Abstract
Voltage-gated calcium channels are evolutionarily related transmembrane signaling proteins that mediate calcium entry during action potentials and other forms of cellular depolarization in order to trigger neurotransmission, secretion, contraction, gene transcription, and other physiological processes. Calcium channels are the molecular targets for several major classes of drugs used in the treatment of cardiovascular disorders, pain, and epilepsy. Recent advances in the structural biology of these proteins using X-ray crystallography and cryogenic electron microscopy have given new insights into the molecular basis of their function and pharmacology. Here I review the major classes of drugs and neurotoxins that act on voltage-gated calcium channels and elucidate their complex pharmacology at the atomic level. New understanding of the diseases and therapeutics of these channel proteins will arise from the emerging mechanistic principles derived from these recent structural analyses.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Calcium Channel Pharmacology
Neurotoxins and calcium channel antagonist drugs inhibit members of each of the three major calcium channel families, often with high specificity and potency (Triggle, 2003; Zamponi et al., 2015). The L-type calcium currents conducted by calcium channels of the CaV1 family are blocked by three chemically distinct classes of drugs: phenylalkylamines, benzothiazepines, and dihydropyridines (Fleckenstein, 1983; Hockerman et al., 1997b; Zamponi et al., 2015; Godfraind, 2017). These drugs are all used in the therapy of cardiovascular disorders. The phenylalkylamine verapamil and the benzothiazepine diltiazem are used primarily in the treatment of atrial arrhythmias, whereas dihydropyridines such as nifedipine and amlodipine are used primarily in the treatment of hypertension and angina pectoris (Fleckenstein, 1983; Hockerman et al., 1997b; Triggle, 2003; Sampson & Kass, 2011; Zamponi et al., 2015; Godfraind, 2017).
N-type calcium currents conducted by CaV2.2 channels, P/Q-type calcium currents conducted by CaV2.1 channels, and R-type calcium currents conducted by CaV2.3 channels trigger exocytosis of neurotransmitters from presynaptic nerve terminals (Olivera et al., 1994; Zamponi et al., 2015). These calcium channels are blocked by peptide neurotoxins, which paralyze the prey of cone snails, spiders, and other venomous animals (Olivera et al., 1994; Zamponi et al., 2015). They are specifically blocked by drugs that are either in current use or in active development for the treatment of epilepsy and chronic pain (Zamponi et al., 2015).
T-type calcium currents conducted by CaV3 channels are important in repetitively firing cells such as the specialized cardiomyocytes of the sino-atrial (SA) node in the heart and the reticular neurons and relay neurons in the thalamus (Perez-Reyes, 2003). Drugs that inhibit these calcium channels are in development for the treatment of cardiac arrhythmia, epilepsy, and chronic pain (Tringham et al., 2012; Bourinet et al., 2014; Zamponi et al., 2015).
Major advances in understanding the complex effects of these drugs on voltage-gated calcium channels have come from detailed electrophysiological studies, and the structural basis for their specific actions has been elucidated through X-ray crystallography and cryogenic electron microscopy (cryo-EM). In the sections below, I review the functional mechanisms for the actions of these drugs and neurotoxins, and then present recent work on the structures of their drug-receptor complexes on calcium channels.
State-Dependent Drug Block of CaV1 Channels
Among the classical voltage-gated calcium channel blockers, the phenylalkylamines and benzothiazepines are used primarily for cardiac arrhythmia (Triggle, 1999; Sampson & Kass, 2011; Godfraind, 2017). They have strongly frequency-dependent block, which enhances their action on calcium channels in rapidly firing injured cardiac myocytes that are responsible for arrhythmia relative to uninjured myocytes contracting at a normal rate (Hondeghem & Katzung, 1984). They are also effective in reducing the rate of rise of action potentials in the atrioventricular (AV) node. Therefore, they are effective in preventing re-entry of action potentials into the atria from the AV node and in slowing the conduction of action potentials from the atria to the ventricles via the AV node (Triggle, 1999; Sampson & Kass, 2011; Godfraind, 2017). In contrast, dihydropyridines are primarily used for hypertension and angina pectoris (Triggle, 1999; Godfraind, 2017). They have strongly voltage-dependent block, which is driven by high-affinity binding to voltage-dependent calcium channels in the inactivated state (Bean, 1984). They also bind with higher affinity to the isoform of CaV1.2 expressed in vascular smooth muscle (Welling et al., 1997). Therefore, through these two mechanisms, they preferentially inhibit calcium channels in continuously depolarized vascular smooth muscle cells that sustain contraction of blood vessels in hypertension and angina pectoris (Godfraind, 2017). State-dependent binding and action is essential for the clinical use of these calcium antagonist drugs.
The state-dependent block of sodium channels by local anesthetic and antiarrhythmic drugs is well described by the classical Modulated Receptor Hypothesis (Hille, 1977; Hondeghem & Katzung, 1977; Bean et al., 1983; Hille, 2001). In this model, drug block is frequency dependent because the receptor site is located in the pore and is more rapidly accessible for drug binding when the pore is open; therefore, generation of action potentials at high frequency increases drug block (Hille, 1977). Drug block is voltage dependent because these drugs bind to the inactivated state of sodium channels with high affinity; therefore, sodium channels in damaged, depolarized cells are preferentially blocked (Hille, 1977; Hondeghem & Katzung, 1984). Together, these mechanisms allow local anesthetic and antiarrhythmic drugs to prevent pain and cardiac arrhythmias without blocking normal sensory and cardiac function (Kanaya et al., 1983; Bean, 1984; Hondeghem & Katzung, 1984). Frequency-dependent block by phenylalkylamines and benzothiazepines results from binding in the pore, which is opened during each action potential and provides rapid drug access to their receptor site(s) (Kanaya et al., 1983). Voltage-dependent block by dihydropyridines results from preferential binding to the inactivated conformation of calcium channels (Bean, 1984). These two characteristic forms of block of CaV1 channels are illustrated in Fig. 1a, b for the model calcium channel CaVAb, a calcium-selective derivative of the ancestral bacterial sodium channel NaVAb (Tang et al., 2014). CaVAb has surprisingly high affinity for calcium-antagonist drugs, which leads to frequency- and voltage-dependent block at concentrations <10-fold higher than in mammalian cardiac calcium channels (Fig. 1; Ren et al., 2001; Tang et al., 2016). The phenylalkylamine verapamil enters the pore when it is open and progressively blocks the ionic current during single depolarizations (Fig. 1a, left). Repetitive stimulations at higher concentrations generate cumulative open channel block (Fig. 1a, right). In contrast, the dihydropyridine nimodipine does not cause rapid pore block during single depolarizing pulses that open the pore (Fig. 1b, left). However, repetitive depolarizations at increasing concentrations cause cumulative voltage-dependent block (Fig. 1b, right). Together, the frequency dependence and voltage dependence of drug action determine the clinical uses of these calcium-antagonist drugs for cardiac arrhythmia vs. hypertension and angina pectoris (Hondeghem & Katzung, 1984; Sampson & Kass, 2011; Godfraind, 2017).
