Abstract
Purpose
To determine the differential points of strangulated ileus with and without irreversible ischaemic changes, especially on preoperative computed tomography (CT) images.
Methods
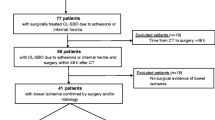
Seventy patients with strangulated ileus underwent emergency operations between January 2009 and July 2016 in our department. Of these patients, 57 met the study requirements, including 30 patients who had irreversible ischaemic changes (ischaemic group; n = 30) and 27 patients who had reversible ischaemic changes during laparotomy (non-ischaemic group; n = 27). We compared the preoperative clinical and radiographic factors between the ischaemic and non-ischaemic groups.
Results
Univariate analysis revealed that a mean CT value of the intestine in an unenhanced image ≥16.5 HU (p < 0.001), a mean CT value ratio of the intestine (enhanced/unenhanced image) <1.5 (p < 0.001), presence of mesenteric fluid (p = 0.002) and presence of free peritoneal fluid (p = 0.009) were associated with the ischaemic group.
Conclusions
Calculation of the mean CT value of a strangulated intestine may be a useful method for predicting irreversible ischaemic changes in addition to the presence of mesenteric fluid or free peritoneal fluid.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Recently, multi-detector computed tomography (MDCT) imaging has become a useful and essential method for the diagnosis of strangulated ileus or acute bowel ischaemia [1, 2].
If the strangulated intestines have irreversible ischaemic changes, resection of the intestine is necessary [3]. Conversely, if the ischaemic change is reversible, an operation may be performed to release the strangulation [3]. Regarding the surgical strategy, for patients with irreversible ischaemic changes, a conversion from laparoscopic surgery to laparotomy is frequently performed, which results in an increased risk of morbidity compared with the operations that do undergo this conversion [4]. To develop a well-considered perioperative strategy, preoperative differentiation of strangulated ileus with and without irreversible ischaemia is essential for surgeons. However, many cases of strangulated ileus with an irreversible ischaemic change are first recognized during surgery. For such cases, it is a challenge to distinguish and predict irreversible ischaemic changes preoperatively. The aim of this study is to determine the differential points of strangulated ileus with and without irreversible ischaemic changes, especially on preoperative MDCT images, and to assess bowel wall enhancement in a quantitative manner using the CT value of the strangulated intestine.
Methods
Study population
Seventy patients diagnosed with strangulated ileus underwent emergency operation between January 2009 and July 2016 in our department. The inclusion criterion for this retrospective study was decided by preoperative CT findings as follows: patients with a finding of strangulation including closed loop sign and whirl sign in their preoperative CT images. The exclusion criteria were as follows: patients did not exhibit an apparent obstruction site on the CT image; patients did not undergo an enhanced CT before the operation and patients who used oral contrast agent before undergoing CT. In total, 57 patients met the study criteria and were included. Of these patients, 30 patients exhibited an irreversible ischaemic change at laparotomy (ischaemic group; n = 30), and 27 patients had a reversible ischaemic change at laparotomy (non-ischaemic group; n = 27). Thirteen patients were excluded from this study. We retrospectively reviewed and compared the preoperative clinical and radiographic factors between the ischaemic and non-ischaemic groups.
Surgical strategy and surgical procedure for strangulated ileus
At our institution, all patients with an acute abdomen that suggests strangulated ileus undergo enhanced MDCT unless the patient has a contraindication, such as an allergy for contrast agents, or exhibits impaired renal function. Patients diagnosed with a strangulated ileus undergo an emergency operation as soon as possible unless the patients are thought to be intolerant to operation. For patients with irreversible ischaemic changes, we resect the strangulated intestine. Conversely, for patients without irreversible ischaemic changes, release of the strangulation is performed. We initially perform laparoscopic surgery before laparotomy for patients diagnosed with strangulated ileus. Conversion to laparotomy is considered when an irreversible ischaemic change or massive adhesions are found. The presence of irreversible ischaemic change is assessed when any of the following findings are confirmed during the operation: (1) an irreversible change of intestine color is found several minutes after release of the strangulation, or (2) an absence of peristalsis is observed several minutes after release of the strangulation.
Pre- and perioperative findings
Preoperative information included gender, age, WBC level, C-reactive protein (CRP) level, creatine kinase level, blood urea nitrogen (BUN) level, creatinine (Cre) level, and radiographic findings of MDCT imaging. The perioperative findings included operation time, time to operation after performing CT, postoperative length of hospital stay, and incidence rate of postoperative complications. Complications were classified according to the grading system proposed by Dindo et al. [5], and grade III or further complications were considered significant.
