Abstract
Introduction
Several operative techniques have been developed for the treatment of Hirschsprung’s disease (HD) in the past decades. Since one-stage transanal pull-through (TAPT) was first performed in 1998, multiple studies have shown favourable short-and midterm results compared to other techniques with shorter operation length, shorter hospital stay and lower complication rates. The aim of this meta-analysis was to determine the longterm results following TAPT for HD.
Methods
A systematic literature search for relevant articles was performed in four databases using the following terms “Hirschsprung/Hirschsprung’s disease”, “aganglionosis”, “transanal”, “pullthrough/pull-through”, “longterm/long-term” “results”, “follow-up” and “outcome”. A meta-analysis was conducted for relevant articles for one-stage transanal pull-through for HD with a minimal follow-up of median 36 months regarding constipation, incontinence/soiling, enterocolitis and secondary operations. Odds ratio (OR) with 95 % confidence intervals (CI) were calculated.
Results
Six studies with 316 patients matched the set criteria and were included in this analysis. Overall 45 (14.2 %) patients had disturbances of bowel function (OR 0.05, 95 % CI 0.03–0.07, p < 0.00001). Of these, 24 (53.3 %) patients experienced constipation, 8 (17.8 %) incontinence/soiling and 13 (28.9 %) enterocolitis. 10 (3.2 %) patients developed complications requiring secondary surgery. Most patients had a daily defecation frequency of 1–3 bowel movements 3 years postoperatively, resembling the stooling patterns of healthy controls.
Conclusion
Nearly 15 % of all patients operated with TAPT for HD continue to experience persistent bowel symptoms with constipation as the main problem. Further studies on the long-term outcome of children operated with this technique for HD are necessary to evaluate stooling patterns, urinary and sexual function as well as general quality of life during adolescence and adulthood.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hirschsprung’s disease (HD) was first described by Harald Hirschsprung in the 1880 [1]. Since the first operation was performed by Swenson and Bill in 1948 [2] treatment for HD has evolved and various operative techniques have been developed over time. Following staged abdominal and laparoscopic surgery, one-stage transanal pull-through (TAPT) was first described in 1998 by De la Torre and Ortega [3]. Since then multiple studies have shown favourable short-and midterm results compared to other techniques with shorter operation length, shorter hospital stay and lower complication rates [4–10]. However, a lot TAPT studies fail to report clinical outcome of HD patients until the bowel training is finished, and therefore, a definite judgement about stooling patterns after TAPT cannot be made. In some HD patients, defecation may be impaired lifelong due to an inadequate bowel length, damaged anatomical structures in the operation area or a dysfunctional residual bowel [11].
The aim of this meta-analysis was to review the existing literature for reports about TAPT with a minimum average follow-up of 36 months and to determine the long-term results, such as constipation, incontinence/soiling, enterocolitis and secondary surgeries.
Methods
Information sources and literature-based search
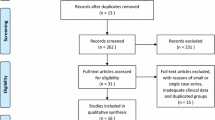
A systematic literature search was performed in PubMed, Ovid Medline, Embase and the Cochrane Library in March 2016 using different combinations of the following words: “Hirschsprung disease/Hirschsprung’s disease”, “aganglionosis”, “transanal”, “pullthrough/pull-through”, “longterm/long-term” “results”, “follow-up” and “outcome”. Additionally, reference lists were screened manually for other potentially relevant studies. Duplicates were deleted (Fig. 1).
Selection criteria and data extraction
Relevant articles were reviewed by title, abstract and keywords and full-text of selected articles were assessed by one of the authors (JZ). Only articles in English language were considered. Included were studies with first time operations only (no re-dos) and entirely transanal pull-through operations (no staged procedures, no open or laparoscopic assistance, no mini-laparotomies, no comparative studies between different operative techniques, no stoma closure in the same session). The follow-up period of the included studies was at least of 36 months average to assure a proper evaluation of the bowel function.
The data were standardized extracted into an electronic database, containing the characteristics of the study (authors, publication year, time-frame of the study, sample size, average follow-up time, number of patients with constipation, incontinence/soiling or enterocolitis as well as secondary operations and daily defecation frequency).