State-dependent block and molecular mapping of the receptor sites for calcium antagonist drugs. (a) Left, top. Barium currents through CaVAb channels during depolarization from −120 mV to 0 mV for 50 ms in control (black) and in the presence of 10 μM Br-verapamil. Left, bottom. Use-Dependent Block of CavAb by 1 μM verapamil. Right. Amplitudes of peak barium currents during repetitive stimulation at 1 Hz at the following concentrations of Br-verapamil: 0 μM (black), 0.1 μM (gray), 0.5 μM (orange), 1 μM (blue), 5 μM (green), and 10 μM (red). (Adapted from Tang et al. 2016). (b) Left, top. Barium currents through CaVAb channels during depolarization from −120 mV to 0 mV for 50 ms in control (black) and 1 μM nimodipine (red). Left, bottom. Use-dependent block of CavAb by 5 μM nimodipine. Right. Amplitudes of peak barium currents during repetitive stimulation at the following concentrations of nimodipine: 5 nM (black), 25 nM (orange), 100 nM (blue), 1 μM (green), and 5 μM (red). (Adapted from Tang et al. 2016). (c) Domain Interface Model for dihydropyridine binding. Hatched segments show the sequences that were photoaffinity labeled with photoreactive drugs. (Adapted from Hockerman et al 1997b)
Drug Receptor Sites for State-Dependent Block of Calcium Channels
The initial molecular-mapping studies of the receptor site for calcium-antagonist drugs were based on photoaffinity labeling with photoreactive derivatives of phenylalkylamines and dihydropyridines (Striessnig et al., 1990, 1991; Nakayama et al., 1991). A photoreactive derivative of verapamil labeled the intracellular end of the S6 segment in domain IV (Striessnig et al., 1990). In contrast, photoreactive derivatives of dihydropyridines specifically labeled the outer half of both the IIIS6 and IVS6 segments (Nakayama et al., 1991; Striessnig et al., 1991). These results led to a domain-interface model for dihydropyridine binding in which dihydropyridines bind in a voltage-dependent manner to a site on the lipid-facing surface of the pore domain that is formed by the IIIS6 and IVS6 segments (Fig. 1c; Catterall & Striessnig, 1992). In contrast, pore-blocking phenylalkylamines were proposed to bind within the pore to a site on the IVS6 segment that is accessible from the intracellular end of the pore in the open state (Fig. 1c). This model of drug binding was confirmed and extended by extensive mapping of the receptor sites for phenylalkylamines (Hockerman et al., 1995; Hockerman et al., 1997a), benzothiazepines (Brauns et al., 1995; Kraus et al., 1996), and dihydropyridines (Mitterdorfer et al., 1996; Peterson et al., 1996) by site-directed mutagenesis, and the receptor site for dihydropyridines was constructed de novo by inserting mutations of nine or ten amino acid residues into the drug-binding IIIS6 and IVS6 transmembrane segments of drug-insensitive CaV2 channels (Hockerman et al., 1997c; Ito et al., 1997; Sinnegger et al., 1997). Altogether, these photoaffinity labeling and site-directed mutagenesis studies gave a detailed two-dimensional view of these separate, but closely spaced, drug receptor sites on calcium channels (Hockerman et al., 1997b; Hofmann et al., 1999; Striessnig, 1999).
Structures of the Drug Receptor Sites on CaVAb Channels
X-ray crystallography revealed two distinct receptor sites for phenylalkylamines and dihydropyridines on CaVAb in three dimensions (Fig. 2a; Tang et al., 2016). As expected, verapamil binds in the pore just at the intracellular exit from the ion selectivity filter into the central cavity (Fig. 2a, bottom; Tang et al., 2016). Its charged amino group projects upward into the pore, forming a complex with the backbone carbonyls of Thr175 at the intracellular end of the ion selectivity filter. Its two flanking aromatic moieties make hydrophobic interactions on either side of the ion-conducting pathway through the ion selectivity filter, staunching ion flow through the selectivity filter like a bandage (Fig. 2a, bottom, inset; Tang et al., 2016). X-ray crystallography studies indicated that the benzothiazepine diltiazem also binds in the pore of CaVAb in a position that partially overlaps the phenylalkylamine binding site (Tang et al., 2019). Moreover, the binding poses for verapamil and diltiazem partially overlap that of the sodium channel-blocking local anesthetic and antiarrhythmic drugs (Tang et al., 2016; Lenaeus et al., 2017; Gamal El-Din et al., 2018), suggesting that frequency-dependent block by both sodium and calcium channel drugs results in a similar drug-receptor complex.
Receptor sites for calcium antagonist drugs. (a) Calcium antagonist drugs at work. Top view. CaVAb with the DHP amlodipine bound. Pore module, gray; voltage sensors, blue. Inset. The dihydropyridine amlodipine bound in its receptor site. Electron density, blue mesh; amlodipine, yellow sticks. Side view. Cross section through CaVAb with the phenylalkylamine (PAA) verapamil (yellow sticks) bound. Inset. Ca2+, green; verapamil. (Adapted from Tang et al. 2016). (b) High resolution views of the indicated calcium agonist and calcium antagonist drugs bound to CaV1.1. (Adapted from Zhao et al., 2019a). Nearby amino acid residues and transmembrane segments are noted
In contrast to the phenylalkylamine and benzothiazepine receptor sites, dihydropyridines such as amlodipine and nimodipine bind to a site on the external lipid-facing surface of the pore module, between two voltage sensors (Fig. 2a, top; Tang et al., 2016). Surprisingly, only a single dihydropyridine molecule bound to the CaVAb homotetramer and induced a quaternary conformational change that prevented binding to the other three analogous positions in the tetrameric structure (Tang et al., 2016). This quaternary conformational change disrupts the fourfold symmetry of CaVAb and causes one Ca2+ ion to bind directly to a carboxyl side chain in one of the coordination sites in the outer selectivity filter, effectively blocking the pore by tightly binding this Ca2+ ion. These results show that binding of dihydropyridines to a site on the lipid-facing surface of the pore module can effectively block Ca2+ conductance by allosterically inducing high-affinity binding of Ca2+ in the pore. This indirect allosteric mode of block was previously inferred from ligand-binding studies showing that binding of Ca2+ in the ion-selectivity filter is required for high-affinity binding of dihydropyridines to their separate receptor sites (Mitterdorfer et al., 1995; Peterson & Catterall, 1995), which implied that drug binding would also strengthen and stabilize the binding of Ca2+ in the pore through reciprocal energetic interactions.
