Abstract
Introduction and hypothesis
The aims of this study were to evaluate the prevalence of levator ani muscle (LAM) avulsions in a selected cohort of patients with primary anterior compartment pelvic organ prolapse (POP) and to assess whether LAM avulsions, as an independent factor, affect the degree of POP symptoms and sexual dysfunction. Additionally, clinical and demographic variables of women with and those without avulsions were compared.
Methods
We carried out a cross-sectional analysis of a prospective cohort study including 197 women scheduled for anterior compartment POP surgery. LAM avulsions were diagnosed on transperineal 4D ultrasound. Preoperative symptom severity and sexual dysfunction were evaluated using validated questionnaires (Pelvic Floor Disability Index [PFDI-20] and Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire-Short Form 12 [PISQ-12]). Linear regression was performed with avulsion as the main independent variable against total PFDI-20 and domain scores, bulge symptoms, and PISQ-12 score. Clinical and demographic variables for women with and without avulsions were compared using independent samples t test, Mann–Whitney U test or Chi-squared test.
Results
The prevalence of LAM avulsions was 50.3%. Avulsions were not associated with symptom severity or sexual dysfunction. “Chronic disease causing pain, fatigue or increased intra-abdominal pressure” was the only independent factor associated with all domains of the PFDI-20. Women with avulsions were younger at presentation, older at their first delivery, had lower BMI, and more often had a history of forceps delivery (p < 0.01).
Conclusions
LAM avulsions were highly prevalent in this preoperative POP cohort. Avulsions were not associated with the severity of POP symptoms or sexual dysfunction. Women with avulsions seem to require fewer additional cofactors for developing POP.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pelvic organ prolapse (POP) has a deleterious impact on the quality of life for a large proportion of women worldwide, with a reported prevalence ranging from 2.9 to 50%, depending on definitions and population groups [1, 2]. The most common form of POP is a defect in the anterior compartment [3]. The development of POP in women is multifactorial, with recognized risk factors being age, obesity, chronic constipation, and above all, vaginal childbirth [4]. If the vaginal delivery causes a major injury to the levator ani muscle (LAM), known as LAM avulsion, the risk of developing POP, particularly in the anterior and mid-compartments, is doubled [5]. LAM avulsions are defined as the detachment of the pubic portion of the most medial part of the LAM from its normal site of insertion at the anterior pubic ramus [6]. Minor levator injuries do not have the same impact on pelvic floor function [7]; thus, the term avulsion is generally reserved for major injuries. The avulsions may be uni- or bilateral [8]. Levator avulsions have been described in 13–20% of women after their first vaginal delivery [8, 9] and an increased risk has been suggested for forceps deliveries and older age at first delivery [9, 10].
Previous studies have indicated that surgeries for POP in women with LAM avulsions are less successful than in women without avulsions owing to a significantly higher risk of recurrence [11]. Therefore, some authors suggest that women with avulsions need a different surgical approach to POP repair than women with intact LAM [11]. For that reason, it is important to identify women with LAM avulsions among patients scheduled for POP surgery to give these women proper counseling before surgery.
As LAM avulsion has been shown to exert an independent impact on pelvic floor symptoms in women 3 months postpartum [12, 13], we wanted to investigate whether that also holds true for women seeking surgical treatment for symptomatic POP.
The aims of the present study were firstly to evaluate the prevalence of LAM avulsions in a cohort of women scheduled for primary surgery for anterior compartment POP and to assess whether avulsions exert an independent impact on the severity of POP symptoms and sexual dysfunction in such a population. The secondary aim of the study was to compare clinical and demographic differences in women with and those without LAM avulsions.
Materials and methods
The present study was a cross-sectional analysis of an ongoing prospective cohort study (clinical trial number NCT 02246387) evaluating anatomical outcomes in women scheduled for surgical correction of anterior compartment prolapse at the Department of Gynecology, Oslo University Hospital, Norway, between October 2014 and June 2016.
Women scheduled for POP surgery due to symptomatic prolapse with a dominating anterior compartment defect and who understood Norwegian or English were offered inclusion. Exclusion criteria were previous POP surgery or previous hysterectomy (total/subtotal). Patients were approached for study enrollment after the decision on surgery had been made. Signed, informed consent was obtained. The study was approved by the Regional Ethics Committee for the South Eastern Region of Norway (reference 2013/2093).
