Abstract
Background
Young children with suspected abusive head trauma often receive skull radiographs to evaluate for fractures as well as computed tomography (CT) of the head to assess for intracranial injury. Using a CT as the primary modality to evaluate both fracture and intracranial injury could reduce exposure to radiation without sacrificing performance.
Objective
To evaluate the sensitivity of CT head with (3-D) reconstruction compared to skull radiographs to identify skull fractures in children with suspected abusive head trauma.
Materials and methods
This was a retrospective (2013-2014) cross-sectional study of infants evaluated for abusive head trauma via both skull radiographs and CT with 3-D reconstruction. The reference standard was skull radiography. All studies were read by pediatric radiologists and neuroradiologists, with ten percent read by a second radiologist to evaluate for interobserver reliability.
Results
One hundred seventy-seven children (47% female; mean/median age: 5 months) were included. Sixty-two (35%) had skull fractures by radiography. CT with 3-D reconstruction was 97% sensitive (95% confidence interval [CI]: 89-100%) and 94% specific (CI: 87-97%) for skull fracture. There was no significant difference between plain radiographs and 3-D CT scan results (P-value = 0.18). Kappa was 1 (P-value <0.001) between radiologist readings of CTs and 0.77 (P = 0.001) for skull radiographs.
Conclusion
CT with 3-D reconstruction is equivalent to skull radiographs in identifying skull fractures. When a head CT is indicated, skull radiographs add little diagnostic value.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Injuries due to head trauma are a common reason for presentation to pediatric emergency departments, resulting in more than 400,000 visits in the United States [1]. In many infants, concern for head trauma that may not be clinically evident or unclear reports of the mechanism of injury prompt neuroimaging. Currently, skull radiographs, often performed as part of a skeletal survey, are used as the standard and most basic imaging tool for diagnosis of skull fractures [2–5]. Although effective in identifying fractures, radiographs are inaccurate at predicting intracranial injury following blunt head trauma [6, 7]. For this reason, many infants routinely have computed tomography (CT) of the brain obtained to evaluate for intracranial injury [7]. It has been estimated that the sensitivity of CT of the brain for skull fractures is as high as 85% with specificity of 100% when postmortem findings were used as the reference standard [8]. The same authors found that, when compared with autopsy findings, skull radiographs missed 19% of fractures, compared to 12% missed by CTs [9].
As 3-D reconstructions have become more common in recent years [10], the added diagnostic value of skull radiographs is unclear [11]. Frequently, children with suspected head trauma will be evaluated in emergency departments after hours when pediatric radiologists are unavailable, resulting in emergency department physicians initially reading skull radiographs and determining management. Interpretation can be challenging due to the superimposition of suture lines, fissures, wormian bones, vascular grooves or other normal variants [10, 12, 13] that may result in false-positive radiographic interpretations and unnecessary medical and social work evaluation. Conversely, missing subtle fractures can result in a child being returned to caregivers in an unsafe environment resulting in additional injury [13]. Prior studies have found that pediatric emergency medicine physicians have limited accuracy (<80% sensitivity) in interpreting skull radiographs in infants and young children [14, 15]. While sensitivity is increased when four-view skull radiographs are obtained [14], most institutions obtain two-view radiographs. Also contentious is which radiographic modality should be used as the reference standard. One recent study found that use of CT with 3-D reconstructions increased the sensitivity of diagnosing linear skull fractures in all children and increased specificity for children younger than 2 years of age when compared to traditional CTs [16]. The goal of our study was to determine the performance characteristics of CT of the brain with 3-D reconstruction in the diagnosis of skull fracture in infants with suspected abusive head trauma. To the best of our knowledge, this is the largest emergency department-based study evaluating this question.
Materials and methods
Institutional Review Board approval was obtained prior to study initiation.
