Abstract
Metastasis, or the spread of cancer cells from a primary tumor to distant sites, is the leading cause of cancer-associated death. Metastasis is a complex multi-step process comprised of invasion, intravasation, survival in circulation, extravasation, and formation of metastatic colonies. Currently, in vitro assays are limited in their ability to investigate these intricate processes and do not faithfully reflect metastasis as it occurs in vivo. Traditional in vivo models of metastasis are limited by their ability to visualize the seemingly sporadic behavior of where and when cancer cells spread (Reymond et al., Nat Rev Cancer 13:858–870, 2013). The avian embryo model of metastasis is a powerful platform to study many of the critical steps in the metastatic cascade including the migration, extravasation, and invasion of human cancer cells in vivo (Sung et al., Nat Commun 6:7164, 2015; Leong et al., Cell Rep 8, 1558–1570, 2014; Kain et al., Dev Dyn 243:216–28, 2014; Leong et al., Nat Protoc 5:1406–17, 2010; Zijlstra et al., Cancer Cell 13:221–234, 2008; Palmer et al., J Vis Exp 51:2815, 2011). The chicken chorioallantoic membrane (CAM) is a readily accessible and well-vascularized tissue that surrounds the developing embryo. When the chicken embryo is grown in a shell-less, ex ovo environment, the nearly transparent CAM provides an ideal environment for high-resolution fluorescent microcopy approaches. In this model, the embryonic chicken vasculature and labeled cancer cells can be visualized simultaneously to investigate specific steps in the metastatic cascade including extravasation. When combined with the proper image analysis tools, the ex ovo chicken embryo model offers a cost-effective and high-throughput platform for the quantitative analysis of tumor cell metastasis in a physiologically relevant in vivo setting. Here we discuss detailed procedures to quantify cancer cell extravasation in the shell-less chicken embryo model with advanced fluorescence microscopy techniques.
Access provided by CONRICYT – Journals CONACYT. Download protocol PDF
Similar content being viewed by others
Key words
- Intravital imaging
- Extravasation
- Chick embryo
- Cancer
- Chorioallantoic membrane
- Fluorescence
- Embryonic vasculature
- Cell migration
- Metastasis
- In vivo
- Shell-less
- GFP
- RFP
- Lectin LCA-fluorescein/rhodamine
1 Introduction
The majority of cancer-related deaths are associated with the onset of metastasis [8]. Currently, there is no accurate test to predict metastasis and no effective therapy to prevent it [9, 10]. In order for cancer cells to metastasize successfully, they must undergo local invasion, intravasation , survival in the circulation, extravasation , and colony expansion in distant metastatic sites [11–15]. Of these steps, extravasation is the least understood, partly due to the lack of effective modeling [1, 16, 17]. The difficulty in capturing a cancer cell extravasating in deep solid tissues has limited our ability to closely study the process of extravasation as it is related to metastatic spread of cancer. Here, we discuss an intravital imaging-based approach using the ex ovo chicken embryo model of metastasis to precisely quantify human cancer cell extravasation.
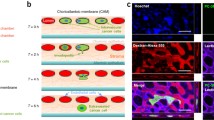
Over the last decade, the chicken embryo model of metastasis has been proven to be a robust and cost-effective research platform to study many aspects of cancer biology. For our purposes, the shell-less chicken embryo model provides a full spectrum of physiologically relevant tissue interactions for studying the metastatic behavior of cancer cells in vivo [7, 18–24]. The easily accessible chick embryo chorioallantoic membrane (CAM), a well-vascularized tissue around the embryo, due to its highly accessible capillary networks, overcomes the deep tissue limitation for microscopic visualization of primary tumor and/or metastatic sites. Intravital imaging in the ex ovo CAM model has shed light on many aspects of the metastasis [25, 26]. Recent advances in “shell-less” embryo preparation coupled with the use of new fluorescent labeling techniques for both host and cancer cells have dramatically enhanced the imaging capabilities of this model in the recent years [2–6, 27–30].