All women had a standardized interview, including clinical and obstetric antecedents. They were objectively assessed using Pelvic Organ Prolapse Quantification (POP-Q) measurements [14], and using 4D transperineal ultrasound. The first author (SO) obtained ultrasound volumes at rest and at maximal pelvic floor muscle contraction using a GE Voluson S8 with a 4- to 8-MHz 4D abdominal probe. Tomographic ultrasound imaging (TUI) with 2.5-mm steps from 5 mm below the plane of minimal dimensions to 12.5 mm above this plane was performed to diagnose uni- and bilateral total LAM avulsions. Only major avulsions were considered [7, 9].
The diagnosis was confirmed off-line, on a desktop computer using 4D View (GE Healthcare, Zipf, Austria). An intra- and inter-rater validation process for the diagnosis of uni- and bilateral levator avulsions was performed a minimum of 3 months after the initial examination. Fifty randomly selected cases were re-examined by both the primary investigator (SO) and an external evaluator (IV). The randomization and renumbering for the re-evaluation of the tomographic images was performed by a third person (RS) using the SPSS randomization function to ensure blinding of both ultrasound image interpreters. Inter- and intra-observer reliabilities were determined using Cohen’s Kappa.
Preoperatively, the women were asked to fill out two validated short form questionnaires. The Pelvic Floor Distress Inventory-Short Form 20 (PFDI-20), consists of three domains (Pelvic Organ Prolapse Distress Inventory 6 [POPDI-6], Colorectal Anal Distress Inventory 8 [CRADI-8], and Urogenital Distress Inventory 6 [UDI-6]), whereas the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire-Short Form 12 (PISQ-12) is treated as a total score [15, 16]. The questionnaires were translated into Norwegian from the linguistically similar validated Swedish versions [17], as none of them had been validated in Norwegian before the start of the study. For women not fluent in Norwegian, but who spoke and understood English, the English versions of the questionnaires were offered [15, 16]. Missing values were accounted for as indicated in the original papers [15, 16]. Symptom scores were treated as continuous variables in the final analyses.
Sample size was originally estimated for the ongoing prospective study on postoperative anatomical outcome. However, a post-study power analysis for this cross-sectional study was performed with an 80% test power and a 5% significance level, supposing a 50% prevalence of LAM avulsion and proposing a difference in Pelvic Floor Disability Index (PFDI-20) outcome of 25 to be clinically relevant (one point increase in mean score of one of the domains). With a SD of 55 (from our own data), the necessary sample size was 152. We included 197 women in our study (see below in the Results section); thus, the test power should be appropriate.
To evaluate the impact of LAM avulsions on symptom severity and sexual function, linear regression analyses were performed. The outcome variables analyzed were the following: total PISQ-12 score, total and domain PFDI-20 scores in addition to the single question: “Do you usually have a bulge or something falling out that you can see or feel in the vaginal area?” (question 3, POPDI-6). The latter question was tested because others have identified the single symptom of a bulge to be the one most strongly correlated with POP severity [18].
Spearman’s correlation was used to analyze independent variables against the above outcomes to identify which factors, in addition to LAM avulsion (the main independent factor), to include in the linear regression analysis. The variables tested were: age, BMI, POP-Q stage of the anterior compartment, parity, previous vacuum delivery, previous forceps delivery, sexual activity, use of local estrogen, in addition to chronic disease causing pain, fatigue or increased intra-abdominal pressure. The latter, represented by entities such as fibromyalgia, chronic fatigue syndrome, irritable bowel syndrome or chronic obstructive lung syndrome, was included as an independent variable because others have found such conditions to correlate closely with pelvic pain [19]. Assumptions for linear regression analyses were adequately met. For each linear regression model, only variables with a p value below 0.1 using Spearman’s correlation were included, in addition to LAM avulsion.
Differences in clinical and demographic variables were tested between women with LAM avulsions and those with intact LAM. Independent samples t test was used when adequate; otherwise, Mann–Whitney U test was used. Pearson’s Chi-squared test was used for categorical variables. Additional analyses were also performed comparing women with unilateral avulsions with those with no avulsions and women with bilateral avulsions with those with no avulsions.
A p value <0.05 was considered statistically significant. The analyses were performed using SPSS version 24.