Imaging diagnostic modality and radiographic parameters
Among the 57 patients included in the study, all patients were preoperatively examined by abdominal MDCT in non-enhanced and enhanced phases using light speed VCT (GE Healthcare, Tokyo, Japan). Nonionic contrast medium (100 mL) was administered with a power injector at a rate of 1.0 mL/s. For the enhanced images of 54 patients, the scans were acquired 130 s after contrast injection. The other three patients underwent dynamic CT. In a dynamic CT, a nonionic contrast medium (100 mL) was administered with a power injector at a rate of 2.5 mL/s. Hence, the CT values of these three patients were calculated in the portal phase and acquired 90 s after the contrast injection as the enhanced image. Two experienced reviewers (A.K. and K.M.: A.K. is a gastroenterological surgeon with 11 years of experience. K.M. is a radiologist with 16 years of experience) retrospectively reviewed the radiographic parameters to determine the mean CT value of the strangulated intestine on both unenhanced and enhanced images, the presence of free peritoneal fluid around the strangulated intestine, and the presence of mesenteric fluid corresponding to the strangulated intestine. Measurements were performed in consensus, and both readers were blinded to the outcome at the time of performing measurements. The mean CT value of a strangulated intestine was calculated as the mean of region-of-interest analysis, which was achieved by circling the expanded intestine, including the fluid in the lumen, on the screen. Circling of the intestine was performed elliptically on an axial image of the CT image. The mean CT value ratio was obtained by dividing the mean CT value of the enhanced image by that of the unenhanced image. In the present study, inclusion criteria of the slice for measuring CT value are summarized as follows: a slice in which the strangulated intestine appeared in the short axis view orthogonal to the long axis view as much as possible; a slice in which the strangulated intestine was well expanded in an elliptical shape with fluids without gases. If more than two slices were found to match the criteria above, we measured as many slices as possible among them. Then, we selected the highest value of the unenhanced and enhanced images for analysis (Fig. 1A, B).
A The figure shows an example of a non-ischaemic case; the mean CT value was 14.79 HU in the unenhanced image and 28.22 HU in the enhanced image. The mean CT values of the strangulated intestine were obtained by circling the expanded intestine, including the fluid in the lumen, on an axial image using region-of-interest analysis. When calculating the mean CT value of the intestine, we made sure to select a part in which the expanded intestine was filled with fluid and the intestine was viewed using a slice in the short axis. B The figure shows an example of an ischaemic case; the mean CT value was 32.79 HU in the unenhanced image and 35.74 HU in the enhanced image
Statistical analysis of the surgical outcomes and clinicoradiological factors
The clinical and radiographic factors of the ischaemic and non-ischaemic groups were compared. Each cut-off value was determined according to the median value or a receiver operating characteristic curve for the estimated probability of the ischaemic group, adjusting to a value easy to use in practice. Pearson’s χ 2 test was used with Yates’ correction to assess nominal variables, and continuous data were compared using the Mann–Whitney U test. All statistical analyses were performed using the Software Package for Social Sciences, version 11.5J for Windows 1 software program (SPSS, Chicago, IL, USA). A p value of <0.05 was considered significant.
Results
Comparison of the clinical factors between the patients in the ischaemic and non-ischaemic groups
Clinical characteristics of the ischaemic and non-ischaemic groups are presented in Table 1. No significant differences in the preoperative laboratory data, including WBC, CRP, CPK, BUN, and Cre, were noted between the groups. The time to operation after performing CT was comparable between the groups. Operation time (106 vs. 71 min; p = 0.040) and postoperative length of hospital stay (16.5 vs. 11 days; p = 0.018) were significantly longer in the ischaemic group compared with the non-ischaemic group. The incident rate of postoperative complications was increased in the ischaemic group (20.0%) compared with the non-ischaemic group (3.7%), but the result was not statistically significant.
Prediction of irreversible ischaemic change in strangulated intestine
Univariate analysis revealed that a mean CT value of the intestine in an unenhanced image of ≥16.5 HU (p < 0.001), a mean CT value ratio of <1.5 (p < 0.001), presence of mesenteric fluid (p = 0.002) and presence of free peritoneal fluid (p = 0.009) were significantly associated with the ischaemic group (Table 2). Patients with a mean CT value of ≥16.5 HU in an unenhanced image of the intestine exhibited 93.3% sensitivity, 96.3% specificity, and 94.7% accuracy for irreversible ischaemic changes, whereas patients with a mean CT value ratio of <1.5 exhibited 93.3% sensitivity, 55.5% specificity, and 75.4% accuracy for irreversible ischaemic changes. Of thirty patients in the ischaemic group, 26 patients had both findings. In other four patients, two patients had one finding each. Thus, no patients lacked both findings in the ischaemic group.
