Abstract
Purpose
Lateralized tibial tubercle is a cause of patellar instability. Before proceeding with reduction of the tibial tubercle-trochlear groove (TT-TG) distance, surgeons prefer to know whether this distance is pathologic. However, the pathological value remains discussed and may vary with the size of the knee.
Methods
We sought to determine variability in the traditional TT-TG distance versus the anthropometric knee size, using dimensions of the distal part of the femur and proximal part of the tibia of 85 CT scans of the knees in two groups of knees, one normal group without history of patellofemoral instability and one pathologic group with history of instability.
Results
The average TT-TG distance measured 13 mm in normal knees and 16.4 mm in pathologic knees. The variability in measurements between normal and pathologic knees varied respectively between ± 5 and ± 15 mm, with as consequence absence of threshold value between normal and pathologic knees. These measurements were supplemented by an analysis of a size ratio coefficient. In the normal group without history of instability, linear regression analysis showed that patients with larger knees tended to have higher TT-TG distances and that the values are associated with the mean ML femoro-tibial width (p = 0.014; Pearson coefficient = 0.4). The knees with history of instability also keep proportional increase of TT-TG with the size of the knee as the knees without history of instability. We developed a nomogram to more appropriately represent the normal values for a given size of the knee. Application of the nomographic model on the CT scan TT-TG data of the patients who have knee instability allows the orthopaedic surgeon to associate the TT-TG distance with the knee size and to evaluate the medial transfer corresponding to the knee size.
Conclusions
The average TT-TG distances in normal and pathologic knees were not identical for each size of the knees.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Acute patellofemoral dislocation is estimated to 3% of all knee injuries. Its incidence is six per 100,000 individuals [1,2,3]. One of the consequences of a patellofemoral dislocation or repeated occurrence is cartilage damage of the patellofemoral compartment but it can also lead to generalized knee osteoarthritis [4,5,6,7]. Furthermore, pain associated with patellofemoral knee instability without dislocation is frequent in physically active patients [8]. Both dislocation and pain are attributed to multiple factors. One of them is increase distance between tibial tubercle and trochlear groove [8, 9].
Lateralization of the tibial tubercle (TT) was the first bone-mark used in assessing patients with patellofemoral instability. To evaluate this lateralization of the TT, Goutallier [10] in 1978 proposed measurement of the mediolateral distance between the anterior TT and the deepest point of the trochlear groove (TG) on an axial radiograph. Measurement of this TT-TG distance on CT scan was popularized by Dejour [11] in 1994. The quantification of the TT-TG distance has evolved over the past four decades with improvement of the precision including protocol of measurement of TT-TG [12,13,14,15] and introduction of MRI for measurement with discussion about normal and pathological values of the TT-TG [9, 16, 17]. Regardless of the measurement technique, current recommendations [11] are generally based on a cut-off value of 15 mm being the frontier between normal and pathologic distances and on a distance of greater than 20 mm being the threshold to consider a tibial tubercle osteotomy as realignment procedure.
However, this absolute value does not respect the now well-established anatomic differences between the knees of males and females and between the knees of different sizes which has been the subject of numerous studies particularly for the choice of the size of knee arthroplasties. TT-TG distance seems to be highly linked to the knee size if we consider this relation in paediatric population [18,19,20], TT-TG distance increases with age (and therefore indirectly with knee size). To date, the topic of differences according to the size of the knee in the surgical management of medial transfer of the TT has garnered more attention. Several authors have hypothesized that an increased TT-TG distance in a small knee might have a bigger pathological impact on patellofemoral instability than in a larger knee [21,22,23,24,25]. However, correlations between TT-TG distance and size of the knee are still discussed, and particularly, the best parameter to represent the size of the knee is unknown: mediolateral width of the femur, of the tibia, or height or weight of the patient?
Therefore, our objectives were (1) to determine whether the TT-TG distance changes with knee size in normal adult knees without instability and to evaluate the best parameter to evaluate knee size; (2) to confirm that a group of adult patients with patellar instability have higher TT-TG distances than a group of patients without instability; and (3) to propose a knee size chart nomogram allowing an individual interpretation of this measure.
