Abstract
Purpose
Resilience to stressful life events (SLEs), which increase risk of psychopathology, is influenced by genetic factors. The purpose of this paper was to map the overlap of etiologic risk factors for resilience onto the broad psychopathological map. Resilience was defined as the difference between the twins’ total score on a broad measure of internalizing symptoms and their predicted score based on their cumulative exposure to SLEs.
Methods
Cholesky decompositions were performed with OpenMx to quantify the overlap in genetic and environmental risk factors between resilience and four phenotypes [major depression (MD), generalized anxiety disorder (GAD), alcohol abuse or dependence (AAD), and antisocial personality disorder (ASPD)].
Results
The genetic factors that influence resilience account for 42 and 61 % of the heritability of MD and GAD, respectively, and 20 and 18 % for AAD and ASPD, respectively. The latent genetic contribution to MD was shared 47 % with resilience, and for AAD, this estimate was lower (23 %). The shared environmental covariance was nominal.
Conclusions
Genetic influences on resilience contribute to internalizing phenotypes to a higher degree than to externalizing phenotypes. Environmental influences can also have an enduring effect on resilience. However, virtually all of the covariance between resilience and the phenotypes was genetic.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Exposure to traumatic and stressful life events (SLEs) increases risk of many psychiatric phenotypes [1, 2], but not uniformly [3]. This variability in response to SLEs has afforded great interest in the identification of the etiologic factors underlying resilience, a term that broadly refers to adaptive functioning in the face of SLEs and other forms of adversity [4]. To that end, we recently quantified psychiatric resilience at two time points in a large sample of twins by computing the residual between actual and predicted level of symptoms of anxiety and depression based on the number of SLEs recently experienced [5]. We found a modest heritability for resilience (~31 %) in our univariate models, and a moderate heritability for resilience (roughly 50 %) in our final model that was unconfounded by measurement error, suggesting that genetic factors influence psychiatric resilience. Two other twin studies have also examined the etiologic sources of resilience and also demonstrated modest genetic influence [6, 7].
Given that our group [5] and others [6, 7] have quantified the degree of genetic and environmental influence on resilience, our primary aim was to expand upon this finding by determining the degree to which genetic and environmental factors contribute to both psychiatric resilience and common psychiatric disorders [e.g., the overlap of etiologic sources on both resilience and psychopathology, such as major depression (MD) and alcohol abuse of dependence (AAD)]. This line of research is of importance, as it can shed light on the degree to which, from a genetic and environmental perspective, the sources of risk to common psychiatric disorders are related to resilience. Furthermore, it may inform upon efforts to identify genes associated with resilience, an undertaking that remains unstudied to date. By far the best-established higher-order structure of common psychopathology has been between internalizing and externalizing [8]; therefore, in this paper, we pick two separate disorders from each domain [MD, generalized anxiety disorder (GAD), AAD, antisocial personality disorder (ASPD)] and clarify the patterns of covariance across the broad landscape of common psychopathology. Our primary aim was to determine whether the genetic and environmental overlap between resilience and each form of psychopathology is uniform within each domain, or whether the genetic and environmental covariance with resilience differs (e.g., is there a greater overlap in the shared genetic contribution between resilience and MD vs. resilience and GAD?). Furthermore, this twin sample was assessed several times for MD and AAD, permitting us to examine the inter-relationship between the temporally stable components of the etiologic sources (genetic and environmental) to our MD and AAD phenotypes and resilience. Given that the relationship between SLEs is generally higher for internalizing disorders [6], we hypothesize that the overlap will be greater between the genetic influences on resilience and the internalizing disorders (MD, GAD) than it will be for the externalizing phenotypes (AAD, ASPD). However, while an SLE-based resilience indicator is likely more applicable to internalizing as compared to externalizing disorders, associations between SLEs and externalizing conditions do exist, and the relevance of this type of resilience determination to externalizing disorders has not been empirically determined, suggesting that the present investigation is worthwhile. Finally, although an overlap in genetic influences is expected, we hypothesize that this (genetic) overlap would not be complete, even for the internalizing phenotypes.
