Abstract
This chapter is focused on animal handling during rodent imaging. Particularly in studies of peripheral organs, the nutritional status of an animal may affect the imaging results. Anesthetics can also have a strong impact on scan data, for example, in drug research or studies of the brain. Physiological parameters like body temperature, heart rate, ventilation frequency, and oxygenation of the blood should always be carefully monitored and be kept close to their normal values or be standardized as much as possible when data from different animals are compared. Most PET and SPECT studies have employed the intravenous route for tracer administration. Several other routes are possible although these are probably not as widely applicable. For many studies, the combination of functional (PET, SPECT, fMRI) and anatomic (CT, US, MRI) imaging offers significant advantages, particularly if functional and anatomic data can be acquired simultaneously.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1 Introduction
This chapter is focused on important issues of animal handling in rodent imaging. Researchers should be aware of the fact that zootechnical procedures (i.e., animal housing, care, and nutrition) have a strong impact on the final outcome of a scanning protocol. Since our own expertise is related mainly to small animal PET (positron emission tomography) and SPECT (single photon emission computed tomography) imaging, emphasis will be placed on these modalities. For similar reasons, the subject matter of the chapter has been limited to the handling of rats and mice. Ferrets, pigs, and nonhuman primates can be used in the preclinical evaluation of nuclear medicine tracers, but a discussion of the handling of these species is outside the scope of this review.
Mice are commonly used in radiotracer development, as this rodent species offers several advantages. Mice are cheap, their biology is well known, and inbred strains and transgenic mouse models of human diseases are readily available. However, since the dimensions of an adult mouse (body weight about 20 g) are small compared to the linear resolution of a PET or SPECT camera (≥1 and 0.3 mm, respectively), small anatomical details in the brain, thorax, or abdomen cannot be distinguished. Moreover, the blood volume of a mouse is small (about 1.5 ml), which limits the possibilities of repeated blood sampling. For this reason, mice are not very suitable for studies which require pharmacokinetic modeling.
Rats offer most of the advantages of mice, although less transgenic models have been developed in this species. The larger dimensions of rats as compared to mice allow the quantification of tracer uptake in individual brain regions rather than the entire brain, and visualization of relevant anatomical details. Since the blood volume of an adult rat is considerable (about 25 ml for an animal of 300 g), repeated blood sampling is possible in this species. Data of such samples can be used for pharmacokinetic modeling.
2 Nutritional Status of the Scanned Animal
Diet composition, food intake, or duration of fasting before the onset of the scan may affect the outcome of rodent imaging. An early biodistribution study reported that glucose ([18F]-FDG) uptake in rat heart, testis, and brown fat are strongly affected by the nutritional status of the animal. In myocardium and brown adipose tissue, tracer uptake was reduced two to threefold after 24 h of fasting, in contrast to the situation in testis, where a small increase was noted (Paul et al. 1987).
Fasting (20 h) of tumor-bearing mice resulted in a strong decline of the levels of blood glucose both in awake and anesthetized animals (ketamine/xylazine or pentobarbital). This decline was accompanied by an almost fourfold increase in tumor glucose ([18F]-FDG) uptake and a significantly improved tumor-to-background contrast in PET images (Lee et al. 2005). In severe combined immunodeficient (SCID) mice bearing a human A431 epidermal carcinoma or U251 glioblastoma, fasting (8–12 h) or warming the animals during the scan significantly reduced [18F]-FDG uptake in brown fat and strongly improved tumor visualization (Fueger et al. 2006). In contrast to [18F]-FDG uptake in peripheral organs (tumor, muscle, and heart), glucose metabolism in the brain of male Black 6 mice (C57BL/6) was not significantly affected by fasting (Wong et al. 2011).
The biodistribution of other metabolic PET tracers (e.g., amino acids) is also affected by nutritional status. An early PET study reported that the uptake of [13N]-glutamate in rat pancreas is significantly higher when animals are subjected to overnight fasting rather than allowed free access to pellet food (Kubota et al. 1983).
Composition of the diet (either standard or high-energy) was shown to affect tumor [18F]-FDG uptake and cell proliferation in mice bearing MC38 colon carcinomas. A high-energy diet induced hyperinsulinemia, activated insulin receptors in tumor cells, and increased tumor uptake of [18F]-FDG. These negative effects of the high-energy diet could be blocked by treating mice with metformin, a drug which reduces hepatic gluconeogenesis and insulin levels in the circulation (Mashhedi et al. 2011).
Uptake of inflammatory markers ([18F]-galacto-RGD, [18F]-FDG) in murine atherosclerotic lesions is related to the lipid/cholesterol content of the diet and reduced after lipid-lowering interventions (Saraste et al. 2012; Silvola et al. 2011).
These limited data indicate that a short period of fasting may be useful in scanning protocols aimed at visualization of the peripheral tumors, the atherosclerotic lesions, the pancreas, or the heart. However, fasting seems to offer no significant advantages in studies of the brain.
3 Anesthesia: A Necessary Evil?
Rodents are usually anesthetized during a scan, in order to prevent them from moving during the imaging procedure. However, anesthetics limit the capability of an animal to maintain homeostasis. Anesthesia affects several physiological parameters, such as myocardial function and blood flow (Cavazzuti et al. 1987; Croteau et al. 2004; Gjedde et al. 1980; Hansen et al. 1988; Hendrich et al. 2001; LaManna et al. 1986; Lenz et al. 1998, 1999; Maekawa et al. 1986; Saija et al. 1989; Todd et al. 1996; Zanelli et al. 1975), blood volume in tissue (Todd et al. 1996; Zanelli et al. 1975), gastrointestinal motion (Yamashita et al. 2011), and inflammatory responses (Chiang et al. 2008; Fortis et al. 2012). Anesthesia is associated with alterations of cerebral energy metabolism (Cavazzuti et al. 1987; Crosby et al. 1982; Dam et al. 1990; Eintrei et al. 1999; Hodes et al. 1985; Lenz et al. 1998, 1999; Maekawa et al. 1986; Ori et al. 1986; Saija et al. 1989; Sokoloff et al. 1977) and neurotransmission (Ford et al. 1986; Shahani et al. 2002). For these reasons, PET findings in anesthetized rodents may not be a proper representation of the physiology of the conscious animal.
Experimental animals can be trained to stay quiet during a PET or MRI scan and be accustomed to a restraining device (Becerra et al. 2011; Chen et al. 2010; Ferris et al. 2006; Hosoi et al. 2005; Itoh et al. 2009; King et al. 2005; Lahti et al. 1998; Lee et al. 2005; Mizuma et al. 2010; Momosaki et al. 2004). Using such a device, the side effects of anesthetics can be avoided since the scanned subject remains conscious. However, physical restraint will always cause some stress, even in trained rodents. PET data of conscious animals kept in a restrainer can therefore not be considered as an exact replica of processes in the undisturbed situation.
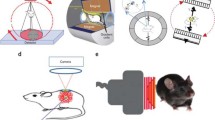
Restraint stress can be avoided by using a portable imaging device such as the RatCap (Schulz et al. 2011) or a system which corrects for motion such as the AwakeSPECT (Baba et al. 2013). Using such devices, imaging data can be acquired from unrestrained animals. However, because of the weight and/or the physical dimensions of the devices, the scanned animals are not stress-free.
Although the impact of anesthetics on scan data is probably great, their exact consequences are frequently unknown. Because of the lack of a true control or an absolute gold standard, evaluation of the impact of anesthetics is difficult. Three different approaches have been used to assess this impact:
-
(i)
Animals are scanned using an identical procedure but different anesthetics (Alstrup et al. 2011; Casteels et al. 2010; Croteau et al. 2004; Elfving et al. 2003; Flores et al. 2008; Fuchs et al. 2013; Kersemans et al. 2011; Matsumura et al. 2003; Yu et al. 2009). This approach may reveal differences between anesthetic drugs, but it cannot indicate which anesthetic procedure results in the smallest disturbance of the normal tissue homeostasis.
-
(ii)
Awake and anesthetized animals are scanned with the same tracer (Chen et al. 2010; Hosoi et al. 2005; Itoh et al. 2009; Lee et al. 2005; McCormick et al. 2011; Mizuma et al. 2010; Momosaki et al. 2004; Yamashita et al. 2011). Using this approach, observed differences between the study groups may be due both to the anesthetic and to restraint stress in the group which is awake.
-
(iii)
Awake rodents are injected with radiotracer and allowed free movement in their home cages or in an open-field arena. After a prolonged interval, when the regional distribution of the tracer has approached a steady state, the animals are anesthetized and a PET scan is made (Fueger et al. 2006; Matsumura et al. 2003; Patel et al. 2008; Radonjic et al. 2013; Schiffer et al. 2007; Shih et al. 2008; Toyama et al. 2004). A great advantage of this approach is that data from the scan represent distribution of the tracer in the conscious state. However, the kinetics of tracer uptake during that state are unknown, and for this reason, tracer-kinetic modeling is not possible. In some cases, tracer distribution volumes can be calculated from a delayed scan using a simulated input function based on validated assumptions (Tantawy et al. 2011).
Anesthesia procedures for rodent imaging have been the subject of several excellent reviews (Alstrup et al. 2013; Gargiulo et al. 2012a, b; Hanusch et al. 2007; Hildebrandt et al. 2008; Tremoleda et al. 2012). Some known effects of anesthetics are discussed below.
3.1 Impact of Anesthetics on Glucose Metabolism
In the ground-breaking paper of Louis Sokoloff concerning measurement of the metabolic rate of glucose with [14C]-deoxyglucose and ex vivo autoradiography, striking regional differences of metabolism were observed in the brain of conscious rats, the highest levels occurring in gray matter of certain cortical areas, e.g., auditory cortex, and the lowest levels in white matter regions. Thiopental anesthesia markedly reduced glucose metabolic rate, particularly in gray matter, and metabolic rate became more uniform throughout the brain (Sokoloff et al. 1977).