Material and method
Patients’ demographic
In this retrospective multicentric study, two groups of patients were included: a control group and an instability group including patellofemoral dislocation (PD) and patellofemoral pain (PP).
For the control group, 36 knees of 18 patients undergoing CT scan of lower limb for other reason than knee pathology (angio-CT) were included. Patients who presented any anterior or actual pathologies of the area around the knee were excluded from the control group. Patients must have a normal trochlear sulcus angle, a normal Caton-Deschamps index, a normal tilt, and a difference between the TT-TG of both sides less than 3 mm. These restrictions and the absence of history of PD or PP permitted to create a “normal knee” group. The angio-CT scans of these 18 mature adults (11 men, 7 women) were selected, randomized, and anonymized from database of three hospital in Europe (HEGP, Paris France; Victor Dupouy hospital, Argenteuil France; Epicura hospital, Baudour Belgium).
For the pathologic group, 49 knees of 26 patients with history of Elmslie surgery practice for PD or PP were included. CT scans of these 26 adults came from three hospitals in Europe (Erasme hospital, Brussels, Belgium; Epicura hospital, Baudour, Belgium). The pathologic group was divided in two sub-groups: operated knees (29 knees) and non-operated knees (20 knees).
The evaluation protocol used was CT acquisition reference mAs/actual 250 mAs, 120 kV, exposure time 0.5 s, reconstruction thickness 0.6 mm, reconstruction spacing 0.4 mm, and display field of view 170 mm. All DICOM pictures were centralized and analyzed with the same software: Horos. From the two-dimensional transversal images with 0.4-mm cuts, three-dimensional reconstructions were made.
Measurements of TT-TG
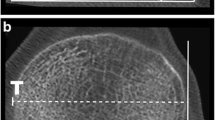
TT-TG was measure in extended position for both groups. The first axial picture of the attachment of the patellar tendon to the tibial tubercle was selected. It has been superposed to the axial picture of the proximal trochlea at the level of the “roman arch.” A tangent line to posterior condyle was drawn. From this line, two perpendicular lines were drawn, one passing through the deepest point of the trochlea and one through the centre of the patellar tendon. Then, the distance between these two lines was measured (Fig. 1).
Assessing knee size
The largest widths, medial to lateral (ML) and anterior to posterior (AP), of the distal femur and proximal tibia have been measured. These measures were performed on an axial view of the distal femur, using the line connecting the posterior femoral condyles as landmark (Fig. 1) for the femur. For the tibia, these measures were performed on an axial view of CT scans at the top of the fibula. A line tangent to the posterior cortex of the tibia and passing through the top of the fibula was used as landmark (Fig. 1).
As the TT-TG is a measure including both femur and tibia, we also included the mean value between the femur and the tibia for each width (called femoro-tibial ML knee size and femoro-tibial AP knee size) in our tests.
Other measurements
Caton-Deschamps index has been measured for all the knees [26]. Trochlea sulcus and slope of the external bank of the trochlea (angle with a line connecting the posterior femoral condyles) were also measured. Patellar tilt was measured as the angle between the line joining the internal to external extremities with the line connecting the posterior femoral condyles.
Statistical analysis
For 28 knees, measures were performed by two independent observers for TT-TG and condyles widths. Deltas were respectively 1.5 and 1.2 mm. The other knees were randomly divided between the two observers. Statistical analysis was performed using software XLSTAT for Windows. The descriptive analysis presented the observed data in the form of tables, expressed using means, standard deviations, and medians, along with illustrative graphs. A p value < 0.05 was considered significant. According to the number of CT cuts (each 0.4 mm) and the matrix (512 × 512), the theoretical accuracy was 0.5 mm for linear measurements and 1° for angular measurements.