Since the CAM is a translucent and easily accessible tissue, the migratory behavior of fluorescently labeled cancer cells can be readily visualized and recorded longitudinally using various intravital imaging techniques [3, 6, 28] and their migration patterns analyzed by image analysis software. Compared to rodent models, intravital imaging in the CAM requires no anesthesia, surgery, or specialized lenses. These techniques can be achieved with standard upright fluorescent wide-field or confocal microscopy. Temperature control with a local microscope-mounted incubation chamber to provide stable humidity and field of view is suggested for longer term time-lapse imaging. The approach described here allows for an easy-to-use and biophysically relevant in vivo quantitative analysis of human cancer cell extravasation and metastasis .
2 Materials
2.1 Preparation of the Shell-Less Ex Ovo Chicken Embryos
-
1.
Fine-point forceps .
-
2.
Circular cover slips 22 mm.
-
3.
Fertilized white Leghorn eggs, incubated for 12–14 days as described [6, 28, 31].
-
4.
Egg incubator , many commercially available models including 1550E from G.Q.F. MGF Company Inc., Savannah, GA, or Marsh Farms Roll-X Flowing Air Incubators, Lyon Electric Company Inc., Chula Vista, CA.
-
5.
Avian embryo imaging unit Innovascreen (Halifax, Canada) (Fig. 1): This is a specialized microscope-mounted enclosure that maintains the avian embryo in a humidified (>90 % humidity) environment while stabilizing the area of CAM to be imaged using a standard cover slip fixed into the lid of the unit. This allows for short- or long-term noninvasive intravital imaging of the CAM using an upright fluorescence microscope.
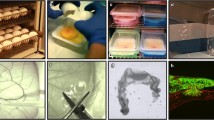
Fig. 1 Overview of the cancer cell intravenous injection . (a) Assembled injection apparatus for IV injection of labeling agents and/or cancer cells. (b) Typical stereomicroscope eye piece view of an injection site. Black arrow points to borosilicate capillary. (c) Example of custom-built incubation unit for in vivo fluorescence imaging of shell-less chicken embryos. Incubation unit is shown with a microscope stage encased in a temperature-regulated enclosure
2.2 Cancer Cell Line Preparation
-
1.
Use cancer cells either transiently or stably transfected with a construct that constitutively expresses a fluorescent protein such as GFP or RFP, or are otherwise fluorescently labeled (e.g., cell membrane dye, fluorescent nanobeads , or fluorescent fusion protein that labels the nucleus such as H1-mCherry) [32–37] (see Notes 1 and 2 ).
-
2.
1× PBS pH 7.4 [37].
-
3.
2.5 % Trypsin (10×).
-
4.
15 mL Conical centrifuge tubes .
-
5.
1.5 mL Microfuge tubes.
-
6.
Benchtop centrifuge .
-
7.
Culture media appropriate for the cell lines used.
-
8.
Hemocytometer for cell counting.
-
9.
Trypan blue (0.4 % trypan blue).
2.3 Intravenous Injection of Cancer Cells or Agents to Visualize Chicken Embryo Vasculature
-
1.
Lectin Lens Culinary Agglutinin (LCA) conjugated with fluorescein or rhodamine (Vector Labs Inc. RL-1042, FL-1041) [38].
-
2.
1 mL Disposable syringes for injections.
-
3.
18-gauge disposable hypodermic needles for injections.
-
4.
Tygon R-3603 laboratory tubing, 50 ft, for injections (1/32 in. inner diameter, 3/32 in. outer diameter, 1/32 in. wall thickness).
-
5.
Vertical pipette puller (David Kopf Instruments, Tujunga, CA; Model 720).
-
6.
Sodium borosilicate glass capillary tubes , outer diameter 1.0 mm, inner diameter 0.58 mm, 10 cm length (Sutter Instrument, Novato, CA).
-
7.
Fine-point forceps .
-
8.
Sterile cotton swabs .
-
9.
Fertilized chicken eggs and egg incubator (see Subheading 2.1). Appropriate microscope(s) and image analysis software (see Note 3 ).
3 Methods
3.1 Cancer Cell Preparation for Injection
-
1.
Culture cancer cell line of interest as required to 80 % confluency . Higher confluency can negatively impact tumor take and extravasation efficiency. Routinely check for absence of mycoplasma contamination. (See [39] for technical considerations on growth of cancer cell lines for in vivo assays.)