Methods
Sample
Participants were derived from two inter-related Virginia Adult Twin Studies of Psychiatric and Substance Use Disorders (VATSPSUD) studies of Caucasians [9], ascertained from the birth certificate-based Virginia Twin Registry. Female–female (FF) twin pairs, born 1934–1974, were eligible if both members responded to a mailed questionnaire in 1987–1988. Nearly all variables used in these analyses were evaluated at the first interview wave (FF1) conducted in 1987–1989, third (FF3) interview conducted in 1992–1995, and fourth wave (FF4) conducted in 1995–1997, with cooperation ranging from 88 to 92 %. Data on the male–male and male–female pairs (MMMF) came from a sample (birth years 1940–1974) initially ascertained with a 72 % cooperation rate from registry records containing all twin births. The first interview (MMMF1) was completed by phone in 1993–1996, and the second interview (MMMF2) was conducted in 1994–1998. Response rates ranged from 72 to 83 %.
Zygosity was determined by discriminate function analyses using standard twin questions validated against DNA genotyping in 496 pairs [10]. The mean (SD) age and years of education of the twins were 35.1 (7.5) and 14.3 (2.2) at the FF4 interview, and 37.0 (9.1) and 13.6 (2.6) at the MMMF2 interview. These analyses utilized data from 7500 twins, including both members of 3084 pairs (503 monozygotic (MZ) FF, 346 dizygotic (DZ) FF, 703 MZ MM, 485 DZ MM, and 1047 opposite sex DZ pairs) and 1325 twins without their cotwin.Footnote 1
Definition of resilience
Participants completed a shortened version of the Symptom Checklist-90 [SCL-90; [11]], which utilized a past month timeframe (FF1, FF3, MMMF1, MMMF2). There were 27 items from four of the SCL subscales: depression (ten items), somatization (five items), anxiety (seven items), phobic anxiety (five items), and three items that assessed sleep difficulty. This measure demonstrated relatively high internal reliability for both waves (Cronbach’s α = .74). We assessed SLEs over the past year that were personal in nature (assault, serious marital problems, divorce, job loss, loss of a confidant, serious illness, major financial problem, being robbed, serious legal problems), and “network” events (i.e., events that occurred primarily to, or in interaction with, an individual in the respondent’s social network): death or severe illness of the respondent’s spouse, child, parent, cotwin, or other relative, and serious trouble getting along with others close to the respondent. Inter-rater reliability for determining the occurrence of the events was high (kappa = .93; [12]). Consistent with prior research on cumulative effects of stressors [5, 13–15], a sum of SLEs was computed.
Resilience was operationalized as the residual of the SCL score after the effect of recent number of SLEs has been regressed out for each wave (i.e., the difference between actual and predicted SCL). The residual was used as a continuous measure of resilience. If a twin’s SCL was lower than predicted by the regression, this would result in a negative residual, reflecting a higher level of resilience; if a twin’s SCL was higher than expected, this would result in a positive residual, reflecting low levels of resilience.
Assessment of psychiatric and alcohol use disorders
Prevalence of psychiatric and alcohol use disorders were assessed at personal interview by trained mental health professionals who were blind to the status of the cotwin, using modifications of the SCID interview and DSM-IV criteria [16, 17]. We assessed for the past 12-month presence of two internalizing conditions, major depression (MD; FF1 MMMF1 interviews) and generalized anxiety disorder (GAD; FFI MMMF2 interviews) for which we required a minimum duration of 1 month, and two externalizing conditions, past 12-month alcohol abuse or dependence (AAD; FF4 MMMF2 interviews) and antisocial personality disorder (ASPD; FF4 MMMF2 interviews) which measured only adult antisocial traits.