Results
Demographic data
Forty-three patients (85 knees) were included. The control group (7 women and 11 men) without patella-femoral instability included 36 knees (12 right; 12 left) from 18 patients; the mean age was 44 years (range 18–58). The instability group included 49 knees (25 right; 24 left) from 26 patients (17 women and 9 men) who presented at least one patella dislocation or patella instability. The mean age was 30 years (range 17–48). There were 17 women and nine men. Table 1 resumes the study population design.
There was no statistical difference between the two groups for widths (AP and ML) of the proximal tibia, the distal femur, and mean femoro-tibial (mean value between tibia and femur), for trochlear sulcus angle and for slope of the external bank of the trochlea and Caton-Deschamps index (Table 1). The TT-TG was higher in the instability group compared to the control group (p < 0.05). The Tilt of the patella was higher in the instability group compared to the control group (p < 0.05). Patients in the control group were older than the pathological group (p < 0.05).
The knees without history of instability
TT-TG distance
The TT-TG values of the 36 knees without history of instability ranged from 5 to 23 mm overall. There was no difference in the mean TT-TG distance with respect to the left and right knees (p = 0.8). The TT-TG distance was significantly different between genders (p = 0.02) with an average value of 11 mm for female and 14 mm for male subjects. When dividing the population of the group without instability in two sub-populations according to femoro-tibial ML width, the mean value of the TT-TG was different (p = 0.02), 11 mm for small knees and 14 mm for large knees (Table 2). The multiple regression analysis performed in all the knees of the group without instability showed that TT-TG distance was better correlated to the mean femoro-tibial ML width than to the femoral or tibial widths alone (Table 1).
Linear regression analysis showed that patients with larger knees tended to have higher TT-TG distances and that the values are associated with the mean ML femoro-tibial width (p = 0.014; Pearson coefficient = 0.4). Figure 2 shows TT-TG distance as a function of size of the knee expressed in millimeters. This size chart shows that curve on the graph approaches for small sizes the normal pediatric TT-TG distance [20] and demonstrates higher values when the size of the knee increases.
Nomogram based on knee size for prediction of TT-GT value
The formula of this augmentation according to the linear regression was “TT-TG measured on CT = 0.23 × (Mean ML femoro-tibial width) − 0.455.” From this formula, we created a TT-TG indexed to knee size called TT-TG indexed. The ratio “TT-TG indexed = (TT-TG measured on CT + 0.455)/(Mean ML femoro-tibial width)” is a constant value equal to 0.23 (CI 95% from 0.21 to 0.24) in the group without instability. From this constant value, we were able to calculate the theoretical normal TT-TG for any knee size. Figures 3 and 4 show the nomograms based on the linear regression model of this formula. Two nomograms were elaborated: one table and one graphic. Their use will be described with three clinical applications.
Nomogram table of the TT-TG indexed to knee size. At the cross section of the femoral width and the tibial width, the theoretical TT-TG for this knee size can be read (examples Fig. 6)
Graphical nomogram of the TT-TG indexed to knee size. First, the line joining the tibia and femoral ML widths must be drawn. The middle of the line is the mean ML femoro-tibial width. At the cross section of the vertical passing by the mean ML femoro-tibial width and the curve, the theoretical TT-TG for this knee size can be read. The nomogram shows that the theoretical TT-TG for the example patient should be 10 mm
Prediction of a normal TT-TG distance
As clinical application, for example a man of 32 years of age is evaluated for the position of the tibial tuberosity with CT scan. Using measuring techniques described above, the physician measures a TT-TG distance of 15 mm. The mediolateral distances of the femur and tibia are respectively 90 and 86 mm. According to the nomogram (Fig. 6 patient a), in this example, the prediction is that this man has a normal TT-TG distance according to the knee size (theoretical TT-TG according to the knee size 15.6 mm).
The knees with history of instability
TT-TG distance
Adult patients with patellar instability history have higher TT-TG distances than the group of patients without instability. The TT-TG values of the 49 knees in the instability group ranged from 9 to 34 mm. The median and mean TT-TG distance values for those knees with instability were 16.4 and 15.6 mm, which was significantly higher than the median and mean (13 and 13 mm) in the normal group (p < 0.001) without history of instability.
