Abstract
Aim
Hesitations concerning the long-term results of transanal endorectal pull-through (TEPT) due to prolonged anal stretching and resultant stricture and continence problems has been started to be questioned. This meta-analysis intended to compare long-term results between TEPT and transabdominal (TAB) pull-through techniques in the surgical management of Hirschsprung’s disease.
Methods
All publications between the years 1998–2021 in the PubMed, Medline, Google Scholar, Cochrane databases were reviewed. Retrospective and prospective comparative studies for TEPT, TAB as well as Laparoscopic-assisted TEPT (LTEPT) were included. Data included age at operation, postoperative constipation, enterocolitis, incontinence, stricture, and soiling rates.
Results
Eighteen publications met the inclusion criteria for TAB and TEPT, and six for TEPT and LTEPT. Patients who underwent TEPT had significantly younger operation age than patients with TAB (SMD − 1.02, 95%Cl − 1.85 to − 0.18, p: 0.0168). Postoperative constipation (OR 0.39, 95% Cl 0.25–0.61 p < 0.0001) and enterocolitis (OR 0.65, 95% Cl 0.46–0.90, p: 0.0108) rates were significantly lower in TEPT groups. Postoperative incontinence (OR 1.06, 95% Cl 0.56–2.01, p: 0.8468), stricture (OR 1.97, 95% Cl 0.81–4.80, p: 0.1352) and soiling rates were similar between the two groups. Furthermore, when TEPT and LTEPT results were compared, incidence of incontinence (OR 7.01, 95% Cl 0.75–65.33, p: 0.0871), constipation (OR 1.95, 95% Cl 0.70–5.37, p: 0.199), enterocolitis (OR 3.16, 95% Cl 0.34–29.55 p: 0.3137), stricture (OR 1.33, 95% Cl 0.29–6.15, p: 0.7188) and soiling (OR 1.57, 95% Cl 0.57–4.31, p: 0.3778) were similar for both techniques.
Discussion
TEPT is superior to TAB in terms of constipation and enterocolitis. Contrary to concerns, postoperative incontinence rates are not statistically different. However, further publications about long-term LTEPT results are necessary for more reliable conclusions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Surgical management of Hirschsprung’s disease (HD) is based on removing the aganglionic intestinal segment of variable length and pull-through of the remaining ganglionic functional bowel. Several surgical approaches have been described over the years in an attempt to improve and attain the best possible functional outcome; remaining length of the healthy intestinal segment also being a determining factor in choosing the preferred surgical approach as well as the experience of the surgeon.
Following the historical attempts of previous unsuccessful surgical procedures and the understanding of the actual pathophysiology of the disease, Swenson et al. in 1948 described their own technique utilizing complete dissection and removal of the aganglionic segment through an abdominal approach and end-to-end anastomosis of the ganglionic segment immediately above the anal canal and successfully treated a child with HD [1]. In 1957, Duhammel described an alternative abdominal pull-through technique where the rectum was left to avoid extensive pelvic dissection and a retro-rectal pull through was established [2]. In 1963, to avoid the risks to damage the pelvic structures during dissection, Soave popularized transabdominal endorectal pull-through which consisted of removing the mucosa and submucosa of the rectum and pull-through of the bowel within an aganglionic muscular cuff [3, 4].
Complete transanal endorectal pull-trough (TEPT), a modified version of Soave–Boley procedure, was described by De La Torre et al. in 1998 [5]. TEPT has become the favored technique due to its several advantages including no necessity for laparotomy, better cosmetic result, etc. [6]. However, the procedure had limitations such as its applicability to aganglionosis confined to the rectosigmoid colon, and also, some authors had some hesitations about the procedure such as possible uncontrolled intraabdominal bleeding from the mesentery or damages to the sphincter complex due to prolonged anal stretching. Some authors reported that anal sphincter damage was more frequent after the TEPT procedure [7, 8]. In addition, transanal operations technically were more difficult in older children [9]. To avoid these drawbacks, laparoscopic-assisted TEPT (LTEPT) has gained wide interest [10].
English literature delivers lots of discussion about the long-term outcomes of surgical techniques for HD; however, there seems to be no consensus concerning which technique is more beneficial for achieving the best outcome especially in terms of incontinence, constipation, enterocolitis, stricture and soiling. TEPT, being performed solely from the anal route, requires anal stretching for adequate exposure for a considerable time, essentially during the whole surgical procedure. The prolonged anal stretching is held responsible for the long-term unfavorable outcome including complications such as stenosis, constipation, soiling and incontinence. We, therefore, aimed to perform a systematic review and meta-analysis of the literature to compare the efficiency of techniques on these outcomes based on long-term results, especially in the frame of transabdominal versus transanal procedures.
