Abstract
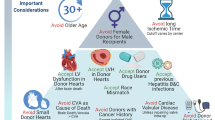
Considering the exponential increase in organ demand with a stable donor supply, cardiac donor management and selection is of utmost importance. The criteria for an acceptable donor have changed dramatically over the last 40 years and transplant teams are accepting older patients, longer ischemic times, donor substance abuse, and sometimes donor infection. Expanding the donor pool to the “increased risk” donors has enforced a more complex balance of donor and recipient components. A risk benefit ratio is commonly explored to provide the best donor to the more stable patient and accept an increased-risk donor in the patient with a shorter life expectancy. Patients with more urgent status designation include those on veno-arterial extracorporeal membrane oxygenation (VA ECMO), with surgically implanted ventricular-assist devices and nondischargeable status or life threatening ventricular arrhythmias. Recently, use of VA ECMO as a bridge to heart transplant has expanded moving patients to the top of the waiting list. The intricacy of this risk-benefit balance will be highlighted in this chapter to provide optimal cardiac transplant outcomes to as many patients as possible and use all resources to their full potential.
Similar content being viewed by others
References
Alexander JW, Vaughn WK (1991) The use of “marginal” donors for organ transplantation. The influence of donor age on outcome. Transplantation 51(1):135–141
Allan DK, Knechtle SJ, Larsen CP, et al (2014) Textbook of organ transplantation. In: Kirk AD, Knechtle SJ, Larsen CP, Madsen JC, Pearson TC, & Webber SA (Eds.). John Wiley & Sons. Organ procurement and allocation, p 268
Brock MV, Salazar JD, Cameron DE et al (2001) The changing profile of the cardiac donor. J Heart Lung Transplant 20:1005–1009
Capatina C, Paluzzi A, Mitchell R, Karavitaki N (2015) Diabetes insipidus after traumatic brain injury. J Clin Med 4(7):1448–1462
Chan BB, Fleischer KJ, Bergin JD et al (1991) Weight is not an accurate criterion for adult cardiac transplant size matching. Ann Thorac Surg 52(6):1230–1235. discussion 1235–6
Cooper DK, Miller LW, Patterson GA (2007) The transplantation and replacement of thoracic organs: the present status of biological and mechanical replacement of the heart and lungs, p 25
Costanzo MR, Dipchand A, Starling R et al (2010) The international society for heart and lung transplantation guidelines for the care of heart transplant recipients. J Heart Lung Transplant 29:914–956
Edwards NM, Chen JM, Mazzeo PA (2005) Cardiac transplantation: the Columbia University Medical Center/New York-Presbyterian Hospital Manual, Contemporary cardiology. Humana Press, Totowa, pp 19–36
Freimark D, Czer LS, Admon D et al (1994) Donors with a history of cocaine use: effect on survival and rejection frequency after heart transplantation. J Heart Lung Transplant 13(6):1138–1144
Freimark D, Aleksic I, Trento A et al (1996) Hearts from donors with chronic alcohol use: a possible risk factor for death after heart transplantation. J Heart Lung Transplant 15:150–159
Gong T, Joseph S, Lima B et al (2018) Donor predicted heart mass as predictor of primary graft dysfunction. J Heart Lung Transplant 37(7):826–835
Hosseinpour AR, Cullen S, Tsang VT (2006) Transplantation for adults with congenital heart disease. Eur J Cardiothorac Surg 30:508–551
Houyel L, Petit J, Nottin R et al (1992) Adult heart transplantation: adverse role of chronic alcoholism in donors on early graft function. J Heart Lung Transplant 11:1184–1187
Jacob KA et al (2015) Chronic alcoholic donors in heart transplantation: A mortality meta-analysis. Int J Cardiol 191:7–10
Jawitz OK, Jawitz NG, Yuh D et al (2013) Impact of ABO compatibility on outcomes after heart transplantation in a national cohort during the past decade. J Thorac Cardiovasc Surg 146(5):1239–1246
John R (2004) Donor management and selection for heart transplantation. Semin Thorac Cardiovasc Surg 16:364–369
John R, Rajasinghe HA, Chen JM et al (2000) Impact of current management practices on early and late mortality in over 500 consecutive heart transplant recipients. Ann Surg 232:302–311
Kerman RH (2007) Understanding the sensitized patient. Heart Fail Clin 3:1–9
Khasati NH, Machaal A, Barnard J, Yonan N (2007) Donor heart selection: the outcome of “unacceptable” donors. J Cardiothorac Surg 2:13–13
Kilic A, Emani S, Sai-Sudhakar CB et al (2014) Donor selection in heart transplantation. J Thorac Dis 6(8):1097–1104
Kransdorf E, Kittleson M, Patel J et al (2017) Predicted heart mass is the optimal metric for size matching in heart transplantation. J Heart Lung Transplant 36(4):S113–S114
Mehra MR et al (2016) The 2016 international society for heart lung transplantation listing criteria for heart transplantation: a 10-year update. J Heart Lung Transplant 35(1):1–23
Nixon JL, Kfoury AG, Brunisholz K et al (2012) Impact of high-dose inotropic donor support on early myocardial necrosis and outcomes in cardiac transplantation. Clin Transpl 26:322–327
Patel SR, Saeed O, Sims D et al (2018) Cardiac transplantation from non-viremic hepatitis C donors. J Heart Lung Transplant 37(4):S137
Peled Y, Lavee J, Arad M et al (2017) The impact of gender mismatching on early and late outcomes following heart transplantation. Esc Heart Fail 4(1):31–39
Schlendorf KH, Zalawadiya S, Shah A et al (2018) Early outcomes using hepatitis C–positive donors for cardiac transplantation in the era of effective direct-acting anti-viral therapies. J Heart Lung Transplant 37(6):763–769
Schüler S, Warnecke H, Loebe M et al (1989) Extended donor age in cardiac transplantation. Circulation 80(5 Pt 2):III133–III139
Stehlik J et al (2011) The registry of the international society for heart and lung transplantation: twenty-eighth adult heart transplant report—2011. J Heart Lung Transplant 30(10):1078–1094
Taylor DO, Edwards LB, Boucek MM et al (2007) Registry of the international society for heart and lung transplantation: twenty-fourth official adult heart transplant report—2007. J Heart Lung Transplant 26:769–781
Tenderich G, Koerner MM, Stuettgen B et al (1998) Extended donor criteria: hemodynamic follow-up of heart transplant recipients receiving a cardiac allograft from donors (over) 60 years of age. Transplantation 66(8):1109–1113
Valantine H (2004) Cardiac allograft vasculopathy after heart transplantation: risk factors and management. J Heart Lung Transplant 23:S187–S193
Velez M, Johnson MR (2009) Management of allosensitized cardiac transplant candidates. Transplant Rev (Orlando, Fla) 23(4):235–247
Ventura HO, Muhammed K (2001) Historical perspectives on cardiac transplantation: the past as prologue to challenges for the 21st century. Curr Opin Cardiol 16:118–123
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this entry
Cite this entry
Schultheis, M., Camacho, M. (2019). Matching Donor to Recipient. In: Bogar, L., Stempien-Otero, A. (eds) Contemporary Heart Transplantation. Organ and Tissue Transplantation. Springer, Cham. https://doi.org/10.1007/978-3-319-33280-2_9-1
Download citation
DOI: https://doi.org/10.1007/978-3-319-33280-2_9-1
Received:
Accepted:
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-33280-2
Online ISBN: 978-3-319-33280-2
eBook Packages: Springer Reference MedicineReference Module Medicine