The multiple regression analysis performed in the instability group showed that TT-TG was not was as well correlated to the mean femoro-tibial ML width as compared as to that was observed in the control group without instability (Table 1). Despite this low correlation, we also observed a not statistical significant difference (p = 0.051) between small and large knees in the pathological group with respectively a mean value of 15 mm for small knees and a mean value of 20 mm for large knees (Table 2). This was also observed when a linear regression was performed (Fig. 5). Regression was statistically significant for the pathologic group (p < 0.05).
Prediction of pathologic values with the nomogram
Therefore, the knees with history of instability also keep proportional increase of TT-TG with the size of the knee (Fig. 5) as the knees without history of instability. Therefore, assuming that the TT-TG distances of the knees without history of instability should be the targets for the TT-GT distances of the knees with instability when the size of the knee is the same, we performed a cross-validation between data of pathologic and normal knees. The data set were divided (higher or lesser) according to the normal value of the TT-TG measured (15 mm) or the TT-TG indexed (constant value 0.23, using the formula previously cited in the group without instability) on knee size. Higher values were considered as pathological and lesser values as normal. Sensitivity, specificity, positive predictive value, and negative predictive value of each TT-TG were measured. Results for the TT-TG measured were respectively 53, 75, 74, and 54%. For TT-TG indexed to knee size sensitivity and negative predictive value were increased compare to TT-TG measured with respectively 82, 64, 75, and 72%, which confirms the efficiency of the nomogram.
Prediction of medial transfer of the tibial tuberosity
A woman of 21 years of age is evaluated for knee instability with CT scan. Using measuring techniques described above, the physician measures a TT-TG distance of 15 mm. The mediolateral distances of the femur and tibia are respectively 72 and 59 mm. Using the nomogram of Fig. 6 (patient b), the TT-TG distance in this example is well above the theoretical TT-TG of this knee size (10.4 mm), indicating that this woman has relatively higher TT-TG distance than the normal knee. Another example is a patient (with patellar instability) with a TT-TG measured by the physician of 23 mm. The mediolateral distances of the femur and the tibia are 79 and 72 mm. Using the nomogram of Fig. 6 (patient c), the TT-TG distance according to knee size should be 12.7 mm. Then, the anterior tibial tuberosity of this patient must be transposed of 10 mm to restore a normal TT-TG.
Description of the utilization of the nomogram in three clinical applications (patients a, b, and c). Patient a has a measured TT-TG of 15 mm on the CT scan and his theoretical TT-TG according to knee size is 15.6 mm (his TT-TG is then normal). Patient b has a measured TT-TG of 15 mm; however, her theoretical TT-TG according to knee size is 10.4 mm; her TT-TG is therefore pathological (higher than the normal value of 10.4 mm). Patient c has a measured TT-TG of 23 mm; however, his theoretical TT-TG according to knee size is 12.7 mm; so, the medial translation of the anterior tibial tubercle should be 10 mm if this procedure is proposed
Discussion
Surgical treatment of patients with patellar instability is frequently discussed according to extensor mechanism malalignment. Quantification of such a malalignment is usually performed by the TT-TG distance measurement which is considered to be objective and reliable. The metric variation of the TT-TG distance is considered to be related to shape variations as trochlea dysplasia or lateralization of the tubercle position on the proximal tibia. Justification for a medializing tibial tubercle osteotomy is usually based on a 20- or 15-mm threshold value with as goal of transfer a reduction of the TT-TG distance to between 10 and 15 mm value [11]. However, as for all the metric values, anatomical variation related to the size of the knee or to the size of the patient is possible. Therefore, the threshold value and the metric target could be different from a patient to another. While some reports have indicated that there is a probable interaction between TT-TG and individual knee size, there is no clear quantification of differences in the TT-TG distance that can be related to size or shape in a comprehensive chart [22, 24, 25]. We therefore developed a knee size chart to better represent the normal values of the TT-TG distance for a given mediolateral size of the knee.