In subsequent years, the [14C]-deoxyglucose method has been applied to study the impact of different anesthetics on cerebral glucose metabolism in rodents. Barbiturates such as phenobarbital (Hodes et al. 1985) or pentobarbital (Saija et al. 1989); inhalation anesthetics such as isoflurane (Lenz et al. 1998, 1999; Maekawa et al. 1986; Ori et al. 1986), sevoflurane (Lenz et al. 1998), or desflurane (Lenz et al. 1999); and propofol, a modulator of GABA receptor-mediated signal transduction (Dam et al. 1990), were found to cause widespread, dose-dependent reductions of glucose metabolism particularly in gray matter areas of the brain. However, ketamine anesthesia resulted in a unique metabolic response, with striking increases of glucose consumption in limbic areas (cingulate gyrus, hippocampus, striatum, extrapyramidal motor system, olfactory tubercle, corpus callosum) and decreases of energy metabolism in somatosensory and auditory systems (Cavazzuti et al. 1987; Crosby et al. 1982; Eintrei et al. 1999; Saija et al. 1989). Ketamine-induced increases of glucose metabolism in limbic areas were blocked after coadministration of diazepam (Eintrei et al. 1999).
Effects of anesthesia on glucose metabolism in rodent tissues have also been studied with PET and 2-deoxy-2-[18F] fluoro-D-glucose ([18F]-FDG). The imaging findings were in accordance with previously reported data from ex vivo autoradiography. In a study comparing six different anesthetics (ketamine, ketamine/xylazine, chloral hydrate, pentobarbital, propofol, isoflurane), all anesthetics – with the exception of ketamine – were found to reduce glucose metabolism in rat brain (Matsumura et al. 2003). Reductions of brain metabolism by anesthetics were a general finding in [18F]-FDG-PET studies, both of mice (Toyama et al. 2004) and rats (Fig. 18.1), but glucose uptake in the myocardium and in implanted tumors was found to be affected by the type of anesthetic, some anesthetics (e.g., isoflurane) causing an increase (Toyama et al. 2004) and others (e.g., ketamine/xylazine, pentobarbital) causing a decline (Lee et al. 2005; Toyama et al. 2004). These differences may be related to the fact that ketamine/xylazine, in contrast to isoflurane or sevoflurane, strongly increases levels of nonradioactive glucose in the blood, which competes with [18F]-FDG for uptake in target tissues (Flores et al. 2008; Fueger et al. 2006; Woo et al. 2008; Yu et al. 2009).
Impact of anesthesia on glucose metabolism in the rat brain. Left image: [18F]-FDG injected intraperitoneally in a conscious rat which was then allowed to explore a novel environment for 45 min. After this period, the animal was anesthetized with isoflurane and a 20 min static scan was made. Right image: [18F]-FDG injected intravenously in an animal which was under anesthesia with pentobarbital. In the conscious animal, striking regional differences of tracer uptake were noted, with particularly high uptake in the forebrain. In the anesthetized animal, glucose uptake was reduced, and although the difference between gray matter and white matter remained visible, regional differences were largely abolished (Unpublished data of A.van Waarde)
Thus, the regional distribution and intensity of glucose metabolism, both in the brain and in peripheral organs, are strongly dependent on animal handling, particularly the duration or depth of anesthesia and the type of anesthetic. Vital parameters (levels of glucose and oxygen in the blood, body temperature, ventilation frequency, and heart rate) should be carefully monitored during PET studies of anesthetized rodents and be maintained at identical levels in all study groups.
3.2 Impact of Anesthetics on Neurotransmission
3.2.1 Dopaminergic System
Since the neurotransmitter dopamine plays an important role in motor function, addiction, and reward, dopaminergic neurotransmission is frequently studied in biomedical research. Changes of dopaminergic neurotransmission are implied in Parkinson’s disease and schizophrenia, and dopamine receptor antagonists are widely employed as antipsychotic drugs. Several findings in experimental animals have indicated that anesthesia may affect the dopaminergic system.
Target-to-nontarget ratios of the dopamine reuptake tracer [125I]-PE2I were decreased after anesthetizing rats with ketamine/xylazine or isoflurane, but unaltered after anesthesia with zoletile mixture or halothane (Elfving et al. 2003). The specific binding fraction and the kinetics of [11C]-cocaine in the brain were different when rats were anesthetized with α-chloralose or isoflurane, suggesting differences of dopamine transporter availability (Du et al. 2009). The binding potential of the dopamine transporter ligand [123I]-ioflupane in awake mice was about 50 % of that which was observed in mice which were anesthetized with isoflurane (Baba et al. 2013).
Binding potential (k3/k4) values of the dopamine D1 receptor tracer [11C]-SCH23390 were significantly increased (by 36–46 %) when rats were anesthetized with chloral hydrate or ketamine and significantly decreased (by 41 %) after anesthesia with pentobarbital (Momosaki et al. 2004). These findings may be related to blood flow changes, since chloral hydrate and ketamine increase and pentobarbital decreases perfusion of the brain (Alstrup et al. 2013). Another possible (but unproven) mechanism is that anesthetics modify the affinity of D1 receptors for radioligand binding.
Binding potential values (distribution volume ratios minus one) of the dopamine D2/D3 ligand [11C]-raclopride in rats anesthetized with isoflurane were twice as high as in animals anesthetized with fentanyl-fluanisone-midazolam (Alstrup et al. 2011). Binding of the dopamine D2/D3 agonist [11C]-(+)-PHNO in rat brain was also increased when animals were anesthetized with isoflurane, and the reduction of [11C]-(+)-PHNO binding by amphetamine was greater in isoflurane-anesthetized animals than in awake rats (McCormick et al. 2011). However, the striatal binding of [11C]-raclopride in animals anesthetized with ketamine/xylazine was not significantly different from that observed in freely moving rodents, and drug challenges (methamphetamine, gamma-vinyl-GABA) affected [11C]-raclopride binding similarly in both study groups (Patel et al. 2008). In contrast to the increases reported for [11C]-raclopride and [11C]-(+)-PHNO, binding potential (BP ND) values of the dopamine D2 receptor ligand [18F]-fallypride in rat striatum were found to be 30 % lower in isoflurane-anesthetized animals compared to awake controls (Tantawy et al. 2011).
Many literature findings indicate that anesthetics alter dopamine transporter activity (Shahani et al. 2002) and trafficking (Byas-Smith et al. 2004; Votaw et al. 2003, 2004), extracellular dopamine concentration (Adachi et al. 2005; Votaw et al. 2003), and metabolism of dopamine to 3,4-dihydroxyphenylacetic acid (Adachi et al. 2005; Ford et al. 1986). Via such mechanisms, anesthetics affect the outcome of PET and SPECT studies of the dopaminergic system.
3.2.2 Serotonergic System
PET and SPECT imaging of other neurotransmitter systems is also influenced by anesthesia. Using a constant infusion protocol and arterial blood sampling, Tokugawa et al. monitored tissue-to-plasma ratios of the serotonin 5-HT1A receptor ligand [18F]-FPWAY in awake and isoflurane-anesthetized rats. Stable ratios were reached within 30 min after the start of tracer infusion. Ratios in lateral hippocampus and cerebellum of anesthetized animals were found to be greater (by 32–63 %) than in awake rats. This difference was explained by the assumption that levels of extracellular serotonin are reduced under isoflurane anesthesia (Tokugawa et al. 2007). In an earlier study, target-to-background ratios of the serotonin transporter ligand [3H]-(S)-citalopram were found to be increased by isoflurane or halothane and decreased by ketamine/xylazine, whereas ratios of the serotonin 5-HT2 ligand [18F]-altanserin were unaffected (Elfving et al. 2003). It is not known whether all of these changes are related to altered concentrations of extracellular serotonin.
3.2.3 Cholinergic System
Using a bolus plus constant infusion protocol, American authors studied the in vivo binding of the muscarinic cholinoceptor ligand N-[18F]-fluoroethyl-piperidinyl benzilate ([18F]-FEPB) in rats (Kilbourn et al. 2007). Both isoflurane and pentobarbital caused a strong (65–90 %) increase of tracer distribution volume in receptor-rich regions of the brain (striatum, cortex, hippocampus). Pretreatment of animals with an acetylcholinesterase inhibitor (phenserine) caused a strong increase of tracer binding (70 %) in awake rats, but not in animals anesthetized with isoflurane or pentobarbital. The mechanisms underlying these phenomena are not understood, but it is evident that anesthesia can affect the outcome of PET studies with cholinergic tracers and may even obscure the result of pharmacological challenges.
3.2.4 Other Aspects of Neurotransmission
Using in vivo saturation experiments with increasing masses of (R)-rolipram and [11C]-(R)-rolipram as tracer, Itoh et al. determined the B max and K d of phospodiesterase-4 in the brain of conscious and isoflurane-anesthetized rats. Significantly higher values (by 29 % and 59 %, respectively) were observed in conscious as opposed to anesthetized animals (Itoh et al. 2009).
The binding of a sigma-1 receptor ligand, particularly to sigma-1 receptors in peripheral tumors, is significantly and time dependently increased when animals are anesthetized with pentobarbital (Rybczynska et al. 2009). Pentobarbital interferes with steroid metabolism, resulting in reduced levels of progesterone and a decreased competition of this endogenous antagonist with the radioligand for binding to the sigma-1 receptor protein (Fig. 18.2). In contrast to the increases induced by pentobarbital, the radioligand binding to sigma-1 receptors is significantly decreased when animals are anesthetized with racemic ketamine (van Waarde et al. 2004). The (R)-enantiomer of ketamine has significant affinity for sigma-1 receptors.