-
2.
To trypsinize cells, wash twice with 1× PBS pH 7.4. Aspirate remaining PBS, then add 0.5 % trypsin–EDTA (e.g., 2 mL to 75 cm2 flask, 3 mL to 175 cm2 flask, 3 mL to 150 cm2 culture dish), and incubate at 37 °C for 2–5 min until all cells detach.
-
3.
Add 5 mL of PBS and transfer cell suspension to 15 mL conical centrifuge tube . Centrifuge at room temperature at 200 × g for 5 min.
-
4.
Use another 10 mL of PBS to wash cells from unnecessary media components such as antibiotics and centrifuge the cells again as in step 3.
-
5.
Discard supernatant and resuspend cells with 1 mL of ice-cold PBS.
-
6.
Take 10 μL of suspension and dilute into 490 μL PBS. Count the number of cells in this diluted suspension using hemocytometer .
-
7.
For intravenous (IV) injection of cells (see Subheading 3.2), concentrate cells to 0.5 × 106 to 1.0 × 106 cells/mL. Use ice-cold 1× PBS to dilute/resuspend cell concentrates (see Notes 1 and 4 ).
3.2 Intravenous Injection of Cancer Cells for Extravasation Assay
Depending on the experimental setup as many as 20 embryos can be analyzed within 1 day. Plan to inject excess numbers (20 %) of embryos to determine the optimal starting time point of cancer cell extravasation and to accommodate for suboptimally injected embryos. Use 12–14-day-old embryos for injection of cancer cells, prepared as described (see Note 5 ).
-
1.
When preparing needles for injection of cancer cells (as in Subheading 2.3, steps 5 and 6), the needle bore must be slightly wider than the diameter of the cancer cell used in order to avoid shearing of the cancer cells.
-
2.
Maintain a homogenous cell suspension . Between injections, look for cell aggregation and cell lysis. If clumping is observed, remove the borosilicate needle and use the syringe plunger to mix the cell suspension until clumps are dispersed. Ensure that any air bubbles are removed from the syringe and the tubing prior to injection.
-
3.
Depending on the cell type, cell aggregates may form and clog the needle head. If this occurs, replace the needle and tubing. It is generally necessary to change the needle after injection of every 2–4 embryos.
-
4.
Distinguish veins from arteries on surface of CAM using a dissecting scope. The arteries and veins intertwine on the CAM surface (Fig. 1b) terminating in the capillary plexus. The CAM acts as a gas exchange organ and the arteries appear dark red because they deliver deoxygenated blood to the CAM, while veins are bright red because they transport oxygenated blood back to the embryo. Under a dissecting scope, this subtle color difference allows veins or arteries to be easily differentiated. One can also observe the direction of blood flow (blood flows towards the embryo in the veins).
-
5.
Identify the vein to be injected. With a sufficiently tapered microneedle very narrow veins can be injected, which will minimize bleeding during and after injection. Avoid injecting into major vessels, as this will impact embryo viability. It is recommended to target only vessels that are tributaries or secondary tributaries of the major veins. Additionally, it is technically easier to pierce the vascular wall of smaller veins compared to larger veins. In our experience, it is easiest to inject veins that are slightly (10–20 %) bigger in diameter than the injection needle tip.
-
6.
Using the assembled injection apparatus (Fig. 1a), press the tip of the borosilicate needle against the surface of a vein and gently press forward in the same direction as blood flow. As you press forward, use your other hand to depress the plunger lightly. When the needle tip successfully enters the vessel lumen, the (clear) solution will stream through the vein away from the tip.
-
7.
Minimize movement of the needle and continue to depress plunger (usually with the cell concentration of 0.5 × 106 cells/mL, 2–10 s is required) until desired volume is injected as indicated by the syringe markings. Injection of a single embryo may take 1–10 min depending on the quality of vessel cannulation. If there is excessive clear fluid buildup at the site of injection, pick another site of injection or use a cotton swab to clear the injection site.
-
8.