Twin modeling
Phenotypic variation in twin models is decomposed into additive genetic factors (A) which contribute twice as much to the correlations between MZ twins as they do for DZ twins, common environmental factors (C) which are the shared factors (e.g., parental attitudes) that make twins reared together similar and contribute equally to the correlation between MZ and DZ twins, and individual-specific environmental (E) sources, which reflect environmental experiences not shared by twins and therefore contribute to differences between the twins and errors of measurement.
To test the degree to which the covariation between resilience and the psychiatric phenotypes results from common factors, we applied a series of bivariate Cholesky models [18]. These models specify three latent factors (A1, C1, and E1) influencing both resilience and the psychiatric phenotype, in addition to three factors (A2, C2, and E2) accounting for residual influences specific to the psychiatric phenotype. We chose to order resilience before the psychiatric phenotypes in the models as it is thought to be more trait-like in nature, whereas the psychiatric phenotypes may have a later onset.
We began by testing for quantitative sex differences (i.e., if there is equality in the estimates of the genetic contribution in males and females) by constraining the estimates of A, C, and E to be equal in males and females. The best-fit model was selected from these quantitative sex effect models, and we then tested for qualitative sex effects (i.e., whether or not the same genetic factors influenced liability to resilience and to the psychiatric phenotype for males and females, quantified by r g-resilience and r g-psychiatric phenotype). We fit three models that were compared to the saturated model (one that constrained to 1.0 r g-resilience only, one that constrained to 1.0 r g-psychiatric phenotype only, and one that constrained both r g parameters to 1.0). Finally, full models (ACE) were tested against nested sub-models with reduced numbers of parameters (AE; CE). To evaluate the fit of the twin models, full information maximum likelihood approach to raw data was implemented in OpenMx. Akaike’s information criterion (AIC) is used as a guide to evaluating different models. AIC produces an index of goodness of fit (i.e., balance of explanatory power and parsimony; [19]).
Measurement models
For MD and AAD, we utilized two waves of data simultaneously in a measurement model that assumes that there is a true latent liability to resilience and the psychiatric phenotypes (longitudinal data were not available for GAD and ASPD). The latent liability of the phenotypes, as well as wave-specific liabilities, was modeled in a standard ACE design with Cholesky decompositions. Sex effects were tested for, starting with quantitative sex effects in which we first constrained the A, C, and E estimates to equality for males and females on both the latent and wave-specific variables. We then allowed the wave-specific estimates to vary by sex and held the constraint at the latent variable level. Based on the best-fit model from these two quantitative models, we then tested for qualitative sex effects as outlined above. In contrast to the bivariate models, the measurement models allow for separate estimates of measurement error and true or enduring individual-specific environmental effects.
Results
Internalizing phenotypes
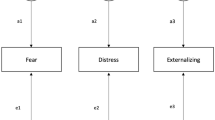
The correlations of resilience and MD were moderate, with somewhat higher correlations seen between resilience and GAD. Tables 1, 2, and 3 display the within-twin and cross-twin correlations for all phenotypes. Table 4 outlines the models that were fitted for resilience and the internalizing phenotypes. For MD, models were compared with the saturated model (I). We began in model II by testing for quantitative sex effects, which were not significant. Models were then tested for qualitative sex effects on resilience only (III), MD only (IV), and both resilience and MD (V). There was no evidence for sex effects, and then, model V was chosen to fit the sub-models (AE; CE).Footnote 2 Results of the sub-models suggested that C could be dropped from the model without sacrificing fit (model VII), but A could not be dropped (model VI). Following, this model, the AE model with no sex effects was the best-fit model (VI; Fig. 1a). Of greatest interest to us, the cross paths from both the genetic and environmental risk factors for resilience to MD were modest and negative (−0.37 and −0.19, respectively). This model estimated the total heritability of MD at 33 %, of which 42 % was shared with resilience and the remaining 58 % was specific to MD. Of the 68 % of variance in liability to MD that was environmental, only 6 % was shared with resilience.
