Abstract
The development and validation of structured training curricula is one of the challenges in current urological robotic surgery to improve patient safety and surgical outcomes. Structured curricula should consist of theoretical training (e-learning, case observation), preclinical simulation-based training (virtual reality simulation, dry and wet lab), clinical modular training, and final evaluation. Tele-mentoring might be mandatory in future curriculum development. To date, several training programs are currently available for robotic urological surgery. However, the majority lack clinical modular training that consists of progressive, proficiency-based training through surgical steps with increasing levels of complexity. Moreover, many of these curricula lack validation.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
20.1 Introduction
Robot-assisted procedures have been increasingly adopted over the last two decades because of the advantages of three-dimensional vision, a shorter learning curve, increased dexterity and precision, and better ergonomics for the surgeon [1]. These advantages have led to robotic surgery becoming the prevalent approach of minimally invasive surgery worldwide, with approximately 4500 Da Vinci robotic systems (Intuitive Surgical Inc., Sunnyvale, CA, USA) in action in 2018 [2, 3], with robot-assisted radical prostatectomy (RARP) as the most commonly performed robotic procedure worldwide [4]. With respect to this, the implementation of robotic surgery in this field has led to equivalent oncological outcomes compared to open or laparoscopic surgery with the advantage of having superior peri-operative and functional outcomes [5].
However, “a fool with a tool, is still a fool.” The rapid increase of robotic systems has not yet been translated into an even greater increase in the training of robotic surgeons. Consequently, a significant proportion of surgeons start using robotics without being adequately trained according to validated training curricula, and therefore expose their patients to unnecessary risks of unfulfilled learning curves [6, 7]. This has resulted in increased adverse events [8].
The phenomenon of inadequate training is not unique to the implementation of robotic surgery, but could be applied to every field in medicine and could result in a significant number of medical errors and preventable complications. In the book “Why Hospitals Should Fly,” the author reported mortality comparisons between the aviation and healthcare industries over a 5-year period between 2001 and 2006, with zero deaths on commercial US flights compared to an estimated 250–500,000 deaths from medical errors in the US healthcare system at the same time [9, 10]. Nonetheless, the structure of training in aviation and robotic surgery has many similarities, and both parties control complex technology with their hands, that if managed inappropriately, could result in fatal consequences. This significant difference in outcomes could be explained by the different approaches to training. The increased standardization, with internationally agreed training standards, forms the basis of pilot training in the airline industry. Evaluation and regulation comprised of benchmarked high-stakes tests related to proficiency-based training, result in quality assurance [10, 11] and should also be the way forward in surgical robotic training since we live in an era of outcome-based surgery. The implementation of structured, standardized, and validated curricula in a non-clinical training environment will form the basis of this process [12]. In these times, it is not justifiable anymore, that living patients are being used as training objects.
20.2 Elements of Training Programs in Robotic Surgery
A structured training curriculum should include theoretical training (e-learning, case observation), preclinical simulation-based training (virtual reality simulation, dry and wet lab), clinical modular training, and a final evaluation [13].
20.2.1 E-learning Instruments
E-learning, and, more generally, video training, are essential tools for acquiring theoretical notions and technical skills. In surgical practice, it allows a proctor to guide his trainee using procedure-specific training videos. New e-learning processes are emerging to spread knowledge about a single procedure [14]. New online learning platforms have the ability to incorporate procedure-specific operative metrics to offer novice surgeons a stepwise approach in technical skill acquirement as part of proficiency-based training curriculum [15]. Furthermore, procedure-specific assessment tools could be used to perform a video-based assessment of a surgical performance [16]. Moreover, these e-learning processes are easily accessible and can be quickly updated [17]. Maertens et al. [18] have shown how e-learning can have higher or equal effectiveness compared with both no intervention and non-learning interventions. Angelo et al. also indicated that implementation of an e-curriculum as concept of a proficiency-based progression (PBP) training methodology led to a significantly lower amount of procedural errors [15]. However, the introduction of these new learning processes is far from simple and requires the introduction of new methods of digital learning assessment and a redefinition of educational roles [19]. To date, there are no e-learning platforms in the robotic surgical field that have undergone an adequate and complete validation process.
20.2.2 Preclinical Simulation-Based Training
Virtual reality simulators are already an integral part of most of the curricula in literature [20,21,22] and have been shown to improve surgical skills in an out-of-hospital setting [12, 23]. The main ones available on the market are: da Vinci Skills Simulator (dVSS) (Intuitive Surgical, Sunnyvale, Santa Clara County, CA, USA), the Robotic Surgical Simulator (RoSS) (Simulated Surgical Systems, Buffalo, NY, USA), SEP robot (SimSurgery, Norway), d-V-Trainer (Mimic Technologies Inc., Seattle, WA, USA), ProMIS (Haptica, Ireland), and RobotiX Mentor (3D Systems, Israel). The most widely used today is the dVSS [24]. However, the d-V-Trainer is considered the most validated [25].
Benchtop simulators are the main tools found inside the dry lab. They are inexpensive, easy to carry, and useful for improving surgical skills. But they are rarely attractive to learners, and are unable to simulate a real surgical setting [23]. They could be used in the simulation phase of robotic docking. Some studies in the literature have established a partial validation of dry lab simulators [26, 27].
Two main simulation models are available in the wet-lab: animals and human cadavers. The animal tissue is of low cost but needs particular facilities for its conservation. Entire deceased animals and living animals are among the best existing simulation models [28]. They allow one to distinguish the consistency of tissues, to replicate the real anatomy and to practice the on-patient operation in a reliable manner. However, this type of training involves very high costs, legal requirements, and availability for single use only [29, 30]. The human cadaveric model is the gold standard for anatomical training; however, it has the same problems as mentioned for the animal model.