After removing needle from CAM, dab the injection site with a cotton swab to remove blood and cancer cells that have spilled onto the surface of the CAM. Cells left behind on the CAM surface may be mistaken as sites of extravasation during imaging.
-
9.
Depending on the user , cancer cells may be injected using either white light or fluorescence stereomicroscope. Use a fluorescence dissection microscope to verify successful injection and to assess uniform distribution of cancer cells throughout the capillary plexus of the CAM. For efficient cancer cell extravasation imaging and quantification approximately 10–30 cells must be present in each imaging field (512 × 512 μm, 25× objective). If multiple cell lines are injected to access their extravasation efficiency injections should be “stacked” to correct for delay injection time (see Note 4 ).
-
10.
Return embryo to incubator.
-
11.
Needles can be reused for multiple injections of the same cell line, but the sharpness will decrease with each injection. If injection becomes difficult, replace the needle.
3.3 Intravenous Injection of Lectin into Chorioallantoic Membrane
Different cell lines may take different times to extravasate out of the vasculature. Additionally, cancer cell extravasation times may vary from one batch of chicken embryos to another. It is recommended to start monitoring embryos for cancer cell extravasation 2–4 h post-injection. Inject lectin into a superfluous embryo to determine if sufficient proportion of cancer cells is extravasated (confocal microscope must be used, see Subheading 3.5). If ~30–50 % of the cells per field of image are out of the vasculature in the control condition proceed to the imaging of the rest of the embryos.
-
1.
Smaller needle diameter (10–20 μm) can be used for lectin injection for convenience.
-
2.
Identify the vein to be injected. In our laboratory, we found that it is easier to use the same injection site for lectin as for the tumor cells.
-
3.
Inject lectin using the same technique as for tumor cell injection (see Subheading 3.2, steps 4–10). It is better to over-inject embryo with lectin than under-inject for ease of cancer cell extravasation imaging and quantification (brighter and sharper signal from vasculature will allow for easier scoring of extravasated cancer cells).
-
4.
After injection, place embryo into the incubator for recovery for 5 min. Inject only one embryo at a time immediately before the imaging.
3.4 Imaging of Cell Extravasation In Vivo
-
1.
Set temperature-regulated microscope chamber to 37 °C ~6 h prior to imaging. This will stabilize temperature and help minimize XYZ drift during imaging.
-
2.
To image cancer cell extravasation a 20× or 25× objective lens is recommended. Allow 10–30 min for imaging of a single embryo (see Note 4 ).
-
3.
Apply a thin layer of vacuum grease to underside of the imaging unit lid to create a secure seal with the cover slip . Gently position a cover slip into the lid and wipe away any excess vacuum grease.
-
4.
Position the embryo in the imaging unit such that the cover slip can be lowered down directly onto an open area of the CAM. Slowly lower the lid onto the embryo until the cover slip just makes contact with the CAM. Tighten the screws to secure the lid in place, and ensure that the lid is level and that the cover slip is not putting any downward pressure on the CAM.
-
5.
If longer (time-lapse) imaging is planned, fill the outer jacket of the embryo imaging unit with water heated to 37 °C and place the unit onto the microscope stage (Fig. 1c). For short-term quantitative imaging, no water is necessary. The embryo imaging unit can be fixed to the microscope stage with tape to minimize XY drift.
-
6.
Acquire multiple (~5–10), random 3D (XYZ) fields (25×) from each embryo. Use field-stitching option in the microscope acquisition software, if available. Images must be acquired with such settings (gains/Z-stack thickness, step) such that it is possible to judge intra- or extravascular localization for ~99 % cells within each field. We routinely use 25× objective and 3 × 3 or 5 × 5 field stitching with 5–10 μm Z-step, 100 μm total thickness. Image at least 300 cells per condition.
3.5 Quantification of Cancer Cell Extravasation
-
1.
Specialized software can be used to determine the intra- or extravascular location of cancer cells. We suggest software packages such as Nikon Elements, Volocity (Perkin Elmer), or ImageJ (NIH) to assist with this. Outlined below are general steps that will assist in quantitation of cancer cell extravasation.
-
2.