Results for GAD are also in Table 4, and the modeling framework followed the same steps as outlined for MD. For GAD, model I, which had no sex effects, was the best-fit model and chosen to fit the sub-models (CE and AE). Model VI, the AE model, provided the best fit to the data (Fig. 1b). In this model, the genetic and environmental cross paths from resilience to GAD were modest and negative (−0.41 and −0.30, respectively). GAD was 28 % heritable, of which 61 % was shared with resilience and the remaining 39 % was specific to GAD. Environmental variance contributed 71 % of the liability to GAD, of which only 12 % was shared with resilience.
In comparing both MD and GAD, the proportion of the covariance was more accounted for by shared genetic factors (58, 49 %, respectively) than by shared unique environmental factors. With respect to genetic correlations, they were −0.65 for MD and −0.78 for GAD.
Externalizing phenotypes
The correlations of resilience and AAD were moderate, and the correlations between resilience and ASPD were slightly higher. Table 5 outlines the models that were fitted, which follow the same modeling framework as described above. The best-fit model for AAD did not have sex effects (model V), and the AE and CE models were subsequently fitted to this model. As shown in Fig. 2a, in the best-fitting model (VI, with A included), the genetic and environmental cross paths from resilience to AAD were modest and negative (−0.33 and −.08, respectively), and the total heritability of AAD was 56 %, of which 20 % was shared with resilience. Of the 45 % of variance attributed to environmental sources, only 2 % was shared with resilience.
As shown in Table 5, for ASPD the most parsimonious model was one without sex effects (V)Footnote 3; the best-fit sub-model (VI, the AE model) is shown in Fig. 2b. This model estimated the total heritability of ASPD to be equal to 46 %, of which 18 % was shared with resilience. Of the 57 % of variance in liability to ASPD that was environmental, only 4 % was shared with resilience. Similar to the internalizing disorders, the proportion of the covariance was more accounted for by shared genetic factors for both AAD and ASPD (56, 44 %, respectively) than by shared unique environmental factors. The genetic correlations were lower for externalizing disorders than for the internalizing disorders (−0.44 for both disorders).
Longitudinal models
Two waves of data were available for MD and AAD, and thus, measurement models were fitted. For MD, there was evidence of a quantitative sex effect when constraining male and female parameters at the latent and measurement-specific levels (Table 6; I vs. II). We then tested to see whether the parameters could be constrained to equality on the latent variable level only (III), which provided a superior fit. No qualitative sex effects were present (IV-VI), and thus, the AE (VII) and CE (VIII) models were fitted from model VI. The best-fit AE model (VII) is presented in Fig. 3. Of the 47 % of variance in the latent MD, nearly half (47 %) overlaps with resilience. The environmental overlap between MD and resilience was 23 % of the overall 53 % of variance in MD accounted for by environmental factors.
The same modeling steps were taken for AAD (Table 6). There was evidence for a quantitative sex effect (I vs. II), but these sex differences were being driven by the occasion-specific estimates, as the model fit improved when the parameters were constrained for the sexes on the latent variable level only (III). Qualitative sex effect testing suggested that for AAD, the rG (.50) could not be constrained to 1 (VI) without deterioration in model fit. From model VI, we determined that C could be dropped from the model (VIII), but A could not (VII; Fig. 4). The latent AAD was highly heritable (.70), and of this genetic contribution, 16 % was overlapping with resilience. The environmental contribution to AAD was 29 %, and of this, 10 % was shared with resilience. A consistent pattern to the bivariate models was found for the longitudinal models in that the covariance was accounted for more by genetic factors than by environmental factors. Similarly, the genetic correlations were higher for MD (−.68) than for AAD (−.40).
Discussion
We sought to determine the degree to which the etiologic contributions to psychiatric resilience index the risk factors for common psychiatric phenotypes to understand the relative importance of: (1) genetic factors that contribute to both resilience and the common psychiatric disorder and (2) environmental factors common to both phenotypes. We conducted Cholesky decompositions with resilience as our upstream/predictor variable, as resilience is theorized to be a relatively stable trait-like construct, and each current psychiatric phenotype as the downstream/dependent variable. We fit two series of longitudinal models to remove the effects of measurement error, thereby examining the stable components of variance and covariance. Overall, the genetic influence for resilience contributes to some degree to all phenotypes examined. However, as expected, resilience does a better job of indexing MD and GAD than it does for AAD and ASPD. By contrast, the environmental risk factors for resilience were largely independent of those for the psychiatric phenotypes.