This was a retrospective cohort study of infants (<1 year old) seen between March 2013 and March 2014 in whom both skeletal surveys and CT of the head were obtained to evaluate for non-accidental trauma. Children were evaluated in the emergency department of a quaternary care children’s hospital that is one of two level 1 trauma centers in Houston, Texas. Skull series of the skeletal survey included two views (anteroposterior, lateral). These skull radiographs were obtained using Siemens Ysio (Siemens Healthcare, Erlangen, Germany), Siemens Axiom Luminos TF (Siemens Healthcare, Erlangen, Germany), Philips Super 80 CP (Philips North America, Andover, MA), General Electric (GE) Precision 500D (GE Healthcare, Little Chalfont, UK), and Shimadzu MobileDart Evolution (Shimadzu Corporation, Kyoto, Japan). With these films, kVp was between 58-74.8 and mAs ranged from 1 to 5.1 depending on equipment type and image orientation. Per hospital protocol, the majority of CT images of the head were helically acquired from the craniocervical junction through the calvarial vertex with an Aquilion ONE™ 320 Toshiba (Toshiba, Tochigi-ken, Japan), utilizing a detector collimation of 0.5 and a pitch of 0.84. The remainder of the CT images were obtained using a GE LightSpeed VCT 64 slice (GE Healthcare, Little Chalfont, UK) machine through which an axial mode was used. Standard images included axial images (5-mm slices); coronal (1.3-mm slices) and sagittal (3-mm slices) images were reconstructed from the axial images. Three-dimensional reconstructions were obtained as the standard of care. These head CT images had a kVp of 120, mAs ranging from 150 to 250, and a 500-ms gantry rotation time. From this acquired data set, without additional radiation to the patient, surface-shaded 3-D volume renderings of the calvarium were obtained. These 3-D images were rotated through 360° at 15-degree intervals for viewing. Radiation associated with the two-view skull radiographs is estimated to be 0.006-0.112 millisieverts (mSv) with a mean of 0.017 and ranged from 2.6 to 5.8 mSv with an average of 4.2 mSv for CT of the head [17, 18]. In comparison, skeletal surveys are estimated to have an exposed dose of radiation of 0.2 mSv [19].
The effective dose from CT head scans was calculated from the methodology described by the American Association of Physicists in Medicine [20]. The patient-specific mAs was used to adjust the CT dose index volume (CTDIvol) measurements from the annual physics testing of the equipment. The resulting CTDIvol was multiplied by the scan range to calculate dose length product (DLP). To account for patient age, k coefficients (mSv/mGy-cm) for the head region were interpolated between the values reported for a 0-year-old (0.011) and a 1-year-old (0.0067). The product of DLP and k coefficient resulted in the reported effective dose (mSv). The effective dose from skull radiographs was calculated using CHILDOSE [21] and the International Commission on Radiological Protection (ICRP) 60 organ weighting factors [22].
All studies were reread by an attending pediatric radiologist (J.E.C. for the skull series) or by an attending pediatric neuroradiologist (J.Y.J. for the CTs). Fifty-eight percent of all studies were also read by a second radiologist (A.R.M.-R. or H.B.T.) to evaluate for interobserver reliability. In cases where there was discordance between the CT and radiograph reads, the second pair of radiologists (A.R.M.-R. and H.B.T.) also read these studies with the majority serving as the deciding interpretation of the presence or absence of fracture. The radiologists were blinded to the original interpretation of the imaging studies. The radiologists had a mean of 18 years in practice post-fellowship (range: 7-44 years). Medical record abstraction was performed for demographics and presence or absence of other injuries. Children were excluded if paired CT and skull series radiographs were unavailable; the CT was done at the referral hospital (due to concerns about quality of the imaging and because 3-D reconstruction was not commonly performed at referring facilities); imaging was obtained post operatively, or the skull radiographs and the CT were performed greater than 72 h apart.
Demographic comparisons between patients with a positive or negative skull fracture determined by head radiography were made using the Pearson chi-square test. With skull radiography as the reference standard, sensitivity, specificity, positive predictive value and negative predictive value were calculated for CT imaging results. McNemar test was utilized to statistically assess the diagnostic agreement between paired CT and skull radiograph results. Results were further stratified on age (0-3 months; 4-8 months; 9-12 months) based on expected neurodevelopment and mobility. Interobserver variation was calculated using the Cohen’s kappa coefficient. Kappa scores of 0-0.2 indicated slight agreement, 0.21-0.4 as fair, 0.41-0.6 as moderate, 0.61-0.8 as substantial and >0.8 as almost perfect agreement [23]. Statistical significance was defined as having a P-value less than 0.05. All analyses were calculated using STATA version 13 software (StataCorp LP, College Station, TX).
Results
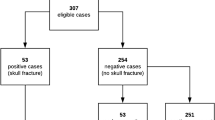
Four hundred and four infants were evaluated for non-accidental trauma during the study period, of whom 177 (43.8%) had paired CT and skull radiographs available for evaluation and met inclusion criteria (Fig. 1). The mean and median ages were both 5 months. There were statistically significant demographic differences between patients with and without a skull fracture identified by radiography (Table 1), with the majority of patients with skull fractures being Hispanic (64.5%). One-half of children with radiography-diagnosed skull fractures were in the 4- to 8-month group. Of those with fractures, 45.2% also had intracranial bleeding with the majority of those bleeds being subdural. Just less than 10% of children without fractures had intracranial bleeding (Table 1).