Results
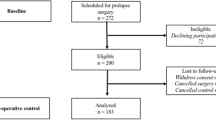
The final study population consisted of 197 women (Fig. 1) 98.5% of whom were of European origin. Mean age was 61 years (SD 12, range 34–86) and mean BMI was 24.9 (SD 3.5, range 17.5–39.4). Systemic estrogen was used by 6.6% and local vaginal estrogen by 43.7%. Median parity was 2 (range 0–7). Six women (3%) were nulliparous; the remaining 97% had undergone at least one vaginal delivery. Of the women having had a minimum of one vaginal delivery, 16.8% (n = 191) had undergone at least one forceps delivery and 5.2% (n = 191) at least one vacuum delivery. Two women had experienced both forceps and vacuum deliveries. For both women, the forceps delivery was performed before the vacuum delivery; thus, they were classified within the forceps group. Mean age at first delivery was 26 years (SD 5.2, range 17–41). Symptom scores were distributed as follows: PFDI-20—mean 102.4 (SD 50.8) and median 99.0 (range 4.2–264.6); POPDI-6—mean 45.7 (SD 21.7) and median 45.8 (range 0–100.0); CRADI-8—mean 22.3 (SD 19.1) and median 18.8 (range 0–81.3); UDI-6—mean 34.3 (SD 22.5) and median 29.2 (range 0–100.0); PISQ-12—mean 14.1 (SD 7.0) and median 14.0 (range 0–32.0).
A total of 39 women in whom primary POP surgery was planned were not included, either because of insufficient Norwegian/English skills or due to missed/denied inclusion (Fig. 1). These women did not differ significantly from the study population regarding age or stage of prolapse in the anterior compartment, but they had a significantly higher BMI (mean 26.9 vs 24.9; p = 0.02).
The prevalence of LAM avulsions was 50.3% (n = 197). Unilateral avulsions were seen in 18.8%, whereas bilateral avulsions were seen in 31.5%. The inter-rater Cohen’s Kappa was 0.82 and the intra-rater Cohen’s Kappa was 0.80 for the diagnosis of LAM avulsion on transperineal ultrasound.
Only “chronic disease causing pain, fatigue or increased intra-abdominal pressure” was significantly associated with all domains of the PFDI-20 symptoms score (p < 0.05), using Spearman’s correlation. Increasing POP-Q stage in the anterior compartment was significantly associated with CRADI-8 (p < 0.05) and the total PFDI-20 score (p < 0.05), whereas parity was significantly associated with UDI-6 score (p < 0.01). None of the clinical and demographic variables were significantly associated with the PISQ-12 score.
In addition to LAM avulsion (main independent variable), variables with p < 0.1 from Spearman’s correlation analyses were entered into the multivariate linear regression model. Table 1 presents the adjusted impact of the independent variables on symptoms scores when using multivariate linear regression analyses.
In the multivariate analyses, LAM avulsion was not significantly associated with any of the outcomes. Nor did testing unilateral and bilateral avulsions separately against the outcomes uncover any significant associations (data not shown). “Chronic disease causing pain, fatigue or increased intra-abdominal pressure” remained significantly associated with all three domain sub-scores of the PFDI-20 and with the total PFDI-20 score (Table 1). Parity remained significantly associated with the total PFDI-20 score and the UDI-6 sub-score, and age was the only factor associated with sexual symptoms (Table 1).
Figure 2 depicts the distribution of total PFDI-20 scores among women with and those without avulsions, illustrating almost identical distributions of subjective pelvic floor distress scores.
Clinical and demographic data for women with and those without LAM avulsions are presented in Table 2. When compared with women without avulsions, those with avulsions were significantly younger at presentation, had a significantly lower BMI, and were significantly older when they gave birth to their first child. Moreover, they had a forceps delivery significantly more often.
Discussion
In our population of women seeking primary surgery for anterior compartment POP, the prevalence of LAM avulsion was 50.3%, at the upper end of the rates previously reported from urogynecological patient populations [20]. A likely explanation is that women in the present study have more severe prolapse and were scheduled for surgery for this condition. Previous studies have found a clear association between LAM avulsions and more severe pelvic floor symptoms 3 months postpartum [12, 13], but such an independent impact of avulsions on the severity of symptoms was not seen in our cohort. The lack of association between avulsions and POP symptom bother has also been indicated in another study; however, this was retrospective and in a heterogeneous urogynecological population [21]. It is plausible that the impact of LAM avulsions on pelvic floor symptoms in the immediate postpartum period is greater because of the more extensive acute vaginal trauma with additional damage to nerves, fascia, and connective tissue that to some extent may be partly reversible with healing and reconstruction over time. A more likely explanation is that that any association between LAM avulsions and POP symptoms could be masked by the fact that all our patients had POP symptoms severe enough to warrant surgical intervention. Some studies have identified that stage of POP alone is associated with the severity of symptoms [22].