During the preclinical simulation-based training, a real-life case observation in a training center by an experienced robotic surgeon is essential as this also includes the circumstances of an operation theater, the associated stress factors, and interhuman relationships.
20.2.3 Clinical Modular Training
It consists of performing supervised surgery in a modular fashion under the expert surgeon’s supervision. Progressive, proficiency-based training through surgical steps with increasing levels of complexity is performed. At the end of the clinical training, the trainee should perform a complete procedure that needs to be recorded and evaluated by certified independent examiners in a blind-review process using recognized assessment tools [31].
20.2.4 Full Immersion Simulation and High-Fidelity Operating Room Simulation
The success of the surgical robotic procedure depends not only on the surgeon’s technical skills, but also on his/her non-technical skills and the preparation of his/her surgical team [32]. Recognition that, besides technical skills, also cognitive (thinking) and non-technical skills (NTS) will contribute to the development of robotic surgery curricula. To develop these skills in a standardized way, the main methods used are the classroom lessons, the full immersion simulation, and high-fidelity operating room simulation [33, 34].
20.2.5 Tele-Mentoring
Although not very relevant at present, tele-mentoring offers several advantages, making it most likely to play a fundamental role in future training and curricula. The possibility that experts in the field can guide novice surgeons, even when being remotely from each other opens perspectives. Moreover, technological advancement and the introduction of the 5G network could, in the future, even allow proctors to take over the master controls in case of an emergency or trouble. Financial, legal, ethical, economic, and security issues still need to be addressed and solved before being able to integrate this ingredient into the training process adequately [35].
20.3 Critical Issues in the Development of a Robotic Training Program
20.3.1 Adequate Training Time to Perform Safe Surgery
The learning curve is the process during which a novice surgeon gains experience, ability, and skills until reaching a plateau of having optimal operative results. Importantly, the initial phase of the learning curve can be burdened by nonoptimal technical, functional, and oncological results [36, 37]. The duration of this learning curve is procedure dependent and is associated with the level of complexity of the specific task. Taking, for example, the learning curve for robotic-assisted radical prostatectomy (RARP), this was estimated by some authors to be between 12 and 250 procedures based on measurable variables, while others showed a substantial reduction of positive surgical margins (PSMs) after 200 and 1600 procedures [38, 39]. Bravi et al. [34] also showed that previous open surgical experience does not correlate with the risk of PSMs during RARP. Implementation of structured and validated training curricula should aim to overcome the learning curve with its suboptimal results, in a non-clinical training center in order not to expose patients to the inexperience of novice surgeons [40].
Over the last decades, there has been a transition of the duties of surgeons in training, with more emphasis on non-clinical bureaucracy work. Moreover, due to an increased number of surgical procedures to learn during training and due to restricted working hours, fewer surgeons are fully trained and able to operate independently at the end of their training [41]. This might affect the patient’s health. Consequently, additional training fellowships to acquire the necessary skills are needed. Validated training curricula with preset proficiency benchmarks should be able to overcome the limited time issues by optimizing the quality of the training [42]. Of note, the foreseen training course should have sufficient length to reach the preset benchmarks and quality standards. For this reason, for example, the initial training period planned for the European Association of Urology Robotic Training Curriculum was 3 months and was then updated to 6 months, to allow all participants a sufficient amount of time to acquire the necessary expertise [43,44,45,46].
20.3.2 Cost of Training
The need for equipment, simulators, dual consoles, wet-lab training materials and the use of facilities at recognized training centers makes robotic surgery training extremely expensive compared to open and laparoscopic surgery. It seems correlated with the length of the learning curve, quantifiable between 95,000 and 1,365,000 dollars [13, 47]. Implementation of validated training curricula and the transition of training outside of the hospital will increase the cost of training further. However, this aims to deliver surgeons who have completed their learning curve and therefore should lead to decreased peri-operative complications. Consequently, this could be translated into lower hospital costs [48].
20.4 Available Robotic Surgical Training Curricula
Table 20.1 shows that several training programs are available [53]. However, the majority are characterized by short training sessions that rely exclusively on preclinical simulation-based training (virtual-reality/dry-lab/wet-lab). Conversely, only a few are all-inclusive fellowship-style programs that include clinical modular training. Of these curricula, a few have been validated [11, 44, 45, 54].
20.4.1 Validated Robotic Surgical Training Curricula (Table 20.1)
-
1.
Fundamental skills of robotic surgery (FSRS): this curriculum was created by the Roswell Cancer Institute in Buffalo, CA, USA, and consists of 4 modules, further subdivided into 16 tasks executed with the aid of the RoSS simulator. Studies have shown the validity of the FSRS curriculum in improving the robotic surgical skills of trainees. It has also been validated for construct validity [11]. The robot-assisted surgical training (RAST), developed by the same center, combines the FSRS with other forms of hands-on training, such as HoST training and wet-lab. Evidence suggests that it has an educational impact on trainees [54].
-
2.
Proficiency-based robotic curriculum: that was developed by the University of Texas Southwestern Medical Center. It consists of an online free tutorial offered by Intuitive Surgical, followed by an interactive hands-on training session on the standard da Vinci system, and finally, the execution of nine inanimate exercises of increasing difficulty. The content, face, and construct validity of this curriculum has been established [49, 55].
-
3.
Basic skills training curriculum (BSTC): It was developed by the University of Toronto and consists of a 4-week training, featuring didactic lectures, theoretical module, 2 hours of hands-on training and exercises at dVSS organized with weekly intervals. This curriculum has been validated and has shown to improve robotic surgical skills [11, 56].
-
4.
