Abstract
Purpose
Studies regarding the best strategy to determine appropriate femoral component rotation during bilateral total knee arthroplasty (TKA) in wind swept deformities (WSD) are very limited. The purpose of this study was (1) to evaluate whether femoral rotational profiles differ between varus and valgus osteoarthritic knees in WSD and (2) to analyze the correlation between femoral rotational profiles and coronal radiologic parameters.
Methods
A total of 40 patients who were diagnosed with bilateral knee osteoarthritis with WSD between January 2010 and December 2020 at a single institution were retrospectively reviewed. On axial computed tomography scans, femoral rotational profile parameters such as the clinical transepicondylar axis (cTEA) and anterior–posterior (AP) axis were compared between valgus and varus osteoarthritic knees. In standing full-limb AP radiographs, coronal radiographic parameters including hip–knee–ankle angle (HKA), valgus correction angle (VCA), lateral distal femoral angle (LDFA), medial proximal tibial angle (MPTA), and joint line convergence angle (JLCA) were measured in both knees. The correlation between the varus-valgus cTEA difference, and differences in coronal radiologic parameters was analyzed.
Results
In valgus osteoarthritic knees, cTEA was significantly increased compared to varus osteoarthritic knees by 1.5° (valgus: 7.65° ± 1.82°, varus: 6.15° ± 1.58°, p < 0.001). All coronal radiologic parameters, including HKA, LDFA, MPTA, JLCA, and VCA, were significantly different between valgus and varus knees. In correlation analysis, the varus-valgus cTEA difference was significantly correlated with LDFA (r = 0.365, p = 0.021), MPTA (r = 0.442, p = 0.004), and HKA differences (r = 0.693, p < 0.001), with the HKA difference showing the strongest correlation with the cTEA difference.
Conclusion
In bilateral knee osteoarthritis with WSD, valgus knees showed significantly increased cTEA compared to varus knees, and the cTEA difference positively correlated with the HKA difference between valgus and varus knees. To determine the optimal femoral component rotation during TKA in WSD, assessment of cTEA with pre-operative CT scans or careful intra-operative measurement is recommended, especially in patients with large HKA difference.
Level of evidence
III, Retrospective cohort study.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Windswept deformity (WSD) is defined by the presence of varus deformity in one knee and valgus deformity in the contralateral knee [14, 20]. Advanced bilateral knee osteoarthritis with WSD is a very rare condition and may require different surgical strategies for the varus and valgus knees to achieve appropriate coronal and rotational alignment of the femoral and tibial components [1, 2, 11, 13, 15, 18].
Previous studies referring to bilateral total knee arthroplasty (TKA) in WSD reported that the clinical outcomes of TKA in WSD were comparable to those of usual bilateral TKAs [3, 8, 14, 21], and stressed the importance of individualization of the valgus correction angles (VCAs) between the two knees [19]. However, studies of femoral rotational profiles in WSD are very limited.
It is known that the clinical transepicondylar axis (cTEA) can be rotated more externally in a valgus knee than in a varus knee due to lateral condylar hypoplasia [12, 16, 17], and that it correlates with coronal limb alignment [4]. However, considering that the right and left knees are viewed to be morphologically similar in various aspects [5, 6, 10], it is not clear whether varied cTEA can be observed in simultaneous varus and valgus deformities such as in WSD.
Therefore, the purpose of this study was to (1) evaluate whether femoral rotational profiles differ between varus and valgus osteoarthritic knees in WSD and (2) to determine the correlation between femoral rotational profiles and coronal radiologic parameters. It was hypothesized that valgus knees in WSD would show more externally rotated cTEA than varus knees, and that the cTEA difference would correlate with the varus-valgus difference in hip–knee–ankle angle (HKA).