Statistical analysis
For the comparative meta-analysis, we used the Review manager (RevMan, version 5.3, The Nordic Cochrane Centre, The Cochrane Collaboration, Copenhagen). Studies for comparative analysis contained data about the number of patients with constipation, incontinence/soiling, enterocolitis and secondary operations. Pooled odds ratio (ORs) were calculated and the difference was considered as statistical significant if p < 0.05 (two-tailed).
Results
During literature search we found that several studies labelled to analyse long-term outcome published data before the children were even bowel trained. Furthermore, a large number of reports categorised their procedure as a TAPT approach, but when looking into the manuscript details, the authors included multi-staged approaches, open techniques, mini-laparotomies, laparoscopic assistances or conversion in their data as well. The studies were strictly excluded to rule out potential damage of any kind of abdominal approach.
Six studies with 316 patients matched the set criteria and were included in this analysis [12–17] (Table 1). The average follow-up time of all included studies was 4.3 years. Of 316 patients, 45 (14.2 %) had disturbances of bowel function (OR 0.05, 95 % CI 0.03–0.07, p < 0.00001, Fig. 2). Of these, 24 (53.3 %) patients experienced constipation, 8 (17.8 %) incontinence/soiling and 13 (28.9 %) enterocolitis (Fig. 3). 10 (3.2 %) patients developed complications requiring secondary surgery. Nine of them were re-do operations, only one was a mucosectomy. Three out of the six included studies reported daily defecation frequencies [14, 15, 17]. Three to four years postoperatively, patients who underwent TAPT had one to three bowel movements daily on average, resembling the stooling patterns of healthy controls.
Discussion
Long-term problems of HD patients entail persistent obstructive symptoms, incontinence/soiling and enterocolitis but frequently an individual child may exhibit a combination of these problems [1].
Many studies report good short- and middle-term outcome of TAPT [4–10] but we found only six entirely TAPT studies with an average follow-up of minimal 36 months. We chose this cut off point to reliably estimate defecation behaviour, such as incontinence or constipation as bowel training can usually be estimated at this age. Due to the limited number of suitable reports we are aware that our result of 14.2 % overall bowel function impairment may underestimate the real incidence of those disturbances, especially as one report by Yang et al. [15] reports only six events out of 137 patients. Otherwise, several reports postulated that after HD surgery defecation patterns get better during progress of childhood [1, 18], which may also have influenced the good overall bowel function of this meta-analysis. Kim and Oh concluded that after TAPT especially neonates require a postoperative stabilization period to develop normal stooling patterns [12]. Aworanti et al. found that incontinence usually improves during time course, but constipation is frequently an ongoing problem [19]. A general problem for the evaluation of outcome studies is the diversity in the definition and of constipation and incontinence and who describes them (patient, parents, medical professionals) [17].
We calculated a constipation rate of 53.3 % among the 45 patients with bowel function problems after TAPT (7.6 % of all 316 patients). The reported incidence of constipation and obstructive syndromes after pull-through procedure varies widely in the literature from 11 up to 44 % [16, 20]. Furthermore, reports about constipation after HD surgery differ from improvement [21, 22] to persistence into adulthood [23, 24].
Likewise, incontinence rates have been reported in inconsistent percentages reaching from none up to 76 % [20, 25–28]. These numbers incorporate our incontinence/soiling rate of 17.8 % in patients with bowel problems, respectively, 2.5 % off all 316 included patients. Reports on continence development over time have been contradictory, ranging from improvement [18, 21, 22] to ongoing problems years after surgery [23, 29]. Recently, Stensrud et al. observed that internal anal sphincter (IAS) defects occur frequently after transanal procedures which were associated with daily faecal incontinence [30]. The authors hypothesized that forceful anal dilatation during the endorectal pull-through procedure contributes to the IAS defects [30].
In our review, 28.9 % of the patients with bowel function disturbances (4.1 % of all 316 patients) experienced enterocolitis during their follow-up. However, a previous literature review by Ruttenstock and Puri reported only 10 % enterocolitis and 2 % recurrence rate after TAPT [31].
