Abstract
Nitric oxide has become one of the most studied molecules in medical history. Almost 30 years after the discovery of endothelium-derived relaxing factor as nitric oxide, there are now over 150,000 published papers on the chemistry and biology of nitric oxide. Over the past 30 years, we have learned much more about the production and regulation of NO as a ubiquitous signaling molecule in humans and other life forms. The first signaling pathway discovered from the oxidation of l-arginine and subsequent activation of soluble guanylyl cyclase by NO may only represent a fraction of the biological effects of NO. Understanding all the signaling aspects of NO will allow for better development of diagnostics and therapeutics.
The original version of this chapter was revised. An erratum to this chapter can be found at DOI 10.1007/978-3-319-46189-2_23
An erratum to this chapter can be found at http://dx.doi.org/10.1007/978-3-319-46189-2_23
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Soluble guanylyl cyclase
- Cyclic GMP
- Nitrite
- Nitrate
- Heme iron nitric oxide synthase
- EDRF
- Nitric oxide synthase
- l-arginine
- Nitrosothiols
- Inflammation
- Free radical
-
Nitric oxide is a key signaling molecule in the cardiovascular, immune, and nervous systems.
-
There are three enzymes that produce NO from l-arginine, two are constitutive and produce low amounts of NO for short periods of time, the other inducible and can produce high levels of NO for prolonged periods.
-
Nitric oxide reacts primarily with transition metals and other free radicals.
-
A number of diseases are associated with dysregulation of NO production.
-
The nitric oxide pathway is a key target for development of new therapies.
Introduction
The discovery in the 1980s of the mammalian biosynthesis of nitric oxide (•NO, nitrogen monoxide) and its roles in the immune [1–5], cardiovascular [6–9], and nervous [10] systems established a startling new paradigm in the history of cellular signaling mechanisms. Prior to this discovery, it was essentially inconceivable that cells would intentionally produce a toxic molecule as a messenger; •NO is a common air pollutant, a constituent of cigarette smoke, and a toxic gas, which appears in the exhaust of motor cars and jet airplanes, causes acid rain, and destroys the ozone layer. Amazingly, despite this nasty reputation, it is now known that •NO is one of a family of reactive signaling molecules, which includes both reactive nitrogen and reactive oxygen species [11, 12]. This is, in fact, a hallmark example of the propensity of nature to seek out and exquisitely utilize the unique properties of unusual molecules. Its best recognized role, for which the 1998 Nobel Prize in Physiology or Medicine was awarded to Robert Furchgott, Louis Ignarro, and Ferid Murad, is as a signal molecule in the vasculature and specifically in the control of blood pressure. In addition to this role, •NO is one of the most important signaling molecules in the body and is involved in virtually every organ system where it is responsible for modulating an astonishing variety of effects. Indeed, there have been over 150,000 publications on •NO, more than half of which have appeared in the last 12 years. •NO has been shown to be involved in and affect (just to list a few major examples) neurotransmission, memory, stroke, glaucoma and neural degeneration, pulmonary hypertension, penile erection, angiogenesis, wound healing, atherogenesis, inflammation such as arthritis, nephritis, colitis, autoimmune diseases (diabetes, inflammatory bowel disease), invading pathogens, tumors, asthma, tissue transplantation, septic shock, platelet aggregation and blood coagulation, sickle cell disease, gastrointestinal motility, hormone secretion, gene regulation, hemoglobin delivery of oxygen, stem cell proliferation and differentiation, and bronchodilation.
Here, we will focus on the physiology/pathophysiology of the three major organ systems originally documented for the importance of •NO as a signal, the cardiovascular, immune, and nervous systems, and understandings relevant to nitrite/nitrate as particularly related to the cardiovascular system. Other important pathologies where •NO also plays critical roles, including cancer [13], sepsis [14], diabetes [15], and lung [16] and kidney injury [17], are covered elsewhere.
Enzymatic NO Synthesis
The first •NO synthase (NOS ) to be isolated and the gene sequenced was the enzyme from rat cerebellum, by Bredt and Snyder in 1991 [18, 19]. Since then, the genes for the two other major NOS isoforms have been identified and cloned, revealing that all three enzymes perform the same basic enzymatic reaction. These heme- and flavin-containing enzymes utilize electrons from NADPH and produce •NO by the mixed-function oxidation of one of the two equivalent guanidine nitrogen atoms of the amino acid l-arginine (Fig. 13.1) [20, 21]. The three major isoforms are most commonly referred to as the neuronal (“nNOS” or NOS1), inducible (“iNOS” or NOS2), and endothelial (“eNOS” or NOS3), classified according to their initially identified location and function. nNOS and eNOS enzymes are constitutive, cytosolic, and Ca2+/calmodulin dependent, and release •NO for short time periods in response to receptor or physical stimulation. The •NO released by these enzymes acts as a signaling mechanism underlying several physiological responses depending on when and where it is produced and producing relatively small amounts of •NO. The other enzyme type (iNOS) is induced after activation of macrophages, endothelial cells, and a number of other cells by endotoxin and pro-inflammatory cytokines, and once expressed, synthesizes NO for long periods of time and at higher levels than the constitutive enzymes. Furthermore, the inducible form is Ca2+ independent since calmodulin is already bound to the enzyme. It is now appreciated that eNOS is found in other cells and tissues beside the endothelium; nNOS is found in other cells than neurons; iNOS is found constitutively in some tissues; and there are inducible forms of both eNOS and nNOS, adding confusion to the nomenclature as it was first described. In addition, the activity and subcellular location of all three enzymes is regulated by a variety of different posttranslational modifications, especially eNOS [22]. Finally, there is evidence of NOS associated with erythrocytes [23] and also mitochondria [24, 25], although these associations are less well characterized.
Interconversions Between •NO and Nitrite/Nitrate
Formation of Nitrite/Nitrate from •NO
The major pathway for •NO metabolism is the stepwise oxidation to nitrite and nitrate [26]. Quantitatively, the major mechanism for •NO metabolism in man in vivo is via reaction with oxyhemoglobin [27]. In plasma or other physiological fluids or buffers, •NO is oxidized almost completely to nitrite, where it remains stable for several hours. •NO and nitrite are rapidly oxidized to nitrate in whole blood. The half-life of nitrite (NO2 −) in human blood is about 110 s when infused systemically [26] or about 90–120 min when taken orally [28]. Nitrate (NO3 −), on the other hand, has a circulating half life of 5–8 h. For years, both nitrite and nitrate have been used as surrogate markers of •NO production in biological tissues. During fasting conditions with low intake of nitrite/nitrate, enzymatic •NO formation from NOS accounts for the majority of nitrite [29], and plasma nitrite reflects eNOS activity [30]. On the basis of these and other studies, it was believed that •NO is acutely terminated by oxidation to nitrite and nitrate; however, as described later, it is now appreciated that nitrite and/or nitrate can recapitulate • NO physiology.