Impact of anesthesia on sigma-1 receptor imaging in a tumor. A rat with a C6 glioma implanted subcutaneously in its right shoulder was scanned twice with [11C]-SA4503. Left image: animal shortly anesthetized (< 20 min before start of the scan). Right image: animal anesthetized for 3 h with pentobarbital. Arrows indicate the position of the tumor. Tumor uptake of the radioligand is significantly increased after prolonged anesthesia (Data from Rybczynska et al. 2009)
In contrast to findings reported for other neuroreceptors, no significant changes in cerebral uptake of the cannabinoid CB1 receptor ligand [18F]-MK-9470 were noted in rats anesthetized with pentobarbital or isoflurane as compared to freely moving animals, neither with in vivo techniques (parametric PET images, statistical parametric mapping) nor with ex vivo autoradiography, although relative tracer uptake in the cortex seemed to be slightly (9–13 %) decreased and relative uptake in cerebellum was slighty (13–14 %) increased (Casteels et al. 2010).
3.2.5 Use Anesthetics with Care
In conclusion, anesthetics can have species-specific and dose-dependent effects on the binding properties of neuroreceptors, transporters, and enzymes. Some anesthetics may even interfere directly with the target receptor. Consideration of the possible undesired effects of anesthesia is necessary when an imaging study is planned, and the applied anesthetic should be carefully chosen, depending on the study target. Vital parameters should be monitored, and the scanning conditions should be standardized as much as possible during PET studies of the brain.
3.3 Monitoring of Physiological Parameters in Anesthetized Rodents
An anesthetized animal is limited in its capability to maintain homeostasis. This limitation becomes more severe when the experimental procedure is more invasive, when the animal is anesthetized longer (Tremoleda et al. 2012) or when drugs are administered which potentiate the effect of anesthetics, such as adenosine A1 receptor agonists (Paul et al. 2014).
Negative side effects of anesthetics are depressions of the respiratory, cardiovascular, and thermoregulatiory systems. For this reason, these systems should be monitored during animal experiments (Tremoleda et al. 2012; Zutphen et al. 2001). Monitoring of the clinical and physiological parameters of an anesthetized animal is required since it allows the investigator to maintain the animal in a steady state, e.g., by adjusting the depth of anesthesia or the settings of an artificial respirator, the animal can be kept in a constant condition (Tremoleda et al. 2012; Zutphen et al. 2001).
Any monitoring procedure starts with checking the condition of the animal before the experiment (Tremoleda et al. 2012). If undesired or unexpected abnormalities in the clinical or physiological parameters are noted during the subsequent experimental procedures, data from the affected animal should be excluded from the final study report.
3.3.1 Respiratory System
Poor exchange of O2 and CO2 or administration of excessive concentrations of anesthetics can cause hypoxia and eventually lead to respiratory arrest. Monitoring of the animal’s breathing frequency and ventilatory motion besides regular inspection for the symptoms of cyanosis can inform the investigator that the animal is developing hypoxia (Tremoleda et al. 2012; Zutphen et al. 2001). Continuous monitoring is possible by using a capnograph which measures CO2 concentration in the exhaled air. The gold standard for measurement of respiratory function is blood gas analysis (Tremoleda et al. 2012; Zutphen et al. 2001).
3.3.2 Cardiovascular System
The cardiovascular system can be monitored by examining heart rate, stroke volume, and capillary refill time (Tremoleda et al. 2012; Zutphen et al. 2001). More advanced techniques are the use of an electrocardiograph (ECG) to monitor the electrical activity of the heart, a pulse oximeter to measure the myocardial pulse and oxygenation level of the arterial blood, and pressure transducers to record changes of blood pressure (Tremoleda et al. 2012; Zutphen et al. 2001).
Some imaging modalities offer the possibility of respiratory and cardiovascular gating. Gating is used to avoid image artifacts due to cardiac and/or respiratory movement or to get information about the cardiac and/or the respiratory cycle (Szymanski et al. 2012; Tahari et al. 2014). Gating software can also be employed to monitor the respiratory and cardiovascular systems of a scanned animal.
3.3.3 Thermoregulatory System
Rodents have a high skin-surface-to-body-weight ratio and a high metabolic rate, which makes them vulnerable to hypothermia and also to hyperthermia when they are artificially heated. For body temperature monitoring, the core temperature of the animal can be measured with a rectal probe and an electronic thermometer (Tremoleda et al. 2012; Zutphen et al. 2001).
For continuous monitoring and maintenance of body temperature close to the physiological value, commercially available controllers can be used (Fig. 18.3). These consist of a temperature probe, an adjustable electronic thermostat, and some source of heat (heating pad, infrared lamp, or circulating water system).
Impact of anesthesia on rodent thermoregulation. An adult rat (body weight 300–350 g) which is anesthetized with pentobarbital (and is kept in this condition with small additional intraperitoneal injections of the drug) is not in a steady state. Body temperature of the animal drops dramatically. The increase of body temperature at 3 h is caused by shivering. When the same rat is anesthetized but artificially warmed, using a heating mat and an electronic temperature controller, the normal tissue homeostasis can be approached much more closely. Rectal temperatures are plotted
For a more detailed overview of monitoring possibilities and their physiological background, the reader is advised to consult textbooks about laboratory animal science.
4 Tracer Administration
4.1 Possible Routes of Tracer Administration
A crucial action in small animal PET/SPECT imaging is the administration or delivery of the radiotracer to the animal. It is important to consider possible routes of administration and their pros and cons during the planning phase. The route of choice will depend on the animal species, sex, experimental design (longitudinal versus single study), pharmacokinetics of the radiotracer, and practical feasibility. This section of our chapter describes the most common administration methods based on the expertise in our institution and on literature data. Administration methods can be divided in four groups.
4.1.1 Transdermal Route
Transdermal means “through the skin.” Although this administration method is technically easy, it is not often used in PET/SPECT imaging. The chemical structure of the radiotracer can prevent its penetration through the skin. Moreover, the transdermal application method can result in a slow delivery of the tracer with unknown kinetics. This causes difficulties for quantification of tracer uptake in the target organ. However, if the labeled compound is quickly absorbed through the skin, this route of application may be suitable for imaging purposes, e.g., the monitoring of transdermal drug delivery (Petroni et al. 2011).
4.1.2 Enteral Route
Enteral (“through the intestines”) refers to oral administration via the food or drinking water or rectal administration. The method is technically easy and results in low discomfort for the animals, but a few things should be taken into account. The chemical structure of the radiotracer can change when it is mixed with food or water and passes the stomach and gut. Addition of the tracer can have a negative effect on the taste of the animal’s diet. This last complication can be avoided by using intragastric gavage (Sarparanta et al. 2011; Yamashita et al. 2011) in anesthetized or conscious animals, although this is associated with some risk of damaging the esophagus. Another option is using a carrier like a silicon capsule or silicon particles for tracer administration (Sarparanta et al. 2011; Shingaki et al. 2012). Since the enteral administration of a radiotracer results in a rather slow entry of radioactivity in the circulation, this route is less suitable for isotopes with short half lives such as 15O, 13 N, and 11C.
4.1.3 Administration Through the Respiratory System
Radioactively labeled gasses such as [15O]-oxygen, carbon dioxide, or carbon monoxide can be administered through the respiratory system, i.e., by inhalation. This method is technically challenging. Animals must be anesthetized and be connected to a closed ventilation system by the use of a trachea tube or tracheotomy (Watabe et al. 2013; Yee et al. 2006). The method also requires additional equipment to control the influx and efflux of gas from the animal’s lungs. This includes an artificial ventilator, additional connecting tubes, and electronic equipment for ventilation monitoring (Watabe et al. 2013; Yee et al. 2006).
The pulmonary deposition of drug aerosols and nanoparticles has been studied, using PET and SPECT. Such studies require an even greater technical effort because the administered aerosols need to meet specific requirements of particle diameter since the pulmonary disposition is directly related to particle size (Asgharian et al. 2003; Kuehl et al. 2012; Palko et al. 2010). Thus, an additional aerosol generator, pump, flow meter, filters, and tubing are required (Asgharian et al. 2003; Kuehl et al. 2012). For the administration of nanoparticles, a flat-tipped syringe placed in the trachea or bronchial gavage may suffice, but with the risk of damaging the esophagus (Palko et al. 2010).
4.1.4 Parenteral Routes
Parenteral indicates the use of an administration route other than transdermal, enteral, or through the respiratory system (Palko et al. 2010). Radiotracers for PET and SPECT are frequently injected. Standard injection methods are (Zutphen et al. 2001):
-
Intracutaneous (i.c.): injection in the skin
-
Subcutaneous (s.c.): injection under the skin
-
Intramuscular (i.m.): injection in the muscle
-
Intraperitoneal (i.p.): injection in the abdominal cavity
-
Intravenous (i.v.): injection in a vein
Since intracutaneous, subcutaneous, and intramuscular injections have the same disadvantages as the transdermal administration route, intraperitoneal and intravenous injections are commonly applied.
4.1.4.1 Intraperitoneal Administration
Injection in the abdominal cavity is relatively easy. A skilled person can do this within seconds with relatively little preparation. Another advantage of this technique is that injections can be done both in anesthetized and awake rodents. Although the method is technically not very challenging, the success rate is lower than expected. Even after taking all the necessary precautions (holding the animal and needle in the proper way), in 15 % of the injections (Vines et al. 2011), the radiotracer ended up in the intestines where it got trapped, resulting in a useless scan. Another disadvantage of intraperitoneal tracer injections is that the technique results in a rather slow entry of the radiotracer in the circulation (Wong et al. 2011; Yoder et al. 2011). In practice this means that i.p. injections may only be suitable for microPET scans with metabolic tracers such as [18F]-FDG. For the same reason, i.p. injections are not appropriate for dynamic scanning protocols or for studies involving pharmacokinetic modeling (Nanni et al. 2007; Vines et al. 2011; Wong et al. 2011; Yoder et al. 2011).