Materials and methods
Study subjects
The data of 67 patients who were diagnosed with bilateral knee osteoarthritis with WSD from January 2010 to December 2020 in a single institution were retrospectively reviewed. Patients who had undergone standing full-lower limb anteroposterior (AP) radiographs read as ‘windswept deformity’ or ‘varus and valgus’ were included. The inclusion criteria were as follows: (1) HKA > 2° on the varus knee and HKA < − 2° on the valgus knee [9] (varus alignment was assigned a positive value), (2) presence of standing full-lower limb radiographs taken with proper lower extremity rotation (patella facing forward), (3) Kellgren–Lawrence (KL)-grade III or IV, and 4) presence of computed tomography (CT) knee scans. Of the 67 patients, 40 patients (80 knees) met this criterion (Fig. 1). The mean patient (37 women and three men) age was 73.15 years ± 7.13 years (range 55–84 years). Patient demographic data and KL grades for each knee are summarized in Table 1. There was no difference in KL grades between varus and valgus knees.
Radiographic studies
Knee CT scans were obtained using a standard 256-slice multi-detector CT (Ingenuity CT elite, Philips Healthcare, Best, The Netherlands) in a fully extended position. Standing full-lower limb AP radiographs were obtained with patella facing forward. To control the rotational position of the AP radiograph, the foot rotation angle was held constant with a reference foot template on the platform of our plane radiographic system. All radiographic images were digitally acquired and processed using a picture archiving and communication system (PACS) with a minimum measuring angle of 0.01° and length of 0.01 mm.
Radiographic parameters
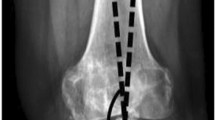
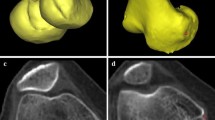
To analyze the condylar twisting of distal femur, the cTEA, defined as the line connecting the peak of both epicondyles, was evaluated rather than surgical TEA. The AP axis was defined as the line connecting the deepest part of the trochlear groove to the top of the femoral notch. The femoral rotational profiles were evaluated by measuring the cTEA angle (the angle between the cTEA and posterior condylar axis [PCA]), AP axis angle (the angle between the line perpendicular to the AP axis and PCA), and lateral angle (the angle between the cTEA and the AP axis) on the axial CT images with the most prominent epicondyles [13] (Figs. 2E and 3). External rotation (ER) was considered positive for both TEA angles.
Radiographic measurements of rotational and coronal parameters. A The hip–knee–ankle (HKA) angle is the angle between the mechanical axis of the tibia and the femur. The valgus correction angle (VCA) is the angle between the mechanical and anatomical axes of the femur. B The lateral distal femoral angle (LDFA) is defined as the lateral angle between the femoral mechanical axis and the tangent of the distal femur. C The medial proximal tibial angle (MPTA) is the medial angle between the tibial mechanical axis and the tangent of the proximal tibia. D The joint line convergence angle (JLCA) is the angle between a line tangential to the distal femoral condyle and the tibial plateau. E cTEA angle is the angle between the cTEA and PCA
To analyze the geometry of the distal femur and determine whether lateral condylar hypoplasia was differentially prominent between the varus and valgus sides in WSD, AP dimensions of both the medial and lateral femoral condyles were measured on axial CT scans [13] (Fig. 3). The AP dimension of the anteromedial, anterolateral, posteromedial, and posterolateral condyles was defined as the distance from the most anterior/posterior point of the respective condyle to cTEA.
The coronal alignment was evaluated by measuring the HKA, valgus correction angle (VCA), lateral distal femoral angle (LDFA), medial proximal tibial angle (MPTA), and joint line convergence angle (JLCA) in standing full-lower limb AP radiographs. The HKA was defined as the angle between the mechanical axis of the tibia and the femur (Fig. 2A). A positive value was given to varus knees. VCA was defined as the angle between the mechanical and anatomical axes of the femur (Fig. 2A). LDFA was defined as the lateral angle between the femoral mechanical axis and the tangent of the distal femur (Fig. 2B). MPTA was defined as the medial angle between the tibial mechanical axis and the tangent of the proximal tibia (Fig. 2C). JLCA was defined as the angle between a line tangential to the distal femoral condyle and the tibial plateau (Fig. 2D). Varus alignment was assigned a positive value.