The predictive accuracy of a mean CT value of the intestine in an unenhanced image and a mean CT value ratio for the ischaemic group could be evaluated by area under the curve analysis, providing values of 0.975 and 0.827, respectively. The cut-off values of these factors were 16.83 HU and 1.413, respectively, according to the receiver operating characteristic curves (Fig. 2).
Discussion
Our findings in this study can be summarized as follows: (1) a mean CT value of the intestine in an unenhanced image of ≥16.5 HU, a mean CT value ratio of <1.5, presence of mesenteric fluid and presence of free peritoneal fluid were significantly associated with the ischaemic group. The cut-off values of a mean CT value of the intestine in an unenhanced image and a mean CT value ratio were 16.83 HU and 1.413, respectively. (2) In patients with irreversible ischaemic changes, the operation time and postoperative length of hospital stay were significantly increased in the ischaemic group compared the nonischemic group.
A variety of CT signs, such as mesenteric fluid, mesenteric venous congestion, free peritoneal fluid, and reduced bowel enhancement, have been reported as findings related to bowel strangulation [6,7,8,9]. In a recent review, Millet et al. reported that a reduced enhanced bowel wall is highly predictive of ischaemia [6]. Geffroy et al. reported that elevation of bowel wall attenuation in an unenhanced image is highly specific for ischaemia with 56% sensitivity and 100% specificity [10]. However, in these reports, the assessment criteria for reduced enhancement of the bowel wall or elevation of bowel wall attenuation were not quantitative. In practice, it seems difficult to judge the presence of enhancement without a quantitative measure, especially if bowel wall attenuation is increased in an unenhanced image. In this study, we assessed the degree of enhancement or bowel wall attenuation by calculating a mean CT value of the strangulated intestine by circling the expanded intestine, including fluids in the lumen. This procedure might obscure the relevance of bowel wall enhancement and intraluminal attenuation. However, measurements of CT values limited to the bowel wall are intricate and difficult to obtain. In general, the bowel wall is fully dilated in the strangulated loop. Therefore, we suggest selecting a slice in which the intestine was well expanded as an elliptical shape to maintain repeatability. Thus, we could perform quantitative assessments in a reproducible and easy fashion.
Our result demonstrated that simultaneous measurement of CT values of the bowel wall and intraluminal is useful for predicting irreversible ischaemic change. We hypothesized that the elevated CT values in an unenhanced CT may represent hemorrhage, whereas the decreased CT ratio may be derived from decreased enhancement in a haemorrhagic wall. Intraluminal attenuation around the irreversible ischaemic bowel may also cause a CT value to exhibit an increased association with some form of hemorrhage [11]. In addition, in the bowel with irreversible ischaemic change, the bowel wall appears thicker on the CT image due to congestion and hemorrhage, resulting in an increased CT value in the unenhanced image. However, this phenomenon was not validated in the present study.
To the best of our knowledge, quantitative findings related to bowel wall attenuation have not been concretely reported in the literature.
CT values are useful for distinguishing various clinical states [11,12,13,14,15]. For example, the CT value of tumors reflects tumor vascularity in intrahepatic cholangiocarcinoma [12]. A recent study suggested that CT values are also useful for judging the severity of acute cholecystitis [13]. Regarding the differentiation of intestinal ischaemic changes, Miyaki et al. reported that the CT values of fluid that accumulated in the expanded intestine were significantly increased in patients with strangulated ileus compared with patients with non-strangulated ileus [11].
Of note, a mean CT value ratio of <1.5, which indicates a reduction of bowel wall enhancement, and a mean CT value of the intestine in an unenhanced image of ≥16.5 HU were associated with irreversible ischaemic change. This finding suggests that calculating a mean CT value of an unenhanced CT may also be a useful method for predicting irreversible ischaemic changes for patients with strangulated ileus, although enhanced CT image is essential for diagnosing strangulation. In our study, a mean CT value of the intestine in an unenhanced image of ≥16.5 HU exhibited 93.3% sensitivity, 96.3% specificity, and 94.7% accuracy for irreversible ischaemic change. This high specificity was comparable to a previous report [10].