Formation of • NO from Nitrite/Nitrate
There are several reports of the biological production of •NO from nitrite which predate the discovery in mammals. The first identification of enzymatic synthesis of •NO was in the 1970s where it was shown that it is produced in plants by the enzymatic reduction of NO2 − as an intermediate in nitrogen fixation [31, 32], although the resulting heme-nitrosyl most probably does not release free •NO. In 1983, formation of •NO from nitrite was proposed as the mechanism whereby nitrite prevents botulism [33]. •NO is a central intermediate in microbial denitrification [34].
It is now recognized that there are non-NOS sources of •NO [35]. The first description of such •NO formation was in 1994 when two independent groups demonstrated •NO detection from acidified nitrite in the stomach [36, 37], which is predictable based on well-established chemistry of acidified nitrite but which may not apply to other, less acidic bodily compartments [38]. Nitrate per se is not metabolized by mammals; however, commensal facultative bacteria in the oral cavity can convert nitrate to nitrite and is a significant source of circulating nitrite. As described in more detail later, there are multiple mechanisms for the reductive conversion of nitrite to •NO that may be therapeutically effective.
Biochemical Actions and Targets of •NO
Reactivity and Diffusivity of •NO
Although commonly characterized as a “highly reactive radical,” the biochemistry of •NO is surprisingly simple since it is determined by one major principle: •NO undergoes chemistry that serves to stabilize its unpaired electron. There are major consequences of this chemistry: (1) •NO interacts almost exclusively with only two species, molecules that also contain an unpaired electron (thus allowing the electrons to pair); and (2) transition metals to which •NO binds, thereby stabilizing the unpaired electron owing to special interactions with the electrons on metals in their d orbitals. As a result of these two phenomena, in general •NO essentially does not react with molecules with covalent bonds (all electrons paired) that do not contain metal ions.
Being an extremely small, uncharged molecule with limited reactivity, •NO is highly diffusible in biological milieu; at first glance, these properties would seem to violate the concept of specificity required for a biological signal and was initially a startling (and controversial) concept. Indeed, modeling studies predicted that with sustained •NO production (such as from iNOS), a gradient of •NO will extend great distances from the source, depending on the half-life of •NO [39, 40]. However, the actions of •NO in some systems are quite spatially confined, and, in fact, are highly localized to the immediate environment surrounding NOS [41]. The explanation for this confinement of a highly diffusible molecule is unclear, but could be explained by rapid reactivity at the source, e.g., with superoxide [42].
Intracellular •NO Targets: Transition Metals
The interaction between •NO and its primary protein target, the enzyme, soluble guanylyl cyclase (cGC), which mediates target cell responses such as vascular smooth muscle relaxation and platelet inhibition, has been well characterized although controversies remain [43, 44]. After entering the target cell, •NO binds to the heme moiety of sGC and activates the enzyme by inducing a conformational change that displaces iron out of the plane of the porphyrin ring [45]. sGC then catalyzes the production of cyclic GMP from GTP to elevate cyclic GMP. Cyclic GMP then triggers a cascade of intracellular events that culminate in a reduction in calcium-dependent vascular smooth muscle tone by inactivating myosin light chain kinase or MLCK [46]. MLCK normally phosphorylates the regulatory set of myosin light chains. This phosphorylation event activates cross-bridge cycling and initiates contraction. cGMP modulates MLCK activity by activating a cGMP-dependent protein kinase that phosphorylates MLCK . Phosphorylation of MLCK diminishes its affinity for calmodulin and, as a consequence, decreases the phosphorylation of myosin light chain, which, in turn, stabilizes the inactive form of myosin. In this manner, cGMP may induce vasorelaxation by indirectly decreasing myosin light chain-dependent myosin activation.
In addition to the heme iron of sGC , there are three other major intracellular iron targets of •NO. As mentioned previously, the reaction of •NO with intraerythrocytic hemoglobin (either oxygenated or deoxygenated) is quantitatively the most important in vivo reaction of •NO [27], the major product of which is nitrate. A very minor reaction comparatively is the formation of S-NO-hemoglobin , which is S-nitrosated at a specific cysteine residue (cysβ93), and which has been proposed as a major mechanism of blood flow and tissue oxygenation modulation in response to hypoxia [47, 48]. This controversial proposal is discussed in more detail later.
Another target of •NO is the mitochondrion , which dates back to 1979 [49]. At relatively low levels, relevant to •NO signaling, •NO binds to the same mitochondrial site(s) as O2, thus exhibiting competitive kinetics with O2 [50]. This competition may have critically important consequences in intracellular signaling events, including the generation of reactive oxygen species (see later), as well as major influences on cellular and tissue distribution of •NO and of O2, and possible contributions to tissue hypoxic vasodilation [40, 51].
Intracellular nonheme iron (NHI) is also a target for •NO. One effect of such •NO binding is to produce iron–•NO complexes, which are visible by electron paramagnetic resonance (EPR) spectroscopy . Observation of these signals was important in developing concepts of cellular actions of •NO in the early stages of the mammalian •NO field [52, 53]. It was initially believed that the origin of the NHI under these conditions is mitochondrial iron–sulfur centers, which are targets of •NO under conditions of high inflammatory levels of •NO, but quantitative and kinetic evidence now appears to support the so-called chelatable iron pool as the iron source [54].
Intracellular •NO Targets: Radicals
•NO reacts at near-diffusion controlled rates with other radicals, and these reactions can have either damaging or protective effects due to three consequences: (1) removal of •NO, (2) removal of the radical with which •NO reacts, and (3) formation of products that may itself also be very reactive [55]. Arguably the most important •NO/radical reaction (certainly the most discussed in the literature, especially with reference to the effects of •NO in disease conditions) is the extremely rapid reaction with the superoxide anion radical (O 2 •− ). O 2 •− is perhaps the “canonical” reactive oxygen species; the discovery in 1969 of the enzyme that detoxifies it (superoxide dismutase) by McCord and Fridovich is responsible for the birth of the entire field [56]. So it might seem that the •NO + O 2 •− reaction would only be protective, but, in fact, the two other effects of the reaction are in principle damaging because it decreases the beneficial activities of •NO and the product (peroxynitrite, ONOO− ) is potentially an even more damaging ROS than O 2 •− [57, 58]. There are several well-established sources of O 2 •− that are relevant to the modulation of •NO signaling, as described later.
