Abstract
Introduction
Continuous ambulatory peritoneal dialysis is an important modality of renal replacement therapy in children. Catheter dysfunction (commonly obstruction) is a major cause of morbidity and is a significant concern that hampers renal replacement therapy. As omentum is a significant cause of obstruction, some recommend routine omentectomy during insertion of the peritoneal dialysis catheter. Omentopexy rather than omentectomy has been described in adults to spare the omentum as it may be needed as a spare part in many conditions. Laparoscopic approach is commonly preferred as it provides global evaluation of the peritoneal space, proper location of the catheteral end in the pelvis and lesser morbidity due to inherent minimally invasive nature.
Aim
The aim of this study is to present the technique of laparoscopic peritoneal dialysis catheter placement in children with concurrent omentopexy.
Methods
We retrospectively evaluated our patients who underwent laparoscopic placement of peritoneal dialysis catheter with concomitant omentopexy or omentectomy.
Results
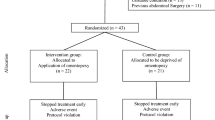
A total of 30 patients were enrolled who received either omentectomy (n = 18) or omentopexy (n = 12). Four catheters were lost in the omentopexy group (33%) and 3 in the omentectomy group (17%), but none were related to omental obstruction. Three out of 4 patients in the omentopexy group and 2 out of 3 patients in the omentectomy group had a previous abdominal operation as a potential cause of catheter loss. Previous history of abdominal surgery was present in 6 patients (50%) in the omentopexy group and 3 patients (17%) in the omentectomy group.
Conclusions
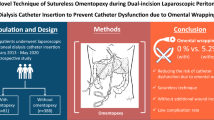
As omentum was associated with catheter failure, omentectomy is commonly recommended. Alternatively, omentopexy can be preferred in children to spare an organ that may potentially be necessary for many surgical reconstructive procedures in the future. Laparoscopic peritoneal dialysis catheter placement with concomitant omentopexy appears as a feasable and reproducible technique. Although the catheter loss seems to be higher in the omentopexy group, none was related with the omentopexy procedure and may be related to the higher rate of history of previous abdominal operations in this group.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Commonly, peritoneal dialysis is the first choice of kidney replacement therapy in children unless preemptive kidney transplantation is available [1]. Although the availability of donor kidneys is more common in children, many children rely on peritoneal dialysis for prolonged durations. In the long run, a significant rate of children need to convert to hemodialysis due to various conditions (loss of peritoneal surface and catheter-related problems). It is estimated that surgical complications within the first 3 months is around 40%, about 25% need revision surgery in the first 6 months [2, 3]. One of the most common, potentially preventable causes of catheter-related complications is obstruction and one of the major causes of obstruction is the omentum [4]. To prevent this complication, omentectomy is commonly recommended in children and adults [5, 6].
In this study, our aim is to evaluate and compare the patients who underwent laparoscopic peritoneal dialysis catheter insertion with concomitant omentectomy or omentopexy.
Materials and methods
The patients who received laparoscopic peritoneal catheter insertion between 2010 and 2023 are enrolled in the study. Omentectomy was the choice of technique employed to reduce the omentum-related catheter dysfunction between 2010 and 2020. After 2020, omentopexy was employed rather than omentectomy while performing peritoneal catheter placement in our patients. Omentopexy was performed by a single surgeon while omentectomy was performed by different attending surgeons. The patients who underwent open surgery, who were converted to open surgery, and who did not receive either omentectomy or omentopexy are not included in the study. The demographics of the patients, the etiology of end-stage kidney disease, catheter survival rates, duration of follow-up and history of previous operations are evaluated, and the surgical technique of omentopexy is described.
Results
A total of 30 patients were enrolled in the study who received either omentectomy (n = 18) or omentopexy (n = 12) during insertion of tunneled peritoneal catheter. Omentectomy Group consisted of 18 patients who underwent laparoscopic catheter insertion with concomitant omentectomy between 2010 and 2020. Median follow-up duration was 14.5 months (1–180 months, min.–max.) Underlying conditions were lower urinary tract dysfunction in 5 (neurogenic bladder dysfunction) and renal parenchymal disease in 13 (nephritic syndrome, nephrotic syndrome, etc.). The mean age of the omentectomy group was 11.87 months (4.28; standard error) with 13 girls (72%) and 5 boys (28%). No complication was encountered during or after surgery in any of the patients in this group. Three catheters (17%) were lost in a median follow-up of 13 months (6–144 months; min.–max.). All were lost due to loss of peritoneal surface (peritonitis, intestinal adhesions) and none was related to omentum. Three patients (16%) in the whole group had a history of previous abdominal surgery (ventriculoperitoneal shunt (VPS), intestinal surgery) and 2 of them were among the patients who had lost the catheter. Seven patients received kidney transplantation and 2 patients deceased during follow-up.