Of all 316 included patients, 3.2 % developed complications requiring secondary operations with the majority needing re-do operations and only one was a mucosectomy. Rall et al. reported the same incidence for re-do operations after pull-through for HD [32]. In contrast, other authors reported rates of 8–40 % for secondary procedures, but these numbers accounted mainly for open and laparoscopic approaches [33–36].
Three out of six studies provided data about the daily defecation frequency [14, 15, 17]. After initial high stool frequencies, patients had an average of one to three bowel movements daily 3 years postoperatively. These numbers resemble the stooling patterns of healthy controls as reported by Graneli et al. [17]. Matching these findings, Khono et al. found that 83 % of the patients who underwent TAPT presented high amplitude contraction during manometry which is suggestive for a normal colonic function [14].
Unfortunately, most of the included studies in this review do not provide enough data about the surgical technique of the performed TAPT procedure wherefore the divergent outcome parameters of the included studies are difficult to compare and interpret. The studies by Khalil and Graneli et al. mention their operative technique simply as TAPT approach and focus on functional outcome parameters, but do not address the cuff length or shape or the level of mucosal incision or anastomosis [13, 17]. Kohno et al. state a Soave style technique without further information [14]. The included data of Dutta refers to the “conventional” TAPT procedure [16]. Although the author describes more extensively a TAPT modification it remains elusive which steps where similar to the used conventional approach [16]. Kim and Oh [12] stated that their technique based on the descriptions of De la Torre and Ortega [3] and Langer [37]: After circumferential incision in the mucosa 0.5–1 cm proximal the dentate line, a proximally submucosal dissection was performed followed by a circumferentially incision of the muscle. The dissection was then conducted proximally along the outer wall of the rectal muscle. The authors then describe that the muscular rectal cuff was divided by V-shape on the posterior rectal wall but do not mention the cuff length itself [12]. The only study providing an extensive description of their surgical procedure with a description of a long cuff dissection of rectal mucosa, a short cuff colo-anal anastomosis and a V-shaped partial resection in the posterior wall of the muscular cuff was accomplished by Yang et al. [15]: After circumferential incision in the mucosa 0.5–1 cm proximal the dentate line, the authors developed a submucosal plane and extended for more than 5 cm until the peritoneal reflection After inversion and extra-anal pull-out the muscular cuff was shortened, leaving a muscular cuff of 2–3 cm. Subsequently, the posterior wall was divided into V-shape with the pointed end of ‘V’ reaching the level of anastomosis [15]. Due to lack of comparable cuff length data we cannot interpret the outcome on bowel function with regard to the surgical technique. However, both advantages and disadvantages of short and long cuffs have been described in the literature [15, 38–40].
In general, the overall long-term quality of life (QoL) after TAPT has been recently reported to be satisfying [13]. Overflow incontinence had a negative effect on QoL, whereas children who were operated at early age had a better QoL in this survey [13]. However, at the current time point most of the existing reports about long-term outcome after HD surgery into adolescence and advanced adulthood deal with of open techniques [18, 23, 24, 41–45] due to their longer practice. The working group of Pakarinen et al. recently published two articles about follow-up studies of HD patients who underwent pull-through operations for HD between 1986 and 2011 [42, 43]. They found that major functional sequelae following pull-through operations were recurrent enterocolitis and occasional faecal soiling which is in contrast to the finding of our meta-analysis about entirely TAPT studies. The reported impairment of faecal control often perpetuated during childhood which diminished with age to a level not different from controls beyond the age of 18 years [43]. However, 50 % of the interviewed adults reported abnormal stooling frequency compared to 10 % of controls. In the same survey, 13 % of all questioned patients stated an enterocolitis episode during the past year but this number decreased to 0 % by adulthood [43]. The authors concluded that most episodes of enterocolitis occur during infancy before the age of 4 years [43]. The overall QoL of HD patients was similar to controls but emotional and sexual problems may prevail in adulthood. These studies [42, 43], however, did not report the outcome of entirely TAPT but only combinations with open techniques, colon biopsies through the umbilicus incision or stoma closure in conjunction which makes the results difficult to interpret and compare with our review.