The European Association of Urology Robotic Urology Section (ERUS) training curriculum (Fig. 20.1): this represents the first structured and validated curriculum in urology. It is built for training on a specific procedure, the RARP. The first version, published in 2015, was followed by a more recent one with a lengthening of the training period from 3 to 6 months. This change is intended to allow even the less experienced trainees to have enough time to continue and finish the full training path [44, 45]. The curriculum initially includes a theoretical study of the robotic platform and the index procedure through e-learning, followed by live case observation and bedside assistance in the host center. At this point, there is a week of intensive hands-on training with virtual simulators, dry-lab, and wet-lab, associated with in-depth theoretical knowledge of technical and nontechnical skills. A recent study by Larcher et al. [57] shows how the use of virtual simulators in the ERUS curriculum preclinical phase improves surgical performance, according to objective measurement indexes. Moreover, in this study, the average total score and the average improvement score that the trainee should reach to move to the next phase are quantified [57]. Subsequently, the curriculum includes a period of modular clinical training, under the supervision of an expert robotic surgeon, and finally, the surgeon will have to record an unedited video of a complete procedure that will be blindly evaluated using adequate scores [31]. Some studies showed that the fulfillment of the ERUS curriculum leads to an early improvement of results [58, 59].
-
5.
The ERUS curriculum for robot-assisted partial nephrectomy (Fig. 20.2): Based on the ERUS curriculum for radical prostatectomy, the same scientific society has developed a training program to prepare surgeons to perform robotic-assisted partial nephrectomy (RAPN). This curriculum consists of the first part of theoretical preparation. Second, a week of intensive training with virtual simulators, dry-lab and wet-lab, followed by the third phase of modular clinical training, in which the procedure is divided into 10 steps which the trainee must reproduce. At the end, there is the final evaluation based on the assessment of an unedited video by an expert surgeon in the blind modality. In the pilot validation phase, this curriculum showed no deterioration in the clinical results of the interventions [51].
-
6.
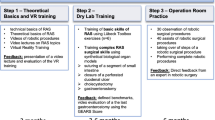
The ERUS curriculum for robot-assisted radical cystectomy (Fig. 20.3): Similarly to the ccERUS for RARP, ERUS also developed a structured training program for robot-assisted radical cystectomy (RARC). The structure of the RARC curriculum was defined as follows: (1) theoretical training; (2) preclinical simulation-based training: 5-day simulation-based activity, using models with increasing complexity (ie, virtual reality, and dry- and wet-laboratory exercises), and nontechnical skills training session; (3) clinical training: modular console activity of at least 6 months at the host center (a RARC case was divided into 11 steps and steps of similar complexity were grouped into five modules); and (4) final evaluation: blind review of a video-recorded RARC case [52].
It is noteworthy that, except for the ERUS training curriculum and the RAPN and RARC curricula, the other validated curricula do not follow the virtual reality simulation phase with dry and wet lab and a modular clinical training phase monitored by an experienced surgeon. This phase appears essential in order to transfer, in a protected and safe setting for the patient, the skills learned on training models into a clinical setting.
An important limitation in these validated curricula is the lack of objective, quantitative assessment tools. The above-mentioned curricula generally use qualitative assessment tools which are prone to high interobserver disagreements and subjective scoring. The development of an objective, quantitative scoring method would make the scoring and comparison of scores more reliable. A possible answer is the use of proficiency-based progression curricula with the implementation of validated, binary performance operative metrics to guide trainees during training and objectively scoring of their operative skills [60].
20.5 Assessment Tools to Evaluate Robotic Skills
Objective and standardized tools that can assess acquired skills are key to developing curricula that can accredit surgeons as being able to perform a specific robotic procedure. At the moment, there are different tools to evaluate the trainees. However, as stated above, it seems increasingly necessary to develop new, simple, objective, standardized, useful, and easy-to-use instruments. The most used tools are:
20.5.1 Global Assessment Tools
-
1.
Robotic objective structured assessment of technical skills (ROSATS) : It is the most commonly used assessment scale in robotic surgery, and it is derived from the objective structured assessment of technical skills (OSATS) in surgery. However, it is a subjective evaluation. In ROSATS, four skill categories are assessed: depth perception and accuracy, force and tissue handling, dexterity, and efficiency. The score assigned for each category is from 1 to 5 [61].
-
2.
Global evaluative assessment of robotic skills (GEARS) (Fig. 20.4): It is developed from a score for the evaluation of laparoscopic intraoperative skills, the global operative assessment of laparoscopic skills (GOALS). Therefore, this instrument was not explicitly developed for robotic surgery but was adapted for this technique. Six domains are assessed by this tool: Depth perception, bimanual dexterity, efficiency, force sensitivity, autonomy, and robotic control. The score assigned for each category is from 1 to 5. Studies showed that this score is a valid, reliable, reproducible measure to evaluate intraoperative robotic surgical skills and is also associated with functional outcomes in RARP [26, 62].
-
3.
Structured assessment of robotic microsurgery skills (SARMS): This is a validated tool. It was adapted to robotic surgery starting from the original structured assessment of microsurgery skills (SAMS) [63].
-
4.
Assessment of robotic console skills (ARCS): It is a validated instrument, consisting of six domains used to verify the adequate acquisition of skills in the use of the robotic console [64].
-
5.
Generic dedicated scoring criteria (GDSC): This is a validated tool used to evaluate the video of a complete procedure performed by the trainees at the end of the ERUS curriculum. The parameters evaluated are instrument use, tissue handling, and errors made. The score assigned for each category is from 1 to 5 [45].
20.5.2 Procedure-specific Assessment Tools
Recently, tools aiming to evaluate specific interventions or steps have been developed. These tools can evaluate both the acquisition of technical skills and the mastery of the procedure, assessing the safety and autonomy of the surgeon in performing the specific intervention. However, to date, no studies have assessed their correlation with clinical outcomes [62]. Specifically, for RARP, we can identify the RARP assessment score, the Robotic Anastomosis Competency Evaluation (RACE), and the Prostatectomy Assessment and Competency Evaluation (PACE) [65,66,67]. For RAPN, we can identify the RAPN assessment score and “Scoring for Partial Nephrectomy” (SPaN) [68]. For pelvic lymphadenectomy, we can identify the Pelvic Lymphadenectomy Appropriateness and Completion Evaluation (PLACE) [69]. Finally, for cystectomy, we can identify Cystectomy Assessment and Surgical Evaluation (CASE) [70].