Methods
Search strategy
This study was structured in accordance with Prisma guidelines. A systematic search in the English language published between the years 1998 and 2021 was conducted in PubMed, Medline, Google Scholar and Cochrane databases. Search terms included ‘Hirschsprung’s disease’, ‘fecal incontinence’, ‘postoperative complications’, ‘treatment of Hirschsprung’s disease’, ‘enterocolitis’ and ‘pull through’ and their combinations, and all titles and abstracts were evaluated, relevant titles/abstracts were identified for further consideration.
Types of operations
Articles that presented long-term results for transanal and transabdominal pull-through procedures were reviewed. Swenson, Duhammel and Soave were assigned as the transabdominal pull through (TAB) group; Transanal endorectal pull through (TEPT) and laparoscopic-assisted transanal endorectal pull-through techniques (LTEPT) were detailed and two different comparative groups were constituted.
Selection criteria and data extraction
Inclusion and exclusion criteria were set in consensus, and literature review was conducted independently by two of the authors (OE, UC). Inclusion criteria were: (1) Randomized control trials and observational clinical studies in the English language, (2) Comparative studies reporting long-term outcomes of 1 year and longer for TAB, TEPT and LTEPT procedures, (3) Studies comprising outcome measures including constipation, enterocolitis, incontinence, stricture and soiling. Exclusion criteria were: (1) Data collected from only abstracts and personal communications, (2) Non-comparative studies, publications consisting of adult patients, (3) Follow-up period of less than one year, (4) Non- English articles, (5) Abstracts in English having non-English manuscripts, (5) Case reports, (6) Editorial letters and reviews. Disagreements were resolved by discussion and consensus was attained.
Data extracted from included studies were the name of the first author, year and journal of publication, number of patients, median age at operation, operative time and long-term results (constipation, soiling, incontinence, stricture, enterocolitis). Identified parameters were recorded both for TEPT-TAB and TEPT-LTEPT groups.
Statistical analysis
For continuous variables, the means along with the standard deviations or the medians along with the minimum and maximum values were extracted from eligible studies. For these variables, standardized mean differences were combined using a random effect meta-analysis for the studies that reported the means. The odds ratios were calculated for constipation, enterocolitis, incontinence, stricture and soiling and combined using a random effects meta-analysis model.
The combined effect sizes along with their precision (95% confidence intervals) and the data from individual studies are presented in forest plots. Cochran’s Q statistic and the related significance test and \({I}^{2}\) are used for assessing heterogeneity. Publication bias checks are conducted via funnel plots, Egger’s linear regression test and fail-safe n calculations. All comparisons are carried out between TAB-TEPT and LTEPT-TEPT separately. The analysis is performed in R statistical programming language.
Results
Literature search results
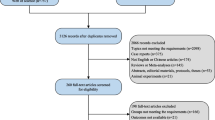
A total of 130 articles were identified to review after titles and abstracts were screened; 117 of those articles did not fulfill the criteria, and thus they were excluded. Exclusion criteria are detailed in Fig. 1. Remaining 23 articles were included for analysis. 18 articles compared the results between TAB and TEPT patients, 6 articles compared TEPT and LTEPT. One of them contained results for both groups. Included articles are listed in Table 1 and Table 2. As mentioned in Tables, all outcome parameters were not available in all articles.
Study characteristics
There were 1340 patients for TAB (n = 745) and TEPT (n = 596) groups. Fifteen articles were retrospective and 3 were prospective. Postoperative enterocolitis was evaluated by 14, constipation by 12, incontinence by 9, soiling by 8 and stricture by 7 studies (Table 1). On the other hand, there were 333 patients in TEPT (n = 180) and LTEPT (n = 153) groups. All of them were retrospective studies. Postoperative enterocolitis was evaluated in 4 and, incontinence, constipation, soiling and stricture in 3 articles (Table 2).
Age at operation
Age at operation for TAB-TEPT
Articles not mentioning the median age at operation were not included in the analysis. Thirteen studies quoted mean age at operation; however, one of them did not present the standard deviation, therefore it was excluded as well (Table1). Ultimately, twelve studies were evaluated for mean age at operation. Overall analysis has shown that patients who had undergone the TEPT procedure had a significantly lower age at operation than the TAB group (SMD − 1.02, 95% Cl − 1.85 to − 0.18, p: 0.0168) (Fig. 2). Random-effects model was constituted, and it has shown a significant heterogeneity (I2: 95.8%) (Fig. 2).
Age at operation for TEPT-LTEPT
There were a limited number of studies to compare TEPT and LTEPT, and not all of the studies mentioned the mean age at operation or standard deviation. Therefore, analysis for comparison for age at operation could not constitute for TEPT and LTEPT groups. Ages at operation were listed for each in Table 2.
Duration of operation
Duration of operation for TAB-TEPT
Seven studies compared operation time for TAB and TEPT groups. Although TEPT group seemed to have a shorter operation time, there was no statistical difference between the two groups (SMD − 0.64, 95% Cl − 1.45 to 0.17, p: 0.121) (Fig. 3). Random-effects model was constituted, and there was significant heterogeneity in the favor of TEPT (I2:91.9%) (Fig. 3).