Sixty-two (35%) children had skull fractures identified on skull radiographs and 67 (38%) by CT (P-value = 0.18) (Table 2). There were no statistically significant differences between the radiographic findings and 3-D CT scan results among all patients and the three age groups using non-parametric testing for matched data (Table 2). Demographics of the children and radiographic findings of discordant results are presented in Table 3. Using skull radiography as the reference standard, CT with 3-D reconstruction was 97% sensitive and 94% specific for identifying skull fractures (Table 4). There were initially six children with apparent skull fractures who were misclassified by 3-D CT (e.g., CT was read as normal, an apparent false-negative CT). The six children’s imaging studies were re-reviewed in a blinded fashion by the second radiologists who originally reviewed the imaging studies for interobserver reliability. Of these 6 studies, 4 (67%) were determined to have no fracture on skull radiograph when reevaluated, showing agreement of the skull radiograph with the original CT read. Upon further review, one prominent vascular groove and one dermoid cyst seen on CT were possibly misclassified as fractures originally on the skull radiographs (Fig. 2). Conversely, there were 11 children in whom the 3-D CT demonstrated a skull fracture that was not identified on skull radiography (these would be apparent false-positive CTs). These studies were also re-reviewed by a second pair of pediatric radiologists and neuroradiologists with 4 of the 11 (37%) found to have the skull fracture confirmed on skull radiograph, showing agreement of the skull radiograph with the original CT read. Upon hospital chart review, the CT findings could be correlated to the clinical diagnosis and management of the child (Fig. 3). It is unclear why these seven fractures were not appreciated on radiography though much of the clinical documentation indicated difficulty seeing the fracture on radiography as compared to the CT. If one uses CT as the reference standard instead of skull radiography, sensitivity and specificity of skull radiography are 90% and 98%, (Table 5) respectively, with positive and negative predictive values of 97% and 94%, respectively.
A 6-month-old boy receiving a medical evaluation for macrocephaly was found to have a left frontal skull fracture noted on skull radiographs. There was no antecedent trauma. Physical examination demonstrated no soft tissue swelling or tenderness in this region. This finding was thought to be a vascular groove when evaluated with the head CT. During his hospitalization, a corresponding head ultrasound also concluded that this area of lucency had an internal vessel. a Skull radiograph identifies area of suspected fracture (arrow). b An axial slice of the CT scan shows the vascular groove (arrow). It can be seen on this image that the defect is within an intact cortex. c A view with 3-D reconstructed CT indicates the vascular groove (arrow)
A 9-month-old boy being evaluated after his parents had identified swelling to the right side of his head. He had no antecedent trauma by history. He was found to have a right parietal skull fracture identified by CT scan. The fracture was not seen on the corresponding skull radiographs. a Lateral view on skull radiograph. b Three-dimensional reconstructed CT scan image indicates a fracture (arrow)
Interobserver concordance was high in this study for CT interpretation. Overall, the concordance between the two imaging modalities was 95%. Radiologists had a Kappa score of 1 (P<0.001) for CT interpretation of skull fracture and a Kappa of 0.77 (P=0.001) for interpretation of skull radiographs.
Discussion
Our study found that there does not appear to be a loss of diagnostic yield by eliminating the skull radiographs in the evaluation of suspected head trauma when the patient will receive a head CT. A head CT will identify both fractures and intracranial injury. From a medical standpoint, operative management is rarely required for non-depressed skull fractures, but the presence of intracranial injury may alter patient management significantly. Finally, CT with 3-D reconstruction may be easier for non-specialists to interpret when real-time radiologist interpretation may be unavailable [24]. There are important ramifications to false-positive and false-negative radiographic interpretations.
Prior data suggest that CT with 3-D reconstruction may be superior to skull radiographs in identifying skull fractures in infants with suspected abusive head trauma. The former modality has enhanced sensitivity and specificity [11, 16], finding subtle fractures while also clarifying normal variants [13]. As seen in this study, when head CT with 3-D reconstruction was used in evaluating abusive head trauma, the presence or absence of skull fractures was accurately identified in more than 93% of cases. Additionally, in some cases where skull fractures were noted by the reference test (skull radiograph), it was concluded with clinical investigation as well as additional imaging studies that these suspected fractures were actually normal variants such as a vascular groove. This suggests that even skilled pediatric radiologists can have difficulty making accurate interpretations from two-view skull radiographs provided on a skeletal survey, especially in cases when a full clinical history is not provided.
