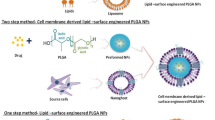
Abstract
Surface engineering facilitates incorporation of various bioactive compounds and provides unique advantages for the specific delivery of imaging and therapeutic agents. Several molecules with imaging, diagnostic, prognostic, sensing, and therapy can be incorporated in the bioformulations with the help of different surface engineering techniques. This chapter reviews drug carriers which were surface engineered for targeted drug delivery at the requisite location. A single or combination of surface engineering has been used for efficient delivery of carriers. The carriers reviewed here were divided into two categories: lipid-based carriers (liposomes and solid lipid nanoparticles) and non-lipid-based carriers (niosomes, polymeric nanoparticles, hydrogels, dendrimers, quantum dots, gold nanoparticles, and mesoporous silica nanoparticles). Various kinds of bioactive compounds along with the involvement of surface engineering techniques in incorporation were also discussed. This chapter focuses on recent advances in the surface engineering of nanocarriers for therapeutic applications.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Surface engineering
- Lipid carriers
- Non-lipid carriers
- Liposomes
- Active targeting
- Solid lipid nanoparticles
- Niosomes
- Polymeric nanoparticles
- Hydrogels
- Dendrimers
- Quantum dots
- Gold nanoparticles
- Mesoporous silica nanoparticles
6.1 Introduction
Surface engineering plays a pivotal role in preparation of nanocarriers. It involves the utilization of synthetic or natural biomaterials for advancement and amenability of biological function, i.e., targeted drug delivery system. The need for new biological materials and novel technologies arises the requirement of surface engineering. It helps in construction of molecular design, easy synthesis, and tailoring broad range of applications. Surface engineering has the ability to manipulate biological interfaces and precise the arrangement with the modification of surface according to the need and requirement, for the development of well-controlled bioformulations.
Three most important approaches for surface modifications are: direct deposition, incorporation, and encapsulation. Direct deposition means the filming of a bioactive compound directly on the surface of a nanocarrier. Whereas, in incorporation various bioactive compounds are integrated in between the surface layer of the nanocarrier using suitable surface modification techniques. Though, enclosing a bioactive compound in a nanocarrier, i.e., the addition of a bioactive compound inside a nanocarrier is called encapsulation. Therefore, the encapsulation of a bioactive compound in a nanocarrier means to encapsulate/surround a bioactive compound inside a nanocarrier, i.e., liposomes. Here in this chapter, we focused on the incorporation of bioactive compound in nanocarriers for drug delivery.
In current healthcare practice, especially in chemotherapy drug toxicity is an important factor for consideration. A conventional drug given to a patient affects both normal and diseased tissues. To decrease the adverse effects on normal tissues, targeting of the diseased tissues can be achieved via surface engineered targeted drug carriers. Many drug carriers, i.e., liposomes, solid lipid nanoparticles (SLNs), niosomes, polymeric nanoparticles (PNPs), hydrogels, dendrimers, quantum dots, gold nanoparticles (AuNPs), and mesoporous silica nanoparticles (MSNPs) have been developed, which include surface engineering for controlled release with enhancement of drug potency [1,2,3,4].
Here, we have categorized drug carriers into two classes, i.e., lipid-based and non-lipid-based carriers and further describes the surface engineering involved in the incorporation of bioactive compounds in these carriers. The difference between these two carriers is explained as follows. Lipid carriers are made up of lipid molecules and form a vesicle or certain structure to carry the desired biomolecules load. Liposomes and solid lipid nanoparticles are the examples of lipid-based carriers. Liposomes have phospholipid bilayers and contain incorporated drugs. Solid lipid nanoparticles have a solid lipid matrix with drug embedded in the matrix or adsorbed on the surface [2]. Non-lipid nanocarriers are those carriers which are composed of materials other than lipids such as nonionic surfactants, polymers, etc. Niosomes have nonionic surfactant bilayers and contain incorporated drugs. Polymeric nanoparticles are composed of natural or synthetic polymers and hydrogels are gels made of hydrophilic polymers. Dendrimers are synthetic polymeric macromolecules. Quantum dot is composed of a semiconductor material.
Applications of lipid-based nanocarriers have an advantage of least toxicity and drug safety. Lipid-based delivery systems include micelles, liposomes, solid lipid nanoparticles, nanoemulsions, and nanosuspensions. Lipid-based nanocarriers are a class of biocompatible and biodegradable vehicles. It provides advanced delivery of therapeutic and imaging agents, with improved pharmacokinetics. In this category, the most extensively studied drug carrier is liposome. A number of non-lipid-based nanocarrier formulations have also been described in terms of incorporation of bioactive compound and their formulation with respect to surface engineering. Most of the non-lipid-based carriers are studied to improve the oral, intranasal, and central nervous system delivery of analgesic agents. This part includes niosomes, polymeric nanoparticles, hydrogels, dendrimers, quantum dots, gold nanoparticles, and mesoporous silica nanoparticles.
6.2 Lipid-Based Nanocarriers
6.2.1 Liposomes
Alec Bangham, the father of liposomes described them for the first time in 1965. First they were called as Banghasomes [5] but later were called as liposomes [6]. Phospholipid is ampiphilic in nature and has hydrophilic head with two hydrophobic fatty acid chains. They form multilamellar vesicles (MLVs) on the hydration of phospholipid film and the hydration is done above the phase transition temperature of the phospholipid. Cholesterol is added to lipid mixture to toughen the liposomes. The presence of charge on the liposomes provides physical stability to liposomes. The addition of DOTAP (1,2-dioleoyl-3-trimethylammoniuum-propane chloride) to lipid mixture provides +ve charge to liposomes. Cationic liposomes are used for the loading of −ve charged nucleic acids. Liposomes can be giant unilamellar vesicles (GUVs), multilamellar vesicles (MLVs), large unilamellar vesicles (LUVs), and small unilamellar vesicles (SUVs). The size range is >1000, >500, >100, and 20–100 nm for GUVs, MLVs, LUVs, and SUVs respectively. LUVs are now used for the drug delivery studies [7, 8].
The extrusion of MLVs through polycarbonate filters generates LUVs. The sonication of MLVs gives SUVs. LUVs are obtained by solvent injection, detergent removal, reverse phase evaporation [7]. The following techniques can be used for the large-scale production of liposomes [7, 9]:
-
Spray drying [12]
-
Freeze drying/lyophilisation [13]
-
Super critical reverse phase evaporation (SCRPE) method [14]
Liposomes applications for targeted drug delivery include the incorporation of bioactive compounds, i.e., anticancer, antibiotic, antifungal, and anti-inflammatory drugs and genes where comes the role of surface engineering. Figure 6.1 illustrates the role of surface engineering to formulate different types of liposomes. In general, biomaterials can be incorporated in liposome by active or passive loading. The surface properties of bioactive materials dictate the final application of liposomes.
Different types of liposomes. a Conventional liposome. b PEGylated liposome. c Ligand-targeted liposome for specific targeting (ligands may be antibodies, peptides, etc). d Theranostic liposome contains an imaging agent such as Gd-DOTA-DSPE for MRI and a therapeutic drug such as paclitaxel which is a hydrophobic anticancer drug
6.2.1.1 Stealth Liposomes/PEGylated Liposomes
Stealth liposomes are the liposomes which show extended blood circulation time while reducing mononuclear phagocyte system uptake. Advancement of liposomal preparation based on lipid composition, size, and charge of the vesicle modulate it into long-circulating liposomes. Inclusion and incorporation of the synthetic polymer poly-(ethylene glycol) (PEG) in liposome composition has developed stealth liposomes (see Fig. 6.1). Further, by synthetic modification of the terminal PEG molecule, stealth liposomes can also be actively targeted with monoclonal antibodies or ligands and incorporation of these active molecules provide high target efficiency and activity. PEG is the universally used polymer for improvement of circulation time among the different polymers investigated to data.
Different surface engineering are involved in the incorporation of PEG on the liposomal surface but the most widely used method is the use of cross-linked lipid, i.e., PEG-distearoyl-phospha-tidylethanolamine (DSPE). Poly(ethylene glycol)-linked phospholipids such as DSPE-PEG 2000 or methoxy PEG 2000-DSPE are commercially available for the preparation of stealth liposomes. DSPE is a synthetic amphiphilic phospholipid. The role of phospholipid portion in poly(ethylene glycol)-linked phospholipid needs to be investigated. Therefore, non-phospholipid-PEGs such as Cholesteryl-PEG (Chol-PEG) are also being developed for the preparation of stealth liposomes [15]. An FDA approved liposomal doxorubicin preparation Doxil® contains stealth liposomes composed of cholesterol, hydrogenated soybean phosphatidylcholine (HSPC), and methoxy PEG 2000-DSPE [16].
Other surface modifications involved are: physical adsorption of the polymer onto the surface of the vesicles, incorporating of PEG-lipid conjugate during liposome preparation, or by covalently attaching reactive groups onto the surface of preformed liposomes.
6.2.1.2 Immunoliposomes
Immunoliposomes are liposomes in which antibodies or their fragments are conjugated onto the surface. The surface modification with antibody increases the therapeutic index of many drugs via targeted drug delivery and controlled release of drugs. Two strategies are involved in coupling of antibody to the liposome surface. One involves covalent cross-linking with a liposomal lipid while another involves incorporation of chemically modified antibody into the bilayer by increasing hydrophobicity of the antibody. These approaches can attach a wide variety of antibodies to various types of liposomes.
For covalent cross-linking, first derivatization of the free amino group of phosphatidlyethanolamine (PE) with amino reactive bifunctional crosslinking molecules have been employed. This modified PE is combined with the bulk lipid to form liposomes. Later approach requires chemical modification of the antibody molecule with a hydrophobic substituent which increases the hydrophobicity of the antibody and hence, increases the affinity for the liposomal bilayer.
Nowadays, PEGlyated antibodies are used for targeted delivery. The lipid is usually cationic such as DOTAP (1,2-dioleoyl-3-trimethylammoniuum-propane chloride) which is added to lipid mixture to provide +ve charge to liposomes. See Fig. 6.2 for structure of DOTAP. A solution of +ve charged lipid along with a helper neutral lipid such as dioleoylphosphatidylcholine (DOPC) is mixed with gene material/nucleic acid which have −ve charge such as DNA. A +ve charged complex between nucleic acid and lipid is formed which is called as lipoplex. Cationic lipids are usually used in the delivery of genes but anionic lipids such as phosphatidic acid can also be used in the presence of divalent metal ions such as Ca2+ [17]. Due to risk of inactivation of whole antibody during the chemical conjugation process, fragment antigen-binding (Fab′) or single-chain fragment variable (scFv) are used to get imunoliposomes. The latter are the smallest fragment of an antibody containing the complete antigen-binding site [18]. Immunoliposomes are used for the delivery of genes which include DNA [19, 20], plasmid-DNA [21, 22], and RNA-based therapeutics such as antisense oligonucleotides and small interfering ribonucleic acid (siRNA) [23, 24].
Immunoliposomes are now extensively used to treat cancer cells in animal models. The targeting of immunoliposomes containing anticancer drugs at the overexpressed receptors in cancer cells resulted in the treatment of cancer. Transferrin receptors (TfRs) are overexpressed in cancers. An improved therapeutic activity was observed using TfR-targeted stealth immunoliposomes against liver cancer [25]. Cationic liposomes are used in the delivery of drugs to brain through blood–brain barrier [26, 27].