Duration of operation for TEPT and LTEPT
Comparation of operation time for TEPT and LTEPT could not evaluate due to a lack of available data. Operation times for each article were listed in Table 2.
Postoperative incontinence
Incontinence rates for TAB and TEPT groups
Postoperative incontinence rate was reported in 9 articles with 692 patients (307 patients in TAB and 385 in TEPT groups, respectively); Seven of them were retrospective and 2 were prospective studies. Incontinence rates were similar for both groups (OR 1.06, 95% Cl 0.56–2.01, p: 0.8468) (Fig. 4). A random-effects model was used for heterogeneity and it showed a moderate heterogeneity (I2: 38.0%). Asymmetry was not observed in the funnel plot (Fig. 4).
Incontinence rates for TEPT-LTEPT groups
Three studies including 127 patients (TEPT: 43 and TAB: 84 patients, respectively) quoted postoperative incontinence rates for TEPT and LTEPT; Although there was no statistically significant difference, LTEPT procedure seemed to have more favorable results (OR 7.01, 95% Cl 0.75–65.33, p: 0.0871) (Fig. 5). No heterogeneity was observed as a result of the random-effects model (I2:0%). There was no obvious asymmetry in the funnel plot (Fig. 5).
Postoperative constipation
Constipation rate for TAB-TEPT groups
Twelve articles, two of which were prospective, reported postoperative constipation rates. A total of 902 patients were included; 509 in TAB and 393 in TEPT Groups. Constipation rate was significantly lower in patients who had undergone the TEPT procedure (OR 0.39, 95% Cl 0.25–0.61 p < 0.0001) (Fig. 6). There was a quite low heterogeneity (I2:4.5%) with a random-effects model. There was no obvious asymmetry in the funnel plot (Fig. 6).
Constipation rate for TEPT and LTEPT groups
Three studies with 222 patients reported postoperative constipation rates for TEPT vs. LTEPT (129 vs. 93 patients, respectively). When constipation rates were compared between TEPT vs. LTEPT, no significant difference was found (OR 1.95, 95% Cl 0.70–5.37, p: 0.1990) (Fig. 7). No heterogeneity was observed as a result of the random-effects model (I2:0%). There was no obvious asymmetry in the funnel plot (Fig. 7).
Postoperative enterocolitis
Enterocolitis rate for TAB and TEPT groups
Postoperative enterocolitis rate was reported in 14 articles for TAB vs TEPT; Three studies were prospective and 11 were retrospective. There were 1004 patients; 526 patients in TEPT and 478 in TAB groups, respectively. Analysis revealed that patients who have undergone TEPT had significantly lower enterocolitis rate (OR 0.65, 95% Cl 0.46–0.90, p: 0.0108) (Fig. 8). Random effects model was established, and no heterogeneity was seen in the data (I2:0%). There was no obvious asymmetry in the funnel plot (Fig. 8).
Enterocolitis rate for TEPT and LTEPT groups
Four articles with 106 patients (TEPT, n = 64 and LTEPT, n = 106) reported postoperative enterocolitis rates after surgery. It was seen that postoperative enterocolitis was reported to be lower after LTEPT; However, there was no statistically significant difference between the two groups (OR 3.16, 95% Cl 0.34–29.55 p: 0.3137) (Fig. 9). A significant heterogeneity was seen with random effects model (I2: 81.4%) (Fig. 9).
Postoperative stricture
Stricture rate for TAB and TEPT groups
Seven studies with 599 patients to compare TAB (n = 344) and TEPT (n = 255) reported postoperative stricture. Overall analysis showed that there was no statistically significant difference between the two groups according to postoperative stricture rate (OR 1.97, 95% Cl 0.81–4.80, p: 0.1352) (Fig. 10). The heterogeneity was low (I2: 16.0%) in random effects model. No obvious asymmetry was observed in the funnel plot (Fig. 10).
Stricture rate for TEPT and LTEPT groups
There were three studies that reported comparative stricture rates for TEPT vs. LTEPT. Totally 111 patients were included in the metanalysis (TEPT/LTEPT: 51/60 patients). Random effects model was constituted, and it displayed a moderate heterogeneity (I2: 31.5%) (Fig. 11); However, there was no difference between the two groups (OR 1.33, 95% Cl 0.29–6.15, p: 0.7188), (Fig. 11).
Postoperative soiling
Soiling rate for TAB and TEPT groups
Eight articles with 511 patients (TAB/TEPT: 356/155 patients) reported postoperative soiling rates for TAB vs. TEPT. Overall analysis has shown that there was no heterogeneity (I2: 0%). Postoperative soiling rates were statistically similar between the two groups (OR 1.13, 95 Cl% 0.68–1.90, p: 0.6324) (Fig. 12). There was no obvious asymmetry in the funnel plot (Fig. 12).