Current Aspects of •NO in Health and Disease: A Janus-Faced Molecule
The Cardiovascular System
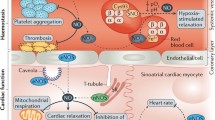
The endothelium is the thin layer of cells that line the interior surface of blood vessels, forming an interface between circulating blood in the lumen and the rest of the vessel wall. Endothelial cells line the entire circulatory system, from the heart to the smallest capillary. Endothelial dysfunction is defined by the loss of normal biochemical processes carried out by the endothelium, and is a hallmark for a plethora of vascular diseases, and often leads to atherosclerosis. Endothelial dysfunction is very common, for example, in patients with diabetes mellitus, hypertension, or other chronic pathophysiological conditions with a substantial cardiovascular component. Abnormal vasodilation as an important component of endothelial dysfunction arises from variations in blood flow observed in patients with atherosclerosis compared with healthy subjects [59]. In healthy subjects, activation of eNOS causes vasodilation in both muscular conduit vessels and resistance arterioles. In contrast, in subjects with atherosclerosis, similar stimulation yields attenuated vasodilation in peripheral vessels and causes paradoxical vasoconstriction in coronary arteries, thus indicating a decrease in the availability of bioactive •NO [60, 61]. Interestingly, endothelial dysfunction can be demonstrated in patients with risk factors for atherosclerosis in the absence of atherosclerosis itself [62, 63]. In addition, feeding healthy volunteers a high-fat meal leads to endothelial vasodilator dysfunction in a time span of just a few hours [64]. Experimental and clinical studies provide evidence that detective endothelial •NO function is not only associated with all major cardiovascular risk factors, such as hyperlipidemia, diabetes, hypertension, smoking, and the severity of established atherosclerosis, but also has a profound predictive value for future atherosclerotic disease progression [59]. This concept is illustrated in Fig. 13.2. Thus, the dysfunctional eNOS/•NO pathway (including both •NO formation and also disappearance) provides an ideal target for therapeutic or preventive intervention once •NO homeostasis is better understood in atherosclerosis.
The innermost lining of the blood vessel is a single layer of endothelial cells . Healthy endothelial cells produce nitric oxide to combat disease and regulate blood pressure. Endothelial dysfunction is defined by the inability of the vessels to transduce •NO activity, either by inability to produce it from l-arginine or inactivation by superoxide (O2 •−) [104]
Potential consequences or manifestations of endothelial dysfunction include increased vascular contraction to vasoconstrictors, such as endothelin-1, thromboxanes, and serotonin [65]; enhanced thrombus formation; and exacerbated smooth muscle cell (SMC) proliferation and migration [66]. Decreased •NO production may be the result of oxidized LDL-mediated displacement of eNOS from plasmalemmal caveolae, thereby inhibiting acetylcholine-induced activation of the enzyme [67]. Moreover, decreased •NO increases the tendency for lesion progression by enhancing vascular smooth muscle proliferation and migration, augmenting platelet activation and thrombosis, possibly participating in intravascular neovascularization, and favoring adverse lipid modification [68]. Once lesions have developed, endothelial dysfunction may exacerbate the risk of developing clinical events. Impaired endothelium may abnormally reduce vascular perfusion, produce factors that decrease plaque stability, and augment the thrombotic response to plaque rupture [69]. Augmentation of •NO or restoration of NOS function seems a logical means by which to inhibit atherosclerosis. However, overexpression of endothelial NOS accelerates lesion formation in apoE-deficient mice [70] demonstrating that enhanced NOS-derived •NO may not always be beneficial, or, perhaps, a reflection of local uncoupling of eNOS in the plaque leading to superoxide generation by eNOS. Supplementation with tetrahydrobiopterin (BH4) reduced the lesion size to those seen in Apo E knockout mice revealing the requirement of enzyme cofactors and consistent with BH4’s role in preventing enzymatic uncoupling (see later). Even with BH4 supplementation, there was still no effect on lesion development.|
The physiological effects of •NO extend well beyond the vascular endothelium. Radomski et al. [71] have shown that human platelets contain a NOS that is activated when platelets are stimulated to aggregate. Thus, platelets themselves also have the enzymatic capacity to synthesize •NO with both a constitutive and inducible form of NOS identified in human megakaryoblasts [72]. NOS activity increases with platelet activation, and this response appears to modulate platelet aggregation, thereby potentially limiting the self-amplification of platelet thrombus formation in vivo [73, 74]. It was also reported early on that human neutrophils inhibit platelet aggregation by releasing an •NO-like factor [75]. These antithrombotic properties of the endothelium may be a consequence of the synergistic action of •NO and prostacyclin. Radomski et al. [76] have shown the synergistic antiaggregatory effects of •NO and prostacyclin on platelets. •NO and prostacyclin may act in concert to oppose local vasospasm or thrombus formation at sites where platelets aggregate and the coagulation cascade is activated. It has also been proposed that the antiplatelet effects of endothelium-derived •NO may prevent thromboembolic events during administration of potent prostacyclin inhibitors such as aspirin [77]. In this regard, •NO acts as an anti-inflammatory molecule.
Endothelial dysfunction in the setting of cardiovascular risk factors has been shown to be, at least in part, dependent on the production of ROS, such as superoxide, and the subsequent decrease in vascular availability of nitric oxide. ROS production has been demonstrated to occur in the endothelial cell and also within the media and adventitia, all of which may impair •NO signaling within vascular tissue to endothelium-dependent but also endothelium-independent vasodilators [59]. More recent experimental but also clinical studies point to the pathophysiological importance of xanthine oxidase, vascular NADPH oxidases, mitochondria, and uncoupled endothelial nitric oxide synthase as significant enzymatic superoxide sources. These phenomena are described later.
The mitochondrial respiratory chain can be a major source of superoxide. During aerobic metabolism, the oxidation/reduction energy of mitochondrial electron transport is converted to the high-energy phosphate bond of ATP via a multicomponent electron transfer complex. Molecular oxygen serves as the final electron acceptor for cytochrome c oxidase (complex IV), the terminal component of the respiratory chain, and is ultimately reduced to water (H2O). Up to 1–4 % of O2 even under normal physiological conditions may be incompletely reduced, resulting in O2 •− formation, mainly at complex I (NADH coenzyme Q reductase ) and complex III (ubiquinol Cyt c reductase ) [78]. Increased mitochondrial O2 •− generation can be enhanced in certain conditions such as conditions of metabolic perturbation, hypoxia–reoxygenation, and ischemia–reperfusion, where the enhanced O2 •− is at least partially responsible for an increase in endothelial permeability [79].