Resilience’s etiologic relationships with MD and GAD
The genetic influences on resilience accounted for 42 % of the total heritability of MD in the bivariate model, and this increased modestly in the longitudinal model that is unconfounded by measurement error (to 46 %). Additionally, 61 % of the heritability of GAD is shared with resilience. The finding that GAD is more closely genetically related to resilience than MD was unexpected given that MD is generally more related to SLEs [9, 20, 21] and our definition of resilience is centered upon reaction to SLEs. However, prior studies have documented a higher prevalence of trauma in those with GAD versus non-anxious controls [22] and higher rates of GAD in an acute post-trauma context compared to general population samples [23]. Second, virtually all of the covariance between resilience and MD and GAD was genetic; a trivial amount was due to unique environmental influences that overlap. This is consistent with a recent investigation reporting that roughly half of the genetic influence on mental well-being overlapped with that of internalizing psychopathology [24].
These results suggest that resilience is genetically indexing something in its own right versus tapping into the presence or absence of high risk of internalizing psychopathology. Although there was overlap in the genetic influences between resilience and MD and GAD, for both disorders there was a substantial portion of the genetic contribution that was independent (i.e., unshared with resilience), suggesting that the construct of resilience as currently defined is not simply indexing risk of internalizing psychopathology. Similarly, a prior multivariate twin analysis in the sample demonstrated that a proportion of the heritable component for internalizing disorders was not captured by neuroticism [25].
Resilience’s etiologic relationships with AAD and ASPD
We found that the genetic influence on resilience modestly overlaps with the genetic contribution to AAD (20 and 18 % of the overall heritability in the bivariate and longitudinal models, respectively) and the genetic contribution to ASPD (18 % of the overall heritability). Conversely, similar to internalizing disorders, the degree of environmental covariation between resilience and externalizing disorders was nominal. These results are striking and suggest that the genes that contribute to resilience also play a role in externalizing phenotypes. The extant literature suggests a relationship between SLEs and externalizing phenotypes, and thus, it is not surprising that the genetic influence on these phenotypes overlaps with that of resilience, which is indexing one’s response to SLEs. Specifically, a recent study found multiple subtypes of offenders meeting ASPD criteria, including a group with greater internalizing disorders and trauma histories [26]. For AAD, there is substantial comorbidity with internalizing disorders [e.g., GAD, MD; 9], and epidemiologic studies generally suggest that the onset of PTSD predates that of AAD which provides support of this self-medication hypothesis [27]. Although not directly tested, it is possible that we are indexing this internalizing pathway via our genetic covariance shared between resilience and our externalizing phenotypes, and this is an empirical question that warrants further study.
Implications
Two extreme hypotheses can be rejected: (1) All of the genes for resilience are the same as those for these disorders (i.e., we “re-discovered” the heritable component to common psychopathology), and (2) the genetic component for resilience is unrelated to risk of psychopathology. Our results suggest something in the middle of these two extremes in that resilience is indexing the genetic component for common psychopathology, but more so for internalizing than externalizing disorders. This pattern of findings is expected, as our definition of resilience is more germane to internalizing symptoms, and because SLEs tend to increase risk of internalizing disorders more so than externalizing disorders [2]. Comparisons of the of cross paths of the genetic and environmental etiologic sources between resilience and the phenotypes can shed light on the degree to which the relationship is causal (i.e., one’s level of resilience exerts a causal influence on their liability for the disorder) or non-causal (i.e., genetic confounding accounts for the relationship). If the relationship between resilience and the disorders was causal, then the genetic and environmental cross-path estimates would be roughly of similar magnitude. That is, if environmental influences that alter the level of resilience in turn directly impacted on the psychiatric disorders causally, we would find that the environmental cross paths would be as strong as the genetic cross paths. However, across all phenotypes, the genetic cross paths are substantially larger than the environmental cross paths, suggesting that genetic covariation rather than phenotypic causality is at play. Although we are not formally testing causal models, the relationship between resilience and the disorders is likely largely non-causal and results mainly from genetic factors which impact both phenotypes. Following, clinicians who are treating these phenotypes may also want to include skills-based approaches for their patients for healthy coping in the face of SLEs, as those with a genetic risk of psychiatric disorders may also have a genetic risk of low resilience in the face of SLEs.