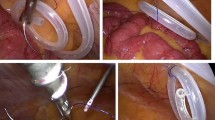
After 2020, 12 patients underwent laparoscopic catheter placement with omentopexy with a median follow-up duration of 10.5 months (1–40 months; min.–max.). All surgeries were performed by a single surgeon with a three port technique. The technique is briefly as follows: a 5-mm port was inserted by an open technique from the umbilical crease. Other 5 mm port sites were arranged in a triangular fashion depending on the patient’s anatomy, previous scars, body habitus and age. After inspection of the peritoneal surface, omentum was imbricated with a nonabsorbable monofilament suture and then fixed either to the falciform ligament (initial four patients) (Fig. 1a) or onto itself close to it's root (Fig. 1b) (remaining eight patients) close to its root. The catheter was introduced into the abdomen from a port site under direct vision and directed to the pelvis with a laparoscopic grasper (see Supplementary Video 1). In the initial five patients, the catheter was fixed to the peritoneum at the lower midline to prevent wandering in the abdomen. However, we quit fixation of the catheter after we experienced a catheter obstruction due to intestinal adhesion to the fixation site causing catheter obstruction (which was relieved by laparoscopic adhesiolysis and the catheter was salvaged) 5 months after initial placement (Fig. 2). Then, the catheter was introduced to the other skin exit site through a subcutaneous or rectus sheath tunnel with the help of a special guiding sharp trocar mounted on the catheter (Fig. 3). In conclusion, the first cuff remained in the extraperitoneal space under the fascial layer and the second cuff remained in the subcutaneous or interfascial space approximately 2 cm away from the skin exit site (Fig. 3). No sutures were needed (nor recommended) for the catheter exit site.
Tunneling of the catheter. Subcutaneous tunnel is performed with the help of a sharp introducer from the port site to a skin exit site (a). Final appearance (b). Note that skin exit is exactly the same diameter with the catheter (even tight) that may potentially reduce the exit site and tunnel complications (granuloma development, infection, leaks..) (c). The final location of the catheteter in the pelvis (d)
Mean age of the patients with omentopexy is 10.63 years (3.32 years; min.–max.) with seven girls (58%) and five boys (42%). Mean surgical duration was 67,666 ± 4707 min in the Omentectomy Group and 65,965 ± 3279 min in the Omentopexy Group (p = 0.517). The underlying cause of end-stage kidney disease was lower urinary tract dysfunction (neurogenic bladder) in 5 patients and renal parenchymal conditions (nephrotic syndrome, cystinosis, etc.) in 7 patients. Four catheters (33%) were lost during follow-up in a median duration of 5.5 months (1–31 months; min.–max.). Six patients (50%) in the whole group had a history of previous abdominal surgery (intestinal/colonic surgery, VPS, transperitoneal nephrectomy) and three of them were among the patients who had lost the catheter. All patients that lost the catheter had at least one episode of peritonitis. Bleeding occurred in one patient during the creation of the rectus sheath tunnel which was stopped after passing the catheter through the tunnel and did not cause any postoperative problems. Two patients received kidney transplantation during follow-up and no patient was deceased.
Discussion
Peritoneal dialysis is the preferred technique for kidney replacement therapy in children with end-stage kidney failure [1, 7]. It is a precious technique in children with many advantages and its endurance in the long term is important as other techniques are not exact substitutes for peritoneal dialysis which increases the burden on the family, the patient, and the health system. Therefore, endurance and longevity of the components of this modality are significantly underscored in children.
The major causes of the need for conversion from peritoneal dialysis to hemodialysis are catheter-related infections, catheter occlusion, and loss of peritoneal surface [2, 3, 6]. Catheter occlusion emerges as a preventable contributor to catheter dysfunction which is often attributed to the omentum, yet it’s not the only cause [4, 8, 9]. Accordingly, prophylactic omentectomy is a common (but not universal) recommendation during the insertion of a dialysis catheter to prevent omentum-related complications [5, 6, 10].
Omentum is a fibro-adipose tissue which was considered useless in earlier times [11]. As it is a lymphoid organ with a high regenerative potential, it is gaining prominence in reconstructive procedures in the abdomen, thorax, and even in the cranium [12,13,14,15]. It can be used in many procedures as a pedunculated flap, free flap, or an implantation field for tissue growth [16,17,18]. Due to these concerns, omentopexy rather than omentectomy is used in adults to preserve the omentum as a spare part for possible future reconstructive purposes [19, 20].