Structures of the Drug Receptor Sites on CaV1.1 Channels
As described in chapter “Subunit Architecture and Atomic Structure of Voltage Gated Ca2+ Channels”, the skeletal muscle calcium channel CaV1.1 has been an essential molecular model for biochemical, molecular biological, and structural studies of CaV channels in general. Its high abundance allowed purification of large amounts in homogeneous form as required for structural studies (Wu et al., 2016). Moreover, its similar pharmacology to CaV1.2 channels has provided a model mammalian CaV channel for structural studies of the channel protein and its receptor sites for calcium-antagonist drugs (Fig. 2b; Wu et al., 2016; Zhao et al., 2019a). As for CaVAb (Tang et al., 2016, 2019), the receptor sites for verapamil and diltiazem are located in the pore in overlapping positions at the exit from the ion selectivity filter into the central cavity (Fig. 2b; Zhao et al., 2019a). Both drugs would physically block the influx of cations in these overlapping binding positions. Dihydroyridine agonists and antagonists bind in almost identical poses in a site formed at the intersection of the S5 and S6 segments in Domains III and IV (Fig. 2b; Zhao et al., 2019a), consistent with the Domain Interface Model for dihydropyridine binding developed from early photoaffinity labeling and site-directed mutagenesis studies (Hockerman et al., 1997b, c; Ito et al., 1997; Sinnegger et al., 1997). However, the binding position for dihydropyridines differs by approximately one helical turn between CaVAb and CaV1.1, suggesting significant evolution in the structure of this drug-receptor site in the calcium channel between bacteria and humans (Zhao et al., 2019a). The detailed structural information now available for calcium-antagonist drugs binding to mammalian CaV1 channels may provide a molecular template for the design of new generations of these highly effective drugs.
Neurotoxin Receptor Sites on CaV2 Channels
Voltage-gated calcium channels in the CaV2 family mediate N-type and P/Q-type calcium currents that trigger the release of neurotransmitters at presynaptic nerve terminals (Olivera et al., 1994; Chapter “Pharmacology and Structure-Function of Venom Peptide Inhibitors of N-Type (Cav2.2) Calcium Channels” by Md. Mahadhi Hasan et al.). Their function is regulated by a wide range of neurotransmitters and hormones working through intracellular second-messenger signaling pathways (Hille, 1994; Chapter “Pharmacology and Structure-Function of Venom Peptide Inhibitors of N-Type (Cav2.2) Calcium Channels” by Md. Mahadhi Hasan et al.). Because of their crucial roles in neuromuscular transmission, they are the molecular targets for many classes of polypeptide neurotoxins from cone snails, spiders, and other venomous species (McCleskey et al., 1987; Olivera et al., 1994).
Conotoxins
The first toxin discovered to work specifically on CaV2 channels was ω-conotoxin GVI-A from the Philippine cone snail Conus geographus (Reynolds et al., 1986). Subsequent work has characterized additional conotoxins that are specific for CaV2.2 channels (Olivera et al., 1987; Hirning et al., 1988; Chapter “Pharmacology and Structure-Function of Venom Peptide Inhibitors of N-Type (Cav2.2) Calcium Channels” by Md. Mahadhi Hasan et al.), as well as a large family of conotoxins with many other molecular targets (Puillandre et al., 2012). Conotoxins are encoded in large preproteins, which undergo disulfide crosslinking, proteolytic processing, and other posttranslational modifications to reach their mature structures (Bulaj & Olivera, 2008). The mature toxins are highly specific for their wide range of molecular targets and bind to their diverse receptor sites with high affinity (Puillandre et al., 2012; Chapter “Pharmacology and Structure-Function of Venom Peptide Inhibitors of N-Type (Cav2.2) Calcium Channels” by Md. Mahadhi Hasan et al.).
Agatoxins
CaV2.1 calcium channels mediate P/Q-type calcium currents (Llinás et al., 1989). ω-Agatoxin-IIIA from the funnel web spider Agelenopsis aperta was the first widely studied toxin that specifically blocks P/Q-type calcium currents (Uchitel et al., 1992). It was shown to block neurotransmission at mammalian neuromuscular junctions and at many synapses in the spinal cord and brain (Mintz et al., 1992a, b; Uchitel et al., 1992). These channels are also the molecular targets of some cone snail toxins, such as ω-conotoxin MVII-C (Hillyard et al., 1992; Chapter _26).