Our findings warrant gene-finding efforts for resilience and suggest that the use of targeted approaches based on the overlap between resilience and the psychiatric disorders may be a fruitful place to start identifying genes for resilience (e.g., examining genetic variants associated with risk of MD, GAD, AAD, ASPD in relation to resilience). However, agnostic approaches, such as genome-wide association studies, are also warranted for resilience, as we would not expect complete shared risk alleles with these common forms of psychopathology.
Limitations
Limitations include that the dependent measure that we defined resilience with is more germane to internalizing symptoms than externalizing symptoms, which may in part account for the finding that resilience is more related to internalizing phenotypes. Although our SLE assessment was thorough, it was not exhaustive, and it did not measure reaction to the events (e.g., fear, helplessness or horror, life threat). Additionally, a simple count of SLEs was utilized in the regression on SLC-90 to obtain the residual score reflecting resilience. There are many nuances that this approach does not capture, such as the potential for forms of SLEs to be differentially impactful, or for the potential of sex-based differences for forms of SLEs. Future research could examine these effects to obtain a more sophisticated metric of resilience (i.e., one that weights traumas or SLEs or combines category and item frequencies). Furthermore, replication of this method in more diverse samples with regard to demographic and trauma type characteristics would allow for further refinement of the method. Regarding the residuals that resulted from the regression, while the assumption of linearity was met, the assumption of homoscedasticity was not. This suggests that as the number of SLEs increases, there is greater error in prediction of SLC-90 and was visually presented in earlier work with this sample and methodology [5]. The increasing variability with greater SLEs may also reflect the effect of an untested variables(s), which future investigations may shed further light onto. Lastly, although population based, our study was composed of white twins from the Mid-Atlantic region of the USA, and therefore generalizability is limited.
Notes
These numbers do not sum because all possible pairings for triplet and quadruplet sets were included.
Model III with a qualitative sex effect for resilience fits slightly better than model V that did not have any sex effects (AICs = 3308.75 vs. 3309.84, respectively), but for parsimony, we chose to fit the nested models from the model without any sex effects.
Model XI with a qualitative sex effect for ASPD fits slightly better than model XIII that did not have any sex effects (AICs = 11,860.41 vs. 11,861.13, respectively), but for parsimony, we chose to fit the nested models from the model without any sex effects.