Soiling rate for TEPT and LTEPT groups
Three studies were detected to compare postoperative soiling rates for TEPT vs. LTEPT. There were 127 patients in TEPT group and 87 in LTEPT (Total: 214). Random effects model revealed that there was no heterogeneity (I2: 0.0%). Two groups had similar soiling rates (OR 1.57, 95% Cl 0.57–4.31, p 0.3778) (Fig. 13).
Discussion
Following the introduction of TEPT by De La Torre and Saldago in 1998 where mucosectomy, colectomy and pull-through are performed exclusively transanally, the operative technique has become readily and widely adopted by many pediatric surgeons throughout the world [5]. The technique had the unique advantage of avoiding laparotomy and performing a literally scarless surgery in the most common rectosigmoid form of HD. However, the technique also had some drawbacks such as being limited to rectosigmoid resection where longer segments still required abdominal access and prolonged stretching of sphincters with unpredictable long-term results, the possibility of bleeding from the mesentery during retraction to be able to maintain visibility, etc.
Despite the multitude of single and multicenter studies addressing the long-term complications and functional results of the most widely performed operations throughout the world, a lack of consensus still exists regarding the best operative procedure to achieve the best functional results with minimum complications and morbidity.
Age at operation and duration of operation
The results of this meta-analysis have shown that age at operation was significantly lower in the TEPT group than in TAB pull-through procedures for HD. Many authors have acknowledged that submucosal dissection is easier in younger children [11, 12]. Vu et al. presenting their experience in TEPT with 51 newborns have reported that they had no significant problems during or after the operation even though they did not use any facilitator technique for submucosal dissection [13]. Zakaria et al. suggested that patients who were operated on at a younger age had significantly better outcomes because the technique was more easily applicable at a younger age [14]. On the other hand, Lu et al. stated that short-term complications such as perianal excoriation, anastomotic leakage and stricture as well as the incidence of incomplete continence as a long-term problem were significantly higher in neonates [15]. However, dilated ganglionic colon could be a more common and serious problem in older ages; thus, laparoscopic-assisted TEPT should be considered in those cases. Contrary to TAB procedures, TEPT and LTEPT groups had a similar age at operation [16, 17].
Although in our meta-analysis no significant difference was found in the operative times for TAB and TEPT, another meta-analysis by Chen et al. has found that the TEPT group had shorter operative time [18]. It is generally agreed in the literature that the operative time for TEPT is shorter especially in younger patients [13, 16, 18]. Guerra et al. reported that laparoscopic-assisted LTEPT had significantly longer operative time than the TEPT group in their own series. They also performed a meta-analysis, and similar to their own series, LTEPT had significantly longer operative time [19].
Incontinence
This meta-analysis revealed that postoperative incontinence rates were similar in TAB and TEPT as well as in LTEPT groups.
Most common argument for TEPT is potentially increased incontinence rates [8, 20, 21]. Overstretching of anal sphincters to attain optimal visual exposure during the transanal approach has the potential to damage the sphincter mechanism further resulting in a decrease in anal canal resting pressures as evidenced by the adult series by van Tests et al. [22]. Similarly, Speakmen et al. advocated that even anal dilatation may cause structural damage to the anal sphincter mechanism [23]. Stensrud et al. have performed anal endosonography in 52 patients after transanal and transabdominal pull-through procedures and observed that internal anal sphincter (IAS) defects were more common after TEPT procedures. In addition, they reported that daily incontinence was more frequent in patients with IAS defects [8]. El-Sawaf et al. reported that TAB patients had two-fold better continence scores than TEPT patients [21]. On the other side, there are also studies that were unable to show any statistically significant differences between TEPT and TAB groups in terms of incontinence rates [24,25,26]. Van Leeuwen et al. in their series of 12 patients, have evaluated the anorectal manometric parameters to determine the effect of the transanal approach, and have shown no significant differences between the transanal and transabdominal pull-through procedures [27].
Zakaria et al. have emphasized that patients with younger age at operation had significantly better results for continence scores after the TEPT procedure; Moreover, they pointed out that TEPT is more reliable and feasible at a younger age [14].
In 1999, Georgeson et al. introduced laparoscopically assisted endorectal pull-through (LTEPT) [10] bringing numerous advantages including reduced risk of intraoperative bleeding during mobilization of the bowel and twisting that may occur during pull-through [28]. The LTEPT procedure also had the advantage of shortening the transanal, and thus, the anal stretching period which in return would reduce the risk and incidence of anal incontinence. However, as in the study by Guerra et al. major complications such as an anastomotic leak, stricture and fecal incontinence were similar between patients with TEPT and LTEPT [19], and laparoscopic mobilization and shortening the transanal period did not seem to add much to continence outcomes [6, 24, 25].
One other alleged reason for anal incontinence may be possible damage to sensory nerve endings in the anal canal during dissection and/or very low coloanal anastomosis at the level of the dentate line [20]. The fact that there is a certain rate of anal continence problems following pull-through procedures varying from one series to another, raises the question whether functional results improve over time. Bjornland et al. have reported that soiling or fecal accidents are less common in older children quoting that ‘fecal control seems to improve with increasing age’ [29]. On the contrary, however, Fosby et al. were not able demonstrate any improvement in anal function over the years in patients who have undergone pull-through operations [30].