Structure of the CaV2.2 Complex with Ziconotide
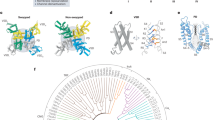
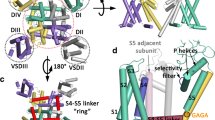
CaV2.2 channels are localized at the nerve terminals of the primary afferent nociceptive neurons, which bring pain information into the spinal cord and activate ascending neurotransmission at synapses in the dorsal horn (Westenbroek et al., 1992, 1998). For this reason, ω-conotoxin GVI-A and related conotoxins prevent pain sensation in many nociceptive circuits and substantially reduce pain in animal models, including rodents and primates (Miljanich & Ramachandran, 1995; Bowersox et al., 1996). Drug discovery efforts led to the formulation of ziconotide, a synthetic derivative of ω-conotoxin GVI-A that is a potent analgesic when administered by intrathecal infusion into the spinal cord (Miljanich, 2004; Snutch, 2005). It is used for the treatment of extreme pain in advanced-stage cancer and other medical conditions. Structure-function studies using site-directed mutagenesis revealed that ω-conotoxin GVI-A binds to the outer mouth of the ion selectivity filter of the CaV2.2 channel and physically blocks it (Ellinor et al., 1994). Based on this information, Gao et al. expressed and purified the human CaV2.2 channel with an α2δ-1 subunit, a β3 subunit, and ziconotide bound and determined its structure at high resolution by cryo-EM (Gao et al., 2021). The resulting ziconotide/channel complex gave a detailed atomic view of the bound drug and the molecular interactions it makes with its receptor site (Fig. 3). The overall structures of apo-Cav2.2 and apo-Cav1.1 can be superimposed with a root mean square deviation (RMSD) of 1.10 Å over 1,728 Cα atoms, and the binding interaction with the α2δ-1 subunit remains essentially identical. On the cytosolic side, the intracellular AID helix following the S6 transmembrane segment in Domain I folds parallel to the membrane plane and interacts with the β3 subunit. Ziconotide, which blocks Cav2.2 with a half-maximal inhibitory concentration of ~1 nM, binds tightly in the electronegative cavity that surrounds the entrance to the selectivity filter (Fig. 3a). Specific recognition is mediated by charged and polar residues on the P1 and P2 helices, and the extracellular linkers in Domains II, III, and IV (Fig. 3b, c; Gao et al., 2021). Ziconotide directly seals the outer entrance to the vestibule of the selectivity filter by neutralizing its electronegativity and physically blocking the ion permeation pathway. A bound Ca2+ ion is shown as a green sphere, and the EEEE motif in the high field-strength site that determines Ca2+ selectivity is shown as thin sticks in Fig. 3c. Sequence comparison showed that four of the eight ziconotide-interacting residues in Cav2.2 (Thr643, Asp1345, Lys1372, and Asp1629) are not conserved in other Cav channels (Fig. 3c, d), providing a structural map of the determinants of drug-binding specificity. The mutations Y13A and R10A substantially reduce pore blocking by ziconotide, and Y13R abolishes its activity completely, consistent with the direct interactions of these amino acid residues with drugs bound in the drug receptor site in CaV2.2. Evidently, the high-affinity interacting surface of ziconotide is large and engages several different amino acid side chains. Nevertheless, development of small molecule inhibitors that engage a portion of this binding surface with high-affinity interactions may yield CaV2.2-specific drugs compatible with oral dosing and broader clinical application than ziconotide.
Specific outer pore blockade of Cav2.2 by ziconotide. (a) Overall structure of the Cav2.2–ziconotide complex at an average resolution of 3.0 Å. CTD, C-terminal domain; Zi, ziconotide. The resolved lipid, cholesterol, and cholesterol hemisuccinate molecules are shown as black sticks. (b) Ziconotide is caged by the extracellular linkers with interacting residues Glu314, Glu663, Glu1365 and Glu1655. The sequence of ziconotide is shown with the three disulfide bonds indicated. The surface electrostatic potential, shown in semi-transparent presentation, was calculated in PyMol. (c) Specific coordination of ziconotide by the α1 subunit of Cav2.2. The residues that are not conserved in Cav channels are labelled blue. (d) Comparison of the conformation of the ziconotide receptor site in the absence and presence of bound drug. (Adapted from Gao et al. 2021)
Drugs Acting on the Auxiliary α2 Subunits of CaV2 Channels
Calcium channels have multiple auxiliary subunits that are required to fine-tune their functional properties and to support maturation and cell-surface expression of the channel complex (Chapter “Subunit Architecture and Atomic Structure of Voltage Gated Ca2+ Channels” by William A. Catterall; Figs. 1a, b and 2a, b; Isom et al., 1994; Gurnett & Campbell, 1996; Davies et al., 2007). However, only a single class of drugs, the gabapentinoid calcium-channel antagonists, gabapentin, and pregabalin, act on the auxiliary subunits (Davies et al., 2007; Hendrich et al., 2008). These drugs are used in the treatment of epilepsy and chronic pain. They bind adjacent to the Von Willebrand Factor Type-A homology domain on the extracellular surface of the α2 subunit and modulate the cell surface expression of CaV2.2 channels, which conduct N-type Ca2+ currents that are required for the release of neurotransmitters in the brain and in nociceptive pathways in the spinal cord (Hendrich et al., 2008). Drug binding disrupts normal recycling of these CaV2.2 channels to the cell surface and thereby reduces nociceptive signaling from the periphery to the central nervous system (Bauer et al., 2009). Although the structure of the Von Willebrand Factor Type-A homology domain has been modeled based on its sequence homology, there are no direct structural studies of the binding and action of gabapentinoid drugs to date.
Drug Receptor Sites on CaV3 Channels
CaV3 channels are important targets for the treatment of epilepsy, chronic pain, and potentially cardiac arrhythmia (Weiss & Zamponi, 2020). Absence epilepsy in GAERS rats arises from inappropriate repetitive firing in the thalamus and cerebral cortex driven by the trisynaptic circuit of inhibitory thalamic reticular neurons, excitatory thalamic relay neurons, and excitatory cortical pyramidal cells, whose normal circadian activity drives sleep spindles and REM sleep (Hosford, 1995; Proft et al., 2017). Specific mutations in CaV3.2 channels cause idiopathic generalized epilepsy (Khosravani et al., 2005). Type-type calcium currents conducted by CaV3 channels are also implicated in chronic pain (Bourinet et al., 2016) and cardiac arrhythmia (Torrente et al., 2020).
Extensive drug discovery and development efforts have been devoted to CaV3.1 and CaV3.2 in academic laboratories and at Zalicus Inc. and its corporate precursor Neuromed Inc. (Powell et al., 2014). Z944 is the most advanced drug to emerge from these studies, and it is effective in animal models of chronic pain (Lee, 2014; LeBlanc et al., 2016) and absence epilepsy (Tringham et al., 2012). Recent structural studies have revealed the molecular basis for the inhibition of CaV3.1 channels by this drug (Zhao et al., 2019b). As shown in Fig. 4a, b, Z944 binds in the central cavity of CaV3.1 channels, covering the outlet from the ion selectivity filter in a similar way as verapamil and diltiazem binding to CaVAb and CaV1 channels. In this position, Z944 would block ion permeation physically and completely inhibit channel function. A detailed analysis of the specific interactions reveals some overlap with the positions of amino acid residues in the CaVAb and CaV1.1 channels that bind the pore blockers verapamil and diltiazem (Fig. 4c–f). Mutation of some of these key residues reduces the affinity for block of ion current, confirming the essential role of these amino acid side chains in drug binding (Fig. 4e). These overlapping regions of drug binding in CaVAb, CaV1, and CaV3 channels are also similar to the binding sites for local anesthetic and antiarrhythmic drugs that have been characterized in NaVAb and the mammalian cardiac sodium channel NaV1.5 (Gamal El-Din et al., 2018; Jiang et al., 2020, 2021; Li et al., 2021), revealing a common mechanism for the molecular pharmacology of these diverse sodium- and calcium-channel blockers.