This study found that the only significant factor that had an impact on all the domains of pelvic floor symptoms was “chronic disease causing pain, fatigue or increased intra-abdominal pressure” (detailed as fibromyalgia, irritable bowel syndrome, chronic obstructive lung disease, etc.). Bump and Norton named some of these chronic conditions “promoting factors” in the natural history of POP development [23], potentially because women with a symptomatic chronic condition have more severe baseline symptoms and thus a lower threshold for seeking medical evaluation for any additional increase in symptom intensity. An association between chronic diseases and sexual function has not been identified to the same extent as for POP symptoms, although poor physical condition has been shown in a study by Laumann et al. to be a risk factor for sexual impairment [24]. In our study of women with symptomatic POP, older age was the only factor associated with preoperative sexual dysfunction.
There are many factors that contribute to sexual dysfunction in POP patients, it is known that many aspects are involved, not just pain, discomfort, and dyspareunia, but also psychological factors, such as embarrassment and reduced libido [25]. The cohort selection may have impeded the possibility of identifying any separate impact from LAM avulsions, as the effect from the stage of prolapse alone may have diluted any impact from the avulsions.
The present study supports acknowledged risk factors for major pelvic floor trauma causing LAM avulsions, such as forceps delivery [9] and older age at first delivery [10], as these were significantly more prevalent among women with avulsions. Although forceps delivery is the most widely accepted risk factor for LAM avulsions, our study indicates that the association between older age at first delivery and avulsions is equally strong. As postulated by others, this may be because older age at first delivery exerts an independent impact on the development of POP, regardless of LAM avulsion [26], possibly because the pelvic floor in older women is less elastic and thus more vulnerable to the delivery-related trauma of nerves, connective tissue, and muscles [11].
High BMI is a commonly accepted risk factor for POP [2]. We found, however, that women with LAM avulsions in this cohort had a significantly lower BMI than women with intact LAM. This supports the notion of women with a fragile, injured LAM needing fewer additional risk factors to develop POP owing to the importance of the LAM for normal pelvic floor function.
In our study, women with avulsions were significantly younger when they presented for POP-related symptoms than women without avulsions, indicating that the time gap between pelvic floor trauma and symptoms is narrowed by the muscle injury per se and not only because women with LAM avulsions gave birth closer to the menopause. Thomas et al. describe a similar association between forceps delivery (causing vaginal trauma) and POP presentation [26]. These findings imply that women with LAM avulsions require fewer additional risk factors to develop symptomatic POP with a need for surgery.
As women with LAM avulsions tend to develop symptomatic POP at a younger age and are possibly at a higher risk of postoperative symptomatic recurrence [11], special surgical methods have been proposed for LAM reconstruction [27]. However, it is not generally acceptable to perform such surgeries (with the inherent risk of unsuccessful postoperative results) in asymptomatic women with avulsions to prevent possible future pelvic floor symptomatology. The main prevention therefore relies on avoiding LAM injury during delivery. In obstetrics, attention has been paid to preventing obstetric anal sphincter injuries by manually slowing the delivery of the infant’s head [28]. A similar focus must be placed on the prevention of levator injuries, while optimizing short- and long-term outcomes for mother and child. Such increased awareness of prevention has reduced the incidence of anal sphincter injuries in Norway over the last decade [28] and it is plausible that the same reduction can be achieved for levator avulsions.
The main strengths of the present study are a clinically well-described population and an adequate sample size. We compared groups of women with and without LAM avulsions of equal size. The calculated inter- and intra-rater reliabilities for ultrasound diagnosis of avulsions were excellent (Cohen’s Kappa values of 0.82 and 0.80 respectively for inter-rater and intra-rater reliability). We were not able to find any information in previous publications on how to dichotomize PFDI-20 and PISQ-12 symptom scores in POP patients; thus, the scores were treated as continuous variables. However, the mean and median symptom scores from the present study may help dichotomization into low/high scores for POP patients in future studies.
The study questionnaires were translations from the validated Swedish versions (Sweden being similar linguistically and socioculturally), implying potential misinterpretations. The PISQ-12 questionnaire on sexual symptoms is only validated for sexually active women in heterosexual relationships; therefore, important information on sexual symptoms in homosexual or “sexually inactive” women could have been lost. Moreover, the expression of sexual symptoms may also vary according to ethnicity [29]; thus, our population of mainly women of European heritage may not be representative of other populations. However, ethnicity has not previously been demonstrated to have an important impact on pelvic floor symptoms [30].