6.2.1.3 Multifunctional Liposomes: Theranostic Liposomes
Surface engineering plays a significant role in preparation of multifunctional liposomes and these are the advanced formulations of nanotechnology having simultaneous functions of diagnostics and therapeutics (theranostics) (see Fig. 6.1). Preparation of theranostic liposome requires the engagement of therapeutic, diagnostic, and imaging agent for defined targeted delivery of drugs which are toxic in free form. Theranostic liposomes are formed by correct utilization of surface engineering of the bilayers [28].
Surface engineered multifunctional liposomes containing UCNPs (lanthanide-doped up converting nanoparticles) and doxorubicin were prepared. UCNPs consisting of Er3+ and Yb3+ co-doped NaGdF4 upon exposure to an excitation wavelength of 890 nm showed a decrease in emission signals (a quenching effect). This allows the monitoring of drug release and drug loading. It was suggested that these prepared liposomes have a potential as theranostic nanocarriers [29]. A theranostic liposomal drug delivery system was reported with paclitaxel, carboplatin loaded as therapeutic agents and Gd-DTPA-BMA as contrast agent for MRI. These liposomes have prolonged circulation time and 36 times higher T1 relaxation-rate as compared to a commercial MRI contrast agent (Omniscan). These theranostic liposomes can carry both hydrophilic and hydrophobic drugs for lung cancer treatment with significant reduction in toxicity. The biodistribution of drugs was imaged via T1-weighted MRI in real time while drug delivery was achieved by the use of targeted tandem chemotherapy. The study offers new possibilities such as the evaluation of therapeutic response by in vivo imaging via T1-weighted MRI [30].
6.2.1.4 Active Loading or Remote Loading of Bioactive Compounds in Liposomes
Passive drug loading in liposomes means loading of drug in the process of formation of liposomes. Conventional liposomes usually have low encapsulation efficiency. Active drug loading requires the modification of surface to enhance the encapsulation efficiency and drug loading was done on preformed liposomes which had a pH gradient. This is known as active or remote drug loading. For desired biomedical application of liposomes, covalent immobilization of bioactive compounds onto the surface plays a significant role. Active loading have several advantages, i.e., high specificity and efficiency. The method of surface functionalization varies according to the final application of liposome formulation. By using surface functionalization, several types of liposomes were prepared and each of them have distinct functions.
In this pH gradient was developed by adding amine solution or basic drug to liposomes in pH 4.0 citrate buffer. To generate a pH gradient, the pH of the external medium was raised to pH 8 [31]. This helps in the incorporation of therapeutic agent in liposomes. The loading of amphiphilic amines (catecholamines), amphipathic (amphiphilic) weak base drugs having amine groups, i.e., anthracyclines were incorporated by pH gradient. In liposomes formulation, i.e., Myocet®, DaunoXome®, doxorubicin drug was loaded by using pH gradient [31,32,33,34]. Ammonium sulfate gradient is another kind of gradient and here liposomes were prepared in 300 mM ammonium sulfate solution (pH 4.0). To create a gradient, the liposomes were dialyzed against pH 7.5 HEPES buffer or diluted in pH 7.5 HEPES buffer [33, 34].
6.2.1.5 Incorporation of Targeting Agents
Targeted delivery is the utmost requirement of today’s research for effective chemotherapy. The aim is to provide required drug to the affected tissues. It is called active targeting of drugs. It involves the attachment of a ligand to the surface of drug carrier which detects and binds to the diseased cells [35]. Active targeting of drug leads to enhanced drug level at targeted site [36]. In active targeting, nanocarriers, i.e., liposomes are surface modified with specific targeting ligands. The ligand binds to overexpressed receptors on target cell surface. Commonly used ligands for active targeting of liposomes include antibodies, peptides, and small molecules [37, 38].
Nanocarriers can be incorporated covalently or non-covalently with a targeting ligand due to their flexible surface chemistry [39]. Ligands for active targeting have been attached directly to lipids or attached covalently to distal end of PEG-chain [40]. Targeting ligand’s optimal density on nanocarrier is also an important aspect of surface modification. High targeting ligand density in optimum range may increase binding at the target site. Issues like aggregation or raised cost may arise by increasing the ligand density beyond optimum range [41].
Targeting ligands provide better internalization of nanocarriers in tumor cells [39]. Ligand-mediated endocytosis plays a vital role in delivery of drugs and genetic materials, i.e., siRNA and oligonucleotide [41]. Active drug targeting has an added advantage of declining the nonspecific distribution to undesired tissues [36]. Therefore, active targeting plays an important role in efficacy and safety of treatment. Table 6.1 describes some examples of targeting ligands and their targeting sites along with their category and drug delivered with the site and type of cancer.
Peptides as Targeting Ligand
Peptides are short chains made up of amino acid monomers. Peptides are also used as targeting ligands for active drug targeting. A peptide, vasoactive intestinal peptide (VIP) has been used in active drug targeting [53]. A VIP-receptor is relatively a new target for active drug targeting. VIP-receptors are overexpressed in human breast and lung cancer cells [54, 55].
99Tc-HMPAO encapsulated liposomes conjugated with VIP as targeting ligand has been developed for theranostic application. 99Tc-HMPAO is a radiopharmaceutical and used as a diagnostic agent in liposomal formulation. Targeted delivery of VIP-conjugated 99Tc-HMPAO in breast tumor model has shown significantly better uptake in breast cancer cells as compared to non-targeted liposomes [42]. VIP has shown no adverse effect on normal tissues mainly due to the fact that VIP-conjugated-carriers extravasates out at only leaky vasculature on disease site [56].
SP94 is another targeting peptide, used on a nanocarrier based on surface modified liposome called protocell. In protocell, a nanoporous silica core is encapsulated by lipid bilayer. The targeting peptide resulted in 10,000 folds higher binding affinity for hepatocellular carcinoma as compared to normal hepatocytes, in vitro [57].
Folate/Folic Acid as Targeting Ligand
Folate (folic acid) is a small-molecule targeting agent [36]. Folate receptors are overexpressed in various human tumors such as lung, breast, brain, colon, kidney, and ovarian cancers [58,59,60]. Folic acid exhibits high affinity for folate receptors and demonstrated better internalization in tumor cells [61]. Another important feature is folate-receptor location. They are located on apical-membrane of epithelial cells reducing the chances for entry of targeted nanocarrier into normal cells [58, 62].
Folic acid being a small molecule has several advantages over antibody ligands. The advantages include non-immunogenicity, nontoxicity, low cost, small size, and higher stability in preparation, storage, and circulation [63]. In folate receptor targeting of nanocarriers, off-target effect should also be considered [36].
Doxorubicin loaded folate-targeted liposomes have been formulated demonstrating 45-folds higher uptake as compared to non-targeted liposomes. Surface modified targeted liposomes demonstrated 85-folds higher cytotoxicity than non-targeted liposomes [43, 64]. Folate conjugated liposomes having 5-fluorouracil or doxorubicin encapsulated have shown improved biodistribution as compared to unconjugated liposomes [65, 66].
Affisomes as Targeting Ligand
Affibody is a small molecule which has been considered as antibody mimics and used as targeting ligand for nanocarriers, i.e., liposomes. Affibodies are small proteins (approximately 8 kDa) having high stability and solubility. Affibodies are expressed in a bacterial system or produced by peptide synthesis. Affibodies have relatively higher binding affinity as compared to corresponding antibodies [67].
A research group has reported formulation of affisomes by surface modification of thermosensitive liposomes for breast cancer treatment. HER2-specific affibody having 8.3-kDa mass was conjugated to thermosensitive liposomes surface [44]. Similarly, EGFR-specific affibody having 14-kDa mass has been conjugated to PEGylated liposomes for the formulation of affisomes targeted at EGFR-expressing cells. Mitoxantrone loaded affisomes has shown increased cytotoxicity against EGFR-expressing cells [45].
Affibodies have different receptor-binding domains than antibodies that may result in altered outcome. Thus, further research is required to establish the advantage of using affibodies as targeting ligands for nanocarriers, i.e., liposomes [67].
Aptamers as Targeting Ligand
Aptamers are RNA or ssDNA oligonucleotides. They show high affinity and recognize target molecules by hydrogen bonding, electrostatic and hydrophobic interactions [68]. Aptamers have several advantages in their application as targeting ligand due to following reasons: smaller size, higher stability, simple synthesis method, easy modification and show high antigen recognition as compared to other ligands, i.e., nucleotide sequence which can be easily altered for better selectivity [69].
sgc8 aptamer-conjugated liposomes have been developed for leukemia. Liposomes were covalently linked to the aptamer using a PEG spacer. Aptamer-conjugated liposomes bound target cells and released the drug within 30 min after cell incubation [46]. A research group has reported aptamer-conjugated multifunctional liposomes encapsulating cisplatin as a therapeutic agent. AS1411 derived aptamer was used as a targeting ligand for cisplatin encapsulated multifunctional liposomes for targeted delivery in breast cancer. AS1411 derived aptamer due to its high binding affinity to nucleolin (NCL) has exhibited anti-proliferative activity in many tumor cell lines such as MCF-7. Therefore, AS1411 derived aptamer is a promising ligand for targeting of breast cancer [47].
Antibody as Targeting Ligand
Monoclonal antibody (mAb) is a promising ligand for active targeting of drugs using a nanocarrier. The surface modification of a nanocarrier can be done with whole antibody or fragment of mAb, enhancing cellular uptake at the diseased site [36]. Use of antibody fragments i.e. Fab (antigen-binding fragment) and ScFv (single-chain variable fragment) not only reduces immunogenicity but also results in substantial size reduction of ligand favoring development of ligand-targeted nanocarriers [41].
Certain configuration should be maintained for antibody and peptide ligands to have the desired binding affinity. So, a high temperature or organic solvent during preparation should be used with caution [41].
The targeting moiety is attached to PEGylated liposomes to target overexpressed surface receptors, e.g., EGFR, HER 2, carbonic anhydrase IX or receptors in tumor vasculature such as VCAM 1, MT1-MMP.
Epidermal Growth Factor Receptor (EGFR)
EGFR immunoliposomes to target EGFR were prepared. The regression in breast cancer was observed compared to nontargeted liposomes [48]. EGFR targeted liposomes containing two anticancer drugs (oxaliplatin, a platinum derivative and cetuximab, a monoclonal antibody) were prepared. In a colorectal cancer (CRC) xenograft model, an increased drug delivery was observed for targeted formulation as compared to non-targeted liposomes [50].
Human Epidermal Growth Factor Receptor 2 (HER2)
HER2-targeted liposomes containing doxorubicin were developed. The liposomes also contained trastuzumab which targets signaling pathway of HER2. The results showed increased anti-tumorigenesis (inhibition of the development of a neoplasm) with no cardiotoxicity or cardiac dysfunction, while on the other hand conventional anthracycline based cancer therapy is associated with cardiac toxicity [51].
Carbonic Anhydrase IX (CA IX)
CA IX is overexpressed due to hypoxia in cancers such as lung cancer [70]. In a study, anti-carbonic anhydrase immunoliposomes containing docetaxel showed growth inhibition in CA IX positive lung cancer cells as compared to free drug or non-targeted drug containing liposomes. The prepared liposomes have an encapsulation efficiency of ~85% and ~144 nm size [52]. In a review, the potential of targeted CA IX immuoliposomes to deliver anticancer drugs to cancer cells in vivo has been discussed [70].