4.1.4.2 Intravenous Injection
The most frequently used method for radiotracer delivery is intravenous injection. Since the tracer is directly administered into the circulation, this technique results in rapid pharmacokinetics and is suitable for dynamic scanning protocols (Nanni et al. 2007; Vines et al. 2011). The method can be applied both in awake and in anesthetized animals. Tracer injection can be done manually (for bolus injections) or with an infusion pump (for bolus injections and/or slow infusions). Intravenous injection is technically more challenging than intraperitoneal tracer administration. It is an invasive method which requires preparations (e.g., the insertion of a cannula) and considerable care before, during, and after the procedure.
When animals are anesthetized with a substance causing vasoconstriction (Nanni et al. 2007; Vines et al. 2011), small veins are hard to find. Vasoconstriction can partly be prevented by heating the tissue around the target vein right after the animal has been anesthetized, using warm water or an infrared lamp. The injection can cause hemorrhages. Bleeding can be prevented by putting pressure on the target vein after injection. Repeated injections or puncturing can cause tissue damage, fibrosis (Vines et al. 2011), and even complete degradation of the vein. It is advised to practice the method in order to gain experience and reduce the chances of failure and discomfort before starting small animal imaging experiments.
4.2 Selection of a Blood Vessel for Tracer Administration
The answer to the question which vein should be employed as an injection pathway depends on many variables. Rats and mice have a very long tail with two lateral veins which can be used for manual or pump-controlled radiotracer injections. Because of the length of this tail, tail veins can be repeatedly used for multiple injections without running the risk of venous degradation. The length of the tail makes it also possible to inject the animal when it is lying in the scanner as the injection site is usually outside the field of view and far from any target organ.
In our institution we use a 29G x 1/2 (0.33 × 12 mm) insulin needle for injections in a preheated mouse tail and a 26G x 3/4 (0.64 × 19 mm) butterfly for injections in a preheated rat tail. Although tail veins are easily accessible, this injection pathway has some disadvantages. Tails cool rapidly, and tail veins are therefore very sensitive to vasoconstriction, especially when anesthetized animals are housed in a cold room. Several studies have shown that even after correct intravenous injection, extravasation of the radiotracer may occur in the upper part of the tail, resulting in a slow release of part of the injected dose from a depot and difficulties in quantitative analysis of the PET data (Groman et al. 2004; Nanni et al. 2007; Vines et al. 2011).
A suitable alternative for the technically challenging tail vein injection is an injection of the radiotracer in the retro-orbital venous sinus (Nanni et al. 2007; Schoell et al. 2009; Steel et al. 2008). Although some expertise is required, several publications indicate that retro-orbital injections are easy, can be rapidly performed, and result in rapid drug delivery to target organs (Nanni et al. 2007; Schoell et al. 2009). The technique is reproducible and can be repeated without any serious complications (Nanni et al. 2007).
However, it is difficult to use this injection route when the animal is lying inside a PET or SPECT camera. Retro-orbital injections are thus not very suitable for dynamic scanning protocols. Moreover, the volume which can be injected is more limited than in tail vein injections; therefore, the injected tracer should have a high specific radioactivity (Nanni et al. 2007; Steel et al. 2008). Finally, it is advised to not use this technique for studies of the brain. Elevated levels of radioactivity at the injection site can result in spillover to regions of interest within the brain and can negatively affect the brain data (Greeuw et al. 2013).
A method which has been widely used in our institution is tracer injection through the penile vein. This method has a success rate of 95 % for rats. The high rate of success is related to the absence of vasoconstriction under normal conditions. Because the penis of a rat or mouse is hidden in a sheath and is kept close to the abdomen, the organ is maintained at body temperature. Pulling the penis out of its sheath causes obstruction of the blood flow in this organ. The penile vein swells, and the tracer can be injected in rats with a 27G x 3/4 (0.4 × 19 mm) needle. The success rate in mice is even higher than 95 %. The penis of a mouse contains a dense capillary microcirculation which is comparable with the retro-orbital area. Injection with a 29G x 1/2 (0.33 × 12 mm) insulin needle just under the skin is enough to deliver the radiotracer into the blood stream. The technique is easy to learn and is suitable for pump infusion (Kononov et al. 1994).
Only in rare cases, penile vein injections fail. Injection failures cause an interstitial swelling which is clearly visible. Animals with such swellings can be excluded from the data analysis. Even when the tracer gets trapped under the skin or in erectile tissue, radioactivity will be slowly released into the blood because of the presence of a dense cluster of blood vessels, especially when the penis is put back in its sheath.
Besides these advantages, penile vein injections have also some disadvantages. For obvious reasons, the method can only be used in male rodents. When repeated injections are required, the penis may develop fibrotic scar tissue which lowers the success rate.
For rats, a catheter in the vena femoralis is a very safe pathway for delivery of the radiotracer. This technique can be combined with a catheter in the arteria femoralis for arterial blood sampling or blood pressure measurements. Although we have employed femoral cannulas only in terminal experiments and anesthetized rodents, it is possible to use such catheters in conscious, freely moving rats (Hall et al. 1984; Peternel et al. 2010).
The ideal position for a vena femoralis catheter is in the deeper part of the groin next to the femoral artery and saphenous nerve (Hall et al. 1984; Jespersen et al. 2012; Peternel et al. 2010). The vein can be easily reached by making a small incision on the ventral side of the animal, 1 or 2 cm from the median (Fig. 18.4). After fixation of the vein, a small hole can be made with a bended 25G x 5/8 (0.5 × 16 mm) needle. Subsequently, a fine bore polythene tube (0.40 mm inner diameter, 0.80 mm outer diameter) can be inserted into the vein and be pushed up almost to the upper part of the inferior vena cava. The whole procedure takes 10–15 min. Because the vena femoralis is a large blood vessel, it is possible to draw some blood as a confirmation that the catheter is in the right position (Hall et al. 1984; Jespersen et al. 2012; Peternel et al. 2010). Because the catheter is close to the upper part of the inferior vena cava, the injected radiotracer reaches the heart almost immediately. From there, it is distributed to the rest of the body. Femoral vein catheters can be used both for manual injections and pump infusion protocols.
5 Combining Different Imaging Modalities
Since PET and SPECT provide specific biochemical but not anatomic information, these nuclear imaging techniques are frequently combined with other imaging modalities (CT or MRI) which can visualize anatomical details. The images of the different modalities are then fused (Jan et al. 2005; Pascau et al. 2012), and in the joined images, the position of radiotracer accumulation can be clearly identified. Structural information from CT or MRI images can also be used to derive a transmission map for object-specific attenuation correction. Hybrid scanners combining PET, SPECT, and CT (Sanchez et al. 2013), PET and MRI (Herzog et al. 2010; Herzog 2012; Judenhofer et al. 2008; Maramraju et al. 2011; Raylman et al. 2007), or fluorescence tomography, SPECT, and CT (Solomon et al. 2013) have been developed, allowing co-registration of radionuclide, optical, and anatomical data with minimized movement of the subject.
A conventional small animal CT scan results in radiation doses ranging from 70 to 400 mGy (Taschereau et al. 2006). Doses of a few Gy can already have significant biological effects (e.g., reduction of tumor growth, damage to rapidly dividing tissues), whereas doses between 6.5 and 7 Gy are lethal to mice. With conventional equipment, repeated CT scanning is possible, but the total number of scans in a single animal is definitely limited. Recent advances in rodent CT scanners (low-dose detector hardware) have resulted in very significant (up to 90 %) reductions in radiation dose, making microCT suitable for longitudinal study protocols (Osborne et al. 2012).
5.1 SPECT/CT
MicroSPECT/CT (using 99mTc-labeled human albumin nanoparticles) has been successfully applied to study the pattern of lymphatic flow from heterotopic abdominal cardiac grafts in mice. Mediastinal lymph nodes were identified as the draining nodes (Brown et al. 2011). Monitoring of stem cell trafficking (Gildehaus et al. 2011) or of viral spread along a lymphatic network (Raty et al. 2007) in the living organism was another application of this form of multimodal imaging. The use of microSPECT/CT rather than microSPECT has been proven to result in a more accurate quantification of heterogeneous intratumoral tracer uptake in human pancreatic cancer xenografts (Carlson et al. 2006) and sarcomas (Umeda et al. 2012). SPECT/CT has proven useful for the localization of pulmonary (Hayakawa et al. 2013) and abdominal (Huhtala et al. 2010; Nayak et al. 2013; Pool et al. 2012) lesions in mouse models of human cancer and atherosclerotic plaques in mouse aorta (Li et al. 2010). Moreover, SPECT/CT has been used for assessment of age-dependent changes of pulmonary function (ventilation/perfusion) in mice (Jobse et al. 2012) and of particle-size-dependent deposition of aerosols in mouse and rat lungs (Kuehl et al. 2012). Focused ultrasound-induced increases of blood-brain barrier permeability in rats (Lin et al. 2009; Yang et al. 2011) and hypoperfusion in a rodent model of stroke (Seo et al. 2007) could also be assessed with this technique.
5.2 SPECT/MRI
MicroSPECT/MRI has been applied to identify the location of atherosclerotic plaques in large blood vessels (Li et al. 2010) and orthotopic pleural mesothelioma in the mouse abdomen (Nayak et al. 2013).
5.3 SPECT/US
Ultrasound-derived partial volume correction resulted in improved quantification of myocardial segmental perfusion with 99mTc-tetrofosmin in rats (Goethals et al. 2012).
5.4 PET/CT
Combination of PET and CT has proven useful for the localization of abdominal lesions in experimental animals, e.g., pancreatic (Fendrich et al. 2011; Flores et al. 2009) and prostate (Garrison et al. 2007) tumors, and for identifying inflammation in murine atherosclerotic plaques (Nahrendorf et al. 2008, 2009. The use of microPET/CT rather than microPET resulted in a more accurate quantification of infarct size in mouse models of myocardial infarction (Gargiulo et al. 2012c; Greco et al. 2012) and of [18F]-FDG uptake in an orthotopic model of glioblastoma multiforme after radiotherapy (Park et al. 2011) and in thymic lymphoma after chemotherapy (Walter et al. 2010). Iodinated contrast media can be used in small animal PET/CT in order to improve tumor delineation and diagnostic performance (Lasnon et al. 2013). Small animal PET/CT has been applied to assess bone damage in ovariectomized rats (Li et al. 2011) and adrenergic activation of interscapular brown adipose tissue in mice (Mirbolooki et al. 2014), using [18F]-fluoride and [18F]-FDG as radiotracers. Copper metabolism in the liver of an animal model of Wilson’s disease could also be studied using this technique (Peng et al. 2012).