Xanthine oxidoreductase (XOR) is a ubiquitous metalloflavoprotein found in one of two interconvertible yet functionally distinct forms, namely, xanthine dehydrogenase (XD ), which is constitutively expressed in vivo, and XO, which is generated by the posttranslational modification of XD [80, 81]. Functionally, both XD and XO catalyze oxidation of hypoxanthine to xanthine and xanthine to urate. However, whereas XD requires NAD+ as an electron acceptor, XO instead requires the reduction of molecular O2, thereby generating O2 •− . The conversion of XD to XO occurs either through reversible thiol oxidation of sulfhydryl residues on XD or via irreversible proteolytic cleavage of a segment of XD during hypoxia, ischemia, or in the presence of various proinflammatory mediators [80], e.g., tumor necrosis factor-α (TNF-α). Dysfunctional or uncoupled NOSs are also a source of O2 •− . The essential NOS cofactor, tetrahydrobiopterin (BH4), appears to have a key role in regulating NOS function by “coupling” the reduction of molecular O2 to l-arginine oxidation as well as maintaining the stability of NOS dimers [81]. Thus, BH4 availability may be a crucial factor in the balance between •NO and O2 •− generation by eNOS. Furthermore, BH4 itself is highly susceptible to oxidative degradation, and the initial oxidative loss of BH4 in response to increased ROS production by NADPH oxidases (see later) has been shown to amplify oxidative stress through the resulting loss of •NO production and increased NOS-dependent O2 •− generation [82]. In addition to increased catabolism or degradation, another reason for BH4 depletion may be its reduced synthesis or incomplete reduction of BH2 back to BH4.
In recent years, it has become apparent that endothelial cells and other nonphagocytic cells constitutively express an O2 •− -generating enzyme analogous to the phagocyte NADPH oxidase of neutrophils [83]. All the classical neutrophil oxidase components are expressed in endothelial cells, but the enzyme nevertheless exhibits several major differences from the neutrophil oxidase; for example, it continuously generates a low level of O2 •− even in unstimulated cells, although its activity can be further increased by several agonists; and a substantial proportion of the O2 –• generated by the enzyme is produced intracellularly, whereas neutrophil oxidase O2 –• generation occurs mainly in the extracellular compartment.
Normal physiological processes are continuously generating superoxide and other oxygen radicals that can quickly and effectively inactivate •NO. Fortunately there are a number of antioxidant systems, both enzymatic and nonenzymatic, that help to limit the amount of ROS produced to preserve •NO activity. It appears the production of •NO is a war of attrition. There are many circumstances in the production pathway that can diminish its output, but there are also many physiological factors that can quickly inactivate •NO once it has been successfully produced.
ROS such as superoxide are produced in abundance by the dysfunctional endothelium, and limitation of ROS generation increases the availability of •NO. For this reason antioxidant therapy with vitamin C and cholesterol-lowering therapy with statins (HMG-CoA reductase inhibitors ) improve endothelial function, at least acutely [59]. An alternative approach to increasing levels of bioactive •NO and to improving endothelial function is to increase the synthesis of •NO. Enhanced synthesis of •NO can be achieved by increased availability of agonists that stimulate release of •NO from the endothelial cells, like bradykinin, assuming a healthy endothelium and sufficient cofactor to supply the NOS enzymes. Another straightforward approach to increasing •NO synthesis is to provide additional substrate (l-arginine) to the endothelial cell [84]. However, in some patients this may not be a beneficial strategy. l-arginine supplementation in postinfarct and PAD patients causes these patients to worsen and actually increases mortality for as yet unclear reasons [85, 86]. Furthermore, l-arginine takes part in protein synthesis, endocrine functions, wound healing, and erectile function. It is not regarded as an essential amino acid as the adult human is able to synthesize l-arginine de novo via the urea cycle. In adults, the synthesis of l-arginine results in l-citrulline, a by-product of glutamine metabolism in the gut and in the liver. Citrulline is excreted into the circulation and is reabsorbed in the kidney and converted to l-arginine. l-citrulline is reformed if l-arginine is shunted through the NOS pathway and is itself shunted through the partial urea cycle to regenerate l-arginine illustrating the requirement of argininosuccinate synthase (ASA) and argininosuccinate lyase (ASL) in the NOS pathway [87]. This protein complex, including ASA, ASL, and NOS, provides a spatial and temporal molecular shuttling of critical NO substrate and cofactors to allow for more efficient NO production. This protein complex also reveals that cells use intracellular pools of l-citrulline, which is then converted to l-arginine, rather than utilizing extracellular l-arginine to make NO. The dietary application of l-arginine is the basic determinant of the l-arginine level in plasma, as the biosynthesis of l-arginine is not able to balance inadequate intake or deficiency. Providing supplementation of substrate to individuals with inadequate •NO, therefore, has been suggested as a rational approach to increase •NO production by the •NO synthase [84], provided the enzyme is functional and the protein complex described earlier is intact [87].
Erythrocytes as Delivery Agents for •NO
The phenomenon of hypoxic vasodilation , whereby peripheral vessels dilate under decreased O2 conditions, has been known for more than a century but the mechanism underlying it is not clear; in particular it is not clear as to what the “sensor” is that detects hypoxia and initiates the response. In 1995 Ellsworth et al. [88] proposed that the sensor is intraerythrocytic hemoglobin , which responds by increasing release of ATP to induce vasodilation. Shortly thereafter, Jia et al. [47] advanced a surprising alternative mechanism for the hemoglobin signal: rather than simply being an irreversible sink for •NO, hemoglobin within the red blood cell actually reacts with the •NO in the lung (where O2 levels are high) forming S-nitrosohemoglobin (SNOHb) and releases it in vascular beds where O2 is low (hypoxia). Important evidence for this hypothesis was the report that the levels of SNOHb are higher in the arterial than the venous circulation, implying liberation of •NO upon transit through the hypoxic region (called the A/V transit ). Gladwin et al. [89] subsequently found no change in SNOHb upon A/V transit; however, there was significant consumption of plasma nitrite upon induction of hypoxia by exercise, and subsequent work suggested that deoxygenation of hemoglobin induces its reaction with nitrite to produce •NO. These three mechanisms of hypoxic vasodilation (ATP, SNOHb, and nitrite) are highly controversial and may in fact be interrelated [90, 91]. What appears to be less controversial is the critical and essential role of NO in the delivery of oxygen to the periphery [92].