Open the 3D file as a Z-stack using the necessary software. If significant XY movement occurred during the image acquisition image may be aligned using ImageJ StackReg plug-in (http://bigwww.epfl.ch/thevenaz/stackreg) or similar Nikon Elements and Volocity document alignment protocols (Fig. 2a).
Fig. 2 Tumor cell extravasation analysis . (a) Typical 25× optical lens 3D image field used for cancer cell (LNCap GFP , green) extravasation analysis. Eight-hour time point is shown. Avian embryo vascular plexus is shown in white (Alexa 647). Main panel shows an optical slice that is located approximately in the middle (Z-axis) of the vascular plexus. Extravasated cells (red arrows) appear dim and below the vascular plexus. Lower panels show two separate XZ optical slices used in the analysis of cancer cell extravasation. Note that the extravasated cells appear below the vascular plexus. (b, c) Typical multi-color cancer cell extravasation analysis (HT1080 RFP and GFP cells). At time = 0, all three cells are located within the vascular plexus (see lower XZ panels). At time = 45 min, the red cell on the right (red arrow) is out of the vasculature
-
3.
Scroll through the XYZ image in the Z direction and designate each cancer cell as in or out of the vasculature. We consider a cell extravasated if more than 80 % of the cell body is located out of the blood vessel .
-
4.
Display your data as a percentage of the extravasated cells at a given time point per condition (i.e., particular cancer cell line mutant). Pull together data from several (at least five animals, 300 cells) animals per condition. As mentioned above it may be easier to use differentially labeled cancer cells (i.e., GFP and RFP). This approach provides an internal experiment “control” and decreases number of animals required (Fig. 2b, c and see Note 2 ).
4 Notes
-
1.
Cancer cells tend to aggregate in PBS within 1–2 h post-trypsinization and therefore should be prepared immediately before injection. Vital cell cytoplasm or membrane-staining dyes (such as CellTracker or CellMask ) tend to diffuse out of the cell within the required incubation times precluding the efficient imaging and should be avoided. Several human cancer cell lines such as LNCaP (prostate cancer) or Saos-2 (osteosarcoma) exhibited decreased survival rates; therefore pilot experiments to increase survival of the cell line used in the experiments may be required.
-
2.
Using differential cancer cell fluorescent labels helps to reduce animal numbers and the time required for each experiment. For example, control cells can be labeled with RFP while mutant tumor cells can be alternatively labeled with GFP. In this case each experiment has a built-in control that corrects for inter-embryo variability. However, careful attention must be paid to ensure equal cell injection and survival of the differentially labeled cells, and that one cell line does not influence the extravasation of the other.
-
3.
For confocal microscopy, we use a Nikon A1r MP confocal microscope. It is equipped with mercury arc lamp four diode-based lasers (405, 491, 561, 647 nm) and tunable (800–1300) Spectra Physics IR laser. For general embryo manipulation and cancer cell injection we use a Zeiss Lumar.V12 stereomicroscope. Less advanced microscope setups can be successfully used for the procedures described in this review. We encourage readers to contact the authors for more detailed recommendations.
-
4.
Depending on the cancer cell type, cells start to extravasate 2–8 h post-injection. Cancer cell extravasation follows a bell-shaped curve and with the majority of the cells leaving the circulation within 2–4 h after the initial extravasation. To correct for this variation, we recommend offsetting embryo injection and imaging for each condition. For example, if two conditions are being studied the chicken embryos should be injected (and imaged) in the following order: condition 1 (embryo 1) … condition 2 (embryo 1) … condition 1 (embryo 2) … condition 2 (embryo 2) … and so on.
-
5.
Chicken embryo CAM vessels mature rapidly between 12 and 14 days post-fertilization. Generally, cancer cell extravasation occurs sooner in younger (12–13 days) embryos (2–6 h) than in older (14 days) embryos (4–10 h). If significant (5×) fold difference in extravasation efficiency between cell lines used in the experiments is expected it may be more convenient to use younger embryos. Since older embryos possess more mature vasculature, 14-day-old embryos should be used to discriminate between cell lines with subtle differences in the extravasation efficiency .