Interobserver reliability was much lower for skull radiographs than for CTs of the head when interpreted by pediatric radiologists and neuroradiologists. Even with extensive training, pediatric radiologists within the same institution had only fair agreement in their evaluation of skull radiographs. With such difficulty seen in these interpretations among experts, accuracy among clinicians in emergency departments or facilities without the benefit of pediatric radiologists is concerning. It is not uncommon for pediatricians, emergency department physicians or radiology resident trainees to interpret imaging studies overnight or daily when radiology subspecialists are unavailable. In these cases, multiple factors can result in misdiagnosis: open sutures, fissures, superimposition of suture lines, rotation, motion artifact and normal variants [2, 10, 13]. These misinterpretations can result in serious repercussions in a case where abusive head trauma is a consideration. False-positive readings of skull radiographs may result in an extensive medical work-up including the involvement of Child Protective Services (CPS) without warrant. False-negative interpretations may result in a child being returned to an unsafe home environment.
Head CT with 3-D reconstruction provides multiple advantages when evaluating a child who is potentially a victim of abusive head trauma without increasing the radiation exposure to the child compared to routine CT of the head without 3-D reconstruction [13]. Clinicians can more accurately visualize fractures and their positioning on the skull, whether it crosses suture lines or is a separate fracture [13, 24]. This enables mechanism of injury provided by the family to be better evaluated to determine whether it would be plausible in causing the fracture, another important factor in deciding if CPS should be called or if further work-up is necessary. When compared with 2-D CT, 3-D reconstruction is better for evaluating sutural diastasis and requires less time for interpretation without decreasing accuracy [25]. Shorter time for interpretation in an emergency department setting also provides several advantages for the patient and for the facility providing care.
This was a retrospective cross-sectional study with limitations. This study was not powered to a statistical endpoint, as few data exist to have driven sample size calculations. Indications for why abusive head trauma evaluations were obtained were not always evident in the medical record. The majority of patients with skull fractures being Hispanic suggests the possibility of a bias in ordering skeletal surveys and initiating a work-up for abusive head trauma in this minority population [26]. The geographical diversity of our facility may also contribute to this variation. While our hospital protocol routinely used 3-D reconstruction of CT images, these findings may not be generalizable to hospitals where this approach is not standardized. In addition, our studies were interpreted by pediatric radiologists, and sensitivity of the imaging studies may differ in settings where these subspecialists are unavailable. The issue of which young children with suspected non-accidental trauma should receive central nervous system imaging remains controversial. However, in our series, 35% of infants in whom CTs were obtained had skull fractures, resulting in a number needed to treat of less than 3. Given the risks of returning a child to an unsafe environment, this is a number needed to treat that most clinicians would consider to be reasonable. The recommendation of child abuse specialists is often to obtain a CT of the head in children 0-12 months of age in whom non-accidental trauma is suspected to evaluate for occult and old injuries that would alter their clinical management and future caregiver [27, 28]. Though magnetic resonance imaging (MRI) of the brain can be considered, it is often unavailable within the time needed in the emergency room for acute management decisions.
Conclusion
Skull radiographs and 3-D reconstructed CT scans are comparable in identifying fractures in pediatric head injury secondary to suspected non-accidental trauma. In cases where there is a concern for head trauma and clinicians require CT scans to adequately access intracranial injury, skull radiographs should be eliminated from the medical work-up. This approach would spare children additional radiation and potentially decrease false-positive findings without compromising reliable findings.