Specific inner pore blockade of CaV3 channels. (a) Chemical structure of Z944. (b) Structural basis for pore blockade by Z944. Left. Cartoon views of Z944 bound in the pore with transmembrane segments S5 and S6 in the indicated domains shown in ribbons. Right. A cut-open surface presentation viewed from the extracellular side. Z944, colored silver, is shown as spheres. (c) EM map for Z944 and surrounding residues contoured at 7σ. A nearby lipid is shown as black sticks. (d) Specific coordination of Z944 by polar residues. The potential electrostatic interactions are indicated by red dashed lines. (e) Functional validation of the coordination of Z944 by the T-type specific Lys. The locus corresponding to Lys1462 is replaced by Phe in Cav1 and Gly in Cav2 channels. Voltage-dependent activation (left) and inactivation (center). The right panel shows that single point mutations K1462F (green) or K1462G (blue) resulted in a change of the IC50 from 311 ± 25.6 nM to 4.2 ± 0.3 μM or 3.1 ± 0.2 μM, respectively. G/Gmax and I/Imax represent normalized conductance and ionic current, respectively. (f) Z944 is surrounded by hydrophobic residues on the S6 tetrahelical bundle. Residues that are not conserved in Cav1 and Cav2 channels are labelled in orange. (Adapted from Gao et al. 2021)
Conclusion
From the initial discoveries of the calcium antagonist drugs in the 1970s through drug screening studies with vascular smooth muscle (Fleckenstein, 1983; Godfraind, 2017), the pharmacology of calcium channels has grown as a field to include clinical uses in cardiovascular diseases such as hypertension, angina pectoris, and cardiac arrhythmia, and in neurological diseases such as epilepsy and chronic pain. These drugs were instrumental in the initial identification, purification, and reconstitution of skeletal muscle calcium channels (see chapter 2 “Subunit Architecture and Atomic Structure of Voltage Gated Ca2+ Channels”), which eventually resulted in the determination of high-resolution structures of all three families of calcium channels with drugs bound in their receptor sites as reviewed here. I look forward to exciting new developments in calcium-channel drug discovery and pharmacology based on these basic research findings.
References
Bauer, C. S., Nieto-Rostro, M., Rahman, W., Tran-Van-Minh, A., Ferron, L., Douglas, L., Kadurin, I., Sri Ranjan, Y., Fernandez-Alacid, L., Millar, N. S., Dickenson, A. H., Lujan, R., & Dolphin, A. C. (2009). The increased trafficking of the calcium channel subunit alpha2delta-1 to presynaptic terminals in neuropathic pain is inhibited by the alpha2delta ligand pregabalin. The Journal of Neuroscience, 29(13), 4076–4088. https://doi.org/10.1523/JNEUROSCI.0356-09.2009
Bean, B. P. (1984). Nitrendipine block of cardiac calcium channels: High-affinity binding to the inactivated state. Proceedings of the National Academy of Sciences of the United States of America, 81, 6388–6392.
Bean, B. P., Cohen, C. J., & Tsien, R. W. (1983). Lidocaine block of cardiac sodium channels. The Journal of General Physiology, 81, 613–642.
Bourinet, E., Altier, C., Hildebrand, M. E., Trang, T., Salter, M. W., & Zamponi, G. W. (2014). Calcium-permeable ion channels in pain signaling. Physiological Reviews, 94(1), 81–140. https://doi.org/10.1152/physrev.00023.2013
Bourinet, E., Francois, A., & Laffray, S. (2016). T-type calcium channels in neuropathic pain. Pain, 157(Suppl 1), S15–S22. https://doi.org/10.1097/j.pain.0000000000000469
Bowersox, S. S., Gadbois, T., Singh, T., Pettus, M., Wang, Y. X., & Luther, R. R. (1996). Selective N-type neuronal voltage-sensitive calcium channel blocker, SNX-111, produces spinal antinociception in rat models of acute, persistent and neuropathic pain. The Journal of Pharmacology and Experimental Therapeutics, 279, 1243–1249.
Brauns, T., Cai, Z. W., Kimball, S. D., Kang, H. C., Haugland, R. P., Berger, W., Berjukov, S., Hering, S., Glossmann, H., & Striessnig, J. (1995). Benzothiazepinone binding domain of purified L-type calcium channels: Direct labeling using a novel fluorescent diltiazem analogue. Biochemistry, 34, 3461–3469.
Bulaj, G., & Olivera, B. M. (2008). Folding of conotoxins: Formation of the native disulfide bridges during chemical synthesis and biosynthesis of Conus peptides. Antioxidants & Redox Signaling, 10(1), 141–155. https://doi.org/10.1089/ars.2007.1856
Catterall, W. A., & Striessnig, J. (1992). Receptor sites for Ca2+ channel antagonists. Trends in Pharmacological Sciences, 13, 256–262.
Davies, A., Hendrich, J., Van Minh, A. T., Wratten, J., Douglas, L., & Dolphin, A. C. (2007). Functional biology of the alpha-2-delta subunits of voltage-gated calcium channels. Trends in Pharmacological Sciences, 28(5), 220–228. https://doi.org/10.1016/j.tips.2007.03.005
Ellinor, P. T., Zhang, J. F., Horne, W. A., & Tsien, R. W. (1994). Structural determinants of the blockade of N-type calcium channels by a peptide neurotoxin. Nature, 372(6503), 272–275. https://doi.org/10.1038/372272a0
Fleckenstein, A. (1983). History of calcium antagonists. Circulation Research, 52(2 Pt 2), I3–I16.
Gamal El-Din, T. M., Lenaeus, M. J., Zheng, N., & Catterall, W. A. (2018). Fenestrations control resting-state block of a voltage-gated sodium channel. Proceedings of the National Academy of Sciences of the United States of America. https://doi.org/10.1073/pnas.1814928115
Gao, S., Yao, X., & Yan, N. (2021). Structure of human Cav2.2 channel blocked by the painkiller ziconotide. Nature, 596(7870), 143–147. https://doi.org/10.1038/s41586-021-03699-6
Godfraind, T. (2017). Discovery and development of calcium channel blockers. Frontiers in Pharmacology, 8, 286. https://doi.org/10.3389/fphar.2017.00286
Gurnett, C. A., & Campbell, K. P. (1996). Transmembrane auxiliary subunits of voltage-dependent ion channels. The Journal of Biological Chemistry, 271, 27975–27978.