5.5 PET/MRI
Simultaneous small animal PET and MRI has been successfully applied for the study of cardiac metabolism and function in mice (Buscher et al. 2010) and rheumatoid arthritis in rats (Zhang et al. 2013). A recent animal study has indicated that FDG-PET and contrast-enhanced MRI may play complementary roles in the imaging of certain types of carcinomas characterized by poor FDG uptake and abundant cancer-associated stroma, as FDG-PET alone is not sufficient to estimate the total tumor burden for radiotherapy planning (Farace et al. 2012).
In conclusion, combination of PET or SPECT imaging with data from other modalities (CT, MRI, and ultrasound) may offer significant advantages. The precise anatomical location of tracer uptake (e.g., in segments of the heart, atherosclerotic plaques, lymph nodes, brown fat, abdominal organs, and small tumor metastases) can be determined. Data from CT or MRI also allow more accurate correction for partial volume effects besides attenuation and scatter of the emitted gamma radiation. Although multimodality imaging may result in longer scanning protocols (and thus may be more challenging from the perspective of animal care and maintenance of homeostasis), the resulting increase of information will definitely have added value. With multimodality scanners, comprehensive data sets can be collected on multiple physiological events, e.g., regional blood flow, glucose metabolism and drug-receptor interaction, or regional brain stimulation and neurotransmitter synthesis.
References
Adachi YU, Yamada S, Satomoto M, Higuchi H, Watanabe K, Kazama T. Isoflurane anesthesia induces biphasic effect on dopamine release in the rat striatum. Brain Res Bull. 2005;67:176–81.
Alstrup AK, Smith DF. Anaesthesia for positron emission tomography scanning of animal brains. Lab Anim. 2013;47:12–8.
Alstrup AK, Simonsen M, Landau AM. Type of anesthesia influences positron emission tomography measurements of dopamine D2/D3 receptor binding in the rat brain. Scand J Lab Anim Sci. 2011;38:195–200.
Alstrup AK, Landau AM, Holden JE, Jakobsen S, Schacht AC, Audrain H, Wegener G, Hansen AK, Gjedde A, Doudet DJ. Effects of anesthesia and species on the uptake or binding of radioligands in vivo in the Göttingen minipig. Biomed Res Int. 2013;2013:808713.
Asgharian B, Kelly JT, Tewksbury EW. Respiratory deposition and inhalability of monodisperse aerosols in Long-Evans rats. Toxicol Sci. 2003;71:104–11.
Baba JS, Endres CJ, Foss CA, Nimmagadda S, Jung H, Goddard JS, Lee S, McKisson J, Smith MF, Stolin AV, Weisenberger AG, Pomper MG. Molecular imaging of conscious, unrestrained mice with AwakeSPECT. J Nucl Med. 2013;54:969–76.
Becerra L, Chang PC, Bishop J, Borsook D. CNS activation maps in awake rats exposed to thermal stimuli to the dorsum of the hindpaw. Neuroimage. 2011;54:1355–66.
Brown K, Badar A, Sunassee K, Fernandes MA, Shariff H, Jurcevic S, Blower PJ, Sacks SH, Mullen GE, Wong W. SPECT/CT lymphoscintigraphy of heterotopic cardiac grafts reveals novel sites of lymphatic drainage and T cell priming. Am J Transplant. 2011;11:225–34.
Buscher K, Judenhofer MS, Kuhlmann MT, Hermann S, Wehrl HF, Schäfers KP, Schäfers M, Pichler BJ, Stegger L. Isochronous assessment of cardiac metabolism and function in mice using hybrid PET/MRI. J Nucl Med. 2010;51:1277–84.
Byas-Smith MG, Li J, Szlam F, Eaton DC, Votaw JR, Denson DD. Isoflurane induces dopamine transporter trafficking into the cell cytoplasm. Synapse. 2004;53:68–73.
Carlson SK, Classic KL, Hadac EM, Bender CE, Kemp BJ, Lowe VJ, Hoskin TL, Russell SJ. In vivo quantitation of intratumoral radioisotope uptake using micro-single photon emission computed tomography/computed tomography. Mol Imaging Biol. 2006;8:324–32.
Casteels C, Bormans G, Van Laere K. The effect of anaesthesia on [18F]MK-9470 binding to the type 1 cannabinoid receptor in the rat brain. Eur J Nucl Med Mol Imaging. 2010;37:1164–73.
Cavazzuti M, Porro CA, Biral GP, Benassi C, Barbieri GC. Ketamine effects on local cerebral blood flow and metabolism in the rat. J Cereb Blood Flow Metab. 1987;7:806–11.
Chen YY, Shih YY, Lo YC, Lu PL, Tsang S, Jaw FS, Liu RS. MicroPET imaging of noxious thermal stimuli in the conscious rat brain. Somatosens Mot Res. 2010;27:69–81.
Chiang N, Schwab JM, Fredman G, Kasuga K, Gelman S, Serhan CN. Anesthetics impact the resolution of inflammation. PLoS One. 2008;3:e1879.
Crosby G, Crane AM, Sokoloff L. Local changes in cerebral glucose utilization during ketamine anesthesia. Anesthesiology. 1982;56:437–43.
Croteau E, Benard F, Bentourkia M, Rousseau J, Paquette M, Lecomte R. Quantitative myocardial perfusion and coronary reserve in rats with 13N-ammonia and small animal PET: impact of anesthesia and pharmacologic stress agents. J Nucl Med. 2004;45:1924–30.
Dam M, Ori C, Pizzolato G, Ricchieri GL, Pellegrini A, Giron GP, Battistin L. The effects of propofol anesthesia on local cerebral glucose utilization in the rat. Anesthesiology. 1990;73:499–505.
Du C, Tully M, Volkow ND, Schiffer WK, Yu M, Luo Z, Koretsky AP, Benveniste H. Differential effects of anesthetics on cocaine’s pharmacokinetic and pharmacodynamic effects in brain. Eur J Neurosci. 2009;30:1565–75.
Eintrei C, Sokoloff L, Smith CB. Effects of diazepam and ketamine administered individually or in combination on regional rates of glucose utilization in rat brain. Br J Anaesth. 1999;82:596–602.
Elfving B, Bjornholm B, Knudsen GM. Interference of anaesthetics with radioligand binding in neuroreceptor studies. Eur J Nucl Med Mol Imaging. 2003;30:912–5.
Farace P, Conti G, Merigo F, Tambalo S, Marzola P, Sbarbati A, Quarta C, D’Ambrosio D, Chondrogiannis S, Nanni C, Rubello D. Potential role of combined FDG PET/CT and contrast enhancement MRI in a rectal carcinoma model with nodal metastases characterized by a poor FDG-avidity. Eur J Radiol. 2012;81:658–62.
Fendrich V, Schneider R, Maitra A, Jacobsen ID, Opfermann T, Bartsch DK. Detection of precursor lesions of pancreatic adenocarcinoma in PET-CT in a genetically engineered mouse model of pancreatic cancer. Neoplasia. 2011;13:180–6.
Ferris CF, Febo M, Luo F, Schmidt K, Brevard M, Harder JA, Kulkarni P, Messenger T, King JA. Functional magnetic resonance imaging in conscious animals: a new tool in behavioural neuroscience research. J Neuroendocrinol. 2006;18:307–18.
Flores JE, McFarland LM, Vanderbilt A, Ogasawara AK, Williams SP. The effects of anesthetic agent and carrier gas on blood glucose and tissue uptake in mice undergoing dynamic FDG-PET imaging: sevoflurane and isoflurane compared in air and in oxygen. Mol Imaging Biol. 2008;10:192–200.
Flores LG, Bertolini S, Yeh HH, Young D, Mukhopadhyay U, Pal A, Ying Y, Volgin A, Shavrin A, Soghomonyan S, Tong W, Bornmann W, Alauddin MM, Logsdon C, Gelovani JG. Detection of pancreatic carcinomas by imaging lactose-binding protein expression in peritumoral pancreas using [18F]fluoroethyl-deoxylactose PET/CT. PLoS One. 2009;4:e7977.
Ford AP, Marsden CA. Influence of anaesthetics on rat striatal dopamine metabolism in vivo. Brain Res. 1986;379:162–6.
Fortis S, Spieth PM, Lu WY, Parotto M, Haitsma JJ, Slutsky AS, Zhong N, Mazer CD, Zhang H. Effects of anesthetic regimes on inflammatory responses in a rat model of acute lung injury. Intensive Care Med. 2012;38:1548–55.
Fuchs K, Kukuk D, Mahling M, Quintanilla-Martinez L, Reischl G, Reutershan J, Lang F, Rocken M, Pichler BJ, Kneilling M. Impact of anesthetics on 3’-[18F]fluoro-3’-deoxythymidine ([18F]FLT) uptake in animal models of cancer and inflammation. Mol Imaging. 2013;12:277–87.
Fueger BJ, Czernin J, Hildebrandt I, Tran C, Halpern BS, Stout D, Phelps ME, Weber WA. Impact of animal handling on the results of 18F-FDG PET studies in mice. J Nucl Med. 2006;47:999–1006.
Gargiulo S, Greco A, Gramanzini M, Esposito S, Affuso A, Brunetti A, Vesce G. Mice anesthesia, analgesia, and care, Part I: anesthetic considerations in preclinical research. ILARJ. 2012a;53:E55–69.
Gargiulo S, Greco A, Gramanzini M, Esposito S, Affuso A, Brunetti A, Vesce G. Mice anesthesia, analgesia, and care, Part II: anesthetic considerations in preclinical imaging studies. ILARJ. 2012b;53:E70–81.