20.5.3 Automated Assessment Tools
These tools automatically acquire data during the execution of the exercise by the trainee. They have the advantage of providing an objective, quantifiable assessment, without loss of time by the evaluator. However, further development of this evaluation method is necessary in order to apply it continuously and on a large scale [62].
20.6 Future Perspectives
To date, the structured and modular training model has appeared to be the most convincing. However, the future seems directed toward a new training methodology: proficiency-based progression (PBP) training. The PBP has not yet been applied to robotic surgery, but prospective studies, randomized in other surgical areas, have shown how the application of this approach improves trainees’ skillsets by 40–70% compared to the level reached using conventional or traditional training [60, 71]. The application of this training model to robotic surgery might be crucial and result in better preparation of the surgeon for the operating room.
20.7 Conclusion
This recent literature analysis suggests that there is an urgent need to develop and validate new structured training curricula for robotic surgery. This allows them to improve the skills of the surgeons and of their team and to prevent patients from being used as a training module, optimizing their safety. Objective and repeatable evaluation systems and metrics might be used to assess the skills of the trainee and allow the attestation of the skills acquired. The road taken with structured curricula seems to be profitable because it takes into account the various theoretical and practical aspects that must be acquired by the robotic surgeon before fully accessing the clinical setting.
Further refinements in the curricula and some validation studies and reports demonstrating improvement in clinical outcomes since the first phase of learning curves seem to be necessary. However, the tendency to move training out of the operating room should be pursued.
Key Points
-
A validated, centralized, and standardized program of robotic surgery training, for each specific procedure is fundamental to guarantee patient safety.
-
A structured training curriculum should include theoretical training (e-learning, case observation), preclinical simulation-based training (virtual reality simulation, dry and wet lab), clinical modular training, and a final evaluation.
-
At the moment, there are different tools to evaluate the trainees. However, it seems increasingly necessary to develop new, simple, objective, standardized, useful, and easy instruments to use.
-
The future seems directed toward a new training methodology: the proficiency-based progression (PBP) training. The application of this training model to robotic surgery might be crucial and result in better preparation of the surgeon for the operating room.
References
Dasgupta P. Robotics in urology. Int J Med Robot Comput Assist Surg [Internet]. 2008 Mar [cited 2018 Jun 22];4(1):1–2. Available from: http://www.ncbi.nlm.nih.gov/pubmed/18314918.
George EI, Brand TC, LaPorta A, Marescaux J, Satava RM. Origins of robotic surgery: from skepticism to standard of care. JSLS J Soc Laparoendosc Surg [Internet]. 2018 Oct 1 [cited 2020 Nov 11];22(4). Available from: https://pubmed.ncbi.nlm.nih.gov/30524184/
Yates DR, Vaessen C, Roupret M. From Leonardo to da Vinci: the history of robot-assisted surgery in urology [Internet]. Vol. 108, BJU International. Blackwell Publishing Ltd; 2011 [cited 2020 Nov 11]. p. 1708–13. Available from: https://pubmed.ncbi.nlm.nih.gov/21951677/
Hakenberg OW. A brief overview of the development of robot-assisted radical prostatectomy. Arab J Urol [Internet]. 2018 Sep 1 [cited 2020 Nov 8];16(3):293–6. Available from: https://pubmed.ncbi.nlm.nih.gov/30140464/
Mottrie A, Larcher A, Patel V. The past, the present, and the future of robotic urology: robot-assisted surgery and human-assisted robots [Internet]. Vol. 4, European Urology Focus. Elsevier B.V.; 2018 [cited 2020 Nov 8]. p. 629–31. Available from: https://pubmed.ncbi.nlm.nih.gov/30337191/
Yuh BE, Hussain A, Chandrasekhar R, Bienko M, Piacente P, Wilding G, et al. Comparative analysis of global practice patterns in urologic robot-assisted surgery. J Endourol [Internet]. 2010 Oct 1 [cited 2020 Nov 11];24(10):1637–44. Available from: https://pubmed.ncbi.nlm.nih.gov/20818990/
Pierorazio PM, Allaf ME. Minimally invasive surgical training: challenges and solutions [Internet]. Vol. 27, Urologic Oncology: Seminars and Original Investigations. Urol Oncol; 2009 [cited 2020 Nov 8]. p. 208–13. Available from: https://pubmed.ncbi.nlm.nih.gov/19285236/
Collins JW, Levy J, Stefanidis D, Gallagher A, Coleman M, Cecil T, et al. Utilising the Delphi process to develop a proficiency-based progression train-the-trainer course for robotic surgery training [Internet]. Vol. 75, European Urology. Elsevier B.V.; 2019 [cited 2020 Nov 8]. p. 775–85. Available from: https://pubmed.ncbi.nlm.nih.gov/30665812/
Logan M. Why hospitals should fly: the ultimate flight plan to patient safety and quality care. Biomed Instrum Technol. 2010 Mar 1;44(2):110.
Collins JW, Wisz P. Training in robotic surgery, replicating the airline industry. How far have we come? World J Urol. 2020 Jul 1;38(7):1645–51.
Fisher RA, Dasgupta P, Mottrie A, Volpe A, Khan MS, Challacombe B, et al. An over-view of robot assisted surgery curricula and the status of their validation [Internet]. Vol. 13, International Journal of Surgery. Elsevier Ltd; 2015 [cited 2020 Nov 8]. p. 115–23. Available from: https://pubmed.ncbi.nlm.nih.gov/25486264/
Puliatti S, Mazzone E, Dell’Oglio P. Training in robot-assisted surgery. Vol. 30, Current Opinion in Urology. Lippincott Williams and Wilkins; 2020. p. 65–72.