Constipation and soiling
The results derived from this meta-analysis have shown that the constipation rate was significantly lower in TEPT than in the TAB groups. Likewise, the LTEPT group also had a lower constipation rate statistically similar to the TEPT groups.
Postoperative constipation is classified as ‘partially preventable complications’ by some authors [31]. Possible causes of constipation include mechanical obstruction, residual aganglionosis, motility disorders involving the dilated ganglionic colon and functional megacolon [31]. A meta-analysis by Yan et al. has shown that postoperative constipation was significantly lower in the TEPT group when compared to the TAB group [32]. In the same study, however, constipation rates following Soave and TEPT groups were found to be similar [32]. Duhammel operation is considered to be more problematic in terms of constipation because of the retained aganglionic rectal pouch [33]. However, in Yan et al. meta-analysis, there was no conclusive information about the assessment of Duhammel and TEPT. In another meta-analysis by Mao et al. outcomes of Duhammel and TEPT patients were compared, however, constipation rates were not evaluated [34].
Some patients complain about fecal accidents even when they have intact anal canals and normal sphincter activity [31]. Soiling rates are reported to be relatively higher than other complications for all types of operations [26, 35, 36], presumably a condition related to constipation in the majority of patients. Resolution of fecal accidents is usually possible through bowel management programs with laxatives and/or enemas. Comparative studies have shown that postoperative soiling rates were similar after transanal or transabdominal surgeries concluding that TEPT is not a reason for soiling [7, 26]. In our analysis, soiling was statistically similar for TEPT vs. TAB and also TEPT vs. LTEPT.
Enterocolitis
Postoperative enterocolitis rate was significantly lower in the TEPT group than TAB in this meta-analysis, and there was no significant difference between TEPT and LTEPT groups.
Enterocolitis is the most serious complication of HD which may also occur postoperatively. Postoperative stricture, mechanical obstruction, patient’s preoperative status or surgical techniques may be related to postoperative enterocolitis [37,38,39]. Ruttenstock et al. reviewed 27 articles including 899 patients and reported a postoperative enterocolitis rate of 10.2% (92/899) after TEPT concluding that TEPT had a beneficial effect to reduce postoperative enterocolitis [39]. Another meta-analysis by Zimmer et al. stated that 28.9% of the patients had postoperative enterocolitis after TEPT [40]. There are also some comparative meta-analyses in the literature [18, 32]. In these analyses, it was mentioned that although TEPT tended to have lower enterocolitis rates when compared to TAB, there was no statistical difference [18, 32].
Stricture
In our analysis, postoperative stricture rates were similar between TEPT and TAB also LTEPT and TEPT groups.
Pratap et al. reported that 2 of 19 patients who had undergone TEPT had anastomotic stricture [41]. They recommended routine anal dilatation for every patient in the early postoperative period [41]. On the other hand, Obermayr et al. recommended that digital examination under general anesthesia should be performed in postoperative six week, and if there is an anastomotic stricture, a dilatation program should be started. Anastomotic stricture was reported in 40% of patients in their series [42]. Also, there was no recurrent stricture after the dilatation program [42]. Ruttenstock et al. detected an anastomotic stricture rate of 8% after TEPT in their meta-analysis [39]. One quite interesting result in their review was that nearly half of the patients who had enterocolitis after the TEPT procedure had anastomotic stricture [39]. Therefore, it is considered that anastomotic stricture may be a contributor to postoperative enterocolitis.
Limitations
There are several limitations of the current meta-analysis. The study included only those that were in the English language, and thus, possible valuable articles in various other languages were omitted. Studies comparing the transabdominal and endorectal pull-through techniques with long-term outcome results are limited in the literature. Therefore, we needed to include different types of open techniques in the “transabdominal pull-through” procedures. Moreover, the outcome parameters were not standardized in the manuscript included in this meta-analysis. The definition and classification of parameters such as enterocolitis, incontinence or constipation varied among publications. Therefore, the definitions of outcomes were not submitted as inclusion criteria. Another limitation is that although both retrospective and prospective studies were included in the meta-analysis, most of the articles were actually retrospective and only a few articles were prospective. To include as many studies in the meta-analysis, we chose to include both prospective and prospective studies. Groups were not similar demographically, TEPT patients had younger operation age than the TAB group, most possibly because TEPT is a more preferred technique in younger patients. Lastly, the definitions of enterocolitis, constipation, soiling and incontinence were not standardized in the included articles.
Conclusion
In conclusion, contrary to popular conviction, transanal endorectal pull-through is not related to incontinence when compared with transabdominal techniques. Moreover, postoperative constipation and enterocolitis are reported to be significantly lower after transanal surgeries. In our opinion, transanal endorectal pull-through is a feasible technique and has favorable long-term outcomes especially in younger patients. Laparoscopic-assisted transanal pull-through may be a useful option for older children who have over-dilated ganglionic segment.