Our main objective was to determine whether the TT-TG distance in adult subjects changes with the size of the knee. Our data strongly suggest that it does. Our primary result is that for the normal knee, variability in TT-TG distance is dominated by size, rather than shape. The results of this series showing TT-TG distance and age interdependence contradict some previously published reports claiming [21, 22] their respective independence. Our data are however in concordance with other reports [24, 25] and with increasing TT-TG distance in paediatric subjects advancing in age and progressing toward skeletal maturity [20]. As the size of the knee increases with age, it appears logical that the TT-TG distance increases in size; however, another reason for an increasing distance with age in children could also be a change in torsion of the limb [27,28,29,30,31,32].
We were able to confirm that the subgroup of patients with patellar instability had higher TT-TG distances than a normal control group. Given a knee size, our patients with patellar instability had significantly higher TT-TG distances than those without patellar instability. The analyses of TT-TG distance size performed in the study for the knees with history of patellar instability were only possible after establishment of reference values with the knee size obtained from general population control individuals. Adequate adjustment in curves was obtained with linear regression, because of the presence of extreme values that could influence the homogeneity of the sample.
We developed a nomogram to more appropriately represent the normal values for a given size of the knee. The major advantage of a nomogram is its easy application: the operator needs only to add the corresponding points of the knee size with CT-derived measurements. Application of the nomographic model on the CT scan TT-TG data of the patients who have knee instability allows the orthaopedic surgeon to associate the TT-TG distance with knee size. This is particularly useful in small knees of women where a “14-mm” TT-TG distance may appear normal when considering for all knees (whatever the size) an absolute 15-mm threshold value as proposed in literature, but in reality, is increased when the knee size is small. At the reverse, a TT-TG distance of 17 mm might be considered as normal for a large knee.
With regard to the surgical treatment, this study supports the idea of normalizing TT-TG to individual patient size. First, this chart allows the orthopaedic surgeon to associate the TT-TG distance with the knee size in patients with patellar instability. That information can help to determine whether a soft-tissue distal realignment procedure should be included as the surgical reconstruction for patients whose TT-TG distance is normal as regard as the size of the knee. At the reverse, when a knee with an increased tibial TT-TG is surgically addressed by medial transfer of the tibial tuberosity, the chart can be used to select the target value according to the size of the patient.
One limitation of our study is that we associated TT-TG distance with only the size of the knee; other metrics, such as lower limb torsion, and trochlear dysplasia are also associated with patellar instability. Information to retrospectively analyze these values was not consistently available in our clinical data base and was therefore not used. There is also potential bias in that we assumed that our patients without history of instability included in the normal group will never develop patellar instability; our data could be skewed if some of these patients were to develop symptoms of instability later. Another limitation is that our data were obtained in Caucasian people, and we cannot extrapolate our results for other ethnic populations [33,34,35].
In conclusion, this study serves as a basis for further investigation into the role of TT-TG distance for evaluating patients with recurrent patellar instability. We showed that TT-TG distance changes with the size of the knee and that a chart representation is an appropriate method to describe normal TT-TG distance for a given size.