Sridhar AN, Briggs TP, Kelly JD, Nathan S. Training in robotic surgery—an overview [Internet]. Vol. 18, Current Urology Reports. Current Medicine Group LLC 1; 2017 [cited 2020 Nov 8]. Available from: https://pubmed.ncbi.nlm.nih.gov/28647793/
De La Garza JR, Kowalewski KF, Friedrich M, Schmidt MW, Bruckner T, Kenngott HG, et al. Does rating the operation videos with a checklist score improve the effect of E-learning for bariatric surgical training? Study protocol for a randomized controlled trial. Trials [Internet]. 2017 Mar 21 [cited 2020 Nov 11];18(1). Available from: https://pubmed.ncbi.nlm.nih.gov/28327195/
Angelo RL, Ryu RKN, Pedowitz RA, Beach W, Burns J, Dodds J, et al. A proficiency-based progression training curriculum coupled with a model simulator results in the acquisition of a superior arthroscopic Bankart skill set. Arthroscopy. 2015 Oct 1;31(10):1854–71.
Prebay ZJ, Peabody JO, Miller DC, Ghani KR. Video review for measuring and improving skill in urological surgery. Nat Rev Urol. 2019 Apr 1;16(4):261–7.
Jayakumar N, Brunckhorst O, Dasgupta P, Khan MS, Ahmed K. E-learning in surgical education: a systematic review. J Surg Educ [Internet]. 2015 [cited 2020 Nov 11];72(6):1145–57. Available from: https://pubmed.ncbi.nlm.nih.gov/26111822/
Maertens H, Madani A, Landry T, Vermassen F, Van Herzeele I, Aggarwal R. Systematic review of e-learning for surgical training [Internet]. Vol. 103, The British Journal of Surgery. John Wiley & Sons Ltd; 2016 [cited 2020 Nov 8]. p. 1428–37. Available from: https://pubmed.ncbi.nlm.nih.gov/27537708/
Chen R, Rodrigues Armijo P, Krause C, Siu KC, Oleynikov D. A comprehensive review of robotic surgery curriculum and training for residents, fellows, and postgraduate surgical education. Surg Endosc. 2020 Jan 1;34(1):361–7.
Bric J, Connolly M, Kastenmeier A, Goldblatt M, Gould JC. Proficiency training on a virtual reality robotic surgical skills curriculum. Surg Endosc. 2014;28(12):3343–8.
Bric JD, Lumbard DC, Frelich MJ, Gould JC. Current state of virtual reality simulation in robotic surgery training: a review. Vol. 30, Surgical Endoscopy. Springer, New York LLC; 2016. p. 2169–2178.
Childs BS, Manganiello MD, Korets R. Novel education and simulation tools in urologic training, vol. 20. Current Urology Reports: Springer; 2019.
Kumar A, Smith R, Patel VR. Current status of robotic simulators in acquisition of robotic surgical skills. Vol. 25, Current Opinion in Urology. Lippincott Williams and Wilkins; 2015. p. 168–174.
Brook NR, Dell’Oglio P, Barod R, Collins J, Mottrie A. Comprehensive training in robotic surgery [Internet]. Vol. 29, Current Opinion in Urology. Lippincott Williams and Wilkins; 2019 [cited 2020 Nov 8]. p. 1–9. Available from: https://pubmed.ncbi.nlm.nih.gov/30394945/
Whitehurst S V., Lockrow EG, Lendvay TS, Propst AM, Dunlow SG, Rosemeyer CJ, et al. Comparison of two simulation systems to support robotic-assisted surgical training: a pilot study (Swine Model). J Minim Invasive Gynecol [Internet]. 2015 Mar 1 [cited 2020 Nov 11];22(3):483–8. Available from: https://pubmed.ncbi.nlm.nih.gov/25543068/
Goh AC, Aghazadeh MA, Mercado MA, Hung AJ, Pan MM, Desai MM, et al. Multi-institutional validation of fundamental inanimate robotic skills tasks. J Urol [Internet]. 2015 Dec 1 [cited 2020 Nov 8];194(6):1751–6. Available from: https://pubmed.ncbi.nlm.nih.gov/26196733/
Ramos P, Montez J, Tripp A, Ng CK, Gill IS, Hung AJ. Face, content, construct and concurrent validity of dry laboratory exercises for robotic training using a global assessment tool. BJU Int. 2014;113(5):836–42.