Vascular Cell Adhesion Molecules (VCAMs)
VCAMs play roles in atherosclerosis (cholesterol or fatty deposition in the arteries) and inflammation. VCAM 1 is overexpressed on cancer vessels [68]. In a study the delivery of anti-inflammatory drugs by liposomes was investigated. Anti-VCAM 1 liposomes were prepared by the coupling of ‘Fab’ with liposomes containing celecoxib (used to treat inflammation) [71].
Matrix Metalloproteases (MMPs)
Several MMPs (enzymes) particularly membrane-type MT1-MMP are involved in angiogenesis (formation of new blood cells) [72]. MT1-MMPs are expressed on cancer cells and angiogenic endothelium cells. Doxorubicin liposomes with ‘Fab’ fragments were prepared. The fragments were used as targeting ligands against MT1-MMP. An enhanced uptake of the liposomes was observed in HT 1080 cancer cells with highly expressed MT1-MMP compared with non-targeted liposomes [49]. In another study, MMP sensitive liposomes were prepared containing: (a) PEG coating, (b) monoclonal antibody (mAb 2C5) for specific targeting to cancer cells, (c) matrix metalloprotease 2-sensitive bond which cleaves in tumor, and (d) cell penetrating peptide such as TATp [73].
6.2.1.6 Stimuli-Sensitive Surface Engineered Liposomes and Their Benefits in Drug Release
Stimuli or triggers have been used to release drugs. The stimuli may be external such as magnetic field or local such as pH. The latter utilizes the local environment of the target/tumor site while the former use an external stimulus such as heat, ultrasound or light [74].
pH Sensitive Liposomes
These liposomes release their drug loads at the acidic environments of tumors. The tumor tissues and inflamed areas have low pH than normal tissues [75].
Various approaches were tried to get pH-sensitive liposomes. In one approach, a pH-sensitive bond (hydrazone bond; =C=N–NH2) was inserted between PEG and bilayer. Such liposomes are stable at neutral pH but release their contents in the acidic environments [75]. In a second approach, fusogenic peptides such as glutamic acid-alanine-leucine-alanine (GALA) were incorporated in liposomes. Such liposomes do not fuse to cells at pH 7.4 but at lower pH fuse into cells and release their contents [76, 77]. In another approach, poly 2-propylacrylic acid (PPAA) based cationic (DOTAP) liposomes were prepared for the delivery of antisense oligonucleotides. PPAA is pH-sensitive hydrophobic polymer. The aim was to silence genes in A2780 human ovarian cancer cells. It was hoped that this system could also be used for the delivery of plasmid-DNA, aptamer, or siRNA [78].
Liposomes containing overexpressed hyaluronic acid (HA) receptors and doxorubicin were reported. These liposomes were also pH-sensitive. In vitro studies showed a higher release in mild acidic conditions than at pH 7.4. Further enhanced antitumor activity was observed in cancer cells with high levels of CD44 than non-targeted liposomes [79].
Temperature Sensitive Liposomes
Thermosensitive liposomes are stable at body temperature but release their contents when temperature is raised. The presence of lysolipids increase permeability in the bilayers. Doxorubicin liposomes containing a lysolipid (10%) were prepared. An increased drug release was observed on producing mild hyperthermia (39–40 °C) [80].
These can be prepared by use of a temperature sensitive polymer. In a study, doxorubicin loaded liposomes containing both temperature sensitive polymer poly(N-isopropylacrylamide) pNiPAAm and pH sensitive polymer 2-propylacrylic acid (PAA) were prepared. The drug was released in the acidic environment of tumors. The drug release was further enhanced by the use of heat which was generated by focussed ultrasound at the specific (cancer) site [81]. Temperature sensitive liposomes containing gadolinium (Gd-DTPA) for MRI and an aptamer (TSLs-AS1411) for specific targeting against cancer cells were developed. At 42 °C, liposomes released gadolinium at the cancer site which was easily detected by MRI. It was suggested that these liposomes could be used for the early detection of cancer [82]. In a study, paclitaxel loaded temperature sensitive liposomes were prepared. The particle size was ~100 nm and encapsulation efficiency was ~95%. The phase transition temperature of the liposomes was 42 °C which was determined by differential scanning calorimetry. At 42 °C, the drug release was higher than at 37 °C [83].
Magnetic Liposomes
These become magnetized on the application of an external magnetic field. This produces instability in the bilayers resulting in the release of drug. In a study, liposomes containing magnetite (Fe3O4, ferriferous oxide) and doxorubicin showed enhanced release of the drug in the tumor due to the application of an external magnetic field of 0.4 T strength [84]. Folate receptor targeted magnetic liposomes loaded with doxorubicin were prepared. The site-specific drug release was observed on the application of alternating magnetic field due to the presence of magnetized particles and hyperthermia produced [85]. Super magnetic cationic liposomes containing anticancer drug paclitaxel showed enhanced drug delivery to the brain of rats. The vesicles were of uniform diameter (20 nm). It was concluded that cationic magnetic liposomes are potential vehicles for the delivery of drugs to the brain [27].
6.2.2 Solid Lipid Nanoparticles (SLNs)
The nanoparticle has a solid lipid matrix. The drug is in the matrix or adsorbed on the surface of the nanoparticle [2]. For hydrophilic drugs, cold homogenization technique is usually used to get SLNs. This technique is also suitable for thermosensitive drugs by dispersing of lipids in the cold aqueous dispersion medium. Hot homogenization technique is used for lipophilic and insoluble drugs. High pressure homogenization at a temperature above the lipids melting point gives o/w emulsion, which gives SLNs after cooling at room temperature [86]. They can also be prepared by supercritical fluid (SCF) technology. SLNs are carriers for drugs, peptides (i.e., cyclosporine A—a cyclic peptide which is an immunosuppressant), proteins (i.e., bovine or human serum albumin BSA/HAS), and antigens (i.e., hepatitis B surface antigen). They are usually administered by IV route and can also be delivered by other routes, i.e., oral, pulmonary, and nasal and transdermal [87].
Their surface can be PEGylated to increase blood circulation time. PEGylated SLNs (having stearic acid lipid core) formulations of methotrexate (MTX) has been reported. The formulations were further evaluated with the help of 99mTc radionuclide. The kinetic studies showed longer blood circulation times for the formulations. SPECT imaging showed efficient tumor uptake of SLNs. The characterization of these nano particles was also done. The particle size found was about 130 nm (via TEM and AFM) and zeta potential was about −34 mV [88]. In another study, paclitaxel (PTX) loaded SLNs (with trimyristin as a solid lipid core and pegylated phospholipid as a stabilizer) were evaluated for biodistribution in organs such as kidneys, heart, and lungs. It was found that the prepared PEGylated SLNs (containing paclitaxel) are similar to Taxol® (a commercial preparation for paclitaxel) because both showed similar biodistribution and circulation times [89].
SLNs have limitations which include low drug entrapment efficiency and possibility of drug degradation during hot dispersion technique. A new generation of SLNs is also known as nanostructured lipid carriers (NLCs) which are free from low drug entrapment efficiency. These have solid matrix with oil nano-compartments containing drug surrounded by a lipid shell. Due to the presence of the nano-compartments, NLCs have high drug loading capacity [2]. Docetaxel-loaded NLCs were produced where the anticancer drug was held in core. These NLCs showed more cytotoxicity than free docetaxel [90].
SLNs have several advantages. They can be called as alternate drug carriers because they can be used in place of liposomes. They can be sterilized by autoclaving or by γ irradiation. Surface modifications can be made to make SLNs site-specific. The ease of scale up to industrial scale production (particularly by hot dispersion technique) is due to the availability of the homogenization production lines for the production of emulsions in pharmaceutical industry. The cost of excipients is low. They can be lyophilized and also spray dried [86].
6.3 Non-lipid Nanocarriers
6.3.1 Niosomes
Niosomes are nonionic surfactant vesicles and, like liposomes, have bilayers. The nonionic surfactant has a polar head and a nonpolar chain (amphiphile). They are formed by the hydration of a nonionic surfactants film. Cholesterol (as rigidizing/stabilizing agent for the bilayer) is added to the nonionic surfactant. The surfactants are biodegradable, inexpensive, and relatively nontoxic. Niosomes are used as an alternate to liposomes as a drug delivery system. Like liposomes, they are multilamellar vesicles (MLVs), large unilamellar vesicles (LUVs), and small unilamellar vesicles (SUVs) and their methods of preparations are similar to those in liposomes. The preparation methods include thin film hydration, ether/alcohol injection, and reverse phase evaporation. The size reduction by extrusion is used to get LUVs.
Proniosomes as a dry product have been prepared which on hydration gives niosomes.
There are some differences between niosomes and liposomes. A phospholipid has two nonpolar chains while nonionic surfactant has one nonpolar chain. Liposomes may be charged or neutral while niosomes are uncharged. Phospholipids can undergo oxidation and hydrolysis. Nonionic surfactants are comparatively chemically stable [86, 91,92,93].
The surface charge is important for the physical stability of niosomes. A charge is produced at the surface of neutral niosomes by the addition of −ve charged dicetyl phosphate, dihexadecyl phosphate or by the +ve charged stearylamine and cetyl pyridinium chloride. The surface charge is measured by zeta potential. As a rough rule, a value greater than 30 mV indicates electrostatic stability while 5–15 mV values indicate limited flocculation and 3–5 mV indicate maximum aggregation. Cationic niosomes containing DC-Cholesterol (+ve charged cholesterol) showed good physical stability and were used for the delivery of genes. A complex is formed between cationic niosomes and −ve charged genes, which helps in the gene transfer [92, 94].
Niosomes have been used for the treatment of various diseases [92]. They are readily taken up by the RES system. They have been successfully used to treat leishmaniasis where parasites attack liver and spleen. Niosomes containing sodium stibogluconate (an antileishmaniasis agent) successfully treated leishmaniasis in mice [95]. Metformin (an oral hypoglycaemic agent) loaded niosomes using Span 40 and Span 60 nonionic surfactants were prepared for oral administration. The best sustained release formulation contained cholesterol and surfactant in equal molar ratio. It was suggested that the sustained release metformin niosomes are useful for the treatment of Type II diabetes [92]. Isoniazid containing niosomes were prepared for the treatment of tuberculosis. The −ve charge was given to niosomes by the use of dicetylphosphate. The drug uptake (about 62%) by macrophage J744 A was observed. The formulations showed decreased drug toxicity and better patient compliance [96]. Niosomes containing paclitaxel (anticancer drug) were prepared for oral administration. The formulations were slow released and formulation with span 40 showed stability against trypsin, chymotrypsin, and pepsin (GIT enzymes) [97]. Niosomes have been used as a topical drug delivery system because of increased drug penetration, sustained drug release, and increased drug stability. In a review, the role of niosomes in dermatology has been discussed [98].
All surface modifications done on liposomes to achieve the goal of targeted drug delivery can be easily done on niosomes. PEGylation of niosomes increase their circulation times. Niosomes containing PEG 4400 and glucose conjugates were used for targeting overexpressed glucose receptors in a carcinoma model. Improved targeting of encapsulated paramagnetic agent such as gadolinium was observed using MRI [99]. Niosomes containing anticancer mitoxantrone and pH sensitive PEG-PMMI-CholC6 copolymer were prepared. The niosomes were more cytotoxic against cancer cell lines (ovarian and breast) than conventional niosomes [100].