To assess inter-observer reliability, two orthopedic surgeons independently measured the radiographic parameters. For intra-observer reliability, radiologic parameters were re-measured twice at 3-week intervals by each examiner. The intra-class correlation (ICC) for both the inter-observer and intra-observer reliability was > 0.8, indicating that the measurements were highly reliable (Table 2).
Statistical analysis
The post hoc power analysis, using the cTEA as primary outcome (varus knee, mean 6.15, SD 1.58; valgus knee, mean 7.65, SD 1.82), yielded a statistical power of over 80% for our selected number of patients (G*Power 3.1.0). Statistical analysis was performed using SPSS (version 26.0; IBM). Student’s t test was used to compare rotational profiles, AP condylar dimensions, and coronal radiologic parameters between varus and valgus osteoarthritic knees in WSD. Pearson’s correlation analysis was used to analyze the correlation between differences in femoral rotational alignments (cTEA), and differences in coronal alignments (HKA, LDFA, and MPTA). The Chi-square test was used to evaluate the severity of osteoarthritis in both knee joints. The level of significance was set at p < 0.05.
Results
In valgus knees, the cTEA angle was significantly increased compared to varus knees by 1.5° [valgus: 7.65° ± 1.82°(range 4.02°–12.15°), varus: 6.15° ± 1.58° (range 3.51°–9.53°), p < 0.001]. Except for the cTEA angle, other rotational profiles and the AP dimensions of the femoral condyle were not significantly different between the varus and valgus sides (Table 3).
In coronal alignment, valgus knees showed significantly decreased VCA (varus: 6.15. ± 1.05°, valgus: 5.13° ± 1.16°, p < 0.001), and LDFA (varus: 87.91. ± 2.35°, valgus: 85.55 ± 2.39°, p < 0.001) compared to varus knees. On the other hand, varus knees showed significantly increased JLCA (varus: 4.52° ± 2.42°, valgus: − 1.65 ± 3.40°, p < 0.001), and decreased MPTA (varus: 85.42 ± 2.87°, valgus: 89.13 ± 2.24°, p < 0.001) compared to valgus knees (Table 4).
In correlation analysis, the cTEA difference between valgus and varus knees was significantly related to the LDFA difference (r = 0.365, p = 0.021), MPTA difference (r = 0.442, p = 0.004), and HKA difference (r = 0.693, p < 0.001). The greater the difference in coronal deformation between the varus and valgus knees, the greater the difference in rotational alignment. Furthermore, the HKA difference showed the strongest correlation with the cTEA difference (Table 5; Fig. 4). The following linear correlation equation was determined between the two variables: cTEA difference° = 0.16 × (HKA difference°) − 0.61 (Fig. 5). Based on this equation, a 10° increase in the HKA difference results in a 1.5° increase in the cTEA difference.
Discussion
The two important findings of this study were that 1) bilateral knee osteoarthritis with WSD is associated with a significantly increased cTEA in valgus knees compared to varus knees, and 2) the cTEA difference positively correlates with the varus–valgus HKA difference.
In this study, femoral condylar orientation, as assessed by cTEA, was characterized by more ER in valgus knees with WSD, corresponding well to previous studies that reported increased cTEA with lateral condylar hypoplasia in valgus knees [4, 13]. However, in contrast to these studies, definite hypoplasia of the lateral femoral condyle was not observed in our study. The relatively smaller difference in the cTEA (1.5°), and AP dimensions (0.15 mm) between valgus and varus knees, compared to that of Matsuda et al. (cTEA difference: 5.0°, AP dimension difference: 2.8 mm), can explain this finding. These results indicate that the increase in the cTEA of the valgus osteoarthritic knee in WSD can be related to the degenerative wear of the posterior condyles rather than hypoplasia of the lateral femoral condyle. Nevertheless, the different femoral rotational profiles between the valgus and varus sides should be considered carefully to achieve optimal femoral component rotation during bilateral TKA.