To improve the health care of children and reserve the omentum for possible future medical conditions, omentopexy stands as a reasonable alternative to omentectomy. Omentopexy can be performed by wrapping on itself, fixation to the abdominal wall, or fixation to the falciform ligament. Although many authors advocated fixing the omentum to the peritoneum of the abdominal wall, we refrained from doing so as it may divide the abdominal cavity into compartments and predispose to a potential hazard of internal herniation of the viscera around the fixation point [19,20,21].
As described previously by others, we performed fixation of the omentum to the falciform ligament by monofilament permanent sutures as it appears as a durable structure that prevents detachment of the omentum and the ligature (Fig. 1a) [22]. After four cases without any incident, we began to perform wrapping of the omentum on itself by monofilament permanent sutures (Fig. 1b). One of the reasons for changing our practice is the theoretical concern about internal herniation around the fixation point of the falciform ligament, raised by the seniors in our clinic. Theoretically, the fixation point is located high in the abdomen relatively away from the intestine and we do not think there remains a significant window for visceral herniation between the liver, the falciform ligament, and the omental radix. Nevertheless, driven by our seniors and relying on the experience of other authors, we performed self-wrapping of the omentum at its basis in the remaining 8 patients [23, 24]. We did not experience any adverse event related to the wrapping of the omentum on itself (bleeding, omental detaching, catheter obstruction by the omentum, etc.). Nevertheless, both, wrapping the omentum on itself or suturing it to the falciform ligament, appears to be safe and reasonable in our limited experience, and can be preferred depending on the attending surgeon’s choice.
In our series, the rate of catheter loss is higher in the Omentopexy Group than in the Omentectomy Group (33% vs. 17%). The cause of the catheter loss was not related to the omentum itself in any of the patients in both groups. A notable difference between the groups of our study is the higher rate of previous abdominal operations in the Omentopexy Group (50% vs. 16%). Among the patients with previous abdominal surgery, 3 out of 4 patients in the Omentopexy Group and 2 out of 3 patients in the Omentectomy Group lost the catheter during follow-up. Although previous abdominal surgery is not a strict contraindication for peritoneal dialysis, it is associated with higher rates of catheter loss [25, 26]. Although the presence of colostomy or VPS is also a risk factor for catheter loss in patients under peritoneal dialysis treatment, it is not considered a strict contraindication but increased risk of complications should be anticipated and shared with the family during the preoperative process [1, 26].
The major limitations of our study are the small sample size of the groups and retrospective design of the study.
Conclusion
Initial experience with laparoscopic dialysis catheter placement with omentopexy in children seems to be a feasible and reproductive technique that spares the omentum. Appearing higher rates of catheter loss in the omentopexy group may be related to the higher rates of previous abdominal surgeries and none was related to the omentopexy procedure. We believe that the laparoscopic approach for peritoneal dialysis catheter insertion with omentopexy can reduce the morbidity and increase the longevity of dialysis therapy in chronically ill patients.
Data availability
Supplementary data is not applicable.
References
de Galasso L, Picca S, Guzzo I (2020) Dialysis modalities for the management of pediatric acute kidney injury. Pediatric Nephrology (Berlin, Germany) 35(5):753–765
Radtke J, Lemke A, Kemper MJ, Nashan B, Koch M (2016) Surgical complications after peritoneal dialysis catheter implantation depend on children’s weight. J Pediatr Surg 51(8):1317–1320
Phan J, Stanford S, Zaritsky JJ, DeUgarte DA (2013) Risk factors for morbidity and mortality in pediatric patients with peritoneal dialysis catheters. J Pediatr Surg 48(1):197–202
Esposito F, Di Serafino M, Ambrosio C, Panico MR, Malacario F, Mercogliano C et al (2016) Chronic peritoneal dialysis in children: the role of ultrasound in the diagnosis of peritoneal catheter obstruction. J Ultrasound 19(3):191–196
David VL, Mussuto E, Stroescu RF, Gafencu M, Boia ES (2023) Peritoneal dialysis catheter placement in children: initial experience with a “2+1”-port laparoscopic-assisted technique. Medicina (Kaunas) 59(5):961
Ladd AP, Breckler FD, Novotny NM (2011) Impact of primary omentectomy on longevity of peritoneal dialysis catheters in children. Am J Surg 201(3):401–404 (discussion 4–5)