Further prospective and standardized multicentric studies are required to determine the downsides or benefits of techniques.
References
Swenson O (2002) Hirschsprung’s disease: a review. Pediatrics 109:914–918. https://doi.org/10.1542/peds.109.5.914
Duhamel B (1960) A new operation for the treatment of hirschsprung’s disease. Arch Dis Child 35:38–39. https://doi.org/10.1136/adc.35.179.38
Soave F (1985) Endorectal pull-through: 20 years experience. Address of the guest speaker, APSA, 1984. J Pediatr Surg 20:568–579. https://doi.org/10.1016/S0022-3468(85)80003-8
Boley SJ, Lafer DJ, Kleinhaus S, Cohn BD, Mestel ALKP (1968) Endorectal pull-through procedure for Hirschsprung’s disease with and without primary anastomosis. J Pediatr Surg 3:258–262
De La Torre-Mondragón L, Ortega-Salgado JA (1998) Transanal endorectal pull-through for Hirschsprung’s disease. J Pediatr Surg 33:1283–1286. https://doi.org/10.1016/S0022-3468(98)90169-5
De la Torre L, Ortega A (2000) Transanal versus open endorectal pull-through for Hirschsprung’s disease. J Pediatr Surg 35:1630–1632. https://doi.org/10.1053/jpsu.2000.18338
Stensrud KJ, Emblem R, Bjørnland K (2010) Functional outcome after operation for Hirschsprung disease-transanal vs transabdominal approach. J Pediatr Surg 45:1640–1644. https://doi.org/10.1016/j.jpedsurg.2010.02.065
Stensrud KJ, Emblem R, Bjørnland K (2015) Anal endosonography and bowel function in patients undergoing different types of endorectal pull-through procedures for Hirschsprung disease. J Pediatr Surg 50:1341–1346. https://doi.org/10.1016/j.jpedsurg.2014.12.024
Zakaria OM, El Labban GM, Shams ME (2012) Fecal incontinence after single-stage Soave’s pull-through: abdominal versus transanal endorectal pull-through. Ann Pediatr Surg 8:5–8. https://doi.org/10.1097/01.XPS.0000407759.30719.57
Georgeson KE, Cohen RD, Hebra A et al (1999) Primary laparoscopic-assisted endorectal colon pull-throughfor Hirschsprung's disease: a new gold standard. Ann Surg 229(5):678–82. https://doi.org/10.1097/00000658-199905000-00010
Höllwarth ME, Rivosecchi M, Schleef J et al (2002) The role of transanal endorectal pull-through in the treatment of Hirschsprung’s disease—a multicenter experience. Pediatr Surg Int 18:344–348. https://doi.org/10.1007/s00383-002-0747-x
Aslan MK, Karaman I, Karaman A et al (2007) Our experience with transanal endorectal pull-through in Hirschsprung’s disease. Eur J Pediatr Surg 17:335–339. https://doi.org/10.1055/s-2007-965447
Vũ PA, Thiên HH, Hiêp PN (2010) Transanal one-stage endorectal pull-through for Hirschsprung disease: experiences with 51 newborn patients. Pediatr Surg Int 26:589–592. https://doi.org/10.1007/s00383-010-2599-0
Zakaria OM (2012) Bowel function and fecal continence after Soave’s trans-anal endorectal pull-through for Hirschsprung’s disease: a local experience. Update Surg 64:113–118. https://doi.org/10.1007/s13304-012-0140-9
Lu C, Hou G, Liu C et al (2017) Single-stage transanal endorectal pull-through procedure for correction of Hirschsprung disease in neonates and nonneonates: a multicenter study. J Pediatr Surg 52:1102–1107. https://doi.org/10.1016/j.jpedsurg.2017.01.061
Van De Ven TJ, Sloots CEJ, Wijnen MHWA et al (2013) Transanal endorectal pull-through for classic segment Hirschsprung’s disease: with or without laparoscopic mobilization of the rectosigmoid? J Pediatr Surg 48:1914–1918. https://doi.org/10.1016/j.jpedsurg.2013.04.025
Bawazir OA (2020) Laparoscopic-assisted transanal pull-through in hirschsprung disease: does laparoscopic dissection minimize anal overstretching? J Laparoendosc Adv Surg Tech 30:338–343. https://doi.org/10.1089/lap.2019.0524
Chen Y, Nah SA, Laksmi NK et al (2013) Transanal endorectal pull-through versus transabdominal approach for Hirschsprung’s disease: a systematic review and meta-analysis. J Pediatr Surg 48:642–651. https://doi.org/10.1016/j.jpedsurg.2012.12.036
Guerra J, Wayne C, Musambe T, Nasr A (2016) Laparoscopic-assisted transanal pull-through (LATP) versus complete transanal pull-through (CTP) in the surgical management of Hirschsprung’s disease. J Pediatr Surg 51(5):770–774. https://doi.org/10.1016/j.jpedsurg.2016.02.020