Our meta-analysis has several limitations, first, the selection bias of suitable manuscripts for this review. The included studies report their results sometimes in a way which makes them problematic to compare with other authors’ results, such as the uniform definition of outcome parameters or the usage of standardized scores for outcome assessment. Therefore, some patients or data were not included in this review, which may lead to a variance in inclusion criteria and outcome evaluation between the studies.
We are aware that our data on long-term outcome of constipation, incontinence/soiling and enterocolitis may underestimate their real incidence compared to other reports, but this discrepancy only demonstrates the lack of accurate long-term assessment of TAPT outcome. Further studies are urgently needed to assess stooling patterns, sexual and bladder function in these patients during childhood into adult age.
References
Dasgupta R, Langer JC (2008) Evaluation and management of persistent problems after surgery for Hirschsprung disease in a child. J Pediatr Gastroenterol Nutr 46(1):13–19. doi:10.1097/01.mpg.0000304448.69305.28
Swenson O, Bill AH Jr (1948) Resection of rectum and rectosigmoid with preservation of the sphincter for benign spastic lesions producing megacolon; an experimental study. Surgery 24(2):212–220
de La Torre-Mondragon L, Ortega-Salgado JA (1998) Transanal endorectal pull-through for Hirschsprung’s disease. J Pediatr Surg 33(8):1283–1286
Tannuri AC, Tannuri U, Romao RL (2009) Transanal endorectal pull-through in children with Hirschsprung’s disease–technical refinements and comparison of results with the Duhamel procedure. J Pediatr Surg 44(4):767–772. doi:10.1016/j.jpedsurg.2008.08.002
Kim AC, Langer JC, Pastor AC et al (2010) Endorectal pull-through for Hirschsprung’s disease-a multicenter, long-term comparison of results: transanal vs transabdominal approach. J Pediatr Surg 45(6):1213–1220. doi:10.1016/j.jpedsurg.2010.02.087
Dahal GR, Wang JX, Guo LH (2011) Long-term outcome of children after single-stage transanal endorectal pull-through for Hirschsprung’s disease. World J Pediatr 7(1):65–69. doi:10.1007/s12519-011-0247-y
Romero P, Kroiss M, Chmelnik M et al (2011) Outcome of transanal endorectal vs. transabdominal pull-through in patients with Hirschsprung’s disease. Langenbecks Arch Surg 396(7):1027–1033. doi:10.1007/s00423-011-0804-9
Chen Y, Nah SA, Laksmi NK et al (2013) Transanal endorectal pull-through versus transabdominal approach for Hirschsprung’s disease: a systematic review and meta-analysis. J Pediatr Surg 48(3):642–651. doi:10.1016/j.jpedsurg.2012.12.036
Mustafawi A, Hassan ME (2012) Quality of life and parents’ satisfaction with Duhamel’s versus transanal endorectal pull-through for the treatment of Hirschsprung’s disease in children. Ann Pediatr Surg 8(4):105–110. doi:10.1097/01.XPS.0000418468.33021.15
Gunnarsdottir A, Larsson LT, Arnbjornsson E (2010) Transanal endorectal vs. Duhamel pull-through for Hirschsprung’s disease. Eur J Pediatr Surg 20(4):242–246. doi:10.1055/s-0030-1252006
Ortiz-Rubio I, Pérez-Aguilera M, Granéli C et al (2013) literature review of the outcome after one-stage transanal endorectal pull-through procedure for Hirschsprung’s disease in children. Surg Sci 04(05):258–262. doi:10.4236/ss.2013.45050
Kim HY, Oh JT (2009) Stabilization period after 1-stage transanal endorectal pull-through operation for Hirschsprung disease. J Pediatr Surg 44(9):1799–1804. doi:10.1016/j.jpedsurg.2008.10.070