Hendrich, J., Van Minh, A. T., Heblich, F., Nieto-Rostro, M., Watschinger, K., Striessnig, J., Wratten, J., Davies, A., & Dolphin, A. C. (2008). Pharmacological disruption of calcium channel trafficking by the alpha2delta ligand gabapentin. Proceedings of the National Academy of Sciences of the United States of America, 105(9), 3628–3633. https://doi.org/10.1073/pnas.0708930105
Hille, B. (1977). Local anesthetics: Hydrophilic and hydrophobic pathways for the drug-receptor reaction. The Journal of General Physiology, 69, 497–515.
Hille, B. (1994). Modulation of ion-channel function by G-protein-coupled receptors. Trends in Neurosciences, 17, 531–536.
Hille, B. (2001). Ionic channels of excitable membranes (3rd ed.). Sinauer Associates Inc.
Hillyard, D. R., Monje, V. D., Mintz, I. M., Bean, B. P., Nadasdi, L., Ramachandran, J., Miljanich, G., Azimi-Zoonooz, A., McIntosh, J. M., Cruz, L. J., & et, a.l. (1992). A new Conus peptide ligand for mammalian presynaptic Ca2+ channels. Neuron, 9(1), 69–77.
Hirning, L. D., Fox, A. P., McCleskey, E. W., Olivera, B. M., Thayer, S. A., Miller, R. J., & Tsien, R. W. (1988). Dominant role of N-type Ca2+ channels in evoked release of norepinephrine from sympathetic neurons. Science, 239, 57–61.
Hockerman, G. H., Johnson, B. D., Scheuer, T., & Catterall, W. A. (1995). Molecular determinants of high affinity phenylaklyamine block of L-type calcium channels. The Journal of Biological Chemistry, 270, 22119–22122.
Hockerman, G. H., Johnson, B. D., Abbott, M. R., Scheuer, T., & Catterall, W. A. (1997a). Molecular determinants of high affinity phenylalkylamine block of L-type calcium channels in transmembrane segment IIIS6 and the pore region of the α1 subunit. The Journal of Biological Chemistry, 272, 18759–18765.
Hockerman, G. H., Peterson, B. Z., Johnson, B. D., & Catterall, W. A. (1997b). Molecular determinants of drug binding and action on L-type calcium channels. Annual Review of Pharmacology and Toxicology, 37, 361–396.
Hockerman, G. H., Peterson, B. Z., Sharp, E., Tanada, T. N., Scheuer, T., & Catterall, W. A. (1997c). Construction of a high-affinity receptor site for dihydropyridine agonists and antagonists by single amino acid substitutions in a non-L-type Ca2+ channel. Proceedings of the National Academy of Sciences of the United States of America, 94, 14906–14911.
Hofmann, F., Lacinová, L., & Klugbauer, N. (1999). Voltage-dependent calcium channels: From structure to function. Reviews of Physiology, Biochemistry and Pharmacology, 139, 33–87.
Hondeghem, L. M., & Katzung, B. G. (1977). Timed- and voltage-dependent interactions of antiarrhythmic drugs with cardiac sodium channels. Biochimica et Biophysica Acta, 472, 373–398.
Hondeghem, L. M., & Katzung, B. G. (1984). Antiarrhythmic agents: The modulated receptor mechanism of action of sodium and calcium channel blocking drugs. Annual Review of Pharmacology and Toxicology, 24, 387–423.
Hosford, D. A. (1995). Models of primary generalized epilepsy. Current Opinion in Neurology, 8(2), 121–125. https://doi.org/10.1097/00019052-199504000-00006
Isom, L. L., De Jongh, K. S., & Catterall, W. A. (1994). Auxiliary subunits of voltage-gated ion channels. Neuron, 12(6), 1183–1194.
Ito, H., Klugbauer, N., & Hofmann, F. (1997). Transfer of the high affinity dihydropyridine sensitivity from L-type to non-L-type calcium channel. Molecular Pharmacology, 52, 735–740.
Jiang, D., Shi, H., Tonggu, L., Gamal El-Din, T. M., Lenaeus, M. J., Zhao, Y., Yoshioka, C., Zheng, N., & Catterall, W. A. (2020). Structure of the cardiac sodium channel. Cell, 180(1), 122–134.e10. https://doi.org/10.1016/j.cell.2019.11.041
Jiang, D., Banh, R., Gamal El-Din, T. M., Tonggu, L., Lenaeus, M. J., Pomès, R., Zheng, N., & Catterall, W. A. (2021). Open-state structure and pore gating mechanism of the cardiac sodium channel. Cell, 184(20), 5151–5162.e11. https://doi.org/10.1016/j.cell.2021.08.021
Kanaya, S., Arlock, P., Katzung, B. G., & Hondeghem, L. M. (1983). Diltiazem and verapamil preferentially block inactivated cardiac calcium channels. Journal of Molecular and Cellular Cardiology, 15, 145–148.
Khosravani, H., Bladen, C., Parker, D. B., Snutch, T. P., McRory, J. E., & Zamponi, G. W. (2005). Effects of Cav3.2 channel mutations linked to idiopathic generalized epilepsy. Annals of Neurology, 57(5), 745–749. https://doi.org/10.1002/ana.20458
Kraus, R., Reichl, B., Kimball, S. D., Grabner, M., Murphy, B. J., Catterall, W. A., & Striessnig, J. (1996). Identification of benz(othi)azepine-binding regions within L-type calcium channel a1 subunits. The Journal of Biological Chemistry, 271, 20113–20118.
LeBlanc, B. W., Lii, T. R., Huang, J. J., Chao, Y. C., Bowary, P. M., Cross, B. S., Lee, M. S., Vera-Portocarrero, L. P., & Saab, C. Y. (2016). T-type calcium channel blocker Z944 restores cortical synchrony and thalamocortical connectivity in a rat model of neuropathic pain. Pain, 157(1), 255–263. https://doi.org/10.1097/j.pain.0000000000000362
Lee, M. (2014). Z944: A first in class T-type calcium channel modulator for the treatment of pain. Journal of the Peripheral Nervous System, 19(Suppl 2), S11–S12. https://doi.org/10.1111/jns.12080_2
Lenaeus, M. J., Gamal El-Din, T. M., Ing, C., Ramanadane, K., Pomes, R., Zheng, N., & Catterall, W. A. (2017). Structures of closed and open states of a voltage-gated sodium channel. Proceedings of the National Academy of Sciences of the United States of America, 114(15), E3051–E3060. https://doi.org/10.1073/pnas.1700761114
Li, Z., Jin, X., Wu, T., Huang, G., Wu, K., Lei, J., Pan, X., & Yan, N. (2021). Structural basis for pore blockade of the human cardiac sodium channel Na. Angewandte Chemie (International Ed. in English), 60(20), 11474–11480. https://doi.org/10.1002/anie.202102196
Llinás, R., Sugimori, M., Lin, J. W., & Cherksey, B. (1989). Blocking and isolation of a calcium channel from neurons in mammals and cephalopods utilizing a toxin fraction (FTX) from funnel-web spider poison. Proceedings of the National Academy of Sciences of the United States of America, 86, 1689–1693.