https://www.orsi-online.com/en/animal-research. Yahoo Search Results Yahoo Search Results [Internet]. [cited 2020 Nov 11]. Available from: https://search.yahoo.com/yhs/search;_ylt= AwrCw LAyFKxf9Xs AzQcPxQt.;_ylc= X1MDMj ExNDcwMDU1OQRfcgMyBGZyA3locy1yb3R6LTAw MQRmcjIDc2I tdG9wBGdwcmlkA2Zp NzAxZ0JnVE15cGFlUWtpQnhhb0EEbl9yc 2x0A zAEbl9zdWdnAz AEb3JpZ2luA3Vz LnNlYXJjaC55YWhvby5jb20EcG9zAzAEcHFzd HIDBHBxc3 RybAMwB HFzdHJsAz Q4BHF1ZXJ5A2h0dHBzJTNBJTJGJTJGd3d3 Lm9yc2ktb25 saW5lLm NvbSUyRmVuJTJGYW5pbWFsLSUyMHJlc2VhcmNoLgR0X3N 0bXADMTYwNTExMjg 5Mg%2D%2 D?p=https%3A%2F%2Fwww.orsi-online.com%2Fen% 2Fanimal -+research.&fr2=sb-top&hspart=rotz & hsimp=yhs-001¶m1=ArFaI WRoNqArQGMVB7sby78oQGR7B7NoN9I8xbFbMmYsQGMVyDMly7IexrFbMnM pQGMV Nos3wCoUwV5bDGUNNEU3wCIWNEQ3vmoWvFM9JmIYvFE9Ia UHwVQ3vCk3w Vw4ISo XNEM4ICISN EM4ICI VwVQ9IaUHNEVcFmI YNEU9JGUIwVM9Jq UKvFQ4 ICILNF dcIaUXNEBcGq QANFdcFCk8NoNdIqYVw VU3vqYTvFE3vCoWw Vw9JmoWwVI3 vmI SvFFdJmIWwVI9I6k3v FQ9JGY TwVxdJCoUv FI9JCoVvmldJq YWvFM3vCIVNVB bFCILNEVb Dmk8NUM9JmoVwVM9JCILNFdbDSk8wVM9ImoVwVQ9ImIWwV A9J6IXwV5c GWUW vmFcHWUI NFM9J6ITvFI9Jm ITwVM9ImIWw VQ9GqUFNFo3wCoUwV5cJqQzNEBcEWUGNF43w HFbMnMbQGMV MqxbNWVbMq V4QGR7BHFaIT8 pxo0qCaRdCaV7C78qvU0rwSQbymIg B81cLU19Mo1dNt%3D%3D¶m2=¶m3=¶m4=&type= mdrue1fc8b293d524278a756
Aydin A, Raison N, Khan MS, Dasgupta P, Ahmed K. Simulation-based training and assessment in urological surgery. Nat Rev Urol. 2016;13:503–19.
Song PH. Current status of simulation-based training and assessment in urological robot-assisted surgery [Internet]. Vol. 57, Investigative and Clinical Urology. Korean Urological Association; 2016 [cited 2020 Nov 8]. p. 375–6. Available from: https://pubmed.ncbi.nlm.nih.gov/27847910/
Goh AC, Goldfarb DW, Sander JC, Miles BJ, Dunkin BJ. Global evaluative assessment of robotic skills: Validation of a clinical assessment tool to measure robotic surgical skills. J Urol [Internet]. 2012 Jan [cited 2020 Nov 11];187(1):247–52. Available from: https://pubmed.ncbi.nlm.nih.gov/22099993/
Collins JW, Dell’Oglio P, Hung AJ, Brook NR. The importance of technical and non-technical skills in robotic surgery training [Figure presented] [Internet]. Vol. 4, European Urology Focus. Elsevier B.V.; 2018 [cited 2020 Nov 8]. p. 674–6. Available from: https://pubmed.ncbi.nlm.nih.gov/30217631/
Van Der Poel H, Brinkman W, Van Cleynenbreugel B, Kallidonis P, Stolzenburg JU, Liatsikos E, et al. Training in minimally invasive surgery in urology: European Association of Urology/International Consultation of Urological Diseases consultation. BJU Int. 2016 Mar 1;117(3):515–30.
Flin R, Yule S, Paterson-Brown S, Maran N, Rowley D, Youngson G. Teaching surgeons about non-technical skills [Internet]. Vol. 5, Surgeon. Edinburgh University Press; 2007 [cited 2020 Nov 11]. p. 86–9. Available from: https://pubmed.ncbi.nlm.nih.gov/17450689/
Hung AJ, Chen J, Shah A, Gill IS. Telementoring and Telesurgery for Minimally Invasive Procedures [Internet]. Vol. 199, Journal of Urology. Elsevier Inc.; 2018 [cited 2020 Nov 8]. p. 355–69. Available from: https://pubmed.ncbi.nlm.nih.gov/28655529/
Lott FM, Siqueira D, Argolo H, Nóbrega BL, Campos FS, Favorito LA. Analysis of the learning curve of surgeons without previous experience in laparoscopy to perform robot-assisted radical prostatectomy. Adv Urol [Internet]. 2018 [cited 2020 Nov 11];2018. Available from: https://pubmed.ncbi.nlm.nih.gov/30510573/
Di Pierro GB, Wirth JG, Ferrari M, Danuser H, Mattei A. Impact of a single-surgeon learning curve on complications, positioning injuries, and renal function in patients undergoing robot-assisted radical prostatectomy and extended pelvic lymph node dissection. Urology [Internet]. 2014 Nov 1 [cited 2020 Nov 11];84(5):1106–11. Available from: https://pubmed.ncbi.nlm.nih.gov/25443913/
Wolanski P, Chabert C, Jones L, Mullavey T, Walsh S, Gianduzzo T. Preliminary results of robot-assisted laparoscopic radical prostatectomy (RALP) after fellowship training and experience in laparoscopic radical prostatectomy (LRP). BJU Int [Internet]. 2012 [cited 2020 Nov 8];110 Suppl 4:64–70. Available from: https://pubmed.ncbi.nlm.nih.gov/23194128/
Bravi CA, Tin A, Vertosick E, Mazzone E, Martini A, Dell’oglio P, et al. The impact of experience on the risk of surgical margins and biochemical recurrence after robot-assisted radical prostatectomy: a learning curve study. J Urol [Internet]. 2019 Jul 1 [cited 2020 Nov 11];202(1):108–13. Available from: https://pubmed.ncbi.nlm.nih.gov/30747873/
Abboudi H, Khan MS, Aboumarzouk O, Guru KA, Challacombe B, Dasgupta P, et al. Current status of validation for robotic surgery simulators a systematic review [Internet]. Vol. 111, BJU International. BJU Int; 2013 [cited 2020 Nov 8]. p. 194–205. Available from: https://pubmed.ncbi.nlm.nih.gov/22672340/
George BC, Bohnen JD, Williams RG, Meyerson SL, Schuller MC, Clark MJ, et al. Readiness of US general surgery residents for independent practice. Ann Surg [Internet]. 2017 Oct 1 [cited 2020 Nov 11];266(4):582–94. Available from: https://pubmed.ncbi.nlm.nih.gov/28742711/
Satava RM, Stefanidis D, Levy JS, Smith R, Martin JR, Monfared S, et al. Proving the effectiveness of the fundamentals of robotic surgery (FRS) skills curriculum: A single-blinded, multispecialty, multi-institutional randomized control trial. Ann Surg [Internet]. 2020 Aug 1 [cited 2020 Nov 8];272(2):384–92. Available from: https://pubmed.ncbi.nlm.nih.gov/30720503/
Gandaglia G, De Lorenzis E, Novara G, Fossati N, De Groote R, Dovey Z, et al. Robot-assisted radical prostatectomy and extended pelvic lymph node dissection in patients with locally-advanced prostate cancer. Eur Urol. 2017;71(2):249–56.