Independent of its validity as the mechanism for hypoxic vasodilation , a series of recent studies have shown that nitrite administration is remarkably salutatory for a variety of clinically significant applications, including myocardial infarction, stroke, hypertension, angiogenesis, and organ transplantation [93]. In addition, a report by Kleinbongard et al. [94] demonstrates that plasma nitrite levels progressively decrease with increasing cardiovascular risk burden indicating a reduction in nitric oxide produced. Risk factors considered include age, hypertension, smoking, and hypercholesterolemia , conditions all known for reduced availability of •NO. Although a correlation exists in plasma, it is not known whether the situation is mirrored in the heart or other tissue at risk for ischemic injury or disease. If so, tissue nitrite may serve as an index of risk, and restoring tissue nitrite may act as a first line of defense for protecting organs from ischemic and/or I/R injury. Since a substantial portion of steady-state nitrite concentrations in blood and tissue are derived from dietary sources, modulation of nitrite intake may provide a first line of defense for cardiovascular disease [93].
The Immune System
•NO is also generated by macrophages and neutrophils as part of the human immune response. •NO is toxic to bacteria and other human pathogens. It is the inducible isoform of NOS that is responsible for macrophage •NO production. Inducible NOS has been found in many cell types, including macrophages [5], and is immunologically activated by exposure to bacterial endotoxin or pro-inflammatory cytokines, such as interleukin-1, or interferon-gamma [95, 96] and tumor necrosis factor. The presence of iNOS message or protein can serve as a biomarker for inflammation in tissues. The iNOS protein may remain present for several days [97]. At these high concentrations and flux rates, •NO is cytotoxic and plays a key role in the immune response of macrophages to bacteria and other pathogens. Antimicrobial activity and •NO production parallel tumor necrosis factor activity, and a strong correlation exists between antimicrobial activity and production of l-Arg-derived •NO by cytokine-activated cells observed during in vitro studies [98]. The precise mechanism of •NO-mediated bactericidal and tumoricidal activity is unknown, but these observations suggest that macrophage •NO production contributes to nonspecific immunity. •NO from activated macrophages may be responsible for the profound loss of vascular tone seen in septic patients [99]. It is this relative overproduction of •NO and the subsequent vasodilation that are thought to mediate •NO’s pathophysiological role during sepsis and multiorgan failure during hypovolemia and hypoxia. Despite the rapid progress in our understanding of the complex physiological and pathophysiological processes involving •NO, uncertainties remain with regard to the critical cellular targets of •NO cytotoxicity, the relative importance of different •NO redox states and carrier molecules, and the importance of the •NO antimicrobial system in human phagocytes. Ultimately, the immunoregulatory and vasoregulatory activities of •NO may prove to be just as important as its antimicrobial properties during infection.
The Nervous System
In the central nervous system, •NO is a neurotransmitter that underpins several functions, including the formation of memory. As in other organ systems, this •NO pathway may also play a role in the pathology of the central nervous system. The NOS isoform in the nervous system is activated by glutamate acting on N-methyl-d-aspartate receptors . In a matter of seconds, the glutamate-induced increase in intracellular calcium concentration activates NOS via the calcium/calmodulin interaction as previously described. Under most circumstances, eNOS and nNOS are constitutive in the sense that their activation does not require new enzyme synthesis. However, both forms of NOS are inducible in that new enzyme synthesis occurs primarily under conditions of traumatic or pathological insult. The calcium influx that accompanies prolonged NMDA receptor activation is associated with degeneration of the neurons through a mechanism(s) that involves •NO, but is still not precisely clear [100]. Thus, the dichotomy of both the protective and deleterious actions of •NO is again revealed in the nervous system.
In the periphery, there is a widespread network of nerves, previously recognized as nonadrenergic and noncholinergic (NANC) , that operate through a •NO-dependent mechanism to mediate some forms of neurogenic vasodilation and regulate various gastrointestinal, respiratory, and genitourinary tract functions, as well as autonomic innervation of smooth muscle in the gastrointestinal tract, the pelvic viscera, the airways, and other systems [101]. NOS has been detected in the gastric mucosa, and •NO appears to play a role in protecting the gastric mucosa during physiologic stress by acting as an endogenous vasodilator and thus supporting mucosal blood flow [102]. The exact mechanism of •NO’s protective effect is unclear, but may relate to vasodilation, inhibition of platelet aggregation in the gastric microvasculature, or a protective effect on the epithelial cells themselves [103]. However, alternative means to enhance •NO in the periphery and stomach will certainly provide benefit to a number of conditions.
Conclusion
Nitric oxide research has expanded rapidly in the past 30 years, and the roles of •NO in physiology and pathology have been extensively studied. The pathways of •NO synthesis, signaling, and metabolism in vascular biological systems have been and continue to be a major area of research. As a gas (in the pure state and under standard temperature and pressure) and free radical with an unshared electron, •NO participates in various biological processes. Understanding its production, regulation, and molecular targets will be essential for the development of new therapies for various pathological conditions characterized by an imbalanced production and metabolism of •NO.
References
Wagner D, Tannenbaum S. Enhancement of nitrate biosynthesis by Escherichia coli lipopolysaccharide. In: Magee PN, editor. Nitrosamines and human cancer. New York: Cold Spring Harbor Press; 1982. p. 437–43.
Hegesh E, Shiloah J. Blood nitrates and infantile methemoglobinemia. Clin Chim Acta. 1982;125(2):107–15.
Stuehr DJ, Marletta MA. Mammalian nitrate biosynthesis: mouse macrophages produce nitrite and nitrate in response to Escherichia coli lipopolysaccharide. Proc Natl Acad Sci U S A. 1985;82(22):7738–42.
Hibbs Jr JB, Taintor RR, Vavrin Z. Macrophage cytotoxicity: role for L-arginine deiminase and imino nitrogen oxidation to nitrite. Science. 1987;235(4787):473–6.
Marletta MA, Yoon PS, Iyengar R, Leaf CD, Wishnok JS. Macrophage oxidation of L-arginine to nitrite and nitrate: nitric oxide is an intermediate. Biochemistry. 1988;27(24):8706–11.
Arnold WP, Mittal CK, Katsuki S, Murad F. Nitric oxide activates guanylate cyclase and increases guanosine 3′:5′-cyclic monophosphate levels in various tissue preparations. Proc Natl Acad Sci U S A. 1977;74(8):3203–7.
Ignarro LJ, Buga GM, Wood KS, Byrns RE, Chaudhuri G. Endothelium-derived relaxing factor produced and released from artery and vein is nitric oxide. Proc Natl Acad Sci U S A. 1987;84:9265–9.
Furchgott RF, Zawadzki JV. The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetycholine. Nature. 1980 27 nov 1980;288(5789):373-6.
Palmer RMJ, Ferrige AG, Moncada S. Nitric oxide release accounts for the biological activity of endothelium-derived relaxing factor. Nature. 1987 11 June 1987;327(6122):524-6.