References
Colvin AC, West RV (2008) Patellar instability. J Bone Joint Surg Am 90:2751–2762. https://doi.org/10.2106/JBJS.H.00211
Fithian DC, Paxton EW, Stone ML et al (2004) Epidemiology and natural history of acute patellar dislocation. Am J Sports Med 32:1114–1121. https://doi.org/10.1177/0363546503260788
Li X, Nielsen NM, Zhou H et al (2013) Surgical treatment of a chronically fixed lateral patella dislocation in an adolescent patient. Orthop Rev 5:45–47. https://doi.org/10.4081/or.2013.e9
Salonen EE, Magga T, Sillanpää PJ et al (2017) Traumatic patellar dislocation and cartilage injury: a follow-up study of long-term cartilage deterioration. Am J Sports Med 45:1376–1382. https://doi.org/10.1177/0363546516687549
Elias DA, White LM, Fithian DC (2002) Acute lateral patellar dislocation at MR imaging: injury patterns of medial patellar soft-tissue restraints and osteochondral injuries of the inferomedial patella. Radiology 225:736–743. https://doi.org/10.1148/radiol.2253011578
Nomura E, Inoue M, Kurimura M (2003) Chondral and osteochondral injuries associated with acute patellar dislocation. Arthrosc J Arthrosc Relat Surg Off Publ Arthrosc Assoc N Am Int Arthrosc Assoc 19:717–721
Vollnberg B, Koehlitz T, Jung T et al (2012) Prevalence of cartilage lesions and early osteoarthritis in patients with patellar dislocation. Eur Radiol 22:2347–2356. https://doi.org/10.1007/s00330-012-2493-3
Rosso F, Rossi R, Governale G et al (2017) Tibial tuberosity anteromedialization for patellofemoral chondral disease. Am J Sports Med 363546517690387. https://doi.org/10.1177/0363546517690387
Lobner S, Krauss C, Reichwein F et al (2017) Surgical treatment of patellar instability: clinical and radiological outcome after medial patellofemoral ligament reconstruction and tibial tuberosity medialisation. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-017-2705-z
Goutallier D, Bernageau J, Lecudonnec B (1978) The measurement of the tibial tuberosity. Patella groove distanced technique and results (author’s transl). Rev Chir Orthop Reparatrice Appar Mot 64:423–428
Dejour H, Walch G, Nove-Josserand L, Guier C (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc Off J ESSKA 2:19–26
Camathias C, Pagenstert G, Stutz U et al (2016) The effect of knee flexion and rotation on the tibial tuberosity-trochlear groove distance. Knee Surg Sports Traumatol Arthrosc Off J ESSKA 24:2811–2817. https://doi.org/10.1007/s00167-015-3508-9
Dietrich TJ, Betz M, Pfirrmann CWA et al (2014) End-stage extension of the knee and its influence on tibial tuberosity-trochlear groove distance (TTTG) in asymptomatic volunteers. Knee Surg Sports Traumatol Arthrosc Off J ESSKA 22:214–218. https://doi.org/10.1007/s00167-012-2357-z
Hirschmann A, Buck FM, Fucentese SF, Pfirrmann CWA (2015) Upright CT of the knee: the effect of weight-bearing on joint alignment. Eur Radiol 25:3398–3404. https://doi.org/10.1007/s00330-015-3756-6
Izadpanah K, Weitzel E, Vicari M et al (2014) Influence of knee flexion angle and weight bearing on the tibial tuberosity-trochlear groove (TTTG) distance for evaluation of patellofemoral alignment. Knee Surg Sports Traumatol Arthrosc Off J ESSKA 22:2655–2661. https://doi.org/10.1007/s00167-013-2537-5
Kulkarni S, Shetty AP, Alva KK et al (2016) Patellar instability in Indian population: relevance of tibial tuberosity and trochlear groove distance. SICOT-J 2:14. https://doi.org/10.1051/sicotj/2016008
Mohammadinejad P, Shekarchi B (2016) Value of CT scan-assessed tibial tuberosity-trochlear groove distance in identification of patellar instability. Radiol Med (Torino) 121:729–734. https://doi.org/10.1007/s11547-016-0647-0
Zivicnjak M, Smolej Narancić N, Szirovicza L et al (2008) Gender-specific growth patterns of transversal body dimensions in Croatian children and youth (2 to 18 years of age). Coll Antropol 32:419–431