Mottrie A, Novara G, van der Poel H, Dasgupta P, Montorsi F, Gandaglia G. The European Association of Urology Robotic Training Curriculum: an update. Eur Urol Focus [Internet]. 2016 Apr 1 [cited 2020 Nov 8];2(1):105–8. Available from: https://pubmed.ncbi.nlm.nih.gov/28723444/
Volpe A, Ahmed K, Dasgupta P, Ficarra V, Novara G, Van Der Poel H, et al. Pilot validation study of the European Association of Urology robotic training curriculum. Eur Urol. 2015 Aug 1;68(2):292–9.
Abboudi M, Ahmed K, Kirby R, Khan MS, Dasgupta P, Challacombe B. Mentorship programmes for laparoscopic and robotic urology [Internet]. Vol. 107, BJU International. BJU Int; 2011 [cited 2020 Nov 8]. p. 1869–71. Available from: https://pubmed.ncbi.nlm.nih.gov/21623939/
Steinberg PL, Merguerian PA, Bihrle W, Seigne JD. The cost of learning robotic-assisted prostatectomy. Urology [Internet]. 2008 Nov [cited 2020 Nov 11];72(5):1068–72. Available from: https://pubmed.ncbi.nlm.nih.gov/18313121/
Vanlander AE, Mazzone E, Collins JW, Mottrie AM, Rogiers XM, van der Poel HG, et al. Orsi Consensus Meeting on European Robotic Training (OCERT): results from the first multispecialty consensus meeting on training in robot-assisted surgery. Eur Urol. 2020;78:713–6.
Dulan G, Rege R V., Hogg DC, Gilberg-Fisher KK, Tesfay ST, Scott DJ. Content and face validity of a comprehensive robotic skills training program for general surgery, urology, and gynecology. Am J Surg [Internet]. 2012 Apr [cited 2020 Nov 8];203(4):535–9. Available from: https://pubmed.ncbi.nlm.nih.gov/22326049/
Valdis M, Chu MWA, Schlachta CM, Kiaii B. Validation of a novel virtual reality training curriculum for robotic cardiac surgery a randomized trial. Innov Technol Tech Cardiothorac Vasc Surg [Internet]. 2015 [cited 2021 Jan 2];10(6):383–8. Available from: https://pubmed.ncbi.nlm.nih.gov/26680752/
Larcher A, De Naeyer G, Turri F, Dell’Oglio P, Capitanio U, Collins JW, et al. The ERUS curriculum for robot-assisted partial nephrectomy: structure definition and pilot clinical validation. Eur Urol [Internet]. 2019 Jun 1 [cited 2020 Nov 8];75(6):1023–31. Available from: https://pubmed.ncbi.nlm.nih.gov/30979635/
Dell’Oglio P, Turri F, Larcher A, D’Hondt F, Sanchez-Salas R, Bochner B, et al. Definition of a structured training curriculum for robot-assisted radical cystectomy with intracorporeal ileal conduit in male patients: a Delphi consensus study led by the ERUS Educational Board. Eur Urol Focus [Internet]. 2021 Jan [cited 2021 Jan 11]; Available from: https://linkinghub.elsevier.com/retrieve/pii/S2405456920303175
Palagonia E, Mazzone E, De Naeyer G, D’Hondt F, Collins J, Wisz P, et al. The safety of urologic robotic surgery depends on the skills of the surgeon. World J Urol [Internet]. 2020 Jun 1 [cited 2020 Nov 8];38(6):1373–83. Available from: https://pubmed.ncbi.nlm.nih.gov/31428847/
Stegemann AP, Ahmed K, Syed JR, Rehman S, Ghani K, Autorino R, et al. Fundamental skills of robotic surgery: A multi-institutional randomized controlled trial for validation of a simulation-based curriculum. Urology [Internet]. 2013 Apr [cited 2020 Nov 8];81(4):767–74. Available from: https://pubmed.ncbi.nlm.nih.gov/23484743/
Dulan G, Rege R V., Hogg DC, Gilberg-Fisher KM, Arain NA, Tesfay ST, et al. Proficiency-b sed training for robotic surgery: Construct validity, workload, and expert levels for nine inanimate exercises. Surg Endosc [Internet]. 2012 [cited 2020 Nov 8];26(6):1516–21. Available from: https://pubmed.ncbi.nlm.nih.gov/22350226/
Foell K, Finelli A, Yasufuku K, Bernardini MQ, Waddell TK, Pace KT, et al. Robotic surgery basic skills training: Evaluation of a pilot multidisciplinary simulation-based curriculum. Can Urol Assoc J [Internet]. 2013 Dec 5 [cited 2021 Jan 2];7(11–12):430. Available from: https://pubmed.ncbi.nlm.nih.gov/24381662/
Larcher A, Turri F, Bianchi L, Dell’Oglio P, Collins J, Capitanio U, et al. Virtual reality validation of the ERUS simulation-based training programmes: results from a high-volume training centre for robot-assisted surgery. Eur Urol. 2019;75:885–7.