In conclusion, our study confirms a high prevalence of LAM avulsions in women with predominant anterior compartment prolapse who were scheduled for surgical intervention. Levator avulsions seem to shorten the time gap between the inciting vaginal birth and symptomatic POP, but do not seem to have an impact on the severity of pelvic floor symptoms or sexual dysfunction. Moreover, our study indicates that older age at first delivery and forceps delivery increase the risk of avulsions, which implies that special care must be taken to avoid major obstetric vaginal trauma, especially in older primiparas.
References
Nygaard I, Barber MD, Burgio KL, Kenton K, Meikle S, Schaffer J, et al. Pelvic Floor Disorders Network. Prevalence of symptomatic pelvic floor disorders in US women. JAMA. 2008;300(11):1311–6. doi:10.1001/jama.300.11.1311.
Awwad J, Sayegh R, Yeretzian J, Deeb ME. Prevalence, risk factors, and predictors of pelvic organ prolapse: a community-based study. Menopause. 2012;19(11):1235–41. doi:10.1097/gme.0b013e31826d2d94.
Hendrix SL, Clark A, Nygaard I, Aragaki A, Barnabei V, McTiernan A. Pelvic organ prolapse in the Women’s Health Initiative: gravity and gravidity. Am J Obstet Gynecol. 2002;186(6):1160–6.
Hallock JL, Handa VL. The epidemiology of pelvic floor disorders and childbirth: an update. Obstet Gynecol Clin N Am. 2016;43(1):1–13. doi:10.1016/j.ogc.2015.10.008.
Dietz HP, Simpson JM. Levator trauma is associated with pelvic organ prolapse. BJOG. 2008;115(8):979–84. doi:10.1111/j.1471-0528.2008.01751.x.
DeLancey JOL, Sorensen HC, Lewicky-Gaupp C, Smith TM. Comparison of the puborectal muscle on MRI in women with POP and levator ani defects with those with normal support and no defect. Int Urogynecol J. 2012;23(1):73–7. doi:10.1007/s00192-011-1527-8.
Dietz HP, Bernardo MJ, Kirby A, Shek KL. Minimal criteria for the diagnosis of avulsion of the puborectalis muscle by tomographic ultrasound. Int Urogynecol J. 2011;22(6):699–704. doi:10.1007/s00192-010-1329-4.
DeLancey JOL, Kearney R, Chou Q, Speights S, Binno S. The appearance of levator ani muscle abnormalities in magnetic resonance images after vaginal delivery. Obstet Gynecol. 2003;101(1):46–53. doi:10.1016/S0029-7844(02)02465-1.
Shek KL, Dietz HP. Intrapartum risk factors for levator trauma. BJOG. 2010;117(12):1485–92. doi:10.1111/j.1471-0528.2010.02704.x.
Rahmanou P, Caudwell-Hall J, Atan IK, Dietz HP. The association between maternal age at first delivery and risk of obstetric trauma. Am J Obstet Gynecol. 2016;215(4):451.e1–7. doi:10.1016/j.ajog.2016.04.032.
Dietz HP, Chantarasorn V, Shek KL. Levator avulsion is a risk factor for cystocele recurrence. Ultrasound Obst Gynecol. 2010;36(1):76–80. doi:10.1002/uog.7678.
Cyr MP, Kruger J, Wong V, Dumoulin C, Girard I, Morin M. Pelvic floor morphometry and function in women with and without puborectalis avulsion in the early postpartum period. Am J Obstet Gynecol. 2016;216(3):274.e1–8 doi:10.1016/j.ajog.2016.11.1049.
Van Delft K, Sultan AH, Thakar R, Schwertner-Tiepelmann N, Kluivers K. The relationship between postpartum levator ani muscle avulsion and signs and symptoms of pelvic floor dysfunction. BJOG. 2014;121(9):1164–1171; discussion 1172. doi:10.1111/1471-0528.12666.
Haylen BT, Maher CF, Barber MD, Camargo S, Dandolu V, Digesu A, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Neurourol Urodyn. 2016;35(2):137–68; doi:10.1002/nau.22922.
Barber MD, Walters MD, Bump RC. Short forms of two condition-specific quality-of-life questionnaires for women with pelvic floor disorders (PFDI-20 and PFIQ-7). Am J Obstet Gynecol. 2005;193(1):103–13. doi:10.1016/j.ajog.2004.12.025.