6.3.2 Polymeric Nanoparticles
The nanoparticle has a polymeric matrix. The drug is dissolved or dispersed in the matrix or adsorbed on the surface of polymeric nanoparticles (PNPs) [2]. See Fig. 6.3 schematic differences between solid lipid nanoparticle (SLN), polymeric nanoparticle (PNP), nanocapsule and nanostructured lipid carrier (NLC). Solid lipid nanoparticle (SLN) and polymeric nanoparticle (PNP) have different matrix, i.e., lipid solid and polymeric matrix. Similarly, nanocapsule and nanostructured lipid carrier (NLC) have different composition of shell, i.e., polymeric and lipid shell. They are made of natural hydrophilic polymer (proteins such as albumin, gelatin, lectins, and polysaccharides such as chitosan, dextran, and alginate) or synthetic hydrophobic polymers. The synthetic polymers are either pre-polymerized polymer such as poly lactic acid (PLA), poly E-caprolactone (PECL) or a polymer which is further polymerized during the process of nanoparticle formation. The latter compounds include poly isobutylcyanoacylate (PICA) which is a monomer [86].
Schematic differences between solid lipid nanoparticle (SLN), polymeric nanoparticle (PNP), nanocapsule and nanostructured lipid carrier (NLC). Solid lipid nanoparticle (SLN) and polymeric nanoparticle (PNP) have different matrix i.e. lipid solid and polymeric matrix. Similarly, nanocapsule and nanostructured lipid carrier (NLC) have different composition of shell i.e. polymeric and lipid shell
Since few synthetic polymers are nontoxic, this limits their use as drug carriers. Poly alkyl cyanoacrylate (PACA) is a biodegradable and nontoxic monomer [86]. Depending upon the polymerization medium, PACA monomers can be polymerized to give various types of nanocarriers such as nanoparticles, nanospheres, and nanocapsules. These can carry a variety of drugs. PACA first appeared in 1979. A review on PACA nanoparticles was published 33 years later (in 2012) by Georgi Yordanov to show their importance as drug carriers. It was suggested to prepare multifunctional PACA-based nanoparticles (for improved drug action) containing a drug, a contrast agent for biodistribution imaging study and a drug stabilizer. These nanoparticles should be decorated with targeting moieties for active drug targeting at the overexpressed receptors [101]. Polysaccharide conjugated PACA nanoparticles have been formulated in aqueous-medium through redox-radical-emulsion polymerization. Drugs, i.e., doxorubicin can be loaded on surface of such nanoparticles by adsorption [102]. PACA nanospheres have been prepared by zwitterionic polymerization. PACA nanospheres were covalently attached with PEG-chains. Polymerization was done at low pH in the presence of PEG or methoxy PEG [103]. Further clinical trials should be initiated for already developed PEGylated nanoparticles particularly for oral and topical use because of lesser danger of systemic toxicity by these routes [101].
PACA nanoparticles containing doxorubicin showed better drug uptake by cancer cells than free drug. It was also found that these doxorubicin containing PACA nanoparticles were also effective in multidrug resistant (MDR) cancer [104]. Stealth/PEG-coated injectable PACA nanoparicles can be prepared by the use of poly (MePEG cyanoacrylate-co-alkyl cyanoacrylate) copolymer [105]. By modifying PACA nanoparticles surface with polysorbate 80 surfactant, the particles can be targeted into brain because these surface modified particles first adsorb apolipoproteins from plasma and then cross brain endothelium through endothelial cells [101]. Nanoparticle-mediated drug delivery to brain is based on coating of nanoparticles with polysorbates, i.e., polysorbate-80. Drugs may be adsorbed or chemically attached to the nanoparticle surface [101]. Another research group has used polylactic acid (PLA) instead of PACA and reported formulation of PLA (Polylactic acid) nanoparticles coated with polysorbate-80 for targeted delivery to brain. Suspension of surfactant-free nanoparticles (SFNPs) was prepared by modified nano-precipitation method. Suspension was prepared by dissolving PLA in acetonitrile and then transferring the solution slowly into 50% ethanol. Suspension was slowly transferred to water with shaking. Surplus water and organic solvents were removed in a vacuum evaporator. Addition of FITC-dextran was done in formulation of SFNPs and incubation was done for 24 h. After this step, Polysorbate-80 was added into formulation and incubation was done for another 24 h. The weight ratio between Polysorbate-80, FITC-dextran, and nanoparticles was 10:1:10. The experimentation involved preparation of two controls, FITC-dextran-loaded nanoparticles and polysorbate-coated nanoparticles. The controls were prepared in similar way as PLA-nanoparticles, only without addition of Polysorbate-80 and FITC-dextran, respectively [106].
Inhalable effervescent doxorubicin containing nanoparticles based on polybutyl cyanoacrylate (monomer) have been reported for curing lung cancer in mice and it was suggested that this noninvasive route for the administration of anticancer drugs might be useful in the treatment of lung cancer [107].
Polyethylene glycol 100 stearate (PEG-100S) coated SLNs containing levothyroxine (a drug to treat hypothyroidism) were reported with development of an oral drug delivery system for hydrophobic drugs. Electron microscopy showed that the coated SLNs were spherical while photon correlation spectroscopy showed a size of about 187 nm. Differential Scanning Calorimetry (DSC) showed that the nanoparticles were in amorphous state, a state that is appropriate for drug delivery. A reduction in zeta potential from −40 to −23 mV occurred due to PEG coating. A controlled drug release from these nanoparticles was observed due to surface modification by PEG. A comparison of drug release from PEG-coated SLNs and uncoated SLNs has been illustrated in in vitro drug release plot. The plot has shown slow drug release from PEG-coated SLNs due to covering effect of coating layer. PEG coating reduces burst release effect because levothyroxine adsorbed on lipid surface was slowly released from PEG-coated SLNs. In fact, coating layer of PEG provides resistance against diffusion of levothyroxine leading to reduced drug release [108].
6.3.3 Hydrogels
Natural or synthetic hydrophilic polymers in water form a three-dimensional cross-linked mesh or network which can entrap drugs, proteins, peptides, monoclonal antibodies, etc. Due to high affinity for water absorption, they have soft consistency. The cross-links help to keep their physical integrity in the presence of water [109]. Physical integrity of hydrogels is maintained by physical and/or chemical cross-links. Physical crosslinks include tie-points and junctions; while, chemical cross-links includes entanglements and crystallites. Chemical crosslinks provide integrity and network structure to hydrogels [109, 110]. Hydrogels, particularly stimuli-sensitive, (pH and enzyme sensitive) are used as an oral drug delivery system because of the controlled release of entrapped drug to a specific site within GIT [109]. Recently, multi-responsive hydrogels have also been developed which release their contents on the application of more than one stimulus (temperature, electric or magnetic field, pH, etc). Hydrogels are finding use in targeted drug delivery, controlled drug release and soft contact lens, wound repair, targeted cell growth/tissue engineering [111]. By the use of osteoblasts (cells from which bone develops) and alginate hydrogel, an improved bone formation was observed [112].
Hydrogels may be classified on the basis of charge as neutral, amphiphilc, cationic, or anionic. They are also classified on the basis of source such as synthetic, natural, or hybrid made from both natural and synthetic polymers. Another classification is based on the bonding such as covalent bonding or non-covalent bonding. The latter are usually weak attraction forces like hydrogen bonding. pH-responsive hydrogels may be cationic or anionic hydrogels [109].
Natural polymers, alginate, and chitosan have been extensively used for the oral delivery of drugs using hydrogels. Alginate, a linear polysaccharide (anionic polymer from sea weed) forms a mesh or gel due to reaction between −ve charged G blocks of the polymer (the polymer is made of alternate G blocks and M Blocks) and Ca2+ ions. Chitosan (cationic polymer) has amino groups on the polymer which are pH sensitive. At low pH, groups are protonated and are dissolved easily. Due to pH response, chitosan hydrogels have been used for the delivery of drugs to stomach [109].
Paclitaxel-loaded chitosan-based temperature-sensitive hydrogel system was developed for the local treatment of cancer by Biosyntech Inc., Canada. The system consists of chitosan-solution neutralized with b-glycerophosphate, liquid at room temperature but becomes gel at the body temperature. Hydrogel containing paclitaxel was formulated by pouring chitosan-solution on sterilized paclitaxel powder and stirring for 4 h. The mixture was then mixed with glycerophosphate solution. The hydrogel formulated contained 6.4% (w/v) paclitaxel. One intratumoral injection of the hydrogel showed controlled drug delivery for a period of over 30 days and was effective as four Taxol® IV injections against cancer cells (EMT-6) in mice [113]. In another study insulin containing chitosan hydrogels were developed. The sustained release of insulin was observed over a period of 21 days. The gel forming material chitosan/glycerol-phosphate was solution at room temperature, but once injected inside the body by injection it becomes gel [114].
β-Cyclodextrin (β-CD, a biopolymer) based multifunctional supramolecular (supramolecular chemistry is based on weak interaction forces to hold groups of molecules together) hydrogel was prepared where β-CD acts as a host by forming a cavity where guest molecule PNIPAAm binds. It contained β-CD dimmers and PNIPAAm whose chains were modified with light-sensitive azobenzene groups. β-CD is commonly used as a host molecule in supramolecular hydrogel formation while other compounds such as crown ethers can also be used for this purpose [111, 115]. Poly(N-isopropyl acrylamide) (PNIPAAm or pNIPAAM or PNIPAm) is a temperature-sensitive polymer which is hydrophilic below 32 °C [116, 117]. See Fig. 6.4 for temperature sensitive hydrogel.
6.3.4 Dendrimers
Dendrimers are synthetic polymeric macromolecules that have three main parts: a small central core to which are attached branches or shells and the outermost shell/part is composed of surface groups. Overall, dendrimers have tree-like structure.
Polyamidoamine or PAMAM dendrimers are the most common dendrimers and have also been extensively studied. These were first introduced in 1978 by Fritz Vogtle. Their generations (G0 to G10) are now commercially available such as Starburst® dendrimers. They have akyl-diamine internal core such as ethylene diamine (2 carbon core) and 1, 4-diaminobutane (4 carbon core) and with repetitive amidoamine branches or tertiary amine branches and primary amine surface groups. They are becoming spherical and by fourth generation they are three-dimensional spheres. They are synthesized by repetitive polymerization and after fourth generation their dimensions can be precisely controlled. When we go to next generation, an increase in size, molecular weight, and number of end groups occurs, e.g., number of end groups increases from 4, 8, 16, 32, and 64 respectively when we go from G0 to G1, G2, G3, and G4. The end groups may be same such as amine group. Dendrimers with different functional end groups such as hydroxyl, carboxyl, etc., are also available. A second generation means two shells outside the central core with more surface groups than first generation. Dendrimers, because of the void spaces, has been used as vehicles/carriers for nano drug delivery. Various routes of administration such as oral, parenteral, local have been tried [118,119,120,121,122,123,124].