References
Reymond N, d’Agua BB, Ridley AA (2013) Crossing the endothelial barrier during metastasis. Nat Rev Cancer 13:858–870
Sung BH, Ketova T, Hoshino D, Zijlstra A, Weaver AM (2015) Directional cell movement through tissues is controlled by exosome secretion. Nat Commun 6:7164
Leong HS, Robertson AE, Stoletov K, Leith SJ, Chin CA, Chien AE et al (2014) Invadopodia are required for cancer cell extravasation and are a therapeutic target for metastasis. Cell Rep 8:1558–1570
Kain KH, Miller JW, Jones-Paris CR, Thomason RT, Lewis JD, Bader DM et al (2014) The chick embryo as an expanding experimental model for cancer and cardiovascular research. Dev Dyn 243:216–228
Leong HS, Steinmetz NF, Ablack A, Destito G, Zijlstra A, Stuhlmann H et al (2010) Intravital imaging of embryonic and tumor neovasculature using viral nanoparticles. Nat Protoc 5:1406–1417
Zijlstra A, Lewis J, Degryse B, Stuhlmann H, Quigley JP (2008) The inhibition of tumor cell intravasation and subsequent metastasis via regulation of in vivo tumor cell motility by the tetraspanin CD151. Cancer Cell 13:221–234
Palmer TD, Lewis J, Zijlstra A (2011) Quantitative analysis of cancer metastasis using an avian embryo model. J Vis Exp 51:2815
Hanahan D, Weinberg RA (2000) The hallmarks of cancer. Cell 100:57–70
van’t Veer LJ, Dai H, van de Vijver MJ, He YD, Hart AA, Mao M et al (2002) Gene expression profiling predicts clinical outcome of breast cancer. Nature 415:530–536
Eccles SA, Welch DR (2007) Metastasis: recent discoveries and novel treatment strategies. Lancet 369:1742–1757
Weber GF (2008) Molecular mechanisms of metastasis. Cancer Lett 270:181–190
Fidler IJ (2001) Seed and soil revisited: contribution of the organ microenvironment to cancer metastasis. Surg Oncol Clin N Am 10:257–269
Chambers AF, Groom AC, MacDonald IC (2002) Dissemination and growth of cancer cells in metastatic sites. Nat Rev Cancer 2:563–572
Pantel K, Brakenhoff RH (2004) Dissecting the metastatic cascade. Nat Rev Cancer 4:448–456
Friedl P, Wolf K (2003) Tumour-cell invasion and migration: diversity and escape mechanisms. Nat Rev Cancer 3:362–374
Stoletov K, Lewis JD (2015) Invadopodia: a new therapeutic target to block cancer metastasis. Expert Rev Anticancer Ther 15:733–735
Leong HS, Chambers AF, Lewis JD (2012) Assessing cancer cell migration and metastatic growth in vivo in the chick embryo using fluorescence intravital imaging. Methods Mol Biol 872:1–14
Leighton J (1964) Invasion and metastasis of heterologous tumors in the chick embryo. Prog Exp Tumor Res 4:98–125
Locker J, Goldblatt PJ, Leighton J (1969) Hematogenous metastasis of Yoshida ascites Hepatoma in the chick embryo liver: ultrastructural changes in tumor cells. Cancer Res 29:1245–1253
McAllister RM, Peer M, Gilden RV, Landing BH (1974) Tumors formed by human rhabdomyosarcoma cells in chorioallantoic membrane of embryonated hens’ eggs. Int J Cancer 13:886–890
Chambers AF, Shafir R, Ling V (1982) A model system for studying metastasis using the embryonic chick. Cancer Res 42:4018–4025
Chambers AF, Wilson S (1985) Cells transformed with a ts viral src mutant are temperature sensitive for in vivo growth. Mol Cell Biol 5:728–733
Gordon JR, Quigley JP (1986) Early spontaneous metastasis in the human epidermoid carcinoma HEp3/chick embryo model: contribution of incidental colonization. Int J Cancer 38:437–444
Chambers AF, Schmidt EE, MacDonald IC, Morris VL, Groom AC (1992) Early steps in hematogenous metastasis of B16F1 melanoma cells in chick embryos studied by high-resolution intravital videomicroscopy. J Natl Cancer Inst 84:797–803