Khalil M (2015) Long-term health-related quality of life for patients with Hirschsprung’s disease at 5 years after transanal endorectal pull-through operation. Qual Life Res 24(11):2733–2738. doi:10.1007/s11136-015-1012-9
Kohno M, Ikawa H, Konuma K et al (2007) Is high amplitude propagated contraction present after transanal endorectal pull-through for Hirschsprung’s disease? Pediatr Surg Int 23(10):981–986. doi:10.1007/s00383-007-1981-z
Yang L, Tang ST, Cao GQ et al (2012) Transanal endorectal pull-through for Hirschsprung’s disease using long cuff dissection and short V-shaped partially resected cuff anastomosis: early and late outcomes. Pediatr Surg Int 28(5):515–521. doi:10.1007/s00383-012-3071-0
Dutta HK (2010) Clinical experience with a new modified transanal endorectal pull-through for Hirschsprung’s disease. Pediatr Surg Int 26(7):747–751. doi:10.1007/s00383-010-2629-y
Graneli C, Stenstrom P, Borjesson A et al (2015) Development of frequency of stools over time in children with Hirschsprung disease posttransanal endorectal one-stage pull-through. Eur J Pediatr Surg 25(4):359–364. doi:10.1055/s-0034-1376396
Yanchar NL, Soucy P (1999) Long-term outcome after Hirschsprung’s disease: patients’ perspectives. J Pediatr Surg 34(7):1152–1160
Aworanti OM, McDowell DT, Martin Im et al (2016) Does functional outcome improve with time postsurgery for Hirschsprung disease? Eur J Pediatr Surg 26(2):192–199. doi:10.1055/s-0034-1544053
Langer JC (2012) Laparoscopic and transanal pull-through for Hirschsprung disease. Semin Pediatr Surg 21(4):283–290. doi:10.1053/j.sempedsurg.2012.07.002
Conway SJ, Craigie RJ, Cooper LH et al (2007) Early adult outcome of the Duhamel procedure for left-sided Hirschsprung disease–a prospective serial assessment study. J Pediatr Surg 42(8):1429–1432. doi:10.1016/j.jpedsurg.2007.03.046
Heikkinen M, Rintala RJ, Louhimo I (1995) Bowel function and quality of life in adult patients with operated Hirschsprung’s disease. Pediatr Surg Int 10(5–6):342–344. doi:10.1007/BF00182219
Jarvi K, Laitakari EM, Koivusalo A et al (2010) Bowel function and gastrointestinal quality of life among adults operated for Hirschsprung disease during childhood: a population-based study. Ann Surg 252(6):977–981. doi:10.1097/SLA.0b013e3182018542
Ieiri S, Nakatsuji T, Akiyoshi J et al (2010) Long-term outcomes and the quality of life of Hirschsprung disease in adolescents who have reached 18 years or older–a 47-year single-institute experience. J Pediatr Surg 45(12):2398–2402. doi:10.1016/j.jpedsurg.2010.08.040
Zhang SC, Bai YZ, Wang W et al (2005) Stooling patterns and colonic motility after transanal one-stage pull-through operation for Hirschsprung’s disease in children. J Pediatr Surg 40(11):1766–1772. doi:10.1016/j.jpedsurg.2005.07.027
Athanasakos E, Starling J, Ross F et al (2006) An example of psychological adjustment in chronic illness: Hirschsprung’s disease. Pediatr Surg Int 22(4):319–325. doi:10.1007/s00383-006-1651-6
Ralls MW, Coran AG, Teitelbaum DH (2012) Reoperative surgery for Hirschsprung disease. Semin Pediatr Surg 21(4):354–363. doi:10.1053/j.sempedsurg.2012.07.011
Elhalaby EA, Hashish A, Elbarbary MM et al (2004) Transanal one-stage endorectal pull-through for Hirschsprung’s disease: a multicenter study. J Pediatr Surg 39(3):345–351 (discussion 345–51)
Mills JL, Konkin DE, Milner R et al (2008) Long-term bowel function and quality of life in children with Hirschsprung’s disease. J Pediatr Surg 43(5):899–905. doi:10.1016/j.jpedsurg.2007.12.038
Stensrud KJ, Emblem R, Bjornland K (2015) Anal endosonography and bowel function in patients undergoing different types of endorectal pull-through procedures for Hirschsprung disease. J Pediatr Surg 50(8):1341–1346. doi:10.1016/j.jpedsurg.2014.12.024