In WSD, coronal alignments were also significantly different between varus and valgus osteoarthritic knees. The decreased LDFA in valgus knees, and decreased MPTA in varus knees can be explained by different phenotypes of distal femur and proximal tibia or different degrees of condylar erosion. The increased VCA of varus knees (6.15 ± 1.05°) compared to valgus knees (5.13 ± 1.16°) in this study are in agreement with the results of Mulaji et al. [19], that reported a VCA of 6.4 ± 1.6° in varus knees, and of 5.4 ± 2° in valgus knees. To achieve an accurate distal femoral cut in WSD, individualized cutting strategy such as digital planning, navigation TKA, and patient specific instrumentation can be helpful.
The other important finding of this study was that cTEA differences positively correlated with HKA differences between varus and valgus osteoarthritic knees with WSD. Based on our linear correlation equation, a 10° increase in the HKA difference results in a 1.5° increase in the cTEA difference. Further studies are necessary to validate this relationship prior to clinical application of this equation. Thus, the HKA difference in the coronal plane can be a useful indicator of a cTEA difference, suggesting that the information obtained from coronal radiologic parameters on plain radiography can decrease the need for costly additional imaging, including knee CT or MRI.
This study has some limitations. First, the retrospective study design and relatively small number of subjects make the study susceptible to unknown selection bias. Considering that the mean HKA of valgus knee was − 5.25° in this study, our findings need to be prospectively validated for more severe valgus deformities. Second, in this study rotational profiles were measured with 2D axial CT scan that has been reported to be less accurate than 3D CT scan [7]. However, based on the ICC values of over 0.8, the accuracy of 2D CT is considered acceptable. Third, femoral rotational profiles were evaluated using axial knee CT scans, which cannot accurately reflect cartilage status. Therefore, the actual value of the intra-operative varus–valgus cTEA difference may have been underestimated. Nevertheless, the fact that asymmetry of femoral rotational profiles in WSD should be considered appropriately to achieve optimal rotational alignment after TKA is a meaningful message.
Conclusion
In bilateral knee osteoarthritis with WSD, valgus knees showed significantly increased cTEA compared to varus knees, and the cTEA difference positively correlated with the HKA difference between valgus and varus knees. To determine the optimal femoral component rotation during TKA in WSD, assessment of cTEA with pre-operative CT scans or careful intra-operative measurement is recommended, especially in patients with large HKA difference.
References
Akagi M, Matsusue Y, Mata T, Asada Y, Horiguchi M, Iida H et al (1999) Effect of rotational alignment on patellar tracking in total knee arthroplasty. Clin Orthop. https://doi.org/10.1097/00003086-199909000-00019155-163
Anouchi YS, Whiteside LA, Kaiser AD, Milliano MT (1993) The effects of axial rotational alignment of the femoral component on knee stability and patellar tracking in total knee arthroplasty demonstrated on autopsy specimens. Clin Orthop 287:170–177
Babu S, Vaish A, Vaishya R (2020) Windswept deformities of the knee are challenging to manage. Knee Surg Relat Res 32:46
Chang MJ, Jeong HJ, Kang SB, Chang CB, Yoon C, Shin JY (2018) Relationship between coronal alignment and rotational profile of lower extremity in patients with knee osteoarthritis. J Arthroplasty 33:3773–3777
Dargel J, Feiser J, Gotter M, Pennig D, Koebke J (2009) Side differences in the anatomy of human knee joints. Knee Surg Sports Traumatol Arthrosc 17:1368–1376
Eckstein F, Müller S, Faber SC, Englmeier KH, Reiser M, Putz R (2002) Side differences of knee joint cartilage volume, thickness, and surface area, and correlation with lower limb dominance—an MRI-based study. Osteoarthritis Cartilage 10:914–921