Gargiulo S, Greco A, Gramanzini M, Petretta MP, Ferro A, Larobina M, Panico M, Brunetti A, Cuocolo A. PET/CT imaging in mouse models of myocardial ischemia. J Biomed Biotechnol. 2012c;2012:541872.
Garrison JC, Rold TL, Sieckman GL, Figueroa SD, Volkert WA, Jurisson SS, Hoffman TJ. In vivo evaluation and small-animal PET/CT of a prostate cancer mouse model using 64Cu bombesin analogs: side-by-side comparison of the CB-TE2A and DOTA chelation systems. J Nucl Med. 2007;48:1327–37.
Gildehaus FJ, Haasters F, Drosse I, Wagner E, Zach C, Mutschler W, Cumming P, Bartenstein P, Schieker M. Impact of indium-111 oxine labelling on viability of human mesenchymal stem cells in vitro, and 3D cell-tracking using SPECT/CT in vivo. Mol Imaging Biol. 2011;13:1204–14.
Gjedde A, Rasmussen M. Pentobarbital anesthesia reduces blood-brain glucose transfer in the rat. J Neurochem. 1980;35:1382–7.
Goethals LR, De GF, Vanhove C, Roosens B, Devos H, Lahoutte T. Improved quantification in pinhole gated myocardial perfusion SPECT using micro-CT and ultrasound information. Contrast Media Mol Imaging. 2012;7:167–74.
Greco A, Petretta MP, Larobina M, Gargiulo S, Panico M, Nekolla SG, Esposito G, Petretta M, Brunetti A, Cuocolo A. Reproducibility and accuracy of non-invasive measurement of infarct size in mice with high-resolution PET/CT. J Nucl Cardiol. 2012;19:492–9.
Greeuw I, Bergstra R. Retro-orbitale injectie van radioactieve stoffen bij gebruik in een PET scanner. Biotechniek. 2013;5:9–14.
Groman EV, Reinhardt CP. Method to quantify tail vein injection technique in small animals. Contemp Top Lab Anim Sci. 2004;43:35–8.
Hall RI, Ross LH, Bozovic M, Grant JP. A simple method of obtaining repeated venous blood samples from the conscious rat. J Surg Res. 1984;36:92–5.
Hansen TD, Warner DS, Todd MM, Vust LJ, Trawick DC. Distribution of cerebral blood flow during halothane versus isoflurane anesthesia in rats. Anesthesiology. 1988;69:332–7.
Hanusch C, Hoeger S, Beck GC. Anaesthesia of small rodents during magnetic resonance imaging. Methods. 2007;43:68–78.
Hayakawa T, Mutoh M, Imai T, Tsuta K, Yanaka A, Fujii H, Yoshimoto M. SPECT/CT of lung nodules using 111In-DOTA-c(RGDfK) in a mouse lung carcinogenesis model. Ann Nucl Med. 2013;27:640–7.
Hendrich KS, Kochanek PM, Melick JA, Schiding JK, Statler KD, Williams DS, Marion DW, Ho C. Cerebral perfusion during anesthesia with fentanyl, isoflurane, or pentobarbital in normal rats studied by arterial spin-labeled MRI. Magn Reson Med. 2001;46:202–6.
Herzog H. PET/MRI: challenges, solutions and perspectives. Z Med Phys. 2012;22:281–98.
Herzog H, Pietrzyk U, Shah NJ, Ziemons K. The current state, challenges and perspectives of MR-PET. Neuroimage. 2010;49:2072–82.
Hildebrandt IJ, Su H, Weber WA. Anesthesia and other considerations for in vivo imaging of small animals. ILARJ. 2008;49:17–26.
Hodes JE, Soncrant TT, Larson DM, Carlson SG, Rapoport SI. Selective changes in local cerebral glucose utilization induced by phenobarbital in the rat. Anesthesiology. 1985;63:633–9.
Hosoi R, Matsumura A, Mizokawa S, Tanaka M, Nakamura F, Kobayashi K, Watanabe Y, Inoue O. MicroPET detection of enhanced 18F-FDG utilization by PKA inhibitor in awake rat brain. Brain Res. 2005;1039:199–202.
Huhtala T, Laakkonen P, Sallinen H, Yla-Herttuala S, Narvanen A. In vivo SPECT/CT imaging of human orthotopic ovarian carcinoma xenografts with 111In-labeled monoclonal antibodies. Nucl Med Biol. 2010;37:957–64.
Itoh T, Abe K, Zoghbi SS, Inoue O, Hong J, Imaizumi M, Pike VW, Innis RB, Fujita M. PET measurement of the in vivo affinity of 11C-(R)-rolipram and the density of its target, phosphodiesterase-4, in the brains of conscious and anesthetized rats. J Nucl Med. 2009;50:749–56.
Jan ML, Chuang KS, Chen GW, Ni YC, Chen S, Chang CH, Wu J, Lee TW, Fu YK. A three-dimensional registration method for automated fusion of micro PET-CT-SPECT whole-body images. IEEE Trans Med Imaging. 2005;24:886–93.
Jespersen B, Knupp L, Northcott CA. Femoral arterial and venous catheterization for blood sampling, drug administration and conscious blood pressure and heart rate measurements. J Vis Exp. 2012;59:(pii: 3496).
Jobse BN, Rhem RG, McCurry CA, Wang IQ, Labiris NR. Imaging lung function in mice using SPECT/CT and per-voxel analysis. PLoS One. 2012;7:e42187.
Judenhofer MS, Wehrl HF, Newport DF, Catana C, Siegel SB, Becker M, Thielscher A, Kneilling M, Lichy MP, Eichner M, Klingel K, Reischl G, Widmaier S, Rocken M, Nutt RE, Machulla HJ, Uludag K, Cherry SR, Claussen CD, Pichler BJ. Simultaneous PET-MRI: a new approach for functional and morphological imaging. Nat Med. 2008;14:459–65.
Kersemans V, Cornelissen B, Hueting R, Tredwell M, Hussien K, Allen PD, Falzone N, Hill SA, Dilworth JR, Gouverneur V, Muschel RJ, Smart SC. Hypoxia imaging using PET and SPECT: the effects of anesthetic and carrier gas on [64Cu]-ATSM, [99mTc]-HL91 and [18F]-FMISO tumor hypoxia accumulation. PLoS One. 2011;6:e25911.
Kilbourn MR, Ma B, Butch ER, Quesada C, Sherman PS. Anesthesia increases in vivo N-([18F]fluoroethyl)piperidinyl benzilate binding to the muscarinic cholinergic receptor. Nucl Med Biol. 2007;34:479–82.
King JA, Garelick TS, Brevard ME, Chen W, Messenger TL, Duong TQ, Ferris CF. Procedure for minimizing stress for fMRI studies in conscious rats. J Neurosci Methods. 2005;148:154–60.
Kononov A, Browne EZ, Alexander F, Porvasnik S. Continuous rat intravenous infusion. Microsurgery. 1994;15:443–5.
Kubota K, Fukuda H, Yamada K, Endo S, Ito M, Abe Y, Yamaguchi T, Fujiwara T, Sato T, Yamaura H. Experimental pancreas imaging study with 13N-glutamate using positron computer tomography. Eur J Nucl Med. 1983;8:528–30.
Kuehl PJ, Anderson TL, Candelaria G, Gershman B, Harlin K, Hesterman JY, Holmes T, Hoppin J, Lackas C, Norenberg JP, Yu H, McDonald JD. Regional particle size dependent deposition of inhaled aerosols in rats and mice. Inhal Toxicol. 2012;24:27–35.
Lahti KM, Ferris CF, Li F, Sotak CH, King JA. Imaging brain activity in conscious animals using functional MRI. J Neurosci Methods. 1998;82:75–83.
LaManna JC, Harik SI. Regional studies of blood-brain barrier transport of glucose and leucine in awake and anesthetized rats. J Cereb Blood Flow Metab. 1986;6:717–23.
Lasnon C, Quak E, Briand M, Gu Z, Louis MH, Aide N. Contrast-enhanced small-animal PET/CT in cancer research: strong improvement of diagnostic accuracy without significant alteration of quantitative accuracy and NEMA NU 4-2008 image quality parameters. EJNMMI Res. 2013;3:5.
Lee KH, Ko BH, Paik JY, Jung KH, Choe YS, Choi Y, Kim BT. Effects of anesthetic agents and fasting duration on 18F-FDG biodistribution and insulin levels in tumor-bearing mice. J Nucl Med. 2005;46:1531–6.
Lenz C, Rebel A, Van AK, Kuschinsky W, Waschke KF. Local cerebral blood flow, local cerebral glucose utilization, and flow-metabolism coupling during sevoflurane versus isoflurane anesthesia in rats. Anesthesiology. 1998;89:1480–8.
Lenz C, Frietsch T, Futterer C, Rebel A, Van AK, Kuschinsky W, Waschke KF. Local coupling of cerebral blood flow to cerebral glucose metabolism during inhalational anesthesia in rats: desflurane versus isoflurane. Anesthesiology. 1999;91:1720–3.
Li D, Patel AR, Klibanov AL, Kramer CM, Ruiz M, Kang BY, Mehta JL, Beller GA, Glover DK, Meyer CH. Molecular imaging of atherosclerotic plaques targeted to oxidized LDL receptor LOX-1 by SPECT/CT and magnetic resonance. Circ Cardiovasc Imaging. 2010;3:464–72.
Li ZC, Jiang SD, Yan J, Jiang LS, Dai LY. Small-animal PET/CT assessment of bone microdamage in ovariectomized rats. J Nucl Med. 2011;52:769–75.
Lin KJ, Liu HL, Hsu PH, Chung YH, Huang WC, Chen JC, Wey SP, Yen TC, Hsiao IT. Quantitative micro-SPECT/CT for detecting focused ultrasound-induced blood-brain barrier opening in the rat. Nucl Med Biol. 2009;36:853–61.