The increased bioavailability of pilocarpine was observed when the drug containing PAMAM dendrimer (with carboxyl or hydroxyl surface groups) eye drops were instilled to the eyes of New Zealand albino rabbit. The study showed the ability of surface modified dendrimers as ocular controlled drug delivery vehicle [125]. Lee et al. [126] conjugated doxorubicin with biodegradable polystyrene dendrimers and found to be effective in the treatment of C-26 colon carcinoma in mice. The long circulation time (half life about 16 h) was achieved through PEGylation. The antitumor effect was similar to equal dose of liposomal doxorubicin injection Doxil® [126]. Amphotericin B (AmB) is an antifungal agent but its use is limited due to its poor water solubility and nephrotoxicity. In a study, its solubility increased in the presence of a third-generation PAMAM dendrimer. The study showed that the drug binding inside dendrimers is responsible for its sustained release [127]. Dendrimers have the ability to cross blood–brain barrier. In a review, the latest research opportunities and challenges in the production of various dendrimers (PAMAM, PPI, and PLL) for the diagnosis and treatment of brain tumor have been discussed [128]. A multifunctional dendrimer may contain one anticancer drug, targeting ligands for overexpressed receptors such as EGFR and a diagnostic agent say for MRI imaging (gadolinium) or gamma imaging(a radionuclide) [121].
6.3.5 Quantum Dots
Quantum dot is composed of a semiconductor material. For medical applications, commonly used quantum dots (QD’s) are cadmium selenide (CdSe), zinc sulfide (ZnS), cadmium telluride (CdTe), indium phosphide (InP), and indium arsenide (InAs). They are fluorescent, spherical nanoparticles or nanocrystals of 2–10 nm size which emit light strongly than fluorescent compounds (organic dyes such as eosin). The surface of QD’s can be PEGylated to increase circulation times. They can be made site-specific by linking suitable ligands [129].
A single quantum dot conjugated to HER2 MAb (monoclonal antibody) has helped in the location of tumors in mice. In vivo, QD’s were followed by the use of confocal microsocope fitted with a high-speed camera [130, 131]. Quantum dots can be incorporated in nano-drug-carriers such as liposomes but long term toxicity particularly in disease state needs to be addressed [132].
QD’s as drug carriers have been reported. QD’s surface is coated with an amphiphilic polymer. The hydrophobic compound, i.e., QD capping compound tri-n-octylphosphine oxide (TOPO) can be placed between quantum dot internal core and the polymer. The hydrophilic therapeutics, i.e., oligodeoxynucleotide (ODN), siRNA are attached to the polymer surface. To the polymer surface, various ligands (aptamers, antibody, and peptide) can also be attached for site-specific targeting. Targeting moieties can be immobilized on hydrophilic portion of amphiphilic polymer by covalent or non-covalent bond. siRNA and peptide have been conjugated to QDs in parallel manner. Targeting ligands, e.g., peptides were prepared and simultaneously linked to QD-surface.
Small interfering RNA containing QD’s have been used to silence genes. The co-transfection of quantum dot and siRNA was done by the use of lipofectamine (a transfection reagent) [133, 134]. In a review, quantum dot preparation, their toxicity, quantum dots as probes and as carriers for targeted delivery have been discussed [135].
6.3.6 Gold Nanoparticles
Gold nanoparticles of different sizes can be prepared by reduction of gold salts in presence of suitable stabilizing agents. Stabilizing agent prevents agglomeration of gold nanoparticles. Many research groups have reported formulation of gold nanoparticles with functional moieties. Functional moieties are anchored with thiolinkers in monolayers of gold nanoparticles. Gold sol (colloidal suspension) containing gold nanoparticles is prepared by the reduction of gold salt such as chloroauric acid (HAuCl4) by a reducing agent such as sodium borohydride (NaBH4) in the presence of appropriate stabilizing agent such as a surfactant, cetyl trimethylammonium bromide (CTAB). In the absence of a stabilizing agent, agglomeration of nanoparticle occurs. Since CTAB is toxic, a thiol capping agent dodecanethiol (a capping agent prevents the growth of nanoparticle) is generally used in its place which also attaches thiol (–SH) groups to the surface of gold particles by forming stable Au:S bonds. Gold particles obtained by this method has 1.5–6 nm diameter and are soluble in nonpolar solvents. The reduction with sodium citrate gives particles of 15–150 nm size [136, 137].
Gold nanoparticles can successfully deliver large biomolecules such as nucleic acids, i.e., RNA or DNA, proteins and peptides, etc [136]. A research group has fabricated DNA-binders through anchoring β-cyclodextrin on periphery of modified oligo(ethylenediamino) gold nanoparticles. The modified gold nanoparticles successfully delivered plasmid-DNA into MCF-7 breast tumor cells [138]. Thiol (–SH) modification of nucleic acid strands has been done for grafting on nanoparticles. A research group has reported conjugation of thiolated-siRNA (SH-siRNA) with gold nanoparticles for cellular delivery [139]. A study has demonstrated gold nanoparticles as carriers of insulin. Gold nanoparticles were stabilized with chitosan. Chitosan-coated gold nanoparticles adsorb insulin on the surface and have been effective in oral delivery of insulin [140].
Based on the surface modification requirement, gold nanoparticle formulations vary in shape and size for different therapeutic applications. Depending upon the method of preparation, various gold nano-forms are produced such as nanospheres, nanorods, nanoshells, and nanocages. Gold nanoshells (50–150 nm) usually have silica core with thin layer of gold, however, pure gold nanoshell can also be prepared. Gold nanorods are 25–45 nm long. Gold nanorods are prepared from chloroauric acid with a gold-seed and a stabilizer, i.e., cetyltrimethylammonium bromide (CTAB). It was found that gold particles with less than 5–6 mm size show enhanced kidney clearance. For drug delivery use, spherical gold nanoparticles are used. The drug is conjugated to the nanoparticles [136, 137]. Further gold cores are nontoxic and biocompatible. Gold nanoparticles can be incorporated into a larger drug carrier such as liposomes for increased diagnostic, therapeutic, and imaging applications. Multifunctional gold particles have also been developed.
To prepare functional nanoparticles, gold nanoparticles are PEGylated to increase circulation times and then various ligands can be attached via thiol-PEG monolayer [141]. Covalent grafting of thiolated-polyethylene glycol (mPEG-SH) was done on gold nanoparticle surface. Thiolated-polyethylene glycol solution was added to citrate-capped gold nanoparticles solution with stirring. Stirring of solution was done for approximately 1 h allowing exchange of citrate-ligands with mPEG-SH. Centrifugation at 15,000 rpm was done for approximately 45 min to remove excessive mPEG-SH. PEG covalently attaches to gold nanoparticles because thiol groups have strong affinity for gold. Colloidal solution obtained was stable for many months [142].
Gold particles have enhanced absorption and scattering of light in near infrared range (NIR), 650–950 nm upon exposure to a near NIR laser source. This property of gold particle is finding use in the diagnosis and treatment of cancer. On exposure to laser source, the scattered light produces hyperthermia in cancer cells due to surface plasmon resonance effect [143]. In a study, a mouse was implanted subcutaneously with colon cancer cells. After IV administration of gold nanoshell-PEG conjugates, the accumulation of gold nanoshells within cancer cells resulted. On exposure to an 808 nm NIR laser, cancer was ablated due to heat [144]. The combined use of NIR laser thermal therapy and MRI imaging via gold nanoshells was effective in the treatment of breast cancer [145]. Since breast cancer is near the skin, the cancer can be easily treated by the limited use of NIR laser. It was concluded that gold particles provide an opportunity/commitment in the treatment of breast cancer [137].
Gold particles as a contrast agent in X-ray CT scans have been extensively studied. Gold nanoparticles provide superior images. They have longer circulation times than conventional iodine based contrast agents enabling prolonged imaging of specific cells [141]. In a study, PEG-coated AuNPs were injected to mice for X-ray CT scan. The scan could be recorded even after 24 h [146]. Gold nanoparticles coated with a Gadolinium chelator Gd-DTDTPA provided images for both CT scan and MRI [147]. van Schooneveld et al. [148] prepared gold/silica nanoparticles for CT scan, MRI, and fluorescent imaging.
6.3.7 Mesoporous Silica Nanoparticles
Mesoporous silica nanoparticles (MSNPs) have emerged as drug delivery devices around two decades ago. They have unique properties: large surface areas, large pore volumes, high loading capacity, biocompatibility, and tunability regarding size and pore diameter. First MSNP was Material MCM-41 (Mobil Composition of Matter no. 41) which was synthesized in Japan and later in the USA at Mobil Corporation. It had 2D hexagonal pore structure, ~60–100 nm size, pore diameter ~1.5–3.5 nm, surface area ~1000 m2 g−1 and pore volume ~1 cm3 g−1. The well-studied MSNPs include MCM-41 and SBA-15. The latter were produced at University of California, Santa Barbara and had pore size ~5–30 nm. MSNPs have surface silanol groups, i.e., free silanol group (≡Si–OH) and geminal silanol group (=S(OH)2) which have affinity for head groups of phospholipids. Thus affinity for adsorbing on cell surfaces that finally leads to endocytosis (transport of substances into cells). The strong silicon-oxygen bonds provide stability to silica nanoparitcles and these are mechanically stable as compared to liposomes.
Surface modification of MSNPs is done by three methods: co-condensation, grafting, and imprint-coating method [149,150,151,152]. They are PEGylated to avoid uptake by the RES system. A research group has reported PEGylation of MSNPs. 25 mg MSNPs was dispersed in 30 ml of pH 4 HCl solution of ethyl-alcohol and water (volume ratio 1:2) with stirring. The solution was termed as solution-A. Dissolution of 100 mg PEGxk-silane was done in 30 ml of ethyl-alcohol. The solution was termed as solution-B. A specific volume of solution-B was added dropwise in solution-A. The mixture of both solutions was vigorously stirred for 24-h and then dried at 100 °C for 12-h in vacuum. The experimentation gave covalently-PEGylated MSNPs [153]. Different ligands can be conjugated to the surface of MSNPs for site-specific targeting of drugs against overexpressed receptors such as Epidermal Growth Factor Receptors (EGFRs) in cancer cells. They are made of constituents such as tetraethyl orthosilicate (ETOS), a silica source and C16TAB (a surfactant) which are not costly. They are used for the controlled release of antibiotics, anti-inflammatory agents, etc. [149,150,151,152].
Stimuli-sensitive MSNPs have been developed for the delivery of drugs at specific sites. The stimuli include external (temperature, electric field, magnetic field, light) and internal (pH, redox potential, enzymes). The stimuli make drug carrier leaky, thereby drug is released at the desired site [154]. In a study, it was found that the combined use of photodynamic therapy using a photosensitizer (porphyrin) and lectin-targeted MSNPs containing anticancer drug (camptothecin) was very effective in the treatment of cancer [155]. Further the combined use of doxorubicin and siRNA employing MSNPs against the target (the P-glycoprotein drug transporter), showed more than 50% efficiency in treating multidrug resistant breast cancer than free drug alone in a xenograft model in mice [156].
6.4 Challenges and Limitations
The drug carriers are not without challenges and limitations. For example, liposomal preparations are advised to be stored at refrigeration temperature, not in a freezer to avoid disruption of lipid bilayers [157]. Solid lipid nanoparticles have low entrapment efficiency [2]. Quantum dots can be incorporated in nano drug carriers such as liposomes but long-term toxicity issue needs to be addressed [132]. A lot of research has been carried out on nanocarriers but more research is required for optimization of nanocarriers using cutting edge surface engineering techniques to tailor a nanocarrier for treatment of fatal diseases, i.e., cancer. In this regard, multifunctional nanocarriers obtained by surface modification of a nanocarrier with a targeting ligand, pro-drug, and imaging agent is the latest approach. Research on multifunctional nanocarriers should be focused for more efficient treatment of diseases. Each nanocarrier should be considered unique and must be individually evaluated. Systematic studies on various aspects of nanocarrier’s surface modification need to be carried out before proceeding to clinical trials [158].