References
Centers for Disease Control and Prevention (2016) Injury prevention and control: Rates of TBI-related emergency department visits by age group – United States, 2001-2010. http://www.cdc.gov/traumaticbraininjury/data/rates_ed_byage.html. Accessed 26 Oct 2015
Kleinman PK (2015) Skeletal imaging strategies. In: Kleinman PK (ed) Diagnostic imaging of child abuse, 3rd edn. Cambridge University Press, United Kingdom, pp 324–332
Kemp AM, Butler A, Morris S et al (2006) Which radiological investigations should be performed to identify fractures in suspected child abuse? Clin Radiol 61:723–736
Bajaj M, Offiah AC (2015) Imaging in suspected child abuse: necessity or radiation hazard? Arch Dis Child 100:1163–1168
Hackney DB (1991) Skull radiography in the evaluation of acute head trauma: a survey of current practice. Radiology 181:711–714
Lloyd DA, Carty H, Patterson M et al (1997) Predictive value of skull radiography for intracranial injury in children with blunt head injury. Lancet 349:821–824
Meyer JS, Gunderman R, Coley BD et al (2011) ACR appropriateness criteria on suspected physical abuse-child. J Am Coll Radiol 8:87–94
Chawla H, Yadav RK, Griwan MS et al (2015) Sensitivity and specificity of CT scan in revealing skull fracture in medico-legal head injury victims. Australas Med J 8:235–238
Chawla H, Malhotra R, Yadav RK et al (2015) Diagnostic utility of conventional radiography in head injury. J Clin Diagn Res 9:TC13–TC15
Sanchez T, Stewart D, Walvick M et al (2010) Skull fracture vs. accessory sutures: how can we tell the difference? Emerg Radiol 17:413–418
Kim Y, Cheong J, Yoon SH (2012) Clinical comparison of the predictive value of the simple skull x-ray and 3 dimensional computed tomography for skull fractures of children. J Korean Neurosurg Soc 52:528–533
Kleinman PK, Coats B, Silvera VM (2015) Abusive head trauma: scalp, subscalp, cranium. In: Kleinman PK (ed) Diagnostic imaging of child abuse, 3rd edn. Cambridge University Press, United Kingdom, pp 357–388
Parisi MT, Wiester RT, Done SL et al (2015) Three-dimensional computed tomography skull reconstructions as an aid to child abuse evaluations. Pediatr Emerg Care 31:779–786
Morrison J, Masse B, Oellet P et al (2013) Four-film X-ray series is more sensitive than 2-film for diagnosis of skull fractures in children. Pediatr Emerg Care 29:1189–1193
Chung S, Schamban N, Wypij D et al (2004) Skull radiograph interpretation of children younger than two years: how good are pediatric emergency physicians? Ann Emerg Med 43:718–722
Orman G, Wagner MW, Seeburg D et al (2015) Pediatric skull fracture diagnosis: should 3D CT reconstructions be added as routine imaging? J Neurosurg Pediatr 16:426–431
American Nuclear Society (2016) Radiation dose chart. http://www.ans.org/pi/resources/dosechart/msv.php. Accessed 27 May 2016
Slovis TL, Strouse PJ, Strauss KJ (2015) Radiation exposure in imaging of suspected child abuse: benefits versus risks. J Pediatr 167:963–968
Berger RP, Panigrahy A, Gottschalk S et al (2016) Effective radiation dose in a skeletal survey performed for suspected child abuse. J Pediatr 171:310–312
McCollough C, Cody D, Edyvean S et al (2008) The measurement, reporting, and management of radiation dose in CT. Report of AAPM Task Group 23. 23:1–28
Hart D, Jones DG, Wall BF (1996) NRPB-R279 coefficients for estimating effective doses from paediatric X-ray examinations. National Radiological Protection Board, Great Britain
International Committee on Radiation Protection (1991) 1990 Recommendations of the International Commission on Radiological Protection. ICRP Publication 60; Ann. ICRP 21:1-3. Pergamon Press, Oxford
Lantz CA, Nebenzahl E (1996) Behavior and interpretation of the kappa statistic: resolution of the two paradoxes. J Clin Epidemiol 49:431–434
Prabhu SP, Newton AW, Perez-Rossello JM et al (2013) Three-dimensional skull models as a problem-solving tool in suspected child abuse. Pediatr Radiol 43:575–581
Dundamadappa SK, Thangasmy S, Resteghini N et al (2015) Skull fractures in pediatric patients on computerized tomogram: comparison between routing bone window images and 3D volume-rendered images. Emerg Radiol 22:367–372
Wood JN, Feudtner C, Medina SP et al (2012) Variation in occult injury screening for children with suspected abuse in selected US children’s hospitals. Pediatrics 130:853–860
Meyer JS, Gunderman R, Coley BD et al (2011) Expert panel on pediatric imaging: ACR appropriateness criteria for suspected physical abuse – child. J Am Coll Radiol 8:87–94
Flaherty EG, Perez-Rosello JM, Levine MA et al (2014) Evaluating children with fractures for child physical abuse. Pediatrics 133:e477–e489
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Culotta, P.A., Crowe, J.E., Tran, QA. et al. Performance of computed tomography of the head to evaluate for skull fractures in infants with suspected non-accidental trauma. Pediatr Radiol 47, 74–81 (2017). https://doi.org/10.1007/s00247-016-3707-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-016-3707-7