Maekawa T, Tommasino C, Shapiro HM, Keifer-Goodman J, Kohlenberger RW. Local cerebral blood flow and glucose utilization during isoflurane anesthesia in the rat. Anesthesiology. 1986;65:144–51.
Maramraju SH, Smith SD, Junnarkar SS, Schulz D, Stoll S, Ravindranath B, Purschke ML, Rescia S, Southekal S, Pratte JF, Vaska P, Woody CL, Schlyer DJ. Small animal simultaneous PET/MRI: initial experiences in a 9.4 T microMRI. Phys Med Biol. 2011;56:2459–80.
Mashhedi H, Blouin MJ, Zakikhani M, David S, Zhao Y, Bazile M, Birman E, Algire C, Aliaga A, Bedell BJ, Pollak M. Metformin abolishes increased tumor [18F]-2-fluoro-2-deoxy-D-glucose uptake associated with a high energy diet. Cell Cycle. 2011;10:2770–8.
Matsumura A, Mizokawa S, Tanaka M, Wada Y, Nozaki S, Nakamura F, Shiomi S, Ochi H, Watanabe Y. Assessment of microPET performance in analyzing the rat brain under different types of anesthesia: comparison between quantitative data obtained with microPET and ex vivo autoradiography. Neuroimage. 2003;20:2040–50.
McCormick PN, Ginovart N, Wilson AA. Isoflurane anaesthesia differentially affects the amphetamine sensitivity of agonist and antagonist D2/D3 positron emission tomography radiotracers: implications for in vivo imaging of dopamine release. Mol Imaging Biol. 2011;13:737–46.
Mirbolooki MR, Upadhyay SK, Constantinescu CC, Pan ML, Mukherjee J. Adrenergic pathway activation enhances brown adipose tissue metabolism: a [18F]FDG PET/CT study in mice. Nucl Med Biol. 2014;41:10–6.
Mizuma H, Shukuri M, Hayashi T, Watanabe Y, Onoe H. Establishment of in vivo brain imaging method in conscious mice. J Nucl Med. 2010;51:1068–75.
Momosaki S, Hatano K, Kawasumi Y, Kato T, Hosoi R, Kobayashi K, Inoue O, Ito K. Rat-PET study without anesthesia: anesthetics modify the dopamine D1 receptor binding in rat brain. Synapse. 2004;54:207–13.
Nahrendorf M, Zhang H, Hembrador S, Panizzi P, Sosnovik DE, Aikawa E, Libby P, Swirski FK, Weissleder R. Nanoparticle PET-CT imaging of macrophages in inflammatory atherosclerosis. Circulation. 2008;117:379–87.
Nahrendorf M, Keliher E, Panizzi P, Zhang H, Hembrador S, Figueiredo JL, Aikawa E, Kelly K, Libby P, Weissleder R. [18F]-4V for PET-CT imaging of VCAM-1 expression in atherosclerosis. JACC Cardiovasc Imaging. 2009;2:1213–22.
Nanni C, Pettinato C, Ambrosini V, Spinelli A, Trespidi S, Rubello D, Al-Nahhas A, Franchi R, Alavi A, Fanti S. Retro-orbital injection is an effective route for radiopharmaceutical administration in mice during small-animal PET studies. Nucl Med Commun. 2007;28:547–53.
Nayak TK, Bernardo M, Milenic DE, Choyke PL, Brechbiel MW. Orthotopic pleural mesothelioma in mice: SPECT/CT and MR imaging with HER1- and HER2-targeted radiolabeled antibodies. Radiology. 2013;267:173–82.
Ori C, Dam M, Pizzolato G, Battistin L, Giron G. Effects of isoflurane anesthesia on local cerebral glucose utilization in the rat. Anesthesiology. 1986;65:152–6.
Osborne DR, Yan S, Stuckey A, Pryer L, Richey T, Wall JS. Characterization of X-ray dose in murine animals using microCT, a New Low-Dose detector and nanoDot dosimeters. PLoS One. 2012;7:e49936.
Palko HA, Fung JY, Louie AY. Positron emission tomography: a novel technique for investigating the biodistribution and transport of nanoparticles. Inhal Toxicol. 2010;22:657–88.
Park SS, Chunta JL, Robertson JM, Martinez AA, Oliver Wong CY, Amin M, Wilson GD, Marples B. MicroPET/CT imaging of an orthotopic model of human glioblastoma multiforme and evaluation of pulsed low-dose irradiation. Int J Radiat Oncol Biol Phys. 2011;80:885–92.
Pascau J, Vaquero JJ, Chamorro-Servent J, Rodriguez-Ruano A, Desco M. A method for small-animal PET/CT alignment calibration. Phys Med Biol. 2012;57:N199–207.
Patel VD, Lee DE, Alexoff DL, Dewey SL, Schiffer WK. Imaging dopamine release with positron emission tomography (PET) and [11C]-raclopride in freely moving animals. Neuroimage. 2008;41:1051–66.
Paul R, Kiuru A, Soderstrom KO, Tuominen J, Johansson R, Haaparanta M, Roeda D, Solin O. Organ and tumor distribution of [18F]-2-fluoro-2-deoxy-D-glucose in fasting and non-fasting rats. Life Sci. 1987;40:1609–16.
Paul S, Khanapur S, Sijbesma JW, Ishiwata K, Elsinga PH, Meerlo P, Dierckx RA, Van Waarde A. Use of [11C]-MPDX and PET to study adenosine A1 receptor occupancy by nonradioactive agonists and antagonists. JNuclMed. 2014;55:315–20.
Peng F, Lutsenko S, Sun X, Muzik O. Imaging copper metabolism imbalance in Atp7b (-/-) knockout mouse model of Wilson’s disease with PET-CT and orally administered [64Cu]Cl2. Mol Imaging Biol. 2012;14:600–7.
Peternel L, Skrajnar S, Cerne M. A comparative study of four permanent cannulation procedures in rats. J Pharmacol Toxicol Methods. 2010;61:20–6.
Petroni D, Menichetti L, Sorace O, Poli M, Vanasia M, Salvadori PA. [11C]diclofenac sodium: synthesis and PET assessment of transdermal penetration. Nucl Med Biol. 2011;38:181–9.
Pool SE, ten Hagen TL, Koelewijn S, de J M, Koning GA. Multimodality imaging of somatostatin receptor-positive tumors with nuclear and bioluminescence imaging. Mol Imaging. 2012;11:27–32.
Radonjic M, Cappaert NL, de Vries EF, de Esch CE, Kuper FC, van Waarde A, Dierckx RA, Wadman WJ, Wolterbeek AP, Stierum RH, de Groot DM. Delay and impairment in brain development and function in rat offspring after maternal exposure to methylmercury. Toxicol Sci. 2013;133:112–24.
Raty JK, Liimatainen T, Huhtala T, Kaikkonen MU, Airenne KJ, Hakumaki JM, Narvanen A, Yla-Herttuala S. SPECT/CT imaging of baculovirus biodistribution in rat. Gene Ther. 2007;14:930–8.
Raylman RR, Majewski S, Velan SS, Lemieux S, Kross B, Popov V, Smith MF, Weisenberger AG. Simultaneous acquisition of magnetic resonance spectroscopy (MRS) data and positron emission tomography (PET) images with a prototype MR-compatible, small animal PET imager. J Magn Reson. 2007;186:305–10.
Rybczynska AA, Elsinga PH, Sijbesma JW, Ishiwata K, de Jong JR, de Vries EF, Dierckx RA, van Waarde A. Steroid hormones affect binding of the sigma ligand [11C]-SA4503 in tumour cells and tumour-bearing rats. Eur J Nucl Med Mol Imaging. 2009;36:1167–75.
Saija A, Princi P, De PR, Costa G. Modifications of the permeability of the blood-brain barrier and local cerebral metabolism in pentobarbital- and ketamine-anaesthetized rats. Neuropharmacology. 1989;28:997–1002.
Sanchez F, Orero A, Soriano A, Correcher C, Conde P, Gonzalez A, Hernandez L, Moliner L, Rodriguez-Alvarez MJ, Vidal LF, Benlloch JM, Chapman SE, Leevy WM. ALBIRA: a small animal PETSPECTCT imaging system. Med Phys. 2013;40:051906.
Saraste A, Laitinen I, Weidl E, Wildgruber M, Weber AW, Nekolla SG, Holzlwimmer G, Esposito I, Walch A, Leppanen P, Lisinen I, Luppa PB, Yla-Herttuala S, Wester HJ, Knuuti J, Schwaiger M. Diet intervention reduces uptake of alphavbeta3 integrin-targeted PET tracer [18F]-galacto-RGD in mouse atherosclerotic plaques. J Nucl Cardiol. 2012;19:775–84.
Sarparanta M, Makila E, Heikkila T, Salonen J, Kukk E, Lehto VP, Santos HA, Hirvonen J, Airaksinen AJ. [18]F-labeled modified porous silicon particles for investigation of drug delivery carrier distribution in vivo with positron emission tomography. MolPharm. 2011;8:1799–806.
Schiffer WK, Mirrione MM, Dewey SL. Optimizing experimental protocols for quantitative behavioral imaging with [18F]-FDG in rodents. J Nucl Med. 2007;48:277–87.
Schoell AR, Heyde BR, Weir DE, Chiang PC, Hu Y, Tung DK. Euthanasia method for mice in rapid time-course pulmonary pharmacokinetic studies. J Am Assoc Lab Anim Sci. 2009;48:506–11.
Schulz D, Southekal S, Junnarkar SS, Pratte JF, Purschke ML, Stoll SP, Ravindranath B, Maramraju SH, Krishnamoorthy S, Henn FA, O’Connor P, Woody CL, Schlyer DJ, Vaska P. Simultaneous assessment of rodent behavior and neurochemistry using a miniature positron emission tomograph. Nat Methods. 2011;8:347–52.