References
Battle CL et al (2004) Childhood maltreatment associated with adult personality disorders: findings from the Collaborative Longitudinal Personality Disorders Study. J Pers Disord 18(2):193–211
Pietrzak RH et al (2011) Prevalence and Axis I comorbidity of full and partial posttraumatic stress disorder in the United States: results from Wave 2 of the National Epidemiologic Survey on Alcohol and Related Conditions. J Anxiety Disord 25(3):456–465
Bonanno GA (2004) Loss, trauma, and human resilience. Have we underestimated the human capacity to thrive after extremely aversive events? Am Psychol 59:20–28
Rutter M (2006) Implications of resilience concepts for scientific understanding. Ann NY Acad Sci 1094:1–12
Amstadter AB, Myers JM, Kendler KS (2014) Psychiatric resilience: longitudinal twin study. Br J Psychiatry J ment sci 205(4):275–280. doi:10.1192/bjp.bp.113.130906
Kim-Cohen J et al (2004) Genetic and environmental processes in young children’s resilience and vulnerability to socioeconomic deprivation. Child Dev 75(3):651–668
Broadman JD, Blalock CL, Button TMM (2008) Sex differences in the heritability of resilience. Twin Res Hum Genet 11(1):12–27
Kendler KS, Myers J (2014) The boundaries of the internalizing and externalizing genetic spectra in men and women. Psychol Med 44(3):647–655. doi:10.1017/S0033291713000585
Kendler KS, Prescott CA (2006) Genes, environment, and psychopathology: understanding the causes of psychiatric and substance use disorders. The Guildford Press, New York
Kendler KS, Prescott CA (1999) A population-based twin study of lifetime major depression in men and women. Arch Gen Psychiatry 56:39–44
Derogatis LR, Lipman RS, Covi L (1973) SCL-90: an outpatient psychiatric rating scale–preliminary report. Psychopharmacol Bull 9(1):13–28
Kendler KS et al (1995) Stressful life events, genetic liability, and onset of an episode of major depression in women. Am J Psychiatry 152:833–842
Amstadter AB et al (2013) Potentially traumatic event exposure, posttraumatic stress disorder, and axis I and II comorbidity in a population based study of Norwegian young adults. Soc Psychiatry Psychiatr Epidemiol 48(2):215–223
Follette VM et al (1996) Cumulative trauma: the impact of child sexual abuse, adult sexual assault, and spouse abuse. J Trauma Stress 9:25–35
Suliman S et al (2009) Cumulative effect of multiple trauma on symptoms of posttraumatic stress disorder, anxiety, and depression in adolescents. Compr Psychiatry 50(2):121–127
American Psychiatric Association (1994) Diagnostic and statistical manual of mental disorders, 4th edn. Author, Washington
Spitzer RL et al (1995) Structured clinical interview for DSM-IV. American Psychiatric Press, Washington
Neale MC, Cardon LR (1992) Methodology for genetic studies of twins and families. Kluwer, Dordrecht
Akaike H (1987) Factor analysis and AIC. Psychometrika 52:317–332
Kendler KS et al (2003) Life event dimensions of loss, humiliation, entrapment, and danger in the prediction of onsets of major depression and generalized anxiety. Arch Gen Psychiatry 60(8):789–796
Kendler KS, Karkowski LM, Prescott CA (1998) Stressful life events and major depression: risk period, long-term contextual threat, and diagnostic specificity. J Nerv Ment Dis 186(11):661–669
Roemer L et al (1998) Preliminary investigation of the role of previous exposure to potentially traumatizing events in generalized anxiety disorder. Depress Anxiety 4(3):134–138
Amstadter AB et al (2009) Posttyphoon prevalence of posttraumatic stress disorder, major depressive disorder, panic disorder, and generalized anxiety disorder in a Vietnamese sample. J Trauma Stress 22(3):180–188
Kendler KS et al (2011) The relationship between genetic and environmental influences on common internalizing psychiatric disorders and mental well-being. Behav Genet 41:641–650
Hettema JM et al (2006) A population-based twin study of the relationship between neuroticism and internalizing disorders. Am J Psychiatry 163(5):857–864
Poythress NG et al (2010) Using the PCL-R to help estimate the validity of two self-report measures of psychopathology with offenders. Assessment 17(2):206–219
Mellman TA et al (1992) Phenomenology and course of psychiatric disorders associated with combat related posttraumatic stress disorder. Am J Psychiatry 149:1568–1574
Acknowledgments
This work was supported in part by NIH Grants K02 AA023239 R01 AA020179, P20 AA10782, R37 AA011408, R37 DA18673 and R01 DA22989. The Mid-Atlantic Twin Registry is supported by NIH Grant UL1RR031990.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no competing interests.
Rights and permissions
About this article
Cite this article
Amstadter, A.B., Maes, H.H., Sheerin, C.M. et al. The relationship between genetic and environmental influences on resilience and on common internalizing and externalizing psychiatric disorders. Soc Psychiatry Psychiatr Epidemiol 51, 669–678 (2016). https://doi.org/10.1007/s00127-015-1163-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-015-1163-6