Mazzone E, Dell’Oglio P, Mottrie A. Outcomes report of the first ERUS robotic urology curriculum-trained surgeon in Turkey: the importance of structured and validated training programs for global outcomes improvement. Turkish J Urol [Internet]. 2019 May 1 [cited 2020 Nov 8];45(3):189–90. Available from: http://www.ncbi.nlm.nih.gov/pubmed/31846420.
Bedir F, Keske M, Demirdögen SO, Kocatürk H, Koç E, Canda AE, et al. Robotic radical prostatectomy in 93 cases: Outcomes of the first ERUS robotic urology curriculum trained surgeon in Turkey. Turkish J Urol [Internet]. 2019 May 1 [cited 2020 Nov 8];45(3):183–8. Available from: https://pubmed.ncbi.nlm.nih.gov/30817280/
Gallagher AG, Ritter EM, Champion H, Higgins G, Fried MP, Moses G, et al. Virtual reality simulation for the operating room: proficiency-based training as a paradigm shift in surgical skills training. Ann Surg. 2005;241:364–72.
Siddiqui NY, Galloway ML, Geller EJ, Green IC, Hur HC, Langston K, et al. Validity and reliability of the robotic objective structured assessment of technical skills. Obstet Gynecol [Internet]. 2014 [cited 2020 Nov 8];123(6):1193–9. Available from: https://pubmed.ncbi.nlm.nih.gov/24807319/
Chen J, Cheng N, Cacciamani G, Oh P, Lin-Brande M, Remulla D, et al. Objective assessment of robotic surgical technical skill: a systematic review [Internet]. Vol. 201, Journal of Urology. Lippincott Williams and Wilkins; 2019 [cited 2020 Nov 8]. p. 461–9. Available from: https://pubmed.ncbi.nlm.nih.gov/30053510/
Alrasheed T, Liu J, Hanasono MM, Butler CE, Selber JC. Robotic microsurgery: validating an assessment tool and plotting the learning curve. Plast Reconstr Surg [Internet]. 2014 [cited 2021 Jan 2];134(4):794–803. Available from: https://pubmed.ncbi.nlm.nih.gov/25357037/
Liu M, Purohit S, Mazanetz J, Allen W, Kreaden US, Curet M. Assessment of Robotic Console Skills (ARCS): construct validity of a novel global rating scale for technical skills in robotically assisted surgery. Surg Endosc [Internet]. 2018 Jan 1 [cited 2021 Jan 2];32(1):526–35. Available from: https://pubmed.ncbi.nlm.nih.gov/28667546/
Lovegrove C, Novara G, Mottrie A, Guru KA, Brown M, Challacombe B, et al. Structured and modular training pathway for Robot-assisted Radical Prostatectomy (RARP): validation of the RARP assessment score and learning curve assessment. Eur Urol [Internet]. 2016 Mar 1 [cited 2020 Nov 8];69(3):526–35. Available from: https://pubmed.ncbi.nlm.nih.gov/26585582/
Raza SJ, Field E, Jay C, Eun D, Fumo M, Hu JC, et al. Surgical competency for urethrovesical anastomosis during robot-assisted radical prostatectomy: development and validation of the robotic anastomosis competency evaluation. Urology [Internet]. 2015 Jan 1 [cited 2020 Nov 8];85(1):27–32. Available from: https://pubmed.ncbi.nlm.nih.gov/25530362/
Hussein AA, Ghani KR, Peabody J, Sarle R, Abaza R, Eun D, et al. Development and validation of an objective scoring tool for robot-assisted radical prostatectomy: prostatectomy assessment and competency evaluation. J Urol [Internet]. 2017 May 1 [cited 2020 Nov 8];197(5):1237–44. Available from: https://pubmed.ncbi.nlm.nih.gov/27913152/
Hussein AA, Abaza R, Rogers C, Boris R, Porter J, Allaf M, et al. PD07-09 development and validation of an objective scoring tool for minimally invasive partial nephrectomy: scoring for partial nephrectomy (span). J Urol. 2018 Apr;199(4S):e159–60.
Hussein AA, Hinata N, Dibaj S, May PR, Kozlowski JD, Abol-Enein H, et al. Development, validation and clinical application of pelvic lymphadenectomy assessment and completion evaluation: intraoperative assessment of lymph node dissection after robot-assisted radical cystectomy for bladder cancer. BJU Int [Internet]. 2017 Jun 1 [cited 2021 Jan 2];119(6):879–84. Available from: http://doi.wiley.com/10.1111/bju.13748
Hussein AA, Sexton KJ, May PR, Maxwell MV, Hosseini A, et al. Development and validation of surgical training tool: cystectomy assessment and surgical evaluation (CASE) for robot-assisted radical cystectomy for men. Surg Endosc [Internet]. 1234 [cited 2021 Jan 2];32:4458–64. Available from: https://doi.org/10.1007/s00464-018-6191-3.
Gallagher A. Proficiency-based progression simulation training for more than an interesting educational experience. J Musculoskelet Surg Res [Internet]. 2018 [cited 2021 Jan 2];2(4):139. Available from: http://www.journalmsr.com/text.asp?2018/2/4/139/244728
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
De Groote, R., Puliatti, S., Mazzone, E., Dell’Oglio, P., Mottrie, A., Gallagher, A.G. (2022). Validated Training Curricula in Robotic Urology. In: Biyani, C.S., Van Cleynenbreugel, B., Mottrie, A. (eds) Practical Simulation in Urology . Springer, Cham. https://doi.org/10.1007/978-3-030-88789-6_20
Download citation
DOI: https://doi.org/10.1007/978-3-030-88789-6_20
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-88788-9
Online ISBN: 978-3-030-88789-6
eBook Packages: MedicineMedicine (R0)