Seo Y, Gao DW, Hasegawa BH, Dae MW, Franc BL. Rodent brain imaging with SPECT/CT. Med Phys. 2007;34:1217–20.
Shahani SK, Lingamaneni R, Hemmings HC. General anesthetic actions on norepinephrine, dopamine, and gamma-aminobutyric acid transporters in stably transfected cells. Anesth Analg. 2002;95:893–9, table.
Shih YY, Chiang YC, Chen JC, Huang CH, Chen YY, Liu RS, Chang C, Jaw FS. Brain nociceptive imaging in rats using [18F]-fluorodeoxyglucose small-animal positron emission tomography. Neuroscience. 2008;155:1221–6.
Shingaki T, Takashima T, Wada Y, Tanaka M, Kataoka M, Ishii A, Shigihara Y, Sugiyama Y, Yamashita S, Watanabe Y. Imaging of gastrointestinal absorption and biodistribution of an orally administered probe using positron emission tomography in humans. Clin Pharmacol Ther. 2012;91:653–9.
Silvola JM, Saraste A, Laitinen I, Savisto N, Laine VJ, Heinonen SE, Yla-Herttuala S, Saukko P, Nuutila P, Roivainen A, Knuuti J. Effects of age, diet, and type 2 diabetes on the development and FDG uptake of atherosclerotic plaques. JACC Cardiovasc Imaging. 2011;4:1294–301.
Sokoloff L, Reivich M, Kennedy C, Des Rosiers MH, Patlak CS, Pettigrew KD, Sakurada O, Shinohara M. The [14C]deoxyglucose method for the measurement of local cerebral glucose utilization: theory, procedure, and normal values in the conscious and anesthetized albino rat. J Neurochem. 1977;28:897–916.
Solomon M, Nothdruft RE, Akers W, Edwards WB, Liang K, Xu B, Suddlow GP, Deghani H, Tai YC, Eggebrecht AT, Achilefu S, Culver JP. Multimodal fluorescence-mediated tomography and SPECT/CT for small-animal imaging. J Nucl Med. 2013;54:639–46.
Steel CD, Stephens AL, Hahto SM, Singletary SJ, Ciavarra RP. Comparison of the lateral tail vein and the retro-orbital venous sinus as routes of intravenous drug delivery in a transgenic mouse model. Lab Anim (NY). 2008;37:26–32.
Szymanski MK, Kruizinga S, Tio RA, Willemsen AT, Schäfers MA, Stegger L, Dierckx RA, Hillege HL, Slart RH. Use of gated [13N]-NH3 micro-PET to examine left ventricular function in rats. Nucl Med Biol. 2012;39:724–9.
Tahari AK, Lodge MA, Wahl RL. Respiratory-gated PET/CT versus delayed images for the quantitative evaluation of lower pulmonary and hepatic lesions. J Med Imaging Radiat Oncol. 2014;58:277–82.
Tantawy MN, Peterson TE, Jones CK, Johnson K, Rook JM, Conn PJ, Baldwin RM, Ansari MS, Kessler RM. Impact of isoflurane anesthesia on D2 receptor occupancy by [18F]fallypride measured by microPET with a modified Logan plot. Synapse. 2011;65:1173–80.
Taschereau R, Chow PL, Chatziioannou AF. Monte Carlo simulations of dose from microCT imaging procedures in a realistic mouse phantom. Med Phys. 2006;33:216–24.
Todd MM, Weeks J. Comparative effects of propofol, pentobarbital, and isoflurane on cerebral blood flow and blood volume. J Neurosurg Anesthesiol. 1996;8:296–303.
Tokugawa J, Ravasi L, Nakayama T, Lang L, Schmidt KC, Seidel J, Green MV, Sokoloff L, Eckelman WC. Distribution of the 5-HT1A receptor antagonist [18F]FPWAY in blood and brain of the rat with and without isoflurane anesthesia. Eur J Nucl Med Mol Imaging. 2007;34:259–66.
Toyama H, Ichise M, Liow JS, Vines DC, Seneca NM, Modell KJ, Seidel J, Green MV, Innis RB. Evaluation of anesthesia effects on [18F]FDG uptake in mouse brain and heart using small animal PET. Nucl Med Biol. 2004;31:251–6.
Tremoleda JL, Kerton A, Gsell W. Anaesthesia and physiological monitoring during in vivo imaging of laboratory rodents: considerations on experimental outcomes and animal welfare. EJNMMI Res. 2012;2:44.
Umeda IO, Tani K, Tsuda K, Kobayashi M, Ogata M, Kimura S, Yoshimoto M, Kojima S, Moribe K, Yamamoto K, Moriyama N, Fujii H. High resolution SPECT imaging for visualization of intratumoral heterogeneity using a SPECT/CT scanner dedicated for small animal imaging. Ann Nucl Med. 2012;26:67–76.
van Waarde A, Buursma AR, Hospers GA, Kawamura K, Kobayashi T, Ishii K, Oda K, Ishiwata K, Vaalburg W, Elsinga PH. Tumor imaging with 2 sigma-receptor ligands, [18F]-FE-SA5845 and [11C]-SA4503: a feasibility study. J Nucl Med. 2004;45:1939–45.
Vines DC, Green DE, Kudo G, Keller H. Evaluation of mouse tail-vein injections both qualitatively and quantitatively on small-animal PET tail scans. J Nucl Med Technol. 2011;39:264–70.
Votaw J, Byas-Smith M, Hua J, Voll R, Martarello L, Levey AI, Bowman FD, Goodman M. Interaction of isoflurane with the dopamine transporter. Anesthesiology. 2003;98:404–11.
Votaw JR, Byas-Smith MG, Voll R, Halkar R, Goodman MM. Isoflurane alters the amount of dopamine transporter expressed on the plasma membrane in humans. Anesthesiology. 2004;101:1128–35.
Walter MA, Hildebrandt IJ, Hacke K, Kesner AL, Kelly O, Lawson GW, Phelps ME, Czernin J, Weber WA, Schiestl RH. Small-animal PET/CT for monitoring the development and response to chemotherapy of thymic lymphoma in Trp53-/- mice. J Nucl Med. 2010;51:1285–92.
Watabe T, Shimosegawa E, Watabe H, Kanai Y, Hanaoka K, Ueguchi T, Isohashi K, Kato H, Tatsumi M, Hatazawa J. Quantitative evaluation of cerebral blood flow and oxygen metabolism in normal anesthetized rats: [15O]-labeled gas inhalation PET with MRI Fusion. J Nucl Med. 2013;54:283–90.
Wong KP, Sha W, Zhang X, Huang SC. Effects of administration route, dietary condition, and blood glucose level on kinetics and uptake of [18F]-FDG in mice. J Nucl Med. 2011;52:800–7.
Woo SK, Lee TS, Kim KM, Kim JY, Jung JH, Kang JH, Cheon GJ, Choi CW, Lim SM. Anesthesia condition for [18F]-FDG imaging of lung metastasis tumors using small animal PET. Nucl Med Biol. 2008;35:143–50.
Yamashita S, Takashima T, Kataoka M, Oh H, Sakuma S, Takahashi M, Suzuki N, Hayashinaka E, Wada Y, Cui Y, Watanabe Y. PET imaging of the gastrointestinal absorption of orally administered drugs in conscious and anesthetized rats. J Nucl Med. 2011;52:249–56.
Yang FY, Wang HE, Lin GL, Teng MC, Lin HH, Wong TT, Liu RS. Micro-SPECT/CT-based pharmacokinetic analysis of [99mTc]-diethylenetriaminepentaacetic acid in rats with blood-brain barrier disruption induced by focused ultrasound. J Nucl Med. 2011;52:478–84.
Yee SH, Lee K, Jerabek PA, Fox PT. Quantitative measurement of oxygen metabolic rate in the rat brain using microPET imaging of briefly inhaled [15O]-labelled oxygen gas. Nucl Med Commun. 2006;27:573–81.
Yoder KK, Mock BH, Zheng QH, McCarthy BP, Riley AA, Hutchins GD. Assessment of i.p. injection of [18F]fallypride for behavioral neuroimaging in rats. J Neurosci Methods. 2011;196:70–5.
Yu M, Guaraldi MT, Bozek J, Kagan M, Azure M, Radeke H, Cdebaca M, Robinson SP. Effects of food intake and anesthetic on cardiac imaging and uptake of BMS747158-02 in comparison with FDG. J Nucl Cardiol. 2009;16:763–8.
Zanelli GD, Lucas PB, Fowler JF. The effect of anaesthetics on blood perfusion in transplanted mouse tumours. Br J Cancer. 1975;32:380–90.
Zhang WT DUXK, Huo TL, Wei ZM, Hao CX, An B. Combination of [18F]-fluorodeoxyglucose positron emission tomography/computed tomography and magnetic resonance imaging is an optimal way to evaluate rheumatoid arthritis in rats dynamically. Chin Med J (Engl). 2013;126:3732–8.
Zutphen LFM, Baumans V, Beynen AC. Principles of laboratory animal science, Revised Edition edn. Amsterdam: Elsevier; 2001.
Disclaimer
This chapter could only discuss some important aspects of animal handling related to our own field of expertise. Species other than mice or rats (e.g., guinea pigs, ferrets, Göttingen minipigs, cynomolgus monkeys, and baboons) are used by many institutions in the preclinical evaluation of PET tracers. For information about such species, the reader should consult the specialized literature.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Sijbesma, J.W.A., Doorduin, J., van Waarde, A. (2017). Zootechnical Issues in Small Animal Imaging. In: Glaudemans, A., Medema, J., van Zanten, A., Dierckx, R., Ahaus, C. (eds) Quality in Nuclear Medicine. Springer, Cham. https://doi.org/10.1007/978-3-319-33531-5_18
Download citation
DOI: https://doi.org/10.1007/978-3-319-33531-5_18
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-33529-2
Online ISBN: 978-3-319-33531-5
eBook Packages: MedicineMedicine (R0)