Hataya H (2018) Current state of peritoneal dialysis in children. Contrib Nephrol 196:129–134
Rasmussen SK (2022) An overview of pediatric peritoneal dialysis and renal replacement therapy in infants: a review for the general pediatric surgeon. Semin Pediatr Surg 31(3):151193
Keramati MR, Abbaszadeh-Kasbi A, Keshvari A (2018) Laparoscopic omentopexy, rectus sheath tunneling and implantation of the peritoneal dialysis catheter using a peritoneal dialysis port peritoneal dialysis international. J Int Soc Peritoneal Dial 38(3):187–191
Schuh MP, Nehus E, Liu C, Ehlayel A, Clark S, Chishti A et al (2021) Omentectomy reduces the need for peritoneal dialysis catheter revision in children: a study from the Pediatric Nephrology Research Consortium. Pediatr Nephrol (Berlin, Germany) 36(12):3953–3959
Liebermann-Meffert D (2000) The greater omentum. Anatomy, embryology, and surgical applications. Surg Clin North Am 80(1):275–293
Mazzaferro D, Song P, Massand S, Mirmanesh M, Jaiswal R, Pu LLQ (2018) The Omental free flap-a review of usage and physiology. J Reconstr Microsurg 34(3):151–169
Botianu PVH (2019) Current indications for the intrathoracic transposition of the omentum. J Cardiothorac Surg 14(1):103
Collins D, Hogan AM, O’Shea D, Winter DC (2009) The omentum: anatomical, metabolic, and surgical aspects. J Gastrointest Surg 13(6):1138–1146
Losken A, Carlson GW, Culbertson JH, Scott Hultman C, Kumar AV, Jones GE et al (2002) Omental free flap reconstruction in complex head and neck deformities. Head Neck 24(4):326–331
Fay LY, Lin YR, Liou DY, Chiu CW, Yeh MY, Huang WC et al (2021) The application of an Omentum graft or flap in spinal cord injury. Int J Mol Sci 22(15)
Kulkarni SB, Barbagli G, Joshi PM, Hunter C, Shahrour W, Kulkarni J et al (2015) Laparoscopic omentoplasty to support anastomotic urethroplasty in complex and redo pelvic fracture urethral defects. Urology 85(5):1200–1205
Wiltfang J, Rohnen M, Egberts JH, Lützen U, Wieker H, Açil Y et al (2016) Man as a living bioreactor: prefabrication of a custom vascularized bone graft in the gastrocolic omentum. Tissue Eng Part C Methods 22(8):740–746
Oğünç G, Tuncer M, Oğünç D, Yardimsever M, Ersoy F (2003) Laparoscopic omental fixation technique versus open surgical placement of peritoneal dialysis catheters. Surg Endosc 17(11):1749–1755
Smith BM, Dan AG (2020) Operative technique for laparoscopic placement of continuous ambulatory peritoneal dialysis catheter. J Laparoendosc Adv Surg Tech A 30(7):815–819
Attaluri V, Lebeis C, Brethauer S, Rosenblatt S (2010) Advanced laparoscopic techniques significantly improve function of peritoneal dialysis catheters. J Am Coll Surg 211(6):699–704
Kou HW, Yeh CN, Tsai CY, Lee CW, Hsu JT, Wang SY et al (2023) A novel technique of sutureless omentopexy during dual-incision laparoscopic peritoneal dialysis catheter insertion to prevent catheter dysfunction due to omental wrapping. Surg Endosc 37(1):148–155
Crabtree JH, Fishman A (2003) Selective performance of prophylactic omentopexy during laparoscopic implantation of peritoneal dialysis catheters. Surg Laparosc Endosc Percutaneous Tech 13(3):180–184
Cao W, Tu C, Jia T, Liu C, Zhang L, Zhao B et al (2019) Prophylactic laparoscopic omentopexy: a new technique for peritoneal dialysis catheter placement. Ren Fail 41(1):113–117
Bouty A, Faure A, Shaw L, Ah Toy J, Dobremez E, O’Brien M et al (2017) Is peritoneal dialysis feasible after laparotomy in children? A case-control series to compare outcomes. J Pediatr Urol 13(6):612.e1–612.e7
Chan EYH, Borzych-Duzalka D, Alparslan C, Harvey E, Munarriz RL, Runowski D et al (2020) Colostomy in children on chronic peritoneal dialysis. Pediatr Nephrol (Berlin, Germany) 35(1):119–126
Funding
No funding is granted for the present study.
Author information
Authors and Affiliations
Contributions
All authors of the manuscript; made substantial contributions to the conception or design of the work, or the acquisition, analysis, or interpretation of data, or the creation of new software used in the work, drafted the work or revised it critically for important intellectual content; approved the version to be published; and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that there is no conflict of interest regarding the current manuscript.
Ethical approval
Institutional ethical review board approval is obtained (ID: 2020/712).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 148982 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yağız, B., Karalı, D.T., Nalçacıoğlu, H. et al. Laparoscopic peritoneal dialysis catheter insertion with omentopexy—sparing the omentum in children. Pediatr Surg Int 40, 128 (2024). https://doi.org/10.1007/s00383-024-05702-3
Accepted:
Published:
DOI: https://doi.org/10.1007/s00383-024-05702-3