Rogers RG, Coates KW, Kammerer-Doak D, Khalsa S, Qualls C. A short form of the pelvic organ prolapse/urinary incontinence sexual questionnaire (PISQ-12). Int Urogynecol J Pelvic Floor Dysfunct. 2003;14(3):164–168; discussion 168. doi:10.1007/s00192-003-1063-2.
Teleman P, Stenzelius K, Iorizzo L, Jakobsson U. Validation of the Swedish short forms of the pelvic floor impact questionnaire (PFIQ-7), pelvic floor distress inventory (PFDI-20) and pelvic organ prolapse/urinary incontinence sexual questionnaire (PISQ-12). Acta Obstet Gynecol Scand. 2011;90(5):483–7. doi:10.1111/j.1600-0412.2011.01085.x.
Ghetti C, Gregory WT, Edwards SR, Otto LN, Clark AL. Pelvic organ descent and symptoms of pelvic floor disorders. Am J Obstet Gynecol. 2005;193(1):53–7. doi:10.1016/j.ajog.2004.12.004.
Yosef A, Allaire C, Williams C, Ahmed AG, Al-Hussaini T, Abdellah MS, et al. Multifactorial contributors to the severity of chronic pelvic pain in women. Am J Obstet Gynecol. 2016;215(6):760.e1–14. doi:10.1016/j.ajog.2016.07.023.
DeLancey JOL, Morgan DM, Fenner DE, Kearney R, Guire K, Miller JM, et al. Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obstet Gynecol. 2007;109(2):295–302. doi:10.1097/01.AOG.0000250901.57095.ba.
Endress E, Shek KL, Dietz HP. Levator avulsion is not associated with symptom bother of female pelvic organ prolapse. Arch Gynecol Obstet. 2015;292(3):629–33. doi:10.1007/s00404-015-3633-1.
Ellerkmann RM, Cundiff GW, Melick CF, Nihira MA, Leffler K, Bent AE. Correlation of symptoms with location and severity of pelvic organ prolapse. Am J Obstet Gynecol. 2001;185(6):1332–1337; discussion 1337-1338. doi:10.1067/mob.2001.119078.
Bump RC, Norton PA. Epidemiology and natural history of pelvic floor dysfunction. Obstet Gynecol Clin N Am. 1998;25(4):723–46. doi:10.1016/S0889-8545(05)70039-5.
Laumann EO, Paik A, Rosen RC. Sexual dysfunction in the United States: prevalence and predictors. JAMA. 1999;281(6):537–44.
Rantell A, Srikrishna S, Robinson D. Assessment of the impact of urogenital prolapse on sexual dysfunction. Maturitas. 2016;92:56–60. doi:10.1016/j.maturitas.2016.07.001.
Thomas V, Shek KL, Guzman Rojas R, Dietz HP. Temporal latency between pelvic floor trauma and presentation for prolapse surgery: a retrospective observational study. Int Urogynecol J. 2015;26(8):1185–9. doi:10.1007/s00192-015-2677-x.
Rostaminia G, Shobeiri SA, Quiroz LH. Surgical repair of bilateral levator ani muscles with ultrasound guidance. Int Urogynecol J. 2013;24(7):1237–9. doi:10.1007/s00192-012-1912-y.
Laine K, Rotvold W, Staff AC. Are obstetric anal sphincter ruptures preventable? Large and consistent rupture rate variations between the Nordic countries and between delivery units in Norway. Acta Obstet Gynecol Scand. 2013;92(1):94–100. doi:10.1111/aogs.12024.
Atallah S, Johnson-Agbakwu C, Rosenbaum T, Abdo C, Byers ES, Graham C, et al. Ethical and sociocultural aspects of sexual function and dysfunction in both sexes. J Sex Med. 2016;13(4):591–606. doi:10.1016/j.jsxm.2016.01.021.
Dessie SG, Adams SR, Modest AM, Hacker MR, Elkadry EA. Bladder symptoms and attitudes in an ethnically diverse population. Female Pelvic Med Reconstr Surg. 2016;22(1):37–42. doi:10.1097/spv.0000000000000213.
Acknowledgements
We are grateful to the patients and staff at the Gynecological Department at Oslo University Hospital, who willingly contributed to this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Financial disclaimer
R. Svenningsen is on the advisory board for and receives speaker fees from Astellas.
Funding
Funded by the institution.
Conflicts of interest
None.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Oversand, S.H., Staff, A.C., Sandvik, L. et al. Levator ani defects and the severity of symptoms in women with anterior compartment pelvic organ prolapse. Int Urogynecol J 29, 63–69 (2018). https://doi.org/10.1007/s00192-017-3390-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-017-3390-8