Miyano G, Koga H, Okawada M et al (2015) Rectal mucosal dissection commencing directly on the anorectal line versus commencing above the dentate line in laparoscopy-assisted transanal pull-through for Hirschsprung’s disease: prospective medium-term follow-up. J Pediatr Surg 50:2041–2043. https://doi.org/10.1016/j.jpedsurg.2015.08.022
El-Sawaf MI, Drongowski RA, Chamberlain JN et al (2007) Are the long-term results of the transanal pull-through equal to those of the transabdominal pull-through? A comparison of the 2 approaches for Hirschsprung disease. J Pediatr Surg 42:41–47. https://doi.org/10.1016/j.jpedsurg.2006.09.007
Van Tets WF, Kuijpers JHC, Tran K et al (1997) Influence of Parks’ anal retractor on anal sphincter pressures. Dis Colon Rectum 40:1042–1045. https://doi.org/10.1007/BF02050926
Speakman CTM, Burnett SJD, Kamm MA, Bartram CI (1991) Sphincter injury after anal dilatation demonstrated by anal endosonography. Br J Surg 78:1429–1430. https://doi.org/10.1002/bjs.1800781206
Aworanti OM, Mcdowell DT, Martin IM et al (2012) Comparative review of functional outcomes post surgery for Hirschsprung’s disease utilizing the paediatric incontinence and constipation scoring system. Pediatr Surg Int 28:1071–1078
Kim AC, Langer JC, Pastor AC et al (2010) Endorectal pull-through for Hirschsprung’s disease-a multicenter, long-term comparison of results: transanal vs transabdominal approach. J Pediatr Surg 45:1213–1220. https://doi.org/10.1016/j.jpedsurg.2010.02.087
Romero P, Kroiss M, Chmelnik M et al (2011) Outcome of transanal endorectal vs. transabdominal pull-through in patients with Hirschsprung’s disease. Langenbeck’s Arch Surg 396:1027–1033. https://doi.org/10.1007/s00423-011-0804-9
Van Leeuwen K, Geiger JD, Barnett JL et al (2002) Stooling and manometric findings after primary pull-throughs in Hirschsprung’s disease: Perineal versus abdominal approaches. J Pediatr Surg 37:1321–1325. https://doi.org/10.1053/jpsu.2002.34999
Georgeson KE (2002) Laparoscopic-assisted pull-through for Hirschsprung’s disease. Semin Pediatr Surg 11:205–210. https://doi.org/10.1053/spsu.2002.35350
Bjørnland K, Pakarinen MP, Stenstrøm P et al (2017) A Nordic multicenter survey of long-term bowel function after transanal endorectal pull-through in 200 patients with rectosigmoid Hirschsprung disease. J Pediatr Surg 52:1458–1464. https://doi.org/10.1016/j.jpedsurg.2017.01.001
Fosby MV, Stensrud KJ, Bjørnland K (2020) Bowel function after transanal endorectal pull-through for Hirschsprung disease—does outcome improve over time? J Pediatr Surg 55:2375–2378. https://doi.org/10.1016/j.jpedsurg.2020.04.010
Peña A, Bischoff A (2015) Surgical treatment of colorectal problems in children. Springer International Publishing, Switzerland
Yan BL, Bi LW, Yang QY et al (2019) Transanal endorectal pull-through procedure versus transabdominal surgery for Hirschsprung disease: a systematic review and meta-analysis. Medicine (United States). https://doi.org/10.1097/MD.0000000000016777
Chatoorgoon K, Pena A, Lawal TA, Levitt M (2011) The problematic duhamel pouch in hirschsprungs disease: manifestations and treatment. Eur J Pediatr Surg 21:366–369. https://doi.org/10.1055/s-0031-1285875
Zhong MY, Tao TS, Li S (2018) Duhamel operation vs. transanal endorectal pull-through procedure for Hirschsprung disease: a systematic review and meta-analysis. J Pediatr Surg 53:1710–1715. https://doi.org/10.1016/j.jpedsurg.2017.10.047
Meinds RJ (2019) Hirschsprung's disease: early diagnosis and long-term outcomes. [Thesis fully internal (DIV), University of Groningen]. Rijksuniversiteit Groningen
Catto-Smith AG, Trajanovska M, Taylor RG (2007) Long-term continence after surgery for Hirschsprung’s disease. J Gastroenterol Hepatol (Australia) 22:2273–2282. https://doi.org/10.1111/j.1440-1746.2006.04750.x
Teitelbaum DH, Cilley RE, Sherman NJ et al (2000) A decade of experience with the primary pull-through for Hirschsprung disease in the newborn period: a multicenter analysis of outcomes. Ann Surg 232:372–380. https://doi.org/10.1097/00000658-200009000-00009
Prato AP, Gentilino V, Giunta C et al (2008) Hirschsprung disease: do risk factors of poor surgical outcome exist? J Pediatr Surg 43:612–619. https://doi.org/10.1016/j.jpedsurg.2007.10.007