Hirschmann MT, Konala P, Amsler F, Iranpour F, Friederich NF, Cobb JP (2011) The position and orientation of total knee replacement components: a comparison of conventional radiographs, transverse 2D-CT slices and 3D-CT reconstruction. J Bone Jt Surg Br 93:629–633
Howell SM, Shelton TJ, Gill M, Hull ML (2021) A cruciate-retaining implant can treat both knees of most windswept deformities when performed with calipered kinematically aligned TKA. Knee Surg Sports Traumatol Arthrosc 29:437–445
Iranpour-Boroujeni T, Li J, Lynch JA, Nevitt M, Duryea J (2014) A new method to measure anatomic knee alignment for large studies of OA: data from the osteoarthritis initiative. Osteoarthritis Cartilage 22:1668–1674
Jang KM, Park JH, Chang M, Kim Y, Lee D, Park S et al (2017) Three-dimensional evaluation of similarity of right and left knee joints. Knee Surg Relat Res 29:307–315
Kinzel V, Ledger M, Shakespeare D (2005) Can the epicondylar axis be defined accurately in total knee arthroplasty? Knee 12:293–296
Matsuda S, Matsuda H, Miyagi T, Sasaki K, Iwamoto Y, Miura H (1998) Femoral condyle geometry in the normal and varus knee. Clin Orthop. https://doi.org/10.1097/00003086-199804000-00022183-188
Matsuda S, Miura H, Nagamine R, Mawatari T, Tokunaga M, Nabeyama R et al (2004) Anatomical analysis of the femoral condyle in normal and osteoarthritic knees. J Orthop Res 22:104–109
Meding JB, Anderson AR, Ritter MA, Faris PM, Keating EM (2000) Windswept deformity in bilateral total knee arthroplasty. J Arthroplasty 15:562–566
Merican AM, Ghosh KM, Iranpour F, Deehan DJ, Amis AA (2011) The effect of femoral component rotation on the kinematics of the tibiofemoral and patellofemoral joints after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 19:1479–1487
Murray PB, Rand JA (1993) Symptomatic valgus knee: the surgical options. J Am Acad Orthop Surg 1:1–9
Phillips MI, Krackow KA (1999) Distal femoral varus osteotomy: indications and surgical technique. Instr Course Lect 48:125–129
Sheth NP, Husain A, Nelson CL (2017) Surgical techniques for total knee arthroplasty: measured resection, gap balancing, and hybrid. J Am Acad Orthop Surg 25:499–508
Shetty GM, Mullaji A, Khalifa AA, Ray A (2017) Windswept deformities—an indication to individualise valgus correction angle during total knee arthroplasty. J Orthop 14:70–72
Smyth EH (1980) Windswept deformity. J Bone Jt Surg Br 62-B:166–167
송인수, 전재균, 김준범 (2008) Total knee arthroplasty for treating valgus and varus in the knees of one person. Knee Surg Relat Res 20(2):110–116
Funding
This research was supported by the Bio & Medical Technology Development Program of the National Research Foundation (NRF) funded by the Korean government (MSIT) (2017M3A9D8063538).
Author information
Authors and Affiliations
Contributions
YSC: design, data acquisition, data analysis, data interpretation, and drafting manuscript. TWK: design, data acquisition, data analysis, data interpretation, and drafting manuscript. SCS: data acquisition, data analysis, and data interpretation. SYK: data acquisition, data analysis, and data interpretation. MJC: data acquisition, data analysis, and data interpretation. S-BK: design, data interpretation, and manuscript revision.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the institutional review board of Seoul National University Seoul Metropolitan Government Boramae Medical Center (IRB NO: 20-2021-36).
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Choi, Y.S., Kim, T.W., Song, S.C. et al. Asymmetric transepicondylar axis between varus and valgus osteoarthritic knees in windswept deformity can be predicted by hip–knee–ankle angle difference. Knee Surg Sports Traumatol Arthrosc 30, 3024–3031 (2022). https://doi.org/10.1007/s00167-021-06661-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06661-1