PEGylation has significantly improved circulation time of liposomes. PEGylation has reduced the liposomal uptake by RES but it does not completely inhibit liposomal uptake [159]. Liposomal uptake is also possible through pathways which are independent of opsonization suggesting more research on surface modification of liposomes for further increment in circulation time [160, 161]. Modification of liposomes by various synthetic components may lead to antibody production against various components of liposomes, if recognized as a foreign particle by the body [162,163,164]. Some liposomal formulations trigger innate immune-response leading to hypersensitivity syndrome called complement activation-related pseudoallergy (CARPA) [165]. Development of new surface modification techniques can resolve the issues and have the potential to decrease immunogenic-reactions to liposome based treatment preventing their loss of efficacy, altered pharmacokinetics, and toxicity.
Impressive-progress has been made in preparation and targeting of nanoparticles for treatment of diseases but only few nanoparticle-based drugs are commercially available. This is due to following main reasons. Nanoparticles have low drug loading capacity, i.e., less than 5% drug with respect to nanocarrier weight. Burst release of drug after administration is another challenge, needs to be addressed. Burst release is rapid drug-fraction release of adsorbed or anchored drug from nanocarrier’s surface leading to lower therapeutic response [166].
Hydrogels typically have higher water content resulting in rapid drug release from gel-matrix especially hydrophilic drugs. The drug release profile of hydrogels is usually shorter than some other nanocarriers. Sensitive molecules, e.g., antibody, proteins, and nucleic acid are deactivated by interaction with hydrogel. Similarly, hydrogel mediated delivery of hydrophobic drugs also requires improvement. Complexation or pre-encapsulation of biomolecules may be helpful in addressing these challenges [167].
Gold nanoparticle is a promising nanocarrier. However, challenges such as toxicity, biodistribution, and pharmacokinetics needs to be addressed [158]. Biodistribution of gold- nanoparticles is often affected by the route of administration. Therefore, nanomaterials should be properly characterized and in vivo studies can be carried out in animal models with apt statistical analysis [168]. Gold nanoparticles have low inherent toxicity [169]. More research on interaction of gold nanoparticles with tumor microenvironment should be done to reduce their toxicity by adapting suitable surface engineering techniques. Detection of toxicity of gold nanoparticle, i.e., core, capping agents and ligands is another research area, needs to be explored. Certain ligands attached to gold nanoparticles cause toxicity, e.g., cationic ligands leads to moderate toxicity [170].
Surface engineering has played a vital role in formulation and optimization of nanocarriers for better targeting, cellular-internalization (endocytosis), and therapeutic response. Surface engineering aided in addressing the challenges and limitations associated with nanocarriers. It can provide multifunctional properties to these nanocarriers, i.e., imaging, prognosis, diagnosis, and additionally theranostics. Research on surface modification and engineering based on the incorporation of desired bioactive compound to get anticipated results will lead to achieve a targeted drug and gene delivery with enhanced drug loading capacity and better cellular uptake for prolonged duration of action.
References
Khodabandehloo H, Zahednasab H, Hafez AA (2016) Nanocarriers usage for drug delivery in cancer therapy. Iran J cancer Prev 9(2):e3966
Calixto G, Fonseca-Santos B, Chorilli M, Bernegossi J (2014) Nanotechnology-based drug delivery systems for treatment of oral cancer: a review. Int J Nanomed 9:3719
Ruiz ME, Gantner ME, Talevi A (2014) Applications of nanosystems to anticancer drug therapy (Part II. Dendrimers, micelles, lipid-based nanosystems). Recent Pat Anticancer Drug Discov 9:99–128
Drbohlavova J, Chomoucka J, Adam V et al (2013) Nanocarriers for anticancer drugs–new trends in nanomedicine. Curr Drug Metab 14:547–564
Bangham AD, Standish MM, Watkins JC (1965) Diffusion of univalent ions across the lamellae of swollen phospholipids. J Mol Biol 13:238–252
Sessa G, Weissmann G (1968) Phospholipid spherules (liposomes) as a model for biological membranes. J Lipid Res 9:310–318
Pattni BS, Chupin VV, Torchilin VP (2015) New developments in liposomal drug delivery. Chem Rev 115:10938–10966
Madni MA, Sarfraz M, Rehman M et al (2014) Liposomal drug delivery: a versatile platform for challenging clinical applications. J Pharm Pharm Sci 17:401–426
Patil YP, Jadhav S (2014) Novel methods for liposome preparation. Chem Phys Lipids 177:8–18
Vemuri S, Yu C-D, Wangsatorntanakun V, Roosdorp N (1990) Large-scale production of liposomes by a microfluidizer. Drug Dev Ind Pharm 16:2243–2256
http://www.microfluidicscorp.com. Accessed 6 Apr 2016
Sollohub K, Cal K (2010) Spray drying technique: II. Current applications in pharmaceutical technology. J Pharm Sci 99:587–597
Chen C, Han D, Cai C, Tang X (2010) An overview of liposome lyophilization and its future potential. J Control Release 142:299–311
Karn PR, Cho W, Park HJ et al (2013) Characterization and stability studies of a novel liposomal cyclosporin a prepared using the supercritical fluid method: comparison with the modified conventional Bangham method. Int J Nanomed 8:365–377
Nag OK, Awasthi V (2013) Surface engineering of liposomes for stealth behavior. Pharmaceutics 5:542–569
Balazs DA, Godbey W, Balazs DA, Godbey W (2011) Liposomes for use in gene delivery. J Drug Deliv 2011:1–12
Mirafzali Z Immunoliposomes. http://www.liposomes.org/2011/09/immunoliposomes.html
Fraley R, Subramani S, Berg P, Papahadjopoulos D (1980) Introduction of liposome-encapsulated SV40 DNA into cells. J Biol Chem 255:10431–10435
Fraley R, Straubinger RM, Rule G et al (1981) Liposome-mediated delivery of deoxyribonucleic acid to cells: enhanced efficiency of delivery related to lipid composition and incubation conditions. Biochemistry 20:6978–6987
Tan Y (2001) Sequential injection of cationic liposome and plasmid DNA effectively transfects the lung with minimal inflammatory toxicity. Mol Ther 3:673–682
Hoekstra SAD (2001) Cationic lipid-mediated transfection in vitro and in vivo. Mol Membr Biol 18:129–143
Straubinger RM, Papahadjopoulos D (1983) [32] Liposomes as carriers for intracellular delivery of nucleic acids. Methods Enzymol 101:512–527
Wyrozumska P, Meissner J, Toporkiewicz M et al (2015) Liposome-coated lipoplex-based carrier for antisense oligonucleotides. Cancer Biol Ther 16:66–76
Li X, Ding L, Xu Y et al (2009) Targeted delivery of doxorubicin using stealth liposomes modified with transferrin. Int J Pharm 373:116–123
Masserini M (2013) Nanoparticles for brain drug delivery. ISRN Biochem 2013:1–8
Zhao M, Chang J, Fu X et al (2012) Nano-sized cationic polymeric magnetic liposomes significantly improves drug delivery to the brain in rats. J Drug Target 20:416–421
Li S, Goins B, Zhang L, Bao A (2012) Novel multifunctional theranostic liposome drug delivery system: construction, characterization, and multimodality MR, near-infrared fluorescent, and nuclear imaging. Bioconjug Chem 23:1322–1332
Huang Y, Hemmer E, Rosei F, Vetrone F (2016) Multifunctional liposome nanocarriers combining upconverting nanoparticles and anticancer drugs. J Phys Chem B 120(22):4992–5001
Ren L, Chen S, Li H et al (2016) MRI-guided liposomes for targeted tandem chemotherapy and therapeutic response prediction. Acta Biomater 35:260–268
Mayer LD, Bally MB, Cullis PR (1986) Uptake of adriamycin into large unilamellar vesicles in response to a pH gradient. Biochim Biophys Acta Biomembr 857:123–126
Gubernator J (2011) Active methods of drug loading into liposomes: recent strategies for stable drug entrapment and increased in vivo activity. Expert Opin Drug Deliv 8:565–580
Fenske DB, Cullis PR (2007) Encapsulation of drugs within liposomes by pH-gradient techniques. In: Gregoriadis G (ed) Liposome technol. Entrapment drugs other mater into liposomes, 3rd edn. Informa Healthcare, New York, pp 27–50
Haran G, Cohen R, Bar LK, Barenholz Y (1993) Transmembrane ammonium sulfate gradients in liposomes produce efficient and stable entrapment of amphipathic weak bases. Biochim Biophys Acta 1151:201–215
Torchilin VP (2010) Passive and active drug targeting: drug delivery to tumors as an example. Springer, Berlin Heidelberg, pp 3–53
Lim SB, Banerjee A, Önyüksel H (2012) Improvement of drug safety by the use of lipid-based nanocarriers. J Control Release 163:34–45
Torchilin VP (2007) Micellar nanocarriers: pharmaceutical perspectives. Pharm Res 24:1–16
Joshi MD, Müller RH (2009) Lipid nanoparticles for parenteral delivery of actives. Eur J Pharm Biopharm 71:161–172
Benhabbour SR, Luft JC, Kim D et al (2012) In vitro and in vivo assessment of targeting lipid-based nanoparticles to the epidermal growth factor-receptor (EGFR) using a novel Heptameric Z EGFR domain. J Control Release 158:63–71
Patel JD, O’Carra R, Jones J et al (2007) Preparation and characterization of nickel nanoparticles for binding to his-tag proteins and antigens. Pharm Res 24:343–352
Feng L, Mumper RJ (2013) A critical review of lipid-based nanoparticles for taxane delivery. Cancer Lett 334:157–175
Dagar S, Krishnadas A, Rubinstein I et al (2003) VIP grafted sterically stabilized liposomes for targeted imaging of breast cancer: in vivo studies. J Control Release 91:123–133
Gabizon A, Tzemach D, Gorin J et al (2010) Improved therapeutic activity of folate-targeted liposomal doxorubicin in folate receptor-expressing tumor models. Cancer Chemother Pharmacol 66:43–52
Puri A, Kramer-Marek G, Campbell-Massa R et al (2008) HER2-specific affibody-conjugated thermosensitive liposomes (Affisomes) for improved delivery of anticancer agents. J Liposome Res 18:293–307