Quigley JP, Armstrong PB (1998) Tumor cell intravasation elucidated: the chick embryo opens the window. Cell 94:281–284
MacDonald IC, Schmidt EE, Morris VL, Chambers AF, Groom AC (1992) Intravital videomicroscopy of the chorioallantoic microcirculation: a model system for studying metastasis. Microvasc Res 44:185–199
Aguirre-Ghiso JA, Ossowski L, Rosenbaum SK (2004) Green fluorescent protein tagging of extracellular signal-regulated kinase and p38 pathways reveals novel dynamics of pathway activation during primary and metastatic growth. Cancer Res 64:7336–7345
Wilson SM, Chambers AF (2004) Experimental metastasis assays in the chick embryo. Curr Protoc Cell Biol Chapter 19:Unit 19 6
Pink DB, Schulte W, Parseghian MH, Zijlstra A, Lewis JD (2012) Real-time visualization and quantitation of vascular permeability in vivo: implications for drug delivery. PLoS One 7:e33760
Cho CF, Ablack A, Leong HS, Zijlstra A, Lewis JD (2011) Evaluation of nanoparticle uptake in tumors in real time using intravital imaging. J Vis Exp 52:2808
Deryugina EI, Quigley JP (2008) Chick embryo chorioallantoic membrane model systems to study and visualize human tumor cell metastasis. Histochem Cell Biol 130:1119–1130
Chishima T, Miyagi Y, Wang X, Yamaoka H, Shimada H, Moossa AR, Hoffman RM (1997) Cancer invasion and micrometastasis visualized in live tissue by green fluorescent protein expression. Cancer Res 57:2042–2047
Naumov GN, Wilson SM, MacDonald IC, Schmidt EE, Morris VL, Groom AC et al (1999) Cellular expression of green fluorescent protein, coupled with high-resolution in vivo videomicroscopy, to monitor steps in tumor metastasis. J Cell Sci 112:1835–1842
Lewis JD, Destito G, Zijlstra A, Gonzalez MJ, Quigley JP, Manchester M et al (2006) Viral nanoparticles as tools for intravital vascular imaging. Nat Med 12:354–360
Sahai E (2007) Illuminating the metastatic process. Nat Rev Cancer 7:737–749
Hoffman RM (2009) Imaging cancer dynamics in vivo at the tumor and cellular level with fluorescent proteins. Clin Exp Metastasis 26:345–355
Hoffman RM (2005) The multiple uses of fluorescent proteins to visualize cancer in vivo. Nat Rev Cancer 5:796–806
Jilani SM, Murphy TJ, Thai SNM, Eichmann A, Alva JA, Irula-Arispe ML (2003) Selective binding of lectins to embryonic chicken vasculature. J Histochem Cytochem 51:597–604
Welch DR (1997) Technical considerations for studying cancer metastasis in vivo. Clin Exp Metastasis 15:272–306
Acknowledgments
This work was supported by Canadian Cancer Society Research Institute Grant #702849 to J.D.L. and K.S. L.W. and D.B. hold US Department of Defense Prostate Cancer Research Program Postdoctoral Training Awards. D.B. also holds an Alberta Innovates Health Solutions PDF Award. Dr. Lewis holds the Frank and Carla Sojonky Chair in Prostate Cancer Research supported by the Alberta Cancer Foundation. All experiments were performed in accordance with the regulations and guidelines of the Institutional Animal Care and Use Committee at the University of Alberta. We thank Desmond Pink for his photography.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Science+Business Media New York
About this protocol
Cite this protocol
Willetts, L., Bond, D., Stoletov, K., Lewis, J.D. (2016). Quantitative Analysis of Human Cancer Cell Extravasation Using Intravital Imaging. In: Ursini-Siegel, J., Beauchemin, N. (eds) The Tumor Microenvironment. Methods in Molecular Biology, vol 1458. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4939-3801-8_3
Download citation
DOI: https://doi.org/10.1007/978-1-4939-3801-8_3
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4939-3799-8
Online ISBN: 978-1-4939-3801-8
eBook Packages: Springer Protocols