McCleskey, E. W., Fox, A. P., Feldman, D. H., Cruz, L. J., Olivera, B. M., Tsien, R. W., & Yoshikami, D. (1987). ω-Conotoxin: Direct and persistent blockade of specific types of calcium channels in neurons but not muscle. Proceedings of the National Academy of Sciences of the United States of America, 84, 4327–4331.
Miljanich, G. P. (2004). Ziconotide: Neuronal calcium channel blocker for treating severe chronic pain. Current Medicinal Chemistry, 11(23), 3029–3040. https://doi.org/10.2174/0929867043363884
Miljanich, G. P., & Ramachandran, J. (1995). Antagonists of neuronal calcium channels: Structure, function, and therapeutic implications. Annual Review of Pharmacology and Toxicology, 35, 707–734.
Mintz, I. M., Adams, M. E., & Bean, B. P. (1992a). P-type calcium channels in rat central and peripheral neurons. Neuron, 9, 85–95.
Mintz, I. M., Venema, V. J., Swiderek, K. M., Lee, T. D., Bean, B. P., & Adams, M. E. (1992b). P-type calcium channels blocked by the spider toxin omega-Aga-IVA. Nature, 355(6363), 827–829.
Mitterdorfer, J., Sinnegger, M. J., Grabner, M., Striessnig, J., & Glossmann, H. (1995). Coordination of Ca2+ by the pore region glutamates is essential for high-affinity dihydropyridine binding to the cardiac Ca2+ channel alpha-1 subunit. Biochemistry, 34, 9350–9355.
Mitterdorfer, J., Wang, Z. Y., Sinnegger, M. J., Hering, S., Striessnig, J., Grabner, M., & Glossmann, H. (1996). Two amino acid residues in the IIIS5 segment of L-type calcium channels differentially contribute to 1,4-dihydropyridine sensitivity. The Journal of Biological Chemistry, 271, 30330–30335.
Nakayama, H., Taki, M., Striessnig, J., Catterall, W. A., & Kanaoka, Y. (1991). Identification of 1,4-dihydropyridine binding regions within the α1 subunit of skeletal muscle Ca2+ channels by photoaffinity labeling with diazipine. Proceedings of the National Academy of Sciences of the United States of America, 88, 9203–9207.
Olivera, B. M., Cruz, L. J., de Santos, V., LeCheminant, G. W., Griffin, D., Zeikus, R., McIntosh, J. M., Galyean, R., Varga, J., Gray, W. R., & Rivier, J. (1987). Neuronal calcium channel antagonists. Discrimination between calcium channel subtypes using ω-conotoxin from Conus magus venom. Biochemistry, 26, 2086–2090.
Olivera, B. M., Miljanich, G. P., Ramachandran, J., & Adams, M. E. (1994). Calcium channel diversity and neurotransmitter release: The omega-conotoxins and omega-agatoxins. Annual Review of Biochemistry, 63, 823–867.
Perez-Reyes, E. (2003). Molecular physiology of low-voltage-activated t-type calcium channels. Physiological Reviews, 83(1), 117–161.
Peterson, B. Z., & Catterall, W. A. (1995). Calcium binding in the pore of L-type calcium channels modulates high affinity dihydropyridine binding. The Journal of Biological Chemistry, 270, 18201–18204.
Peterson, B. Z., Tanada, T. N., & Catterall, W. A. (1996). Molecular determinants of high affinity dihydropyridine binding in L-type calcium channels. The Journal of Biological Chemistry, 271, 5293–5296.
Powell, K. L., Cain, S. M., Snutch, T. P., & O’Brien, T. J. (2014). Low threshold T-type calcium channels as targets for novel epilepsy treatments. British Journal of Clinical Pharmacology, 77(5), 729–739. https://doi.org/10.1111/bcp.12205
Proft, J., Rzhepetskyy, Y., Lazniewska, J., Zhang, F. X., Cain, S. M., Snutch, T. P., Zamponi, G. W., & Weiss, N. (2017). The Cacna1h mutation in the GAERS model of absence epilepsy enhances T-type Ca. Scientific Reports, 7(1), 11513. https://doi.org/10.1038/s41598-017-11591-5
Puillandre, N., Koua, D., Favreau, P., Olivera, B. M., & Stöcklin, R. (2012). Molecular phylogeny, classification and evolution of conopeptides. Journal of Molecular Evolution, 74(5-6), 297–309. https://doi.org/10.1007/s00239-012-9507-2
Ren, D., Navarro, B., Xu, H., Yue, L., Shi, Q., & Clapham, D. E. (2001). A prokaryotic voltage-gated sodium channel. Science, 294(5550), 2372–2375.
Reynolds, I. J., Wagner, J. A., Snyder, S. H., Thayer, S. A., Olivera, B. M., & Miller, R. J. (1986). Brain voltage-sensitive calcium channel subtypes differentiated by omega-conotoxin fraction GVIA. Proceedings of the National Academy of Sciences of the United States of America, 83(22), 8804–8807. https://doi.org/10.1073/pnas.83.22.8804
Sampson, K. J., & Kass, R. K. (2011). Antiarrhyhthmic drugs. In Goodman & Gilman’s (Eds.), Pharmacological basis of therapeutics (pp. 815–848).
Sinnegger, M. J., Wang, Z. Y., Grabner, M., Hering, S., Striessnig, J., Glossmann, H., & Mitterdorfer, J. (1997). Nine L-type amino acid residues confer full 1,4-dihydropyridine sensitivity to the neuronal calcium channel α1A subunit – Role of L-type MET. The Journal of Biological Chemistry, 272, 27686–27693.
Snutch, T. P. (2005). Targeting chronic and neuropathic pain: The N-type calcium channel comes of age. NeuroRx, 2(4), 662–670. https://doi.org/10.1602/neurorx.2.4.662
Striessnig, J. (1999). Pharmacology, structure and function of cardiac L-type calcium channels. Cellular Physiology and Biochemistry, 9(4-5), 242–269.