Ruttenstock E, Puri P (2010) Systematic review and meta-analysis of enterocolitis after one-stage transanal pull-through procedure for Hirschsprung’s disease. Pediatr Surg Int 26(11):1101–1105. doi:10.1007/s00383-010-2695-1
Ralls MW, Freeman JJ, Rabah R et al (2014) Redo pullthrough for Hirschsprung disease: a single surgical group’s experience. J Pediatr Surg 49(9):1394–1399. doi:10.1016/j.jpedsurg.2014.04.009
Fortuna RS, Weber TR, Tracy TF Jr et al (1996) Critical analysis of the operative treatment of Hirschsprung’s disease. Arch Surg 131(5):520–524 (discussion 524–525)
Nah SA, de Coppi P, Kiely EM et al (2012) Duhamel pull-through for Hirschsprung disease: a comparison of open and laparoscopic techniques. J Pediatr Surg 47(2):308–312. doi:10.1016/j.jpedsurg.2011.11.025
Pini-Prato A, Mattioli G, Giunta C et al (2010) Redo surgery in Hirschsprung disease: what did we learn? Unicentric experience on 70 patients. J Pediatr Surg 45(4):747–754. doi:10.1016/j.jpedsurg.2009.08.001
Wang NL, Lee HC, Yeh ML et al (2004) Experience with primary laparoscopy-assisted endorectal pull-through for Hirschsprung’s disease. Pediatr Surg Int 20(2):118–122. doi:10.1007/s00383-003-1102-6
Langer JC, Minkes RK, Mazziotti MV et al (1999) Transanal one-stage Soave procedure for infants with Hirschsprung’s disease. J Pediatr Surg 34(1):148–151 (discussion 152)
de La Torre L, Langer JC (2010) Transanal endorectal pull-through for Hirschsprung disease: technique, controversies, pearls, pitfalls, and an organized approach to the management of postoperative obstructive symptoms. Semin Pediatr Surg 19(2):96–106. doi:10.1053/j.sempedsurg.2009.11.016
Wester T, Rintala RJ (2004) Early outcome of transanal endorectal pull-through with a short muscle cuff during the neonatal period. J Pediatr Surg 39(2):157–160 (discussion 157–60)
Dickie BH, Webb KM, Eradi B et al (2014) The problematic Soave cuff in Hirschsprung disease: manifestations and treatment. J Pediatr Surg 49(1):77–80. doi:10.1016/j.jpedsurg.2013.09.034 (discussion 80–1)
Gunnarsdottir A, Sandblom G, Arnbjornsson E et al (2010) Quality of life in adults operated on for Hirschsprung disease in childhood. J Pediatr Gastroenterol Nutr 51(2):160–166. doi:10.1097/MPG.0b013e3181cac1b6
Neuvonen MI, Kyrklund K, Lindahl HG et al (2015) A population-based, complete follow-up of 146 consecutive patients after transanal mucosectomy for Hirschsprung disease. J Pediatr Surg 50(10):1653–1658. doi:10.1016/j.jpedsurg.2015.02.006
Neuvonen MI, Kyrklund K, Rintala RJ et al (2016) Bowel function and quality of life after transanal endorectal pull-through for Hirschsprung disease: controlled outcomes up to adulthood. Ann Surg. doi:10.1097/SLA.0000000000001695
Xiong X, Chen X, Wang G et al (2015) Long term quality of life in patients with Hirschsprung’s disease who underwent heart-shaped anastomosis during childhood: a twenty-year follow-up in China. J Pediatr Surg 50(12):2044–2047. doi:10.1016/j.jpedsurg.2015.08.027
Zhang SC, Bai YZ, Wang W et al (2007) Long-term outcome, colonic motility, and sphincter performance after Swenson’s procedure for Hirschsprung’s disease: a single-center 2-decade experience with 346 cases. Am J Surg 194(1):40–47. doi:10.1016/j.amjsurg.2006.10.018
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zimmer, J., Tomuschat, C. & Puri, P. Long-term results of transanal pull-through for Hirschsprung’s disease: a meta-analysis. Pediatr Surg Int 32, 743–749 (2016). https://doi.org/10.1007/s00383-016-3908-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-016-3908-z