One of the limitations of this study is its retrospective nature and single-centre location. Additional external validation is necessary to confirm that these findings are applicable to other patient groups. Another limitation is that some parts of the intestine are still alive in the strangulated intestine, whereas other parts are not, resulting in different CT values by location. Thus, in some cases, it is difficult to determine the candidate loop of the intestine to calculate the CT value. In the present study, we resolved this problem by selecting the higher CT value when the strangulated intestine exhibits variation in CT values by location.
In addition, two readers obtained CT value measurements via a consensus read. It was desirable to perform measurement by several readers independently. Finally, the majority of patients were subject to CT scanning at 130 s after contrast injection, which was later than the typical portal venous scan.
In conclusion, a mean CT value of the intestine in an unenhanced image and a mean CT value ratio were useful factors for predicting irreversible ischaemic changes in patients with a strangulated ileus in addition to the presence of mesenteric fluid or free peritoneal fluid.
References
Maglinte DD, Howard TJ, Lillemoe KD, Sandrasegaran K, Rex DK (2008) Small-bowel obstruction: state-of-the-art imaging and its role in clinical management. Clin Gastroenterol Hepatol 6:130–139
Wiesner W, Khurana B, Ji H, Ros PR (2003) CT of acute bowel. Radiology 226:635–650
Takahashi R, Akagi Y, Tanaka T, et al. (2014) Clinicopathological evaluation of anoxic mucosal injury in strangulation ileus. BMC Surg 14:79
O’Connor DB, Winter DC (2012) The role of laparoscopy in the management of acute small-bowel obstruction: a review of over 2,000 cases. Surg Endosc 26:12–17
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Millet I, Taourel P, Ruyer A, Molinari N (2015) Value of CT findings to predict surgical ischemia in small bowel obstruction: a systematic review and meta-analysis. Eur Radiol 25:1823–1835
Hayakawa K, Tanikake M, Yoshida S, et al. (2013) CT findings of small bowel strangulation: the importance of contrast enhancement. Emerg Radiol 20:3–9
Sheedy SP, Earnest F IV, Fletcher JG, Fidler JL, Hoskin TL (2006) CT of small-bowel ischemia associated with obstruction in emergency department patients: diagnostic performance evaluation. Radiology 241:729–736
Wiesner W, Mortele K (2011) Small bowel ischemia caused by strangulation in complicated small bowel obstruction. CT findings in 20 cases with histopathological correlation. JBR-BTR 94:309–314
Geffroy Y, Boulay-Coletta I, Jullès MC, et al. (2014) Increased unenhanced bowel-wall attenuation at multidetector CT is highly specific of ischemia complicating small-bowel obstruction. Radiology 270:159–167
Miyaki Y, Yamaguchi A, Isogai M, et al. (2008) Utility of CT value measurement of fluid accumulated in expanded intestinal lumen in the diagnosis of strangulated small bowel obstruction. Jpn J Gastroenterol Surg 41:464–468 (in Japanese)
Yamamoto Y, Türkoğlu MA, Aramaki T, et al. (2016) Vascularity of intrahepatic cholangiocarcinoma on computed tomography is predictive of lymph node metastasis. Ann Surg Oncol 23:485–493
Maehira H, Itoh A, Kawasaki M, et al. (2016) Use of dynamic computed tomography attenuation value for diagnosis of acute gangrenous cholecystitis. Am J Emerg Med. doi:10.1016/j.ajem.2016.08.033
Jiang B, Wang J, Jia P, Le M (2013) The value of CT attenuation in distinguishing atypical adenomatous hyperplasia from adenocarcinoma in situ. Zhongguo Fei Ai Za Zhi 16:579–583
Edwards RM, Godwin JD, Hippe DS, Kicska G (2016) A quantitative approach to distinguish pneumonia from atelectasis using computed tomography attenuation. J Comput Assist Tomogr 40:746–751
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflict of interest
The authors declare that they have no conflict of interest. The authors have no direct or indirect commercial or financial incentives associated with publishing this article.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Institutional and/or National Research Committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. For this type of study formal consent is not required. The study protocol was approved by the Institutional Review Board. The study does not include any animal experiments.
Informed consent
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
This retrospective study is for academic communication only and is not for other purposes.
Rights and permissions
About this article
Cite this article
Kohga, A., Kawabe, A., Yajima, K. et al. CT value of the intestine is useful predictor for differentiate irreversible ischaemic changes in strangulated ileus. Abdom Radiol 42, 2816–2821 (2017). https://doi.org/10.1007/s00261-017-1227-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-017-1227-z