Striessnig, J., Glossmann, H., & Catterall, W. A. (1990). Identification of a phenylalkylamine binding region within the α1 subunit of skeletal muscle Ca2+ channels. Proceedings of the National Academy of Sciences of the United States of America, 87, 9108–9112.
Striessnig, J., Murphy, B. J., & Catterall, W. A. (1991). The dihydropyridine receptor of L-type Ca2+ channels: Identification of binding domains for (+)-[3H]PN200-110 and [3H]azidopine within the alpha-1 subunit. Proceedings of the National Academy of Sciences of the United States of America, 88, 10769–10773.
Tang, L., Gamal El-Din, T. M., Payandeh, J., Martinez, G. Q., Heard, T. M., Scheuer, T., Zheng, N., & Catterall, W. A. (2014). Structural basis for Ca2+ selectivity of a voltage-gated calcium channel. Nature, 505(7481), 56–61. https://doi.org/10.1038/nature12775
Tang, L., Gamal El-Din, T. M., Swanson, T. M., Pryde, D. C., Scheuer, T., Zheng, N., & Catterall, W. A. (2016). Structural basis for inhibition of a voltage-gated Ca2+ channel by Ca2+ antagonist drugs. Nature, 537, 117–121. https://doi.org/10.1038/nature19102
Tang, L., Gamal El-Din, T. M., Lenaeus, M. J., Zheng, N., & Catterall, W. A. (2019). Structural basis for diltiazem block of a voltage-gated Ca2+ channel. Molecular Pharmacology, 96(4), 485–492. https://doi.org/10.1124/mol.119.117531
Torrente, A. G., Mesirca, P., Bidaud, I., & Mangoni, M. E. (2020). Channelopathies of voltage-gated L-type Cav1.3/α. Pflügers Archiv, 472(7), 817–830. https://doi.org/10.1007/s00424-020-02421-1
Triggle, D. J. (1999). The pharmacology of ion channels: With particular reference to voltage-gated Ca2+ channels. European Journal of Pharmacology, 375, 311–325.
Triggle, D. J. (2003). Drug targets in the voltage-gated calcium channel family: Why some are and some are not. Assay and Drug Development Technologies, 1(5), 719–733.
Tringham, E., Powell, K. L., Cain, S. M., Kuplast, K., Mezeyova, J., Weerapura, M., Eduljee, C., Jiang, X., Smith, P., Morrison, J. L., Jones, N. C., Braine, E., Rind, G., Fee-Maki, M., Parker, D., Pajouhesh, H., Parmar, M., O’Brien, T. J., & Snutch, T. P. (2012). T-type calcium channel blockers that attenuate thalamic burst firing and suppress absence seizures. Science Translational Medicine, 4(121), 121ra19. https://doi.org/10.1126/scitranslmed.3003120
Uchitel, O. D., Protti, D. A., Sanchez, V., Cherksey, B. D., Sugimori, M., & Llinás, R. (1992). P-type voltage-dependent calcium channel mediates presynaptic calcium influx and transmitter release in mammalian synapses. Proceedings of the National Academy of Sciences of the United States of America, 89, 3330–3333.
Weiss, N., & Zamponi, G. W. (2020). Genetic T-type calcium channelopathies. Journal of Medical Genetics, 57(1), 1–10. https://doi.org/10.1136/jmedgenet-2019-106163
Welling, A., Ludwig, A., Zimmer, S., Klugbauer, N., Flockerzi, V., & Hofmann, F. (1997). Alternatively spliced IS6 segments of the alpha 1C gene determine the tissue-specific dihydropyridine sensitivity of cardiac and vascular smooth muscle L-type Ca2+ channels. Circulation Research, 81(4), 526–532. https://doi.org/10.1161/01.res.81.4.526
Westenbroek, R. E., Hell, J. W., Warner, C., Dubel, S. J., Snutch, T. P., & Catterall, W. A. (1992). Biochemical properties and subcellular distribution of an N-type calcium channel alpha-1 subunit. Neuron, 9(6), 1099–1115.
Westenbroek, R. E., Hoskins, L., & Catterall, W. A. (1998). Localization of Ca2+ channel subtypes on rat spinal motor neurons, interneurons, and nerve terminals. The Journal of Neuroscience, 18, 6319–6330.
Wu, J., Yan, Z., Li, Z., Qian, X., Lu, S., Dong, M., Zhou, Q., & Yan, N. (2016). Structure of the voltage-gated calcium channel CaV1.1 at 3.6 A resolution. Nature, 537(7619), 191–196. https://doi.org/10.1038/nature19321
Zamponi, G. W., Striessnig, J., Koschak, A., & Dolphin, A. C. (2015). The physiology, pathology, and pharmacology of voltage-gated calcium channels and their future therapeutic potential. Pharmacological Reviews, 67(4), 821–870. https://doi.org/10.1124/pr.114.009654
Zhao, Y., Huang, G., Wu, J., Wu, Q., Gao, S., Yan, Z., Lei, J., & Yan, N. (2019a). Molecular basis for ligand modulation of a mammalian voltage-gated calcium channel. Cell, 177(6), 1495–1506.e12. https://doi.org/10.1016/j.cell.2019.04.043
Zhao, Y., Huang, G., Wu, Q., Wu, K., Li, R., Lei, J., Pan, X., & Yan, N. (2019b). Cryo-EM structures of apo and antagonist-bound human CaV3.1. Nature, 576(7787), 492–497. https://doi.org/10.1038/s41586-019-1801-3
Acknowledgements
Research in my laboratory on sodium and calcium channels is supported by research grants from the National Institutes of Health: R35 NS111573 and R01 HL112808. Special thanks to Dr. Ning Zheng (Professor of Pharmacology, University of Washington, and Investigator of the Howard Hughes Medical Institute), whose deeps insights into structural biology have been crucial in all of our studies of sodium- and calcium-channel structure.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Catterall, W.A. (2022). Pharmacology of Voltage-Gated Calcium Channels at Atomic Resolution. In: Zamponi, G.W., Weiss, N. (eds) Voltage-Gated Calcium Channels . Springer, Cham. https://doi.org/10.1007/978-3-031-08881-0_25
Download citation
DOI: https://doi.org/10.1007/978-3-031-08881-0_25
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-08880-3
Online ISBN: 978-3-031-08881-0
eBook Packages: Physics and AstronomyPhysics and Astronomy (R0)