Chan EF, Harjanto R, Asahara H et al (2012) Structural and functional maturation of distal femoral cartilage and bone during postnatal development and growth in humans and mice. Orthop Clin North Am 43:173–185, v. https://doi.org/10.1016/j.ocl.2012.01.005
Dickens AJ, Morrell NT, Doering A et al (2014) Tibial tubercle-trochlear groove distance: defining normal in a pediatric population. J Bone Joint Surg Am 96:318–324. https://doi.org/10.2106/JBJS.M.00688
Dornacher D, Reichel H, Kappe T (2016) Does tibial tuberosity-trochlear groove distance (TT-TG) correlate with knee size or body height? Knee Surg Sports Traumatol Arthrosc Off J ESSKA 24:2861–2867. https://doi.org/10.1007/s00167-015-3526-7
Pennock AT, Alam M, Bastrom T (2014) Variation in tibial tubercle-trochlear groove measurement as a function of age, sex, size, and patellar instability. Am J Sports Med 42:389–393. https://doi.org/10.1177/0363546513509058
Balcarek P, Jung K, Frosch K-H, Stürmer KM (2011) Value of the tibial tuberosity-trochlear groove distance in patellar instability in the young athlete. Am J Sports Med 39:1756–1761. https://doi.org/10.1177/0363546511404883
Ferlic PW, Runer A, Dirisamer F et al (2017) The use of tibial tuberosity-trochlear groove indices based on joint size in lower limb evaluation. Int Orthop. https://doi.org/10.1007/s00264-017-3531-1
Hingelbaum S, Best R, Huth J et al (2014) The TT-TG index: a new knee size adjusted measure method to determine the TT-TG distance. Knee Surg Sports Traumatol Arthrosc Off J ESSKA 22:2388–2395. https://doi.org/10.1007/s00167-014-3204-1
Caton J (1989) Method of measuring the height of the patella. Acta Orthop Belg 55:385–386
Bruce WD, Stevens PM (2004) Surgical correction of miserable malalignment syndrome. J Pediatr Orthop 24:392–396
Cooke TD, Price N, Fisher B, Hedden D (1990) The inwardly pointing knee. An unrecognized problem of external rotational malalignment. Clin Orthop:56–60
Lee TQ, Morris G, Csintalan RP (2003) The influence of tibial and femoral rotation on patellofemoral contact area and pressure. J Orthop Sports Phys Ther 33:686–693. https://doi.org/10.2519/jospt.2003.33.11.686
Nelitz M, Dreyhaupt J, Williams SRM, Dornacher D (2015) Combined supracondylar femoral derotation osteotomy and patellofemoral ligament reconstruction for recurrent patellar dislocation and severe femoral anteversion syndrome: surgical technique and clinical outcome. Int Orthop 39:2355–2362. https://doi.org/10.1007/s00264-015-2859-7
Steensen RN, Bentley JC, Trinh TQ et al (2015) The prevalence and combined prevalences of anatomic factors associated with recurrent patellar dislocation: a magnetic resonance imaging study. Am J Sports Med 43:921–927. https://doi.org/10.1177/0363546514563904
Tensho K, Akaoka Y, Shimodaira H et al (2015) What components comprise the measurement of the tibial tuberosity-trochlear groove distance in a patellar dislocation population? J Bone Joint Surg Am 97:1441–1448. https://doi.org/10.2106/JBJS.N.01313
Barnes CL, Iwaki H, Minoda Y et al (2010) Analysis of sex and race and the size and shape of the distal femur using virtual surgery and archived computed tomography images. J Surg Orthop Adv 19:200–208
Xie X, Lin L, Zhu B et al (2014) Will gender-specific total knee arthroplasty be a better choice for women? A systematic review and meta-analysis. Eur J Orthop Surg Traumatol Orthop Traumatol 24:1341–1349. https://doi.org/10.1007/s00590-013-1396-6
Yan M, Wang J, Wang Y et al (2014) Gender-based differences in the dimensions of the femoral trochlea and condyles in the Chinese population: correlation to the risk of femoral component overhang. Knee 21:252–256. https://doi.org/10.1016/j.knee.2012.11.005
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Hernigou, J., Chahidi, E., Bouaboula, M. et al. Knee size chart nomogram for evaluation of tibial tuberosity-trochlear groove distance in knees with or without history of patellofemoral instability. International Orthopaedics (SICOT) 42, 2797–2806 (2018). https://doi.org/10.1007/s00264-018-3856-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-3856-4