Garthwaite J, Charles SL, Chess-Williams R. Endothelium-derived relaxing factor release on activation of NMDA receptors suggests role as intercellular messenger in the brain. Nature. 1988;336(6197):385–8.
Forman HJ, Maiorino M, Ursini F. Signaling functions of reactive oxygen species. Biochemistry. 2010;49(5):835–42.
Hill BG, Dranka BP, Bailey SM, Lancaster Jr JR, Darley-Usmar VM. What part of NO don’t you understand? Some answers to the cardinal questions in nitric oxide biology. J Biol Chem. 2010;285(26):19699–704.
Fukumura D, Kashiwagi S, Jain RK. The role of nitric oxide in tumour progression. Nat Rev Cancer. 2006;6(7):521–34.
Fernandes D, Assreuy J. Nitric oxide and vascular reactivity in sepsis. Shock. 2008;30 Suppl 1:10–3.
Capellini VK, Celotto AC, Baldo CF, Olivon VC, Viaro F, Rodrigues AJ, et al. Diabetes and vascular disease: basic concepts of nitric oxide physiology, endothelial dysfunction, oxidative stress and therapeutic possibilities. Curr Vasc Pharmacol. 2010;8(4):526–44.
Mehta S. The effects of nitric oxide in acute lung injury. Vascul Pharmacol. 2005;43(6):390–403.
Baylis C. Nitric oxide deficiency in chronic kidney disease. Am J Physiol Renal Physiol. 2008;294(1):F1–9.
Bredt DS, Snyder SH. Isolation of nitric oxide synthetase, a calmodulin-requiring enzyme. Proc Natl Acad Sci U S A. 1990;87(2):682–5.
Bredt DS, Hwang PM, Glatt CE, Lowenstein C, Reed RR, Snyder SH. Cloned and expressed nitric oxide synthase structurally resembles cytochrome P-450 reductase. Nature. 1991;351(6329):714–8.
Li H, Poulos TL. Structure-function studies on nitric oxide synthases. J Inorg Biochem. 2005;99(1):293–305.
Daff S. NO synthase: structures and mechanisms. Nitric Oxide. 2010;23(1):1–11.
Michel T, Vanhoutte PM. Cellular signaling and NO production. Pflugers Arch. 2010;459(6):807–16.
Ozuyaman B, Grau M, Kelm M, Merx MW, Kleinbongard P. RBC NOS: regulatory mechanisms and therapeutic aspects. Trends Mol Med. 2008;14(7):314–22.
Finocchietto PV, Franco MC, Holod S, Gonzalez AS, Converso DP, Antico Arciuch VG, et al. Mitochondrial nitric oxide synthase: a masterpiece of metabolic adaptation, cell growth, transformation, and death. Exp Biol Med (Maywood). 2009;234(9):1020–8.
Lacza Z, Pankotai E, Busija DW. Mitochondrial nitric oxide synthase: current concepts and controversies. Front Biosci (Landmark Ed). 2009;14:4436-43.
Kelm M. Nitric oxide metabolism and breakdown. Biochim Biophys Acta. 1999;1411:273–89.
Wennmalm A, Benthin G, Edlund A, Kieler-Jensen N, Lundin S, Petersson AS, et al. Nitric oxide synthesis and metabolism in man. Ann N Y Acad Sci. 1994;714:158–64.
Greenway FL, Predmore BL, Flanagan DR, Giordano T, Qiu Y, Brandon A, et al. Single-dose pharmacokinetics of different oral sodium nitrite formulations in diabetes patients. Diabetes Technol Ther. 2012;14(7):552–60.
Rhodes P, Leone AM, Francis PL, Struthers AD, Moncada S, Rhodes PM. The L-arginine:nitric oxide pathway is the major source of plasma nitrite in fasted humans. Biochem Biophys Res Commun. 1995;209(2):590–6.
Kleinbongard P, Dejam A, Lauer T, Rassaf T, Schindler A, Picker O, et al. Plasma nitrite reflects constitutive nitric oxide synthase activity in mammals. Free Radic Biol Med. 2003;35(7):790–6.
Aparicio PJ, Knaff DB, Malkin R. The role of an iron-sulfur center and siroheme in spinach nitrite reductase. Arch Biochem Biophys. 1975;169(1):102–7.
Lancaster JR, Vega JM, Kamin H, Orme-Johnson NR, Orme-Johnson WH, Krueger RJ, et al. Identification of the iron-sulfur center of spinach ferredoxin-nitrite reductase as a tetranuclear center, and preliminary EPR studies of mechanism. J Biol Chem. 1979;254(4):1268–72.
Reddy D, Lancaster Jr JR, Cornforth DP. Nitrite inhibition of Clostridium botulinum: electron spin resonance detection of iron-nitric oxide complexes. Science. 1983;221(4612):769–70.
Goretski J, Hollocher TC. Trapping of nitric oxide produced during denitrification by extracellular hemoglobin. J Biol Chem. 1988;263(5):2316–23.
Lundberg JO, Weitzberg E. NO-synthase independent NO generation in mammals. Biochem Biophys Res Commun. 2010;396(1):39–45.
Lundberg JO, Weitzberg E, Lundberg JM, Alving K. Intragastric nitric oxide production in humans: measurements in expelled air. Gut. 1994;35(11):1543–6.
Benjamin N, O’Driscoll F, Dougall H, Duncan C, Smith L, Golden M, et al. Stomach NO synthesis. Nature. 1994;368(6471):502.
Butler AR, Ridd JH. Formation of nitric oxide from nitrous acid in ischemic tissue and skin. Nitric Oxide. 2004;10(1):20–4.
Lancaster Jr JR. A tutorial on the diffusibility and reactivity of free nitric oxide. Nitric Oxide. 1997;1(1):18–30.
Thomas DD, Liu X, Kantrow SP, Lancaster JRJ. The biological lifetime of nitric oxide: implications for the perivascular dynamics of NO and O2. Proc Natl Acad Sci U S A. 2001;98:355–60.
Hare JM. Nitric oxide and excitation-contraction coupling. J Mol Cell Cardiol. 2003;35(7):719–29.
Tziomalos K, Hare JM. Role of xanthine oxidoreductase in cardiac nitroso-redox imbalance. Front Biosci (Landmark Ed). 2009;14:237-62.
Derbyshire ER, Marletta MA. Biochemistry of soluble guanylate cyclase. Handb Exp Pharmacol. 2009;191:17–31.
Garthwaite J. New insight into the functioning of nitric oxide-receptive guanylyl cyclase: physiological and pharmacological implications. Mol Cell Biochem. 2010;334(1-2):221–32.
Ignarro LJ. Signal transduction mechanisms involving nitric oxide. Biochem Pharmacol. 1991;41(4):485–90.