Ruttenstock E, Puri P (2010) Systematic review and meta-analysis of enterocolitis after one-stage transanal pull-through procedure for Hirschsprung’s disease. Pediatr Surg Int 26:1101–1105. https://doi.org/10.1007/s00383-010-2695-1
Zimmer J, Tomuschat C, Puri P (2016) Long-term results of transanal pull-through for Hirschsprung’s disease: a meta-analysis. Pediatr Surg Int 32:743–749. https://doi.org/10.1007/s00383-016-3908-z
Pratap A, Chandra Shakya V, Kumar Biswas B et al (2007) Single-stage transanal endorectal pull-through for Hirschsprung’s disease: perspective from a developing country. J Pediatr Surg 42:532–535. https://doi.org/10.1016/j.jpedsurg.2006.10.049
Obermayr F, Szavay P, Beschorner R, Fuchs J (2009) Outcome of transanal endorectal pull-through in patients with Hirschsprung’s disease. Eur J Pediatr Surg 19:220–223. https://doi.org/10.1055/s-0029-1220682
Hadidi A (2003) Transanal endorectal pull-through for Hirschsprung’s disease: a comparison with the open technique. Eur J Pediatr Surg 13:176–180
Menezes M, Corbally M, Puri P (2006) Long-term results of bowel function after treatment for Hirschsprung’s disease: a 29-year review. Pediatr Surg Int 22:987–990. https://doi.org/10.1007/s00383-006-1783-8
Aslanabadi S, Ghalehgolab-Behbahan A, Zarrintan S et al (2008) Transanal one-stage endorectal pull-through for Hirschsprung’s disease: a comparison with the staged procedures. Pediatr Surg Int 24:925–929. https://doi.org/10.1007/s00383-008-2186-9
Gunnarsdóttir A, Larsson LT, Arnbjörnsson E (2010) Transanal endorectal vs. duhamel pull-through for Hirschsprung’s disease. Eur J Pediatr Surg 20:242–246. https://doi.org/10.1055/s-0030-1252006
Tannuri ACA, Tannuri U, Romão RLP (2009) Transanal endorectal pull-through in children with Hirschsprung’s disease-technical refinements and comparison of results with the Duhamel procedure. J Pediatr Surg 44:767–772. https://doi.org/10.1016/j.jpedsurg.2008.08.002
Ca S, Bj M (2011)Surgery for Hirschsprung’s disease: comparison between the Duhamel method and the transanal endorectal pull-through based on 59 patients and a review of the literature, SERVAL, https://serval.unil.ch/resource/serval:BIB_4101ACC38EB3.P001/REF
Onishi S, Nakame K, Yamada K et al (2016) Long-term outcome of bowel function for 110 consecutive cases of Hirschsprung’s disease: Comparison of the abdominal approach with transanal approach more than 30 years in a single institution—is the transanal approach truly beneficial for bowel function? J Pediatr Surg 51:2010–2014. https://doi.org/10.1016/j.jpedsurg.2016.09.029
Tannuri ACA, Ferreira MAE, Mathias AL, Tannuri U (2017) Long-term results of the Duhamel technique are superior to those of the transanal pullthrough: a study of fecal continence and quality of life. J Pediatr Surg 52:449–453. https://doi.org/10.1016/j.jpedsurg.2016.10.007
Gunadi KSM, Dwihantoro A (2018) Outcomes in patients with hirschsprung disease following definitive surgery. BMC Res Notes 11:644. https://doi.org/10.1186/s13104-018-3751-5
Fahmy M, Abd El Hamid S, Elsamahy O, Mohammed H (2019) Comparative study between transanalendorectal pull-through and modified Duhamel’s procedure in management of Hirshsprung’s disease. Egyptian J Hospital Med 74(3):679–683. https://doi.org/10.21608/ejhm.2019.23799
Dahal GR, Wang JX, Guo LH (2011) Long-term outcome of children after single-stage transanal endorectal pull-through for Hirschsprung’s disease. World J Pediatr 7:65–69. https://doi.org/10.1007/s12519-011-0247-y
Shawkat A, Elbarbary M, Saleh G et al (2020) Outcome of laparoscopic assisted endorectal pull through versus trans anal approach in management of hirshsprung disease. Indian J Public Health Res Develop 11(4):534–539
Funding
None.
Author information
Authors and Affiliations
Contributions
A-C wrote the main manuscript B prepared the statistical analysis All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Celtik, U., Yavuz, I. & Ergün, O. Transanal endorectal or transabdominal pull-through for Hirschsprung’s disease; which is better? A systematic review and meta-analysis. Pediatr Surg Int 39, 89 (2023). https://doi.org/10.1007/s00383-023-05378-1
Accepted:
Published:
DOI: https://doi.org/10.1007/s00383-023-05378-1