Beuttler J, Rothdiener M, Müller D et al (2009) Targeting of epidermal growth factor receptor (EGFR)-expressing tumor cells with sterically stabilized affibody liposomes (SAL). Bioconjug Chem 20:1201–1208
Kang H, O’Donoghue MB, Liu H, Tan W (2010) A liposome-based nanostructure for aptamer directed delivery. Chem Commun (Camb) 46:249–251
Cao Z, Tong R, Mishra A et al (2009) Reversible cell-specific drug delivery with aptamer-functionalized liposomes. Angew Chem Int Ed 48:6494–6498
Mamot C, Drummond DC, Noble CO et al (2005) Epidermal growth factor receptor-targeted immunoliposomes significantly enhance the efficacy of multiple anticancer drugs in vivo. Cancer Res 65:11631–11638
Hatakeyama H, Akita H, Ishida E et al (2007) Tumor targeting of doxorubicin by anti-MT1-MMP antibody-modified PEG liposomes. Int J Pharm 342:194–200
Zalba S, Contreras AM, Haeri A et al (2015) Cetuximab-oxaliplatin-liposomes for epidermal growth factor receptor targeted chemotherapy of colorectal cancer. J Control Release 210:26–38
Reynolds JG, Geretti E, Hendriks BS et al (2012) HER2-targeted liposomal doxorubicin displays enhanced anti-tumorigenic effects without associated cardiotoxicity. Toxicol Appl Pharmacol 262:1–10
Chi B, Wong K, Qin L (2014) Carbonic anhydrase IX-directed immunoliposomes for targeted drug delivery to human lung cancer cells in vitro. Dovepress, Auckland, pp 993–1001
Önyüksel H, Jeon E, Rubinstein I (2009) Nanomicellar paclitaxel increases cytotoxicity of multidrug resistant breast cancer cells. Cancer Lett 274:327–330
Moody TW, Gozes I (2007) Vasoactive intestinal peptide receptors: a molecular target in breast and lung cancer. Curr Pharm Des 13:1099–1104
Gespach C, Bawab W, De Cremoux P, Calvo F (1988) Pharmacology, molecular identification and functional characteristics of vasoactive intestinal peptide receptors in human breast cancer cells. Cancer Res 48:5079–5083
Koo OM, Rubinstein I, Onyuksel H (2005) Role of nanotechnology in targeted drug delivery and imaging: a concise review. Nanomed Nanotechnol Biol Med 1:193–212
Ashley CE, Carnes EC, Phillips GK et al (2011) The targeted delivery of multicomponent cargos to cancer cells by nanoporous particle-supported lipid bilayers. Nat Mater 10:389–397
Low PS, Antony AC (2004) Folate receptor-targeted drugs for cancer and inflammatory diseases. Adv Drug Deliv Rev 56:1055–1058
Elnakat H, Ratnam M (2004) Distribution, functionality and gene regulation of folate receptor isoforms: Implications in targeted therapy. Adv Drug Deliv Rev 56:1067–1084
Alexis F, Basto P, Levy-Nissenbaum E et al (2008) HER-2-targeted nanoparticle-affibody bioconjugates for cancer therapy. ChemMedChem 3:1839–1843
Leamon CP, Pastan I, Low PS (1993) Cytotoxicity of folate-Pseudomonas exotoxin conjugates toward tumor cells: contribution of translocation domain. J Biol Chem 268:24847–24854
Low PS, Kularatne SA (2009) Folate-targeted therapeutic and imaging agents for cancer. Curr Opin Chem Biol 13:256–262
Wu J, Liu Q, Lee RJ (2006) A folate receptor-targeted liposomal formulation for paclitaxel. Int J Pharm 316:148–153
Lee RJ, Low PS (1995) Folate-mediated tumor cell targeting of liposome-entrapped doxorubicin in vitro. BBA Biomembr 1233:134–144
Shmeeda H, Mak L, Tzemach D et al (2006) Intracellular uptake and intracavitary targeting of folate-conjugated liposomes in a mouse lymphoma model with up-regulated folate receptors. Mol Cancer Ther 5:818–824
Gupta Y, Jain A, Jain P, Jain SK (2007) Design and development of folate appended liposomes for enhanced delivery of 5-FU to tumor cells. J Drug Target 15:231–240
Puri A, Loomis K, Smith B et al (2009) Lipid-based nanoparticles as pharmaceutical drug carriers: from concepts to clinic. Crit Rev Ther Drug Carrier Syst 26:523–580
Deshpande PP, Biswas S, Torchilin VP (2013) Current trends in the use of liposomes for tumor targeting. Nanomedicine (Lond) 8:1509–1528
Edwards KA, Wang Y, Baeumner AJ (2010) Aptamer sandwich assays: human α-thrombin detection using liposome enhancement. Anal Bioanal Chem 398:2645–2654
Helena Ng HL, Lu A, Lin G et al (2014) The potential of liposomes with carbonic anhydrase IX to deliver anticancer ingredients to cancer cells in vivo. Int J Mol Sci 16:230–255
Il KD, Lee S, Lee JT et al (2011) Preparation and in vitro evaluation of anti-VCAM-1-Fab’-conjugated liposomes for the targeted delivery of the poorly water-soluble drug celecoxib. J Microencapsul 28:220–227
Handsley MM, Edwards DR (2005) Metalloproteinases and their inhibitors in tumor angiogenesis. Int J Cancer 115:849–860
Zhu L, Kate P, Torchilin VP (2012) Matrix metalloprotease 2-responsive multifunctional liposomal nanocarrier for enhanced tumor targeting. ACS Nano 6:3491–3498
Bibi S, Lattmann E, Mohammed AR, Perrie Y (2012) Trigger release liposome systems: local and remote controlled delivery? J Microencapsul 29:262–276
Torchilin VP (2014) Multifunctional, stimuli-sensitive nanoparticulate systems for drug delivery. Nat Rev Drug Discov 13:813–827
Li W, Nicol F, Szoka FC (2004) GALA: a designed synthetic pH-responsive amphipathic peptide with applications in drug and gene delivery. Adv Drug Deliv Rev 56:967–985
Yao L, Daniels J, Wijesinghe D et al (2013) PHLIP®-mediated delivery of PEGylated liposomes to cancer cells. J Control Release 167:228–237
Peddada LY, Garbuzenko OB, Devore DI et al (2014) Delivery of antisense oligonucleotides using poly(alkylene oxide)-poly(propylacrylic acid) graft copolymers in conjunction with cationic liposomes. J Control Release 194:103–112
Paliwal SR, Paliwal R, Agrawal GP, Vyas SP (2016) Hyaluronic acid modified pH-sensitive liposomes for targeted intracellular delivery of doxorubicin. J Liposome Res 2104:1–12
Mills JK, Needham D (2006) Temperature-triggered nanotechnology for chemotherapy: rapid release from lysolipid temperature-sensitive liposomes. Small 2:5–8
pH and Temperature Sensitive Polymer Modified Liposomes. http://www.bu.edu/medal/research/chemotherapy/. Accessed 11 May 2016
Zhang K, Liu M, Tong X et al (2015) Aptamer-modified temperature-sensitive liposomal contrast agent for magnetic resonance imaging. Biomacromolecules 16:2618–2623
Wang Z-Y, Zhang H, Yang Y et al (2016) Preparation, characterization, and efficacy of thermosensitive liposomes containing paclitaxel. Drug Deliv 23:1222–1231
Nobuto H, Sugita T, Kubo T et al (2004) Evaluation of systemic chemotherapy with magnetic liposomal doxorubicin and a dipole external electromagnet. Int J Cancer 109:627–635
Pradhan P, Banerjee R, Bahadur D et al (2010) Targeted magnetic liposomes loaded with doxorubicin. In: Weissig V (ed) Liposomes, vol 605. Methods molecular biology. Humana Press, New Jersey, pp 279–293
Vyas SP, Khar RK (2002) Nanoparticles. In: Targeted & controlled drug delivery. CBS Publishers & Distributors, New Delhi, pp 331–386
Almeida AJ, Souto E (2007) Solid lipid nanoparticles as a drug delivery system for peptides and proteins. Adv Drug Deliv Rev 59:478–490
Kakkar D, Dumoga S, Kumar R et al (2015) PEGylated solid lipid nanoparticles: design, methotrexate loading and biological evaluation in animal models. Med Chem Commun 6:1452–1463
Li R, Eun JS, Lee MK (2011) Pharmacokinetics and biodistribution of paclitaxel loaded in pegylated solid lipid nanoparticles after intravenous administration. Arch Pharm Res 34:331–337
Liu D, Liu Z, Wang L et al (2011) Nanostructured lipid carriers as novel carrier for parenteral delivery of docetaxel. Colloids Surf B Biointerfaces 85:262–269
Kuotsu K, Karim K, Mandal A et al (2010) Niosome: a future of targeted drug delivery systems. J Adv Pharm Technol Res 1:374
Sankhyan A, Pawar P (2012) Recent trends in niosome as vesicular drug delivery system. J Appl Pharm Sci 2:20–32
Huang Y, Yu F, Liang W (2010) Niosomal delivery system for macromolecular drugs. In: Fanun M (ed) Colloids in drug delivery. CRC Press, Boca Raton, pp 355–364
Baillie AJ, Coombs GH, Dolan TF, Laurie J (1986) Non-ionic surfactant vesicles, niosomes, as a delivery system for the anti-leishmanial drug, sodium stibogluconate. J Pharm Pharmacol 38:502–505
Singh G, Dwivedi H, Saraf SK, Saraf SA (2011) Niosomal delivery of isoniazid—development and characterization. Trop J Pharm Res 10:203–210
Taylor MJ, Tanna S, Sahota T (2010) In vivo study of a polymeric glucose-sensitive insulin delivery system using a rat model. J Pharm Sci 99:4215–4227
Hamishehkar H, Rahimpour Y, Kouhsoltani M (2013) Niosomes as a propitious carrier for topical drug delivery. Expert Opin Drug Deliv 10:261–272
Luciani A, Olivier J-C, Clement O et al (2004) Glucose-receptor MR imaging of tumors: study in mice with PEGylated paramagnetic niosomes. Radiology 231:135–142
Tila D, Yazdani-Arazi SN, Ghanbarzadeh S et al (2015) PH-sensitive, polymer modified, plasma stable niosomes: promising carriers for anti-cancer drugs. EXCLI J 14:21–32
Yordanov G (2012) Poly (alkyl cyanoacrylate) nanoparticles as drug carriers: 33 years later. Bulg J Chem 1:61–73
Alhareth K, Vauthier C, Gueutin C et al (2011) Doxorubicin loading and in vitro release from poly(alkylcyanoacrylate) nanoparticles produced by redox radical emulsion polymerization. J Appl Polym Sci 119:816–822
Zhang Y, Zhu S, Yin L et al (2008) Preparation, characterization and biocompatibility of poly(ethylene glycol)-poly(n-butyl cyanoacrylate) nanocapsules with oil core via miniemulsion polymerization. Eur Polym J 44:1654–1661
Vauthier C, Dubernet C, Chauvierre C et al (2003) Drug delivery to resistant tumors: the potential of poly(alkyl cyanoacrylate) nanoparticles. J Control Release 93:151–160
Peracchia MT, Desmae D, Couvreur P, Angelo J (1997) Synthesis of a novel poly (MePEG cyanoacrylate-co-alkyl cyanoacrylate) amphiphilic copolymer for nanoparticle technology. Macromolecules 30:846–851
Sun W, Xie C, Wang H, Hu Y (2004) Specific role of polysorbate 80 coating on the targeting of nanoparticles to the brain. Biomaterials 25:3065–3071
Roa WH, Azarmi S, Al-Hallak MHDK et al (2011) Inhalable nanoparticles, a non-invasive approach to treat lung cancer in a mouse model. J Control Release 150:49–55