Francis SH, Busch JL, Corbin JD, Sibley D. cGMP-dependent protein kinases and cGMP phosphodiesterases in nitric oxide and cGMP action. Pharmacol Rev. 2010;62(3):525–63.
Jia L, Bonaventura C, Bonaventura J, Stamler JS. S-nitrosohaemoglobin: a dynamic activity of blood involved in vascular control. Nature. 1996;380:221–6.
Allen BW, Stamler JS, Piantadosi CA. Hemoglobin, nitric oxide and molecular mechanisms of hypoxic vasodilation. Trends Mol Med. 2009;15(10):452–60.
Stevens TH, Brudvig GW, Bocian DF, Chan SI. Structure of cytochrome a3-Cua3 couple in cytochrome c oxidase as revealed by nitric oxide binding studies. Proc Natl Acad Sci U S A. 1979;76(7):3320–4.
Brunori M, Giuffre A, Sarti P. Cytochrome c oxidase, ligands and electrons. J Inorg Biochem. 2005;99(1):324–36.
Erusalimsky JD, Moncada S. Nitric oxide and mitochondrial signaling: from physiology to pathophysiology. Arterioscler Thromb Vasc Biol. 2007;27(12):2524–31.
Lancaster Jr JR, Hibbs Jr JB. EPR demonstration of iron-nitrosyl complex formation by cytotoxic activated macrophages. Proc Natl Acad Sci U S A. 1990;87(3):1223–7.
Pellat C, Henry Y, Drapier JC. IFN-gamma-activated macrophages: detection by electron paramagnetic resonance of complexes between L-arginine-derived nitric oxide and non-heme iron proteins. Biochem Biophys Res Commun. 1990;166(1):119–25.
Toledo Jr JC, Bosworth CA, Hennon SW, Mahtani HA, Bergonia HA, Lancaster Jr JR. Nitric oxide-induced conversion of cellular chelatable iron into macromolecule-bound paramagnetic dinitrosyliron complexes. J Biol Chem. 2008;283(43):28926–33.
Bryan NS, Rassaf T, Maloney RE, Rodriguez CM, Saijo F, Rodriguez JR, et al. Cellular targets and mechanisms of nitros(yl)ation: an insight into their nature and kinetics in vivo. Proc Natl Acad Sci U S A. 2004;101(12):4308–13.
McCord JM, Fridovich I. Superoxide dismutase. An enzymic function for erythrocuprein (hemocuprein). J Biol Chem. 1969;244(22):6049–55.
Beckman JS, Beckman TW, Chen J, Marshall PA, Freeman BA. Apparent hydroxyl radical production by peroxynitrite: implications for endothelial injury from nitric oxide and superoxide. Proc Natl Acad Sci U S A. 1990;87(4):1620–4.
Pacher P, Beckman JS, Liaudet L. Nitric oxide and peroxynitrite in health and disease. Physiol Rev. 2007;87(1):315–424.
Forstermann U. Nitric oxide and oxidative stress in vascular disease. Pflugers Arch. 2010;459(6):923–39.
Lieberman EH, Gerhard MD, Uehata A, Selwyn AP, Ganz P, Yeung AC, et al. Flow-induced vasodilation of the human brachial artery is impaired in patients <40 years of age with coronary artery disease. Am J Cardiol. 1996;78(11):1210–4.
Ludmer PL, Selwyn AP, Shook TL, Wayne RR, Mudge GH, Alexander RW, et al. Paradoxical vasoconstriction induced by acetylcholine in atherosclerotic coronary arteries. N Engl J Med. 1986;315(17):1046–51.
Creager MA, Cooke JP, Mendelsohn ME, Gallagher SJ, Coleman SM, Loscalzo J, et al. Impaired vasodilation of forearm resistance vessels in hypercholesterolemic humans. J Clin Invest. 1990;86(1):228–34.
Celermajer DS, Sorensen KE, Georgakopoulos D, Bull C, Thomas O, Robinson J, et al. Cigarette smoking is associated with dose-related and potentially reversible impairment of endothelium-dependent dilation in healthy young adults. Circulation. 1993;88(5 Pt 1):2149–55.
Esposito K, Nappo F, Giugliano F, Giugliano G, Marfella R, Giugliano D. Effect of dietary antioxidants on postprandial endothelial dysfunction induced by a high-fat meal in healthy subjects. Am J Clin Nutr. 2003;77(1):139–43.
Lamping K, Faraci F. Enhanced vasoconstrictor responses in eNOS deficient mice. Nitric Oxide. 2003;8(4):207–13.
Huang PL. Endothelial nitric oxide synthase and endothelial dysfunction. Curr Hypertens Rep. 2003;5(6):473–80.
Blair A, Shaul PW, Yuhanna IS, Conrad PA, Smart EJ. Oxidized low density lipoprotein displaces endothelial nitric-oxide synthase (eNOS) from plasmalemmal caveolae and impairs eNOS activation. J Biol Chem. 1999;274(45):32512–9.
Loscalzo J. Nitric oxide insufficiency, platelet activation, and arterial thrombosis. Circ Res. 2001;88(8):756–62.
Faxon DP, Fuster V, Libby P, Beckman JA, Hiatt WR, Thompson RW, et al. Atherosclerotic vascular disease conference: Writing Group III: pathophysiology. Circulation. 2004;109(21):2617–25.
Ozaki M, Kawashima S, Yamashita T, Hirase T, Namiki M, Inoue N, et al. Overexpression of endothelial nitric oxide synthase accelerates atherosclerotic lesion formation in apoE-deficient mice. J Clin Invest. 2002;110(3):331–40.
Radomski MW, Palmer RM, Moncada S. An L-arginine/nitric oxide pathway present in human platelets regulates aggregation. Proc Natl Acad Sci U S A. 1990;87(13):5193–7.
Sase K, Michel T. Expression of constitutive endothelial nitric oxide synthase in human blood platelets. Life Sci. 1995;57(22):2049–55.
Freedman JE, Loscalzo J, Barnard MR, Alpert C, Keaney JF, Michelson AD. Nitric oxide released from activated platelets inhibits platelet recruitment. J Clin Invest. 1997;100(2):350–6.
Freedman JE, Sauter R, Battinelli EM, Ault K, Knowles C, Huang PL, et al. Deficient platelet-derived nitric oxide and enhanced hemostasis in mice lacking the NOSIII gene. Circ Res. 1999;84(12):1416–21.
Salvemini D, de Nucci G, Gryglewski RJ, Vane JR. Human neutrophils and mononuclear cells inhibit platelet aggregation by releasing a nitric oxide-like factor. Proc Natl Acad Sci U S A. 1989;86(16):6328–32.
