Rupprecht M, Jauch SY, Sellenschloh K, Püschel K, Morlock MM, Rueger JM, Lehmann W (2013) Cement augmentation of the proximal femoral nail antirotation for the treatment of osteoporotic pertrochanteric fractures—a biomechanical cadaver study. Injury 44:802–807
Firoozbakhsh K, Behzadi K, DeCoster TA, Moneim MS, Naraghi FF (1995) Mechanics of retrograde nail versus plate fixation for supracondylar femur fractures. J Orthop Trauma 9:152–157
Greiwe RM, Archdeacon MT (2007) Locking plate technology: current concepts. J Knee Surg 20:50–55
Gwathmey FW, Jones-Quaidoo SM, Kahler D, Hurwitz S, Cui Q (2010) Distal femoral fractures: current concepts. J Am Acad Orthop Surg 18:597–607
Hartin NL, Harris I, Hazratwala K (2006) Retrograde nailing versus fixed-angle blade plating for supracondylar femoral fractures: a randomized controlled trial. ANZ J Surg 76:290–294
Heiney JP, Barnett MD, Vrabec GA, Schoenfeld AJ, Baji A, Njus GO (2009) Distal femoral fixation: a biomechanical comparison of trigen retrograde intramedullary (i.m.) nail, dynamic condylar screw (DCS), and locking compression plate (LCP) condylar plate. J Trauma 66:443–449
Hente R, Füchtmeier B, Schlegel U, Ernstberger A, Perren SM (2004) The influence of cyclic compression and distraction on the healing of experimental tibial fractures. J Orthop Res 22:709–715
Hwang JH, Oh JK, Oh CW, Yoon YC, Choi HW (2012) Mismatch of anatomically pre-shaped locking plate on Asian femurs could lead to malalignment in the minimally invasive plating of distal femoral fractures: a cadaveric study. Arch Orthop Trauma Surg 132:51–56
Hüfner T, Citak M, Suero EM, Miller B, Kendoff D, Krettek C (2011) Femoral malrotation after unreamed intramedullary nailing: an evaluation of influencing operative factors. J Orthop Trauma 25:224–227
Kenwright J, Goodship AE (1989) Controlled mechanical stimulation in the treatment of tibial fractures. Clin Orthop Relat Res 241:36–47
Kreb DL, Blokhuis TJ, van Wessem KJ, Bemelman M, Lansink KW, Leenen LP (2013) Intramedullary nailing without interlocking screws for femoral and tibial shaft fractures. Arch Orthop Trauma Surg 133:1109–1113
Kregor PJ, Stannard JA, Zlowodzki M, Cole PA (2004) Treatment of distal femur fractures using the less invasive stabilization system: surgical experience and early clinical results in 103 fractures. J Orthop Trauma 18:509–520
Leggon RE, Feldmann DD (2001) Retrograde femoral nailing: a focus on the knee. Am J Knee Surg 14:109–118
Link BC, Babst R (2012) Current concepts in fractures of the distal femur. Acta Chir Orthop Traumatol Cech 79:11–20
Meyer RW, Plaxton NA, Postak PD, Gilmore A, Froimson MI, Greenwald AS (2000) Mechanical comparison of a distal femoral side plate and a retrograde intramedullary nail. J Orthop Trauma 14:398–404
Miclau T, Holmes W, Martin RE, Krettek C, Schandelmaier P (1998) Plate osteosynthesis of the distal femur: surgical techniques and results. J South Orthop Assoc 7:161–170
Moed BR, Watson JT (1995) Retrograde intramedullary nailing, without reaming, of fractures of the femoral shaft in multiply injured patients. J Bone Joint Surg Am 77:1520–1527
Neubauer T, Krawany M, Leitner L, Karlbauer A, Wagner M, Plecko M (2012) Retrograde femoral nailing in elderly patients: outcome and functional results. Orthopedics 35:e855–e861
Ng AC, Drake MT, Clarke BL, Sems SA, Atkinson EJ, Achenbach SJ, Melton LJ (2012) Trends in subtrochanteric, diaphyseal, and distal femur fractures, 1984–2007. Osteoporos Int 23:1721–1726
Niedhart C, Braun K, Graf Stenbock-Fermor N, Bours F, Schneider P, Zilkens KW, Niethard FU (2003) The value of peripheral quantitative computed tomography (pQCT) in the diagnosis of osteoporosis. Z Orthop Ihre Grenzgeb 141:135–142
Perren SM (2002) Evolution of the internal fixation of long bone fractures. The scientific basis of biological internal fixation: choosing a new balance between stability and biology. J Bone Joint Surg Br 84:1093–1110
Ricci WM, Bellabarba C, Evanoff B, Herscovici D, DiPasquale T, Sanders R (2001) Retrograde versus antegrade nailing of femoral shaft fractures. J Orthop Trauma 15:161–169