Kashanian S, Rostami E (2014) PEG-stearate coated solid lipid nanoparticles as levothyroxine carriers for oral administration. J Nanoparticle Res 16(3):1–10
Sharpe LA, Daily AM, Horava SD, Peppas NA (2014) Therapeutic applications of hydrogels in oral drug delivery. Expert Opin Drug Deliv 11:901–915
Peppas NA, Bures P, Leobandung W, Ichikawa H (2000) Hydrogels in pharmaceutical formulations. Eur J Pharm Biopharm 50:27–46
Knipe JM, Peppas NA (2014) Multi-responsive hydrogels for drug delivery and tissue engineering applications. Regen Biomater 1:57–65
Augst AD, Kong HJ, Mooney DJ (2006) Alginate hydrogels as biomaterials. Macromol Biosci 6:623–633
Ruel-Gariépy E, Shive M, Bichara A et al (2004) A thermosensitive chitosan-based hydrogel for the local delivery of paclitaxel. Eur J Pharm Biopharm 57:53–63
Khodaverdi E, Tafaghodi M, Ganji F et al (2012) In vitro insulin release from thermosensitive chitosan hydrogel. AAPS PharmSciTech 13:460–466
Guan Y, Zhao H-B, Yu L-X et al (2014) Multi-stimuli sensitive supramolecular hydrogel formed by host–guest interaction between PNIPAM-Azo and cyclodextrin dimers. RSC Adv 4:4955–4959
Poly(N-isopropylacrylamide). https://en.wikipedia.org/wiki/Poly(N-isopropylacrylamide
Sun J, Tan H (2013) Alginate-based biomaterials for regenerative medicine applications. Materials (Basel) 6:1285–1309
Arseneault M, Wafer C, Morin J-F (2015) Recent advances in click chemistry applied to dendrimer synthesis. Molecules 20:9263–9294
Hannah H (2008) The role of dendrimers in topical drug delivery. Pharm Technol 32:88–98
Abbasi E, Aval S, Akbarzadeh A et al (2014) Dendrimers: synthesis, applications, and properties. Nanoscale Res Lett 9:247–256
Leiro V, Garcia JP, Tomás H, Pêgo AP (2015) The present and the future of degradable dendrimers and derivatives in theranostics. Bioconjug Chem 26:1185–1197
PAMAM Dendrimers. http://www.dendritech.com/pamam.html
PAMAM Dendrimers. http://www.sigmaaldrich.com/materials-science/material-science-products.html?TablePage=9539880
PAMAM Dendrimers. http://www.andrewschemservices.com/
Vandamme TF, Brobeck L (2005) Poly(amidoamine) dendrimers as ophthalmic vehicles for ocular delivery of pilocarpine nitrate and tropicamide. J Control Release 102:23–38
Lee CC, Gillies ER, Fox ME et al (2006) A single dose of doxorubicin-functionalized bow-tie dendrimer cures mice bearing C-26 colon carcinomas. Proc Natl Acad Sci USA 103:16649–16654
Jose J, Rn C (2016) Prolonged drug delivery system of an antifungal drug by association with polyamidoamine dendrimers. Int J Pharm Investig 6:123
Dwivedi N, Shah J, Mishra V et al (2016) Dendrimer-mediated approaches for the treatment of brain tumor. J Biomater Sci Polym Ed 5063:1–24
Krishnan SR, George SK (2014) Nanotherapeutics in cancer prevention, diagnosis and treatment. In: Gowder S (ed) Pharmacology and therapeutics. InTech, Rijeka. doi:10.5772/58419
Singh R, Lillard JW (2009) Nanoparticle-based targeted drug delivery. Exp Mol Pathol 86:215–223
Tada H, Higuchi H, Wanatabe TM, Ohuchi N (2007) In vivo real-time tracking of single quantum dots conjugated with monoclonal anti-HER2 antibody in tumors of mice. Cancer Res 67:1138–1144
Ghaderi S, Ramesh B, Seifalian AM (2011) Fluorescence nanoparticles “quantum dots” as drug delivery system and their toxicity: a review. J Drug Target 19:475–486
Qi L, Gao X (2008) Emerging application of quantum dots for drug delivery and therapy. Expert Opin Drug Deliv 5:263–267
Chen AA, Derfus AM, Khetani SR, Bhatia SN (2005) Quantum dots to monitor RNAi delivery and improve gene silencing. Nucleic Acids Res 33(22):e190
Yong KT, Wang Y, Roy I et al (2012) Preparation of quantum dot/drug nanoparticle formulations for traceable targeted delivery and therapy. Theranostics 2:681–694
Ghosh P, Han G, De M et al (2008) Gold nanoparticles in delivery applications. Adv Drug Deliv Rev 60:1307–1315
Lee J, Chatterjee DK, Lee MH, Krishnan S (2014) Gold nanoparticles in breast cancer treatment: promise and potential pitfalls. Cancer Lett 347:46–53
Wang H, Chen Y, Li X-Y, Liu Y (2006) Synthesis of oligo(ethylenediamino)-beta-cyclodextrin modified gold nanoparticle as a DNA concentrator. Mol Pharm 4:189–198
Oishi M, Nakaogami J, Ishii T, Nagasaki Y (2006) Smart PEGylated gold nanoparticles for the cytoplasmic delivery of siRNA to induce enhanced gene silencing. Chem Lett 35:1046–1047
Bhumkar DR, Joshi HM, Sastry M, Pokharkar VB (2007) Chitosan reduced gold nanoparticles as novel carriers for transmucosal delivery of insulin. Pharm Res 24:1415–1426
Mieszawska AJ, Mulder WJM, Fayad ZA, Cormode DP (2013) Multifunctional gold nanoparticles for diagnosis and therapy of disease. Mol Pharm 10:831–847
Rahme K, Chen L, Hobbs RG et al (2013) AuNP92-PEGylated gold nanoparticles: polymer quantification as a function of PEG lengths and nanoparticle dimensions. RSC Adv 3:6085
Huang X, Jain PK, El-Sayed IH, El-Sayed MA (2007) Gold nanoparticles: interesting optical properties and recent applications in cancer diagnostics and therapy. Nanomedicine (Lond) 2:681–693
O’Neal DP, Hirsch LR, Halas NJ et al (2004) Photo-thermal tumor ablation in mice using near infrared-absorbing nanoparticles. Cancer Lett 209:171–176
Hirsch LR, Stafford RJ, Bankson JA et al (2003) Nanoshell-mediated near-infrared thermal therapy of tumors under magnetic resonance guidance. Proc Natl Acad Sci USA 100:13549–13554
Cai Q-Y, Kim SH, Choi KS et al (2007) Colloidal gold nanoparticles as a blood-pool contrast agent for X-ray computed tomography in mice. Invest Radiol 42:797–806
Alric C, Taleb J, Le DG et al (2008) Contrast agents for both X-ray computed tomography and magnetic resonance imaging. J Am Chem Soc 130:5908–5915
Van Schooneveld MM, Cormode DP, Koole R et al (2010) A fluorescent, paramagnetic and PEGylated gold/silica nanoparticle for MRI, CT and fluorescence imaging. Contrast Media Mol Imaging 5:231–236
Slowing II, Vivero-Escoto JL, Wu C-W, Lin VSY (2008) Mesoporous silica nanoparticles as controlled release drug delivery and gene transfection carriers. Adv Drug Deliv Rev 60:1278–1288
Roggers R, Kanvinde S, Boonsith S, Oupický D (2014) The practicality of mesoporous silica nanoparticles as drug delivery devices and progress toward this goal. AAPS PharmSciTech 15:1163–1171
Kwon S, Singh RK, Perez RA et al (2013) Silica-based mesoporous nanoparticles for controlled drug delivery. J Tissue Eng 4(1):2041731413503357
Mesoporous silica. https://en.wikipedia.org/wiki/Mesoporous_silica
He Q, Zhang J, Shi J et al (2010) The effect of PEGylation of mesoporous silica nanoparticles on nonspecific binding of serum proteins and cellular responses. Biomaterials 31:1085–1092
Martínez-carmona M, Colilla M, Vallet-regí M (2015) Smart mesoporous nanomaterials for antitumor therapy. Nanomaterials 5:1906–1937
Gary-Bobo M, Hocine O, Brevet D et al (2012) Cancer therapy improvement with mesoporous silica nanoparticles combining targeting, drug delivery and PDT. Int J Pharm 423:509–515
Meng H, Mai WX, Zhang H et al (2013) Codelivery of an optimal drug/siRNA combination using mesoporous silica nanoparticles to overcome drug resistance in breast cancer in vitro and in vivo. ACS Nano 7:994–1005
JOINT FORMULARY COMMITTEE (2014) Section 8: malignant disease and immunosuppression. In: British National Formulary, 68th edn (Sep 2014–Mar 2015). BMJ Group and Pharmaceutical Press, London, pp 562–645
Arvizo R, Bhattacharya R, Mukherjee P (2010) Gold nanoparticles: opportunities and challenges in nanomedicine. Expert Opin Drug Deliv 7:753–763
Ishida T, Harashima H, Kiwada H (2001) Interactions of liposomes with cells in vitro and in vivo: opsonins and receptors. Curr Drug Metab 2:397–409
Laverman P, Carstens MG, Storm G, Moghimi SM (2001) Recognition and clearance of methoxypoly(ethyleneglycol)2000-grafted liposomes by macrophages with enhanced phagocytic capacity: Implications in experimental and clinical oncology. Biochim Biophys Acta Gen Subj 1526:227–229
Sawant RR, Torchilin VP (2012) Challenges in development of targeted liposomal therapeutics. AAPS J 14:303–315
Dams ET, Laverman P, Oyen WJ et al (2000) Accelerated blood clearance and altered biodistribution of repeated injections of sterically stabilized liposomes. J Pharmacol Exp Ther 292:1071–1079
Ishida T, Masuda K, Ichikawa T et al (2003) Accelerated clearance of a second injection of PEGylated liposomes in mice. Int J Pharm 255:167–174
Ishida T, Ichihara M, Wang X et al (2006) Injection of PEGylated liposomes in rats elicits PEG-specific IgM, which is responsible for rapid elimination of a second dose of PEGylated liposomes. J Control Release 112:15–25
Moghimi SM, Hunter C (2001) Capture of stealth nanoparticles by the body’s defences. Crit Rev Ther Drug Carr Syst 18:24
Couvreur P (2013) Nanoparticles in drug delivery: past, present and future. Adv Drug Deliv Rev 65:21–23
Hoare TR, Kohane DS (2008) Hydrogels in drug delivery: progress and challenges. Polymer (Guildf) 49:1993–2007
Hillyer JF, Albrecht RM (2001) Gastrointestinal persorption and tissue distribution of differently sized colloidal gold nanoparticles. J Pharm Sci 90:1927–1936
Shukla R, Bansal V, Chaudhary M et al (2005) Biocompatibility of gold nanoparticles and their endocytotic fate inside the cellular compartment: a microscopic overview. Langmuir 21:10644–10654
Goodman CM, McCusker CD, Yilmaz T, Rotello VM (2004) Toxicity of gold nanoparticles functionalized with cationic and anionic side chains. Bioconjug Chem 15:897–900
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Riaz, M.K., Tyagi, D., Yang, Z. (2017). Surface Engineering: Incorporation of Bioactive Compound. In: Yan, B., Zhou, H., Gardea-Torresdey, J. (eds) Bioactivity of Engineered Nanoparticles. Nanomedicine and Nanotoxicology. Springer, Singapore. https://doi.org/10.1007/978-981-10-5864-6_6
Download citation
DOI: https://doi.org/10.1007/978-981-10-5864-6_6
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-10-5863-9
Online ISBN: 978-981-10-5864-6
eBook Packages: Chemistry and Materials ScienceChemistry and Material Science (R0)