Radomski MW, Palmer RM, Moncada S. The anti-aggregating properties of vascular endothelium: interactions between prostacyclin and nitric oxide. Br J Pharmacol. 1987;92(3):639–46.
Bednar MM, Gross CE, Howard DB, Russell SR, Thomas GR. Nitric oxide reverses aspirin antagonism of t-PA thrombolysis in a rabbit model of thromboembolic stroke. Exp Neurol. 1997;146(2):513–7.
Lambert AJ, Brand MD. Reactive oxygen species production by mitochondria. Methods Mol Biol. 2009;554:165–81.
Pearlstein DP, Ali MH, Mungai PT, Hynes KL, Gewertz BL, Schumacker PT. Role of mitochondrial oxidant generation in endothelial cell responses to hypoxia. Arterioscler Thromb Vasc Biol. 2002;22(4):566–73.
Meneshian A, Bulkley GB. The physiology of endothelial xanthine oxidase: from urate catabolism to reperfusion injury to inflammatory signal transduction. Microcirculation. 2002;9(3):161–75.
Vasquez-Vivar J, Kalyanaraman B, Martasek P. The role of tetrahydrobiopterin in superoxide generation from eNOS: enzymology and physiological implications. Free Radic Res. 2003;37(2):121–7.
Landmesser U, Dikalov S, Price SR, McCann L, Fukai T, Holland SM, et al. Oxidation of tetrahydrobiopterin leads to uncoupling of endothelial cell nitric oxide synthase in hypertension. J Clin Invest. 2003;111(8):1201–9.
Lambeth JD. NOX enzymes and the biology of reactive oxygen. Nat Rev Immunol. 2004;4(3):181–9.
Boger RH. L-Arginine therapy in cardiovascular pathologies: beneficial or dangerous? Curr Opin Clin Nutr Metab Care. 2008;11(1):55–61.
Schulman SP, Becker LC, Kass DA, Champion HC, Terrin ML, Forman S, et al. L-arginine therapy in acute myocardial infarction: the vascular interaction with age in myocardial infarction (VINTAGE MI) randomized clinical trial. JAMA. 2006;295(1):58–64.
Wilson AM, Harada R, Nair N, Balasubramanian N, Cooke JP. L-arginine supplementation in peripheral arterial disease: no benefit and possible harm. Circulation. 2007;116(2):188–95.
Erez A, Nagamani SC, Shchelochkov OA, Premkumar MH, Campeau PM, Chen Y, et al. Requirement of argininosuccinate lyase for systemic nitric oxide production. Nat Med. 2011;17(12):1619–26.
Ellsworth ML. The red blood cell as an oxygen sensor: what is the evidence. Acta Physiol Scand. 2000;168:551–9.
Gladwin MT, Shelhamer JH, Schechter AN, Pease-Fye ME, Waclawiw MA, Panza JA, et al. Role of circulating nitrite and S-nitrosohemoglobin in the regulation of regional blood flow in humans. Proc Natl Acad Sci U S A. 2000;97(21):11482–7.
Robinson JM, Lancaster Jr JR. Hemoglobin-mediated, hypoxia-induced vasodilation via nitric oxide: mechanism(s) and physiologic versus pathophysiologic relevance. Am J Respir Cell Mol Biol. 2005;32(4):257–61.
Jensen FB. The dual roles of red blood cells in tissue oxygen delivery: oxygen carriers and regulators of local blood flow. J Exp Biol. 2009;212(Pt 21):3387–93.
Zhang R, Hess DT, Qian Z, Hausladen A, Fonseca F, Chaube R, et al. Hemoglobin betaCys93 is essential for cardiovascular function and integrated response to hypoxia. Proc Natl Acad Sci U S A. 2015;112(20):6425–30.
Bryan NS, Ivy JL. Inorganic nitrite and nitrate: evidence to support consideration as dietary nutrients. Nutr Res. 2015;35(8):643–54.
Kleinbongard P, Dejam A, Lauer T, Jax T, Kerber S, Gharini P, et al. Plasma nitrite concentrations reflect the degree of endothelial dysfunction in humans. Free Radic Biol Med. 2006;40(2):295–302.
Stuehr DJ, Marletta MA. Induction of nitrite/nitrate synthesis in murine macrophages by BCG infection, lymphokines, or interferon-gamma. J Immunol. 1987;139(2):518–25.
Ding AH, Nathan CF, Stuehr DJ. Release of reactive nitrogen intermediates and reactive oxygen intermediates from mouse peritoneal macrophages. Comparison of activating cytokines and evidence for independent production. J Immunol. 1988;141(7):2407–12.
Xie QW, Cho HJ, Calaycay J, Mumford RA, Swiderek KM, Lee TD, et al. Cloning and characterization of inducible nitric oxide synthase from mouse macrophages. Science. 1992;256(5054):225–8.
Nathan CF, Hibbs Jr JB. Role of nitric oxide synthesis in macrophage antimicrobial activity. Curr Opin Immunol. 1991;3(1):65–70.
Cauwels A. Nitric oxide in shock. Kidney Int. 2007;72(5):557–65.
Garthwaite G, Garthwaite J. Differential dependence on Ca2+ of N-methyl-D-aspartate and quisqualate neurotoxicity in young rat hippocampal slices. Neurosci Lett. 1989;97(3):316–22.
Zhang J, Snyder SH. Nitric oxide in the nervous system. Annu Rev Pharmacol Toxicol. 1995;35:213–33.
Whittle BJ, Boughton-Smith NK, Moncada S. Biosynthesis and role of the endothelium-derived vasodilator, nitric oxide, in the gastric mucosa. Ann N Y Acad Sci. 1992;664:126–39.
Calatayud S, Barrachina D, Esplugues JV. Nitric oxide: relation to integrity, injury, and healing of the gastric mucosa. Microsc Res Tech. 2001;53(5):325–35.
Munzel T, Sinning C, Post F, et al. Pathophysiology, diagnosis and prognostic implications of endothelial dysfunction. Ann Med. 2008;40(3):180–96.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Bryan, N.S., Lancaster, J.R. (2017). Nitric Oxide Signaling in Health and Disease. In: Bryan, N., Loscalzo, J. (eds) Nitrite and Nitrate in Human Health and Disease. Nutrition and Health. Humana Press, Cham. https://doi.org/10.1007/978-3-319-46189-2_13
Download citation
DOI: https://doi.org/10.1007/978-3-319-46189-2_13
Published:
Publisher Name: Humana Press, Cham
Print ISBN: 978-3-319-46187-8
Online ISBN: 978-3-319-46189-2
eBook Packages: MedicineMedicine (R0)