Ricci WM, Streubel PN, Morshed S, Collinge C, Nork SE, Gardner MJ (2013) Risk factors for failure of locked plate fixation of distal femur fractures: an analysis of 335 cases. J Orthop Trauma 28:83–89
Ruchholtz S, El-Zayat B, Kreslo D, Bücking B, Lewan U, Krüger A, Zettl R (2013) Less invasive polyaxial locking plate fixation in periprosthetic and peri-implant fractures of the femur—a prospective study of 41 patients. Injury 44:239–248
Sasaki D, Hatori M, Kotajima S, Kokubun S (2005) Fatigue fracture of the distal femur arising in the elderly. Arch Orthop Trauma Surg 125:422–425
Schütz M, Müller M, Regazzoni P, Höntzsch D, Krettek C, Van der Werken C, Haas N (2005) Use of the less invasive stabilization system (LISS) in patients with distal femoral (AO33) fractures: a prospective multicenter study. Arch Orthop Trauma Surg 125:102–108
Sievänen H, Koskue V, Rauhio A, Kannus P, Heinonen A, Vuori I (1998) Peripheral quantitative computed tomography in human long bones: evaluation of in vitro and in vivo precision. J Bone Miner Res 13:871–882
Singh SK, El-Gendy KA, Chikkamuniyappa C, Houshian S (2006) The retrograde nail for distal femoral fractures in the elderly: high failure rate of the condyle screw and nut. Injury 37:1004–1010
Soveid M, Serati AR, Masoompoor M (2005) Incidence of hip fracture in Shiraz, Iran. Osteoporos Int 16:1412–1416
Topp T, Müller T, Huss S, Kann PH, Weihe E, Ruchholtz S, Zettl RP (2012) Embalmed and fresh frozen human bones in orthopedic cadaveric studies: which bone is authentic and feasible? Acta Orthop 83:543–547
Wang Z, Bhattacharyya T (2011) Trends in incidence of subtrochanteric fragility fractures and bisphosphonate use among the US elderly, 1996–2007. J Bone Miner Res 26:553–560
Weiss RJ, Montgomery SM, Al Dabbagh Z, Jansson KA (2009) National data of 6409 Swedish inpatients with femoral shaft fractures: stable incidence between 1998 and 2004. Injury 40:304–308
Wähnert D, Hoffmeier K, Fröber R, Hofmann GO, Mückley T (2011) Distal femur fractures of the elderly—different treatment options in a biomechanical comparison. Injury 42:655–659
Wähnert D, Hofmann-Fliri L, Götzen M, Kösters C, Windolf M, Raschke MJ (2013) Feasibility study on the potential of a spiral blade in osteoporotic distal femur fracture fixation. Arch Orthop Trauma Surg 133:1675–1679
Zlowodzki M, Bhandari M, Marek DJ, Cole PA, Kregor PJ (2006) Operative treatment of acute distal femur fractures: systematic review of 2 comparative studies and 45 case series (1989 to 2005). J Orthop Trauma 20:366–371
Zlowodzki M, Williamson S, Cole PA, Zardiackas LD, Kregor PJ (2004) Biomechanical evaluation of the less invasive stabilization system, angled blade plate, and retrograde intramedullary nail for the internal fixation of distal femur fractures. J Orthop Trauma 18:494–502
Zlowodzki M, Williamson S, Zardiackas LD, Kregor PJ (2006) Biomechanical evaluation of the less invasive stabilization system and the 95-degree angled blade plate for the internal fixation of distal femur fractures in human cadaveric bones with high bone mineral density. J Trauma 60:836–840
Acknowledgments
Zimmer Inc., Freiburg, Germany is acknowledged for providing the implants. We received no additional financial support for the execution of this study. In addition the Institutes of Anatomy and Cell Biology of Philipps University Marburg are acknowledged for their cooperation in making available the specimen.
Conflict of interest
S. R. and R. Z. are teaching consultants for Zimmer Inc. Freiburg, Germany. All other authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bliemel, C., Buecking, B., Mueller, T. et al. Distal femoral fractures in the elderly: biomechanical analysis of a polyaxial angle-stable locking plate versus a retrograde intramedullary nail in a human cadaveric bone model. Arch Orthop Trauma Surg 135, 49–58 (2015). https://doi.org/10.1007/s00402-014-2111-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-014-2111-8